A Survey of Health Disparities, Social Determinants of Health, and Converging Morbidities in a County Jail: A Cultural-Ecological Assessment of Health Conditions in Jail Populations
Abstract
1. Introduction
- Describe Characteristics of Incarcerated Individuals in Northern Arizona. Describe the current county jail sample in terms of demographic information, income status, living conditions prior to incarceration, and general health measures.
- Identify the Infectious Disease, Chronic Illness, Behavioral Health, Substance Use, and Global Health Conditions Prevalent in a County Jail. Of the current sample of incarcerated individuals in Northern Arizona, what is the prevalence of self-reported health conditions in the jail population, and what are the typical co-morbidity patterns identified by self-report?
2. Materials and Methods
2.1. Instrument Development
2.2. Subject Recruitment
2.3. Measures
2.4. Statistical Analysis
3. Results
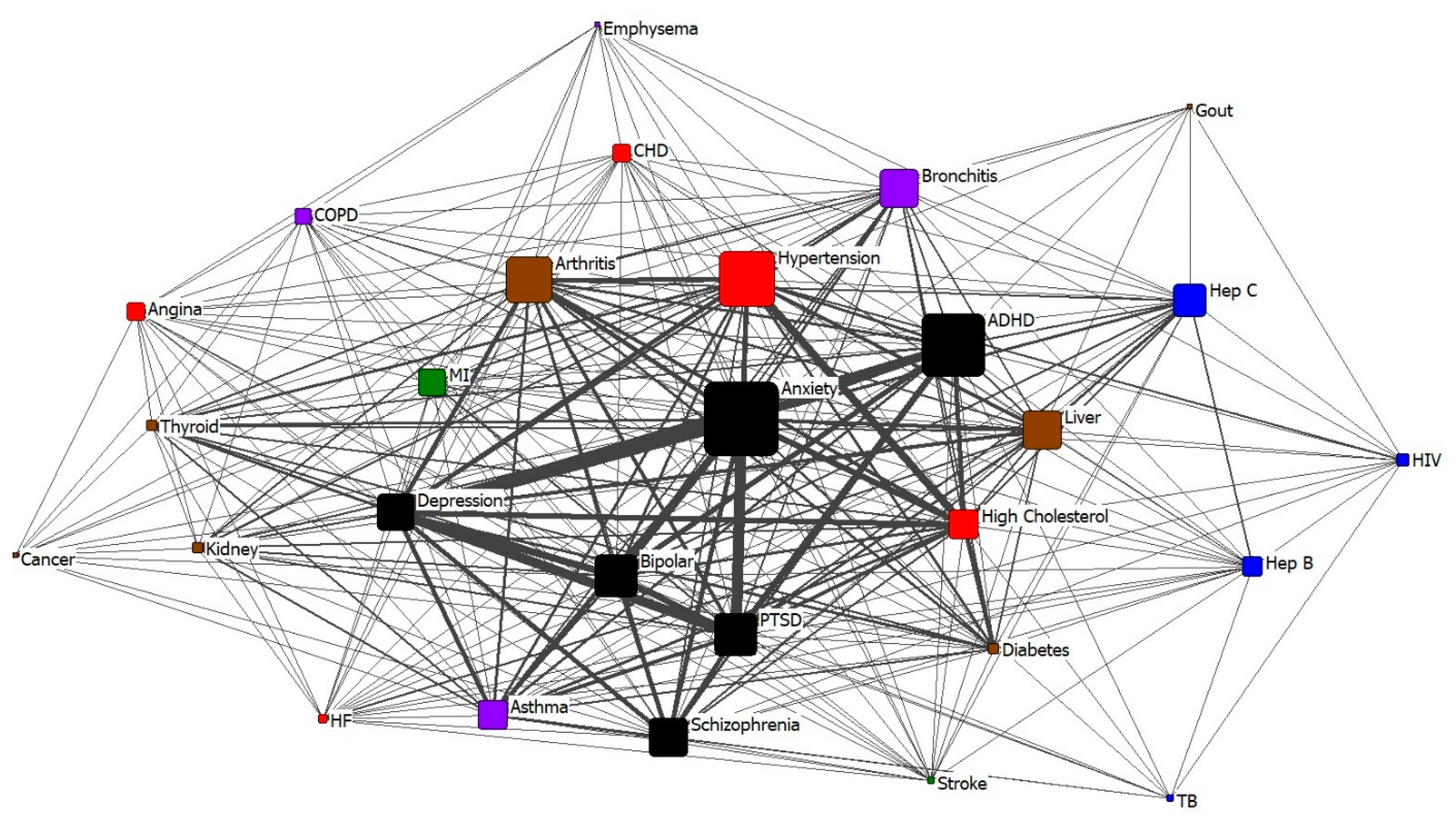
Comorbidity Conditions
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Ahalt, C.; Bolano, M.; Wang, E.A.; Williams, B. The state of research funding from the National Institutes of Health for criminal justice health research. Ann. Intern. Med. 2015, 162, 345–352. [Google Scholar] [CrossRef] [PubMed]
- Binswanger, I.A.; Redmond, N.; Steiner, J.F.; Hicks, L.S.; Binswanger, I.A.; Redmond, N.; Steiner, J.F.; Hicks, L.S. Health disparities and the criminal justice system: An agenda for further research and action. J. Urban Health 2012, 89, 98–107. [Google Scholar] [CrossRef] [PubMed]
