Important Difference between Occupational Hazard Exposure among Shift Workers and Other Workers; Comparing Workplace before and after 1980
Abstract
1. Introduction
2. Materials and Methods
3. Results
3.1. Hazard Exposure
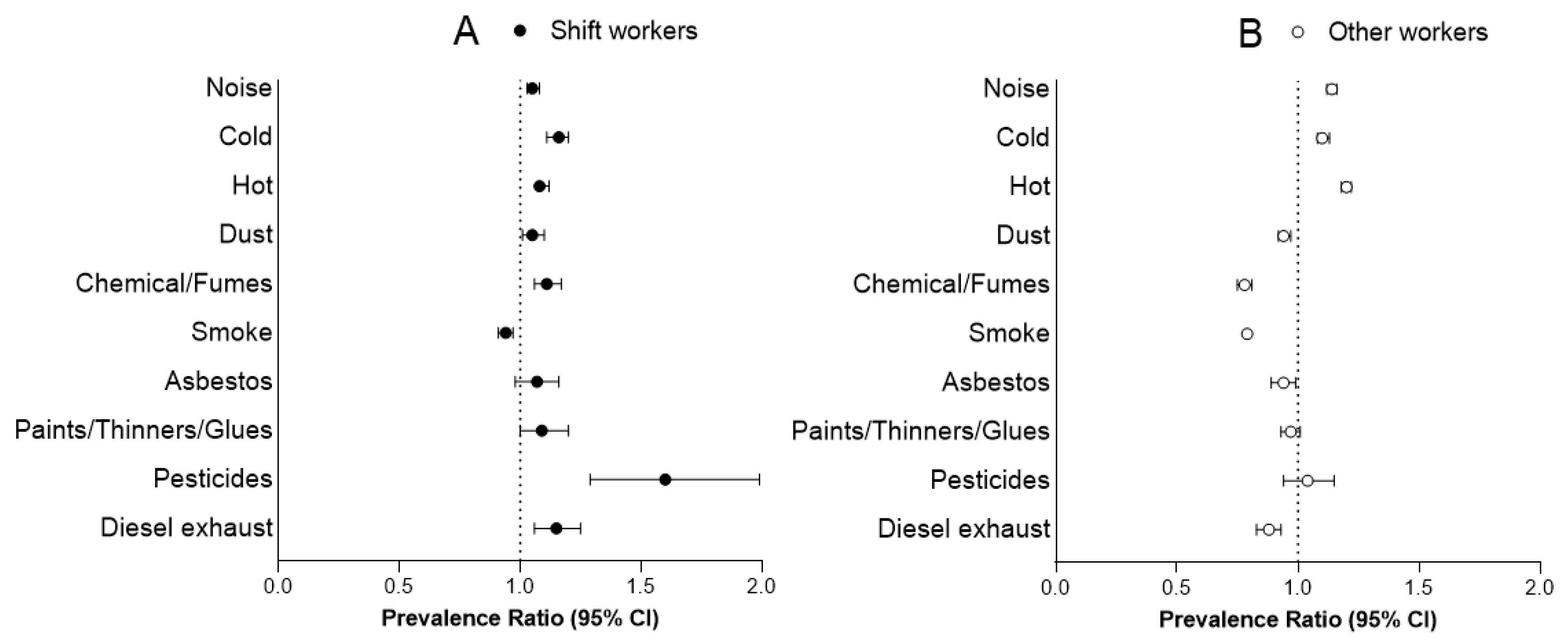
3.1.1. Comparison between Shift and Other Workers
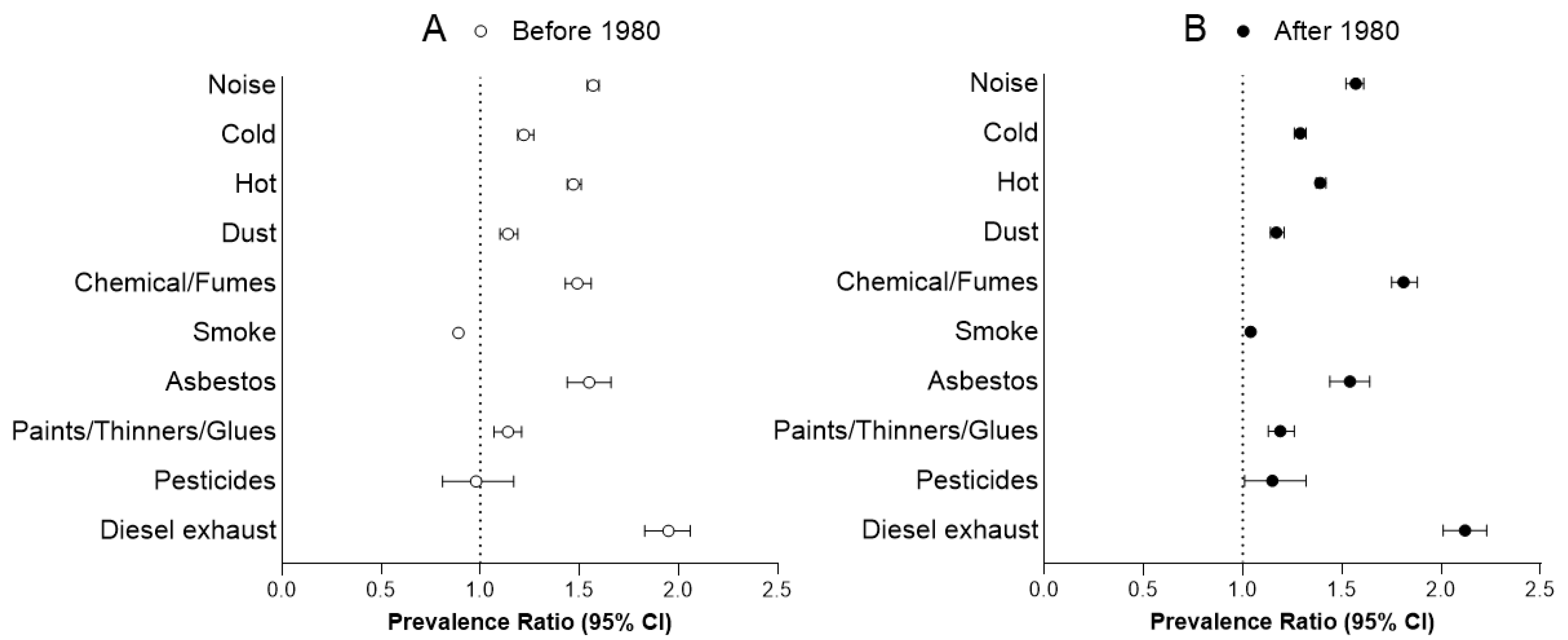
3.1.2. Comparison Between Before 1980 and After 1980
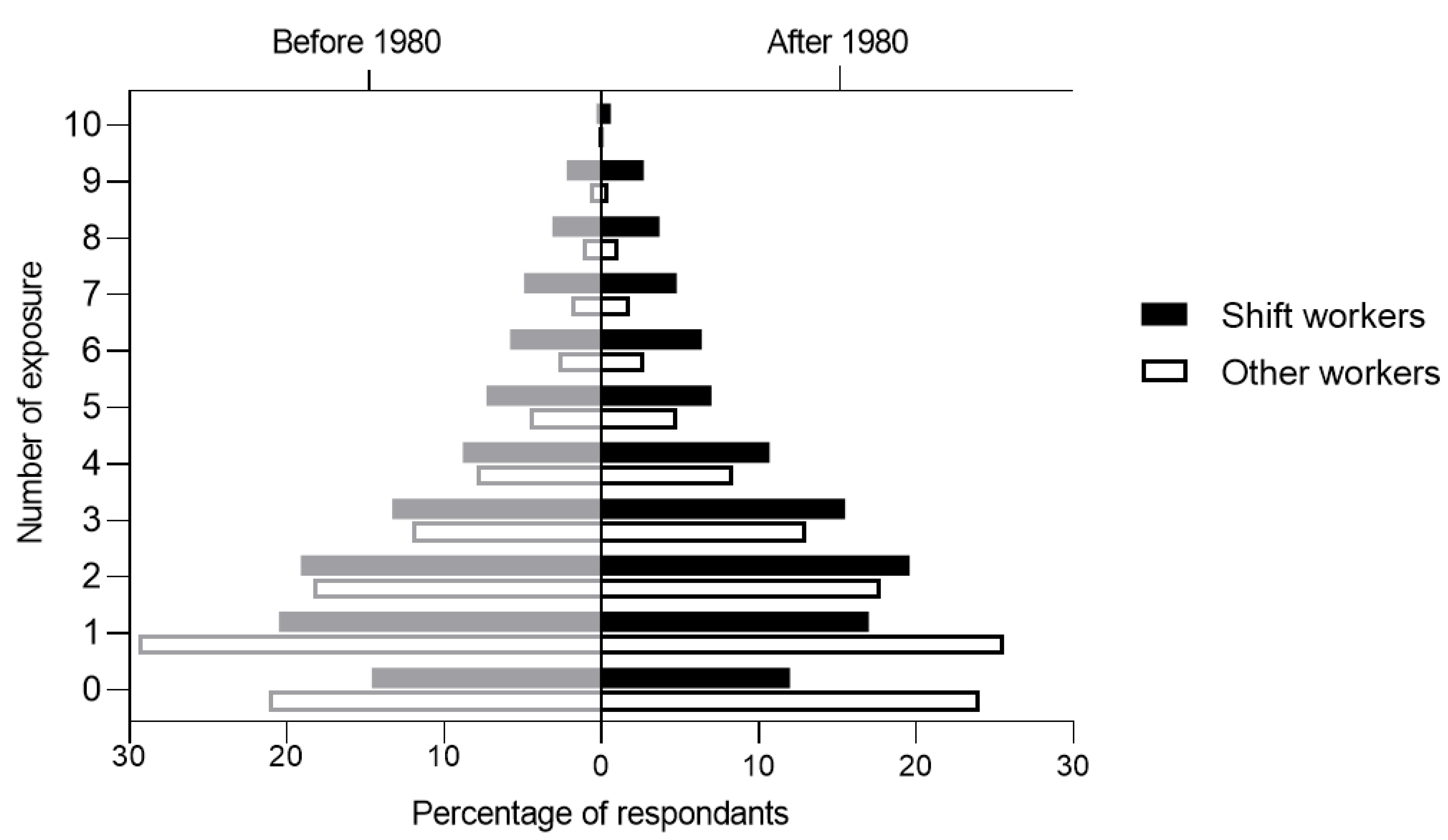
3.1.3. Multiple Hazards Exposure
3.2. Sensitivity Analyses
4. Discussion
5. Conclusions
Supplementary Materials
Availability of Data and Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Ethics Approval and Consent to Participate
References
- Obelenis, V.; Malinauskiene, V. The influence of occupational environment and professional factors on the risk of cardiovascular disease. Medicina 2007, 43, 96. [Google Scholar] [CrossRef] [PubMed]
