Abstract
Mortality in many parts of the world has a seasonal pattern, with a marked excess of deaths during winter. To date, however, there is very little published evidence on the nature of this wintertime excess in low- and middle-income countries. In this study, we aimed to quantify the extent of the death peak in winter and to assess effect modification on excess winter death (EWD) by individual characteristics and cause of deaths in China. We used a Cosinor model to examine seasonal patterns for specific causes of deaths and a case-only analysis of deaths in winter compared with other seasons to assess effect modification by individual characteristics. A total of 398,529 deaths were investigated between January 2010 and December 2013 in Zhejiang Province, China. Deaths peaked in winter, and overall mortality was around 30% higher in winter than in summer. Although diseases of the respiratory and circulatory systems were highly seasonal, surprisingly we observed that deaths from mental and behavioral disorders exhibited greater fluctuation. Males, the elderly and illiterate individuals suffered high EWD. EWDs were also particularly common in emergency rooms, at home, on the way to hospitals, and in nursing homes/family wards. This study highlighted the high EWD in some previously unreported groups, indicating new information to facilitate the targeting of necessary preventive measures to those at greatest risk in order to mitigate wintertime death burdens.
1. Background
Despite long-term improvements in healthcare, housing and other factors, seasonal variation in mortality remains a problem in many parts of the world, with a marked excess of deaths still present during winter months [1]. Much of this excess winter mortality can be attributed to exposure to wintertime weather, especially ambient temperature; however, other factors such as seasonal infections are also important. A common and straightforward way to measure this wintertime excess is to calculate the Excess Winter Death (EWD) statistic. This metric is the ratio of deaths in the winter period compared with deaths in the non-winter period [2]. Although subject to interpretational limitations [3], the EWD value is a useful tool to quantify the overall health burden associated with the winter months and it is readily comparable between different populations. A population-based study in the UK showed a 30% increase in winter deaths [4], and similar winter increases have been found in other countries in Europe and also in the United States, Canada, Australia, New Zealand and Japan [5,6,7,8,9,10].
To date, however, there is very little published evidence on the nature of this wintertime excess in low- and middle-income countries [11]. EWD was explored in a study from Burkina Faso; however, this was based on only 4098 deaths [12]. Although the explicit relationships between temperature and mortality have now been characterized in China [13], evidence of EWD in Chinese populations is still very limited despite the large populations involved and the varied climatic and socio-economic conditions. The Ou et al. study reported a 26% wintertime excess in all-cause mortality in the subtropical city of Guangzhou, China [14]. Mortality records from China contain rich information on individual characteristics such as education level and place of death and so allow for the EWD metric to be calculated for important sub-groups of the population which can inform more targeted interventions. Previous studies did consider EWD modification by cause of death, sex, age, education and place of death, but categorizations were limited.
Evidence of EWD-modification by disease mainly relates to broad cause-of-death groups. Although influenza epidemics contribute to the winter increase in mortality, the effect is more general with variation in other respiratory, cardiovascular and cerebrovascular diseases [6]. The winter increase is apparent at all ages but is greatest in relative and absolute terms in elderly people [4]. Besides factors associated with biological and genetic considerations that have been linked with reduced health status, the health of a population is influenced by a large number of factors such as socioeconomic status, behavioral patterns and environmental parameters [7,15]. Some studies have also reported that EWD risk is greater in more deprived groups; however, these are usually based on area-level measures of deprivation [16]. Other factors such as place of death and more specific causes of death have generally not been fully explored in most settings around the world, usually because of power limitations. Assessment of the large populations of China allows us to address this research gap.
Understanding seasonal patterns in mortality and the underlying causes of excess winter mortality have clear implications for many aspects of public health as these could be used to guide targeted health-related interventions. In this study, we examined all-cause mortality in Zhejiang Province in China to quantify the extent to which deaths peak in winter and to explore differences according to the primary cause of death. We also examined the degree to which excess winter mortality is modified by individual socio-demographic characteristics. We hypothesize that some sub-groups of the population will exhibit greater EWD and thus should be the priority for public health intervention measures.
2. Methods
2.1. Study Setting
Zhejiang is an eastern coastal province of China. It has a mainly subtropical monsoon climate, with a clear division of four seasons. Winters are often dry and cold with low temperatures and little rainfall; summers are usually wet and hot with high temperatures. The average annual temperature in Zhejiang Province is 15–18 °C, and its coldest and hottest days are usually seen in January and July, respectively. The province is divided into eleven prefecture-level divisions, and they are subdivided into 90 county-level divisions (32 districts, 22 county-level cities, 36 counties). Han Chinese people make up the vast majority of the population.
2.2. Data Source
Death data were collected from the Chinese National Disease Surveillance System. We obtained a total of 30 county-level surveillance sites across the whole Zhejiang Province from January 2010 to December 2013. The death certificate includes demographic and other important information, such as gender, nationality (race), marital status, education, date of death, date of birth, and place of death. Medical conditions are also listed on death certificates according to the International Classification of Diseases, 10th Revision (ICD-10). In China, either a medical practitioner or a coroner is required to certify the cause of death, and they should report on all underlying conditions that directly caused or contributed to the death.
2.3. Statistical Analysis
In a descriptive analysis, we plotted the monthly number of deaths in all regions by ICD chapter. The plots showed a strong annual seasonal pattern, and hence we examined the effect of season for specific causes using a Cosinor model and assumed a single annual cycle [17]. We fitted a separate model for each ICD chapter and adjusted for a linear trend over time. The Cosinor model estimates the increase in seasonal deaths (amplitude) and the location of the peak increase (phase). Due to low numbers of deaths (fewer than 50), we excluded the following ICD chapters for analysis: Diseases of the eye and adnexa; Diseases of the ear and mastoid process; and Pregnancy, childbirth and the puerperium.
