Effects of Mind-Body Exercises for Mood and Functional Capabilities in Patients with Stroke: An Analytical Review of Randomized Controlled Trials
Abstract
:1. Introduction
2. Methods
2.1. Search Strategy
2.2. Inclusion Criteria and Study Selection
2.3. Data Extraction from Eligible Randomized Controlled Trials
2.4. Methodological Quality Assessment
2.5. Data Synthesis
3. Results
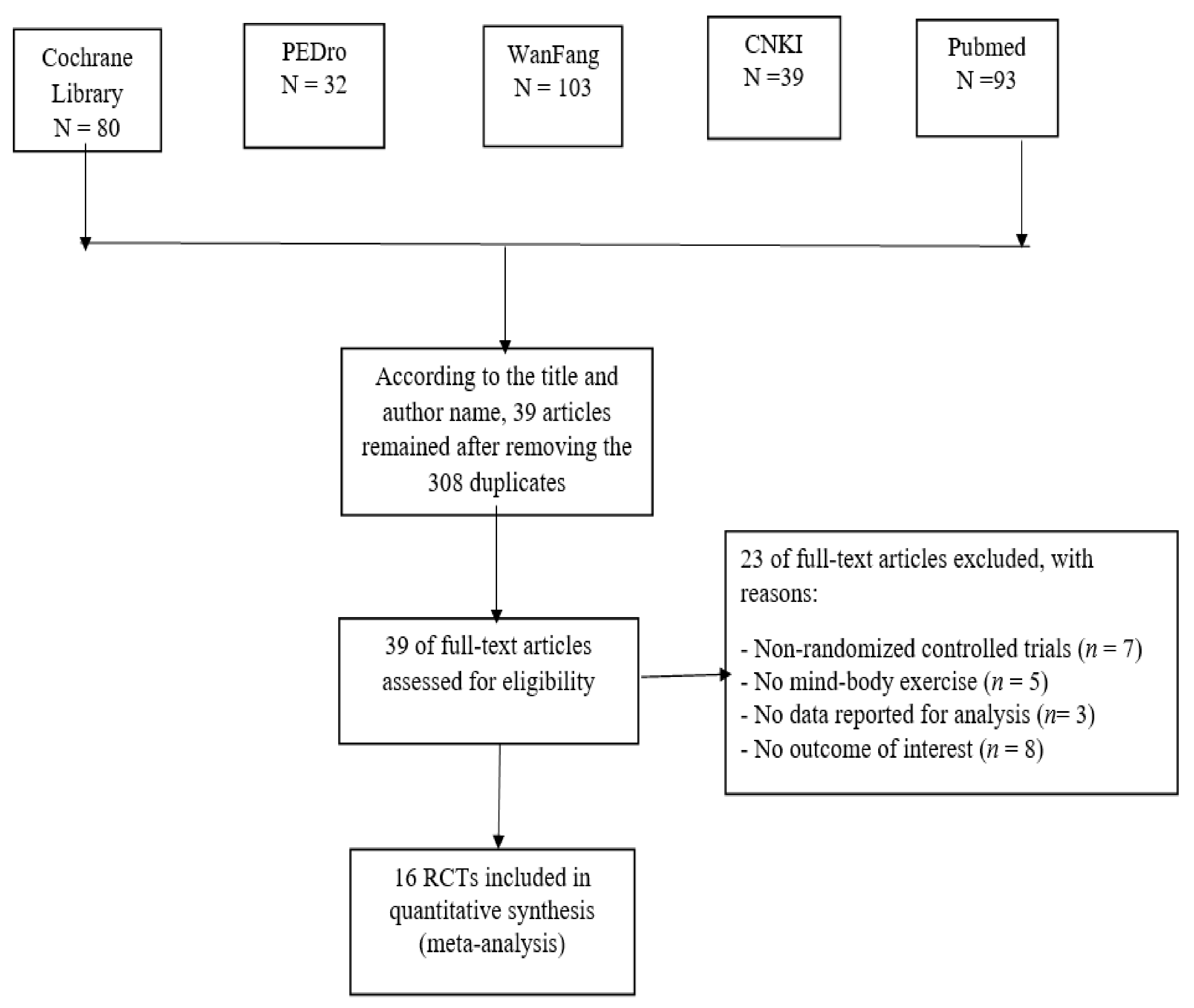
3.1. Literature Search
3.2. Study Characteristics
3.3. Methodological Quality
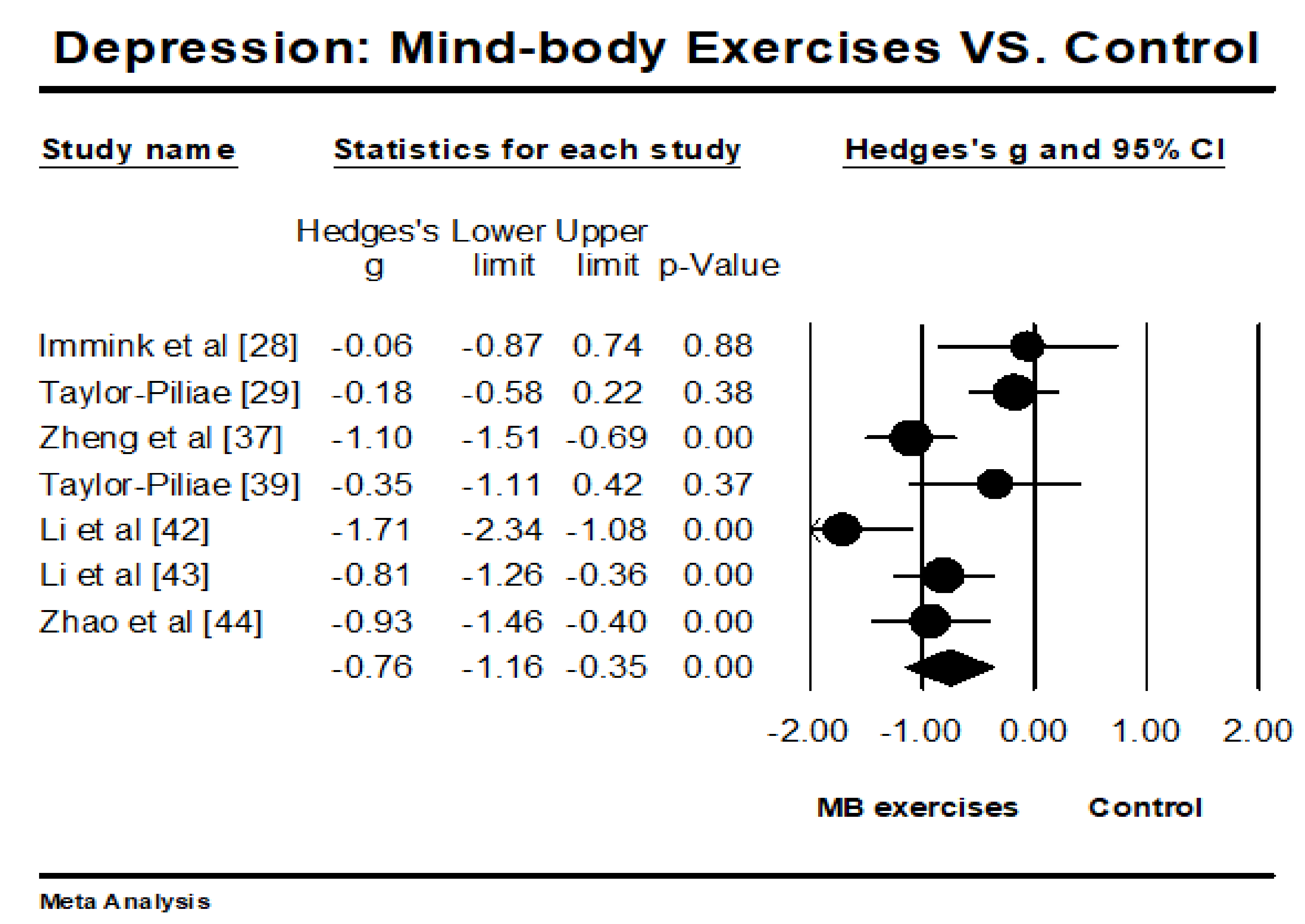
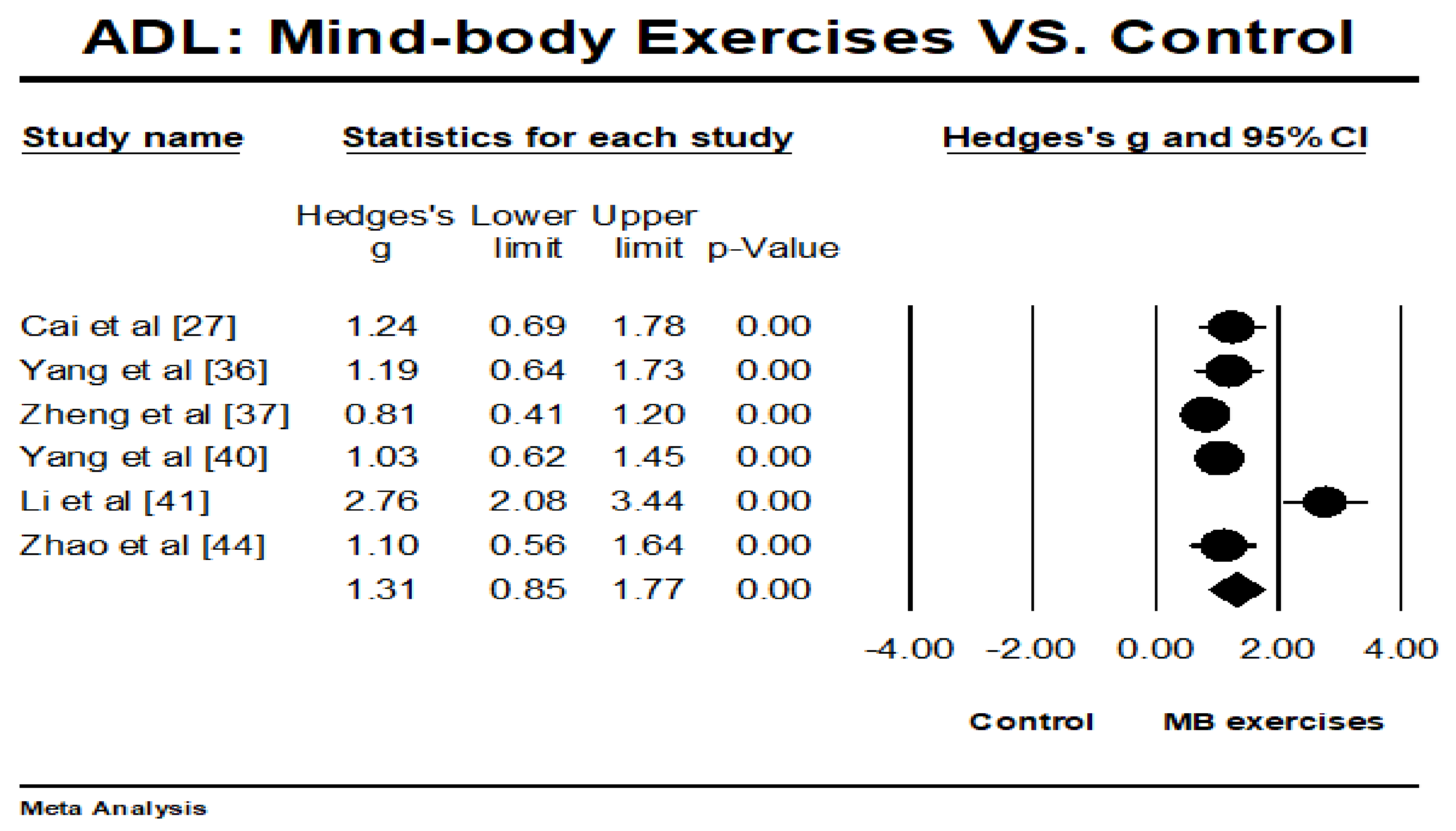
