The Value of Local Heatwave Impact Assessment: A Case-Crossover Analysis of Hospital Emergency Department Presentations in Tasmania, Australia
Abstract
1. Introduction
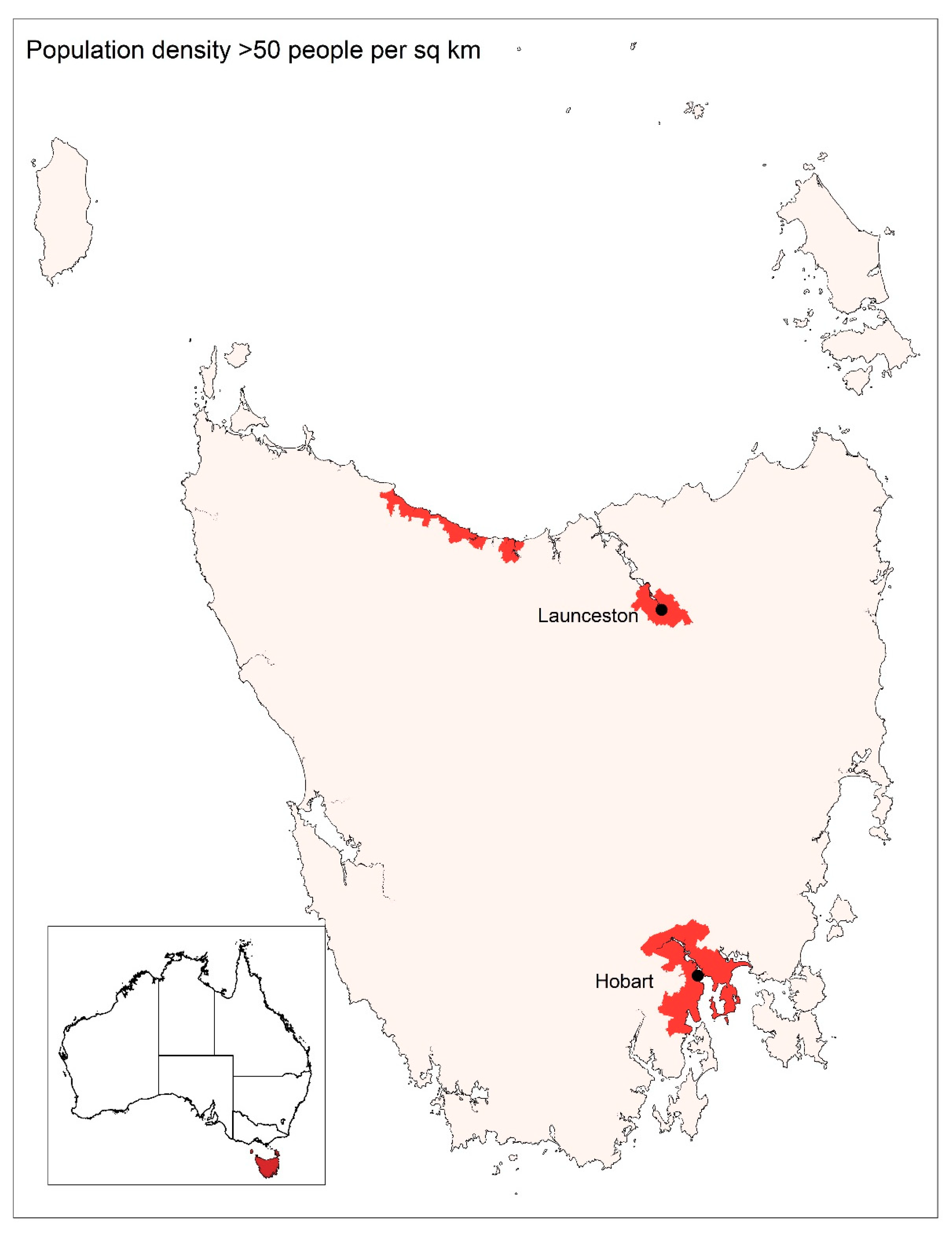
1.1. Study Setting
1.2. Research Aim
2. Materials and Methods
2.1. Exposure Data
2.2. Outcome Data
2.3. Study Design
2.4. Analyses
- Age group (0–5, 0–15 and over 65)
- Gender
- Socio-Economic Index for Areas (SEIFA) category (by suburb of patient address), using the Index of Relative Socio-Economic Disadvantage
- Diagnostic group.
