Evaluation of Inflammation by Cytokine Production Following Combined Exposure to Ultraviolet and Radiofrequency Radiation of Mobile Phones on 3D Reconstructed Human Skin In Vitro
Abstract
1. Introduction
1.1. RF Exposure of Mobile Wireless Technology
1.2. Skin Exposure to RF
1.3. Skin Exposure to UV
1.4. Combined Exposure to RF and Other Physical Agents
2. Materials and Methods
2.1. The 3D Full Thickness In Vitro Skin Model
2.2. Cell Viability–MTT Assay
2.3. Matrix Metalloproteinase-1 (MMP-1)
2.4. Cytokines
2.5. Exposure System and Dosimetry
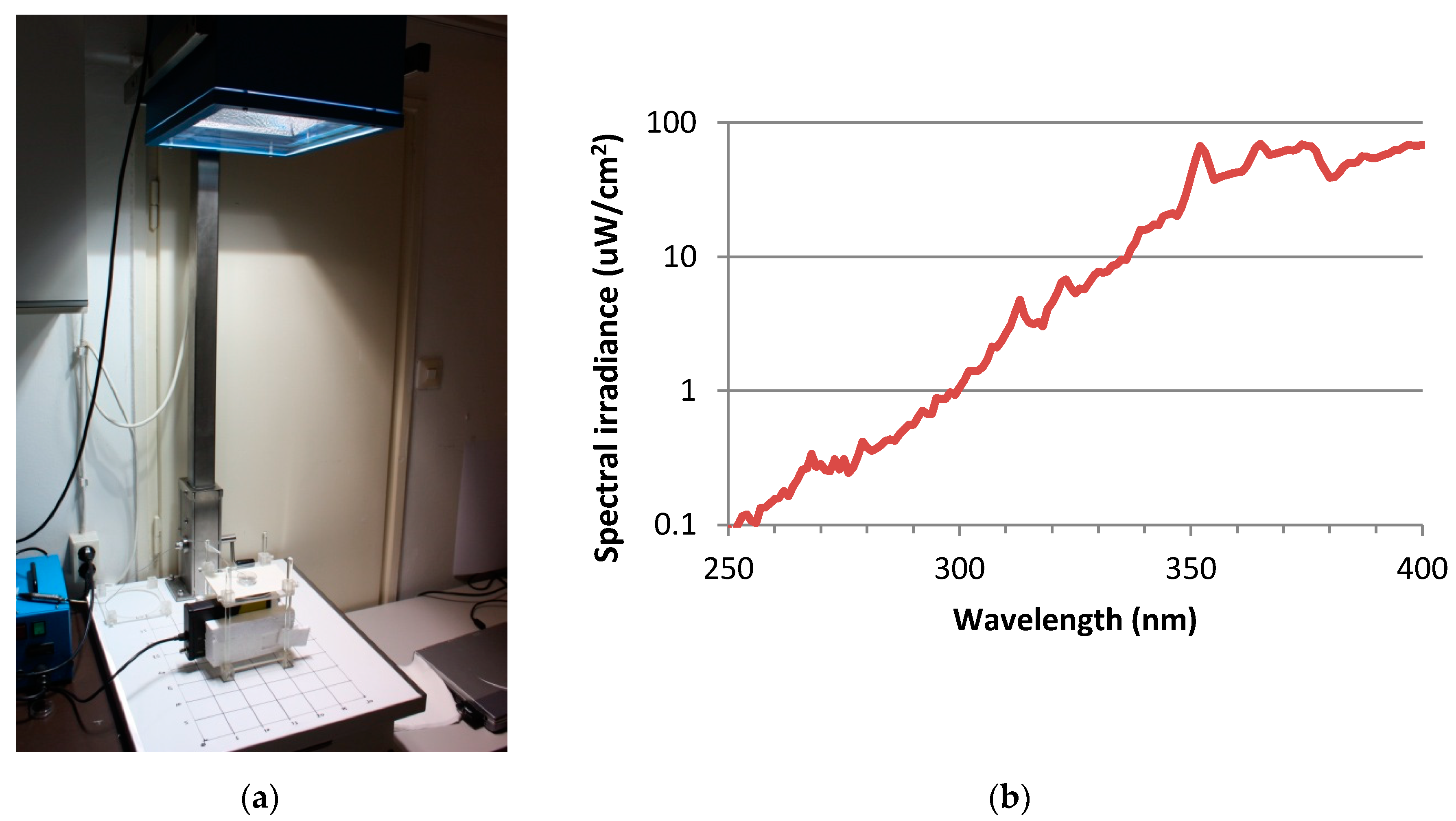
2.5.1. Exposure to Solar UV Radiation
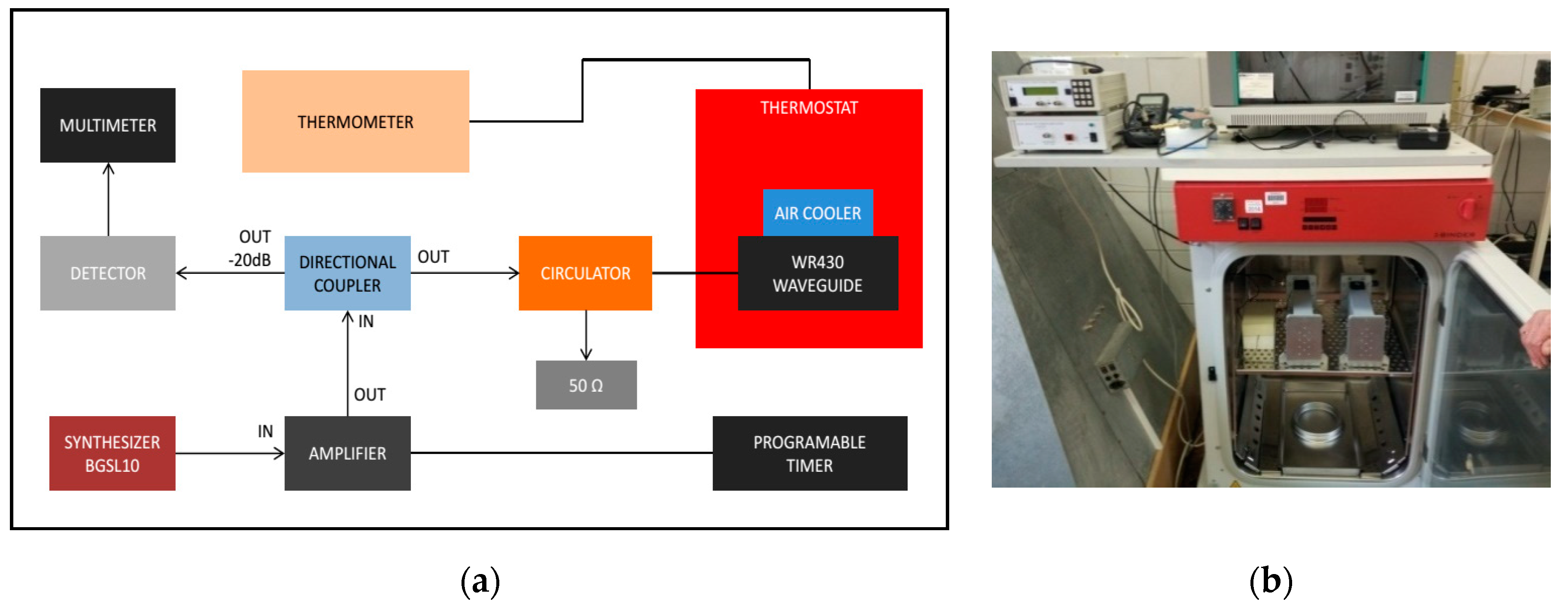
2.5.2. RF Exposure System and Dosimetry
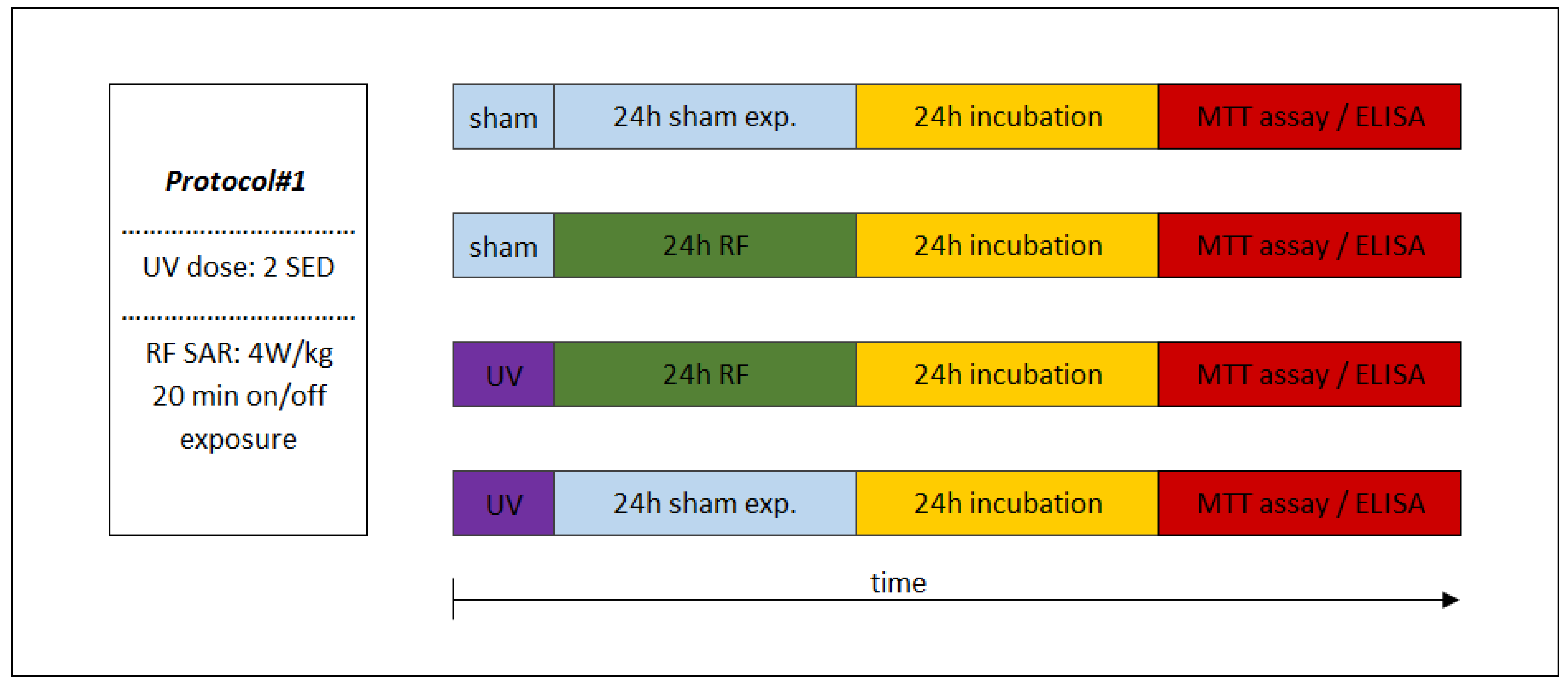
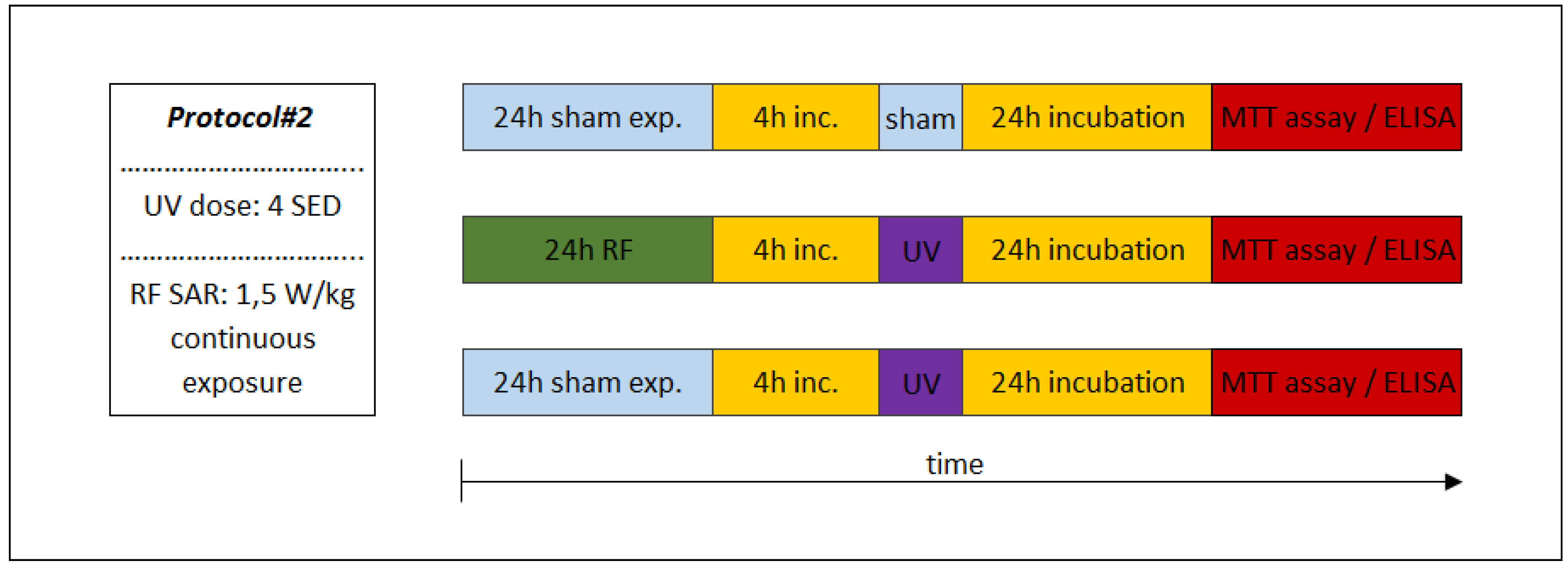
2.6. Experimental Protocols
