Shadow Puppets and Neglected Diseases: Evaluating a Health Promotion Performance in Rural Indonesia
Abstract
1. Introduction
2. Methods
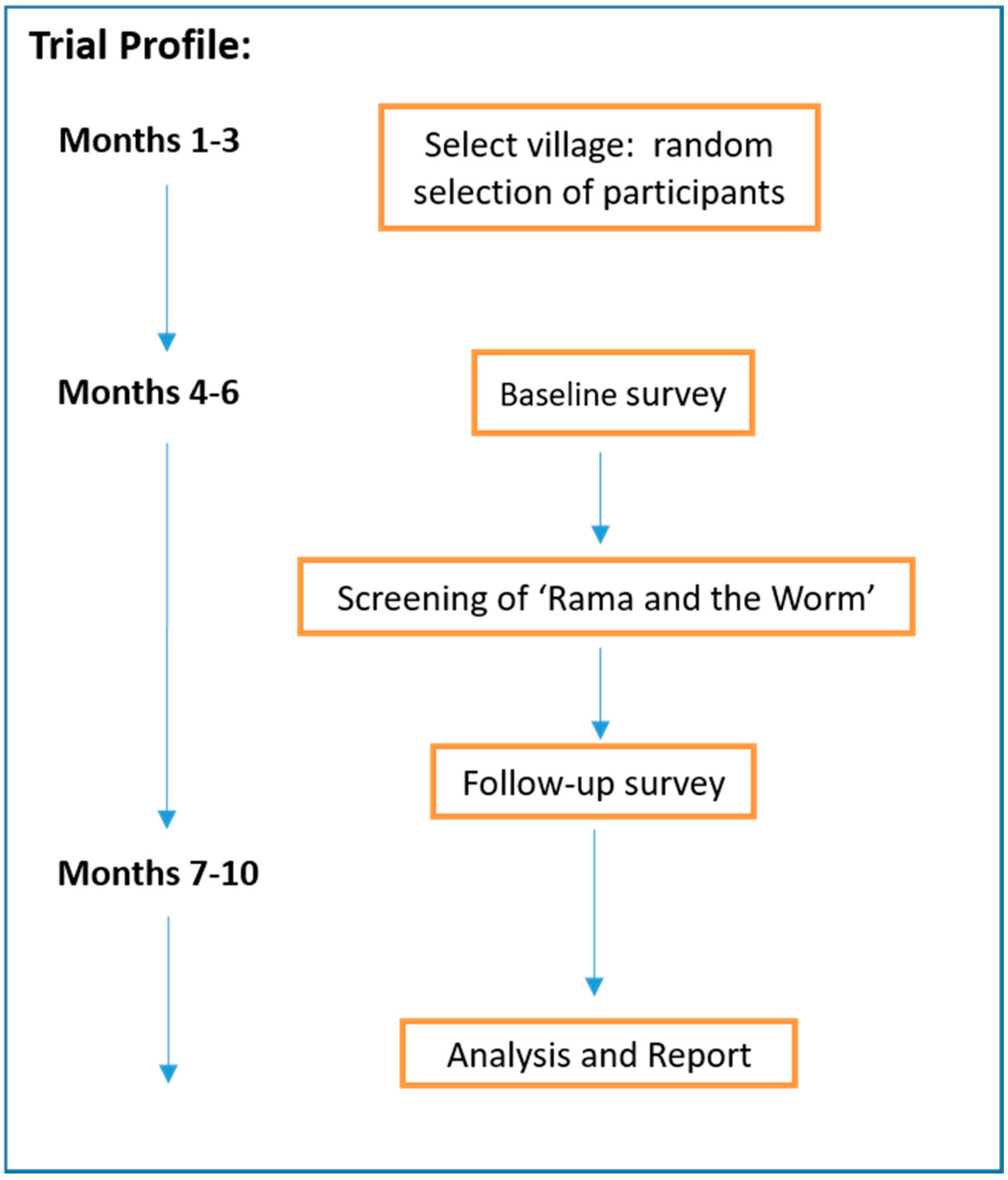
2.1. Study Design
2.2. Study Location and Participants
