Environmental Surveillance of Legionellosis within an Italian University Hospital—Results of 15 Years of Analysis
Abstract
:1. Introduction
2. Materials and Methods
2.1. Hospital Structure
2.2. Sampling
2.3. Isolation and Serological Identification of Legionella Spp.
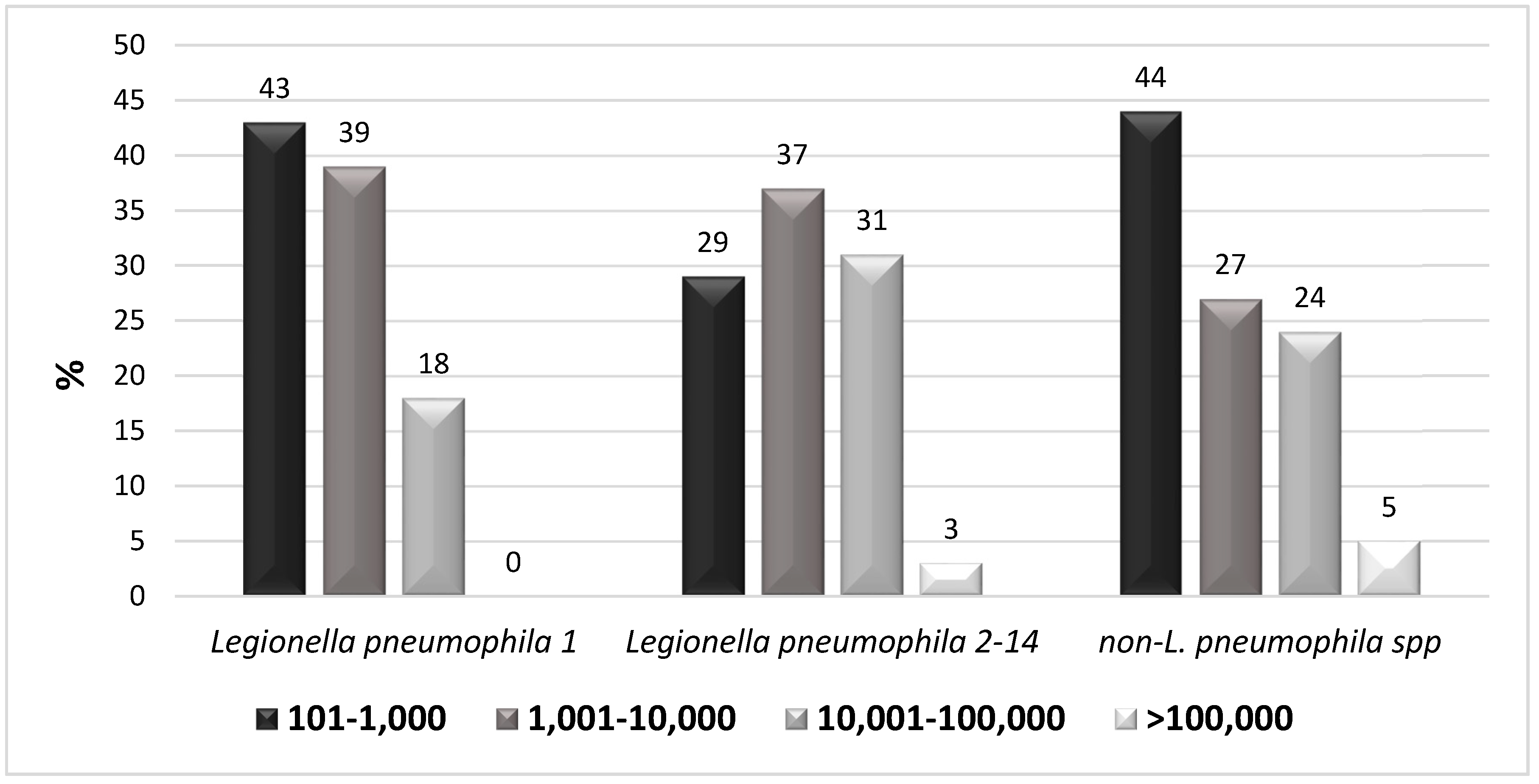
- 1 = 101–1000 CFU/L;
- 2 = 1001–10,000 CFU/L;
- 3 = 10,001–100,000 CFU/L;
- 4 > 100,000 CFU/L.
