A One-Year Prospective Follow-Up Study on the Health Profile of Hikikomori Living in Hong Kong
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design and Setting
2.2. Procedures of the Follow-Up Interviews
2.3. The Instrument and Anthropometric Measurements
2.4. Statistical Analysis
3. Results
3.1. The Follow-Up Cohort
3.2. Improvements in the Health Profile and Lifestyle Practice
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Yuen, J.W.M.; Yan, Y.K.Y.; Wong, V.C.W.; Tan, W.W.S.; So, K.; Chien, W.T. A physical health profile of youths living with a “Hikikomori” lifestyle. Int. J. Enivron. Res. Public Health 2018, 15, 315. [Google Scholar] [CrossRef] [PubMed]
- Wong, V.C.W. Youth locked in time and space? Defining features of social withdrawal and practice implications. J. Soc. Work Pract. 2009, 23, 337–352. [Google Scholar] [CrossRef]
- Wong, V.; Ying, W. Social Withdrawal of Young People in Hong Kong: A Social Exclusion Perspective. Hong Kong J. Soc. Work 2006, 40, 61–91. [Google Scholar] [CrossRef]
- Wong, P.W.C.; Li, T.M.H.; Chan, M.; Law, Y.W.; Chau, M.; Cheng, C.; Fu, K.W.; Bacon-Shone, J.; Yip, P.S.F. The prevalence and correlates of severe social withdrawal (hikikomori) in Hong Kong: A cross-sectiona telephone-based survey study. Int. J. Soc. Psychiatry 2015, 61, 330–342. [Google Scholar] [CrossRef] [PubMed]
- Tajan, N.; Yukiko, H.; Pionnié-Dax, N. Hikikomori: The Japanese Cabinet Office’s 2016 survey of acute social withdrawal. Asia-Pac. J. 2017, 15, 1–11. [Google Scholar]
- Guedj-Bourdiau, M.J. Home confinement of the adolescent. Hikikomori. Annal. Med. Psychiatry 2011, 169, 668–672. [Google Scholar]
- Takasu, N.N.; Toichi, M.; Nakamura, W. Importance of regular lifestyle with daytime bright light exposure on circadian rhythm sleep-wake disorders in pervasive development disorders. Jap. Dental Sci. Rev. 2011, 47, 141–149. [Google Scholar] [CrossRef]
- Yong, R. Exploring Hikikomori—A Mixed Methods Qualitative Approach. Int. J. Behav. Med. 2010, 17, 81–82. [Google Scholar]
- Watts, J. Tokyo—Public health experts concerned about “hikikomori”. Lancet 2002, 359, 1131. [Google Scholar] [CrossRef]
- Kondo, N.; Sakai, M.; Kuroda, Y.; Kiyota, Y.; Kitabata, Y.; Kurosawa, M. General condition of hikikomori (prolonged social withdrawal) in Japan: Psychiatric diagnosis and outcome in mental health welfare centres. Int. J. Soc. Psychiatry 2013, 59, 79–86. [Google Scholar] [CrossRef]
- Nagata, T.; Yamada, H.; Teo, A.R.; Yoshimura, C.; Nakajima, T.; van Vliet, I. Comorbid social withdrawal (hikikomori) in outpatients with social anxiety disorder: Clinical characteristics and treatment response in a case series. Int. J. Soc. Psychiatry 2013, 59, 73–78. [Google Scholar] [CrossRef] [PubMed]
- Zielenziger, M. Shutting Out the Sun: How Japan Created Its Own Lost Generation, 1st ed.; Talese, N.A., Ed.; Vintage: New York, NY, USA, 2006. [Google Scholar]
- Goodman, R.; Imoto, Y.; Toivonen, T. A Sociology of Japanese Youth: From Returnees to NEETs; Routledge: New York, NY, USA; Abingdon, UK, 2012. [Google Scholar]
