Repeat Self-Harm Following Hospital-Presenting Intentional Drug Overdose among Young People—A National Registry Study
Abstract
:1. Introduction
2. Materials and Methods
2.1. Setting and Sample
2.2. Data Items
2.3. Statistical Analyses and Reporting
3. Results
3.1. Characteristics of Index and Repeat Self-Harm Presentations
3.2. Characteristics of Repeat Presentations Following an Index Episode of IDO
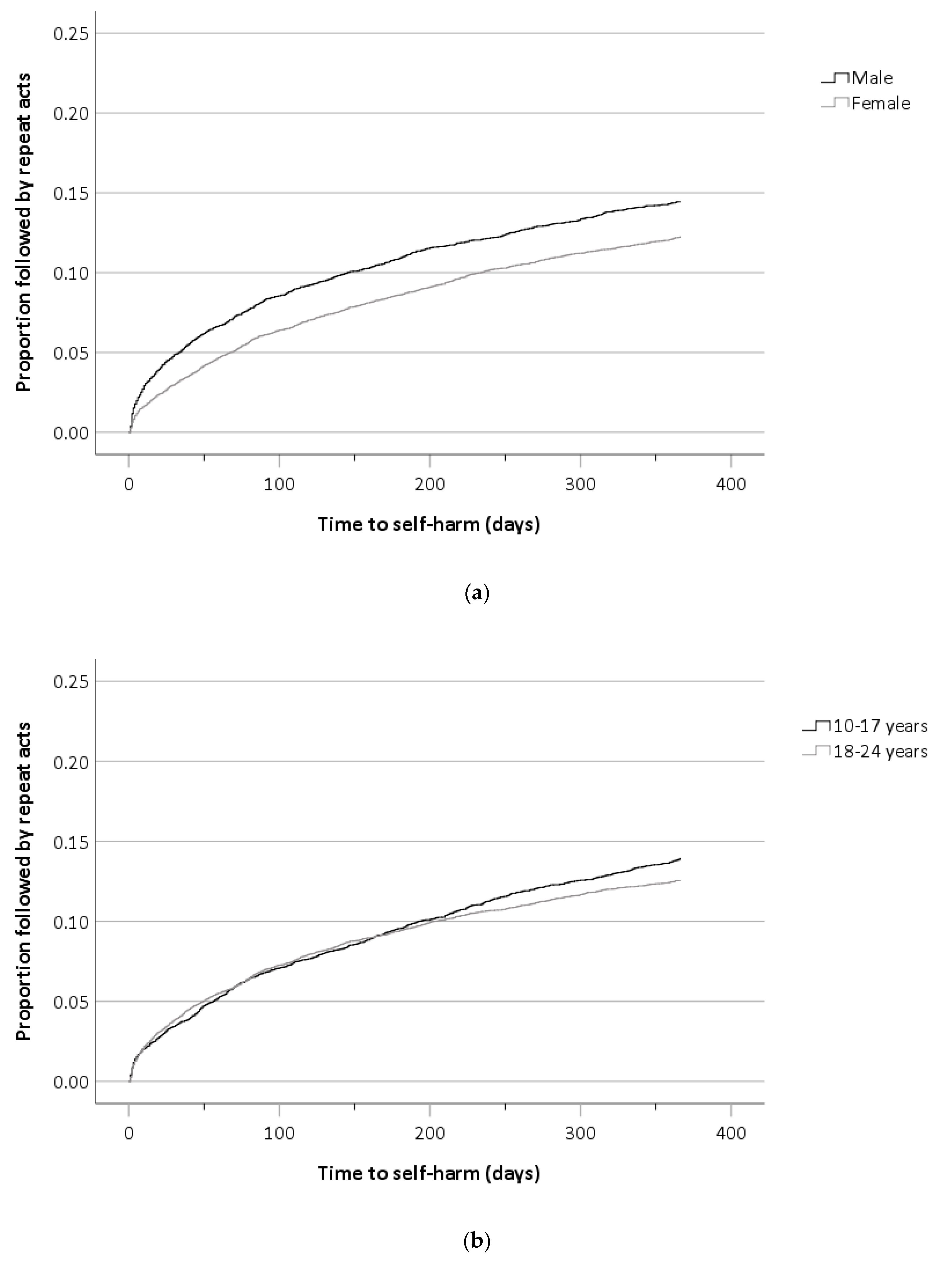
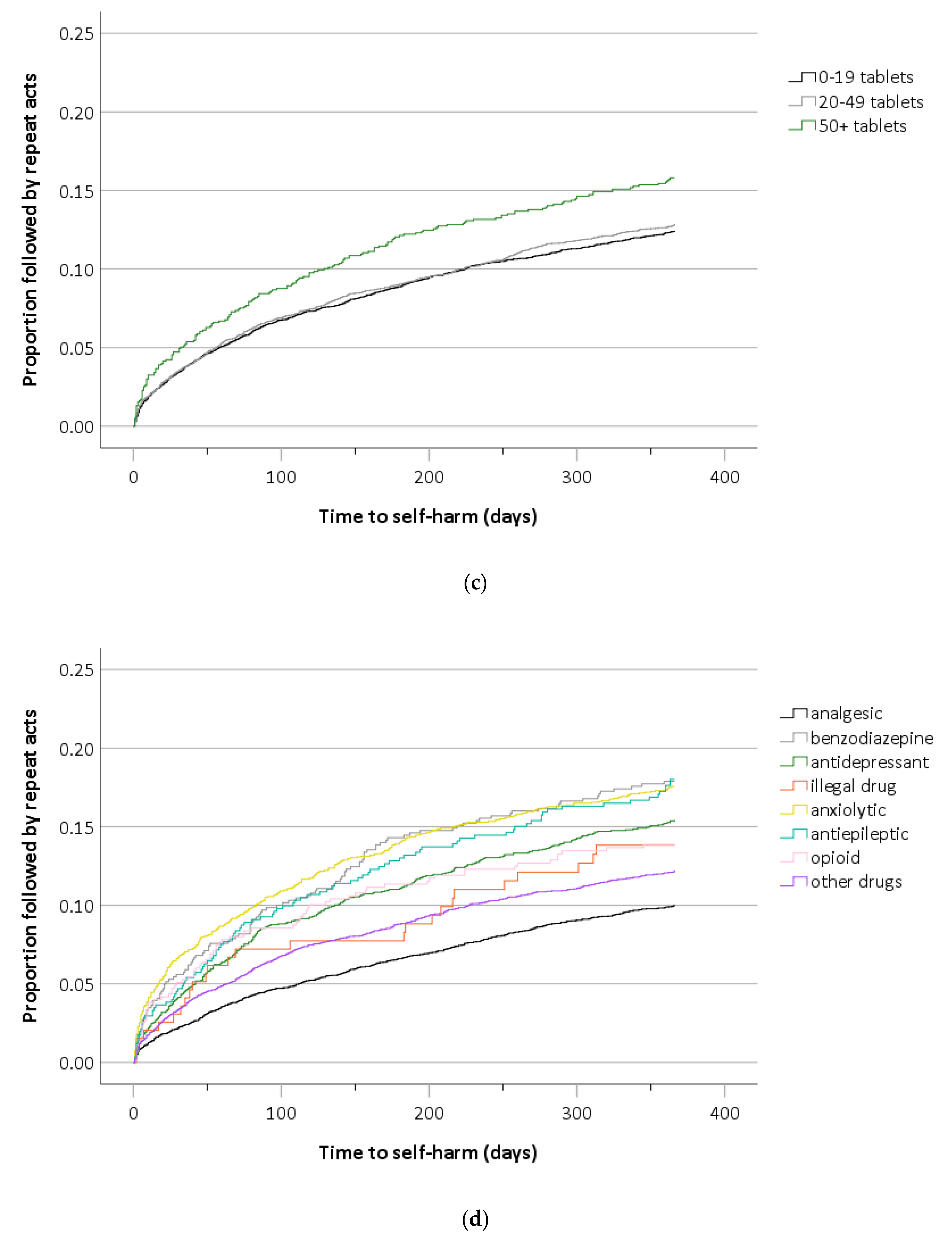
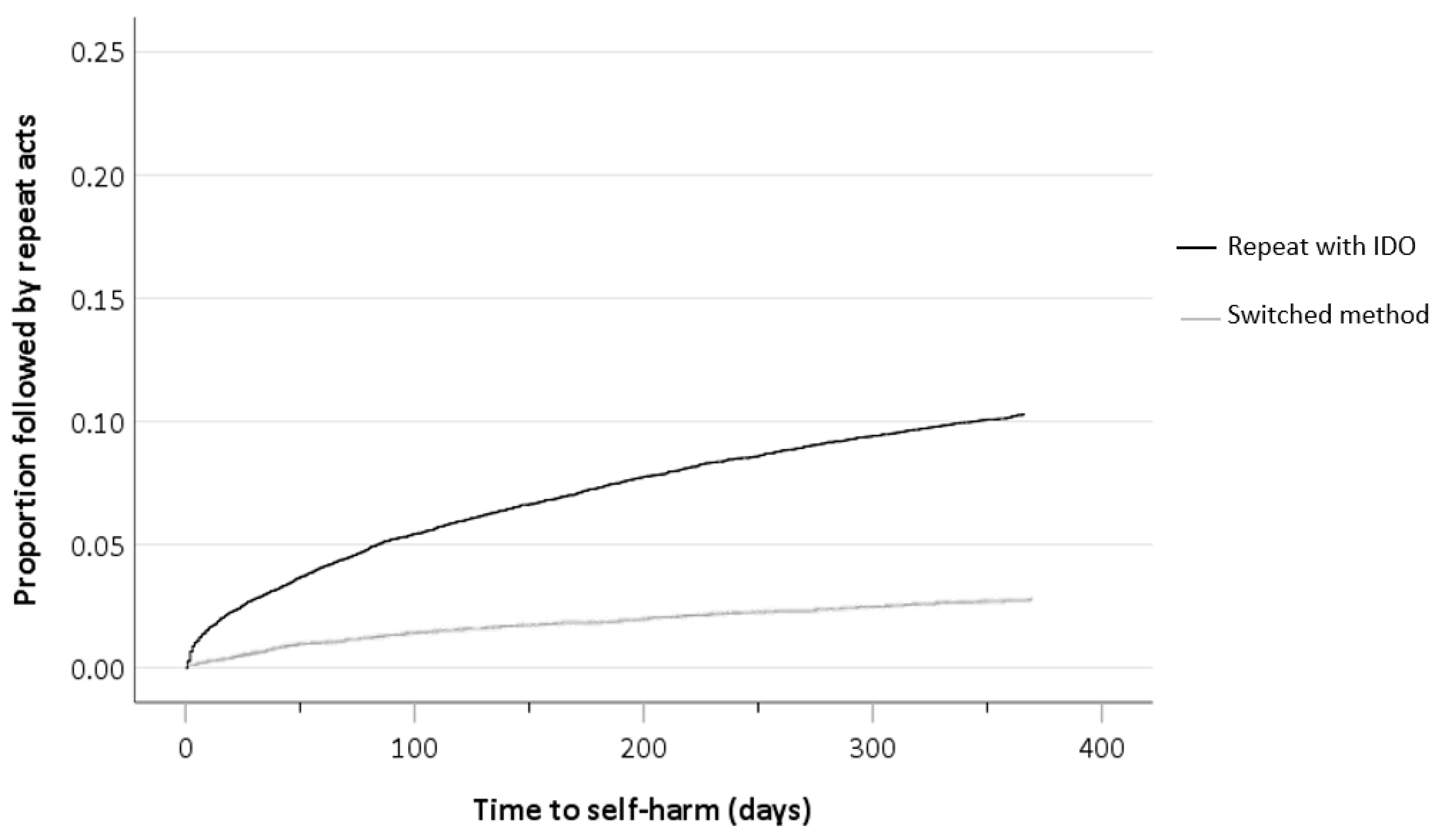
3.3. Methods Used in Self-Harm Repetition
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Griffin, E.; McTernan, N.; Wrigley, C.; Nicholson, S.; Arensman, E.; Williamson, E. National Self-Harm Registry Ireland Annual Report 2018; National Suicide Research Foundation: Cork, Ireland, 2019; Available online: https://www.nsrf.ie/wp-content/uploads/2019/10/NSRF-National-Self-Harm-Registry-Ireland-Annual-Report-2018-for-website.pdf (accessed on 19 June 2020).
- Kwok, C.L.; Yip, P.S.; Gunnell, D.; Kuo, C.J.; Chen, Y.Y. Non-fatal repetition of self-harm in Taipei City, Taiwan: Cohort study. Br. J. Psychiatry 2014, 204, 376–382. [Google Scholar] [CrossRef] [Green Version]
- Griffin, E.; McMahon, E.; McNicholas, F.; Corcoran, P.; Perry, I.J.; Arensman, E. Increasing rates of self-harm among children, adolescents and young adults: A 10-year national registry study 2007–2016. Soc. Psychiatry Psychiatr. Epidemiol. 2018, 53, 663–671. [Google Scholar] [CrossRef] [PubMed]
- Hiscock, H.; Neely, R.J.; Lei, S.; Freed, G. Paediatric mental and physical health presentations to emergency departments, Victoria, 2008–2015. Med. J. Aust. 2018, 208, 343–348. [Google Scholar] [CrossRef] [PubMed]
- Morgan, C.; Webb, R.T.; Carr, M.J.; Kontopantelis, E.; Green, J.; Chew-Graham, C.A.; Kapur, N.; Ashcroft, D.M. Incidence, clinical management, and mortality risk following self harm among children and adolescents: Cohort study in primary care. BMJ 2017, 359, j4351. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Gilley, M.; Sivilotti, M.L.A.; Juurlink, D.N.; Macdonald, E.; Yao, Z.; Finkelstein, Y. Trends of intentional drug overdose among youth: A population-based cohort study. Clin. Toxicol. Phila. 2020, 58, 711–715. [Google Scholar] [CrossRef]
- Tyrrell, E.G.; Orton, E.; Sayal, K.; Baker, R.; Kendrick, D. Differing patterns in intentional and unintentional poisonings among young people in England, 1998–2014: A population-based cohort study. J. Public Health Oxf. 2017, 39, e1–e9. [Google Scholar] [CrossRef] [Green Version]