2.3. Data Collection
2.4. Data Management and Analysis
3. Results
3.1. Respondent Demographics
3.2. Participant History of Gastrointestinal Disease and Presence of Symptoms
3.3. Latrine Habits
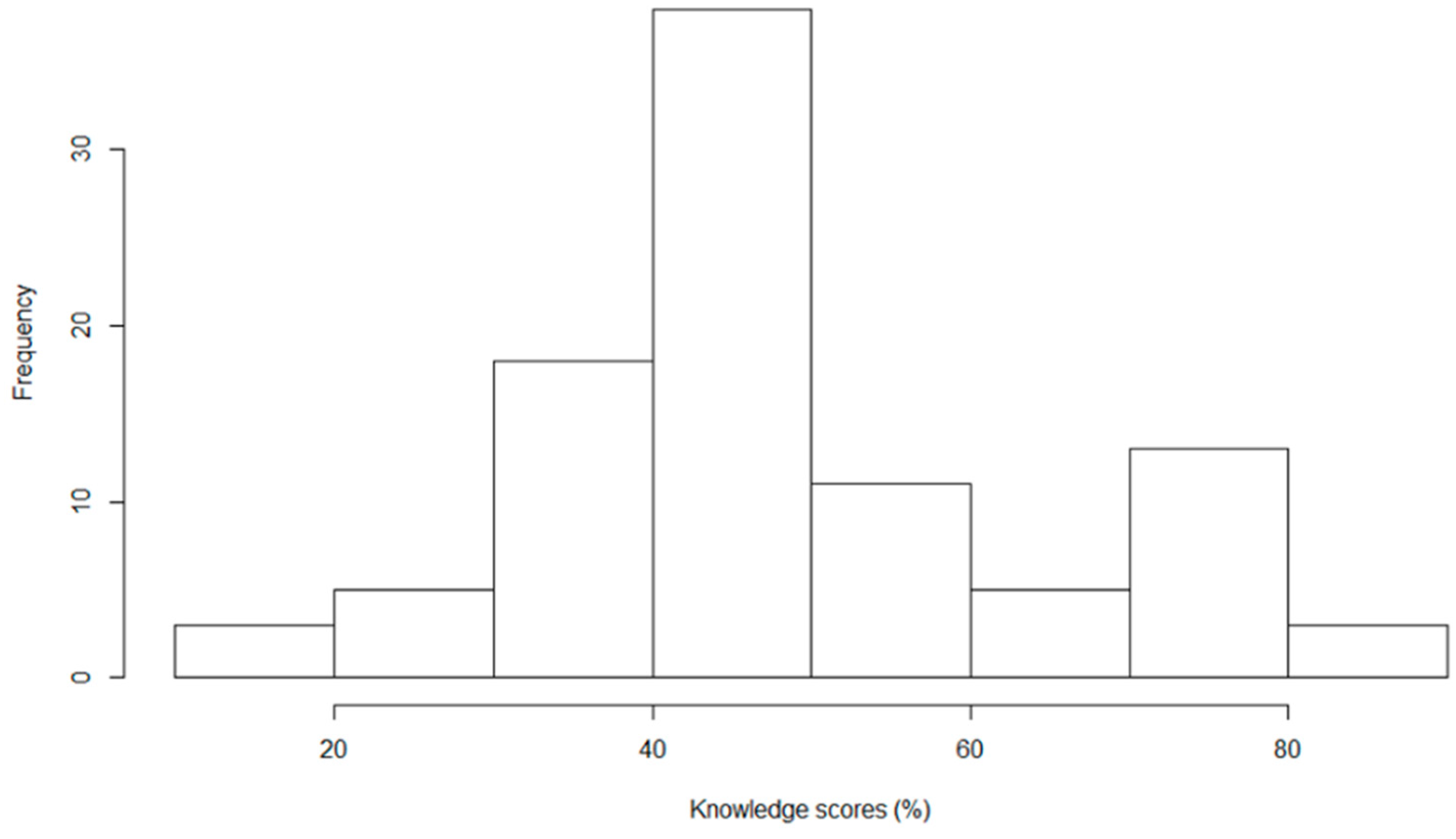
