Waterpipe Use among Adolescents in Germany: Prevalence, Associated Consumer Characteristics, and Trends (German Health Interview and Examination Survey for Children and Adolescents, KiGGS)
Abstract
1. Introduction
2. Materials and Methods
2.1. Methods
2.2. Measurements
2.3. Statistical Analyses
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- WHO Study Group on Tobacco Product Regulation (TobReg). Advisory Note: Water-Pipe Tobacco Smoking: Health Effects, Research Needs and Recommended Actions by Regulators. 2015. Available online: https://www.who.int/tobacco/publications/prod_regulation/waterpipesecondedition/en/ (accessed on 3 January 2020).
- Rastam, S.; Ward, K.D.; Eissenberg, T.; Maziak, W. Estimating the beginning of the waterpipe epidemic in Syria. BMC Public Health 2004, 4, 32. [Google Scholar] [CrossRef] [PubMed]
- Maziak, W.; Taleb, Z.B.; Bahelah, R.; Islam, F.; Jaber, R.; Auf, R.; Salloum, R.G. The global epidemiology of waterpipe smoking. Tob. Control 2015, 24, i3–i12. [Google Scholar] [CrossRef] [PubMed]
- Maziak, W.; Ward, K.D.; Afifi Soweid, R.A.; Eissenberg, T. Tobacco smoking using a waterpipe: A re-emerging strain in a global epidemic. Tob. Control 2004, 13, 327–333. [Google Scholar] [CrossRef] [PubMed]
- German Cancer Research Centre (DKFZ). Waterpipes. Facts about Smoking. [Deutsches Krebsforschungszentrum Wasserpfeifen. Fakten zum Rauchen]. 2018. Available online: https://www.dkfz.de/de/tabakkontrolle/download/Publikationen/FzR/FzR_2018_Wasserpfeifen.pdf (accessed on 12 February 2020).
- Federal Institute for Risk Assessment (BfR). Tobacco-Free Waterpipes Can also Be a Health Hazard [Auch Tabakfreie Wasserpfeifen Können die Gesundheit Gefährden]; Statement 034/2016 of the BfR of 29 November 2016; Federal Institute for Risk Assessment (BfR): Berlin, Germany, 2016. [Google Scholar] [CrossRef]
- Federal Government Commissioner. Report on Drugs and Addiction 2019 [Drogenbeauftrage der Bundesregierung Drogen- und Suchtbericht 2019]; Federal Ministry of Health: Berlin, Germany, 2019; pp. 33–51. [Google Scholar]
- Schwarzer, M.; Thomas, J.; Nedela-Morales, M.; Kaltenbach, M.; Herrmann, E.; Groneberg, D. Self-assessment of adolescents regarding water pipe consumption. Psychiatr. Prax. 2015, 42, 47–49. [Google Scholar] [CrossRef] [PubMed]
- Ali, M.; Jawad, M. Health effects of waterpipe tobacco use: Getting the public health message just right. Tob. Use Insights 2017. [Google Scholar] [CrossRef]
- Roditis, M.; Delucchi, K.; Cash, D.; Halpern-Felsher, B. Adolescents’ perceptions of health risks, social risks, and benefits differ across tobacco products. J. Adolesc. Health 2016, 58, 558–566. [Google Scholar] [CrossRef]