We used a case-only analysis to identify individual characteristics that may increase the risk of dying during winter. This is a logistic regression model with winter death (yes/no) as the dependent variable and individual characteristics (e.g., age, gender, education) as the independent variables. We started with a model with all the available individual characteristics and then removed variables that appeared to be co-linear based on the variance inflation factor (VIF). We present the results as prevalence ratios and 95% confidence intervals (CIs) rather than odds ratios, as prevalence ratios are easier to interpret because they can be used as direct multipliers (e.g., twice as likely to die in winter) [18].
The case-only design was originally proposed to improve efficiency in the study of gene-environment interactions by examining the prevalence of a specific genotype only among cases. As Gouveia suggested [19], this approach can be used to investigate how individual characteristics that do not vary over time (e.g., gender or socioeconomic status) modify the effect of a time-varying exposure (e.g., season) on the outcome of interest by restricting the sample to cases (e.g., deaths). In our study, we applied this approach by comparing the individual characteristics of those dying in winter with those dying in other seasons. If an individual characteristic increases the risk of dying in winter, the proportion of deaths with that characteristic will be larger in winter. However, it should be noted that in the case-only design, a negative rate ratio does not necessarily indicate a decrease in the risk of dying for the group of individuals examined. Rather, this indicates that the increase in the risk of dying is less pronounced in winter for that group of individuals [20].