- Kim, K.-W.; Won, Y.L.; Ko, K.S.; Heo, K.-H.; Chung, Y.H. The Effects of Hazardous Chemical Exposure on Cardiovascular Disease in Chemical Products Manufacturing Workers. Toxicol. Res. 2012, 28, 269–277. [Google Scholar] [CrossRef] [PubMed]
- Rizi, H.A.Y.; Hasanzadeh, A. Noise exposure as a risk factor of cardiovascular diseases in workers. J. Educ. Heal. Promot. 2013, 2, 14. [Google Scholar] [CrossRef] [PubMed]
- Stave, G.M.; Wald, P.H. Physical and Biological Hazards of the Workplace; John Wiley & Sons: Hoboken, NJ, USA, 2016. [Google Scholar]
- Skogstad, M.; Johannessen, H.A.; Tynes, T.; Mehlum, I.S.; Nordby, K.-C.; Lie, A. Systematic review of the cardiovascular effects of occupational noise. Occup. Med. 2016, 66, 10–16. [Google Scholar] [CrossRef] [PubMed]
- Kwak, K.M.; Paek, D.; Zoh, K.-D. Exposure to asbestos and the risk of colorectal cancer mortality: A systematic review and meta-analysis. Occup. Environ. Med. 2019, 76, 861–871. [Google Scholar] [CrossRef] [PubMed]
- Leso, V.; Capitanelli, I.; Lops, E.A.; Ricciardi, W.; Iavicoli, I. Occupational chemical exposure and diabetes mellitus risk. Toxicol. Ind. Health 2016, 33, 222–249. [Google Scholar] [CrossRef] [PubMed]
- Sekhotha, M.M.; Monyeki, K.D.; Sibuyi, M.E. Exposure to Agrochemicals and Cardiovascular Disease: A Review. Int. J. Environ. Res. Public Health 2016, 13, 229. [Google Scholar] [CrossRef]
- Costa, G. Flexibility of working hours in the 24-hour society. Med. Lav. 2006, 97, 280–287. [Google Scholar]
- 5th European Working Conditions Survey: Overview Report; European Foundation for the Improvement of Living and Working Conditions: Dublin, Ireland, 2012.