- Akl, E.A.; Jawad, M.; Lam, W.Y.; Co, C.N.; Obeid, R.; Irani, J. Motives, beliefs and attitudes towards waterpipe tobacco smoking: A systematic review. Harm Reduct. J. 2013, 10, 12. [Google Scholar] [CrossRef]
- Cobb, C.; Ward, K.D.; Maziak, W.; Shihadeh, A.L.; Eissenberg, T. Waterpipe tobacco smoking: An emerging health crisis in the United States. Am. J. Health Behav. 2010, 34, 275–285. [Google Scholar] [CrossRef]
- Kowitt, S.D.; Goldstein, A.O.; Sutfin, E.L.; Osman, A.; Meernik, C.; Heck, C.; Ranney, L.M. Adolescents’ first tobacco products: Associations with current multiple tobacco product use. PLoS ONE 2019, 14, e0217244. [Google Scholar] [CrossRef]
- Lampert, T.; Kuntz, B. Tobacco and alcohol consumption among 11- to 17-year-old adolescents: Results of the KiGGS study: First follow-up (KiGGS Wave 1) [Tabak- und Alkoholkonsum bei 11- bis 17-jährigen Jugendlichen: Ergebnisse der KiGGS Studie—Erste Folgebefragung (KiGGS Welle 1)]. Bundesgesundheitsblatt-Gesundh. Gesundh. 2014, 57, 830–839. [Google Scholar] [CrossRef][Green Version]
- Jawad, M.; Charide, R.; Waziry, R.; Darzi, A.; Ballout, R.A.; Akl, E.A. The prevalence and trends of waterpipe tobacco smoking: A systematic review. PLoS ONE 2018, 13, e0192191. [Google Scholar] [CrossRef]
- Kuntz, B.; Lampert, T.; KiGGS Study Group. Waterpipe (shisha) smoking among adolescents in Germany: Results of the KiGGS study: First follow-up (KiGGS Wave 1). [Wasserpfeifenkonsum (Shisha-Rauchen) bei Jugendlichen in Deutschland: Ergebnisse der KiGGS-Studie—Erste Folgebefragung (KiGGS Welle 1)]. Bundesgesundheitsblatt-Gesundh. Gesundh. 2015, 58, 467–473. [Google Scholar] [CrossRef]
- Soneji, S.; Sargent, J.D.; Tanski, S.E.; Primack, B.A. Associations between initial water pipe tobacco smoking and snus use and subsequent cigarette smoking: Results from a longitudinal study of US adolescents and young adults. JAMA Pediatr. 2015, 169, 129–136. [Google Scholar] [CrossRef] [PubMed]
- Bahelah, R.; Ward, K.D.; Ben Taleb, Z.; DiFranza, J.R.; Eissenberg, T.; Jaber, R.; Maziak, W. Determinants of progression of nicotine dependence symptoms in adolescent waterpipe smokers. Tob. Control 2019, 28, 254–260. [Google Scholar] [CrossRef]
- Ben Taleb, Z.; Breland, A.; Bahelah, R.; Kalan, M.E.; Vargas-Rivera, M.; Jaber, R.; Eissenberg, T.; Maziak, W. Flavored versus nonflavored waterpipe tobacco: A comparison of toxicant exposure, puff topography, subjective experiences, and harm perceptions. Nicotine Tob. Res. 2019, 21, 1213–1219. [Google Scholar] [CrossRef]
