Impact of the Introduction of the Electronic Health Insurance Card on the Use of Medical Services by Asylum Seekers in Germany
Abstract
1. Introduction
2. Study-Design & Methods
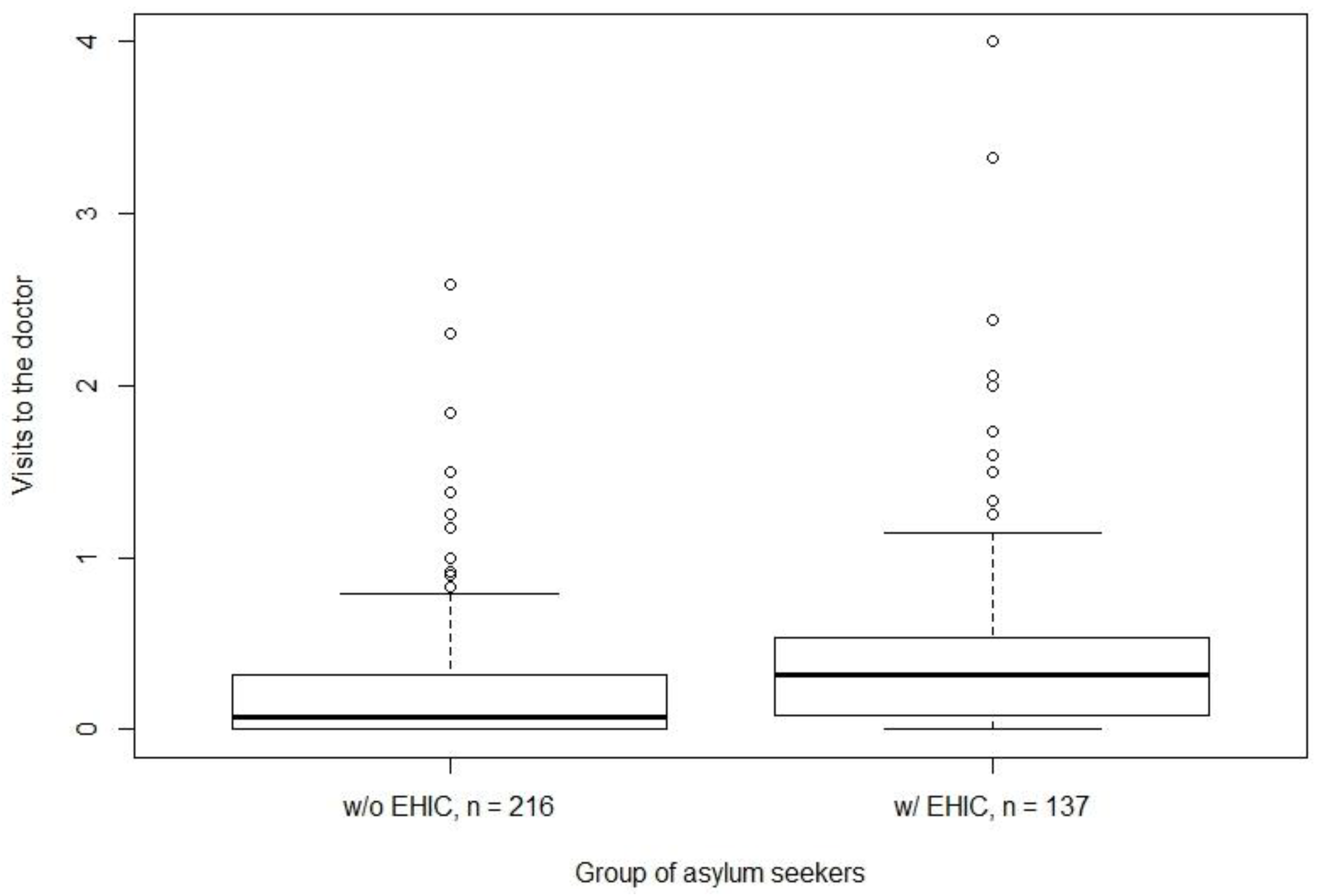
3. Results
4. Discussion
5. Conclusions
Author Contributions
Acknowledgments
Ethical Approval
Conflicts of Interest
Abbreviations
| EHIC | Electronic Health Insurance Card |
| CR | Consultation Rate of Ambulant Physicians |
| VIF | Variation Inflation Factors |
| PTSD | Post-Traumatic Stress Disorder |
References
- UNHCR. UNHCR Global Trends-Forced Displacement in 2016. Available online: http://www.unhcr.org/globaltrends2016/ (accessed on 29 December 2017).
- Bundesamt für Migration und Flüchtlinge. Aktuelle Zahlen zu Asyl 2017. Available online: http://www.bamf.de/SharedDocs/Anlagen/DE/Downloads/Infothek/Statistik/Asyl/aktuelle-zahlen-zu-asyl-januar-2017.pdf?__blob=publicationFile (accessed on 15 January 2018).
