One-Year Follow-Up after Multimodal Rehabilitation for Patients with Whiplash-Associated Disorders
Abstract
1. Introduction
2. Material and Methods
2.1. Design
2.2. Patients
2.3. Multimodal Rehabilitation Program, MMR
2.4. Measures
2.4.1. The Short Form Health Survey (SF36) Standard Swedish Version 1.0
2.4.2. The Hospital Anxiety and Depression Scale (HAD)
2.4.3. Numeric Rating Scale (NRS)
2.4.4. Multidimensional Pain Inventory (MPI)
2.5. Data Analysis
2.6. Ethics
3. Results
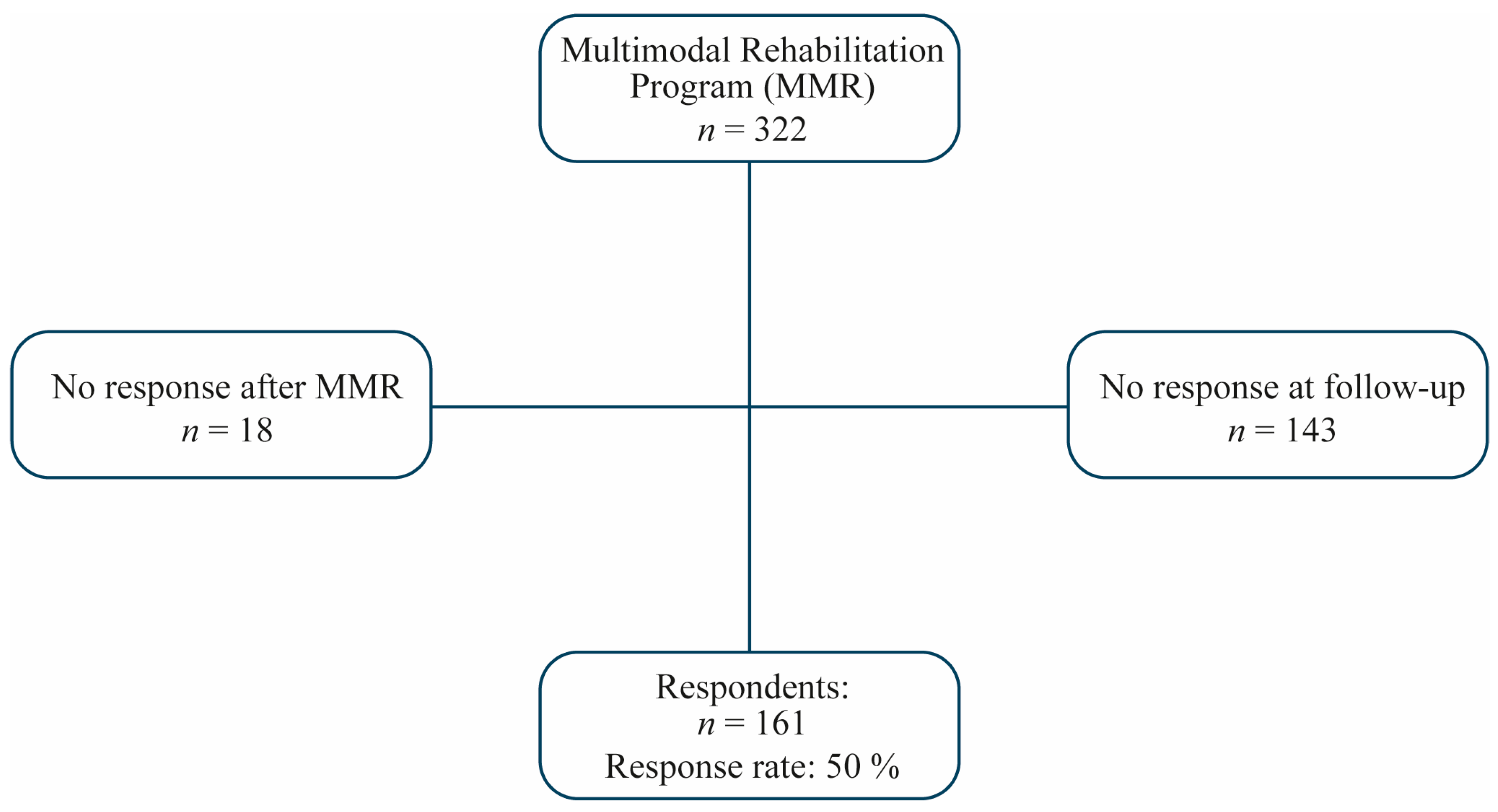
3.1. Patients
3.2. Analysis of Non-Respondents
3.3. Patient Characteristics for the Analyzed Group
3.4. Physical and Mental Health (Primary Outcomes)
3.5. Pain Intensity, Anxiety and Depression, Interference with Life (Secondary Outcomes)
4. Discussion
Strengths and Limitations
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Sterner, Y.; Toolanen, G.; Gerdle, B.; Hildingsson, C. The Incidence of Whiplash Trauma and the Effects of Different Factors on Recovery. J. Spinal Disord. Tech. 2003, 16, 195–199. [Google Scholar] [CrossRef] [PubMed]
- Jansen, G.B.; Edlund, C.; Grane, P.; Hildingsson, C.; Karlberg, M.; Link, H.; Måve, U.; Portala, K.; Rydevik, B.; Sterner, Y. Whiplash injuries: Diagnosis and early management. The Swedish Society of Medicine and the Whiplash Commission Medical Task Force. Eur Spine J. 2008, 17, S355–S417. [Google Scholar]
- Sterner, Y.; Gerdle, B. Acute and chronic whiplash disorders--a review. J. Rehabilitation Med. 2004, 36, 193–210. [Google Scholar] [CrossRef] [PubMed]
- Spitzer, W.; Skovron, M.L.; Salmi, L.R.; Cassidy, J.D.; Duranceau, J.; Suissa, S.; Zeiss, E. Scientific monograph of the Quebec Task Force on Whiplash-Associated Disorders: Redefining "whiplash" and its management. Spine 1995, 20, 1S–73S. [Google Scholar]
- Carroll, L.J.; Holm, L.W.; Hogg-Johnson, S.; Cote, P.; Cassidy, J.D.; Haldeman, S.; Nordin, M.; Hurwitz, E.L.; Carragee, E.J.; van der Velde, G. Course and prognostic factors for neck pain in whiplash-associated disorders (WAD): Results of the Bone and Joint Decade 2000-2010 Task Force on Neck Pain and Its Associated Disorders. Spine (Phila Pa 1976) 2008, 33, S83–S92. [Google Scholar] [CrossRef]