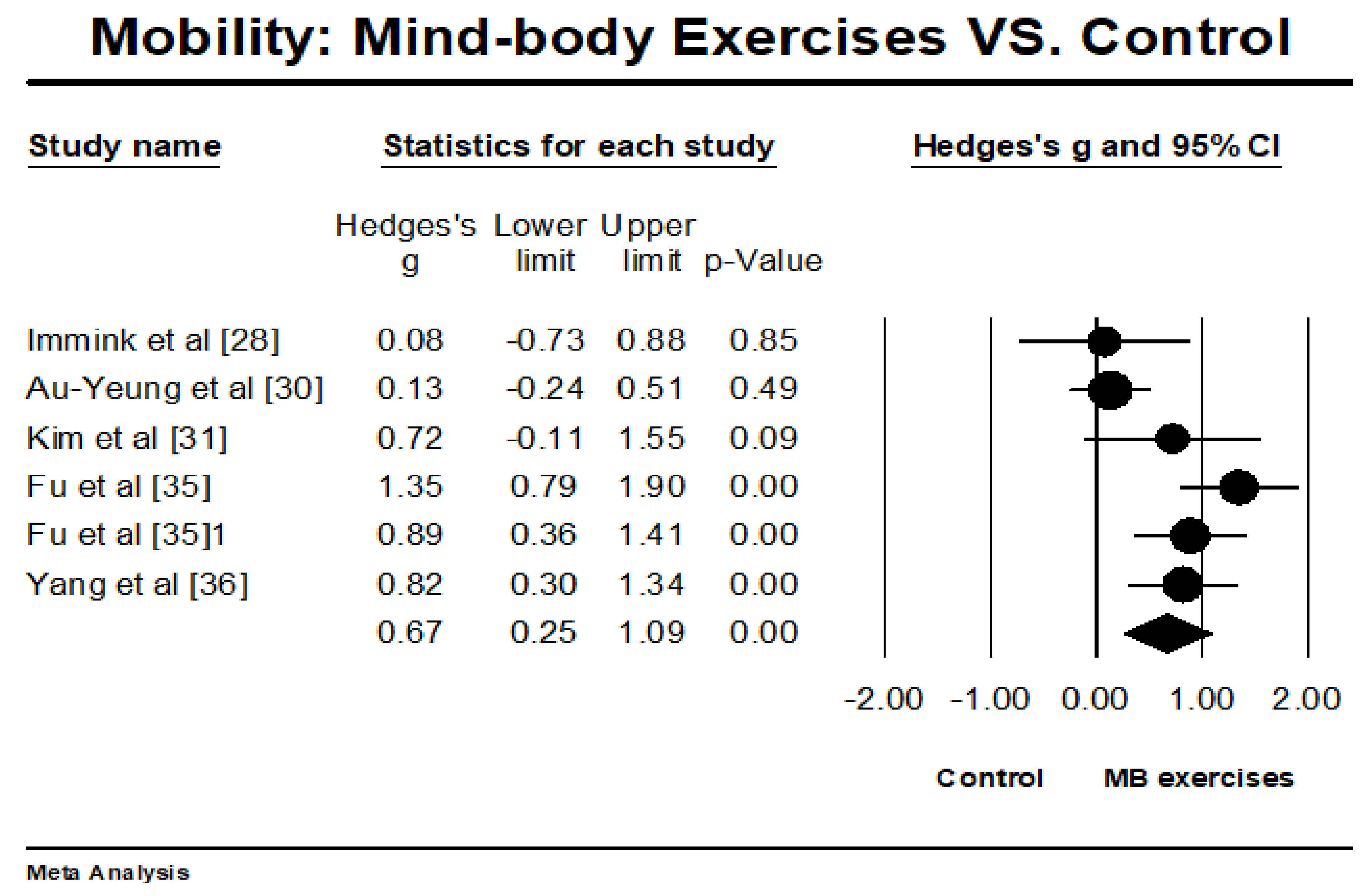
3.4. Meta-Analysis of Outcome Measured
4. Discussion
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Hall, S.; DeFrances, C. Hospitalization for Stroke in U.S. Hospitals, 1989–2009; National Center for Health Statistics: Hyattsville, MD, USA, 2012.