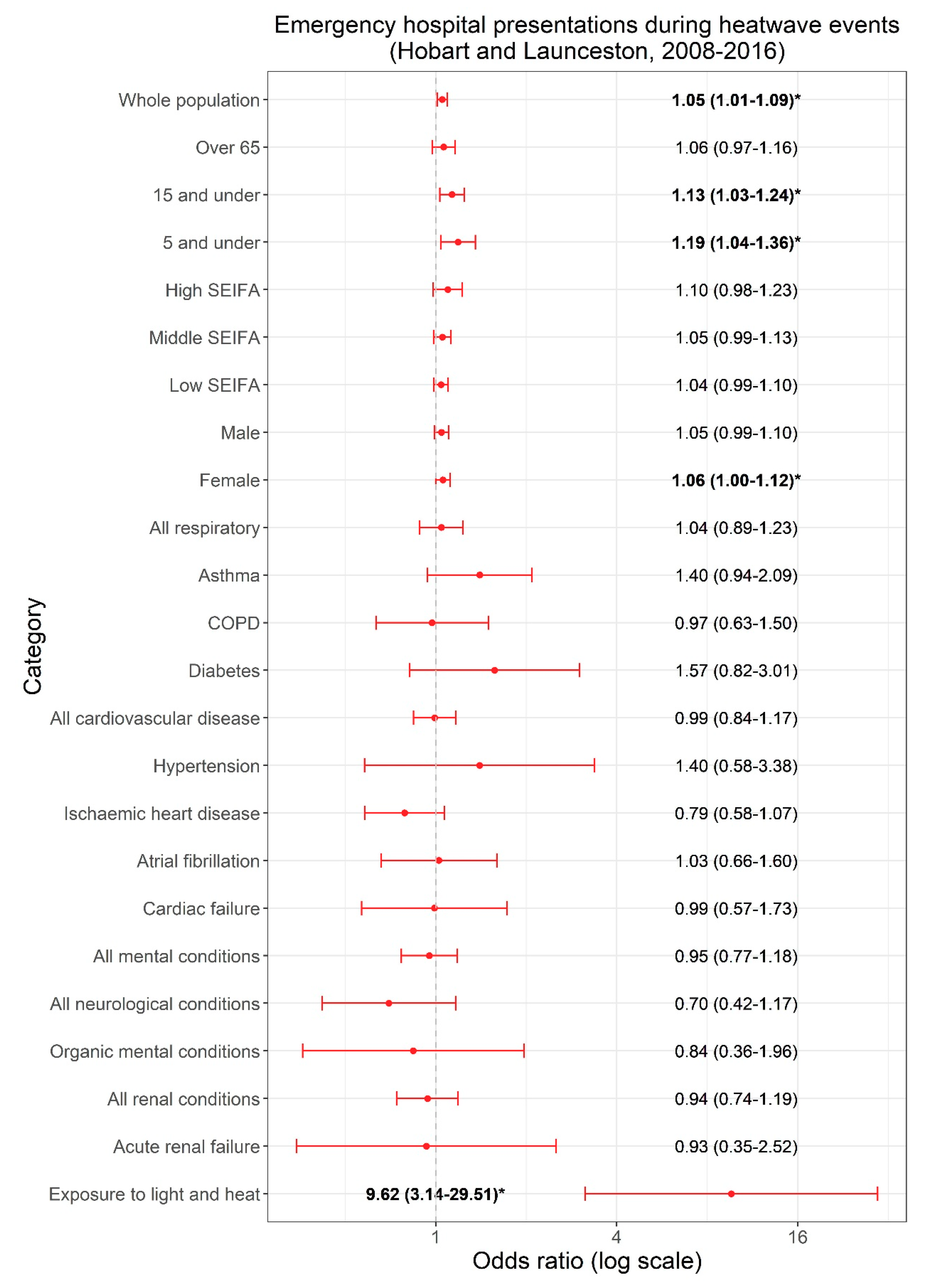
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Watts, N.; Adger, W.N.; Agnolucci, P.; Blackstock, J.; Byass, P.; Cai, W.; Chaytor, S.; Colbourn, T.; Collins, M.; Cooper, A.; et al. Health and climate change: Policy responses to protect public health. Lancet 2015, 386, 1861–1914. [Google Scholar] [CrossRef]
- Blashki, G.; Armstrong, G.; Berry, H.L.; Weaver, H.J.; Hanna, E.G.; Peng, B.; Harley, D.; Spickett, J.T. Preparing Health Services for Climate Change in Australia. Asia Pac. J. Public Health 2011, 23, 133S–143S. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Atlas of Health and Climate Change; World Health Organization: Geneva, Switzerland, 2012. [Google Scholar]
- Intergovernmental Panel on Climate Change. Climate Change 2013: The Physical Science Basis. Contribution of Working Group I to the Fifth Assessment Report of the Intergovernmental Panel on Climate Change; Intergovernmental Panel on Climate Change: Cambridge, UK, 2013. [Google Scholar]
- Perkins, S.E.; Alexander, L.V.; Nairn, J.R. Increasing frequency, intensity and duration of observed global heatwaves and warm spells. Geophys. Res. Lett. 2012, 39, L20714. [Google Scholar] [CrossRef]
- Coates, L.; Haynes, K.; O’Brien, J.; McAneney, J.; Dimer-deOliveira, F. Exploring 167 years of vulnerability: An examination of extreme heat events in Australia 1844–2010. Environ. Sci. Policy 2014, 42, 33–44. [Google Scholar] [CrossRef]
- Campbell, S.; Remenyi, T.A.; White, C.J.; Johnston, F.H. Heatwave and health impact research: A global review. Health Place 2018, 53, 210–218. [Google Scholar] [CrossRef] [PubMed]
- Bi, P.; Williams, S.; Loughnan, M.; Lloyd, G.; Hansen, A.; Kjellstrom, T.; Dear, K.; Saniotis, A. The Effects of Extreme Heat on Human Mortality and Morbidity in Australia: Implications for Public Health. Asia Pac. J. Public Health 2011, 23, 27S–36S. [Google Scholar] [CrossRef]
- Benmarhnia, T.; Deguen, S.; Kaufman, J.S.; Smargiassi, A. Vulnerability to heat-related mortality: A systematic review, meta-analysis, and meta-regression analysis. Epidemiology 2015, 26, 781–793. [Google Scholar] [CrossRef]
