Associations between School Food Environments, Body Mass Index and Dietary Intakes among Regional School Students in Victoria, Australia: A Cross-Sectional Study
Abstract
1. Introduction
- Determine what school-level characteristics are associated with having low, medium and highly scored school food environments.
- Understand associations between characteristics of the school food environment with school students’ dietary intake in primary schools, with adjustment for confounders such as socioeconomic status (SES), sex and school size.
- To assess the strength of associations between the healthiness of the school food environment and with the level of overweight and obesity within a school with adjustment for SES, sex and school size.
2. Materials and Methods
2.1. Sampling
2.2. Ethical Approval
2.3. Statistical Analysis
3. Results
3.1. Sample Demographics and School Food Environment Charactertistics
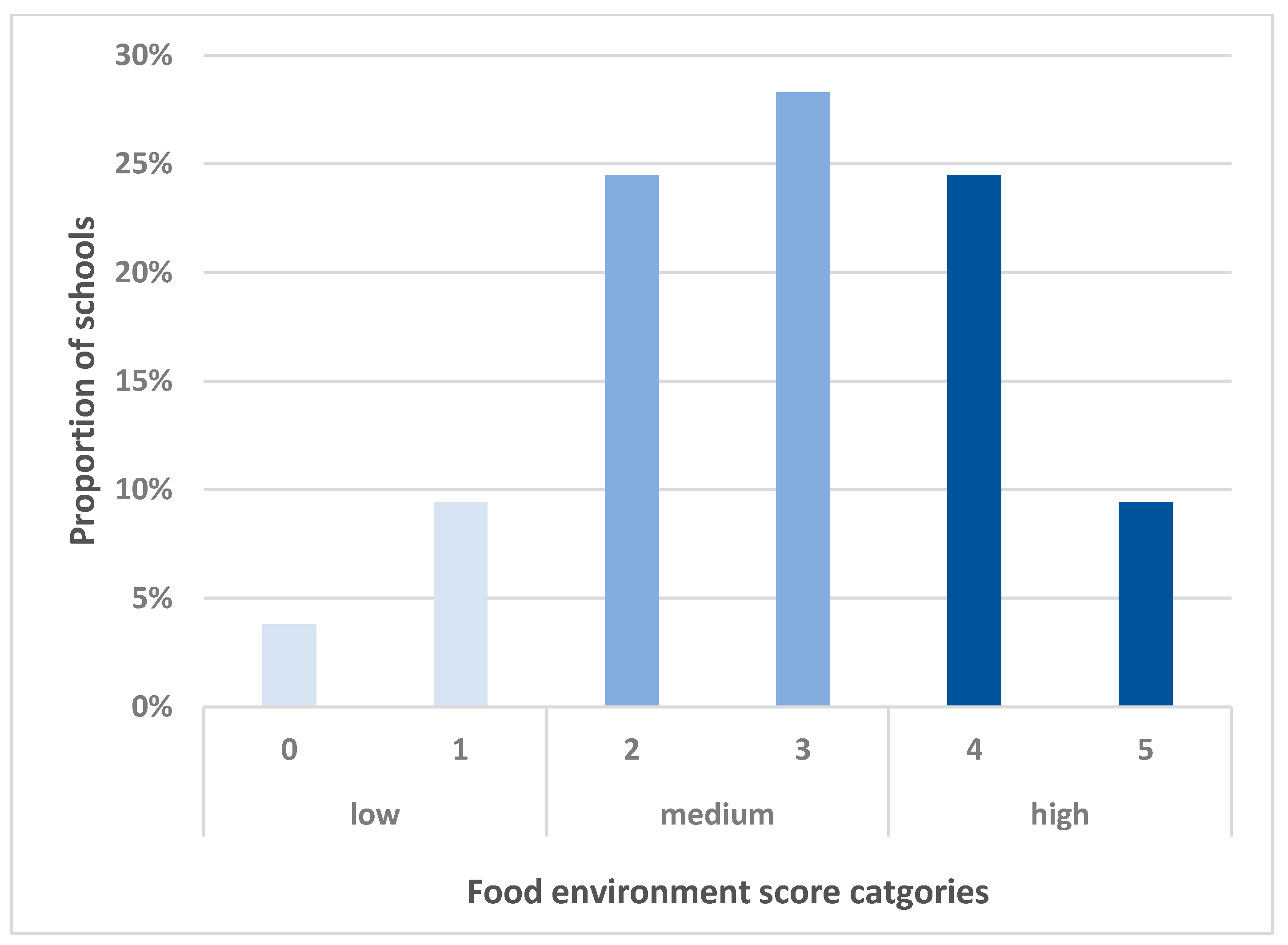
3.2. School Food Environment Scores and Their Relationship to School Characteristics
4. Discussion
5. Conclusions
Availability of Data and Materials
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- World Health Organisation. Childhood Overweight and Obesity. 2019. Available online: https://www.who.int/dietphysicalactivity/childhood/en/ (accessed on 8 April 2019).
