Risk Factors for Obstructive Sleep Apnea Syndrome in Children: State of the Art
Abstract
1. Introduction
2. Risk Factors
2.1. Obesity
2.2. Adenoid and/or Tonsil Hypertrophy
2.3. Allergic Rhinitis
2.4. Craniofacial Abnormalities and Genetics
2.5. Inflammatory Factors and Biomarkers
3. Clinical Presentation
4. Diagnosis
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
Abbreviations
| AASM | American Association Sleep Medicine |
| AHI | Apnea-Hypopnea index |
| AT | Adenotonsillectomy |
| AR | Allergic Rhinitis |
| BMI | Body Mass Index |
| CPAP | Continuous Positive Airway Pressure |
| CRP | Reactive C- Protein |
| DISE | Drug Induced Sleep Endoscopy |
| ERS | European Respiratory Society |
| ESS | Epworth Sleepiness Scale |
| ICSD-3 | International Classification of Sleep Disorders |
| ODI | Oxygen Desaturation Index |
| OSA | Obstructive sleep apnea |
| OSAS | Obstructive sleep apnea syndrome |
| PSG | Polysomnography |
| PSQ | Pediatric Sleep Questionnaire |
| RDI | Respiratory Disease Index |
| REM | Rapid Eye Movement |
| RERAs | Respiratory Effort Related Arousal |
| RSD | Respiratory Sleep Disorder |
| SSSDR | Sleeping Sleepless Sleepy Disturbed Rest questionnaire |
References
- Schechter, M.S. Technical report: Diagnosis and management of childhood obstructive sleep apnea syndrome. Pediatrics 2002, 109, 69. [Google Scholar] [CrossRef] [PubMed]
- Gozal, D.; Kheirandish-Gozal, L. Obesity and excessive daytime sleepiness in prepubertal children with obstructive sleep apnea. Pediatrics 2009, 123, 13–18. [Google Scholar] [CrossRef] [PubMed]
- American Academy of Sleep Medicine. International Classification of Sleep Disorders, 3rd ed.; American Academy of Sleep Medicine: Darien, IL, USA, 2014. [Google Scholar]
- Berry, R.B.; Budhiraja, R.; Gottlieb, D.J.; Gozal, D.; Iber, C.; Kapur, V.K.; Marcus, C.L.; Mehra, R.; Parthasarathy, S.; Quan, S.F.; et al. The AASM Manual for the Scoring of Sleep and Associated Events: Rules, Terminology and Technical Specifications. Version 2.3; American Academy of Sleep Medicine: Darien, IL, USA, 2016. [Google Scholar]
- Ruehland, W.R.; Rochford, P.D.; O’Donoghue, F.J.; Pierce, R.J.; Singh, P.; Thornton, A.T. The new AASM criteria for scoring hypopneas: Impact on the apnea hypopnea index. Sleep 2009, 32, 150–157. [Google Scholar] [CrossRef] [PubMed]
- Redline, S.; Kapur, V.K.; Sanders, M.H.; Quan, S.F.; Gottlieb, D.J.; Rapoport, D.M.; Bonekat, W.H.; Smith, P.L.; Kiley, J.P.; Iber, C. Effects of varying approaches for identifying respiratory disturbances on sleep apnea assessment. Am. J. Respir. Crit. Care. Med. 2000, 161, 369–374. [Google Scholar] [CrossRef] [PubMed]
- Duce, B.; Milosavljevic, J.; Hukins, C. The 2012 AASM respiratory event criteria increase the incidence of hypopneas in an adult sleep center population. J. Clin. Sleep Med. 2015, 11, 1425–1431. [Google Scholar] [CrossRef] [PubMed]
- Vicini, C.; De Vito, A.; Iannella, G.; Gobbi, R.; Corso, R.M.; Montevecchi, F.; Polimeni, A.; De Vincentiis, M.; Meccariello, G.; D’agostino, G.; et al. The aging effect on upper airways collapse of patients with obstructive sleep apnea syndrome. Eur. Arch. Otorhinolaryngol. 2018, 275, 2983–2990. [Google Scholar] [CrossRef] [PubMed]
- Marcus, C.L.; Brooks, L.J.; Draper, K.A.; Gozal, D.; Halbower, A.C.; Jones, J.; Schechter, M.S.; Ward, S.D.; Sheldon, S.H.; Shiffman, R.N.; et al. Diagnosis and Management of Childhood Obstructive Sleep Apnea Syndrome. Pediatrics 2012, 130, 576–584. [Google Scholar] [CrossRef] [PubMed]
- Katz, E.S.; D’Ambrosio, C.M. Pathophysiology of Pediatric Obstructive Sleep Apnea. Proc. Am. Thorac. Soc. 2008, 5, 253–262. [Google Scholar] [CrossRef]
- Kaditis, A.G.; Alonso Alvarez, M.L.; Boudewyns, A.; Alexopoulos, E.I.; Ersu, R.; Joosten, K.; Larramona, H.; Miano, S.; Narang, I.; Trang, H.; et al. Obstructive sleep disordered breathing in 2- to 18-year-old children: Diagnosis and management. Eur. Respir. J. 2016, 47, 69–94. [Google Scholar] [CrossRef]
- Carter, K.A.; Hathaway, N.E.; Lettieri, C.F. Common sleep disorders in children. Am. Fam. Physician 2014, 89, 368–377. [Google Scholar]
- Gozal, D.; Kheirandish-Gozal, L. New approaches to the diagnosis of sleep-disordered breathing in children. Sleep Med. 2010, 11, 708–713. [Google Scholar] [CrossRef] [PubMed]
- Tan, H.L.; Gozal, D.; Kheirandish-Gozal, L. Obstructive sleep apnea in children: A critical update. Nat. Sci. Sleep 2013, 5, 109–123. [Google Scholar] [PubMed]
- Lumeng, J.C.; Chervin, R.D. Epidemiology of pediatric obstructive sleep apnea. Proc. Am. Thorac. Soc. 2008, 5, 242–252. [Google Scholar] [CrossRef] [PubMed]
- Li, Z.; Celestin, J.; Lockey, R.F. Pediatric Sleep Apnea Syndrome: An Update. J. Allergy Clin. Immunol. Pract. 2016, 4, 852–861. [Google Scholar] [CrossRef] [PubMed]
- Van de Graaff, W.B. Thoracic traction on the trachea: Mechanisms and magnitude. J. Appl. Physiol. 1991, 70, 1328–1336. [Google Scholar] [CrossRef] [PubMed]
