Residential Ambient Traffic in Relation to Childhood Pneumonia among Urban Children in Shandong, China: A Cross-Sectional Study
Abstract
1. Background
2. Methods
2.1. Studied Population and Questionnaire
2.2. Assessment of Residential Traffic
- q1. Whether the residence close to main traffic road (yes vs. no)?
- q1a. If q1 is yes, how far linear distance (m) between residence and main traffic road?
- q1b. If q1 is yes, how many lane counts of the main traffic road near residence?
- q1c. If q1 is yes, whether heavy truck passes through the main traffic road near residence?
- q1d. If q1 is yes, whether bedroom faces to the main road near residence?
- q2. Whether the residence close to filling station (yes vs. no)?
- q2a. If q2 is yes, how far linear distance (m) between residence and filling station?
- q3. Whether the residence close to automobile 4S shop (yes vs. no)?
- q3a. If q3 is yes, how far linear distance (m) between residence and automobile 4S shop?
- q4. Whether ground car park exists in the residential community (yes vs. no)?
- q4a. If q4 is yes, how many cars are parked in the ground car park per day averagely?
2.3. Assessment of Childhood Pneumonia
2.4. Covariates and Statistical Analyses
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Availability of Data and Materials
References
- GBD 2015 LRI Collaborators. Estimates of the global, regional, and national morbidity, mortality, and aetiologies of lower respiratory tract infections in 195 countries: A systematic analysis for the Global Burden of Disease Study 2015. Lancet Infect. Dis. 2017, 17, 1133–1161. [Google Scholar]
- Walker, C.L.; Rudan, I.; Liu, L.; Nair, H.; Theodoratou, E.; Bhutta, Z.A.; O’Brien, K.L.; Campbell, H.; Black, R.E. Global burden of childhood pneumonia and diarrhoea. Lancet 2013, 381, 1405–1416. [Google Scholar] [CrossRef]
- Brauer, M.; Freedman, G.; Frostad, J.; van Donkelaar, A.; Martin, R.V.; Dentener, F.; van Dingenen, R.; Estep, K.; Amini, H.; Apte, J.S.; et al. Ambient air pollution exposure estimation for the Global Burden of Disease 2013. Environ. Sci. Technol. 2016, 50, 79–88. [Google Scholar] [CrossRef] [PubMed]
- Aguilera, I.; Pedersen, M.; Garcia-Esteban, R.; Ballester, F.; Basterrechea, M.; Esplugues, A.; Fernández-Somoano, A.; Lertxundi, A.; Tardón, A.; Sunyer, J. Early-life exposure to outdoor air pollution and respiratory health, ear infections, and eczema in infants from the INMA study. Environ. Health Perspect. 2013, 121, 387–392. [Google Scholar] [CrossRef] [PubMed]
- Fuertes, E.; MacIntyre, E.; Agius, R.; Beelen, R.; Brunekreef, B.; Bucci, S.; Cesaroni, G.; Cirach, M.; Cyrys, J.; Forastiere, F.; et al. Associations between particulate matter elements and early-life pneumonia in seven birth cohorts: Results from the ESCAPE and TRANSPHORM projects. Int. J. Hyg. Environ. Health 2004, 217, 819–829. [Google Scholar] [CrossRef] [PubMed]
- Lipfert, F.W. A critical review of the ESCAPE project for estimating long-term health effects of air pollution. Environ. Int. 2017, 99, 87–96. [Google Scholar] [CrossRef] [PubMed]
- MacIntyre, E.A.; Gehring, U.; Mölter, A.; Fuertes, E.; Klümper, C.; Krämer, U.; Quass, U.; Hoffmann, B.; Gascon, M.; Brunekreef, B.; et al. Air pollution and respiratory infections during early childhood: An analysis of 10 European birth cohorts within the ESCAPE project. Environ. Health Perspect. 2014, 122, 107–113. [Google Scholar] [CrossRef] [PubMed]
- Mehta, S.; Shin, H.; Burnett, R.; North, T.; Cohen, A.J. Ambient particulate air pollution and acute lower respiratory infections: A systematic review and implications for estimating the global burden of disease. Air Qual. Atmos. Health 2013, 6, 69–83. [Google Scholar] [CrossRef] [PubMed]
