Has the Efficiency of China’s Healthcare System Improved after Healthcare Reform? A Network Data Envelopment Analysis and Tobit Regression Approach
Abstract
1. Introduction
2. Materials and Methods
2.1. Network DEA Methodology
2.2. Variables and Data
3. Results
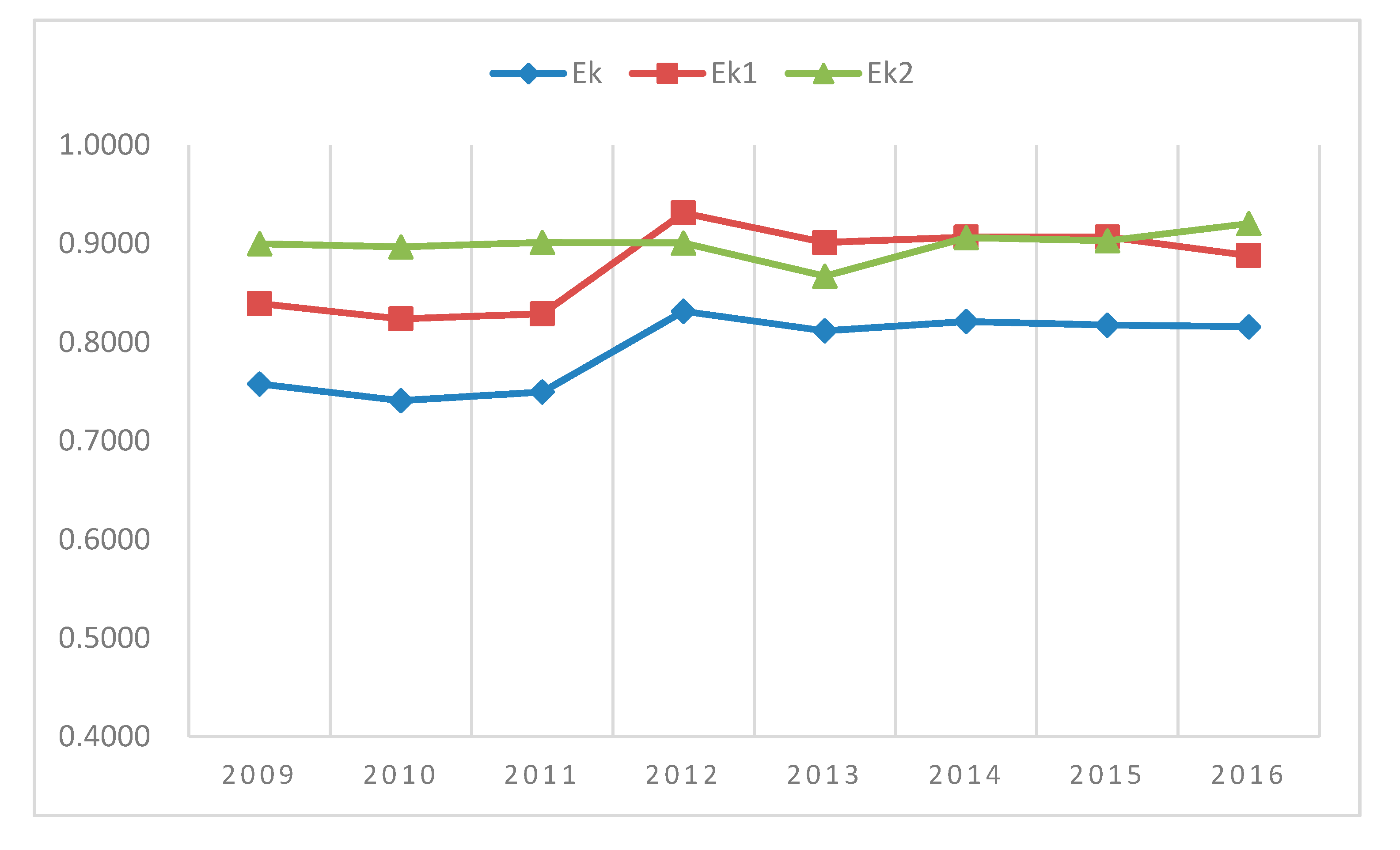
3.1. Results of Network DEA
3.2. Results of Tobit Regression Analysis
4. Discussion
5. Conclusions and Policy Recommendations
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- World Health Organization (WHO). The World Health Report; WHO: Geneva, Switzerland, 2000. [Google Scholar]
- Hu, R.; Shen, C.; Zou, H. Health Care System Reform in China: Issues, Challenges and Options. CEMA Working Papers, China Economics and Management Academy, Central University of Finance and Economics. Available online: https://ideas.repec.org/p/cuf/wpaper/517.html (accessed on 25 July 2019).