- Morgan, O.; Kuramoto, F.; Emmet, W.; Stange, J.L.; Nobunaga, E. The Impact of the Affordable Care Act on Behavioral Health Care for Individuals From Racial and Ethnic Communities. J. Soc. Work Disabil. Rehabil. 2014, 13, 139–161. [Google Scholar] [CrossRef] [PubMed]
- Heidari, E.; Dickson, C.; Newton, T.; Dickinson, C. An overview of the prison population and the general health status of prisoners. Br. Dent. J. 2014, 217, 15–19. [Google Scholar] [CrossRef] [PubMed]
- Binswanger, I.A.; Krueger, P.M.; Steiner, J.F. Prevalence of chronic medical conditions among jail and prison inmates in the USA compared with the general population. J. Epidemiol. Community Health 2009, 63, 912–919. [Google Scholar] [CrossRef] [PubMed]
- Massoglia, M. Incarceration as exposure: The prison, infectious disease, and other stress-related illnesses. J. Health Soc. Behav. 2008, 49, 56–71. [Google Scholar] [CrossRef] [PubMed]
- Fazel, S.; Danesh, J. Serious mental disorder in 23 000 prisoners: A systematic review of 62 surveys. Lancet 2002, 359, 545. [Google Scholar] [CrossRef]
- Schnittker, J.; John, A. Enduring stigma: The long-term effects of incarceration on health. J. Health Soc. Behav. 2007, 48, 115–130. [Google Scholar] [CrossRef] [PubMed]
- Vaughn, M.G.; Salas-wright, C.P.; Delisi, M.; Piquero, A.R. Health associations of drug-involved and criminal-justice-involved adults in the united states. Crim. Justice Behav. 2014, 41, 318–336. [Google Scholar] [CrossRef]
- Summary Health Statistics for US Adults: National Interview Survey: National Center for Health Statistics, Atlanta, GA USA, 2014. Available online: https://www.cdc.gov/nchs/products/series/series10.htm (accessed on 10 September 2017).
