Patterns of Signs That Telephone Crisis Support Workers Associate with Suicide Risk in Telephone Crisis Line Callers
Abstract
1. Introduction
1.1. Signs That Suicidality Might Be Present
1.2. The Role of Pattern Recognition in Identifying the Risk That a Caller Might Be Suicidal
1.3. The Influence of Callers’ Gender When Identifying Suicide Risk
1.4. The Influence of Telephone Crisis Workers’ Own Gender When Identifying Suicide Risk
1.5. The Current Study
2. Methods
2.1. Participants
2.2. Design
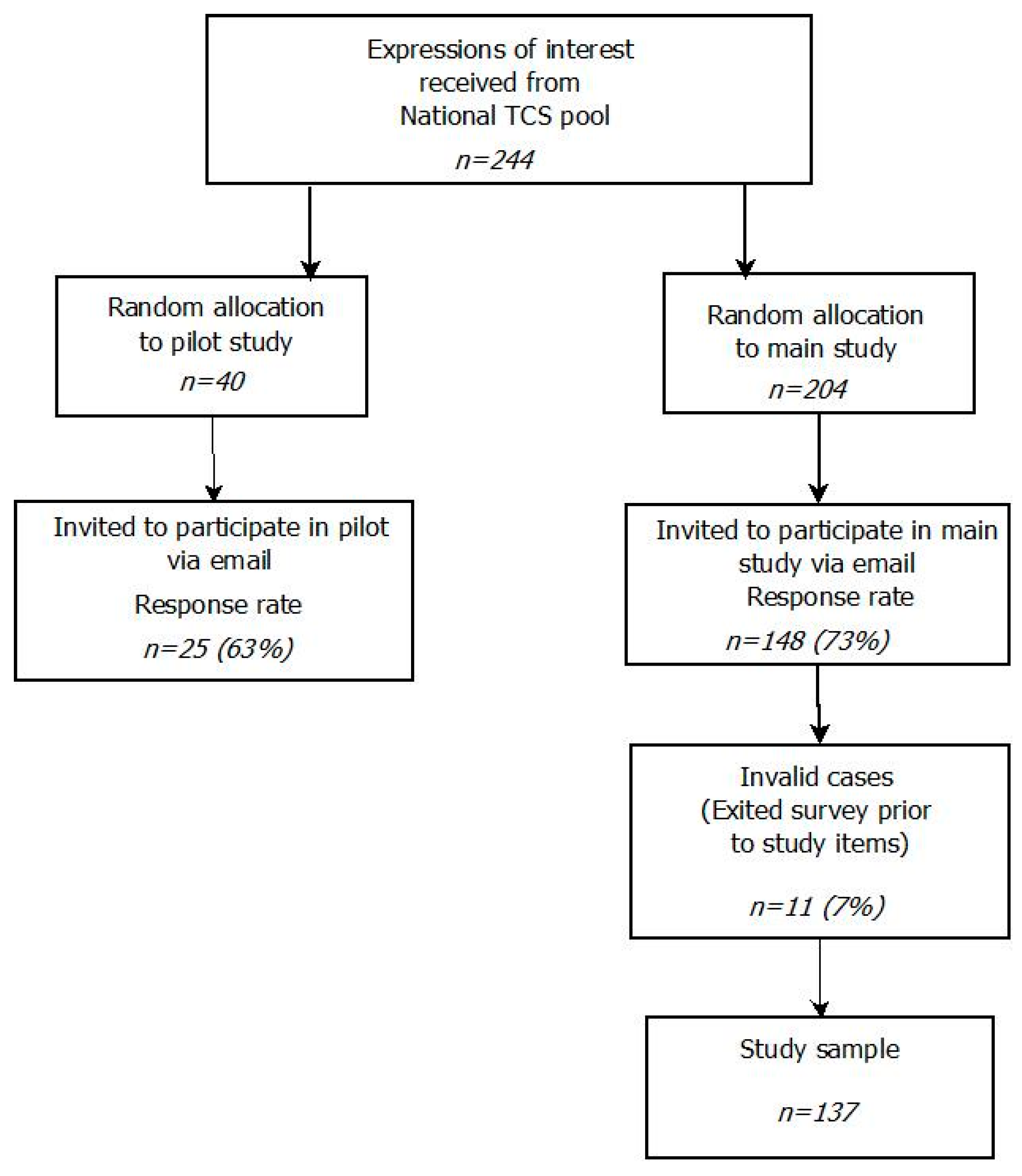
2.2.1. Recruitment
2.2.2. Main Study Procedure
2.3. Measures
2.4. Data Screening and Analysis
3. Results
4. Discussion
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Covington, D.; Hovan, M. Suicide Care in Systems Framework; National Action Alliance Clinical Care & Intervention Task Force: Washington, DC, USA, 2011. [Google Scholar]
- Gould, M.S.; Lake, A.M.; Munfakh, J.L.; Galfalvy, H.C.; Kleinman, M.; Williams, C.; Glass, A.; McKeon, R. Helping callers to the National Suicide Prevention Lifeline who are at imminent risk for suicide: Evaluation of caller risk profiles and interventions implemented. Suicide Life-Threat. Behav. 2016, 46, 172–190. [Google Scholar] [CrossRef] [PubMed]
- Gould, M.S.; Kalafat, J.; Harrismunfakh, J.; Kleinman, M. An evaluation of crisis hotline outcomes. Part 2: Suicidal callers. Suicide Life. Threat. Behav. 2007, 37, 338–352. [Google Scholar] [CrossRef] [PubMed]
- Bryan, C.J.; Rudd, M.D. The importance of temporal dynamics in the transition from suicidal thought to behavior. Clin. Psychol. Sci. Pract. 2016, 23, 21–25. [Google Scholar] [CrossRef]
- Deisenhammer, E.A.; Ing, C.; Strauss, R.; Kemmler, G.; Hinterhuber, H.; Weiss, E.M. The duration of the suicidal process: How much time is left for intervention between consideration and accomplisment of a suicide attempt? J. Clin. Psychiatry 2009, 70, 19–23. [Google Scholar] [CrossRef] [PubMed]
- Kattimani, S.; Sarkar, S.; Menon, V.; Muthuramalingam, A.; Nancy, P. Duration of suicide process among suicide attempters and characteristics of those providing window of opportunity for intervention. J. Neurosci. Rural Pract. 2016, 7. [Google Scholar] [CrossRef]
