Risk of Cancer after Lower Urinary Tract Infection: A Population-Based Cohort Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Data Source
2.2. Patient Selection (Exposure of UTI Infection)
2.3. Propensity Score Matching (PSM)
2.4. Outcome Measurement of Cancer Event
2.5. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Appendix A
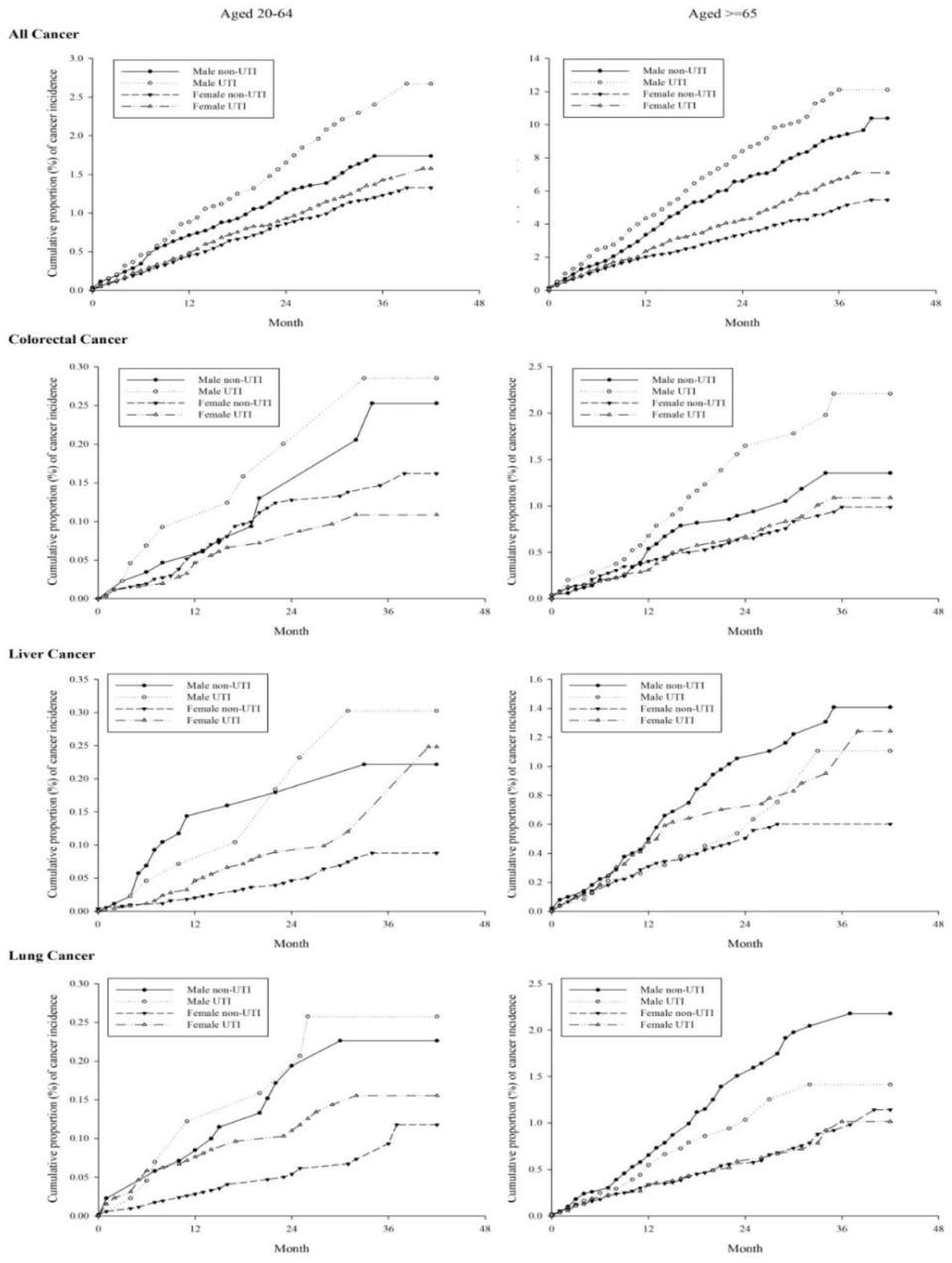
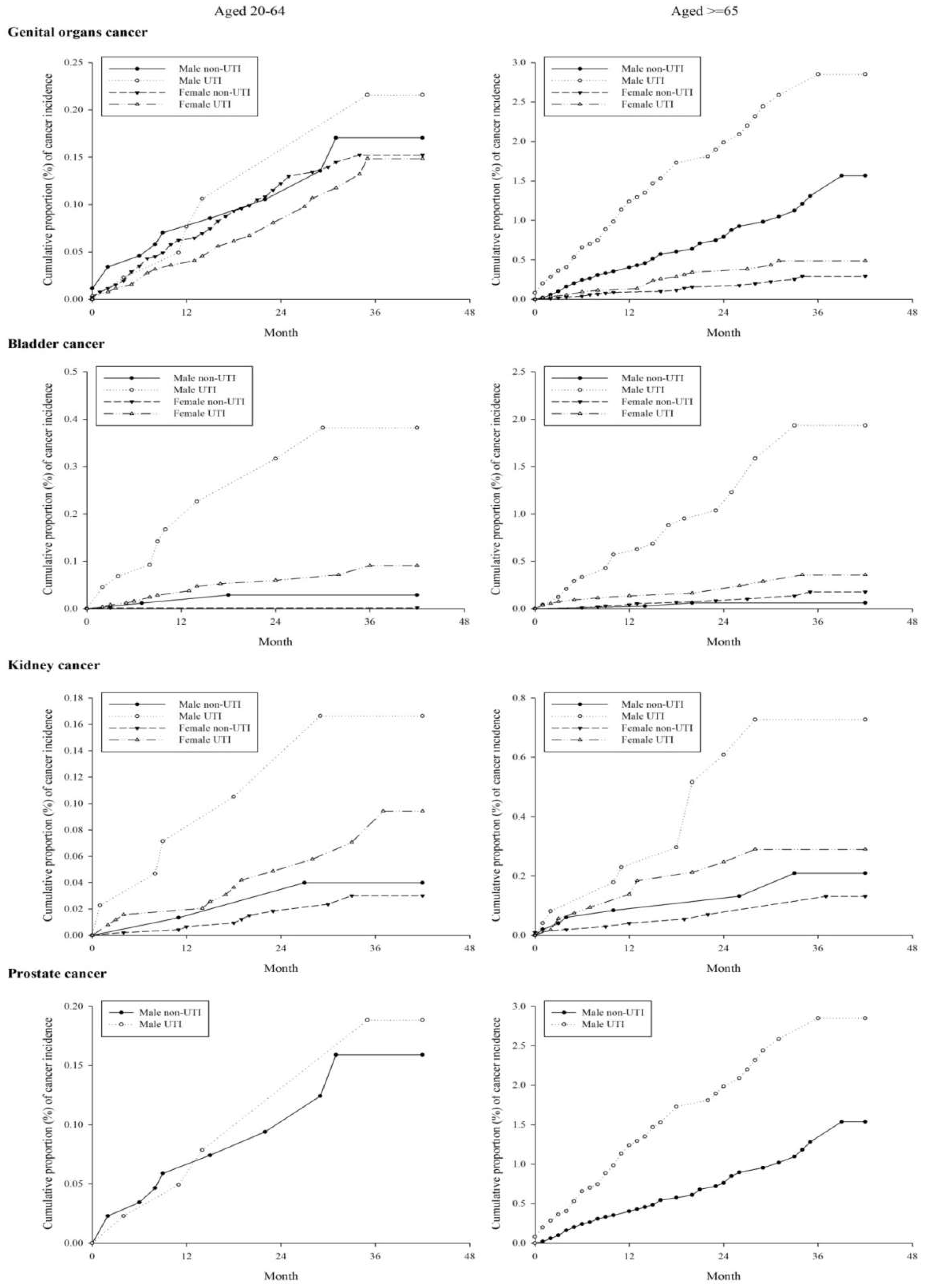

References
- Nicolle, L.E. Urinary tract infection. Crit. Care Clin. 2013, 29, 699–715. [Google Scholar] [CrossRef] [PubMed]
- Sun, L.M.; Lin, C.L.; Liang, J.A.; Liu, S.H.; Sung, F.C.; Chang, Y.J.; Kao, C.H. Urinary tract infection increases subsequent urinary tract cancer risk: A population-based cohort study. Cancer Sci. 2013, 104, 619–623. [Google Scholar] [CrossRef] [PubMed]
- Erdem, I.; Kara Ali, R.; Ardic, E.; Elbasan Omar, S.; Mutlu, R.; Topkaya, A.E. Community-acquired lower urinary tract infections: Etiology, antimicrobial resistance, and treatment results in female patients. J. Glob. Infect. Dis. 2018, 10, 129–132. [Google Scholar] [CrossRef] [PubMed]
- Arnold, J.J.; Hehn, L.E.; Klein, D.A. Common questions about recurrent urinary tract infections in women. Am. Family Phys. 2016, 93, 560–569. [Google Scholar]
- Rowe, T.A.; Juthani-Mehta, M. Diagnosis and management of urinary tract infection in older adults. Infect. Disease Clin. N. Am. 2014, 28, 75–89. [Google Scholar] [CrossRef] [PubMed]
- Anderson-Otunu, O.; Akhtar, S. Chronic infections of the urinary tract and bladder cancer risk: A systematic review. Asian Pac. J. Cancer Prev. APJCP 2016, 17, 3805–3807. [Google Scholar] [PubMed]
- Vermeulen, S.H.; Hanum, N.; Grotenhuis, A.J.; Castano-Vinyals, G.; van der Heijden, A.G.; Aben, K.K.; Mysorekar, I.U.; Kiemeney, L.A. Recurrent urinary tract infection and risk of bladder cancer in the nijmegen bladder cancer study. Br. J. Cancer 2015, 112, 594–600. [Google Scholar] [CrossRef] [PubMed]