- Nutt, D.; King, L.A.; Saulsbury, W.; Blakemore, C. Development of a rational scale to assess the harm of drugs of potential misuse. Lancet 2007, 369, 1047–1053. [Google Scholar] [CrossRef]
- Hauser, C.D.; Mailig, R.; Stadtler, H.; Reed, J.; Chen, S.; Uffman, E.; Bernd, K. Waterpipe tobacco smoke toxicity: The impact of waterpipe size. Tob. Control 2020, 29 (Suppl. 2), 90–94. [Google Scholar] [CrossRef]
- Rezk-Hanna, M.; Mosenifar, Z.; Benowitz, N.L.; Rader, F.; Rashid, M.; Davoren, K.; Moy, N.B.; Doering, L.; Robbins, W.; Sarna, L.; et al. High carbon monoxide levels from charcoal combustion mask acute endothelial dysfunction induced by hookah (waterpipe) smoking in young adults. Circulation 2019, 139, 2215–2224. [Google Scholar] [CrossRef]
- Haddad, L.; Kelly, D.L.; Weglicki, L.S.; Barnett, T.E.; Ferrell, A.V.; Ghadban, R. A systematic review of effects of waterpipe smoking on cardiovascular and respiratory health outcomes. Tob. Use Insights 2016, 9, 13–28. [Google Scholar] [CrossRef]
- Rezk-Hanna, M.; Benowitz, N.L. Cardiovascular effects of hookah smoking: Potential implications for cardiovascular risk. Nicotine Tob. Res. 2018, 21, 1151–1161. [Google Scholar] [CrossRef]
- Toukan, Y.; Hakim, F.; Bentur, Y.; Aharon-Peretz, J.; Elemy, A.; Gur, M.; Hanna, M.; Fisher, T.; Scherb, I.; Bentur, L. The effect of a 30-minute water-pipe smoking session on cognitive measures and cardio-pulmonary parameters. Nicotine Tob. Res. 2019, 22, 1347–1353. [Google Scholar] [CrossRef] [PubMed]
- Waziry, R.; Jawad, M.; Ballout, R.A.; Al Akel, M.; Akl, E.A. The effects of waterpipe tobacco smoking on health outcomes: An updated systematic review and meta-analysis. Int. J. Epidemiol. 2017, 46, 32–43. [Google Scholar] [CrossRef]
- Martinasek, M.; Rivera, Z.; Ferrer, A.; Freundt, E. A pilot study to assess the bacterial contaminants in hookah pipes in a community setting. Int. J. Tuberc. Lung Dis. 2018, 22, 579–584. [Google Scholar] [CrossRef] [PubMed]
- Federal Statistical Office (Destatis). Press Release No. 16 of 15 January 2020 [Statistisches Bundesamt (Destatis) Pressemitteilung Nr. 16 vom 15. Januar 2020]. Available online: https://www.destatis.de/DE/Presse/Pressemitteilungen/2020/01/PD20_016_799.html (accessed on 2 April 2020).
- Kotecha, S.; Jawad, M.; Iliffe, S. Knowledge, attitudes and beliefs towards waterpipe tobacco smoking and electronic shisha (e-shisha) among young adults in London: A qualitative analysis. Prim. Health Care Res. Dev. 2016, 17, 166–174. [Google Scholar] [CrossRef] [PubMed]
