Prevalence of Stress in Healthcare Professionals during the COVID-19 Pandemic in Northeast Mexico: A Remote, Fast Survey Evaluation, Using an Adapted COVID-19 Stress Scales
Abstract
1. Introduction
Psychological Impact on Healthcare Workers
2. Materials and Methods
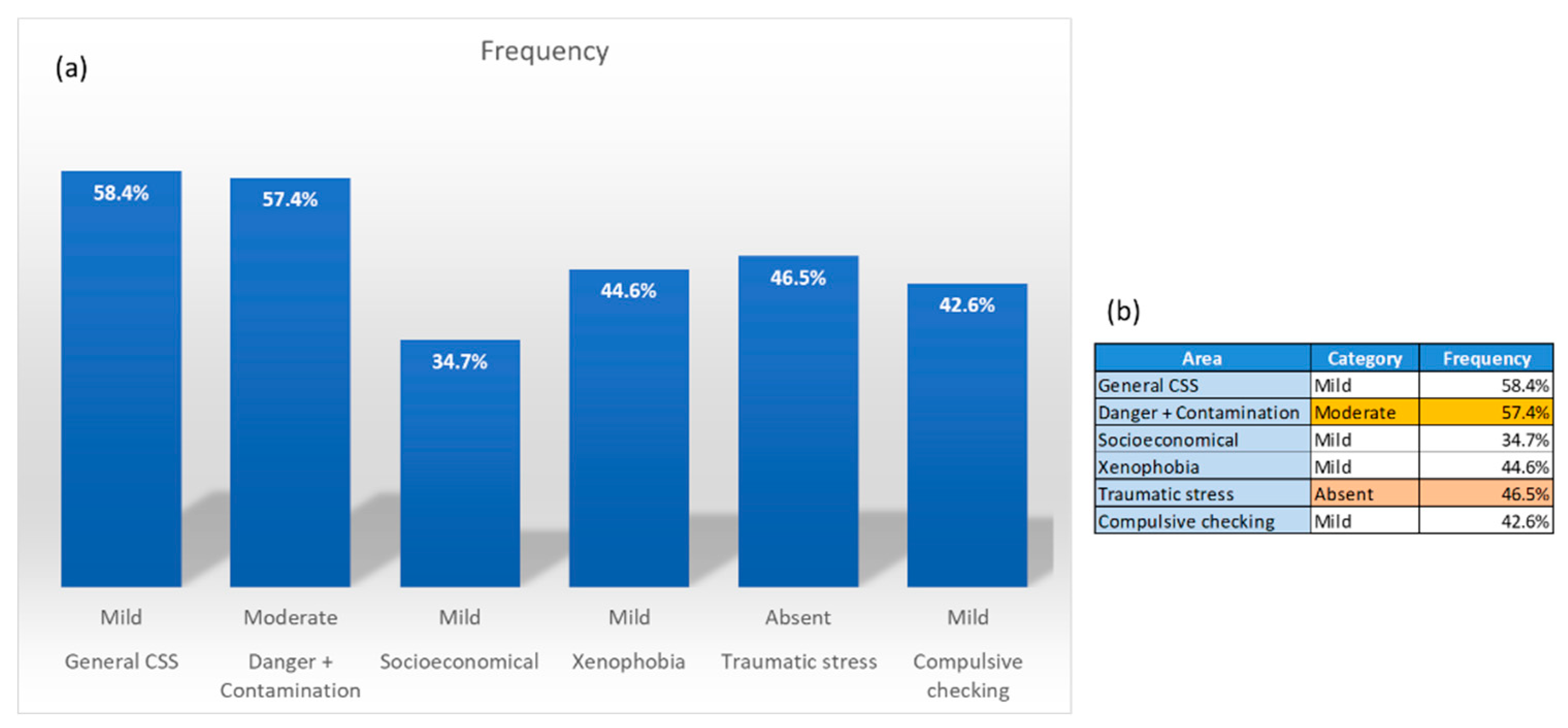
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- McDonnell, P.J. For the First Time, Mexico Records More COVID-19 Deaths in a Day than the U.S. L.A. Times. 4 June 2020. Available online: https://www.latimes.com/world-nation/story/2020-06-04/mexico-tops-1-000-deaths-in-one-day-this-is-not-new-york-president-says (accessed on 2 August 2020).
