Facebook Groups on Chronic Obstructive Pulmonary Disease: Social Media Content Analysis
Abstract
1. Introduction
2. Materials and Methods
2.1. Theoretical Framework
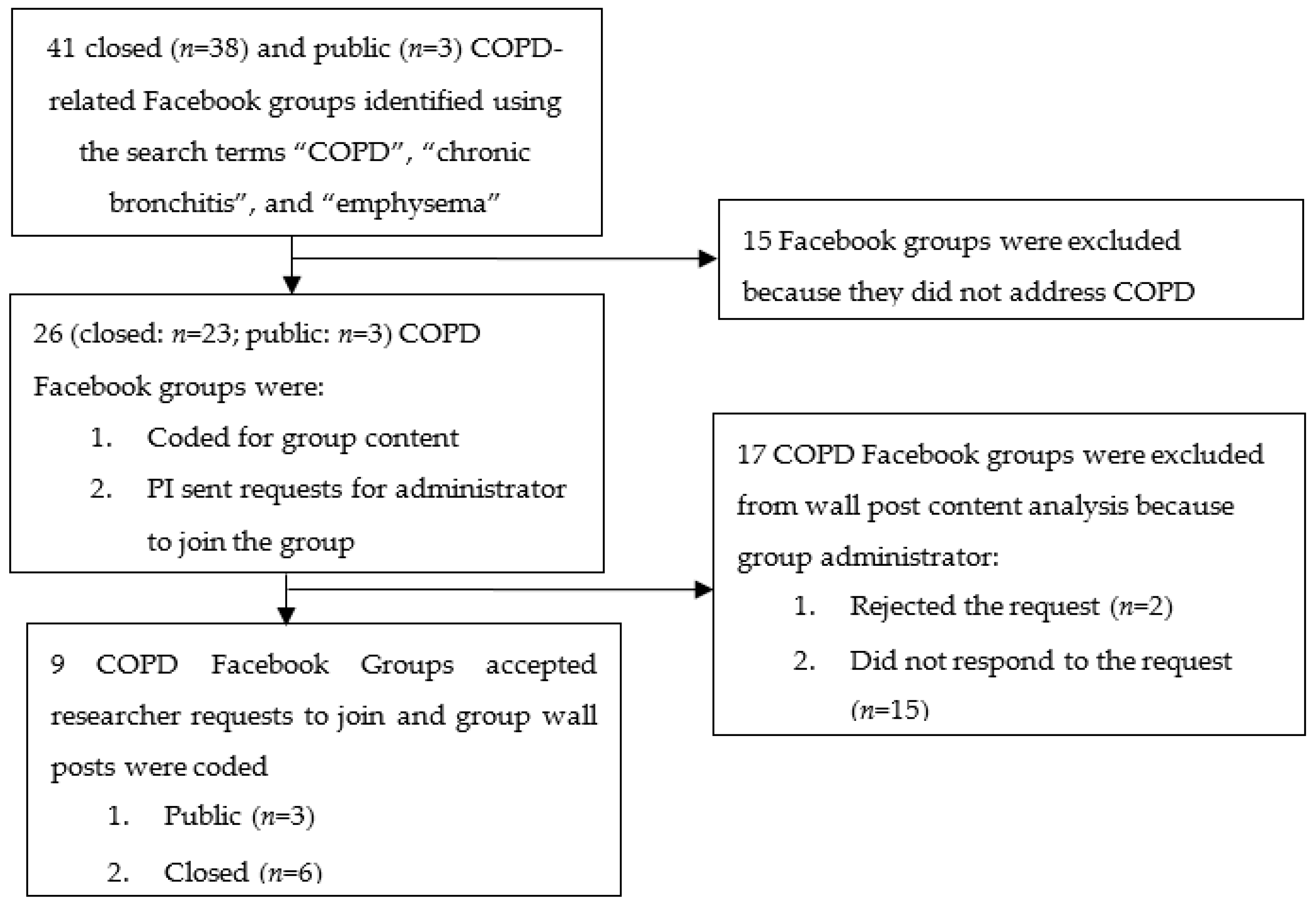
2.2. Search Procedures
2.3. Inclusion/Exclusion Criteria
2.4. Data Collection
2.5. Measures
2.6. Coder Training
2.7. Data Analysis
3. Results
3.1. Data Reliability
3.2. Group Characteristics
3.3. Group Size
3.4. Wall Post Content and Characteristics
3.5. Group Wall Post Engagement
3.6. Wall Post Communication Strategy and Self-Management
3.6.1. Wall Post Communication Strategy and Medication Management
3.6.2. Wall Post Communication Strategy and Hospitalizations/Doctor Visits
3.7. Engagement with COPD Wall Posts according to Communication Strategy
4. Discussion
Limitations
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Centers for Disease Control and Prevention. Chronic Obstructive Pulmonary Disease. 2017. Available online: https://www.cdc.gov/copd/index.html (accessed on 5 July 2019).