3. Results
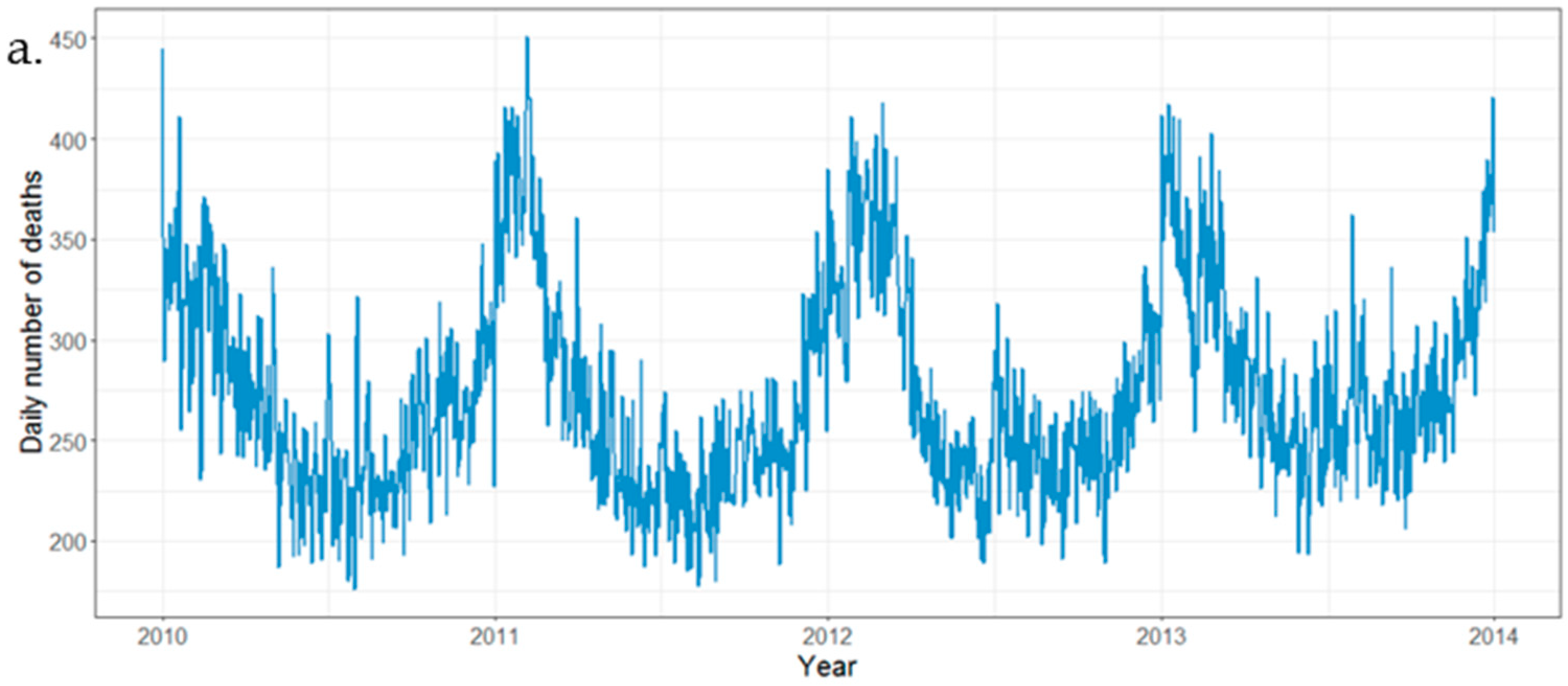
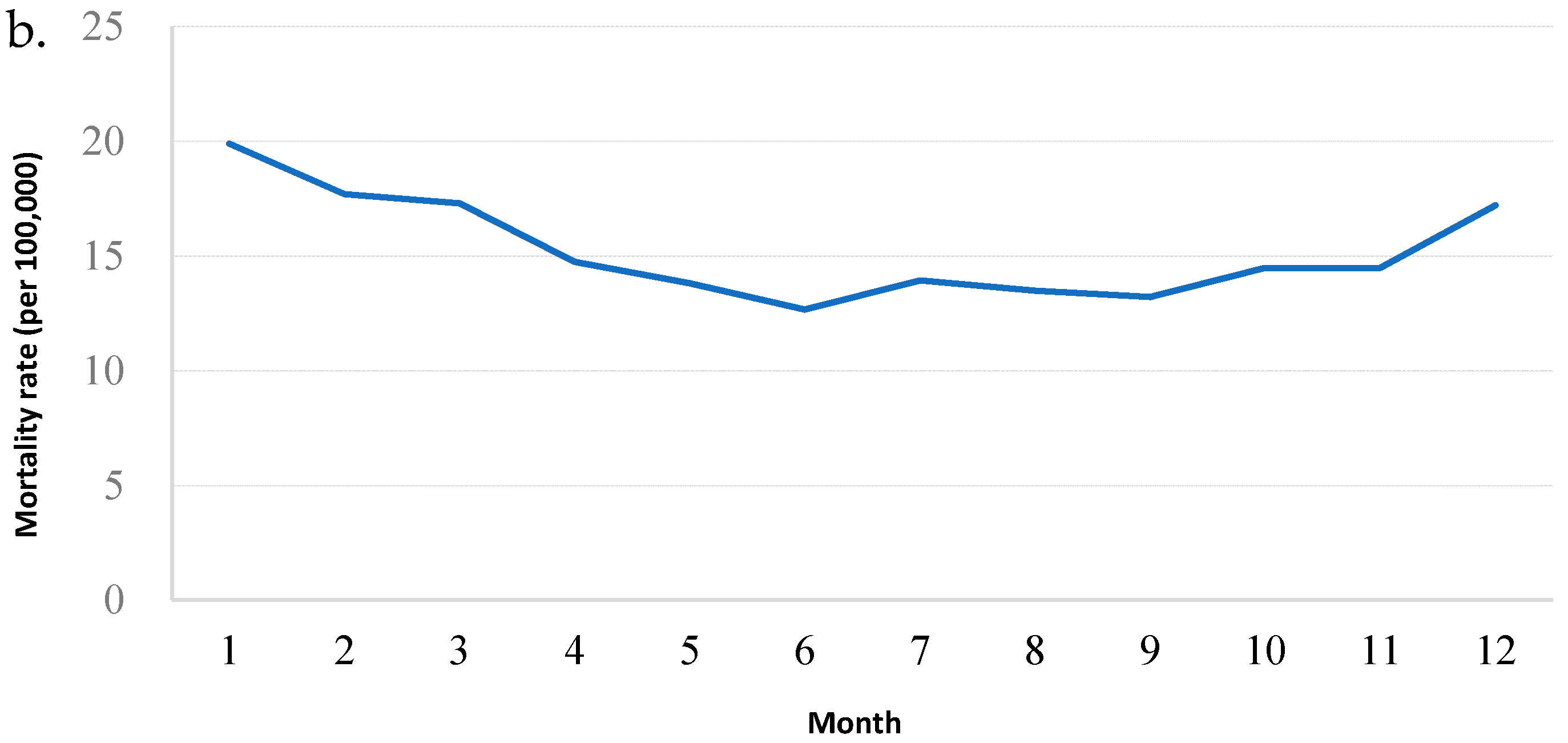
During the four-year period of 2010–2013, there were 398,529 deaths registered in 30 counties in Zhejiang Province, with an average of 364 deaths per day (Table 1). Deaths peaked in the winter months of December, January and February, and were lower in the summer months of June, July and August, varying by 30% or more between the highest and the lowest months (Figure 1). The overall rate ratio between winter and non-winter months was 1.61 (60% winter increase), and the average number of deaths per day was 442 in winter and 275 in summer. There was little evidence that the ratio varied by geographical region.

Table 1.
Summary statistics for total deaths (2010–2013), prevalence ratios and 95% CIs for winter deaths compared with deaths in other seasons a.
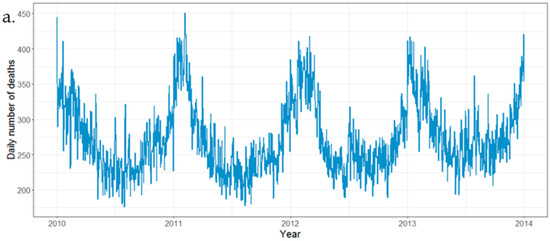
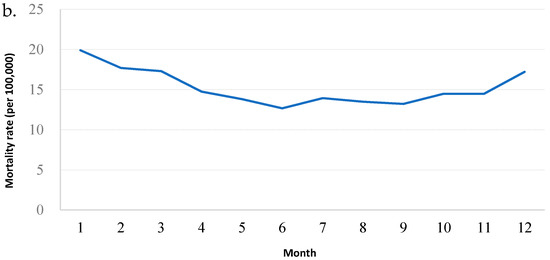
Figure 1.
Summary statistics for death data, 2010–2013. (a). Time series of daily deaths; (b). Mortality rate (per 100,000 persons), 2010–2013. This was calculated based on the Chinese census in 2010.
Almost 80% of the deaths occurred at home, and approximately 15% of deaths were among people admitted to a hospital (both hospital ward and emergency room). Most deaths were among Han nationality (99.9%) who had no education (57%) (Table 1). More than 80% of deaths occurred among people aged 60 or over, and the median/mean age of death was 72 years old (70 for males and 75 for females).
