Epidemiology of Suicide and the Psychiatric Perspective
Abstract
1. Introduction
2. Methods
3. Epidemiology
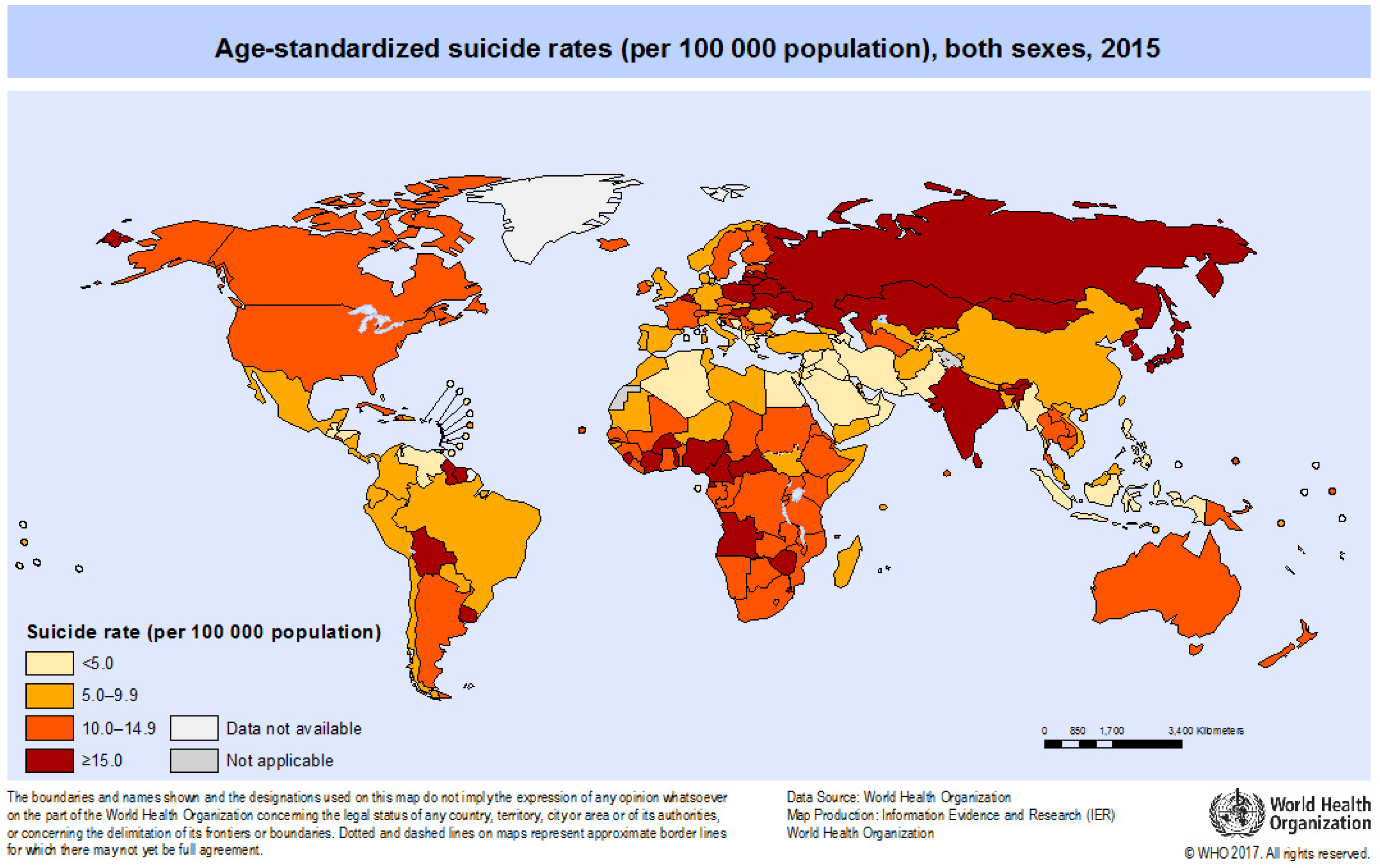
3.1. Suicide Worldwide
3.2. Age
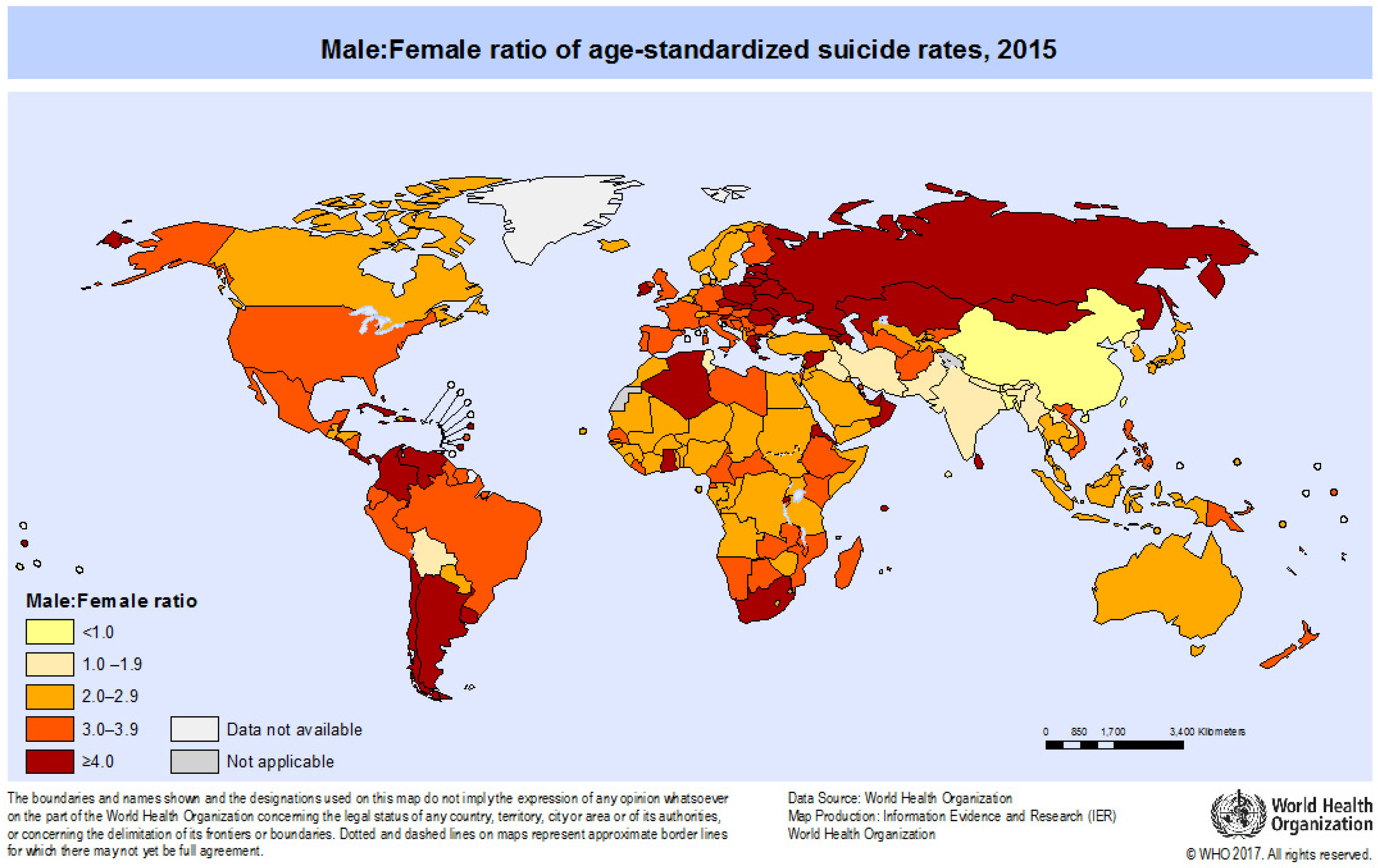
3.3. Gender
3.4. Socioeconomics
- (a)
- Demographic parameters: age, gender, ethnicity, and related parameters;
- (b)
- Social status: low income, income inequality, unemployment, low education, and low social support;
- (c)
- Social change: in a societal realm, e.g., urbanization, or on an individual basis, e.g., change in income;
- (d)
- Neighborhood: inadequate housing, overcrowding, violence and others;
- (e)
- Environmental incidences: climate change, natural catastrophe, war, conflict, and migration.
