Assessing the Pilot Implementation of the Integrated Multimorbidity Care Model in Five European Settings: Results from the Joint Action CHRODIS-PLUS
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design and Participants
2.2. IMCM Interventions
2.3. Measures
2.4. Data Analysis
3. Results
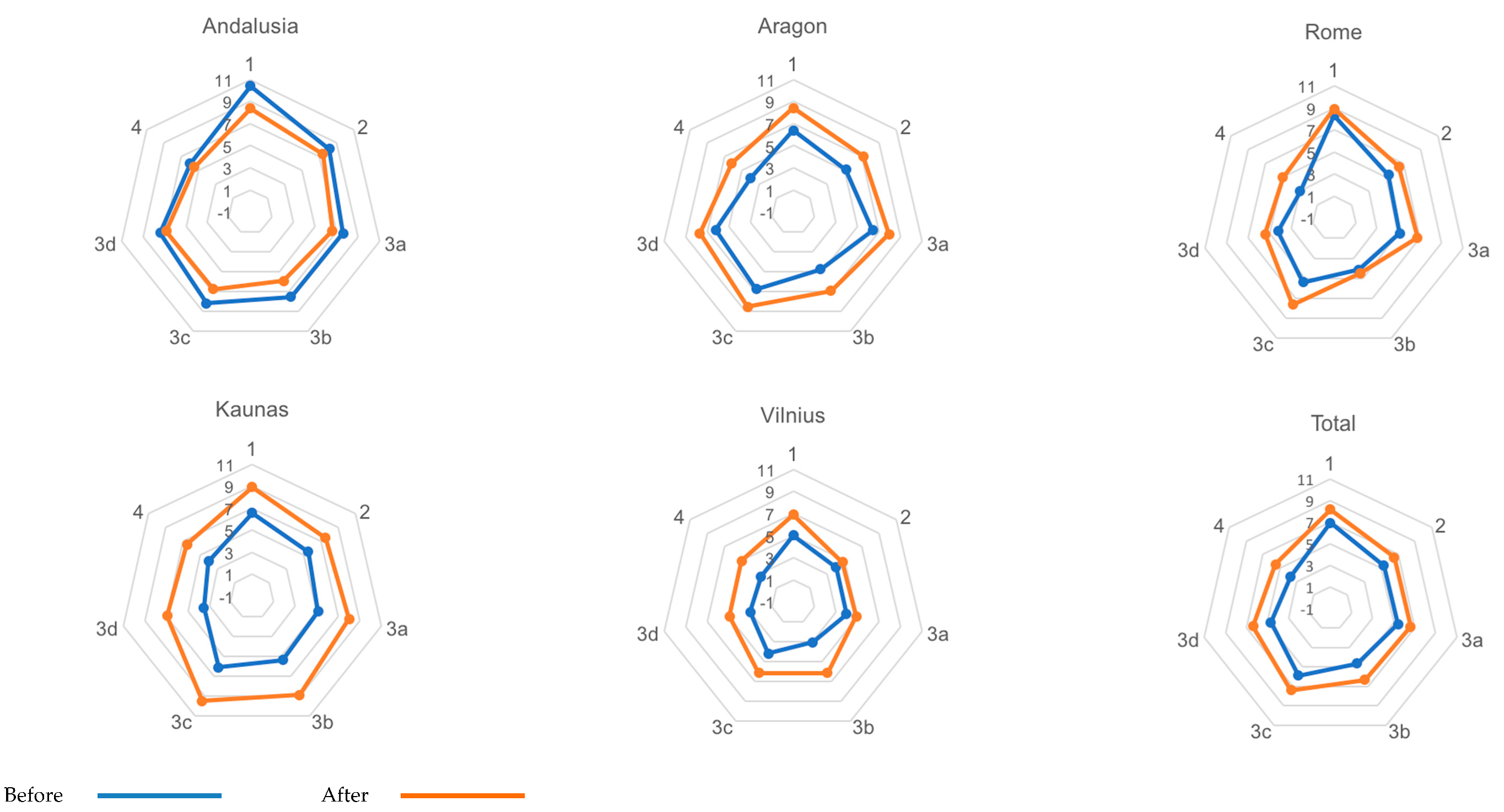
3.1. ACIC Results
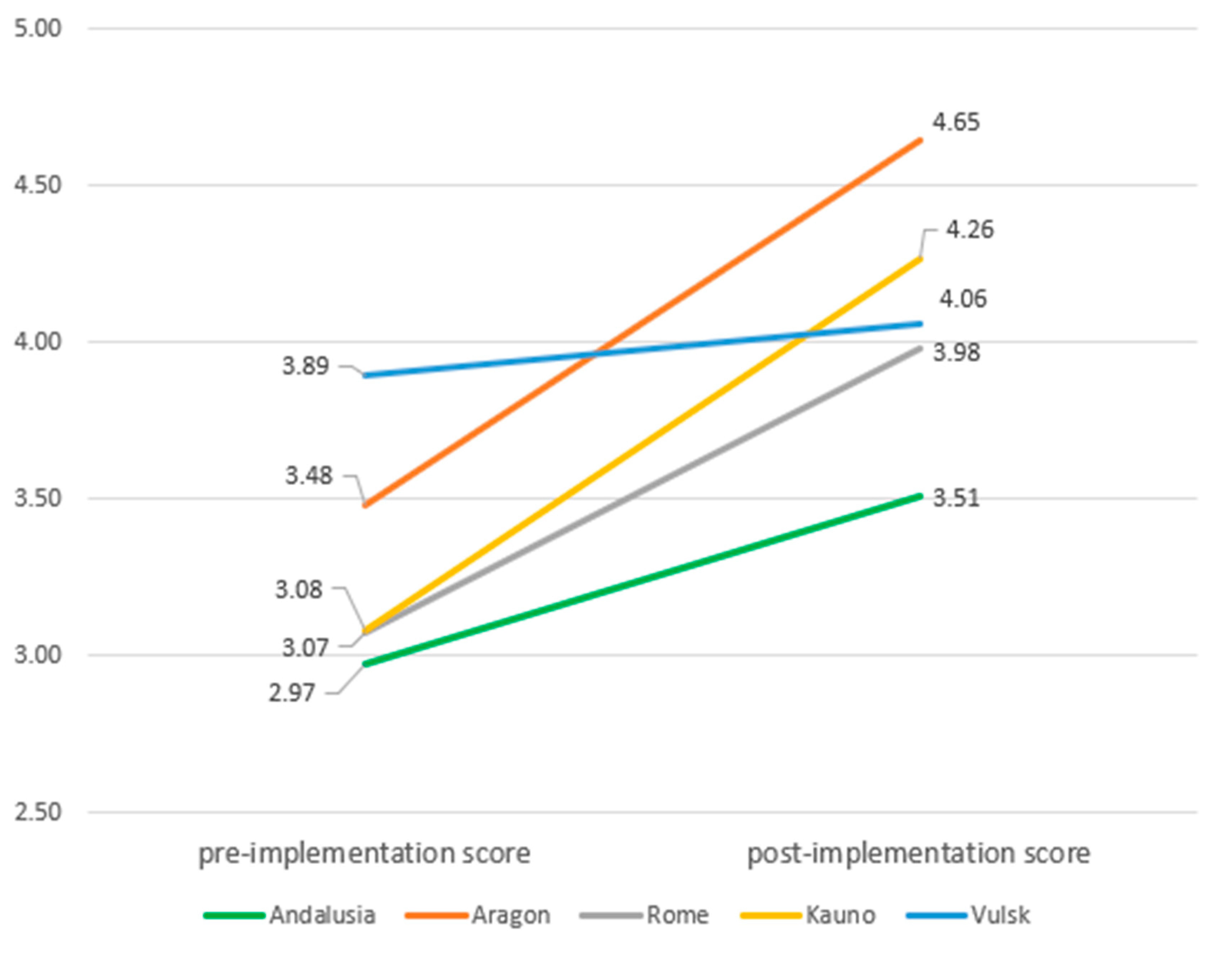
3.2. PACIC+ Results
4. Discussion
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- The Lancet. Making more of multimorbidity: An emerging priority. Lancet 2018, 391, 1637. [Google Scholar] [CrossRef]
- Melis, R.; Marengoni, A.; Angleman, S.; Fratiglioni, L. Incidence and predictors of multimorbidity in the elderly: A population-based longitudinal study. PLoS ONE 2014, 9, e103120. [Google Scholar] [CrossRef] [PubMed]
- Forjaz, M.J.; Rodriguez-Blazquez, C.; Ayala, A.; Rodriguez-Rodriguez, V.; de Pedro-Cuesta, J.; Garcia-Gutierrez, S.; Prados-Torres, A. Chronic conditions, disability, and quality of life in older adults with multimorbidity in Spain. Eur. J. Intern. Med. 2015, 26, 176–181. [Google Scholar] [CrossRef] [PubMed]
- Multimorbidity: A Priority for Global Health Research. Available online: https://acmedsci.ac.uk/policy/policy-projects/multimorbidity (accessed on 5 June 2020).