- Li, M.; Gu, S.; Bi, P.; Yang, J.; Liu, Q. Heat waves and morbidity: Current knowledge and further direction-a comprehensive literature review. Int. J. Environ. Res. Public Health 2015, 12, 5256–5283. [Google Scholar] [CrossRef]
- Fouillet, A.; Rey, G.; Laurent, F.; Pavillon, G.; Bellec, S.; Guihenneuc-Jouyaux, C.; Clavel, J.; Jougla, E.; Hémon, D. Excess mortality related to the August 2003 heat wave in France. Int. Arch. Occup. Environ. Health 2006, 80, 16–24. [Google Scholar] [CrossRef]
- Kue, R.C.; Dyer, K.S. The impact of heat waves on transport volumes in an urban Emergency Medical Services system: a retrospective review. Prehosp. Disaster Med. 2013, 28, 610–615. [Google Scholar] [CrossRef]
- Nitschke, M.; Tucker, G.R.; Bi, P. Morbidity and mortality during heatwaves in metropolitan Adelaide. Med. J. Aust. 2007, 187, 662–665. [Google Scholar] [CrossRef]
- Williams, S.; Nitschke, M.; Weinstein, P.; Pisaniello, D.L.; Parton, K.A.; Bi, P. The impact of summer temperatures and heatwaves on mortality and morbidity in Perth, Australia 1994–2008. Environ. Int. 2012, 40, 33–38. [Google Scholar] [CrossRef] [PubMed]
- Orlov, A.; Sillmann, J.; Aaheim, A.; Aunan, K.; de Bruin, K. Economic Losses of Heat-Induced Reductions in Outdoor Worker Productivity: A Case Study of Europe. Econ. Disasters Clim. Chang. 2019. [Google Scholar] [CrossRef]
- Lindstrom, S.J.; Nagalingam, V.; Newnham, H.H. Impact of the 2009 Melbourne heatwave on a major public hospital. Intern. Med. J. 2013, 43, 1246–1250. [Google Scholar] [CrossRef] [PubMed]
- Nitschke, M.; Tucker, G.R.; Hansen, A.L.; Williams, S.; Zhang, Y.; Bi, P. Impact of two recent extreme heat episodes on morbidity and mortality in Adelaide, South Australia: A case-series analysis. Environ. Health 2011, 10. [Google Scholar] [CrossRef] [PubMed]
- Khalaj, B.; Lloyd, G.; Sheppeard, V.; Dear, K. The health impacts of heat waves in five regions of New South Wales, Australia: A case-only analysis. Int. Arch. Occup. Environ. Health 2010, 83, 833–842. [Google Scholar] [CrossRef] [PubMed]
- Toloo, G.S.; Yu, W.; Aitken, P.; FitzGerald, G.; Tong, S. The impact of heatwaves on emergency department visits in Brisbane, Australia: A time series study. Crit. Care 2014, 18, R69. [Google Scholar] [CrossRef] [PubMed]