- Nhung, N.T.T.; Amini, H.; Schindler, C.; Kutlar Joss, M.; Dien, T.M.; Probst-Hensch, N.; Perez, L.; Künzli, N. Short-term association between ambient air pollution and pneumonia in children: A systematic review and meta-analysis of time-series and case-crossover studies. Environ. Pollut. 2017, 230, 1000–1008. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Z.; Hong, Y.; Liu, N. Association of ambient Particulate matter 2.5 with intensive care unit admission due to pneumonia: A distributed lag non-linear model. Sci. Rep. 2017, 7, 8679. [Google Scholar] [CrossRef] [PubMed]
- Brauer, M.; Hoek, G.; Van Vliet, P.; Meliefste, K.; Fischer, P.H.; Wijga, A.; Koopman, L.P.; Neijens, H.J.; Gerritsen, J.; Kerkhof, M.; et al. Air pollution from traffic and the development of respiratory infections and asthmatic and allergic symptoms in children. Am. J. Respir. Crit. Care Med. 2002, 166, 1092–1098. [Google Scholar] [CrossRef] [PubMed]
- Brunekreef, B.; Janssen, N.A.; de Hartog, J.; Harssema, H.; Knape, M.; van Vliet, P. Air pollution from truck traffic and lung function in children living near motorways. Epidemiology 1997, 8, 298–303. [Google Scholar] [CrossRef] [PubMed]
- Brunekreef, B.; Stewart, A.W.; Anderson, H.R.; Lai, C.K.; Strachan, D.P.; Pearce, N.; the ISAAC Phase 3 Study Group. Self-reported truck traffic on the street of residence and symptoms of asthma and allergic disease: A global relationship in ISAAC phase 3. Environ. Health Perspect. 2009, 117, 1791–1798. [Google Scholar] [CrossRef] [PubMed]
- Eckel, S.P.; Berhane, K.; Salam, M.T.; Rappaport, E.B.; Linn, W.S.; Bastain, T.M.; Zhang, Y.; Lurmann, F.; Avol, E.L.; Gilliland, F.D. Residential traffic-related pollution exposures and exhaled nitric oxide in the children’s health study. Environ. Health Perspect. 2011, 119, 1472–1477. [Google Scholar] [CrossRef] [PubMed]
- El-Zein, A.; Nuwayhid, I.; El-Fadel, M.; Mroueh, S. Did a ban on diesel-fuel reduce emergency respiratory admissions for children? Sci. Total Environ. 2007, 384, 134–140. [Google Scholar] [CrossRef] [PubMed]
- Gauderman, W.J.; Vora, H.; McConnell, R.; Berhane, K.; Gilliland, F.; Thomas, D.; et al. Effect of exposure to traffic on lung development from 10 to 18 years of age: A cohort study. Lancet 2007, 369, 571–577. [Google Scholar] [CrossRef]
- Gonzalez-Barcala, F.J.; Pertega, S.; Garnelo, L.; Castro, T.P.; Sampedro, M.; Lastres, J.S.; Gonzalez, M.A.; Bamonde, L.; Valdes, L.; Carreira, J.M.; et al. Truck traffic related air pollution associated with asthma symptoms in young boys: A cross-sectional study. Public Health 2013, 127, 275–281. [Google Scholar] [CrossRef] [PubMed]
- Hu, Y.; Liu, W.; Huang, C.; Zou, Z.J.; Zhao, Z.H.; Shen, L.; Sundell, J. Home dampness, childhood asthma, hay fever, and airway symptoms in Shanghai, China: Associations, dose-response relationships, and lifestyle’s influences. Indoor Air 2014, 24, 450–463. [Google Scholar] [CrossRef] [PubMed]
- Kim, J.J.; Huen, K.; Adams, S.; Smorodinsky, S.; Hoats, A.; Malig, B.; Lipsett, M.; Ostro, B. Residential Traffic and Children’s Respiratory Health. Environ. Health Perspect. 2008, 116, 1274–1279. [Google Scholar] [CrossRef] [PubMed]
- McConnell, R.; Islam, T.; Shankardass, K.; Jerrett, M.; Lurmann, F.; Gilliland, F.; Gauderman, J.; Avol, E.; Künzli, N.; Yao, L.; et al. Childhood incident asthma and traffic-related air pollution at home and school. Environ. Health Perspect. 2010, 118, 1021–1026. [Google Scholar] [CrossRef] [PubMed]
