Association between Psychosocial Working Conditions and Perceived Physical Exertion among Eldercare Workers: A Cross-Sectional Multilevel Analysis of Nursing Homes, Wards and Workers
Abstract
1. Introduction
2. Materials and Methods
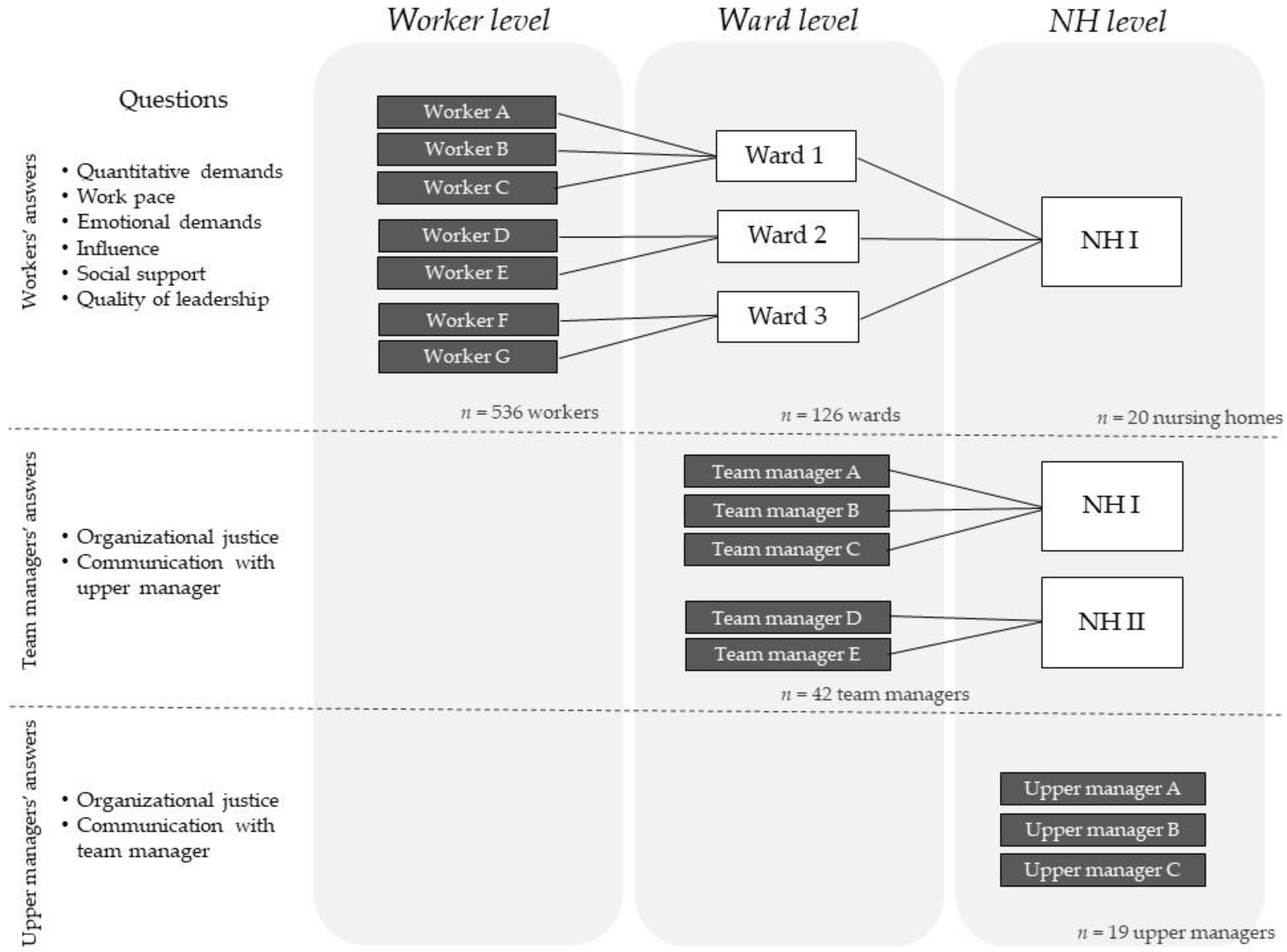
2.1. Study Population
2.2. Data Collection
2.2.1. Psychosocial Working Conditions (Predictors)
2.2.2. Perceived Physical Exertion (Outcome)
2.2.3. Covariates
2.3. Statistical Analysis
3. Results
3.1. Descriptive Characteristics of the Study Population
3.2. Association between Psychosocial Conditions Reported by Workers and Physical Exertion
3.3. Association between Psychosocial Conditions Reported by Managers and Physical Exertion
4. Discussion
4.1. Psychosocial Data Provided by Eldercare Workers
4.2. Psychosocial Data Provided by Managers
4.3. Methodological Considerations
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Pelissier, C.; Fontana, L.; Fort, E.; Agard, J.P.; Couprie, F.; Delaygue, B.; Glerant, V.; Perrier, C.; Sellier, B.; Vohito, M.; et al. Occupational risk factors for upper-limb and neck musculoskeletal disorder among health-care staff in nursing homes for the elderly in France. Ind. Health 2014, 52, 334–346. [Google Scholar] [CrossRef] [PubMed]
- Clausen, T.; Andersen, L.L.; Holtermann, A.; Jorgensen, A.F.B.; Aust, B.; Rugulies, R. Do self-reported psychosocial working conditions predict low back pain after adjustment for both physical work load and depressive symptoms? A prospective study among female eldercare workers. Occup. Environ. Med. 2013, 70, 538–544. [Google Scholar] [CrossRef] [PubMed]
- Taulaniemi, A.; Kuusinen, L.; Tokola, K.; Kankaanpãã, M.; Suni, J. Bio-psychosocial factors are associated with pain intensity, physical functioning, and ability to work in female healthcare personnel with recurrent low back pain. J. Rehabil. Med. 2017, 49, 667–676. [Google Scholar] [CrossRef] [PubMed]
- Clausen, T.; Nielsen, K.; Carneiro, I.G.; Borg, V. Job demands, job resources and long-term sickness absence in the Danish eldercare services: A prospective analysis of register-based outcomes. J. Adv. Nurs. 2012, 68, 127–136. [Google Scholar] [CrossRef] [PubMed]
- Andersen, L.L.; Clausen, T.; Persson, R.; Holtermann, A. Perceived physical exertion during healthcare work and risk of chronic pain in different body regions: Prospective cohort study. Int. Arch. Occup. Environ. Health 2013, 86, 681–687. [Google Scholar] [CrossRef] [PubMed]
- Gonge, H.; Jensen, L.D.; Bonde, J.P. Do psychosocial strain and physical exertion predict onset of low-back pain among nursing aides? Scand. J. Work Environ. Health 2001, 27, 388–394. [Google Scholar] [CrossRef] [PubMed]
