Influence of Gender on Associations of Obstructive Sleep Apnea Symptoms with Chronic Conditions and Quality of Life
Abstract
1. Introduction
2. Materials and Methods
2.1. Sleep Variables
2.2. Chronic Conditions
2.3. Statistical Analysis
3. Results
3.1. Diagnosed OSA
3.1.1. Sleep Characteristics and OSA Risk Factors
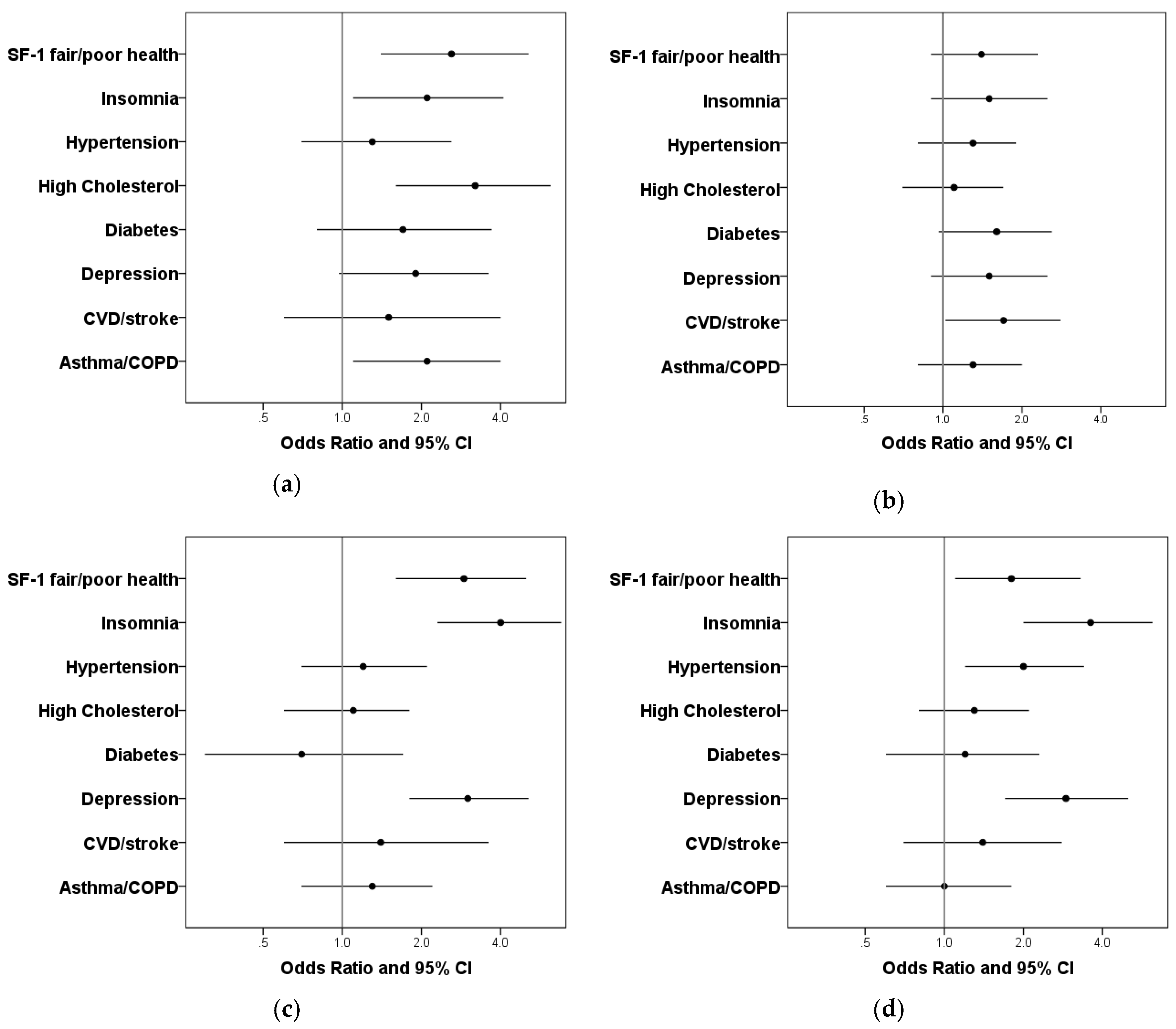
3.1.2. Chronic Conditions
3.1.3. Health-Related Quality of Life
3.2. OSA Symptoms Not Diagnosed
3.2.1. Sleep Characteristics and OSA Risk Factors
3.2.2. Chronic Conditions
3.2.3. Health-Related Quality of Life
4. Discussion
5. Conclusions
Author Contributions
Conflicts of Interest
References
- Franklin, K.; Sahlin, C.; Stenlund, H.; Lindberg, E. Sleep apnoea is a common occurrence in females. Eur. Respir. J. 2013, 41, 610–615. [Google Scholar] [CrossRef] [PubMed]
- Heinzer, R.; Vat, S.; Marques-Vidal, P.; Marti-Soler, H.; Andries, D.; Tobback, N.; Mooser, V.; Preisig, M.; Malhotra, A.; Waeber, G.; et al. Prevalence of sleep-disordered breathing in the general population: The HypnoLaus study. Lancet Respir. Med. 2015, 3, 310–318. [Google Scholar] [CrossRef]
- Collop, N.A.; Adkins, D.; Phillips, B.A. Gender differences in sleep and sleep-disordered breathing. Clin. Chest Med. 2004, 25, 257–268. [Google Scholar] [CrossRef] [PubMed]
- Gaines, J.; Vgontzas, A.N.; Fernandez-Mendoza, J.; Kritikou, I.; Basta, M.; Bixler, E.O. Gender differences in the association of sleep apnea and inflammation. Brain Behav. Immun. 2015, 47, 211–217. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Lin, C.M.; Davidson, T.M.; Ancoli-Israel, S. Gender differences in obstructive sleep apnea and treatment implications. Sleep Med. Rev. 2008, 12, 481–496. [Google Scholar] [CrossRef] [PubMed]
- Ye, L.; Pien, G.W.; Weaver, T.E. Gender differences in the clinical manifestation of obstructive sleep apnea. Sleep Med. 2009, 10, 1075–1084. [Google Scholar] [CrossRef] [PubMed]
- Lindberg, E.; Benediktsdottir, B.; Franklin, K.A.; Holm, M.; Johannessen, A.; Jögi, R.; Gislason, T.; Real, F.G.; Schlünssen, V.; Janson, C. Women with symptoms of sleep-disordered breathing are less likely to be diagnosed and treated for sleep apnea than men. Sleep Med. 2017, 35, 17–22. [Google Scholar] [CrossRef] [PubMed]
- Young, T.; Hutton, R.; Finn, L.; Badr, S.; Palta, M. The gender bias in sleep apnea diagnosis. Are women missed because they have different symptoms? Arch. Intern. Med. 1996, 156, 2445–2451. [Google Scholar] [CrossRef] [PubMed]
- Quintana-Gallego, E.; Carmona-Bernal, C.; Capote, F.; Sanchez-Armengol, A.; Botebol-Benhamou, G.; Polo-Padillo, J.; Castillo-Gomez, J. Gender differences in obstructive sleep apnea syndrome: A clinical study of 1166 patients. Respir. Med. 2004, 98, 984–989. [Google Scholar] [CrossRef] [PubMed]