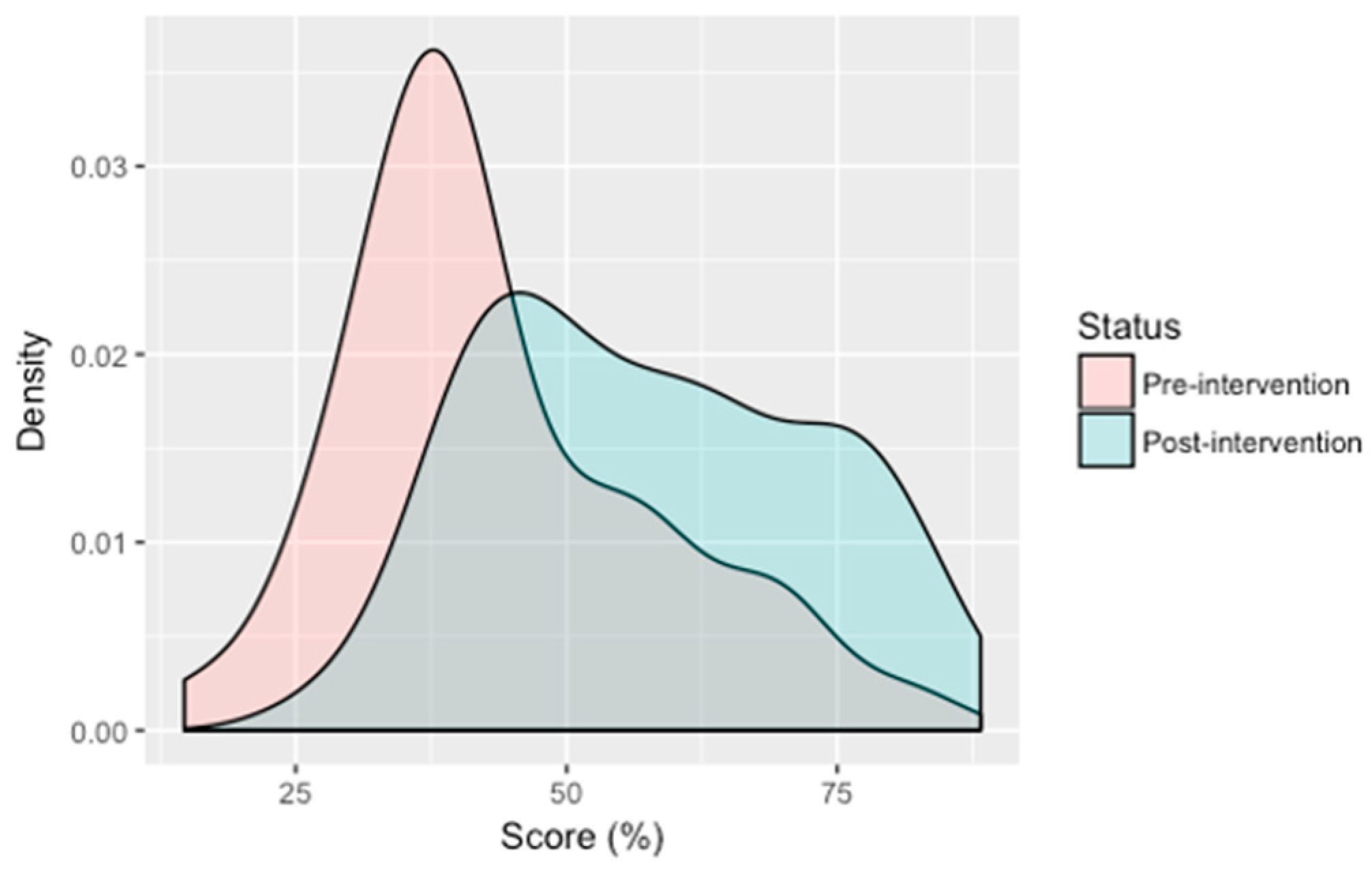
3.4. Knowledge of Gastrointestinal and Helminth-Related Disease Transmission, Symptoms and Prevention
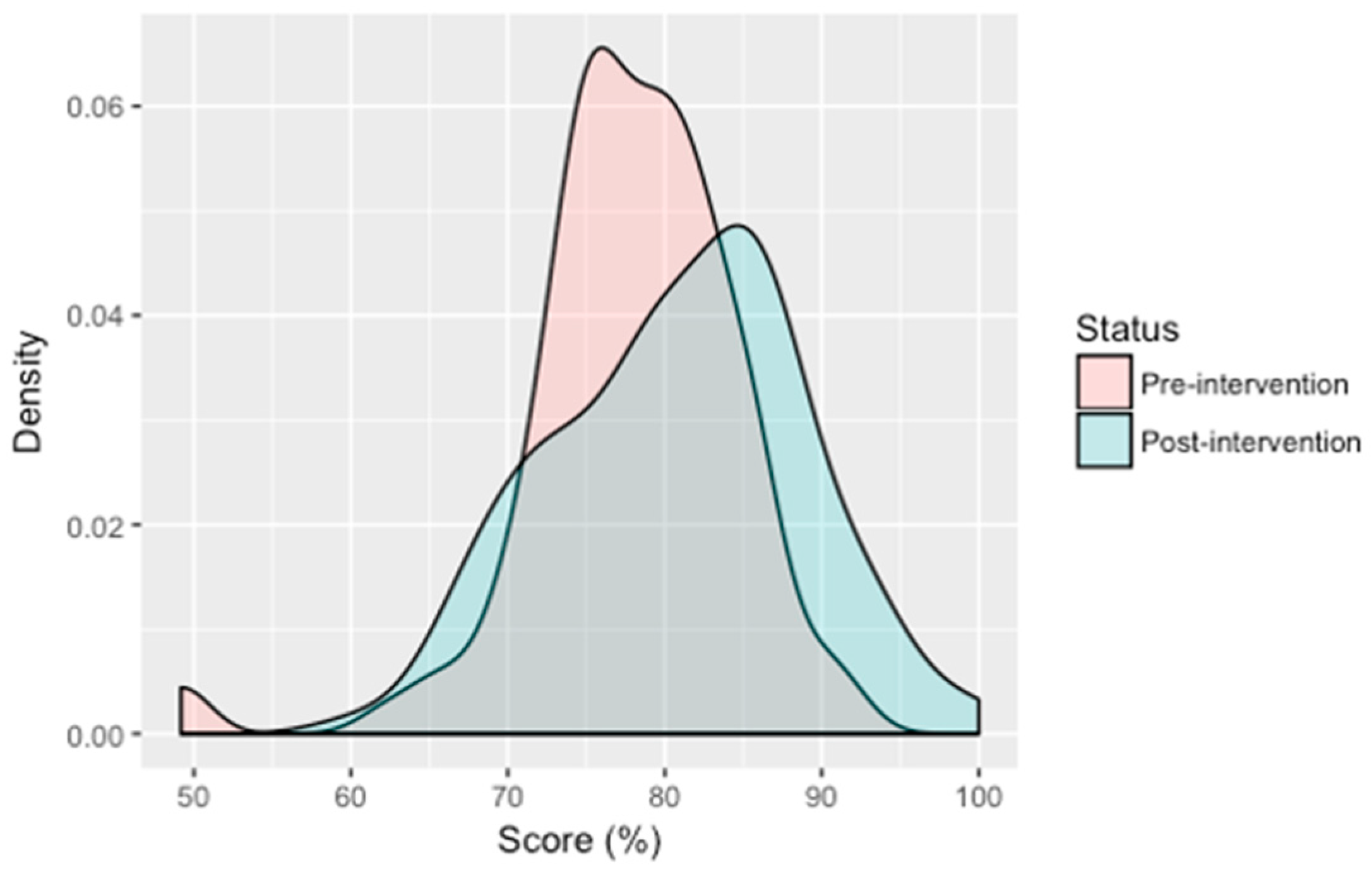
3.5. Behaviours Related to Gastrointestinal and Helminth Disease
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- WHO. Who Fact Sheet: Soil-Transmitted Helminth Infections. Available online: http://www.who.int/en/news-room/fact-sheets/detail/soil-transmitted-helminth-infections (accessed on 17 November 2017).