- Orth, B.; Merkel, C. The Drug Affinity of Young People in the Federal Republic of Germany 2019. Smoking, Alcohol Consumption and Use of Illegal Drugs: Current Distribution and Trends [Die Drogenaffinität Jugendlicher in der Bundesrepublik Deutschland 2019. Rauchen, Alkoholkonsum und Konsum illegaler Drogen: Aktuelle Verbreitung und Trends]; BZgA-Forschungsbericht: Cologne, Germany, 2020. [Google Scholar] [CrossRef]
- DAK. DAK-Präventionsradar 2017/2018; DAK: Hamburg, Germany, 2018. [Google Scholar]
- Isensee, B.; Goecke, M.; Hanewinkel, R. Cigarette, shisha, e-cigarette and tobacco heater: Frequency and pattern of consumption of different nicotine products in adolescence [Zigarette, Shisha, E-Zigarette und Tabakerhitzer: Häufigkeit und Muster des Konsums unterschiedlicher Nikotinprodukte im Jugendalter]. Suchtmedizin 2018, 20, 306–314. [Google Scholar]
- Jawad, M.; Lee, J.T.; Millett, C. Waterpipe tobacco smoking prevalence and correlates in 25 Eastern Mediterranean and Eastern European countries: Cross-sectional analysis of the Global Youth Tobacco Survey. Nicotine Tob. Res. 2015, 18, 395–402. [Google Scholar] [CrossRef] [PubMed]
- Cooper, M.; Pacek, L.R.; Guy, M.C.; Barrington-Trimis, J.L.; Simon, P.; Stanton, C.; Kong, G. Hookah use among US youth: A systematic review of the literature from 2009 to 2017. Nicotine Tob. Res. 2019, 21, 1590–1599. [Google Scholar] [CrossRef] [PubMed]
- Hoffmann, R.; Lange, M.; Butschalowsky, H.; Houben, R.; Schmich, P.; Allen, J.; Kuhnert, R.; Schaffrath Rosario, A.; Gößwald, A. KiGGS Wave 2 cross-sectional study—Participant acquisition, response rates and representativeness. J. Health Monit. 2018, 3, 78–91. [Google Scholar] [CrossRef]
- Frank, L.; Yesil-Jürgens, R.; Born, S.; Hoffmann, R.; Santos-Hövener, C.; Lampert, T. Improving the inclusion and participation of children and adolescents with a migration background in KiGGS Wave 2. J. Health Monit. 2018, 3, 126–142. [Google Scholar] [CrossRef]
- Kamtsiuris, P.; Lange, M.; Rosario, A.S. The German Health Interview and Examination Survey for Children and Adolescents (KiGGS): Sample design, response and nonresponse analysis [Der Kinder- und Jugendgesundheitssurvey (KiGGS): Stichprobendesign, Response und Nonresponse-Analyse]. Bundesgesundheitsblatt-Gesundh. Gesundh. 2007, 50, 547–556. [Google Scholar] [CrossRef]
- Lange, M.; Butschalowsky, H.; Jentsch, F.; Kuhnert, R.; Rosario, A.S.; Schlaud, M.; Kamtsiuris, P. The first KiGGS follow-up (KiGGS Wave 1): Study conduct, sample design, and response [Die erste KiGGS-Folgebefragung (KiGGS Welle 1): Studiendurchführung, Stichprobendesign und Response]. Bundesgesundheitsblatt-Gesundh. Gesundh. 2014, 57, 747–761. [Google Scholar] [CrossRef]