3.5. Special Groups
3.6. Methods of Suicide
3.7. Suicide Attempts
4. Suicide and Mental Illness
4.1. Suicide According to Selected Diagnoses
4.2. Comorbidities
4.3. Suicide and Physical Illness
5. Prevention
5.1. Primary Prevention
5.2. Secondary Prevention
6. Discussion
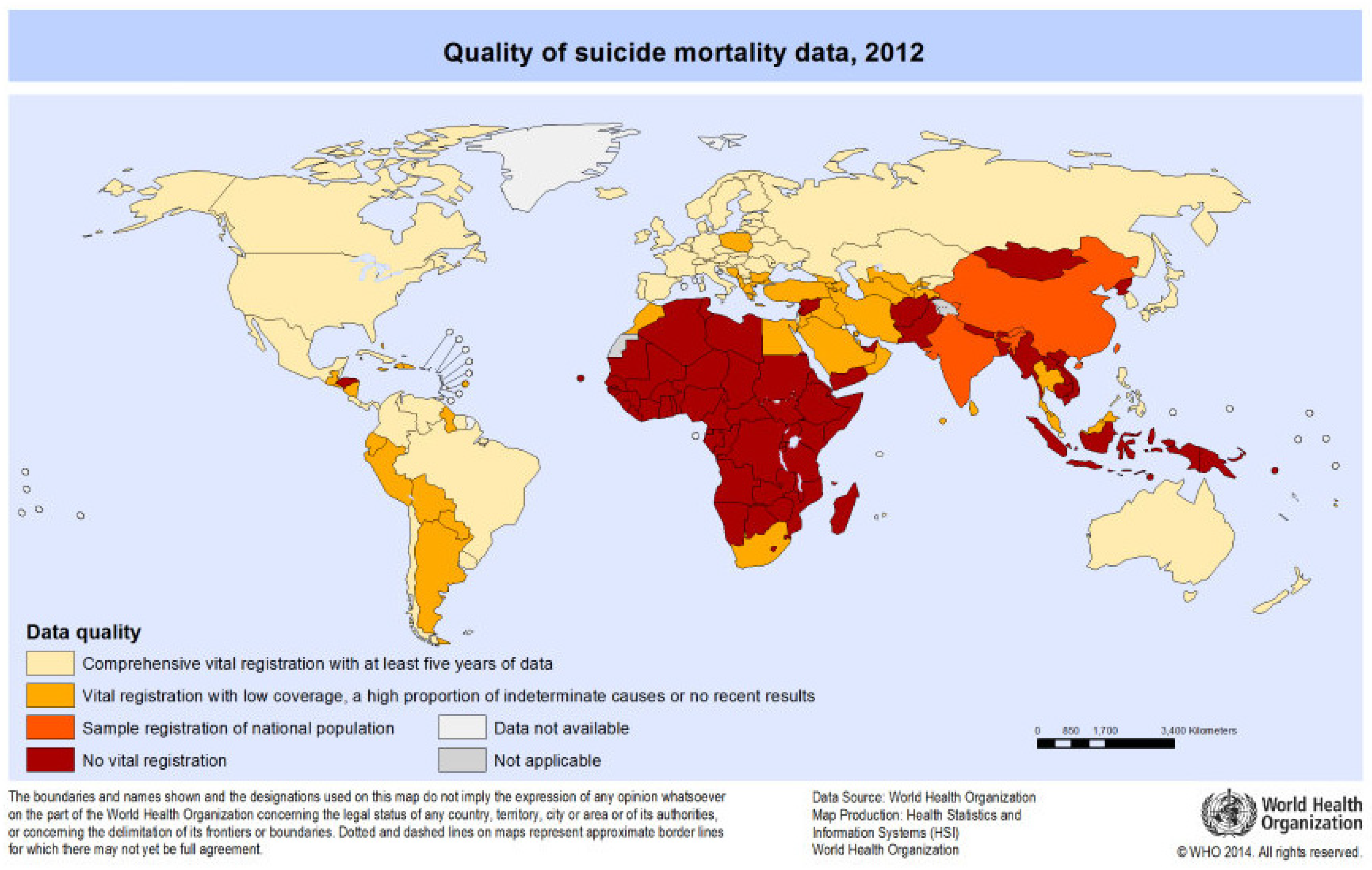
Quality of Data
7. Conclusions
Funding
Conflicts of Interest
Abbreviations and Explanations
| HIC | high income countries |
| LMIC | low and middle income countries |
| Suicide rate | per 100,000 persons, where the weights are the proportions of persons in the corresponding age groups of the WHO standard population |
| Crude suicide rate | number of suicide deaths in a year (and a rate: geographic area), divided by the population (in this area) and multiplied by 100,000 |
| Age-standardized suicide rate | a weighted average of the age-specific suicide rates |
References
- WHO Mental Health. Prevention of Suicidal Behaviours: A Task for All. Available online: http://www.who.int/mental_health/prevention/suicide/background (accessed on 15 October 2017).
- Dammann, G.; Gerisch, B. Narzistische Persönlichkeitsstörungen und Suizidalität: Behandlungsschwierigkeiten aus psychodynamischer Perspektive. [Narcissistic personality disorder and suicidality. Difficulties during psychodynamic treatment]. Schweiz. Arch. Neurol. Psychiatr. 2005, 156, 299–309. [Google Scholar]
- Pfab, R.; Eyer, F.; Jetzinger, E.; Zilker, T. Cause and motivation in cases of non-fatal drug overdoses in opiate addicts. Clin. Toxicol. 2006, 44, 255–259. [Google Scholar] [CrossRef]
- Yuodelis-Flores, C.; Ries, R.K. Addiction and suicide: A review. Am. J. Addict. 2015, 24, 98–104. [Google Scholar] [CrossRef] [PubMed]
- American Psychiatric Association. DSM-5, Diagnostic and Statistical Manual of Mental Disorders, 5th ed.; American Psychiatric Publishing: Arlington, VA, USA, 2013. [Google Scholar]
- Geneva Global Health Hub. WHO Member States. Available online: g2h2.org/watch-this/geneva-institutions/who-member-states/ (accessed on 22 June 2018).
- WHO. Preventing Suicide: A Global Imperative; WHO, Ed.; World Health Organization: Geneva, Switzerland, 2014; pp. 7, 20, 40. [Google Scholar]
- Bertolote, J.M.; Fleischmann, A. A global perspective in the epidemiology of suicide. Suicidology 2002, 7, 6–8. [Google Scholar] [CrossRef]
- Värnik, P. Suicide in the world. Int. J. Environ. Res. Public Health 2012, 9, 760–771. [Google Scholar] [CrossRef] [PubMed]
- WHO Figure: Age-Standardized Suicide Rates: Male: Female Ratio (Per 100,000). Available online: http://www.who.int/gho/mental_health/suicide_rates_male_female/en/ (accessed on 10 October 2017).
- Matsubayashi, T.; Michiko, U. The effect of national suicide prevention programs on suicide rates in 21 OECD nations. Soc. Sci. Med. 2011, 73, 1395–1400. [Google Scholar] [CrossRef] [PubMed]
- Bertolote, J.M.; Fleischmann, A. Suicide and psychiatric diagnosis: A worldwide perspective. World Psychiatry 2002, 1, 181–185. [Google Scholar] [PubMed]
- Vijayakumar, L. Suicide prevention: The urgent need in developing countries. World Psychiatry 2004, 3, 158–159. [Google Scholar] [PubMed]
- National Center for Injury Prevention and Control. Using WISQARSTM 10 Leading Causes of Death by Age Group, United States–2016. Available online: https://www.cdc.gov/injury/wisqars/LeadingCauses.html (accessed on 4 July 2018).
- WHO. WHO Mortality Database. Available online: http://apps.who.int/healthinfo/statistics/mortality/whodpms/ (accessed on 10 October 2017).
- Shah, A. Suicide rates: Age-associated trends and their correlates. J. Inj. Violence Res. 2012, 4, 79–86. [Google Scholar] [CrossRef] [PubMed]
- Pitman, A.; Krysinska, K.; Osborn, D.; King, M. Suicide in young men. Lancet 2012, 379, 2383–2392. [Google Scholar] [CrossRef]
- Yip, P.S.; Caine, E.; Yousuf, S.; Chang, S.S.; Wu, K.C.; Chen, Y.Y. Means restriction for suicide prevention. Lancet 2012, 379, 2393–2399. [Google Scholar] [CrossRef]
- American Foundation for Suicide Prevention. Available online: https://afsp.org/about-suicide/suicide-statistics/ (accessed on 15 October 2017).
- Mars, B.; Burrows, S.; Hjelmeland, H.; Gunnell, D. Suicidal behaviour across the African continent: A review of the literature. BMC Publi. Health 2014, 14, 606. [Google Scholar] [CrossRef] [PubMed]
- Jordans, M.J.; Kaufman, A.; Brenman, N.F.; Adhikari, R.P.; Luitel, N.P.; Tol, W.A.; Komproe, I. Suicide in South Asia: A scoping review. BMC Psychiatry 2014, 14, 358. [Google Scholar] [CrossRef] [PubMed]
- WHO Global Health Observatory Data Repository. Available online: http://apps.who.int/gho/data/node.main.MHSUICIDE?lang=en (accessed on 14 October 2017).
- WHO. Figure: Male: Female Ratio of Age-Standardized Suicide Rates (Per 100 000 Population); WHO: Geneva, Switzerland, 2015. [Google Scholar]
- Patel, V.; Chisholm, D.; Parikh, R.; Charlson, F.J.; Degenhardt, L.; Dua, T.; Ferrari, A.J.; Hyman, S.; Laxminarayan, R.; Levin, C.; et al. Global Priorities for Addressing the Burden of Mental, Neurological, and Substance Use Disorders. In Mental, Neurological, and Substance Use Disorders: Disease Control Priorities, Third Edition; Patel, V., Chisholm, D., Dua, T., Laxminarayan, R., Medina-Mora, M.E., Eds.; The International Bank for Reconstruction and Development/The World Bank: Washington, DC, USA, 2016; Volume 4. [Google Scholar]
- WHO Suicide. Fact Sheet. Available online: http://www.who.int/mediacentre/factsheets/fs398/en/ (accessed on 10 October 2017).