- Sohrabi, C.; Alsafi, Z.; O’Neill, N.; Khan, M.; Kerwan, A. World Health Organization declares global emergency: A review of the 2019 novel coronavirus (COVID-19). Int. J. Surg. 2020, 76, 71–76. [Google Scholar] [CrossRef] [PubMed]
- Sharif, A.; Aloui, C.; Yarovaya, L. COVID-19 pandemic, oil prices, stock market, geopolitical risk and policy uncertainty nexus in the U.S. economy: Fresh evidence from the waveletbased approach. Int. Rev. Financ. Anal. 2020, 70, 101496. [Google Scholar] [CrossRef]
- Sesagiri Raamkumar, A.; Tan, S.G.; Wee, H.-L. Measuring the Outreach Efforts of Public Health Authorities and the Public Response on Facebook during the COVID-19 Pandemic in Early 2020: A Cross-Country Comparison (Preprint). J. Med. Internet Res. 2020, 22, e19334. [Google Scholar] [CrossRef]
- Petzold, M.B.; Plag, J.; Ströhle, A. Dealing with psychological distress by healthcare professionals during the COVID-19 pandemia. Nervenarzt 2020, 91, 417–421. [Google Scholar] [CrossRef] [PubMed]
- Dubey, S.; Biswas, P.; Ghosh, R.; Chatterjee, S.; Dubey, J.M.; Chatterjee, S.; Lahiri, D.; Lavie, C.J. Psychosocial impact of COVID-19. Diabetes Metab. Syndr. Clin. Res. Rev. 2020, 14, 779–788. [Google Scholar] [CrossRef] [PubMed]
- WHO. WHO Announces COVID-19 Outbreak a Pandemic. Available online: http://www.euro.who.int/en/health-topics/health-emergencies/coronavirus-covid-19/news/news/2020/3/who-announces-covid-19-outbreak-a-pandemic (accessed on 10 August 2020).
- Welfens, P.J.J. Macroeconomic and health care aspects of the coronavirus epidemic: EU, U.S. and global perspectives. Int. Econ. Econ. Policy 2020, 17, 1–68. [Google Scholar] [CrossRef]
- El-Erianl, M.A. COVID-19: What Are the Biggest Concerns for the Developing World? 2020. World Economic Forum Web Site. Available online: https://www.weforum.org/agenda/2020/04/developing-world-covid19 (accessed on 12 August 2020).
- León-Cortés, J.L.; Leal Fernández, G.; Sánchez-Pérez, H.J. Health reform in Mexico: Governance and potential outcomes. Int. J. Equity Health 2019, 18, 1–6. [Google Scholar] [CrossRef]
- Doubova, S.V.; García-Saisó, S.; Pérez-Cuevas, R.; Sarabia-González, O.; Pacheco-Estrello, P.; Leslie, H.H.; Santamaría, C.; Torres-Arreola, L.D.P.; Infante-Castañeda, C. Barriers and opportunities to improve the foundations for high-quality healthcare in the Mexican Health System. Health Policy Plan. 2018, 33, 1073–1082. [Google Scholar] [CrossRef]
- Mohd Fadhli, M.F.; Hanizad Mod, Y.; Rosnawati, R.; Nur Adibah, M.S.; Khairil Idham, I.; Ahmad Fridaus, M.H. Doctors’ Mental Health in the Midst of COVID-19 Pandemic: The Roles of Work Demands and Recovery Experiences. Int. J. Environ. Res. Public Health 2020, 17, 7340. [Google Scholar] [CrossRef]
- Cordova-Villalobos, J.A.; Macias, A.E.; Hernandez-Avila, M.; Dominguez-Cherit, G.; Lopez-Gatell, H.; Alpuche-Aranda, C.; de León-Rosales, S.P. The 2009 pandemic in Mexico: Experience and lessons regarding national preparedness policies for seasonal and epidemic influenza. Gac. Med. Mex. 2017, 153, 102–110. [Google Scholar]
- Sierra-Madero, J.G.; Belaunzaran-Zamudio, P.F.; Crabtree-Ramírez, B.; Magis-Rodriguez, C. Mexico’s fragmented health system as a barrier to HIV care. Lancet HIV 2019, 6, e74–e75. [Google Scholar] [CrossRef]
- Secretaria de Salud. Medidas Restrictivas Permitirán Ilegar a la Fase 3 con Menor Impacto Epidémico por COVID-19. Available online: https://www.gob.mx/salud/prensa/096-medidas-restrictivas-permitiran-llegar-a-la-fase-3-con-menor-impacto-epidemico-por-covid-19?idiom=es (accessed on 15 June 2020).