- Woodward, W.; Wyllie, C. Helplines, tele-web support services, and suicide prevention. In The International Handbook of Suicide Prevention; O’Connor, R.C., Pirkis, J., Eds.; John Wiley & Sons, Ltd.: Chichester, UK, 2016; pp. 490–504. [Google Scholar]
- Pirkis, J.; Middleton, A.; Bassilios, B.; Harris, M.; Spittal, M.J.; Fedszyn, I.; Chondros, P.; Gunn, J. Frequent callers to telephone helplines: New evidence and a new service model. Int. J. Ment. Health Syst. 2016, 10. [Google Scholar] [CrossRef] [PubMed]
- Coman, G.J.; Burrows, G.D.; Evans, B.J. Telephone counselling in Australia: Applications and considerations for use. J. Guid. Couns. 2001, 29, 247–258. [Google Scholar] [CrossRef]
- Lester, D. The unique qualities of telephone therapy. Psychother. Theory, Res. Pract. 1974, 11, 219–221. [Google Scholar] [CrossRef]
- Hunt, T.; Wilson, C.J.; Woodward, A.; Caputi, P.; Wilson, I. Intervention among suicidal men: Future directions for telephone crisis support research. Front. Public Ment. Heal. 2018. [Google Scholar] [CrossRef]
- Krysinska, K.; De Leo, D. Telecommunication and suicide prevention: Hopes and challenges for the new century. OMEGA J. Death Dying 2007, 55, 237–253. [Google Scholar] [CrossRef] [PubMed]
- Jollant, F.; Lawrence, N.L.; Olié, E.; Guillaume, S.; Courtet, P. The suicidal mind and brain: A review of neuropsychological and neuroimaging studies The suicidal mind and brain. World J. Biol. Psychiatry 2011, 12, 319–339. [Google Scholar] [CrossRef] [PubMed]
- Keilp, J.G.; Gorlyn, M.; Russell, M.; Oquendo, M.A.; Burke, A.K.; Harkavy-Friedman, J.; Mann, J.J. Neuropsychological function and suicidal behavior: Attention control, memory and executive dysfunction in suicide attempt. Psychol. Med. 2013, 43, 539–551. [Google Scholar] [CrossRef] [PubMed]
- Wilson, C.J.; Thomas, S.D.M.; Furlong, S.T. Help-negation. In Encyclopedia of Adolescence; Levesque, R.J.R., Ed.; Springer International Publishing: Cham, Switzerland, 2017; pp. 140–142. [Google Scholar]
- Wilson, C.J. A caution for suicide prevention focused on help-seeking in young people. Aust. N. Z. J. Psychiatry 2017, 51, 1255. [Google Scholar] [CrossRef] [PubMed]