- Mauz, E.; Gößwald, A.; Kamtsiuris, P.; Hoffmann, R.; Lange, M.; von Schenk, U.; Allen, J.; Butschalowsky, H.; Frank, L.; Hölling, H.; et al. New data for action. Data collection for KiGGS Wave 2 has been completed. J. Health Monit. 2017, 2, 2–27. [Google Scholar] [CrossRef]
- Lampert, T.; Hoebel, J.; Kuntz, B.; Müters, S.; Kroll, L.E. Socioeconomic status and subjective social status measurement in KiGGS Wave 2. J. Health Monit. 2018, 3, 108–125. [Google Scholar]
- Kuntz, B.; Waldhauer, J.; Moor, I.; Rathmann, K.; Richter, M.; Orth, B.; Piontek, D.; Kraus, L.; Zeiher, J.; Lampert, T. Trends in educational inequalities in smoking among adolescents in Germany: Evidence from four population-based studies. Bundesgesundheitsblatt-Gesundh. Gesundh. 2018, 61, 7–19. [Google Scholar] [CrossRef]
- Schenk, L.; Neuhauser, H.; Ellert, U.; Poethko-Müller, C.; Kleiser, C.; Mensink, G. German Health Interview and Examination Survey for Children and Adolescents (KiGGS 2003–2006): Children and Young People with a Migration Background in Germany [Kinder- und Jugendgesundheitssurvey (KiGGS 2003–2006): Kinder und Jugendliche mit Migrationshintergrund in Deutschland]; Robert Koch-Institut: Berlin, Germany, 2008; p. 129. [Google Scholar]
- Orth, B. The Drug Affinity of Young People in the Federal Republic of Germany 2015. Smoking, Alcohol Consumption and Use of Illegal Drugs: Current Prevalence and Trends [Die Drogenaffinität Jugendlicher in der Bundesrepublik Deutschland 2015. Rauchen, Alkoholkonsum und Konsum illegaler Drogen: Aktuelle Verbreitung und Trends]; BZgA-Forschungsbericht; Bundeszentrale für gesundheitliche Aufklärung: Cologne, Germany, 2016. [Google Scholar]
- Hojni, M.; Delcour, J.; Strizek, J.; Uhl, A. ESPAD Österreich. European School Survey Project on Alcohol and other Drugs. Band 1: Forschungsbericht. Gesundheit; Gesundheit Österreich GmbH: Wien, Austria, 2019. [Google Scholar]
- Kraus, L.; Piontek, D.; Seitz, N.N.; Schoeppe, M. European School Survey Project on Alcohol and other Drugs 2015 (ESPAD): Survey of 9th and 10th Grade Students in Bavaria [Europäische Schülerstudie zu Alkohol und anderen Drogen 2015 (ESPAD): Befragung von Schülerinnen und Schülern der 9. und 10. in Bayern]; Institut für Therapieforschung (IFT): München, Germany, 2016. [Google Scholar]
- Maziak, W.; Ben Taleb, Z.; Jawad, M.; Afifi, R.; Nakkash, R.; Akl, E.A.; Ward, K.D.; Salloum, R.G.; Barnett, T.E.; Primack, B.A.; et al. Expert Panel on Waterpipe Assessment in Epidemiological, Studies. Consensus statement on assessment of waterpipe smoking in epidemiological studies. Tob. Control 2017, 26, 338–343. [Google Scholar] [CrossRef]