- Wilhelm, M.; Meng, Y.Y.; Rull, R.P.; English, P.; Balmes, J.; Ritz, B. Environmental public health tracking of childhood asthma using California health interview survey, traffic, and outdoor air pollution data. Environ. Health Perspect. 2008, 116, 1254–1260. [Google Scholar] [CrossRef] [PubMed]
- Chen, F.; Lin, Z.; Chen, R.; Norback, D.; Liu, C.; Kan, H.; Deng, Q.; Huang, C.; Hu, Y.; Zou, Z.; et al. The effects of PM2.5 on asthmatic and allergic diseases or symptoms in preschool children of six Chinese cities, based on China, Children, Homes and Health (CCHH) project. Environ. Pollut. 2018, 232, 329–337. [Google Scholar] [CrossRef] [PubMed]
- Gao, J.; Woodward, A.; Vardoulakis, S.; Kovats, S.; Wilkinson, P.; Li, L.; Xu, L.; Li, J.; Yang, J.; Li, J.; et al. Haze, public health and mitigation measures in China: A review of the current evidence for further policy response. Sci. Total Environ. 2017, 578, 148–157. [Google Scholar] [CrossRef] [PubMed]
- Kan, H.; Chen, R.; Tong, S. Ambient air pollution, climate change, and population health in China. Environ. Int. 2012, 42, 10–19. [Google Scholar] [CrossRef] [PubMed]
- Khreis, H.; Kelly, C.; Tate, J.; Parslow, R.; Lucas, K.; Nieuwenhuijsen, M. Exposure to traffic-related air pollution and risk of development of childhood asthma: A systematic review and meta-analysis. Environ. Int. 2017, 100, 1–31. [Google Scholar] [CrossRef] [PubMed]
- Liu, W.; Huang, C.; Hu, Y.; Fu, Q.; Zou, Z.; Sun, C.; Shen, L.; Wang, X.; Cai, J.; Pan, J.; et al. Associations of gestational and early life exposures to ambient air pollution with childhood respiratory diseases in Shanghai, China: A retrospective cohort study. Environ. Int. 2016, 92, 284–293. [Google Scholar] [CrossRef] [PubMed]
- Lu, C.; Deng, Q.; Yu, C.; Sundell, J.; Ou, C. Effects of ambient air pollution on the prevalence of pneumonia in children: Implication for national ambient air quality standards in China. Indoor Built. Environ. 2014, 23, 259–269. [Google Scholar] [CrossRef]
- Lv, C.; Wang, X.; Pang, N.; Wang, L.; Wang, Y.; Xu, T.; Zhang, X.; Zhou, T.; Li, W. The impact of airborne particulate matter on pediatric hospital admissions for pneumonia among children in Jinan, China: A case-crossover study. J. Air Waste Manag. Assoc. 2017, 67, 669–676. [Google Scholar] [CrossRef] [PubMed]
- Tao, Y.; Mi, S.; Zhou, S.; Wang, S.; Xie, X. Air pollution and hospital admissions for respiratory diseases in Lanzhou, China. Environ. Pollut. 2014, 185, 196–201. [Google Scholar] [CrossRef] [PubMed]
- Wu, Y.; Zhang, S.; Hao, J.; Liu, H.; Wu, X.; Hu, J.; Walsh, M.P.; Wallington, T.J.; Zhang, K.M.; Stevanovic, S. On-road vehicle emissions and their control in China: A review and outlook. Sci. Total Environ. 2017, 574, 332–349. [Google Scholar] [CrossRef] [PubMed]
- Zhao, Y.; Wang, S.; Lang, L.; Huang, C.; Ma, W.; Lin, H. Ambient fine and coarse particulate matter pollution and respiratory morbidity in Dongguan, China. Environ. Pollut. 2017, 222, 126–131. [Google Scholar] [CrossRef] [PubMed]
- Fan, X.J.; Yang, C.; Zhang, L.; Fan, Q.; Li, T.; Bai, X.; Zhao, Z.H.; Zhang, X.; Norback, D. Asthma symptoms among Chinese children: The role of ventilation and PM10 exposure at school and home. Int. J. Tuberc. Lung Dis. 2017, 21, 1187–1193. [Google Scholar] [CrossRef] [PubMed]
- Sundell, J.; Levin, H.; Nazaroff, W.W.; Cain, W.S.; Fisk, W.J.; Grimsrud, D.T.; Gyntelberg, F.; Li, Y.; Persily, A.K.; Pickering, A.C.; et al. Ventilation rates and health: Multidisciplinary review of the scientific literature. Indoor Air 2011, 21, 191–204. [Google Scholar] [CrossRef] [PubMed]
- Wang, X.; Liu, W.; Hu, Y.; Zou, Z.; Shen, L.; Huang, C. Home environment, lifestyles behaviors, and rhinitis in childhood. Int. J. Hyg. Environ. Health 2016, 219, 220–231. [Google Scholar] [CrossRef] [PubMed]
