Brief Psychological Intervention Through Mobile App and Conference Calls for the Prevention of Depression in Non-Professional Caregivers: A Pilot Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Participants
2.2. Instruments
2.3. Intervention
2.4. Statistical Analysis
3. Results
3.1. Characteristics of the Sample
3.2. Incidence of Depression
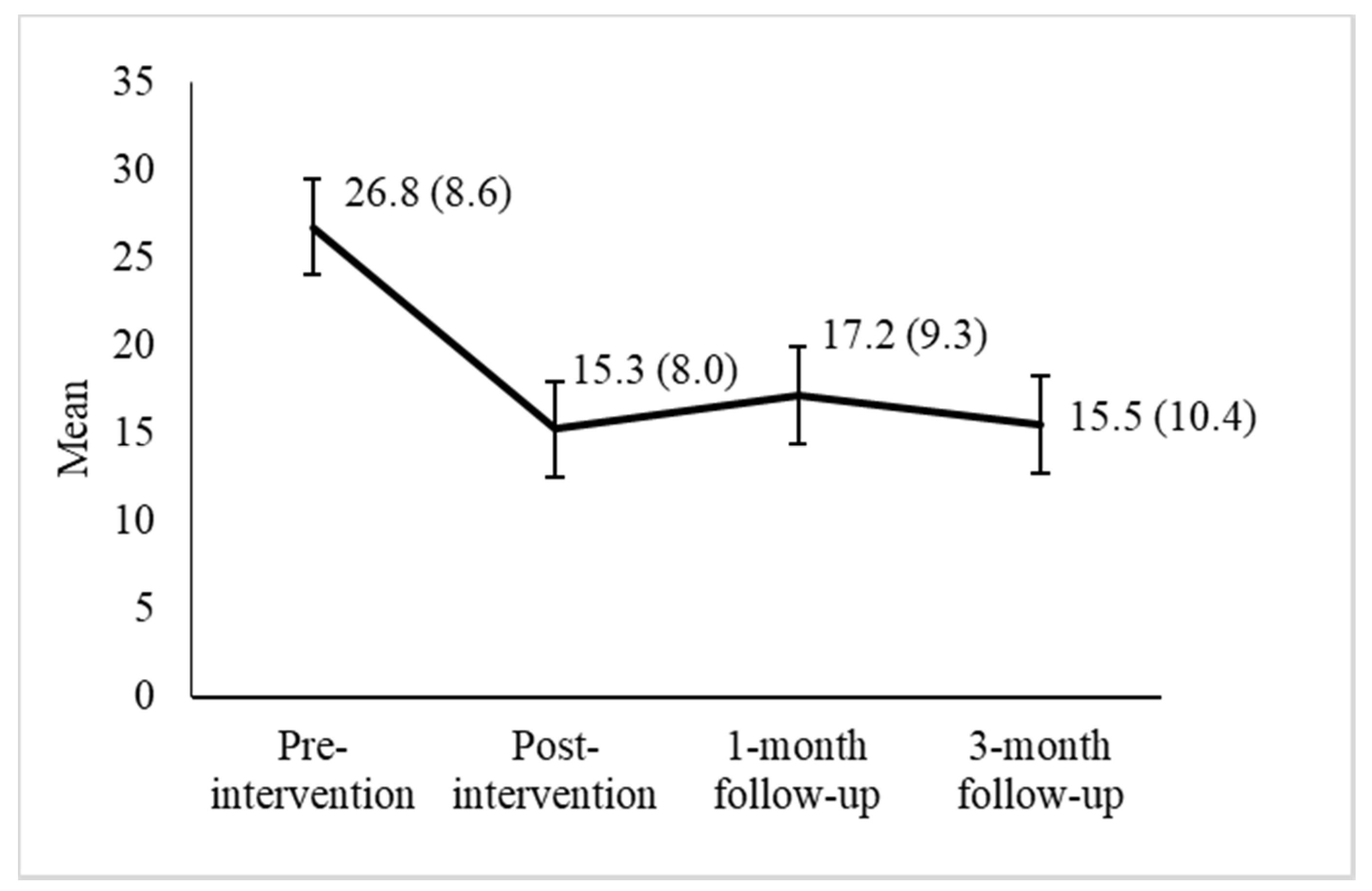
3.3. Depressive Symptomatology
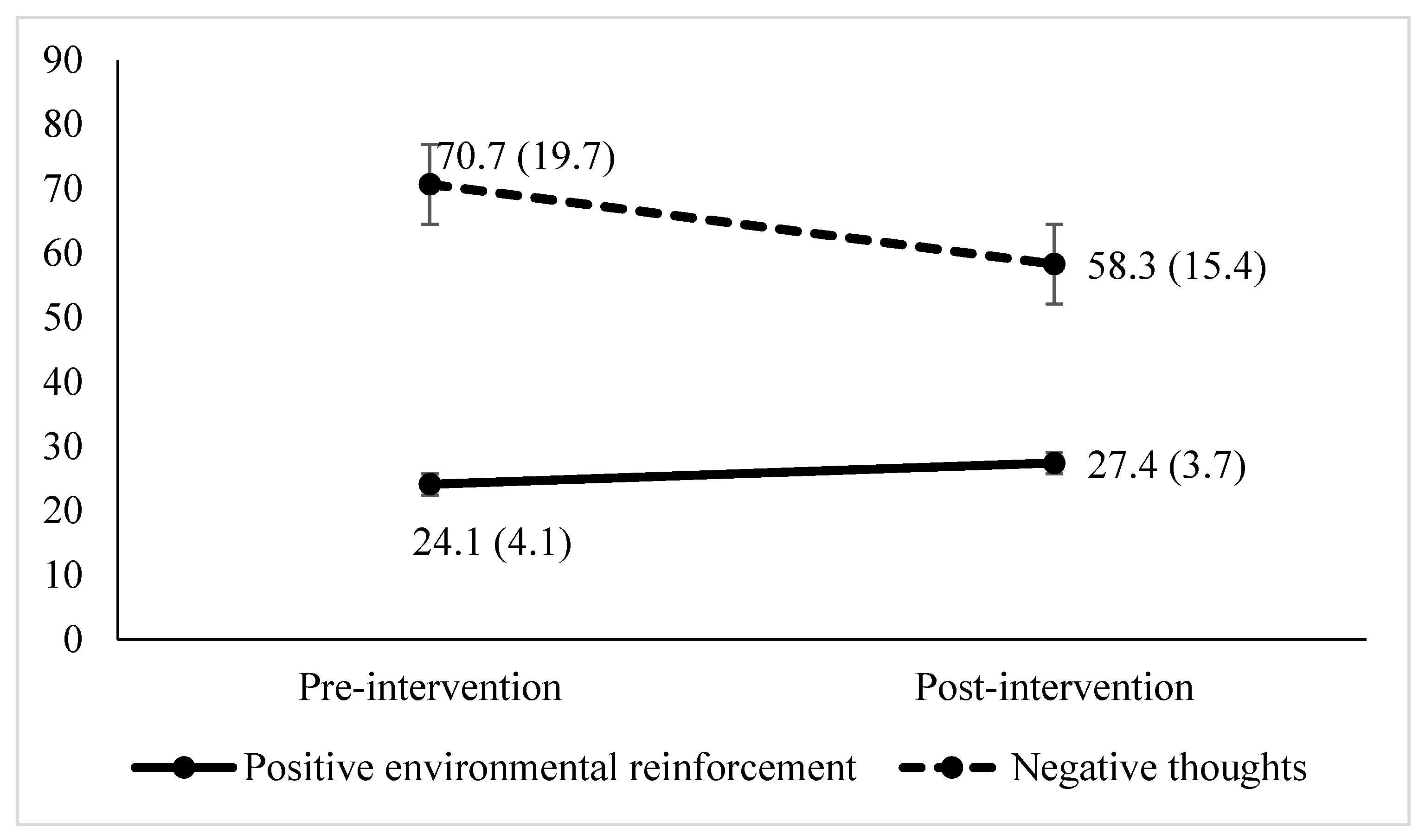
3.4. Variables for the Theoretical Model and Their Association with Depressive Symptoms
3.5. Variables Predictive for the Results for Depressive Symptoms
3.6. Adherence and Satisfaction with the Intervention
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Triantafillou, J.; Naiditch, M.; Repkova, K.; Stiehr, K.; Carretero, S.; Emilsson, T.; Di Santo, P.; Bednarik, R.; Brichtova, L.; Ceruzzi, F.; et al. Informal Care in the Long-Term Care System: European Overview Paper; Interlinks: Athens, Vienna, 2010. [Google Scholar]
- Palacios-Ceña, D.; Famoso-Pérez, P.; Salom-Moreno, J.; Carrasco-Garrido, P.; Pérez-Corrales, J.; Paras-Bravo, P.; Güeita-Rodriguez, J. “Living an Obstacle Course”: A qualitative study examining the experiences of caregivers of children with Rett syndrome. Int. J. Environ. Res. Public Health 2019, 16, 41. [Google Scholar] [CrossRef]
- Vázquez, F.L.; López, L.; Blanco, V.; Otero, P.; Torres, A.J.; Ferraces, M.J. The impact of decreased environmental reward in predicting depression severity in caregivers. An. Psychol. 2019, 35, 357–363. [Google Scholar]
- Simón, M.A.; Bueno, A.; Otero, P.; Blanco, V.; Vázquez, F.L. Caregiver burden and sleep quality in dependent people’s family caregivers. J. Clin. Med. 2019, 8, 1072. [Google Scholar] [CrossRef] [PubMed]
- Simón, M.A.; Bueno, A.; Otero, P.; Blanco, V.; Vázquez, F.L. Insomnia in female family caregivers of totally dependent patients with dementia: An exploratory study. Behav. Psychol. 2019, 27, 107–119. [Google Scholar]
- Meuser, T.M.; Marwit, S.J. A comprehensive, stage-sensitive model of grief in dementia caregiving. Gerontologist 2001, 41, 658–670. [Google Scholar] [CrossRef] [PubMed]
- Madruga, M.; Gozalo, M.; Prieto, J.; Adsuar, J.C.; Gusi, N. Psychological symptomatology in informal caregivers of persons with dementia: Influences on health-related quality of life. Int. J. Environ. Res. Public Health 2020, 17, 1078. [Google Scholar] [CrossRef] [PubMed]
- Perpiñá-Galvañ, J.; Orts-Beneito, N.; Fernández-Alcántara, M.; García-Sanjuán, S.; García-Caro, M.P.; Cabañero-Martínez, M.J. Level of burden and health-related quality of life in caregivers of palliative care patients. Int. J. Environ. Res. Public Health 2019, 16, 4806. [Google Scholar] [CrossRef]