- Rudd, M.D. Suicide warning signs in clinical practice. Curr. Psychiatry Rep. 2008, 10, 87–90. [Google Scholar] [CrossRef] [PubMed]
- Rudd, M.D.; Berman, A.L.; Joiner, T.E.; Nock, M.K.; Silverman, M.M.; Mandrusiak, M.; Van Orden, K.; Witte, T. Warning signs for suicide: Theory, research, and clinical applications. Suicide Life. Threat. Behav. 2006, 36, 255–262. [Google Scholar] [CrossRef] [PubMed]
- Pompili, M.; Murri, M.B.; Patti, S.; Innamorati, M.; Lester, D.; Girardi, P.; Amore, M. The communication of suicidal intentions: A meta-analysis. Psychol. Med. 2016, 46, 2239–2253. [Google Scholar] [CrossRef] [PubMed]
- Tucker, R.P.; Crowley, K.J.; Davidson, C.L.; Gutierrez, P.M. Risk factors, warning signs, and drivers of suicide: What are they, how do they differ, and why does it matter? Suicide Life-Threat. Behav. 2015. [Google Scholar] [CrossRef] [PubMed]
- Loveday, T.; Wiggins, M.; Festa, M.; Schelll, D.; Twigg, D. Pattern recognition as an indicator of diagnostic expertise. In Pattern Recognition: Applications and Methods; Carmona, P.L., Sánchez, J.S., Fred, A.L.N., Eds.; Springer: Berlin/Heidelberg, Germany, 2013; pp. 1–11. [Google Scholar]
- Klein, G. A naturalistic decision making perspective on studying intuitive decision making. J. Appl. Res. Mem. Cogn. 2015, 4, 164–168. [Google Scholar] [CrossRef]
- Croskerry, P. A universal model of diagnostic reasoning. Acad. Med. 2009, 84, 1022–1028. [Google Scholar] [CrossRef] [PubMed]
- Croskerry, P. Clinical cognition and diagnostic error: Applications of a dual process model of reasoning. Adv. Health Sci. Educ. Theory Pract. 2009, 14, 27–35. [Google Scholar] [CrossRef] [PubMed]
- Campbell, S.G.; Croskerry, P.; Bond, W.F. Profiles in patient safety: A “perfect storm” in the emergency department. Acad. Emerg. Med. 2007, 14, 743–749. [Google Scholar] [PubMed]
- Tversky, A.; Kahneman, D. Judgment under Uncertainty: Heuristics and Biases. Science 1974, 185, 1124–1131. [Google Scholar] [CrossRef] [PubMed]
- Gigerenzer, G.; Gaissmaier, W. Heuristic Decision Making. Annu. Rev. Pscyhol. 2011, 62, 451–482. [Google Scholar] [CrossRef] [PubMed]
- LivingWorks. Available online: https://www.livingworks.net/ (accessed on 1 November 2017).