- Reilly, J.J.; Kelly, J. Long term impact of overweight and obesity in childhood and adolescence on morbidity and premature mortality in adulthood: Systematic review. Int. J. Obes. 2011, 35, 891. [Google Scholar] [CrossRef] [PubMed]
- Hebestreit, A.; Intemann, T.; Siani, A.; De Henauw, S.; Eiben, G.; Kourides, Y.A.; Kovacs, E.; Moreno, L.A.; Veidebaum, T.; Krogh, V.; et al. Dietary Patterns of European Children and Their Parents in Association with Family Food Environment: Results from the I. Fam. Study Nutr. 2017, 9, 126. [Google Scholar] [CrossRef] [PubMed]
- Verstraeten, R.; Leroy, J.L.; Pieniak, Z.; Ochoa-Avilès, A.; Holdsworth, M.; Verbeke, W.; Maes, L.; Kolsteren, P. Individual and Environmental Factors Influencing Adolescents’ Dietary Behavior in Low- and Middle-Income Settings. PLoS ONE 2016, 11, e0157744. [Google Scholar] [CrossRef] [PubMed]
- Carter, M.A. Measuring the ’obesogenic’ food environment in New Zealand primary schools. Heal. Promot. Int. 2004, 19, 15–20. [Google Scholar] [CrossRef] [PubMed]
- Peterson, K.E.; Fox, M.K. Addressing the Epidemic of Childhood Obesity through School-Based Interventions: What Has Been Done and Where Do We Go from Here? J. Law Med. Ethic. 2007, 35, 113–130. [Google Scholar] [CrossRef] [PubMed]
- Driessen, C.E.; Cameron, A.; Thornton, L.E.; Lai, S.K.; Barnett, L.M. Effect of changes to the school food environment on eating behaviours and/or body weight in children: A systematic review. Obes. Rev. 2014, 15, 968–982. [Google Scholar] [CrossRef] [PubMed]
- Cullen, K.W.; Hartstein, J.; Reynolds, K.D.; Vu, M.; Resnicow, K.; Greene, N. Improving the school food environment: Results from a pilot study in middle schools. J. Am. Diet Assoc. 2007, 107, 484–489. [Google Scholar] [CrossRef][Green Version]
- Madden, A.M.; Harrex, R.; Radalowicz, J.; Boaden, D.C.; Lim, J.; Ash, R. A kitchen based intervention to improve nutritional intake from school lunches in children aged 12 16 years. J. Hum. Nutr. Diet. 2013, 26, 243–251. [Google Scholar] [CrossRef]
- Cullen, K.W.; Watson, K.; Zakeri, I.; Ralston, K. Exploring changes in middle-school student lunch consumption after local school food service policy modifications. Public Health Nutr. 2006, 9, 814–882. [Google Scholar] [CrossRef]
- Vericker, T.C. Limited evidence that competitive food and beverage practices affect adolescent consumption behaviors. Health Educ. Behav. 2013, 40, 19–23. [Google Scholar] [CrossRef]
- Taber, D.R.; Chriqui, J.F.; Powell, L.M.; Chaloupka, F.J. Banning all sugar sweetened beverages in middle schools: Reduction of in school access and purchasing but not overall consumption. Arch. Pediatr. Adolesc. Med. 2012, 166, 256–262. [Google Scholar] [CrossRef] [PubMed]
- Fox, M.K.; Dodd, A.H.; Wilson, A.; Gleason, P.M. Association between School Food Environment and Practices and Body Mass Index of US Public School Children. J. Am. Diet. Assoc. 2009, 109, S108–S117. [Google Scholar] [CrossRef] [PubMed]