- Benjamin, J.; Blaha, J.; Chiuve, S.; Cushman, M.; Das, S.; De Ferranti, S.; Floyd, J.; Fornage, M.; Gillespie, C.; On Behalf of the American Heart Association Statistics Committee and Stroke Statistics Subcommittee; et al. Heart disease and stroke statistics—2017 update: A report from the American Heart Association. Circulation 2017, 135, e229–e445. [Google Scholar] [CrossRef] [PubMed]
- Wang, D. China Stroke Prevention Report; Peking Union Medical College Press: Beijing, China, 2015. [Google Scholar]
- Jette, D.U.; Latham, N.K.; Smout, R.J.; Gassaway, J.; Slavin, M.D.; Horn, S.D. Physical Therapy Interventions for Patients with Stroke in Inpatient Rehabilitation Facilities. Phys. Ther. 2005, 85, 238–248. [Google Scholar] [PubMed]
- Sivan, M.; Gallagher, J.; Makower, S.; Keeling, D.; Bhakta, B.; O’Connor, R.J.; Levesley, M. Home-based computer assisted arm rehabilitation (hCAAR) robotic device for upper limb exercise after stroke: Results of a feasibility study in home setting. J. Neuroeng. Rehabil. 2014, 11, 163. [Google Scholar] [CrossRef] [PubMed]
- Morone, G.; Paolucci, S.; Cherubini, A.; De Angelis, D.; Venturiero, V.; Coiro, P.; Iosa, M. Robot-assisted gait training for stroke patients: Current state of the art and perspectives of robotics. Neuropsychiatr. Dis. Treat. 2017, 13, 1303–1311. [Google Scholar] [CrossRef] [PubMed]
- Chang, W.; Kim, Y. Robot-assisted Therapy in Stroke Rehabilitation. J. Stroke 2013, 15, 174–181. [Google Scholar] [CrossRef] [PubMed]
- Gordon, F.; Gulanick, M.; Costa, F.; Fletcher, G.; Franklin, B.; Roth, E.; Shephard, T. Physical activity and exercise recommendations for stroke survivors: An American Heart Association scientific statement from the Council on Clinical Cardiology, Subcommittee on Exercise, Cardiac Rehabilitation, and Prevention; the Council on Cardiovascular Nursing; the Council on Nutrition, Physical Activity, and Metabolism; and the Stroke Council. Circulation 2004, 109, 2031–2041. [Google Scholar] [PubMed]
- Lan, C.; Lai, J.; Chen, S. Tai Chi Chuan: Tai Chi Chuan: An ancient wisdom on exercise and health promotion. Sports Med. 2002, 32, 217–224. [Google Scholar] [CrossRef] [PubMed]
- Van Duijnhoven, H.; Heeren, A.; Peters, M.; Veerbeek, J.; Kwakkel, G.; Geurts, A.; Weerdesteyn, V. Effects of Exercise Therapy on Balance Capacity in Chronic Stroke: Systematic Review and Meta-Analysis. Stroke 2016, 47, 2603–2610. [Google Scholar] [CrossRef] [PubMed]
- Lubetzky-Vilnai, A.; Kartin, D. The Effect of balance training on balance performance in individuals post-stroke: A Systematic Review. J. Neurol. Phys. Ther. 2010, 34, 127–137. [Google Scholar] [CrossRef] [PubMed]
- Vanderbeken, I.; Kerckhofs, E. Select this result for bulk action: A systematic review of the effect of physical exercise on cognition in stroke and traumatic brain injury patients. NeuroRehabilitation 2017, 40, 33–48. [Google Scholar] [CrossRef] [PubMed]
- Kim, S.; Choi-Kwon, S. Post-stroke depression and emotional incontinence: Correlation with lesion location. Neurology 2000, 54, 1805–1810. [Google Scholar] [CrossRef] [PubMed]
- Niall, M.; Terence, J.; Azmil, A.; Matthew, W.; Jonathan, E. Depression and anxiety symptoms post-stroke/TIA: Prevalence and associations in cross-sectional data from a regional stroke registry. BMC Neurol. 2014, 14, 198. [Google Scholar]
- Almeida, O.; Xiao, J. Mortality associated with incident mental health disorders after stroke. Aust. N. Z. J. Psychiatry 2007, 41, 274–281. [Google Scholar] [CrossRef] [PubMed]
- Zou, L.; Pan, Z.; Yeung, A.; Talwar, S.; Wang, C.; Liu, Y.; Shu, Y.; Chen, X.; Thomas, G. A Review Study on the Beneficial Effects of Baduanjin. J. Altern. Complement. Med. 2017. [Google Scholar] [CrossRef] [PubMed]