- Dune, T.J.; Price, T.K.; Hilt, E.E.; Thomas-White, K.J.; Kliethermes, S.; Brincat, C.; Brubaker, L.; Schreckenberger, P.; Wolfe, A.J.; Mueller, E.R. Urinary symptoms and their associations with urinary tract infections in urogynecologic patients. Obstet. Gynecol. 2017, 130, 718–725. [Google Scholar] [CrossRef] [PubMed]
- Russell, B.; Garmo, H.; Beckmann, K.; Stattin, P.; Adolfsson, J.; Van Hemelrijck, M. A case-control study of lower urinary-tract infections, associated antibiotics and the risk of developing prostate cancer using pcbase 3.0. PLoS ONE 2018, 13, e0195690. [Google Scholar] [CrossRef] [PubMed]
- Chastain, D.B.; King, S.T.; Stover, K.R. Rethinking urinary antibiotic breakpoints: Analysis of urinary antibiotic concentrations to treat multidrug resistant organisms. BMC Res. Notes 2018, 11, 497. [Google Scholar] [CrossRef] [PubMed]
- Parsons, L.S. Performing a 1: N case-control match on propensity score. In Proceedings of the 29th Annual SAS Users Group International Conference, Montreal, QC, Canada, 9–12 May 2004; p. 165-29. [Google Scholar]
- Maj, M.; Bajek, A.; Nalejska, E.; Porowinska, D.; Kloskowski, T.; Gackowska, L.; Drewa, T. Influence of mesenchymal stem cells conditioned media on proliferation of urinary tract cancer cell lines and their sensitivity to ciprofloxacin. J. Cell. Biochem. 2017, 118, 1361–1368. [Google Scholar] [CrossRef] [PubMed]
- Batalha, P.N.; Vieira de Souza, M.C.; Pena-Cabrera, E.; Cruz, D.C.; da Costa Santos Boechat, F. Quinolones in the search for new anticancer agents. Curr. Pharm. Des. 2016, 22, 6009–6020. [Google Scholar] [CrossRef] [PubMed]
- Marcus, J.L.; Leyden, W.A.; Chao, C.R.; Horberg, M.A.; Klein, D.B.; Quesenberry, C.P., Jr.; Towner, W.J.; Silverberg, M.J. Immunodeficiency, aids-related pneumonia, and risk of lung cancer among hiv-infected individuals. AIDS 2017, 31, 989–993. [Google Scholar] [CrossRef] [PubMed]