- Turner, L.R.; Connell, D.; Tong, S. The effect of heat waves on ambulance attendances in Brisbane, Australia. Prehosp. Disaster Med. 2013, 28, 482–487. [Google Scholar] [CrossRef]
- Tong, S.; Wang, X.Y.; Yu, W.; Chen, D.; Wang, X. The impact of heatwaves on mortality in Australia: A multicity study. BMJ Open 2014, 4. [Google Scholar] [CrossRef]
- Dalip, J.; Phillips, G.A.; Jelinek, G.A.; Weiland, T.J. Can the elderly handle the heat? a retrospective case-control study of the impact of heat waves on older patients attending an inner city Australian emergency department. Asia Pac. J. Public Health 2015, 27, NP1837–NP1846. [Google Scholar] [CrossRef]
- Hansen, A.L.; Bi, P.; Ryan, P.; Nitschke, M.; Pisaniello, D.; Tucker, G. The effect of heat waves on hospital admissions for renal disease in a temperate city of Australia. Int. J. Epidemiol. 2008, 37, 1359–1365. [Google Scholar] [CrossRef] [PubMed]
- Australian Bureau of Statistics. Australian Statistical Geography Standard (ASGS): Volume 5-Remoteness Structure; Commonwealth Government: Canberra, Australia, 2011; Volume 1270.0.55.005.
- Australian Bureau of Statistics. 3235.0—Regional Population by Age and Sex, Australia; Commonwealth Government: Canberra, Australian, 2018.
- Bureau of Meteorology. Tasmania in 2009: Wet and Warm. Available online: www.bom.gov.au/climate/current/annual/tas/archive/2009.summary.shtml (accessed on 30 September 2018).
- Bureau of Meteorology. Tasmania in Summer 2012–2013: A Warm and Dry Summer. Available online: www.bom.gov.au/climate/current/season/tas/archive/201302.summary.shtml (accessed on 30 September 2018).
- Tasmanian Government. 2013 Tasmanian Bushfires Inquiry; Tasmanian Government: Hobart, Australia, 2013; Volume 1.
- Australian Bureau of Statistics. Australian Demographic Statistics Commonwealth Government of Australia: 2018; Australian Bureau of Statistics: Canberra, Australia, 2018.
- Department of Health. State of Public Health Report; Tasmanian Government: Hobart, Australia, 2018.
- Department of Health and Human Services. Report on the Tasmanian Population Health Survey 2016; Tasmanian Government: Hobart, Australia, 2016.
