Adapting Digital Social Prescribing for Suicide Bereavement Support: The Findings of a Consultation Exercise to Explore the Acceptability of Implementing Digital Social Prescribing within an Existing Postvention Service
Abstract
:1. Introduction
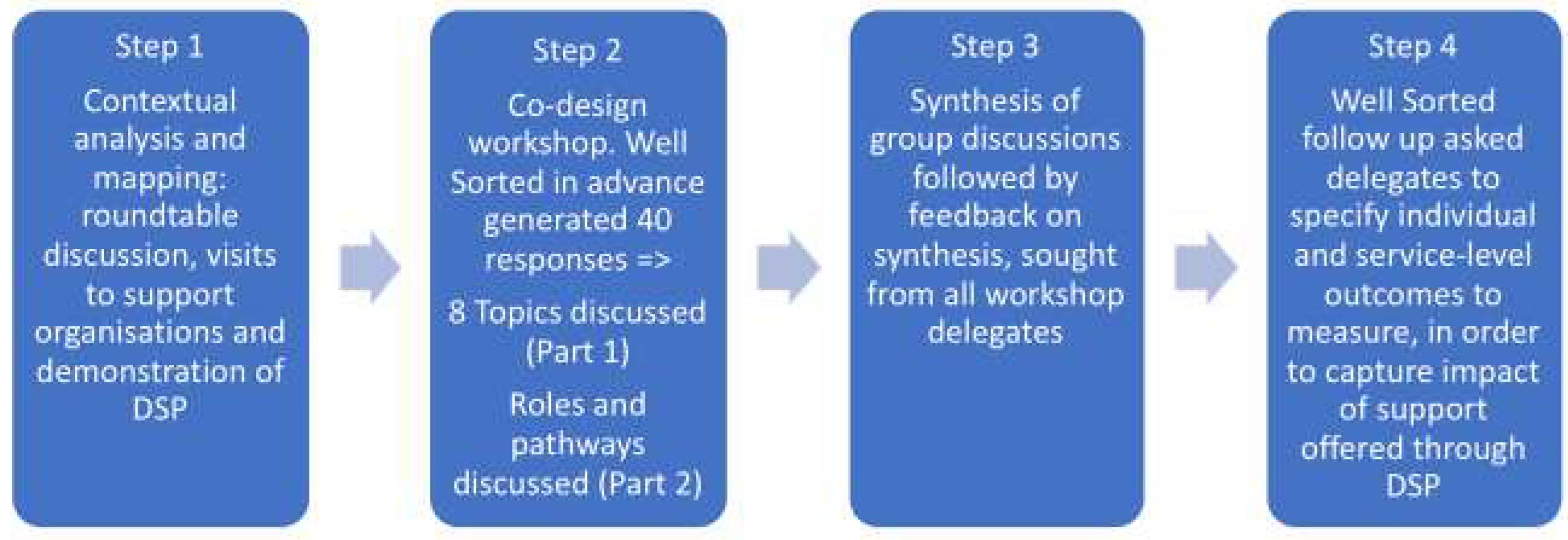
2. Materials and Methods
Statement on Ethics
3. Results
3.1. Step One
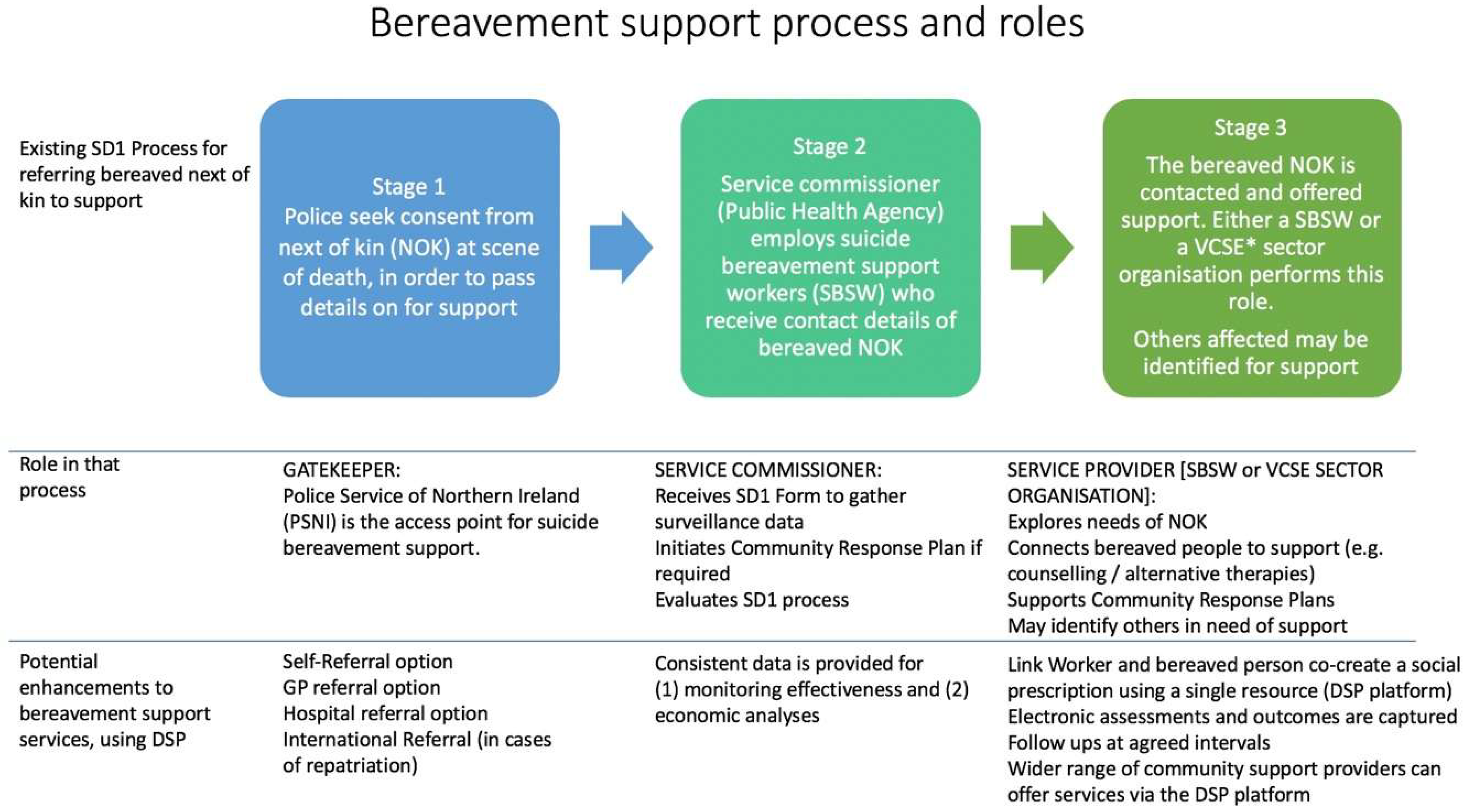
3.2. Step Two
3.3. Step Three
3.3.1. Addressing the Stigma of Suicide Bereavement and Impact on Help-Seeking
3.3.2. Reluctance to Access Support
3.3.3. Was It Accidental Death due to Drugs/Alcohol or Was It Suicide?
3.3.4. The Impact on Wider Communities
3.3.5. Supporting Those Beyond the Next of Kin
3.3.6. Matching Types of Support to Needs
3.3.7. Does the Term Digital Put People off?
3.3.8. Timing of Service Provision (in Relation to Loss)
3.4. Step Four
4. Discussion
4.1. Ethical Challenges Identified
4.2. Limitations
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- The King’s Fund. What Is Social Prescribing? Available online: https://www.kingsfund.org.uk/publications/social-prescribing (accessed on 26 November 2017).
- Andriessen, K.; Krysinska, K.; Hill, N.T.; Reifels, L.; Robinson, J.; Reavley, N.; Pirkis, J. Effectiveness of interventions for people bereaved through suicide: A systematic review of controlled studies of grief, psychosocial and suicide-related outcomes. BMC Psychiatry 2019, 19, 49. [Google Scholar] [CrossRef]
- Centres for Disease Control and Protection. Suicide: Risk and Protective Factors. 2019. Available online: https://www.cdc.gov/violenceprevention/suicide/riskprotectivefactors.html (accessed on 13 March 2019).