- Zou, L.; SasaKi, J.; Wang, H.; Xiao, Z.; Fang, Q.; Zhang, M. A Systematic Review and Meta-Analysis Baduanjin Qigong for Health Benefits: Randomized Controlled Trials. Evid. Based Complement. Altern. Med. 2017, 2017, 4548706. [Google Scholar] [CrossRef] [PubMed]
- Zou, L.; Wang, C.; Chen, K.; Shu, Y.; Chen, X.; Luo, L.; Zhao, X. The Effect of Taichi Practice on Attenuating Bone Mineral Density Loss: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. Int. J. Environ. Res. Public Health 2017, 14, 1000. [Google Scholar] [CrossRef] [PubMed]
- Zou, L.; Wang, H.; Xiao, Z.; Fang, Q.; Zhang, M.; Li, T.; Du, G.; Liu, Y. Tai chi for health benefits in patients with multiple sclerosis: A systematic review. PLoS ONE 2017, 12, e0170212. [Google Scholar] [CrossRef] [PubMed]
- Lou, L.; Zou, L.; Fang, Q.; Wang, H.; Liu, Y.; Tian, Z.; Han, Y. Effect of Taichi Softball on Function-Related Outcomes in Older Adults: A Randomized Control Trial. Evid. Based Complement. Altern. Med. 2017, 2017, 4585424. [Google Scholar] [CrossRef] [PubMed]
- Zou, L.; Wang, C.; Wang, H. Effect of a long-term modified Tai Chi-based intervention in attenuating bone mineral density in postmenopausal women in southeast China: Study protocol for a randomized controlled trial. Clin. Trials Degener. Dis. 2017, 2, 46–55. [Google Scholar]
- Zou, L.; Wang, H.; Li, T.; Shu, Y.; Wang, C. Traditional Chinese exercise intervention improves symptoms in a patient with ankylosing spondylitis: A case study. Int. J. Adv. Res. 2017, 5, 888–895. [Google Scholar] [CrossRef]
- Zou, L.; Wang, H.; Li, T.; Lu, L. Effect of Health-Qigong on spinal mobility and disease activity in people with ankylosing spondylitis. Trav. Hum. 2017, 80, 1585–1598. [Google Scholar]
- Yeung, A.; Chan, J.; Cheung, J.; Zou, L. Qigong and Tai-Chi. For mood regulation. Focus-Am. Psychiatr. Publ. 2018, 16, 40–47. [Google Scholar] [CrossRef]
- Zou, L.; Wang, C.; Tian, Z.; Wang, H.; Shu, Y. Effect of Yang-Style Tai Chi on Gait Parameters and Musculoskeletal Flexibility in Healthy Chinese Older Women. Sports 2017, 5, 52. [Google Scholar] [CrossRef]
- Kachan, D.; Olano, H.; Tannenbaum, S.; Annane, D.; Mehta, A.; Arheart, K.; Fleming, L.; Yang, X.; McClure, L.; Lee, D. Prevalence of Mindfulness Practices in the U.S. Workforce: National Health Interview Survey. Prev. Chronic Dis. 2017, 14, 160034. [Google Scholar] [CrossRef] [PubMed]
- Cai, W.; Liang, C. Effects of sitting Baduanjin on the ability of activities daily living of patients with stroke sequelae in community. J. Nurs. Adm. 2011, 11, 810–811. [Google Scholar]
- Immink, M.; Hillier, S.; Petkov, J. Randomized controlled trial of yoga for chronic poststroke hemiparesis: Motor function, mental health, and quality of life outcomes. Top. Stroke Rehabil. 2014, 21, 256–271. [Google Scholar] [CrossRef] [PubMed]
- Taylor-Piliae, R.; Hoke, T.; Hepworth, J.; Latt, L.; Najafi, B.; Coull, B. Effect of Tai Chi on physical function, fall rates and quality of life among older stroke survivors. Arch. Phys. Med. Rehabil. 2014, 95, 816–824. [Google Scholar] [CrossRef] [PubMed]
- Au-Yeung, S.; Hui-Chan, C.; Tang, J. Short-form Tai Chi improves standing balance of people with chronic stroke. Neurorehabil. Neural Repair 2009, 23, 515–522. [Google Scholar] [CrossRef] [PubMed]
- Kim, H.; Kim, Y.; Lee, S. Effects of therapeutic Tai Chi on balance, gait, and quality of life in chronic stroke patients. Int. J. Rehabil. Res. 2015, 38, 156–161. [Google Scholar] [CrossRef] [PubMed]
- Wang, W.; Sawada, M.; Noriyama, Y.; Arita, K.; Ota, T.; Sadamatsu, M.; Kiyotou, R.; Hirai, M.; Kishimoto, T. Tai Chi exercise versus rehabilitation for the elderly with cerebral vascular disorder: A single-blinded randomized controlled trial. Psychogeriatrics 2010, 10, 160–166. [Google Scholar] [CrossRef] [PubMed]