- Secretaría de Salud. Datos Abiertos—Dirección General de Epidemiología, 2020. Gob Web Site. Available online: https://www.gob.mx/salud/documentos/datos-abiertos-152127 (accessed on 15 June 2020).
- Morales, G. Live Updates: COVID-19 Death Toll in Mexico, 2020. El Universal Web Site. Available online: https://www.eluniversal.com.mx/english/covid-19-live-updates-mexico (accessed on 15 August 2020).
- Sheridan, M.B. Mexico Adds 1000 Deaths to Official Coronavirus Toll, Most in a Single Day. The Washington Post, 15 August 2020. [Google Scholar]
- CONACYT. COVID-19 Mexico. Available online: https://coronavirus.gob.mx/datos/ (accessed on 15 August 2020).
- Friganoviü, A.; Selič, P.; Ilič, B.; Sedič, B. Stress and burnout syndrome and their associations with coping and job satisfaction in critical care nurses: A literature review. Psychiatr. Danub. 2019, 31, 21–31. [Google Scholar]
- Medina Mora, M.E.; Borgues, G.; Muñoz, C.L.; Benjet, C.; Blanco Jaimes, J.; Bautista, C.F.; Villatoro Velazquez, J.; Rojas Guiot, E.; Zambrano Ruiz, J.; Casanova Rodas, L.; et al. Prevalencia de trastornos mentales y uso de servicios: Resultados de la Encuesta Nacional de Epidemiología Psiquiátrica en México. Salud Ment. 2003, 26, 1–16. [Google Scholar]
- Shah, K.; Chaudhari, G.; Kamrai, D.; Lail, A.; Patel, R.S. How Essential Is to Focus on Physician’s Health and Burnout in Coronavirus (COVID-19) Pandemic? Cureus 2020, 12, 10–12. [Google Scholar] [CrossRef]
- Kang, L.; Li, Y.; Hu, S.; Chen, M.; Yang, C.; Yang, B.X.; Wang, Y.; Hu, J.; Lai, J.; Ma, X.; et al. The mental health of medical workers in Wuhan, China dealing with the 2019 novel coronavirus. Lancet Psychiatry 2020, 7, e14. [Google Scholar] [CrossRef]
- Rodrigues, H.; Cobucci, R.; Oliveira, A.; Cabral, J.V.; Medeiros, L.; Gurgel, K.; Souza, T.; Gonçalves, A.K. Burnout syndrome among medical residents: A systematic review and meta-analysis. PLoS ONE 2018, 13, e0206840. [Google Scholar] [CrossRef]
- Blake, H.; Bermingham, F.; Johnson, G.; Tabner, A. Mitigating the psychological impact of covid-19 on healthcare workers: A digital learning package. Int. J. Environ. Res. Public Health 2020, 17, 2997. [Google Scholar] [CrossRef]
- Taylor, S.; Landry, C.A.; Paluszek, M.M.; Fergus, T.A.; McKay, D.; Asmundson, G.J.G. Development and initial validation of the COVID Stress Scales. J. Anxiety Disord. 2020, 72, 102232. [Google Scholar] [CrossRef]
- Wang, C.; Pan, R.; Wan, X.; Tan, Y.; Xu, L.; Ho, C.S.; Ho, R.C. Immediate Psychological Responses and Associated Factors during the Initial Stage of the 2019 Coronavirus Disease (COVID-19) Epidemic among the General Population in China. Int. J. Environ. Res. Public Health 2020, 17, 1729. [Google Scholar] [CrossRef]
- Yaribeygi, H.; Panahi, Y.; Sahraei, H.; Johnston, T.P.; Sahebkar, A. The impact of stress on body function: A review. EXCLI J. 2017, 16, 1057–1072. [Google Scholar] [CrossRef]