- Cairns, R.; Karanges, E.A.; Wong, A.; Brown, J.A.; Robinson, J.; Pearson, S.A.; Dawson, A.H.; Buckley, N.A. Trends in self-poisoning and psychotropic drug use in people aged 5–19 years: A population-based retrospective cohort study in Australia. BMJ Open 2019, 9, e026001. [Google Scholar] [CrossRef]
- Hawton, K.; Bergen, H.; Waters, K.; Ness, J.; Cooper, J.; Steeg, S.; Kapur, N. Epidemiology and nature of self-harm in children and adolescents: Findings from the multicentre study of self-harm in England. Eur. Child. Adolesc. Psychiatry 2012, 21, 369–377. [Google Scholar] [CrossRef]
- Hawton, K.; Bale, L.; Brand, F.; Townsend, E.; Ness, J.; Waters, K.; Clements, C.; Kapur, N.; Geulayov, G. Mortality in children and adolescents following presentation to hospital after non-fatal self-harm in the Multicentre Study of Self-harm: A prospective observational cohort study. Lancet Child. Adolesc. Health 2020, 4, 111–120. [Google Scholar] [CrossRef]
- Hawton, K.; Harriss, L. Deliberate self-harm by under-15-year-olds: Characteristics, trends and outcome. J. Child. Psychol. Psychiatry 2008, 49, 441–448. [Google Scholar] [CrossRef]
- Bennardi, M.; McMahon, E.; Corcoran, P.; Griffin, E.; Arensman, E. Risk of repeated self-harm and associated factors in children, adolescents and young adults. BMC Psychiatry 2016, 16, 421. [Google Scholar] [CrossRef] [PubMed]
- Daly, C.; Griffin, E.; Ashcroft, D.M.; Webb, R.T.; Perry, I.J.; Arensman, E. Frequently used drug types and alcohol involvement in intentional drug overdoses in Ireland: A national registry study. Eur. J. Public Health 2018, 28, 681–686. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Finkelstein, Y.; Macdonald, E.M.; Hollands, S.; Sivilotti, M.L.; Hutson, J.R.; Mamdani, M.M.; Koren, G.; Juurlink, D.N. Repetition of intentional drug overdose: A population-based study. Clin. Toxicol. Phila. 2016, 54, 585–589. [Google Scholar] [CrossRef] [PubMed]
- Diggins, E.; Kelley, R.; Cottrell, D.; House, A.; Owens, D. Age-related differences in self-harm presentations and subsequent management of adolescents and young adults at the emergency department. J. Affect. Disord. 2017, 208, 399–405. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Chen, V.C.; Tan, H.K.; Chen, C.Y.; Chen, T.H.; Liao, L.R.; Lee, C.T.; Dewey, M.; Stewart, R.; Prince, M.; Cheng, A.T.A. Mortality and suicide after self-harm: Community cohort study in Taiwan. Br. J. Psychiatry 2011, 198, 31–36. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Perry, I.J.; Corcoran, P.; Fitzgerald, A.P.; Keeley, H.S.; Reulbach, U.; Arensman, E. The incidence and repetition of hospital-treated deliberate self harm: Findings from the world’s first national registry. PLoS ONE 2012, 7, e31663. [Google Scholar] [CrossRef]
