Heatwave Events and Mortality Outcomes in Memphis, Tennessee: Testing Effect Modification by Socioeconomic Status and Urbanicity
Abstract
1. Introduction
2. Methods
2.1. Study Period and Population
2.2. Data Sources
2.3. Statistical Analysis
3. Results
3.1. Daily Temperature Descriptive Statistics
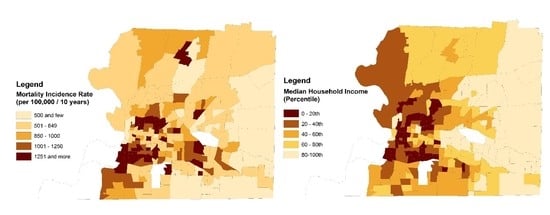
3.2. Descriptive Statistics of Mortality
3.2.1. Mortality Attributed to Exposure to Excessive Natural Heat (X30)
3.2.2. All-Cause, Cardiovascular Disease, and Respiratory Mortality
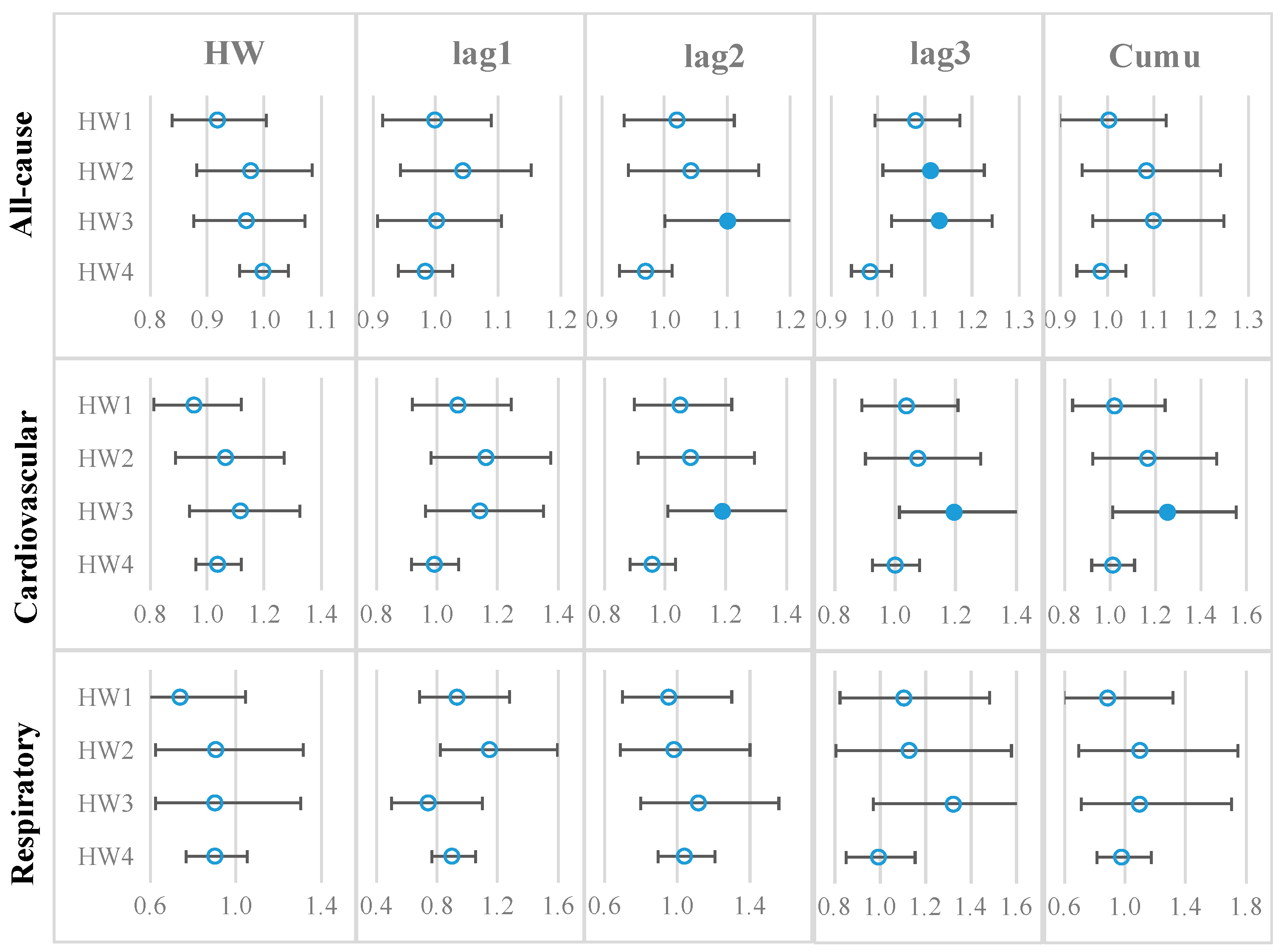
3.3. Association between Heatwaves and Mortality
3.4. Interactive Effects of Sociodemographic Variables and Urbanicity
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
References
- McGregor, G.R.; Bessemoulin, P.; Ebi, K.L.; Menne, B. Heatwaves and Health: Guidance on Warning-System Development; World Meteorological Organization: Geneva, Switzerland, 2015. [Google Scholar]
- Bridger, C.A.; Ellis, F.P.; Taylor, H.L. Mortality in St. Louis, Missouri, during heat waves in 1936, 1953, 1954, 1955, and 1966. Environ. Res. 1976, 12, 38–48. [Google Scholar] [CrossRef]
- Greenberg, J.H.; Bromberg, J.; Reed, C.M.; Gustafson, T.L.; Beauchamp, R.A. The epidemiology of heat-related deaths, Texas—1950, 1970–79, and 1980. Am. J. Public Health 1983, 73, 805–807. [Google Scholar] [CrossRef] [PubMed]
- Bark, N. Deaths of psychiatric patients during heat waves. Psychiatr. Serv. 1998, 49, 1088–1090. [Google Scholar] [CrossRef] [PubMed]
- Gasparrini, A.; Armstrong, B. The impact of heat waves on mortality. Epidemiology 2011, 22, 68–73. [Google Scholar] [CrossRef] [PubMed]
- Fowler, D.R.; Mitchell, C.S.; Brown, A.; Pollock, T.; Bratka, L.A.; Paulson, J.; Noller, A.C.; Mauskapf, R.; Oscanyan, K.; Vaidyanathan, A.; et al. Heat-Related Deaths After an Extreme Heat Event—Four States, 2012, and United States, 1999–2009. MMWR 2013, 62, 433–436. [Google Scholar]
- Allen, M.J.; Sheridan, S.C. Mortality risks during extreme temperature events (ETEs) using a distributed lag non-linear model. Int. J. Biometeorol. 2018, 62, 57–67. [Google Scholar] [CrossRef] [PubMed]