- Kitchener, B.A.; Jorm, A.F.; Kelly, C.M. Mental Health First Aid Manual, 4th ed.; Mental Health First Aid Australia: Melbourne, Australia, 2017. [Google Scholar]
- Jorm, A.F. Mental health literacy: Public knowledge and beliefs about mental disorders. Br. J. Psychiatry 2000, 177, 396–401. [Google Scholar] [CrossRef] [PubMed]
- Gould, M.S.; Jamieson, P.; Romer, D. Media contagion and suicide among the young. Am. Behav. Sci. 2003, 46, 1269–1284. [Google Scholar] [CrossRef]
- Connell, R.W. Masculinities, 2nd ed.; University of California Press: Oakland, CA, USA, 2005; ISBN 0520246985. [Google Scholar]
- Ridgeway, C.L.; Correll, S.J. Unpacking the gender system: A theoretical perspective on gender beliefs and social relations. Gend. Soc. 2004, 18, 510–531. [Google Scholar] [CrossRef]
- Connell, R. Gender, health and theory: Conceptualizing the issue, in local and world perspective. Soc. Sci. Med. 2012, 74, 1675–1683. [Google Scholar] [CrossRef] [PubMed]
- Canetto, S.S.; Sakinofsky, I. The gender paradox in suicide. Suicide Life. Threat. Behav. 1998, 28, 1–23. [Google Scholar] [PubMed]
- Johnston, A.K.; Pirkis, J.E.; Burgess, P.M. Suicidal thoughts and behaviours among Australian adults: Findings from the 2007 National Survey of Mental Health and Wellbeing. Aust. N. Z. J. Psychiatry 2009, 43, 635–643. [Google Scholar] [CrossRef] [PubMed]
- World Health Organisation. Preventing Suicide: A Global Imperative; World Health Organisation: Geneva, Switzerland, 2014. [Google Scholar]
- Jaworski, K. The gender-ing of suicide. Aust. Fem. Stud. 2010, 25, 47–61. [Google Scholar] [CrossRef]
- Scourfield, J.; Jacob, N.; Smalley, N.; Prior, L.; Greenland, K. Young people’s gendered interpretations of suicide and attempted suicide. Child Fam. Soc. Work 2007, 12, 248–257. [Google Scholar] [CrossRef]
- Cleary, A. Suicidal action, emotional expression, and the performance of masculinities. Soc. Sci. Med. 2012, 74, 498–505. [Google Scholar] [CrossRef] [PubMed]
- Fullagar, S.P.; O’Brien, W. Speaking of Suicide as a Gendered Problematic: Suicide Attempts and Recovery within Women’s Narratives of Depression. In Critical Suicidology: Transforming Suicide Research and Prevention for the 21st Century; Hume White, J., Marsh, I., Michael, J., Kral, J.M., Eds.; University of British Columbia Press: Vancouver, BC, Canada, 2015; pp. 94–144. [Google Scholar]
- Owens, H.; Lambert, C. Mad, bad or heroic? Gender, identity and accountability in lay portrayals of suicide in late twentieth-century England. Cult. Med. Psychiatry 2012, 36, 348–371. [Google Scholar] [CrossRef] [PubMed]
- Scourfield, J.; Fincham, B.; Langer, S.; Shiner, M. Sociological autopsy: An integrated approach to the study of suicide in men. Soc. Sci. Med. 2012, 74, 466–473. [Google Scholar] [CrossRef] [PubMed]
- Canetto, S.S. She died for love and he for glory: Gender myths of suicidal behaviour. Omega 1992, 26, 1–17. [Google Scholar] [CrossRef]
- McAndrew, F.T.; Garrison, A.J. Beliefs about gender differences in methods and causes of suicide. Arch. Suicide Res. 2007, 11, 271–279. [Google Scholar] [CrossRef] [PubMed]