- Norasakkunkit, V.; Uchida, Y.; Toivonen, T. Caught between culture, society, and globalization: Youth marginalization in post-industrial Japan. Soc. Personal. Psychol. Compass 2012, 6, 361–378. [Google Scholar] [CrossRef]
- Furuhashi, Y. Comparison between Teen-Onset Hikikomori and Adult-Onset Hikikomori in Japan. Eur. Psychiatry 2012, 27, 1. [Google Scholar] [CrossRef]
- Sakamoto, N.; Martin, R.G.; Kumano, H.; Kuboki, T.; Al-Adawi, S. Hikikomori, is it a culture-reactive or culture-bound syndrome? Nidotherapy and a clinical vignette from Oman. Int. J. Psychiatry Med. 2005, 35, 191–198. [Google Scholar] [CrossRef] [PubMed]
- Koyama, A.; Miyake, Y.; Kawakami, N.; Tsuchiya, M.; Tachimori, H.; Takeshima, T. Lifetime prevalence, psychiatric comorbidity and demographic correlates of “hikikomori” in a community population in Japan. Psychiatry Res. 2010, 176, 69–74. [Google Scholar] [CrossRef] [PubMed]
- Lee, Y.S.; Lee, J.Y.; Choi, T.Y.; Choi, J.T. Home visitation program for detecting, evaluating and treating socially withdrawn youth in Korea. Psych. Clin. Neurosci. 2013, 67, 193–202. [Google Scholar] [CrossRef] [PubMed]
- Furuhashi, T.; Tsuda, H.; Ogawa, T.; Suzuki, K.; Shimizu, M.; Teruyama, J.; Horiguchi, S.; Shimizu, K.; Sedooka, A.; Figueiredo, C.; et al. Current situation, commonalities and differences between socially withdrawn young adults (Hikikomori) in France and Japan. Evol. Psychiatr. 2013, 78, 249–266. [Google Scholar] [CrossRef]
- Kato, T.A.; Tateno, M.; Shinfuku, N.; Fujisawa, D.; Teo, A.R.; Sartorius, N.; Akiyama, T.; Ishida, T.; Choi, T.Y.; Balhara, Y.P.; et al. Does the ‘hikikomori’ syndrome of social withdrawal exist outside Japan? A preliminary international investigation. Soc. Psychiatr. Psychiatr. Epidemiol. 2012, 47, 1061–1075. [Google Scholar] [CrossRef]
- Hayakawa, K.; Kato, T.A.; Watabe, M.; Teo, A.R.; Horikawa, H.; Kuwano, N.; Shimokawa, N.; Sato-Kasai, M.; Kubo, H.; Ohgidani, M.; et al. Blood biomarkers of hikikomori, a severe social withdrawal syndrome. Sci. Rep. 2018, 8, 2884. [Google Scholar] [CrossRef]
- British Heart Foundation. Health at Work Questionnaire—How Healthy is Your Diet? Available online: https://www.bhf.org.uk/informationsupport/publications/health-at-work/health-at-work-how-healthy-is-your-diet-questionnaire (accessed on 2 January 2019).
- Vogel, S.H. Japanese society under stress. Asian Surv. 2012, 52, 687–713. [Google Scholar]
- Umeda, M.; Kawakami, N. Association of childhood family environments with the risk of social withdrawal (‘hikikomori’) in the community population in Japan. Psychiatry Clin. Neurosci. 2012, 66, 121–129. [Google Scholar] [CrossRef] [PubMed]
- Ohashi, N. Exploring the Psychic Roots of Hikikomori in Japan; Proquest, Umi Dissertation Publishing: Ann Arbor, MI, USA, 2011. [Google Scholar]
- Chan, H.Y.; Lo, T.W. Quality of life of the hidden youth in Hong Kong. Appl. Res. Qual. Life 2014, 9, 951–969. [Google Scholar] [CrossRef]
- Teychenne, M.; Ball, K.; Salmon, J. Sedentary Behavior and Depression among adults: A Review. Int. J. Behav. Med. 2010, 17, 246–254. [Google Scholar] [CrossRef] [PubMed]
- Centre for Health Protection. Hypertension. Available online: http://www.chp.gov.hk/en/healthtopics/content/25/35390.html (accessed on 2 January 2019).
