The Importance of Using Public Health Impact Criteria to Develop Environmental Health Indicators: The Example of the Indoor Environment in New Zealand
Abstract
1. Introduction
2. The Context
- to monitor trends in the state of the environment;
- to monitor trends in health outcomes linked to environmental hazards and exposures;
- to compare the environmental health status of geographic areas and population groups;
- to monitor the effectiveness of policies and other interventions on environmental health;
- to help raise awareness about environmental health issues; and
- to help initiate further investigations into links between the environment and health.
3. Methods
3.1. Scoping Stage
3.2. Selection Stage
3.3. Assessing the Public Health Impact of Potential Indicators
3.4. Finalising the Set of Environmental Health Indicators to Monitor
- Core set of indicators: the most important indicators to monitor to be produced annually, with factsheets, webpages, and data in an online atlas;
- Indicators for further investigation: indicators that may become core indicators but need further work and/or data to become available before a final decision is made; and
- Attributable burden indicators: to be produced occasionally (for example, every 3–5 years) to update the burden of disease attributable to a specific environmental exposure.
3.5. Design and Implementation Stage
4. Results
4.1. Scoping Stage
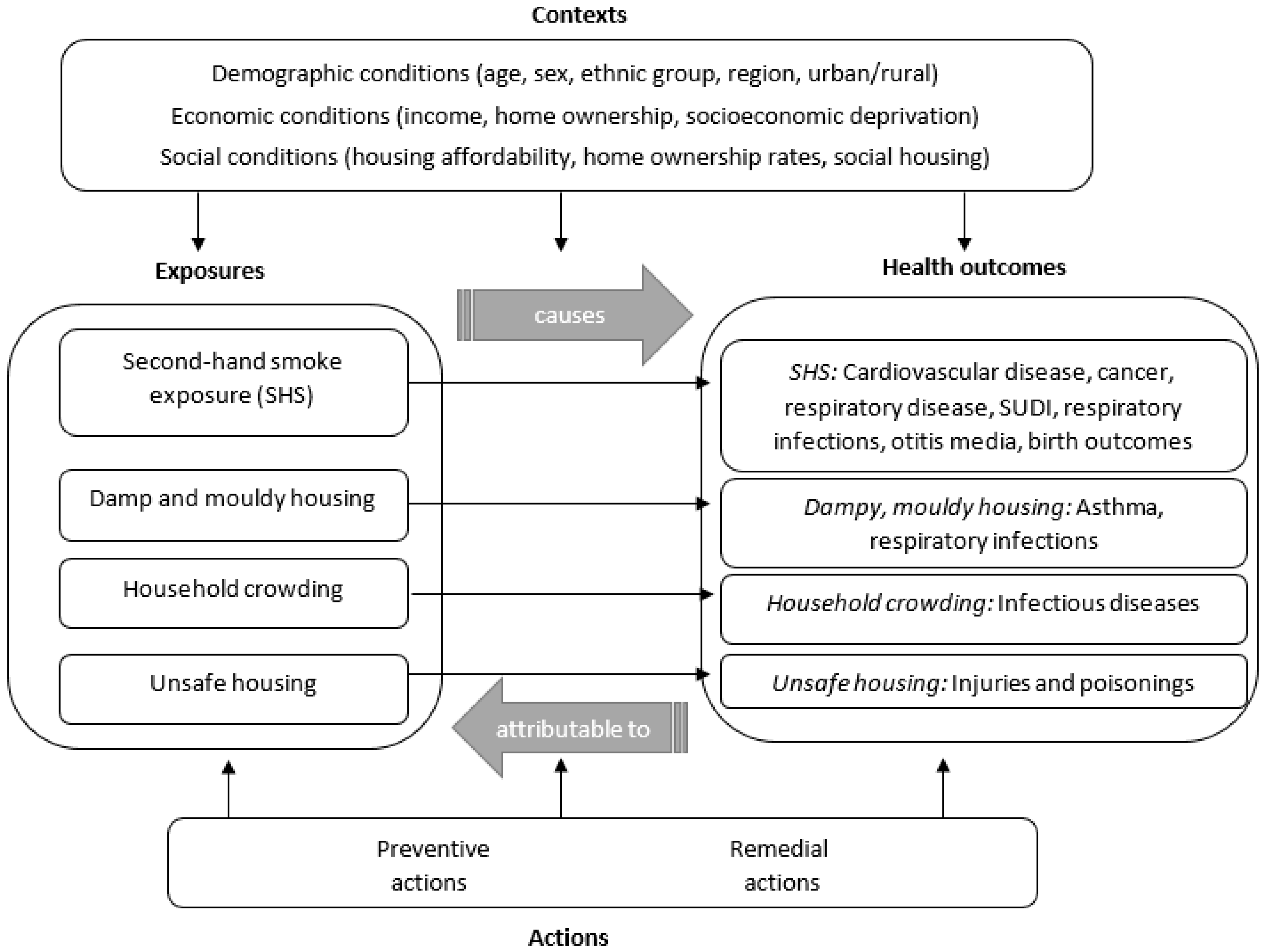
4.2. Identifying Causal Relationships
4.3. Identifying and Evaluating Potential Indicators against Indicator Selection Criteria
4.4. Assessing the Public Health Impact
4.5. Finalising the Set of Environmental Health Indicators for the Indoor Environment
4.6. Designing the Final Set of Indicators
5. Discussion
5.1. The Importance of Using a ‘Public Health Impact’ Approach to Develop Environmental Health Indicators
5.2. Findings from the Indoor Environment Indicators
5.3. Limitations of Our Approach
6. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Corválan, C.; Briggs, D.J.; Kjellstrom, T. Development of environmental health indicators. In Linkage Methods for Environment and Health Analysis. General Guidelines; Briggs, D.J., Corválan, C., Nurminen, M., Eds.; United Nations Environmental Programme, United States Environmental Protection Agency, Office of Global and Integrated Health, World Health Organization: Geneva, Switzerland, 1996; pp. 19–53. [Google Scholar]