- Azagba, S.; Latham, K.; Shan, L. Waterpipe tobacco smoking trends among middle and high school students in the United States from 2011 to 2017. Drug Alcohol Depend. 2019, 200, 19–25. [Google Scholar] [CrossRef]
- Kuntz, B.; Lampert, T. “Smoke on the water“—Wasserpfeifenkonsum bei Jugendlichen in Deutschland (Ergebnisse aus KiGGS Welle 1). Umw. Mensch Inf. 2016, 2016, 18–25. [Google Scholar]
- Lampert, T.; Burger, M. Distribution and patterns of tobacco consumption in Germany [Verbreitung und Strukturen des Tabakkonsums in Deutschland]. Bundesgesundheitsblatt-Gesundh. Gesundh. 2005, 48, 1231–1241. [Google Scholar]
- Orth, B.; Merkel, C. The decline in cigarette consumption by adolescents and young adults in Germany and the increasing importance of hookahs, e-cigarettes and e-shishas [Der Rückgang des Zigarettenkonsums Jugendlicher und junger Erwachsener in Deutschland und die zunehmende Bedeutung von Wasserpfeifen, E-Zigaretten und E-Shishas]. Bundesgesundheitsblatt-Gesundh. Gesundh. 2018, 61, 1377–1387. [Google Scholar] [CrossRef]
- Häder, M. Erhebungsmethoden. In Empirische Sozialforschung; VS Verlag für Sozialwissenschaften: Berlin, Germany, 2010; pp. 187–337. [Google Scholar] [CrossRef]
| Characteristics | Current WP User ♦ n = 446 | Last 12-Month WP User n = 1101 | Ever WP User n = 1415 | |||
|---|---|---|---|---|---|---|
| % | 95% CI | % | 95% CI | % | 95% CI | |
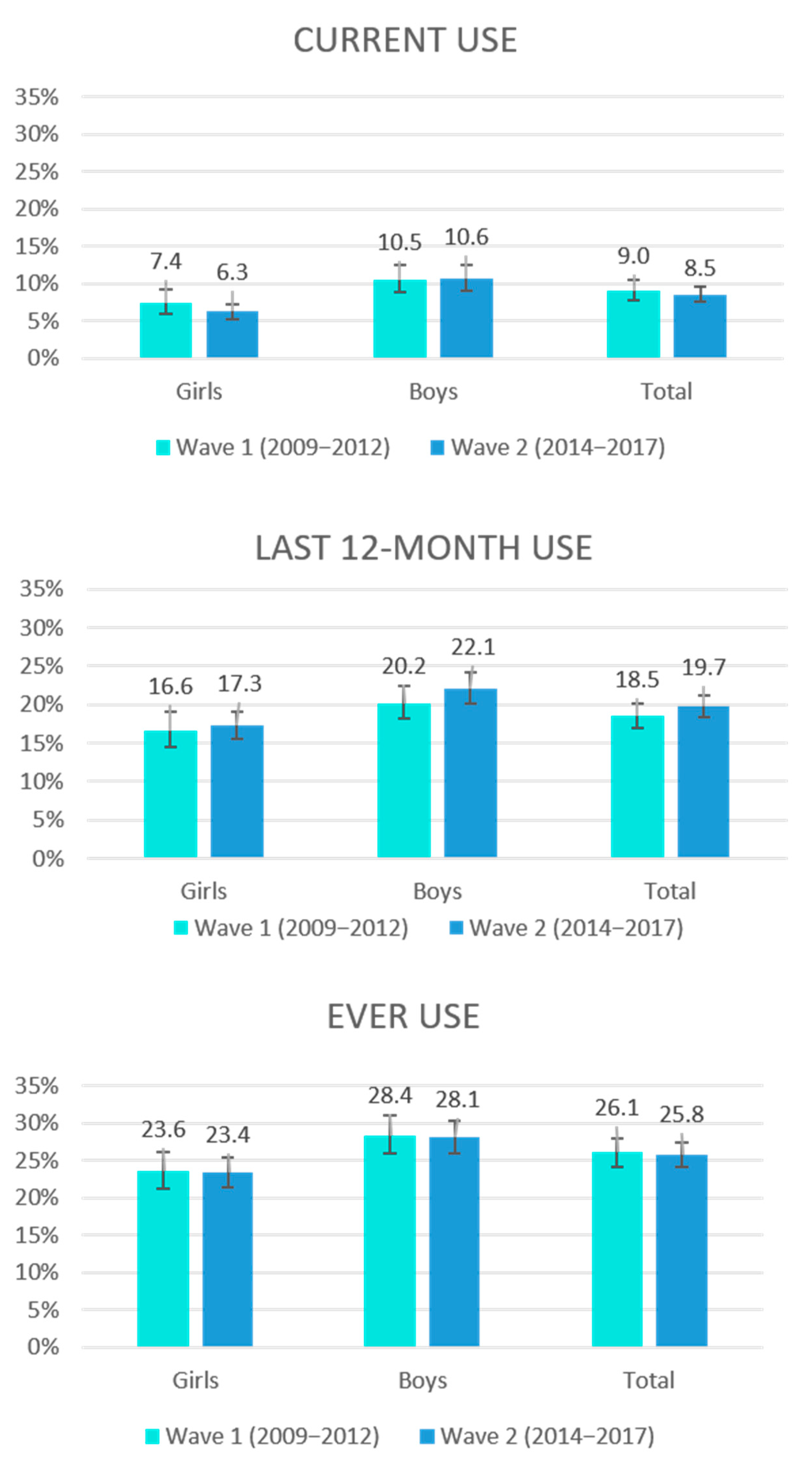
| Total (Girls and Boys) | 8.5 | (7.5–9.6) | 19.7 | (18.3–21.2) | 25.8 | (24.2–27.5) |
| Girls | 6.3 | (5.3–7.3) | 17.3 | (15.6–19.1) | 23.4 | (21.4–25.5) |
| Age, years | ||||||
| 11 | − | − | 0.1 | (0.0–0.7) | 0.7 | (0.2–3.0) |
| 12 | 0.6 | (0.1–3.2) | 1.5 | (0.6–3.5) | 3.7 | (2.0–6.8) |
| 13 | 0.7 | (0.3–1.5) | 6.3 | (3.9–9.9) | 8.7 | (5.7–12.9) |
| 14 | 6.1 | (3.9–9.4) | 15.5 | (12.1–19.7) | 18.9 | (14.9–23.6) |
| 15 | 9.5 | (6.6–13.5) | 22.1 | (17.4–27.6) | 28.3 | (22.9–34.4) |
| 16 | 12.1 | (8.9–16.2) | 36.6 | (31.1–42.5) | 46.1 | (40.1–52.3) |
| 17 | 12.9 | (9.6–17.1) | 33.8 | (28.2–40.0) | 50.6 | (44.2–56.9) |
| Socioeconomic status * | ||||||
| Low | 7.0 | (4.5–10.8) | 20.5 | (16.2–25.5) | 30.2 | (25.0–36.0) |
| Middle | 6.8 | (5.6–8.2) | 17.4 | (15.4–19.6) | 23.1 | (20.6–25.7) |
| High | 4.1 | (2.6–6.2) | 12.9 | (10.0–16.5) | 16.2 | (13.0–20.1) |
| Education ≠ | ||||||
| Secondary/Middle/Comprehensive school | 6.6 | (5.1–8.4) | 18.8 | (16.4–21.5) | 25.1 | (22.1–28.3) |
| Technical/Academic secondary school | 5.9 | (4.6–7.5) | 15.5 | (13.4–18.0) | 21.5 | (18.9–24.3) |
| Migration background ° | ||||||