- Jensen, L.D.; Ryom, P.K.; Christensen, M.V.; Andersen, J.H. Differences in risk factors for voluntary early retirement and disability pension: A 15-year follow-up in a cohort of nurses’ aides. BMJ Open 2012, 2, e000991. [Google Scholar] [CrossRef][Green Version]
- Andersen, L.L.; Villadsen, E.; Clausen, T. Influence of physical and psychosocial working conditions for the risk of disability pension among healthy female eldercare workers: Prospective cohort. Scand. J. Public Health 2019, 1–8. [Google Scholar] [CrossRef]
- Sejbaek, C.S.; Nexo, M.A.; Borg, V. Work-related factors and early retirement intention: A study of the Danish eldercare sector. Eur. J. Public Health 2013, 23, 611–616. [Google Scholar] [CrossRef][Green Version]
- Yassi, A.; Cooper, J.E.; Tate, R.B.; Gerlach, S.; Muir, M.; Trottier, J.; Massey, K. A randomized controlled trial to prevent patient lift and transfer injuries of health care workers. Spine 2001, 26, 1739–1746. [Google Scholar] [CrossRef]
- Holtermann, A.; Clausen, T.; Jørgensen, M.B.; Aust, B.; Mortensen, O.S.; Burdorf, A.; Fallentin, N.; Andersen, L.L. Does rare use of assistive devices during patient handling increase the risk of low back pain? A prospective cohort study among female healthcare workers. Int. Arch. Occup. Environ. Health 2015, 88, 335–342. [Google Scholar] [CrossRef] [PubMed]
- Gold, J.E.; Punnett, L.; Gore, R.J. Predictors of low back pain in nursing home workers after implementation of a safe resident handling programme. Occup. Environ. Med. 2017, 74, 389–395. [Google Scholar] [CrossRef] [PubMed]
- Hegewald, J.; Berge, W.; Heinrich, P.; Staudte, R.; Freiberg, A.; Scharfe, J.; Girbig, M.; Nienhaus, A.; Seidler, A. Do technical aids for patient handling prevent musculoskeletal complaints in health care workers?—A systematic review of intervention studies. Int. J. Environ. Res. Public Health 2018, 15, 476. [Google Scholar] [CrossRef] [PubMed]
- Koppelaar, E.; Knibbe, J.J.; Miedema, H.S.; Burdorf, A. Determinants of implementation of primary preventive interventions on patient handling in healthcare: A systematic review. Occup. Environ. Med. 2009, 66, 353–360. [Google Scholar] [CrossRef] [PubMed]
- Van Der Beek, A.J.; Dennerlein, J.T.; Huysmans, M.A.; Mathiassen, S.E.; Burdorf, A.; Van Mechelen, W.; Van Dieën, J.H.; Frings-Dresen, M.H.W.; Holtermann, A.; Janwantanakul, P.; et al. A research framework for the development and implementation of interventions preventing work-related musculoskeletal disorders. Scand. J. Work Environ. Health 2017, 43, 526–539. [Google Scholar] [CrossRef]
- Roquelaure, Y. Musculoskeletal Disorders and Psychosocial Factors at Work. ETUI Res. Pap. Rep. 2018, 142, 29–48. [Google Scholar] [CrossRef]
- Bongers, P.M.; Ijmker, S.; Van Den Heuvel, S.; Blatter, B.M. Epidemiology of work related neck and upper limb problems: Psychosocial and personal risk factors (Part I) and effective interventions from a bio behavioural perspective (Part II). J. Occup. Rehabil. 2006, 16, 279–302. [Google Scholar] [CrossRef]