- Anderson, G.B.; Bell, M.L. Heat Waves in the United States: Mortality Risk during Heat Waves and Effect Modification by Heat Wave Characteristics in 43 U.S. Communities. Environ. Health Perspect. 2011, 119, 210–218. [Google Scholar] [CrossRef]
- Sheridan, S.C.; Lee, C.C.; Allen, M.J. The Mortality Response to Absolute and Relative Temperature Extremes. Int. J. Environ. Res. Public Health 2019, 16, 1493. [Google Scholar] [CrossRef]
- Chien, L.C.; Guo, Y.M.; Zhang, K. Spatiotemporal analysis of heat and heat wave effects on elderly mortality in Texas, 2006–2011. Sci. Total Environ. 2016, 562, 845–851. [Google Scholar] [CrossRef]
- Gronlund, C.J.; Berrocal, V.J.; White-Newsome, J.L.; Conlon, K.C.; O’Neill, M.S. Vulnerability to extreme heat by socio-demographic characteristics and area green space among the elderly in Michigan, 1990–2007. Environ. Res. 2015, 136, 449–461. [Google Scholar] [CrossRef]
- Semenza, J.C.; Rubin, C.H.; Falter, K.H.; Selanikio, J.D.; Flanders, W.D.; Howe, H.L.; Wilhelm, J.L. Heat-related deaths during the July 1995 heat wave in Chicago. N. Engl. J. Med. 1996, 335, 84–90. [Google Scholar] [CrossRef]
- Wainwright, S.H.; Buchanan, S.D.; Mainzer, M.; Parrish, R.G.; Sinks, T.H. Cardiovascular mortality—The hidden peril of heat waves. Prehosp. Disaster Med. 1999, 14, 18–27. [Google Scholar] [CrossRef]
- Peng, R.D.; Bobb, J.F.; Tebaldi, C.; McDaniel, L.; Bell, M.L.; Dominici, F. Toward a Quantitative Estimate of Future Heat Wave Mortality under Global Climate Change. Environ. Health Perspect. 2011, 119, 701–706. [Google Scholar] [CrossRef] [PubMed]
- Wu, J.; Zhou, Y.; Gao, Y.; Fu, J.S.; Johnson, B.A.; Huang, C.; Kim, Y.-M.; Liu, Y. Estimation and uncertainty analysis of impacts of future heat waves on mortality in the eastern United States. Environ. Health Perspect. 2014, 122, 10–16. [Google Scholar] [CrossRef]
- Applegate, W.B.; Runyan, J.W., Jr.; Brasfield, L.; Williams, M.L.; Konigsberg, C.; Fouche, C. Analysis of the 1980 heat wave in Memphis. J. Am. Geriatr. Soc. 1981, 29, 337–342. [Google Scholar] [CrossRef] [PubMed]