- Sachverständigenrat deutscher Stiftungen für Integration und Migration. Fakten zur Asylpolitik; Sachverständigenrat deutscher Stiftungen für Integration und Migration: Berlin, Germany, 2017. [Google Scholar]
- BAMF-Bundesamt für Migration und Flüchtlinge Asyl und Flüchtlingsschutz. Available online: http://www.bamf.de/DE/Fluechtlingsschutz/fluechtlingsschutz-node.html (accessed on 19 January 2018).
- Schenk, L. Migrationssensible Gesundheitsforschung; Freie Universität Berlin: Berlin, Germany, 2016. [Google Scholar]
- Razum, O.; Zeeb, H.; Rohrmann, S. The “healthy migrant effect”–not merely a fallacy of inaccurate denominator figures. Int. J. Epidemiol. 2000, 29, 191–192. [Google Scholar] [CrossRef] [PubMed]
- van Burg, J.L.; Verver, S.; Borgdorff, M.W. The epidemiology of tuberculosis among asylum seekers in the Netherlands: Implications for screening. Int. J. Tuberc. Lung Dis. 2003, 7, 139–144. [Google Scholar] [PubMed]
- Clark, R.C.; Mytton, J. Estimating infectious disease in UK asylum seekers and refugees: A systematic review of prevalence studies. J. Public Health 2007, 29, 420–428. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Seilmaier, M.; Guggemos, W.; Alberer, M.; Wendtner, C.M.; Spinner, C.D. Infektionen bei Flüchtlingen. Notf. Rettungsmedizin 2017, 20, 216–227. [Google Scholar] [CrossRef]
- Silove, D.; Sinnerbrink, I.; Field, A.; Manicavasagar, V.; Steel, Z. Anxiety, depression and PTSD in asylum-seekers: Assocations with pre-migration trauma and post-migration stressors. Br. J. Psychiatry 1997, 170, 351–357. [Google Scholar] [CrossRef] [PubMed]
- Crumlish, N.; O’Rourke, K. A Systematic Review of Treatments for Post-Traumatic Stress Disorder among Refugees and Asylum-Seekers. J. Nerv. Ment. Dis. 2010, 198, 237. [Google Scholar] [CrossRef] [PubMed]
- Frank, L.; Yesil-Jürgens, R.; Razum, O.; Bozorgmehr, K.; Schenk, L.; Gilsdorf, A.; Rommel, A.; Lampert, T. Health and healthcare provision to asylum seekers and refugees in Germany. J. Health Monit. 2017, 21, 22–41. [Google Scholar] [CrossRef]
- Gavranidou, M.; Niemiec, B.; Magg, B.; Rosner, R. Traumatische Erfahrungen, aktuelle Lebensbedingungen im Exil und psychische Belastung junger Flüchtlinge. Kindh. Entwickl. 2008, 17, 224–231. [Google Scholar] [CrossRef]
- Izutsu, T.; Tsutsumi, A.; Sato, T.; Naqibullah, Z.; Wakai, S.; Kurita, H. Nutritional and Mental Health Status of Afghan Refugee Children in Peshawar, Pakistan: A Descriptive Study. Asia Pac. J. Public Health 2005, 17, 93–98. [Google Scholar] [CrossRef] [PubMed]
- Ellison, C.G.; Boardman, J.D.; Williams, D.R.; Jackson, J.S. Religious Involvement, Stress, and Mental Health: Findings from the 1995 Detroit Area Study. Soc. Forces 2001, 80, 215–249. [Google Scholar] [CrossRef]
- Gäbel, U.; Ruf, M.; Schauer, M.; Odenwald, M.; Neuner, F. Prävalenz der Posttraumatischen Belastungsstörung (PTSD) und Möglichkeiten der Ermittlung in der Asylverfahrenspraxis. Z. Klin. Psychol. Psychother. 2006, 35, 12–20. [Google Scholar] [CrossRef]
- Fazel, M.; Wheeler, J.; Danesh, J. Prevalence of serious mental disorder in 7000 refugees resettled in western countries: A systematic review. Lancet 2005, 365, 1309–1314. [Google Scholar] [CrossRef]
- Robert-Koch-Institut. RKI-Pressemitteilungen-Schwerpunktthema Gesundheit von Migranten und Geflüchteten. Available online: https://www.rki.de/DE/Content/Service/Presse/Pressemitteilungen/2016/08_2016.html (accessed on 22 July 2017).
- Bundesministerium der Justiz und für Verbraucherschutz Asylbewerberleistungsgesetz in der Fassung der Bekanntmachung vom 5. August 1997 (BGBl. I S. 2022), das zuletzt durch Artikel 4 des Gesetzes vom 17. Juli 2017 (BGBl. I S. 2541) geändert worden ist, 5 August 1997.