- Braga, A.L.F.; Zanobetti, A.; Schwartz, J. The Time Course of Weather-Related Deaths. Epidemiology 2001, 12, 662–667. [Google Scholar] [CrossRef] [PubMed]
- Su, C.-H.; Eizenberg, N.; Steinle, P.; Jakob, D.; Fox-Hughes, P.; White, C.J.; Rennie, S.; Franklin, C.; Dharssi, I.; Zhu, H. BARRA v1.0: The Bureau of Meteorology Atmospheric high-resolution Regional Reanalysis for Australia. Geosci. Model Dev. 2019, 12, 2049–2068. [Google Scholar] [CrossRef]
- Nairn, J.; Fawcett, R. The Excess Heat Factor: A Metric for Heatwave Intensity and Its Use in Classifying Heatwave Severity. Int. J. Environ. Res. Public Health 2015, 12, 227–253. [Google Scholar] [CrossRef] [PubMed]
- Bureau of Meteorology. Heatwave Service for Australia. Available online: www.bom.gov.au/australia/heatwave (accessed on 3 March 2019).
- Scalley, B.D.; Spicer, T.; Jian, L.; Xiao, J.; Nairn, J.; Robertson, A.; Weeramanthri, T. Responding to heatwave intensity: Excess Heat Factor is a superior predictor of health service utilisation and a trigger for heatwave plans. Aust. N. Z. J. Public Health 2015, 39, 582–587. [Google Scholar] [CrossRef]
- Urban, A.; Hondula, D.; Hanzlíková, H.; Kyselý, J. The predictability of heat-related mortality in Prague, Czech Republic, during summer 2015—A comparison of selected thermal indices. Int. J. Biometeorol. 2019, 63, 535–548. [Google Scholar] [CrossRef]
- Zeileis, A.; Grothendieck, G.; Ryan, J.A.; Ulrich, J.M.; Andrews, F. S3 Infrastructure for Regular and Irregular Time Series (Z’s Ordered Observations). Available online: https://cran.r-project.org/web/packages/zoo/zoo.pdf (accessed on 12 December 2018).
- Montel, M. Python-Holidays. Available online: https://github.com/dr-prodigy/python-holidays (accessed on 7 March 2019).
- Jaakkola, J.J.K. Case-crossover design in air pollution epidemiology. Eur. Respir. J. 2003, 21, 81s–85s. [Google Scholar] [CrossRef]
- Maclure, M. The Case-Crossover Design: A Method for Studying Transient Effects on the Risk of Acute Events. Am. J. Epidemiol. 1991, 133, 144–153. [Google Scholar] [CrossRef]
- Wang, X.Y.; Barnett, A.G.; Yu, W.; FitzGerald, G.; Tippett, V.; Aitken, P.; Neville, G.; McRae, D.; Verrall, K.; Tong, S. The impact of heatwaves on mortality and emergency hospital admissions from non-external causes in Brisbane, Australia. Occup. Environ. Med. 2012, 69, 163–169. [Google Scholar] [CrossRef]
- Basagana, X.; Sartini, C.; Barrera-Gomez, J.; Dadvand, P.; Cunillera, J.; Ostro, B.; Sunyer, J.; Medina-Ramon, M. Heat waves and cause-specific mortality at all ages. Epidemiology 2011, 22, 765–772. [Google Scholar] [CrossRef]
- Tong, S.; Wang, X.Y.; Guo, Y. Assessing the short-term effects of heatwaves on mortality and morbidity in Brisbane, Australia: Comparison of case-crossover and time series analyses. PLoS ONE 2012, 7, e37500. [Google Scholar] [CrossRef] [PubMed]
- Basu, R.; Dominici, F.; Samet, J.M. Temperature and Mortality among the Elderly in the United States: A Comparison of Epidemiologic Methods. Epidemiology 2005, 16, 58–66. [Google Scholar] [CrossRef] [PubMed]
- Therneau, T.; Lumley, T. Package ‘Survival’. Available online: https://cran.r-project.org/web/packages/survival/survival.pdf (accessed on 12 December 2018).