- The Whiplash Commission Final Report 2005. Available online: http://www.whiplashkommissionen.se/ (accessed on 2 July 2020).
- Malfliet, A.; De Kooning, M.; Inghelbrecht, E.; Willems, B.; Bernheim, J.; Nijs, J.; Hachimi-Idrissi, S. Sex Differences in Patients with Chronic Pain Following Whiplash Injury: The Role of Depression, Fear, Somatization, Social Support, and Personality Traits. Pain Pr. 2014, 15, 757–764. [Google Scholar] [CrossRef]
- Côté, P.; Cassidy, J.D.; Carroll, L.; Frank, J.W.; Bombardier, C. A Systematic Review of the Prognosis of Acute Whiplash and a New Conceptual Framework to Synthesize the Literature. Spine 2001, 26, E445–E458. [Google Scholar] [CrossRef]
- Sarrami, P.; Armstrong, E.; Naylor, J.M.; Harris, I.A. Factors predicting outcome in whiplash injury: A systematic meta-review of prognostic factors. J. Orthop. Traumatol. 2016, 18, 9–16. [Google Scholar] [CrossRef]
- Hogg-Johnson, S.; van der Velde, G.; Carroll, L.J.; DrMedSc, L.W.H.; Cassidyet, J.D.; Guzman, J.; Côté, P.; Haldemanal, S.; Ammendolia, C.; Carragee, E.; et al. The burden and determinants of neck pain in the general population. Results of the Bone and Joint Decade 2000–2010 Task Force on Neck Pain and Its Associated Disorders. Eur. Spine J. 2008, 33, S39–S51. [Google Scholar] [CrossRef]
- Van Der Velde, G.; Yu, H.; Paulden, M.; Côté, P.; Varatharajan, S.; Shearer, H.M.; Wong, J.J.; Randhawa, K.; Southerst, D.; Mior, S.; et al. Which interventions are cost-effective for the management of whiplash-associated and neck pain-associated disorders? A systematic review of the health economic literature by the Ontario Protocol for Traffic Injury Management (OPTIMa) Collaboration. Spine J. 2016, 16, 1582–1597. [Google Scholar] [CrossRef]
- Jull, G.A.; Sterling, M. Bring back the biopsychosocial model for neck pain disorders. Man. Ther. 2009, 14, 117–118. [Google Scholar] [CrossRef] [PubMed]
- Rehabilitering vid långvarig smärta. En systematisk litteraturöversikt. Stockholm: Statens beredning för medicinsk utvärdering (SBU), SBU–Swedish Agency for Health Technology Assessment and Assessment of Social Services: Stockholm, Sweden, 2010; SBU-rapport nr 198. ISBN 978-91-85413-34-8.