- Vázquez, F.L.; Otero, P.; Simón, M.A.; Bueno, A.M.; Blanco, V. Psychometric properties of the Spanish version of the Caregiver Burden Inventory. Int. J. Environ. Res. Public Health 2019, 16, 217. [Google Scholar] [CrossRef]
- Schulz, R.; O’Brien, A.T.; Bookwala, J.; Fleissner, K. Psychiatric and physical morbidity effects of dementia caregiving: Prevalence, correlates, and causes. Gerontologist 1995, 35, 771–791. [Google Scholar] [CrossRef]
- Cuijpers, P. Depressive disorders in caregivers of dementia patients: A systematic review. Aging Ment. Health 2005, 9, 325–330. [Google Scholar] [CrossRef]
- Torres, Á.; Blanco, V.; Vázquez, F.L.; Díaz, O.; Otero, P.; Hermida, E. Prevalence of major depressive episodes in non-professional caregivers. Psychiatry Res. 2015, 226, 333–339. [Google Scholar] [CrossRef] [PubMed]
- Ayuso-Mateos, J.L.; Vázquez-Barquero, J.L.; Dowrick, C.; Lehtinen, V.; Dalgard, O.S.; Casey, P.; Wilkinson, C.; Lasa, L.; Page, H.; Dunn, G.; et al. Depressive disorders in Europe: Prevalence figures from the ODIN study. Br. J. Psychiatry 2001, 179, 308–316. [Google Scholar] [CrossRef] [PubMed]
- GBD 2017 Disease and Injury Incidence and Prevalence Collaborators. Global, regional, and national incidence, prevalence, and years lived with disability for 354 diseases and injuries for 195 countries and territories, 1990–2017: A systematic analysis for the Global Burden of Disease Study 2017. Lancet 2018, 392, 1789–1858. [Google Scholar] [CrossRef]
- Hardeveld, F.; Spijker, J.; De Graaf, R.; Nolen, W.A.; Beekman, A.T.F. Recurrence of major depressive disorder and its predictors in the general population: Results from the Netherlands Mental Health Survey and Incidence Study (NEMESIS). Psychol. Med. 2013, 43, 39–48. [Google Scholar] [CrossRef]
- Hoertel, N.; Blanco, C.; Oquendo, M.A.; Wall, M.M.; Olfson, M.; Falissard, B.; Franco, S.; Peyre, H.; Lemogne, C.; Limosin, F. A comprehensive model of predictors of persistence and recurrence in adults with major depression: Results from a national 3-year prospective study. J. Psychiatr. Res. 2017, 95, 19–27. [Google Scholar] [CrossRef]
- ten Have, M.; de Graaf, R.; van Dorsselaer, S.; Tuithof, M.; Kleinjan, M.; Penninx, B.W.J.H. Recurrence and chronicity of major depressive disorder and their risk indicators in a population cohort. Acta Psychiatr. Scand. 2018, 137, 503–515. [Google Scholar] [CrossRef]
- Greenberg, P.E.; Fournier, A.A.; Sisitsky, T.; Pike, C.T.; Kessler, R.C. The economic burden of adults with major depressive disorder in the United States (2005 and 2010). J. Clin. Psychiatry 2015, 76, 155–162. [Google Scholar] [CrossRef]
- Williamson, G.M.; Shaffer, D.R. Relationship quality and potentially harmful behaviors by spousal caregivers: How we were then, how we are now. Psychol. Aging 2001, 16, 217–226. [Google Scholar] [CrossRef]