| Yes, one-sided | 6.7 | (3.8–11.6) | 19.0 | (14.0–25.3) | 23.1 | (17.5–29.8) |
| Yes, both-sided | 3.7 | (2.0–6.8) | 11.2 | (7.8–15.8) | 18.1 | (13.6–23.7) |
| No | 6.8 | (5.7–7.9) | 18.4 | (16.5–20.5) | 24.7 | (22.5–26.9) |
| Current smoking status | ||||||
| Smoker | 35.1 | (28.0–42.9) | 73.8 | (64.9–81.1) | 86.3 | (77.6–92.0) |
| Non-smoker | 4.2 | (3.3–5.2) | 13.2 | (11.5–15.0) | 18.9 | (17.0–21.1) |
| Boys | 10.6 | (9.1–12.4) | 22.1 | (20.2–24.2) | 28.1 | (25.9–30.3) |
| Age, years | ||||||
| 11 | − | 1.7 | (0.7–4.2) | 2.0 | (0.9–4.4) | |
| 12 | 0.5 | (0.2–1.6) | 2.4 | (1.2–4.5) | 3.1 | (1.7–5.5) |
| 13 | 3.9 | (1.8–8.1) | 8.2 | (5.3–12.4) | 12.0 | (8.6–16.5) |
| 14 | 5.7 | (3.4–9.5) | 17.6 | (13.6–22.5) | 22.4 | (17.8–27.7) |
| 15 | 12.4 | (8.7–17.2) | 29.8 | (24.1–36.3) | 38.3 | (32.0–45.0) |
| 16 | 21.5 | (15.4–29.1) | 37.9 | (31.0–45.3) | 47.9 | (41.4–54.5) |
| 17 | 26.4 | (20.9–32.8) | 50.3 | (43.5–57.2) | 61.6 | (54.9–67.9) |
| Socioeconomic status * | ||||||
| Low | 11.6 | (7.1–18.3) | 22.5 | (16.7–29.6) | 28.2 | (21.7–35.6) |
| Middle | 10.5 | (8.7–12.6) | 22.9 | (20.4–25.6) | 29.1 | (26.3–32.2) |
| High | 10.7 | (8.0–14.2) | 19.1 | (15.9–22.9) | 24.1 | (20.6–28.0) |
| Education ≠ | ||||||
| Secondary/Middle/Comprehensive school | 9.8 | (7.6–12.5) | 21.1 | (18.3–24.1) | 27.2 | (23.8–30.9) |
| Technical/Academic secondary school | 10.4 | (8.1–13.1) | 21.9 | (18.6–25.5) | 27.5 | (24.4–30.8) |
| Migration background ° | ||||||
| Yes, one-sided | 17.9 | (11.0–27.8) | 30.4 | (22.4–39.9) | 36.3 | (27.9–45.7) |
| Yes, both-sided | 11.5 | (7.2–17.8) | 19.9 | (14.2–27.1) | 27.9 | (21.5–35.4) |
| No | 9.7 | (8.2–11.4) | 21.7 | (19.6–23.9) | 27.2 | (24.9–29.6) |
| Current smoking status | ||||||
| Smoker | 46.8 | (37.2–56.7) | 84.5 | (75.4–90.7) | 93.5 | (87.5–96.7) |
| Non-smoker | 8.2 | (6.7–10.0) | 18.1 | (16.2–20.2) | 23.7 | (21.5–26.1) |
| Covariates † | OR (95% CI) | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Model (I) Current WP Use ♦ vs. Never WP Use | Model (II) Last 12-Month WP Use vs. Never WP Use | Model (III) Ever WP Use vs. Never WP Use | ||||||||||
| Girls | Boys | Girls | Boys | Girls | Boys | |||||||
| Age, Years > | 1.97 *** | (1.69–2.29) | 2.20 *** | (1.92–2.52) | 1.94 *** | (1.77–2.14) | 1.92 *** | (1.74–2.13) | 1.91 *** | (1.75–2.08) | 1.91 *** | (1.74–2.10) |
| Socioeconomic status ‡ | ||||||||||||
| Low | 1.60 | (0.71–3.58) | 0.72 | (0.31–1.70) | 1.27 | (0.74–2.17) | 0.95 | (0.53–1.69) | 1.66 * | (1.02–2.71) | 0.92 | (0.54–1.57) |
| Middle | 1.13 | (0.59–2.18) | 0.76 | (0.45–1.28) | 0.99 | (0.66–1.48) | 1.06 | (0.73–1.55) | 1.13 | (0.79–1.61) | 1.10 | (0.77–1.58) |