- Salisbury, C.; Man, M.-S.; Bower, P.; Guthrie, B.; Chaplin, K.; Gaunt, D.M.; Brookes, S.; Fitzpatrick, B.; Gardner, C.; Hollinghurst, S.; et al. Management of multimorbidity using a patient-centred care model: A pragmatic cluster-randomised trial of the 3D approach. Lancet 2018, 392, 41–50. [Google Scholar] [CrossRef]
- Muth, C.; van den Akker, M.; Blom, J.W.; Mallen, C.D.; Rochon, J.; Schellevis, F.G.; Becker, A.; Beyer, M.; Gensichen, J.; Kirchner, H.; et al. The Ariadne principles: How to handle multimorbidity in primary care consultations. BMC Med. 2014, 12, 223. [Google Scholar] [CrossRef] [PubMed]
- Prados-Torres, A.; del Cura-González, I.; Prados-Torres, D.; López-Rodríguez, J.A.; Leiva-Fernández, F.; Calderón-Larrañaga, A.; López-Verde, F.; Gimeno-Feliu, L.A.; Escortell-Mayor, E.; Pico-Soler, V.; et al. Effectiveness of an intervention for improving drug prescription in primary care patients with multimorbidity and polypharmacy: Study protocol of a cluster randomized clinical trial (Multi-PAP project). Implement. Sci. 2017, 12, 54. [Google Scholar] [CrossRef] [PubMed]
- Multimorbidity: Clinical Assessment and Management. Available online: https://www.nice.org.uk/guidance/ng56 (accessed on 5 June 2020).
- Wagner, E.H. Chronic disease management: What will it take to improve care for chronic illness? Eff. Clin. Pract. 1998, 1, 2–4. [Google Scholar]
- Epping-Jordan, J.E. Improving the quality of health care for chronic conditions. Qual. Saf. Heal. Care 2004, 13, 299–305. [Google Scholar] [CrossRef]
- Palmer, K.; Marengoni, A.; Forjaz, M.J.; Jureviciene, E.; Laatikainen, T.; Mammarella, F.; Muth, C.; Navickas, R.; Prados-Torres, A.; Rijken, M.; et al. Multimorbidity care model: Recommendations from the consensus meeting of the Joint Action on Chronic Diseases and Promoting Healthy Ageing across the Life Cycle (JA-CHRODIS). Health Policy (New. York). 2018, 122, 4–11. [Google Scholar] [CrossRef]
- Forjaz, M.; Rodriguez-Blazquez, C.; Guerrero-Fernández de Alba, I.; Gimeno-Miguel, A.; Bliek-Bueno, K.; Prados-Torres, A.; on behalf of the CHRODIS Expert Group on Multimorbidity. Application of the JA-CHRODIS Integrated Multimorbidity Care Model (IMCM) to a Case Study of Diabetes and Mental Health. Int. J. Environ. Res. Public Health 2019, 16, 5151. [Google Scholar] [CrossRef]
- Palmer, K.; Carfì, A.; Angioletti, C.; Di Paola, A.; Navickas, R.; Dambrauskas, L.; Jureviciene, E.; João Forjaz, M.; Rodriguez-Blazquez, C.; Prados-Torres, A.; et al. A Methodological Approach for Implementing an Integrated Multimorbidity Care Model: Results from the Pre-Implementation Stage of Joint Action CHRODIS-PLUS. Int. J. Environ. Res. Public Health 2019, 16, 5044. [Google Scholar] [CrossRef] [PubMed]
- Plan Andaluz de Atención Integrada a Pacientes con Enfermedades Crónicas. Available online: https://www.juntadeandalucia.es/organismos/saludyfamilias/areas/planificacion/plan-integral/paginas/paier.html (accessed on 5 June 2020).
- Proceso asistencial integrado de Atención a pacientes pluripatológicos. Available online: https://www.juntadeandalucia.es/export/drupaljda/salud_5af1956d9925c_atencion_pacientes_pluripatologicos_2018.pdf (accessed on 5 June 2020).
- Estrategia de Cuidados de Andalucía: Nuevos retos en el Cuidado de la Ciudadaní. Available online: https://www.sspa.juntadeandalucia.es/servicioandaluzdesalud/el-sas/planes-marco-y-estrategias/estrategia-de-cuidados-de-andalucia (accessed on 5 June 2020).
- Observatory of Innovative Practices for Complex Chronic Diseases Management. Available online: https://www.opimec.org/ (accessed on 5 June 2020).