- Briefel, R.R.; Crepinsek, M.K.; Cabili, C.; Wilson, A.; Gleason, P.M. School Food Environments and Practices Affect Dietary Behaviors of US Public School Children. J. Am. Diet. Assoc. 2009, 109, S91–S107. [Google Scholar] [CrossRef] [PubMed]
- Somerset, S.; Markwell, K. Impact of a school-based food garden on attitudes and identification skills regarding vegetables and fruit: A 12-month intervention trial. Public Health Nutr. 2009, 12, 214–221. [Google Scholar] [CrossRef] [PubMed]
- Terry-McElrath, Y.M.; O’Malley, P.M.; Johnston, L.D. Accessibility Over Availability: Associations Between the School Food Environment and Student Fruit and Green Vegetable Consumption. Child. Obes. 2014, 10, 241–250. [Google Scholar] [CrossRef] [PubMed]
- Mâsse, L.C.; De Niet-Fitzgerald, J.E.; Watts, A.W.; Naylor, P.J.; Saewyc, E.M. Associations between the school food environment, student consumption and body mass index of Canadian adolescents. Int. J. Behav. Nutr. Phys. Act. 2014, 11, 29. [Google Scholar] [CrossRef] [PubMed]
- Allender, S.; Millar, L.; Hovmand, P.; Bell, C.; Moodie, M.; Carter, R.; Swinburn, B.; Strugnell, C.; Lowe, J.; De La Haye, K.; et al. Whole of Systems Trial of Prevention Strategies for Childhood Obesity: WHO STOPS Childhood Obesity. Int. J. Environ. Res. Public Health 2016, 13, 1143. [Google Scholar] [CrossRef]
- Hoare, E.; Crooks, N.; Hayward, J.; Allender, S.; Strugnell, C. Associations between combined overweight and obesity, lifestyle behavioural risk and quality of life among Australian regional school children: Baseline findings of the Goulburn Valley health behaviours monitoring study. Health Qual. Life Outcomes 2019, 17, 16. [Google Scholar] [CrossRef]
- Australian Bureau of Statistics. Australian Statistical Geography Standard (ASGS). 2018. Available online: https://www.abs.gov.au/websitedbs/D3310114.nsf/home/Australian+Statistical+Geography+Standard+(ASGS) (accessed on 30 July 2019).
- Crooks, N.; Strugnell, C.; Bell, C.; Allender, S. Establishing a sustainable childhood obesity monitoring system in regional Victoria. Health Promot. J. Austr. 2017, 28, 96–102. [Google Scholar] [CrossRef]
- Onis, M.D.; Onyango, A.W.; Borghi, E.; Siyam, A.; Nishida, C.; Siekmann, J. Development of a WHO growth reference for school aged children and adolescents. Bull. World Health Organ. 2007, 85, 660–667. [Google Scholar] [CrossRef]
- Hayward, J.; Jacka, F.N.; Skouteris, H.; Millar, L.; Strugnell, C.A.; Swinburn, B.; Allender, S. Lifestyle factors and adolescent depressive symptomatology: Associations and effect sizes of diet, physical activity and sedentary behaviour. Aust. N. Z. J. Psychiatry 2016, 50, 1064–1073. [Google Scholar]
- National Health and Medical Research Council. Australian Dietary Guidelines; National Health and Medical Research Council: Canberra, Australia, 2016.