- Bantjes, J.; Iemmi, V.; Coast, E.; Channer, K.; Leone, T.; McDaid, D.; Palfreyman, A.; Stephens, B.; Lund, C. Poverty and suicide research in low- and middle-income countries: Systematic mapping of literature published in English and a proposed research agenda. Glob. Ment. Health 2017, 3, e32. [Google Scholar] [CrossRef] [PubMed]
- Kim, D. The associations between US state and local social spending, income inequality, and individual all-cause and cause-specific mortality: The National Longitudinal Mortality Study. Prev. Med. 2015, 84, 62–68. [Google Scholar] [CrossRef] [PubMed]
- Tjepkema, M.; Wilkins, R.; Long, A. Cause-specific mortality by income adequacy in Canada: A 16-year follow-up study. Health Rep. 2013, 24, 14–22. [Google Scholar] [PubMed]
- Inoue, K.; Nishimura, Y.; Okazazi, Y.; Fukunaga, T. Discussion based on analysis of the suicide rate and the average disposable income per household in Japan. West. Indian Med. J. 2014, 63, 340–343. [Google Scholar] [CrossRef] [PubMed]
- Fountoulakis, K.N.; Kawohl, W.; Theodorakis, P.N.; Kerkhof, A.J.; Navickas, A.; Hoschl, C.; Lecic-Tosevski, D.; Sorel, E.; Rancans, E.; Palova, E.; et al. Relationship of suicide rates to economic variables in Europe: 2000–2011. Br. J. Psychiatry 2014, 205, 486–496. [Google Scholar] [CrossRef] [PubMed]
- Poor, F.B.; Tabatabaei, S.M.; Bakhshani, N.M. Epidemiology of Suicide and its Associated Socio-demographic Factors in Patients Admitted to Emergency Department of Zahedan Khatam-Al-Anbia Hospital. Int. J. High Risk Behav. Addict. 2015, 3, e22637. [Google Scholar]
- Spears, M.; Montgomery, A.A.; Gunnell, D.; Araya, R. Factors associated with the development of self-harm amongst a socio-economically deprived cohort of adolescents in Santiago, Chile. Soc. Psychiatry Psychiatr. Epidemiol. 2013, 49, 629–637. [Google Scholar] [CrossRef] [PubMed]
- Knipe, D.W.; Carroll, R.; Thomas, K.H.; Pease, A.; Gunnell, D.; Metcalfe, C. Association of socio-economic position and suicide/attempted suicide in low and middle income countries in South and South-East Asia —A systematic review. BMC Public Health 2015, 15, 1055. [Google Scholar] [CrossRef] [PubMed]
- Knipe, D.W.; Gunnell, D.; Pieris, R.; Priyadarshana, C.; Weerasinghe, M.; Pearson, M.; Jayamanne, S.; Dawson, A.H.; Mohamed, F.; Gawarammana, I.; et al. Is socioeconomic position associated with risk of attempted suicide in rural Sri Lanka? A cross-sectional study of 165,000 individuals. BMJ Open 2017, 7, e014006. [Google Scholar] [CrossRef] [PubMed]
- Bhui, K.; Craig, T.; Mohamud, S.; Warfa, N.; Stansfeld, S.A.; Thornicroft, G.; Curtis, S.; McCrone, P. Mental disorders among Somali refugees: Developing culturally appropriate measures and assessing socio-cultural risk factors. Soc. Psychiatry Psychiatr. Epidemiol. 2006, 41, 400–408. [Google Scholar] [CrossRef] [PubMed]
- Shepard, D.S.; Gurewich, D.; Lwin, A.K.; Reed, G.A., Jr.; Silverman, M.M. Suicide and Suicidal Attempts in the United States: Costs and Policy Implications. Suicide Life Threat. Behav. 2015, 46, 352–362. [Google Scholar] [CrossRef] [PubMed]
- O’Dea, D.; Tucker, S. The Cost of Suicide to Society; Ministry of Health: Wellington, New Zealand, 2005. [Google Scholar]
- Platt, S.; McLean, J.; McCollam, A.; Blamey, A.; Mackenzie, M.; McDaid, D.; Woodhouse, A. Evaluation of the First Phase of Choose Life: The National Strategy and Action Plan to Prevent Suicide in Scotland; Scottish Executive Social Research: Edinburgh, UK, 2006; p. 219. [Google Scholar]
- Kennelly, B. The economic cost of suicide in Ireland. Crisis 2007, 28, 89–94. [Google Scholar] [CrossRef] [PubMed]
- Milner, A.; Witt, K.; Maheen, H.; LaMontagne, A.D. Suicide among emergency and protective service workers: A retrospective mortality study in Australia, 2001 to 2012. Work 2017, 57, 281–287. [Google Scholar] [CrossRef] [PubMed]
- Gradus, J.L.; Shipherd, J.C.; Suvak, M.K.; Giasson, H.L.; Miller, M. Suicide attempts and suicide among Marines: A decade of follow-up. Suicide Life Threat. Behav. 2012, 43, 39–49. [Google Scholar] [CrossRef] [PubMed]
- Nock, M.K.; Stein, M.B.; Heeringa, S.G.; Ursano, R.J.; Colpe, L.J.; Fullerton, C.S.; Hwang, I.; Naifeh, J.A.; Sampson, N.A.; Schoenbaum, M.; et al. Prevalence and correlates of suicidal behavior among soldiers: Results from the Army Study to Assess Risk and Resilience in Servicemembers (Army STARRS). JAMA Psychiatry 2014, 71, 514–522. [Google Scholar] [CrossRef] [PubMed]
- Jones, R.M.; Hales, H.; Butwell, M.; Ferriter, M.; Taylor, P.J. Suicide in high security hospital patients. Soc. Psychiatry Psychiatr. Epidemiol. 2010, 46, 723–731. [Google Scholar] [CrossRef] [PubMed]
- McSpadden, L.A. Ethiopian refugee resettlement in the Western United States: Social context and psychological well-being. Int. Migr. Rev. 1987, 21, 796–819. [Google Scholar] [CrossRef] [PubMed]
- Fekadu, A.; Hanlon, C.; Gebre-Eyesus, E.; Agedew, M.; Solomon, H.; Teferra, S.; Gebre-Eyesus, T.; Baheretibeb, Y.; Medhin, G.; Shibre, T.; et al. Burden of mental disorders and unmet needs among street homeless people in Addis Ababa, Ethiopia. BMC Med. 2014, 12, 138. [Google Scholar] [CrossRef] [PubMed]
- Lindert, J.; Schouler-Ocak, M.; Heinz, A.; Priebe, S. Mental health, health care utilisation of migrants in Europe. Eur. Psychiatry 2008, 23 (Suppl. 1), 14–20. [Google Scholar] [CrossRef]
- Kalt, A.; Hossain, M.; Kiss, L.; Zimmerman, C. Asylum seekers, violence and health: A systematic review of research in high-income host countries. Am. J. Public Health 2013, 103, e30–e42. [Google Scholar] [CrossRef] [PubMed]
- Ougrin, D.; Banarsee, R.; Dunn-Toroosian, V.; Majeed, A. Suicide survey in a London borough: Primary care and public health perspectives. J. Public Health 2011, 33, 385–391. [Google Scholar] [CrossRef] [PubMed]
- Bauwelinck, M.; Deboosere, P.; Willaert, D.; Vandenheede, H. Suicide mortality in Belgium at the beginning of the 21st century: Differences according to migrant background. Eur. J. Public Health 2017, 27, 111–116. [Google Scholar] [CrossRef] [PubMed]
- Spallek, J.; Reeske, A.; Norredam, M.; Nielsen, S.S.; Lehnhardt, J.; Razum, O. Suicide among immigrants in Europe--a systematic literature review. Eur. J. Public Health 2014, 25, 63–71. [Google Scholar] [CrossRef] [PubMed]
- Kõlves, K.; De Leo, D. Are immigrants responsible for the recent decline in Australian suicide rates? Epidemiol. Psychiatr. Sci. 2014, 24, 241–248. [Google Scholar] [CrossRef] [PubMed]
- Law, C.K.; Kolves, K.; De Leo, D. Suicide mortality in second-generation migrants, Australia, 2001–2008. Soc. Psychiatry Psychiatr. Epidemiol. 2013, 49, 601–608. [Google Scholar] [CrossRef] [PubMed]
- Singh, G.K.; Miller, B.A. Health, life expectancy, and mortality patterns among immigrant populations in the United States. Can. J. Public Health 2004, 95, 14–21. [Google Scholar]
- Garssen, M.J.; Hoogenboezem, J.; Kerkhof, A.J. [Suicide among migrant populations and native Dutch in The Netherlands]. Ned. Tijdschr. Geneeskd. 2006, 150, 2143–2149. [Google Scholar] [PubMed]
- Lipsicas, C.B.; Mäkinen, I.H. Immigration and suicidality in the young. Can. J. Psychiatry 2010, 55, 274–281. [Google Scholar] [CrossRef] [PubMed]
- Honkaniemi, H.; Bacchus-Hertzman, J.; Fritzell, J.; Rostila, M. Mortality by country of birth in the Nordic countries—A systematic review of the literature. BMC Public Health 2017, 17, 511. [Google Scholar] [CrossRef] [PubMed]