- Michaud, D.S. Chronic inflammation and bladder cancer. Urol. Oncol. 2007, 25, 260–268. [Google Scholar] [CrossRef] [PubMed]
- Ferraz, R.; Costa-Rodrigues, J.; Fernandes, M.H.; Santos, M.M.; Marrucho, I.M.; Rebelo, L.P.; Prudencio, C.; Noronha, J.P.; Petrovski, Z.; Branco, L.C. Antitumor activity of ionic liquids based on ampicillin. ChemMedChem 2015, 10, 1480–1483. [Google Scholar] [CrossRef] [PubMed]
- Hasegawa, R.; Murasaki, G.; St John, M.K.; Zenser, T.V.; Cohen, S.M. Evaluation of nitrofurantoin on the two stages of urinary bladder carcinogenesis in the rat. Toxicology 1990, 62, 333–347. [Google Scholar] [CrossRef]
- Kijima, A.; Ishii, Y.; Takasu, S.; Matsushita, K.; Kuroda, K.; Hibi, D.; Suzuki, Y.; Nohmi, T.; Umemura, T. Chemical structure-related mechanisms underlying in vivo genotoxicity induced by nitrofurantoin and its constituent moieties in gpt delta rats. Toxicology 2015, 331, 125–135. [Google Scholar] [CrossRef] [PubMed]
- Williams, G.M. Classification of genotoxic and epigenetic hepatocarcinogens using liver culture assays. Ann. N. Y. Acad. Sci. 1980, 349, 273–282. [Google Scholar] [CrossRef]
- International Agency for Research on Cancer. Monographs on the Evaluation of Carcinogen Risk to Humans: Some Industrial Chemicals; International Agency for Research on Cancer: Lyon, France, 1994. [Google Scholar]
- Kimura, M.; Mizukami, S.; Watanabe, Y.; Hasegawa-Baba, Y.; Onda, N.; Yoshida, T.; Shibutani, M. Disruption of spindle checkpoint function in rats following 28 days of repeated administration of renal carcinogens. J. Toxicol. Sci. 2016, 41, 91–104. [Google Scholar] [CrossRef] [PubMed]
- Tsuchiya, T.; Kijima, A.; Ishii, Y.; Takasu, S.; Yokoo, Y.; Nishikawa, A.; Yanai, T.; Umemura, T. Role of oxidative stress in the chemical structure-related genotoxicity of nitrofurantoin in nrf2-deficient gpt delta mice. J. Toxicol. Pathol. 2018, 31, 169–178. [Google Scholar] [CrossRef] [PubMed]