- Arens, R.; Sin, S.; Nandalike, K.; Rieder, J.; Khan, U.I.; Freeman, K.; Wylie-Rosett, J.; Lipton, M.L.; Wootton, D.M.; McDonough, J.M.; et al. Upper airway structure and body fat composition in obese children with obstructive sleep apnea syndrome. Am. J. Respir. Crit. Care Med. 2011, 183, 782–787. [Google Scholar] [CrossRef] [PubMed]
- Hannon, T.S.; Rofey, D.L.; Ryan, C.M.; Clapper, D.A.; Chakravorty, S.; Arslanian, S.A. Relationships among obstructive sleep apnea, anthropometric measures, and neurocognitive functioning in adolescents with severe obesity. J. Pediatr. 2012, 160, 732–735. [Google Scholar] [CrossRef] [PubMed]
- NCD Risk Factor Collaboration (NCD-RisC). Worldwide trends in body-mass index, underweight, overweight, and obesity from 1975 to 2016: A pooled analysis of 2416 population-based measurement studies in 128·9 million children, adolescents, and adults. Lancet 2017, 390, 2627–2642. [Google Scholar] [CrossRef]
- Su, M.S.; Zhang, H.L.; Cai, X.H.; Lin, Y.; Liu, P.N.; Zhang, Y.B.; Hu, W.Z.; Li, C.C.; Xiao, Y.F. Obesity in children with different risk factors for obstructive sleep apnea: A community-based study. Eur. J. Pediatr. 2016, 175, 211–220. [Google Scholar] [CrossRef]
- O’Brien, I.M.; Sitha, S.; Baur, L.A.; Waters, K.A. Obesity increases the risk for persisting obstructive sleep apnea after treatment in children. Int. J. Pediatr. Otorhinolaryngol. 2006, 70, 1555–1560. [Google Scholar] [CrossRef]
- Mitchell, R.B.; Kelly, J. Outcome of adenotonsillectomy for obstructive sleep apnea in obese and normal-weight children. Otolaryngol. Head Neck Surg. 2007, 137, 43–48. [Google Scholar] [CrossRef] [PubMed]
- Marcus, C.L.; Rosen, G.; Ward, S.L.; Halbower, A.C.; Sterni, L.; Lutz, J.; Stading, P.J.; Bolduc, D.; Gordon, N. Adherence to and effectiveness of positive airway pressure therapy in children with obstructive sleep apnea. Pediatrics 2006, 117, e442–e451. [Google Scholar] [CrossRef] [PubMed]
- Marcus, C.L.; Ward, S.L.; Mallory, G.B.; Rosen, C.L.; Beckerman, R.C.; Weese-Mayer, D.E.; Brouillette, R.T.; Trang, H.T.; Brooks, L.J. Use of nasal continuous positive airway pressure as treatment of childhood obstructive sleep apnea. J. Pediatr. 1995, 127, 88–94. [Google Scholar] [CrossRef]
- Xu, Z.; Jiaqing, A.; Yuchuan, L.; Shen, K. A case-control study of obstructive sleep apnea-hypopnea syndrome in obese and nonobese Chinese children. Chest 2008, 133, 684–689. [Google Scholar] [CrossRef] [PubMed]
- Verhulst, S.L.; Franckx, H.; Van Gaal, L.; De Backer, W.; Desager, K. The effect of weight loss on sleep-disordered breathing in obese teenagers. Obesity 2009, 17, 1178–1183. [Google Scholar] [PubMed]
- Siegfried, W.; Siegfried, A.; Rabenbauer, M.; Hebebrand, J. Snoring and sleep apnea in obese adolescents: Effect of long-term weight loss-rehabilitation. Sleep Breath. 1999, 3, 83–88. [Google Scholar] [CrossRef]
- Van Hoorenbeeck, K.; Franckx, H.; Debode, P.; Aerts, P.; Wouters, K.; Ramet, J.; Van Gaal, L.F.; Desager, K.N.; De Backer, W.A.; Verhulst, S.L. Weight loss and sleep-disordered breathing in childhood obesity: Effects on inflammation and uric acid. Obesity 2012, 20, 172–177. [Google Scholar] [CrossRef]
- Andersen, I.G.; Holmb, J.C.; Homøea, P. Impact of weight-loss management on children and adolescents with obesity and obstructive sleep apnea. Int. J. Pediatr. Otorhinolaryngol. 2019, 123, 57–62. [Google Scholar] [CrossRef]
- Marcus, C.L. Pathophysiology of childhood obstructive sleep apnea: Current concepts. Respir. Physiol. 2000, 119, 143–154. [Google Scholar] [CrossRef]
- Jeans, W.D.; Fernando, D.C.; Maw, A.R.; Leighton, B.C. A longitudinal study of the growth of the nasopharynx and its contents in normal children. Br. J. Radiol. 1981, 54, 117–121. [Google Scholar] [CrossRef]
- Kurnatowski, P.; Putynski, L.; Łapienis, M.; Kowalska, B. Physical and emotional disturbances in children with adenotonsillar hypertrophy. J. Laryngol. Otol. 2008, 122, 931–935. [Google Scholar] [CrossRef] [PubMed]
- Brietzke, S.E.; Gallagher, D. The effectiveness of tonsillectomy and adenoidectomy in the treatment of pediatric obstructive sleep apnea/hypopnea syndrome: A meta-analysis. Otolaryngol. Head Neck Surg. 2006, 134, 979–984. [Google Scholar] [CrossRef] [PubMed]
- Tang, A.L.; Cohen, A.P.; Benke, J.R.; Stierer, K.D.; Stanley, J.; Ishman, S.L. Obstructive Sleep Apnea Resolution in Hypopnea- versus Apnea-Predominant Children after Adenotonsillectomy. Otolaryngol. Head Neck Surg. 2016, 155, 670–675. [Google Scholar] [CrossRef] [PubMed]
- El-Kersh, K.; Cavallazzi, R.; Senthilvel, E. Outcomes of adenotonsillectomy in severe pediatric obstructive sleep apnea. Ear Nose Throat J. 2017, 96, E6–E9. [Google Scholar] [PubMed]
- Senchak, A.J.; McKinlay, A.J.; Acevedo, J.; Swain, B.; Tiu, M.C.; Chen, B.S.; Robitschek, J.; Ruhl, D.S.; Williams, L.L.; Camacho, M.; et al. The effect of tonsillectomy alone in adult obstructive sleep apnea. Otolaryngol. Head Neck Surg. 2015, 152, 969–973. [Google Scholar] [CrossRef]
- Kang, K.T.; Koltai, P.J.; Lee, C.H.; Lin, M.T.; Hsu, W.C. Lingual tonsillectomy for treatment of pediatric obstructive sleep apnea: A meta-analysis. JAMA Otolaryngol. Head Neck Surg. 2017, 143, 561–568. [Google Scholar] [CrossRef] [PubMed]