- Kaiser, R.; Le Tertre, A.; Schwartz, J.; Gotway, C.A.; Daley, W.R.; Rubin, C.H. The effect of the 1995 heat wave in Chicago on all-cause and cause-specific mortality. Am. J. Public Health 2007, 97, 158–162. [Google Scholar] [CrossRef] [PubMed]
- Madrigano, J.; Ito, K.; Johnson, S.; Kinney, P.L.; Matte, T. A case-only study of vulnerability to heat wave—Related mortality in New York City (2000–2011). Environ. Health Perspect. 2015, 123, 672–678. [Google Scholar] [CrossRef]
- Medina-Ramón, M.; Zanobetti, A.; Cavanagh, D.P.; Schwartz, J. Extreme temperatures and mortality: Assessing effect modification by personal characteristics and specific cause of death in a multi-city case-only analysis. Environ. Health Perspect. 2006, 114, 1331–1336. [Google Scholar] [CrossRef]
- Schuman, S.H. Patterns of urban heat-wave deaths and implications for prevention: Data from New York and St. Louis during July, 1966. Environ. Res. 1972, 5, 59–75. [Google Scholar] [CrossRef]
- Isaksen, T.B.; Fenske, R.A.; Hom, E.K.; Ren, Y.; Lyons, H.; Yost, M.G. Increased mortality associated with extreme-heat exposure in King County, Washington, 1980–2010. Int. J. Biometeorol. 2016, 60, 85–98. [Google Scholar] [CrossRef]
- U.S. Census Bureau. QuickFacts, Memphis City, Tennessee. Available online: https://www.census.gov/quickfacts/memphiscitytennessee (accessed on 10 September 2019).
- Shelby County Health Department. Community Health Improvement Plan; Shelby County Health Department: Memphis, TN, USA, 2015.
- Kent, S.T.; McClure, L.A.; Zaitchik, B.F.; Smith, T.T.; Gohlke, J.M. Heat Waves and Health Outcomes in Alabama (USA): The Importance of Heat Wave Definition. Environ. Health Perspect. 2014, 122, 151–158. [Google Scholar] [CrossRef] [PubMed]
- U.S. Census Bureau. Population in the U.S.—Shelby County. Available online: https://www.google.com/publicdata/explore?ds=kf7tgg1uo9ude_&met_y=population&idim=county:47157:47037&hl=en&dl=en#!ctype=l&strail=false&bcs=d&nselm=h&met_y=population&scale_y=lin&ind_y=false&rdim=country&idim=county:47157&ifdim=country&hl=en_US&dl=en&ind=false (accessed on 10 September 2019).