- Scascighini, L.; Toma, V.; Dober-Spielmann, S.; Sprott, H. Multidisciplinary treatment for chronic pain: A systematic review of interventions and outcomes. Rheumatol. 2008, 47, 670–678. [Google Scholar] [CrossRef] [PubMed]
- Jensen, I.; Bergström, G.; Ljungquist, T.; Bodin, L.; Nygren, ÅL. A randomized controlled component analysis of a behavioral medicine rehabilitation program for chronic spinal pain: Are the effects dependent on gender? Pain 2001, 91, 65–78. [Google Scholar] [CrossRef]
- Cedraschi, C.; Desmeules, J.; Rapiti, E.; Baumgartner, E.; Cohen, P.; Finckh, A.; Allaz, A.F.; Vischer, T.L. Fibromyalgia: A randomised, controlled trial of a treatment programme based on self management. Ann. Rheum. Dis. 2004, 63, 290–296. [Google Scholar] [CrossRef] [PubMed]
- Kole-Snijders, A.M.; Vlaeyen, J.W.; Goossens, M.E.; Rutten-van Molken, M.P.; Heuts, P.H.; van Breukelen, G.; van Eek, H. Chronic low-back pain: What does cognitive coping skills training add to operant behavioral treatment? Results of a randomized clinical trial. J. Consult. Clin Psychol. 1999, 67, 931–944. [Google Scholar] [CrossRef] [PubMed]
- Sterner, M.L.Y. Early interdisciplinary rehabilitation programme for whiplash associated disorders. Disabil. Rehabil. 2001, 23, 422–429. [Google Scholar] [CrossRef] [PubMed]
- Angst, F.; Gysi, F.; Verra, M.; Lehmann, S.; Jenni, W.; Aeschlimann, A. Interdisciplinary rehabilitation after whiplash injury: An observational prospective outcome study. J. Rehabil. Med. 2010, 42, 350–356. [Google Scholar] [CrossRef]
- E Lamb, S.; A Williams, M.; Williamson, E.M.; Gates, S.; Withers, E.J.; Mt-Isa, S.; Ashby, D.; Castelnuovo, E.; Underwood, M.; Cooke, M.W. Managing Injuries of the Neck Trial (MINT): A randomised controlled trial of treatments for whiplash injuries. Heal. Technol. Assess. 2012, 16, 1–141. [Google Scholar] [CrossRef]
- Jull, G.A.; Sterling, M.; Kenardy, J.; Beller, E. Does the presence of sensory hypersensitivity influence outcomes of physical rehabilitation for chronic whiplash?—A preliminary RCT. Pain 2007, 129, 28–34. [Google Scholar] [CrossRef]
- Sutton, D.; Côté, P.; Wong, J.J.; Varatharajan, S.; Randhawa, K.; Yu, H.; Southerst, D.; Shearer, H.M.; Van Der Velde, G.; Nordin, M.; et al. Is multimodal care effective for the management of patients with whiplash-associated disorders or neck pain and associated disorders? A systematic review by the Ontario Protocol for Traffic Injury Management (OPTIMa) Collaboration. Spine J. 2016, 16, 1541–1565. [Google Scholar] [CrossRef]
- NRS (in Swedish) (Swedish Quality Registry for Pain Rehabilitation, SQRP). 2016. Available online: http://www.ucr.uu.se/nrs/ (accessed on 2 July 2020).