- Pullan, R.L.; Smith, J.L.; Jasrasaria, R.; Brooker, S.J. Global numbers of infection and disease burden of soil transmitted helminth infections in 2010. Parasit Vectors 2014, 7, 37. [Google Scholar] [CrossRef] [PubMed]
- Silver, Z.A.; Kaliappan, S.P.; Samuel, P.; Venugopal, S.; Kang, G.; Sarkar, R.; Ajjampur, S.S.R. Geographical distribution of soil transmitted helminths and the effects of community type in South Asia and South East Asia—A systematic review. PLoS Negl. Trop. Dis. 2018, 12, e0006153. [Google Scholar] [CrossRef] [PubMed]
- Gordon, C.; Kurscheid, J.; Jones, M.; Gray, D.; McManus, D. Soil-transmitted helminths in tropical Australia and Asia. Trop. Med. Infect. Dis. 2017, 2, 56. [Google Scholar] [CrossRef]
- Amoah, I.D.; Singh, G.; Stenström, T.A.; Reddy, P. Detection and quantification of soil-transmitted helminths in environmental samples: A review of current state-of-the-art and future perspectives. Acta Trop. 2017, 169, 187–201. [Google Scholar] [CrossRef] [PubMed]
- Brooker, S.; Hotez, P.J.; Bundy, D.A. Hookworm-related anaemia among pregnant women: A systematic review. PLoS Negl. Trop. Dis. 2008, 2, e291. [Google Scholar] [CrossRef] [PubMed]
- Gyorkos, T.W.; Gilbert, N.L. Blood drain: Soil-transmitted helminths and anemia in pregnant women. PLoS Negl. Trop. Dis. 2014, 8, e2912. [Google Scholar] [CrossRef] [PubMed]
- Awasthi, S.; Pande, V.K.; Fletcher, R.H. Effectiveness and cost-effectiveness of albendazole in improving nutritional status of pre-school children in urban slums. Indian Pediatr. 2000, 37, 19–29. [Google Scholar] [PubMed]
- Guernier, V.; Brennan, B.; Yakob, L.; Milinovich, G.; Clements, A.C.; Soares Magalhaes, R.J. Gut microbiota disturbance during helminth infection: Can it affect cognition and behaviour of children? BMC Infect. Dis. 2017, 17, 58. [Google Scholar] [CrossRef] [PubMed]
- Stoltzfus, R.J.; Kvalsvig, J.D.; Chwaya, H.M.; Montresor, A.; Albonico, M.; Tielsch, J.M.; Savioli, L.; Pollitt, E. Effects of iron supplementation and anthelmintic treatment on motor and language development of preschool children in Zanzibar: Double blind, placebo controlled study. BMJ 2001, 323, 1389–1393. [Google Scholar] [CrossRef] [PubMed]
- Novianty, S.; Dimyati, Y.; Pasaribu, S.; Pasaribu, A.P. Risk factors for soil-transmitted helminthiasis in preschool children living in farmland, North Sumatera, Indonesia. J. Trop. Med. 2018, 2018, 6706413. [Google Scholar] [CrossRef] [PubMed]
- Tan, M.; Kusriastuti, R.; Savioli, L.; Hotez, P.J. Indonesia: An emerging market economy beset by neglected tropical diseases (NTDs). PLoS Negl. Trop. Dis. 2014, 8, e2449. [Google Scholar] [CrossRef] [PubMed]
- WHO and Ministry of Health Indonesia. Neglected Tropical Diseases in Indonesia: An Integrated Plan of Action 2011–2015; WHO and Ministry of Health Indonesia: Jakarta, Indonesia, 2010. [Google Scholar]
- Moser, W.; Schindler, C.; Keiser, J. Efficacy of recommended drugs against soil transmitted helminths: Systematic review and network meta-analysis. BMJ 2017, 358, j4307. [Google Scholar] [CrossRef] [PubMed]
- Soeripto, N. Reinfection and infection rates of soil-transmitted-helminths in Kemiri Sewu, Yogyakarta, Indonesia. Southeast Asian J. Trop. Med. Public Health 1991, 22, 216–221. [Google Scholar] [PubMed]