- Koppelaar, E.; Knibbe, J.J.; Miedema, H.S.; Burdorf, A. The influence of individual and organisational factors on nurses’ behaviour to use lifting devices in healthcare. Appl. Ergon. 2013, 44, 532–537. [Google Scholar] [CrossRef]
- Costello, H.; Walsh, S.; Cooper, C.; Livingston, G. A systematic review and meta-analysis of the prevalence and associations of stress and burnout among staff in long-term care facilities for people with dementia. Int. Psychogeriatr. 2018, 31, 1203–1216. [Google Scholar] [CrossRef]
- Aronsson, G.; Theorell, T.; Grape, T.; Hammarström, A.; Hogstedt, C.; Marteinsdottir, I.; Skoog, I.; Träskman-Bendz, L.; Hall, C. A systematic review including meta-analysis of work environment and burnout symptoms. BMC Public Health 2017, 17, 264. [Google Scholar] [CrossRef]
- Vogel, B.; De Geest, S.; Fierz, K.; Beckmann, S.; Zúñiga, F. Dementia care worker stress associations with unit type, resident, and work environment characteristics: A cross-sectional secondary data analysis of the Swiss Nursing Homes Human Resources Project (SHURP). Int. Psychogeriatr. 2017, 29, 441–454. [Google Scholar] [CrossRef] [PubMed]
- Elovainio, M.; Heponiemi, T.; Sinervo, T.; Magnavita, N. Organizational justice and health; review of evidence. G. Ital. Med. Lav. Ergon. 2010, 32, B5–B9. [Google Scholar] [PubMed]
- Bao, S.S.; Kapellusch, J.M.; Merryweather, A.S.; Thiese, M.S.; Garg, A.; Hegmann, K.T.; Silverstein, B.A. Relationships between job organisational factors, biomechanical and psychosocial exposures. Ergonomics 2016, 59, 179–194. [Google Scholar] [CrossRef] [PubMed]
- Thiese, M.S.; Hegmann, K.T.; Kapellusch, J.; Merryweather, A.; Bao, S.; Silverstein, B.; Garg, A. Associations between Distal Upper Extremity Job Physical Factors and Psychosocial Measures in a Pooled Study. Biomed Res. Int. 2015, 2015, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Eijckelhof, B.H.W.; Huysmans, M.A.; Bruno Garza, J.L.; Blatter, B.M.; Van Dieën, J.H.; Dennerlein, J.T.; Van Der Beek, A.J. The effects of workplace stressors on muscle activity in the neck-shoulder and forearm muscles during computer work: A systematic review and meta-analysis. Eur. J. Appl. Physiol. 2013, 113, 2897–2912. [Google Scholar] [CrossRef] [PubMed]
- Simon, M.; Tackenberg, P.; Nienhaus, A.; Estryn-Behar, M.; Maurice Conway, P.; Hasselhorn, H.M. Back or neck-pain-related disability of nursing staff in hospitals, nursing homes and home care in seven countries—results from the European NEXT-Study. Int. J. Nurs. Stud. 2008, 45, 24–34. [Google Scholar] [CrossRef] [PubMed]