- Glasgow, R.E.; Wagner, E.H.; Schaefer, J.; Mahoney, L.D.; Reid, R.J.; Greene, S.M. Development and Validation of the Patient Assessment of Chronic Illness Care (PACIC). Med. Care 2005, 43, 436–444. [Google Scholar] [CrossRef] [PubMed]
- Bonomi, A.E.; Wagner, E.H.; Glasgow, R.E.; VonKorff, M. Assessment of Chronic Illness Care (ACIC): A Practical Tool to Measure Quality Improvement. Health Serv. Res. 2002, 37, 791–820. [Google Scholar] [CrossRef] [PubMed]
- Sunaert, P.; Bastiaens, H.; Feyen, L.; Snauwaert, B.; Nobels, F.; Wens, J.; Vermeire, E.; Van Royen, P.; De Maeseneer, J.; De Sutter, A.; et al. Implementation of a program for type 2 diabetes based on the Chronic Care Model in a hospital-centered health care system: “the Belgian experience”. BMC Health Serv. Res. 2009, 9, 152. [Google Scholar] [CrossRef] [PubMed]
- Whitlock, E. Evaluating primary care behavioral counseling interventions: An evidence-based approach. Am. J. Prev. Med. 2002, 22, 267–284. [Google Scholar] [CrossRef]
- Glasgow, R.E.; Whitesides, H.; Nelson, C.C.; King, D.K. Use of the Patient Assessment of Chronic Illness Care (PACIC) With Diabetic Patients: Relationship to patient characteristics, receipt of care, and self-management. Diabetes Care 2005, 28, 2655–2661. [Google Scholar] [CrossRef] [PubMed]
- Statistical Power Analysis for the Behavioral Sciences. Available online: http://www.utstat.toronto.edu/~brunner/oldclass/378f16/readings/CohenPower.pdf (accessed on 5 June 2020).
- Hopman, P.; de Bruin, S.R.; Forjaz, M.J.; Rodriguez-Blazquez, C.; Tonnara, G.; Lemmens, L.C.; Onder, G.; Baan, C.A.; Rijken, M. Effectiveness of comprehensive care programs for patients with multiple chronic conditions or frailty: A systematic literature review. Health Policy 2016, 120, 818–832. [Google Scholar] [CrossRef]
- Cramm, J.M.; Strating, M.M.; Tsiachristas, A.; Nieboer, A.P. Development and validation of a short version of the Assessment of Chronic Illness Care (ACIC) in Dutch Disease Management Programs. Health Qual. Life Outcomes 2011, 9, 49. [Google Scholar] [CrossRef]
- Wolff, J.L.; Giovannetti, E.R.; Boyd, C.M.; Reider, L.; Palmer, S.; Scharfstein, D.; Marsteller, J.; Wegener, S.T.; Frey, K.; Leff, B.; et al. Effects of Guided Care on Family Caregivers. Gerontologist 2010, 50, 459–470. [Google Scholar] [CrossRef]
- Ford, J.A.; Lenaghan, E.; Salter, C.; Turner, D.; Shiner, A.; Clark, A.B.; Murdoch, J.; Green, C.; James, S.; Koopmans, I.; et al. Can goal-setting for patients with multimorbidity improve outcomes in primary care? Cluster randomised feasibility trial. BMJ Open 2019, 9, e025332. [Google Scholar] [CrossRef]
- Zeugfang, D.; Wisetborisut, A.; Angkurawaranon, C.; Aramrattana, A.; Wensing, M.; Szecsenyi, J.; Krug, K. Translation and validation of the PACIC+ questionnaire: The Thai version. BMC Fam. Pract. 2018, 19, 123. [Google Scholar] [CrossRef] [PubMed]
