The Effect of an Automated Phone Warning and Health Advisory System on Adaptation to High Heat Episodes and Health Services Use in Vulnerable Groups—Evidence from a Randomized Controlled Study
Abstract
1. Introduction
2. Material and Method
2.1. Description of the Intervention
2.2. Methodology
2.2.1. Outcome Measurement Variables
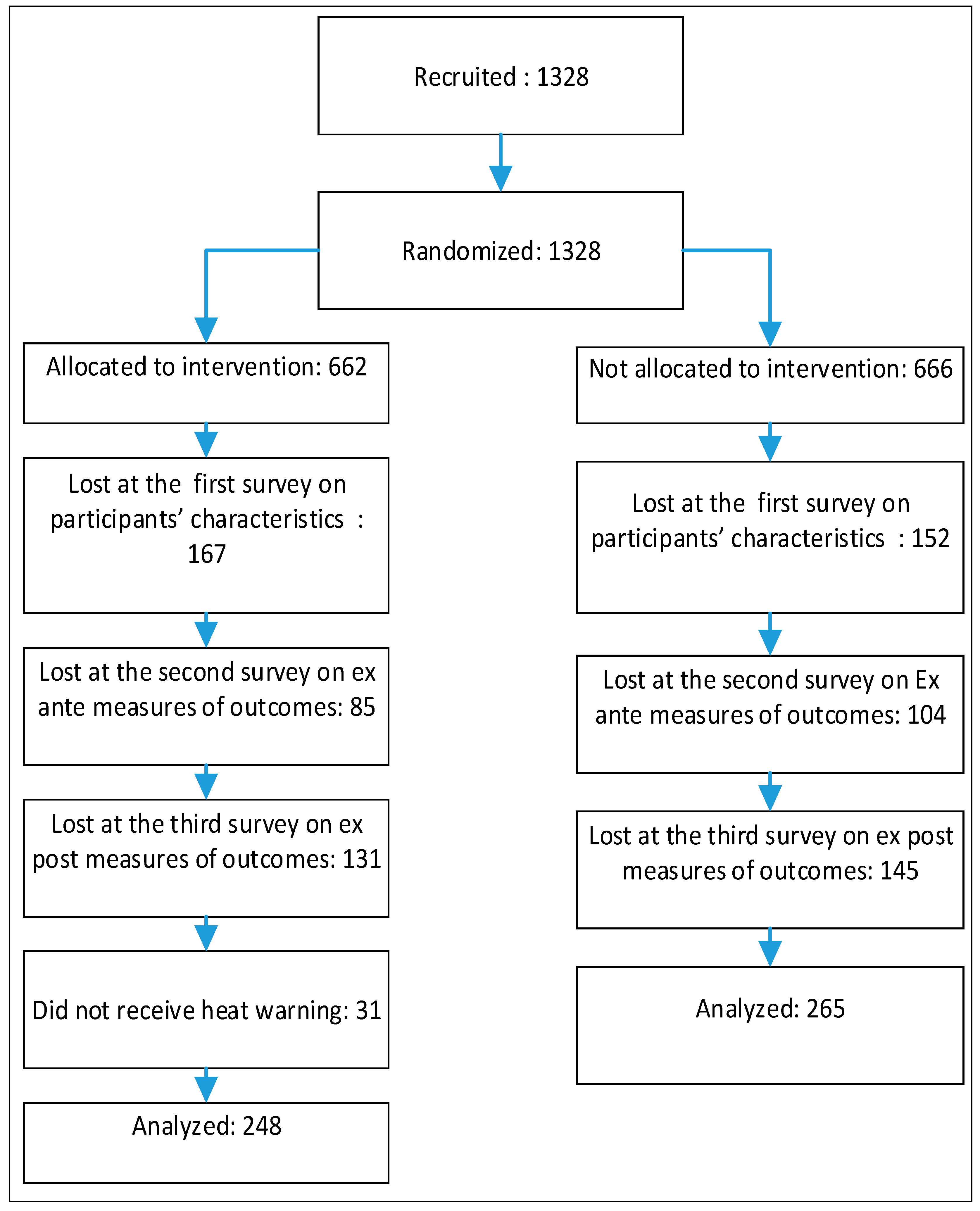
2.2.2. Recruiting Participants and Assigning Groups
2.2.3. Data Collection
2.2.4. Data Analysis
3. Results
3.1. Sample Characteristics
3.2. The Quality of the Heat Episode Warning
3.3. Baseline Differences
3.4. Effects of Automated Phone Warnings
3.4.1. Effects on Awareness of Heat Episode and Heat Protective Behaviours
3.4.2. Effects on the Adoption of Recommended Protective Behaviours
3.4.3. Health Outcomes
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Mehl, A.; Tobaldi, C. More intense, more frequent, and longer lasting heat waves in the 21st century. Science 2004, 305, 994–997. [Google Scholar] [CrossRef] [PubMed]
- Bélanger, D.; Gosselin, P.; Valois, P.; Abdous, B. Perceived adverse health effects of heat and their determinants in deprived neighbourhoods: A cross-sectional survey of nine cities in Canada. Int. J. Environ. Res. Public Health 2014, 11, 11028–11053. [Google Scholar]
- Bobb, J.F.; Peng, R.D.; Bell, M.; Dominici, F. Heat-related mortality and adaptation to heat in the United States. Environ. Health Perspect. 2014, 122, 811–816. [Google Scholar] [CrossRef] [PubMed]
- Bustinza, R.; Lebel, G.; Gosselin, P.; Bélanger, D.; Chebana, F. Health impacts of the July 2010 heat wave in Québec, Canada. BMC Public Health 2014, 21, 13–56. [Google Scholar] [CrossRef] [PubMed]
- McGeehin, M.A.; Mirabelli, M. The potential impacts of climate variability and change on temperature-related morbidity and mortality in the United States. Environ. Health Perspect. 2001, 109, 185–189. [Google Scholar] [CrossRef] [PubMed]
- O’Neill, M.S.; Ebi, K.L. Temperature extremes and health: Impacts of climate variability and change in the United States. J. Occup. Environ. Med. 2009, 51, 13–25. [Google Scholar] [CrossRef] [PubMed]
- Hajat, S.; Kovats, R.S.; Lachowycz, K. Heat-related and cold-related deaths in England and Wales: Who is at risk? Occup. Environ. Med. 2007, 64, 93–100. [Google Scholar] [CrossRef] [PubMed]
- Bélanger, D.; Gosselin, P.; Valois, P.; Abdous, B. Neighbourhood and dwelling characteristics associated with the self-reported adverse health effects of heat in most deprived urban areas: A cross-sectional study in 9 cities. Health Place 2015, 32, 8–18. [Google Scholar] [CrossRef] [PubMed]
- Hatvani-Kovacs, G.; Belusko, M.; Skinner, N.; Pockett, J.; Boland, J. Heat stress risk and resilience in the urban environment. Sustain. Cities Soc. 2016, 26, 278–288. [Google Scholar] [CrossRef]