- Valipour, A.; Lothaller, H.; Rauscher, H.; Zwick, H.; Burghuber, O.C.; Lavie, P. Gender-related differences in symptoms of patients with suspected breathing disorders in sleep. Sleep 2007, 30, 312–319. [Google Scholar] [CrossRef] [PubMed]
- Basoglu, O.K.; Tasbakan, M.S. Gender differences in clinical and polysomnographic features of obstructive sleep apnea: A clinical study of 2827 patients. Sleep Breath. 2017. [Google Scholar] [CrossRef] [PubMed]
- Nigro, C.A.; Dibur, E.; Borsini, E.; Malnis, S.; Ernst, G.; Bledel, I.; González, S.; Arce, A.; Nogueira, F. The influence of gender on symptoms associated with obstructive sleep apnea. Sleep Breath. 2018. [Google Scholar] [CrossRef] [PubMed]
- Pillar, G.; Lavie, P. Psychiatric symptoms in sleep apnea syndrome: Effects of gender and respiratory disturbance index. Chest 1998, 114, 697–703. [Google Scholar] [CrossRef] [PubMed]
- Alotair, H.; BaHammam, A. Gender differences in Saudi patients with obstructive sleep apnea. Sleep Breath. 2008, 12, 323–329. [Google Scholar] [CrossRef] [PubMed]
- Vagiakis, E.; Kapsimalis, F.; Lagogianni, I.; Perraki, H.; Minaritzoglou, A.; Alexandropoulou, K.; Roussos, C.; Kryger, M. Gender differences on polysomnographic findings in Greek subjects with obstructive sleep apnea syndrome. Sleep Med. 2006, 7, 424–430. [Google Scholar] [CrossRef] [PubMed]
- Greenberg-Dotan, S.; Reuveni, H.; Simon-Tuval, T.; Oksenberg, A.; Tarasiuk, A. Gender differences in morbidity and health care utilization among adult obstructive sleep apnea patients. Sleep 2007, 30, 1173–1180. [Google Scholar] [CrossRef] [PubMed]
- Silva, G.E.; Goodwin, J.L.; Vana, K.D.; Quan, S.F. Obstructive Sleep Apnea and Quality of Life: Comparison of the SAQLI, FOSQ, and SF-36 Questionnaires. Southwest J. Pulm. Crit. Care 2016, 13, 137–149. [Google Scholar] [CrossRef] [PubMed]
- Sullivan, C.; Berthon-Jones, M.; Issa, F.; Eves, L. Reversal of obstructive sleep apnoea by continuous positive airway pressure applied through the nares. Lancet 1981, 317, 862–865. [Google Scholar] [CrossRef]
- Adams, R.; Appleton, S.; Taylor, A.; McEvoy, R.; Wittert, G. Are the International Classification of Sleep Disorders (ICSD-3) criteria for the sleep apnoea syndrome too inclusive? Lancet Respir. Med. 2016, 4, e19–e20. [Google Scholar] [CrossRef]
- Grant, J.F.; Taylor, A.W.; Ruffin, R.E.; Wilson, D.H.; Phillips, P.J.; Adams, R.J.; Price, K.; The North West Adelaide Health Study Team. Cohort Profile: The North West Adelaide Health Study (NWAHS). Int. J. Epidemiol. 2008, 38, 1479–1486. [Google Scholar] [CrossRef] [PubMed]