- Briggs, D.J. Making a Difference: Indicators to Improve Children’s Environmental Health; World Health Organization: Geneva, Switzerland, 2003. [Google Scholar]
- World Health Organization. Environmental Health Indicators: Framework and Methodologies; WHO: Geneva, Switzerland, 1999. [Google Scholar]
- World Health Organization. Development of Environment and Health Indicators for European Union Countries: Results of a Pilot Study: Report On a WHO Working Group Meeting, Bonn, Germany, 7–9 July 2004; WHO Regional Office for Europe: Copenhagen, Denmark, 2004. [Google Scholar]
- Rigby, M. Principles and challenges of child health and safety indicators. Int. J. Inj. Control Saf. Promot. 2005, 12, 71–78. [Google Scholar] [CrossRef] [PubMed]
- Rigby, M.; Köhler, L. Child Health Indicators of Life and Development (CHILD): Report to the European Commission; European Union Community Health Monitoring Programme: Keele, UK, 2002. [Google Scholar]
- Commission for Environmental Cooperation. Children’s Health and the Environment in North America: A First Report on Available Indicators and Measures; Commission for Environmental Cooperation: Montreal, QC, Canada, 2006. [Google Scholar]
- Hambling, T.; Weinstein, P.; Slaney, D. A review of frameworks for developing environmental health indicators for climate change and health. Int. J. Environ. Res. Public Health 2011, 8, 2854–2875. [Google Scholar] [CrossRef] [PubMed]
- Advisory Committee on Official Statistics. Good Practice Guidelines for the Development and Reporting of Indicators; Statistics New Zealand: Wellington, New Zealand, 2009.
- World Health Organization. Environmental Health Indicators: Development of a Methodology for the WHO European Region; Interim Report; WHO Regional Office for Europe: Copenhagen, Denmark, 2000. [Google Scholar]
- Braubach, M.; Jacobs, D.; Ormandy, D. Environmental Burden of Disease Associated with Inadequate Housing; World Health Organization: Copenhagen, Denmark, 2011. [Google Scholar]
- Johnson, A.; Howden-Chapman, P.; Eaqub, S. A Stocktake of New Zealand’s Housing; New Zealand Government: Wellington, New Zealand, 2018.