- Erlangsen, A.; Runeson, B.; Bolton, J.M.; Wilcox, H.C.; Forman, J.L.; Krogh, J.; Shear, M.K.; Nordentoft, M.; Conwell, Y. Association between spousal suicide and mental, physical, and social health outcomes a longitudinal and nationwide register-based study. JAMA Psychiatry 2017, 74, 456–464. [Google Scholar] [CrossRef]
- Pitman, A.L.; Osborn, D.P.J.; Rantell, K.; King, M.B. Bereavement by suicide as a risk factor for suicide attempt: A cross-sectional national UK-wide study of 3432 young bereaved adults. BMJ Open 2016, 6, e009948. [Google Scholar] [CrossRef]
- Berman, A.L. Estimating the population of survivors of suicide: Seeking an evidence base. Suicide Life-Threat. Behav. 2011, 41, 110–116. [Google Scholar] [CrossRef]
- Cerel, J.; Brown, M.M.; Maple, M.; Singleton, M.; van de Venne, J.; Moore, M.; Flaherty, C. How Many People Are Exposed to Suicide? Not Six. Suicide Life-Threat. Behav. 2019, 49, 529–534. [Google Scholar] [CrossRef]
- Pitman, A.; Osborn, D.; King, M.; Erlangsen, A. Effects of suicide bereavement on mental health and suicide risk. Lancet Psychiatry 2014, 1, 86–94. [Google Scholar] [CrossRef]
- Maple, M.; Cerel, J.; Jordan, J.; McKay, K. Uncovering and Identifying the Missing Voices in Suicide Bereavement. Suicidol. Online 2014, 5, 1–12. [Google Scholar]
- Mallon, S.; Galway, K. Towards an Understanding of the Role of Bereavement in the Pathway to Suicide; Knowledge Exchange Seminar Series (KESS); Northern Ireland Assembly: Belfast, UK, 2015.
- Young, I.T.; Iglewicz, A.; Glorioso, D.; Lanouette, N.; Seay, K.; Ilapakurti, M.; Zisook, S. Suicide bereavement and complicated grief. Dialogues Clin. Neurosci. 2012, 14, 177–186. [Google Scholar]
- ONS. Suicides in the UK. 2019. Available online: https://www.ons.gov.uk/peoplepopulationandcommunity/birthsdeathsandmarriages/deaths/datasets/suicidesintheunitedkingdomreferencetables (accessed on 27 August 2019).
- Andriessen, K.; Rahman, B.; Draper, B.; Dudley, M.; Mitchell, P.B. Prevalence of exposure to suicide: A meta-analysis of population-based studies. J. Psychiatry Res. 2017, 88, 113–120. [Google Scholar] [CrossRef]
- Bolton, J.M.; Au, W.; Leslie, W.D.; Martens, P.J.; Enns, M.W.; Roos, L.L.; Katz, L.Y.; Wilcox, H.C.; Erlangsen, A.; Chateau, D.; et al. Parents bereaved by offspring suicide: A population-based longitudinal case-control study. JAMA Psychiatry 2013, 70, 158–167. [Google Scholar] [CrossRef]
- Pitman, A.L.; Rantell, K.; Moran, P.; Sireling, L.; Marston, L.; King, M.; Osborn, D. Support received after bereavement by suicide and other sudden deaths: A cross-sectional UK study of 3432 young bereaved adults. BMJ Open 2017, 7, e014487. [Google Scholar] [CrossRef]
- Leavey, G.; Mallon, S.; Rondon-Sulbaran, J.; Galway, K.; Rosato, M.; Hughes, L. The failure of suicide prevention in primary care: family and GP perspectives–a qualitative study. BMC Psychiatry 2017, 17, 369. [Google Scholar] [CrossRef]
- Leavey, G.; Galway, K.; Hughes, L.; Mallon, S.; Sulbarán, J.R.; Rosato, M. Understanding Suicide and Help-Seeking in Urban and Rural Areas in Northern Ireland; Bamford Centre for Mental Health and Wellbeing, Ulster University: Belfast, UK, 2016. [Google Scholar]
- World Health Organisation. National Suicide Prevention Strategies Progress, Examples and Indicators; World Health Organisation: Geneva, Switzerland, 2018. [Google Scholar]
- McLean, J.; Maxwell, M.; Platt, S.; Harris, F.; Jepson, R. Risk and Protective Factors for Suicide and Suicidal Behaviour: A Literature Review; Scottish Government Social Research: Edinburgh, UK, 2008.