- E Ware, J.; Gandek, B. Overview of the SF-36 Health Survey and the International Quality of Life Assessment (IQOLA) Project. J. Clin. Epidemiol. 1998, 51, 903–912. [Google Scholar] [CrossRef]
- Sullivan, M.; Karlsson, J.; Taft, C. SF-36 Hälsoenkät: Svensk Manual och tolkningsguide., 2nd ed.; Sahlgrenska University Hospital: Gothenburg, Sweden, 2002. [Google Scholar]
- Zigmond, A.S.; Snaith, R.P. The Hospital Anxiety and Depression Scale. Acta Psychiatr. Scand. 1983, 67, 361–370. [Google Scholar] [CrossRef] [PubMed]
- Farrar, J.T.; Young, J.P.; Lamoreaux, L.; Werth, J.L.; Poole, M.R. Clinical importance of changes in chronic pain intensity measured on an 11-point numerical pain rating scale. Pain 2001, 94, 149–158. [Google Scholar] [CrossRef]
- Kerns, R.D.; Turk, D.C.; Rudy, T.E. The West Haven-Yale Multidimensional Pain Inventory (WHYMPI). Pain 1985, 23, 345–356. [Google Scholar] [CrossRef]
- Scholten-Peeters, G.; Der Steen, C.W.M.N.-V.; Van Der Windt, D.A.W.M.; Hendriks, E.J.M.; Verhagen, A.P.; Oostendorp, R.A.B.; Van Der Windt, D.A.W.M. Education by General Practitioners or Education and Exercises by Physiotherapists for Patients With Whiplash-Associated Disorders? A Randomized Clinical Trial. Spine 2006, 31, 723–731. [Google Scholar] [CrossRef]
- Nyberg, V.; Novo, M.; Sjölund, B.H. Do Multidimensional Pain Inventory Scale score changes indicate risk of receiving sick leave benefits 1 year after a pain rehabilitation programme?? Disabil. Rehabilitation 2011, 33, 1548–1556. [Google Scholar] [CrossRef]
- Fillingim, R.B.; King, C.D.; Ribeiro-Dasilva, M.C.; Rahim-Williams, B.; Riley, J.L. Sex, Gender, and Pain: A Review of Recent Clinical and Experimental Findings. J. Pain 2009, 10, 447–485. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. International Classification of Functioning, Disability and Health (ICF). Available online: http://www.who.int/classifications/icf/en/ (accessed on 2 July 2020).
- Carragee, E.J.; Hurwitz, E.L.; Cheng, I.; Carroll, L.; Nordin, M.; Guzman, J.; Peloso, P.; Holm, L.W.; Côté, P.; Hogg-Johnson, S.; et al. Treatment of Neck Pain. J. Manip. Physiol. Ther. 2009, 32, S176–S193. [Google Scholar] [CrossRef]
| Total Respondents | Women | Men | p-Value | |
|---|---|---|---|---|
| N | 161 | 109 | 52 | |
| Percentage frequency | 100% | 68% | 32% | |
| Age (mean, SD) | 39 (11.1) | 38.5 (11.3) | 41 (10.7) | |
| Highest educational level (within gender) | n.s | |||
| Primary school | 8.10% | 7.30% | 9.60% | |
| Secondary school | 54.70% | 48.60% | 67.30% | |
| University | 32.90% | 38.50% | 21.20% | |
| Other | − | 5.50% | 1.90% | |
| Missing data | − | − | − | |
| Place of birth (within gender) | 0.017 | |||
| Sweden | 59.40% | 66% | 44.20% | |
| Nordic country | 1.90% | 2.80% | 0.00% | |
| Europe | 5.00% | 3.70% | 7.70% | |
| Country outside Europe | 33.80% | 26.90% | 48.10% | |
| Missing data | 0.60% | 0.60% | − | |
| Job status (within gender) | n.s | |||
| Employed | 90.10% | 88.10% | 94.20% | |
| Unemployed | 3.70% | 3.70% | 3.80% | |
| Unemployed | 1.20% | 1.80% | 0% | |
| Not acquisition worker | 1.20% | 1.80% | 0% | |
| Missing data | − | − | − |
| n | Total Respondents | n | Women | n | Men | p-Value | |
|---|---|---|---|---|---|---|---|
| Pain duration (median, quartiles 25; 75) | 153 | 91 days (51.5; 158.5) | 101 | 97 days (51.5; 171.5) | 52 | 90 days (52; 128) | n.s |
| How convinced are you about recovery? | 150 | n.s | |||||
| 1–3: Positive outlook | 122 | 75.80% | 82 | 75.30% | 40 | 76.90% | |
| 4–5: Negative outlook | 28 | 17.40% | 18 | 16.50% | 10 | 19.20% | |
| Missing data | 11 | 6.80% | 9 | 8.30% | 2 | 3.80% | |
| How do you think it will be to return to work, to study, or extend working hours? | 93 | n.s | |||||