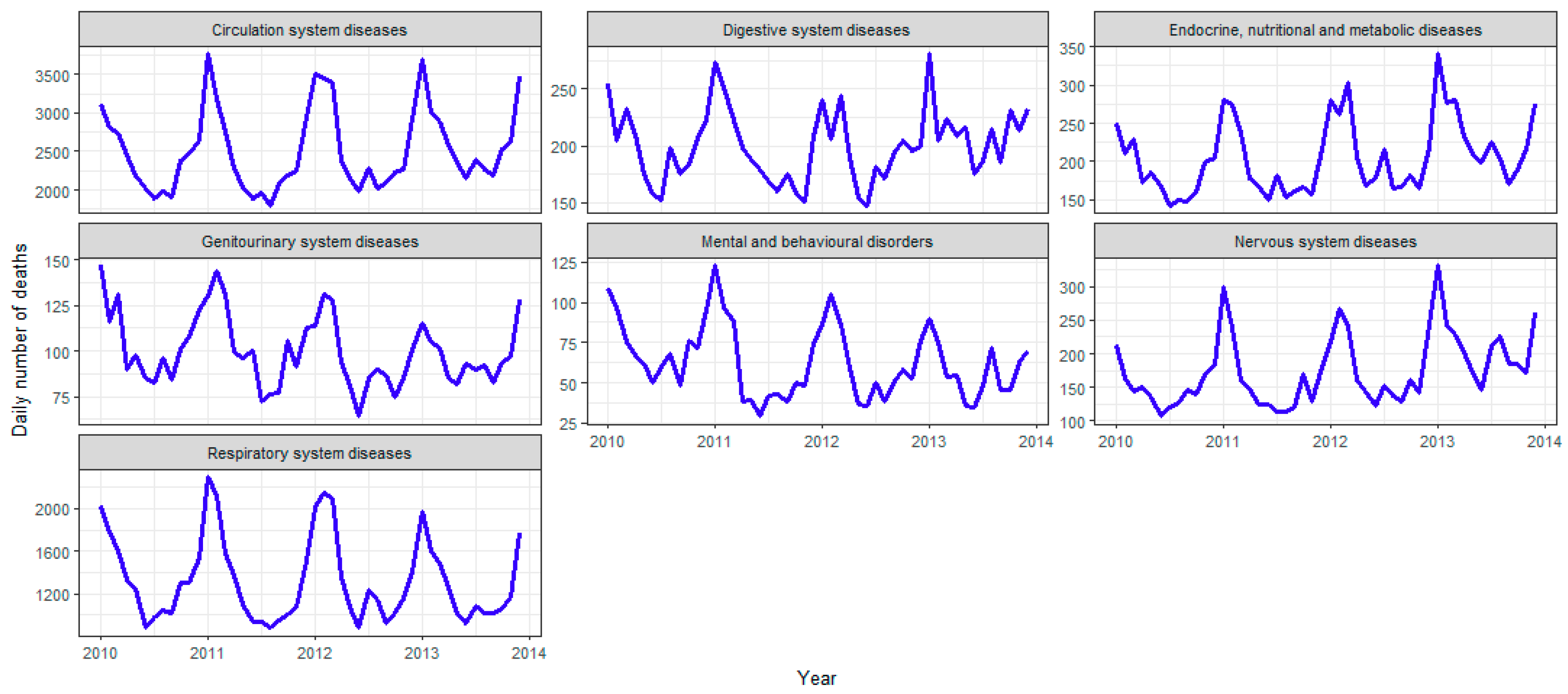
The leading underlying causes of death were circulatory diseases, neoplasms and respiratory diseases, which accounted for 75% of all deaths (Table 2). Many diseases appeared to have strong seasonal patterns with a winter peak, such as diseases of the circulatory system, respiratory system, nervous system, digestive system, genitourinary system, mental and behavioral disorders, and endocrine, nutritional and metabolic (Figure 2). Other causes, including external causes of morbidity and mortality, certain conditions originating in the perinatal period, diseases of the blood and blood-forming organs, did not display a clear seasonal pattern.

Table 2.
Causes of death by ICD chapter.
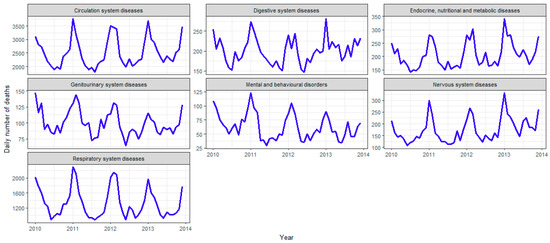
Figure 2.
Time series of daily deaths by specific causes of death with seasonal pattern.
We found that the seasonal effect differs greatly for various causes of death (Table 3), and many causes are highly seasonal, including mental and behavioral disorders, diseases of the respiratory and circulatory system. However, a noticeable exception is cancer (although a large number of deaths were attributable to neoplasms, there was only a 2.5% increase in winter), which is almost equally spread amongst all seasons after removing the increasing trend (Figure 2 and Table 3). The results show that the seasonality of deaths is not inevitable for all persons who happen to be ill during winter. Instead, the mechanisms for increased winter mortality are specific to particular causes of death.

Table 3.
Seasonal patterns in deaths by ICD chapter.
We compared winter deaths with deaths in other seasons using a case-only analysis. Based on a high VIF, we dropped marital status from the model. We found that males were slightly more susceptible during winter than females (Table 1). Those without education were also more likely to die in winter compared with other education groups. People who died in an emergency room, at home, on the way to hospital, in nursing home and family ward, were more likely to die in winter than those who died in a hospital ward. Deaths outside of the city were less likely in winter. Age was a strong predictor of winter death; young people were at a slightly increased risk, and the old were much more likely to die in winter with an increased risk above age 60.