2.7. Statistical Analysis
3. Results
3.1. MTT Assay
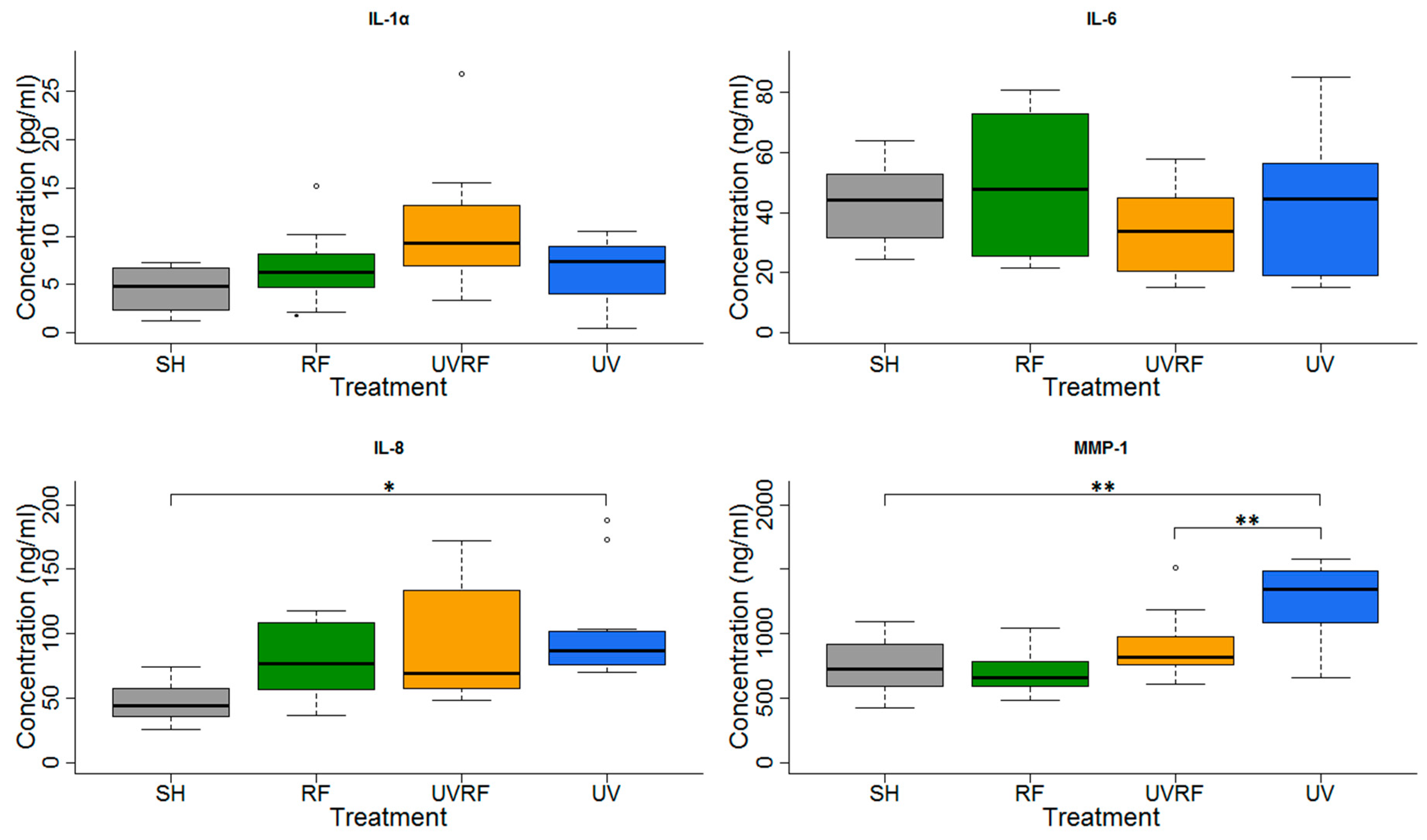
3.2. Cooperative Effects of RF (Protocol#1)
3.3. Protective Effects (Adaptive Response) (Protocol#2)
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Ericcsson. Ericcsson Mobility Report November. 2019. Available online: https://www.ericsson.com/en/mobility-report/reports (accessed on 8 April 2020).
