Factors Influencing Patient Adherence to Tuberculosis Treatment in Ethiopia: A Literature Review
Abstract
1. Introduction
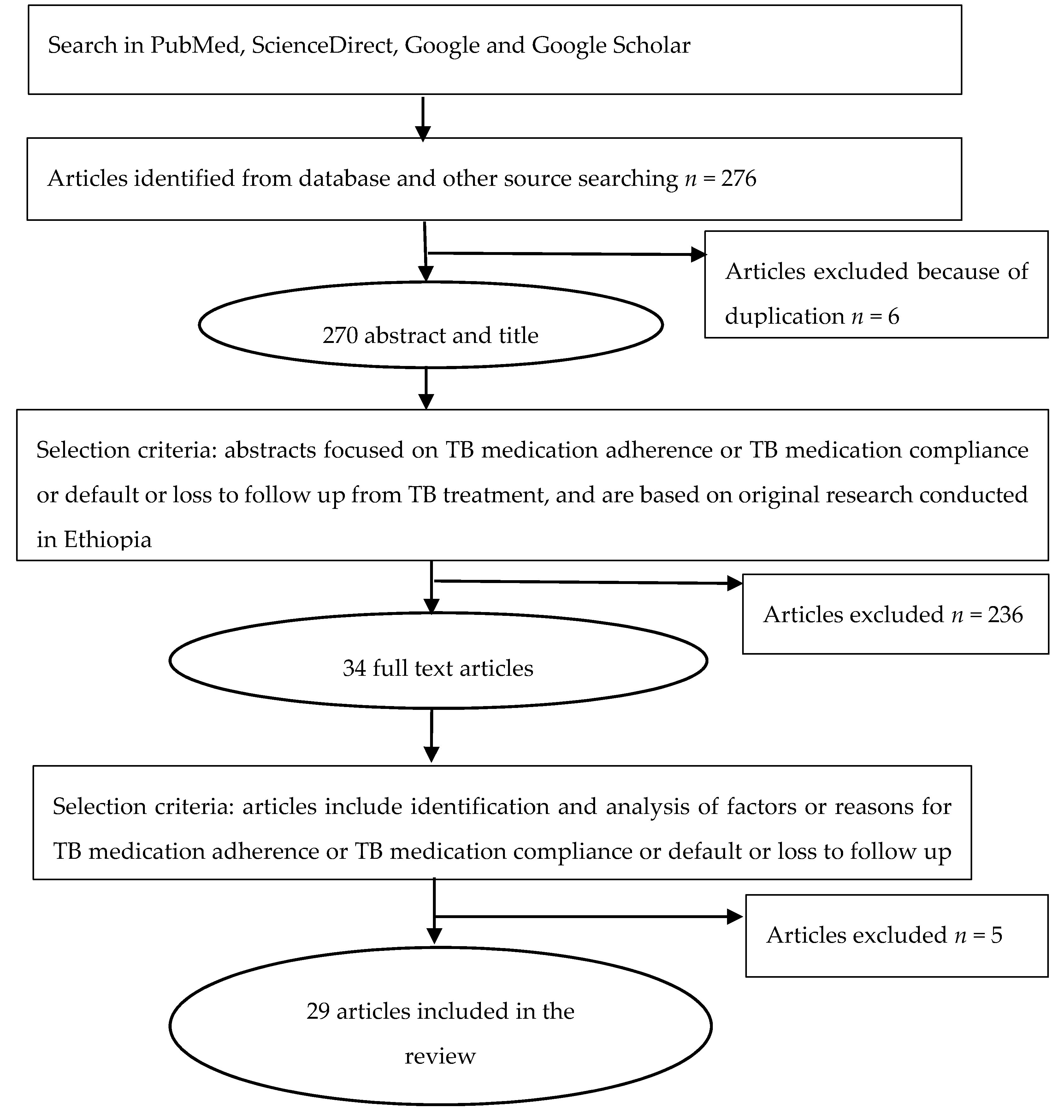
2. Methods
3. Findings
3.1. Patient-Centred Factors
3.2. Social Factors
3.3. Economic Factors
3.4. Health System Factors
3.5. Therapy Factors
3.6. Lifestyle Factors
3.7. Geographical Access Factors
4. Discussion
5. Limitations
6. Conclusions
Definition of Term
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Appendix A
| First Author (Year) | Region | Study Design | Sample Size | Population | Associated Factors of Non-Adherence to TB Medication and Loss to Follow up/Default from TB Treatment |
|---|---|---|---|---|---|
| Daba et al. (2019) [27] | Oromia | Prospective cohort | 268 | Active TB patients | Khat (herbal stimulant) and alcohol use was associated with non-adherence with TB medication. Educational and occupational status were also associated with non-adherence to TB medication. |
| Sahile et al. (2018) [13] | Addis Ababa | A qualitative study | 10 | Active TB patients | Forgetfulness is the factor of TB medication non-adherence. The perceived risk and perceived wellness were also associated with TB medication non-adherence. |
| Mekonnen et al. (2018) [14] | Amhara | Cross-sectional study | 314 | Active TB patients | Being in the continuation phase of treatment, the presence of more than one co-morbidity, inadequate knowledge of TB and its treatment, poor patient–provider relationships, and alcohol use were statistically associated non-adherence to TB treatment. Additionally, forgetting to take medication, being busy with work, and out of home/town were the reasons mentioned by patients for non-adherence. |
| Gube et al. (2018) [40] | SNNPR | Cross-sectional study | 271 | Active TB patients | Drug side effects, a far distance from the health facility, and prolonged wait time to get healthcare service were statistically associated with non-adherence. |
| Woimo et al. (2017) [22] | SNNPR | Cross-sectional study | 261 | Active pulmonary TB patients | Inadequate knowledge of TB and its treatment, health information at each medication refill visits, a far distance from a health facility (more than 10 km), transportation cost, and cost of medications other than anti-TB. |
| Tola et al. (2017) [28] | Addis Ababa | Cross-sectional study | 698 | Active TB patients | Perceived barrier over and perceived benefits directly associated with non-adherence TB medication. Cue to action and psychological distress were indirectly influence non-adherence mediated through perceived barriers and benefits. |
| Tola et al. (2017) [29] | Addis Ababa | Cross-sectional study | 698 | Active TB patients | ART status, economic status, alcohol use, perceived barrier, and psychological distress were statistically associated with non-adherence to TB medication. |
| Gugsa et al. (2017) [36] | SNNPR | A qualitative study | 22 | Active TB patients | Lack of adequate food, poor communication between healthcare providers and patients, beliefs in traditional healing, unavailability of the healthcare service in nearby, drug side-effect and pill burden, stigma, and discrimination. |
| Getahun et al. 2017 [32] | Addis Ababa | Mixed method design | 649 | Active TB patients and healthcare provider | Among lost to follow-up patients inadequate information about TB, healthcare provider–patient relationship (respect and value to patients), lack of support such as transport and nutrition support, and less commitment of healthcare provider towards the patients were reported as reasons for lost to follow-up. |