- Haas, A.P.; Eliason, M.; Mays, V.M.; Mathy, R.M.; Cochran, S.D.; D’Augelli, A.R.; Silverman, M.M.; Fisher, P.W.; Hughes, T.; Rosario, M.; et al. Suicide and suicide risk in lesbian, gay, bisexual, and transgender populations: Review and recommendations. J. Homosex. 2011, 58, 10–51. [Google Scholar] [CrossRef] [PubMed]
- Virupaksha, H.G.; Muralidhar, D.; Ramakrishna, J. Suicide and Suicidal Behavior among Transgender Persons. Indian J. Psychol. Med. 2016, 38, 505–509. [Google Scholar] [CrossRef] [PubMed]
- Bertolote, J.M.; Fleischmann, A. Suicidal behavior prevention: WHO perspectives on research. In American Journal of Medical Genetics Part C: Seminars in Medical Genetics; Wiley Subscription Services, Inc.: Hoboken, NJ, USA, 2005. [Google Scholar]
- Colucci, E. The cultural facet of suicidal behaviour: Its importance and negligence. Adv. Ment. Health 2006, 5, 1–13. [Google Scholar] [CrossRef]
- Osafo, J.; Hjelmeland, H.; Akotia, C.S.; Knizek, B.L. Social Injury: An interpretative phenomenological analysis of the attitudes toward suicide of lay persons in Ghana. Int. J. Qual. Stud. Health Well-Being 2011, 6, 8708. [Google Scholar] [CrossRef] [PubMed]
- Osafo, J.; Knizek, B.L.; Akotia, C.S.; Hjelmeland, H. Attitudes of psychologists and nurses toward suicide and suicide prevention in Ghana: A qualitative study. Int. J. Nurs. Stud. 2012, 49, 691–700. [Google Scholar] [CrossRef] [PubMed]
- Petridou, E.; Papadopoulos, F.C.; Frangakis, C.E.; Skalkidou, A.; Trichopoulos, D. A role of sunshine in the triggering of suicide. Epidemiology 2002, 13, 106–109. [Google Scholar] [CrossRef] [PubMed]
- Hiltunen, L.; Suominen, K.; Lonnqvist, J.; Partonen, T. Relationship between daylength and suicide in Finland. J. Circadian Rhythms 2011, 9, 10. [Google Scholar] [CrossRef] [PubMed]
- Nejar, K.A.; Bensenor, I.M.; Lotufo, P.A. Sunshine and suicide at the tropic of Capricorn, Sao Paulo, Brazil, 1996–2004. Rev. Saude Publ. 2007, 41, 1062–1064. [Google Scholar] [CrossRef]
- Schmidtke, A.; Häfner, H. The Werther effect after television films: New evidence for an old hypothesis. Psychol. Med. 1988, 18, 665–676. [Google Scholar] [CrossRef] [PubMed]
- Etzersdorfer, E.; Voracek, M.; Sonneck, G. A dose-response relationship between imitational suicides and newspaper distribution. Arch. Suicide Res. 2004, 8, 137–145. [Google Scholar] [CrossRef] [PubMed]
- Sisask, M.; Värnik, A. Media Roles in Suicide Prevention: A Systematic Review. Int. J. Environ. Res. Public Health 2012, 9, 123–138. [Google Scholar] [CrossRef] [PubMed]
- Vijayakumar, L.; Phillips, M.R.; Silverman, M.M.; Gunnell, D.; Carli, V. Suicide. In Mental, Neurological, and Substance Use Disorders: Disease Control Priorities, 3rd ed.; Patel, V., Chisholm, D., Dua, T., Laxminarayan, R., Medina-Mora, M.E., Eds.; The International Bank for Reconstruction and Development/The World Bank: Washington, DC, USA, 2015; Volume 4, pp. 163–181. [Google Scholar]
- Ajdacic-Gross, V.; Weiss, M.G.; Ring, M.; Hepp, U.; Bopp, M.; Gutzwiller, F.; Rössler, W. Methods of suicide: International suicide patterns derived from the WHO mortality database. Bull. World Health Organ. 2008, 86, 726–732. [Google Scholar] [CrossRef] [PubMed]
- Park, S.; Kim, Y. Prevalence, correlates, and associated psychological problems of substance use in Korean adolescents. BMC Public Health 2016, 16, 79. [Google Scholar] [CrossRef] [PubMed]
- Kõlves, K.; de Leo, D. Suicide methods in children and adolescents. Eur. Child Adolesc. Psychiatry 2016, 26, 155–164. [Google Scholar] [CrossRef] [PubMed]
- Spicer, R.S.; Miller, T.R. Suicide acts in 8 states: Incidence and case fatality rates by demographics and method. Am. J. Public Health 2000, 90, 1885–1891. [Google Scholar] [PubMed]
- Wasserman, D. Suicide: An Unnecessary Death; Martin Dunitz Ltd.: London, UK, 2001. [Google Scholar]
- Bertolote, J.M.; Fleischmann, A.; De Leo, D.; Bolhari, J.; Botega, N.; De Silva, D.; Tran Thi Thanh, H.; Phillips, M.; Schlebusch, L.; Varnik, A.; et al. Suicide attempts, plans, and ideation in culturally diverse sites: The WHO SUPRE-MISS community survey. Psychol. Med. 2005, 35, 1457–1465. [Google Scholar] [CrossRef] [PubMed]
- Bertolote, J.M.; Fleischmann, A.; De Leo, D.; Phillips, M.R.; Botega, N.J.; Vijayakumar, L.; De Silva, D.; Schlebusch, L.; Nguyen, V.T.; Sisask, M.; et al. Repetition of suicide attempts: Data from emergency care settings in five culturally different low- and middle-income countries participating in the WHO SUPRE-MISS Study. Crisis 2010, 31, 194–201. [Google Scholar] [CrossRef] [PubMed]
- Centers for Disease Control and Prevention. Suicide. Available online: http://www.cdc.gov/ViolencePrevention/pdf/Suicide_DataSheet-a.pdf (accessed on 21 November 2017).
- Weissman, M.M.; Bland, R.C.; Canino, G.J.; Greenwald, S.; Hwu, H.G.; Joyce, P.R.; Karam, E.G.; Lee, C.K.; Lellouch, J.; Lépine, J.P.; et al. Prevalence of suicide ideation and suicide attempts in nine countries. Psychol. Med. 1999, 29, 9–17. [Google Scholar] [CrossRef] [PubMed]
- Bernal, M.; Haro, J.M.; Bernert, S.; Brugha, T.; de Graaf, R.; Bruffaerts, R.; Lepine, J.P.; de Girolamo, G.; Vilagut, G.; Gasquet, I.; et al. Risk factors for suicidality in Europe: Results from the ESEMED study. J. Affect. Disord. 2007, 101, 27–34. [Google Scholar] [CrossRef] [PubMed]
- Bertolote, J.M.; Fleischmann, A.; De Leo, D.; Wasserman, D. Psychiatric diagnoses and suicide: Revisiting the evidence. Crisis 2004, 25, 147–155. [Google Scholar] [CrossRef] [PubMed]
- Chang, B.; Gitlin, D.; Patel, R. The depressed patient and suicidal patient in the emergency department: Evidence-based management and treatment strategies. Emerg. Med. Pract. 2011, 13, 23–24. [Google Scholar]
- Ferrari, A.J.; Norman, R.E.; Freedman, G.; Baxter, A.J.; Pirkis, J.E.; Harris, M.G.; Page, A.; Carnahan, E.; Degenhardt, L.; Vos, T. The burden attributable to mental and substance use disorders as risk factors for suicide: Findings from the Global Burden of Disease Study 2010. PLoS ONE 2014, 9, e91936. [Google Scholar] [CrossRef] [PubMed]
- Röcker, S.; Bachmann, S. Suicidality in mental illness—Prevention and therapy. Ther. Umsch. 2015, 72, 611–617. [Google Scholar] [CrossRef] [PubMed]
- Van Dulmen, M.; Mata, A.; Claxton, S.; Klipfel, K.; Schinka, K.; Swahn, M.; Bossarte, R. Longitudinal associations between violence and suicidality from adolescence into adulthood. Suicide Life Threat. Behav. 2013, 43, 523–531. [Google Scholar] [CrossRef] [PubMed]
- Kiss, L.; Pocock, N.S.; Naisanguansri, V.; Suos, S.; Dickson, B.; Thuy, D.; Koehler, J.; Sirisup, K.; Pongrungsee, N.; Nguyen, V.A.; et al. Health of men, women, and children in post-trafficking services in Cambodia, Thailand, and Vietnam: An observational cross-sectional study. Lancet Glob. Health 2015, 3, e154–e161. [Google Scholar] [CrossRef]
- Lacey, K.K.; Parnell, R.; Mouzon, D.M.; Matusko, N.; Head, D.; Abelson, J.M.; Jackson, J.S. The mental health of US Black women: The roles of social context and severe intimate partner violence. BMJ Open 2015, 5, e008415. [Google Scholar] [CrossRef] [PubMed]
- Grubisic-Ilic, M.; Kozaric-Kovacic, D.; Grubisic, F.; Kovacic, Z. Epidemiological study of suicide in the Republic of Croatia—Comparison of war and post-war periods and areas directly and indirectly affected by war. Eur. Psychiatry 2002, 17, 259–264. [Google Scholar] [CrossRef]
- Selakovic-Bursic, S.; Haramic, E.; Leenaars, A.A. The Balkan Piedmont: Male suicide rates pre-war, wartime, and post-war in Serbia and Montenegro. Arch. Suicide Res. 2006, 10, 225–238. [Google Scholar] [CrossRef] [PubMed]