- Wagstaff, A.; Yip, W.; Lindelow, M.; Hsiao, W.C. China’s health system and its reform: a review of recent studies. Health Econ. 2009, 18 (Suppl. 2), S7–S23. [Google Scholar] [CrossRef]
- Burns, L.R.; Liu, G.G. China’s Health Care and Reform; Cambridge University Press: New York, NY, USA, 2017. [Google Scholar]
- Mirhedayatian, S.M.; Azadi, M.; Farzipoor Saen, R. A novel network data envelopment analysis model for evaluating green supply chain management. Int. J. Prod. Econ. 2014, 147, 544–554. [Google Scholar] [CrossRef]
- Ng, Y.C. The productive efficiency of Chinese hospitals. China Econ. Rev. 2011, 22, 428–439. [Google Scholar] [CrossRef]
- Cheng, Z.; Tao, H.; Cai, M. Using a two-stage data envelopment analysis to estimate the efficiency of county hospitals in China: A panel data study. Lancet 2015, 386 (Suppl. 1), S64. [Google Scholar] [CrossRef]
- Wu, S.; Wang, C.; Zhang, G. Has China’s new health care reform improved efficiency at the provincial level? Evidence from a panel data of 31 Chinese provinces. J. Asian Public Policy 2015, 8, 36–55. [Google Scholar] [CrossRef]
- Jiang, S.; Wu, W.; Fang, P. Evaluating the effectiveness of public hospital reform from the perspective of efficiency and quality in Guangxi, China. Springer Plus 2016, 5, 1922. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Jiang, S.; Min, R.; Fang, P. The impact of healthcare reform on the efficiency of public county hospitals in China. BMC Health Serv. Res. 2017. [Google Scholar] [CrossRef] [PubMed]
- Leng, Y.; Liu, W.; Xiao, N.; Li, Y.; Deng, J. The impact of policy on the intangible service efficiency of the primary health care institution—Based on China’s health care reform policy in 2009. Int. J. Equtiy Health 2019. [Google Scholar] [CrossRef]
- Kao, C. Efficiency decomposition in network data envelopment analysis: A relational model. Eur. J Oper. Res. 2009, 192, 949–962. [Google Scholar] [CrossRef]
- Färe, R.; Grosskopf, S. Network DEA. Socio Econ. Plan. Sci. 2000, 1, 35–49. [Google Scholar] [CrossRef]
- Hao, Y. Universal health insurance coverage for 1.3 billion people: What accounts for China’s success? Health Policy 2015, 9, 1145–1152. [Google Scholar]
- Weissman, J.S.; Epstein, A.M. Falling Through the Safety Net: Insurance Status and Access to Health Care; Johns Hopkins University Press: Baltimore, MD, USA, 1994. [Google Scholar]
- Pan, J.; Lei, X.; Liu, G. Does Health Insurance Lead to Better Health? Econ. Res. J. 2013, 4, 132–142. [Google Scholar]
- Kao, C.; Hwang, S. Efficiency decomposition in two–stage data envelopment analysis: An application to non–life insurance companies in Taiwan. Eur. J. Oper. Res. 2008, 185, 418–429. [Google Scholar] [CrossRef]
- Samut, P.K.; Cafrı, R. Analysis of the Efficiency Determinants of Health Systems in OECD Countries by DEA and Panel Tobit. Soc. Indic. Res. 2016, 129, 113–132. [Google Scholar] [CrossRef]