3. Results
4. Discussion
5. Conclusions
6. Limits of the Study
Author Contributions
Funding
Conflicts of Interest
References
- Edelstein, P.H.; Cianciotto, N.P. Legionella. In Mandell, Douglas, and Bennett’s Principles and Practice of Infectious Diseases, 6th ed.; Mandell, G.L., Bennet, J.E., Dolin, R., Eds.; Elsevier: Philadelphia, PA, USA, 2005; pp. 2711–2724. [Google Scholar]
- Winn, W.C. Legionella. In Bergey’s Manual of Systematic Bacteriology, 2th ed.; Brenner, D.J., Krieg, N.R., Staley, J.T., Eds.; Springer: New York, NY, USA, 2005; Volume 2, Part B, pp. 212–236. [Google Scholar]
- Linee Guida per la Prevenzione e il Controllo della Legionellosi. 2015. Available online: http://www.salute.gov.it/imgs/C_17_pubblicazioni_2362_allegato.pdf (accessed on 12 December 2018).
- Pierre, D.M.; Baron, J.; Yu, V.L.; Stout, J.E. Diagnostic testing for Legionnaires’ disease. Ann. Clin. Microbiol. Antimicrob. 2017, 16, 59. [Google Scholar] [CrossRef]
- Ditommaso, S.; Giacomuzzi, M.; Rivera, S.R.; Raso, R.; Ferrero, P.; Zotti, C.M. Virulence of Legionella pneumophila strains isolated from hospital water system and healthcare-associated Legionnaires’ disease in Northern Italy between 2004 and 2009. BMC Infect. Dis. 2014, 14, 483. [Google Scholar] [CrossRef] [PubMed]
- Ministero della Salute. Decreto Ministeriale 15 Dicembre 1990 “Sistema Informativo delle Malattie Infettive e Diffusive” GU 8/01/1991, n. 6. Available online: http://www.salute.gov.it/imgs/C_17_ normativa_1357_allegato.pdf (accessed on 15 December 2018).
- European Centre for Disease Control and Prevention (ECDC). Legionnaires’ Disease Surveillance in Europe, 2014. Stockholm: ECDC. 2016. Available online: http://ecdc.europa.eu/en/publications-data/legionnaires-disease-europe-2014 (accessed on 15 December 2018).
- Annual Reports of Legionellosis. Istituto Superiore di Sanità. Available online: www.iss.it (accessed on 9 December 2018).
- Pignato, S.; Coniglio, M.A.; Faro, G.; Cantaro, P.; Carini, S.A.; Mangano, G.; Cunsolo, R.; Coco, G.; Giammanco, G. Legionella contamination in the hospital environment: Monitoring of the hot water distribution systems of three hospitals in Catania (Italy). Ig. Sanità Pubbl. 2006, 62, 635–652. [Google Scholar]
- Sikora, A.; Wójtowicz-Bobin, M.; Kozioł-Montewka, M.; Magryś, A.; Gładysz, I. Prevalence of Legionella pneumophila in water distribution systems in hospitals and public buildings of the Lublin region of eastern Poland. Ann. Agric. Environ. Med. 2015, 22, 195–201. [Google Scholar] [CrossRef]
- Delia, S.; Laganà, P.; Minutoli, E. Occurrence of legionella in beach shower facilities. J. Prev. Med. Hyg. 2007, 48, 114–117. [Google Scholar] [PubMed]
- Delia, S.; Laganà, P.; Minutoli, E.; Cannavò, G.; Parisi, S. Prevention of legionellosis in hotel establishments: A proposal to introduce a plan of action in accordance with Provision 13 January 2005 (Italy). Ig. Sanità Pubbl. 2008, 64, 489–511. [Google Scholar]