- Institute of Medicine. Reducing Risks for Mental Disorders: Frontiers for Preventive Intervention Research; National Academic Press: Washington, DC, USA, 1994. [Google Scholar]
- Muñoz, R.F.; Beardslee, W.R.; Leykin, Y. Major depression can be prevented. Am. Psychol. 2012, 67, 285–295. [Google Scholar] [CrossRef]
- Vázquez, F.L.; Otero, P.; Torres, A.; Hermida, E.; Blanco, V.; Díaz, O. A brief problem-solving indicated-prevention intervention for prevention of depression in nonprofessional caregivers. Psicothema 2013, 25, 87–92. [Google Scholar]
- Otero, P.; Smit, F.; Cuijpers, P.; Torres, A.; Blanco, V.; Vázquez, F.L. Long-term efficacy of indicated prevention of depression in non-professional caregivers: Randomized controlled trial. Psychol. Med. 2015, 45, 1401–1412. [Google Scholar] [CrossRef] [PubMed]
- López, L.; Smit, F.; Cuijpers, P.; Otero, P.; Blanco, V.; Torres, Á.; Vázquez, F.L. Problem-solving intervention to prevent depression in non-professional caregivers: A randomized controlled trial with 8 years of follow-up. Psychol. Med. 2020, 50, 1002–1009. [Google Scholar] [CrossRef] [PubMed]
- Vázquez, F.L.; Hermida, E.; Torres, A.; Otero, P.; Blanco, V.; Díaz, O. Eficacia de una intervención preventiva cognitivo conductual en cuidadoras con síntomas depresivos elevados. [Efficacy of a brief cognitive-behavioral intervention in female caregivers with high depressive symptoms]. Behav. Psychol. 2014, 22, 79–96. [Google Scholar]
- Vázquez, F.L.; Torres, Á.; Blanco, V.; Otero, P.; Díaz, O.; Ferraces, M.J. Long-term follow-up of a randomized clinical trial assessing the efficacy of a brief cognitive-behavioral depression prevention intervention for caregivers with elevated depressive symptoms. Am. J. Geriatr. Psychiatry 2016, 24, 421–432. [Google Scholar] [CrossRef] [PubMed]
- Blanco, V.; Otero, P.; López, L.; Torres, Á.; Vázquez, F.L. Predictores del cambio clínicamente significativo en una intervención de prevención de la depresión. [Clinically significant predictors of change in an intervention for the prevention of depression]. Rev. Iberoam. Psicol. Salud. 2017, 8, 9–20. [Google Scholar] [CrossRef]
- Reese, R.J.; Conoley, C.W.; Brossart, D.F. The attractiveness of telephone counseling: An empirical investigation of client perceptions. J. Couns. Dev. 2006, 84, 54–60. [Google Scholar] [CrossRef]
- Vázquez, F.L.; López, L.; Torres, Á.J.; Otero, P.; Blanco, V.; Díaz, O.; Páramo, M. Analysis of the components of a cognitive-behavioral intervention for the prevention of depression administered via conference call to nonprofessional caregivers: A randomized controlled trial. Int. J. Environ. Res. Public Health 2020, 17, 2067. [Google Scholar] [CrossRef]