| Ayele et al. (2017) [15] | Amhara | Cross-sectional study | 154 | Latent TB-HIV patients | Lack of information about isoniazid preventive therapy (IPT), drug side effect, forgetfulness, and being away from home were found as factors for non-adherence to isoniazid preventive therapy (IPT). |
| Diriba et al. (2016) [26] | Oromia | Cross-sectional study | 67 | Active TB patients | Lack of family support, a far distance from the health facility, drug side-effects, extremely ill, feeling better, education level, and being HIV positive were the factors that led to non-adherence to TB medication. |
| Ayele et al. (2016) [37] | SNNPR | Prospective cohort | 162 | Latent TB-HIV patients | Patients experiencing a high level of HIV stigma and having opportunistic infections statistically associated with non-adherence to isoniazid preventive therapy (IPT). |
| Tesfahuneygn et al. 2015 [16] | Amhara | Cross-sectional study | 200 | Active TB patients | Forgetfulness, being away from home, drug side effects, being unable to go to the health facilities on the date of appointment, being hospitalized, TB-HIV infected, alcohol use, smoking, khat (herbal stimulant) chewing, unsatisfied with healthcare service, and long waiting time to get the health service were significantly associated. |
| Yasin et al. (2015) [17] | Oromia | Cross-sectional study | 53 | Active TB-HIV co-infected | Forgetfulness, a far distance from the health facility, and low income were the factors for non-adherence to TB medication. |
| Mindachew et al. (2014) [18] | Addis Ababa | A qualitative study | 12 | Latent TB-HIV patients | Forgetfulness, lack of patient information, knowledge about the disease and its treatment, mental health status make them reluctant to attend follow-up and clinic appointment, not disclosing their HIV status to their family members because of fear of stigma and discrimination and lack of support from family led them to non-adhere to isoniazid preventive therapy (IPT). |
| Kiros et al. (2014) [23] | Tigray | Cross-sectional study | 278 | Active TB patients | The drug side effect and knowledge about TB prevention were associated with non-adherence to TB medication. |
| Eticha et al. (2014) [19] | Tigray | Cross-sectional study | 120 | Active TB-HIV co-infected | Patients who do not have caregivers and people who do not have to remind them to take their medications more likely non-adhere to TB medications. Forgetfulness, feeling sick, and being far away from health facilities were the mention of the main reasons of the TB-HIV co-infected patients for missing medication. |
| Berhe et al. (2014) [34] | Addis Ababa | Cross-sectional study | 381 | Latent TB-HIV patients | Patients who took their medication for ≥ 5 or months were highly likely to be adherent compared to those who took it for 1-2 months. Patients’ friends’ decision to take the medication made them less likely to be non-adherent to isoniazid preventive therapy (IPT). |
| Nezenega et al. (2011) [39] | SNNPR | Cross-sectional study | 531 | Active TB patients | Employment status, area of residence, perceived time spent with a healthcare provider, perceived accessibility, perceived waiting time, perceived professional care, and overall patient satisfaction were associated with non-adherence to TB medication. |
| Adane et al. (2013) [20] | Amhara | Cross-sectional study | 280 | Active TB patients | Forgetfulness, being in the continuation phase, HIV co-infection, and persistent symptoms of tuberculosis were the factors for non-adherence to TB medication. |
