Health-Care Services as a Platform for Building Community Resilience among Minority Communities: An Israeli Pilot Study during the COVID-19 Outbreak
Abstract
1. Introduction
1.1. Community Resilience and the Role of Health-Care Services
1.2. Community Resilience of Minority Groups
1.3. The Current Study
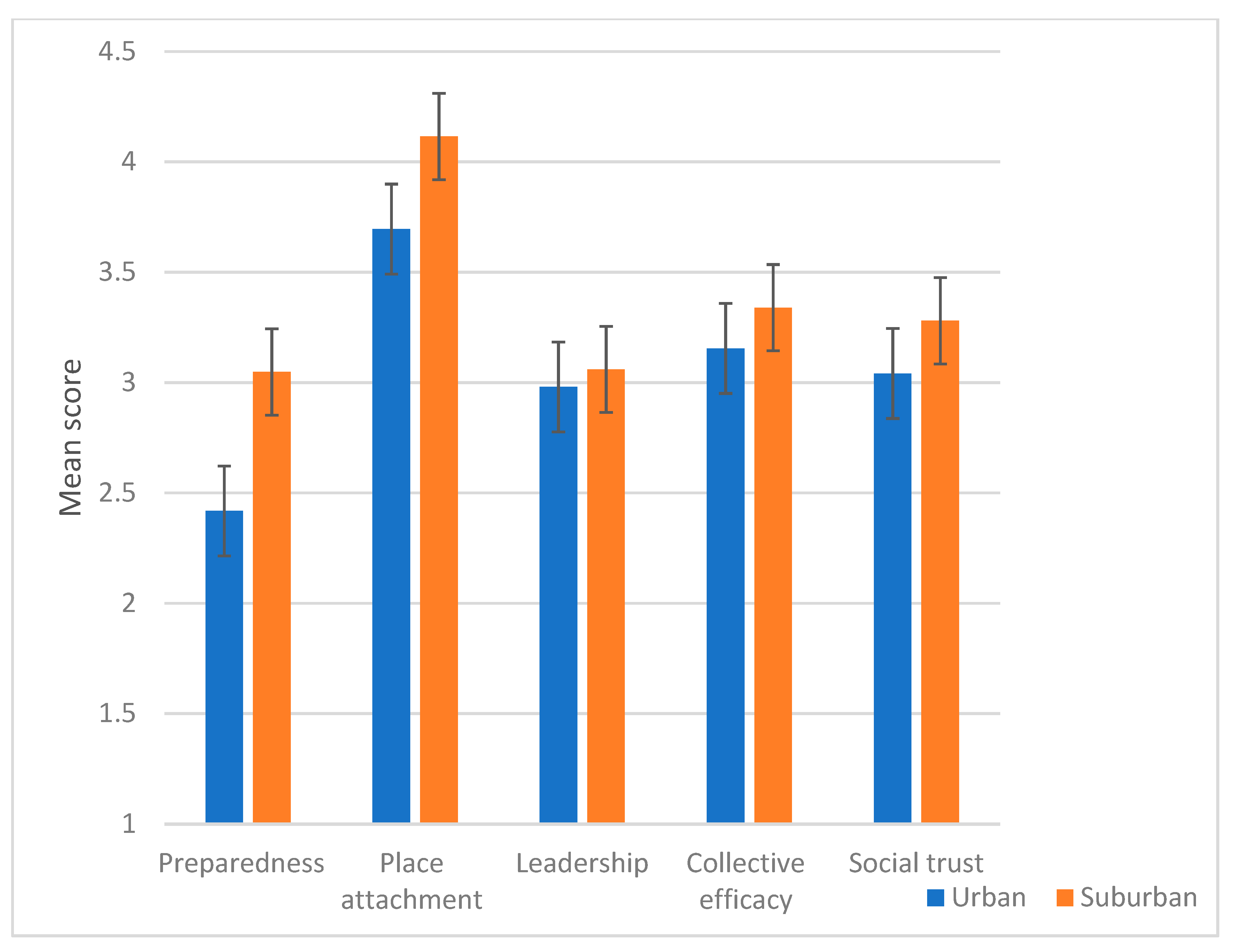
- Higher levels of community resilience will be scored in the suburban community, a smaller local council that may be more socially cohesive than the urban community.