- Morin, C.M.; Belleville, G.; Belanger, L.; Ivers, H. The Insomnia Severity Index: Psychometric indicators to detect insomnia cases and evaluate treatment response. Sleep 2011, 34, 601–608. [Google Scholar] [CrossRef] [PubMed]
- Appleton, S.L.; Ruffin, R.E.; Wilson, D.H.; Taylor, A.W.; Adams, R.J.; North West Adelaide Cohort Health Study Team. Cardiovascular disease risk associated with asthma and respiratory morbidity might be mediated by short-acting beta2-agonists. J. Allergy Clin. Immunol. 2009, 123, 124–130. [Google Scholar] [CrossRef] [PubMed]
- Tucker, G.; Adams, R.; Wilson, D. Observed agreement problems between sub-scales and summary components of the SF-36 version 2—An alternative scoring method can correct the problem. PLoS ONE 2013, 8, e61191. [Google Scholar] [CrossRef] [PubMed]
- Taylor, A.W.; Dal Grande, E.; Grant, J.; Appleton, S.; Gill, T.K.; Shi, Z.; Adams, R.J. Weighting of the data and analytical approaches may account for differences in overcoming the inadequate representativeness of the respondents to the third wave of a cohort study. J. Clin. Epidemiol. 2013, 66, 461–464. [Google Scholar] [CrossRef] [PubMed]
- Subramanian, S.; Jayaraman, G.; Majid, H.; Aguilar, R.; Surani, S. Influence of gender and anthropometric measures on severity of obstructive sleep apnea. Sleep Breath. 2012, 16, 1091–1095. [Google Scholar] [CrossRef] [PubMed]
- Mukherjee, S.; Hillman, D.; Lee, J.; Fedson, A.; Simpson, L.; Ward, K.; Love, G.; Edwards, C.; Szegner, B.; Palmer, L.J. Cohort profile: The Western Australian Sleep Health Study. Sleep Breath. 2012, 16, 205–215. [Google Scholar] [CrossRef] [PubMed]
- Chen, H.; Lowe, A.A.; Bai, Y.; Hamilton, P.; Fleetham, J.A.; Almeida, F.R. Evaluation of a portable recording device (ApneaLink) for case selection of obstructive sleep apnea. Sleep Breath. 2009, 13, 213–219. [Google Scholar] [CrossRef] [PubMed]
- Berry, R.B.; Budhiraja, R.; Gottlieb, D.J.; Gozal, D.; Iber, C.; Kapur, V.K.; Marcus, C.L.; Mehra, R.; Parthasarathy, S.; Quan, S.F.; et al. Rules for scoring respiratory events in sleep: Update of the 2007 AASM manual for the scoring of sleep and associated events. J. Clin. Sleep Med. 2012, 8, 597–619. [Google Scholar] [CrossRef] [PubMed]
- Alonso, J.; Ferrer, M.; Gandek, B.; Ware, J.E., Jr.; Aaronson, N.K.; Mosconi, P.; Rasmussen, N.K.; Bullinger, M.; Fukuhara, S.; Kaasa, S.; et al. Health-related quality of life associated with chronic conditions in eight countries: Results from the International Quality of Life Assessment (IQOLA) Project. Qual. Life Res. Int. J. Qual. Life Asp. Treat. Care Rehabil. 2004, 13, 283–298. [Google Scholar] [CrossRef]