- Baan, R.; Grosse, Y.; Lauby-Secretan, B.; El Ghissassi, F.; Bouvard, V.; Benbrahim-Tallaa, L.; Guha, N.; Islami, F.; Galichet, L.; Straif, K. Carcinogenicity of radiofrequency electromagnetic fields. Lancet Oncol. 2011, 12, 624–626. [Google Scholar] [CrossRef]
- El Ghissassi, F.; Baan, R.; Straif, K.; Grosse, Y.; Secretan, B.; Bouvard, V.; Benbrahim-Tallaa, L.; Guha, N.; Freeman, C.; Galichet, L.; et al. A review of human carcinogens—Part D: Radiation. Lancet Oncol. 2009, 10, 751–752. [Google Scholar] [CrossRef]
- Roach, W.P. Radio Frequency Radiation Dosimetry Handbook, 5th ed.; Roach, W.P., Ed.; Air Force Research Laboratory, 711 Human Performance Wing: Brooks City-Base, TX, USA, 2009. [Google Scholar]
- Gabriel, C.; Gabriel, S.; Corthout, E. The dielectric properties of biological tissues. 1. Literature survey. Phys. Med. Biol. 1996, 41, 2231–2249. [Google Scholar] [CrossRef] [PubMed]
- Gabriel, S.; Lau, R.W.; Gabriel, C. The dielectric properties of biological tissues. 3. Parametric models for the dielectric spectrum of tissues. Phys. Med. Biol. 1996, 41, 2271–2293. [Google Scholar] [CrossRef] [PubMed]
- Alekseev, S.I.; Radzievsky, A.A.; Logani, M.K.; Ziskin, M.C. Millimeter wave dosimetry of human skin. Bioelectromagnetics 2008, 29, 65–70. [Google Scholar] [CrossRef]
- Schmid, G.; Kuster, N. The Discrepancy vetween Maximum in Vitro Exposure Levels and Realistic Conservative Exposure Levels of Mobile Phones Operating at 900/1800 MHz. Bioelectromagnetics 2015, 36, 133–148. [Google Scholar] [CrossRef]
- Funahashi, D.; Hirata, A.; Kodera, S.; Foster, K.R. Area-Averaged Transmitted Power Density at Skin Surface as Metric to Estimate Surface Temperature Elevation. IEEE Access 2018, 6, 77665–77674. [Google Scholar] [CrossRef]
- WHO. WHO Fact Sheet No.193. (Reviewed in October 2014). Available online: https://www.who.int/news-room/fact-sheets/detail/electromagnetic-fields-and-public-health-mobile-phones (accessed on 30 March 2020).
- Vijayalaxmi; Prihoda, T.J. Genetic damage in mammalian somatic cells exposed to radiofrequency radiation: A meta-analysis of data from 63 publications (1990–2005). Radiat. Res. 2008, 169, 561–574. [Google Scholar] [CrossRef]
- Vijayalaxmi; Prihoda, T.J. Genetic damage in human cells exposed to non-ionizing radiofrequency fields: A meta-analysis of the data from 88 publications (1990–2011). Mutat. Res. Genet. Toxicol. Environ. Mutagenesis 2012, 749, 1–16. [Google Scholar] [CrossRef]
- Vijayalaxmi; Prihoda, T.J. Comprehensive Review of Quality of Publications and Meta-analysis of Genetic Damage in Mammalian Cells Exposed to Non-Ionizing Radiofrequency Fields. Radiat. Res. 2019, 191, 20–30. [Google Scholar] [CrossRef]
- Anderson, V.; Rowley, J. Measurements of skin surface temperature during mobile phone use. Bioelectromagnetics 2007, 28, 159–162. [Google Scholar] [CrossRef] [PubMed]
- Straume, A.; Oftedal, G.; Johnsson, A. Skin temperature increase caused by a mobile phone: A methodological infrared camera study. Bioelectromagnetics 2005, 26, 510–519. [Google Scholar] [CrossRef] [PubMed]
- Kageyama, I.; Masuda, H.; Morimatsu, Y.; Ishitake, T.; Sakakibara, K.; Hikage, T.; Hirata, A. Comparison of temperature elevation between in physical phantom skin and in human skin during local exposure to a 28 GHz millimeter-wave. In Proceedings of the 2019 Joint International Symposium on Electromagnetic Compatibility, Sapporo and Asia-Pacific International Symposium on Electromagnetic Compatibility (EMC Sapporo/APEMC), IEEE, Sapporo, Japan, 23–27 May 2019; pp. 766–769. [Google Scholar] [CrossRef]
- Ghosn, R.; Thuróczy, G.; Loos, N.; Brenet-Dufour, V.; Liabeuf, S.; De Seze, R.; Selmaoui, B. Effects of GSM 900 MHz on Middle Cerebral Artery Blood Flow Assessed by Transcranial Doppler Sonography. Radiat. Res. 2013, 178, 543–550. [Google Scholar] [CrossRef]
- Kubat, N.J.; Moffett, J.; Fray, L.M. Effect of pulsed electromagnetic field treatment on programmed resolution of inflammation pathway markers in human cells in culture. J. Inflamm. Res. 2015, 8, 59–69. [Google Scholar] [CrossRef]
- Millenbaugh, N.J.; Roth, C.; Sypniewska, R.; Chan, V.; Eggers, J.S.; Kiel, J.L.; Blystone, R.V.; Mason, P.A. Gene expression changes in the skin of rats induced by prolonged 35 GHz millimeter-wave exposure. Radiat. Res. 2008, 169, 288–300. [Google Scholar] [CrossRef] [PubMed]