- Community resilience would be positively associated with increased confidence and satisfaction with health-care services (primary and specialized).
- Community type would play a unique role in community resilience, over and above the perceptions of health-care services as a provider of medical treatment.
2. Materials and Methods
2.1. Study Design, Setting, and Participants
2.2. Instruments
2.3. Data Analysis
2.4. Ethical Approval
3. Results
3.1. Demographic Characteristics of Study Participants
3.2. Community Resilience and Community Type
3.3. The Role of the Health-Care Services in Predicting Community Resilience
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Adams, V. Markets of Sorrow, Labors of Faith: New Orleans in the Wake of Katrina; Duke University Press: Durham, NC, USA, 2013. [Google Scholar]
- Elliott, J.R.; Bellone-Hite, A.; Devine, J. Unequal return: The uneven resettlements of New Orleans’s uptown neighborhoods. Org. Environ. 2009, 22, 410–421. [Google Scholar] [CrossRef]
- Weber, L.; Messias, D.K.H. Mississippi front-line recovery work after Hurricane Katrina: An analysis of the intersections of gender, race, and class in advocacy, power relations, and health. Soc. Sci. Med. 2012, 74, 1833–1841. [Google Scholar] [CrossRef] [PubMed]
- Davidson, T.M.; Price, M.; McCauley, J.L.; Ruggiero, K.J. Disaster impact across cultural groups: Comparison of Whites, African Americans, and Latinos. Am. J. Community Psychol. 2013, 52, 97–105. [Google Scholar] [CrossRef] [PubMed]
- Centers for Disease Control and Prevention. COVID-19, 2020. Available online: https://www.cdc.gov/coronavirus/2019-ncov/index.html (accessed on 13 October 2020).
- Kimhi, S.; Eshel, Y.; Marciano, H.; Adini, B. Distress and Resilience in the Days of COVID-19: Comparing Two Ethnicities. Int. J. Environ. Res. Public Health 2020, 17, 3956. [Google Scholar] [CrossRef]
- Davis, R.; Cook, D.; Cohen, L. A community resilience approach to reducing ethnic and racial disparities in health. Am. J. Public Health 2005, 95, 2168–2173. [Google Scholar] [CrossRef]
- Patel, S.S.; Rogers, M.B.; Amlôt, R.; Rubin, G.J. What do we mean by ‘Community Resilience’? A systematic literature review of how it is defined in the literature. PLoS Curr. 2017. [Google Scholar] [CrossRef]
- Magis, K. Community resilience: An indicator of social sustainability. Soc. Nat. Res. 2010, 23, 401–416. [Google Scholar] [CrossRef]
- Norris, F.H.; Stevens, S.P.; Pfefferbaum, B.; Wyche, K.F.; Pfefferbaum, R.L. Community resilience as a metaphor, theory, set of capacities, and strategy for disaster readiness. Am. J. Community Psychol. 2008, 41, 127–150. [Google Scholar] [CrossRef]
- Cohen, O.; Goldberg, A.; Lahad, M.; Ahronsonn-Daniel, L. Building resilience: The relationship between information provided by municipal authorities during emergency situations and community resilience. Technol. Forecast. Soc. Chang. 2017, 121, 119–125. [Google Scholar] [CrossRef]
- Madsen, W.; O’Mullan, C. Perception of community resilience after natural disaster in a rural Australian town. J. Community Psychol. 2016, 44, 277–292. [Google Scholar] [CrossRef]
- Chandra, A.; Acosta, J.; Howard, S.; Uscher-Pines, L.; Williams, M.; Yeung, D.; Garnett, J.; Meredith, L.S. Building community resilience to disasters: A way forward to enhance national health security. Rand. Health Q. 2011. [Google Scholar] [CrossRef]
- Cohen, O.; Shapira, S.; Aharonson-Daniel, L.; Shamian, J. Confidence in health-services availability during disasters and emergency situations-does it matter?-Lessons learned from an Israeli population survey. Int. J. Environ. Res. Public Health 2019, 16, 3519. [Google Scholar] [CrossRef] [PubMed]
- Rapaport, C.; Hornik-Lurie, T.; Cohen, O.; Lahad, M.; Leykin, D.; Aharonson-Daniel, L. The relationship between community type and community resilience. Int. J. Disaster Risk Reduct. 2018, 31, 470–477. [Google Scholar] [CrossRef]
- Pickett, S.T.A.; Cadenasso, J.M.; Grove, M. Resilient cities: Meaning, models, and metaphor for integrating the ecological, socio-economic, and planning realms. Landsc. Urban Plan. 2004, 69, 369–384. [Google Scholar] [CrossRef]
- Pierce, J.C.M.; Budd, W.W.; Lovrich, N.P., Jr. Resilience and sustainability in US urban areas. Environ. Polit. 2011, 20, 566–584. [Google Scholar] [CrossRef]
- Flora, C.B.; Flora, J.L. Rural Communities: Legacy and Change; Westview: Boulder, CO, USA, 2004. [Google Scholar]
- Centers for Disease Control and Prevention. PUBLIC Health Preparedness Capabilities: National Standards for State and Local Planning, 2011. Available online: https://www.cdc.gov/cpr/readiness/00_docs/DSLR_capabilities_July.pdf (accessed on 13 October 2020).