- Cully, G.; Corcoran, P.; Leahy, D.; Griffin, E.; Dillon, C.; Cassidy, E.; Shiely, G.; Arensman, E. Method of self-harm and risk of self-harm repetition: Findings from a national self-harm registry. J. Affect. Disord. 2019, 246, 843–850. [Google Scholar] [CrossRef]
- Martin, C.A.; Chapman, R.; Rahman, A.; Graudins, A. A retrospective descriptive study of the characteristics of deliberate self-poisoning patients with single or repeat presentations to an Australian emergency medicine network in a one year period. BMC Emerg. Med. 2014, 14, 21. [Google Scholar] [CrossRef] [Green Version]
- Cooper, J.; Kapur, N.; Dunning, J.; Guthrie, E.; Appleby, L.; Mackway-Jones, K. A clinical tool for assessing risk after self-harm. Ann. Emerg. Med. 2006, 48, 459–466. [Google Scholar] [CrossRef]
- Taylor, D.M.; Cameron, P.A.; Eddey, D. Recurrent overdose: Patient characteristics, habits, and outcomes. J. Accid. Emerg. Med. 1998, 15, 257–261. [Google Scholar] [CrossRef] [Green Version]
- Mayo, J.A. Psychopharmacological roulette: A follow-up study of patients hospitalized for drug overdose. Am. J. Public Health 1974, 64, 616–617. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Witt, K.; Daly, C.; Arensman, E.; Pirkis, J.; Lubman, D. Patterns of self-harm methods over time and the association with methods used at repeat episodes of non-fatal self-harm and suicide: A systematic review. J. Affect. Disord. 2019, 245, 250–264. [Google Scholar] [CrossRef]
- Owens, D.; Kelley, R.; Munyombwe, T.; Bergen, H.; Hawton, K.; Cooper, J.; Ness, J.; Waters, K.; West, R.; Kapur, N. Switching methods of self-harm at repeat episodes: Findings from a multicentre cohort study. J. Affect. Disord. 2015, 180, 44–51. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Huang, Y.C.; Wu, Y.W.; Chen, C.K.; Wang, L.J. Methods of suicide predict the risks and method-switching of subsequent suicide attempts: A community cohort study in Taiwan. Neuropsychiatr. Dis. Treat. 2014, 10, 711–718. [Google Scholar] [PubMed] [Green Version]