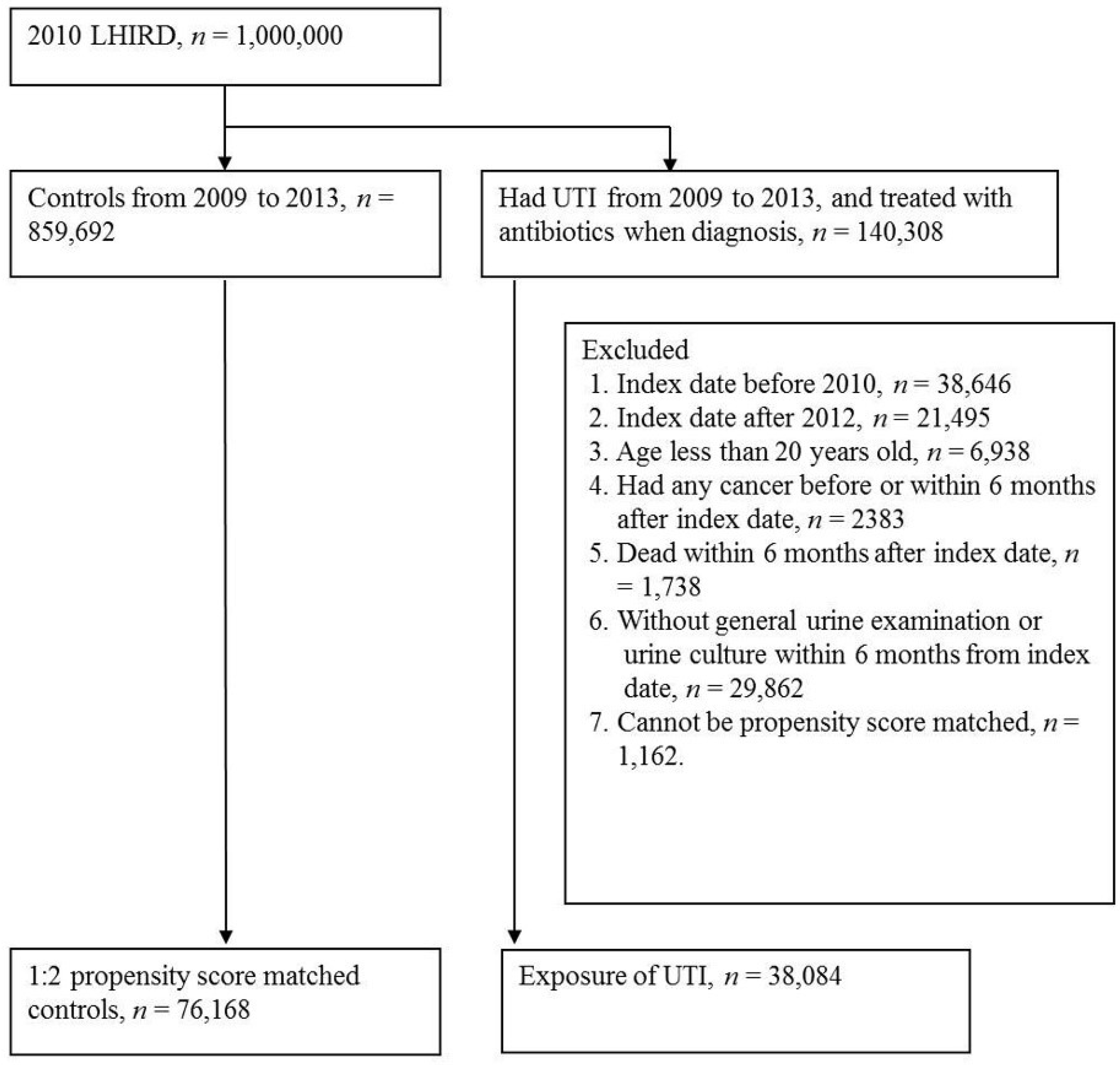
| Male | p Value | Female | p Value | |||
|---|---|---|---|---|---|---|
| Non-UTI N = 13,824 | UTI N = 6,912 | Non-UTI N = 62,344 | UTI N = 31,172 | |||
| Age | 0.8332 | 0.4579 | ||||
| 20–44 | 4355 (31.5%) | 2201 (31.84%) | 31112 (49.90%) | 15513 (49.77%) | ||
| 45–65 | 4411 (31.91%) | 2209 (31.96%) | 20540 (32.95%) | 10212 (32.76%) | ||
| ≥65 | 5058 (36.59%) | 2502 (36.20%) | 10692 (17.15%) | 5447 (17.47%) | ||
| CCIs | 0.8214 | 0.1808 | ||||
| 0 | 6503 (47.04%) | 3260 (47.16%) | 37784 (60.61%) | 18906 (60.65%) | ||
| 1–2 | 5215 (37.72%) | 2604 (37.67%) | 20116 (32.27%) | 9961 (31.95%) | ||
| 3–4 | 1670 (12.08%) | 846 (12.24%) | 3765 (6.04%) | 1921 (6.16%) | ||
| ≥5 | 436 (3.15%) | 202 (2.92%) | 679 (1.09%) | 384 (1.23%) | ||
| Co-morbidity | ||||||
| Hypertension | 5270 (38.12%) | 2661 (38.50%) | 0.5993 | 13847 (22.21%) | 6963 (22.34%) | 0.6605 |
| Diabetes | 2484 (17.97%) | 1248 (18.06%) | 0.8781 | 7391 (11.86%) | 3730 (11.97%) | 0.6221 |
| Hyperlipidemia | 2842 (20.56%) | 1414 (20.46%) | 0.8648 | 10363 (16.62%) | 5189 (16.65%) | 0.9258 |
| Rheumatic diseases | 399 (2.89%) | 207 (2.99%) | 0.6619 | 2650 (4.25%) | 1317 (4.22%) | 0.8544 |
| Coronary artery disease | 1943 (14.06%) | 957 (13.85%) | 0.6814 | 4702 (7.54%) | 2367 (7.59%) | 0.7795 |
| COPD | 2083 (15.07%) | 1047 (15.15%) | 0.8801 | 4970 (7.97%) | 2594 (8.32%) | 0.0645 |
| CKD | 470 (3.40%) | 231 (3.34%) | 0.8279 | 723 (1.16%) | 397 (1.27%) | 0.1312 |
| Pneumonia | 254 (1.84%) | 628 (9.09%) | <0.0001 | 388 (0.62%) | 716 (2.30%) | <0.0001 |
| 20–64 y/o | aHR | ≥65 y/o | aHR | |||
|---|---|---|---|---|---|---|
| Incidence Rate | Incidence Rate | |||||
| Non-UTI | UTI | Non-UTI | UTI | |||
| Male | ||||||
| All cancer | 5.05 | 6.93 | 1.37 (1.02–1.86) | 27.70 | 35.40 | 1.29 (1.08–1.54) |
| Colorectal | 0.58 | 0.77 | 1.32 (0.54–3.23) | 3.78 | 5.96 | 1.59 (1.01–2.52) |