- Iannella, G.; Magliulo, G.; Montevecchi, F.; De Vito, A.; Polimeni, A.; De Vincentiis, M.; Meccariello, G.; D’Agostino, G.; Gobbi, R.; Cammaroto, G.; et al. Lingual tonsil lymphatic tissue regrowth in patients undergoing transoral robotic surgery. Laryngoscope 2018. [Google Scholar] [CrossRef] [PubMed]
- Pynnonen, M.; Brinkmeier, J.V.; Thorne, M.C.; Chong, L.Y.; Burton, M.J. Coblation versus other surgical techniques for tonsillectomy. Cochrane Database Syst. Rev. 2017, 8, CD004619. [Google Scholar] [CrossRef]
- Lee, C.F.; Hsu, W.C.; Lee, C.H.; Lin, M.T.; Kang, K.T. Treatment outcomes of supraglottoplasty for pediatric obstructive sleep apnea: A meta-analysis. Int. J. Pediatr. Otorhinolaryngol. 2016, 87, 18–27. [Google Scholar] [CrossRef]
- Kimple, A.; Ishman, S. Allergy and sleep-disordered breathing. Curr. Opin. Otolaryngol. Head Neck Surg. 2013, 21, 277–281. [Google Scholar] [CrossRef]
- Miljeteig, H.; Hoffstein, V.; Cole, P. The effect of unilateral and bilateral nasal obstruction on snoring and sleep apnoea. Laryngoscope 1992, 102, 1150–1152. [Google Scholar] [CrossRef] [PubMed]
- Young, T.; Finn, L.; Kim, H. Nasal obstruction as a risk factor for sleep-disordered breathing. J. Allergy Clin. Immunol. 1997, 99, S757–S762. [Google Scholar] [CrossRef]
- Magliulo, G.; de Vincentiis, M.; Iannella, G.; Ciofalo, A.; Pasquariello, B.; Manno, A.; Angeletti, D.; Polimeni, A. Olfactory evaluation in obstructive sleep apnoea patients. Acta Otorhinolaryngol. Ital. 2018, 38, 338–345. [Google Scholar] [PubMed]
- Magliulo, G.; Iannella, G.; Ciofalo, A.; Polimeni, A.; de Vincentiis, M.; Pasquariello, B.; Montevecchi, F.; Vicini, C. Nasal pathologies in patients with obstructive sleep apnoea. Acta Otorhinolaryngol. Ital. 2019. [Google Scholar] [CrossRef] [PubMed]
- Lofaso, F.; Coste, A.; d’Ortho, M.P.; Zerah-Lancner, F.; Delclaux, C.; Goldenberg, F.; Harf, A. Nasal obstruction as a risk factor for sleep apnoea syndrome. Eur. Respir. J. 2000, 16, 639–643. [Google Scholar] [CrossRef] [PubMed]
- McNicholas, W.T.; Tarlo, S.; Cole, P.; Zamel, N.; Rutherford, R.; Griffin, D.; Phillipson, E.A. Obstructive apneas during sleep in patients with seasonal allergic rhinitis. Am. Rev. Respir. Dis. 1982, 126, 625–628. [Google Scholar] [PubMed]
- Liistro, G.; Rombaux, P.; Belge, C.; Dury, M.; Aubert, G.; Rodenstein, D.O. High Mallampati score and nasal obstruction are associated risk factors for obstructive sleep apnoea. Eur. Respir. J. 2003, 21, 248–252. [Google Scholar] [CrossRef] [PubMed]
- Di Francesco, R.; Alvarez, J. Allergic rhinitis affects the duration of rapid eye movement sleep in children with sleep-disordered breathing without sleep apnea. Int. Forum Allergy Rhinol. 2016, 6, 465–471. [Google Scholar] [CrossRef]
- Cao, Y.; Wu, S.; Zhang, L.; Yang, Y.; Cao, S.; Li, Q. Association of allergic rhinitis with obstructive sleep apnea: A meta-analysis. Medicine 2018, 97, 13783. [Google Scholar] [CrossRef]
- Kheirandish-Gozal, L.; Bhattacharjee, R.; Bandla, H.P.R.; Gozal, D. Antinflammatory therapy outcomes for mild osa in children. Chest 2014, 146, 88–95. [Google Scholar] [CrossRef]
- Kheirandish-Gozal, L.; Bandla, H.P.; Gozal, D. Montelukast for children with obstructive sleep apnea: Results of a double-blind, randomized, placebocontrolled trial. Ann. Am. Thorac. Soc. 2016, 13, 1736–1741. [Google Scholar] [CrossRef] [PubMed]
- Brouillette, R.T.; Manoukian, J.J.; Ducharme, F.M.; Oudjhane, K.; Earle, L.G.; Ladan, S.; Morielli, A. Efficacy of fluticasone nasal spray for pediatric obstructive sleep apnea. J. Pediatr. 2001, 138, 838–844. [Google Scholar] [CrossRef] [PubMed]
- Myer, C.M., 3rd; Reed, J.M.; Cotton, R.T.; Willging, J.P.; Shott, S.R. Airway management in Pierre Robin sequence. Otolaryngol. Head Neck Surg. 1998, 118, 630–635. [Google Scholar] [CrossRef] [PubMed]
- Scott, A.R.; Tibesar, R.J.; Sidman, J.D. Pierre Robin sequence: Evaluation, management, indications for surgery, and pit-falls. Otolaryngol. Clin. North Am. 2012, 45, 695–710. [Google Scholar] [CrossRef] [PubMed]
- Cohen, M.; Hamilton, J.; Narang, I. Clinically important age-related differences in sleep related disordered breathing in infants and children with Prader-Willi Syndrome. PLoS ONE 2014, 9, 101012. [Google Scholar] [CrossRef] [PubMed]
- Follmar, A.; Dentino, K.; Abramowicz, S.; Padwa, B.L. Prevalence of sleep disordered breathing in patients with Beckwith-Wiedemann syndrome. J. Craniofac. Surg. 2014, 25, 1814–1817. [Google Scholar] [CrossRef]
- Gozal, D.; Capdevila, O.S.; Kheirandish-Gozal, L.; Crabtree, V.M. APOE epsilon 4 allele, cognitive dysfunction, and obstructive sleep apnea in children. Neurology 2007, 69, 243–249. [Google Scholar] [CrossRef]
- Khalyfa, A.; Serpero, L.D.; Kheirandish-Gozal, L.; Capdevila, O.S.; Gozal, D. TNFalpha gene polymorphisms and excessive daytime sleepiness in pediatric obstructive sleep apnea. J. Pediatr. 2011, 158, 77–82. [Google Scholar] [CrossRef]
- Zaffanello, M.; Antoniazzi, F.; Tenero, L.; Nosetti, L.; Piazza, M.; Piacentini, G. Sleep-disordered breathing in paediatric setting: Existing and upcoming of the genetic disorders. Ann. Transl. Med. 2018, 6, 343. [Google Scholar] [CrossRef]