- Wang, L.J.; Huang, Y.C.; Lee, S.Y.; Wu, Y.W.; Chen, C.K. Switching suicide methods as a predictor of completed suicide in individuals with repeated self-harm: A community cohort study in northern Taiwan. Aust. N. Z. J. Psychiatry 2015, 49, 65–73. [Google Scholar] [CrossRef] [PubMed]
- Deisenhammer, E.; Kuen, D.; Ing, C.-M.; Kemmler, G.; Defrancesco, M.; Gleissenthall, G.; von Weiss, E. Stability in the choice of method during the period preceding a suicide attempt and in attempt repeaters. Eur. J. Psychiatry 2016, 30, 205–217. [Google Scholar]
- Platt, S.; Bille-Brahe, U.; Kerkhof, A.; Schmidtke, A.; Bjerke, T.; Crepet, P.; de Leo, D.; Haring, C.; Lonnqvist, J.; Michel, K.; et al. Parasuicide in Europe: The WHO/EURO multicentre study on parasuicide. I. Introduction and preliminary analysis for 1989. Acta Psychiatr. Scand. 1992, 85, 97–104. [Google Scholar] [CrossRef]
- Miller, M.; Hempstead, K.; Nguyen, T.; Barber, C.; Rosenberg-Wohl, S.; Azrael, D. Method choice in nonfatal self-harm as a predictor of subsequent episodes of self-harm and suicide: Implications for clinical practice. Am. J. Public Health 2013, 103, e61–e68. [Google Scholar] [CrossRef]
- World Health Organization. Collaborating Centre for Drug Statistics Methodology, Guidelines for ATC Classification and DDD Assignment. 2020. Available online: https://www.whocc.no/atc_ddd_index_and_guidelines/atc_ddd_index/ (accessed on 19 June 2020).
- Misuse of Drugs Act. 1984. Available online: http://www.irishstatutebook.ie/eli/1984/act/18/enacted/en/html (accessed on 19 June 2020).
- Misuse of Drugs Act. 1977. Available online: http://www.irishstatutebook.ie/eli/1977/act/12/enacted/en/html (accessed on 19 June 2020).
- Larkin, C.; di Blasi, Z.; Arensman, E. Risk factors for repetition of self-harm: A systematic review of prospective hospital-based studies. PLoS ONE 2014, 9, e84282. [Google Scholar] [CrossRef]
- Mickey, R.M.; Greenland, S. The impact of confounder selection criteria on effect estimation. Am. J. Epidemiol. 1989, 129, 125–137. [Google Scholar] [CrossRef]
- Zou, G. A modified poisson regression approach to prospective studies with binary data. Am. J. Epidemiol. 2004, 159, 702–706. [Google Scholar] [CrossRef] [PubMed]
- STROBE. Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) Statement: Guidelines for Reporting Observational Studies. 2009. Available online: https://www.strobe-statement.org/index.php?id=available-checklists (accessed on 19 June 2020).
- Rodway, C.; Tham, S.G.; Ibrahim, S.; Turnbull, P.; Windfuhr, K.; Shaw, J.; Kapur, N.; Appleby, L. Suicide in children and young people in England: A consecutive case series. Lancet Psychiatry 2016, 3, 751–759. [Google Scholar] [CrossRef] [Green Version]