- Family Council. Family Project Cohort Study. Available online: https://www.family.org.hk/wp-content/uploads/2015/07/KT25.pdf (accessed on 2 January 2019).
- Zhou, B.; Bentham, J.; Di Cesare, M.; Bixby, H.; Danaei, G.; Cowan, M.J.; Paciorek, C.J.; Singh, G.; Hajifathalian, K.; Bennett, J.E. Worldwide trends in blood pressure from 1975 to 2015: A pooled analysis of 1479 population-based measurement studies with 19.1 million participants. Lancet 2017, 389, 37–55. [Google Scholar] [CrossRef]
- World Health Organization. 2003 World Health Organization (WHO)/International Society of Hypertension (ISH) statement on management of hypertension. J. Hypertens. 2003, 21, 1983–1992. [Google Scholar] [CrossRef]
- Goel, M.; Pal, P.; Agrawal, A.; Ashok, C. Relationship of body mass index and other life style factors with hypertension in adolescents. Ann. Pediatr. Cardiol. 2016, 9, 29–34. [Google Scholar] [PubMed]
- Hagberg, J.M.; Park, J.; Brown, M.D. The role of exercise training in the treatment of hypertension. Sports Med. 2000, 30, 193–206. [Google Scholar] [CrossRef]
- Cooper, A.R.; Moore, L.A.R.; McKenna, J.; Riddoch, C.J. What is the magnitude of blood pressure response to a programme of moderate intensity exercise? Randomised controlled trial among sedentary adults with unmedicated hypertension. Br. J. Gen. Pract. 2000, 50, 958–962. [Google Scholar]
- Pescatello, L.S.; Franklin, B.A.; Fagard, R.; Farquhar, W.B.; Kelley, G.A.; Ray, C.A. Exercise and hypertension. Med. Sci. Sports Exerc. 2004, 36, 533–553. [Google Scholar] [CrossRef]