- Sun, J.; Luo, H. Evaluation on equality and efficiency of health resources allocation and health services utilization in China. Int. J. Equity Health 2017, 16, 127. [Google Scholar] [CrossRef] [PubMed]
- Novignon, J.; Olakojo, S.A.; Nonvignon, J. The effects of public and private health care expenditure on health status in sub-Saharan Africa: new evidence from panel data analysis. Health Econ. Rev. 2012. [CrossRef]
- Tam, W. Failing to Treat: Why Public Hospitals in China Do Not Work. China Rev. 2008, 8, 103–130. [Google Scholar]
- Restuccia, J.; Shwartz, M.; Ash, A.; Payne, S. High hospital admission rates and inappropriate care. Health Aff. 1996, 15, 156–163. [Google Scholar] [CrossRef]
- Fusco, M.; Buja, A.; Piergentili, P.; Golfetto, M.T.; Serafin, G.; Gallo, S.; Barba, L.D.; Baldo, V. Individual and hospital-related determinants of potentially inappropriate admissions emerging from administrative records. Health Police 2016, 120, 1304–1312. [Google Scholar] [CrossRef]
- Huang, Y.; Liu, Y.; Yang, X.; Li, J.; Fang, P. Global budget payment system helps to reduce outpatient medical expenditure of hypertension in China. Springer Plus 2016. [Google Scholar] [CrossRef]
- Dong, K. Medical insurance system evolution in China. China Econ. Rev. 2009, 20, 591–597. [Google Scholar] [CrossRef]
- You, X.; Kobayashi, Y. Determinants of out-of-pocket health expenditure in China. Appl. Health Econ. Health Policy 2011, 9, 39. [Google Scholar] [CrossRef] [PubMed]
- Lei1, S.; Zhang, Y.; Li, H.; Su, D.; Chang, J.; Hu, X.; Ye, Q. Determinants of inappropriate admissions of children to county hospitals: A cross–sectional study from rural China. BMC Health Serv. Res. 2019, 19, 126. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Y.; Chen, Y.; Zhang, X.; Zhang, L. Current level and determinants of inappropriate admissions to township hospitals under the new rural cooperative medical system in China: A cross–sectional study. BMC Health Serv. Res. 2014, 14, 649. [Google Scholar] [CrossRef] [PubMed]
- Tam, W. Organizational corruption by public hospitals in China. Crime Law Soc. Change 2011, 56, 265. [Google Scholar] [CrossRef]
- Zhang, H.; Hu, H.; Wu, C.; Yu, H.; Dong, H. Impact of China’s Public Hospital Reform on Healthcare Expenditures and Utilization: A Case Study in ZJ Province. PLoS ONE 2015, 10, e143130. [Google Scholar] [CrossRef]
- Li, J.; He, P.; He, R. Theoretical and empirical analysis of the supplier induced demand in the health care market in China. Grey Syst. Theory Appl. 2019, 4, 207–220. [Google Scholar] [CrossRef]
- Zhang, T.; Xu, Y.; Ren, J.; Sun, L.; Liu, C. Inequality in the distribution of health resources and health services in China: hospitals versus primary care institutions. Int. J. Equity Health 2017, 16, 42. [Google Scholar] [CrossRef]
- China Daily. Hierarchical Diagnosis is Irreplaceable to ‘Healthy China’ Strategy. Available online: http://www.chinadaily.com.cn/m/2016jilin/2018–03/19/content_35875467.htm (accessed on 19 March 2018).