- Loos, N.; Thuroczy, G.; Ghosn, R.; Brenet-Dufour, V.; Liabeuf, S.; Selmaoui, B.; Libert, J.P.; Bach, V.; Diouf, M.; de Seze, R. Is the Effect of Mobile Phone Radiofrequency Waves on Human Skin Perfusion Non-Thermal? Microcirculation 2013, 20, 629–636. [Google Scholar] [CrossRef]
- Monfrecola, G.; Moffa, G.; Procaccini, E.M. Non-ionizing electromagnetic radiations, emitted by a cellular phone, modify cutaneous blood flow. Dermatology 2003, 207, 10–14. [Google Scholar] [CrossRef]
- Vecsei, Z.; Csatho, A.; Thuroczy, G.; Hernadi, I. Effect of a Single 30 min UMTS Mobile Phone-Like Exposure on the Thermal Pain Threshold of Young Healthy Volunteers. Bioelectromagnetics 2013, 34, 530–541. [Google Scholar] [CrossRef]
- Xu, S.S.; Chen, G.D.; Chen, C.J.; Sun, C.; Zhang, D.Y.; Murbach, M.; Kuster, N.; Zeng, Q.L.; Xu, Z.P. Cell Type-Dependent Induction of DNA Damage by 1800 MHz Radiofrequency Electromagnetic Fields Does Not Result in Significant Cellular Dysfunctions. PLoS ONE 2013, 8, e54906. [Google Scholar] [CrossRef]
- Karinen, A.; Heinavaara, S.; Nylund, R.; Leszczynski, D. Mobile phone radiation might alter protein expression in human skin. BMC Genom. 2008, 9. [Google Scholar] [CrossRef]
- Mahamoud, Y.S.; Aite, M.; Martin, C.; Zhadobov, M.; Sauleau, R.; Le Drean, Y.; Habauzit, D. Additive Effects of Millimeter Waves and 2-Deoxyglucose Co-Exposure on the Human Keratinocyte Transcriptome. PLoS ONE 2016, 11, e0160810. [Google Scholar] [CrossRef]
- Kimata, H. Enhancement of allergic skin wheal responses in patients with atopic eczema/dermatitis syndrome by playing video games or by a frequently ringing mobile phone. Eur. J. Clin. Investig. 2003, 33, 513–517. [Google Scholar] [CrossRef]
- Miller, C.S. Toxicant-induced loss of tolerance–An emerging theory of disease? Environ. Health Perspect. 1997, 105, 445–453. [Google Scholar] [CrossRef]
- Miller, C.S. The compelling anomaly of chemical intolerance. Ann. N. Y. Acad. Sci. 2001, 933, 1–23. [Google Scholar] [CrossRef]
- IARC. Radiation; IARC: Lyon, France, 2012; Volume 100D, pp. 35–101. [Google Scholar]
- Diffey, B.L. Solar Ultraviolet-Radiation Effects on Biological-Systems. Phys. Med. Biol. 1991, 36, 299–328. [Google Scholar] [CrossRef]
- Ullrich, S.E.; Kripke, M.; Ananthaswamy, H.N. Mechanisms underlying UV-induced immune suppression: Implications for sunscreen design. Exp. Dermatol. 2002, 11, 13–16. [Google Scholar] [CrossRef]
- Dahle, J.; Kvam, E. Induction of delayed mutations and chromosomal instability in fibroblasts after UVA-, UVB-, and X-radiation. Cancer Res. 2003, 63, 1464–1469. [Google Scholar]
- Young, A.R.; Potten, C.S.; Nikaido, O.; Parsons, P.G.; Boenders, J.; Ramsden, J.M.; Chadwick, C.A. Human melanocytes and keratinocytes exposed to UVB or UVA in vivo show comparable levels of thymine dimers. J. Investig. Dermatol. 1998, 111, 936–940. [Google Scholar] [CrossRef]
- Sander, C.S.; Chang, H.; Hamm, F.; Elsner, P.; Thiele, J.J. Role of oxidative stress and the antioxidant network in cutaneous carcinogenesis. Int. J. Dermatol. 2004, 43, 326–335. [Google Scholar] [CrossRef]
- Phillipson, R.P.; Tobi, S.E.; Morris, J.A.; McMillan, T.J. UV-A induces persistent genomic instability in human keratinocytes through an oxidative stress mechanism. Free Radic. Bio. Med. 2002, 32, 474–480. [Google Scholar] [CrossRef]
- Shorrocks, J.; Paul, N.D.; McMillan, T.J. The dose rate of UVA treatment influences the cellular response of HaCaT keratinocytes. J. Investig. Dermatol. 2008, 128, 685–693. [Google Scholar] [CrossRef]
- Limoli, C.L.; Giedzinski, E.; Bonner, W.M.; Cleaver, J.E. UV-induced replication arrest in the xeroderma pigmentosum variant leads to DNA double-strand breaks, gamma-H2AX formation, and Mre11 relocalization. Proc. Natl. Acad. Sci. USA 2002, 99, 233–238. [Google Scholar] [CrossRef]
- Limoli, C.L.; Giedzinski, E.; Morgan, W.F.; Cleaver, J.E. Polymerase eta deficiency in the xeroderma pigmentosum variant uncovers an overlap between the S phase checkpoint and double-strand break repair. Proc. Natl. Acad. Sci. USA 2000, 97, 7939–7946. [Google Scholar] [CrossRef]
- Greinert, R.; Volkmer, B.; Henning, S.; Breitbart, E.W.; Greulich, K.O.; Cardoso, M.C.; Rapp, A. UVA-induced DNA double-strand breaks result from the repair of clustered oxidative DNA damages. Nucleic Acids Res. 2012, 40, 10263–10273. [Google Scholar] [CrossRef]