| High (ref) | 1 | 1 | 1 | 1 | 1 | 1 | ||||||
| Education ≠ | ||||||||||||
| Secondary/Middle/Comprehensive school | 1.56 | (1.00–2.45) | 1.48 | (0.91–2.41) | 1.82 *** | (1.32–2.51) | 1.27 | (0.90–1.78) | 1.63 ** | (1.22–2.17) | 1.28 | (0.95–1.72) |
| Technical/Academic secondary school (ref) | 1 | 1 | 1 | 1 | 1 | 1 | ||||||
| Migration background ° | ||||||||||||
| Yes, one-sided | 0.98 | (0.43–2.23) | 3.03 ** | (1.36–6.77) | 0.91 | (0.50–1.65) | 2.04 * | (1.18–3.54) | 0.79 | (0.46–1.33) | 2.01 ** | (1.23–3.27) |
| Yes, both-sided | 0.34 * | (0.15–0.80) | 1.19 | (0.55–2.61) | 0.38 *** | (0.22–0.65) | 0.87 | (0.49–1.55) | 0.44 *** | (0.27–0.70) | 0.90 | (0.56–1.46) |
| No (ref) | 1 | 1 | 1 | 1 | 1 | 1 | ||||||
| Current smoking status | ||||||||||||
| Smoker | 48.27 *** | (24.12–96.59) | 67.57 *** | (18.02–253.32) | 28.03 *** | (14.26–55.08) | 40.60 *** | (15.38–107.13) | 21.55 *** | (10.99–42.28) | 33.45 *** | (13.10–85.40) |
| Non-smoker (ref) | 1 | 1 | 1 | 1 | 1 | 1 | ||||||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Klosterhalfen, S.; Kotz, D.; Kuntz, B.; Zeiher, J.; Starker, A. Waterpipe Use among Adolescents in Germany: Prevalence, Associated Consumer Characteristics, and Trends (German Health Interview and Examination Survey for Children and Adolescents, KiGGS). Int. J. Environ. Res. Public Health 2020, 17, 7740. https://doi.org/10.3390/ijerph17217740
Klosterhalfen S, Kotz D, Kuntz B, Zeiher J, Starker A. Waterpipe Use among Adolescents in Germany: Prevalence, Associated Consumer Characteristics, and Trends (German Health Interview and Examination Survey for Children and Adolescents, KiGGS). International Journal of Environmental Research and Public Health. 2020; 17(21):7740. https://doi.org/10.3390/ijerph17217740
Chicago/Turabian StyleKlosterhalfen, Stephanie, Daniel Kotz, Benjamin Kuntz, Johannes Zeiher, and Anne Starker. 2020. "Waterpipe Use among Adolescents in Germany: Prevalence, Associated Consumer Characteristics, and Trends (German Health Interview and Examination Survey for Children and Adolescents, KiGGS)" International Journal of Environmental Research and Public Health 17, no. 21: 7740. https://doi.org/10.3390/ijerph17217740
APA StyleKlosterhalfen, S., Kotz, D., Kuntz, B., Zeiher, J., & Starker, A. (2020). Waterpipe Use among Adolescents in Germany: Prevalence, Associated Consumer Characteristics, and Trends (German Health Interview and Examination Survey for Children and Adolescents, KiGGS). International Journal of Environmental Research and Public Health, 17(21), 7740. https://doi.org/10.3390/ijerph17217740