- Redwood-Campbell, L.; Abrahams, J. Primary health care and disasters-the current state of the literature: What we know, gaps and next steps. Prehosp. Disaster. Med. 2011, 26, 184–191. [Google Scholar] [CrossRef]
- Framework for the NHSS. Assistant Secretary for Preparedness and Response. Available online: https://www.phe.gov/about/aspr/Pages/default.aspx (accessed on 13 October 2020).
- Charney, R.L.; Rebmann, T.; Esguerra, C.R.; Lai, C.W.; Dalawari, P. Public perceptions of hospital responsibilities to those presenting without medical injury or illness during a disaster. J. Emerg. Med. 2013, 45, 78–584. [Google Scholar] [CrossRef]
- Wells, M. Resilience in rural community-dwelling older adults. J. Rural. Health 2009, 25, 415–419. [Google Scholar] [CrossRef]
- Drury, J.; Cocking, C.; Reicher, S. Everyone for themselves? A comparative study of crowd solidarity among emergency survivors. Br. J. Soc. Psychol. 2009, 48, 487–506. [Google Scholar] [CrossRef]
- Weine, S.; Kulauzovic, Y.; Klebic, A.; Besic, S.; Mujagic, A.; Muzurovic, J.; Rolland, J. Evaluating a multiple-family group access intervention for refugees with PTSD. J. Marital. Fam. Ther. 2008, 43, 149–164. [Google Scholar] [CrossRef]
- Slobodin, O.; de Jong, J.T. Mental health interventions for traumatized asylum seekers and refugees: What do we know about their efficacy? Int. J. Soc. Psychiatr. 2015, 61, 17–26. [Google Scholar] [CrossRef] [PubMed]
- Eisenman, D.P.; Wold, C.; Fielding, J.; Long, A.; Setodji, C.; Hickey, S.; Gelberg, L. Differences in individual-level terrorism preparedness in Los Angeles County. Am. J. Prev. Med. 2006, 30, 1–6. [Google Scholar] [CrossRef]
- Eisenman, D.P.; Zhou, Q.; Ong, M.; Asch, S.; Glik, D.; Long, A. Variations in disaster preparedness by mental health, perceived general health, and disability status. Disaster. Med. Public Health Prep. 2009, 3, 33–41. [Google Scholar] [CrossRef] [PubMed]
- Hawkins, R.L.; Maurer, K. ‘You fix my community, you have fixed my life’: The disruption and rebuilding of ontological security in New Orleans. Disasters 2011, 35, 143–159. [Google Scholar] [CrossRef] [PubMed]
- Bethel, J.W.; Burke, S.C.; Britt, A.F. Disparity in disaster preparedness between racial/ethnic groups. Disaster Health 2013, 1, 110–116. [Google Scholar] [CrossRef]
- Guha-Sapir, D. EMDAT and Trends in Natural Disasters; CRED, Louvain School of Medicine Brussels: Venice, Italy, 2011. [Google Scholar]
- Pole, N.; Gone, G.P.; Kulkarni, M. Posttraumatic stress disorder among ethnoracial minorities in the United States. Clin. Psychol. 2008, 15, 35–61. [Google Scholar] [CrossRef]
- Ungar, M. The social ecology of resilience. Addressing contextual and cultural ambiguity of a nascent construct. Am. J. Orthopsychiatr. 2011, 81, 1–17. [Google Scholar] [CrossRef]
- Bracken, P.J. Trauma: Culture, Meaning and Philosophy; Whurr Publishers Ltd: London, UK, 2002. [Google Scholar]
- Westoby, P. Developing a community-development approach through engaging resettling Southern Sudanese refugees within Australia. Community. Dev. J. 2008, 43, 483–495. [Google Scholar] [CrossRef]