4. Discussion
This study provides evidence for obvious seasonal mortality in Zhejiang Province, China, where deaths peaked in winter and overall mortality was around 30% higher in winter than summer. Deaths are predictable to some extent, in that they occur more often for particular causes such as cardiovascular and respiratory disease, mental and behavioral disorders. Individual characteristics such as age, gender, education are important predictors of seasonal mortality. Males, those older than 60 and those without education were more susceptible during winter. Also more common in winter were deaths in the emergency room, at home, on the way to hospital, in a nursing home and family ward.
The season of the year exerts an influence on total mortality, driven by a strong seasonal pattern in deaths due to circulatory and respiratory diseases. Mortality from respiratory disease was strongly influenced by season, with winter mortality estimates 35.9% higher than expected from non-winter seasons. As for the determinants of excess winter mortality from respiratory disease, cold weather is usually regarded as playing a dominant role. Other factors, such as influenza and other infections, are also involved in driving this kind of clear seasonal pattern [21].
Winter increases in circulatory disease mortality have been observed in other countries [19,22,23,24,25]. This was true in our study when deaths from circulatory disease had the largest absolute winter increase, as it comprised 30% of total mortality. Several explanations have been put forward, from misclassification of circulatory disease deaths [26] to changes in air temperature [27]. In addition, circulatory risk factors (e.g., waist circumference, blood pressure) showed a seasonal pattern characterized by higher levels in winter. This pattern could contribute to the seasonality of circulatory mortality [28], offering another potential explanation.
In our study, deaths attributable to mental and behavioral disorders had the strongest seasonal pattern (37.4% increase in winter), but this grouping contributed only 0.8% of total winter mortality. Previous studies on seasonality of bipolar disorder and depressive disorder showed a clear peak in the winter months [29,30,31]. A longitudinal study conducted in Ireland reported the highest levels of depressive symptoms in winter, and those who live in areas with longer daily hours of sunshine experienced lower occurrence rate of depressive symptoms [32]. In addition, the Kadotani et al. study revealed a higher rate of suicide attempts after a few days with lower levels of sunlight in Japan [33]. Similar associations were also found in Australia and in Austria [34,35]. However, studies in the Northern Hemisphere, including Ireland, England, and Scotland, have shown that the peak time of the first hospital entries for mental disorders occurs in summer [36,37]. It could be explained that most of them were conducted in developed populations where weather characteristics, socio-economic conditions, and culture differ from those in China. In addition, ambient temperature has long been suspected of being a cause of psychotic exacerbation in mental and behavioral disorders [38]. Hence, we speculate that low ambient temperature in winter may contribute to more frequent onset of mental and behavioral disorders exacerbation.
Analysis using ICD chapters may have limitations as these categories are broad and are not based strictly on etiology. For example, the Wilkinson et al. study [4] noted that respiratory disease seemed to be a strong determinant of cardiovascular but not respiratory death. A previous analysis of New Zealand deaths with infectious disease causes found that only 10% of those records were coded to the infectious disease chapter [39]. The specificity of association may have been obscured by misclassification of cause of death, but analyses of deaths with any mention of respiratory/infectious causes also did not show an association with pre-existing illness.
Healy argued that low socioeconomic status increased the risk of winter deaths in Europe [40]. Hales found that there was an increased risk of dying in winter for most New Zealanders, but more so among low-income people [7]. It also seems that in China, winter mortality is increased amongst people of lower socioeconomic status (e.g., illiteracy group, people died at home). There are some possible explanations, including poorer health status, scarce medical resources, and low indoor temperatures due to inadequate heating and household crowding. In a more recent study, education serving as a proxy for socioeconomic status has also been highlighted as a determinant for seasonal mortality patterns [40]. However, exact causal mechanisms are not known. Hence, further work is needed to disentangle the complex relationships between different indicators of housing quality and other measures of socioeconomic deprivation, and then to clarify their effects on seasonal mortality.
Previous studies have shown that females are more vulnerable than males to winter mortality. In the UK, women had a larger risk than men for reasons other than their greater age, health status, social isolation, or socioeconomic position [4]. In New Zealand, the risk for females was 9% higher than for males after adjusting for all major covariates [39]. The existing evidence seems to indicate that the lower capability of producing maximum heat vasoconstriction puts females at greater risk during cold spells [41,42,43]. Whereas there is an inverse result in China, although only a slight difference exists between genders. The higher risk of dying in winter among Chinese men does not seem to be due to clinic or socioeconomic differences, but we know that smoking rate in China is much higher for men than for women. Although it is not fully explained, this may imply that smoking could be an important lifestyle risk factor for higher winter mortality.
One hypothesis to explain these seasonal variations in mortality is that they simply represent shifts in the timing of events that lead to death. The effect of season could be seen as a kind of “harvesting (sometimes known as mortality displacement)” of vulnerable members of the population, such as elderly people. This view might be supported by the age gradients and causes of death, which demonstrate the greatest seasonal variation. A study in France showed a clear seasonal pattern both in pulmonary embolism (PE) incidence and mortality. In addition, the study supported an association of age on the PE seasonal variations [44]. However, it would require a detailed prospective study involving information about the pre-existing illness of those dying in different seasons to investigate this hypothesis further [6].
Previous studies have shown that excess winter deaths are higher in out-of-hospital mortality than in-hospital deaths [14,45]. As hospitals are well-equipped with heating equipment, people who lived in hospitals are less likely to be exposed to low ambient temperature conditions. That is a possible explanation for the lower winter increase in in-hospital mortality than out-of-hospital mortality. Our study also confirmed this; people are more likely to die during winter when they are at home, on the way to hospital, emergency home, family ward or nursing home than in hospital.