- Taylor, K.; Silver, L. Smartphone Ownership is Growing Rapidly around the World, but not Always Equally; Pew Research Center: Washington, DC, USA, 2019. [Google Scholar]
- Andersson, G.; Cuijpers, P. Internet-based and other computerized psychological treatments for adult depression: A meta-analysis. Cogn. Behav. Ther. 2009, 38, 196–205. [Google Scholar] [CrossRef]
- Nicholas, J.; Ringland, K.E.; Graham, A.K.; Knapp, A.A.; Lattie, E.G.; Kwasny, M.J.; Mohr, D.C. Stepping up: Predictors of ‘stepping’ within an iCBT stepped-care intervention for depression. Int. J. Environ. Res. Public Health 2019, 16, 4689. [Google Scholar] [CrossRef]
- Arean, P.A.; Hallgren, K.A.; Jordan, J.T.; Gazzaley, A.; Atkins, D.C.; Heagerty, P.J.; Anguera, J.A. The use and effectiveness of mobile Apps for depression: Results from a fully remote clinical trial. J. Med. Internet Res. 2016, 18, e330. [Google Scholar] [CrossRef]
- Ly, K.H.; Trüschel, A.; Jarl, L.; Magnusson, S.; Windahl, T.; Johansson, R.; Carlbring, P.; Andersson, G. Behavioural activation versus mindfulness-based guided self-help treatment administered through a smartphone application: A randomised controlled trial. BMJ Open 2014, 4, e003440. [Google Scholar] [CrossRef] [PubMed]
- Swift, J.K.; Greenberg, R.P. Premature discontinuation in adult psychotherapy: A meta-analysis. J. Consult. Clin. Psychol. 2012, 80, 547–559. [Google Scholar] [CrossRef] [PubMed]
- Otero, P.; Vázquez, F.L.; Hermida, E.; Díaz, O.; Torres, Á. Relationship of cognitive behavioral therapy effects and homework in an indicated prevention of depression intervention for non-professional caregivers. Psychol. Rep. 2015, 116, 841–854. [Google Scholar] [CrossRef] [PubMed]
- Miltenberger, R.G. Behavior Modification: Principles and Procedures, 5th ed.; Wadsworth/Thomson Learning: Belmont, MA, USA, 2012. [Google Scholar]
- Radloff, L.S. The CES-D Scale: A self-report depression scale for research in the general population. Appl. Psychol. Meas. 1977, 1, 385–401. [Google Scholar] [CrossRef]
- Vázquez, F.L.; Blanco, V.; López, M. An adaptation of the Center for Epidemiologic Studies Depression Scale for use in non-psychiatric Spanish populations. Psychiatry Res. 2007, 149, 247–252. [Google Scholar] [CrossRef]
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders; American Psychiatric Association: Washington, DC, USA, 2013. [Google Scholar]
- First, M.B.; Williams, J.B.W.; Karg, R.S.; Spitzer, R.L. Structured Clinical Interview for DSM-5® Disorders—Clinician Version (SCID-5-CV); American Psychiatric Association Publishing: Arlington, VA, USA, 2015. [Google Scholar]