| Liver | 0.72 | 0.77 | 1.05 (0.44–2.47) | 4.04 | 2.61 | 0.65 (0.36–1.19) |
| Lung | 0.67 | 0.77 | 1.46 (0.75–2.86) | 5.98 | 4.10 | 1.13 (0.75–1.70) |
| Genital organs | 0.48 | 0.48 | 1.05 (0.36–3.09) | 3.52 | 8.39 | 2.37 (1.55–3.64) |
| Bladder | 0.10 | 1.15 | 12.10 (2.70–54.19) | 0.18 | 5.03 | 28.60 (6.80–120.28) |
| Kidney | 0.10 | 0.48 | 5.20 (1.01–26.82) | 0.53 | 2.05 | 3.85 (1.42–10.42) |
| Prostate | 0.43 | 0.38 | 0.96 (0.29–3.15) | 3.43 | 8.39 | 2.44 (1.59–3.74) |
| Female | ||||||
| All cancer | 3.52 | 3.95 | 1.13 (0.97–1.32) | 14.49 | 18.96 | 1.30 (1.11–1.53) |
| Colorectal | 0.45 | 0.32 | 0.70 (0.42–1.17) | 2.76 | 2.91 | 1.06 (0.71–1.57) |
| Liver | 0.21 | 0.36 | 1.75 (1.00–3.04) | 1.94 | 3.06 | 1.54 (1.02–2.33) |
| Lung | 0.25 | 0.47 | 1.22 (0.86–1.71) | 2.56 | 2.52 | 0.75 (0.43–1.32) |
| Genital organs | 0.46 | 0.36 | 0.79 (0.49–1.28) | 0.74 | 1.38 | 1.86 (0.98–3.56) |
| Bladder | 0.01 | 0.24 | 30.02 (3.97–227.28) | 0.39 | 0.92 | 2.34 (1.01–5.42) |
| Kidney | 0.07 | 0.21 | 2.90 (1.24–6.78) | 0.27 | 0.92 | 3.40 (1.34–8.64) |
| Breast | 1.16 | 1.04 | 0.90 (0.68–1.21) | 1.51 | 1.68 | 1.10 (0.65–1.85) |
| Crude HR | 95% C.I. | p Value | aHR † | 95% C.I. | p Value | |
|---|---|---|---|---|---|---|
| UTI (Ref: No) | ||||||
| Yes | 1.27 | 1.09–1.48 | 0.0023 | 1.32 | 1.12–1.54 | 0.0007 |
| Age (Ref: 20-44) | ||||||
| 45-65 | 5.21 | 3.50–7.76 | <0.0001 | 4.69 | 3.14–7.03 | <0.0001 |
| ≥65 | 16.37 | 11.26–23.79 | <0.0001 | 12.32 | 8.29–18.31 | <0.0001 |
| CCIs score (Ref: 0) | ||||||
| 1–2 | 2.34 | 1.94–2.82 | <0.0001 | 1.28 | 1.03–1.58 | 0.0230 |
| 3–4 | 3.87 | 3.11–4.81 | <0.0001 | 1.50 | 1.13–1.99 | 0.0046 |
| ≥5 | 5.42 | 3.92–7.49 | <0.0001 | 1.88 | 1.24–2.84 | 0.0027 |
| Co-morbidity | ||||||
| Hypertension | 2.69 | 2.31–3.14 | <0.0001 | 1.12 | 0.94–1.34 | 0.1901 |
| Diabetes | 1.76 | 1.49–2.09 | <0.0001 | 0.90 | 0.73–1.10 | 0.2867 |
| Hyperlipidemia | 1.38 | 1.16–1.64 | 0.0002 | 0.93 | 0.77–1.12 | 0.4413 |