- Titova, O.E.; Lindberg, E.; Elmståhl, S.; Lind, L.; Schiöth, H.B.; Benedict, C. Association between shift work history and performance on the trail making test in middle-aged and elderly humans: The EpiHealth study. Neurobiol. Aging 2016, 45, 23–29. [Google Scholar] [CrossRef]
- Jacobs, D.I.; Hansen, J.; Fu, A.; Stevens, R.G.; Tjønneland, A.; Vogel, U.; Zheng, T.; Zhu, Y. Methylation alterations at imprinted genes detected among long-term shiftworkers. Environ. Mol. Mutagen. 2012, 54, 141–146. [Google Scholar] [CrossRef]
- Sun, M.; Feng, W.; Wang, F.; Li, P.; Li, Z.; Li, M.; Tse, G.; Vlaanderen, J.; Vermeulen, R.; Tse, L.A. Meta-analysis on shift work and risks of specific obesity types. Obes. Rev. 2017, 19, 28–40. [Google Scholar] [CrossRef] [PubMed]
- Morris, C.J.; Purvis, T.E.; Mistretta, J.; Scheer, F.A.J.L. Effects of the Internal Circadian System and Circadian Misalignment on Glucose Tolerance in Chronic Shift Workers. J. Clin. Endocrinol. Metab. 2016, 101, 1066–1074. [Google Scholar] [CrossRef]
- Lunde, L.-K.; Skare, Ø.; Mamen, A.; Sirnes, P.A.; Aass, H.C.D.; Øvstebø, R.; Goffeng, E.; Matre, D.; Nielsen, P.; Heglum, H.S.A.; et al. Cardiovascular Health Effects of Shift Work with Long Working Hours and Night Shifts: Study Protocol for a Three-Year Prospective Follow-Up Study on Industrial Workers. Int. J. Environ. Res. Public Health 2020, 17, 589. [Google Scholar] [CrossRef]
- Antunes, L.C.; Levandovski, R.; Dantas, G.; Caumo, W.; Hidalgo, M.P. Obesity and shift work: Chronobiological aspects. Nutr. Res. Rev. 2010, 23, 155–168. [Google Scholar] [CrossRef]
- Smolensky, M.H.; Reinberg, A.E.; Fischer, F.M. Working Time Society consensus statements: Circadian time structure impacts vulnerability to xenobiotics—Relevance to industrial toxicology and nonstandard work schedules. Ind. Health 2019, 57, 158–174. [Google Scholar] [CrossRef]
- Bøggild, H.; Burr, H.; Tüchsen, F.; Jeppesen, H.J. Work environment of Danish shift and day workers. Scand. J. Work. Environ. Health 2001, 27, 97–105. [Google Scholar] [CrossRef]
- Jay, S.M.; Gander, P.H.; Eng, A.; Cheng, S.; Douwes, J.; Ellison-Loschmann, L.; McLean, D.; Pearce, N.; ‘Tmannetje, A. New Zealanders working non-standard hours also have greater exposure to other workplace hazards. Chrono Int. 2017, 34, 519–526. [Google Scholar] [CrossRef]
- Parkes, K.R. Shiftwork and environment as interactive predictors of work perceptions. J. Occup. Health Psychol. 2003, 8, 266–281. [Google Scholar] [CrossRef]
- Barlow, C.A.; Sahmel, J.; Paustenbach, D.J.; Henshaw, J.L. History of knowledge and evolution of occupational health and regulatory aspects of asbestos exposure science: 1900–1975. Crit. Rev. Toxicol. 2017, 47, 286–316. [Google Scholar] [CrossRef] [PubMed]
- Drechsel, D.A.; Barlow, C.A.; Bare, J.L.; Jacobs, N.F.; Henshaw, J.L. Historical evolution of regulatory standards for occupational and consumer exposures to industrial talc. Regul. Toxicol. Pharmacol. 2018, 92, 251–267. [Google Scholar] [CrossRef]
- Kennedy, A.; Schulz, S.; Szpejna, M. Health and safety at work Fact Sheets on the European Union European Parliament, March 2020. Available online: https://www.europarl.europa.eu/factsheets/en/sheet/56/health-and-safety-at-work (accessed on 22 June 2020).