- Ludt, S.; van Lieshout, J.; Campbell, S.M.; Rochon, J.; Ose, D.; Freund, T.; Wensing, M.; Szecsenyi, J. Identifying factors associated with experiences of coronary heart disease patients receiving structured chronic care and counselling in European primary care. BMC Health Serv. Res. 2012, 12, 221. [Google Scholar] [CrossRef] [PubMed]
- Gensichen, J.; Serras, A.; Paulitsch, M.A.; Rosemann, T.; König, J.; Gerlach, F.M.; Petersen, J.J. The Patient Assessment of Chronic Illness Care Questionnaire: Evaluation in Patients with Mental Disorders in Primary Care. Community Ment. Health J. 2011, 47, 447–453. [Google Scholar] [CrossRef] [PubMed]
- Pilipovic-Broceta, N.; Vasiljevic, N.; Marinkovic, J.; Todorovic, N.; Jankovic, J.; Ostric, I.; Kalimanovska-Ostric, D.; Racic, M. Assessment of hypertension chronic care model: Pacic application in Bosnia and Herzegovina. PLoS ONE 2018, 13, e0202250. [Google Scholar] [CrossRef] [PubMed]
- Peters-Klimm, F.; Campbell, S.; Hermann, K.; Kunz, C.U.; Müller-Tasch, T.; Szecsenyi, J. Case management for patients with chronic systolic heart failure in primary care: The HICMan exploratory randomised controlled trial. Trials 2010, 11, 56. [Google Scholar] [CrossRef] [PubMed]
| Andalusia | Aragon | Rome | Kaunas | Vilnius | Total | |||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Mean | SD | p | Mean | SD | p | Mean | SD | p | Mean | SD | p | Mean | SD | p | Mean | SD | p | ES | ||
| Part 1 | Pre | 10.42 | 0.59 | 6.39 | 1.89 | 8.33 | 1.41 | 6.58 | 0.35 | 5.01 | 0.87 | 6.91 | 2.16 | |||||||
| Post | 8.40 | 1.46 | 8.44 | 1.51 | 8.92 | 0.59 | 8.92 | 0.35 | 6.88 | 1.42 | 8.16 | 1.39 | ||||||||
| Diff | −2.02 | 0.130 | 2.05 | 0.216 | 0.59 | 0.644 | 2.34 | 0.022 | 1.87 | 0.066 | 1.25 | 1.65 | 0.072 | 0.58 | ||||||
| Part 2 | Pre | 8.17 | 0.24 | 5.11 | 1.68 | 5.33 | 0.47 | 5.50 | 1.18 | 4.00 | 1.25 | 5.33 | 1.72 | |||||||
| Post | 7.40 | 2.16 | 7.11 | 1.83 | 6.50 | 2.12 | 7.50 | 0.24 | 4.75 | 0.63 | 6.58 | 1.84 | ||||||||
| Diff | −0.77 | 0.657 | 2.00 | 0.236 | 1.17 | 0.527 | 2.00 | 0.143 | 0.75 | 0.324 | 1.25 | 0.86 | 0.071 | 0.72 | ||||||
| Part 3a | Pre | 7.62 | 0.88 | 6.42 | 2.31 | 5.12 | 3.00 | 5.12 | 0.88 | 3.94 | 1.16 | 5.44 | 1.98 | |||||||
| Post | 6.60 | 1.72 | 7.92 | 1.91 | 6.75 | 3.18 | 8.00 | 0.35 | 4.88 | 1.76 | 6.61 | 2.00 | ||||||||
| Diff | −1.02 | 0.475 | 1.5 | 0.435 | 1.63 | 0.652 | 2.88 | 0.051 | 0.94 | 0.408 | 1.17 | 1.35 | 0.128 | 0.59 | ||||||
| Part 3b | Pre | 7.50 | 1.06 | 4.75 | 2.54 | 4.13 | 2.30 | 5.38 | 0.88 | 3.06 | 0.43 | 4.65 | 2.01 | |||||||
| Post | 5.90 | 2.07 | 6.89 | 1.05 | 4.50 | 2.83 | 8.88 | 1.18 | 6.13 | 1.45 | 6.34 | 1.92 | ||||||||
| Diff | −1.60 | 0.362 | 2.14 | 0.249 | 0.37 | 0.898 | 3.50 | 0.032 | 3.07 | 0.007 | 1.69 | 1.21 | 0.026 | 0.84 | ||||||
| Part 3c | Pre | 8.17 | 0.71 | 6.72 | 2.04 | 5.42 | 0.59 | 6.08 | 0.59 | 4.17 | 0.76 | 5.86 | 1.73 | |||||||
| Post | 6.73 | 1.30 | 8.50 | 1.20 | 7.67 | 0.71 | 9.50 | 0.47 | 6.13 | 1.74 | 7.38 | 1.65 | ||||||||
| Diff | −1.44 | 0.216 | 1.78 | 0.263 | 2.25 | 0.074 | 3.42 | 0.024 | 1.96 | 0.085 | 1.52 | 1.74 | 0.026 | 0.88 | ||||||
| Part 3d | Pre | 7.40 | 1.41 | 6.20 | 3.12 | 4.20 | 1.41 | 3.50 | 1.27 | 3.00 | 0.54 | 4.68 | 2.28 | |||||||