- Galea, S.; Ahern, J.; Resnick, H.; Kilpatrick, D.; Bucuvalas, M.; Gold, J.; Vlahov, D. Psychological sequelae of the September 11 terrorist attacks in New York City. N. Engl. J. Med. 2002, 346, 982–987. [Google Scholar] [CrossRef]
- Heck, N.C. The potential to promote resilience: Piloting a minority stress-informed, GSA-based, mental health promotion program for LGBTQ youth. Psychol. Sex Orientat. Gend. Divers. 2015, 2, 225–231. [Google Scholar] [CrossRef]
- Norris, F.H.; Sherrieb, K.; Pfefferbaum, B. Community resilience: Concepts, assessment, and implications for intervention. In Resilience and Mental Health: Challenges across the Lifespan; Southwick, S.M., Litz, B.T., Charney, D., Friedman, M.J., Eds.; Cambridge University Press: Cambridge, UK, 2011; pp. 149–161. [Google Scholar] [CrossRef]
- Hobfoll, S.E.; Palmieri, P.A.; Johnson, R.J.; Canetti-Nisim, D.; Hall, B.J.; Galea, S. Trajectories of resilience, resistance, and distress during ongoing terrorism: The case of Jews and Arabs in Israel. J. Consult. Clin. Psychol. 2009, 77, 138–148. [Google Scholar] [CrossRef] [PubMed]
- Kimchi, S.; Dror, G.; Sapir, S. Resilience among students from the majority and minority group: The Israeli case. J. Psychol. Behav. Sci. 2017, 5, 37–46. [Google Scholar]
- Marciano, H.; Eshel, Y.; Kimhi, S. Predictors of Individual, Community and National Resiliencies of Israeli Jews and Arabs. Int. J. Psychol. 2019. [Google Scholar] [CrossRef] [PubMed]
- Braun-Lewensohn, O.; Sagy, S. Community resilience and sense of coherence as protective factors in explaining stress reactions: Comparing cities and rural communities during missiles attacks. Community Ment. Health J. 2014, 50, 229–234. [Google Scholar] [CrossRef]
- Nakash, O.; Nagar, M.; Danilovich, E.; Bentov-Gofrit, D.; Lurie, I.; Steiner, E.; Sadeh-Sharvit, S.; Szor, H.; Levav, I. Ethnic disparities in mental health treatment gap in a community-based survey and in access to care in psychiatric clinics. Int. J. Soc. Psychiatr. 2013, 60, 575–583. [Google Scholar] [CrossRef]
- Middle East Report. IDENTITY Crisis: Israel and Its Arab Citizens, 2004. Available online: https://www.crisisgroup.org/middle-east-north-africa/eastern-mediterranean/israelpalestine/identity-crisis-israel-and-its-arab-citizens (accessed on 13 October 2020).
- Vardi-Saliternik, R.; Friedlander, Y.; Cohen, T. Consanguinity in a population sample of Israeli Muslim Arabs, Christian Arabs and Druze. Ann. Hum. Biol. 2002, 29, 422–431. [Google Scholar] [CrossRef]
- Baron-Epel, O.; Garty, N.; Green, M.S. Inequalities in use of health services among Jews and Arabs in Israel. Health Ser. Res. 2007, 42, 1008–1019. [Google Scholar] [CrossRef]
- Khatib, M. Health of Arab Women in Israel, the Galilee Society—The Arab National Society for Health Research and Services, 2012. Available online: https://arab.org/directory/the-galilee-society-the-arab-national-society-for-health-research-and-services/ (accessed on 13 October 2020).