Other explanations for the observed seasonal patterns of mortality are due to particular characteristics of the environment, such as extremes of temperature and humidity, different exposure to either indoor or outdoor air pollution, changing patterns in the frequency of seasonally-variable infectious agents, and season-related changes in lifestyle (e.g., diet, physical activity). Specifically, cold weather has been reported to be associated with increased risk of death from cardiovascular and respiratory diseases [46,47,48].
Indoor air quality may be worse in winter due to the use of polluting indoor heaters. As a study in France showed, the nitrogen dioxide concentration in indoor air particularly increased only during winter and was well correlated with the formic acid concentration [49]. In addition, inadequate and poorly designed ventilation in crowded places may boost exposure to air-borne pathogens by increasing their concentration in stagnant air and by re-circulating contaminated air. Furthermore, low ventilation rates were associated with increased behavior problems and health symptoms [50].
Although much of the winter excess seems to be related to cold, some countries have a larger seasonal fluctuation in mortality than others despite having milder winters [51]. Different from cold-related mortality, excess winter deaths reflect excess mortality during winter when compared with other seasons, and are influenced by low temperature, individual characteristics and potential diseases. Thus, concentrating solely on cold-driven deaths is far from reducing the high death rate during the winter season. Heating measures and adjusting indoor temperature should go along with identifying and protecting populations who are vulnerable to winter season. Hence, understanding the significance of EWD has a fundamental public health importance.
Exploring the effects modification by meteorological variables (e.g., temperature, humidity) or confounders with other seasonal exposures (e.g., air pollution, influenza) on EWD was beyond the scope of this research. Further research should explore more detailed or broader range of pathways, so that more targeted interventions can be achieved. For example, if EWD were associated with low indoor temperatures, campaigns to reduce winter mortality need to enhance protection against outdoor as well as indoor chill. If there exists a link between winter death peaks and influenza epidemics, then greater emphasis might be placed on more comprehensive influenza vaccination programme. Future research could also explore other seasonal exposures that may have potential to simulate EWD, such as air pollution, behavior patterns and household crowding [39].
This research has provided rare evidence on individual characteristics of risk for winter deaths in China. Since winter increases are predictable for specific causes of disease and vulnerable population groups, public health measures might play a part. The fact that the risk of dying in winter is far greater in the elderly suggests that additional measures are needed to reach all those at risk.
5. Conclusions
Increased winter mortality is an important public health problem in China. Investigating seasonal patterns of death can help explain changes in the health of a population, and provide insight into risk factors that contribute to the burden of higher winter mortality. Death data are particularly useful for understanding the health of the overall population, investigating differences in the patterns between population groups, and informing health policy, planning, investment and administration of the health care system.
Author Contributions
C.H. and A.G.B. conceived the study. C.H., A.G.B. and Y.H. conducted the study, performed the statistical analysis and drafted the manuscript. X.Z. assisted with data acquisition. M.R., J.B. and S.H. provided substantial scientific input in the interpretation of the results and contributed to the revision of the manuscript. All authors read and approved the final manuscript.
Acknowledgments
This work was supported by grants from National Key R&D Program of China (2018YFA0606201), the Asia-Pacific Network for Global Change (CRRP2016-10MYSG02-Huang), the Natural Science Foundation of Guangdong Province (2016A030313216).
Conflicts of Interest
The authors declare no conflict of interest.
References
- Huang, C.; Barnett, A. Human Impacts Winter Weather and Health. Nat. Clim. Chang. 2014, 4, 173–174. [Google Scholar] [CrossRef]
- Department of Health Regional Public Health Group in the South East. Health and Winter Warmth: Reducing Health Inequalities. In Regional Public Health Group Fact Sheet; London DH: London, UK, 2009. [Google Scholar]
- Hajat, S.; Gasparrini, A. The Excess Winter Deaths Measure: Why Its Use Is Misleading for Public Health Understanding of Cold-related Health Impacts. Epidemiology 2016, 27, 486–491. [Google Scholar] [CrossRef] [PubMed]