- Tynes, T.; Aagestad, C.; Thorsen, S.V.; Andersen, L.L.; Perkio-Makela, M.; García, F.J.P.; Blanco, L.G.; Vermeylen, G.; Parent-Thirion, A.; Hooftman, W.E.; et al. Physical working conditions as covered in European monitoring questionnaires. BMC Public Health 2017, 17, 544. [Google Scholar] [CrossRef] [PubMed]
- Sudlow, C.; Gallacher, J.; Allen, N.; Beral, V.; Burton, P.; Danesh, J.; Downey, P.; Elliott, P.; Green, J.; Landray, M.; et al. UK Biobank: An Open Access Resource for Identifying the Causes of a Wide Range of Complex Diseases of Middle and Old Age. PLoS Med. 2015, 12, e1001779. [Google Scholar] [CrossRef]
- De Matteis, S.; Jarvis, D.; Young, H.; Young, A.; Allen, N.; Potts, J.; Darnton, A.; Rushton, L.; Cullinan, P. Occupational self-coding and automatic recording (OSCAR): A novel web-based tool to collect and code lifetime job histories in large population-based studies. Scand. J. Work. Environ. Health 2016, 43, 181–186. [Google Scholar] [CrossRef]
- Bycroft, C.; Freeman, C.; Petkova, D.; Band, G.; Elliott, L.T.; Sharp, K.; Motyer, A.; Vukcevic, D.; Delaneau, O.; O’Connell, J.; et al. The UK Biobank resource with deep phenotyping and genomic data. Nat. Cell Biol. 2018, 562, 203–209. [Google Scholar] [CrossRef]
- Rukh, G.; Dang, J.; Olivo, G.; Ciuculete, D.-M.; Rask-Andersen, M.; Schiöth, H.B. Personality, lifestyle and job satisfaction: Causal association between neuroticism and job satisfaction using Mendelian randomisation in the UK biobank cohort. Transl. Psychiatry 2020, 10, 1–9. [Google Scholar] [CrossRef]
- Wyse, C.; Celis-Morales, C.; Graham, N.; Fan, Y.; Ward, J.; Curtis, A.M.; Mackay, D.; Smith, D.J.; Bailey, M.E.S.; Biello, S.; et al. Adverse metabolic and mental health outcomes associated with shiftwork in a population-based study of 277,168 workers in UK biobank. Ann. Med. 2017, 49, 411–420. [Google Scholar] [CrossRef] [PubMed]
- De Barros, A.J.D.; Hirakata, V.N. Alternatives for logistic regression in cross-sectional studies: An empirical comparison of models that directly estimate the prevalence ratio. BMC Med Res. Methodol. 2003, 3, 1–13. [Google Scholar] [CrossRef] [PubMed]