- Holst, G.J.; Høst, A.; Doekes, G.; Meyer, H.W.; Madsen, A.M.; Plesner, K.B.; Sigsgaard, T. Allergy and respiratory health effects of dampness and dampness-related agents in schools and homes: A cross-sectional study in Danish pupils. Indoor Air 2016, 26, 880–891. [Google Scholar] [CrossRef] [PubMed]
- Zheng, X.H.; Qian, H.; Zhao, Y.L.; Shen, H.P.; Zhao, Z.H.; Sun, Y.X.; Sundell, J. Home risk factors for childhood pneumonia in Nanjing, China. Chin. Sci. Bull. 2013, 58, 4230–4236. [Google Scholar] [CrossRef]
- Liu, W.; Huang, C.; Hu, Y.; Zou, Z.J.; Sundell, J. Associations between indoor environmental smoke and respiratory symptoms among preschool children in Shanghai, China. Chin. Sci. Bull. 2013, 58, 4211–4216. [Google Scholar] [CrossRef]
- Clougherty, J.E. A growing role for gender analysis in air pollution epidemiology. Environ. Health Perspect. 2010, 118, 167–176. [Google Scholar] [CrossRef] [PubMed]
- Dong, G.H.; Chen, T.; Liu, M.M.; Wang, D.; Ma, Y.N.; Ren, W.H.; Lee, Y.L.; Zhao, Y.D.; He, Q.C. Gender differences and effect of air pollution on asthma in children with and without allergic predisposition: Northeast Chinese children health study. PLoS ONE 2011, 6, e22470. [Google Scholar] [CrossRef] [PubMed]
- Spencer-Hwang, R.; Soret, S.; Ghamsary, M.; Rizzo, N.; Baum, M.; Juma, D.; Montgomery, B. Gender differences in respiratory health of school children exposed to rail yard-generated air pollution: The ENRRICH study. J. Environ. Health 2016, 78, 8–16. [Google Scholar] [PubMed]
- Chang, J.; Liu, W.; Hu, Y.; Zou, Z.; Shen, L.; Wang, X.; Cai, J.; Sun, C.; Huang, C. Associations between heavy traffic near residence and childhood health outcomes as modified by bedroom floor level and bedroom ventilation. Build. Environ. 2017, 114, 56–67. [Google Scholar] [CrossRef]
- Zhou, J.; Zhao, Q.; Zhang, X.; Chen, M. Preliminary investigation on distribution trend of inhalable particles in indoor air at different floors of a building. J. Environ. Hyg. 2017, 7, 348–350. (In Chinese) [Google Scholar]
- Zhang, Y.P.; Li, B.Z.; Huang, C.; Yang, X.; Qian, H.; Deng, Q.H.; Zhao, Z.H.; Li, A.G.; Zhao, J.N.; Zhang, X.; et al. Ten cities cross-sectional questionnaire survey of children asthma and other allergies in China. Chin. Sci. Bull. 2013, 58, 4182–4189. [Google Scholar] [CrossRef]
- Asher, M.I.; Keil, U.; Anderson, H.R.; Beasley, R.; Crane, J.; Martinez, F.; Mitchell, E.A.; Pearce, N.; Sibbald, B.; Stewart, A.W.; et al. International study of asthma and allergies in childhood (ISAAC): Rationale and methods. Eur. Respir. J. 1995, 8, 483–491. [Google Scholar] [CrossRef] [PubMed]
- Bornehag, C.G.; Sundell, J.; Sigsgaard, T. Dampness in buildings and health (DBH): Report from an ongoing epidemiological investigation on the association between indoor environmental factors and health effects among children in Sweden. Indoor Air 2004, 14, 59–66. [Google Scholar] [CrossRef] [PubMed]
- Wang, L.; Qu, F.; Zhang, Y.; Weschler, L.B.; Sundell, J. Home environment in relation to allergic rhinitis among preschool children in Beijing, China: A cross-sectional study. Build. Environ. 2015, 93, 54–63. [Google Scholar] [CrossRef]
- Ministry of Construction of the People’s Republic of China. Code for Design of Civil Building (GB50352-2005); Ministry of Construction of the People’s Republic of China: Beijing, China, 2005; p. 6. (In Chinese)
- Dales, R.; Wheeler, A.; Mahmud, M.; Frescura, A.M.; Smith-Doiron, M.; Nethery, E.; Liu, L. The influence of living near roadways on spirometry and exhaled nitric oxide in elementary schoolchildren. Environ. Health Perspect. 2008, 116, 1423–1427. [Google Scholar] [CrossRef] [PubMed]