- Wilkinson, P.; Pattenden, S.; Armstrong, B.; Fletcher, A.; Kovats, R.S.; Mangtani, P.; McMichael, A.J. Vulnerability to winter mortality in elderly people in Britain: Population based study. BMJ 2004, 329, 647. [Google Scholar] [CrossRef] [PubMed]
- Barnett, A.G.; de Looper, M.; Fraser, J.F. The seasonality in heart failure deaths and total cardiovascular deaths. Aust. N. Z. J. Public Health 2008, 32, 408–413. [Google Scholar] [CrossRef] [PubMed]
- Gemmell, I.; McLoone, P.; Boddy, F.A.; Dickinson, G.J.; Watt, G.C.M. Seasonal variation in mortality in Scotland. Int. J. Epidemiol. 2000, 29, 274–279. [Google Scholar] [CrossRef] [PubMed]
- Hales, S.; Blakely, T.; Foster, R.H.; Baker, M.G.; Howden-Chapman, P. Seasonal patterns of mortality in relation to social factors. J. Epidemiol. Commun. Health 2012, 66, 379–384. [Google Scholar] [CrossRef] [PubMed]
- Kalkstein, A.J. Regional similarities in seasonal mortality across the United States: An examination of 28 metropolitan statistical areas. PLoS ONE 2013, 8, e63971. [Google Scholar] [CrossRef] [PubMed]
- Nakaji, S.; Parodi, S.; Fontana, V.; Umeda, T.; Suzuki, K.; Sakamoto, J.; Fukuda, S.; Wada, S.; Sugawara, K. Seasonal changes in mortality rates from main causes of death in Japan (1970–1999). Eur. J. Epidemiol. 2004, 19, 905–913. [Google Scholar] [CrossRef] [PubMed]
- Fowler, T.; Waite, R.J.T.; Harrell, R.; Kovats, S.; Bone, A.; Doyle, Y.; Murray, V. Excess winter deaths in Europe: A multi-country descriptive analysis. Eur. J. Public Health 2015, 25, 339–345. [Google Scholar] [CrossRef] [PubMed]
- Moore, S.E. Commentary: Patterns in mortality governed by the seasons. Int. J. Epidemiol. 2006, 35, 435–437. [Google Scholar] [CrossRef] [PubMed]
- Kynast-Wolf, G.; Hammer, G.P.; Muller, O.; Kouyate, B.; Becher, H. Season of death and birth predict patterns of mortality in Burkina Faso. Int. J. Epidemiol. 2006, 35, 427–435. [Google Scholar] [CrossRef] [PubMed]
- Ban, J.; Xu, D.; He, M.Z.; Sun, Q.; Chen, C.; Wang, W.; Zhu, P.; Li, T. The effect of high temperature on cause-specific mortality: A multi-county analysis in China. Environ. Int. 2017, 106, 19–26. [Google Scholar] [CrossRef] [PubMed]
- Ou, C.Q.; Song, Y.F.; Yang, J.; Chau, P.Y.; Yang, L.; Chen, P.Y.; Wong, C.M. Excess winter mortality and cold temperatures in a subtropical city, Guangzhou, China. PLoS ONE 2013, 8, e77150. [Google Scholar] [CrossRef] [PubMed]
- Aylin, P.; Morris, S.; Wakefield, J.; Grossinho, A.; Jarup, L.; Elliott, P. Temperature, housing, deprivation and their relationship to excess winter mortality in Great Britain, 1986–1996. Int. J. Epidemiol. 2001, 30, 1100–1108. [Google Scholar] [CrossRef] [PubMed]
- Stacey, D.; Pritchard, C. An ecological study of excess winter mortality in England and deprivation. Public Health 2016, 141, 207–209. [Google Scholar] [CrossRef] [PubMed]
- Barnett, A.G.; Dobson, A.J. Analysing Seasonal Health Data; Springer: Berlin, Germany, 2010. [Google Scholar]
- Deddens, J.A.; Petersen, M.R. Approaches for estimating prevalence ratios. Occup. Environ. Med. 2008, 65, 501–506. [Google Scholar] [CrossRef] [PubMed]
- Gouveia, N.; Hajat, S.; Armstrong, B. Socioeconomic differentials in the temperature-mortality relationship in Sao Paulo, Brazil. Int. J. Epidemiol. 2003, 32, 390–397. [Google Scholar] [CrossRef] [PubMed]
- Medina-Ramon, M.; Zanobetti, A.; Cavanagh, D.P.; Schwartz, J. Extreme temperatures and mortality: Assessing effect modification by personal characteristics and specific cause of death in a multi-city case-only analysis. Environ. Health Perspect. 2006, 114, 1331–1336. [Google Scholar] [CrossRef] [PubMed]
- Von Klot, S.; Zanobetti, A.; Schwartz, J. Influenza epidemics, seasonality, and the effects of cold weather on cardiac mortality. Environ. Health 2012, 11, 74. [Google Scholar] [CrossRef] [PubMed]
- Revich, B.; Shaposhnikov, D. Temperature-induced excess mortality in Moscow, Russia. Int. J. Biometeorol. 2008, 52, 367–374. [Google Scholar]
- Rocklov, J.; Ebi, K.; Forsberg, B. Mortality related to temperature and persistent extreme temperatures: A study of cause-specific and age-stratified mortality. Occup. Environ. Med. 2011, 68, 531–536. [Google Scholar] [CrossRef] [PubMed]
- Rocklov, J.; Forsberg, B.; Meister, K. Winter mortality modifies the heat-mortality association the following summer. Eur. Respir. J. 2009, 33, 245–251. [Google Scholar] [CrossRef] [PubMed]
- Yu, W.; Hu, W.; Mengersen, K.; Guo, Y.; Pan, X.; Connell, D.; Tong, S. Time course of temperature effects on cardiovascular mortality in Brisbane, Australia. Heart 2011, 97, 1089–1093. [Google Scholar] [CrossRef] [PubMed]
- Wexelman, B.A.; Eden, E.; Rose, K.M. Survey of New York City resident physicians on cause-of-death reporting, 2010. Prev. Chronic Dis. 2013, 10, E76. [Google Scholar] [CrossRef] [PubMed]
- Ballester, F.C.D.; Pérez-Hoyos, S.; Sáez, M.; Hervás, A. Mortality as a function of temperature. A study in Valencia, Spain, 1991–1993. Int. J. Epidemiol. 1997, 26, 551–561. [Google Scholar] [CrossRef] [PubMed]