| 1–3: very easy | 36 | 38.70% | 26 | 39.40% | 10 | 37% | |
| 4–5: very difficult | 32 | 34.40% | 21 | 31.80% | 11 | 40.2 | |
| Missing data | 25 | 26.90% | 19 | 28.80% | 6 | 22.20% | |
| When do you expect to return to work, to study, or to extend your working hours? | 93 | n.s | |||||
| 1–3: as soon as possible | 55 | 57.60% | 38 | 57.60% | 17 | 63% | |
| 4–5: never | 8 | 8.70% | 5 | 7.60% | 3 | 11.10% | |
| Missing data | 30 | 32.30% | 23 | 34.80% | 7 | 25.90% |
| n | Missing | Before | After | One-Year Follow-Up | p-Value | p-Value | p-Value | |
|---|---|---|---|---|---|---|---|---|
| (a) | (b) | (c) | Friedman test | (a–b) | (a–c) | |||
| PCS SF-36 | ||||||||
| median (range) | ||||||||
| Women | 101 | 8 | 32 (18–51) | 34 (19–52) | 34 (11–57) | 0.007 * | 0.021 * | 0.003 * |
| Men | 50 | 2 | 31 (15–54) | 33 (17–54) | 34.5 (15–58) | 0.020 * | 0.014 * | 0.002 * |
| Total | 151 | 10 | 32 (15–54) | 34 (17–54) | 34 (11–58) | <0.001 * | 0.001 * | <0.001 * |
| MCS SF-36 | ||||||||
| Women | 101 | 8 | 29 (8–60) | 30 (9–61) | 39 (11–58) | <0.001 * | 0.214 | <0.001 * |
| Men | 50 | 2 | 32 (11–52) | 32 (9–61) | 33 (10–59) | 0.805 | 0.933 | 0.157 |
| Total | 151 | 10 | 29.5 (8–60) | 30.5 (9–61) | 37 (10–59) | <0.001 * | 0.208 | <0.001 * |
| HAD-A | ||||||||
| Median(range) | ||||||||
| Women | 109 | − | 10.0 (0–21) | 9.0 (0-21) | 9.0 (0–21) | 0.011* | 0.159 | 0.002 * |
| Men | 52 | − | 10.0 (2–18) | 8.5 (1-21) | 8.5 (0–21) | 0.044 * | 0.008 * | 0.118 |
| Total | 161 | − | 10.0 (0–21) | 9.0 (0-21) | 9.0 (0–21) | 0.002 * | 0.011 * | 0.001 * |
| HAD-D | ||||||||
| Women | 109 | − | 8.0 (0–20) | 8.0 (0–18) | 6.0 (0–21) | 0.004 * | 0.103 | 0.001 * |
| Men | 52 | − | 9.0 (0–19) | 8.0 (0–20) | 9.5 (0–20) | 0.284 | 0.142 | 0.807 |
| Total | 161 | − | 8.0 (0–20) | 8.0 (0–20) | 7.0 (0–21) | 0.044 * | 0.029 * | 0.011 * |
| NRS | ||||||||
| median (range) | ||||||||
| Women | 102 | 7 | 7.0 (1–10) | 6.0 (1–10) | 6.0 (0–10) | <0.001 * | <0.001 * | <0.001 * |
| Men | 47 | 5 | 7.0 (2–10) | 5.0 (1–9) | 6.0 (0–9) | <0.001 * | <0.001 * | <0.001 * |
| Total | 149 | 12 | 7.0 (1–10) | 6.0 (1–10) | 6.0 (0–10) | <0.001 * | <0.001 * | <0.001 * |
| MPI interference | ||||||||
| Median (range) | ||||||||
| Women | 108 | 1 | 4.3 (0.36–6) | 4.1 (0.6–6) | 3.9 (0–6) | 0.001 * | 0.088 * | <0.001 * |
| Men | 52 | − | 4 (0.6–5.9) | 4 (0.45–5.9) | 3.9 (0.1–6) | 0.013 * | 0.019 * | 0.011 * |
| Total | 160 | 1 | 4.2 (0.7–6) | 4.1 (0.45–6) | 3.9 (0–6) | <0.001 * | 0.004 * | <0.001 * |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Björsenius, V.; Löfgren, M.; Stålnacke, B.-M. One-Year Follow-Up after Multimodal Rehabilitation for Patients with Whiplash-Associated Disorders. Int. J. Environ. Res. Public Health 2020, 17, 4784. https://doi.org/10.3390/ijerph17134784
Björsenius V, Löfgren M, Stålnacke B-M. One-Year Follow-Up after Multimodal Rehabilitation for Patients with Whiplash-Associated Disorders. International Journal of Environmental Research and Public Health. 2020; 17(13):4784. https://doi.org/10.3390/ijerph17134784
Chicago/Turabian StyleBjörsenius, Viktor, Monika Löfgren, and Britt-Marie Stålnacke. 2020. "One-Year Follow-Up after Multimodal Rehabilitation for Patients with Whiplash-Associated Disorders" International Journal of Environmental Research and Public Health 17, no. 13: 4784. https://doi.org/10.3390/ijerph17134784
APA StyleBjörsenius, V., Löfgren, M., & Stålnacke, B.-M. (2020). One-Year Follow-Up after Multimodal Rehabilitation for Patients with Whiplash-Associated Disorders. International Journal of Environmental Research and Public Health, 17(13), 4784. https://doi.org/10.3390/ijerph17134784