- Laganà, P.; Gambuzza, M.E.; Delia, S. Prevalence and distribution of Legionella pneumophila in cruise ships and ferries. Ann. Agric. Environ. Med. 2017, 24, 276–282. [Google Scholar] [CrossRef] [PubMed]
- Iatta, R.; Cuna, T.; Napoli, C.; de Giglio, O.; Montagna, M.T. Environmental surveillance and molecular investigation of Legionella spp. in Apulia, in the years 2008–2011. Ann. Ig. 2013, 25, 435–441. [Google Scholar] [PubMed]
- Laganà, P.; Soraci, L.; Gambuzza, M.E.; Delia, S. Innate immune surveillance in the central nervous system in Legionella pneumophila infection. CNS Neurol Disord. Drug Targets 2017, 16, 1080–1089. [Google Scholar] [CrossRef] [PubMed]
- Laganà, P.; Caruso, G.; Piccione, D.; Pino, R.; Gioffrè, M.E.; Delia, S. Legionella spp., amoebae and not-fermenting Gram negative bacteria in an Italian university hospital water system. Ann. Agric. Environ. Med. 2014, 21, 489–493. [Google Scholar] [CrossRef]
- O’Neill, E.; Humphreysa, H. Surveillance of hospital water and primary prevention of nosocomial legionellosis: What is the evidence? J. Hosp. Infect. 2005, 59, 273–279. [Google Scholar] [CrossRef]
- Montagna, M.T.; Napoli, C.; Tatò, D.; Spilotros, G.; Barbuti, G.; Barbuti, S. Clinical-environmental surveillance of legionellosis: An experience in Southern Italy. Eur. J. Epidemiol. 2006, 21, 325–331. [Google Scholar] [CrossRef]
- Fields, B.S. Legionella in the environment. In Legionella pneumophila. Pathogenesis and Immunity; Hoffman, P., Friedman, H., Bendinelli, M., Eds.; Springer: New York, NY, USA, 2007; pp. 85–94. [Google Scholar]
- Marchesi, I.; Marchegiano, P.; Bargellini, A.; Cencetti, S.; Frezza, G.; Miselli, M.; Borella, P. Effectiveness of different methods to control Legionella in the water supply: Ten-year experience in an Italian university hospital. J. Hosp. Infect. 2011, 77, 47–51. [Google Scholar] [CrossRef] [PubMed]
- Bédard, E.; Fey, S.; Charron, D.; Lalancette, C.; Cantin, P.; Dolcé, P.; Laferrière, C.; Déziel, E.; Prévost, M. Temperature diagnostic to identify high risk areas and optimize Legionella pneumophila surveillance in hot water distribution systems. Water Res. 2015, 71, 244–256. [Google Scholar]
- Guyot, S.; Goy, J.J.; Gersbach, P.; Jaton, K.; Blanc, D.S.; Zanetti, G. Legionella pneumophila aortitis in a heart transplant recipient. Transpl. Infect. Dis. 2007, 9, 58–59. [Google Scholar] [CrossRef] [PubMed]
- Cunha, B.A.; Burillo, A.; Bouza, E. Legionnaires’ disease. Lancet 2016, 23, 376–385. [Google Scholar] [CrossRef]
- Nazemi, S.; Mirzaii, M.; Yaslianifard, S.; Darban-Sarokhalil, D.; Khoramrooz, S.S.; Norozi, P.; Davardoost, F. Microbiological qualification of air, water and dialysate in a haemodialysis centre: A new focus on Legionella spp. Iran J. Microbiol. 2016, 8, 219–225. [Google Scholar] [PubMed]