- Oron Ostre, I. Wars and suicides in Israel, 1948–2006. Int. J. Environ. Res. Public Health 2012, 9, 1927–1938. [Google Scholar] [CrossRef] [PubMed]
- Bertolote, J.M.; Fleischmann, A.; De Leo, D.; Wasserman, D. Suicide and mental disorders: Do we know enough? Br. J. Psychiatry 2003, 183, 382–383. [Google Scholar] [CrossRef] [PubMed]
- Hübner-Liebermann, B.; Spiessl, H.; Cording, C. [Suicides in psychiatric in-patient treatment]. Psychiatr. Prax. 2001, 28, 330–334. [Google Scholar] [CrossRef] [PubMed]
- Fujita, T.; Kurisu, E. Suicide deaths among psychiatric patients—A study based on vital statistics. Nihon Koshu Eisei Zasshi 1992, 39, 858–864. [Google Scholar] [PubMed]
- Ganesvaran, T.; Shah, A.K. Psychiatric in-patient suicide rates: A 21-year study. Med. Sci. Law 1997, 37, 202–209. [Google Scholar] [CrossRef] [PubMed]
- Large, M.M.; Chung, D.T.; Davidson, M.; Weiser, M.; Ryan, C.J. In-patient suicide: Selection of people at risk, failure of protection and the possibility of causation. BJPsych Open 2017, 3, 102–105. [Google Scholar] [CrossRef] [PubMed]
- Goldacre, M.; Seagroatt, V.; Hawton, K. Suicide after discharge from psychiatric inpatient care. Lancet 1993, 342, 283–286. [Google Scholar] [CrossRef]
- Geddes, J.R.; Juszczak, E.; O’Brien, F.; Kendrick, S. Suicide in the 12 months after discharge from psychiatric inpatient care, Scotland 1968-92. J. Epidemiol. Community Health 1997, 51, 430–434. [Google Scholar] [CrossRef] [PubMed]
- Isometsä, E.; Sund, R.; Pirkola, S. Post-discharge suicides of inpatients with bipolar disorder in Finland. Bipolar Disord. 2014, 16, 867–874. [Google Scholar] [CrossRef] [PubMed]
- Chung, D.T.; Ryan, C.J.; Hadzi-Pavlovic, D.; Singh, S.P.; Stanton, C.; Large, M.M. Suicide Rates After Discharge From Psychiatric Facilities: A Systematic Review and Meta-analysis. JAMA Psychiatry 2017, 74, 694–702. [Google Scholar] [CrossRef] [PubMed]
- Kim, J.P.; Hyun, M.Y. Depression and suicidal ideation in elders with dementia. J. Korean Acad. Nurs. 2013, 43, 296–303. [Google Scholar] [CrossRef] [PubMed]
- Sabodash, V.; Mendez, M.F.; Fong, S.; Hsiao, J.J. Suicidal behavior in dementia: A special risk in semantic dementia. Am. J. Alzheimers Dis. Other Demen. 2013, 28, 592–599. [Google Scholar] [CrossRef] [PubMed]
- Fonseca, L.; Machado, A. Suicidal behaviour in frontotemporal dementia patients—A retrospective study. Int. J. Geriatr. Psychiatry 2014, 29, 217–218. [Google Scholar] [CrossRef] [PubMed]
- Richard-Devantoy, S.; Berlim, M.T.; Jollant, F. Suicidal behaviour and memory: A systematic review and meta-analysis. World J. Biol. Psychiatry 2014, 16, 544–566. [Google Scholar] [CrossRef] [PubMed]
- Koyama, A.; Fujise, N.; Matsushita, M.; Ishikawa, T.; Hashimoto, M.; Ikeda, M. Suicidal ideation and related factors among dementia patients. J. Affect. Disord. 2015, 178, 66–70. [Google Scholar] [CrossRef] [PubMed]
- Serafini, G.; Calcagno, P.; Lester, D.; Girardi, P.; Amore, M.; Pompili, M. Suicide Risk in Alzheimer’s Disease: A Systematic Review. Curr. Alzheimer Res. 2016, 13, 1083–1099. [Google Scholar] [CrossRef] [PubMed]
- Davis, D.S. Alzheimer disease and pre-emptive suicide. J. Med. Ethics 2013, 40, 543–549. [Google Scholar] [CrossRef] [PubMed]
- Dresser, R. Pre-emptive suicide, precedent autonomy and preclinical Alzheimer disease. J. Med. Ethics 2013, 40, 550–551. [Google Scholar] [CrossRef] [PubMed]
- Whiteford, H.A.; Degenhardt, L.; Rehm, J.; Baxter, A.J.; Ferrari, A.J.; Erskine, H.E.; Charlson, F.J.; Norman, R.E.; Flaxman, A.D.; Johns, N.; et al. Global burden of disease attributable to mental and substance use disorders: Findings from the Global Burden of Disease Study 2010. Lancet 2013, 382, 1575–1586. [Google Scholar] [CrossRef]
- Driessen, M.; Veltrup, C.; Weber, J.; John, U.; Wetterling, T.; Dilling, H. Psychiatric co-morbidity, suicidal behaviour and suicidal ideation in alcoholics seeking treatment. Addiction 1998, 93, 889–894. [Google Scholar] [CrossRef] [PubMed]
- Darvishi, N.; Farhadi, M.; Haghtalab, T.; Poorolajal, J. Alcohol-related risk of suicidal ideation, suicide attempt, and completed suicide: A meta-analysis. PLoS ONE 2015, 10, e0126870. [Google Scholar] [CrossRef] [PubMed]
- Sher, L. Alcohol consumption and suicide. QJM 2006, 99, 57–61. [Google Scholar] [CrossRef] [PubMed]
- Vijayakumar, L.; Kumar, M.S.; Vijayakumar, V. Substance use and suicide. Curr. Opin. Psychiatry 2011, 24, 197–202. [Google Scholar] [CrossRef] [PubMed]
- Hung, G.C.; Cheng, C.T.; Jhong, J.R.; Tsai, S.Y.; Chen, C.C.; Kuo, C.J. Risk and protective factors for suicide mortality among patients with alcohol dependence. J. Clin. Psychiatry 2015, 76, 1687–1693. [Google Scholar] [CrossRef] [PubMed]
- Sher, L. Functional magnetic resonance imaging in studies of the neurobiology of suicidal behavior in adolescents with alcohol use disorders. Int. J. Adolesc. Med. Health 2007, 19, 11–18. [Google Scholar] [CrossRef] [PubMed]
- Conner, K.R.; Huguet, N.; Caetano, R.; Giesbrecht, N.; McFarland, B.H.; Nolte, K.B.; Kaplan, M.S. Acute use of alcohol and methods of suicide in a US national sample. Am. J. Public Health 2013, 104, 171–178. [Google Scholar] [CrossRef] [PubMed]
- Kennedy, M.C.; Marshall, B.D.; Hayashi, K.; Nguyen, P.; Wood, E.; Kerr, T. Heavy alcohol use and suicidal behavior among people who use illicit drugs: A cohort study. Drug Alcohol Depend. 2015, 151, 272–277. [Google Scholar] [CrossRef] [PubMed]
- Wetterling, T.; Schneider, B. Alcohol intoxication and suicidality. Psychiatr. Prax. 2013, 40, 259–263. [Google Scholar] [PubMed]
- Fadem, B. Behavioral Science in Medicine; Lippincott Williams & Wilkins: Philadelphia, PA, USA, 2004; p. 217. [Google Scholar]
- Youssef, N.A.; Rich, C.L. Does acute treatment with sedatives/hypnotics for anxiety in depressed patients affect suicide risk? A literature review. Ann. Clin. Psychiatry 2008, 20, 157–169. [Google Scholar] [CrossRef] [PubMed]
- Dodds, T.J. Prescribed Benzodiazepines and Suicide Risk: A Review of the Literature. Prim. Care Companion CNS Disord. 2017, 19. [Google Scholar] [CrossRef] [PubMed]
- Darke, S.; Ross, J. Suicide among heroin users: Rates, risk factors and methods. Addiction 2002, 97, 1383–1394. [Google Scholar] [CrossRef] [PubMed]
- Ayd, F.J. Lexicon of Psychiatry, Neurology, and the Neurosciences, 2nd ed.; Lippincott Williams & Wilkins: Philadelphia, PA, USA, 2000; p. 256. [Google Scholar]
- Darke, S.; Kaye, S.; McKetin, R.; Duflou, J. Major physical and psychological harms of methamphetamine use. Drug. Alcohol. Rev. 2008, 27, 253–262. [Google Scholar] [CrossRef] [PubMed]
- Donoghue, K.; Doody, G.A.; Murray, R.M.; Jones, P.B.; Morgan, C.; Dazzan, P.; Hart, J.; Mazzoncini, R.; Maccabe, J.H. Cannabis use, gender and age of onset of schizophrenia: Data from the AESOP study. Psychiatry Res. 2014, 215, 528–532. [Google Scholar] [CrossRef] [PubMed]
- Leite, R.T.; Nogueira Sde, O.; do Nascimento, J.P.; de Lima, L.S.; da Nobrega, T.B.; Virginio Mda, S.; Moreno, L.M.; Sampaio, B.H.; de Matos, E.S.F.G. The Use of Cannabis as a Predictor of Early Onset of Bipolar Disorder and Suicide Attempts. Neural Plast. 2015, 2015, 434127. [Google Scholar] [CrossRef] [PubMed]
- Pompili, M.; Amador, X.F.; Girardi, P.; Harkavy-Friedman, J.; Harrow, M.; Kaplan, K.; Krausz, M.; Lester, D.; Meltzer, H.Y.; Modestin, J. Suicide risk in schizophrenia: Learning from the past to change the future. Ann. Gen. Psychiatry 2007, 6, 10. [Google Scholar] [CrossRef] [PubMed]
- Van Os, J.; Kapur, S. Schizophrenia. Lancet 2009, 374, 635–645. [Google Scholar] [CrossRef]