- Taylor, A.W.; Dal Grande, E.; Gill, T.K.; Chittleborough, C.R.; Wilson, D.H.; Adams, R.J.; Grant, J.F.; Phillips, P.; Appleton, S.; Ruffin, R.E. How valid are self-reported height and weight? A comparison between CATI self-report and clinic measurements using a large cohort study. Aust. N. Z. J. Public Health 2006, 30, 238–246. [Google Scholar] [CrossRef] [PubMed]
- Kriegsman, D.M.; Penninx, B.W.; van Eijk, J.T.; Boeke, A.J.; Deeg, D.J. Self-reports and general practitioner information on the presence of chronic diseases in community dwelling elderly. A study on the accuracy of patients’ self-reports and on determinants of inaccuracy. J. Clin. Epidemiol. 1996, 49, 1407–1417. [Google Scholar] [CrossRef]
- Rahman, A.; Gibney, L.; Person, S.D.; Williams, O.D.; Kiefe, C.; Jolly, P.; Roseman, J. Validity of self-reports of reasons for hospitalization by young adults and risk factors for discordance with medical records: The Coronary Artery Risk Development in Young Adults (CARDIA) Study. Am. J. Epidemiol. 2005, 162, 491–498. [Google Scholar] [CrossRef] [PubMed]
- Adams, R.J.; Appleton, S.L.; Vakulin, A.; Lang, C.; Martin, S.A.; Taylor, A.W.; McEvoy, R.D.; Antic, N.A.; Catcheside, P.G.; Wittert, G.A. Association of daytime sleepiness with obstructive sleep apnoea and comorbidities varies by sleepiness definition in a population cohort of men. Respirology 2016, 21, 1314–1321. [Google Scholar] [CrossRef] [PubMed]
- Mirer, A.G.; Young, T.; Palta, M.; Benca, R.M.; Rasmuson, A.; Peppard, P.E. Sleep-disordered breathing and the menopausal transition among participants in the Sleep in Midlife Women Study. Menopause 2017, 24, 157–162. [Google Scholar] [CrossRef] [PubMed]
- Manson, J.E.; Chlebowski, R.T.; Stefanick, M.L.; Aragaki, A.K.; Rossouw, J.E.; Prentice, R.L.; Anderson, G.; Howard, B.V.; Thomson, C.A.; LaCroix, A.Z.; et al. Menopausal hormone therapy and health outcomes during the intervention and extended poststopping phases of the Women’s Health Initiative randomized trials. JAMA 2013, 310, 1353–1368. [Google Scholar] [CrossRef] [PubMed]
- Stuenkel, C.A.; Davis, S.R.; Gompel, A.; Lumsden, M.A.; Murad, M.H.; Pinkerton, J.V.; Santen, R.J. Treatment of Symptoms of the Menopause: An Endocrine Society Clinical Practice Guideline. J. Clin. Endocrinol. Metab. 2015, 100, 3975–4011. [Google Scholar] [CrossRef] [PubMed]
- Australian Bureau of Statistics. Australian Health Survey: Biomedical Results for Chronic Diseases, 2011–12; Cat No. 4364.0.55.005; Australian Bureau of Statistics: Canberra, Australia, 2013.