- Zou, L.; Yeung, A.; Quan, X.; Hui, S.; Hu, X.; Chan, J.; Wang, C.; Boyden, S.; Sun, L.; Wang, H. Mindfulness-based Baduanjin exercise for depression and anxiety in people with physical or mental illnesses: A Systematic Review and Meta-analysis of randomized controlled trials. Int. J. Environ. Res. Public Health 2018, 15, 321. [Google Scholar] [CrossRef] [PubMed]
- Zou, L.; Yeung, A.; Quan, X.; Wang, H. A Systematic review and Meta-analysis of Mindfulness-based (Baduanjin) exercise for alleviating musculoskeletal pain and improving sleep quality in people with chronic diseases. Int. J. Environ. Res. Public Health 2018, 15, 206. [Google Scholar] [CrossRef] [PubMed]
- Fu, C.; Zhang, Q. Effects of Taijiquan on balance function and walking ability of stroke hemiplegic patients in convalescent phase. J. Rehabil. Med. 2016, 31, 536–539. [Google Scholar]
- Yang, H.; Tang, Q. Effects of Tai Chi Quan on motor function among stroke survivors. Chin. J. Rehabil. Med. Res. 2016, 31, 1146–1148. [Google Scholar]
- Zheng, W.; Zhang, Y.; Jiang, X.; Chen, R.; Xiao, W. Effects of persistent Tai Chi exercise on rehabilitation in ischemic stroke: A prospective randomized controlled trial. J. Integr. Chin. Med. 2015, 13, 304–307. [Google Scholar]
- Zhou, Q.; Xu, J.; Hu, A.; Jiang, W.; Wang, L.; Yang, L.; Yang, B.; Du, H. Observation on recover of cerebral infraction patients by TaijiQuan training. Chin. J. Pract. Nerv. Dis. 2010, 13, 20–22. [Google Scholar]
- Taylor-Piliae, R.; Coull, B. Community-based Yang-style Tai Chi is safe and feasible in chronic stroke: A pilot study. Clin. Rehabil. 2011, 26, 121–131. [Google Scholar] [CrossRef] [PubMed]
- Yang, Z.; Liu, D.; Chang, Y.; Sun, P.; Zhao, G.; Jia, L. The therapeutic effects of Tai Chi balance training for stroke with balance disorders. Contemp. Med. 2013, 19, 5–6. [Google Scholar]
- Li, X.; Yang, S.; Li, T.; Cai, S. The rehabilitative effects of Tai Chi motor imagery for stroke survivors. Fujian J. Trad. Chin. Med. 2011, 42, 5–6. [Google Scholar]
- Li, Y.; Hu, S.; Cui, L. Clinical observation on sitting Tai Chi exercise used for 30 cases of patients with depression after stroke. Chin. Nurs. Res. 2012, 26, 2254–2255. [Google Scholar]
- Li, Y.; Ling, H.; Wen, X. Application of sitting Tai Chi exercise in the rehabilitation training in patients with post-stoke depression. Qilu J. Nurs. 2013, 19, 4–6. [Google Scholar]
- Zhao, B.; Tang, Q.; Wang, Y.; Zhu, L.; Yang, H.; Ye, T. Effects of Taijiquan on motor function and depression in patients with post-stroke depression. Chin. J. Rehabil. Theory Pract. 2017, 23, 334–337. [Google Scholar]
- Saunders, D.; Sanderson, M.; Hayes, S.; Kilrane, M.; Greig, C.; Brazzelli, M.; Mead, G. Physical fitness training for stroke patients. Cochrane Database Syst. Rev. 2016, 24, cd003316. [Google Scholar] [CrossRef] [PubMed]
- Matos, L.; Sousa, C.; Gonçalves, M.; Gabriel, J.; Machado, J.; Greten, H. Qigong as a Traditional Vegetative Biofeedback Therapy: Long-term conditioning of physiological mind-body effects. BioMed Res. Int. 2015, 2015, e531789. [Google Scholar] [CrossRef] [PubMed]
- Oken, B.; Zajdel, D.; Kishiyama, S.; Flegal, K.; Dehen, C.; Haas, M.; Kraemer, D.; Lawrence, J.; Leyva, J. Randomized, controlled, six-month trial of yoga in healthy seniors: Effects on cognition and quality of life. Altern. Ther. Health Med. 2006, 12, 40–47. [Google Scholar] [PubMed]
- Garrett, R.; Immink, M.; Hillier, S. Becoming connected: The lived experience of yoga participation after stroke. Disabil. Rehabil. 2011, 33, 2404–2415. [Google Scholar] [CrossRef] [PubMed]
- Payne, P.; Crane-Godreau, M. Meditative movement for depression and anxiety. Front. Psychiatry 2013, 24, 71. [Google Scholar] [CrossRef] [PubMed]