- American Lung Association. What is COPD? Available online: http://www.lung.org/lung-health-and-diseases/lung-disease-lookup/copd/learn-about-copd/what-is-copd.html (accessed on 5 July 2019).
- COPD Foundation. Is COPD the Third of Fourth Leading Cause of Death? Available online: https://www.copdfoundation.org/COPD360social/Community/COPD-Digest/Article/1399/Is-COPD-the-Third-or-Fourth-Leading-Cause-of-Death.aspx (accessed on 5 July 2019).
- Rabe, K.; Watz, H. Chronic obstructive pulmonary disease. Lancet 2017, 389, 1931–1940. [Google Scholar] [CrossRef]
- National Heart, Lung and Blood Institute. What is COPD? Available online: https://www.nhlbi.nih.gov/health/health-topics/topics/copd/# (accessed on 5 July 2019).
- National Institutes of Health. Chronic Obstructive Pulmonary Disease (COPD). 2013. Available online: https://report.nih.gov/nihfactsheets/ViewFactSheet.aspx?csid=77&key=C#C (accessed on 5 July 2019).
- Lamprecht, B.; Soriano, J.; Studnicka, M.; Kaiser, B.; Vanfleteren, L.; Gnatiuc, L.; Burney, P.; Miravitlles, M. Determinants of underdiagnosis of COPD in national and international surveys. Chest 2015, 148, 971–985. [Google Scholar] [CrossRef] [PubMed]
- Sobnath, D.D.; Philip, N.; Kayyali, R.; Nabhani-Gebara, S.; Pierscionek, B.; Vaes, A.W.; Spruit, M.A.; Kaimakamis, E. Features of a mobile support app for patients with chronic obstructive pulmonary disease: Literature review and current applications. JMIR 2017, 5. [Google Scholar] [CrossRef] [PubMed]
- Koutnik-Fotopoulos, E. COPD: Challenges and Consequences for Stakeholders. Available online: https://www.managedhealthcareconnect.com/article/copd-challenges-and-consequences-stakeholders (accessed on 5 July 2019).
- Ford, E.; Murphy, L.; Khavjou, O.; Giles, W.; Holt, J.; Croft, J. Total and state-specific medical and absenteeism costs of COPD among adults aged 18 years in the United States for 2010 and projections through 2020. Chest 2015, 147, 31–45. [Google Scholar] [CrossRef] [PubMed]
- American Thoracic Society. Exacerbation of COPD. Am. J. Respir. Crit. Care Med. 2014, 189, 11–12. [Google Scholar] [CrossRef] [PubMed]
- Wier, L.M.; Elixhauser, A.; Pfuntner, A.; Au, D.H. Agency for Healthcare Research and Quality. Overview of Hospitalizations among Patients with COPD, 2008. HCUP Statistical Brief #106. Agency for Healthcare Research and Quality. Available online: http://www.hcup-us.ahrq.gov/reports/statbriefs/sb106.pdf (accessed on 5 July 2019).