- Zuo, J.; Pullen, S.; Palmer, J.; Bennetts, H.; Chileshe, N.; Ma, T. Impacts of heat waves and corresponding measures: A review. J. Clean. Prod. 2015, 92, 1–12. [Google Scholar] [CrossRef]
- Basher, R. Global early warning systems for natural hazards: Systematic and people-centred. Philos. Trans. R. Soc. A 2006, 364, 2167–2182. [Google Scholar] [CrossRef] [PubMed]
- Hajat, S.; O’Connor, M.; Kosatsky, T. Health effects of hot weather: From awareness of risk factors to effective health protection. Lancet 2010, 375, 856–863. [Google Scholar] [CrossRef]
- United Nations. Report on Early Warning for Hydrometeorological Hazards Including Drought; IDNDR Secretariat: Geneva, Switzerland, 1997. [Google Scholar]
- Xu, Z.; FitzGerald, G.; Guo, Y.; Jalaludin, B.; Tong, S. Impact of heatwave on mortality under different heatwave definitions: A systematic review and meta-analysis. Environ. Int. 2016, 89, 193–203. [Google Scholar] [CrossRef] [PubMed]
- Basu, R.; Samet, J.M. Relation between elevated ambient temperature and mortality: A review of the epidemiologic evidence. Epidemiol. Rev. 2002, 24, 190–202. [Google Scholar] [CrossRef] [PubMed]
- Kovats, R.S.; Hajat, S. Heat stress and public health: A critical review. Ann. Rev. Public Health 2008, 29, 41–55. [Google Scholar] [CrossRef] [PubMed]
- Kenny, G.P.; Yardley, J.C.; Brown, R.J.; Sigal, J.O. Heat stress in older individuals and patients with common chronic diseases. Can. Med. Assoc. J. 2010, 182, 1053–1060. [Google Scholar] [CrossRef] [PubMed]
- Smargiassi, A.; Goldberg, M.; Plante, C.; Fournier, M.; Baudouin, Y.; Kosatsky, T. Variation of daily warm season mortality as a function of micro-urban heat islands. J. Epidemiol. Community Health 2009, 63, 659–664. [Google Scholar] [CrossRef] [PubMed]
- Boeckmann, M.; Rohn, I. Is planned adaptation to heat reducing heat-related mortality and illness? A systematic review. BMC Public Health 2014, 14, 1112–1125. [Google Scholar] [CrossRef] [PubMed]
- Kalkstein, A.J.; Sheridan, S.C. The social impacts of the heat-health watch/warning system in Phoenix, Arizona: Assessing the perceived risk and response of the public. Int. J. Biometeorol. 2007, 52, 43–55. [Google Scholar] [CrossRef] [PubMed]
- Mackie, B. Warning Fatigue: Insights from the Australian Bushfire Context. Ph.D. Thesis, University of Canterbyry, Christchurch, New Zealand, 2013. [Google Scholar]
- Das, S. Awareness as an adaption strategy for reducing mortality from heat waves: Evidence from a disaster risk management program in India. Clim. Chang. Econ. 2012, 3, 1250010. [Google Scholar] [CrossRef]
- Sheridan, S.C. A survey of public perception and response to heat warnings across four North American cities: An evaluation of municipal effectiveness. Int. J. Biometeorol. 2007, 52, 3–15. [Google Scholar] [CrossRef] [PubMed]