- Lee, S.; Dwyer, J.; Paul, E.; Clarke, D.; Treleaven, S.; Roseby, R. Differences by age and sex in adolescent suicide. Aust. N. Z. J. Public Health 2019, 43, 248–253. [Google Scholar] [CrossRef] [PubMed]
- Knipe, D.; Metcalfe, C.; Hawton, K.; Pearson, M.; Dawson, A.; Jayamanne, S.; Konradsen, F.; Eddleston, M.; Gunnell, D. Risk of suicide and repeat self-harm after hospital attendance for non-fatal self-harm in Sri Lanka: A cohort study. Lancet Psychiatry 2019, 6, 659–666. [Google Scholar] [CrossRef] [Green Version]
- Hu, N.; Glauert, R.A.; Li, J.; Taylor, C.L. Risk factors for repetition of a deliberate self-harm episode within seven days in adolescents and young adults: A population-level record linkage study in Western Australia. Aust. N. Z. J. Psychiatry 2016, 50, 154–166. [Google Scholar] [CrossRef]
- Olfson, M.; Wall, M.; Wang, S.; Crystal, S.; Bridge, J.A.; Liu, S.M.; Blanco, C. Suicide after deliberate self-harm in adolescents and young adults. Pediatrics 2018, 141, e20173517. [Google Scholar] [CrossRef] [Green Version]
- Hawton, K.; Haw, C.; Casey, D.; Bale, L.; Brand, F.; Rutherford, D. Self-harm in Oxford, England: Epidemiological and clinical trends, 1996–2010. Soc. Psychiatry Psychiatr. Epidemiol. 2015, 50, 695–704. [Google Scholar] [CrossRef] [Green Version]
- Hawton, K.; Simkin, S.; Gunnell, D.; Sutton, L.; Bennewith, O.; Turnbull, P.; Kapur, N. A multicentre study of coproxamol poisoning suicides based on coroners’ records in England. Br. J. Clin. Pharm. 2005, 59, 207–212. [Google Scholar] [CrossRef] [Green Version]
- Tournier, M.; Grolleau, A.; Cougnard, A.; Molimard, M.; Verdoux, H. Factors associated with choice of psychotropic drugs used for intentional drug overdose. Eur. Arch. Psychiatry Clin. Neurosci. 2009, 259, 86–91. [Google Scholar] [CrossRef]
- Hiremath, M.; Craig, S.; Graudins, A. Adolescent deliberate self-poisoning in South-East Melbourne. Emerg. Med. Australas. 2016, 28, 704–710. [Google Scholar] [CrossRef]
- O’Connor, R.C.; Kirtley, O.J. The integrated motivational-volitional model of suicidal behaviour. Philos. Trans. R. Soc. Lond. Ser. B Biol. Sci. 2018, 373, e268. [Google Scholar] [CrossRef] [Green Version]
- The National Institute for Health and Care Excellence. Depression in Children and Young People: Identification and Management. 2019. Available online: https://www.nice.org.uk/guidance/ng134. (accessed on 19 June 2020).