| Variables | Definition | Measurement |
|---|---|---|
| Inputs | ||
| Health technicians per 1000 Persons | Health technicians include doctors with authorization, registered nurses, pharmacists, laboratory physician, radiologists, and other medical professionals. | Density per 1000 population |
| Beds per 1000 Persons | Beds are the total number of beds that are available in medical institution, excluding beds for observation, extra beds, etc. | Density per 1000 population |
| Per capital total health expenditure | The ratio of the total amount of money raised from the whole society for health services to the population of a region in a certain period of time. | Yuan |
| Outputs | ||
| Maternal mortality rate | The maternal mortality rate is the number of maternal deaths per 100,000 women. | Per 100,000 |
| Perinatal survival rate | Perinatal mortality is the number of perinatal deaths, which occurs in the second trimester, during yield and within 7 days of birth. | Per 1000 |
| Life expectancy | Life expectancy at birth measures how long, on average, a newborn can be expected to live. | Years |
| Intermediates | ||
| Outpatients visit | Total number of outpatient visits during the Financial year. | Per 100,000 |
| Inpatients visit | Total number of inpatient visits during the Financial year. | Per 100,000 |
| Inpatient days | It is calculated by the total number of days discharged patients are in bed divided by the number discharged patients. | Days |
| Independent variables | ||
| Region | China is divided into the east region, middle region and western region, according to the geographical location and the level of economic development. | |
| Per capital GDP | The level of per capital GDP is measured by dividing the gross domestic productof each province by the average population | Billion yuan |
| Education | Education level is reflected by comparing the number of higher education students per 100,000 population in each province with the average of higher education students per 100,000 population. | Per 100,0000 population |
| Government health expenditure | Government health expenditure are the funds used by governments at all levels for medical and health services, medical security subsidies, health and medical security administration, population and family planning affairs expenditures, and other undertakings. | 10,000 yuan |
| Social health expenditure | Social health expenditure is outside government expenditure: all sectors of society invest in health. | Billion yuan |
| Personal health expenditure | Personal health expenditure are the cash payment by residents when receiving various health services. | Billion yuan |
| public hospital | Number of public hospitals are the total number of hospitals that are owned or controlled by a government unit or other public corporations. | |
| private hospital | Number of private hospitals are total number of hospitals that are not owned or controlled by government or other public organizations. | |