- Ye, R.; Gao, Y.; Yang, Y.; Chen, Y. Using log-binomial model for estimating the prevalence ratio. Zhonghua Liu Xing Bing Xue Za Zhi 2010, 31, 576–578. [Google Scholar] [PubMed]
- Nguyen, T.-H.-Y.; Bertin, M.; Bodin, J.; Fouquet, N.; Bonvallot, N.; Roquelaure, Y. Multiple Exposures and Coexposures to Occupational Hazards Among Agricultural Workers: A Systematic Review of Observational Studies. Saf. Heal. Work. 2018, 9, 239–248. [Google Scholar] [CrossRef]
- Guidotti, T.L. Global Occupational Health; Oxford University Press: Oxford, UK, 2011. [Google Scholar] [CrossRef]
- Berthelsen, M.; Pallesen, S.; Bjorvatn, B.; Knardahl, S. Shift schedules, work factors, and mental health among onshore and offshore workers in the Norwegian petroleum industry. Ind. Health 2015, 53, 280–292. [Google Scholar] [CrossRef]
- Verra, S.E.; Benzerga, A.; Jiao, B.; Eruggeri, K. Health Promotion at Work: A Comparison of Policy and Practice Across Europe. Saf. Health Work. 2019, 10, 21–29. [Google Scholar] [CrossRef] [PubMed]
- Di Muzio, M.; Diella, G.D.; Di Simone, E.; Novelli, L.; Alfonsi, V.; Scarpelli, S.; Annarumma, L.; Salfi, F.; Pazzaglia, M.; Giannini, A.M.; et al. Nurses and Night Shifts: Poor sleep quality exacerbates psychomotor performance. Front. Neurosci. 2020, 14. [Google Scholar] [CrossRef]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
| Shift Workers n = 17,239 | Non-Shift Worker n = 102,174 | |
|---|---|---|
| Sex—Female | 46.3 (7986) | 57.2 (58,468) |
| Ethnicity—White British | 89.8 (15,428) | 92.2 (93,857) |
| Education—College or University | 42.4 (7248) | 48.3 (48,991) |
| Age (Mean ± Standard Deviation) | 55.2 ± 7.8 | 56.2 ± 7.6 |
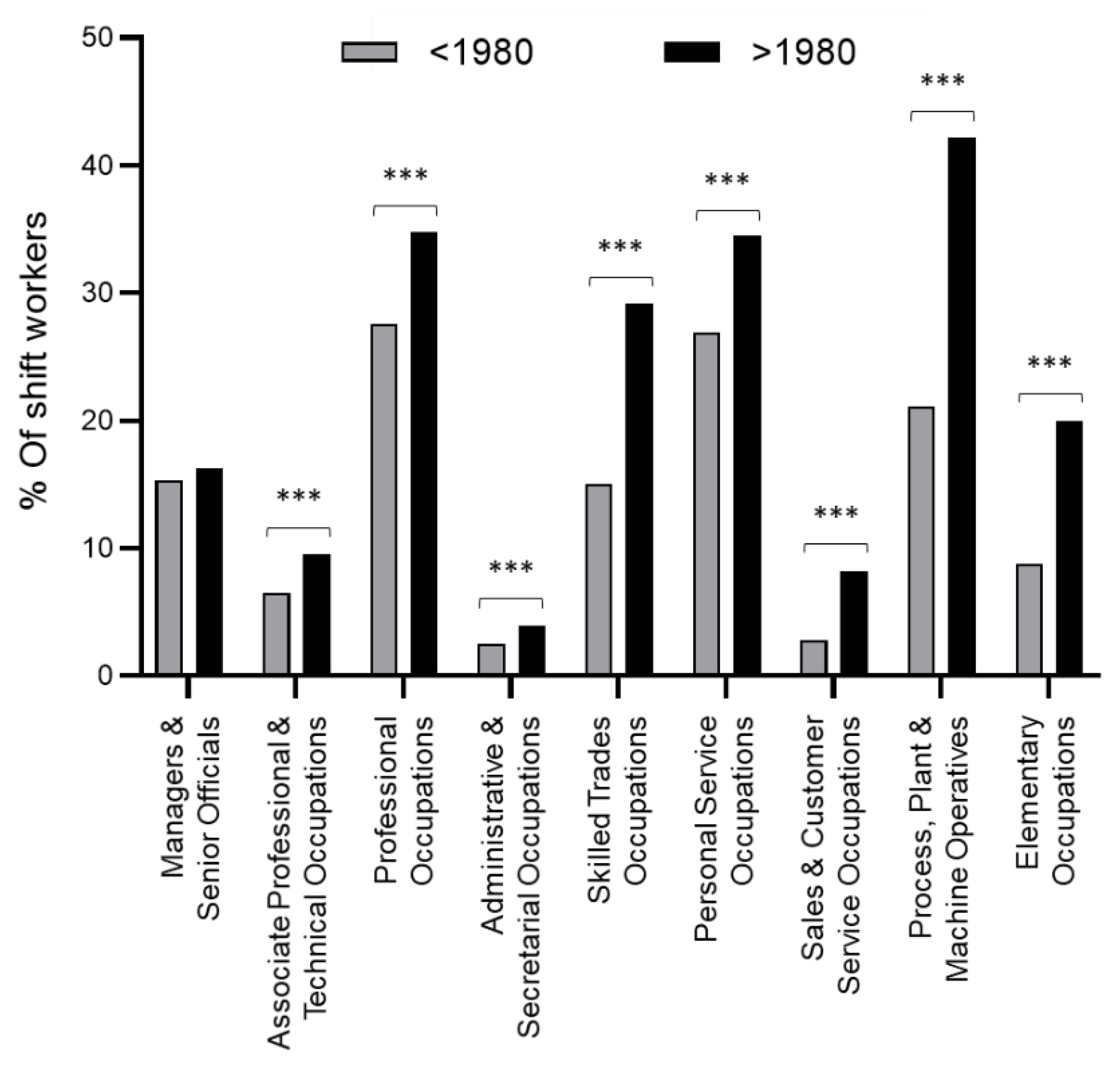
| Managers and Senior Officials | 1361 (7.9) | 7125 (7.0) |
| Professional Occupations | 2898 (16.8) | 32,004 (31.3) |
| Associate Professional and Technical Occupations | 7018 (40.7) | 15,302 (15.0) |
| Administrative and Secretarial Occupations | 772 (4.5) | 24,955 (24.4) |
| Skilled Trades Occupations | 1817 (10.5) | 6.650 (6.5) |
| Personal Service Occupations | 1143 (6.6) | 2.632 (2.6) |