- Takahashi, N.; Nakao, R.; Ueda, K.; Ono, M.; Kondo, M.; Honda, Y.; Hashizume, M. Community trial on heat related-illness prevention behaviors and knowledge for the elderly. Int. J. Environ. Res. Public Health 2015, 12, 3188–3214. [Google Scholar] [CrossRef] [PubMed]
- Chau, P.H.; Chan, K.C.; Woo, J. Hot weather warning might help to reduce elderly mortality in Hong Kong. Int. J. Biometeorol. 2009, 53, 461–468. [Google Scholar] [CrossRef] [PubMed]
- Ebi, K.L.; Teisberg, T.J.; Kalkstein, L.S.; Robinson, L.; Weiher, R.F. Heat watch/warning systems save lives: Estimated costs and benefits for Philadelphia 1995-98. Bull. Am. Meteorol. Soc. 2004, 85, 1067–1074. [Google Scholar] [CrossRef]
- Kalkstein, L.; Greene, S.; Mills, D.; Samenow, J. An evaluation of the progress in reducing heat-related human mortality in major U.S. cities. Nat. Hazards 2011, 56, 113–129. [Google Scholar] [CrossRef]
- Nitschke, M.; Tucker, G.; Hansen, A.; Williams, S.; Zhang, Y.; Bi, P. Evaluation of a heat warning system in Adelaide, South Australia, using case-series analysis. BMJ Open 2016, 6, e012125. [Google Scholar] [CrossRef] [PubMed]
- Toloo, G.; FitzGerald, G.; Aitken, P.; Verral, K.; Tong, S. Evaluating the effectiveness of heat warning systems: Systematic review of epidemiological evidence. Int. J. Public Health 2013, 58, 667–681. [Google Scholar] [CrossRef] [PubMed]
- Goldberg, M.; Gasparrini, A.; Armstrong, B.; Valois, M. The short-term influence of temperature on daily mortality in the temperate climate of Montreal, Canada. Environ. Res. 2011, 111, 853–860. [Google Scholar] [CrossRef] [PubMed]
- United Nations. Developing early warning system: A check list. In Proceedings of the Third International Conference on Early Warning System, Bonn, Germany, 27–29 March 2006. [Google Scholar]
- Kim, M.; Kim, H.; You, M. The role of public awareness in health-protective behaviours to reduce heat wave risk. Meteorol. Appl. 2014, 21, 867–872. [Google Scholar] [CrossRef]
- Knowlton, K.; Rotkin-Ellman, M.; King, G.; Margolis, H.G.; Smith, D.; Solomon, G.; Trent, R.; English, P. The 2006 California heat wave: Impacts on hospitalizations and emergency department visits. Environ. Health Perspect. 2009, 117, 61–67. [Google Scholar] [CrossRef] [PubMed]
- Kovats, R.S.; Kristie, L.E. Heatwaves and public health in Europe. Eur. J. Public Health 2006, 16, 592–599. [Google Scholar] [CrossRef] [PubMed]
- Mastrangelo, G.; Fedeli, U.; Visentin, C.; Milan, G.; Fadda, E.; Spolaore, P. Pattern and determinants of hospitalization during heat waves: An ecologic study. BMC Public Health 2007, 7, 200. [Google Scholar] [CrossRef] [PubMed]
- Abadie, A. Semiparametric difference-in-difference estimators. Rev. Econ. Stud. 2005, 72, 1–19. [Google Scholar] [CrossRef]