| Provinces | 2009 | 2010 | 2011 | 2012 | 2013 | 2014 | 2015 | 2016 |
|---|---|---|---|---|---|---|---|---|
| Beijing | 0.3500 | 0.3660 | 0.3982 | 0.6715 | 0.6988 | 0.7121 | 0.7186 | 0.7234 |
| Tianjin | 0.5623 | 0.5458 | 0.5971 | 0.8854 | 0.8739 | 0.9016 | 0.8840 | 0.9415 |
| Hebei province | 0.8305 | 0.7593 | 0.7922 | 0.8798 | 0.8582 | 0.8927 | 0.8772 | 0.8794 |
| Shanxi province | 0.6959 | 0.7516 | 0.7675 | 0.7747 | 0.7768 | 0.7678 | 0.8078 | 0.8315 |
| Inner Mongolia | 0.7353 | 0.6864 | 0.6750 | 0.7585 | 0.7182 | 0.7299 | 0.7306 | 0.7498 |
| Liaoning province | 0.5713 | 0.5606 | 0.6214 | 0.7059 | 0.6804 | 0.7375 | 0.7928 | 0.7467 |
| Jilin province | 0.6299 | 0.6259 | 0.6681 | 0.7836 | 0.7678 | 0.7912 | 0.7847 | 0.7802 |
| Heilongjiang province | 0.6631 | 0.6232 | 0.6542 | 0.7679 | 0.7388 | 0.7762 | 0.7945 | 0.7940 |
| Shanghai | 0.4201 | 0.3619 | 0.3891 | 0.7368 | 0.7247 | 0.7517 | 0.7249 | 0.7575 |
| Jiangsu province | 0.7197 | 0.7121 | 0.7033 | 0.7959 | 0.7546 | 0.7561 | 0.7476 | 0.7459 |
| Zhejiang province | 0.6891 | 0.6728 | 0.6823 | 0.7877 | 0.7915 | 0.7897 | 0.7634 | 0.7709 |
| Anhui province | 0.9454 | 0.9258 | 0.9289 | 0.9271 | 0.9375 | 0.9378 | 0.9455 | 0.9642 |
| Fujian province | 0.8401 | 0.7970 | 0.7831 | 0.8901 | 0.8263 | 0.8624 | 0.8648 | 0.9114 |
| Jiangxi province | 1 | 0.9493 | 0.9514 | 0.9525 | 0.9459 | 0.9362 | 0.9478 | 0.9457 |
| Shandong province | 0.7065 | 0.6909 | 0.6946 | 0.7233 | 0.7225 | 0.7841 | 0.7749 | 0.7879 |
| Henan province | 0.8743 | 0.8332 | 0.8586 | 0.8369 | 0.8537 | 0.8640 | 0.8457 | 0.8466 |
| Hubei province | 0.8131 | 0.7961 | 0.7562 | 0.7827 | 0.7398 | 0.7662 | 0.8487 | 0.7051 |
| Hunan province | 0.8829 | 0.9296 | 0.8903 | 0.8723 | 0.8125 | 0.8551 | 0.7898 | 0.7922 |
| Guangdong province | 0.7636 | 0.7310 | 0.7306 | 0.9298 | 0.9299 | 0.9410 | 0.9402 | 0.9306 |
| Guangxi province | 1 | 0.9166 | 0.9884 | 0.9676 | 0.9344 | 0.9841 | 0.9872 | 0.9301 |
| Hainan province | 0.8138 | 0.8933 | 0.8777 | 0.9825 | 0.9462 | 0.9582 | 0.9130 | 0.9365 |
| Chongqing | 0.8627 | 0.8195 | 0.8220 | 0.8089 | 0.8257 | 0.8159 | 0.7976 | 0.7782 |
| Sichuan province | 0.8274 | 0.7896 | 0.8145 | 0.8034 | 0.7922 | 0.8013 | 0.7732 | 0.7668 |
| Guizhou province | 1 | 1 | 1 | 1 | 0.9847 | 0.9268 | 0.9103 | 0.8748 |
| Yunnan province | 0.9280 | 0.8513 | 0.8818 | 0.9474 | 0.8773 | 0.9384 | 0.8840 | 0.8809 |
| Shaanxi province | 0.6969 | 0.7670 | 0.6825 | 0.7152 | 0.6956 | 0.7055 | 0.6997 | 0.7016 |
| Gansu province | 0.8811 | 0.8374 | 0.8315 | 0.8578 | 0.8355 | 0.8588 | 0.8519 | 0.8501 |
| Qinghai province | 0.7128 | 0.7160 | 0.7590 | 0.8901 | 0.9391 | 0.7075 | 0.7190 | 0.7366 |
| Ningxia | 0.6981 | 0.7090 | 0.7241 | 0.8402 | 0.7477 | 0.7453 | 0.7557 | 0.7600 |
| Sinkiang | 0.6194 | 0.6066 | 0.5629 | 0.6719 | 0.6192 | 0.6360 | 0.6479 | 0.6538 |
| Degree of efficiency = 1 | 3 | 1 | 1 | 1 | 0 | 0 | 0 | 0 |
| Between mean and 1 | 12 | 15 | 15 | 13 | 14 | 13 | 13 | 13 |