- Buckett, N.; Marston, N.; Saville-Smith, K.; Jowett, J.; Jones, M. Preliminary BRANZ 2010 Housing Condition Survey Report, 2nd ed.; BRANZ Study Report 240; BRANZ Ltd.: Judgeford, New Zealand, 2011. [Google Scholar]
- Öberg, M.; Jaakkola, M.S.; Prüss-Üstün, A.; Schweizer, C.; Woodward, A. Second-Hand Smoke: Assessing the Burden of Disease at National and Local Levels; WHO Environmental Burden of Disease Series, No. 18; World Health Organization: Geneva, Switzerland, 2010. [Google Scholar]
- Public Health Advisory Committee. A Guide to Health Impact Assessment: A Policy Tool for New Zealand; Public Health Advisory Committee: Wellington, New Zealand, 2005. [Google Scholar]
- Mason, K.; Borman, B. Burden of disease from second-hand smoke exposure in New Zealand. N. Z. Med. J. 2016, 129, 16–25. [Google Scholar] [PubMed]
- Baker, M.; McDonald, A.; Zhang, J.; Howden-Chapman, P. Infectious Diseases Attributable to Household Crowding in New Zealand: A Systematic Review and Burden of Disease Estimate; He Kainga Oranga/Housing and Health Research Programme, University of Otago: Wellington, New Zealand, 2013. [Google Scholar]
- Fisk, W.J.; Lei-Gomez, Q.; Mendell, M.J. Meta-analyses of the associations of respiratory health effects with dampness and mold in homes. Indoor Air 2007, 17, 284–296. [Google Scholar] [CrossRef] [PubMed]
- Statistics New Zealand. Perceptions of Housing Quality in 2014/15. Available online: http://archive.stats.govt.nz/browse_for_stats/people_and_communities/housing/perceptions-housing-quality-2014-15.aspx (accessed on 28 May 2018).
- Telfar Barnard, L.; Zhang, J. The Impact of Respiratory Disease in New Zealand: 2016 Update; Asthma and Respiratory Foundation NZ: Wellington, New Zealand, 2016. [Google Scholar]
- Gulliver, P.; Dow, N.; Simpson, J. The epidemiology of home injuries to children under five years in New Zealand. Aust. N. Z. J. Public Health 2005, 29, 29–34. [Google Scholar] [CrossRef] [PubMed]
- Eayres, D. Commonly Used Public Health Statistics and Their Confidence Intervals: Technical Briefing 3; Association of Public Health Observatories: York, UK, 2008. [Google Scholar]
- Atkinson, J.; Salmond, C.; Crampton, P. NZDep2013 Index of Deprivation; Department of Public Health, University of Otago, Wellington: Wellington, New Zealand, 2014. [Google Scholar]
- Statistics New Zealand. Living in a Crowded House: Exploring Ethnicity and Well-Being of People in Crowded Households; Statistics New Zealand: Wellington, New Zealand, 2018.
- Ministry of Health. Tobacco Use 2012/13: New Zealand Health Survey; Ministry of Health: Wellington, New Zealand, 2014.
- Prezant, B.; Douwes, J. Calculating the Burden of Disease Attributable to Indoor Dampness in New Zealand. 2011. Available online: http://www.academia.edu/27232468/Calculating_the_burden_of_disease_attributable_to_indoor_dampness_in_NZ (accessed on 28 May 2018).
- U.S. Department of Health and Human Services. The Health Consequences of Smoking—50 Years of Progress. A Report of the Surgeon General; U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, National Center for Chronic Disease Prevention and Health Promotion, Office on Smoking and Health: Atlanta, GA, USA, 2014.
- U.S. Surgeon General. The Health Consequences of Involuntary Exposure to Tobacco Smoke—A Report of the Surgeon General; U.S. Department of Health and Human Services, Public Health Service, Office of the Surgeon General: Rockville, MD, USA, 2006.
- Cal-EPA. Proposed Identification of Environmental Tobacco Smoke as a Toxic Air Contaminant; California Environmental Protection Agency, Air Resources Board: Sacramento, CA, USA, 2005.