- Mehiriz, K. The impacts of intergovernmental grants on municipal infrastructure: Evidence from the Canada-Quebec Infrastructure Works 2000 program. Eval. Program Plan. 2017, 58, 184–193. [Google Scholar] [CrossRef] [PubMed]
- Ravallion, M. Evaluating anti-poverty programs. In Handbook of Development Economics; Schultz, P., Strauss, J., Eds.; Elsevier: Amsterdam, The Netherlands, 2008; pp. 3788–3846. [Google Scholar]
- Mehiriz, K.; Gosselin, P. Municipalities’ preparedness for weather hazards and response to weather warnings. PLoS ONE 2016, 11, e0163390. [Google Scholar] [CrossRef] [PubMed]
- Aström, D.; Forsberg, D.; Rocklöv, J. Heat wave impact on morbidity and mortality in the elderly population. A review of recent studies. Maturitas 2011, 69, 99–105. [Google Scholar] [CrossRef] [PubMed]
- Bélanger, D.; Abdous, A.; Valois, P.; Gosselin, P.; Laouan, S. A multilevel analysis to explain self-reported adverse health effects and adaptation to urban heat: A cross-sectional survey in the deprived areas of 9 Canadian cities. BMC Public Health 2016, 16, 144. [Google Scholar] [CrossRef] [PubMed]
- Charkoudian, N. Skin blood flow in adult human thermoregulation: How it works, when it does not, and why. Mayo Clin. Proc. 2003, 78, 603–612. [Google Scholar] [CrossRef] [PubMed]
- Gagnon, D.; Kenny, G.P. Does sex have an independent effect on thermoeffector responses during exercise in the heat? J. Physiol. 2012, 590, 5963–5973. [Google Scholar] [CrossRef] [PubMed]
- Kennedy, B.K.; Berger, S.L.; Brunt, A.; Champisi, J.; Cuervo, A.M.; Epel, E.S.; Franceschi, C.; Lithgow, G.J.; Morimoto, R.I.; Pessin, J.E.; et al. Geroscience: Linking aging to chronic disease. Cell 2014, 159, 709–713. [Google Scholar] [CrossRef] [PubMed]
- McGregor, G.R.; Bessemoulin, P.; Ebi, K.L.; Menne, B. Heatwaves and Health: Guidance on Warning-System Development; World Meteorological Organization: Geneva, Switzerland, 2015; ISBN 978-92-63-11142-5. [Google Scholar]
- Alberini, A.; Gans, W.; Alhassan, M. Individual and public program adaptation: Coping with heat waves in five cities in Canada. Int. J. Environ. Res. Public Health 2011, 8, 4679–4701. [Google Scholar] [CrossRef] [PubMed]
- Khandker, S.; Koolwal, G.; Samad, H. Handbook on Impact Evaluation: Quantitative Methods and Practices; The World Bank: Washington, DC, USA, 2009. [Google Scholar]
| Variable | Treatment | Control | p Value | ||
|---|---|---|---|---|---|
| N | % | N | % | ||
| Cardiovascular disease | 492 | 51.0 | 508 | 52.9 | 0.54 |
| Bronchial or lung disease | 491 | 22.6 | 507 | 22.5 | 0.96 |
| Diabetes | 489 | 19.4 | 509 | 20.0 | 0.81 |
| Kidney failure | 488 | 4.9 | 509 | 4.9 | 1.00 |
| Neurological diseases | 487 | 7.8 | 510 | 7.3 | 0.84 |
| 65 years or over | 495 | 87.1 | 511 | 86.3 | 0.87 |
| Women | 479 | 74.5 | 500 | 75.8 | 0.65 |