- American Lung Association. What Causes COPD. Available online: http://www.lung.org/lung-health-and-diseases/lung-disease-lookup/copd/symptoms-causes-risk-factors/what-causes-copd.html (accessed on 5 July 2019).
- National Institutes of Health. Alpha-1 Antitrypsin Deficiency. Available online: https://ghr.nlm.nih.gov/condition/alpha-1-antitrypsin-deficiency (accessed on 5 July 2019).
- Martinez, C.; Miguel, D.; Mannino, D. Defining COPD-related comorbidities. Chronic Obstr. Pulm. Dis. 2014, 1, 51–63. [Google Scholar] [CrossRef] [PubMed]
- Mayo Clinic. COPD. 2017. Available online: https://www.mayoclinic.org/diseases-conditions/copd/diagnosis-treatment/drc-20353685 (accessed on 5 July 2019).
- DiMatteo, M. Variations in patients’ adherence to medical recommendations: A quantitative review of 50 years of research. Med. Care 2004, 42, 200–209. [Google Scholar] [CrossRef] [PubMed]
- Jones, R.C.M.; Hyland, M.; Hanney, K.; Erwin, J. A qualitative study of compliance with medication and lifestyle modification in chronic obstructive pulmonary disease (COPD). Prim. Care Respir. J. 2004, 13, 149–154. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Fox, S.; Purcell, K. Chronic Disease and the Internet. Available online: http://www.pewinternet.org/files/old-media/Files/Reports/2010/PIP_Chronic_Disease_with_topline.pdf (accessed on 5 July 2019).
- Stellefson, M.; Chaney, B.; Chaney, D.; Paige, S.; Payne-Purvis, C.; Tennant, B.; Walsh-Childers, K.; Sriram, P.S.; Alber, J. Engaging community stakeholders to evaluate the design, usability, and acceptability of a chronic obstructive pulmonary disease social media resource center. JMIR Res. Protoc. 2015, 4, e17. [Google Scholar] [CrossRef] [PubMed]
- Stellefson, M.; Shuster, J.; Chaney, B.; Paige, S.; Alber, J.; Chaney, D.; Sriram, P. Web-based health information seeking and eHealth literacy among patients living with chronic obstructive pulmonary disease (COPD). Health Commun. 2017, 33, 1410–1424. [Google Scholar] [CrossRef] [PubMed]
- Williams, V.; Price, J.; Hardinge, M.; Tarassenko, L.; Farmer, A. Using a mobile health application to support self-management in COPD: A qualitative study. Br. J. Gen. Pract. 2014, 64, 392–400. [Google Scholar] [CrossRef]
- Health Information National Trends Survey. U.S. Social Media Use and Health Communication. Available online: https://permanent.access.gpo.gov/gpo59550/HINTS_Brief_19.pdf (accessed on 5 July 2019).
- Pew Research Center. Social Media Fact Sheet. 2017. Available online: http://www.pewinternet.org/fact-sheet/social-media/ (accessed on 5 July 2019).
- Pew Research Center. Social Media Use in 2018. Available online: http://assets.pewresearch.org/wp-content/uploads/sites/14/2018/03/01105133/PI_2018.03.01_Social-Media_FINAL.pdf (accessed on 5 July 2019).