- Franklin, S.S.; Pio, J.R.; Wong, N.D.; Larson, M.G.; Leip, E.P.; Vasan, R.S.; Levy, D. Predictors of new-onset diastolic and systolic hypertension: The Framingham Heart Study. Circulation 2005, 111, 1121–1127. [Google Scholar] [CrossRef]
- Grebla, R.C.; Rodriguez, C.J.; Borrell, L.N.; Pickering, T.G. Prevalence and determinants of isolated systolic hypertension among young adults: The 1999–2004 US National Health and Nutrition Examination. Surv. J. Hypertens. 2010, 28, 15–23. [Google Scholar] [CrossRef] [PubMed]
- Schnall, P.L.; Pieper, C.; Schwartz, J.E. The relationship between ‘job strain’, workplace diastolic blood pressure, and left ventricular mass index. J. Am. Med. Assoc. 1990, 263, 1929–1935. [Google Scholar] [CrossRef]
- Matthews, K.A.; Cottington, E.M.; Talbott, E.; Kuller, L.H.; Siegel, J.M. Stressful work conditions and diastolic blood pressure among blue collar factory workers. Am. J. Epidemiol. 1987, 126, 280–290. [Google Scholar] [CrossRef] [PubMed]
- Payne, N.; Jones, F.; Harris, P.R. Employees’ perceptions of the impact of work on health behaviours. J. Health Psychol. 2012, 18, 887–899. [Google Scholar] [CrossRef] [PubMed]
- Payne, N.; Jones, F.; Harrism, P.R. The impact of working life on health behavior: The effect of job strain on the cognitive predictors of exercise. J. Occup. Health Psychol. 2002, 7, 342–353. [Google Scholar] [CrossRef] [PubMed]
- Virtanen, M.; Kivimäki, M.; Josensuu, M.; Virtanen, P.; Elovainio, M. Temporary employment and health: A review. Int. J. Epidemiol. 2005, 34, 610–622. [Google Scholar] [CrossRef] [PubMed]