- Pitman, A.; Rantell, K.; Marston, L.; King, M.; Osborn, D. Perceived stigma of sudden bereavement as a risk factor for suicidal thoughts and suicide attempt: Analysis of British cross-sectional survey data on 3387 young bereaved adults. Int. J. Environ. Res. Public Health 2017, 14, 286. [Google Scholar] [CrossRef]
- Kinchin, I.; Doran, C.M. The cost of youth suicide in Australia. Int. J. Environ. Res. Public Health 2018, 15, 672. [Google Scholar] [CrossRef]
- Wilson, P.; Booth, A. Evidence to inform commissioners on social prescribing. Center for Reviews and Dissemination. 2015. Available online: https://www.york.ac.uk/media/crd/Ev%20briefing_social_prescribing.pdf (accessed on 14 November 2019).
- Maughan, D.L.; Patel, A.; Parveen, T.; Braithwaite, I.; Cook, J.; Lillywhite, R.; Cooke, M. Primary-care-based social prescribing for mental health: An analysis of financial and environmental sustainability. Prim. Heal. Care Res. Dev. 2016, 17, 114–121. [Google Scholar] [CrossRef]
- National Health Service. NHS Long Term Plan. 2019. Available online: https://www.longtermplan.nhs.uk/ (accessed on 13 March 2019).
- Millman, C.; McAnuff, A. Evaluation of the SD1 and CRP Processes in Northern Ireland as a Response to Suspected Suicide; Public Health Agency for Northern Ireland: Belfast, UK, 2018. [Google Scholar]
- Andriessen, K.; Dransart, D.A.C.; Cerel, J.; Maple, M. Current postvention research and priorities for the future: Results of a Survey. Crisis 2017, 38, 202–206. [Google Scholar] [CrossRef]
- Craig, P.; Dieppe, P.; Macintyre, S.; Michie, S.; Nazareth, I.; Petticrew, M. Developing and evaluating complex interventions: New guidance. BMJ 2008, 337, a1655. [Google Scholar] [CrossRef]
- Santin, O.; McShane, T.; Hudson, P.; Prue, G. Using a six-step co-design model to develop and test a peer-led web-based resource (PLWR) to support informal carers of cancer patients. Psycho-Oncology 2018, 28, 518–524. [Google Scholar] [CrossRef]
- Rycroft-Malone, J.; Harvey, G.; Seers, K.; Kitson, A.; McCormack, B.; Titchen, A. An exploration of the factors that influence the implementation of evidence into practice. J. Clin. Nurs. 2004, 13, 913–924. [Google Scholar] [CrossRef]
- NIHR Involve, Budgeting for Involvement: June 2013. Available online: https://www.invo.org.uk/posttypepublication/budgeting-for-involvement/ (accessed on 4 November 2019).
- Kitson, A.L.; Rycroft-Malone, J.; Harvey, G.; McCormack, B.; Seers, K.; Titchen, A. Evaluating the successful implementation of evidence into practice using the PARiHS framework: Theoretical and practical challenges. Implement. Sci. 2008, 3, 1. [Google Scholar] [CrossRef]
- Pescheny, J.V.; Pappas, Y.; Randhawa, G. Facilitators and barriers of implementing and delivering social prescribing services: A systematic review. BMC Health Serv. Res. 2018, 18, 86. [Google Scholar] [CrossRef]
- Methven, T.S.; Padilla, S.; Corne, D.W.; Chantler, M.J. Research strategy generation: Avoiding academic “animal farm”. In Proceedings of the Companion Publication of the 17th ACM Conference on Computer Supported Cooperative Work & Social Computing; ACM: New York, NY, USA, 2014; pp. 25–28. [Google Scholar]
- Health Research Authority. Decision Tool. Available online: http://www.hra-decisiontools.org.uk/research/index.html (accessed on 5 March 2018).