- Lai, J.; Ma, S.; Wang, Y.; Cai, Z.; Hu, J.; Wei, N.; Wu, J.; Du, H.; Chen, T.; Li, R.; et al. Factors Associated With Mental Health Outcomes Among Health Care Workers Exposed to Coronavirus Disease 2019. JAMA 2020, 3, e203976. [Google Scholar] [CrossRef] [PubMed]
- Redaccion Animal Politico. Pico de epidemia será en agosto y se deberá fortalecer el distanciamiento, advierte OPS a México. Animal Politic. 4 August 2020. Available online: https://www.animalpolitico.com/2020/08/pico-epidemia-agosto-distanciamiento-ops-mexico/ (accessed on 15 August 2020).
- Miranda, P. Julio, hasta ahora, el mes más letal de la pandemia. El Universal. 14 August 2020. Available online: https://www.eluniversal.com.mx/nacion/julio-hasta-ahora-el-mes-mas-letal-de-la-pandemia (accessed on 15 August 2020).
- Marsden, P.V.; Wright, J.D. Handbook of Survey Research, 2nd ed.; Emerald Publishing Limited: Bingley, UK, 2010; ISBN 978-1848552241. [Google Scholar]
- Luken, M.; Sammons, A. Systematic Review of Mindfulness Practice for Reducing Job Burnout. Am. J. Occup. Ther. 2016, 70, 7002250020. [Google Scholar] [CrossRef]
- Lee Sherman, A. Coronavirus Anxiety Scale: A brief mental health screener for COVID-19 related anxiety. Death Stud. 2020, 44, 393–401. [Google Scholar] [CrossRef]
- Moukarzel, A.; Michelet, P.; Durand, A.C.; Sebbane, M.; Bourgeois, S.; Markarian, T.; Bompard, C.; Gentile, S. Burnout syndrome among emergency department staff: Prevalence and associated factors. BioMed Res. Int. 2019, 2019, 6462472. [Google Scholar] [CrossRef]
- Javelle, E.; Raoult, D. COVID-19 pandemic more than a century after the Spanish flu. Lancet Infect. Dis. 2020, 3099, 30650. [Google Scholar] [CrossRef]
- Ashton, J. COVID-19 and the ‘Spanish’ flu. J. R. Soc. Med. 2020, 113, 197–198. [Google Scholar] [CrossRef]
- Yang, Y.; Peng, F.; Wang, R.; Guan, K.; Jiang, T.; Xu, G.; Sun, J.; Chang, C. The Deadly Coronaviruses: The 2003 SARS Pandemic and The 2020 Novel Coronavirus Epidemic in China. J. Autoimmun. 2020, 109, 102434. [Google Scholar] [CrossRef] [PubMed]
- West, C.P.; Dyrbye, L.N.; Shanafelt, T.D. Physician burnout: Contributors, consequences and solutions. J. Intern. Med. 2018, 283, 516–529. [Google Scholar] [CrossRef] [PubMed]
- Liu, M.; Cheng, S.; Xu, K.; Yang, Y.; Zhu, Q.; Zhang, H.; Yand, D.-Y.; Cheng, S. Use of personal protective equipment against coronavirus disease 2019 by healthcare professionals in Wuhan, China: Cross sectional study. BMJ 2020, 369, m2195. [Google Scholar] [CrossRef] [PubMed]
- Suárez, V.; Suarez Quezada, M.; Oros Ruiz, S.; De Jesús, E.R. Epidemiología de COVID-19 en México: Del 27 de febrero al 30 de abril de 2020. Rev. Clínica Española 2020, 1–9. [Google Scholar] [CrossRef]
- Brito, M.O. COVID-19 in the Americas: Who’s looking after refugees and migrants? Ann. Glob. Health 2020, 86, 1–3. [Google Scholar] [CrossRef] [PubMed]
- Zhang, X.; Martinez-Donate, A.P.; Simon, N.J.E.; Hovell, M.F.; Rangel, M.G.; Magis-Rodriguez, C.; Sipan, C.L. Risk behaviours for HIV infection among travelling Mexican migrants: The Mexico–US border as a contextual risk factor. Glob. Public Health 2017, 12, 65–83. [Google Scholar] [CrossRef][Green Version]