| Post | 6.84 | 0.92 | 7.67 | 2.68 | 5.40 | 0.85 | 6.90 | 1.27 | 4.90 | 1.99 | 6.34 | 1.81 | ||||||||
| Diff | −0.56 | 0.548 | 1.47 | 0.571 | 1.20 | 0.412 | 3.40 | 0.116 | 1.90 | 0.115 | 1.66 | 3.32 | 0.035 | 0.73 | ||||||
| Part 4 | Pre | 6.00 | 0.47 | 3.94 | 2.42 | 2.92 | 1.30 | 4.08 | 0.35 | 2.71 | 0.77 | 3.74 | 1.63 | |||||||
| Post | 5.50 | 1.60 | 6.11 | 1.84 | 4.92 | 0.59 | 6.58 | 1.06 | 4.96 | 1.81 | 5.54 | 1.50 | ||||||||
| Diff | −0.50 | 0.697 | 2.17 | 0.285 | 2.00 | 0.185 | 2.5 | 0.087 | 2.25 | 0.063 | 1.8 | 0.976 | 0.011 | 1.10 | ||||||
| Total | Pre | 7.90 | 0.29 | 5.65 | 2.20 | 5.06 | 1.50 | 5.18 | 0.43 | 3.70 | 0.72 | 5.23 | 1.78 | |||||||
| Post | 6.77 | 1.39 | 7.52 | 1.64 | 6.38 | 1.35 | 8.04 | 0.14 | 5.52 | 1.30 | 6.71 | 1.45 | ||||||||
| Diff | −1.13 | 0.330 | 1.87 | 0.303 | 1.32 | 0.454 | 2.86 | 0.012 | 1.82 | 0.051 | 1.48 | 1.41 | 0.022 | 0.83 | ||||||
| Andalusia (n = 52) | Aragon (n = 18) | Rome (n = 61) | Kaunas (n = 50) | Vilnius (n = 45) | Total (n = 226) | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| n | % | n | % | n | % | n | % | n | % | n | % | ||
| Sex | Man | 25 | 48.1 | 10 | 55.6 | 33 | 54.1 | 18 | 36.0 | 22 | 48.9 | 108 | 47.8 |
| Woman | 27 | 51.9 | 8 | 44.4 | 28 | 45.9 | 32 | 64.0 | 23 | 51.1 | 118 | 52.2 | |
| Civil status | Single | 3 | 5.77 | 0 | 0.00 | 48 | 78.7 | 1 | 2.0 | 2 | 4.44 | 54 | 23.9 |
| Married/with partner | 34 | 65.4 | 12 | 66.7 | 11 | 18.0 | 24 | 48.0 | 35 | 77.8 | 116 | 51.3 | |
| Widowed | 13 | 25.0 | 5 | 27.8 | 0 | 0.00 | 13 | 26.0 | 3 | 6.7 | 34 | 15.0 | |
| Separated/divorced | 2 | 3.85 | 1 | 5.56 | 2 | 3.28 | 12 | 24.0 | 5 | 11.1 | 22 | 9.73 | |
| Education | Primary complete or incomplete | 30 | 57.7 | 15 | 83.3 | 22 | 36.1 | 0 | 0.0 | 0 | 0.0 | 67 | 29.7 |
| Secondary | 12 | 23.1 | 1 | 5.56 | 30 | 49.2 | 22 | 44.0 | 6 | 13.3 | 71 | 31.4 | |
| University | 5 | 9.62 | 2 | 11.1 | 3 | 4.92 | 28 | 56.0 | 29 | 64.4 | 67 | 29.7 | |
| Other | 5 | 9.62 | 0 | 0.00 | 6 | 9.84 | 0 | 0.0 | 10 | 22.2 | 21 | 9.3 | |
| Activity | Employee | 4 | 7.69 | 0 | 0.00 | 9 | 14.8 | 13 | 26.0 | 22 | 48.9 | 48 | 21.2 |
| Housewife | 11 | 21.2 | 1 | 5.56 | 3 | 4.92 | 0 | 0.0 | 1 | 2.2 | 16 | 7.1 | |
| Unemployed | 3 | 5.77 | 0 | 0.00 | 16 | 26.2 | 0 | 0.0 | 1 | 2.2 | 20 | 8.85 | |
| Retired | 30 | 57.7 | 17 | 94.4 | 21 | 34.4 | 34 | 68.0 | 20 | 44.4 | 122 | 54.0 | |
| Other | 4 | 7.69 | 0 | 0.00 | 12 | 19.7 | 3 | 6.0 | 1 | 2.2 | 20 | 8.85 | |
| Change score | No change or worse (1–4) | 11 | 26.2 | 4 | 22.2 | -- | -- | 31 | 36.0 | 12 | 42.9 | 58 | 42.0 |
| Better (5–7) | 31 | 73.8 | 14 | 77.8 | -- | -- | 19 | 64.0 | 16 | 57.1 | 80 | 58.0 | |
| M | SD | M | SD | M | SD | M | SD | M | SD | M | SD | ||
| Age (years) | 72.3 | 12.9 | 80.1 | 9.5 | 46.7 | 19.4 | 68.5 | 6.4 | 61.0 | 9.1 | 62.9 | 17.1 | |
| Change score (1–7) | 5.31 | 1.14 | 5.8 | 1.2 | -- | -- | 4.4 | 1.0 | 4.7 | 0.8 | 4.9 | 1.1 | |