- Szumilas, M. Explaining odds ratios. Journal of the Canadian Academy of Child and Adolescent Psychiatry. J. Acad. Can. Psychiatr. Enfant Adolesc. 2010, 19, 227–229. [Google Scholar]
- World Health Organization. International Statistical Classification of Diseases and Related Health Problems 2010 Edition; World Health Organization: Geneva, Switzerland, 2011; Volume 2. [Google Scholar]
- Schaffer, A.; Muscatello, D.; Broome, R.; Corbett, S.; Smith, W. Emergency department visits, ambulance calls, and mortality associated with an exceptional heat wave in Sydney, Australia, 2011: A time-series analysis. Environ. Health 2012, 11. [Google Scholar] [CrossRef] [PubMed]
- Fuhrmann, C.M.; Sugg, M.M.; Konrad, C.E., II; Waller, A. Impact of Extreme Heat Events on Emergency Department Visits in North Carolina (2007–2011). J. Community Health 2016, 41, 146–156. [Google Scholar] [CrossRef] [PubMed]
- Sun, X.M.; Sun, Q.; Yang, M.J.; Zhou, X.F.; Li, X.P.; Yu, A.Q.; Geng, F.H.; Guo, Y.M. Effects of temperature and heat waves on emergency department visits and emergency ambulance dispatches in Pudong New Area, China: A time series analysis. Environ. Health 2014, 13. [Google Scholar] [CrossRef] [PubMed]
- Zhang, K.; Chen, T.-H.; Begley, C.E. Impact of the 2011 heat wave on mortality and emergency department visits in Houston, Texas. Environ. Health A Glob. Access Sci. Source 2015, 14. [Google Scholar] [CrossRef]
- Leonardi, G.S.; Hajat, S.; Kovats, R.S.; Smith, G.E.; Cooper, D.; Gerard, E. Syndromic surveillance use to detect the early effects of heat-waves: An analysis of NHS direct data in England. Soz. Prav. 2006, 51, 194–201. [Google Scholar] [CrossRef] [PubMed]
- Knowlton, K.; Rotkin-Ellman, M.; King, G.; Margolis, H.G.; Smith, D.; Solomon, G.; Trent, R.; English, P. The 2006 California Heat Wave: Impacts on Hospitalizations and Emergency Department Visits. Environ. Health Perspect. 2009, 117, 61–67. [Google Scholar] [CrossRef]
- Michelozzi, P.; de Donato, F.; Bisanti, L.; Russo, A.; Cadum, E.; DeMaria, M.; D’Ovidio, M.; Costa, G.; Perucci, C.A. The impact of the summer 2003 heat waves on mortality in four Italian cities. Euro surveillance: Bulletin Europeen sur les maladies transmissibles. Eur. Commun. Dis. Bull. 2005, 10, 161–165. [Google Scholar]
- Xiao, J.; Spicer, T.; Jian, L.; Yun, G.Y.; Shao, C.; Nairn, J.; Fawcett, R.J.B.; Robertson, A.; Weeramanthri, T.S. Variation in Population Vulnerability to Heat Wave in Western Australia. Front. Public Health 2017, 5, 64. [Google Scholar] [CrossRef] [PubMed]
- Loughnan, M.E.; Nicholls, N.; Tapper, N.J. The effects of summer temperature, age and socioeconomic circumstance on Acute Myocardial Infarction admissions in Melbourne, Australia. Int. J. Health Geogr. 2010, 9. [Google Scholar] [CrossRef] [PubMed]
- Kim, E.J.; Kim, H. Effect modification of individual- and regional-scale characteristics on heat wave-related mortality rates between 2009 and 2012 in Seoul, South Korea. Sci. Total Environ. 2017, 595, 141–148. [Google Scholar] [CrossRef] [PubMed]