- Hu, Z.; Zhao, Y.N.; Cheng, Y.; Guo, C.Y.; Wang, X.; Li, N.; Liu, J.Q.; Kang, H.; Xia, G.G.; Hu, P.; et al. Living near a major road in Beijing: Association with lower ling function, airway acidification, and chronic cough. Chin. Med, J. 2016, 129, 2l84–2190. [Google Scholar]
- Brown, M.S.; Sarnat, S.E.; DeMuth, K.A.; Brown, L.A.; Whitlock, D.R.; Brown, S.W.; Tolbert, P.E.; Fitzpatrick, A.M. Residential proximity to a major roadway is associated with features of asthma control in children. PLoS ONE 2012, 7, e37044. [Google Scholar] [CrossRef] [PubMed]
- Perez, L.; Lurmann, F.; Wilson, J.; Pastor, M.; Brandt, S.J.; Künzli, N.; McConnell, R. Near-roadway pollution and childhood asthma: Implications for developing “win-win” compact urban development and clean vehicle strategies. Environ. Health Perspect. 2012, 120, 1619–1626. [Google Scholar] [CrossRef] [PubMed]
- Ryan, P.H.; LeMasters, G.; Biagini, J.; Bernstein, D.; Grinshpun, S.A.; Shukla, R.; Wilson, K.; Villareal, M.; Burkle, J.; Lockey, J. Is it traffic type, volume, or distance? Wheezing in infants living near truck and bus traffic. J. Allergy Clin. Immunol. 2005, 116, 279–284. [Google Scholar] [CrossRef] [PubMed]
- Shirinde, J.; Wichmann, J.; Voyi, K. Allergic rhinitis, rhinoconjunctivitis and hay fever symptoms among children are associated with frequency of truck traffic near residences: A cross sectional study. Environ. Health 2015, 14, 84. [Google Scholar] [CrossRef] [PubMed]
- Jung, K.H.; Bernabé, K.; Moors, K.; Yan, B.; Chillrud, S.N.; Whyatt, R.; Camann, D.; Kinney, P.L.; Perera, F.P.; Miller, R.L. Effects of floor level and building type on residential levels of outdoor and indoor polycyclic aromatic hydrocarbons, black carbon, and particulate matter in New York City. Atmosphere 2011, 2, 96–109. [Google Scholar] [CrossRef] [PubMed]
- Yang, F.; Kang, Y.; Gao, Y.; Zhong, K. Numerical simulations of the effect of outdoor pollutants on indoor air quality of buildings next to a street canyon. Build. Environ. 2015, 87, 10–22. [Google Scholar] [CrossRef]
- Zhang, Y.; Kwok, K.C.; Liu, X.P.; Niu, J.L. Characteristics of air pollutant dispersion around a high-rise building. Environ. Pollut. 2015, 204, 280–288. [Google Scholar] [CrossRef] [PubMed]
- Zhao, Z.; Zhang, Z.; Wang, Z.; Ferm, M.; Liang, Y.; Norbäck, D. Asthmatic symptoms among pupils in relation to winter indoor and outdoor air pollution in schools in Taiyuan, China. Environ. Health Perspect. 2008, 116, 90–97. [Google Scholar] [CrossRef] [PubMed]
- Sun, Y.X.; Sundell, J. On associations between housing characteristics, dampness and asthma and allergies among children in Northeast Texas. Indoor Built. Environ. 2013, 22, 678–684. [Google Scholar] [CrossRef]
- Cai, J.; Liu, W.; Huang, C.; Wang, X.; Shen, L.; Zou, Z.; Hu, Y.; Sun, C.; Wei, X.; Chang, J.; et al. Validity of subjective questionnaire in evaluating dwelling characteristics, home dampness, and indoor odors in Shanghai, China: Cross-sectional survey and on-site inspection. Energy Build. 2016, 127, 1019–1027. [Google Scholar] [CrossRef]
- Hagerhed-Engman, L.; Bornehag, C.G.; Sundell, J. How valid are parents’ questionnaire responses regarding building characteristics, mouldy odour, and signs of moisture problems in Swedish homes? Scand. J. Public Health 2007, 35, 125–132. [Google Scholar] [CrossRef] [PubMed]

| Items | Sample Size, n (%) a |
|---|---|
| Total | 5640 (100.0) |
| Sex | |
| Boys | 2906 (52.3) |
| Girls | 2650 (47.7) |
| Age | |
| 3-year-olds | 945 (16.9) |
| 4-year-olds | 1862 (33.2) |
| 5-year-olds | 1866 (33.3) |
| 6-year-olds | 931 (16.6) |
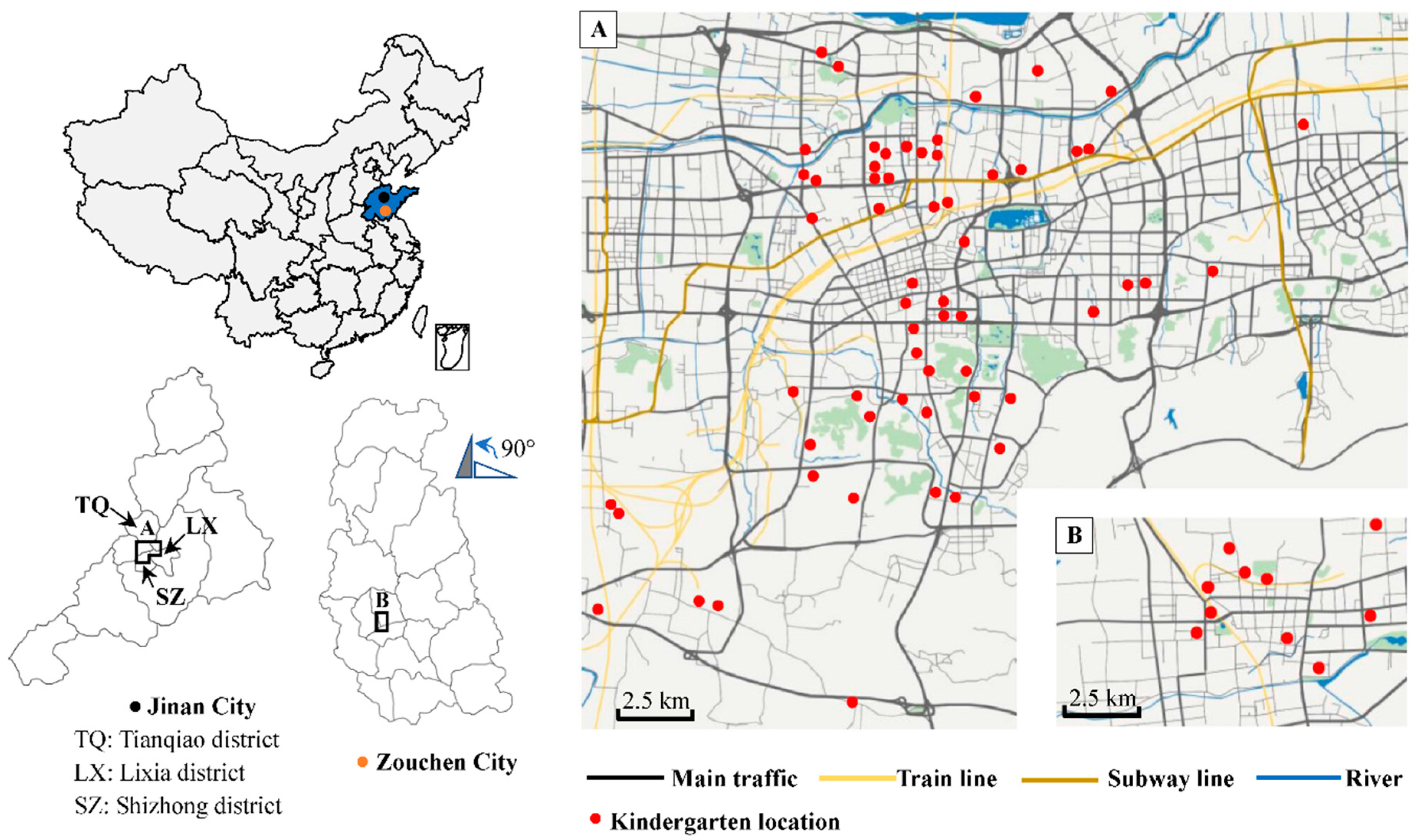
| Residence-located area | |