- Onodera, K.; Sakata, H.; Niikuni, N.; Nonaka, T.; Kobayashi, K.; Nakajima, I. Survey of the present status of sleep-disordered breathing in children with achondroplasia Part, I. A questionnaire survey. Int. J. Pediatr. Otorhinolaryngol. 2005, 69, 457–461. [Google Scholar] [CrossRef]
- Collins, W.O.; Choi, S.S. Otolaryngologic manifestations of achondroplasia. Arch. Otolaryngol. Head Neck Surg. 2007, 133, 237–244. [Google Scholar] [CrossRef]
- Cielo, C.M.; Konstantinopoulou, S.; Hoque, R. OSAS in Specific Pediatric Populations. Curr. Probl. Pediatr. Adolesc. Health Care. 2016, 46, 11–18. [Google Scholar] [CrossRef] [PubMed]
- Slaats, M.A.L.J.; Loterman, D.; van Holsbeke, C.; Vos, W.; Van Hoorenbeeck, K.; de Backer, J.; de Backer, W.; Wojciechowski, M.; Boudewyns, A.; Verhulst, S. The Role of Functional Respiratory Imaging in Treatment Selection of Children With Obstructive Sleep Apnea and Down Syndrome. J. Clin. Sleep Med. 2018, 14, 651–659. [Google Scholar] [CrossRef] [PubMed]
- Pavone, M.; Caldarelli, V.; Khirani, S.; Colella, M.; Ramirez, A.; Aubertin, G.; Crinò, A.; Brioude, F.; Gastaud, F.; Beydon, N.; et al. Sleep disordered breathing in patients with Prader-Willi syndrome: A multicenter study. Pediatr. Pulmonol. 2015, 50, 1354–1359. [Google Scholar] [CrossRef] [PubMed]
- Guilleminault, C.; Primeau, M.; Chiu, H.Y.; Yuen, K.M.; Leger, D.; Metlaine, A. Sleep-disordered breathing in Ehlers-Danlos syndrome: A genetic model of OSA. Chest 2013, 144, 1503–1511. [Google Scholar] [CrossRef] [PubMed]
- Robin, P. Glossoptosis due to atresia and hypotrophy of the mandible. Am. J. Dis. Child. 1934, 48, 541–547. [Google Scholar] [CrossRef]
- Kalaskar, R.; Kalaskar, A.R. Oral manifestations of Ellis-van Creveld syndrome. Contemp. Clin. Dent. 2012, 3, S55–S59. [Google Scholar] [CrossRef]
- Strauss, T.; Sin, S.; Marcus, C.L.; Mason, T.B.A.; McDonough, J.M.; Allen, J.L.; Caboot, J.B.; Bowdre, C.Y.; Jawad, A.F.; Smith-Whitley, K.; et al. Upper airway lymphoid tissue size in children with sickle cell disease. Chest 2012, 142, 94–100. [Google Scholar] [CrossRef]
- Cardiel Ríos, S.A. Correction of a severe Class II malocclusion in a patient with Noonan syndrome. Am. J. Orthod. Dentofac. Orthop. 2016, 150, 511–520. [Google Scholar] [CrossRef]
- Marcus, C.L.; Lutz, J.; Carroll, J.L.; Bamford, O. Arousal and ventilatory responses during sleep in children with obstructive sleep apnea. J. Appl. Physiol. 1998, 84, 1926–1936. [Google Scholar] [CrossRef]
- Tauman, R.; Gozal, D. Obstructive sleep apnea syndrome in children. ExpertRev. Respir. Med. 2011, 5, 425–440. [Google Scholar] [CrossRef] [PubMed]
- Saxby, C.; Stephenson, K.A.; Steele, K.; Ifeacho, S.; Wyatt, M.E.; Samuels, M. The Effect of Midface Advancement Surgery on Obstructive Sleep Apnoea in Syndromic Craniosynostosis. J. Craniofac. Surg. 2018, 29, 92–95. [Google Scholar] [CrossRef] [PubMed]
- Verse, T.; Hörmann, K. The surgical treatment of sleep-related upper airway obstruction. Dtsch. Arztebl. Int. 2011, 108, 216–221. [Google Scholar] [CrossRef] [PubMed]
- Camacho, M.; Chang, E.T.; Song, S.A.; Abdullatif, J.; Zaghi, S.; Pirelli, P.; Certal, V.; Guilleminault, C. Rapid maxillary expansion for pediatric obstructive sleep apnea: A systematic review and meta-analysis. Laryngoscope 2017, 127, 1712–1719. [Google Scholar] [CrossRef] [PubMed]
- Villa, M.P.; Bernkopf, E.; Pagani, J.; Broia, V.; Montesano, M.; Ronchetti, R. Randomized controlled study of an oral jaw-positioning appliance for the treatment of obstructive sleep apnea in children with malocclusion. Am. J. Respir. Crit. Care. Med. 2002, 165, 123–127. [Google Scholar] [CrossRef] [PubMed]
- Gileles-Hillel, A.; Alonso-Álvarez, M.L.; Kheirandish-Gozal, L.; Peris, E.; Cordero-Guevara, J.A.; Terán-Santos, J.; Martinez, M.G.; Jurado-Luque, M.J.; Corral-Peñafiel, J.; Duran-Cantolla, J.; et al. Inflammatory markers and obstructive sleep apnea in obese children: The NANOS study. Mediat. Inflamm. 2014, 2014, 605280. [Google Scholar] [CrossRef] [PubMed]
- Tam, C.S.; Wong, M.; McBain, R.; Bailey, S.; Waters, K.A. Inflammatory measures in children with obstructive sleep apnoea. J. Paediatr. Child. Health 2006, 42, 277–282. [Google Scholar] [CrossRef]
- Gozal, D.; Serpero, L.D.; Sans Capdevila, O.; Kheirandish-Gozal, L. Systemic inflammation in non-obese children with obstructive sleep apnea. Sleep Med. 2008, 9, 254–259. [Google Scholar] [CrossRef]
- Ciccone, M.M.; Scicchitano, P.; Mitacchione, G.; Zito, A.; Gesualdo, M.; Caputo, P.; Damiani, M.F.; Sassara, M.; Favale, S.; Resta, O.; et al. Is there a correlation between OSAS duration/severity and carotid intima-media thickness? Respir. Med. 2012, 106, 740–746. [Google Scholar] [CrossRef]
- Lu, D.; Li, N.; Yao, X.; Zhou, L. Potential inflammatory markers in obstructive sleep apnea-hypopnea syndrome. Bosn. J. Basic Med. Sci. 2017, 17, 47–53. [Google Scholar] [CrossRef]