- Cheng, J.; Xu, Z.; Bambrick, H.; Prescott, V.; Wang, N.; Zhang, Y.; Su, H.; Tong, S.; Hu, W. Cardiorespiratory effects of heatwaves: A systematic review and meta-analysis of global epidemiological evidence. Environ. Res. 2019, 177, 108610. [Google Scholar] [CrossRef] [PubMed]
- Johnston, F.H.; Hanigan, I.C.; Henderson, S.B.; Morgan, G.G. Evaluation of interventions to reduce air pollution from biomass smoke on mortality in Launceston, Australia: Retrospective analysis of daily mortality, 1994–2007. Br. Med. J. 2013, 346, e8446. [Google Scholar] [CrossRef] [PubMed]
- Johnston, F.H.; Purdie, S.; Jalaludin, B.; Martin, K.L.; Henderson, S.B.; Morgan, G.G. Air pollution events from forest fires and emergency department attendances in Sydney, Australia 1996–2007: A case-crossover analysis. Environ. Health 2014, 13, 105. [Google Scholar] [CrossRef] [PubMed]
- Edwards, L.J.; Williamson, G.; Williams, S.A.; Veitch, M.G.K.; Salimi, F.; Johnston, F.H. Did Fine Particulate Matter from the Summer 2016 Landscape Fires in Tasmania Increase Emergency Ambulance Dispatches? A Case Crossover Analysis. Fire 2018, 1, 26. [Google Scholar] [CrossRef]
- Johnston, F.H.; Salimi, F.; Williamson, G.J.; Henderson, S.B.; Yao, J.; Dennekamp, M.; Smith, K.; Abramson, M.J.; Morgan, G.G. Ambient Particulate Matter and Paramedic Assessments of Acute Diabetic, Cardiovascular, and Respiratory Conditions. Epidemiology 2019, 30, 11–19. [Google Scholar] [CrossRef]
- Xu, Z.; Huang, C.; Hu, W.; Turner, L.R.; Su, H.; Tong, S. Extreme temperatures and emergency department admissions for childhood asthma in Brisbane, Australia. Occup. Environ. Med. 2013, 70, 730–735. [Google Scholar] [CrossRef]
- Parker, W. Reanalyses and Observations: What’s the Difference? Bull. Am. Meteorol. Soc. 2016. [Google Scholar] [CrossRef]
- Raghavendra, A.; Dai, A.; Milrad, S.M.; Cloutier-Bisbee, S.R. Floridian heatwaves and extreme precipitation: Future climate projections. Clim. Dyn. 2019, 52, 495–508. [Google Scholar] [CrossRef]
- Parkyn, K.; Yeo, C.; Bannister, T. Meteorological Lessons Learned from ‘Black Saturday’, the 7 February 2009 Victorian Fires; Bureau of Meteorology: Melbourne, Australia, 2010.
- The Mercury. Ten Best Ways to Keep Your Cool as City Scorches. 2017. Available online: www.themercury.com.au/lifestyle/ten-best-ways-to-keep-your-cool-as-city-scorches/news-story/4b7599f5346103e8aeca75a638c7bf6d (accessed on 20 September 2019).
| Diagnostic Condition | ICD-10 Code |
|---|---|
| All respiratory | J00–J99 |
| Asthma | J45–J46 |
| Chronic obstructive pulmonary disease (COPD) | J40–J44, J47, J67 |
| Diabetes | E10–E11, E13–E14 |
| All cardiovascular | I00–I99, G45–G46 |
| Hypertensive | I10–I13 |
| Ischemic heart disease | I20–I25 |
| Atrial fibrillation | I48 |
| Cardiac failure | I50 |
| All mental disorders | F00–F99 |
| Dementia | F00–F03 |
| Neuroses | F40–F48 |
| Psychoses | F80–F89 |
| Organic mental disorders (including depression, anxiety) | F00–F09 |
| All renal disorders | N00–N39 |
| Acute renal failure | N17 |
| Renal calculus | N20–N21 |
| Heat and light disorders (including sunburn, heat stroke) | T67, X30 |
| Population Characteristic/Diagnostic Group | Total Number (% of Total) | Mean Daily Presentations | Standard Deviation | Minimum/Maximum Presentations |