- Williams, S.M. Poverty in the US: Trends, Issues, and Measurements. In Economic Issues, Problems, and Perspectives; Nova Science Publishers: Hauppauge, NY, USA, 2011; p. 302. [Google Scholar]
- Kaba, F.; Solimo, A.; Graves, J.; Glowa-Kollisch, S.; Vise, A.; MacDonald, R.; Waters, A.; Rosner, Z.; Dickey, N.; Angell, S.; et al. Disparities in Mental Health Referral and Diagnosis in the New York City Jail Mental Health Service. Am. J. Public Health 2015, 105, 1911–1916. [Google Scholar] [CrossRef] [PubMed]
- Chodos, A.H.; Ahalt, C.; Cenzer, I.S.; Myers, J.; Goldenson, J.; Williams, B.A. Older Jail Inmates and Community Acute Care Use. Am. J. Public Health 2014, 104, 1728–1733. [Google Scholar] [CrossRef] [PubMed]
- Lim, S.; Nash, D.; Hollod, L.; Harris, T.G.; Lennon, M.C.; Thorpe, L.E. Influence of Jail Incarceration and Homelessness Patterns on Engagement in HIV Care and HIV Viral Suppression among New York City Adults Living with HIV/AIDS. PLoS ONE 2015, 10, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Clear, T.R.; Austin, J. Reducing Mass Incarceration: Implications of the Iron Law of Prison Populations. Harv. Law Policy Rev. 2009, 3, 307–324. [Google Scholar]
- Zeng, Z. Jail Inmates in 2016; Bereau of Justice Statistics: Washington, DC, USA, 2018.
- Ramaswamy, M.; Diaz, F.; Pankey, T.; Hunt, S.L.; Park, A.; Kelly, P.J. Correlates of Preincarceration Health Care Use Among Women and Men in Jail. J. Correct. Health Care 2015, 21, 286–297. [Google Scholar] [CrossRef] [PubMed]
- Greenberg, G.A.; Rosenheck, R.A.; Greenberg, G.A.; Rosenheck, R.A. Jail incarceration, homelessness, and mental health: a national study. Psychiatr. Serv. 2008, 59, 170–177. [Google Scholar] [CrossRef] [PubMed]
- Boyd, A.T.; Song, D.L.; Meyer, J.P.; Altice, F.L. Emergency department use among HIV-infected released jail detainees. J. Urban Health 2015, 92, 108–135. [Google Scholar] [CrossRef] [PubMed]
- Wakeman, S.E.; McKinney, M.E.; Rich, J.D. Filling the gap: The importance of Medicaid continuity for former inmates. J. Gen. Intern. Med. 2009, 24, 860–862. [Google Scholar] [CrossRef] [PubMed]
- Evans, C.A.; Cheema, J. As Roughly 700,000 Prisoners Are Released Annually, About Half Will Gain Health Coverage And Care Under Federal Laws. Health Aff. (Millwood) 2012, 31, 931–938. [Google Scholar] [CrossRef]
- Estelle v. Gamble, Vol. 429; 0976. 1976. Available online: https://supreme.justia.com/cases/federal/us/429/97/ (accessed on 4 September 2018).
- Trotter, R., II; Camplain, R.; Eaves, E.; Fofanov, V.; Drmitrieva, N.; Hepp, C.; Warren, M.; Barrios, B.; Pagel, N.; Mayer, A.; et al. Health Disparities in Jail Populations Protocol. JMIR Res. Protoc. 2018, in press. [Google Scholar]
- Collective Impact (SSIR). Available online: https://ssir.org/articles/entry/collective_impact (accessed on 4 September 2018).
- Collective Impact. Available online: https://www.councilofnonprofits.org/tools-resources/collective-impact (accessed on 4 September 2018).
- Centers for Disease Control and Prevention; Peterlin, B.L.; Rosso, A.L.; Rapoport, A.M.; Scher, A.I. National Health and Nutrition Examination Survey. Obes. Migraine Eff. Age Gend. Adipose Tissue Dispos. 2010, 50, 52–62. [Google Scholar]
- Kessler, R.C.; Andrews, G.; Colpe, L.J.; Hiripi, E.; Mroczek, D.K.; Normand, S.L.T.; Walters, E.E.; Zaslavsky, A.M. Short screening scales to monitor population prevalences and trends in non-specific psychological distress. Psychol. Med. 2002, 32, 959–976. [Google Scholar] [CrossRef] [PubMed]
- Maruschak, L.M. Medical Problems of State and Federal Prisoners and Jail Inmates, 2011–12. 2015; 23p. Available online: https://www.bjs.gov/content/pub/pdf/mpsfpji1112.pdf (accessed on 4 September 2018).