- Epping, B. Medizinische Versorgung von Flüchtlingen: Teure Hürden. Z. Orthop. Unfallchirurgie 2017, 155, 129–134. [Google Scholar] [CrossRef] [PubMed]
- Kasl, S.V.; Cobb, S. Health Behavior, Illness Behavior and Sick Role behavior: I. Health and Illness Behavior. Arch. Environ. Health Int. J. 1966, 12, 246–266. [Google Scholar] [CrossRef]
- § 264 SGB V, Übernahme der Krankenbehandlung für nicht Versi...—Gesetze des Bundes und der Länder. Available online: http://www.lexsoft.de/cgi-bin/lexsoft/justizportal_nrw.cgi?xid=137489,351 (accessed on 19 January 2018).
- Wächter-Raquet, M. Einführung der Gesundheitskarte für Asylsuchende und Flüchtlinge. 2016, Gütersloh, Bertelsmann Stiftung. Available online: https://www.bertelsmann-stiftung.de/fileadmin/files/BSt/Publikationen/GrauePublikationen/Studie_VV_Gesundheitskarte_Fluechtlinge_2016.pdf (accessed on 20 December 2017).
- Ministerium für Gesundheit, Emanzipation, Pflege und Alter des Landes Nordrhein-Westfalen (MGEPA). Rahmenvereinbarung zur Übernahme der Gesundheitsversorgung für nicht Versicherungspflichtige gegen Kostenerstattung nach § 264 Absatz 1 SGB V in Verbindung mit §§ 1,1a Asylbewerberleistungsgesetz in Nordrhein-Westfalen. p. 27.05.2017. Available online: https://www.mhkbg.nrw/mediapool/pdf/gesundheit/Gesundheitskarte_Fluechtlinge/Rahmenvereinbarung_Online.pdf (accessed on 25 December 2017).
- Deutsche Ärztezeitung Flüchtlinge: Union gegen E-Card für Asylbewerber. Available online: http://www.aerztezeitung.de/politik_gesellschaft/gp_specials/fluechtlinge/article/893399/fluechtlinge-union-e-card-asylbewerber.html (accessed on 20 January 2018).
- Faul, F.; Erdfelder, E.; Lang, A.G.; Buchner, A. G*Power 3: A flexible statistical power analysis program for the social, behavioral, and biomedical sciences. Behav. Res. Methods 2007, 39, 175–191. [Google Scholar] [CrossRef] [PubMed]
- Ruxton, G.D. The unequal variance t-test is an underused alternative to Student’s t-test and the Mann–Whitney U test. Behav. Ecol. 2006, 17, 688–690. [Google Scholar] [CrossRef]
- GBD 2016 Disease and Injury Incidence and Prevalence Collaborators. Global, regional, and national incidence, prevalence, and years lived with disability for 328 diseases and injuries for 195 countries, 1990–2016: A systematic analysis for the Global Burden of Disease Study 2016. Lancet 2017, 390, 1211–1259. [Google Scholar] [CrossRef]
- Wollschläger, D. R Kompakt; Springer: Berlin/Heidelberg, Germany, 2016; ISBN 978-3-662-49101-0. [Google Scholar]
- Ohr, D. Lineare Regression: Modellannahmen und Regressionsdiagnostik. In Handbuch der Sozialwissenschaftlichen Datenanalyse; Wolf, C., Best, H., Eds.; VS Verlag für Sozialwissenschaften: Wiesbaden, Germany, 2010; pp. 639–675. ISBN 978-3-531-16339-0. [Google Scholar]
- Rattay, P.; Butschalowsky, H.; Rommel, A.; Prütz, F.; Jordan, S.; Nowossadeck, E.; Domanska, O.; Kamtsiuris, P. Inanspruchnahme der ambulanten und stationären medizinischen Versorgung in Deutschland: Ergebnisse der Studie zur Gesundheit Erwachsener in Deutschland (DEGS1). Bundesgesundheitsblatt-Gesundheitsforschung-Gesundheitsschutz 2013, 56, 832–844. [Google Scholar] [CrossRef] [PubMed]
- Sönmez, E.; Jesuthasan, J.; Abels, I.; Nassar, R.; Kurmeyer, C.; Schouler-Ocak, M. Study on female refugees–A representative research study on refugee women in Germany. Eur. Psychiatry 2017, 41, 251. [Google Scholar] [CrossRef]
- Flatten, G.; Gast, U.; Hofmann, A.; Knaevelsrud, C.; Lampe, A.; Liebermann, P.; Maercker, A.; Reddemann, L.; Wöller, W. S3—Leitlinie Posttraumatische Belastungsstörung. Trauma und Gewalt 2011, 3, 202–210. [Google Scholar]
- Burmester, F. Auswirkungen der Zusammenarbeit mit der AOK Bremen/Bremerhaven aus Sicht der Behörde für Arbeit, Soziales, Familie und Integration; Behörde für Arbeit, Soziales, Familie und Integration Hamburg: Hamburg, Germany, 2014. [Google Scholar]