- Moyer-Gusé, E. Toward a theory of entertainment persuasion: Explaining the persuasive effects of entertainment-education messages. Commun. Theory 2008, 18, 407–425. [Google Scholar] [CrossRef]
- Singhal, A.; Rogers, E.M. The status of entertainment-education worldwide. In Entertainment-Education and Social Change: History, Research, and Practice; Lawrence Erlbaum Associates Publishers: Mahwah, NJ, USA, 2004; pp. 3–20. [Google Scholar]
- Kaiser Family Foundation. Entertainment Education and Health in the United States; The Henry J. Kaiser Family Foundation: Washington, DC, USA, 2004. [Google Scholar]
- Bieri, F.A.; Gray, D.J.; Williams, G.M.; Raso, G.; Li, Y.S.; Yuan, L.; He, Y.; Li, R.S.; Guo, F.Y.; Li, S.M.; et al. Health-education package to prevent worm infections in Chinese schoolchildren. N. Engl. J. Med. 2013, 368, 1603–1612. [Google Scholar] [CrossRef] [PubMed]
- Bendrups, D.; Stewart, D.; Susilo, J. Rama and the Worm: A performance-based approach to health promotion in rural Indonesia. In Music, Health and Wellbeing: Exploring Music for Health Equity and Social Justice; Sunderland, N., Lewandowski, N., Bendrups, D., Bartleet, B.-L., Eds.; Palgrave Macmillan: London, UK, 2018; pp. 155–175. [Google Scholar]
- Park, M.J.; Clements, A.C.; Gray, D.J.; Sadler, R.; Laksono, B.; Stewart, D.E. Quantifying accessibility and use of improved sanitation: Towards a comprehensive indicator of the need for sanitation interventions. Sci. Rep. 2016, 6, 30299. [Google Scholar] [CrossRef] [PubMed]
- Medcalc Statistical Software Version 17.6; MedCalc Software bvba: Osten, Belgium, 2017.
- GBD 2015 Mortality and Causes of Death Collaborators. Global, regional, and national life expectancy, all-cause mortality, and cause-specific mortality for 249 causes of death, 1980–2015: A systematic analysis for the global burden of disease study 2015. Lancet 2016, 388, 1459–1544. [Google Scholar] [CrossRef]
- Ministry of Health Indonesia; (Jakarta, Indonesia). Personal communication, 2017.
- Smart Development Works Organization (SNV). Behaviour Change Communication Guidelines: Sustainable Sanitation & Hygiene for All; Smart Development Works Organization: Bhutan, India, 2016. [Google Scholar]
- Dway, N.S.; Soonthornworasiri, N.; Jandee, K.; Lawpoolsri, S.; Pan-Ngum, W.; Sinthuvanich, D.; Kaewkungwal, J. Effects of edutainment on knowledge and perceptions of Lisu mothers about the immunisation of their children. Health Educ. J. 2015, 75, 131–143. [Google Scholar] [CrossRef]
- Nasr, N.A.; Al-Mekhlafi, H.M.; Ahmed, A.; Roslan, M.A.; Bulgiba, A. Towards an effective control programme of soil-transmitted helminth infections among Orang Asli in rural Malaysia. Part 2: Knowledge, attitude, and practices. Parasit Vectors 2013, 6, 28. [Google Scholar] [CrossRef] [PubMed]
- Gyorkos, T.W.; Maheu-Giroux, M.; Blouin, B.; Casapia, M. Impact of health education on soil-transmitted helminth infections in schoolchildren of the peruvian amazon: A cluster-randomized controlled trial. PLoS Negl. Trop. Dis. 2013, 7, e2397. [Google Scholar] [CrossRef] [PubMed]
- Contzen, N.; De Pasquale, S.; Mosler, H.-J. Over-reporting in handwashing self-reports: Potential explanatory factors and alternative measurements. PLoS ONE 2015, 10, e0136445. [Google Scholar] [CrossRef] [PubMed]