- Hagberg, M.; Punnett, L.; Bergqvist, U.; Burdorf, A.; Härenstam, A.; Kristensen, T.S.; Lillienberg, L.; Quinn, M.; Smith, T.J.; Westberg, H. Consensus report. Broadening the view of exposure assessment. Scand. J. Work Environ. Health 2001, 27, 354–357. [Google Scholar] [CrossRef]
- Marklund, S.; Bolin, M.; von Essen, J. Can individual health differences be explained by workplace characteristics?-A multilevel analysis. Soc. Sci. Med. 2008, 66, 650–662. [Google Scholar] [CrossRef] [PubMed]
- Hjarsbech, P.U.; Christensen, K.B.; Andersen, R.V.; Borg, V.; Aust, B.; Rugulies, R. Do psychosocial working conditions modify the effect of depressive symptoms on long-term sickness absence? Am. J. Ind. Med. 2013, 56, 1329–1340. [Google Scholar] [CrossRef] [PubMed]
- Christensen, K.B.; Nielsen, M.L.; Rugulies, R.; Smith-Hansen, L.; Kristensen, T.S. Workplace levels of psychosocial factors as prospective predictors of registered sickness absence. J. Occup. Environ. Med. 2005, 47, 933–940. [Google Scholar] [CrossRef]
- Rugulies, R. Studying the effect of the psychosocial work environment on risk of ill-health: Towards a more comprehensive assessment of working conditions. Scand. J. Work Environ. Health 2012, 38, 187–191. [Google Scholar] [CrossRef] [PubMed]
- Honda, A.; Date, Y.; Abe, Y.; Aoyagi, K.; Honda, S. Communication, support and psychosocial work environment affecting psychological distress among working women aged 20 to 39 years in Japan. Ind. Health 2016, 54, 5–13. [Google Scholar] [CrossRef] [PubMed]
- Karstad, K.; Jørgensen, A.F.B.; Greiner, B.A.; Burdorf, A.; Søgaard, K.; Rugulies, R.; Holtermann, A. Danish Observational Study of Eldercare work and musculoskeletal disorderS (DOSES): A prospective study at 20 nursing homes in Denmark. BMJ Open 2018, 8, e019670. [Google Scholar] [CrossRef] [PubMed]
- Pejtersen, J.H.; Kristensen, T.S.; Borg, V.; Bjorner, J.B. The second version of the Copenhagen Psychosocial Questionnaire. Scand. J. Public Health 2010, 38, 8–24. [Google Scholar] [CrossRef] [PubMed]
- Borg, G.A. Psychophysical bases of perceived exertion. Med. Sci. Sports Exerc. 1982, 14, 377–381. [Google Scholar] [CrossRef] [PubMed]
- Lallukka, T.; Viikari-Juntura, E.; Viikari, J.; Kähönen, M.; Lehtimäki, T.; Raitakari, O.T.; Solovieva, S. Early work-related physical exposures and low back pain in midlife: The Cardiovascular Risk in Young Finns Study. Occup. Environ. Med. 2017, 74, 163–168. [Google Scholar] [CrossRef] [PubMed]
- Andersen, L.L.; Clausen, T.; Persson, R.; Holtermann, A. Dose–response relation between perceived physical exertion during healthcare work and risk of long-term sickness absence. Scand. J. Work Environ. Health 2012, 38, 582–589. [Google Scholar] [CrossRef] [PubMed]
- Lagerström, M.; Hansson, T.; Hagberg, M. Work-related low-back problems in nursing. Scand. J. Work Environ. Health 1998, 24, 449–464. [Google Scholar] [CrossRef] [PubMed]