- Guo, Y.; Gasparrini, A.; Armstrong, B.G.; Tawatsupa, B.; Tobias, A.; Lavigne, E.; Zanotti Stagliorio Coelho, M.d.S.; Pan, X.; Kim, H.; Hashizume, M.; et al. Heat Wave and Mortality: A Multicountry, Multicommunity Study. Environ. Health Perspect. 2017, 125, 087006. [Google Scholar] [CrossRef] [PubMed]
- Anderson, B.G.; Bell, M.L. Weather-Related Mortality How Heat, Cold, and Heat Waves Affect Mortality in the United States. Epidemiology 2009, 20, 205–213. [Google Scholar] [CrossRef] [PubMed]
- Tan, J.; Zheng, Y.; Song, G.; Kalkstein, L.S.; Kalkstein, A.J.; Tang, X. Heat wave impacts on mortality in Shanghai, 1998 and 2003. Int. J. Biometeorol. 2007, 51, 193–200. [Google Scholar] [CrossRef] [PubMed]
- Yin, Q.; Wang, J. The association between consecutive days’ heat wave and cardiovascular disease mortality in Beijing, China. BMC Public Health 2017, 17, 223. [Google Scholar] [CrossRef] [PubMed]
- U.S. Census Bureau. 2010 Census Urban and Rural Classfication and Urban Area Criteria. Available online: https://www.census.gov/programs-surveys/geography/guidance/geo-areas/urban-rural/2010-urban-rural.html (accessed on 20 August 2019).
- U.S. Census Bureau. Income, Poverty and Health Insurance Coverage in the United States: 2010. Available online: https://www.census.gov/newsroom/releases/archives/income_wealth/cb11-157.html (accessed on 20 March 2019).
- Krewski, D.; Jerrett, M.; Burnett, R.T.; Ma, R.; Hughes, E.; Shi, Y.; Turner, M.C.; Pope, C.A.; Thurston, G.; Calle, E.E.; et al. Extended Follow-up and Spatial Analysis of the American Cancer Society Study Linking Particulate Air Pollution and Mortality; Research Report; Health Effects Institute: Boston, MA, USA, 2009; pp. 5–114; discussion 115–136. [Google Scholar]
- Bell, M.L.; Dominici, F.; Samet, J.M. A meta-analysis of time-series studies of ozone and mortality with comparison to the national morbidity, mortality, and air pollution study. Epidemiology 2005, 16, 436–445. [Google Scholar] [CrossRef]
- Faustini, A.; Rapp, R.; Forastiere, F. Nitrogen dioxide and mortality: Review and meta-analysis of long-term studies. Eur. Respir. J. 2014, 44, 744–753. [Google Scholar] [CrossRef]
- Basu, R. High ambient temperature and mortality: A review of epidemiologic studies from 2001 to 2008. Environ. Health 2009, 8, 40. [Google Scholar] [CrossRef]
- Jia, C.; James, W.; Kedia, S. Relationship of Racial Composition and Cancer Risks from Air Toxics Exposure in Memphis, Tennessee, USA. Int. J. Environ. Res. Public Health 2014, 11, 7713–7724. [Google Scholar] [CrossRef]
- Madrigano, J.; Jack, D.; Anderson, G.B.; Bell, M.L.; Kinney, P.L. Temperature, ozone, and mortality in urban and non-urban counties in the northeastern United States. Environ. Health 2015, 14, 3. [Google Scholar] [CrossRef]
- U.S. EPA. Air Data: Air Quality Data Collected at Outdoor Monitors Across the US. Available online: https://aqs.epa.gov/api (accessed on 12 April 2019).