- Nordentoft, M.; Madsen, T.; Fedyszyn, I. Suicidal behavior and mortality in first-episode psychosis. J. Nerv. Ment. Dis. 2015, 203, 387–392. [Google Scholar] [CrossRef] [PubMed]
- Remschmidt, H.; Theisen, F. Early-onset schizophrenia. Neuropsychobiology 2012, 66, 63–69. [Google Scholar] [CrossRef] [PubMed]
- Bagaric, D.; Brecic, P.; Ostojic, D.; Jukic, V.; Goles, A. The relationship between depressive syndrome and suicidal risk in patients with acute schizophrenia. Croat. Med. J. 2013, 54, 436–443. [Google Scholar] [CrossRef] [PubMed]
- Kjelby, E.; Sinkeviciute, I.; Gjestad, R.; Kroken, R.A.; Loberg, E.M.; Jorgensen, H.A.; Hugdahl, K.; Johnsen, E. Suicidality in schizophrenia spectrum disorders: The relationship to hallucinations and persecutory delusions. Eur. Psychiatry 2015, 30, 830–836. [Google Scholar] [CrossRef] [PubMed]
- Gomez-Duran, E.L.; Martin-Fumado, C.; Hurtado-Ruiz, G. Clinical and epidemiological aspects of suicide in patients with schizophrenia. Actas Esp. Psiquiatr. 2012, 40, 333–345. [Google Scholar] [PubMed]
- Jovanovic, N.; Podlesek, A.; Medved, V.; Grubisin, J.; Mihaljevic-Peles, A.; Goran, T.; Lovretic, V. Association between psychopathology and suicidal behavior in schizophrenia. A cross-sectional study of 509 participants. Crisis 2013, 34, 374–381. [Google Scholar] [CrossRef] [PubMed]
- Mork, E.; Walby, F.A.; Harkavy-Friedman, J.M.; Barrett, E.A.; Steen, N.E.; Lorentzen, S.; Andreassen, O.A.; Melle, I.; Mehlum, L. Clinical characteristics in schizophrenia patients with or without suicide attempts and non-suicidal self-harm—A cross-sectional study. BMC Psychiatry 2013, 13, 255. [Google Scholar] [CrossRef] [PubMed]
- Popovic, D.; Benabarre, A.; Crespo, J.M.; Goikolea, J.M.; Gonzalez-Pinto, A.; Gutierrez-Rojas, L.; Montes, J.M.; Vieta, E. Risk factors for suicide in schizophrenia: Systematic review and clinical recommendations. Acta Psychiatr Scand. 2014, 130, 418–426. [Google Scholar] [CrossRef] [PubMed]
- Weiser, M.; Kapra, O.; Werbeloff, N.; Goldberg, S.; Fenchel, D.; Reichenberg, A.; Yoffe, R.; Ginat, K.; Fruchter, E.; Davidson, M. A population-based longitudinal study of suicide risk in male schizophrenia patients: Proximity to hospital discharge and the moderating effect of premorbid IQ. Schizophr. Res. 2015, 169, 159–164. [Google Scholar] [CrossRef] [PubMed]
- Ferrari, A.J.; Charlson, F.J.; Norman, R.E.; Patten, S.B.; Freedman, G.; Murray, C.J.; Vos, T.; Whiteford, H.A. Burden of depressive disorders by country, sex, age, and year: Findings from the global burden of disease study 2010. PLoS Med. 2013, 10, e1001547. [Google Scholar] [CrossRef] [PubMed]
- WHO. Mental Health Atlas 2014; WHO: Geneva, Switzerland, 2015. [Google Scholar]
- Ösby, U.; Brandt, L.; Correia, N.; Ekbom, A.; Sparen, P. Excess mortality in bipolar and unipolar disorder in Sweden. Arch. Gen. Psychiatry 2001, 58, 844–850. [Google Scholar] [CrossRef] [PubMed]
- Lépine, J.P.; Briley, M. The increasing burden of depression. Neuropsychiatr. Dis. Treat. 2011, 7 (Suppl. 1), 3–7. [Google Scholar] [PubMed]
- Ganguli, M.; Dodge, H.H.; Mulsant, B.H. Rates and predictors of mortality in an aging, rural, community-based cohort: The role of depression. Arch. Gen. Psychiatry 2002, 59, 1046–1052. [Google Scholar] [CrossRef] [PubMed]
- Vythilingam, M.; Chen, J.; Bremner, J.D.; Mazure, C.M.; Maciejewski, P.K.; Nelson, J.C. Psychotic depression and mortality. Am. J. Psychiatry 2003, 160, 574–576. [Google Scholar] [CrossRef] [PubMed]
- Simpson, S.G.; Jamison, K.R. The risk of suicide in patients with bipolar disorders. J. Clin. Psychiatry 1999, 60, 53–56. [Google Scholar] [PubMed]
- Schaffer, A.; Isometsa, E.T.; Tondo, L.; H Moreno, D.; Turecki, G.; Reis, C.; Cassidy, F.; Sinyor, M.; Azorin, J.M.; Kessing, L.V.; et al. International Society for Bipolar Disorders Task Force on Suicide: Meta-analyses and meta-regression of correlates of suicide attempts and suicide deaths in bipolar disorder. Bipolar Disord. 2014, 17, 1–16. [Google Scholar] [CrossRef] [PubMed]
- Angelakis, I.; Gooding, P.; Tarrier, N.; Panagioti, M. Suicidality in obsessive compulsive disorder (OCD): A systematic review and meta-analysis. Clin. Psychol. Rev. 2015, 39, 1–15. [Google Scholar] [CrossRef] [PubMed]
- Sareen, J.; Houlahan, T.; Cox, B.J.; Asmundson, G.J. Anxiety disorders associated with suicidal ideation and suicide attempts in the National Comorbidity Survey. J. Nerv. Ment. Dis. 2005, 193, 450–454. [Google Scholar] [CrossRef] [PubMed]
- Cougle, J.R.; Keough, M.E.; Riccardi, C.J.; Sachs-Ericsson, N. Anxiety disorders and suicidality in the National Comorbidity Survey-Replication. J. Psychiatr. Res. 2009, 43, 825–829. [Google Scholar] [CrossRef] [PubMed]
- Panagioti, M.; Gooding, P.A.; Tarrier, N. A meta-analysis of the association between posttraumatic stress disorder and suicidality: The role of comorbid depression. Compr. Psychiatry 2012, 53, 915–930. [Google Scholar] [PubMed]
- Lee, D.J.; Liverant, G.I.; Lowmaster, S.E.; Gradus, J.L.; Sloan, D.M. PTSD and reasons for living: Associations with depressive symptoms and alcohol use. Psychiatry Res. 2014, 219, 550–555. [Google Scholar] [CrossRef] [PubMed]
- Cougle, J.R.; Resnick, H.; Kilpatrick, D.G. PTSD, depression, and their comorbidity in relation to suicidality: Cross-sectional and prospective analyses of a national probability sample of women. Depress. Anxiety 2009, 26, 1151–1157. [Google Scholar] [CrossRef] [PubMed]
- Wherry, J.N.; Baldwin, S.; Junco, K.; Floyd, B. Suicidal thoughts/behaviors in sexually abused children. J. Child Sex. Abus 2013, 22, 534–551. [Google Scholar] [CrossRef] [PubMed]
- Selaman, Z.M.; Chartrand, H.K.; Bolton, J.M.; Sareen, J. Which symptoms of post-traumatic stress disorder are associated with suicide attempts? J. Anxiety Disord. 2014, 28, 246–251. [Google Scholar] [CrossRef] [PubMed]
- LeBouthillier, D.M.; McMillan, K.A.; Thibodeau, M.A.; Asmundson, G.J. Types and Number of Traumas Associated With Suicidal Ideation and Suicide Attempts in PTSD: Findings From a U.S. Nationally Representative Sample. J. Trauma. Stress 2015, 28, 183–190. [Google Scholar] [CrossRef] [PubMed]
- Tintinalli, J.E. Emergency Medicine: A Comprehensive Study Guide; McGraw-Hill Companies: New York, NY, USA, 2010; pp. 1940–1946. [Google Scholar]
- Hoang, U.; Goldacre, M.; James, A. Mortality following hospital discharge with a diagnosis of eating disorder: National record linkage study, England, 2001–2009. Int. J. Eat Disord. 2014, 47, 507–515. [Google Scholar] [CrossRef] [PubMed]
- Lieb, K.; Zanarini, M.C.; Schmahl, C.; Linehan, M.M.; Bohus, M. Borderline personality disorder. Lancet 2004, 364, 453–461. [Google Scholar] [CrossRef]
- Pompili, M.; Girardi, P.; Ruberto, A.; Tatarelli, R. Suicide in borderline personality disorder: A meta-analysis. Nord. J. Psychiatry 2005, 59, 319–324. [Google Scholar] [CrossRef] [PubMed]
- Stone, M.H. Long-Term Course of Borderline Personality Disorder. Psychodyn. Psychiatry 2016, 44, 449–474. [Google Scholar] [CrossRef] [PubMed]
- Paris, J. Is hospitalization useful for suicidal patients with borderline personality disorder? J. Pers. Disord. 2004, 18, 240–247. [Google Scholar] [CrossRef] [PubMed]
- Goodman, M.; Roiff, T.; Oakes, A.H.; Paris, J. Suicidal risk and management in borderline personality disorder. Curr. Psychiatry Rep. 2011, 14, 79–85. [Google Scholar] [CrossRef] [PubMed]