- Allen, C.; Vassiley, I.; Kennedy, A.; Rogers, A. Long-term condition self-management support in online communities: A meta-synthesis of qualitative papers. J. Med. Internet Res. 2016, 18, e61. [Google Scholar] [CrossRef] [PubMed]
- Paige, S.R.; Stellefson, M.; Chaney, B.H.; Alber, J.M. Pinterest as a resource for health information on chronic obstructive pulmonary disease (COPD): A social media content analysis. Am. J. Health Educ. 2015, 46, 241–251. [Google Scholar] [CrossRef]
- Angelis, G.D.; Wells, G.A.; Davies, B.; King, J.; Shallwni, S.M.; McEwan, J.; Cavallo, S.; Brosseau, L. The use of social media among health professionals to facilitate chronic disease self-management with their patients: A systematic review. Digit. Health 2018, 4. [Google Scholar] [CrossRef] [PubMed]
- Moorhead, S.A.; Hazlett, D.E.; Harrison, L.; Carroll, J.K.; Irwin, A.; Hoving, C. A new dimension of health care: Systematic review of the uses, benefits, and limitations of social media for health communication. JMIR 2013, 15, e85. [Google Scholar] [CrossRef]
- Patel, R.; Chang, T.; Greysen, S.R.; Chopra, V. Social media use in chronic disease: A systematic review and novel taxonomy. Am. J. Med. 2015, 128, 1335–1350. [Google Scholar] [CrossRef] [PubMed]
- Gu, D.; Guo, J.; Liang, C.; Lu, W.; Zhao, S.; Liu, B.; Long, T. Social media-based health management systems and sustained health engagement: TPB perspective. Int. J. Environ. Res. Public Health 2019, 16, 1495. [Google Scholar] [CrossRef]
- Krivak, T. Information Today. Facebook 101: Ten Things You Need to Know About Facebook. 2008. Available online: http://www.infotoday.com/IT/mar08/Krivak.shtml (accessed on 7 September 2019).
- Facebook. Statistics. 2017. Available online: https://newsroom.fb.com/company-info/ (accessed on 5 July 2019).
- Thackeray, R.; VanWagenen, S.; Koch Smith, A.; Neiger, B.; Prier, K. Adoption and use of social media among state health departments. BMC Public Health 2011, 12, 242. [Google Scholar] [CrossRef]
- Antheunis, M.; Tates, K.; Nieboer, T. Patients’ and health professionals’ use of social media in health care: Motives, barriers and expectations. Patient Educ. Couns. 2013, 92, 426–431. [Google Scholar] [CrossRef]
- Facebook. Facebook tips. What’s the Difference Between a Facebook Page and Group? 2010. Available online: https://www.facebook.com/notes/facebook/facebook-tips-whats-the-difference-between-a-facebook-page-and-group/324706977130/ (accessed on 5 July 2019).
- Bender, J.L.; Jimenez-Marroquin, M.C.; Jadad, A.R. Seeking support on facebook: A content analysis of breast cancer groups. JMIR 2011, 13, e16. [Google Scholar] [CrossRef]
- Lerman, B.; Lewis, S.; Lumley, M.; Grogan, G.; Hudson, C.; Johnson, E. Teen depression groups of facebook: A content analysis. J. Adolesc. Res. 2016, 32, 719–741. [Google Scholar] [CrossRef]
- Zhang, Y.; He, D.; Sang, Y. Facebook as a platform for health information and communication: A case study of a diabetes group. J. Med. Syst. 2013, 37, 9942. [Google Scholar] [CrossRef] [PubMed]
- Leventhal, H.; Phillips, A.; Burns, E. The common sense model of self-regulation (CSM): A dynamic framework for understanding illness self-management. J. Behav. Med. 2016, 39, 935–946. [Google Scholar] [CrossRef] [PubMed]
- Skiba, D.J. Face with tears of joy is word of the year: Are emoji a sign of things to come in health care? Nurs. Educ. Perspect. 2002, 37, 56–57. [Google Scholar] [CrossRef]
- Neiger, B.; Thackeray, R.; Van Wagenen, S.; Hanson, C.; West, J.; Barnes, M.; Fagen, M. Use of social media in health promotion: Purposes, key performance indicators, and evaluation metrics. Health Promot. Pract. 2012, 13, 159–164. [Google Scholar] [CrossRef]
- Greene, J.; Choudhry, N.; Kilabuk, E.; Shrank, W. Online social networking by patients with diabetes: A qualitative evaluation of communication with facebook. J. Gen. Intern. Med. 2011, 26, 287–292. [Google Scholar] [CrossRef] [PubMed]
- Centers for Disease Control and Prevention (CDC). Managing Chronic Obstructive Pulmonary Disease (COPD). Available online: https://www.cdc.gov/learnmorefeelbetter/programs/copd.htm (accessed on 5 July 2019).
