Food Insecurity and Geriatric Hospitalization
Abstract
1. Introduction
2. Materials and Methods
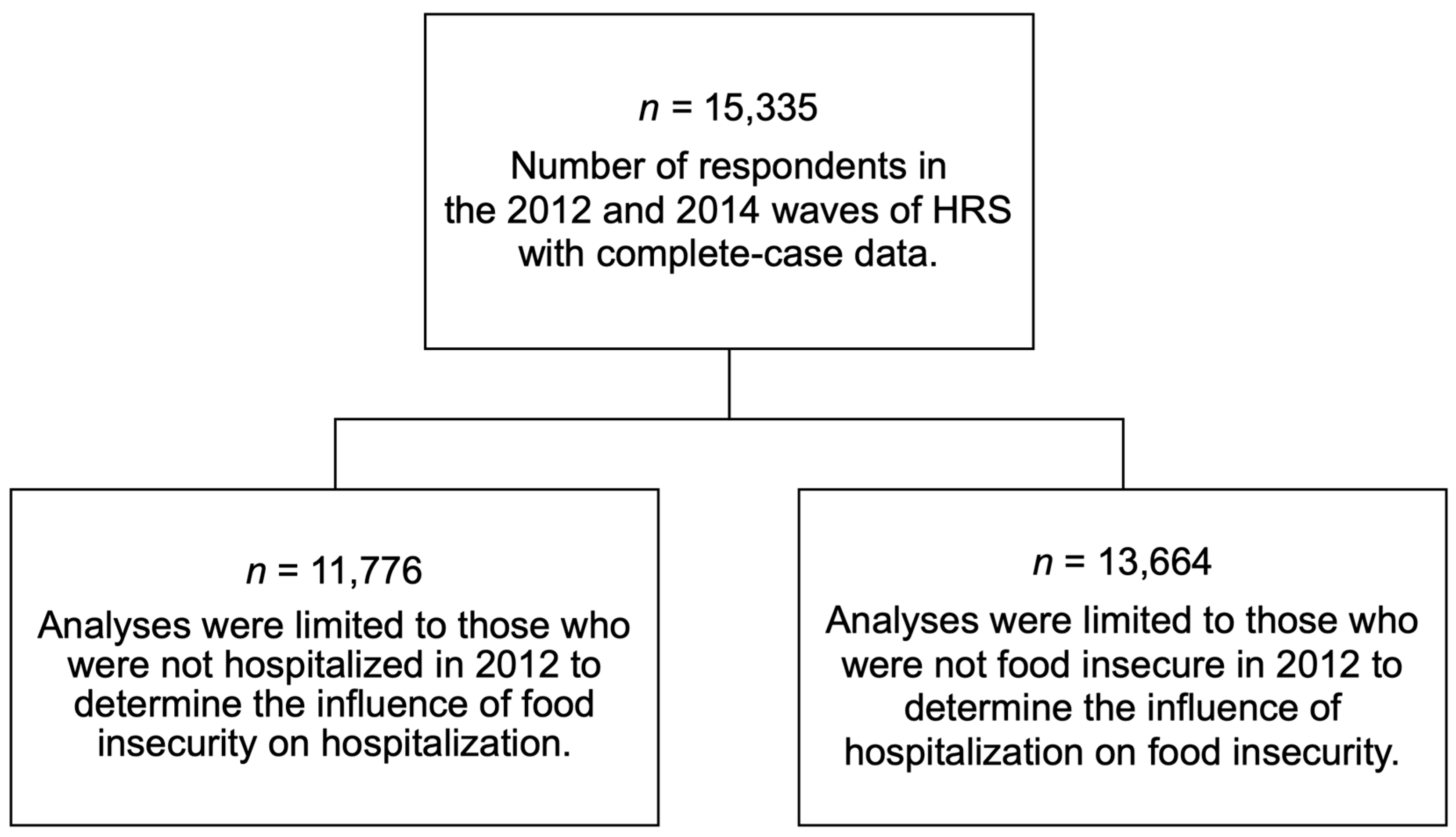
2.1. Sample
2.2. Measures
2.2.1. Food Insecurity
2.2.2. Hospitalization
2.2.3. Depression
2.2.4. Covariates
2.3. Statistical Approach
3. Results
4. Discussion
Limitations
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Creditor, M.C. Hazards of hospitalization of the elderly. Ann. Int. Med. 1993, 118, 219–223. [Google Scholar] [CrossRef] [PubMed]
- Martin, A.B.; Hartman, M.; Washington, B.; Catlin, A. The National Health Expenditure Accounts Team. National Health Care Spending In 2017: Growth Slows to Post—Great Recession Rates; Share of GDP Stabilizes. Health Aff. 2018, 38. [Google Scholar] [CrossRef]
- Gill, T.M.; Allore, H.G.; Gahbauer, E.A.; Murphy, T.E. Changing in disability after hospitalization or restricted activity in older persons. JAMA 2010, 304, 1919. [Google Scholar] [CrossRef] [PubMed]
- Fried, L.P.; Guralnik, J.M. Disability in Older Adults: Evidence Regarding Significance, Etiology, and Risk. J. Am. Geriatr. Soc. 1997, 45, 92–100. [Google Scholar] [CrossRef]
- Zayas, C.E.; He, Z.; Yuan, J.; Maldonado-Molina, M.; Hogan, W.; Modave, F.; Guo, Y.; Bian, J. Examining Healthcare Utilization Patterns of Elderly Middle-Aged Adults in the United States. In Proceedings of the Twenty-Ninth International Flairs Conference, Key Largo, FL, USA, 16–18 May 2016; pp. 361–366. [Google Scholar]
- Cooper, R.A.; Cooper, M.A.; McGinley, E.L.; Fan, X.; Rosenthal, J.T. Poverty, Wealth, and Health Care Utilization: A Geographic Assessment. J. Urban Health 2012, 89, 828–847. [Google Scholar] [CrossRef]
- Sinha, S.K.; Bennett, J.; Ramsden, R.; Bon, J.; Chalk, T. Delivering improved patient and system outcomes for hospitalized older adults through an Acute Care for Elders Strategy. Healthc. Manag. Forum 2018, 31, 126–132. [Google Scholar] [CrossRef] [PubMed]
- Coleman-Jensen, A.; Rabbitt, M.P.; Gregory, C.A.; Singh, A. Household Food Security in the United States in 2017; U.S. Department of Agriculture, Economic Research Service: Washington, DC, USA, 2018.