- Medicines Management Programme. Guidance on Appropriate Prescribing of Benzodiazepines and z-Drugs (BZRA) in the Treatment of Anxiety and Insomnia. 2018. Available online: https://www.hse.ie/eng/about/who/cspd/ncps/medicines-management/bzra-for-anxiety-insomnia/bzraguidancemmpfeb18.pdf (accessed on 19 June 2020).
- Steeg, S.; Quinlivan, L.; Nowland, R.; Carroll, R.; Casey, D.; Clements, C.; Cooper, J.; Davies, L.; Knipe, D.; Ness, J.; et al. Accuracy of risk scales for predicting repeat self-harm and suicide: A multicentre, population-level cohort study using routine clinical data. BMC Psychiatry 2018, 18, 113. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Doak, M.W.; Nixon, A.C.; Lupton, D.J.; Waring, W.S. Self-poisoning in older adults: Patterns of drug ingestion and clinical outcomes. Age Ageing 2009, 38, 407–411. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- The National Institute for Health and Care Excellence. Self-Harm in Over 8s: Long Term Management. NICE Guideline CG16. 2011. Available online: https://www.nice.org.uk/guidance/cg133/resources/selfharm-in-over-8s-longterm-management-pdf-35109508689349 (accessed on 19 June 2020).
- The National Institute for Health and Care Excellence. Suicide Prevention: Optimising Medicines and Reducing Access to Medicines as a Means of Suicide. 2019. Available online: https://www.nice.org.uk/advice/ktt24 (accessed on 19 June 2020).
- O’Driscoil, D.R.J.; Brogan, C.; Henman, M. The DUMP Campaign. Irish Pharmacist. 2019. Available online: http://www.tara.tcd.ie/bitstream/handle/2262/56870/IPJUN09DUMPCAMPAIGN.PDF?sequence=1&isAllowed=y (accessed on 19 June 2020).
- The National Institute for Health and Care Excellence. Depression in Adults with a Chronic Physical Health Problem: Recognition and Management. 2009. Available online: https://www.nice.org.uk/guidance/cg91. (accessed on 19 June 2020).
- Hawton, K.; Bergen, H.; Simkin, S.; Dodd, S.; Pocock, P.; Bernal, W.; Gunnell, D.; Kapur, N. Long term effect of reduced pack sizes of paracetamol on poisoning deaths and liver transplant activity in England and Wales: Interrupted time series analyses. BMJ 2013, 346, f403. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Steeg, S.; Carr, M.J.; Mok, P.L.H.; Pedersen, C.B.; Antonsen, S.; Ashcroft, D.M.; Kapur, N.; Erlangsen, A.; Nordentoft, M.; Webb, R.T. Temporal trends in incidence of hospital-treated self-harm among adolescents in Denmark: National register-based study. Soc. Psychiatry Psychiatr. Epidemiol. 2020, 55, 415–421. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Smyth, B.P.; Daly, A.; Elmusharaf, K.; McDonald, C.; Clarke, M.; Craig, S.; Cullen, W. Legislation targeting head shops selling new psychoactive substances and changes in drug-related psychiatric admissions: A national database study. Early Interv. Psychiatry 2020, 14, 53–60. [Google Scholar] [CrossRef]
- Lilley, R.; Owens, D.; Horrocks, J.; House, A.; Noble, R.; Bergen, H.; Hawton, K.; Casey, D.; Simkin, S.; Murphy, E.; et al. Hospital care and repetition following self-harm: Multicentre comparison of self-poisoning and self-injury. Br. J. Psychiatry 2008, 192, 440–445. [Google Scholar] [CrossRef]
- Arensman, E.; Larkin, C.; Corcoran, P.; Reulbach, U.; Perry, I.J. Factors associated with self-cutting as a method of self-harm: Findings from the Irish National Registry of Deliberate Self-Harm. Eur. J. Public Health 2014, 24, 292–297. [Google Scholar] [CrossRef] [Green Version]
- Health Service Executive. National Clinical Programme for the Assessment and Management of Patients Presenting to the Emergency Department Following Self-Harm. 2016. Available online: https://www.hse.ie/eng/about/who/cspd/ncps/mental-health/self-harm/ (accessed on 19 June 2020).