- Gasparrini, A. Modeling exposure-lag-response associations with distributed lag non-linear models. Stat. Med. 2014, 33, 900. [Google Scholar] [CrossRef]
- Chen, K.; Bi, J.; Chen, J.; Chen, X.; Huang, L.; Zhou, L. Influence of heat wave definitions to the added effect of heat waves on daily mortality in Nanjing, China. Sci. Total Environ. 2015, 506, 18–25. [Google Scholar] [CrossRef] [PubMed]
- Vaidyanathan, A.; Saha, S.; Vicedo-Cabrera, A.M.; Gasparrini, A.; Abdurehman, N.; Jordan, R.; Hawkins, M.; Hess, J.; Elixhauser, A. Assessment of extreme heat and hospitalizations to inform early warning systems. Proc. Natl. Acad. Sci. USA 2019, 116, 5420–5427. [Google Scholar] [CrossRef] [PubMed]
- Gasparrini, A. Distributed Lag Linear and Non-Linear Models in R: The Package dlnm. J. Stat. Softw. 2011, 43, 1–20. [Google Scholar] [CrossRef] [PubMed]
- Armstrong, B.; Sera, F.; Vicedo-Cabrera Ana, M.; Abrutzky, R.; Åström Daniel, O.; Bell Michelle, L.; Chen, B.-Y.; de Sousa Zanotti Stagliorio Coelho, M.; Correa Patricia, M.; Dang Tran, N.; et al. The Role of Humidity in Associations of High Temperature with Mortality: A Multiauthor, Multicity Study. Environ. Health Perspect. 2019, 127, 097007. [Google Scholar] [CrossRef] [PubMed]
- Xu, Z.; FitzGerald, G.; Guo, Y.; Jalaludin, B.; Tong, S. Impact of heatwave on mortality under different heatwave definitions: A systematic review and meta-analysis. Environ. Int. 2016, 89, 193–203. [Google Scholar] [CrossRef] [PubMed]
- D’Ippoliti, D.; Michelozzi, P.; Marino, C.; de’Donato, F.; Menne, B.; Katsouyanni, K.; Kirchmayer, U.; Analitis, A.; Medina-Ramon, M.; Paldy, A.; et al. The impact of heat waves on mortality in 9 European cities: Results from the EuroHEAT project. Environ. Health 2010, 9, 37. [Google Scholar] [CrossRef]
- Arbuthnott, K.G.; Hajat, S. The health effects of hotter summers and heat waves in the population of the United Kingdom: A review of the evidence. Environ. Health 2017, 16, 1–13. [Google Scholar] [CrossRef]
- Ma, W.J.; Zeng, W.L.; Zhou, M.G.; Wang, L.J.; Rutherford, S.; Lin, H.L.; Liu, T.; Zhang, Y.H.; Xiao, J.P.; Zhang, Y.W.; et al. The short-term effect of heat waves on mortality and its modifiers in China: An analysis from 66 communities. Environ. Int. 2015, 75, 103–109. [Google Scholar] [CrossRef]
- Oyana, T.J.; Podila, P.; Wesley, J.M.; Lomnicki, S.; Cormier, S. Spatiotemporal patterns of childhood asthma hospitalization and utilization in Memphis Metropolitan Area from 2005 to 2015. J. Asthma 2017, 54, 842–855. [Google Scholar] [CrossRef]
- Shin, E.K.; Shaban-Nejad, A. Urban Decay and Pediatric Asthma Prevalence in Memphis, Tennessee: Urban Data Integration for Efficient Population Health Surveillance. IEEE Access 2018, 6, 46281–46289. [Google Scholar] [CrossRef]