| <Mean | 15 | 14 | 14 | 16 | 16 | 17 | 17 | 17 |
| mean | 0.7578 | 0.7408 | 0.7495 | 0.8316 | 0.8116 | 0.8210 | 0.8174 | 0.8158 |
| Maximum | 1 | 1 | 1 | 1 | 0.9847 | 0.9841 | 0.9872 | 0.9642 |
| Minimum | 0.3500 | 0.3619 | 0.3891 | 0.6715 | 0.6192 | 0.6360 | 0.6479 | 0.6538 |
| standard deviation | 0.1596 | 0.1546 | 0.1488 | 0.0936 | 0.0959 | 0.0916 | 0.0850 | 0.0860 |
| Provinces | 2009 | 2010 | 2011 | 2012 | 2013 | 2014 | 2015 | 2016 |
|---|---|---|---|---|---|---|---|---|
| Beijing | 0.5690 | 0.5972 | 0.5856 | 0.9123 | 0.8532 | 0.8064 | 0.8190 | 0.8041 |
| Tianjin | 0.6512 | 0.6333 | 0.6984 | 1 | 1 | 1 | 1 | 1 |
| Hebei province | 0.8305 | 0.7593 | 0.8207 | 0.9348 | 0.9243 | 0.9401 | 0.9331 | 0.9236 |
| Shanxi province | 0.8408 | 0.8710 | 0.9784 | 0.9742 | 0.9640 | 0.9538 | 1 | 1 |
| Inner Mongolia | 0.7850 | 0.7328 | 0.7843 | 0.8764 | 0.8262 | 0.8218 | 0.8438 | 0.8459 |
| Liaoning province | 0.7117 | 0.6969 | 0.7788 | 0.8918 | 0.8547 | 0.9099 | 0.9781 | 0.8977 |
| Jilin province | 0.6463 | 0.6383 | 0.7039 | 0.8439 | 0.8351 | 0.8561 | 0.8599 | 0.8307 |
| Heilongjiang province | 0.7654 | 0.7226 | 0.8116 | 0.9497 | 0.9018 | 0.9802 | 0.9703 | 0.9652 |
| Shanghai | 0.5552 | 0.4871 | 0.4872 | 0.8900 | 0.8374 | 0.8634 | 0.8405 | 0.8029 |
| Jiangsu province | 0.9872 | 0.9929 | 0.8563 | 0.9711 | 0.8784 | 0.9306 | 0.8540 | 0.8634 |
| Zhejiang province | 0.9028 | 0.8992 | 0.8667 | 1 | 0.9411 | 0.9071 | 0.8888 | 0.8785 |
| Anhui province | 0.9500 | 0.9303 | 0.9711 | 1 | 1 | 1 | 1 | 0.9995 |
| Fujian province | 0.8759 | 0.8304 | 0.7831 | 0.8901 | 0.8263 | 0.8624 | 0.8648 | 0.9114 |
| Jiangxi province | 1 | 0.9493 | 0.9707 | 1 | 1 | 0.9796 | 1 | 1 |
| Shandong province | 0.7264 | 0.7447 | 0.7239 | 0.79457 | 0.8119 | 0.8636 | 0.8419 | 0.8292 |
| Henan province | 1 | 0.9951 | 1 | 1 | 1 | 1 | 1 | 1 |
| Hubei province | 0.9150 | 0.9211 | 0.8706 | 0.9150 | 0.8565 | 0.8603 | 1 | 0.8083 |
| Hunan province | 0.9360 | 0.9837 | 0.9650 | 0.9346 | 0.8889 | 0.9293 | 0.8639 | 1 |
| Guangdong province | 1 | 0.9333 | 0.7658 | 0.9993 | 0.9861 | 1 | 1 | 1 |
| Guangxi province | 1 | 0.9166 | 1 | 0.9899 | 0.9523 | 1 | 0.9893 | 0.9301 |
| Hainan province | 0.8138 | 0.8933 | 0.9076 | 1 | 1 | 1 | 0.9504 | 0.9365 |
| Chongqing | 0.9588 | 0.9108 | 0.9255 | 0.9552 | 0.9311 | 0.8825 | 0.8499 | 0.8194 |
| Sichuan province | 0.9780 | 0.9367 | 0.9085 | 0.9244 | 0.9243 | 0.9155 | 0.9219 | 0.9157 |
| Guizhou province | 1 | 1 | 1 | 1 | 0.9847 | 0.9268 | 0.9103 | 0.8819 |
| Yunnan province | 1 | 0.9291 | 0.8921 | 1 | 0.9356 | 1 | 0.9267 | 0.8809 |
| Shaanxi province | 0.7775 | 0.8582 | 0.7913 | 0.8367 | 0.7883 | 0.7839 | 0.7600 | 0.7573 |
| Gansu province | 0.9288 | 0.8701 | 0.8960 | 0.9547 | 0.9327 | 0.9639 | 0.9675 | 0.9120 |
| Qinghai province | 0.7128 | 0.7160 | 0.7590 | 0.9199 | 0.9391 | 0.7907 | 0.8004 | 0.7921 |
| Ningxia | 0.7406 | 0.7538 | 0.7986 | 0.9067 | 0.8420 | 0.8339 | 0.9190 | 0.7991 |
| Sinkiang | 0.6194 | 0.6066 | 0.5629 | 0.6719 | 0.6192 | 0.6360 | 0.6479 | 0.6538 |