- Bloom, B.; Cohen, R.A.; Freeman, G. Summary health statistics for U.S. children: National Health Interview Survey, 2009. Vital Health Stat. Ser. 10 2010, 1–82. [Google Scholar]
- Nelson, D.E.; Holtzman, D.; Waller, M. 1998: Objectives and Design of the Behavioral Risk Factor Surveillance System. Available online: http://citeseerx.ist.psu.edu/viewdoc/download;jsessionid=77B74BFE62A4580681EAF502166EFF0D?doi=10.1.1.540.4109&rep=rep1&type=pdf (accessed on 4 September 2018).
- Gilbert, L.K.; Breiding, M.J.; Merrick, M.T.; Thompson, W.W.; Ford, D.C.; Dhingra, S.S.; Parks, S.E. Childhood Adversity and Adult Chronic Disease: An Update from Ten States and the District of Columbia, 2010. Am. J. Prev. Med. 2015, 48, 345–349. [Google Scholar] [CrossRef] [PubMed]
- Kroenke, K.; Spitzer, R.L.; Williams, J.B.W.; Löwe, B. The Patient Health Questionnaire Somatic, Anxiety, and Depressive Symptom Scales: A systematic review. Gen. Hosp. Psychiatry 2010, 32, 345–359. [Google Scholar] [CrossRef] [PubMed]
- Broderick, J.E.; DeWitt, E.M.; Rothrock, N.; Crane, P.K.; Forrest, C.B. Advances in Patient-Reported Outcomes: The NIH PROMIS(®) Measures. EGEMS Wash. DC 2013, 1, 1015. [Google Scholar] [CrossRef] [PubMed]
- Brim, O.G.; Ryff, C.D.; Kessler, R.C. How Healthy Are We?: A National Study of Well-Being at Midlife; The John D. and Catherine T. MacArthur Foundation Series on Mental Health and Development; Studies on Successful Midlife Development; University of Chicago Press: Chicago, IL, USA, 2004; ISBN 0-226-07475-7. [Google Scholar]
- Brief Symptom Inventory 18. Available online: https://www.pearsonclinical.com/psychology/products/100000638/brief-symptom-inventory-18-bsi18.html (accessed on 4 September 2018).
- Cohen, S. Psychosocial influences on immunity and infectious disease in humans. In Handbook of Human Stress and Immunity; Glaser, R., Kiecolt-Glaser, J.K., Eds.; Academic Press: San Diego, CA, USA, 1994; pp. 301–319. ISBN 978-0-12-285960-1. [Google Scholar]
- Craig, C.L.; Marshall, A.L.; Sjostrom, M.; Bauman, A.E.; Booth, M.L.; Ainsworth, B.E.; Pratt, M.; Ekelund, U.; Yngve, A.; Sallis, J.F.; et al. International Physical Activity Questionnaire--Long Format. Int. Phys. Act. Quest. 12-Ctry. Reliab. Validity 2003, 35, 1381–1395. [Google Scholar]
- Bureau of Justice Statistics (BJS)—National Inmate Survey (NIS). Available online: https://www.bjs.gov/index.cfm?ty=dcdetail&iid=278 (accessed on 4 September 2018).