- Armento, M.E.A.; Hopko, D.R. The Environmental Reward Observation Scale (EROS): Development, validity, and reliability. Behav. Ther. 2007, 38, 107–119. [Google Scholar] [CrossRef]
- Barraca, J.; Pérez-Álvarez, M. Adaptación española del Environmental Reward Observation Scale (EROS) [Spanish adaptation of Environmental Reward Observation Scale (EROS)]. Ansiedad Estrés 2010, 16, 95–107. [Google Scholar]
- Hollon, S.D.; Kendall, P.C. Cognitive self-statements in depression: Development of an automatic thoughts questionnaire. Cognit. Ther. Res. 1980, 4, 383–395. [Google Scholar] [CrossRef]
- Otero, P.; Vázquez, F.L.; Blanco, V.; Torres, Á. Propiedades psicométricas del Cuestionario de Pensamientos Automáticos (ATQ) en la población de cuidadores familiares [Psychometric properties of the Automatic Thoughts Questionnaire (ATQ) in family caregivers]. Behav. Psychol. 2017, 25, 387–403. [Google Scholar]
- Larsen, D.L.; Attkisson, C.C.; Hargreaves, W.A.; Nguyen, T.D. Assessment of client/patient satisfaction: Development of a general scale. Eval. Program Plan. 1979, 2, 197–207. [Google Scholar] [CrossRef]
- Vázquez, F.L.; Torres, Á.; Otero, P.; Blanco, V.; Attkisson, C.C. Psychometric properties of the Castilian Spanish version of the Client Satisfaction Questionnaire (CSQ-8). Curr. Psychol. 2019, 38, 829–835. [Google Scholar] [CrossRef]
- Lewinsohn, P.M.; Hoberman, H.; Teri, L.; Hautzinger, M. An integrative theory of depression. In Theoretical Issues in Behaviour Therapy; Reiss, S., Bootzin, R.R., Eds.; Academic Press: New York, NY, USA, 1985; pp. 313–359. [Google Scholar]
- Cohen, J. Statistical Power Analysis for the Behavioural Sciences, 2nd ed.; Lawrence Erlbaum Associates, Inc.: Hillsdale, NJ, USA, 1988. [Google Scholar]
- Domenéch, J.M.; Navarro, J.B. Regresión Lineal Múltiple con Predictores Cuantitativos y Categóricos [Multiple Regression with Quantitative and Cathegorical Predictors]; Signo: Barcelona, Spain, 2006. [Google Scholar]
- Vázquez, F.L.; Otero, P.; López, L.; Blanco, V.; Torres, A.; Díaz, O. La prevención de la depresión en cuidadores a través de multiconferencia telefónica [Prevention of depression in caregivers through conference calls]. Clin. Salud. 2018, 29, 14–20. [Google Scholar] [CrossRef]
- Muñoz, R.F.; Cuijpers, P.; Smit, F.; Barrera, A.Z.; Leykin, Y. Prevention of major depression. Annu. Rev. Clin. Psychol. 2010, 6, 181–212. [Google Scholar] [CrossRef] [PubMed]
- Hollon, S.D.; Muñoz, R.F.; Barlow, D.H.; Beardslee, W.R.; Bell, C.C.; Bernal, G.; Clarke, G.N.; Franciosi, L.P.; Kazdin, A.E.; Kohn, L.; et al. Psychosocial intervention development for the prevention and treatment of depression: Promoting innovation and increasing access. Biol. Psychiatry 2002, 52, 610–630. [Google Scholar] [CrossRef]