- Deloitte Access Economics, Asleep on the Job: Costs of Inadequate Sleep in Australia. 2016. Available online: https://www.sleephealthfoundation.org.au/public-information/special-reports/asleep-on-the-job.html (accessed on 7 May 2018).
| Male (n = 753) | Female (n = 808) | p | Total | |
|---|---|---|---|---|
| Sleep disorders and symptoms, % (n) | ||||
| Diagnosed OSA | 12.6 (95) | 3.3 (27) | <0.001 | 7.8 (122) |
| Snoring: loud or bothered others | 38.4 (285) | 20.6 (161) | <0.001 | 29.3 (446) |
| Witnessed breathing pauses | 15.9 (118) | 10.0 (78) | 0.002 | 12.6 (196) |
| ≥2 of 3 daytime sleepiness problems | 37.9 (286) | 38.7 (312) | 0.77 | 38.3 (598) |
| Loud snoring and ≥2 daytime sleepiness problems | 17.1 (129) | 9.7 (78) | <0.001 | 13.3 (207) |
| Insomnia Severity Index ≥10 | 16.2 (120) | 21.3 (165) | 0.010 | 18.8 (285) |
| Nocturia | 28.6 (212) | 32.4 (253) | 0.11 | 30.6 (465) |
| Body mass index (kg/m2) | <0.001 | |||
| ≤24.9 | 23.8 (179) | 36.1 (283) | 30.1 (462) | |
| 25.0–29.9 | 47.3 (356) | 32.5 (255) | 39.8 (611) | |
| ≥30.0 | 28.9 (217) | 31.5 (247) | 30.2 (464) | |
| Current smoker | 13.0 (98) | 10.8 (87) | 0.27 | 11.9 (185) |
| Demographics, % (n) | ||||
| Age (mean (SD)) | 53.2 (14.8) | 54.9 (15.5) | 0.027 | 54.1 (15.2) |
| Highest educational attainment | <0.001 | |||
| High school or less | 34.8 (262) | 46.2 (373) | 40.7 (635) | |
| Certificate (including Trade) or Diploma | 38.9 (293) | 23.9 (193) | 31.1 (486) | |
| Bachelor degree or higher | 25.0 (188) | 26.0 (210) | 25.5 (398) | |
| Not stated | 1.3 (10) | 4.0 (32) | 2.7 (42) | |
| Annual household income | <0.001 | |||
| <$40,000 | 19.5 (147) | 27.6 (223) | 23.7 (370) | |
| $40,001–$80,000 | 24.6 (185) | 21.8 (176) | 23.1 (361) | |
| ≥$80,001 | 47.7 (359) | 34.0 (275) | 40.6 (633) | |
| Not stated | 8.2 (62) | 16.6 (134) | 12.6 (196) | |
| Financial stress 1 | 0.18 | |||
| Yes | 74.0 (557) | 73.1 (591) | 73.5 (1148) | |
| No | 19.8 (149) | 16.2 (131) | 17.9 (280) | |
| Not stated | 6.2 (47) | 10.6 (86) | 8.5 (133) | |
| Partner/relationship | 77.2 (581) | 66.2 (535) | <0.001 | 71.5 (1116) |
| Private health insurance | 61.9 (466) | 66.2 (488) | 0.134 | 61.1 (954) |
| Males | Females | |||||
|---|---|---|---|---|---|---|
| No OSA | Diagnosed OSA | OSA Symptoms not Diagnosed | No OSA | Diagnosed OSA | OSA Symptoms not Diagnosed | |
| (n = 563) | (n = 95) | (n = 96) | (n = 709) | (n = 27) | (n = 71) | |
| Snoring: loud/bothered others | 23.4 (129) | 63.8 (60) 3 | 100.0 (96) | 11.0 (75) | 59.3 (16) 3 | 100.0 (71) |