- Eisenwort, B.; Till, B.; Hinterbuchinger, B.; Niederkrotenthaler, T. Sociable, mentally disturbed women and angry, rejected men: Cultural scripts for the suicidal behavior of women and men in the Austrian print media. Sex Roles 2014, 71, 246–260. [Google Scholar] [CrossRef]
- Fitch, W.T.; Giedd, J. Morphology and development of the human vocal tract: A study using magnetic resonance imaging. J. Acoust. Soc. Am. 1999, 106, 1511–1522. [Google Scholar] [CrossRef] [PubMed]
- Mullennix, J.W.; Johnson, K.; Topcu-Durgun, M.; Farnsworth, L.M. The perceptual representation of voice gender. J. Acoust. Soc. Am. 1995, 98, 3080–3095. [Google Scholar] [CrossRef] [PubMed]
- Belin, P.; Fecteau, S.; Bédard, C. Thinking the voice: Neural correlates of voice perception. Trends Cogn. Sci. 2004, 8, 129–135. [Google Scholar] [CrossRef] [PubMed]
- Stangor, C.; Lynch, L.; Duan, C.; Glas, B. Categorization of individuals on the basis of multiple social features. J. Pers. Soc. Psychol. 1992, 62, 207–218. [Google Scholar] [CrossRef]
- Sandhu, H.; Adams, A.; Singleton, L.; Clark-Carter, D.; Kidd, J. The impact of gender dyads on doctor-patient communication: A systematic review. Patient Educ. Couns. 2009, 76, 348–355. [Google Scholar] [CrossRef] [PubMed]
- Brink-Muinen, A.V.D.; Van Dulmen, S.; Messerli-Rohrbach, V.; Bensing, J. Do gender-dyads have different communication patterns? A comparative study in Western-European general practices. Patient Educ. Couns. 2002, 48, 253–264. [Google Scholar] [CrossRef]
- Hall, J.A.; Irish, J.T.; Roter, D.L.; Ehrlich, C.M.; Miller, L.H.; Daninhirsch, C.; Cans, L.; Harrity, J.; Lee, H.; Spencer, S. Gender in medical encounters: An analysis of physician and patient communication in a primary care setting. Health Psychol. 1994, 13, 384–392. [Google Scholar] [CrossRef] [PubMed]
- Tabenkin, H.; Goodwin, M.A.; Zyzanski, S.J.; Stange, K.C.; Medalie, J.H. Gender differences in time spent during direct observation of doctor-patient encounters. J. Women’s Health 2004, 13, 341–349. [Google Scholar] [CrossRef] [PubMed]
- Hunt, T.; Wilson, C.; Woodward, A.; Caputi, P.; Wilson, I. A community-academic partnership model for suicide prevention research. 2017; Submitted for publication. [Google Scholar]
- Hunt, T.; Wilson, C.J.; Caputi, P.; Woodward, A.; Wilson, I. Signs of suicide in men: A systematic review. PLoS ONE 2017, 12, e0174675. [Google Scholar] [CrossRef] [PubMed]
- Ajzen, I. Constructing a TpB Questionnaire: Conceptual and Methodological Considerations. Available online: people.umass.edu/~aizen/pdf/tpb.measurement.pdf (accessed on 5 April 2015).
- Ajzen, I. The theory of planned behavior. Organ. Behav. Hum. Decis. Process. 1991, 50, 179–211. [Google Scholar] [CrossRef]
- Ford, J.K.; MacCallum, R.C.; Tait, M. The application of exploratory factor analysis in applied psychology: A critical review and analysis. Pers. Psychol. 1986, 39, 291–314. [Google Scholar] [CrossRef]
- Costello, A.B.; Osborne, J. Best practices in exploratory factor analysis: Four recommendations for getting the most from your analysis. Pract. Assess. Res. Eval. 2005, 10, 1–9. [Google Scholar]