- Bozorgmehr, K.; Razum, O. Effect of Restricting Access to Health Care on Health Expenditures among Asylum-Seekers and Refugees: A Quasi-Experimental Study in Germany, 1994–2013. PLoS ONE 2015, 10, e0131483. [Google Scholar] [CrossRef] [PubMed]
| Characteristic | Percentage |
|---|---|
| Age in years (mean ± SD) | 31.12 ± 9.49 |
| Sex | |
| Male | 80% |
| Country of origin | |
| Syria | 30% |
| Iraq | 14% |
| Afghanistan | 10% |
| Iran | 7% |
| Albania | 1% |
| Eritrea | 5% |
| Pakistan | 2% |
| Serbia | 1% |
| Other | 30% |
| Family status | |
| Single | 56% |
| Married | 39% |
| Divorced | 3% |
| Widowed | 2% |
| Education | |
| College degree | 17% |
| General qualification for university entrance | 25% |
| Vocational training | 5% |
| Other | 16% |
| No educational degree | 37% |
| Children | |
| None | 60% |
| One child | 9% |
| Two children | 12% |
| More than two children | 19% |
| Municipality | |
| Bochum | 72% |
| Datteln | 23% |
| Herne | 5% |
| Point of the Survey | |
| 2016 | 39% |
| 2017 | 61% |
| Months in Germany (mean ± SD) | 14.32 ± 10.54 |
| German language skills | |
| 1—very bad | 18% |
| 2—bad | 23% |
| 3—average | 33% |
| 4—good | 21% |
| 5—very good | 4% |
| Currently on medication | |
| Yes | 23% |
| Missing information | 4% |
| Chronic Disease | |
| Yes | 60% |
| Missing information | 1% |
| Diseases | |
| Heart disease | 5% |
| Psychiatric disorder | 17% |
| Joint disease | 7% |
| Diabetes | 4% |
| Back pain | 12% |
| Cancer | 1% |
| Thyroid disease | 3% |
| Other | 20% |
| Electronic Health Insurance Card (EHIC) | |
| Yes | 57% |
| Consultation rate of ambulant physicians (CR; visits to the doctor per month) (mean + SD) | 0.32 ± 0.49 |
| Contacts to further physicians | |
| Hospital | 35% |
| Volunteers (e.g., in camp) | 9% |
| Characteristic | Coefficient (Standard Error) | P-Value |
|---|---|---|
| Health system related variables | ||
| Electronic Health Insurance Card (yes vs. no) | 0.31 (0.06) | 0.00 |
| Medication (yes vs. no) | 0.14 (0.06) | 0.02 |
| Language skills | ||
| German (per increase on a scale from 1 to 5) | 0.02 (0.02) | 0.50 |
| Diseases | ||
| Heart disease (yes vs. no) | 0.25 (0.13) | 0.05 |
| Psychiatric disorders (yes vs. no) | 0.30 (0.07) | 0.00 |
| Joint disease (yes vs. no) | −0.03 (0.11) | 0.81 |
| Municipality | ||
| Datteln (yes vs. no, compared to Bochum) | 0.10 (0.07) | 0.18 |
| Herne (yes vs. no, compared to Bochum) | 0.45 (0.12) | 0.00 |
| Time variables | ||
| Point of the survey (2017, compared to 2016) | −0.16 (0.06) | 0.01 |
| Months in Germany (per additional month) | 0.00 (0.00) | 0.25 |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Claassen, K.; Jäger, P. Impact of the Introduction of the Electronic Health Insurance Card on the Use of Medical Services by Asylum Seekers in Germany. Int. J. Environ. Res. Public Health 2018, 15, 856. https://doi.org/10.3390/ijerph15050856
Claassen K, Jäger P. Impact of the Introduction of the Electronic Health Insurance Card on the Use of Medical Services by Asylum Seekers in Germany. International Journal of Environmental Research and Public Health. 2018; 15(5):856. https://doi.org/10.3390/ijerph15050856
Chicago/Turabian StyleClaassen, Kevin, and Pia Jäger. 2018. "Impact of the Introduction of the Electronic Health Insurance Card on the Use of Medical Services by Asylum Seekers in Germany" International Journal of Environmental Research and Public Health 15, no. 5: 856. https://doi.org/10.3390/ijerph15050856
APA StyleClaassen, K., & Jäger, P. (2018). Impact of the Introduction of the Electronic Health Insurance Card on the Use of Medical Services by Asylum Seekers in Germany. International Journal of Environmental Research and Public Health, 15(5), 856. https://doi.org/10.3390/ijerph15050856