- Na’amnih, W.; Muhsen, K.; Tarabeia, J.; Saabneh, A.; Green, M.S. Trends in the gap in life expectancy between Arabs and Jews in Israel between 1975 and 2004. Int. J. Epidemiol. 2010, 39, 1324–1332. [Google Scholar] [CrossRef]
- Ministry of Health. The Novel Coronavirus. 2020. Available online: https://www.health.gov.il/English/Topics/Diseases/corona/Pages/default.aspx (accessed on 13 October 2020).
- Staff, T. Checkpoints Dismantled as Lockdown of Virus-Hit Arab Towns in North Lifted. The Times of Israel. 25 April 2020. Available online: https://www.timesofisrael.com/checkpoints-dismantled-as-lockdown-of-virus-hit-arab-towns-in-north-lifted/ (accessed on 13 October 2020).
- Slobodin, O.; Cohen, O. A culturally-competent approach to emergency management: What lessons can we learn from the COVID-19? Psychol. Trauma. 2020, 12, 470–473. [Google Scholar] [CrossRef]
- Ebenstein, R. Fighting Back Against COVID-19 in Israel’s Bedouin Community. Fathom. (1 April 2020). Available online: https://fathomjournal.org/fighting-back-against-covid-19-in-the-bedouin-community/ (accessed on 13 October 2020).
- Cohen, J. Statistical Power Analysis for the Behavioral Sciences; Routledge Academic: New York, NY, USA, 1992. [Google Scholar]
- Cohen, O.; Leykin, D.; Lahad, M.; Goldberg, A.; Aharonson-Daniel, L. The conjoint community resiliency assessment measure as a baseline for profiling and predicting community resilience for emergencies. Technol. Forecast. Soc. Chang. 2013. [Google Scholar] [CrossRef]
- Leykin, D.; Lahad, M.; Cohen, O.; Goldberg, A.; Aharonson-Daniel, L. Conjoint community Resiliency assessment measure-28/10 items (CCRAM28 and CCRAM10): A self-report tool for assessing community resilience. Am. J. Community Psychol. 2013, 52, 313–323. [Google Scholar] [CrossRef] [PubMed]
- Bombak, A.E. Self-rated health and public health: A critical perspective. Front. Public Health 2013, 1, 15. [Google Scholar] [CrossRef] [PubMed]
- Strawbridge, W.J.; Wallhagen, M.I. Self-rated health and mortality over three decades: Results from a time-dependent covariate analysis. Res. Aging. 1999. [Google Scholar] [CrossRef]
- Brammli-Greenberg, S.; Medina-Artom, T.; Belinsky, A. Summary of Findings from the Eleventh Survey of Public Opinion on the Level of Service and Performance of the Healthcare System; Myers-JDC-Brookdale Institute: Jerusalem, Israel, 2017. [Google Scholar]
- IBM Corp. IBM SPSS Statistics for Windows, Version 26.0; IBM Corp: Armonk, NY, USA, 2019. [Google Scholar]
- Beggs, J.J.; Haines, V.A.; Hurlbert, J.S. Revisiting the rural-urban contrast: Personal networks in nonmetropolitan and metropolitan settings. Rural. Soc. 1996, 61, 306–325. [Google Scholar] [CrossRef]
- Lev-Wiesel, R. Indicators constituting the construct of ‘perceived community cohesion’. Community Dev. J. 2003, 38, 332–343. [Google Scholar] [CrossRef]
- Van der Gaag, M.; van der Heide, I.; Spreeuwenberg, P.M.M.; Brabers, A.E.M.; Rasemakers, J.D.J.M. Health literacy and primary health care use of ethnic minorities in the Netherlands. BMC Health Serv. Res. 2017, 17, 350. [Google Scholar] [CrossRef]