- Lee, C.C.; Middaugh, N.A.; Howie, S.R.; Ezzati, M. Association of secondhand smoke exposure with pediatric invasive bacterial disease and bacterial carriage: A systematic review and meta-analysis. PLoS Med. 2010, 7, e1000374. [Google Scholar] [CrossRef] [PubMed]
- Murray, R.L.; Britton, J.; Leonardi-Bee, J. Second hand smoke exposure and the risk of invasive meningococcal disease in children: Systematic review and meta-analysis. BMC Public Health 2012, 12, 1062. [Google Scholar] [CrossRef] [PubMed]
- Johnson, K.C.; Miller, A.B.; Collishaw, N.E.; Palmer, J.R.; Hammond, S.K.; Salmon, A.G.; Cantor, K.P.; Miller, M.D.; Boyd, N.F.; Millar, J.; et al. Active smoking and secondhand smoke increase breast cancer risk: The report of the Canadian expert panel on tobacco smoke and breast cancer risk (2009). Tob. Control 2011, 20, e2. [Google Scholar] [CrossRef] [PubMed]
- Eisner, M.D.; Balmes, J.; Katz, P.P.; Trupin, L.; Yelin, E.H.; Blanc, P.D. Lifetime environmental tobacco smoke exposure and the risk of chronic obstructive pulmonary disease. Environ. Health 2005, 4, 7. [Google Scholar] [CrossRef] [PubMed]
- Kanchongkittiphon, W.; Mendell, M.J.; Gaffin, J.M.; Wang, G.; Phipatanakul, W. Indoor environmental exposures and exacerbation of asthma: An update to the 2000 review by the institute of medicine. Environ. Health Perspect. 2015, 123, 6–20. [Google Scholar] [CrossRef] [PubMed]
- Palaty, C.; Shum, M. Health Effects from Mould Exposure or Dampness in Indoor Environments; National Collaborating Centre for Environmental Health: Vancouver, BC, Canada, 2012. [Google Scholar]
- BPAC. The Changing Face of Helicobacter pylori Testing; Best Tests; BPAC: Dunedin, New Zealand, 2014. [Google Scholar]
- Das, D.; Baker, M.; Venugopal, K.; McAllister, S. Why the tuberculosis incidence rate is not falling in New Zealand. N. Z. Med. J. 2006, 119, U2248. [Google Scholar] [PubMed]
- Ministry of Health. New Zealand Maternity Clinical Indicators 2016; Ministry of Health: Wellington, New Zealand, 2018.
- Ministry of Health. Annual Update of Key Results 2015/16: New Zealand Health Survey; Ministry of Health: Wellington, New Zealand, 2016.
- HQSC. Atlas of Healthcare Variation Methodology: Asthma; Health Quality and Safety Commission: Wellington, New Zealand, 2016.
- Simpson, J.; Duncanson, M.; Oben, G.; Adams, J.; Wicken, A.; Butchard, M.; Pierson, M.; Lilley, R.; Gallagher, S. The Health Status of Children and Young People in New Zealand 2015; New Zealand Child and Youth Epidemiology Service, University of Otago: Dunedin, New Zealand, 2016. [Google Scholar]
- Ministry of Health. Fetal and Infant Deaths 2014; Ministry of Health: Wellington, New Zealand, 2017.
- Pond, K.; Kim, R.; Carroquino, M.-J.; Pirard, P.; Gore, F.; Cucu, A.; Nemer, L.; MacKay, M.; Smedje, G.; Georgellis, A.; et al. Workgroup report: Developing environmental health indicators for European children: World Health Organization working group. Environ. Health Perspect. 2007, 115, 1376–1382. [Google Scholar] [CrossRef] [PubMed]

| Indicator Selection Criteria | Explanation |
|---|---|
| Data availability | Indicator must have data that can be easily and reliably extracted. |
| Scientifically valid | Indicator must have an established, scientifically sound link to the environmental health issue. |
| Sensitive | Indicator should respond relatively quickly and noticeably to changes but not show false movements. |
| Consistent | Indicator should be consistent with those used in other indicator programmes (including internationally) so comparisons can be made. |
| Comparable | Indicator should be consistent to allow comparisons over time. |
| Methodologically sound measurement | Indicator measurement needs to be methodologically sound. |
| Intelligible and easily interpreted | Indicator should be sufficiently simple to be interpreted in practice and be intuitive in the sense that it is obvious what the indicator is measuring. |
| Able to be disaggregated | Indicator needs to be able to be broken down into population subgroups or areas of particular interest, such as ethnic groups or regional areas. |
| Timely | Data needs to be collected and reported regularly and frequently to ensure it is reflecting current and not historical trends. |