- Francois Watkins, L.K.; Toews, K.E.; Harris, A.M.; Davidson, S.; Ayers-Millsap, S.; Lucas, C.E.; Hubbard, B.C.; Kozak-Muiznieks, N.A.; Khan, E.; Kutty, P.K. Lessons from an outbreak of legionnaires’ disease on a hematology-oncology unit. Infect. Control. Hosp. Epidemiol. 2017, 38, 306–313. [Google Scholar] [CrossRef]
- Lanternier, F.; Ader, F.; Pilmis, B.; Catherinot, E.; Jarraud, S.; Lortholary, O. Legionnaire’s disease in compromised hosts. Infect Dis. Clin. N. Am. 2017, 31, 123–135. [Google Scholar] [CrossRef]
- Laganà, P.; Avventuroso, E.; Casale, M.; Delia, S.; Dattilo, G. Risk Assessment of legionellosis in cardiology units. J. Prev. Med. Hyg. 2017, 58, E173–E176. [Google Scholar]
- Troiano, G.; Messina, G.; Zanieri, E.; Li Donni, V.; Nante, N.; Magisti, L.; Pulci, M.B.; Niccolini, F. Qualità microbiologica delle acque per emodialisi: Quali i fattori di rischio? G. Ital. Nefrol. 2018, 5, 144–150. [Google Scholar]
- Conferenza Permanente per i Rapporti Tra Lo Stato, le Regioni e le Province Autonome di Trento e Bolzano. Linee Guida per la Prevenzione e il Controllo della Legionellosi. Gazzetta Ufficiale, 2000; pp. 1–35. Available online: http://www.gazzettaufficiale.it/eli/gu/2000/05/05/103/sg/pdf (accessed on 9 December 2018).
- Leoni, E.; de Luca, G.; Legnani, P.P.; Sacchetti, R.; Stampi, S.; Zanetti, F. Legionella waterline colonization: Detection of Legionella species in domestic, hotel and hospital systems. J. Appl. Microbiol. 2005, 98, 373–379. [Google Scholar] [CrossRef]
- Perola, O.; Kauppinen, J.; Kusnetsov, J.; Karkkainen, U.M.; Luck, P.C.; Katila, M.L. Persistent Legionella pneumophila colonization of a hospital water supply: Efficacy of control methods and amolecular epidemiological analysis. APMIS 2005, 113, 45–53. [Google Scholar] [CrossRef]
- Triassi, M.; Di Popolo, A.; Ribera D’Alcala, G.; Albanese, Z.; Cuccurullo, S.; Montegrosso, S.; Crispino, M.; Borella, P.; Zerrilli, R. Clinical and environmental distribution of Legionella pneumophila in a university hospital in Italy: Efficacy of ultraviolet disinfection. J. Hosp. Infect. 2006, 62, 494–501. [Google Scholar] [CrossRef]
- Darelid, J.; Lofgren, S.; Malmval, B.E. Control of nosocomial Legionnaires’ disease by keeping the circulating hot water temperature above 55 degrees C: Experience from a 10-year surveillance programme in a district general hospital. J. Hosp. Infect. 2002, 50, 213–219. [Google Scholar] [CrossRef] [PubMed]
- Hosein, I.K.; Hill, D.W.; Tan, T.Y.; Butchart, E.G.; Wilson, K.; Finlay, G.; Burge, S.; Ribeiro, C.D. Point of care controls for nosocomial legionellosis combined with chlorine dioxide potable water decontamination: A two-year survey at a Welsh teaching hospital. J. Hosp. Infect. 2005, 61, 100–106. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization (WHO). Legionella and the Prevention of Legionellosis. 2007. Available online: http://www.who.int/water_sanitation_health/emerging/legionella.pdf (accessed on 12 December 2018).