- New Freedom Commission on Mental Health. Achieving the Promise: Transforming Mental Health Care in America; DHHS: Rockville, MD, USA, 2003. [Google Scholar]
- Muñoz, R.F.; Mrazek, P.J.; Haggerty, R.J. Institute of Medicine report on prevention of mental disorders: Summary and commentary. Am. Psychol. 1996, 51, 1116–1122. [Google Scholar] [CrossRef] [PubMed]
| Module | Content |
|---|---|
| Module 1 | Presentation of group members |
| Purpose of the program | |
| Information about depression and active coping of symptoms | |
| Mood rating | |
| Training in diaphragmatic breathing | |
| Self-reinforcement | |
| Homework: Mood rating, practice breathing control technique, self-reinforcement | |
| Module 2 | Explanation of the relationship between pleasant activities and mood |
| Guidelines and strategies to increase pleasant activities | |
| Planning pleasant activities | |
| Behavioral contract | |
| Homework: Mood rating, practice breathing control technique, self-reinforcement, perform the planned pleasant activities | |
| Module 3 | Explanation of the relationship between thoughts and mood |
| Thought management techniques (direct approach, priming, distraction) | |
| Planning pleasant activities | |
| Behavioral contract | |
| Homework: Mood rating, practice breathing control technique, self-reinforcement, perform the planned pleasant activities, practice the thought management techniques | |
| Module 4 | Explanation of the relationship between social contact and mood |
| Guidelines and strategies to increase and improve social relationships | |
| Planning pleasant and social activities | |
| Homework: Mood rating, practice breathing control technique, self-reinforcement, perform the planned pleasant activities, practice the thought management techniques, make social contacts | |
| Module 5 | Review of what was learned. Maintaining progress |
| Relapse prevention | |
| Farewell and closure |
| Sociodemographic Variables | n = 31 | % |
|---|---|---|
| Sex | ||
| Men | 2 | 6.5 |
| Women | 29 | 93.5 |
| Age | ||
| M | 54 | |
| SD | 9.4 | |
| Range | 41–71 | |
| Marital status | ||
| With partner | 29 | 93.5 |
| No partner (single, separated, divorced, widowed) | 2 | 6.5 |
| Social class | ||
| Low/lower middle | 18 | 58.1 |
| Middle/upper middle | 13 | 41.9 |
| Monthly household income | ||
| Up to €999 | 7 | 22.6 |
| Between 1000 and 1999 euros | 18 | 58.1 |
| €2000 or more | 6 | 19.3 |
| Level of education | ||
| Up to primary school education | 14 | 45.2 |
| Secondary/University | 17 | 54.8 |
| Primary activity | ||
| Active worker | 15 | 48.4 |
| Unemployed/retired/housework | 16 | 51.6 |
| Care situation variables | ||
| Care recipient sex | ||
| Male | 16 | 51.6 |
| Female | 15 | 48.4 |
| Care recipient age | ||
| M | 54 | |