| Public Health Impact Selection Criteria | Explanation |
|---|---|
| Public health impact | Indicator needs to relate to an environmental health issue of significant public health impact to New Zealand. This health impact may include affecting a large number of people, a vulnerable population, or Māori health; or having substantial policy relevance. |
| (i) Affecting a large number of people | Priority should be given to health effects affecting larger numbers of people (i.e., with a higher burden of disease attributable to the environmental exposure (e.g., measured as deaths, hospitalisations, or disability-adjusted life years (DALYs))), within the country/area of interest. |
| (ii) Severity of impact | Priority should be given to health conditions with severe impacts, such as severity of illness, long-term repercussions (such as disability or long-term illness), and/or risk of death. |
| (iii) Affecting vulnerable populations and/or having large inequalities | Priority should be given to health effects that particularly affect vulnerable population groups and/or have large health inequalities. |
| (iv) Relating to multiple exposures or health effects | Priority should be given to health indicators that link to multiple environmental exposures. |
| (v) Relevant to policy | Priority should be given to indicators where there is potential for policy actions about the environmental exposure to make a difference; and/or the issue is of current policy interest. |
| Environmental Exposure | Pathway | People Exposed | Health Effects—Causal (Level 1) | Health Effects—Suggestive (Level 2) |
|---|---|---|---|---|
| Household crowding | Household crowding | Children living in crowded households | GastroenteritisPneumonia/lower respiratory tract infection Bronchiolitis from respiratory syncytial virus (RSV) infection Haemophilus influenzae (Hib disease) Meningococcal disease | Upper respiratory tract infection Serious skin infections Acute rheumatic fever |
| People (all ages) living in crowded households | Hepatitis A Helicobacter pylori infection Tuberculosis | |||
| Second-hand smoke (SHS) exposure | Maternal smoking and/or exposure to SHS | Babies exposed to SHS through maternal smoking | Sudden unexpected death in infancy (SUDI) | |
| Maternal exposure to SHS during pregnancy | Babies exposed to SHS in utero (non-smoking mother exposed to SHS) | Small for gestational age (low birthweight) | Preterm delivery | |
| Second-hand smoke exposure in the home | Children exposed to SHS in the home | Asthma Lower respiratory tract infection (including bronchitis, bronchiolitis, pneumonia, and acute respiratory infection) Otitis media | Meningococcal disease | |
| Non-smoking adults exposed to SHS in the home | Ischaemic heart disease Stroke Lung cancer | Asthma (induction, exacerbation) Breast cancer Chronic obstructive pulmonary disease (COPD) | ||
| Damp, mouldy, cold houses | Damp and mould | Children living in damp and mouldy houses | Asthma exacerbation | Respiratory infections, bronchitis |
| Adults living in damp and mouldy houses | Asthma exacerbation Respiratory infections, bronchitis | |||
| Unsafe home environment | Physical hazards in the home | Children | Falls Burns | Drowning |
| Hazardous chemicals in the home | Children | Poisonings |
| Potential Indicator | Data Source | Meet All Criteria? | Indicator Selection Criteria | Comments | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Data Availability | Scientifically Valid | Sensitive to Change | Consistent | Comparable | Methodologically Sound | Intelligible and Easily Interpreted | Able to Be Disaggregated | Timely | ||||
| Exposure indicators | ||||||||||||
| People living in crowded households | Census | Yes | √ | √ | √ | √ | √ | √ | √ | √ | √ | Both children and total population are important to monitor. |
| People exposed to SHS in the home | NZHS | Yes | √ | √ | √ | √ | √ | √ | √ | √ | √ | Both children and adults are important to monitor. |
| Mothers smoking at two weeks postnatal | Maternity | Yes | √ | √ | √ | √ | √ | √ | √ | √ | √ | |