| Sales and Customer Service Occupations | 237 (1.4) | 4768 (4.7) |
| Process, Plant and Machine Operatives | 1089 (6.3) | 2692 (2.6) |
| Elementary Occupations | 904 (5.2) | 6046 (5.9) |
| Job Ended Before 1980 n = 59,692 | Job Ended After 1980 n = 59,721 | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Exposure | % Shift Workers | % Other Workers | PR | 95% CI | p Value | % Shift Workers | % Other Workers | PR | 95% CI | p Value | ||
| Noise | 64.0 | 39.6 | 1.57 | 1.54 | 1.60 | <0.001 | 70.3 | 43.4 | 1.57 | 1.52 | 1.61 | <0.001 |
| Cold | 35.3 | 27.0 | 1.22 | 1.19 | 1.27 | <0.001 | 43.7 | 29.7 | 1.29 | 1.26 | 1.32 | <0.001 |
| Hot | 56.7 | 36.2 | 1.47 | 1.44 | 1.51 | <0.001 | 64.3 | 43.4 | 1.39 | 1.37 | 1.42 | <0.001 |
| Dust | 29.8 | 25.2 | 1.14 | 1.10 | 1.19 | <0.001 | 32.2 | 23.9 | 1.17 | 1.14 | 1.21 | <0.001 |
| Chemical/fumes | 26.2 | 16.1 | 1.49 | 1.43 | 1.56 | <0.001 | 29.5 | 13.8 | 1.81 | 1.75 | 1.88 | <0.001 |
| Smoke | 48.4 | 53.2 | 0.89 | 0.87 | 0.91 | <0.001 | 45.5 | 40.3 | 1.04 | 1.02 | 1.06 | 0.001 |
| Asbestos | 13.6 | 7.1 | 1.55 | 1.44 | 1.66 | <0.001 | 13.1 | 5.9 | 1.54 | 1.44 | 1.64 | <0.001 |
| Paints/thinners/glues | 13.2 | 10.2 | 1.14 | 1.07 | 1.21 | <0.001 | 15.2 | 10.5 | 1.19 | 1.13 | 1.26 | <0.001 |
| Pesticides | 2.0 | 1.8 | 0.98 | 0.81 | 1.17 | 0.79 | 2.8 | 2.0 | 1.15 | 1.01 | 1.32 | 0.037 |
| Diesel exhaust | 16.5 | 6.8 | 1.95 | 1.83 | 2.06 | <0.001 | 20.1 | 6.5 | 2.12 | 2.01 | 2.23 | <0.001 |
| Exposed to ≥2hazards | 64.8 | 49.5 | 1.25 | 1.21 | 1.30 | <0.001 | 71.0 | 50.2 | 1.34 | 1.30 | 1.38 | <0.001 |
| Shift Workers n = 17,239 | Other Workers n = 102,174 | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Exposure | % before 1980 | % after 1980 | PR | 95% CI | p Value | % before 1980 | % after 1980 | PR | 95% CI | p Value | ||
| Noise | 64.0 | 70.3 | 1.05 | 1.03 | 1.08 | <0.001 | 39.6 | 43.4 | 1.14 | 1.12 | 1.16 | <0.001 |
| Cold | 35.3 | 43.7 | 1.16 | 1.11 | 1.20 | <0.001 | 27.0 | 29.7 | 1.10 | 1.08 | 1.13 | <0.001 |
| Hot | 56.7 | 64.3 | 1.08 | 1.06 | 1.12 | <0.001 | 36.2 | 43.4 | 1.20 | 1.18 | 1.22 | <0.001 |