- Garcia, S.P.; Haddix, A.; Barnett, K. Incremental Health Care Costs Associated with Food Insecurity and Chronic Conditions among Older Adults. Prev. Chronic Dis. 2018, 15. [Google Scholar] [CrossRef]
- Standards of Medical Care in Diabetes—2018. Available online: http://diabetesed.net/wp-content/uploads/2017/12/2018-ADA-Standards-of-Care.pdf (accessed on 27 June 2019).
- Bergmans, R.S.; Palta, M.; Robert, S.A.; Berger, L.M.; Ehrenthal, D.B.; Malecki, K. Associations between food security status and dietary inflammatory potential within lower-income adults from the United States National Health and Nutrition Examination Survey (NHANES), cycles 2007 to 2014. J. Acad. Nutr. Diet 2018, 118, 994–1005. [Google Scholar] [CrossRef]
- Bergmans, R.S.; Zivin, K.; Mezuk, B. Depression, food insecurity and diabetic morbidity: Evidence from the Health and Retirement Study. J. Psychosom. Res. 2019, 117, 22–29. [Google Scholar] [CrossRef]
- Bengle, R.; Broyles, S.T.; Johnson, T.; Johnson, M.A.; Arvine, B.; Lee, J.S. Food Insecurity Is Associated with Cost-Related Medication Non-Adherence in Community-Dwelling, Low-Income Older Adults in Georgia. J. Nutr. Elder. 2010, 29, 170–191. [Google Scholar] [CrossRef] [PubMed]
- Ippolito, M.M.; Lyles, C.R.; Prendergast, K.; Marshall, M.B.; Waxman, E.; Seligman, H.K. Food insecurity and diabetes self-management among food pantry clients. Public Health Nutr. 2017, 20, 183–189. [Google Scholar] [CrossRef] [PubMed]
- Seligman, H.K.; Bolger, A.F.; Guzman, D.; López, A.; Bibbins-Domingo, K. Exhaustion of Food Budgets at Month’s End and Hospital Admissions for Hypoglycemia. Health Aff. 2014, 33, 116–123. [Google Scholar] [CrossRef] [PubMed]
- Huang, B.Y.; Cornoni-Huntley, J.; Hays, J.C.; Huntley, R.R.; Galanos, A.N.; Blazer, D.G. Impact of Depressive Symptoms on Hospitalization Risk in Community-Dwelling Older Persons. J. Am. Geriatr. Soc. 2000, 48, 1279–1284. [Google Scholar] [CrossRef] [PubMed]
- Kuzuya, M.; Hirakawa, Y.; Suzuki, Y.; Iwata, M.; Enoki, H.; Hasegawa, J.; Iguchi, A. Association between Unmet Needs for Medication Support and All-Cause Hospitalization in Community-Dwelling Disabled Elderly People. J. Am. Geriatr. Soc. 2008, 56, 881–886. [Google Scholar] [CrossRef] [PubMed]