- De Luca Canto, G.; Pacheco-Pereira, C.; Aydinoz, S.; Major, P.W.; Flores-Mir, C.; Gozal, D. Diagnostic capability of biological markers in assessment of obstructive sleep apnea: A systematic review and meta-analysis. J. Clin. Sleep Med. 2015, 11, 27–36. [Google Scholar] [CrossRef] [PubMed]
- De Luca Canto, G.; Pacheco-Pereira, C.; Aydinoz, S.; Major, P.W.; Flores-Mir, C.; Gozal, D. Biomarkers associated with obstructive sleep apnea: A scoping re- view. Sleep Med. Rev. 2014, 23C, 28–45. [Google Scholar]
- Park, C.S.; Guilleminault, C.; Park, H.J.; Cho, J.H.; Lee, H.K.; Son, H.L.; Hwang, S.H. Correlation of salivary alpha amylase level and adenotonsillar hypertrophy with sleep disordered breathing in pediatric subjects. J. Clin. Sleep Med. 2014, 10, 559–566. [Google Scholar] [CrossRef] [PubMed]
- Gozal, D.; Jortani, S.; Snow, A.B.; Kheirandish-Gozal, L.; Bhattacharjee, R.; Kim, J.; Capdevila, O.S. Two-dimensional differential in-gel electrophoresis proteomic approaches reveal urine candidate biomarkers in pediatric obstructive sleep apnea. Am. J. Respir. Crit. Care Med. 2009, 180, 1253–1261. [Google Scholar] [CrossRef] [PubMed]
- Villa, M.P.; Supino, M.C.; Fedeli, S.; Rabasco, J.; Vitelli, O.; Del Pozzo, M.; Gentile, G.; Lionetto, L.; Barreto, M.; Simmaco, M. Urinary concentration of 8-isoprostane as marker of severity of pediatric OSAS. Sleep Breath 2014, 18, 723–729. [Google Scholar] [CrossRef] [PubMed]
- Kaditis, A.G.; Alexopoulos, E.; Chaidas, K.; Ntamagka, G.; Karathanasi, A.; Tsilioni, I.; Kiropoulos, T.S.; Zintzaras, E.; Gourgoulianis, K. Urine concentrations of cysteinyl leukotrienes in children with obstructive sleep-disordered breathing. Chest 2009, 135, 1496–1501. [Google Scholar] [CrossRef] [PubMed]
- Magliulo, G.; Iannella, G.; Polimeni, A.; De Vincentiis, M.; Meccariello, G.; Gulotta, G.; Pasquariello, B.; Montevecchi, F.; De Vito, A.; D’Agostino, G.; et al. Laryngopharyngeal reflux in obstructive sleep apnoea patients: Literature review and meta-analysis. Am. J. Otolaryngol. 2018, 39, 776–780. [Google Scholar] [CrossRef] [PubMed]
- Kheirandish-Gozal, L.; Gileles-Hillel, A.; Alonso-Álvarez, M.L.; Peris, E.; Bhattacharjee, R.; Terán-Santos, J.; Duran-Cantolla, J.; Gozal, D. Effects of adenotonsillectomy on plasma inflammatory biomarkers in obese children with obstructive sleep apnea: A community-based study. Int. J. Obes. 2015, 39, 1094–1100. [Google Scholar] [CrossRef]
- Katz, E.S.; D’Ambrosio, C.M. Pediatric obstructive sleep apnea syndrome. Clin. Chest Med. 2010, 31, 221–234. [Google Scholar] [CrossRef]
- Nisbet, L.C.; Yiallourou, S.R.; Walter, L.M.; Horne, R.S. Blood pressure regulation, autonomic control and sleep disordered breathing in children. Sleep Med. Rev. 2014, 18, 179–189. [Google Scholar] [CrossRef]
- Beebe, D.W. Neurobehavioral morbidity associated with disordered breathing during sleep in children: A comprehensive review. Sleep 2006, 29, 1115–1134. [Google Scholar] [CrossRef] [PubMed]
- Beebe, D.W.; Rausch, J.; Byars, K.C.; Lanphear, B.; Yolton, K. Persistent snoring in preschool children: Predictors and behavioral and developmental correlates. Pediatrics 2012, 130, 382–389. [Google Scholar] [CrossRef] [PubMed]
- Abman, S.H.; Ivy, D.D. Recent progress in understanding pediatric pulmonary hypertension. Curr. Opin. Pediatr. 2011, 23, 298–304. [Google Scholar] [CrossRef] [PubMed]
- Ingram, D.G.; Matthews, C.K. Effect of adenotonsillectomy on c-reactive protein levels in children with obstructive sleep apnea: A meta-analysis. Sleep Med. 2013, 14, 172–176. [Google Scholar] [CrossRef] [PubMed]
- O’Brien, L.M.; Serpero, L.D.; Tauman, R.; Gozal, D. Plasma adhesion molecules in children with sleep-disordered breathing. Chest 2006, 129, 947–953. [Google Scholar] [CrossRef]
- Kim, J.; Bhattacharjee, R.; Snow, A.B.; Capdevila, O.S.; Kheirandish-Gozal, L.; Gozal, D. Myeloid-related protein 8/14 levels in children with obstructive sleep apnoea. Eur. Respir. J. 2010, 35, 843–850. [Google Scholar] [CrossRef] [PubMed]
- Bhushan, B.; Khalyfa, A.; Spruyt, K.; Kheirandish-Gozal, L.; Capdevila, O.S.; Bhattacharjee, R.; Kim, J.; Keating, B.; Hakonarson, H.; Gozal, D. Fatty-acid binding protein 4 gene polymorphisms and plasma levels in children with obstructive sleep apnea. Sleep Med. 2011, 12, 666–671. [Google Scholar] [CrossRef]
- Kaditis, A.G.; Alexopoulos, E.I.; Damani, E.; Karadonta, I.; Kostadima, E.; Tsolakidou, A.; Gourgoulianis, K.; Syrogiannopoulos, G.A. Obstructive sleep-disordered breathing and fasting insulin levels in nonobese children. Pediatr. Pulmonol. 2005, 40, 515–523. [Google Scholar] [CrossRef]
- Lesser, D.J.; Bhatia, R.; Tran, W.H.; Oliveira, F.; Ortega, R.; Keens, T.G.; Mittelman, S.D.; Khoo, M.C.; Davidson Ward, S.L. Sleep fragmentation and intermittent hypoxemia are associated with decreased insulin sensitivity in obese adolescent Latino males. Pediatr. Res. 2012, 72, 293–298. [Google Scholar] [CrossRef]
- Chervin, R.D.; Hedger, K.; Dillon, J.E.; Pituch, K.J. Pediatric sleep questionnaire (PSQ): Validity and reliability of scales for sleep-disordered breathing, snoring, sleepiness, and behavioural problems. Sleep Med. 2000, 1, 21–32. [Google Scholar] [CrossRef]