| Rheumatic diseases | 1.31 | 0.89–1.94 | 0.1747 | 1.00 | 0.67–1.48 | 0.9981 |
| Coronary artery disease | 2.44 | 2.06–2.89 | <0.0001 | 1.25 | 1.04–1.49 | 0.0165 |
| COPD | 2.02 | 1.70–2.40 | <0.0001 | 1.05 | 0.86–1.27 | 0.6569 |
| CKD | 2.21 | 1.62–3.03 | <0.0001 | 0.98 | 0.70–1.37 | 0.8845 |
| Pneumonia | 2.15 | 1.61–2.88 | <0.0001 | 0.95 | 0.70–1.29 | 0.7612 |
| Crude HR | 95% C.I. | p Value | aHR † | 95% C.I. | p Value | |
|---|---|---|---|---|---|---|
| UTI (Ref: No) | ||||||
| Yes | 1.21 | 1.09–1.36 | 0.0007 | 1.21 | 1.08–1.35 | 0.0009 |
| Age (Ref: 20-44) | ||||||
| 45–65 | 4.68 | 3.94–5.57 | <0.0001 | 4.41 | 3.68–5.27 | <0.0001 |
| ≥65 | 10.78 | 9.09–12.78 | <0.0001 | 9.00 | 7.37–11.00 | <0.0001 |
| CCIs score (Ref: 0) | ||||||
| 1–2 | 2.16 | 1.92–2.44 | <0.0001 | 1.24 | 1.08–1.43 | 0.0023 |
| 3–4 | 3.86 | 3.27–4.57 | <0.0001 | 1.40 | 1.13–1.74 | 0.0024 |
| ≥5 | 5.47 | 4.02–7.44 | <0.0001 | 1.54 | 1.03–2.29 | 0.0349 |
| Co-morbidity | ||||||
| Hypertension | 3.08 | 2.76–3.43 | <0.0001 | 1.11 | 0.97–1.26 | 0.1444 |
| Diabetes | 2.39 | 2.10–2.71 | <0.0001 | 0.95 | 0.81–1.11 | 0.4982 |
| Hyperlipidemia | 1.94 | 1.72–2.19 | <0.0001 | 0.88 | 0.78–1.01 | 0.0774 |
| Rheumatic diseases | 1.28 | 1.00–1.63 | 0.0478 | 0.93 | 0.72–1.18 | 0.5332 |
| Coronary artery disease | 2.51 | 2.18–2.91 | <0.0001 | 1.05 | 0.90–1.23 | 0.5270 |
| COPD | 1.63 | 1.39–1.93 | <0.0001 | 0.91 | 0.76–1.09 | 0.3035 |
| CKD | 3.76 | 2.84–4.97 | <0.0001 | 1.51 | 1.09–2.10 | 0.0141 |
| Pneumonia | 2.18 | 1.52–3.13 | <0.0001 | 0.97 | 0.67–1.41 | 0.8892 |
| Non-UTI and Non-Pneumonia | Only UTI | Only Pneumonia | UTI Combined Pneumonia | p for Interaction | |
|---|---|---|---|---|---|
| Male | |||||
| All cancer | Reference | 1.35 (1.15–1.59) | 1.24 (0.75–2.06) | 1.14 (0.80–1.64) | 0.2270 |
| Colorectal | Reference | 1.54 (0.99–2.38) | 1.90 (0.58–6.19) | 1.76 (0.75–4.16) | 0.4963 |
| Liver | Reference | 0.86 (0.52–1.41) | 1.12 (0.27–4.65) | 0.23 (0.03–1.69) | 0.2585 |