- Rosa, C.B.; Garces, S.B.B.; Hansen, D.; Brunelli, Â.V.; Bianchi, P.D.; Coser, J.; de Rosso Krug, M.; Helena, C. Augustin Schwanke. Malnutrition risk and hospitalization in elderly assisted in Primary Care. Cien. Saude Colet. 2017, 22, 575–582. [Google Scholar] [CrossRef][Green Version]
- Bhargava, V.; Lee, J.S. Food Insecurity and Health Care Utilization among Older Adults. J. Appl. Gerontol. 2017, 36, 1415–1432. [Google Scholar] [CrossRef] [PubMed]
- Bhargava, V.; Lee, J.S. Food Insecurity and Health Care Utilization among Older Adults in the United States. J. Nutr. Gerontol. Geriatr. 2016, 35, 177–192. [Google Scholar] [CrossRef]
- Sonnega, A.; Faul, J.D.; Ofstedal, M.B.; Langa, K.M.; Phillips, J.W.; Weir, D.R. Cohort Profile: The Health and Retirement Study (HRS). Int. J. Epidemiol. 2014, 43, 576–585. [Google Scholar] [CrossRef] [PubMed]
- Tarasuk, V.; Mitchell, A.; McLaren, L.; McIntyre, L. Chronic Physical and Mental Health Conditions among Adults May Increase Vulnerability to Household Food Insecurity. J. Nutr. 2013, 143, 1785–1793. [Google Scholar] [CrossRef]
- Radimer, K.L.; Kathy, L. Measurement of household food security in the USA and other industrialised countries. Public Health Nutr. 2002, 5, 859–864. [Google Scholar] [CrossRef] [PubMed]
- Hager, E.R.; Quigg, A.M.; Black, M.M.; Coleman, S.M.; Heeren, T.; Rose-Jacobs, R.; Cook, J.T.; de Cuba, S.A.E.; Casey, P.H.; Chilton, M.; et al. Development and validity of a 2-item screen to identify families at risk for food insecurity. Pediatrics 2010, 126, 26–32. [Google Scholar] [CrossRef] [PubMed]
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, 5th ed.; American Psychiatric Publishing: Washington, DC, USA, 2013. [Google Scholar]
- Steffick, D.E. Documentation of Affective Functioning Measures in the Health and Retirement Study; University of Michigan Survey Research Center: Ann Arbor, MI, USA, 2000. [Google Scholar]
- Semega, J.L.; Fontenot, K.R.; Kollar, M.A. Income and Poverty in the United States: 2016; U.S. Government Printing Office: Washington, DC, USA, 2017.