| Andalusia (n = 42) | Aragon (n = 18) | Rome (n = 60) | Kaunas (n = 50) | Vilnius (n = 40) | Total (n = 210) | |||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Mean | SD | p | Mean | SD | p | Mean | SD | p | Mean | SD | p | Mean | SD | p | Mean | SD | p | Effect Size | ||
| Assess | Pre | 2.96 | 1.14 | 3.45 | 0.35 | 3.28 | 1.11 | 3.20 | 0.93 | 3.95 | 0.84 | 3.34 | 1.03 | |||||||
| Post | 3.56 | 1.10 | 4.58 | 0.39 | 4.09 | 0.76 | 4.44 | 0.75 | 4.05 | 0.83 | 4.10 | 0.88 | ||||||||
| Diff | 0.60 | 0.87 | <0.001 | 1.13 | 0.39 | <0.001 | 2.02 | 1.50 | <0.001 | 1.24 | 0.98 | <0.001 | 0.10 | 0.54 | 0.226 | 0.77 | 0.96 | <0.001 | 0.75 | |
| Advise | Pre | 3.20 | 0.91 | 3.20 | 1.07 | 3.28 | 1.10 | 3.24 | 0.95 | 4.10 | 0.73 | 3.42 | 0.99 | |||||||
| Post | 3.69 | 0.88 | 4.60 | 0.48 | 4.14 | 0.66 | 4.36 | 0.68 | 4.23 | 0.70 | 4.16 | 0.75 | ||||||||
| Diff | 0.49 | 1.04 | 0.004 | 1.21 | 0.73 | <0.001 | 0.87 | 1.05 | <0.001 | 1.12 | 0.94 | <0.001 | 0.14 | 0.62 | 0.177 | 0.74 | 0.97 | <0.001 | 0.75 | |
| Agree | Pre | 3.00 | 1.02 | 3.41 | 0.61 | 3.18 | 1.06 | 2.90 | 1.18 | 3.87 | 0.90 | 3.23 | 1.07 | |||||||
| Post | 3.54 | 1.10 | 4.53 | 0.39 | 4.07 | 0.68 | 4.09 | 0.93 | 4.09 | 0.77 | 4.01 | 0.87 | ||||||||
| Diff | 0.53 | 0.93 | 0.001 | 1.13 | 0.49 | <0.001 | 0.82 | 1.11 | <0.001 | 1.18 | 1.24 | <0.001 | 0.21 | 0.73 | 0.072 | 0.78 | 1.01 | <0.001 | 0.73 | |
| Assist | Pre | 2.48 | 1.03 | 2.81 | 0.68 | 2.93 | 1.14 | 3.20 | 0.86 | 3.78 | 1.04 | 3.05 | 1.08 | |||||||
| Post | 3.10 | 1.02 | 3.98 | 0.76 | 3.94 | 0.76 | 4.17 | 0.76 | 3.87 | 0.82 | 3.82 | 0.90 | ||||||||
| Diff | 0.62 | 0.92 | <0.001 | 1.16 | 0.67 | <0.001 | 0.54 | 1.25 | <0.001 | 0.97 | 0.93 | <0.001 | 0.09 | 0.79 | 0.475 | 0.76 | 0.96 | <0.001 | 0.70 | |
| Arrange | Pre | 2.03 | 1.01 | 2.20 | 0.57 | 2.62 | 1.15 | 2.26 | 1.07 | 3.17 | 1.09 | 2.48 | 1.11 | |||||||
| Post | 2.70 | 1.05 | 3.63 | 0.94 | 3.82 | 0.89 | 3.71 | 0.98 | 3.43 | 0.88 | 3.48 | 1.03 | ||||||||
| left | 0.66 | 0.98 | <0.001 | 1.44 | 0.60 | <0.001 | 0.93 | 1.29 | <0.001 | 1.45 | 1.40 | <0.001 | 0.26 | 0.77 | 0.040 | 0.99 | 1.19 | <0.001 | 0.89 | |
| 5As Summary | Pre | 2.91 | 0.96 | 3.38 | 0.54 | 3.17 | 1.01 | 3.05 | 0.87 | 3.90 | 0.78 | 3.25 | 0.95 | |||||||
| Post | 3.46 | 0.97 | 4.55 | 0.35 | 4.07 | 0.66 | 4.23 | 0.81 | 4.07 | 0.75 | 4.03 | 0.82 | ||||||||
| Diff | 0.54 | 0.85 | <0.001 | 1.17 | 0.58 | <0.001 | 0.72 | 1.05 | <0.001 | 1.19 | 0.93 | <0.001 | 0.17 | 0.62 | 0.093 | 0.78 | 0.90 | <0.001 | 0.82 | |
| Model | Standardized Beta | t | Sig. | 95% Confidence Interval | R2 | ||
|---|---|---|---|---|---|---|---|
| Assess | (Constant) | 6.085 | <0.001 | 1.665 | 3.261 | 0.44 | |
| Assess pre | −0.604 | −10.849 | <0.001 | −0.667 | −0.462 | ||
| ACIC1 diff. | 0.335 | 4.220 | <0.001 | 0.107 | 0.296 | ||
| ACIC4 diff. | −0.212 | −2.767 | 0.006 | −0.359 | −0.060 | ||
| Advise | (Constant) | 8.925 | <0.001 | 2.488 | 3.899 | 0.55 | |
| ACIC1 diff. | 0.266 | 3.742 | <0.001 | 0.077 | 0.248 | ||
| Advise pre | −0.716 | −14.543 | <0.001 | −0.803 | −0.611 | ||
| Agree | (Constant) | 7.247 | <0.001 | 2.015 | 3.522 | 0.48 | |
| ACIC1 diff. | 0.243 | 3.172 | 0.002 | 0.058 | 0.250 | ||