| Tianqiao district | 1724 (30.6) |
| Shizhong district | 1688 (29.9) |
| Lixia district | 896 (15.9) |
| Zouchen city | 1332 (23.6) |
| Family history of atopy | |
| Yes | 524 (9.4) |
| No | 5076 (90.6) |
| Residence ownership | |
| Owner | 3971 (72.2) |
| Renter | 1532 (27.8) |
| Breastfeeding duration | |
| ≤6 months | 1057 (19.1) |
| >6 months | 4472 (80.9) |
| Household dampness-related exposure | |
| Yes | 4515 (81.2) |
| No | 1047 (18.8) |
| Household environmental tobacco smoke (ETS) | |
| Yes | 2892 (52.0) |
| No | 2670 (48.0) |
| Household renovation during early lifetime | |
| Yes | 1703 (31.8) |
| No | 3646 (68.2) |
| The child’s bedroom floor level | |
| 1st–3rd floors | 2723 (50.9) |
| 4th–6th floors | 2040 (38.1) |
| ≥7th floors | 586 (11.0) |
| Frequency of opening bedroom windows during night | |
| Often | 3950 (71.7) |
| Not often | 1559 (28.3) |
| Pneumonia prevalence | |
| Yes | 1429 (25.9) |
| No | 4092 (74.1) |
| Indictors for Residential Traffic | Sample Size, n (%) | Prevalence, n (%) | p-Value a |
|---|---|---|---|
| Main traffic road near residence within 200 m | |||
| Yes | 2225 (40.6) | 630 (29.0) | |
| No | 3259 (59.4) | 762 (23.9) | <0.001 |
| Linear distance between residence and the main traffic road | |||
| ≤50 m | 669 (13.5) | 186 (28.6) | |
| 51–100 m | 475 (9.6) | 139 (29.6) | |
| 101–200 m | 555 (11.2) | 149 (27.2) | |
| >200 m | 3259 (65.7) | 762 (23.9) | 0.005 |
| Lane counts of the main traffic road near residence within 200 m | |||
| ≤2 lanes | 499 (31.3) | 123 (25.5) | |
| 3–5 lanes | 662 (41.5) | 197 (30.2) | |
| ≥6 lanes | 434 (27.2) | 134 (31.4) | 0.109 |
| Heavy truck passed through the main traffic road near residence within 200 m | |||
| Yes | 827 (50.0) | 222 (27.3) | |
| No | 828 (50.0) | 235 (29.0) | 0.445 |
| Bedroom faced to the main traffic road near residence within 200 m | |||
| Yes | 802 (47.7) | 221 (28.3) | |
| No | 879 (52.3) | 249 (28.7) | 0.874 |
| Filling station near residence within 200 m | |||
| Yes | 234 (4.1) | 71 (30.7) | |
| No | 5189 (95.7) | 1302 (25.6) | 0.081 |
| Linear distance between residence and the filling station | |||
| ≤100 m | 105 (1.9) | 41 (39.0) | |
| 101–200 m | 129 (2.4) | 30 (23.8) | |
| >200 m | 5189 (95.7) | 1302 (25.6) | 0.007 |
| Automobile 4S shop near residence within 200 m | |||
| Yes | 117 (2.1) | 41 (35.3) | |
| No | 5327 (97.9) | 1338 (25.6) | 0.018 |
| Linear distance between residence and the automobile 4S shop | |||
| ≤100 m | 72 (1.3) | 26 (36.6) | |
| 101–200 m | 45 (0.8) | 15 (33.3) | |
| >200 m | 5327 (97.9) | 1338 (25.6) | 0.056 |
| Ground car park in the residential community | |||
| Yes | 3234 (59.8) | 909 (28.6) | |
| No | 2175 (40.2) | 467 (21.9) | <0.001 |
| Average number of cars parked in the ground car park per day | |||
| ≤20 | 1014 (36.2) | 251 (25.2) | |
| 21–50 | 795 (28.4) | 233 (29.7) | |
| 51–100 | 532 (19.0) | 159 (30.2) | |
| >100 | 459 (16.4) | 151 (34.0) | 0.004 |
| Indictors for Residential Traffic | OR, 95%CI (p-Value) a | ||
|---|---|---|---|
| Crude | Adjusted Model 1 b | Adjusted Model 2 c | |
| Main traffic road near residence within 200 m | |||
| No | 1.00 | 1.00 | 1.00 |
| Yes | 1.30, 1.15–1.47 (<0.001) | 1.23, 1.08–1.40 (0.002) | 1.21, 1.05–1.38 (0.007) |
| Linear distance between residence and the main traffic road | |||
| >200 m | 1.00 | 1.00 | 1.00 |
| 101–200 m | 1.20, 0.97–1.47 (0.089) | 1.13, 0.91–1.41 (0.277) | 1.09, 0.87–1.37 (0.452) |
| 51–100 m | 1.34, 1.09–1.67 (0.007) | 1.33, 1.06–1.68 (0.013) | 1.30, 1.03–1.64 (0.030) |
| ≤50 m | 1.28, 1.06–1.55 (0.010) | 1.16, 0.94–1.42 (0.163) | 1.10, 0.90–1.36 (0.355) |
| Lane counts of the main traffic road near residence within 200 m | |||