- Mathews, L.; Kremer, P.; Sanigorski, A.; Simmons, A.; Nichols, M.; Moodie, M.; Swinburn, B.A. Nutrition and Physical Activity in Children and Adolescents: Report 1: Methods and Tools; Department of Health and Human Services, Ed.; Victorian State Government: Melbourne, Australia, 2009.
- Australian Curriculm Assessment and Reporting Authority. Index of Community Socio Educational Advantage (ICSEA). 2015. Available online: http://docs.acara.edu.au/resources/About_icsea_2014.pdf (accessed on 18 April 2019).
- Australian Government Department of Education and Training. Australian Education Act. 2013. Available online: https://www.education.gov.au/australian education act 2013 (accessed on 18 April 2019).
- Cullen, K.W.; Chen, T.A. The contribution of the USDA school breakfast and lunch program meals to student daily dietary intake. Prev. Med. Rep. 2017, 5, 82–85. [Google Scholar] [CrossRef] [PubMed]
- Bagordo, F.; De Donno, A.; Grassi, T.; Guido, M.; DeVoti, G.; Ceretti, E.; Zani, C.; Feretti, D.; Villarini, M.; Moretti, M.; et al. Lifestyles and socio-cultural factors among children aged 6–8 years from five Italian towns: The MAPEC_LIFE study cohort. BMC Public Health 2017, 17, 204. [Google Scholar] [CrossRef] [PubMed]
- Zani, C.; Ceretti, E.; Grioni, S.; Viola, G.C.V.; Donato, F.; Feretti, D.; Festa, A.; Bonizzoni, S.; Bonetti, A.; Monarca, S.; et al. Are 6-8 year old Italian children moving away from the Mediterranean diet? Ann. Med. Prev. Comunita 2016, 28, 339–348. [Google Scholar]
- Woods, J.; Bressan, A.; Langelaan, C.; Mallon, A.; Palermo, C. Australian school canteens: Menu guideline adherence or avoidance? Health Promot. J. Aust. 2014, 25, 110–115. [Google Scholar] [CrossRef] [PubMed]
- State Government of Victoria. Healthy Canteens. 2018. Available online: https://www.education.vic.gov.au/school/teachers/health/Pages/canteen.aspx (accessed on 17 April 2019).
- de Silva-Sanigorski, A.; Breheny, T.; Jones, L.; Lacy, K.; Kremer, P.; Carpenter, L.; Swinburn, B. Government food service policies and guidelines do not create healthy school canteens. Aust. N. Z. J. Public Health 2011, 35, 117–121. [Google Scholar] [CrossRef] [PubMed]
- Mullally, M.L.; Taylor, J.P.; Kuhle, S.; Bryanton, J.; Hernandez, K.J.; MacLellan, D.L.; McKenna, M.L.; Gray, R.J.; Veugelers, P.J. A province-wide school nutrition policy and food consumption in elementary school children in Prince Edward Island. Can. J. Public Health 2010, 101, 40–43. [Google Scholar] [PubMed]
| Variable | Schools (n) | Schools (% of Sample) | Students (n) | Students (% of Sample) |
|---|---|---|---|---|
| Total | 53 | 100 | 3496 | 100 |
| School size | ||||
| Small (≥11 to ≤200 students) | 31 | 58.5 | 1086 | 31.0 |
| Medium (>200 to <300 students) | 13 | 24.5 | 964 | 27.6 |