- Stetler, C.B.; Legro, M.W.; Rycroft-Malone, J.; Bowman, C.; Curran, G.; Guihan, M.; Wallace, C.M. Role of" external facilitation" in implementation of research findings: a qualitative evaluation of facilitation experiences in the Veterans Health Administration. Implement. Sci. 2006, 1, 23. [Google Scholar] [CrossRef]
| Priority Identified | Discussions and Potential Solutions |
|---|---|
| The stigma of suicide bereavement | DSP offers a potential solution for overcoming the stigma of suicide bereavement by providing connectivity and a safe, knowledge-based support system through personal empowerment via the range of support that could be offered. |
| Reluctance to access support | Educating people about vulnerabilities and how to address them could ease the stigma around seeking support. |
| Was it accidental death due to drugs/alcohol or was it suicide? | The sensitivities around suicide deaths involving drugs and/or alcohol misuse, and also acceptance of the term ‘suicide’, requires language consideration within any system of support. ‘Traumatic death’ is more sensitive than ‘suicide’. |
| The impact on wider communities | Distinguish between post-suicide activities that carry a risk of leading to heightened emotions versus those that are useful for raising awareness. To counter any negative impact, there needs to be wider roll-out and publicity of support services. Future development of the digital solution could also include self-referral. |
| Supporting those beyond next of kin | There is a need to develop more effective means of identifying and supporting those beyond the next of kin. See also: Reluctance to Access Support and Impact on Wider Communities. |
| Matching types of support to needs | Gaps in provision should be identified. Consider links with Coroners’ services. |
| Does the term ‘digital’ put people off? | Capacity building for using a digital social prescribing platform should be offered through software training. Use of champions models to cascade awareness and training could assist with changing the management process. |
| Timing of service provision (in relation to loss) | The bereaved clients could be followed up at different stages post bereavement; support should be tailored to the needs of the individual; initially focusing on practical hurdles, later providing emotional support options. |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Galway, K.; Forbes, T.; Mallon, S.; Santin, O.; Best, P.; Neff, J.; Leavey, G.; Pitman, A. Adapting Digital Social Prescribing for Suicide Bereavement Support: The Findings of a Consultation Exercise to Explore the Acceptability of Implementing Digital Social Prescribing within an Existing Postvention Service. Int. J. Environ. Res. Public Health 2019, 16, 4561. https://doi.org/10.3390/ijerph16224561
Galway K, Forbes T, Mallon S, Santin O, Best P, Neff J, Leavey G, Pitman A. Adapting Digital Social Prescribing for Suicide Bereavement Support: The Findings of a Consultation Exercise to Explore the Acceptability of Implementing Digital Social Prescribing within an Existing Postvention Service. International Journal of Environmental Research and Public Health. 2019; 16(22):4561. https://doi.org/10.3390/ijerph16224561
Chicago/Turabian StyleGalway, Karen, Trisha Forbes, Sharon Mallon, Olinda Santin, Paul Best, Jennifer Neff, Gerry Leavey, and Alexandra Pitman. 2019. "Adapting Digital Social Prescribing for Suicide Bereavement Support: The Findings of a Consultation Exercise to Explore the Acceptability of Implementing Digital Social Prescribing within an Existing Postvention Service" International Journal of Environmental Research and Public Health 16, no. 22: 4561. https://doi.org/10.3390/ijerph16224561
APA StyleGalway, K., Forbes, T., Mallon, S., Santin, O., Best, P., Neff, J., Leavey, G., & Pitman, A. (2019). Adapting Digital Social Prescribing for Suicide Bereavement Support: The Findings of a Consultation Exercise to Explore the Acceptability of Implementing Digital Social Prescribing within an Existing Postvention Service. International Journal of Environmental Research and Public Health, 16(22), 4561. https://doi.org/10.3390/ijerph16224561