| ≤2 lanes | 1.00 | 1.00 | 1.00 |
| 3–5 lanes | 1.26, 0.97–1.64 (0.085) | 1.24, 0.93–1.66 (0.144) | 1.24, 0.92–1.68 (0.156) |
| ≥6 lanes | 1.34, 1.00–1.78 (0.050) | 1.32, 0.96–1.82 (0.087) | 1.40, 1.01–1.94 (0.045) |
| Heavy truck passed through the main traffic road near residence within 200 m | |||
| No | 1.00 | 1.00 | 1.00 |
| Yes | 0.92, 0.74–1.14 (0.445) | 0.79, 0.63–1.01 (0.053) | 0.83, 0.65–1.06 (0.135) |
| Bedroom faced to the main traffic road near residence within 200 m | |||
| No | 1.00 | 1.00 | 1.00 |
| Yes | 0.98, 0.79–1.22 (0.874) | 1.02, 0.81–1.28 (0.863) | 1.02, 0.81–1.29 (0.840) |
| Filling station near residence within 200 m | |||
| No | 1.00 | 1.00 | 1.00 |
| Yes | 1.29, 0.97–1.72 (0.081) | 1.22, 0.89–1.66 (0.222) | 1.17, 0.85–1.61 (0.338) |
| Linear distance between residence and the filling station | |||
| >200 m | 1.00 | 1.00 | 1.00 |
| 101–200 m | 0.91, 0.60–1.38 (0.648) | 0.89, 0.57–1.39 (0.615) | 0.87, 0.56–1.38 (0.567) |
| ≤100 m | 1.86, 1.25–2.77 (0.002) | 1.71, 1.10–2.65 (0.017) | 1.60, 1.02–2.52 (0.039) |
| Automobile 4S shop near residence within 200 m | |||
| No | 1.00 | 1.00 | 1.00 |
| Yes | 1.59, 1.08–2.33 (0.018) | 1.76, 1.16–2.67 (0.008) | 1.43, 0.94–2.20 (0.098) |
| Linear distance between residence and the automobile 4S shop | |||
| >200 m | 1.00 | 1.00 | 1.00 |
| 101–200 m | 1.45, 0.78–2.71 (0.238) | 1.80, 0.92–3.50 (0.086) | 1.52, 0.77–2.99 (0.223) |
| ≤100 m | 1.68, 1.03–2.73 (0.035) | 1.74, 1.03–2.95 (0.039) | 1.37, 0.80–2.35 (0.252) |
| Ground car park in the residential community | |||
| No | 1.00 | 1.00 | 1.00 |
| Yes | 1.43, 1.26–1.62 (<0.001) | 1.24, 1.08–1.42 (0.002) | 1.20, 1.04–1.39 (0.014) |
| Average number of car parked in the ground car park per day | |||
| ≤20 | 1.00 | 1.00 | 1.00 |
| 21–50 | 1.26, 1.02–1.55 (0.034) | 1.21, 0.96–1.52 (0.100) | 1.24, 0.98–1.56 (0.075) |
| 51–100 | 1.29, 1.02–1.63 (0.035) | 1.21, 0.94–1.56 (0.146) | 1.25, 0.97–1.63 (0.088) |
| >100 | 1.53, 1.20–1.95 (0.001) | 1.41, 1.08–1.84 (0.011) | 1.49, 1.13–1.95 (0.004) |
| Indictors for Residential Traffic | OR, 95%CI (p-Value) [p-Value for Interaction] a | ||
|---|---|---|---|
| Crude | Adjusted Model 1 b | Adjusted Model 2 c | |
| 1. Main traffic road near residence within 200 m (yes vs. no) | |||
| Stratified by the child’s sex | |||
| Boys | 1.42, 1.19–1.71 (<0.001) | 1.32, 1.09–1.60 (0.005) | 1.27, 1.04–1.55 (0.018) |
| Girls | 1.18, 1.00–1.40 (0.055) [0.009] | 1.15, 0.96–1.38 (0.124) [0.035] | 1.14, 0.94–1.37 (0.176) [0.058] |
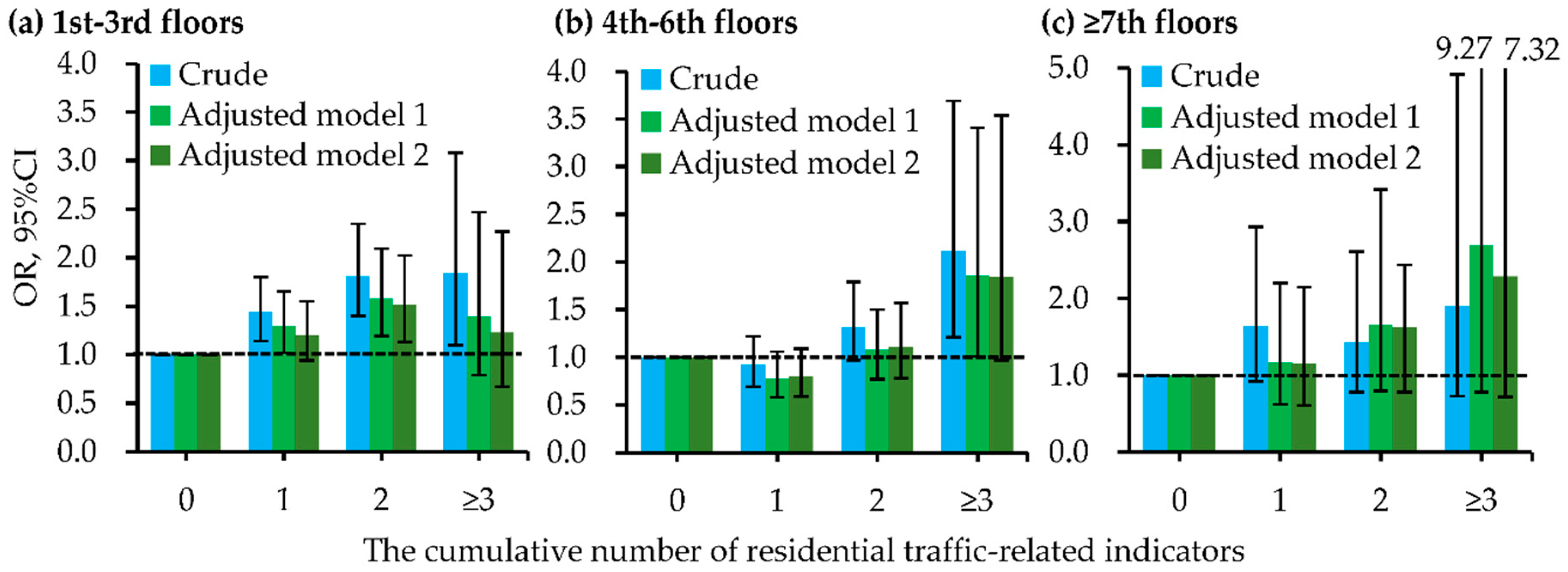
| Stratified by bedroom floor level | |||
| 1st–3rd floors | 1.37, 1.14–1.63 (0.001) | 1.29, 1.06–1.56 (0.010) | 1.27, 1.04–1.54 (0.019) |
| 4th–6th floors | 1.24, 1.01–1.52 (0.039) | 1.18, 0.95–1.47 (0.130) | 1.15, 0.92–1.43 (0.228) |
| ≥7th floors | 1.14, 0.79–1.63 (0.494) [0.015] | 1.09, 0.73–1.61 (0.681) [0.124] | 1.08, 0.73–1.60 (0.683) [0.197] |
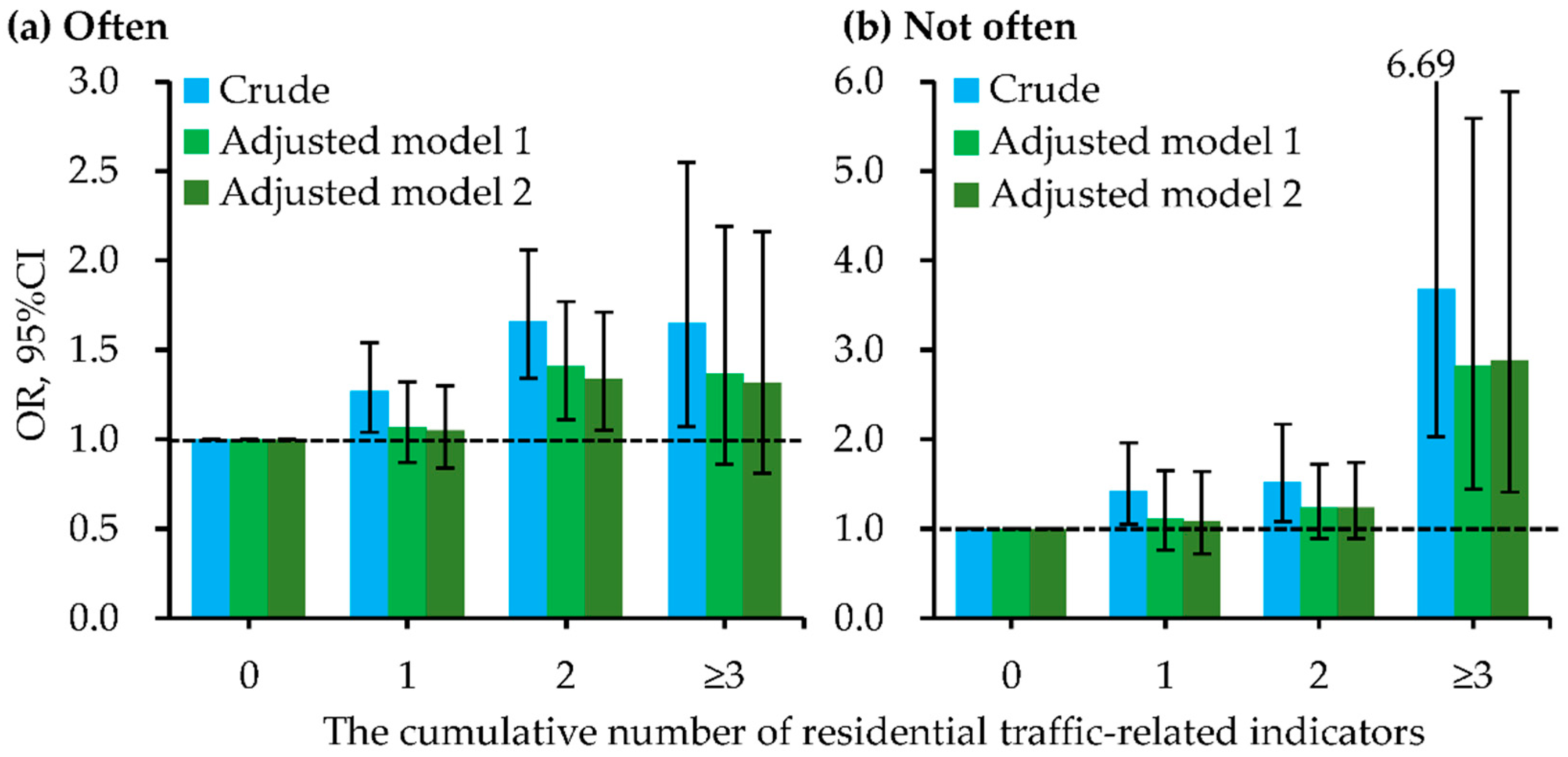
| Stratified by bedroom ventilation habit (open the bedroom windows during night) | |||
| Often | 1.26, 1.01–1.59 (0.047) | 1.16, 0.90–1.49 (0.257) | 1.22, 0.93–1.61 (0.142) |
| Not often | 1.29, 1.11–1.49 (0.001) [0.012] | 1.23, 1.05–1.44 (0.011) [0.013] | 1.21, 1.03–1.42 (0.022) [0.083] |
| 2. Filling station near residence within 200 m (yes vs. no) | |||
| Stratified by the child’s sex | |||
| Boys | 1.41, 0.96–2.06 (0.078) | 1.42, 0.95–2.14 (0.087) | 1.37, 0.90–2.08 (0.137) |
| Girls | 1.08, 0.69–1.70 (0.724) [0.049] | 0.98, 0.60–1.61 (0.928) [0.082] | 0.96, 0.58–1.60 (0.885) [0.093] |
| Stratified by bedroom floor level | |||
| 1st–3rd floors | 1.17, 0.76–1.81 (0.472) | 1.05, 0.65–1.69 (0.848) | 0.93, 0.57–1.51 (0.758) |