- Global Initiative for Chronic Obstructive Lung Disease (GOLD). Global Strategy for the Diagnosis, Management, and Prevention of Chronic Obstructive Pulmonary Disease. Available online: https://goldcopd.org/wp-content/uploads/2018/11/GOLD-2019-v1.7-FINAL-14Nov2018-WMS.pdf (accessed on 5 July 2019).
- Hale, E.D.; Treharne, G.J.; Kitas, G.D. The common-sense model of self-regulation of health and illness: How can we use it to understand and respond to our patients’ needs? Rheumatology 2007, 46, 904–906. [Google Scholar] [CrossRef]
- Brennan, R.L.; Prediger, D.J. Coefficient kappa: Some uses, misuses, and alternatives. Educ. Psychol. Meas. 1981, 41, 687–699. [Google Scholar] [CrossRef]
- Bakeman, R. Behavioral observation and coding. In Handbook of Research Methods in Social and Personality Psychology, 2nd ed.; Reis, H.T., Judge, C.M., Eds.; Cambridge University Press: New York, NY, USA, 2000; pp. 138–159. ISBN 978-110-760-075-1. [Google Scholar]
- Lombard, M.; Snyder-Duch, J.; Bracken, C. Content analysis in mass communication: Assessment and reporting of intercoder reliability. Hum. Commun. Res. 2002, 28, 587–604. [Google Scholar] [CrossRef]
- Roberts, N.J.; Ghiassi, R.; Partridge, M.R. Health literacy in COPD. Int. J. Chron Obstruct. Pulmon. Dis. 2008, 3, 499–507. [Google Scholar]
- Write Effective Links. Available online: https://www.plainlanguage.gov/guidelines/web/write-effective-links/ (accessed on 1 October 2019).
- Lyles, C.; Fruchterman, J.; Youdelman, M.; Schillinger, D. Legal, practical, and ethical considerations for making online patient portals accessible for all. Am. J. Public Health 2017, 107, 1608–1611. [Google Scholar] [CrossRef] [PubMed]
- Partridge, S.R.; Gallagher, P.; Freeman, B.; Gallagher, R. Facebook Groups for the management of chronic diseases. J. Med. Internet Res. 2018, 20, e21. [Google Scholar] [CrossRef] [PubMed]
| Code | Definition | Code Source | Illness Self-Regulation Representation a |
|---|---|---|---|
| Group Purpose | |||
| Building Awareness/Sharing Information | Created to bring attention to the importance of COPD and share COPD-related information | Bender et al. [37] | Comorbid identities, causes, curability, consequences |
| Providing Support | Created to meet the emotional needs of COPD patients and their caregivers | Bender et al. [37] | Comorbid identities, causes, curability, consequences |
| Fundraising | Created to attract financial resources for COPD | Bender et al. [37] | N/A |
| Marketing/Promoting a Product/Service | Created to promote a COPD-related product or service | Bender et al. [37] | Curability |
| Media Modality | |||
| Text | Text included in the post | Neiger et al. [42] | N/A |
| Video | Video included in the post | Neiger et al. [42] | N/A |
| Photo | Photo included in the post | Neiger et al. [42] | N/A |
| Infographic | Infographic included in the post | Neiger et al. [42] | N/A |
| Communication Strategies | |||
| Self-Disclosures | Information was self-disclosed about personal experiences with COPD | Lerman et al. [38] | Comorbid identities, causes, curability, consequences |
| Referrals | Providing information about COPD through links to external websites, pages, groups, or documents | Lerman et al. [38] | Comorbid identities, causes, curability, consequences |