| Reference | Participant Characteristics | Mind-Body Intervention | ||||||
|---|---|---|---|---|---|---|---|---|
| ISZ (AT) MB/CG | Mean Age or Age Range | Course of Disease | Ischemic/Hemorrhage | Training Frequency and Length (MB Component) | Training Mode | Outcomes/Instrument | FU | |
| Cai et al. [27], China | 60 (0%) 30/30 | MB: 60.27 (10.48) CG: 61.27 (7.42) | MB: 29.7 (7.38) wk CG: 28.81 (5.37) wk | MB: 21/9 CG: 24/6 | MB: 30 min × 4–5 sessions/wk, 12 wks (Baduanjin qigong) + educational program; CG: educational program | Group | Activities of daily living (Barthel Scale) | No |
| Immink et al. [28], Austria | 25 (12%) 12/13 | MB: 56.1 (13.6) CG: 63.2 (17.4) | MB: 81.6 (77.5) M CG: 23.3 (12.5) M | NR | MB: 90 min × 1 session/wk (group-based), 10 wks + 6 × 40 min/session (individual) (yoga); CG: no treatment | Mixed | mobility (2-MWD), depression (GDS), anxiety (STAI) | No |
| Taylor-Piliae [29], USA | 145 (10%) MB: 53 CG1: 44 CG2: 48 | MB: 71.5 (10.3) CG1: 69.6 (9.4) CG2: 68.2 (10.3) | MB: 39 (40.2) M CG1: 33 (58.7) M CG2: 38.7 (46.7) M | MB: 33/12 CG1: 32/8 CG2: 30/14 16 unknown | MB: 60 min × 3 sessions/wk, 12 wks (24-style tai chi); CG1: strength and range of movement exercises; CG2: weekly phone call | Group | depression (CES-D), sleep quality (PSQI) | No |
| Au-Yeung et al. [30], China | 136 (16%) 74/62 | MB: 61.7 (10.5) CG: 65.9 (10.7) | MB: 54.1 (79.2) M CG: 64.2 (106.4) M | NR | MB: 60 min × 1 session/wk (group) + 60 min × 3 sessions/wk (self-practice), 12 wks (simplified tai chi); CG: General exercises rehabilitation | Mixed | mobility (TUG) | 6-wk |
| Kim et al. [31], Korea | 24 (8%) 12/12 | MB: 53.45 (11.54) CG: 55.18 (10.2) | NR | NR | MB: 60 min × 2 sessions/wk, 6 wks (simplified tai chi) + (general rehabilitation + physical therapy); CG: general rehabilitation + physical therapy | Group | mobility (TUG) | No |
| Wang et al. [32], Japan | 34 (14.7%) 17/17 | MB: 76.53 (9.74) CG: 77.59 (12.33) | NR | NR | MB: 50 min × 1 session/wk, 12 wks (24-style tai chi) + usual treatment; CG: Usual treatment and exercise rehabilitation | Group | sleep quality (PSQI) | No |
| Fu et al. [35], China | 60 (0%) 30/30 | MB: 59.7 (7.6) CG: 60.3 (8.4) | Less than 3 months | MB: 13/17 CG: 10/20 | MB: 15 min × 6 sessions/wk, 8 wks (24-style tai chi) + General rehabilitation CG: General rehabilitation | Individual | mobility (FAC) | No |
| Yang et al. [36], China | 60 (0%) 30/30 | MB: 58 (11.27) CG: 60.07 (7.87) | NR | NR | MB: 15 min × 7 sessions/wk, 4 wks (Tai Chi balance training) + General rehabilitation; CG: General rehabilitation | NR | mobility (FAC), Activities of daily living (Barthel Scale) | No |
| Zheng et al. [37], China | 112 (5%) 56/56 | MB: 59 (13) CG: 60 (12) | NR | 112/0 | MB: 60 min × unclear, 12 wks (tai chi) + General rehabilitation; CG: General rehabilitation | NR | Activities of daily living (Barthel Scale), anxiety (HAMA), depression (HAMB) | 12-M |
| Zhou et al. [38], China | 68 (0%) 34/34 | 65.2 (8.5) for all participants | NR | 0/68 | MB: unclear × 2 sessions/wk, 4 wks (24-style tai chi) + General rehabilitation; CG: General rehabilitation + drug treatment | NR | anxiety (HAMA) | No |
| Taylor-Piliae et al. [39], China | 28 (11%) 16/12 | MB: 72.8 (10.1) CG: 64.5 (10.9) | MB: 58.3 (46.7) M CG: 47.9 (42.5) M | MB: 12/4 CG: 9/3 | MB: 60 min × 3 sessions/wk, 12 wks (24-style tai chi); CG: usual treatment | Group | depression (CES-D), sleep quality (PSQI) | No |
| Yang et al. [40], China | 100 (0%) 50/50 | MB: 54.3 (13.8) CG: 55.2 (14.6) | MB: 44.7 (18.4) d CG: 42.6 (16.7) d | unable to identify | MB: 45 min × 6 sessions/wk, 4 wks (tai chi balance training); CG: exercise rehabilitation | NR | activity of daily living (Barthel Scale) | No |