| People living in damp and mouldy houses | Census (living in damp and mouldy houses) | No | × | √ | √ | √ | √ | √ | √ | √ | √ | Data about people living in damp and mouldy houses are not currently available but will be available in 2019 from the 2018 Census. Not known if this data will be collected again. |
| NZGSS | No | × | √ | √ | √ | √ | √ | √ | ? | ? | Only adults are covered, not children. Data collected twice (2010 and 2014)—unknown if it will be collected again. | |
| Census (no source of home heating) | No | √ | × | √ | √ | √ | √ | √ | √ | √ | Data about households with no source of home heating could be a proxy for cold houses, which are associated with damp and mouldy housing. However, this is not a good measure of cold houses (for example, some people do not use available home heating due to cost) or damp and mouldy houses and will mis-measure the true value. | |
| Health indicators | ||||||||||||
| Lower respiratory tract infection hospitalisations in children | NMDS | Yes | √ | √ | √ | √ | √ | √ | √ | √ | √ | Evidence for 0–1 years (SHS) and 0–5 years (household crowding) |
| Bronchiolitis from RSV hospitalisations | NMDS | Yes | √ | √ | √ | √ | √ | √ | √ | √ | √ | Bronchiolitis is also included in the definition for lower respiratory tract infection. |
| Helicobacter pylori infection hospitalisations | NMDS | No | √ | √ | × | √ | √ | √ | √ | √ | √ | Hospitalisations are for sequelae of H. pylori infection, including non-cardia gastric cancer, peptic ulcer, gastritis, and duodenitis. There can be a large lag time between exposure and health effects. |
| Gastroenteritis hospitalisations | NMDS | Yes | √ | √ | √ | √ | √ | √ | √ | √ | √ | |
| Tuberculosis hospitalisations | NMDS | Yes | √ | √ | √ | √ | √ | √ | √ | √ | √ | |
| Meningococcal disease notifications | EpiSurv | Yes | √ | √ | √ | √ | √ | √ | √ | √ | √ | Evidence for 0–16 years (household crowding) and suggested link with SHS |
| Hepatitis A hospitalisations | NMDS | Yes | √ | √ | √ | √ | √ | √ | √ | √ | √ | |
| Haemophilus influenzae (Hib disease) hospitalisations | NMDS | Yes | √ | √ | √ | √ | √ | √ | √ | √ | √ | One of the ICD-10-AM codes for Hib disease (J14) is also included in the definition for lower respiratory tract infection. |
| Asthma prevalence in children | NZHS | Yes | √ | √ | √ | √ | √ | √ | √ | √ | √ | Evidence for 0–14 years (SHS, dampness/mould). |
| Asthma hospitalisations in children | NMDS | Yes | √ | √ | √ | √ | √ | √ | √ | √ | √ | Evidence for 0–14 years (SHS, dampness/mould). Asthma hospitalisations are a proxy for asthma exacerbation. |
| Sudden unexpected death in infancy (SUDI) | MoH | Yes | √ | √ | √ | √ | √ | √ | √ | √ | √ | Strong evidence for mothers smoking after birth |
| Otitis media/grommets hospitalisations in children | NMDS | Yes | √ | √ | √ | √ | √ | √ | √ | √ | √ | |
| Ischaemic heart disease hospitalisations/deaths in non-smoking adults | NMDS/Mort | No | × | √ | × | √ | √ | √ | √ | √ | √ | Difficult to get data for non-smokers. Lag-time of 1–5 years after exposure. |
| Stroke hospitalisations/deaths in non-smoking adults | NMDS/Mort | No | × | √ | × | √ | √ | √ | √ | √ | √ | Difficult to get data for non-smokers. Lag-time of 1–5 years after exposure. |
| Lung cancer registrations/deaths in non-smoking adults | Cancer/Mort | No | × | √ | × | √ | √ | √ | √ | √ | √ | Difficult to get data for non-smokers. Lag-time of 10–20 years after exposure. |
| Small for gestational age (low birthweight) | Maternity | Yes | √ | √ | √ | √ | √ | √ | √ | √ | √ | Data are available for proportion of all babies born at term gestation who are small for their gestational age. |
| Unintentional injuries in the home in children | NMDS | Yes | √? | √ | √ | √ | √ | √ | √ | √ | √ | The data exists, but it depends whether location data is robust enough to include. Needs further investigation. |
| Falls in the home in children | NMDS | Yes | √? | √ | √ | √ | √ | √ | √ | √ | √ | |
| Burns in the home in children | NMDS | Yes | √? | √ | √ | √ | √ | √ | √ | √ | √ | |
| Poisonings in the home in children | NMDS | Yes | √? | √ | √ | √ | √ | √ | √ | √ | √ | |