- Osborne, J.W. What is rotating in exploratory factor analysis? Pract. Assess. Res. Eval. 2015, 20, 1–7. [Google Scholar]
- Cattell, R.B. The scree test for the numbers of factors. Multivar. Behav. Res. 1966, 1, 245–276. [Google Scholar] [CrossRef] [PubMed]
- Hair, J.F.; Anderson, R.E.; Tatham, R.L.; Black, W.C. Multivariate Data Analysis; Prentice-Hall International: London, UK, 1998. [Google Scholar]
- Schönrock-Adema, J.; Heijne-Penninga, M.; Van Hell, E.A.; Cohen-Schotanus, J. Necessary steps in factor analysis: Enhancing validation studies of educational instruments. Med. Teach. 2009, 31, 226–233. [Google Scholar] [CrossRef] [PubMed]
- Distefano, C.; Zhu, M.; Mîndrilă, D. Understanding and using factor scores: Considerations for the applied researcher. Pract. Assess. Res. Eval. 2009, 14, 1–11. [Google Scholar]
- Large, M.; Kaneson, M.; Myles, N.; Myles, H.; Gunaratne, P.; Ryan, C. Meta-analysis of longitudinal cohort studies of suicide risk assessment among psychiatric patients: Heterogeneity in results and lack of improvement over time. PLoS ONE 2016, 11, e0156322. [Google Scholar] [CrossRef] [PubMed]
- Large, M.M.; Ryan, C.J.; Carter, G.; Kapur, N. Can we usefully stratify patients according to suicide risk? BMJ 2017, 359, 1–5. [Google Scholar] [CrossRef] [PubMed]
- Sweeney, L.; Owens, C. Communication and interpretation of emotional distress within the friendships of young Irish men prior to suicide: A qualitative study. Health Soc. Care Community 2015, 23, 150–158. [Google Scholar] [CrossRef] [PubMed]
- Graber, M.L.; Kissam, S.; Payne, V.L.; Meyer, A.N.D.; Sorensen, A.; Lenfestey, N.; Tant, E.; Henriksen, K.; LaBresh, K.; Singh, H. Cognitive interventions to reduce diagnostic error: A narrative review. BMJ Qual. Saf. 2012, 21, 535–557. [Google Scholar] [CrossRef] [PubMed]
- Monteiro, S.M.; Norman, G. Diagnostic reasoning: Where we’ve been, where we’re going. Teach. Learn. Med. 2013, 25, S26–S32. [Google Scholar] [CrossRef] [PubMed]
- Croskerry, P.; Singhal, G.; Mamede, S. Cognitive debiasing 1: Origins of bias and theory of debiasing. BMJ Qual. Saf. 2013, 22, 58–65. [Google Scholar] [CrossRef] [PubMed]
| Demographics | Range | Female | Male | Total | |||
|---|---|---|---|---|---|---|---|
| n | % | n | % | n | % | ||
| Age | >25 | 10 | 10.2 | 1.0 | 2.6 | 11.0 | 8.0 |
| 26–35 | 11 | 11.2 | 0.0 | 0.0 | 11.0 | 8.0 | |
| 36–45 | 20 | 20.4 | 4.0 | 10.3 | 24.0 | 17.5 | |
| 46–55 | 26 | 26.5 | 8.0 | 20.5 | 34.0 | 24.8 | |
| 56–65 | 21 | 21.4 | 18.0 | 46.2 | 39.0 | 28.5 | |
| 66< | 10 | 10.2 | 8.0 | 20.5 | 18.0 | 13.1 | |
| Home Location | Metropolitan | 61 | 62.2 | 19 | 48.7 | 80 | 58.4 |
| Regional | 30 | 30.6 | 15 | 38.5 | 45 | 32.8 | |
| Rural/Remote | 7 | 7.1 | 5 | 12.8 | 12 | 8.8 | |
| Lived experience of suicide | Yes | 71 | 72.4 | 27 | 69.2 | 98 | 71.5 |
| No | 26 | 26.5 | 12 | 30.8 | 38 | 27.7 | |
| Prefer not to respond | 1 | 1.0 | 0 | 0.0 | 1 | 0.7 | |
| Lifeline position | Volunteer | 85 | 86.7 | 31 | 79.5 | 116 | 84.7 |
| Employee | 13 | 13.3 | 8 | 20.5 | 21 | 15.3 | |
| Years as a TCS | 0–2 years | 52 | 53.1 | 14 | 35.9 | 66 | 48.2 |
| 3–5 years | 24 | 24.5 | 10 | 25.6 | 34 | 24.8 | |
| 6–8 years | 9 | 9.2 | 6 | 15.4 | 15 | 10.9 | |