- Bell, M.L.; McDermott, A.; Zeger, S.L.; Samet, J.M.; Dominici, F. Ozone and short-term mortality in 95 US urban communities, 1987–2000. JAMA 2004, 292, 2372–2378. [Google Scholar] [CrossRef] [PubMed]
- Ramlow, J.M.; Kuller, L.H. Effects of the summer heat wave of 1988 on daily mortality in Allegheny County, PA. Public Health Rep. 1990, 105, 283. [Google Scholar] [PubMed]
- Kovach, M.M.; Konrad, C.E.; Fuhrmann, C.M. Area-level risk factors for heat-related illness in rural and urban locations across North Carolina, USA. Appl. Geogr. 2015, 60, 175–183. [Google Scholar] [CrossRef]
- Li, M.; Shaw, B.A.; Zhang, W.; Vásquez, E.; Lin, S. Impact of Extremely Hot Days on Emergency Department Visits for Cardiovascular Disease among Older Adults in New York State. Int. J. Environ. Res. Public Health 2019, 16, 2119. [Google Scholar] [CrossRef]
| Heatwave Abbreviation | Definition | Reference | Total HW Days |
|---|---|---|---|
| HW1 | Minimum daily temperature >95th percentile for ≥2 consecutive days 1 | Anderson and Bell 2011 [8] | 45 |
| HW2 | Mean daily temperature >95th percentile for ≥2 consecutive days | Anderson and Bell 2011 [8] | 32 |
| HW3 | Maximum daily temperature >95th percentile for ≥2 consecutive days | Anderson and Bell 2011 [8] | 35 |
| HW4 | Maximum daily temperature >35 °C (95 °F) for ≥1 day | Tan et al. 2007 [28] | 215 |
| Descriptive Statistics | Daily Temperature Metric (°F) | ||
|---|---|---|---|
| Maximum | Minimum | Average | |
| Mean | 88.1 | 69.8 | 78.9 |
| Maximum | 106 | 84 | 94.5 |
| Minimum | 58 | 36 | 47 |
| 95th percentile | 98 | 79 | 88 |
| 99th percentile | 100 | 81 | 90 |
| All-Cause Mortality | Cardiovascular Morality | Respiratory Mortality | |||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Total | HW1 | HW2 | HW3 | HW4 | Total | HW1 | HW2 | HW3 | HW4 | Total | HW1 | HW2 | HW3 | HW4 | |
| Total | 17,935 | 486 | 371 | 400 | 2530 | 6081 | 171 | 137 | 150 | 882 | 1673 | 38 | 34 | 36 | 223 |
| Age | |||||||||||||||
| Age 65–79 | 7948 | 228 | 164 | 181 | 1116 | 2446 | 73 | 58 | 57 | 337 | 748 | 16 | 15 | 19 | 109 |
| Age 80+ | 9987 | 258 | 207 | 219 | 1414 | 3635 | 98 | 79 | 93 | 545 | 925 | 22 | 19 | 17 | 114 |
| Poverty | |||||||||||||||
| Low | 9072 | 252 | 186 | 214 | 1280 | 3192 | 85 | 65 | 81 | 467 | 782 | 21 | 18 | 19 | 96 |
| High | 8863 | 234 | 185 | 186 | 1250 | 2889 | 86 | 72 | 69 | 415 | 891 | 17 | 16 | 17 | 127 |
| Urbanicity | |||||||||||||||
| Rural | 1573 | 35 | 28 | 33 | 221 | 493 | 13 | 9 | 8 | 69 | 179 | 2 | 3 | 4 | 29 |
| Urban | 16,362 | 451 | 343 | 367 | 2309 | 5588 | 158 | 128 | 142 | 813 | 1494 | 36 | 31 | 32 | 194 |
| Gender | |||||||||||||||
| Female | 7883 | 216 | 211 | 179 | 1095 | 2698 | 76 | 60 | 65 | 375 | 775 | 16 | 16 | 18 | 94 |
| Male | 10,051 | 270 | 160 | 221 | 1435 | 3382 | 95 | 77 | 85 | 507 | 898 | 22 | 18 | 18 | 129 |
| Race | |||||||||||||||