| Tadesse et al. (2013) [30] | Amhara | A qualitative | 26 | Active TB | Access to health facilities, financial burdens, quality of health services, and social support were the main reason for failing to fully adhere to TB medication. |
| Kebede et al. (2012) [21] | SNNPR | Cross-sectional study | 24 | Active TB-HIV co-infected | The educational status was associated with non-adherence to TB medication. Forgetfulness and transportation cost were mentioned as reasons for non-adherence to medication. |
| Mindachew et al. (2011) [35] | Addis Ababa | Cross-sectional study | 319 | Latent TB-HIV patients | Patients who did not receive information about IPT, patients not comfortable taking IPT in front of other people, patients who did not attend regular clinic appointments, and drug side effects were associated to non-adherence to isoniazid preventive therapy (IPT). |
| Gebremariam et al. (2010) [31] | Addis Ababa | A qualitative study | 38 | Active TB-HIV co-infected and healthcare providers | Side effects, pill burden, economic constraints, lack of food, stigma with lack of disclosure, and lack of adequate communication with health professionals were barriers for adherence. While beliefs in the curability of TB, beliefs in the severity of TB in the presence of HIV infection and lack of support from families and health professionals influenced non-adherence to TB medication. |
| Mesfin et al. (2009) [38] | Tigray | Cross-sectional | 237 | Active TB patients | Lack of supervision and incapability of dealing with patients’ illness more likely to interrupt and default from treatment. |
| Sagbakken et al. (2008) [33] | Addis Ababa | A qualitative study | 50 | Active TB patients, healthcare providers and relatives | Transportation costs, poor health status due to illness or slow progression, not having social support, and not managing to restore their health and social status were factors for non-adherence. |
| Shargie et al. (2007) [41] | SNNPR | Prospective cohort study | 404 | Active TB patients | Continuation phase of treatment, a far distance from the treatment centre, and necessity to use public transport were the factors for default from TB treatment. |
| Michael et al. (2004) [25] | Oromia | Cross-sectional study | 114 | Defaulted TB patients | Far distance from the health institution, transportation cost, and being unaware about TB were the major reasons contributing to defaulting. |
| Tekle et al. (2002) [24] | Oromia | Case-control | 1367 | Active TB patients | Being in the continuation phase of treatment, lack of family support, inadequate knowledge about treatment duration and drug side effects. |
References
- World Health Organization. Global Tuberculosis Report 2019; WHO: Geneva, Switzerland, 2019. [Google Scholar]
- Deribew, A.; Deribe, K.; Dejene, T.; Tessema, G.A.; Melaku, Y.A.; Lakew, Y.; Amare, A.T.; Bekele, T.; Abera, S.F.; Dessalegn, M.; et al. Tuberculosis Burden in Ethiopia from 1990 to 2016: Evidence from the Global Burden of Diseases 2016 Study. Ethiop. J. Health Sci. 2018, 28, 519–528. [Google Scholar]
- World Health Organization. Treatment of Tuberculosis Guidelines for National Programmes; WHO: Geneva, Switzerland, 2003. [Google Scholar]
- Awofeso, N. Anti-tuberculosis medication side-effects constitute major factor for poor adherence to tuberculosis treatment. Bull. World Health Organ. 2008, 86, B–D. [Google Scholar] [CrossRef]
- World Health Organization. Adherence to Long-Term Therapies Evidence for Action; WHO: Geneva, Switzerland, 2003. [Google Scholar]