- Carpenter, C.J. A meta-analysis of the effectiveness of health belief model variables in predicting behavior. Health Commun. 2010, 25, 661–669. [Google Scholar] [CrossRef]
- Abraham, C.; Sheeran, P. Chapter 2: The Health Belief Model. Predicting Health Behaviour: Research and Practice with Social Condition Models; Open University Press: New York, NY, USA, 2005; pp. 28–80. [Google Scholar]
- Haase, A.; Steptoe, A.; Sallis, J.F.; Wardle, J. Leisure-time physical activity in university students from 23 countries: Associations with health beliefs, risk awareness, and national economic development. Prev. Med. 2004, 39, 182–190. [Google Scholar] [CrossRef]
- Wong, V. Social withdrawal as invisible youth disengagement: Government inaction and NGO responses in Hong Kong. Int. J. Sociol Soc. Policy 2012, 32, 415–430. [Google Scholar] [CrossRef]
- Wong, V. Social work with youth in social withdrawal: In-home and beyond-home intervention modalities. Chin. J. Soc. Work 2014, 7, 161–174. [Google Scholar] [CrossRef]
- Wong, V.; Au-Yeung, T.C. Expediting youth’s entry into employment whilst overlooking precariousness: Flexi-employability and disciplinary activation in Hong Kong. Soc. Policy Admin. 2018, 1–17. [Google Scholar] [CrossRef]
- Howe, C.J.; Cole, S.R.; Lau, B.; Napravnik, S.; Eron, J.J. Selection bias due to loss to follow up in cohort studies. Epidemiology 2016, 27, 91–97. [Google Scholar] [CrossRef] [PubMed]
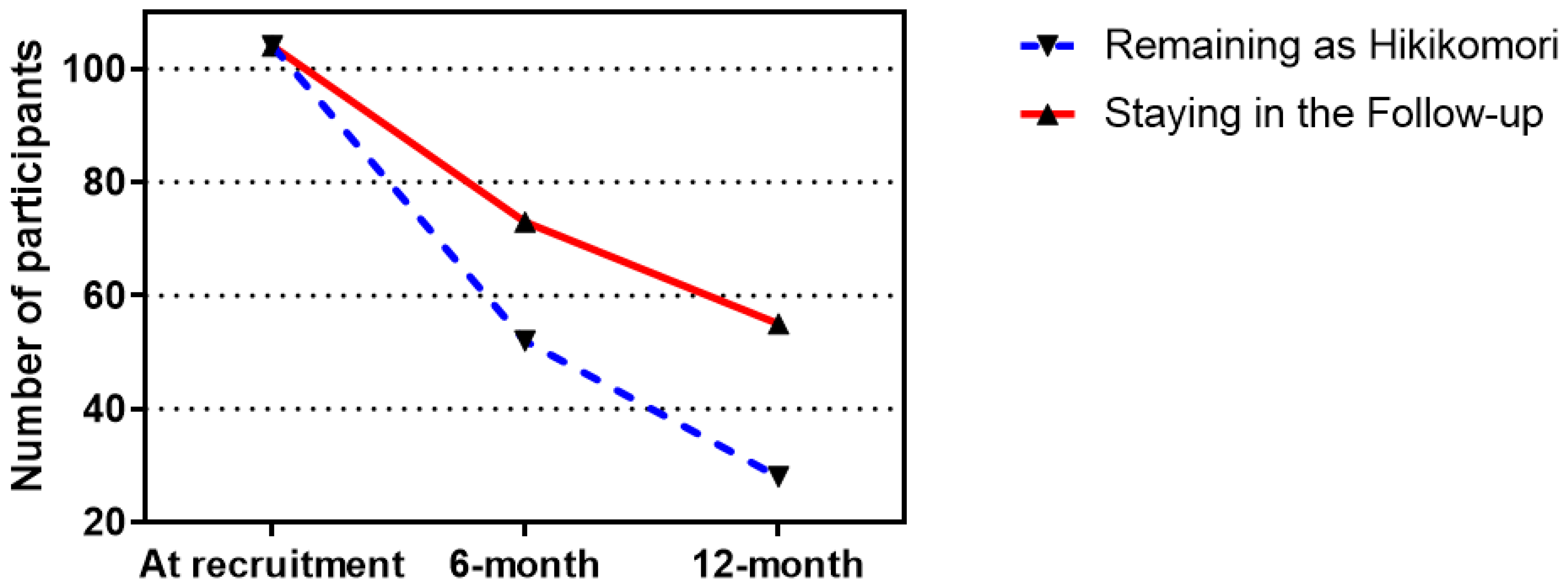
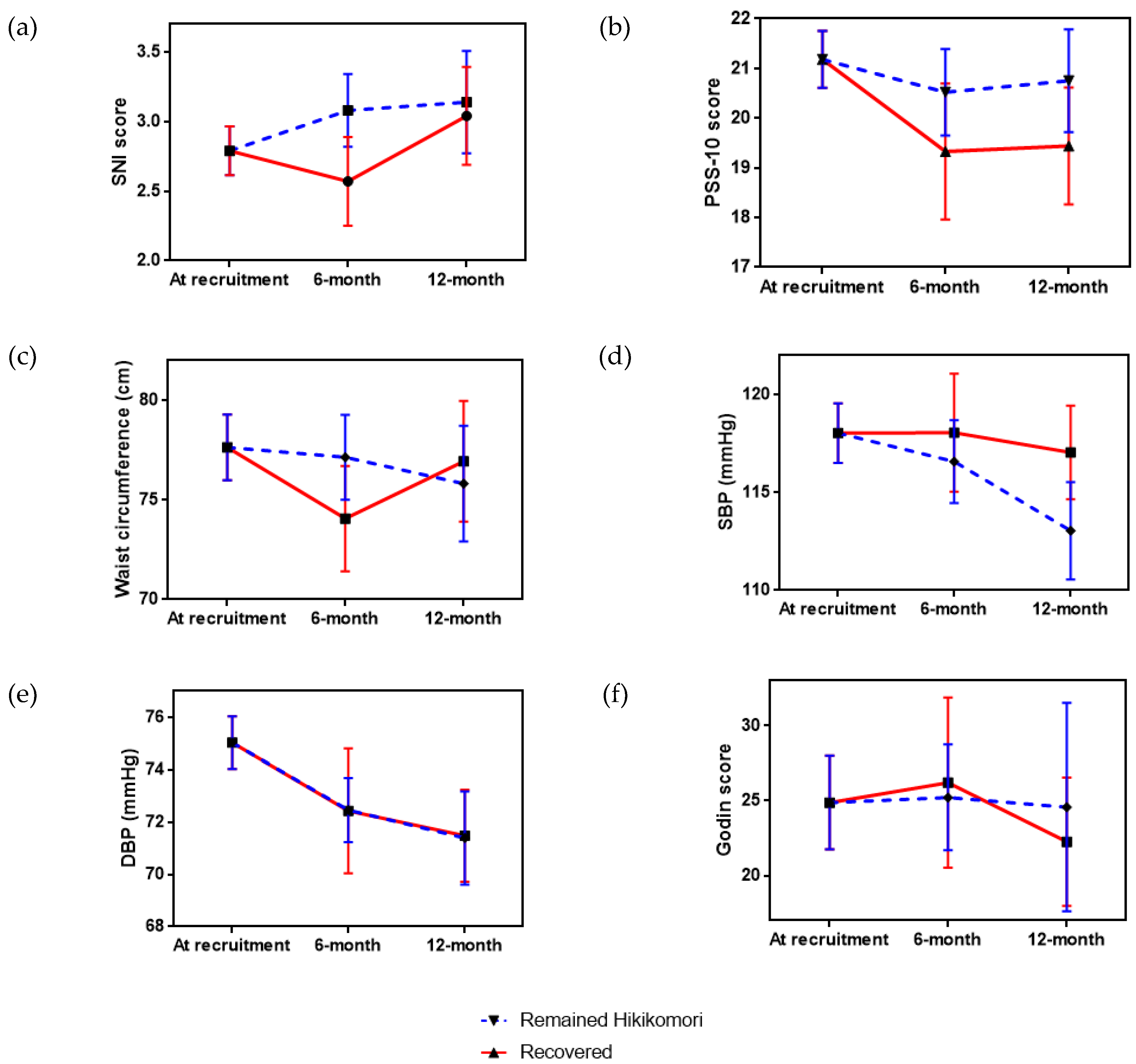