- Diaz, C.J.; Zeng, L.; Martinez-Donate, A.P. Investigating Health Selection Within Mexico and Across the US Border. Popul. Res. Policy Rev. 2018, 37, 181–204. [Google Scholar] [CrossRef] [PubMed]
- Martinez-Donate, A.P.; Ejebe, I.; Zhang, X.; Guendelman, S.; Rangel, G.; Gonzalez-Fagoaga, E.; Hovell, M.F.; Amuedo-Dorantes, C. Access to Health Care Among Mexican Migrants and Immigrants: A Comparison Across Migration Phases. J. Health Care Poor Underserved 2018. [Google Scholar] [CrossRef] [PubMed]
| Initial Questions | |
|---|---|
| 1 | ¿Desea usted participar en el cuestionario? |
| 2 | ¿Cuál es su profesión? |
| 3 | ¿En qué área trabaja? |
| 4 | ¿Trabaja usted con pacientes con coronavirus? |
| 5 | ¿Con cuántos pacientes trabaja diariamente? |
| Section 1 (Danger) ** | |
| 6 | Estoy preocupado por contraer el virus |
| 7 | Estoy preocupado de ya tener el virus y ser asintomático * |
| 8 | Me preocupa que la higiene básica (por ejemplo, el lavado de manos) no sea suficiente para mantenerme a salvo del virus |
| 9 | Me preocupa que nuestro sistema de salud no pueda mantenerme a salvo del virus |
| 10 | Me preocupa no poder mantener a mi familia a salvo del virus |
| 11 | Me preocupa que nuestro sistema de salud no pueda proteger a mis seres queridos |
| 12 | Me preocupa que el distanciamiento social no sea suficiente para mantenerme a salvo del virus |
| Section 2 (Socialeconomical) | |
| 13 | Me preocupa que las tiendas de comestibles se queden sin comida |
| 14 | Me preocupa que las tiendas de comestibles se queden sin remedios para el resfriado o la gripe |
| 15 | Me preocupa que las farmacias se queden sin medicamentos recetados |
| 16 | Me preocupa que las tiendas de comestibles se queden sin agua |
| 17 | Me preocupa que las tiendas de comestibles se queden sin productos de limpieza o desinfectantes. |
| 18 | Me preocupa que las tiendas de comestibles cierren |
| Section 3 (Xenophobia) | |
| 19 | Me preocupa que personas fuera del estado estén propagando el virus. |
| 20 | Me preocupa que las personas que conozco, que viven fuera de mi estado, puedan tener el virus. |
| 21 | Me preocupa entrar en contacto con personas fuera del estado porque pueden tener el virus. |
| 22 | Me preocupa que personas extranjeras estén propagando el virus porque no están tan limpios como nosotros |
| 23 | Si fuera a un restaurante especializado en alimentos extranjeros, me preocuparía contraer el virus |
| 24 | Si estuviera en un elevador con un grupo de extranjeros, me preocuparía que estén infectados con el virus. |
| Section 4 (Fear of Contamination) ** | |
| 25 | Me preocupa que las personas a mi alrededor me infecten con el virus |
| 26 | Me preocupa que si tocara algo en un espacio público (por ejemplo, pasamanos, manija de la puerta), pueda contraer el virus |