| Lung | Reference | 0.79 (0.50–1.24) | 1.32 (0.48–3.68) | 0.78 (0.31–1.93) | 0.6723 |
| Genital organs | Reference | 2.23 (1.49–3.35) | 0.60 (0.08–4.36) | 1.25 (0.49–3.17) | 0.9541 |
| Bladder | Reference | 21.64 (7.71–60.77) | Can not estimate | 7.63 (1.37–42.42) | 0.9879 |
| Kidney | Reference | 4.10 (1.72–9.80) | Can not estimate | 3.84 (0.78–18.87) | 0.9908 |
| Prostate | Reference | 2.29 (1.51–3.45) | 0.61 (0.08–4.45) | 1.28 (0.51–3.26) | 0.9426 |
| Female | |||||
| All cancer | Reference | 1.20 (1.08–1.35) | 0.85 (0.42–1.72) | 1.24 (0.81–1.90) | 0.6554 |
| Colorectal | Reference | 0.92 (0.68–1.26) | 0.68 (0.10–4.93) | 0.35 (0.05–2.50) | 0.6741 |
| Liver | Reference | 1.57 (1.12–2.21) | 0.72 (0.10–5.19) | 1.76 (0.70–4.41) | 0.6862 |
| Lung | Reference | 1.26 (0.91–1.75) | 2.13 (0.676.79) | 1.95 (0.78–4.85) | 0.6684 |
| Genital organs | Reference | 1.03 (0.70–1.52) | Can not estimate | 1.63 (0.39–6.77) | 0.9735 |
| Bladder | Reference | 4.84 (2.39–9.80) | Can not estimate | 4.60 (0.58–36.22) | 0.9944 |
| Kidney | Reference | 3.43 (1.81–6.51) | 6.44 (0.83–50.19) | Can not estimate | 0.9768 |
| Breast | Reference | 0.96 (0.75–1.24) | 0.79 (0.11–5.66) | 0.43 (0.06–3.08) | 0.6890 |
| Days of Antibiotics Prescriptions within 6 Months before Index Date | p for Trend | |||
|---|---|---|---|---|
| 1–6 days | 7–13 days | ≥14 days | ||
| Male | n = 17241 | n = 1940 | n = 1555 | |
| All cancer | Reference | 1.02 (0.75–1.40) | 1.45 (1.09–1.91) | 0.0130 |
| Colorectal | Reference | 1.16 (0.54–2.46) | 1.05 (0.49–2.23) | 0.8669 |
| Liver | Reference | 0.93 (0.32–2.72) | 1.35 (0.51–3.56) | 0.5874 |
| Lung | Reference | 1.43 (0.60–3.41) | 1.39 (0.58–3.30) | 0.4213 |
| Genital organs | Reference | 0.81 (0.37–1.77) | 1.44 (0.78–2.66) | 0.2860 |
| Bladder | Reference | 1.23 (0.50–3.02) | 2.73 (1.32–5.64) | 0.0066 |
| Kidney | Reference | 0.68 (0.18–2.55) | 1.14 (0.37–3.54) | 0.8995 |