- World Health Organization. An expanded DOTS framework for effective tuberculosis control. Int. J. Tuberc. Lung Dis. 2002, 6, 378–388. [Google Scholar]
- Fiseha, D.; Demissie, M. Assessment of Directly Observed Therapy (DOT) following tuberculosis regimen change in Addis Ababa, Ethiopia: A qualitative study. BMC Infect. Dis. 2015, 15, 405. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Zegeye, A.; Dessie, G.; Wagnew, F.; Gebrie, A.; Islam, S.M.S.; Tesfaye, B.; Kiross, D. Prevalence and determinants of anti-tuberculosis treatment non-adherence in Ethiopia: A systematic review and meta-analysis. PLoS ONE 2019, 14, e0210422. [Google Scholar] [CrossRef] [PubMed]
- Tola, H.H.; Holakouie-Naieni, K.; Tesfaye, E.; Mansournia, M.A.; Yaseri, M. Prevalence of tuberculosis treatment non-adherence in Ethiopia: A systematic review and meta-analysis. Int. J. Tuberc. Lung Dis. 2019, 23, 741–749. [Google Scholar] [CrossRef]
- Osterberg, L.; Blaschke, T. Adherence to medication. N. Engl. J. Med. 2005, 353, 487–497. [Google Scholar] [CrossRef] [PubMed]
- Subbaraman, R.; de Mondesert, L.; Musiimenta, A.; Pai, M.; Mayer, K.H.; Thomas, B.E.; Haberer, J. Digital adherence technologies for the management of tuberculosis therapy: Mapping the landscape and research priorities. BMJ Glob. Health 2018, 3, e001018. [Google Scholar] [CrossRef] [PubMed]
- Ogundele, O.A.; Moodley, D.; Seebregts, C.J.; Pillay, A.W. (Eds.) An ontology for tuberculosis treatment adherence behaviour. In SAICSIT 2015, Proceedings of the 2015 Annual Research Conference on South African Institute of Computer Scientists and Information Technologists, Stellenbosch, South Africa, 28–30 September 2015; Association for Computing Machinery: New York, NY, USA, 2015. [Google Scholar]
- Sahile, Z.; Yared, A.; Kaba, M. Patients’ experiences and perceptions on associates of TB treatment adherence: A qualitative study on DOTS service in public health centers in Addis Ababa, Ethiopia. BMC Public Health 2018, 18, 462. [Google Scholar] [CrossRef]
- Mekonnen, H.S.; Azagew, A.W. Non-adherence to anti-tuberculosis treatment, reasons and associated factors among TB patients attending at Gondar town health centers, Northwest Ethiopia. BMC Res. Notes 2018, 11, 691. [Google Scholar] [CrossRef]
- Ayele, A.A.; Asrade Atnafie, S.; Balcha, D.D.; Weredekal, A.T.; Woldegiorgis, B.A.; Wotte, M.M.; Gebresillasie, B.M. Self-reported adherence and associated factors to isoniazid preventive therapy for latent tuberculosis among people living with HIV/AIDS at health centers in Gondar town, North West Ethiopia. Patient Prefer. Adher. 2017, 11, 743–749. [Google Scholar] [CrossRef] [PubMed]
- Tesfahuneygn, G.; Medhin, G.; Legesse, M. Adherence to Anti-tuberculosis treatment and treatment outcomes among tuberculosis patients in Alamata District, northeast Ethiopia. BMC Res. Notes 2015, 8, 503. [Google Scholar] [CrossRef] [PubMed]
- Yasin Mohammed, A.; Kaso Adem, M. Treatment Adherence among Tuberculosis and Human Immuno Deficiency Virus Coinfected Patients in Ginnir Referral Hospital. Am. J. Public Health Res. 2014, 2, 239–243. [Google Scholar] [CrossRef]
- Mindachew, M.; Deribew, A.; Memiah, P.; Biadgilign, S. Perceived barriers to the implementation of Isoniazid preventive therapy for people living with HIV in resource constrained settings: A qualitative study. Pan Afr. Med. J. 2014, 17, 26. [Google Scholar] [CrossRef]
- Eticha, T.; Kassa, E. Non-adherence to anti-TB drugs and its predictors among TB/HIV co-infected patients in Mekelle, Ethiopia. J. Bioanal. Biomed. 2014, 6, 061–064. [Google Scholar] [CrossRef]