- Nabe-Nielsen, K.; Tüchsen, F.; Christensen, K.B.; Garde, A.H.; Diderichsen, F. Differences between day and nonday workers in exposure to physical and psychosocial work factors in the Danish eldercare sector. Scand. J. Work Environ. Health 2009, 35, 48–55. [Google Scholar] [CrossRef]
- Saltin, B.; Grimby, G. Physiological analysis of middle-aged and old former athletes. Comparison with still active athletes of the same ages. Circulation 1968, 38, 1104–1115. [Google Scholar] [CrossRef]
- Andersen, L.L.; Clausen, T.; Mortensen, O.S.; Burr, H.; Holtermann, A. A prospective cohort study on musculoskeletal risk factors for long-term sickness absence among healthcare workers in eldercare. Int. Arch. Occup. Environ. Health 2012, 85, 615–622. [Google Scholar] [CrossRef] [PubMed]
- Trinkoff, A.M.; Johantgen, M.; Muntaner, C.; Le, R. Staffing and worker injury in nursing homes. Am. J. Public Health 2005, 95, 1220–1225. [Google Scholar] [CrossRef] [PubMed]
- Heck, R.; Thomas, S.; Tabata, L. Multilevel and Longitudinal Modeling with IBM SPSS, 2nd ed.; Quantitative Methodology Series; Routledge: New York, NY, USA, 2013; ISBN 978-0-203-70124-9. [Google Scholar]
- Mathieu, J.E.; Taylor, S.R. A framework for testing meso-mediational relationships in Organizational Behavior. J. Organ. Behav. 2007, 28, 141–172. [Google Scholar] [CrossRef]
- Peugh, J.L.; Enders, C.K. Using the SPSS Mixed Procedure to Fit Cross-Sectional and Longitudinal Multilevel Models. Educ. Psychol. Meas. 2005, 65, 717–741. [Google Scholar] [CrossRef]
- Podsakoff, P.M.; MacKenzie, S.B.; Lee, J.Y.; Podsakoff, N.P. Common Method Biases in Behavioral Research: A Critical Review of the Literature and Recommended Remedies. J. Appl. Psychol. 2003, 88, 879–903. [Google Scholar] [CrossRef] [PubMed]
- Fjell, Y.; Österberg, M.; Alexanderson, K.; Karlqvist, L.; Bildt, C. Appraised leadership styles, psychosocial work factors, and musculoskeletal pain among public employees. Int. Arch. Occup. Environ. Health 2007, 81, 19–30. [Google Scholar] [CrossRef] [PubMed]
- Nabe-Nielsen, K.; Fallentin, N.; Christensen, K.B.; Jensen, J.N.; Diderichsen, F. Comparison of two self-reported measures of physical work demands in hospital personnel: A cross-sectional study. BMC Musculoskelet. Disord. 2008, 9, 61. [Google Scholar] [CrossRef] [PubMed]
- Fjelltun, A.M.; Henriksen, N.; Norberg, A.; Gilje, F.; Normann, H.K. Functional levels and nurse workload of elderly awaiting nursing home placement and nursing home residents: A comparative study. Scand. J. Caring Sci. 2009, 23, 736–747. [Google Scholar] [CrossRef] [PubMed]
- Mathiassen, S.E.; Winkel, J. Physiological comparison of three interventions in light assembly work: Reduced work pace, increased break allowance and shortened working days. Int. Arch. Occup. Environ. Health 1996, 68, 94–108. [Google Scholar] [CrossRef] [PubMed]