| Degree of efficiency = 1 | 6 | 1 | 3 | 8 | 5 | 7 | 7 | 6 |
| Between mean and 1 | 10 | 17 | 12 | 9 | 11 | 11 | 13 | 9 |
| <Mean | 14 | 12 | 15 | 13 | 14 | 12 | 10 | 15 |
| mean | 0.8393 | 0.8237 | 0.8288 | 0.9312 | 0.9011 | 0.9066 | 0.9067 | 0.8880 |
| Maximum | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 1 |
| Minimum | 0.5552 | 0.4871 | 0.4872 | 0.6719 | 0.6192 | 0.6360 | 0.6479 | 0.6538 |
| standard deviation | 0.1431 | 0.1394 | 0.1329 | 0.0749 | 0.0846 | 0.0861 | 0.0863 | 0.0880 |
| Provinces | 2009 | 2010 | 2011 | 2012 | 2013 | 2014 | 2015 | 2016 |
|---|---|---|---|---|---|---|---|---|
| Beijing | 0.6151 | 0.6129 | 0.6800 | 0.8190 | 0.7385 | 0.8830 | 0.8774 | 0.8997 |
| Tianjin | 0.8634 | 0.8619 | 0.8549 | 0.8739 | 0.7881 | 0.9016 | 0.8840 | 0.9415 |
| Hebei province | 1 | 1 | 0.9653 | 0.9285 | 0.8457 | 0.9495 | 0.9401 | 0.9521 |
| Shanxi province | 0.8276 | 0.8629 | 0.7845 | 0.8058 | 0.7802 | 0.8051 | 0.8078 | 0.8315 |
| Inner Mongolia | 0.9367 | 0.9367 | 0.8606 | 0.8694 | 0.8440 | 0.8882 | 0.8658 | 0.8864 |
| Liaoning province | 0.8028 | 0.8045 | 0.7978 | 0.7961 | 0.7398 | 0.8105 | 0.8105 | 0.8318 |
| Jilin province | 0.9746 | 0.9805 | 0.9492 | 0.9193 | 0.8487 | 0.9241 | 0.9126 | 0.9392 |
| Heilongjiang province | 0.8664 | 0.8625 | 0.8060 | 0.8192 | 0.7771 | 0.7919 | 0.8188 | 0.8227 |
| Shanghai | 0.7568 | 0.7429 | 0.7986 | 0.8654 | 0.7837 | 0.8706 | 0.8625 | 0.9435 |
| Jiangsu province | 0.7290 | 0.7172 | 0.8213 | 0.8591 | 0.8315 | 0.8124 | 0.8753 | 0.8639 |
| Zhejiang province | 0.7633 | 0.7482 | 0.7872 | 0.8410 | 0.8045 | 0.8705 | 0.8589 | 0.8775 |
| Anhui province | 0.9951 | 0.9951 | 0.9565 | 0.9375 | 0.9241 | 0.9378 | 0.9455 | 0.9647 |
| Fujian province | 0.9592 | 0.9598 | 1 | 1 | 0.9720 | 1 | 1 | 1 |
| Jiangxi province | 1 | 1 | 0.9802 | 0.9459 | 0.9285 | 0.9557 | 0.9478 | 0.9457 |
| Shandong province | 0.9727 | 0.9278 | 0.9595 | 0.8898 | 0.8534 | 0.9080 | 0.9204 | 0.9502 |
| Henan province | 0.8743 | 0.8374 | 0.8586 | 0.8537 | 0.8509 | 0.8640 | 0.8457 | 0.8466 |
| Hubei province | 0.8886 | 0.8642 | 0.8686 | 0.8637 | 0.8501 | 0.8906 | 0.8487 | 0.8723 |
| Hunan province | 0.9434 | 0.9450 | 0.9226 | 0.9141 | 0.8943 | 0.9201 | 0.9142 | 0.7922 |
| Guangdong province | 0.7636 | 0.7832 | 0.9540 | 0.9430 | 0.9148 | 0.9410 | 0.9402 | 0.9306 |
| Guangxi province | 1 | 1 | 0.9884 | 0.9812 | 0.9198 | 0.9841 | 0.9979 | 1 |
| Hainan province | 1 | 1 | 0.9670 | 0.9462 | 0.9045 | 0.9582 | 0.9607 | 1 |
| Chongqing | 0.8997 | 0.8997 | 0.8882 | 0.8868 | 0.8589 | 0.9245 | 0.9385 | 0.9497 |
| Sichuan province | 0.8460 | 0.8430 | 0.8966 | 0.8570 | 0.8252 | 0.8752 | 0.8387 | 0.8374 |
| Guizhou province | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 0.9919 |
| Yunnan province | 0.9280 | 0.9163 | 0.9884 | 0.9376 | 0.9384 | 0.9384 | 0.9538 | 1 |
| Shaanxi province | 0.8964 | 0.8938 | 0.8625 | 0.8825 | 0.8699 | 0.9000 | 0.9206 | 0.9265 |