| Witnessed breathing pauses | 4.0 (22) | 66.7 (62) 3 | 35.1 (34) 3 | 6.9 (47) | 70.4 (19) 3 | 18.3 (13) 3 |
| ≥2 of 3 sleepiness problems 1 | 25.6 (144) | 48.4 (46) 3 | 100.0 (96) | 32.1 (228) | 48.1 (13) | 100.0 (71) |
| Loud snoring and ≥2 sleepiness problems | 0.0 (0) | 35.8 (34) | 100.0 (96) | 0.0 (0) | 25.9 (7) | 100.0 (71) |
| Insomnia Severity Index ≥10 | 13.7 (77) | 18.9 (18) | 27.1 (26) 3 | 17.3 (123) | 29.6 (8) | 52.1 (37) 3 |
| Nocturia | 24.0 (132) | 41.5 (39) 3 | 43.2 (41) 3 | 30.9 (211) | 25.9 (7) | 49.3 (35) 2 |
| BMI (kg/m2) ≥30.0 | 23.6 (133) | 52.6 (50) 3 | 35.8 (34) | 27.8 (191) | 77.8 (21) 3 | 50.7 (36) 3 |
| BMI (mean (SD)) | 27.6 (4.3) | 30.8 (5.5) 3 | 29.5 (4.3) 3 | 27.5 (6.0) | 34.4 (6.5) 3 | 30.1 (7.6) 2 |
| Neck circumference >43 cm | 28.3 (120) | 41.6 (32) 3 | 29.3 (32) 3 | 4.0 (20) | 31.8 (7) 3 | 12.2 (6) 3 |
| Current smoker | 10.2 (57) | 17.0 (16) | 27.1 (26) 3 | 11.2 (78) | 18.5 (5) | 7.0 (5) |
| Insufficient physical activity | 29.9 (159) | 37.8 (39) | 50.0 (45) | 41.5 (275) | 75.0 (18) 3 | 65.1 (41) 2 |
| Hormone replacement therapy | 4.4 (31) | 7.1 (2) | 12.7 (9) 3 | |||
| Age (mean (SD), years) | 52.2 (15.1) | 62.0 (10.9) | 50.4 (14.0) | 54.8 (15.8) | 63.3 (10.7) 2 | 52.6 (11.9) |
| Age ≥55 years | 37.1 (209) | 71.3 (67) 3 | 35.7 (34) | 44.1 (313) | 85.2 (23) 3 | 40.8 (29) |
| Married/partner | 74.5 (420) | 76.6 (72) | 93.7(89) | 65.4 (464) | 66.7 (18) | 73.2 (52) |
| Private health insurance | 63.1 (355) | 51.6 (49) 2 | 64.2 (62) | 61.5 (436) | 42.9 (12) | 56.3 (40) |
| Chronic Condition, % (n) | No OSA | Diagnosed OSA | OSA Symptoms Not Diagnosed | Total, % |
|---|---|---|---|---|
| Male | (n = 563) | (n = 94) | (n = 95) | |
| Doctor-Diagnosed | ||||
| Diabetes (or medication) | 8.7 (49) | 26.6 (25) 3 | 9.5 (9) | 11.0 |
| Cardiovascular disease/stroke | 6.9 (39) | 21.3 (20) 3 | 8.3 (8) | 8.9 |
| Hypertension (or medication) | 27.5 (155) | 23.9 (20) 3 | 40.6 (39) 3 | 32.8 |
| High cholesterol | 23.4 (132) | 36.2 (34) 3 | 33.3 (32) 2 | 26.3 |
| Kidney disease | 1.8 (10) | 10.5 (10) 3 | 1.0 (1) | 2.8 |
| Obstructive lung disease | 25.4 (143) | 27.7 (26) | 16.7 (16) | 24.6 |
| Depression (CESD) | 20.7 (114) | 23.9 (22) | 34.4 (33) 3 | 22.9 |
| SF-1 fair-poor general health | 10.8 (60) | 30.1 (28) 3 | 37.9 (36) 3 | 16.7 |
| Female | (n = 710) | (n = 27) | (n = 71) | |
| Doctor-Diagnosed | ||||
| Diabetes (or medication) | 8.0 (57) | 22.2 (6) 2 | 5.6 (4) | 8.3 |
| Cardiovascular disease/stroke | 5.6 (40) | 14.8 (4) | 5.6 (4) | 5.9 |