| Elementary school diploma | 487 | 15.6 | 502 | 12.2 | 0.12 |
| Secondary school diploma | 487 | 32.9 | 502 | 34.1 | 0.69 |
| College diploma | 487 | 20.9 | 502 | 19.7 | 0.63 |
| University degree | 487 | 30.6 | 502 | 34.1 | 0.24 |
| Household income (Thousands $): Less than 25 Between 25 and 50 Between 51 and 75 More than 75 | 395 | 38.1 | 394 | 31.1 | 0.04 |
| 395 | 33.3 | 394 | 36.2 | 0.38 | |
| 395 | 17.5 | 394 | 18.5 | 0.72 | |
| 395 | 11.2 | 394 | 14.2 | 0.20 | |
| 1 | 2 | 3 | 4 | 5 | |
|---|---|---|---|---|---|
| Reliability of the heat warning (1: very reliable, 4: very unreliable) | 78.3% | 21.7% | 0% | 0% | NA |
| Usefulness of the heat warning (1: totally useful, 5: totally useless) | 66.6% | 28.5% | 2.7% | 0.5% | 1.6% |
| Ease of understanding the heat warning message (1: very easy, 5: very difficult) | 75.2% | 20.2% | 1.6% | 0.8% | 2.2% |
| Level of satisfaction of the heat warning (1: very satisfied, 5: very dissatisfied) | 70.6% | 25.13% | 2.4% | 1.1% | 0.8% |
| Outcomes | Treatment Group | Control Group | p Value | ||
|---|---|---|---|---|---|
| N | Mean or % | N | Mean or % | ||
| Were informed of the heat episode | 247 | 96.3% | 262 | 95.4% | 0.60 |
| Were informed of the heat episode before its onset | 216 | 59.3% | 225 | 56.4% | 0.55 |
| Average number of recommended heat protection measures cited (a t-test was used) | 247 | 2.2 | 265 | 2.2 | 1.00 |
| Frequency of drinking water | 245 | 4.08 | 260 | 4.01 | 0.27 |
| Frequency of physical effort | 238 | 3.93 | 259 | 3.91 | 0.87 |
| Took cool showers or baths | 245 | 75.6% | 260 | 69.6% | 0.20 |
| Frequency of taking cool showers or baths more than usual | 181 | 3.52 | 180 | 3.49 | 0.47 |
| Visited cool or air-conditioned places | 246 | 45.5% | 259 | 38.6% | 0.12 |
| Went outside during heat episode | 242 | 69.8% | 258 | 72.4% | 0.51 |
| Frequency of spending time in cool or air-conditioned places | 110 | 3.25 | 100 | 3.18 | 0.29 |
| Frequency of staying in the shade | 160 | 3.83 | 179 | 3.78 | 0.56 |
| Used fans | 180 | 86.1% | 173 | 89.0% | 0.41 |
| Frequency of using fans | 154 | 4.31 | 152 | 4.13 | 0.08 |
| Used air conditioner | 193 | 96.8% | 222 | 96.8% | 0.98 |
| Frequency of using air conditioner | 185 | 4.28 | 214 | 4.10 | 0.03 |
| Suffered heat episode related symptoms | 246 | 55.6% | 259 | 47.9% | 0.08 |
| Used health care system | 246 | 8.5% | 259 | 9.3% | 0.77 |
| Outcomes | Treatment Group | Control Group | p Value | ||
|---|---|---|---|---|---|
| N | Mean or % | N | Mean or % | ||
| Were informed of the heat episode | 245 | 98.9% | 265 | 97.4% | 0.24 |
| Were informed of the heat episode before its onset | 217 | 75.6% | 222 | 68.0% | 0.08 |
| Number of recommended heat protection measures cited (a t-test was used) | 247 | 2.32 | 265 | 2.07 | 0.02 |