- Villa, M.P.; Paolino, M.C.; Castaldo, R.; Vanacore, N.; Rizzoli, A.; Miano, S.; Del Pozzo, M.; Montesano, M. Sleep Clinical Record: an aid to rapid and accurate diagnosis of Paediatric Sleep Disordered Breathing. Eur. Respir. J. 2013, 41, 1355–1361. [Google Scholar] [CrossRef] [PubMed]
- Borgstrom, A.; Nerfeldt, P.; Friberg, D. Questionnaire OSA-18 has poor validity compared to polysomnography in pediatric obstructive sleep apnea. Int. J. Pediatr. Otorhinolaryngol. 2013, 77, 1864–1868. [Google Scholar] [CrossRef] [PubMed]
- Kadmon, G.; Chung, S.A.; Shapiro, C.M. I’M SLEEPY: A short pediatric sleep apnea questionnaire. Int. J. Pediatr. Otorhinolaryngol. 2014, 78, 2116–2120. [Google Scholar] [CrossRef] [PubMed]
- Moore, S. A pediatric ‘sleep formula’ and ‘red flag’ system. In Proceedings of the AAMS (Academy of Applied Myofunctional Sciences) poster session, Rome, Italy, 5–10 September 2018. [Google Scholar]
- Burghard, M.; Brożek-Mądry, E.; Krzeski, A. Sleep disordered breathing in children—Diagnostic questionnaires, comparative analysis. Int. J. Pediatr. Otorhinolaryngol. 2019, 120, 108–111. [Google Scholar] [CrossRef] [PubMed]
- Brooks, L.J.; Stephens, B.M.; Bacevice, A.M. Adenoid size is related to severity but not the number of episodes of obstructive apnea in children. J. Pediatr. 1998, 132, 682–686. [Google Scholar] [CrossRef]
- Lam, Y.Y.; Chan, E.Y.; Ng, D.K.; Chan, C.H.; Cheung, J.M.; Leung, S.Y.; Chow, P.Y.; Kwok, K.L. The correlation among obesity, apnea-hypopnea index, and tonsil size in children. Chest 2006, 130, 1751–1756. [Google Scholar] [CrossRef] [PubMed]
- Goldberg, S.; Shatz, A.; Picard, E.; Wexler, I.; Schwartz, S.; Swed, E.; Zilber, L.; Kerem, E. Endoscopic findings in children with obstructive sleep apnea: Effects of age and hypotonia. Pediatr. Pulmonol. 2005, 40, 205–210. [Google Scholar] [CrossRef]
- Zettergren-Wijk, L.; Forsberg, C.M.; Linder-Aronson, S. Changes in dentofacial morphology after adeno-/tonsillectomy in young children with obstructive sleep apnoea--a 5-year follow-up study. Eur. J. Orthod. 2006, 28, 319–326. [Google Scholar] [CrossRef]
- Kirk, V.G.; Bohn, S.G.; Flemons, W.W.; Remmers, J.E. Comparison of home oximetry monitoring with laboratory polysomnography in children. Chest 2003, 124, 1702–1708. [Google Scholar] [CrossRef]
- Scholle, S.; Scholle, H.C.; Kemper, A.; Glaser, S.; Rieger, B.; Kemper, G.; Zwacka, G. First night effect in children and adolescents undergoing polysomnography for sleepdisordered breathing. Clin. Neurophysiol. 2003, 114, 2138–2145. [Google Scholar] [CrossRef]
- Zucconi, M.; Calori, G.; Castronovo, V.; Ferini-Strambi, L. Respiratory monitoring by means of an unattended device in children with suspected uncomplicated obstructive sleep apnea: A validation study. Chest 2003, 124, 602–607. [Google Scholar] [CrossRef] [PubMed]
- Goodwin, J.L.; Enright, P.L.; Kaemingk, K.L.; Rosen, G.M.; Morgan, W.J.; Fregosi, R.F.; Quan, S.F. Feasibility of using unattended polysomnography in children for research report of the Tucson Children’s Assessment of Sleep Apnea study (TuCASA). Sleep 2001, 24, 937–944. [Google Scholar] [CrossRef] [PubMed]
- Redline, S.; Budhiraja, R.; Kapur, V.; Marcus, C.L.; Mateika, J.H.; Mehra, R.; Parthasarthy, S.; Somers, V.K.; Strohl, K.P.; Sulit, L.G.; et al. The scoring of respiratory events in sleep: Reliability and validity. J. Clin. Sleep Med. 2007, 3, 169–200. [Google Scholar] [PubMed]
- Katz, E.S.; Greene, M.G.; Carson, K.A.; Galster, P.; Loughlin, G.M.; Carroll, J.; Marcus, C.L. Night-to-night variability of polysomnography in children with suspected obstructive sleep apnea. J. Pediatr. 2002, 140, 589–594. [Google Scholar] [CrossRef] [PubMed]
- Li, A.M.; Wing, Y.K.; Cheung, A.; Chan, D.; Ho, C.; Hui, S.; Fok, T.F. Is a 2-night polysomnographic study necessary in childhood sleep-related disordered breathing? Chest 2004, 126, 1467–1472. [Google Scholar] [CrossRef] [PubMed]
- Aurora, R.N.; Zak, R.S.; Karippot, A.; Lamm, C.I.; Morgenthaler, T.I.; Auerbach, S.H.; Bista, S.R.; Casey, K.R.; Chowdhuri, S.; Kristo, D.A.; et al. Practice parameters for the respiratory indications for polysomnography in children. Sleep 2011, 34, 379–388. [Google Scholar] [CrossRef] [PubMed]
- Chan, D.K.; Liming, B.J.; Horn, D.L.; Parikh, S.R. A new scoring system for upper airway pediatric sleep endoscopy. JAMA Otolaryngol. Head Neck Surg. 2014, 140, 595–602. [Google Scholar] [CrossRef]
- Chen, J.; He, S. Drug-induced sleep endoscopy-directed adenotonsillectomy in pediatric obstructive sleep apnea with small tonsils. PLoS ONE 2019, 14, 0212317. [Google Scholar] [CrossRef]
- Croft, C.B.; Pringle, M. Sleep nasendoscopy: A technique of assessment in snoring and obstructive sleep apnoea. Clin. Otolaryngol. Allied Sci. 1991, 16, 504–509. [Google Scholar] [CrossRef]
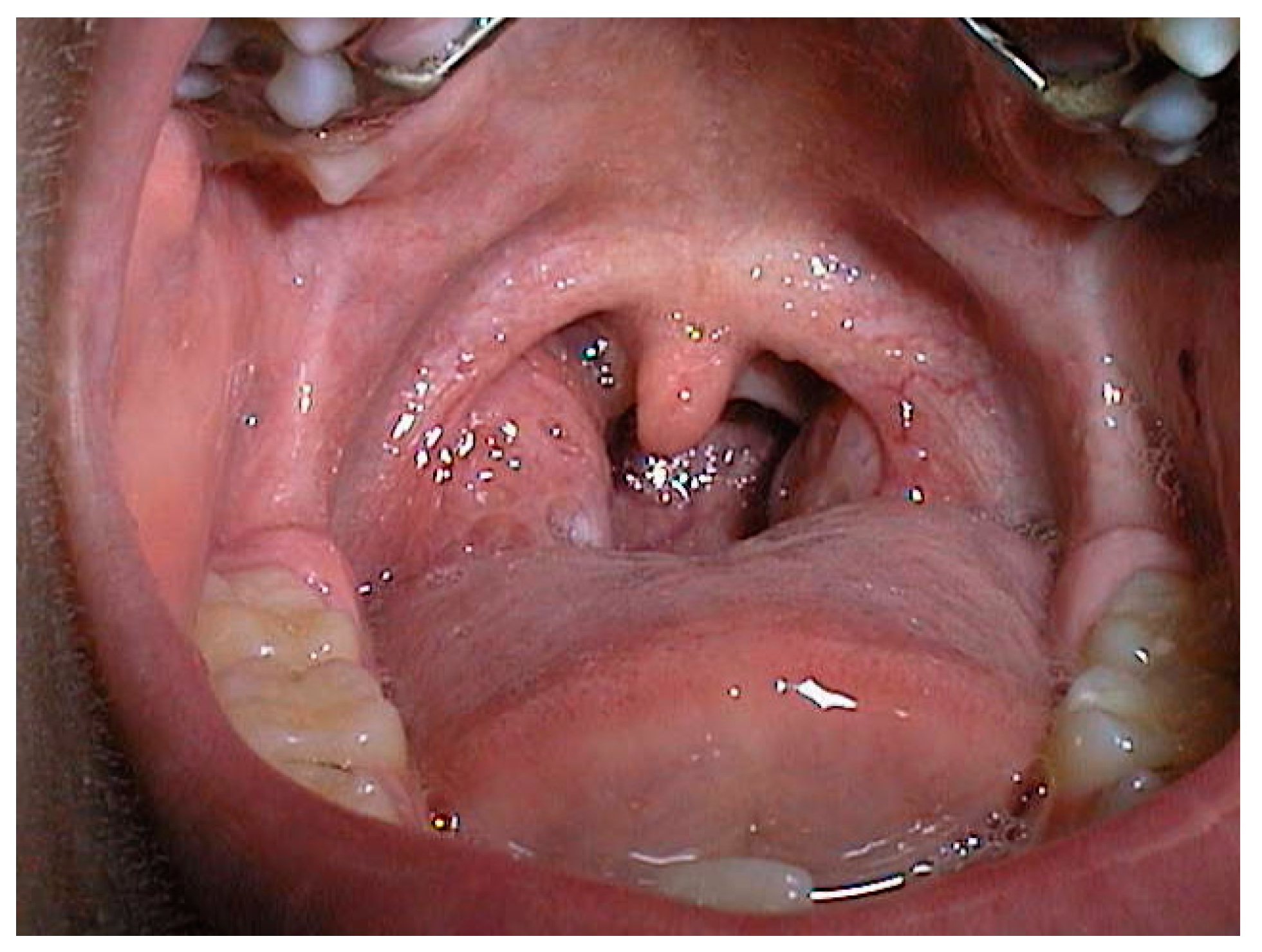
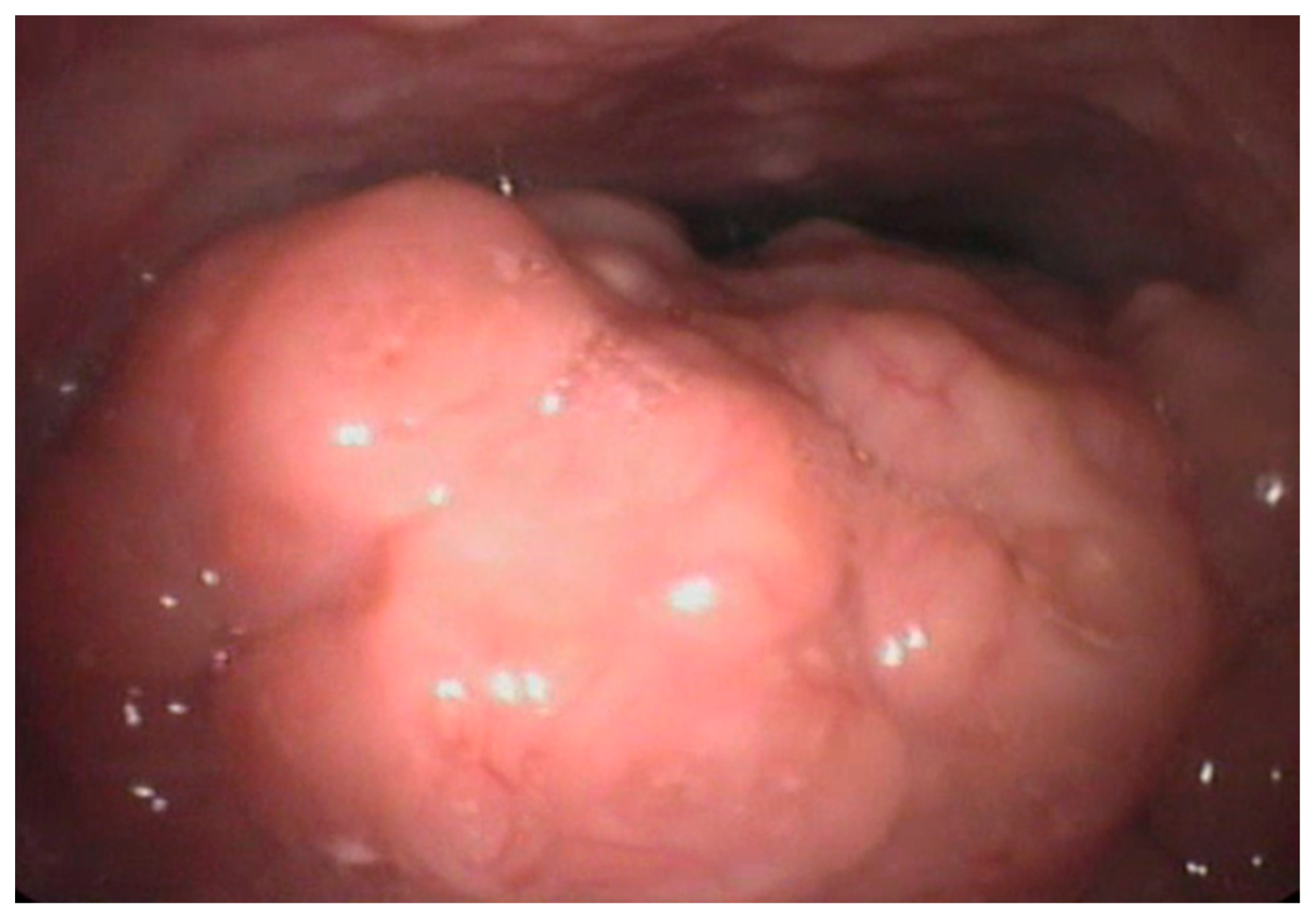
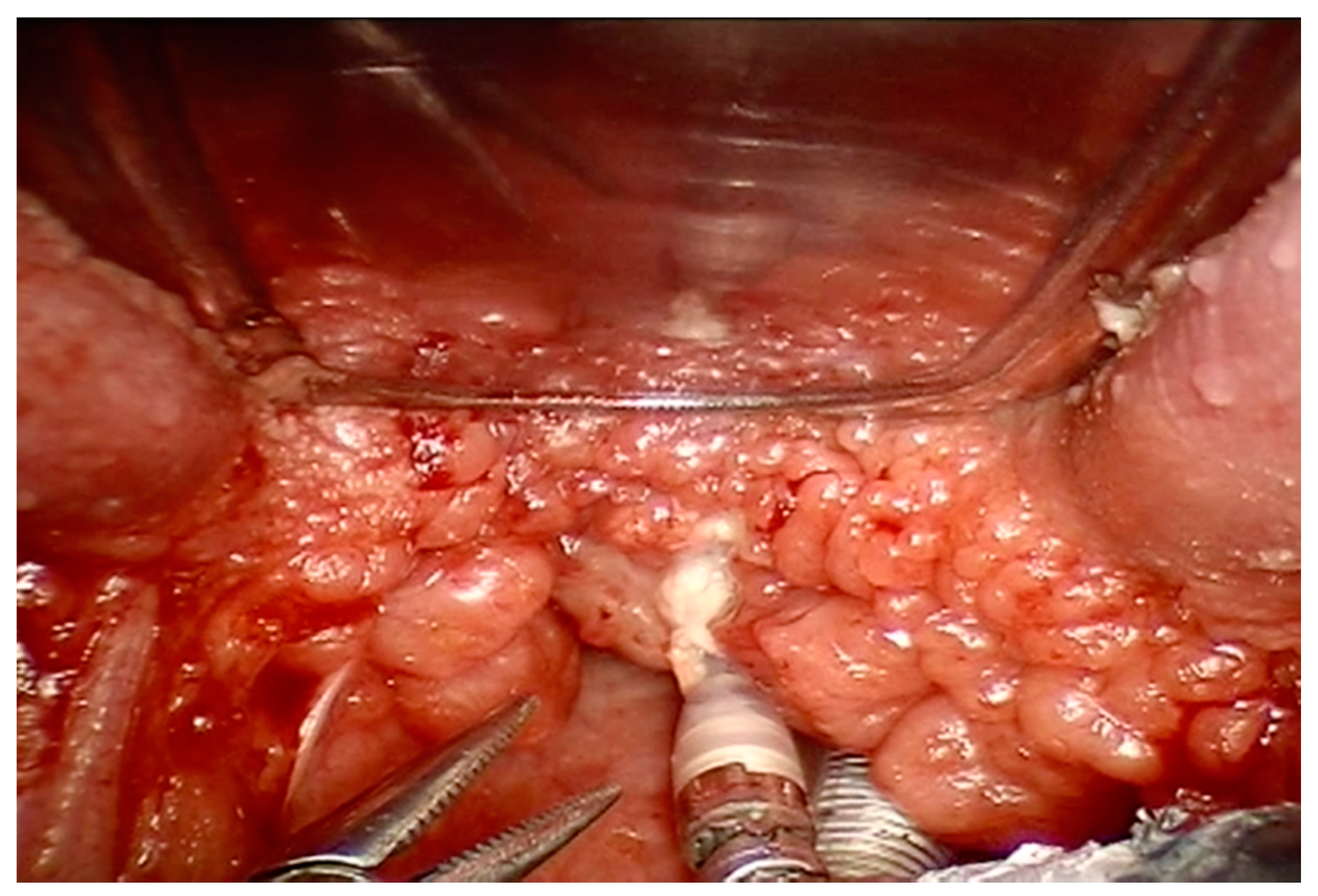
| Study | Year | Type of Study | Patients Number | Age | Parameters Evaluated | Conclusions |
|---|---|---|---|---|---|---|