| Dust | 29.8 | 32.2 | 1.05 | 1.01 | 1.10 | 0.019 | 25.2 | 23.9 | 0.94 | 0.92 | 0.97 | <0.001 |
| Chemical/fumes | 26.2 | 29.5 | 1.11 | 1.06 | 1.17 | <0.001 | 16.1 | 13.8 | 0.78 | 0.75 | 0.81 | <0.001 |
| Smoke | 48.4 | 45.5 | 0.94 | 0.91 | 0.97 | <0.001 | 53.2 | 40.3 | 0.79 | 0.78 | 0.80 | <0.001 |
| Asbestos | 13.6 | 13.1 | 1.07 | 0.98 | 1.16 | 0.118 | 7.1 | 5.9 | 0.94 | 0.89 | 0.99 | 0.015 |
| Paints/thinners/glues | 13.2 | 15.2 | 1.09 | 1.00 | 1.20 | 0.054 | 10.2 | 10.5 | 0.97 | 0.93 | 1.01 | 0.161 |
| Pesticides | 2.0 | 2.8 | 1.60 | 1.29 | 1.99 | <0.001 | 1.8 | 2.0 | 1.04 | 0.94 | 1.15 | 0.475 |
| Diesel exhaust | 16.5 | 20.1 | 1.15 | 1.06 | 1.25 | 0.001 | 6.8 | 6.5 | 0.88 | 0.83 | 0.93 | <0.001 |
| Exposed to ≥2hazards | 64.8 | 71.0 | 1.04 | 1.01 | 1.06 | 0.003 | 49.5 | 50.2 | 1.04 | 1.02 | 1.05 | <0.001 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Miguet, M.; Rukh, G.; Titova, O.E.; Schiöth, H.B. Important Difference between Occupational Hazard Exposure among Shift Workers and Other Workers; Comparing Workplace before and after 1980. Int. J. Environ. Res. Public Health 2020, 17, 7495. https://doi.org/10.3390/ijerph17207495
Miguet M, Rukh G, Titova OE, Schiöth HB. Important Difference between Occupational Hazard Exposure among Shift Workers and Other Workers; Comparing Workplace before and after 1980. International Journal of Environmental Research and Public Health. 2020; 17(20):7495. https://doi.org/10.3390/ijerph17207495
Chicago/Turabian StyleMiguet, Maud, Gull Rukh, Olga E. Titova, and Helgi B. Schiöth. 2020. "Important Difference between Occupational Hazard Exposure among Shift Workers and Other Workers; Comparing Workplace before and after 1980" International Journal of Environmental Research and Public Health 17, no. 20: 7495. https://doi.org/10.3390/ijerph17207495
APA StyleMiguet, M., Rukh, G., Titova, O. E., & Schiöth, H. B. (2020). Important Difference between Occupational Hazard Exposure among Shift Workers and Other Workers; Comparing Workplace before and after 1980. International Journal of Environmental Research and Public Health, 17(20), 7495. https://doi.org/10.3390/ijerph17207495