- Laganà, P.; Moscato, U.; Poscia, A.; La Milia, D.I.; Boccia, S.; Avventuroso, E.; Delia, S. Geostatistics—A Tool Applied to the Distribution of Legionella pneumophila in a Hospital Water System. Ann. Agric. Environ. Med. 2015, 22, 655–660. [Google Scholar] [CrossRef]
- Montagna, M.T.; de Giglio, O.; Napoli, C.; Cannova, L.; Cristina, M.L.; Deriu, M.G.; Delia, S.A.; Giuliano, A.; Guida, M.; Laganà, P.; et al. Legionella spp. contamination in indoor air: Preliminary results of an Italian multicenter study. Epidemiol. Prev. 2014, 38, 62–65. [Google Scholar] [PubMed]
- Montagna, M.T.; Cristina, M.L.; de Giglio, O.; Spagnolo, A.M.; Napoli, C.; Cannova, L.; Deriu, M.G.; Delia, S.; Giuliano, A.; Guida, M.; et al. Serological and molecular identification of Legionella spp. in water and surrounding air samples in Italian healthcare facilities. Environ. Res. 2016, 146, 47–50. [Google Scholar] [CrossRef] [PubMed]
- Montagna, M.T.; De Giglio, O.; Cristina, M.L.; Napoli, C.; Pacifico, C.; Agodi, A.; Baldovin, T.; Casini, B.; Coniglio, M.A.; D’Errico, M.M.; et al. Evaluation of Legionella air contamination in healthcare facilities by different sampling methods: An Italian multicenter study. Int. J. Environ. Res. Public Health 2017, 14, 670. [Google Scholar] [CrossRef]
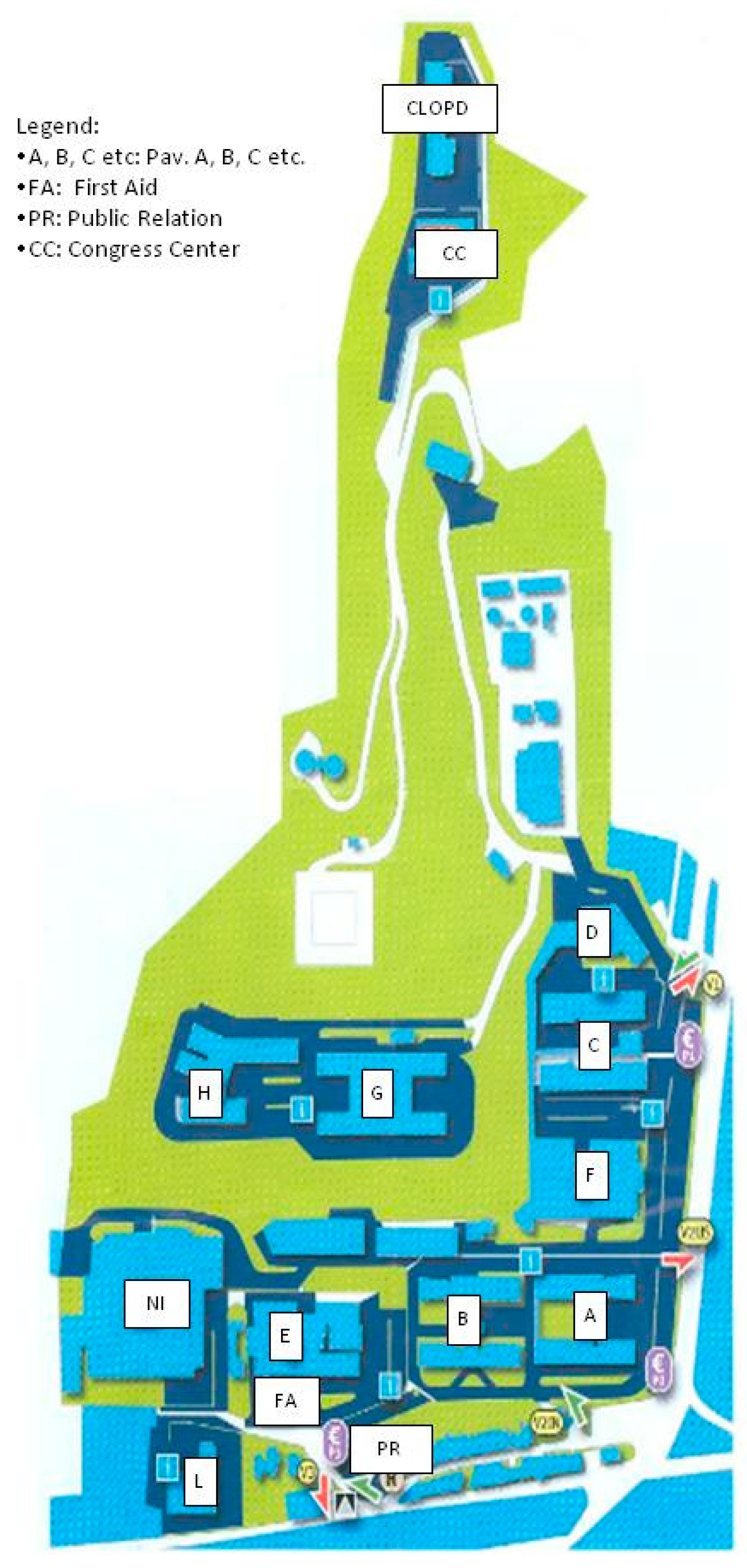
| Building | Wards | Total | Negative | Positive | Positive for LP 1 | Positive for LP 2–14 | Positive for Non-LP spp. |
|---|---|---|---|---|---|---|---|
| A | Obstetrics Gynecology | 87 (6%) | 25 (29%) | 62 (71%) | 4 (6%) | 44 (71%) | 17 (27%) |
| B | Internal Medicine | 67 (5%) | 29 (43%) | 38 (57%) | 0 | 21 (55%) | 20 (53%) |
| C | Cardiology-Nephrology | 95 (7%) | 68 (72%) | 27 (28%) | 0 | 26 (96%) | 1 (4%) |
| D | Pathological Anatomy | 76 (6%) | 37 (49%) | 39 (51%) | 2 (5%) | 37 (95%) | 4 (10%) |
| E | ICU Neurosurgery-Orthopedics | 280 (21%) | 64 (23%) | 216 (77%) | 112 (52%) | 101 (47%) | 28 (25%) |