- Ansell, E.B.; Wright, A.G.; Markowitz, J.C.; Sanislow, C.A.; Hopwood, C.J.; Zanarini, M.C.; Yen, S.; Pinto, A.; McGlashan, T.H.; Grilo, C.M. Personality disorder risk factors for suicide attempts over 10 years of follow-up. Pers. Disord. 2015, 6, 161–167. [Google Scholar] [CrossRef] [PubMed]
- Heisel, M.J.; Links, P.S.; Conn, D.; van Reekum, R.; Flett, G.L. Narcissistic personality and vulnerability to late-life suicidality. Am. J. Geriatr. Psychiatry 2007, 15, 734–741. [Google Scholar] [CrossRef] [PubMed]
- Blasco-Fontecilla, H.; Baca-Garcia, E.; Dervic, K.; Perez-Rodriguez, M.M.; Lopez-Castroman, J.; Saiz-Ruiz, J.; Oquendo, M.A. Specific features of suicidal behavior in patients with narcissistic personality disorder. J. Clin. Psychiatry 2009, 70, 1583–1587. [Google Scholar] [CrossRef] [PubMed]
- Pincus, A.L.; Ansell, E.B.; Pimentel, C.A.; Cain, N.M.; Wright, A.G.C.; Levy, K.N. Initial construction and validation of the Pathological Narcissism Inventory. Psychol. Assess. 2009, 21, 365–379. [Google Scholar] [CrossRef] [PubMed]
- Hansen, P.E.; Wang, A.G.; Stage, K.B.; Kragh-Sorensen, P. Comorbid personality disorder predicts suicide after major depression: A 10-year follow-up. Acta Psychiat. Scand. 2003, 107, 436–440. [Google Scholar] [CrossRef] [PubMed]
- Buckley, P.F.; Brown, E.S. Prevalence and consequences of dual diagnosis. J. Clin. Psychiatry 2006, 67, e01. [Google Scholar] [CrossRef] [PubMed]
- Pallanti, S.; Rossi, N.B.; Hollander, E. Pathological Gambling. In Clinical Manual of Impulse-Control Disorders; Hollander, E.S.D.J., Ed.; American Psychiatric Publishing: Arlington, VA, USA, 2006; p. 253. [Google Scholar]
- Hansen, M.; Rossow, I. Gambling and suicidal behaviour. Tidsskr. Nor. Laegeforen. 2008, 128, 174–176. [Google Scholar] [PubMed]
- Oliveira, M.P.; Silveira, D.X.; Silva, M.T. Pathological gambling and its consequences for public health. Rev. Saude Publ. 2008, 42, 542–549. [Google Scholar] [CrossRef]
- Allebeck, P.; Bolund, C.; Ringback, G. Increased suicide rate in cancer patients. A cohort study based on the Swedish Cancer-Environment Register. J. Clin. Epidemiol. 1989, 42, 611–666. [Google Scholar] [CrossRef]
- Anguiano, L.; Mayer, D.K.; Piven, M.L.; Rosenstein, D. A literature review of suicide in cancer patients. Cancer Nurs. 2011, 35, E14–E26. [Google Scholar] [CrossRef] [PubMed]
- Lee, S.J.; Park, J.H.; Park, B.Y.; Kim, S.Y.; Lee, I.H.; Kim, J.H.; Koh, D.H.; Kim, C.H.; Sohn, M.S. Depression and suicide ideas of cancer patients and influencing factors in South Korea. Asian Pac. J. Cancer Prev. 2014, 15, 2945–2950. [Google Scholar] [CrossRef] [PubMed]
- Keiser, O.; Spoerri, A.; Brinkhof, M.W.; Hasse, B.; Gayet-Ageron, A.; Tissot, F.; Christen, A.; Battegay, M.; Schmid, P.; Bernasconi, E. Suicide in HIV-infected individuals and the general population in Switzerland, 1988–2008. Am. J. Psychiatry 2009, 167, 143–150. [Google Scholar] [CrossRef] [PubMed]
- Schlebusch, L.; Vawda, N. HIV-infection as a self-reported risk factor for attempted suicide in South Africa. Afr. J. Psychiatry 2010, 13, 280–283. [Google Scholar] [CrossRef]
- Guimaraes, P.M.; Passos, S.R.; Calvet, G.A.; Hokerberg, Y.H.; Lessa, J.L.; Andrade, C.A. Suicide risk and alcohol and drug abuse in outpatients with HIV infection and Chagas disease. Rev. Bras. Psiquiatr. 2014, 36, 131–137. [Google Scholar] [PubMed]
- Schlebusch, L.; Govender, R.D. Elevated Risk of Suicidal Ideation in HIV-Positive Persons. Depress. Res. Treat. 2015, 2015, 609172. [Google Scholar] [CrossRef] [PubMed]
- Pompili, M.; Forte, A.; Palermo, M.; Stefani, H.; Lamis, D.A.; Serafini, G.; Amore, M.; Girardi, P. Suicide risk in multiple sclerosis: A systematic review of current literature. J. Psychosom. Res. 2012, 73, 411–417. [Google Scholar] [PubMed]
- Chung, J.H.; Kim, S.H.; Lee, Y.W. Suicidal ideation and suicide attempts among asthma. Ann. Gen. Psychiatry 2016, 15, 35. [Google Scholar] [CrossRef] [PubMed]
- Tian, N.; Cui, W.; Zack, M.; Kobau, R.; Fowler, K.A.; Hesdorffer, D.C. Suicide among people with epilepsy: A population-based analysis of data from the U.S. National Violent Death Reporting System, 17 states, 2003–2011. Epilepsy Behav. 2016, 61, 210–217. [Google Scholar] [CrossRef] [PubMed]
- Tsigebrhan, R.; Hanlon, C.; Medhin, G.; Fekadu, A. Help seeking and suicidality among people with epilepsy in a rural low income country setting: Cross-sectional survey. Int. J. Ment. Health Syst. 2017, 11, 44. [Google Scholar] [PubMed]
- Simpson, G.K.; Tate, R.L. Preventing suicide after traumatic brain injury: Implications for general practice. Med. J. Aust. 2007, 187, 229–232. [Google Scholar] [PubMed]
- Khazaeipour, Z.; Taheri-Otaghsara, S.M.; Naghdi, M. Depression Following Spinal Cord Injury: Its Relationship to Demographic and Socioeconomic Indicators. Top. Spinal Cord Inj. Rehabil. 2015, 21, 149–155. [Google Scholar] [CrossRef] [PubMed]
- Eriksson, M.; Glader, E.L.; Norrving, B.; Asplund, K. Poststroke suicide attempts and completed suicides: A socioeconomic and nationwide perspective. Neurology 2015, 84, 1732–1738. [Google Scholar] [CrossRef] [PubMed]
- Backman, O.; Stockeld, D.; Rasmussen, F.; Naslund, E.; Marsk, R. Alcohol and substance abuse, depression and suicide attempts after Roux-en-Y gastric bypass surgery. Br. J. Surg. 2016, 103, 1336–1342. [Google Scholar] [CrossRef] [PubMed]
- Kovacs, Z.; Valentin, J.B.; Nielsen, R.E. Risk of psychiatric disorders, self-harm behaviour and service use associated with bariatric surgery. Acta Psychiat. Scand. 2016, 135, 149–158. [Google Scholar] [CrossRef] [PubMed]
- Tseng, M.C.; Cheng, I.C.; Hu, F.C. Standardized mortality ratio of inpatient suicide in a general hospital. J. Formos. Med. Assoc. 2011, 110, 267–269. [Google Scholar] [CrossRef]
- Pompili, M.; Innamorati, M.; Forte, A.; Long, L.; Mazzetta, C.; Erbuto, D.; Ricci, F.; Palermo, M.; Stefani, H.; Seretti, M.E. Insomnia as a predictor of high-lethality suicide attempts. Int. J. Clin. Pract. 2013, 67, 1311–1316. [Google Scholar] [CrossRef] [PubMed]
- Yip, P.S.F. (Ed.) Suicide in Asia: Causes and Prevention; Hong Kong University Press, HKU: Hong Kong, China, 2008; pp. 7–17. [Google Scholar]
- Fishbain, D.A.; Cutler, R.; Rosomoff, H.L.; Rosomoff, R.S. Chronic Pain-Associated Depression: Antecedent or Consequence of Chronic Pain? A Review. Clin. J. Pain 1997, 13, 116–137. [Google Scholar] [CrossRef] [PubMed]
- Harstall, C.; Ospina, M. How Prevalent Is Chronic Pain? Pain Clin. Updat. 2003, 11, 1–4. [Google Scholar]
- Tang, N.K.Y.; Crane, C. Suicidality in chronic pain: A review of the prevalence, risk factors and psychological links. Psychol. Med. 2006, 36, 575–586. [Google Scholar] [CrossRef] [PubMed]
- Campbell, G.; Darke, S.; Bruno, R.; Degenhardt, L. The prevalence and correlates of chronic pain and suicidality in a nationally representative sample. Aust. N. Z. J. Psychiatry 2015, 49, 803–811. [Google Scholar] [CrossRef] [PubMed]
- Ratcliffe, G.E.; Enns, M.W.; Belik, S.-L.; Sareen, J. Chronic Pain Conditions and Suicidal Ideation and Suicide Attempts: An Epidemiologic Perspective. Clin. J. Pain 2008, 24, 204–210. [Google Scholar] [CrossRef] [PubMed]
- Hegerl, U.; Mergl, R.; Havers, I.; Schmidtke, A.; Lehfeld, H.; Niklewski, G.; Althaus, D. Sustainable effects on suicidality were found for the Nuremberg alliance against depression. Eur. Arch. Psychiatry Clin. Neurosci. 2010, 260, 401–406. [Google Scholar] [CrossRef] [PubMed]
- Statistica. Deaths by Suicide Per 100,000 Resident Population in South Korea from 2012 to 2016. Available online: www.statista.com/statistics/789337/south-korea-suicide-death-rate/ (accessed on 4 July 2018).