- Jobe, J.B. Cognitive psychology and self-reports: models and methods. Qual. Life Res. 2003, 12, 219–227. [Google Scholar] [CrossRef] [PubMed]
- Willis, G.B.; Royston, P.; Bercini, D. The Use of Verbal Report Methods in the Development and Testing of Survey Questionnaires. Appl. Cogn. Psychol. 1991, 5, 251–267. [Google Scholar] [CrossRef]
- Bernard, H. Research Methods In Anthropology: Qualitative and Quantitative Approaches, 3rd ed.; Alta Mira Press: Walnut Creek, CA, USA, 2002. [Google Scholar]
- Creswell, J.W. Research Design: Qualitative, Quantitative and Mixed Methods Approaches, 2nd ed.; Sage Publishers: Thousand Oaks, CA, USA, 2003. [Google Scholar]
- Etikan, I.; Musa, S.; Alkassim, R. Comparison of Convenience Sampling and Purposive Sampling. Am. J. Theor. Appl. Stat. 2016, 5, 1–4. [Google Scholar] [CrossRef]
- Borgatti, S.; Everett, M.; Freeman, L. Ucinet for Windows: Software for Social Network Analysis; Analytic Technologies: Harvard, MA, USA, 2002. [Google Scholar]
- Opsahl, T.; Agneessens, F.; Skvoretz, J. Node centrality in weighted networks: Generalizing degree and shortest paths. Soc. Netw. 2010, 32, 245–251. [Google Scholar] [CrossRef]
- Freeman, L.C. Centrality in social networks conceptual clarification. Soc. Netw. 1978, 1, 215–239. [Google Scholar] [CrossRef]
- Newman, M.E.J. A measure of betweenness centrality based on random walks. Soc. Netw. 2005, 27, 39–54. [Google Scholar] [CrossRef]
- Brandes, U. On variants of shortest-path betweenness centrality and their generic computation. Soc. Netw. 2008, 30, 136–145. [Google Scholar] [CrossRef]
- Singer, M.; Clair, S. Syndemics and public health: reconceptualizing disease in bio-social context. Med. Anthropol. Q. 2003, 17, 423–441. [Google Scholar] [CrossRef] [PubMed]
- Sanderson, K.; Williamson, H.; Eaves, E.; Barger, S.; Hepp, C.; Elwell, K.; Camplain, R.; Winfree, K.; Trotter, R.; Baldwin, J. Advancing Wellbeing in Northern Arizona: A Regional Health Equity Assessment; Center for Health Equity Research: Flagstaff, AZ, USA, 2017. [Google Scholar]
- Barger, S.D.; Cribbet, M.R.; Muldoon, M.F. Participant-Reported Health Status Predicts Cardiovascular and All-Cause Mortality Independent of Established and Nontraditional Biomarkers: Evidence From a Representative US Sample. J. Am. Heart Assoc. 2016, 5, e003741. [Google Scholar] [CrossRef] [PubMed]
- Marmot, M.; Friel, S.; Bell, R.; Houweling, T.A.; Taylor, S. Closing the gap in a generation: Health equity through action on the social determinants of health. Lancet 2008, 372, 1661–1669. [Google Scholar] [CrossRef]
| Variables | Frequency | Percent |
|---|---|---|
| Sex (n = 199) | ||
| Male | 157 | 78.9 |
| Female | 42 | 21.1 |
| Education (n = 199) | ||