- Wischermann, K.; Popp, S.; Moshir, S.; Scharffetter-Kochanek, K.; Wlaschek, M.; de Gruijl, F.; Hartschuh, W.; Greinert, R.; Volkmer, B.; Faust, A.; et al. UVA radiation causes DNA strand breaks, chromosomal aberrations and tumorigenic transformation in HaCaT skin keratinocytes (vol 27, pg 4269, 2008). Oncogene 2008, 27, 4269–4280. [Google Scholar] [CrossRef]
- Meltz, M.L.; Walker, K.A.; Erwin, D.N. Radiofrequency (microwave) radiation exposure of mammalian cells during UV-induced DNA repair synthesis. Radiat. Res. 1987, 110, 255–266. [Google Scholar] [CrossRef]
- Dicarlo, A.L.; Hargis, M.T.; Penafiel, L.M.; Litovitz, T.A. Short-term magnetic field exposures (60 Hz) induce protection against ultraviolet radiation damage. Int. J. Radiat. Biol. 1999, 75, 1541–1549. [Google Scholar] [CrossRef]
- Zhijian, C.; Xiaoxue, L.; Yezhen, L.; Deqiang, L.; Shijie, C.; Lifen, J.; Jianlin, L.; Jiliang, H. Influence of 1.8-GHz (GSM) radiofrequency radiation (RFR) on DNA damage and repair induced by X-rays in human leukocytes in vitro. Mutat. Res. 2009, 677, 100–104. [Google Scholar] [CrossRef]
- Litovitz, T.A.; Montrose, C.J.; Doinov, P.; Brown, K.M.; Barber, M. Superimposing spatially coherent electromagnetic noise inhibits field-induced abnormalities in developing chick embryos. Bioelectromagnetics 1994, 15, 105–113. [Google Scholar] [CrossRef]
- Litovitz, T.A.; Penafiel, L.M.; Farrel, J.M.; Krause, D.; Meister, R.; Mullins, J.M. Bioeffects induced by exposure to microwaves are mitigated by superposition of ELF noise. Bioelectromagnetics 1997, 18, 422–430. [Google Scholar] [CrossRef]
- Dimova, E.G.; Bryant, P.E.; Chankova, S.G. “Adaptive response”—Some underlying mechanisms and open questions. Genet. Mol. Biol. 2008, 31, 396–408. [Google Scholar] [CrossRef]
- Vijayalaxmi; Cao, Y.; Scarfi, M.R. Adaptive response in mammalian cells exposed to non-ionizing radiofrequency fields: A review and gaps in knowledge. Mutat. Res. Rev. Mutat. 2014, 760, 36–45. [Google Scholar] [CrossRef]
- Heikkinen, P.; Kosma, V.M.; Alhonen, L.; Huuskonen, H.; Komulainen, H.; Kumlin, T.; Laitinen, J.T.; Lang, S.; Puranen, L.; Juutilainen, J. Effects of mobile phone radiation on UV-induced skin tumourigenesis in ornithine decarboxylase transgenic and non-transgenic mice. Int. J. Radiat. Biol. 2003, 79, 221–233. [Google Scholar] [CrossRef] [PubMed]
- Faller, C.; Bracher, M.; Dami, N.; Roguet, R. Predictive ability of reconstructed human epidermis equivalents for the assessment of skin irritation of cosmetics. Toxicol. Vitr. 2002, 16, 557–572. [Google Scholar] [CrossRef]
- OECD. OECD 439 (2013) Guidelines for the Testing of Chemicals In Vitro Skin Irritation: Reconstructed Human Epidermis Test Method. Available online: https://ntp.niehs.nih.gov/iccvam/suppdocs/feddocs/oecd/oecd-tg439-2013-508.pdf (accessed on 9 April 2020).
- Afaq, F.; Abu Zaid, M.; Khan, N.; Dreher, M.; Mukhtar, H. Protective effect of pomegranate-derived products on UVB-mediated damage in human reconstituted skin. Exp. Dermatol. 2009, 18, 553–561. [Google Scholar] [CrossRef]
- Brennan, M.; Bhatti, H.; Nerusu, K.C.; Bhagavathula, N.; Kang, S.; Fisher, G.J.; Varani, J.; Voorhees, J.J. Matrix metalloproteinase-1 is the major collagenolytic enzyme responsible for collagen damage in UV-irradiated human skin. Photochem. Photobiol. 2003, 78, 43–48. [Google Scholar] [CrossRef]
- Watanabe, H.; Shimizu, T.; Nishihira, J.; Abe, R.; Nakayama, T.; Taniguchi, M.; Sabe, H.; Ishibashi, T.; Shimizu, H. Ultraviolet A-induced production of matrix metalloproteinase-1 is mediated by macrophage migration inhibitory factor (MIF) in human dermal fibroblasts. J. Biol. Chem. 2004, 279, 1676–1683. [Google Scholar] [CrossRef]
- Pittayapruek, P.; Meephansan, J.; Prapapan, O.; Komine, M.; Ohtsuki, M. Role of Matrix Metalloproteinases in Photoaging and Photocarcinogenesis. Int. J. Mol. Sci. 2016, 17. [Google Scholar] [CrossRef]
- Chung, J.H.; Youn, S.H.; Koh, W.S.; Eun, H.C.; Cho, K.H.; Park, K.C.; Youn, J.I. Ultraviolet B irradiation-enhanced interleukin (IL)-6 production and mRNA expression are mediated by IL-1 alpha in cultured human keratinocytes. J. Investig. Dermatol. 1996, 106, 715–720. [Google Scholar] [CrossRef][Green Version]
- Calabrese, M.L.; d’Ambrosio, G.; Massa, R.; Petraglia, G. A high-efficiency waveguide applicator for in vitro exposure of mammalian cells at 1.95 GHz. IEEE Trans. Microw. Theory 2006, 54, 2256–2264. [Google Scholar] [CrossRef]