| Arens R et al. [18] | 2018 | Case-control study | 44 | 12.5 ± 2.8 | Anatomical findings in obese children affected by OSAS compared to the ones in obese children | Significant upper airway lymphoid hypertrophy in obese children with OSAS. Larger parapharyngeal fat in obese children with OSAS but not a direct association with severity of OSAS or with obesity |
| Su M. et al. [21] | 2016 | Epidemiological study | 5930 | 3–11 | Age and sex; | No positive correlation between OSA and BMI |
| AHI; | ||||||
| Arousal index; | ||||||
| BMI; | ||||||
| Mallampati; | ||||||
| AT hypertrophy; | ||||||
| Nocturnal/daytime symptoms | ||||||
| Xu Z. et al. [26] | 2008 | Case-control Study | 198 | 10.3 ± 2.1 | Age and sex; | Positive relation between OSAS and degree of obesity |
| BMI; | ||||||
| Waist circumference; | ||||||
| Neck circumference; | ||||||
| Waist-to-Height Ratio; | ||||||
| Symptoms; | ||||||
| AHI, Obstructive Apnea Index, Central Apnea, MinSaO2; | ||||||
| AT hypertrophy | ||||||
| Andersen I.G. et al. [30] | 2019 | Longitudinal study | 62 | 13.4 ± 3.1 | Age and sex; | AHI normalization in 44% of patients and positive correlation between BMI and AHI parameters |
| BMI; | ||||||
| AT hypertrophy; | ||||||
| AHI; | ||||||
| Sleep time (hours); | ||||||
| ODI |
| Grade | Description |
|---|---|
| 0 | No tonsils seen |
| I | In tonsillar fossa |
| II | Visible beyond anterior pillars |
| III | Extended ¾ of way to midline |
| IV | Completely obstructing airway (kissing tonsils) |
| Study | Year | Type of Study | Patients n° | Age | Parameters Evaluated | Conclusions |
|---|---|---|---|---|---|---|
| Kurnatowski P. et al. [33] | 2007 | Case–control study | 225 | 10–13 | Age and sex; | Negative emotional effect of adenotonsillar hypertrophy induced obstructive sleep disordered breathing |
| Total sleep time; | ||||||
| AHI, ODI; | ||||||
| AT grade sec. Friedman; | ||||||
| Spielberger test; | ||||||
| Capra and Pastorelli scale | ||||||
| Brietzke S.E. et al. [34] | 2006 | Meta-analysis (14 studies) | 28 (mean) | 4.9 (pooled mean age) | Age; | AT effective in reducing severity of OSAS in majority of patients |
| Pre AT AHI; | ||||||
| Post AT AHI; | ||||||
| Success of AT; | ||||||
| Kang K.T. et al. [38] | 2017 | Meta-analysis (4 studies) | 18.25 (mean) | 8.3 ± 1.1 (mean) | Age; | Effectiveness of lingual tonsillectomy for children with OSA caused by lingual tonsil hypertrophy |
| BMI; | ||||||
| Other comorbidities; | ||||||
| CT, RMN, DISE; | ||||||
| Preoperative AHI; | ||||||
| Postoperative AHI | ||||||
| Preoperative ODI; | ||||||
| Postoperative ODI | ||||||
| Lee C.F. et al. [41] | 2016 | Meta-analysis (11 studies) | 11 (mean) | 3.7 (mean) | Age; | Effectiveness in reducing AHI and MinSaO2, but complete resolution not achieved in most cases |
| BMI; | ||||||
| Preoperative AHI; | ||||||
| Postoperative AHI | ||||||
| Preoperative ODI; | ||||||
| Postoperative ODI |
| Study | Year | Type of Study | Patients n° | Age | Parameters Evaluated | Conclusions |
|---|---|---|---|---|---|---|
| Cao Y. et al. [51] | 2018 | Meta-analysis (44 studies) | 6086 total patients | 47.97 (adults) 7.73 (children) | Age and Sex; | Children with OSA suffering from a higher incidence of AR. OSA adults with AR do not have any influences on sleep parameters |
| BMI; | ||||||
| Neck circumference; | ||||||
| AHI; | ||||||
| ESS; | ||||||
| AR prevalence | ||||||
| Kheirandish-Gozal L. et al. [52] | 2014 | Retrospective review | 3071 | 2–14 | Age and Sex; | Effective alternative to adenotonsillectomy, particularly in younger and non-obese Children |
| BMI; | ||||||
| Pretreatment: AT grade; | ||||||
| Mallampati; | ||||||
| Total sleep time; | ||||||
| AHI, ODI; | ||||||
| Posttreatment: Pretreatment: AT grade; | ||||||
| Mallampati; | ||||||
| Total sleep time; | ||||||
| AHI, ODI | ||||||
| Kheirandish-Gozal L. et al. [53] | 2016 | Prospective randomized trial study | 92 | 2–10 | Age and Sex; | Beneficial effects (reduction of AHI and ODI) in 71% of children treated with montelukast. No changes in those treated with placebo. |
| BMI; | ||||||
| Pretreatment: AT grade; | ||||||
| Mallampati; | ||||||
| Total sleep time; | ||||||
| AHI, ODI; | ||||||
| Posttreatment: Pretreatment: AT grade; | ||||||
| Mallampati; | ||||||
| Total sleep time; | ||||||
| AHI, ODI | ||||||
| Brouillette R.T. et al. [54] | 2001 | Triple-blind randomized placebo-controlled trial | 25 | 1–10 | Age and Sex; | Decrease in AHI/ODI values in 12/13 of fluticasone group. No changes in placebo group |
| Pretreatment: | ||||||
| AHI, ODI; | ||||||
| Total sleep time; | ||||||
| AT grade; | ||||||
| AR symptoms | ||||||
| Posttreatment: AHI, ODI; | ||||||
| Total sleep time; | ||||||
| AT grade; | ||||||
| AR symptoms |
| Study | Year | Type of Study | Patients Number | Age | Parameters Evaluated | Conclusions |
|---|---|---|---|---|---|---|
| Follmar A. et al. [58] | 2014 | Retrospective cohort study | 118 | 1 day–15 years | RDI; | Multifactorial etiology of RSD in children affected by Prader–Willi Syndrome |
| Laryngomalacia; | ||||||