- Januario, L.B.; Madeleine, P.; Cid, M.M.; Samani, A.; Oliveira, A.B. Can exposure variation be promoted in the shoulder girdle muscles by modifying work pace and inserting pauses during simulated assembly work? Appl. Ergon. 2018, 66, 151–160. [Google Scholar] [CrossRef] [PubMed]
- Escorpizo, R.; Moore, A. The effects of cycle time on the physical demands of a repetitive pick-and-place task. Appl. Ergon. 2007, 38, 609–615. [Google Scholar] [CrossRef] [PubMed]
- Kivimäki, M.; Elovainio, M.; Vahtera, J.; Ferrie, J.E. Organisational justice and health of employees: Prospective cohort study. Occup. Environ. Med. 2003, 60, 27–33. [Google Scholar] [CrossRef] [PubMed]
- Hauke, A.; Flintrop, J.; Brun, E.; Rugulies, R. The impact of work-related psychosocial stressors on the onset of musculoskeletal disorders in specific body regions: A review and meta-analysis of 54 longitudinal studies. Work Stress 2011, 25, 243–256. [Google Scholar] [CrossRef]
- Torp, S.; Riise, T.; Moen, B.E. The impact of psychosocial work factors on musculoskeletal pain: A prospective study. J. Occup. Environ. Med. 2001, 43, 120–126. [Google Scholar] [CrossRef] [PubMed]
- Munch-Hansen, T.; Wieclaw, J.; Agerbo, E.; Westergaard-Nielsen, N.; Bonde, J.P. Global measure of satisfaction with psychosocial work conditions versus measures of specific aspects of psychosocial work conditions in explaining sickness absence. BMC Public Health 2008, 8, 270. [Google Scholar] [CrossRef] [PubMed]
- Tehseen, S.; Ramayah, T.; Sajilan, S. Testing and Controlling for Common Method Variance: A Review of Available Methods. J. Manag. Sci. 2017, 4, 142–168. [Google Scholar] [CrossRef]
- Jakobsen, M.D.; Sundstrup, E.; Brandt, M.; Jay, K.; Aagaard, P.; Andersen, L.L. Physical exercise at the workplace reduces perceived physical exertion during healthcare work: Cluster randomized controlled trial. Scand. J. Public Health 2015, 43, 713–720. [Google Scholar] [CrossRef]
- Koch, M.; Lunde, L.K.; Gjulem, T.; Knardahl, S.; Veiersted, K.B. Validity of questionnaire and representativeness of objective methods for measurements of mechanical exposures in construction and health care work. PLoS ONE 2016, 11, e0162881. [Google Scholar] [CrossRef]
- Kwak, L.; Proper, K.I.; Hagströmer, M.; Sjöström, M. The repeatability and validity of questionnaires assessing occupational physical activity - a systematic review. Scand. J. Work Environ. Health 2011, 37, 6–29. [Google Scholar] [CrossRef]
- Unge, J.; Hansson, G.Å.; Ohlsson, K.; Nordander, C.; Axmon, A.; Winkel, J.; Skerfving, S. Validity of self-assessed reports of occurrence and duration of occupational tasks. Ergonomics 2005, 48, 12–24. [Google Scholar] [CrossRef]
| Variables | Mean (SD) | Variance Components | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Nursing Home Level | Ward Level | Worker Level | ||||||||