- Uiters, E.; Deville, W.; Foets, M.; Spreeuwenberg, P.; Groenewegen, P.P. Differences between immigrant and non-immigrant groups in the use of primary medical care; a systematic review. BMC Health. Serv. Res. 2009, 9, 76. [Google Scholar] [CrossRef]
- Hayek, S.; Derhy, S.; Smith, M.L.; Towne, S.D.; Zelber-Sagi, S. Patient satisfaction with primary care physician performance in a multicultural population. Isr. J. Health Policy Res. 2020, 9, 13. [Google Scholar] [CrossRef]
- Kimhi, S.; Shamai, M. Community resilience and the impact of stress: Adult response to Israel’s withdrawal from Lebanon. J. Community Psychol. 2004, 32, 439–451. [Google Scholar] [CrossRef]
- Leykin, D.; Lahad, M.; Cohen, R.; Goldberg, A.; Aharonson-Daniel, L. The dynamics of Community Resilience between routine and emergency situations. Int. J. Disaster Risk Reduct. 2016. [Google Scholar] [CrossRef]
- Shamai, M.; Kimhi, S.; Enosh, G. Social systems and personal reactions to threats of war. J. Soc. Per. Relatsh. 2007, 24, 747–764. [Google Scholar] [CrossRef]
- De Filippo, O.; D’Ascenzo, F.; Angelini, F.; Bocchino, P.P.; Conrotto, F.; Saglietto, A.; Secco, G.G.; Campo, G.; Gallone, G.; Verardi, R.; et al. Reduced rate of hospital admissions for ACS during Covid-19 outbreak in Northern Italy. N. Eng. J. Med. 2020, 383, 88–89. [Google Scholar] [CrossRef]
- Guo, H.; Zhou, Y.; Liu, X.; Tan, J. The impact of the COVID-19 epidemic on the utilization of emergency dental services. J. Dent. Sci. 2020. [Google Scholar] [CrossRef] [PubMed]
- Raphael, B. When Disaster Strikes: How Individuals and Communities Cope with Catastrophe; Basic Books: New York, NY, USA, 1986. [Google Scholar]
- Kapucu, N.; Hawkins, C.V.; Rivera, F.I. Disaster preparedness and resilience for rural communities. Risk. Hazards Crisis Public Policy 2013, 4. [Google Scholar] [CrossRef]
- Richards, L.; Howden, S.M. Transformational adaptation: Agriculture and climate change. Crop. Pasture Sci. 2012, 63, 240. [Google Scholar] [CrossRef]
- World Health Organization. Role of Primary Care in the COVID-19 Response. 2020. Available online: https://apps.who.int/iris/bitstream/handle/10665/331921/Primary-care-COVID-19-eng.pdf?sequence=1&isAllowed=y (accessed on 13 October 2020).
- Hall, M.; Mazarakis, A.; Chorley, M.; Caton, S. Editorial of the special issue on following user pathways: Key contributions and future directions in cross-platform social media research. Int. J. Hum-Comput. Int. 2018, 34, 895–912. [Google Scholar] [CrossRef]
- World Health Organization. World Report on Health Policy and Systems Research. 2017. Available online: https://www.who.int/alliance-hpsr/resources/publications/worldreport-hpsr/en/ (accessed on 13 October 2020).
- Haque, M.; Islam, T.; Rahman, N.A.A.; McKimm, J.; Abdullah, A.; Dhingra, S. Strengthening primary health-care services to help prevent and control long-term (chronic) non-communicable diseases in low- and middle-income countries. Risk Manag. Healthc. Policy 2020, 13, 409–426. [Google Scholar] [CrossRef]
- Bennett, S.; Glandon, D.; Rasanathan, K. Governing multisectoral action for health in low-income and middle-income countries: Unpacking the problem and rising to the challenge. BMJ. Glob. Health 2018, 3, e000880. [Google Scholar] [CrossRef]