| Information Providing | COPD-related information was shared in the post | Greene et al. [43] | Comorbid identities, causes, curability, consequences |
| Information Requesting | COPD-related queries were posed to the group | Greene et al. [43] | Comorbid identities, causes, curability, consequences |
| Demonstrating Support | Emotional support was provided to the group | Greene et al. [43] | Comorbid identities, causes, curability, consequences |
| Product/Service Promotion | A product or service was promoted | Greene et al. [43] | Curability |
| Self-Management Content Area | |||
| Mental Health | Mentions mental health issues such as depression, anxiety, etc. | CDC [44] | Comorbid identities, Consequences |
| Medications | ‘Mentions medications such as antibiotics, inhalers, etc. | CDC [44] | Curability |
| Hospitalizations/Doctor Visits | Mentions hospitalization or doctors visit related to COPD | GOLD [45] | Consequences |
| Asthma | Mentions asthma specifically | GOLD [45] | Comorbid identities |
| Smoking | Mentions smoking such as cigarette smoking, vaping, e-cigarette use, etc. | GOLD [45] | Causes |
| Breathing Techniques | Mentions specific breathing techniques to cope with exacerbations | CDC [44] | Curability |
| Nutrition | Mentions nutrition such as recipes and health eating habits | CDC [44] | Curability |
| Physical Activity | Mentions physical activity such as walking, stair climbing, etc. | CDC [44] | Curability, Consequences |
| Engagement | |||
| Like | Number of times members reacted to the post by pressing the thumbs up icon | Neiger et al. [42] | N/A |
| Love | Number of times members reacted to the post by pressing the heart emoji | Neiger et al. [42] | N/A |
| Sad | Number of times members reacted to the post by pressing the sad emoji | Neiger et al. [42] | N/A |
| Angry | Number of times members reacted to the post by pressing the angry emoji | Neiger et al. [42] | N/A |
| Laugh | Number of times members reacted to the post by pressing the haha emoji | Neiger et al. [42] | N/A |
| Surprised | Number of times members reacted to the post by pressing the wow emoji | Neiger et al. [42] | N/A |
| Comment | Number of times members reacted to the post by replying with text, gif, etc. | Neiger et al. [42] | N/A |
| Share | Number of times members reacted to a post by sharing it | Neiger et al. [42] | N/A |
| Self-Management Content Area | Cohen’s Kappa |
| Mental Health | >0.99 |
| Medications | >0.99 |
| Hospitalizations/Doctor Visits | 0.91 |
| Asthma | >0.99 |
| Smoking | >0.99 |
| Breathing Techniques | 0.66 |
| Nutrition | >0.99 |
| Physical Activity | 0.66 |
| Mean | 0.90 |
| SD | 0.15 |
| Wall Post Characteristics | Cohen’s Kappa |
| Post Included Text | 0.66 |
| Post Included Video | >0.99 |
| Post Included Photo | 0.87 |
| Post Included Infographic | >0.99 |
| Information Providing | >0.99 |
| Information Requesting | 0.95 |
| Demonstrating Support | 0.75 |
| Personal Self-Disclosure | 0.95 |
| Referral to Other Resources | >0.99 |
| Product/Service Promotion | >0.99 |
| Mean | 0.91 |
| SD | 0.12 |
| Group Name | Privacy Setting | Group Purpose | Number of Members | Number of New Members in Past 30 Days | Number of Posts in Past 30 Days | Months in Operation |