- Marti-Soler, H.; Gubelmann, C.; Aeschbacher, S.; Alves, L.; Bobak, M.; Bongard, V.; Clays, E.; de Gaetano, G.; Di Castelnuovo, A.; Elosua, R.; et al. Seasonality of cardiovascular risk factors: An analysis including over 230,000 participants in 15 countries. Heart 2014, 100, 1517–1523. [Google Scholar] [CrossRef] [PubMed]
- Lee, H.C.; Tsai, S.Y.; Lin, H.-C. Seasonal variations in bipolar disorder admissions and the association with climate: A population-based study. J. Affect. Disord. 2007, 97, 61–69. [Google Scholar] [CrossRef] [PubMed]
- Morken, G.; Lilleeng, S.; Linaker, O.M. Seasonal variation in suicides and in admissions to hospital for mania and depression. J. Aff. Dis. 2002, 69, 39–45. [Google Scholar] [CrossRef]
- Licanin, I.; Fisekovic, S.; Babic, S. Admission rate of patients with most common psychiatric disorders in relation to seasons and climatic factors during 2010/2011. Mater. Socio-Med. 2012, 24, 94–99. [Google Scholar] [CrossRef] [PubMed]
- O’Hare, C.; O’Sullivan, V.; Flood, S.; Kenny, R.A. Seasonal and meteorological associations with depressive symptoms in older adults: A geo-epidemiological study. J. Affect. Disord. 2016, 191, 172–179. [Google Scholar] [CrossRef] [PubMed]
- Kadotani, H.; Nagai, Y.; Sozu, T. Railway suicide attempts are associated with amount of sunlight in recent days. J. Affect. Disord. 2014, 152–154, 162–168. [Google Scholar] [CrossRef] [PubMed]
- Vyssoki, B.; Kapusta, N.D.; Praschak-Rieder, N.; Dorffner, G.; Willeit, M. Direct effect of sunshine on suicide. JAMA Psychiatry 2014, 71, 1231–1237. [Google Scholar] [CrossRef] [PubMed]
- Lambert, G.; Reid, C.; Kaye, D.; Jennings, G.; Esler, M. Increased suicide rate in the middle-aged and its association with hours of sunlight. Am. J. Psychiatry 2003, 160, 793–795. [Google Scholar] [CrossRef] [PubMed]
- Amr, M.; Volpe, F.M. Seasonal influences on admissions for mood disorders and schizophrenia in a teaching psychiatric hospital in Egypt. J. Affect. Disord. 2012, 137, 56–60. [Google Scholar] [CrossRef] [PubMed]
- Shiloh, R.; Weizman, A.; Stryjer, R.; Kahan, N.; Waitman, D.A. Altered thermoregulation in ambulatory schizophrenia patients: A naturalistic study. World J. Biol. Psychiatry 2009, 10, 163–170. [Google Scholar] [CrossRef] [PubMed]
- McMichael, A.J.; Woodruff, R.E.; Hales, S. Climate change and human health: Present and future risks. Lancet 2006, 367, 859–869. [Google Scholar] [CrossRef]
- Davie, G.S.; Baker, M.G.; Hales, S.; Carlin, J.B. Trends and determinants of excess winter mortality in New Zealand: 1980 to 2000. BMC Public Health 2007, 7, 263. [Google Scholar] [CrossRef] [PubMed]
- Roland, R. Seasonality in Human Mortality. In A Demographic Approach; Springer: Berlin, Germany, 2006. [Google Scholar]
- Astrand, I. Aerobic work capacity in men and women with special reference to age. Acta Phys. Scand Suppl. 1960, 49, 1–92. [Google Scholar]
- Burse, R.L. Sex differences in human thermoregulatory response to heat and cold stress. Hum. Factors 1979, 21, 687–699. [Google Scholar] [CrossRef] [PubMed]
- Elsworth, R.; Buskirk, R.H.T.; Whedon, G.D. Metabolic responses to cold air in men and women in relation to total body fat content. J. Appl. Physiol. 1963, 18, 603–612. [Google Scholar]
- Olié V, B.C. Pulmonary embolism: Does the seasonal effect depend on age? A 12-year nationwide analysis of hospitalization and mortality. Thromb. Res. 2016, 150, 96–100. [Google Scholar] [CrossRef] [PubMed]
- O’Neill, M.S.; Zanobetti, A.; Schwartz, J. Modifiers of the temperature and mortality association in seven US cities. Am. J. Epidemiol. 2003, 157, 1074–1082. [Google Scholar] [CrossRef] [PubMed]
- Analitis, A.; Katsouyanni, K.; Biggeri, A.; Baccini, M.; Forsberg, B.; Bisanti, L.; Kirchmayer, U.; Ballester, F.; Cadum, E.; Goodman, P.G.; et al. Effects of cold weather on mortality: Results from 15 European cities within the PHEWE project. Am. J. Epidemiol. 2008, 168, 1397–1408. [Google Scholar] [CrossRef] [PubMed]
- Olson, A.L.; Swigris, J.J.; Raghu, G.; Brown, K.K. Seasonal variation: Mortality from pulmonary fibrosis is greatest in the winter. Chest 2009, 136, 16–22. [Google Scholar] [CrossRef] [PubMed]
- Stewart, S.; McIntyre, K.; Capewell, S.; McMurray, J.J. Heart failure in a cold climate: Seasonal variation in heart failure-related morbidity and mortality. J. Am. Coll. Cardiol. 2002, 39, 760–766. [Google Scholar] [CrossRef]
- Uchiyama, S.; Tomizawa, T.; Tokoro, A.; Aoki, M.; Hishiki, M.; Yamada, T.; Tanaka, R.; Sakamoto, H.; Yoshida, T.; Bekki, K.; et al. Gaseous chemical compounds in indoor and outdoor air of 602 houses throughout Japan in winter and summer. Environ. Res. 2015, 137, 364–372. [Google Scholar] [CrossRef] [PubMed]
- Sundell, J.; Levin, H.; Nazaroff, W.W.; Cain, W.S.; Fisk, W.J.; Grimsrud, D.T.; Gyntelberg, F.; Li, Y.; Persily, A.K.; Pickering, A.C.; et al. Ventilation rates and health: Multidisciplinary review of the scientific literature. Indoor Air 2011, 21, 191–204. [Google Scholar] [CrossRef] [PubMed]
- Healy, J.D. Excess winter mortality in Europe: A cross country analysis identifying key risk factors. J. Epidemiol. Commun. Health 2003, 57, 784–789. [Google Scholar] [CrossRef]
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).