- Adane, A.A.; Alene, K.A.; Koye, D.N.; Zeleke, B.M. Non-adherence to anti-tuberculosis treatment and determinant factors among patients with tuberculosis in northwest Ethiopia. PLoS ONE 2013, 8, e78791. [Google Scholar] [CrossRef]
- Kebede, A.; Wabe, N.T. Medication adherence and its determinants among patients on concomitant tuberculosis and antiretroviral therapy in South West Ethiopia. N. Am. J. Med. Sci. 2012, 4, 67–71. [Google Scholar]
- Woimo, T.T.; Yimer, W.K.; Bati, T.; Gesesew, H.A. The prevalence and factors associated for anti-tuberculosis treatment non-adherence among pulmonary tuberculosis patients in public health care facilities in South Ethiopia: A cross-sectional study. BMC Public Health 2017, 17, 269. [Google Scholar] [CrossRef]
- Kiros, Y.K.; Teklu, T.; Desalegn, F.; Tesfay, M.; Klinkenberg, E.; Mulugeta, A. Adherence to anti-tuberculosis treatment in Tigray, Northern Ethiopia. Public Health Action 2014, 4 (Suppl. 3), S31–S36. [Google Scholar] [CrossRef]
- Tekle, B.; Mariam, D.H.; Ali, A. Defaulting from DOTS and its determinants in three districts of Arsi Zone in Ethiopia. Int. J. Tuberc. Lung Dis. 2002, 6, 573–579. [Google Scholar]
- Michael, K.W.; Belachew, T.; Jira, C. Tuberculosis defaulters from the “dots” regimen in Jimma zone, southwest Ethiopia. Ethiop. Med. J. 2004, 42, 247–253. [Google Scholar] [PubMed]
- Diriba Daksa, M.; Melaku Kebede, T.; Dahjejot, M. Patients’ adherence to anti-tuberculosis medicines and associated factors for non-adherence at a tertiary teaching hospital, South West Ethiopia. Eur. J. Ther. 2016, 22, 55–62. [Google Scholar]
- Daba, M.; Tesfaye, M.; Adorjan, K.; Krahl, W.; Tesfaye, E.; Yitayih, Y.; Strobl, R.; Grill, E. Khat and Alcohol Use Disorders Predict Poorer Adherence to Anti-Tuberculosis Medications in Southwest Ethiopia: A Prospective Cohort Study. Prepr. Lancet 2019. [Google Scholar] [CrossRef]
- Tola, H.H.; Karimi, M.; Yekaninejad, M.S. Effects of sociodemographic characteristics and patients’ health beliefs on tuberculosis treatment adherence in Ethiopia: A structural equation modelling approach. Infect. Dis. Poverty 2017, 6, 167. [Google Scholar] [CrossRef] [PubMed]
- Tola, H.H.; Garmaroudi, G.; Shojaeizadeh, D.; Tol, A.; Yekaninejad, M.S.; Ejeta, L.T.; Kebede, A.; Kassa, D. The Effect of Psychosocial Factors and Patients’ Perception of Tuberculosis Treatment Non-Adherence in Addis Ababa, Ethiopia. Ethiop. J. Health Sci. 2017, 27, 447–458. [Google Scholar]
- Tadesse, T.; Demissie, M.; Berhane, Y.; Kebede, Y.; Abebe, M. Long distance travelling and financial burdens discourage tuberculosis DOTs treatment initiation and compliance in Ethiopia: A qualitative study. BMC Public Health 2013, 13, 424. [Google Scholar] [CrossRef]
- Gebremariam, M.K.; Bjune, G.A.; Frich, J.C. Barriers and facilitators of adherence to TB treatment in patients on concomitant TB and HIV treatment: A qualitative study. BMC Public Health 2010, 10, 651. [Google Scholar] [CrossRef]
- Getahun, B.; Nkosi, Z.Z. Is directly observed tuberculosis treatment strategy patient-centered? A mixed method study in Addis Ababa, Ethiopia. PLoS ONE 2017, 12, e0181205. [Google Scholar] [CrossRef]
- Sagbakken, M.; Frich, J.C.; Bjune, G. Barriers and enablers in the management of tuberculosis treatment in Addis Ababa, Ethiopia: A qualitative study. BMC Public Health 2008, 8, 11. [Google Scholar] [CrossRef]