| Less than high school | 60 | 30.2 |
| High school diploma or GED | 76 | 38.2 |
| Some college or higher | 63 | 31.6 |
| Race (n = 199) | ||
| American Indian/Alaska Native | 117 | 58.8 |
| White | 55 | 27.6 |
| Other (Black, Asian, and Other) | 31 | 15.6 |
| Ethnicity (n = 196) | ||
| Hispanic/Latino | 29 | 14.8 |
| Not Hispanic/Latino | 167 | 85.2 |
| Marital Status (n = 192) | ||
| Divorced or Widowed | 43 | 22.4 |
| Married | 31 | 16.1 |
| Separated | 15 | 7.8 |
| Single | 103 | 53.7 |
| Annual Household Income (n = 194) | ||
| 0–9999 | 89 | 45.9 |
| 10,000–19,999 | 19 | 9.8 |
| 20,000–29,999 | 14 | 7.2 |
| 30,000–39,999 | 13 | 6.7 |
| 40,000–49,999 | 6 | 3.1 |
| Greater than or equal to 50,000 | 20 | 10.3 |
| Don’t know | 33 | 17.0 |
| Variables | Frequency | Percent |
|---|---|---|
| Living Status Prior to Incarceration (n = 194) | ||
| House, apartment, or mobile home | 136 | 70.1 |
| On the street or homeless shelter | 39 | 20.1 |
| Other | 19 | 9.8 |
| Ever Been Homeless (n = 163) | ||
| Yes | 69 | 42.4 |
| No | 93 | 57.6 |
| Employment Prior to Incarceration (n = 199) | ||
| Working for pay | 91 | 45.7 |
| Self-employed | 30 | 15.1 |
| Looking for work | 39 | 19.6 |
| Permanently Disabled | 12 | 6.0 |
| Student | 7 | 3.5 |
| Other | 20 | 10.1 |
| Health Insurance Status (n = 197) | ||
| Insured | 156 | 79.2 |
| Uninsured | 41 | 20.8 |
| Time Since Most Recent Health Care Visit (n = 189) | ||
| ≤ 6 months | 106 | 56.1 |
| 6 months–≤ 1 year | 36 | 19.1 |
| 1–2 years | 25 | 13.2 |
| ≥2 years | 22 | 11.6 |
| Number of Emergency Room Visits * (n = 199) | ||
| None | 60 | 31.4 |
| 1 | 53 | 26.9 |
| 2–3 | 56 | 28.3 |
| ≥4 | 26 | 13.3 |
| Variables | Frequency | Percent |
|---|---|---|
| General Health (n = 195) | ||
| Excellent | 16 | 8.2 |
| Very good | 39 | 20.0 |
| Good | 68 | 34.9 |
| Fair | 57 | 29.2 |
| Poor | 15 | 7.7 |
| Body Mass Index Categories (n =1 91) | ||
| Underweight or Normal (<25 kg/m2) | 74 | 38.7 |
| Overweight (25–29.9 kg/m2) | 72 | 37.7 |
| Obese (≥30 kg/m2) | 45 | 23.6 |
| Medical Conditions | ||
| Hypertension (n = 192) | 69 | 35.9 |
| High Cholesterol (n = 191) | 34 | 17.8 |
| Arthritis (n = 194) | 34 | 17.5 |
| Asthma (n = 195) | 29 | 14.9 |
| Prediabetes or Diabetes (n = 196) | 24 | 12.3 |
| Liver Condition (n = 193) | 23 | 11.9 |
| Bronchitis (n = 195) | 14 | 7.2 |
| Mental Health Conditions | ||
| Anxiety (n = 197) | 72 | 36.5 |
| Depression (n = 197) | 66 | 33.5 |
| PTSD (n = 198) | 52 | 26.3 |
| ADD/ADHD (n = 195) | 45 | 23.1 |
| Bipolar Disorder (n = 196) | 39 | 19.9 |
| Schizophrenia (n = 196) | 22 | 11.2 |
| Infectious Diseases | ||
| Hepatitis C (n = 199) | 14 | 7.0 |
| HIV (n = 102) * | 5 | 4.9 |