| Hypertension (or medication) | 33.1 (235) | 48.1 (13) | 26.8 (19) | 33.1 |
| High cholesterol | 28.5 (202) | 63.0 (17) 3 | 32.4 (23) | 30.0 |
| Kidney disease | 1.8 (13) | 0.0 (0) | 4.2 (3) | 2.0 |
| Obstructive lung disease | 29.4 (209) | 48.1 (13) 2 | 21.1 (15) | 29.3 |
| Depression (CESD) | 29.0 (196) | 33.3 (9) | 64.3 (31) 3 | 32.3 |
| SF-1 fair-poor general health | 18.8 (132) | 46.2 (12) 3 | 47.8 (33) 3 | 22.2 |
| No OSA | Diagnosed OSA | OSA Symptoms Not Diagnosed | Total | |
|---|---|---|---|---|
| Unadjusted mean scores | ||||
| Males | ||||
| PCS 1 | 49.6 (8.9) | 44.8 (11.4) 2 | 43.7 (11.5) 2 | 48.2 (9.9) |
| MCS 1 | 49.6 (9.4) | 46.2 (11.4) 2 | 45.7 (10.2) 2 | 48.7 (9.9) |
| Females | ||||
| PCS 1 | 48.2 (9.9) | 37.9 (12.2) 2 | 40.5 (9.8) 2 | 47.2 (10.3) |
| MCS 1 | 47.0 (10.2) | 40.9 (11.6) 2 | 36.4 (11.9) 2 | 45.9 (10.9) |
| Linear regression Unstandardized B coefficients | ||||
| Males | ||||
| PCS | −1.2 (−3.1, 0.6) | −4.0 (−6.3, −1.6) 3 | ||
| MCS | −1.8 (−3.8, 0.21) | −5.3 (−7.7, −2.8) 3 | ||
| Females | ||||
| PCS | −4.6 (−7.8, −1.3) 3 | −6.4 (−9.1, −3.8) 3 | ||
| MCS | −3.5 (−7.0, 0.03) | −8.1 (−11.0, −5.2) 3 | ||
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Appleton, S.; Gill, T.; Taylor, A.; McEvoy, D.; Shi, Z.; Hill, C.; Reynolds, A.; Adams, R. Influence of Gender on Associations of Obstructive Sleep Apnea Symptoms with Chronic Conditions and Quality of Life. Int. J. Environ. Res. Public Health 2018, 15, 930. https://doi.org/10.3390/ijerph15050930
Appleton S, Gill T, Taylor A, McEvoy D, Shi Z, Hill C, Reynolds A, Adams R. Influence of Gender on Associations of Obstructive Sleep Apnea Symptoms with Chronic Conditions and Quality of Life. International Journal of Environmental Research and Public Health. 2018; 15(5):930. https://doi.org/10.3390/ijerph15050930
Chicago/Turabian StyleAppleton, Sarah, Tiffany Gill, Anne Taylor, Douglas McEvoy, Zumin Shi, Catherine Hill, Amy Reynolds, and Robert Adams. 2018. "Influence of Gender on Associations of Obstructive Sleep Apnea Symptoms with Chronic Conditions and Quality of Life" International Journal of Environmental Research and Public Health 15, no. 5: 930. https://doi.org/10.3390/ijerph15050930
APA StyleAppleton, S., Gill, T., Taylor, A., McEvoy, D., Shi, Z., Hill, C., Reynolds, A., & Adams, R. (2018). Influence of Gender on Associations of Obstructive Sleep Apnea Symptoms with Chronic Conditions and Quality of Life. International Journal of Environmental Research and Public Health, 15(5), 930. https://doi.org/10.3390/ijerph15050930