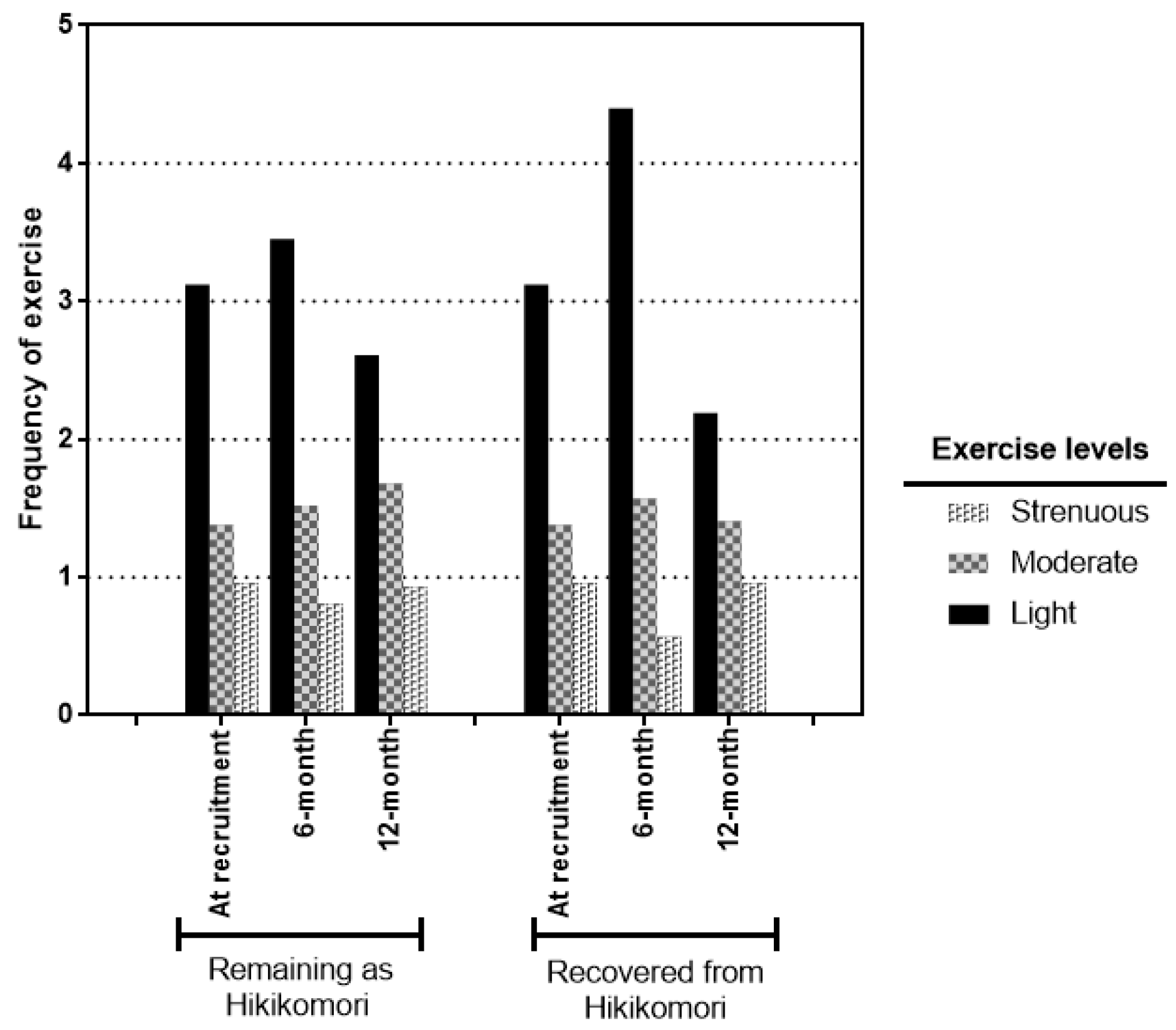
| Variables | Time Point 1 (n = 104) | Time Point 2 (n = 73) | Time Point 3 (n = 55) | X2 p-Value | |
|---|---|---|---|---|---|
| Number (Percentage) | |||||
| Gender | Male | 62 (59.6) | 42 (57.5) | 31 (56.4) | 0.916 |
| Age (years) | Mean ± SD | 19.02 ± 3.62 | 20.21 ± 3.50 | 20.84 ± 3.64 | 0.006 ∆ |
| Range | 13–31 | 13–31 | 14–32 | ||
| Age group 13–17 | 41 (39.4) | 18 (26.0) | 11 (20.0) | 0.090 | |
| Age group 18–24 | 54 (51.9) | 47 (63.0) | 37 (67.3) | ||
| Age group 25–34 | 9 (8.7) | 8 (11.0) | 7 (12.7) | ||
| Duration of being hikikomori (Months) | Mean ± SD | 16.14 ± 20.16 | 25.16 ± 22.73 | 34.96 ± 25.76 | <0.001 ∆ |
| Range | 3–120 ‡ | 7–127 | 13–132 | ||
| Living | Alone | 2 (1.9) | 3 (4.1) | 1 (1.8) | 0.874 |
| With immediate family | 100 (96.2) | 68 (93.2) | 54 (98.2) | ||
| With relative †/friends | 2 (1.9) | 2 (2.8) | 0 (0) | ||
| Residential | Self-owned/self-rented | 2 (1.9) | 2 (2.7) | 1 (1.8) | 0.773 |
| Not self-owned/Not self-rented | 102 (98.1) | 71 (97.3) | 54 (98.2) | ||
| Financial source | Self | 23 (22.1) | 25 (34.2) | 21 (38.2) | 0.297 |
| Family/relatives | 80 (76.9) | 47 (64.4) | 34 (61.8) | ||
| Smoker | Current | 13 (12.5) | 6 (8.2) | 5 (9.1) | 0.861 |
| Quitted | 10 (9.6) | 7 (9.6) | 4 (7.3) | ||
| Never | 81 (77.9) | 60 (82.2) | 46 (83.6) | ||
| Variables | Time Point 1 | Time Point 2 | Time Point 3 | RMANOVA F | (Imputed) p-Value | GEE Beta | p-Value | |
|---|---|---|---|---|---|---|---|---|
| (n = 104) | (n = 73) | (n = 55) | ||||||
| Mean ± SD | ||||||||