| Prostate | Reference | 0.82 (0.38–1.78) | 1.36 (0.73–2.54) | 0.3822 |
| Female | n = 80515 | n = 9014 | n = 3987 | |
| All cancer | Reference | 1.08 (0.88–1.32) | 1.10 (0.87–1.40) | 0.3605 |
| Colorectal | Reference | 1.00 (0.54–1.85) | 1.31 (0.68–2.54) | 0.4775 |
| Liver | Reference | 1.19 (0.67–2.10) | 1.12 (0.58–2.19) | 0.6352 |
| Lung | Reference | 1.53 (0.87–2.69) | 1.49 (0.78–2.85) | 0.1511 |
| Genital organs | Reference | 2.06 (1.10–3.85) | 0.33 (0.08–1.41) | 0.7254 |
| Bladder | Reference | 0.41 (0.12–1.44) | 2.30 (1.01–5.25) | 0.1283 |
| Kidney | Reference | 2.34 (0.97–5.66) | 1.73 (0.58–5.20) | 0.1741 |
| Breast | Reference | 1.13 (0.70–1.83) | 1.42 (0.81–2.49) | 0.2356 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Huang, C.-H.; Chou, Y.-H.; Yeh, H.-W.; Huang, J.-Y.; Yang, S.-F.; Yeh, C.-B. Risk of Cancer after Lower Urinary Tract Infection: A Population-Based Cohort Study. Int. J. Environ. Res. Public Health 2019, 16, 390. https://doi.org/10.3390/ijerph16030390
Huang C-H, Chou Y-H, Yeh H-W, Huang J-Y, Yang S-F, Yeh C-B. Risk of Cancer after Lower Urinary Tract Infection: A Population-Based Cohort Study. International Journal of Environmental Research and Public Health. 2019; 16(3):390. https://doi.org/10.3390/ijerph16030390
Chicago/Turabian StyleHuang, Chia-Hung, Ying-Hsiang Chou, Han-Wei Yeh, Jing-Yang Huang, Shun-Fa Yang, and Chao-Bin Yeh. 2019. "Risk of Cancer after Lower Urinary Tract Infection: A Population-Based Cohort Study" International Journal of Environmental Research and Public Health 16, no. 3: 390. https://doi.org/10.3390/ijerph16030390
APA StyleHuang, C.-H., Chou, Y.-H., Yeh, H.-W., Huang, J.-Y., Yang, S.-F., & Yeh, C.-B. (2019). Risk of Cancer after Lower Urinary Tract Infection: A Population-Based Cohort Study. International Journal of Environmental Research and Public Health, 16(3), 390. https://doi.org/10.3390/ijerph16030390