- SAS Institute Inc. SAS Software Version 9.4; SAS Institute Inc.: Cary, NC, USA, 2013. [Google Scholar]
- StataCorp. Stata Statistical Software: Release 15; StataCorp LLC: College Station, TX, USA, 2017. [Google Scholar]
- Jeon, J. The strengths and limitations of the statistical modeling of complex social phenomenon: Focusing on SEM, path analysis, or multiple regression models. Int. J. Soc. Behav. Educ. Econ. Bus. Ind. Eng. 2015, 9, 1597–1605. [Google Scholar]
- Molendijk, M.; Molero, P.; Sánchez-Pedreño, F.O.; Van der Does, W.; Martínez-González, M.A. Diet quality and depression risk: A systematic review and dose-response meta-analysis of prospective studies. J. Affect. Disord. 2018, 226, 346–354. [Google Scholar] [CrossRef] [PubMed]
- Mickelson, K.D.; Williams, S.L. Perceived stigma of poverty and depression: Examination of interpersonal and intrapersonal mediators. J. Soc. Clin. Psychol. 2008, 27, 903–930. [Google Scholar] [CrossRef]
- Davydow, D.S.; Katon, W.J.; Lin, E.H.B.; Ciechanowski, P.; Ludman, E.; Oliver, M.; Von Korff, M. Depression and Risk of Hospitalizations for Ambulatory Care-Sensitive Conditions in Patients with Diabetes. J. Gen. Intern. Med. 2013, 28, 921–929. [Google Scholar] [CrossRef]
- Katon, W.J. Clinical and health services relationships between major depression, depressive symptoms, and general medical illness. Biol. Psychiatry 2003, 54, 216–226. [Google Scholar] [CrossRef]
- Roy, M.-A.; Payette, H. Meals-On-Wheels improves energy and nutrient intake in a frail free-living elderly population. J. Nutr. Health Aging 2006, 10, 554–560. [Google Scholar]
- Bergmans, R.S.; Berger, L.M.; Palta, M.; Robert, S.A.; Ehrenthal, D.B.; Malecki, K. Participation in the Supplemental Nutrition Assistance Program and maternal depressive symptoms: Moderation by program perception. Soc. Sci. Med. 2018, 197, 1–8. [Google Scholar] [CrossRef]
- Hwang, J.-Y.; Kim, B.; Kim, K. A Qualitative Study on Attitude, Acceptability, and Adaptation for Home-delivered Meal Services in the Korean Elderly from the Perspective of Life Context. Korean J. Commun. Nutr. 2014, 19, 459. [Google Scholar] [CrossRef][Green Version]
- Campbell, A.D.; Godfryd, A.; Buys, D.R.; Locher, J.L. Does Participation in Home-delivered Meals Programs Improve Outcomes for Older Adults? Results of a Systematic Review. J. Nutr. Gerontol. Geriatr. 2015, 34, 124–167. [Google Scholar] [CrossRef]
| Characteristics | Total Sample | Hospitalized | p Value c | |
|---|---|---|---|---|
| No | Yes | |||
| n = 11,776 | n = 9788 | n = 1988 | ||
| Female | 6858 (54.7) | 5715 (54.8) | 1143 (54.3) | 0.7075 |
| Age Category | <0.0001 | |||
| 51 to <65 | 6036 (58.9) | 5300 (61.7) | 736 (43.5) | |
| 65 to <75 | 3188 (25.9) | 2578 (24.8) | 610 (31.6) | |
| 75 to 106 | 2552 (15.2) | 1910 (13.4) | 642 (25.0) | |
| Race/Ethnicity | 0.2995 | |||
| Non-Hispanic White | 7519 (78.0) | 6169 (77.8) | 1350 (79.1) | |
| Non-Hispanic Black | 2222 (9.5) | 1869 (9.5) | 353 (9.7) | |
| Other | 2035 (12.5) | 1750 (12.7) | 285 (11.2) | |
| Marital Status | <0.0001 | |||
| Married | 6998 (62.4) | 5898 (63.6) | 1100 (55.8) | |
| Separated or divorced | 1724 (14.6) | 1439 (14.4) | 285 (15.5) | |
| Widowed | 1800 (11.3) | 1411 (10.4) | 389 (16.1) | |
| Single or never married | 1254 (11.7) | 1040 (11.5) | 214 (12.6) | |
| Baseline educational attainment d | <0.0001 | |||
| <High school | 1979 (11.7) | 1618 (11.3) | 361 (13.5) | |
| High school degree or equivalent | 3894 (31.3) | 3158 (30.0) | 736 (37.9) | |