- Rasanathan, K.; Atkins, V.; Mwansambo, C.; Soucat, A.; Bennett, S. Governing multisectoral action for health in low-income and middle-income countries: An agenda for the way forward. BMJ Glob. Health 2018, 3, e000890. [Google Scholar] [CrossRef]
- Ramli, A.S.; Lakshmanan, S.; Haniff, J.; Selvarajah, S.; Tong, S.F.; Bujang, M.-A.; Abdul-Razak, S.; Shafie, A.A.; Lee, V.K.M.; Abdul-Rahman, T.H.; et al. Study protocol of empower participatory action research (empower-par): A pragmatic cluster randomized controlled trial of multifaceted chronic disease management strategies to improve diabetes and hypertension outcomes in primary care. BMC Fam. Pract. 2014, 15, 151. [Google Scholar] [CrossRef]
- Bachmann, M.O.; Bateman, E.D.; Stelmach, R.; Cruz, Á.A.; de Andrade, M.P.; Zonta, R.; Zepeda, J.; Natal, S.; Cornick, R.; Wattrus, C.; et al. Integrating primary care of chronic respiratory disease, cardiovascular disease, and diabetes in Brazil: Practical Approach to Care Kit (PACK Brazil): Study protocol for randomized controlled trials. J. Thorac. Dis. 2018, 10, 4667–4677. [Google Scholar] [CrossRef] [PubMed]
- Van Meel, C.; Kidd, M.R. Why strengthening primary health care is essential to achieving universal health coverage. CMAJ 2018, 190, E463–E466. [Google Scholar] [CrossRef] [PubMed]
- Palagyi, A.; Dodd, R.; Jan, S.; Nambiar, D.; Joshi, R.; Tian, M.; Abimbola, S.; Peiris, D. Organisation of primary health care in the Asia-Pacific region: Developing a prioritised research agenda. BMJ. Global. Health 2019, 4, e001467. [Google Scholar] [CrossRef] [PubMed]
- Hirschhorn, L.R.; Langlois, E.V.; Bitton, A.; Ghaffar, A. What kind of evidence do we need to strengthen primary healthcare in the 21st century? BMJ. Global. Health 2019, 4, e001668. [Google Scholar] [CrossRef]
- Löckenhoff, C.E.; De Fruyt, F.; Terracciano, A.; McCrae, R.R.; De Bolle, M.; Costa, P.T., Jr.; Aguilar-Vafaie, M.E.; Ahn, C.K.; Ahn, H.N.; Alcalay, L.; et al. Perceptions of aging across 26 cultures and their culture-level associates. Psychol. Aging. 2009, 24, 941–954. [Google Scholar] [CrossRef]
- Slobodin, O.; Clempert, N.; Kula, Y.; Cohen, O. Educating health professionals for cultural competence in emergency situations: A study protocol for a randomized controlled trial. J. Adv. Nurs. 2020, 76, 380–386. [Google Scholar] [CrossRef]
- Ginzburg, C. Deciphering the sabbath. In Early Modern European Witchcraft: Centres and Peripheries; Ankarloo, B., Henningsen, G., Eds.; Oxford University Press: New York, NY, USA, 1990; pp. 121–138. [Google Scholar]
- Mack, A. In Time of Plague: The History and Social Consequences of Lethal Epidemic Disease; Oxford University Press: New York, NY, USA, 1991. [Google Scholar]
- Porter, R. The case of consumption. In Understanding Catastrophe; Bourriau, J., Ed.; Cambridge University Press: Cambridge, UK, 1992; pp. 179–203. [Google Scholar]
- US Department of Homeland Security. Homeland Security Presidential directive 21. Public Health and Medical Preparedness. October 2007. Available online: https://fas.org/irp/offdocs/nspd/hspd-21.htm (accessed on 13 October 2020).