|---|---|---|---|---|---|---|
| Ultimate Pulmonary Wellness: COPD, PF, Pulmonary Hypertension and Others | Closed | Providing Support | 12,337 | 245 | 632 | 36 |
| COPD Warriors Hope, Support, Love & Laughter | Closed | Providing Support | 10,451 | 692 | 2764 | 60 |
| COPD/Emphysema/Pulmonary Disease- I have COPD- COPD does not have me! | Closed | Building Awareness/Sharing Information | 7952 | 0 | 367 | 60 |
| COPD- GET EDUCATED! | Closed | Providing Support | 6837 | 0 | 277 | 24 |
| (COPD) Emphysema/Chronic Bronchitis Support Group | Closed | Providing Support | 5537 | 0 | 67 | 120 |
| COPD Information and Support | Closed | Building Awareness/Sharing Information | 5028 | 294 | 1087 | 48 |
| Let’s Talk COPD Support Group | Closed | Providing Support | 4139 | 213 | 672 | 24 |
| Support Group for People with COPD, Emphysema, Asthma, Bronchitis | Closed | Providing Support | 3938 | 192 | 233 | 84 |
| Emphysema | Closed | Providing Support | 3794 | 84 | 243 | 96 |
| COPD Xplained- USA | Closed | Building Awareness/Sharing Information | 3748 | 90 | 291 | 108 |
| COPD Support Group | Closed | Providing Support | 3049 | 229 | 551 | 36 |
| COPD/ A WARM LOVING PLACE TO HANG OUT | Closed | Providing Support | 3027 | 97 | 1998 | 48 |
| COPD Breathing Buddies | Closed | Providing Support | 2776 | 0 | 660 | 60 |
| Lift Up- COPD Support Group | Closed | Providing Support | 2438 | 282 | 381 | 12 |
| COPD- New Treatments and Advice | Closed | Building Awareness/Sharing Information | 2238 | 0 | 34 | 48 |
| COPD/COAD Support | Closed | Building Awareness/Sharing Information | 2223 | 0 | 125 | 96 |
| COPD/ALPHA 1 | Public | Providing Support | 1273 | 4 | 59 | 60 |
| COPD- A BREATH OF FRESH AIR | Closed | Providing Support | 974 | 0 | 272 | 48 |
| COPD-Emphysema-Chronic Bronchitis | Closed | Providing Support | 886 | 0 | 6 | 96 |
| COPD Tackling it Together | Closed | Providing Support | 868 | 0 | 103 | 132 |
| COPD Service | Public | Providing Support | 830 | 0 | 0 | 60 |
| COPD CRAZINESS AND SUPPORT | Closed | Providing Support | 810 | 0 | 301 | 120 |
| Chronic Obstructive Pulmonary Disease | Closed | Providing Support | 781 | 0 | 7 | 96 |
| C.O.P.D Warriors | Closed | Building Awareness/Sharing Information | 700 | 0 | 343 | 24 |
| Support & Awareness for COPD, Emphysema and Chronic Bronchitis | Public | Building Awareness/Sharing Information | 295 | 0 | 6 | 132 |
| Chronic Bronchitis Support & Awareness | Closed | Providing Support | 153 | 0 | 0 | 12 |
| Wall Post Communication Strategies | Posts Addressing COPD Self-Management n (%) | Posts Not Addressing COPD Self-Management n (%) | p Value |
|---|---|---|---|
| Self-Disclosure | |||
| Yes (n = 80) | 50 (62.5) ** | 30 (37.5) | 0.0001 |
| No (n = 100) | 28 (28) | 72 (72) | |
| Referral to External Information Source | |||
| Yes (n = 53) | 13 (24.5) * | 40 (75.5) | 0.001 |
| No (n = 127) | 65 (51.2) | 62 (48.8) | |
| Information Provided | |||
| Yes (n = 45) | 19 (42.2) | 26 (57.8) | 0.862 |
| No (n = 135) | 59 (43.7) | 76 (56.3) | |
| Information Requested (i.e., Asks a Question) | |||
| Yes (n = 69) | 42 (60.9) ** | 27 (39.1) | 0.0001 |
| No (n = 111) | 36 (32.4) | 75 (67.6) | |
| Offers Support | |||
| Yes (n = 26) | 2 (7.7) ** | 24 (92.3) | 0.0001 |
| No (n = 154) | 76 (49.4) | 78 (50.6) | |