| Social † support | SNI score (0–7) a | 2.79 ± 1.80 | 2.93 ± 2.06 | 3.09 ± 1.87 | 12.174 | <0.001 | 0.275 | 0.009 |
| ISEL total score (0–48) b | 24.60 ± 6.30 | 24.63 ± 5.99 | 24.75 ± 6.89 | 1.074 | 0.302 | 0.269 | 0.493 | |
| Appraisal (0–12) b | 6.81 ± 2.16 | 6.90 ± 1.87 | 7.11 ± 2.18 | 2.463 | 0.096 | 0.170 | 0.267 | |
| Tangible (0–12) b | 6.20 ± 1.71 | 6.29 ± 1.53 | 6.20 ± 1.73 | 0.618 | 0.496 | −0.010 | 0.933 | |
| Belonging (0–12) b | 6.00 ± 2.45 | 5.89 ± 2.53 | 6.05 ± 2.44 | 2.343 | 0.104 | 0.136 | 0.342 | |
| Self-esteem (0–12) b | 5.59 ± 2.08 | 5.55 ± 2.14 | 5.38 ± 2.39 | 0.544 | 0.577 | −0.052 | 0.685 | |
| Psychological † | Perceived stress (0–40) c | 21.18 ± 5.87 | 20.18 ± 6.25 | 20.11 ± 5.79 | 3.437 | 0.045 | −0.709 | 0.028 |
| Depression (0–63) d | 17.17 ± 11.49 | 16.48 ± 10.87 | 15.76 ± 11.80 | 1.327 | 0.265 | −0.658 | 0.241 | |
| T-anxiety (20–80) e | 44.22 ± 12.17 | 46.48 ± 12.97 | 42.45 ± 11.16 | 2.105 | 0.131 | −0.621 | 0.291 | |
| Physical | SBP (mmHg) | 118 ± 16 | 117 ± 15 | 115 ± 13 | 0.955 | 0.386 | −1.212 | 0.108 |
| DBP (mmHg) | 75 ± 10 | 73 ± 9 | 71 ± 9 | 10.223 | <0.001 | −2.058 | <0.001 | |
| BMI (kg/m2) f | 22.28 ± 6.88 | 22.02 ± 5.75 | 22.71 ± 6.58 | 1.753 | 0.180 | 0.127 | 0.156 | |
| Waist circumference (cm) g | 77.64 ± 16.87 | 76.26 ± 12.13 | 76.37 ± 15.44 | 2.043 | 0.138 | −0.643 | 0.050 | |
| Waist-to-hip ratio | 0.82 ± 0.09 | 0.81 ± 0.75 | 0.81 ± 0.09 | 3.967 | 0.024 | −0.009 | 0.012 | |
| Variables | Time Point 1 | Time Point 2 | Time Point 3 | RMANOVA | Imputed | GEE | p-Value |
|---|---|---|---|---|---|---|---|