| Potential Health Indicator | Health Condition (Relating to Potential Health Indicator) | Age Group for Attributable Burden Evidence | Met All Other Indicator Selection Criteria? | Public Health Impact Criteria | Recommend | |||||
|---|---|---|---|---|---|---|---|---|---|---|
| (i) Proportion Attributable (PAF, %) | (i) Attributable Burden | (ii) Severity of Impact | (iv) Vulnerable Populations Affected and/or Inequalities | (iii) Multiple Exposures | (v) Specific Policy Relevance of Indicator | |||||
| Household Crowding Indicators | Annual Attributable Hospitalisations (2007–2011) [17] | |||||||||
| Lower respiratory tract infection hospitalisations | Lower respiratory infections/pneumonia | 0–5 years | Yes | 10% | 669 | Short-term, rarely fatal | Children, Māori, Pacific | Yes | Core | |
| Bronchiolitis hospitalisations | Bronchiolitis from RSV | 0–3 years | Yes | 16% | 644 | Short-term, rarely fatal | Children, Māori, Pacific | |||
| Hospitalisations for sequelae of Helicobacter pylori infection | Helicobacter pylori infection | 0+ years | Yes | 8% | 102 | Long-term, can lead to other health problems; not all H. pylori infection leads to health impacts | Māori, Pacific peoples | |||
| Gastroenteritis hospitalisations | Gastroenteritis | 0–5 years | Yes | 2% | 42 | Short-term, rarely fatal in New Zealand | Children | |||
| Tuberculosis notifications | Tuberculosis | 15+ years | Yes | 19% | 22 | Long-term; takes a long time to treat and cure; can have some sequelae. | Māori adults, Pacific adults | In New Zealand, little disease transmission takes place within-country | ||
| Meningococcal disease notifications | Meningococcal disease | 0–16 years | Yes | 15% | 5 | Can be fatal and may cause long-term disability | Children, Māori, Pacific peoples | Yes (second-hand smoke Level 2) | An epidemic in the 2000s led to national vaccination campaign | Core |
| Hepatitis A hospitalisations | Hepatitis A | 0+ years | Yes | 5% | 1 | |||||
| Hospitalisations for Haemophilus influenza type b | Haemophilus influenzae type b | 0–6 years | Yes | 10% | 0.7 | Children | ||||
| Second-Hand Smoke Exposure Indicators | Attributable DALYs (2006) [16] | |||||||||
| Ischaemic heart disease hospitalisations/deaths in non-smoking adults | Ischaemic heart disease | 15+ years non-smokers | No | 1.5% | 1033 | Can be fatal | ||||
| Stroke hospitalisations/deaths in non-smoking adults | Stroke | 35+ years non-smokers | No | 1.3% | 389 | Can be fatal, cause long-term disability | ||||
| Lung cancer registrations/deaths in non-smoking adults | Lung cancer | 15+ years non-smokers | No | 2.2% | 96 | Often fatal | ||||
| Sudden unexpected death in infancy (SUDI) | SUDI | 0 years | Yes | 11.3% | 596 | Fatal | Children, Māori | SUDI prevention activities are funded in New Zealand | Core | |
| Asthma prevalence | Asthma (onset, ever had asthma) | 0–14 years | Yes | 3.1% | 93 | Long-term, rarely fatal | Children, Māori | Yes | Core | |
| Lower respiratory tract infection hospitalisations | Lower respiratory tract infections | 0–1 years | Yes | 3.1% | 42 | Short-term, rarely fatal | Children, Māori | Yes | Core | |
| Otitis media hospitalisations (acute; grommets) | Otitis media | 0–14 years | Yes | 2.6% | 31 | Short-term | Children, Māori | |||
| Small for gestational age | Low birthweight at term | 0 years | Yes | 2.5% | 6 | Can lead to long-term effects | Children, Māori | |||
| Damp and Mouldy Housing Indicator | Annual Attributable Hospitalisations (2015) | |||||||||
| Asthma hospitalisations | Asthma exacerbation | 0–14 years | Yes | 15% | 537 | Long-term illness | Children, Māori, Pacific | Yes | Core | |
| Unsafe Environments Indicator | Annual Impacts (1989–1998) [21] | |||||||||
| Unintentional injuries hospitalistations (for injuries occurring in the home) | Unintentional injuries in the home | 0–4 years | Yes | Not available | 39 deaths; 2464 hospital admissions (total numbers) | Can be fatal, may cause long-term disability | Children | Core, but subject to further investigation of data quality for location data | ||
| Indicator | Age Group | Data Source | Design Details | Latest Results for New Zealand (Year of Data) |
|---|---|---|---|---|
| Exposures | ||||