| Frequency of drinking water | 246 | 4.19 | 262 | 4.04 | 0.02 |
| Frequency of physical effort | 242 | 3.99 | 261 | 3.95 | 0.64 |
| Took cool showers or baths | 247 | 81.4% | 265 | 73.4% | 0.04 |
| Frequency of taking cool showers or baths more than usual | 200 | 3.65 | 195 | 3.51 | 0.06 |
| Visited cool or air-conditioned places | 246 | 38.6% | 264 | 38.6% | 1.00 |
| Frequency of spending time in cool or air-conditioned places | 95 | 3.57 | 99 | 3.18 | 0.00 |
| Went outside during heat episode | 245 | 62.0% | 263 | 70.3% | 0.05 |
| Frequency of staying in the shade | 146 | 3.87 | 174 | 3.84 | 0.65 |
| Used fans | 191 | 0.91 | 185 | 0.88 | 0.44 |
| Used air conditioner | 194 | 97.4% | 221 | 99.1% | 0.19 |
| Used health care system | 247 | 7.7% | 265 | 9.4% | 0.48 |
| Used health care system (women) | 176 | 5.7% | 203 | 11.3% | 0.05 |
| Used health care system (women with chronic illness) | 129 | 6.2% | 148 | 13.5% | 0.04 |
| Outcomes | Odds Ratio (Standard Error) | Confidence Interval (95%) | p Value |
|---|---|---|---|
| Frequency of using fans | 1.38 (0.51) | (0.67–2.84) | 0.38 |
| Frequency of using air conditioning | 0.67 (0.21) | (0.35–1.23) | 0.19 |
| Suffered heat episode related symptoms | 1.18 (0.38) | (0.63–2.23) | 0.60 |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Mehiriz, K.; Gosselin, P.; Tardif, I.; Lemieux, M.-A. The Effect of an Automated Phone Warning and Health Advisory System on Adaptation to High Heat Episodes and Health Services Use in Vulnerable Groups—Evidence from a Randomized Controlled Study. Int. J. Environ. Res. Public Health 2018, 15, 1581. https://doi.org/10.3390/ijerph15081581
Mehiriz K, Gosselin P, Tardif I, Lemieux M-A. The Effect of an Automated Phone Warning and Health Advisory System on Adaptation to High Heat Episodes and Health Services Use in Vulnerable Groups—Evidence from a Randomized Controlled Study. International Journal of Environmental Research and Public Health. 2018; 15(8):1581. https://doi.org/10.3390/ijerph15081581
Chicago/Turabian StyleMehiriz, Kaddour, Pierre Gosselin, Isabelle Tardif, and Marc-André Lemieux. 2018. "The Effect of an Automated Phone Warning and Health Advisory System on Adaptation to High Heat Episodes and Health Services Use in Vulnerable Groups—Evidence from a Randomized Controlled Study" International Journal of Environmental Research and Public Health 15, no. 8: 1581. https://doi.org/10.3390/ijerph15081581
APA StyleMehiriz, K., Gosselin, P., Tardif, I., & Lemieux, M.-A. (2018). The Effect of an Automated Phone Warning and Health Advisory System on Adaptation to High Heat Episodes and Health Services Use in Vulnerable Groups—Evidence from a Randomized Controlled Study. International Journal of Environmental Research and Public Health, 15(8), 1581. https://doi.org/10.3390/ijerph15081581