| Hepatitis B (n = 199) * | 5 | 2.5 |
| Tuberculosis (n = 199) * | 4 | 2.0 |
| Substance Ever Use | ||
| Marijuana (n = 195) | 159 | 81.5 |
| Cocaine (n = 196) | 97 | 49.5 |
| Methamphetamine (n = 196) | 113 | 57.7 |
| Other Amphetamines (n = 195) | 64 | 32.8 |
| LSD (n = 194) | 61 | 31.4 |
| Other Opiates (n = 195) | 59 | 30.3 |
| Heroin (n = 196) | 57 | 29.1 |
| Crack (n = 193) | 51 | 26.4 |
| Ecstasy (n = 193) | 50 | 25.9 |
| Barbiturates (n = 195) | 46 | 23.6 |
| Tranquilizers (n = 196) | 39 | 19.9 |
| PCP (n = 194) | 24 | 12.4 |
| Methaqualone (n = 195) | 18 | 9.2 |
| Alcohol Use a (n = 188) | ||
| Yes | 143 | 76.1 |
| No | 45 | 23.9 |
| Arthritis | Gout | HF | CHD | Angina | MI | Stroke | Emphysema | Thyroid | Bronchitis | Liver | COPD | Asthma | Kidney | Cancer | Hypertension | High Cholesterol | Diabetes | Hep B | Hep C | TB | HIV | Anxiety | Depression | Bipolar | Schizophrenia | PTSD | ADHD | |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Arthritis | ||||||||||||||||||||||||||||
| Gout | 1 | |||||||||||||||||||||||||||
| HF | 1 | 0 | ||||||||||||||||||||||||||
| CHD | 2 | 0 | 2 | |||||||||||||||||||||||||
| Angina | 1 | 0 | 1 | 1 | ||||||||||||||||||||||||
| MI | 3 | 0 | 3 | 3 | 3 | |||||||||||||||||||||||
| Stroke | 1 | 0 | 2 | 1 | 2 | 2 | ||||||||||||||||||||||
| Emphysema | 1 | 0 | 0 | 1 | 1 | 1 | 0 | |||||||||||||||||||||
| Thyroid | 6 | 0 | 2 | 1 | 2 | 2 | 0 | 0 | ||||||||||||||||||||
| Bronchitis | 7 | 2 | 0 | 1 | 1 | 1 | 0 | 1 | 3 | |||||||||||||||||||
| Liver | 7 | 1 | 2 | 1 | 1 | 1 | 1 | 0 | 4 | 4 | ||||||||||||||||||
| COPD | 3 | 0 | 0 | 1 | 1 | 1 | 0 | 1 | 1 | 2 | 1 | |||||||||||||||||
| Asthma | 10 | 0 | 2 | 0 | 1 | 2 | 1 | 0 | 4 | 5 | 3 | 2 | ||||||||||||||||
| Kidney | 4 | 0 | 2 | 1 | 1 | 1 | 0 | 0 | 2 | 2 | 2 | 1 | 4 | |||||||||||||||
| Cancer | 2 | 0 | 0 | 0 | 1 | 1 | 0 | 0 | 1 | 0 | 0 | 1 | 2 | 1 | ||||||||||||||
| Hypertension | 18 | 1 | 3 | 2 | 2 | 4 | 2 | 1 | 8 | 5 | 12 | 0 | 9 | 4 | 1 | |||||||||||||
| High Cholesterol | 15 | 0 | 4 | 2 | 0 | 3 | 2 | 1 | 4 | 6 | 4 | 3 | 8 | 4 | 0 | 29 | ||||||||||||
| Diabetes | 8 | 0 | 2 | 1 | 0 | 1 | 2 | 0 | 4 | 5 | 5 | 1 | 6 | 1 | 0 | 9 | 19 | |||||||||||
| Hep B | 1 | 0 | 1 | 1 | 0 | 1 | 1 | 0 | 0 | 1 | 2 | 0 | 1 | 0 | 0 | 1 | 2 | 1 | ||||||||||
| Hep C | 4 | 1 | 0 | 2 | 0 | 2 | 1 | 1 | 0 | 2 | 8 | 1 | 3 | 0 | 0 | 3 | 7 | 2 | 4 | |||||||||
| TB | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 1 | 0 | 0 | 0 | 2 | 0 | 1 | 0 | ||||||||
| HIV | 0 | 1 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 1 | 1 | 0 | 0 | 0 | 0 | 4 | 0 | 0 | 1 | 1 | 1 | |||||||
| Anxiety | 17 | 1 | 2 | 1 | 1 | 3 | 2 | 1 | 9 | 11 | 14 | 3 | 19 | 6 | 3 | 17 | 25 | 6 | 2 | 8 | 3 | 1 | ||||||