| Mean ± SD | F | p-Value | Beta | ||||
| PSQI score | 6.57 ± 2.98 | 7.44 ± 6.24 | 6.45 ± 2.97 | 1.622 | 0.208 | 0.009 | 0.953 |
| Weekly Leisure Activity | 24.88 ± 31.81 | 25.51 ± 25.42 | 23.44 ± 30.31 | 2.731 | 0.081 | 0.826 | 0.638 |
| Healthy Eating score | 12.57 ± 4.85 | 12.21 ± 5.22 | 12.25 ± 4.98 | 0.200 | 0.813 | −0.017 | 0.928 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Yuen, J.W.M.; Wong, V.C.W.; Tam, W.W.S.; So, K.W.; Chien, W.T. A One-Year Prospective Follow-Up Study on the Health Profile of Hikikomori Living in Hong Kong. Int. J. Environ. Res. Public Health 2019, 16, 546. https://doi.org/10.3390/ijerph16040546
Yuen JWM, Wong VCW, Tam WWS, So KW, Chien WT. A One-Year Prospective Follow-Up Study on the Health Profile of Hikikomori Living in Hong Kong. International Journal of Environmental Research and Public Health. 2019; 16(4):546. https://doi.org/10.3390/ijerph16040546
Chicago/Turabian StyleYuen, John W. M., Victor C. W. Wong, Wilson W. S. Tam, Ka Wing So, and Wai Tong Chien. 2019. "A One-Year Prospective Follow-Up Study on the Health Profile of Hikikomori Living in Hong Kong" International Journal of Environmental Research and Public Health 16, no. 4: 546. https://doi.org/10.3390/ijerph16040546
APA StyleYuen, J. W. M., Wong, V. C. W., Tam, W. W. S., So, K. W., & Chien, W. T. (2019). A One-Year Prospective Follow-Up Study on the Health Profile of Hikikomori Living in Hong Kong. International Journal of Environmental Research and Public Health, 16(4), 546. https://doi.org/10.3390/ijerph16040546