| F | General Surgeries | 163 (12%) | 69 (42%) | 94 (58%) | 2 (2%) | 88 (94%) | 5 (5%) |
| G | Laboratories | 136 (10%) | 52 (38%) | 84 (62%) | 26 (31%) | 58 (69%) | 2 (2%) |
| H | Pulmonology, Infectious Dis., Thoracic Surg., Oncology | 173 (13%) | 41 (24%) | 132 (76%) | 0 | 118 (89%) | 14 (11%) |
| NI | Pediatrics | 160 (12%) | 60 (38%) | 100 (62%) | 1 (1%) | 93 (93%) | 10 (10%) |
| W | Clinics | 13 (1%) | 11 (85%) | 2 (15%) | 0 | 1 (50%) | 1 (50%) |
| CLOPD | Dentistry | 96 (7%) | 78 (81%) | 18 (19%) | 0 | 1 (5%) | 17 (95%) |
| Total (%) | 1346 | 534 (40%) | 812 (60%) | 147 (18%) | 588 (72%) | 119 (15%) |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Laganà, P.; Facciolà, A.; Palermo, R.; Delia, S. Environmental Surveillance of Legionellosis within an Italian University Hospital—Results of 15 Years of Analysis. Int. J. Environ. Res. Public Health 2019, 16, 1103. https://doi.org/10.3390/ijerph16071103
Laganà P, Facciolà A, Palermo R, Delia S. Environmental Surveillance of Legionellosis within an Italian University Hospital—Results of 15 Years of Analysis. International Journal of Environmental Research and Public Health. 2019; 16(7):1103. https://doi.org/10.3390/ijerph16071103
Chicago/Turabian StyleLaganà, Pasqualina, Alessio Facciolà, Roberta Palermo, and Santi Delia. 2019. "Environmental Surveillance of Legionellosis within an Italian University Hospital—Results of 15 Years of Analysis" International Journal of Environmental Research and Public Health 16, no. 7: 1103. https://doi.org/10.3390/ijerph16071103
APA StyleLaganà, P., Facciolà, A., Palermo, R., & Delia, S. (2019). Environmental Surveillance of Legionellosis within an Italian University Hospital—Results of 15 Years of Analysis. International Journal of Environmental Research and Public Health, 16(7), 1103. https://doi.org/10.3390/ijerph16071103