| SD | 28.1 | |
| Range | 5–93 | |
| Relationship to caregiver | ||
| Son/daughter | 12 | 38.7 |
| Father/mother | 9 | 29 |
| Other family members | 10 | 32.3 |
| Care recipient diagnosis | ||
| Mental/neurological disorders/brain damage | 15 | 48.4 |
| Diseases of the skeletomuscular/connective tissue/cardiovascular/respiratory systems | 7 | 22.6 |
| Chromosomal/congenital/perinatal abnormalities | 5 | 16.1 |
| Others | 4 | 12.9 |
| Daily hours of care | ||
| M | 15.7 | |
| SD | 7.6 | |
| Care duration (years) | ||
| M | 15.9 | |
| SD | 11.9 | |
| Clinical variables | ||
| CES-D Score | ||
| M | 26.8 | |
| SD | 8.6 | |
| EROS Score | ||
| M | 24.1 | |
| SD | 4.1 | |
| ATQ Score | ||
| M | 70.7 | |
| SD | 19.9 |
| t | p | d | 95% CI | ||
|---|---|---|---|---|---|
| Variables | Minimum | Maximum | |||
| Depressive symptomatology (CES-D) | |||||
| Pre-intervention vs. post-intervention | 7.62 | <0.001 | 1.37 | 0.87 | 1.86 |
| Pre-intervention vs. one-month follow-up | 5.09 | <0.001 | 0.91 | 0.49 | 1.33 |
| Pre-intervention vs. three-month follow-up | 6.89 | <0.001 | 1.24 | 0.76 | 1.7 |
| Positive Environmental Reinforcement (EROS) | |||||
| Pre-intervention vs. post-intervention | −5.61 | <0.001 | 1.01 | 0.57 | 1.43 |
| Automatic negative thoughts (ATQ) | |||||
| Pre-intervention vs. post-intervention | 3.47 | <0.001 | 0.62 | 0.23 | 1 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Otero, P.; Hita, I.; Torres, Á.J.; Vázquez, F.L. Brief Psychological Intervention Through Mobile App and Conference Calls for the Prevention of Depression in Non-Professional Caregivers: A Pilot Study. Int. J. Environ. Res. Public Health 2020, 17, 4578. https://doi.org/10.3390/ijerph17124578
Otero P, Hita I, Torres ÁJ, Vázquez FL. Brief Psychological Intervention Through Mobile App and Conference Calls for the Prevention of Depression in Non-Professional Caregivers: A Pilot Study. International Journal of Environmental Research and Public Health. 2020; 17(12):4578. https://doi.org/10.3390/ijerph17124578
Chicago/Turabian StyleOtero, Patricia, Isabel Hita, Ángela J. Torres, and Fernando L. Vázquez. 2020. "Brief Psychological Intervention Through Mobile App and Conference Calls for the Prevention of Depression in Non-Professional Caregivers: A Pilot Study" International Journal of Environmental Research and Public Health 17, no. 12: 4578. https://doi.org/10.3390/ijerph17124578
APA StyleOtero, P., Hita, I., Torres, Á. J., & Vázquez, F. L. (2020). Brief Psychological Intervention Through Mobile App and Conference Calls for the Prevention of Depression in Non-Professional Caregivers: A Pilot Study. International Journal of Environmental Research and Public Health, 17(12), 4578. https://doi.org/10.3390/ijerph17124578