| 27 | Me preocupa que, si alguien tosiera o estornudara cerca de mí, podría contraer el virus. |
| 28 | Me preocupa que pueda contraer el virus al manejar dinero o usar una máquina de tarjeta de débito/crédito |
| 29 | Estoy preocupado por hacer transacciones en efectivo |
| 30 | Me preocupa que mi paquetería/correo haya sido contaminado por los manejadores de correo |
| Section 5 (Traumatic stress) | |
| 31 | Tuve problemas para dormir porque me preocupaba el virus |
| 32 | Tuve malos sueños sobre el virus |
| 33 | Pensé en el virus cuando no quise |
| 34 | Aparecieron en mi mente, contra mi voluntad, imágenes mentales inquietantes sobre el virus |
| 35 | Tuve problemas para concentrarme porque seguía pensando en el virus |
| 36 | Los recordatorios del virus me provocaron reacciones físicas, como sudoración o latidos fuertes del corazón. |
| Section 6 (Compulsive Checking) | |
| 37 | Reviso ubicaciones en redes sociales sobre COVID-19 |
| 38 | Reviso videos de YouTube sobre COVID-19 |
| 39 | Solicitó tranquilidad a amigos o familiares sobre COVID-19 |
| 40 | Reviso mi propio cuerpo en busca de signos de infección (p. Ej., Tomando mi temperatura) |
| 41 | Pido consejo a los profesionales de la salud (por ejemplo, médicos o farmacéuticos) sobre COVID-19 |
| 42 | Busco en Internet tratamientos para COVID-19 |
| Final questions for future follow-up | |
| 43 | Ha sido diagnosticado con COVID 19 |
| 44 | ¿Le interesaría en un futuro participar en un cuestionario para seguimiento de su salud mental? *** |
| 45 | Le agradecemos su interés y le pedimos, por favor nos deje una dirección de correo electrónico *** |
| CSS General Score | COVID Danger + Contamination | |||||||
|---|---|---|---|---|---|---|---|---|
| N Observed | N Expected | Residue | % | N Observed | N Expected | Residue | % | |
| Absent | 9 | 25.3 | −16.3 | 8.9 | 3 | 25.3 | −22.3 | 3.0 |
| Mild | 59 | 25.3 | 33.8 | 58.4 | 23 | 25.3 | −2.3 | 22.8 |
| Moderate | 28 | 25.3 | 2.8 | 27.7 | 58 | 25.3 | 32.8 | 57.4 |
| Severe | 5 | 25.3 | −20.3 | 5.0 | 17 | 25.3 | −8.3 | 16.8 |
| COVID Socioeconomic Consequences | COVID Xenophobia | |||||||
| N Observed | N Expected | Residue | % | N Observed | N Expected | Residue | % | |
| Absent | 30 | 25.3 | 4.8 | 29.7 | 15 | 25.3 | −10.3 | 14.9 |
| Mild | 35 | 25.3 | 9.8 | 34.7 | 45 | 25.3 | 19.8 | 44.6 |
| Moderate | 24 | 25.3 | −1.3 | 23.8 | 29 | 25.3 | 3.8 | 28.7 |
| Severe | 12 | 25.3 | −13.3 | 11.9 | 12 | 25.3 | −13.3 | 11.9 |
| COVID Traumatic Stress | COVID Compulsive Checking | |||||||
| N Observed | N Expected | Residue | % | N Observed | N Expected | Residue | % | |
| Absent | 47 | 25.3 | 21.8 | 46.5 | 26 | 25.3 | 0.8 | 25.7 |
| Mild | 25 | 25.3 | −0.3 | 24.8 | 43 | 25.3 | 17.8 | 42.6 |
| Moderate | 21 | 25.3 | −4.3 | 20.8 | 22 | 25.3 | −3.3 | 21.8 |
| Severe | 8 | 25.3 | −17.3 | 7.9 | 10 | 25.3 | −15.3 | 9.9 |
| CSS | area 1 + 4 | area 2 | area 3 | area 5 | area 6 | |||
| Pearson’s chi-square | 72.109 a | 64.980 a | 11.673 a | 27.119 a | 31.238 a | 22.129 a | ||