| Large (≥300 students) | 9 | 17.0 | 1446 | 41.4 |
| School socio economic status | ||||
| ICSEA 1 < 1000 | 33 | 62.3 | 2231 | 64.0 |
| ICSEA > 1000 | 20 | 37.7 | 1265 | 36.0 |
| Reported presence of healthy policy and food environment components | ||||
| Nutrition policy or practice | 28 | 54.9 | 1638 | 48.4 |
| Cooking classes | 37 | 71.2 | 2464 | 73.3 |
| Vegetable garden | 48 | 90.6 | 3231 | 92.4 |
| Breakfast program | 23 | 46.0 | 1476 | 46.7 |
| Healthy canteen program | 17 | 37.8 | 1639 | 53.1 |
| Males (%) | Females (%) | P Value (Chi2) | Total (%) | |
|---|---|---|---|---|
| Met vegetable guidelines | 14.9 | 18.5 | 0.02 | 16.6 |
| Met fruit guidelines | 73.4 | 79.4 | 0.01 | 76.4 |
| Takeaway less than once per week | 86.9 | 92.3 | <0.001 | 89.6 |
| Snack foods once per day or less | 51.8 | 57.0 | 0.01 | 54.3 |
| SSBs less than once per day | 80.6 | 85.3 | 0.03 | 82.9 |
| Met daily water consumption guidelines | 56.3 | 58.8 | NS | 57.5 |
| School Characteristics | School Food Environment Scores | P Value (Chi2) | ||
|---|---|---|---|---|
| Low % (n) | Medium % (n) | High % (n) | ||
| SES (ICSEA) | ||||
| Lower ICSEA | 9.0 (3) | 51.5 (17) | 39.4 (13) | |
| Higher ICSEA | 20.0 (4) | 55.0 (11) | 25.0 (5) | <0.001 |
| School size (enrolments) | ||||
| Small | 12.9 (4) | 54.8 (17) | 32.2 (10) | |
| medium | 15.4 (2) | 53.9 (7) | 30.7 (4) | |
| large | 11.1 (1) | 44.4 (4) | 44.4 (4) | <0.001 |
| Odds Ratio (95% Confidence Interval) | |||||||
|---|---|---|---|---|---|---|---|
| Meeting Vegetable Recommendations | Meeting Fruit Recommendations | Takeaway Less Than Once Per Week | Snack Foods Once Per Day or Less | SSBs Less Than 1x Day | Meeting Daily Water Consumption Recommendations | Healthy BMI | |
| School environment score (p value for overall model) | P = 0.88 | P = 0.06 | P = 0.22 | P = 0.83 | P = 0.88 | P = 0.04 | |
| High (reference) | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 | 1.0 |
| Medium | 1.06 (0.77, 1.47) | 1.29 (0.98, 1.69) | 0.69 (0.4, 1.06) | 1.01 (0.78, 1.31) | 0.89 (0.53, 1.50) | 1.20 * (0.93, 1.55) | 0.85 (0.73, 1.00) |
| Low | 0.98 (0.59, 1.57) | 1.55 * (1.02, 2.37) | 0.89 (0.45, 1.06) | 0.91 (0.61, 1.34) | 1.00 (0.45, 2.19) | 0.77 (0.54, 1.12) | 0.87 (0.68, 1.12) |
| Odds Ratio (95% Confidence Interval) | |||||||
|---|---|---|---|---|---|---|---|
| Meeting Vegetable Recommendations | Meeting Fruit Recommendations | Takeaway Once Per Week or Less | Snack Foods Once Per Day or Less | SSBs Less Than 1x Day | Meeting Daily Water Consumption Recommendations | Healthy BMI | |
| School environment score | P < 0.001 | P < 0.001 | P < 0.001 | P = 0.02 | P < 0.001 | P = 0.13 | P = 0.02 |
| High (reference) | 1.00 | 1.00 | 1.00 | 1.00 | 1.00 | 1.00 | 1.0 |