- Schoch-Spana, M.; Courtney, B.; Franco, C.; Norwood, A.; Nuzzo, J.B. Community resilience roundtable on the implementation of Homeland Security Presidential Directive 21 (HSPD-21). Biosecur. Bioterror. 2008, 6, 269–278. [Google Scholar] [CrossRef]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
| Variable | Urban Community (n = 112) | Suburban Community (n = 84) | Difference | |
|---|---|---|---|---|
| Age M (SD) | 31.46 (15.13) | 39.73 (11.89) | t (194) = −4.176, p = 0.000 | |
| Gender | Male | 34 | 27 | χ2 (1) =0.03, p = 0.85 |
| Female | 76 | 57 | ||
| Religious affiliation | Religiously observant. | 36 | 41 | χ2 (1) =7.04, p = 0.03 |
| Traditional | 70 | 42 | ||
| Secular | 6 | 1 | ||
| Years of education | <8 | 16 | 7 | χ2 (1) = 3.40, p = 183 |
| Highschool | 29 | 17 | ||
| Academic | 64 | 59 | ||
| Community resilience M (SD) | 3.08 (0.71) | 3.37 (0.58) | F (1,185) = 3.98, p = 0.048 | |
| Satisfaction with community health services M (SD) | 3.99 (0.62) | 4.12 (0.57) | F (1,185) = 7.20, p = 0.008 | |
| Satisfaction with specialized health services M (SD) | 4.03 (0.73) | 4.28 (0.66) | F (1,184) = 7.77, p = 0.006 | |
| Confidence in health services | 3.45 (0.69) | 3.47 (0.77) | F (1,184) = 3.75, p = 0.054 | |
| Age | Gender | Community Type | Satisfaction with Primary Health Services | Satisfaction with Specialized Health Services | Confidence in Health Services | Community Resilience | Self-Rated Health | |
|---|---|---|---|---|---|---|---|---|
| Age | 1 | −0.32 ** | 0.27 ** | 0.16 * | 0.09 | 0.11 | 0.09 | −0.36 ** |
| Gender | 1 | −0.01 | 0.16 * | 0.17 * | 0.08 | 0.01 | 0.11 | |
| Community type | 1 | 0.12 | 0.17 * | 0.09 | 0.19 ** | −0.02 | ||
| Satisfaction with primary healthcare services | 1 | 0.60 ** | 0.56 ** | 0.33 ** | 0.18 * | |||
| Satisfaction with specialized healthcare services | 1 | 0.40 ** | 0.28 ** | 0.14 | ||||
| Confidence in healthcare services | 1 | 0.18 * | −0.001 | |||||
| Community resilience | 1 | 0.08 | ||||||
| Self-rated health | 1 |
| Step | Unstandardized Coefficients | Standardized Coefficients | F | |||
|---|---|---|---|---|---|---|
| B | Std. Error | Beta | Adj. R Square | |||
| 1 | Age | 0.01 | 0.01 | 0.12 | 1.20 | 0.004 |
| Gender | 0.01 | 0.14 | 0.01 | |||
| Self-rated health | 0.06 | 0.04 | 0.155 | |||
| 2 | Age | 0.004 | 0.01 | 0.08 | 1.85 | 0.20 |
| Gender | −0.00 | 0.14 | −0.01 | |||
| Self-rated health | 0.06 | 0.04 | 0.12 | |||
| Community type | 0.25 | 0.13 | 0.16 | |||
| 3 | Age | 0.01 | 0.01 | 0.13 | 4.40 *** | 0.124 |
| Gender | −0.07 | 0.14 | −0.04 | |||
| Self-rated health | 0.03 | 0.04 | 0.07 | |||
| Community type | 0.15 | 0.13 | 0.09 | |||
| Satisfaction with primary healthcare services | 0.41 | 0.14 | 0.31 ** | |||
| Satisfaction with specialized healthcare services | 0.08 | 0.11 | 0.07 | |||
| Confidence in healthcare services | −0.003 | 0.10 | −0.003 | |||
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Cohen, O.; Mahagna, A.; Shamia, A.; Slobodin, O. Health-Care Services as a Platform for Building Community Resilience among Minority Communities: An Israeli Pilot Study during the COVID-19 Outbreak. Int. J. Environ. Res. Public Health 2020, 17, 7523. https://doi.org/10.3390/ijerph17207523
Cohen O, Mahagna A, Shamia A, Slobodin O. Health-Care Services as a Platform for Building Community Resilience among Minority Communities: An Israeli Pilot Study during the COVID-19 Outbreak. International Journal of Environmental Research and Public Health. 2020; 17(20):7523. https://doi.org/10.3390/ijerph17207523
Chicago/Turabian StyleCohen, Odeya, Alaa Mahagna, Asmaa Shamia, and Ortal Slobodin. 2020. "Health-Care Services as a Platform for Building Community Resilience among Minority Communities: An Israeli Pilot Study during the COVID-19 Outbreak" International Journal of Environmental Research and Public Health 17, no. 20: 7523. https://doi.org/10.3390/ijerph17207523
APA StyleCohen, O., Mahagna, A., Shamia, A., & Slobodin, O. (2020). Health-Care Services as a Platform for Building Community Resilience among Minority Communities: An Israeli Pilot Study during the COVID-19 Outbreak. International Journal of Environmental Research and Public Health, 17(20), 7523. https://doi.org/10.3390/ijerph17207523