| Agree pre | −0.658 | −12.304 | <0.001 | −0.717 | −0.519 | ||
| Assist | (Constant) | 6.940 | <0.001 | 1.844 | 3.307 | 0.46 | |
| ACIC1 diff. | 0.296 | 3.737 | <0.001 | 0.085 | 0.273 | ||
| ACIC4 diff. | −0.225 | −3.050 | 0.003 | −0.369 | −0.079 | ||
| Assist pre | −0.656 | −11.762 | <0.001 | −0.684 | −0.488 | ||
| Arrange | (Constant) | 6.553 | <0.001 | 2.023 | 3.765 | 0.46 | |
| ACIC1 diff. | 0.287 | 3.679 | <0.001 | 0.099 | 0.328 | ||
| ACIC4 diff. | −0.242 | −3.283 | 0.001 | −0.476 | −0.119 | ||
| Arrange pre | −0.649 | −11.836 | <0.001 | −0.806 | −0.576 | ||
| 5As summary | (Constant) | 6.867 | <0.001 | 1.802 | 3.254 | 0.45 | |
| ACIC1 diff. | 0.299 | 3.812 | <0.001 | 0.082 | 0.258 | ||
| ACIC4 diff. | −0.178 | −2.333 | 0.021 | −0.306 | −0.026 | ||
| 5As summary pre | −0.625 | −11.270 | <0.001 | −0.697 | −0.490 | ||
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Rodriguez-Blazquez, C.; João Forjaz, M.; Gimeno-Miguel, A.; Bliek-Bueno, K.; Poblador-Plou, B.; Pilar Luengo-Broto, S.; Guerrero-Fernández de Alba, I.; Maria Carriazo, A.; Lama, C.; Rodríguez-Acuña, R.; et al. Assessing the Pilot Implementation of the Integrated Multimorbidity Care Model in Five European Settings: Results from the Joint Action CHRODIS-PLUS. Int. J. Environ. Res. Public Health 2020, 17, 5268. https://doi.org/10.3390/ijerph17155268
Rodriguez-Blazquez C, João Forjaz M, Gimeno-Miguel A, Bliek-Bueno K, Poblador-Plou B, Pilar Luengo-Broto S, Guerrero-Fernández de Alba I, Maria Carriazo A, Lama C, Rodríguez-Acuña R, et al. Assessing the Pilot Implementation of the Integrated Multimorbidity Care Model in Five European Settings: Results from the Joint Action CHRODIS-PLUS. International Journal of Environmental Research and Public Health. 2020; 17(15):5268. https://doi.org/10.3390/ijerph17155268
Chicago/Turabian StyleRodriguez-Blazquez, Carmen, Maria João Forjaz, Antonio Gimeno-Miguel, Kevin Bliek-Bueno, Beatriz Poblador-Plou, Sara Pilar Luengo-Broto, Inmaculada Guerrero-Fernández de Alba, Ana Maria Carriazo, Carmen Lama, Rafael Rodríguez-Acuña, and et al. 2020. "Assessing the Pilot Implementation of the Integrated Multimorbidity Care Model in Five European Settings: Results from the Joint Action CHRODIS-PLUS" International Journal of Environmental Research and Public Health 17, no. 15: 5268. https://doi.org/10.3390/ijerph17155268
APA StyleRodriguez-Blazquez, C., João Forjaz, M., Gimeno-Miguel, A., Bliek-Bueno, K., Poblador-Plou, B., Pilar Luengo-Broto, S., Guerrero-Fernández de Alba, I., Maria Carriazo, A., Lama, C., Rodríguez-Acuña, R., Cosano, I., Bedoya, J. J., Angioletti, C., Carfì, A., Di Paola, A., Navickas, R., Jureviciene, E., Dambrauskas, L., Liseckiene, I., ... Prados-Torres, A. (2020). Assessing the Pilot Implementation of the Integrated Multimorbidity Care Model in Five European Settings: Results from the Joint Action CHRODIS-PLUS. International Journal of Environmental Research and Public Health, 17(15), 5268. https://doi.org/10.3390/ijerph17155268