- Romeo, S.; D’Avino, C.; Pinchera, D.; Zeni, O.; Scarfi, M.R.; Massa, R. A Waveguide Applicator for in Vitro Exposures to Single or Multiple ICT Frequencies. IEEE Trans. Microw. Theory 2013, 61, 1994–2004. [Google Scholar] [CrossRef]
- Mbonjo, H.N.M.; Streckert, J.; Hansen, A.B.V.; Glasmachers, A.; Gencol, S.; Rozic, D. Generic UMTS test signal for RF bioelectromagnetic studies. Bioelectromagnetics 2004, 25, 415–425. [Google Scholar] [CrossRef]
- Gruber, J.V.; Holtz, R.; In Yang, S. In vitro examination of an oleosome-based sun protection product on the influence of UVB-induced inflammation markers in human epidermal skin equivalent tissue model. J. Photochem. Photobiol. B Biol. 2018, 179, 39–45. [Google Scholar] [CrossRef] [PubMed]
- Meloni, M.; Farina, A.; de Servi, B. Molecular modifications of dermal and epidermal biomarkers following UVA exposures on reconstructed full-thickness human skin. Photochem. Photobiol. Sci. 2010, 9, 439–447. [Google Scholar] [CrossRef] [PubMed]
- Lantow, M.; Schuderer, J.; Hartwig, C.; Simko, M. Free radical release and HSP70 expression in two human immune-relevant cell lines after exposure to 1800 MHz radiofrequency radiation. Radiat. Res. 2006, 165, 88–94. [Google Scholar] [CrossRef]
- Yamada, K.I.; Murugesan, R.; Devasahayam, N.; Cook, J.A.; Mitchell, J.B.; Subramanian, S.; Krishna, M.C. Evaluation and comparison of pulsed and continuous wave Radiofrequency electron paramagnetic resonance techniques for in vivo detection and imaging of free radicals. J. Magn. Reson. 2002, 154, 287–297. [Google Scholar] [CrossRef] [PubMed]
- Bouji, M.; Lecomte, A.; Gamez, C.; Blazy, K.; Villegier, A.S. Impact of Cerebral Radiofrequency Exposures on Oxidative Stress and Corticosterone in a Rat Model of Alzheimer’s Disease. J. Alzheimers Dis. 2020, 73, 467–476. [Google Scholar] [CrossRef] [PubMed]
- Tsoy, A.; Saliev, T.; Abzhanova, E.; Turgambayeva, A.; Kaiyrlykyzy, A.; Akishev, M.; Saparbayev, S.; Umbayev, B.; Askarova, S. The Effects of Mobile Phone Radiofrequency Electromagnetic Fields on beta-Amyloid-Induced Oxidative Stress in Human and Rat Primary Astrocytes. Neuroscience 2019, 408, 46–57. [Google Scholar] [CrossRef]
- Alkis, M.E.; Bilgin, H.M.; Akpolat, V.; Dasdag, S.; Yegin, K.; Yavas, M.C.; Akdag, M.Z. Effect of 900-, 1800-, and 2100-MHz radiofrequency radiation on DNA and oxidative stress in brain. Electromagn. Biol. Med. 2019, 38, 32–47. [Google Scholar] [CrossRef]
- Pandey, N.; Giri, S. Melatonin attenuates radiofrequency radiation (900 MHz)-induced oxidative stress, DNA damage and cell cycle arrest in germ cells of male Swiss albino mice. Toxicol. Ind. Health 2018, 34, 315–327. [Google Scholar] [CrossRef]
- Diem, E.; Schwarz, C.; Adlkofer, F.; Jahn, O.; Rudiger, H. Non-thermal DNA breakage by mobile-phone radiation (1800 MHz) in human fibroblasts and in transformed GFSH-R17 rat granulosa cells in vitro. Mutat. Res. 2005, 583, 178–183. [Google Scholar] [CrossRef] [PubMed]
- Franzellitti, S.; Valbonesi, P.; Ciancaglini, N.; Biondi, C.; Contin, A.; Bersani, F.; Fabbri, E. Transient DNA damage induced by high-frequency electromagnetic fields (GSM 1.8 GHz) in the human trophoblast HTR-8/SVneo cell line evaluated with the alkaline comet assay. Mutat. Res. 2010, 683, 35–42. [Google Scholar] [CrossRef] [PubMed]
- Smith-Roe, S.L.; Wyde, M.E.; Stout, M.D.; Winters, J.W.; Hobbs, C.A.; Shepard, K.G.; Green, A.S.; Kissling, G.E.; Shockley, K.R.; Tice, R.R.; et al. Evaluation of the genotoxicity of cell phone radiofrequency radiation in male and female rats and mice following subchronic exposure. Environ. Mol. Mutagenesis 2020, 61, 276–290. [Google Scholar] [CrossRef]
- Jasti, A.C.; Wetzel, B.J.; Aviles, H.; Vesper, D.N.; Nindl, G.; Johnson, M.T. Effect of a wound healing electromagnetic field on inflammatory cytokine gene expression in rats. Biomed. Sci. Instrum. 2001, 37, 209–214. [Google Scholar] [PubMed]
- Jensen, L.E. Targeting the IL-1 family members in skin inflammation. Curr. Opin. Investig. Drugs 2010, 11, 1211–1220. [Google Scholar]
- Cao, Y.; Tong, J. Adaptive Response in Animals Exposed to Non-Ionizing Radiofrequency Fields: Some Underlying Mechanisms. Int. J. Environ. Res. Pub. Health 2014, 11, 4441–4448. [Google Scholar] [CrossRef]
- Sannino, A.; Zeni, O.; Romeo, S.; Massa, R.; Gialanella, G.; Grossi, G.; Manti, L.; Vijayalaxmi; Scarfi, M.R. Adaptive response in human blood lymphocytes exposed to non-ionizing radiofrequency fields: Resistance to ionizing radiation-induced damage. J. Radiat. Res. 2014, 55, 210–217. [Google Scholar] [CrossRef]