- Berhe, M.; Demissie, M.; Tesfaye, G. Isoniazid preventive therapy adherence and associated factors among HIV positive patients in Addis Ababa, Ethiopia. Adv. Epidemiol. 2014, 2014, 230587. [Google Scholar] [CrossRef]
- Mindachew, M.; Deribew, A.; Tessema, F.; Biadgilign, S. Predictors of adherence to isoniazid preventive therapy among HIV positive adults in Addis Ababa, Ethiopia. BMC Public Health 2011, 11, 916. [Google Scholar] [CrossRef] [PubMed]
- Gugssa Boru, C.; Shimels, T.; Bilal, A.I. Factors contributing to non-adherence with treatment among TB patients in Sodo Woreda, Gurage Zone, Southern Ethiopia: A qualitative study. J. Infect. Public Health 2017, 10, 527–533. [Google Scholar] [CrossRef] [PubMed]
- Ayele, H.T.; van Mourik, M.S.; Bonten, M.J. Predictors of adherence to isoniazid preventive therapy in people living with HIV in Ethiopia. Int. J. Tuberc. Lung Dis. 2016, 20, 1342–1347. [Google Scholar] [CrossRef] [PubMed]
- Mesfin, M.M.; Newell, J.N.; Walley, J.D.; Gessessew, A.; Tesfaye, T.; Lemma, F.; Madeley, R.J. Quality of tuberculosis care and its association with patient adherence to treatment in eight Ethiopian districts. Health Policy Plan. 2009, 24, 457–466. [Google Scholar] [CrossRef] [PubMed]
- Nezenega, Z.S.; Gacho, Y.H.; Tafere, T.E. Patient satisfaction on tuberculosis treatment service and adherence to treatment in public health facilities of Sidama zone, South Ethiopia. BMC Health Serv. Res. 2013, 13, 110. [Google Scholar] [CrossRef]
- Gube, A.A.; Debalkie, M.; Seid, K.; Bisete, K.; Mengesha, A.; Zeynu, A.; Shimelis, F.; Gebremeskel, F. Assessment of Anti-TB Drug Nonadherence and Associated Factors among TB Patients Attending TB Clinics in Arba Minch Governmental Health Institutions, Southern Ethiopia. Tuberc. Res. Treat. 2018, 2018, 3705812. [Google Scholar] [CrossRef]
- Shargie, E.B.; Lindtjørn, B. Determinants of treatment adherence among smear-positive pulmonary tuberculosis patients in Southern Ethiopia. PLoS Med. 2007, 4, e37. [Google Scholar] [CrossRef]
- Tola, H.H.; Tol, A.; Shojaeizadeh, D.; Garmaroudi, G. Tuberculosis treatment non-adherence and lost to follow up among TB patients with or without HIV in developing countries: A systematic review. Iran. J. Public Health 2015, 44, 1. [Google Scholar]
| AND | (TB) OR (Tuberculosis) |
| AND | (“medication adherence”) OR (adherence) OR (“treatment adherence”) OR (“medication compliance”) OR (compliance) OR (default) OR (“loss to follow up”) |
| AND | Ethiopia |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Nezenega, Z.S.; Perimal-Lewis, L.; Maeder, A.J. Factors Influencing Patient Adherence to Tuberculosis Treatment in Ethiopia: A Literature Review. Int. J. Environ. Res. Public Health 2020, 17, 5626. https://doi.org/10.3390/ijerph17155626
Nezenega ZS, Perimal-Lewis L, Maeder AJ. Factors Influencing Patient Adherence to Tuberculosis Treatment in Ethiopia: A Literature Review. International Journal of Environmental Research and Public Health. 2020; 17(15):5626. https://doi.org/10.3390/ijerph17155626
Chicago/Turabian StyleNezenega, Zekariyas Sahile, Lua Perimal-Lewis, and Anthony John Maeder. 2020. "Factors Influencing Patient Adherence to Tuberculosis Treatment in Ethiopia: A Literature Review" International Journal of Environmental Research and Public Health 17, no. 15: 5626. https://doi.org/10.3390/ijerph17155626
APA StyleNezenega, Z. S., Perimal-Lewis, L., & Maeder, A. J. (2020). Factors Influencing Patient Adherence to Tuberculosis Treatment in Ethiopia: A Literature Review. International Journal of Environmental Research and Public Health, 17(15), 5626. https://doi.org/10.3390/ijerph17155626