| Knowledge Variable | Pre-Intervention Mean Score (%) | Post-Intervention Mean Score (%) | p-Value | |
|---|---|---|---|---|
| Causes of bowel infections | 7.3 | 22.7 | <0.001 a | |
| Worm infection preventative measures | Wash hands before eating | 50.2 | 77.5 | 0.014 b |
| Regularly cut fingernails | 66.0 | 76.0 | 0.009 c | |
| Wash eating/kitchen utensils with clean water | 69.0 | 79.5 | 0.006 d | |
| Keep food away from insects | 65.5 | 79.0 | 0.001 e | |
| Buy covered foods | 63.5 | 77.0 | 0.001 f | |
| Drink boiled water | 70.0 | 79.5 | 0.014 g | |
| Overall | 67.1 | 78.2 | 0.001 h | |
| Worms can cause illness | 91.7 | 95.8 | 0.235 i | |
| Symptoms of roundworm infection | 18.7 | 32.7 | <0.001 j | |
| Human faeces can contain bacteria and worm eggs | 40.5 | 63.5 | <0.001 k | |
| Defecating in river/bush can spread disease and worms | 47.0 | 65.5 | <0.001 l | |
| Faeces of healthy people can contain diseases and worm eggs | 36.0 | 55.5 | <0.001 m | |
| Defecating in river or garden is not good health behaviour | 45.0 | 63.5 | <0.001 n | |
| Overall knowledge score | 48.6 | 62.8 | <0.001 o | |
| Practices | Pre-Intervention Mean Score (%) | Post-Intervention Mean Score (%) | p-Value |
|---|---|---|---|
| Handwashing | 81.0 | 82.1 | 0.439 a |
| Soap use during handwashing | 84.0 | 87.2 | 0.261 b |
| Wearing shoes when in the paddy fields | 92.2 | 96.2 | 0.132 c |
| Wash/peel fruit | 78.2 | 81.2 | 0.441 d |
| Avoid eating raw or unboiled vegetables | 56.5 | 63.5 | 0.177 e |
| Use utensils for eating | 65.0 | 71.2 | 0.010 f |
| Avoid flies getting into food | 79.5 | 86.7 | 0.048 g |
| Avoid buying uncovered food from street vendors | 48.7 | 52.5 | 0.454 h |
| Cut fingernails frequently | 92.7 | 96.0 | 0.100 i |
| Avoid biting fingernails/sucking fingers | 96.8 | 95.8 | 0.702 j |
| Overall behaviour score | 77.4 | 80.6 | 0.004 k |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kurscheid, J.; Bendrups, D.; Susilo, J.; Williams, C.; Amaral, S.; Laksono, B.; Stewart, D.E.; Gray, D.J. Shadow Puppets and Neglected Diseases: Evaluating a Health Promotion Performance in Rural Indonesia. Int. J. Environ. Res. Public Health 2018, 15, 2050. https://doi.org/10.3390/ijerph15092050
Kurscheid J, Bendrups D, Susilo J, Williams C, Amaral S, Laksono B, Stewart DE, Gray DJ. Shadow Puppets and Neglected Diseases: Evaluating a Health Promotion Performance in Rural Indonesia. International Journal of Environmental Research and Public Health. 2018; 15(9):2050. https://doi.org/10.3390/ijerph15092050
Chicago/Turabian StyleKurscheid, Johanna, Dan Bendrups, Joko Susilo, Courtney Williams, Salvador Amaral, Budi Laksono, Donald E. Stewart, and Darren J. Gray. 2018. "Shadow Puppets and Neglected Diseases: Evaluating a Health Promotion Performance in Rural Indonesia" International Journal of Environmental Research and Public Health 15, no. 9: 2050. https://doi.org/10.3390/ijerph15092050
APA StyleKurscheid, J., Bendrups, D., Susilo, J., Williams, C., Amaral, S., Laksono, B., Stewart, D. E., & Gray, D. J. (2018). Shadow Puppets and Neglected Diseases: Evaluating a Health Promotion Performance in Rural Indonesia. International Journal of Environmental Research and Public Health, 15(9), 2050. https://doi.org/10.3390/ijerph15092050