- Sannino, A.; Sarti, M.; Reddy, S.B.; Prihoda, T.J.; Vijayalaxmi; Scarfi, M.R. Induction of Adaptive Response in Human Blood Lymphocytes Exposed to Radiofrequency Radiation. Radiat. Res. 2009, 171, 735–742. [Google Scholar] [CrossRef]
- Sannino, A.; Zeni, O.; Sarti, M.; Romeo, S.; Reddy, S.B.; Belisario, M.A.; Prihoda, T.J.; Vijayalaxmi; Scarfi, M.R. Induction of adaptive response in human blood lymphocytes exposed to 900 MHz radiofrequency fields: Influence of cell cycle. Int. J. Radiat. Biol. 2011, 87, 993–999. [Google Scholar] [CrossRef]
- Andrianome, S.; Gobert, J.; Hugueville, L.; Stephan-Blanchard, E.; Telliez, F.; Selmaoui, B. An assessment of the autonomic nervous system in the electrohypersensitive population: A heart rate variability and skin conductance study. J. Appl. Physiol. 2017, 123, 1055–1062. [Google Scholar] [CrossRef]
- Andrianome, S.; Hugueville, L.; de Seze, R.; Selmaoui, B. Increasing levels of saliva alpha amylase in electrohypersensitive (EHS) patients. Int. J. Radiat. Biol. 2017, 93, 841–848. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Selmaoui, B.; Andrianome, S.; Ghosn, R.; de Seze, R. Effect of acute exposure to radiofrequency electromagnetic fields emitted by a mobile phone (GSM 900 MHz) on electrodermal responsiveness in healthy human. Int. J. Radiat. Biol. 2018, 94, 890–895. [Google Scholar] [CrossRef] [PubMed]
- Rodier, F.; Coppe, J.P.; Patil, C.K.; Hoeijmakers, W.A.M.; Munoz, D.P.; Raza, S.R.; Freund, A.; Campeau, E.; Davalos, A.R.; Campisi, J. Persistent DNA damage signalling triggers senescence-associated inflammatory cytokine secretion (vol 11, pg 973, 2009). Nat. Cell Biol. 2009, 11, 973–979. [Google Scholar] [CrossRef]
- Sennott, H.; Makwana, A.; Kubilus, J.; Klausner, M. Presence of Hydrocortisone Dramatically Affects Cytokine Production Following Uv Irradiation in 3-Dimensional Skin Model Epiderm. J. Investig. Dermatol. 1997, 4, 665. [Google Scholar]
- Weindl, G.; Castello, F.; Schafer-Korting, M. Evaluation of Anti-inflammatory and Atrophogenic Effects of Glucocorticoids on Reconstructed Human Skin. Atla-Altern. Lab. Anim. 2011, 39, 173–187. [Google Scholar] [CrossRef]


| Protocol#1 | ||
| Treatment | % Viability | |
| Mean ± SD | p-Values 1 | |
| SH | 100 ± 2.7 | |
| RF | 99.15 ± 3.17 | 0.996 |
| 2 SED UV + RF | 91.95 ± 3.89 | 0.245 |
| 2 SED UV | 89.54 ± 8.16 | 0.105 |
| Protocol#2 | ||
| Treatment | % Viability | |
| Mean ± SD | p-Values 1 | |
| SH | 100 ± 9.21 | |
| RF + 4 SED UV | 83.34 ± 9.35 | 0.052 |
| 4 SED UV | 79.23 ± 6.39 | 0.019 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Szilágyi, Z.; Németh, Z.; Bakos, J.; Necz, P.P.; Sáfár, A.; Kubinyi, G.; Selmaoui, B.; Thuróczy, G. Evaluation of Inflammation by Cytokine Production Following Combined Exposure to Ultraviolet and Radiofrequency Radiation of Mobile Phones on 3D Reconstructed Human Skin In Vitro. Int. J. Environ. Res. Public Health 2020, 17, 4401. https://doi.org/10.3390/ijerph17124401
Szilágyi Z, Németh Z, Bakos J, Necz PP, Sáfár A, Kubinyi G, Selmaoui B, Thuróczy G. Evaluation of Inflammation by Cytokine Production Following Combined Exposure to Ultraviolet and Radiofrequency Radiation of Mobile Phones on 3D Reconstructed Human Skin In Vitro. International Journal of Environmental Research and Public Health. 2020; 17(12):4401. https://doi.org/10.3390/ijerph17124401
Chicago/Turabian StyleSzilágyi, Zsófia, Zsuzsanna Németh, József Bakos, Péter Pál Necz, Anna Sáfár, Györgyi Kubinyi, Brahim Selmaoui, and György Thuróczy. 2020. "Evaluation of Inflammation by Cytokine Production Following Combined Exposure to Ultraviolet and Radiofrequency Radiation of Mobile Phones on 3D Reconstructed Human Skin In Vitro" International Journal of Environmental Research and Public Health 17, no. 12: 4401. https://doi.org/10.3390/ijerph17124401
APA StyleSzilágyi, Z., Németh, Z., Bakos, J., Necz, P. P., Sáfár, A., Kubinyi, G., Selmaoui, B., & Thuróczy, G. (2020). Evaluation of Inflammation by Cytokine Production Following Combined Exposure to Ultraviolet and Radiofrequency Radiation of Mobile Phones on 3D Reconstructed Human Skin In Vitro. International Journal of Environmental Research and Public Health, 17(12), 4401. https://doi.org/10.3390/ijerph17124401