- Statistica. Number of Suicides Per 100,000 Inhabitants in Japan from 2008 to 2017. Available online: www.statista.com/statistics/622249/japan-suicide-number-per-100-000-inhabitants (accessed on 4 July 2018).
- The MONSUE Consortium MOnitoring SUicidal Behaviour in Europe (MONSUE). Final Report on the Implementation of Action. Available online: https://kiedit.ki.se/sites/default/files/final_report_monsue.pdf (accessed on 22 November 2017).
- O’Carroll, P.W.; Silverman, M.M.; Berman, A.L. Community Suicide Prevention: The Effectiveness of Bridge Barriers. Suicide Life-Threat. Behav. 1994, 24, 89–99. [Google Scholar] [PubMed]
- Lubin, G.; Werbeloff, N.; Halperin, D.; Shmushkevitch, M.; Weiser, M.; Knobler, H.Y. Decrease in Suicide Rates After a Change of Policy Reducing Access to Firearms in Adolescents: A Naturalistic Epidemiological Study. Suicide Life-Threat. Behav. 2010, 40, 421–424. [Google Scholar] [CrossRef] [PubMed]
- Pearson, M.; Metcalfe, C.; Jayamanne, S.; Gunnell, D.; Weerasinghe, M.; Pieris, R.; Priyadarshana, C.; Knipe, D.W.; Hawton, K.; Dawson, A.H.; et al. Effectiveness of household lockable pesticide storage to reduce pesticide self-poisoning in rural Asia: A community-based, cluster-randomised controlled trial. Lancet 2017, 390, 1863–1872. [Google Scholar] [CrossRef]
- Niederkrotenthaler, T.; Fu, K.W.; Yip, P.S.; Fong, D.Y.; Stack, S.; Cheng, Q.; Pirkis, J. Changes in suicide rates following media reports on celebrity suicide: A meta-analysis. J. Epidemiol. Community Health 2012, 66, 1037–1042. [Google Scholar] [CrossRef] [PubMed]
- WHO Preventing Suicide: A Resource for Media Professionals. Available online: http://apps.who.int/iris/bitstream/10665/258814/1/WHO-MSD-MER-17.5-eng.pdf (accessed on 22 November 2017).
- Coveney, C.M.; Pollock, K.; Armstrong, S.; Moore, J. Callers’ experiences of contacting a national suicide prevention helpline. Crisis 2012, 33, 313–324. [Google Scholar] [CrossRef] [PubMed]
- Mishara, B.L.; Chagnon, F.; Daigle, M.; Balan, B.; Raymond, S.; Marcoux, I.; Bardon, C.; Campbell, J.K.; Berman, A. Comparing models of helper behavior to actual practice in telephone crisis intervention: A silent monitoring study of calls to the U.S. 1-800-SUICIDE Network. Suicide Life Threat. Behav. 2007, 37, 291–307. [Google Scholar] [CrossRef] [PubMed]
- Soubrier, J.P. Collaboration between psychiatrists and other physicians. In Suicide–An Unnecessary Death; Wasserman, D., Ed.; Martin Dunitz Ltd.: London, UK, 2001; pp. 231–236. [Google Scholar]
- WHO mhGAP Intervention Guide for Mental, Neurological and Substance Use Disorders in Non-Specialized Health Settings. Available online: http://whqlibdoc.who.int/publications/ (accessed on 20 November 2017).
- Pirkis, J.; Burgess, P. Suicide and recency of health care contacts. A systematic review. Br. J. Psychiatry 1998, 173, 462–474. [Google Scholar] [CrossRef] [PubMed]
- Luoma, J.B.; Martin, C.E.; Pearson, J.L. Contact with Mental Health and Primary Care Providers before Suicide: A Review of the Evidence. Am. J. Psychiatry 2002, 159, 909–916. [Google Scholar] [CrossRef] [PubMed]
- Rihmer, Z.; Rutz, W.; Barsi, J. Suicide rate, prevalence of diagnosed depression and prevalence of working physicians in Hungary. Acta Psychiatr. Scand. 1993, 88, 391–394. [Google Scholar] [CrossRef] [PubMed]
- Jagodič, H.K.; Rokavec, T.; Agius, M.; Pregelj, P. Availability of mental health service providers and suicide rates in Slovenia: A nationwide ecological study. Croat. Med. J. 2013, 54, 444–452. [Google Scholar] [CrossRef]
- Wang, D.W.L.; Colucci, E. Should compulsory admission to hospital be part of suicide prevention strategies? BJPsych Bull. 2017, 41, 169–171. [Google Scholar] [CrossRef] [PubMed]
- Ozawa-de Silva, C. Too lonely to die alone: Internet suicide pacts and existential suffering in Japan. Cult. Med. Psychiatry 2008, 32, 516–551. [Google Scholar] [CrossRef] [PubMed]
- Durkee, T.; Hadlaczky, G.; Westerlund, M.; Carli, V. Internet Pathways in Suicidality: A Review of the Evidence. Int. J. Environ. Res. Public Health 2011, 8, 3938–3952. [Google Scholar] [CrossRef] [PubMed]
- Lee, L.; Roser, M.; Ortiz-Ospina, E. Suicide. Available online: https://ourworldindata.org/suicide/ (accessed on 13 October 2017).
- WHO. Practice Manual for Establishing and Maintaining Surveillance Systems for Suicide Attempts and Self-Harm; World Health Organization: Geneva, Switzerland, 2016. [Google Scholar]
- De Leo, D.; Cimitan, A.; Dyregrov, K.; Grad, O.; Andriessen, K. Bereavement after Traumatic Death—Helping the Survivors; Hogrefe Publishing: Boston, MA, USA, 2014. [Google Scholar]
- WHO. WHO Methods and Data Sources for Country-Level Causes of Death 2000–2015; Global Health Estimates Technical Paper WHO/HIS/IER/GHE/2016.3; World Health Organization: Geneva, Switzerland, 2017; p. 56. [Google Scholar]
- WHO ICD-10, International Statistical Classification of Diseases and Related Health Problems 10th Revision. Available online: http://apps.who.int/classifications/icd10/browse/2016/en (accessed on 15 November 2017).
- WHO Figure: Quality of Suicide Mortality Data. Available online: http://www.who.int/mental_health/suicide-prevention/mortality_data_quality/en/ (accessed on 10 October 2017).
© 2018 by the author. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Bachmann, S. Epidemiology of Suicide and the Psychiatric Perspective. Int. J. Environ. Res. Public Health 2018, 15, 1425. https://doi.org/10.3390/ijerph15071425
Bachmann S. Epidemiology of Suicide and the Psychiatric Perspective. International Journal of Environmental Research and Public Health. 2018; 15(7):1425. https://doi.org/10.3390/ijerph15071425
Chicago/Turabian StyleBachmann, Silke. 2018. "Epidemiology of Suicide and the Psychiatric Perspective" International Journal of Environmental Research and Public Health 15, no. 7: 1425. https://doi.org/10.3390/ijerph15071425
APA StyleBachmann, S. (2018). Epidemiology of Suicide and the Psychiatric Perspective. International Journal of Environmental Research and Public Health, 15(7), 1425. https://doi.org/10.3390/ijerph15071425