| 9–11 years | 6 | 6.1 | 4 | 10.3 | 10 | 7.3 | |
| 12–14 years | 4 | 4.1 | 4 | 10.3 | 8 | 5.8 | |
| 15 years or longer | 3 | 3.1 | 1 | 2.6 | 4 | 2.9 | |
| Shift frequency | More than once per week | 9 | 9.2 | 6 | 15.4 | 15 | 10.9 |
| Once per week | 38 | 38.8 | 21 | 53.8 | 59 | 43.1 | |
| Once per fortnight | 46 | 46.9 | 12 | 30.8 | 58 | 42.3 | |
| Once per month | 4 | 4.1 | 0 | 0.0 | 4 | 2.9 | |
| Less than once per month | 1 | 1.0 | 0 | 0.0 | 1 | 0.7 | |
| Shift recency | Less than 1 week ago | 44 | 44.9 | 21 | 53.8 | 65 | 47.4 |
| 1 week ago | 22 | 22.4 | 6 | 15.4 | 28 | 20.4 | |
| 2 weeks ago | 15 | 15.3 | 7 | 17.9 | 22 | 16.1 | |
| 3 weeks ago | 7 | 7.1 | 1 | 2.6 | 8 | 5.8 | |
| 4 weeks ago | 3 | 3.1 | 3 | 7.7 | 6 | 4.4 | |
| More than 4 weeks ago | 7 | 7.1 | 1 | 2.6 | 8 | 5.8 | |
| Suicide Signs | Loadings | ||
|---|---|---|---|
| 1 | 2 | 3 | |
| Intent to seek revenge | 1.03 | ||
| Intense feelings of anger | 0.56 | ||
| Recklessness, or engagement in risky activities | 0.45 | ||
| Inability to sleep, or sleeps all the time | 0.99 | ||
| Agitation or restlessness | 0.80 | ||
| Dramatic changes in mood | 0.59 | ||
| Future is hopeless | 0.86 | ||
| No reason for living | 0.69 | ||
| Feels trapped, or stuck like there is no way out | 0.67 | ||
| Cronbach’s alpha | 0.79 | 0.87 | 0.74 |
| Suicide Signs | Loadings | ||
|---|---|---|---|
| 1 | 2 | 3 | |
| Agitation or restlessness | 0.83 | ||
| Dramatic changes in mood | 0.78 | ||
| Inability to sleep, or sleeps all the time | 0.78 | ||
| Withdrawing from friends, family or society | 0.64 | ||
| Increased alcohol or drug use | 0.60 | ||
| Future is hopeless | 0.83 | ||
| No reason for living | 0.66 | ||
| Feels trapped, or stuck like there is no way out | 0.61 | ||
| Intense feelings of anger | 0.80 | ||
| Intent to seek revenge | 0.76 | ||
| Cronbach’s alpha | 0.83 | 0.73 | 0.79 |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Hunt, T.; Wilson, C.; Caputi, P.; Wilson, I.; Woodward, A. Patterns of Signs That Telephone Crisis Support Workers Associate with Suicide Risk in Telephone Crisis Line Callers. Int. J. Environ. Res. Public Health 2018, 15, 235. https://doi.org/10.3390/ijerph15020235
Hunt T, Wilson C, Caputi P, Wilson I, Woodward A. Patterns of Signs That Telephone Crisis Support Workers Associate with Suicide Risk in Telephone Crisis Line Callers. International Journal of Environmental Research and Public Health. 2018; 15(2):235. https://doi.org/10.3390/ijerph15020235
Chicago/Turabian StyleHunt, Tara, Coralie Wilson, Peter Caputi, Ian Wilson, and Alan Woodward. 2018. "Patterns of Signs That Telephone Crisis Support Workers Associate with Suicide Risk in Telephone Crisis Line Callers" International Journal of Environmental Research and Public Health 15, no. 2: 235. https://doi.org/10.3390/ijerph15020235
APA StyleHunt, T., Wilson, C., Caputi, P., Wilson, I., & Woodward, A. (2018). Patterns of Signs That Telephone Crisis Support Workers Associate with Suicide Risk in Telephone Crisis Line Callers. International Journal of Environmental Research and Public Health, 15(2), 235. https://doi.org/10.3390/ijerph15020235