| Presentation Characteristics | Total Cohort: N = 16,800 | Individuals Repeating with Any Method: N = 2136 | Univariate Model | Multivariate Model f | ||
|---|---|---|---|---|---|---|
| N | N (%) | HR (95% CI) | p | HR (95% CI) | p | |
| Gender | ||||||
| Male | 6197 | 874 (14.1) | 1.21 (1.11–1.31) | ≤0.001 | 1.13 (1.03–1.24) | 0.009 |
| Female | 10,603 | 1262 (11.9) | 1.00 | – | 1.00 | – |
| Age | ||||||
| 10–17 yrs | 6357 | 862 (13.6) | 1.12 (1.02–1.22) | 0.012 | 1.29 (1.18–1.41) | ≤0.001 |
| 18–24 yrs | 10,443 | 1274 (12.2) | 1.00 | – | 1.00 | – |
| Number of Drug Types a | ||||||
| Single drug IDO | 7901 | 1065 (12.0) | 0.89 (0.81–0.96) | 0.005 | 0.97 (0.88–1.06) | 0.493 |
| Multiple drug IDO | 8897 | 1071 (13.6) | 1.00 | – | 1.00 | – |
| Number of Tablets b | ||||||
| 0–19 | 6733 | 812 (12.1) | 1.00 | – | 1.00 | – |
| 20–49 | 4984 | 623 (12.5) | 1.03 (0.93–1.15) | 0.543 | 1.05 (0.94–1.17) | 0.391 |
| ≥50 | 1236 | 190 (15.4) | 1.30 (1.11–1.52) | 0.001 | 1.27 (1.07–1.49) | 0.005 |
| Drug Type c | ||||||
| Analgesic | 7075 | 767 (10.8) | 0.75 (0.69–0.82) | ≤0.001 | 0.92 (0.79–1.07) | 0.261 |
| Benzodiazepine | 3332 | 598 (17.9) | 1.64 (1.50–1.81) | ≤0.001 | 1.67 (1.40–1.98) | ≤0.001 |
| Antidepressant | 2737 | 421 (15.4) | 1.29 (1.16–1.44) | ≤0.001 | 1.36 (1.18–1.56) | ≤0.001 |
| Anxiolytic | 2238 | 391 (17.5) | 1.53 (1.37–1.71) | ≤0.001 | 0.97 (0.81–1.15) | 0.709 |
| Illegal drugs | 1259 | 178 (14.1) | 1.14 (0.98–1.33) | 0.096 | 0.97 (0.82–1.15) | 0.728 |
| Antiepileptic | 606 | 107 (17.7) | 1.43 (1.18–1.74) | ≤0.001 | 1.25 (1.02–1.54) | 0.035 |
| Opioid | 552 | 75 (13.6) | 1.08 (0.86–1.36) | 0.517 | – | – |
| Other drugs | 5042 | 604 (12.0) | 0.91 (0.83–1.00) | 0.055 | 1.10 (0.93–1.30) | 0.274 |
| Method/s | ||||||
| IDO alone | 14,691 | 1789 (12.2) | 1.00 | – | 1.00 | – |
| IDO and self-cutting | 1464 | 240 (16.4) | 1.40 (1.22–1.60) | ≤0.001 | 1.37 (1.20–1.58) | ≤0.001 |
| IDO and hanging | 236 | 41 (17.4) | 1.47 (1.08–2.00) | 0.015 | 1.28 (0.93–1.76) | 0.129 |
| IDO and unspecified method | 154 | 21 (13.6) | 1.17 (0.76–1.80) | 0.467 | 1.11 (0.71–1.71) | 0.650 |
| IDO and poisoning | 99 | 16 (16.2) | 1.36 (0.83–2.22) | 0.224 | 1.25 (0.77–2.05) | 0.365 |
| IDO and drowning | 61 | 8 (13.1) | 1.15 (0.57–2.30) | 0.697 | 1.09 (0.54–2.21) | 0.811 |
| Alcohol Involved d | 4534 | 577 (12.7) | 0.99 (0.90–1.09) | 0.897 | – | – |
| Recommended Next Care | ||||||
| Admitted to a ward | 5556 | 728 (13.1) | 1.10 (1.00–1.21) | 0.046 | 1.09 (0.99–1.20) | 0.079 |
| Admitted to psychiatric ward or unit | 567 | 110 (19.4) | 1.67 (1.37–2.03) | ≤0.001 | 1.51 (1.24–1.85) | ≤0.001 |
| Refused or left without being seen | 1702 | 225 (13.2) | 1.11 (0.96–1.28) | 0.157 | 1.08 (0.93–1.25) | 0.315 |
| Not admitted | 8975 | 1073 (12.0) | 1.00 | – | 1.00 | – |
| Mental Health Assessment e | ||||||
| No | 2337 | 295 (12.6) | 0.97 (0.85–1.11) | 0.689 | – | – |
| Yes | 6501 | 842 (13.0) | 1.00 | – | – | – |
| Presentation Characteristics | Individuals Who Repeated N = 2136 | Individuals Who Switched Method N = 378 | Univariate Model | Multivariate Model d | |||
|---|---|---|---|---|---|---|---|
| N | N (%) | RR (95% CI) | p | RR (95% CI) | p | ||
| Gender | Male | 874 | 194 (22.2) | 1.52 (1.27–1.83) | ≤0.001 | 1.36 (1.11–1.66) | 0.006 |