| gl | 3 | 3 | 3 | 3 | 3 | 3 | ||
| Asymptotic sig. | <0.001 | <0.001 | 0.009 | <0.001 | <0.001 | <0.001 | ||
| Total CSS | Danger + Contamination | Socioeconomic Consequences | |
|---|---|---|---|
| Medical professions | p < 0.977 | p < 0.840 | p < 0.367 |
| Medical vs. nursing professionals | p < 0.849 | p < 0.629 | p < 0.321 |
| Work area | p < 0.275 | p < 0.998 | p < 0.498 |
| Previous COVID-positive diagnosis | p < 0.664 | p < 0.542 | p < 0.664 |
| Work with COVID patients | p < 0.303 | p < 0.266 | p < 0.786 |
| Total number of COVID patients per day | p < 0.076 | p < 0.122 | p < 0.521 |
| Fear of being an asymptomatic patient (FOBAP) | p < 0.001 | p < 0.003 | p < 0.638 |
| Xenophobia | Traumatic Stress | Compulsive Checking | |
| Medical professions | p < 0.931 | p < 0.108 | p < 0.524 |
| Medical vs. nursing professionals | p < 0.700 | p < 0.677 | p < 0.357 |
| Work area | p < 0.045 | p < 0.144 | p < 0.250 |
| Previous COVID-positive diagnostic | p < 0.653 | p < 0.781 | p < 0.666 |
| Work with COVID patients | p < 0.553 | p < 0.001 | p < 0.121 |
| Total number of COVID patients per day | p < 0.077 | p < 0.027 | p < 0.047 |
| Fear of being an asymptomatic patient (FOBAP) | p < 0.047 | p < 0.002 | p < 0.024 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Delgado-Gallegos, J.L.; Montemayor-Garza, R.d.J.; Padilla-Rivas, G.R.; Franco-Villareal, H.; Islas, J.F. Prevalence of Stress in Healthcare Professionals during the COVID-19 Pandemic in Northeast Mexico: A Remote, Fast Survey Evaluation, Using an Adapted COVID-19 Stress Scales. Int. J. Environ. Res. Public Health 2020, 17, 7624. https://doi.org/10.3390/ijerph17207624
Delgado-Gallegos JL, Montemayor-Garza RdJ, Padilla-Rivas GR, Franco-Villareal H, Islas JF. Prevalence of Stress in Healthcare Professionals during the COVID-19 Pandemic in Northeast Mexico: A Remote, Fast Survey Evaluation, Using an Adapted COVID-19 Stress Scales. International Journal of Environmental Research and Public Health. 2020; 17(20):7624. https://doi.org/10.3390/ijerph17207624
Chicago/Turabian StyleDelgado-Gallegos, Juan Luis, Rene de Jesús Montemayor-Garza, Gerardo R. Padilla-Rivas, Héctor Franco-Villareal, and Jose Francisco Islas. 2020. "Prevalence of Stress in Healthcare Professionals during the COVID-19 Pandemic in Northeast Mexico: A Remote, Fast Survey Evaluation, Using an Adapted COVID-19 Stress Scales" International Journal of Environmental Research and Public Health 17, no. 20: 7624. https://doi.org/10.3390/ijerph17207624
APA StyleDelgado-Gallegos, J. L., Montemayor-Garza, R. d. J., Padilla-Rivas, G. R., Franco-Villareal, H., & Islas, J. F. (2020). Prevalence of Stress in Healthcare Professionals during the COVID-19 Pandemic in Northeast Mexico: A Remote, Fast Survey Evaluation, Using an Adapted COVID-19 Stress Scales. International Journal of Environmental Research and Public Health, 17(20), 7624. https://doi.org/10.3390/ijerph17207624