| Black | 10,202 | 265 | 200 | 235 | 1,454 | 3359 | 92 | 78 | 88 | 501 | 1136 | 26 | 20 | 25 | 165 |
| White | 7529 | 217 | 168 | 162 | 1055 | 2645 | 77 | 59 | 60 | 374 | 521 | 11 | 14 | 11 | 54 |
| Other | 204 | 4 | 3 | 3 | 21 | 77 | 2 | 0 | 2 | 7 | 16 | 1 | 0 | 0 | 4 |
| All-Cause | Age | p | Poverty | p | Urban | p | Sex | p | Race | p |
|---|---|---|---|---|---|---|---|---|---|---|
| HW1 | −0.109 | 0.249 | −0.054 | 0.562 | 0.221 | 0.229 | −0.020 | 0.828 | 0.109 | 0.204 |
| HW2 | 0.003 | 0.978 | 0.016 | 0.879 | 0.168 | 0.413 | 0.034 | 0.749 | 0.134 | 0.169 |
| HW3 | −0.040 | 0.701 | −0.122 | 0.239 | 0.069 | 0.715 | −0.033 | 0.750 | −0.068 | 0.473 |
| HW4 | 0.008 | 0.858 | −0.003 | 0.950 | 0.006 | 0.936 | 0.032 | 0.467 | −0.018 | 0.654 |
| Cardiovascular | ||||||||||
| HW1 | −0.103 | 0.542 | 0.113 | 0.497 | 0.065 | 0.820 | 0.001 | 0.995 | 0.060 | 0.677 |
| HW2 | −0.087 | 0.642 | 0.205 | 0.268 | 0.225 | 0.509 | 0.028 | 0.881 | −0.044 | 0.786 |
| HW3 | 0.098 | 0.594 | −0.064 | 0.716 | 0.452 | 0.208 | 0.047 | 0.791 | −0.150 | 0.337 |
| HW4 | 0.101 | 0.209 | −0.024 | 0.758 | 0.038 | 0.776 | 0.093 | 0.238 | −0.065 | 0.337 |
| Respiratory | ||||||||||
| HW1 | 0.111 | 0.742 | −0.350 | 0.295 | 0.784 | 0.237 | 0.173 | 0.608 | −0.080 | 0.791 |
| HW2 | 0.027 | 0.940 | −0.253 | 0.471 | 0.220 | 0.691 | −0.033 | 0.926 | 0.435 | 0.137 |
| HW3 | −0.329 | 0.336 | −0.247 | 0.470 | −0.041 | 0.933 | −0.153 | 0.654 | −0.040 | 0.896 |
| HW4 | −0.192 | 0.189 | 0.173 | 0.240 | −0.256 | 0.193 | 0.193 | 0.192 | −0.383 | 0.006 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Li, Y.; Akkus, C.; Yu, X.; Joyner, A.; Kmet, J.; Sweat, D.; Jia, C. Heatwave Events and Mortality Outcomes in Memphis, Tennessee: Testing Effect Modification by Socioeconomic Status and Urbanicity. Int. J. Environ. Res. Public Health 2019, 16, 4568. https://doi.org/10.3390/ijerph16224568
Li Y, Akkus C, Yu X, Joyner A, Kmet J, Sweat D, Jia C. Heatwave Events and Mortality Outcomes in Memphis, Tennessee: Testing Effect Modification by Socioeconomic Status and Urbanicity. International Journal of Environmental Research and Public Health. 2019; 16(22):4568. https://doi.org/10.3390/ijerph16224568
Chicago/Turabian StyleLi, Ying, Cem Akkus, Xinhua Yu, Andrew Joyner, Jennifer Kmet, David Sweat, and Chunrong Jia. 2019. "Heatwave Events and Mortality Outcomes in Memphis, Tennessee: Testing Effect Modification by Socioeconomic Status and Urbanicity" International Journal of Environmental Research and Public Health 16, no. 22: 4568. https://doi.org/10.3390/ijerph16224568
APA StyleLi, Y., Akkus, C., Yu, X., Joyner, A., Kmet, J., Sweat, D., & Jia, C. (2019). Heatwave Events and Mortality Outcomes in Memphis, Tennessee: Testing Effect Modification by Socioeconomic Status and Urbanicity. International Journal of Environmental Research and Public Health, 16(22), 4568. https://doi.org/10.3390/ijerph16224568