| Product/Service Promotion | |||
| Yes (n = 5) | 3 (60) | 2 (40) | 0.446 |
| No (n = 175) | 75 (42.9) | 100 (57.1) | |
| Communication Strategy | Post Addressed Medication Management n (%) | Post Did Not Address Medication Management n (%) | p Value |
|---|---|---|---|
| Self-Disclosure | |||
| Yes (n = 80) | 32 (40) ** | 48 (60) | 0.0001 |
| No (n = 100) | 16 (16) | 84 (84) | |
| Referral to External Information Source | |||
| Yes (n = 53) | 7 (13.2) * | 46 (86.8) | 0.008 |
| No (n = 127) | 41 (32.3) | 86 (67.7) | |
| Information Provided | |||
| Yes (n = 45) | 10 (22.2) | 35 (77.8) | 0.436 |
| No (n = 135) | 38 (28.1) | 97 (71.9) | |
| Information Requested (i.e., Asks a Question) | |||
| Yes (n = 69) | 30 (43.5) ** | 39 (56.5) | 0.0001 |
| No (n = 111) | 18 (16.2) | 93 (83.8) | |
| Offers Support | |||
| Yes (n = 26) | 0 (0) * | 26 (100) | 0.001 |
| No (n = 154) | 48 (31.2) | 106 (68.8) | |
| Product/Service Promotion | |||
| Yes (n = 5) | 1 (20) | 4 (80) | 0.732 |
| No (n = 175) | 47 (26.9) | 128 (73.1) | |
| Type of Communication Strategy | Post Addressed Hospitalizations/Doctor Visits n (%) | Post Did Not Address Hospitalizations/Doctor Visits n (%) | p Value |
|---|---|---|---|
| Self-Disclosure | |||
| Yes (n = 80) | 27 (33.8) ** | 53 (66.2) | 0.0001 |
| No (n = 100) | 1 (1) | 99 (99) | |
| Referral to External Information Source | |||
| Yes (n = 53) | 0 (0) ** | 53 (100) | 0.0001 |
| No (n = 127) | 28 (22.0) | 99 (78.0) | |
| Information Provided | |||
| Yes (n = 45) | 1 (2.2) * | 44 (97.8) | 0.004 |
| No (n = 135) | 27 (20) | 108 (80) | |
| Information Requested (i.e., Asks a Question) | |||
| Yes (n = 69) | 15 (21.7) | 54 (78.3) | 0.071 |
| No (n = 111) | 13 (11.7) | 98 (88.3) | |
| Offers Support | |||
| Yes (n = 26) | 2 (7.7) | 24 (92.3) | 0.232 |
| No (n = 154) | 26 (16.9) | 128 (83.1) | |
| Product/Service Promotion | |||
| Yes (n = 5) | 0 (0) | 5 (100) | 0.330 |
| No (n = 175) | 28 (16) | 147 (84) | |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Apperson, A.; Stellefson, M.; Paige, S.R.; Chaney, B.H.; Chaney, J.D.; Wang, M.Q.; Mohan, A. Facebook Groups on Chronic Obstructive Pulmonary Disease: Social Media Content Analysis. Int. J. Environ. Res. Public Health 2019, 16, 3789. https://doi.org/10.3390/ijerph16203789
Apperson A, Stellefson M, Paige SR, Chaney BH, Chaney JD, Wang MQ, Mohan A. Facebook Groups on Chronic Obstructive Pulmonary Disease: Social Media Content Analysis. International Journal of Environmental Research and Public Health. 2019; 16(20):3789. https://doi.org/10.3390/ijerph16203789
Chicago/Turabian StyleApperson, Avery, Michael Stellefson, Samantha R. Paige, Beth H. Chaney, J. Don Chaney, Min Qi Wang, and Arjun Mohan. 2019. "Facebook Groups on Chronic Obstructive Pulmonary Disease: Social Media Content Analysis" International Journal of Environmental Research and Public Health 16, no. 20: 3789. https://doi.org/10.3390/ijerph16203789
APA StyleApperson, A., Stellefson, M., Paige, S. R., Chaney, B. H., Chaney, J. D., Wang, M. Q., & Mohan, A. (2019). Facebook Groups on Chronic Obstructive Pulmonary Disease: Social Media Content Analysis. International Journal of Environmental Research and Public Health, 16(20), 3789. https://doi.org/10.3390/ijerph16203789