|---|---|---|---|---|
| Whole population | 841,965 (100%) | 256.1 | 31.4 | 153/358 |
| Age | ||||
| ≤5 | 85,450 (10.1%) | 26.0 | 7.2 | 5/56 |
| ≤15 | 160,315 (19.0%) | 48.8 | 10.9 | 18/108 |
| 16–65 | 521,072 (61.9%) | 158.5 | 20.3 | 90/232 |
| >65 | 160,500 (19.1%) | 48.8 | 10.3 | 21/85 |
| Gender | ||||
| Male | 434,660 (51.6%) | 132.2 | 18.3 | 80/201 |
| Female | 407,032 (48.3%) | 123.8 | 17.6 | 67/181 |
| SEIFA | ||||
| Low | 437,577 (52.0%) | 133.1 | 17.6 | 75/194 |
| Middle | 252,039 (30.0%) | 76.7 | 11.7 | 36/118 |
| High | 135,392 (16.0%) | 41.2 | 8.7 | 15/78 |
| All respiratory | 67,439 (8.0%) | 20.5 | 7.6 | 3/63 |
| Asthma | 8546 (1.0%) | 2.7 | 1.6 | 1/10 |
| COPD | 10,365 (1.2%) | 3.4 | 1.9 | 1/14 |
| All cardiovascular | 49,436 (5.9%) | 15.0 | 4.3 | 3/31 |
| Cardiac failure | 5199 (0.6%) | 2.0 | 1.1 | 1/9 |
| Hypertensive | 1312 (0.2%) | 1.2 | 0.5 | 1/5 |
| Atrial fibrillation | 2724 (0.3%) | 2.2 | 1.2 | 1/8 |
| Ischemic heart disease | 13,964 (1.7%) | 4.3 | 2.1 | 1/15 |
| Diabetes | 1994 (0.2%) | 1.3 | 0.6 | 1/5 |
| All mental disorders | 34,509 (4.1%) | 10.5 | 3.7 | 1/27 |
| Dementia | 655 (0.1%) | 1.3 | 0.4 | 1/4 |
| Neuroses | 6459 (0.8%) | 2.3 | 1.3 | 1/9 |
| Organic mental | 2639 (0.3%) | 1.5 | 0.8 | 1/7 |
| Psychoses | 21 (0.002%) | 1.0 | 0 | 1/1 |
| All renal | 20,914 (2.5%) | 6.4 | 2.6 | 1/19 |
| Acute renal failure | 1416 (0.2%) | 1.3 | 0.5 | 1/5 |
| Renal calculus | 120 (0.01%) | 1.1 | 0.3 | 1/2 |
| Exposure to light and heat | 199 (0.02%) | 1.3 | 1.1 | 1/12 |
| Region | Low Intensity Days | Severe Days | Extreme Days |
|---|---|---|---|
| South (Hobart) | 85 | 9 | 1 |
| North (Launceston) | 153 | 18 | 5 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Campbell, S.L.; Remenyi, T.A.; Williamson, G.J.; White, C.J.; Johnston, F.H. The Value of Local Heatwave Impact Assessment: A Case-Crossover Analysis of Hospital Emergency Department Presentations in Tasmania, Australia. Int. J. Environ. Res. Public Health 2019, 16, 3715. https://doi.org/10.3390/ijerph16193715
Campbell SL, Remenyi TA, Williamson GJ, White CJ, Johnston FH. The Value of Local Heatwave Impact Assessment: A Case-Crossover Analysis of Hospital Emergency Department Presentations in Tasmania, Australia. International Journal of Environmental Research and Public Health. 2019; 16(19):3715. https://doi.org/10.3390/ijerph16193715
Chicago/Turabian StyleCampbell, Sharon L., Tomas A. Remenyi, Grant J. Williamson, Christopher J. White, and Fay H. Johnston. 2019. "The Value of Local Heatwave Impact Assessment: A Case-Crossover Analysis of Hospital Emergency Department Presentations in Tasmania, Australia" International Journal of Environmental Research and Public Health 16, no. 19: 3715. https://doi.org/10.3390/ijerph16193715
APA StyleCampbell, S. L., Remenyi, T. A., Williamson, G. J., White, C. J., & Johnston, F. H. (2019). The Value of Local Heatwave Impact Assessment: A Case-Crossover Analysis of Hospital Emergency Department Presentations in Tasmania, Australia. International Journal of Environmental Research and Public Health, 16(19), 3715. https://doi.org/10.3390/ijerph16193715