| macroglossia, | ||||||
| AT hypertrophy; | ||||||
| GERD. | ||||||
| Onodera K. et al. [62] | 2005 | Case–control study | 30 | 3.8 ± 1.4 (20) 7.9 ± 3 (10) | Questionnaire items: | Significant presence of RSD in patients affected by achondroplasia (AP) |
| Snoring; | ||||||
| AHI; | ||||||
| Mouth breathing; | ||||||
| Occlusion; | ||||||
| Height and weight; | ||||||
| Ages of the eruption of deciduous teeth | ||||||
| Pavone M. et al. [66] | 2015 | Retrospective study | 88 | 1–14.5 | Anthropometric data; | No correlations between MOAHI and age or BMI, positive correlations between MOAHI and Sp02 |
| BMI; | ||||||
| MOAHI, RDI, SpO2 | ||||||
| Guilleminault C. et al. [67] | 2013 | Retrospective study | 34 patients | 26.55 | Clinical evaluation; | Commonly unrecognized abnormal breathing and its correlation with daytime fatigue and poor sleep in Ehlers–Danlos patients |
| Rhinomanometry; | ||||||
| AHI, RDI, Sa02 | ||||||
| Kalaskar R et al. [69] | 2012 | Case report study | 1 | 11 years old boy | Anatomical finding; orthodontic conformation | Association between Ellis–van Creveld syndrome and OSA |
| Cardiel Rios S.A. et al. [71] | 2016 | Case report study | 1 | 10 years old boy | Anatomical finding; orthodontic conformation | Association between Noonan syndrome, malocclusion and OSA |
| Saxby C. et al. [74] | 2018 | Retrospective study | 65 | Not specified | Patients demographics; Type of midface advancement; | Positive outcomes after midface advancement in patients with craniosynostosis |
| Preoperative: AHI, RDI, SaO2; | ||||||
| Postoperative: AHI, RDI, SaO2; | ||||||
| Blood pressure; | ||||||
| Villa M.P. et al. [77] | 2002 | Randomized controlled study | 32 | 4–10 | Brouillette questionnaire; | Improved respiratory symptoms in patients who underwent oral appliance treatments |
| physical examinations: | ||||||
| AHI, RDI, SaO2 |
| Study | Year | Type of Study | Patients n° | Age | Parameters Evaluated | Conclusions |
|---|---|---|---|---|---|---|
| Gozal D. et al. [59] | 2007 | Prospective study | 355 | 5–7 | AHI, RDI, SaO2; | Positive correlation between APOE epsilon4 allele and OSA and neurocognitive deficits |
| Neurocognitive tests; | ||||||
| Blood draw. | ||||||
| Khalyfa A. et al. [60] | 2011 | Case–control study | 140 | <6 | ESS questionnaire; | Positive correlation between high TNF- α levels and OSAS |
| AHI, RDI, SaO2M; | ||||||
| Serum TNF- α | ||||||
| Tam C.S. et al. [79] | 2006 | Case–control study | 113 | 7.3 ± 3.7 | C-reactive protein; | Significantly elevated IFN-gamma levels and elevated IL-8 levels |
| Cytokines: IL-1beta, IL-2, IL-4, IL-6, IL-8, IL-10, IL-12, GM-CSF, IFN-gamma and TNF-alpha. | ||||||
| Gozal et al. [80] | 2008 | Case–control study | 40 | 6.5 ± 0.7 | Age and sex; | Higher levels of IL-6 and IL-10 |
| Ethnicity; | ||||||
| BMI: | ||||||
| AHI, RDI; | ||||||
| IL-6, IL-10. | ||||||
| Park C.S. et al. [85] | 2014 | Case–control study | 67 | 6 (3–16) | Age and sex; | High level of serum alpha amilase in severe OSAS children compared to moderate and mild ones and to the control group |
| BMI; | ||||||
| AHI, RDI; | ||||||
| OSA-18 questionnaire; | ||||||
| Alpha amilase levels. | ||||||
| Gozal D. et al. [86] | 2009 | Case–control study | 60 | 6.6 ± 0.7 | Clinical questionnaires; | Consistent alterations in urinary concentrations of specific protein clusters in OSA patients |
| Height and weight; | ||||||
| BMI; | ||||||
| AHI; RDI, SaO2; | ||||||
| Urine collection |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Gulotta, G.; Iannella, G.; Vicini, C.; Polimeni, A.; Greco, A.; de Vincentiis, M.; Visconti, I.C.; Meccariello, G.; Cammaroto, G.; De Vito, A.; et al. Risk Factors for Obstructive Sleep Apnea Syndrome in Children: State of the Art. Int. J. Environ. Res. Public Health 2019, 16, 3235. https://doi.org/10.3390/ijerph16183235
Gulotta G, Iannella G, Vicini C, Polimeni A, Greco A, de Vincentiis M, Visconti IC, Meccariello G, Cammaroto G, De Vito A, et al. Risk Factors for Obstructive Sleep Apnea Syndrome in Children: State of the Art. International Journal of Environmental Research and Public Health. 2019; 16(18):3235. https://doi.org/10.3390/ijerph16183235
Chicago/Turabian StyleGulotta, Giampiero, Giannicola Iannella, Claudio Vicini, Antonella Polimeni, Antonio Greco, Marco de Vincentiis, Irene Claudia Visconti, Giuseppe Meccariello, Giovanni Cammaroto, Andrea De Vito, and et al. 2019. "Risk Factors for Obstructive Sleep Apnea Syndrome in Children: State of the Art" International Journal of Environmental Research and Public Health 16, no. 18: 3235. https://doi.org/10.3390/ijerph16183235
APA StyleGulotta, G., Iannella, G., Vicini, C., Polimeni, A., Greco, A., de Vincentiis, M., Visconti, I. C., Meccariello, G., Cammaroto, G., De Vito, A., Gobbi, R., Bellini, C., Firinu, E., Pace, A., Colizza, A., Pelucchi, S., & Magliulo, G. (2019). Risk Factors for Obstructive Sleep Apnea Syndrome in Children: State of the Art. International Journal of Environmental Research and Public Health, 16(18), 3235. https://doi.org/10.3390/ijerph16183235