| Medium | 1.12 (0.86, 1.48) | 1.21 (0.95, 1.55) | 0.66 (0.46, 0.94) * | 0.92 (0.54, 1.16) | 0.64 (0.37, 1.07) | 1.21 (0.94, 1.56) | 1.09 (0.78, 1.30) |
| Low | 0.94 (0.61, 1.43) | 1.33 (1.13, 1.82) | 0.70 (0.46, 0.95) | 0.79 (0.72, 1.20) | 0.77 (0.55, 1.08) | 00.78 (0.54, 1.13) | 1.01 (0.92, 1.28) |
| SES (ISCEA) | |||||||
| Low ICSEA | 1.00 | 1.00 | 1.00 | 1.00 | 1.00 | 1.00 | 1.00 |
| High ICSEA (reference) | 1.26 (0.96, 1.63) | 1.44(1.14, 1.78) * | 2.28 (1.58, 3.28) * | 1.24 (0.98, 1.58) | 3.30 (2.31, 4.72) * | 1.04 (0.81, 1.32) | 1.24 (1.05, 1.45) * |
| School size | |||||||
| Small (reference) | 1.00 | 1.00 | 1.00 | 1.00 | 1.00 | 1.00 | 1.00 |
| Medium | 1.13 (0.83, 1.56) | 1.01 (0.77, 1.32) | 1.17 (0.80, 1.72) | 1.00 (0.76, 1.32) | 1.41 (0.96, 2.05) | 0.88 (0.67, 1.15) | 0.98 (0.81, 1.18) |
| Large | 1.68 (1.26, 2.24) * | 1.14 (0.88, 1.47) | 1.20 (0.82, 1.75) | 0.77 (0.59, 1.01) | 0.92 (0.64, 1.31) | 1.08 (0.82, 1.42) | 0.85 (0.72, 1.02) |
| Sex | |||||||
| Boys (reference) | 1.00 | 1.00 | 1.00 | 1.00 | 1.00 | 1.00 | 1.0 |
| Girls | 1.28 (1.02, 1.59) * | 1.36 (1.12, 1.66) * | 1.80 (1.35, 2.36) * | 1.05 (1.05, 1.48) * | 1.36 (1.08, 1.70) * | 1.11 (0.93, 1.32) | 0.97 (0.84, 1.12) |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Alston, L.; Crooks, N.; Strugnell, C.; Orellana, L.; Allender, S.; Rennie, C.; Nichols, M. Associations between School Food Environments, Body Mass Index and Dietary Intakes among Regional School Students in Victoria, Australia: A Cross-Sectional Study. Int. J. Environ. Res. Public Health 2019, 16, 2916. https://doi.org/10.3390/ijerph16162916
Alston L, Crooks N, Strugnell C, Orellana L, Allender S, Rennie C, Nichols M. Associations between School Food Environments, Body Mass Index and Dietary Intakes among Regional School Students in Victoria, Australia: A Cross-Sectional Study. International Journal of Environmental Research and Public Health. 2019; 16(16):2916. https://doi.org/10.3390/ijerph16162916
Chicago/Turabian StyleAlston, Laura, Nicholas Crooks, Claudia Strugnell, Liliana Orellana, Steven Allender, Claire Rennie, and Melanie Nichols. 2019. "Associations between School Food Environments, Body Mass Index and Dietary Intakes among Regional School Students in Victoria, Australia: A Cross-Sectional Study" International Journal of Environmental Research and Public Health 16, no. 16: 2916. https://doi.org/10.3390/ijerph16162916
APA StyleAlston, L., Crooks, N., Strugnell, C., Orellana, L., Allender, S., Rennie, C., & Nichols, M. (2019). Associations between School Food Environments, Body Mass Index and Dietary Intakes among Regional School Students in Victoria, Australia: A Cross-Sectional Study. International Journal of Environmental Research and Public Health, 16(16), 2916. https://doi.org/10.3390/ijerph16162916