| 4th–6th floors | 1.18, 0.74–1.87 (0.483) | 1.23, 0.75–2.02 (0.422) | 1.21, 0.72–2.02 (0.467) |
| ≥7th floors | 1.28, 0.59–2.81 (0.530) [0.243] | 1.34, 0.56–3.17 (0.511) [0.309] | 1.31, 0.56–3.10 (0.533) [0.241] |
| Stratified by bedroom ventilation habit (open the bedroom windows during night) | |||
| Often | 1.14, 0.80–1.63 (0.470) | 1.12, 0.77–1.65 (0.553) | 1.10, 0.74–1.63 (0.626) |
| Not often | 1.75, 1.07–2.87 (0.026) [0.002] | 1.42, 0.82–2.45 (0.209) [0.700] | 1.33, 0.76–2.33 (0.310) [0.678] |
| 3. Automobile 4S shop near residence within 200 m (yes vs. no) | |||
| Stratified by the child’s sex | |||
| Boys | 2.09, 1.27–3.44 (0.003) | 2.55, 1.49–4.38 (0.001) | 2.12, 1.22–3.69 (0.008) |
| Girls | 0.88, 0.45–1.73 (0.705) [0.002] | 1.05, 0.52–2.12 (0.883) [<0.001] | 0.87, 0.43–1.78 (0.702) [0.005] |
| Stratified by bedroom floor level | |||
| 1st–3rd floors | 1.07, 0.59–1.95 (0.821) | 0.95, 0.48–1.90 (0.884) | 0.73, 0.36–1.49 (0.389) |
| 4th–6th floors | 2.49, 1.36–4.58 (0.002) | 2.77, 1.49–5.16 (0.001) | 2.47, 1.31–4.68 (0.005) |
| ≥7th floors | 2.04, 0.61–6.79 (0.235) [0.002] | 3.62, 0.83–15.85 (0.088) [<0.001] | 3.63, 0.83–15.87 (0.087) [0.002] |
| Stratified by bedroom ventilation habit (open the bedroom windows during night) | |||
| Often | 1.26, 0.75–2.10 (0.388) | 1.47, 0.84–2.57 (0.178) | 1.17, 0.66–2.08 (0.583) |
| Not often | 1.99, 1.08–3.69 (0.026) [0.008] | 1.81, 0.94–3.50 (0.076) [0.016] | 1.60, 0.81–3.16 (0.172) [0.068] |
| 4. Ground car park in the residential community (yes vs. no) | |||
| Stratified by the child’s sex | |||
| Boys | 1.46, 1.21–1.77 (<0.001) | 1.26, 1.03–1.54 (0.022) | 1.22, 1.01–1.49 (0.044) |
| Girls | 1.39, 1.16–1.66 (<0.001) [<0.001] | 1.22, 1.01–1.48 (0.040) [0.007] | 1.21, 0.98–1.49 (0.075) [0.022] |
| Stratified by bedroom floor level | |||
| 1st–3rd floors | 1.48, 1.23–1.77 (<0.001) | 1.34, 1.10–1.63 (0.003) | 1.25, 1.02–1.53 (0.035) |
| 4th–6th floors | 1.22, 0.98–1.52 (0.075) | 1.05, 0.83–1.33 (0.679) | 1.12, 0.88–1.43 (0.344) |
| ≥7th floors | 1.29, 0.84–1.99 (0.250) [0.013] | 1.09, 0.68–1.75 (0.718) [0.293] | 1.08, 0.68–1.74 (0.735) [0.330] |
| Stratified by bedroom ventilation habit (open the bedroom windows during night) | |||
| Often | 1.31, 1.12–1.52 (0.001) | 1.16, 0.98–1.37 (0.079) | 1.14, 0.96–1.35 (0.127) |
| Not often | 1.71, 1.34–2.18 (<0.001) [0.017] | 1.38, 1.06–1.80 (0.016) [0.042] | 1.38, 1.06–1.81 (0.018) [0.035] |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Chang, J.; Liu, W.; Huang, C. Residential Ambient Traffic in Relation to Childhood Pneumonia among Urban Children in Shandong, China: A Cross-Sectional Study. Int. J. Environ. Res. Public Health 2018, 15, 1076. https://doi.org/10.3390/ijerph15061076
Chang J, Liu W, Huang C. Residential Ambient Traffic in Relation to Childhood Pneumonia among Urban Children in Shandong, China: A Cross-Sectional Study. International Journal of Environmental Research and Public Health. 2018; 15(6):1076. https://doi.org/10.3390/ijerph15061076
Chicago/Turabian StyleChang, Jing, Wei Liu, and Chen Huang. 2018. "Residential Ambient Traffic in Relation to Childhood Pneumonia among Urban Children in Shandong, China: A Cross-Sectional Study" International Journal of Environmental Research and Public Health 15, no. 6: 1076. https://doi.org/10.3390/ijerph15061076
APA StyleChang, J., Liu, W., & Huang, C. (2018). Residential Ambient Traffic in Relation to Childhood Pneumonia among Urban Children in Shandong, China: A Cross-Sectional Study. International Journal of Environmental Research and Public Health, 15(6), 1076. https://doi.org/10.3390/ijerph15061076