| Variance | 95% CI | ICC | Variance | 95% CI | ICC | Variance | 95% CI | ICC | ||
| Eldercare workers’ responses | ||||||||||
| Physical exertion (0–10) | 6.8 (2.0) | 0.2 | 0.1–0.7 | 5.6 | 0.4 | 0.2–0.9 | 11.1 * | 3.2 | 2.8–3.7 | 83.3 * |
| Quantitative demands (0–100) | 44.4 (20.2) | 38.0 | 14.2–101.4 | 9.1 * | 11.5 | 1.1–124.3 | 2.8 | 365.4 | 319.5–417.9 | 88.1 * |
| Work pace (0–100) | 60.9 (18.0) | 22.1 | 6.4–75.8 | 6.7 | 22.4 | 7.7–65.3 | 6.8 ** | 283.2 | 247.7–323.7 | 86.4 * |
| Emotional demands (0–100) | 51.4 (15.5) | 2.9 | 0.2–35.4 | 1.2 | 6.5 | 0.4–97.7 | 2.7 | 232.6 | 203.0–266.5 | 96.1 * |
| Influence (0–100) | 57.1 (19.7) | 19.0 | 5.6–64.6 | 4.9 | 16.3 | 2.4–111.5 | 4.2 | 353.1 | 308.1–404.6 | 90.9 * |
| Social support (0–100) | 71.7 (17.4) | 6.3 | 0.9–43.0 | 2.5 | 13.9 | 3.5–54.9 | 5.5 | 232.2 | 203.2–265.2 | 92.0 * |
| Quality of leadership (0–100) | 60.6 (17.4) | 58.1 | 25.5–132.2 | 19.1 * | 40.2 | 21.0–76.9 | 13.2 * | 205.9 | 179.6–235.9 | 67.7 * |
| Team managers’ responses | ||||||||||
| Communication (0–10) | 8.3 (2.3) | 4.8 | 2.5–9.1 | 80.5 * | 1.2 | 1.0–1.3 | 19.5 * | |||
| Justice (0–100) | 71.6 (15.5) | 117.2 | 59.3–231.8 | 44.7 * | 145.3 | 128.6–164.2 | 55.3 * | |||
| Upper managers’ responses | ||||||||||
| Communication (0–10) | 9.1 (1.0) | 1.0 | 0.9–1.1 | 100.0 † | ||||||
| Justice (0–100) | 75.0 (10.8) | 116.7 | 101.1–134.6 | 100.0 † | ||||||
| Predictors | Crude Model | Adjusted Model a | ||||
|---|---|---|---|---|---|---|
| Β | p | 95% CI | Β | p | 95% CI | |
| Quantitative demands | ||||||
| Nursing home level | −0.015 | 0.50 | −0.059–0.029 | −0.019 | 0.40 | −0.065–0.026 |
| Ward level | 0.020 | 0.07 | −0.002–0.041 | 0.025 | 0.03 | 0.003–0.048 |
| Worker level | 0.025 | <0.001 | 0.016–0.033 | 0.025 | <0.001 | 0.015–0.034 |
| Pace | ||||||
| Nursing home level | −0.014 | 0.55 | −0.060–0.032 | −0.027 | 0.24 | −0.073–0.019 |
| Ward level | 0.041 | <0.001 | 0.019–0.062 | 0.045 | <0.001 | 0.023–0.067 |
| Worker level | 0.027 | <0.001 | 0.017–0.037 | 0.026 | <0.001 | 0.016–0.037 |
| Emotional demands | ||||||
| Nursing home level | −0.061 | 0.23 | −0.164–0.041 | −0.060 | 0.23 | −0.157–0.040 |
| Ward level | 0.009 | 0.51 | −0.018–0.037 | 0.022 | 0.15 | −0.008–0.052 |
| Worker level | 0.019 | <0.001 | 0.008–0.030 | 0.017 | 0.01 | 0.006–0.029 |
| Influence | ||||||
| Nursing home level | −0.045 | 0.07 | −0.094–0.004 | −0.066 | 0.01 | −(0.115–0.016) |
| Ward level | 0.002 | 0.86 | −0.020–0.024 | 0.006 | 0.58 | −0.017–0.030 |
| Worker level | −0.017 | <0.001 | −(0.027–0.008) | −0.019 | <0.001 | −(0.029–0.010) |
| Social support | ||||||
| Nursing home level | −0.008 | 0.83 | −0.083–0.067 | −0.032 | 0.38 | −0.110–0.042 |
| Ward level | −0.018 | 0.18 | −0.045–0.008 | −0.009 | 0.52 | −0.039–0.020 |