| Gansu province | 0.9487 | 0.9624 | 0.9280 | 0.8958 | 0.8763 | 0.8909 | 0.8805 | 0.9321 |
| Qinghai province | 1 | 1 | 1 | 1 | 1 | 0.8948 | 0.8984 | 0.9298 |
| Ningxia | 0.9426 | 0.9406 | 0.9067 | 0.8880 | 0.8476 | 0.8938 | 0.8223 | 0.9511 |
| Sinkiang | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 1 |
| Degree of efficiency = 1 | 7 | 7 | 4 | 4 | 3 | 3 | 3 | 5 |
| Between mean and 1 | 9 | 10 | 11 | 9 | 10 | 16 | 10 | 14 |
| <Mean | 14 | 13 | 15 | 17 | 17 | 11 | 17 | 11 |
| mean | 0.8998 | 0.8966 | 0.9010 | 0.9007 | 0.8670 | 0.9062 | 0.9029 | 0.9204 |
| Maximum | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 1 |
| Minimum | 0.6151 | 0.6129 | 0.6800 | 0.7961 | 0.7385 | 0.7919 | 0.8078 | 0.7922 |
| standard deviation | 0.1001 | 0.1013 | 0.0835 | 0.0597 | 0.0730 | 0.0563 | 0.0589 | 0.0610 |
| Parameter Regions | Coef. | Std. Error | p | 95% [Conf. Interval] | |
|---|---|---|---|---|---|
| Regions | 0.055156 | 0.010163 | 0.000 | 0.035237 | 0.075074 |
| Per capital GDP | −0.006501 | 0.005211 | 0.212 | −0.016714 | 0.003711 |
| Number of high education enrollment | −0.000070 | 0.000009 | 0.000 | −0.000087 | -0.000053 |
| Governmen health expenditure | 0.000821 | 0.000101 | 0.000 | 0.000624 | 0.001019 |
| Social health expenditure | −0.000233 | 0.000050 | 0.000 | −0.000330 | -0.000136 |
| Personal health expenditure | −0.000171 | 0.000087 | 0.050 | −0.000341 | 0.000000 |
| Number of public hospitals | −0.000212 | 0.000046 | 0.000 | −0.000301 | -0.000123 |
| Number of private hospitals | −0.000063 | 0.000033 | 0.057 | −0.000127 | 0.000002 |
| cons | 0.904079 | 0.029746 | 0.000 | 0.845779 | 0.962379 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Gong, G.; Chen, Y.; Gao, H.; Su, D.; Chang, J. Has the Efficiency of China’s Healthcare System Improved after Healthcare Reform? A Network Data Envelopment Analysis and Tobit Regression Approach. Int. J. Environ. Res. Public Health 2019, 16, 4847. https://doi.org/10.3390/ijerph16234847
Gong G, Chen Y, Gao H, Su D, Chang J. Has the Efficiency of China’s Healthcare System Improved after Healthcare Reform? A Network Data Envelopment Analysis and Tobit Regression Approach. International Journal of Environmental Research and Public Health. 2019; 16(23):4847. https://doi.org/10.3390/ijerph16234847
Chicago/Turabian StyleGong, Guangwen, Yingchun Chen, Hongxia Gao, Dai Su, and Jingjing Chang. 2019. "Has the Efficiency of China’s Healthcare System Improved after Healthcare Reform? A Network Data Envelopment Analysis and Tobit Regression Approach" International Journal of Environmental Research and Public Health 16, no. 23: 4847. https://doi.org/10.3390/ijerph16234847
APA StyleGong, G., Chen, Y., Gao, H., Su, D., & Chang, J. (2019). Has the Efficiency of China’s Healthcare System Improved after Healthcare Reform? A Network Data Envelopment Analysis and Tobit Regression Approach. International Journal of Environmental Research and Public Health, 16(23), 4847. https://doi.org/10.3390/ijerph16234847