| Some college | 2962 (25.9) | 2476 (26.1) | 486 (24.8) | |
| College degree and above | 2941 (31.1) | 2536 (32.5) | 405 (23.7) | |
| Work for Pay | 5342 (52.3) | 4667 (54.5) | 675 (40.6) | <0.0001 |
| Income-to-Poverty Ratio, median, (minimum, maximum) e | 3.8 (0.0, 340.3) | 4.0 (0.0, 340.3) | 3.2 (0.0, 333.3) | <0.0001 |
| Food Security Status f | ||||
| Previously food insecure | 1167 (8.5) | 960 (8.4) | 207 (9.2) | 0.4054 |
| Recently food insecure | 1084 (7.6) | 874 (7.2) | 210 (9.6) | 0.0020 |
| Depression e,g | ||||
| Symptom score, median, (minimum, maximum) | 0 (0, 7) | 0 (0, 7) | 0 (0, 7) | <0.0001 |
| Met criteria for major depression | 873 (7.6) | 630 (6.7) | 243 (12.7) | <0.0001 |
| Complete-Case 2012 and 2014 Sample (n = 15,335) | ||||||
| Model | 2012 Food Insecurity c | p-Value d | 2014 Food Insecurity c | p-Value d | ||
| No | Yes | No | Yes | |||
| Crude | Reference | 1.4 (1.2, 1.7) | <0.0001 | Ref. | 1.7 (1.4, 2.0) | <0.0001 |
| Adjusted e | Reference | 1.4 (1.2, 1.7) | 0.0005 | Ref. | 1.7 (1.4, 2.0) | <0.0001 |
| Restricted to Those Not Hospitalized in 2012 (n = 11,776) | ||||||
| Model | 2012 Food Insecurity c | p-Value d | 2014 Food Insecurity c | p-Value d | ||
| No | Yes | No | Yes | |||
| Crude | Reference. | 1.1 (0.9, 1.4) | 0.41 | Ref. | 1.4 (1.1, 1.7) | 0.0020 |
| Adjusted e | Reference. | 1.1 (0.9, 1.4) | 0.39 | Ref. | 1.4 (1.1, 1.8) | 0.0017 |
| Complete-Case 2012 and 2014 Sample (n = 16,455) | ||||||
| Model | 2012 Food Insecurity c | p-Value | 2014 Food Insecurity c | p-Value | ||
| No | Yes | No | Yes | |||
| Crude | Reference | 0.19 (0.12, 0.27) | <0.0001 | Ref. | 0.31 (0.20, 0.41) | <0.0001 |
| Adjusted d | Reference | 0.16 (0.08, 0.24) | 0.0001 | Ref. | 0.28 (0.17, 0.38) | <0.0001 |
| Restricted to Those Not Hospitalized in 2012 (n = 11,776) | ||||||
| Model | 2012 Food Insecurity c | p-Value | 2014 Food Insecurity c | p-Value | ||
| No | Yes | No | Yes | |||
| Crude | Reference | 0.03 (−0.02, 0.08) | 0.24 | Ref. | 0.11 (0.04, 0.18) | 0.0034 |
| Adjusted d | Reference | 0.02 (−0.03, 0.08) | 0.41 | Ref. | 0.11 (0.03, 0.19) | 0.0065 |
| Complete-Case 2012 and 2014 Sample (n = 15,335) | |||
| Model | 2012 Hospitalization c | p-Value d | |
| No | Yes | ||
| Crude | Reference | 1.7 (1.5, 2.1) | <0.0001 |
| Adjusted e | Reference | 1.7 (1.3, 2.1) | <0.0001 |
| Restricted to Those Not Food Insecure in 2012 (n = 13,664) | |||
| Model | 2012 Hospitalization c | p-Value d | |
| No | Yes | ||
| Crude | Reference | 1.5 (1.2, 2.0) | 0.0006 |
| Adjusted e | Reference | 1.5 (1.2, 2.0) | 0.0020 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Bergmans, R.S.; Mezuk, B.; Zivin, K. Food Insecurity and Geriatric Hospitalization. Int. J. Environ. Res. Public Health 2019, 16, 2294. https://doi.org/10.3390/ijerph16132294
Bergmans RS, Mezuk B, Zivin K. Food Insecurity and Geriatric Hospitalization. International Journal of Environmental Research and Public Health. 2019; 16(13):2294. https://doi.org/10.3390/ijerph16132294
Chicago/Turabian StyleBergmans, Rachel S., Briana Mezuk, and Kara Zivin. 2019. "Food Insecurity and Geriatric Hospitalization" International Journal of Environmental Research and Public Health 16, no. 13: 2294. https://doi.org/10.3390/ijerph16132294
APA StyleBergmans, R. S., Mezuk, B., & Zivin, K. (2019). Food Insecurity and Geriatric Hospitalization. International Journal of Environmental Research and Public Health, 16(13), 2294. https://doi.org/10.3390/ijerph16132294