| Proportion of people living in crowded households | 0–14 years, Total population | Census | People living in a house requiring one or more additional bedrooms, according to the Canadian National Occupancy Standard [24] | 10% of total population; 16% of children; 25% of Māori children; and 43% of Pacific children (2013) |
| Proportion of children and non-smoking adults exposed to second-hand smoke in the home | 0–14 years 15+ years | New Zealand Health Survey | People reporting that someone smoked inside the house [25] | 5.0% of children; 3.7% of non-smoking adults; and 9.2% of Māori children (2012/13) |
| Mothers smoking at two weeks postnatal | All mothers who gave birth in that year | New Zealand Maternity Clinical Indicators | Mothers who reported that they smoked at two weeks after birth, among all mothers who reported a smoking status at two weeks after birth [38] | 12% of mothers; and 32% of Māori mothers (2015) |
| Health Effects | ||||
| Prevalence of asthma in children | 2–14 years | New Zealand Health Survey publications | Children aged 2–14 years who have been diagnosed by a doctor as having asthma, and who are currently using inhalers, medicine, tablets, pills, or other medication for it [39] | 16.6% of children; 24.0% of Māori children; and 17.4% of Pacific children (2015/2016) |
| Asthma hospitalisations in children | 0–14 years | National Minimum Dataset | Acute and semi-acute hospitalisations with asthma (ICD-10AM J45–J46) or wheeze (R06.2) as the primary diagnosis, for children aged 0–14 years. Analyses excluded overseas visitors, deaths, and transfers within and between hospitals. Wheeze is included as there is evidence that paediatricians are more likely to diagnose suspected asthma as wheeze for younger children in New Zealand [40,41]. | 682 hospitalisations per 100,000 children; 838 per 100,000 (Māori); and 1324 per 100,000 (Pacific) (2016) |
| Lower respiratory tract infection hospitalisations in children | 0–4 years | National Minimum Dataset | Acute and semi-acute hospitalisations with pneumonia (ICD-10AM J12–J16, J18), bronchitis (J20), bronchiolitis (J21) or unspecified acute lower respiratory tract infection (J22) as the primary diagnosis, for children aged 0–4 years. | 3050 hospitalisations per 100,000 children; 4254 per 100,000 (Māori); and 6711 per 100,000 (Pacific) (2016) |
| Meningococcal notifications | 0–14 years | EpiSurv | Notifications of meningococcal disease, in children aged 0–14 years. | 35 notifications; highest rates in Māori and Pacific children (2016) |
| Sudden unexpected death in infancy (SUDI) | 0 years | Fetal and infant deaths publication | Deaths in children aged under one year of age (<1 year old) with an underlying cause of death in the following ICD-10AM codes: R95, R96, R98, R99, W75, W78, W79. Rates are presented per 1000 live births [42]. | 45 deaths; highest rate in Māori babies (2014) |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Mason, K.; Lindberg, K.; Read, D.; Borman, B. The Importance of Using Public Health Impact Criteria to Develop Environmental Health Indicators: The Example of the Indoor Environment in New Zealand. Int. J. Environ. Res. Public Health 2018, 15, 1786. https://doi.org/10.3390/ijerph15081786
Mason K, Lindberg K, Read D, Borman B. The Importance of Using Public Health Impact Criteria to Develop Environmental Health Indicators: The Example of the Indoor Environment in New Zealand. International Journal of Environmental Research and Public Health. 2018; 15(8):1786. https://doi.org/10.3390/ijerph15081786
Chicago/Turabian StyleMason, Kylie, Kirstin Lindberg, Deborah Read, and Barry Borman. 2018. "The Importance of Using Public Health Impact Criteria to Develop Environmental Health Indicators: The Example of the Indoor Environment in New Zealand" International Journal of Environmental Research and Public Health 15, no. 8: 1786. https://doi.org/10.3390/ijerph15081786
APA StyleMason, K., Lindberg, K., Read, D., & Borman, B. (2018). The Importance of Using Public Health Impact Criteria to Develop Environmental Health Indicators: The Example of the Indoor Environment in New Zealand. International Journal of Environmental Research and Public Health, 15(8), 1786. https://doi.org/10.3390/ijerph15081786