| Li et al. [41], China | 67 (0%) 35/32 | MB: 56 (5.58) CG: 54 (6.23) | NR | NR | MB: 30–35 min × 5 sessions/wk, 6 wks (tai chi motor imagery) + General rehabilitation; CG: General rehabilitation | Individual | activities of daily living (Barthel Scale) | No |
| Li et al. [42], China | 68 (12%) 36/32 | 38–76 years | NR | NR | MB: 30 min × 2 sessions/wk, 5 wks (sitting-style tai chi) + usual nursing; CG: usual nursing | Group | Depression (HAMB) | No |
| Li et al. [43], China | 89 (10%) 47/42 | 33–78 years | 2 wks or below | NR | MB: 30 min × 2 sessions/wk, 5 wks (sitting-style tai chi) + usual nursing; CG: usual nursing | Group | Depression (HAMB) | No |
| Zhao et al. [44], China | 60 (0%) 30/30 | MB: 53.85 (11.69) CG: 51.38 (14.83) | MB: 40.58 (23.11) d CG: 42.16 (19.82) d | NR | MB: 30 min × 5 sessions/wk, 8 wks (simplified three-form tai chi) + General rehabilitation; CG: General rehabilitation | Group | Depression (HAMB), activities of daily living (Barthel Scale) | No |
| Author [Reference] | Item 1 | Item 2 | Item 3 | Item 4 | Item 5 | Item 6 | Item 7 | Item 8 | Item 9 | Score |
|---|---|---|---|---|---|---|---|---|---|---|
| Cai et al. [27] | 1 | 0 | 1 | 0 | 1 | 1 | 1 | 1 | 1 | 7/9 |
| Immink et al. [28] | 1 | 1 | 1 | 1 | 1 | 0 | 1 | 1 | 1 | 8/9 |
| Taylor-Piliae et al. [29] | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 9/9 |
| Au-Yeung et al. [30] | 1 | 0 | 1 | 1 | 0 | 1 | 1 | 1 | 1 | 7/9 |
| Kim et al. [31] | 1 | 0 | 1 | 0 | 1 | 0 | 1 | 1 | 1 | 6/9 |
| Wang et al. [32] | 1 | 0 | 1 | 1 | 1 | 0 | 1 | 1 | 1 | 7/9 |
| Fu et al. [35] | 1 | 0 | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 8/9 |
| Yang et al. [36] | 1 | 0 | 0 | 0 | 1 | 1 | 1 | 1 | 1 | 6/9 |
| Zheng et al. [37] | 1 | 0 | 1 | 0 | 1 | 0 | 1 | 1 | 1 | 6/9 |
| Zhou et al. [38] | 1 | 0 | 1 | 0 | 1 | 1 | 1 | 1 | 1 | 7/9 |
| Taylor-Piliae et al. [39] | 1 | 1 | 1 | 1 | 1 | 0 | 0 | 1 | 1 | 7/9 |
| Yang et al. [40] | 1 | 0 | 1 | 0 | 1 | 1 | 1 | 1 | 1 | 7/9 |
| Li et al. [41] | 1 | 0 | 1 | 0 | 1 | 0 | 1 | 1 | 1 | 6/9 |
| Li et al. [42] | 1 | 0 | 1 | 0 | 1 | 0 | 1 | 0 | 1 | 5/9 |
| Li et al. [43] | 1 | 0 | 1 | 0 | 1 | 0 | 1 | 0 | 1 | 5/9 |
| Zhao et al. [44] | 1 | 0 | 1 | 0 | 1 | 1 | 1 | 1 | 1 | 7/9 |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Zou, L.; Yeung, A.; Zeng, N.; Wang, C.; Sun, L.; Thomas, G.A.; Wang, H. Effects of Mind-Body Exercises for Mood and Functional Capabilities in Patients with Stroke: An Analytical Review of Randomized Controlled Trials. Int. J. Environ. Res. Public Health 2018, 15, 721. https://doi.org/10.3390/ijerph15040721
Zou L, Yeung A, Zeng N, Wang C, Sun L, Thomas GA, Wang H. Effects of Mind-Body Exercises for Mood and Functional Capabilities in Patients with Stroke: An Analytical Review of Randomized Controlled Trials. International Journal of Environmental Research and Public Health. 2018; 15(4):721. https://doi.org/10.3390/ijerph15040721
Chicago/Turabian StyleZou, Liye, Albert Yeung, Nan Zeng, Chaoyi Wang, Li Sun, Garrett Anthony Thomas, and Huiru Wang. 2018. "Effects of Mind-Body Exercises for Mood and Functional Capabilities in Patients with Stroke: An Analytical Review of Randomized Controlled Trials" International Journal of Environmental Research and Public Health 15, no. 4: 721. https://doi.org/10.3390/ijerph15040721
APA StyleZou, L., Yeung, A., Zeng, N., Wang, C., Sun, L., Thomas, G. A., & Wang, H. (2018). Effects of Mind-Body Exercises for Mood and Functional Capabilities in Patients with Stroke: An Analytical Review of Randomized Controlled Trials. International Journal of Environmental Research and Public Health, 15(4), 721. https://doi.org/10.3390/ijerph15040721