| Worker level | −0.012 | 0.04 | −0.023–0.000 | −0.013 | 0.04 | −(0.025–0.001) |
| Quality of leadership | ||||||
| Nursing home level | −0.034 | 0.09 | −0.074–0.005 | −0.047 | 0.02 | −(0.086–0.008) |
| Ward level | 0.014 | 0.29 | −0.012–0.040 | 0.016 | 0.24 | −0.011–0.044 |
| Worker level | −0.017 | 0.01 | −(0.030–0.005) | −0.013 | 0.05 | −0.025–0.000 |
| Predictors | Crude Model | Adjusted Model a | ||||
|---|---|---|---|---|---|---|
| β | p | 95% CI | β | p | 95% CI | |
| Team managers’ responses | ||||||
| Communication (0–10) | ||||||
| Nursing home level | 0.003 | 0.98 | −0.232–0.237 | 0.022 | 0.85 | −0.218–0.263 |
| Ward level | −0.007 | 0.94 | −0.193–0.180 | −0.016 | 0.87 | −0.220–0.186 |
| Justice (0–100) | ||||||
| Nursing home level | 0.009 | 0.58 | −0.024–0.042 | 0.004 | 0.76 | −0.026–0.035 |
| Ward level | −0.022 | 0.01 | −(0.038–0.006) | −0.022 | 0.01 | −(0.038–0.005) |
| Upper managers’ responses | ||||||
| Communication (0–10) | −0.097 | 0.50 | −0.403–0.208 | −0.062 | 0.63 | −0.318–0.194 |
| Justice (0–100) | −0.004 | 0.79 | −0.034–0.026 | −0.003 | 0.77 | −0.031–0.023 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Januario, L.B.; Karstad, K.; Rugulies, R.; Bergström, G.; Holtermann, A.; Hallman, D.M. Association between Psychosocial Working Conditions and Perceived Physical Exertion among Eldercare Workers: A Cross-Sectional Multilevel Analysis of Nursing Homes, Wards and Workers. Int. J. Environ. Res. Public Health 2019, 16, 3610. https://doi.org/10.3390/ijerph16193610
Januario LB, Karstad K, Rugulies R, Bergström G, Holtermann A, Hallman DM. Association between Psychosocial Working Conditions and Perceived Physical Exertion among Eldercare Workers: A Cross-Sectional Multilevel Analysis of Nursing Homes, Wards and Workers. International Journal of Environmental Research and Public Health. 2019; 16(19):3610. https://doi.org/10.3390/ijerph16193610
Chicago/Turabian StyleJanuario, Leticia Bergamin, Kristina Karstad, Reiner Rugulies, Gunnar Bergström, Andreas Holtermann, and David M. Hallman. 2019. "Association between Psychosocial Working Conditions and Perceived Physical Exertion among Eldercare Workers: A Cross-Sectional Multilevel Analysis of Nursing Homes, Wards and Workers" International Journal of Environmental Research and Public Health 16, no. 19: 3610. https://doi.org/10.3390/ijerph16193610
APA StyleJanuario, L. B., Karstad, K., Rugulies, R., Bergström, G., Holtermann, A., & Hallman, D. M. (2019). Association between Psychosocial Working Conditions and Perceived Physical Exertion among Eldercare Workers: A Cross-Sectional Multilevel Analysis of Nursing Homes, Wards and Workers. International Journal of Environmental Research and Public Health, 16(19), 3610. https://doi.org/10.3390/ijerph16193610