| Depression | 18 | 0 | 2 | 1 | 1 | 3 | 2 | 1 | 8 | 9 | 12 | 3 | 16 | 6 | 3 | 18 | 24 | 8 | 0 | 7 | 2 | 0 | 58 | |||||
| Bipolar | 10 | 0 | 3 | 1 | 2 | 3 | 1 | 0 | 7 | 5 | 5 | 1 | 10 | 4 | 2 | 8 | 11 | 2 | 1 | 4 | 2 | 1 | 34 | 31 | ||||
| Schizophrenia | 7 | 0 | 2 | 0 | 1 | 2 | 1 | 0 | 3 | 2 | 5 | 1 | 8 | 3 | 1 | 5 | 7 | 2 | 1 | 2 | 2 | 1 | 19 | 19 | 17 | |||
| PTSD | 14 | 0 | 3 | 2 | 2 | 4 | 2 | 0 | 7 | 5 | 8 | 2 | 15 | 5 | 2 | 18 | 12 | 3 | 1 | 5 | 3 | 1 | 46 | 42 | 28 | 19 | ||
| ADHD | 9 | 2 | 3 | 2 | 1 | 3 | 2 | 1 | 5 | 6 | 7 | 1 | 8 | 3 | 0 | 9 | 17 | 3 | 1 | 7 | 1 | 1 | 34 | 30 | 22 | 11 | 26 |
| Condition | Degree Centrality | Betweeness Centrality |
|---|---|---|
| Anxiety | 346 | 10.351478 |
| ADHD | 215 | 8.6119423 |
| Hypertension | 193 | 7.442946 |
| Arthritis | 170 | 6.1652584 |
| Bipolar | 215 | 5.5080433 |
| PTSD | 275 | 5.5080433 |
| Schizophrenia | 141 | 5.0631657 |
| Liver | 111 | 5.0189047 |
| Depression | 324 | 4.7398615 |
| Hep C | 75 | 4.1134052 |
| High Cholesterol | 211 | 3.7165437 |
| Asthma | 140 | 3.5543275 |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Trotter, R.T., II; Lininger, M.R.; Camplain, R.; Fofanov, V.Y.; Camplain, C.; Baldwin, J.A. A Survey of Health Disparities, Social Determinants of Health, and Converging Morbidities in a County Jail: A Cultural-Ecological Assessment of Health Conditions in Jail Populations. Int. J. Environ. Res. Public Health 2018, 15, 2500. https://doi.org/10.3390/ijerph15112500
Trotter RT II, Lininger MR, Camplain R, Fofanov VY, Camplain C, Baldwin JA. A Survey of Health Disparities, Social Determinants of Health, and Converging Morbidities in a County Jail: A Cultural-Ecological Assessment of Health Conditions in Jail Populations. International Journal of Environmental Research and Public Health. 2018; 15(11):2500. https://doi.org/10.3390/ijerph15112500
Chicago/Turabian StyleTrotter, Robert T, II, Monica R Lininger, Ricky Camplain, Viacheslav Y Fofanov, Carolyn Camplain, and Julie A Baldwin. 2018. "A Survey of Health Disparities, Social Determinants of Health, and Converging Morbidities in a County Jail: A Cultural-Ecological Assessment of Health Conditions in Jail Populations" International Journal of Environmental Research and Public Health 15, no. 11: 2500. https://doi.org/10.3390/ijerph15112500
APA StyleTrotter, R. T., II, Lininger, M. R., Camplain, R., Fofanov, V. Y., Camplain, C., & Baldwin, J. A. (2018). A Survey of Health Disparities, Social Determinants of Health, and Converging Morbidities in a County Jail: A Cultural-Ecological Assessment of Health Conditions in Jail Populations. International Journal of Environmental Research and Public Health, 15(11), 2500. https://doi.org/10.3390/ijerph15112500