| Female | 1262 | 184 (14.6) | 1.00 | – | – | – | |
| Age | 10–17 yrs | 862 | 136 (15.8) | 0.83 (0.69–1.01) | 0.083 | 0.89 (0.73–1.09) | 0.309 |
| 18–24 yrs | 1274 | 242 (19.0) | 1.00 | – | |||
| Number of Drug Types a | Single drug IDO | 1065 | 207 (19.4) | 1.22 (1.01–1.46) | 0.057 | 1.25 (1.03–1.52) | 0.045 |
| Multiple drug IDO | 1071 | 171 (16.0) | 1.00 | – | – | – | |
| Number of Tablets b | 0–19 | 812 | 124 (15.3) | 1.00 | – | – | – |
| 20–49 | 623 | 108 (17.3) | 1.14 (0.89–1.44) | 0.335 | – | – | |
| 50+ | 190 | 27 (14.2) | 0.93 (0.63–1.37) | 0.735 | – | – | |
| Drug Type | Analgesic | 767 | 118 (15.4) | 0.81 (0.66–0.99) | 0.058 | 1.01 (0.79–1.31) | 0.925 |
| Benzodiazepine | 598 | 103 (17.2) | 0.96 (0.78–1.18) | 0.746 | – | – | |
| Antidepressant | 421 | 61 (14.5) | 0.78 (0.61–1.01) | 0.082 | 0.93 (0.70–1.24) | 0.657 | |
| Illegal drugs | 178 | 54 (30.3) | 1.83 (1.43–2.34) | ≤0.001 | 1.63 (1.25–2.14) | 0.003 | |
| Anxiolytic | 391 | 64 (16.4) | 0.91 (0.71–1.16) | 0.490 | – | – | |
| Antiepileptic | 107 | 19 (17.8) | 1.00 (0.66–1.53) | 0.988 | – | – | |
| Opioid | 75 | 11 (14.7) | 0.82 (0.47–1.43) | 0.526 | – | – | |
| Other drugs | 604 | 126 (20.9) | 1.27 (1.05–1.54) | 0.029 | 1.10 (0.86–1.41) | 0.498 | |
| Alcohol Involved | Yes | 577 | 113 (19.6) | 1.15 (0.94–1.41) | 0.208 | – | – |
| Recommended Next Care | Admitted to a ward | 728 | 125 (17.2) | 1.02 (0.83–1.25) | 0.879 | – | – |
| Admitted to psychiatric ward or unit | 110 | 20 (18.2) | 1.08 (0.71–1.64) | 0.750 | – | – | |
| Refused or left without being seen | 225 | 52 (23.1) | 1.37 (1.04–1.80) | 0.045 | 1.23 (0.94–1.62) | 0.191 | |
| Not admitted | 1073 | 181 (16.9) | 1.00 | – | – | – | |
| Mental Health Assessment c | No | 295 | 49 (16.6) | 0.92 (0.67–1.23) | 0.612 | – | – |
| Yes | 842 | 152 (18.1) | 1.00 | – | – | – | |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Daly, C.; Griffin, E.; McMahon, E.; Corcoran, P.; Webb, R.T.; Witt, K.; Ashcroft, D.M.; Arensman, E. Repeat Self-Harm Following Hospital-Presenting Intentional Drug Overdose among Young People—A National Registry Study. Int. J. Environ. Res. Public Health 2020, 17, 6159. https://doi.org/10.3390/ijerph17176159
Daly C, Griffin E, McMahon E, Corcoran P, Webb RT, Witt K, Ashcroft DM, Arensman E. Repeat Self-Harm Following Hospital-Presenting Intentional Drug Overdose among Young People—A National Registry Study. International Journal of Environmental Research and Public Health. 2020; 17(17):6159. https://doi.org/10.3390/ijerph17176159
Chicago/Turabian StyleDaly, Caroline, Eve Griffin, Elaine McMahon, Paul Corcoran, Roger T. Webb, Katrina Witt, Darren M. Ashcroft, and Ella Arensman. 2020. "Repeat Self-Harm Following Hospital-Presenting Intentional Drug Overdose among Young People—A National Registry Study" International Journal of Environmental Research and Public Health 17, no. 17: 6159. https://doi.org/10.3390/ijerph17176159
APA StyleDaly, C., Griffin, E., McMahon, E., Corcoran, P., Webb, R. T., Witt, K., Ashcroft, D. M., & Arensman, E. (2020). Repeat Self-Harm Following Hospital-Presenting Intentional Drug Overdose among Young People—A National Registry Study. International Journal of Environmental Research and Public Health, 17(17), 6159. https://doi.org/10.3390/ijerph17176159








