Contemplative Practices: A Strategy to Improve Health and Reduce Disparities
Abstract
1. Introduction
2. Health
3. Contemplative Practices
4. Spiritual Awareness
5. Compassion
6. Contemplative Practices and Stress in the Context of Health and Disease
7. The Way Forward: In What Way Might Contemplative Practices Improve Health and Reduce Health Disparities?
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Brook, R.H. Should the definition of health include a measure of tolerance? JAMA 2017, 317, 585–586. [Google Scholar] [CrossRef] [PubMed]
- Van Doorn, M. The nature of tolerance and the social circumstances in which it emerges. Curr. Soc. 2014, 62, 905–927. [Google Scholar] [CrossRef]
- World Health Organization. Constitution of WHO: Principles. Available online: https://www.who.int/about/mission/en/ (accessed on 29 August 2018).
- Online Etymology Dictionary. Health. Available online: https://www.etymonline.com/word/health (accessed on 29 August 2018).
- Levine, G.N.; Lange, R.A.; Bairey-Merz, C.N.; Davidson, R.J.; Jamerson, K.; Mehta, P.K.; Michos, E.D.; Norris, K.; Ray, I.B.; Saban, K.L.; et al. Meditation and cardiovascular risk reduction: A scientific statement from the american heart association. J. Am. Heart Assoc. 2017, 6, e002218. [Google Scholar] [CrossRef] [PubMed]
- Abbott, R.A.; Whear, R.; Rodgers, L.R.; Bethel, A.; Thompson Coon, J.; Kuyken, W.; Stein, K.; Dickens, C. Effectiveness of mindfulness-based stress reduction and mindfulness based cognitive therapy in vascular disease: A systematic review and meta-analysis of randomised controlled trials. J. Psychosom. Res. 2014, 76, 341–351. [Google Scholar] [CrossRef] [PubMed]
- Anheyer, D.; Haller, H.; Barth, J.; Lauche, R.; Dobos, G.; Cramer, H. Mindfulness-based stress reduction for treating low back pain: A systematic review and meta-analysis. Ann. Intern. Med. 2017, 166, 799–807. [Google Scholar] [CrossRef] [PubMed]
- Lauche, R.; Cramer, H.; Dobos, G.; Langhorst, J.; Schmidt, S. A systematic review and meta-analysis of mindfulness-based stress reduction for the fibromyalgia syndrome. J. Psychosom. Res. 2013, 75, 500–510. [Google Scholar] [CrossRef] [PubMed]
- Cushing, R.E.; Braun, K.L. Mind-body therapy for military veterans with post-traumatic stress disorder: A systematic review. J. Altern. Complement. Med. 2018, 24, 106–114. [Google Scholar] [CrossRef] [PubMed]
- Albert Einstein: “A Human Being is Part of A Whole, Called by us the ‘Universe’ —A Part Limited in Time and Space”. Available online: https://www.wildmind.org/blogs/quote-of-the-month/quote-einstein-connectedness (accessed on 28 May 2018).
- Lawler-Row, K.A.; Elliott, J. The role of religious activity and spirituality in the health and well-being of older adults. J. Health Psychol. 2009, 14, 43–52. [Google Scholar] [CrossRef] [PubMed]
- Koenig, H.G.; George, L.K.; Titus, P. Religion, spirituality, and health in medically ill hospitalized older patients. J. Am. Geriatr. Soc. 2004, 52, 554–562. [Google Scholar] [CrossRef] [PubMed]
- Sprecher, S.; Fehr, B. Enhancement of mood and self-esteem as a result of giving and receiving compassionate love. Curr. Res. Soc. Psychol. 2006, 11, 227–242. [Google Scholar]
- Bruce, M.A.; Griffith, D.M.; Thorpe, R.J. Stress and the kidney. Adv. Chron. Kidney Dis. 2015, 22, 46–53. [Google Scholar] [CrossRef] [PubMed]
- Cohen, S.; Kessler, R.C.; Gordon, L.U. Personality characteristics as moderators of the relationship between stress and disorder. In Measuring Stress: A Guide for Health and Social Scientists; Cohen, S., Kessler, R.C., Gordon, L.U., Eds.; Oxford University Press: New York, NY, USA, 1995; pp. 3–26. [Google Scholar]
- Holmes, T.H.; Rahe, R.H. The social readjustment rating scale. J. Psychosom. Res. 1967, 11, 213–218. [Google Scholar] [CrossRef]
- Thoits, P.A. Stress, coping, and social support processes: Where are we? What next? J. Health Soc. Behav. 1995, 53–79. [Google Scholar] [CrossRef]
- Thoits, P.A. Stress and health: Major findings and policy implications. J. Health Soc. Behav. 2010, 51, S41–S53. [Google Scholar] [CrossRef] [PubMed]
- McEwen, B.S. Protective and damaging effects of stress mediators. N. Engl. J. Med. 1998, 338, 171–179. [Google Scholar] [CrossRef] [PubMed]
- Auchincloss, A.H.; Diez Roux, A.V.; Brown, D.G.; O’Meara, E.S.; Raghunathan, T.E. Association of insulin resistance with distance to wealthy areas: The multi-ethnic study of atherosclerosis. Am. J. Epidemiol. 2007, 165, 389–397. [Google Scholar] [CrossRef] [PubMed]
- Black, P.H. The inflammatory response is an integral part of the stress response: Implications for atherosclerosis, insulin resistance, type II diabetes and metabolic syndrome X. Brain Behav. Immun. 2003, 17, 350–364. [Google Scholar] [CrossRef]
- Clark, R.; Benkert, R.A.; Flack, J.M. Large arterial elasticity varies as a function of gender and racism-related vigilance in black youth. J. Adolesc. Health 2006, 39, 562–569. [Google Scholar] [CrossRef] [PubMed]
- Harris, C.W.; Edwards, J.L.; Baruch, A.; Riley, W.A.; Pusser, B.E.; Rejeski, W.J.; Herrington, D.M. Effects of mental stress on brachial artery flow-mediated vasodilation in healthy normal individuals. Am. Heart J. 2000, 139, 405–411. [Google Scholar] [PubMed]
- Kop, W.J.; Verdino, R.J.; Gottdiener, J.S.; O’Leary, S.T.; Bairey Merz, C.N.; Krantz, D.S. Changes in heart rate and heart rate variability before ambulatory ischemic events. J. Am. Coll. Cardiol. 2001, 38, 742–749. [Google Scholar] [CrossRef]
- Kovach, J.A.; Nearing, B.D.; Verrier, R.L. Angerlike behavioral state potentiates myocardial ischemia-induced T-wave alternans in canines. J. Am. Coll. Cardiol. 2001, 37, 1719–1725. [Google Scholar] [CrossRef]
- Lind, L.; Johansson, K.; Hall, J. The effects of mental stress and the cold pressure test on flow-mediated vasodilation. Blood Press. 2002, 11, 22–27. [Google Scholar] [CrossRef] [PubMed]
- Rosmond, R. Role of stress in the pathogenesis of the metabolic syndrome. Psychoneuroendocrinology 2005, 30, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Williams, J.E.; Nieto, F.J.; Sanford, C.P.; Couper, D.J.; Tyroler, H.A. The association between trait anger and incident stroke risk: The atherosclerosis risk in communities (ARIC) study. Stoke 2002, 30, 13–19. [Google Scholar] [CrossRef]
- Williams, J.E.; Nieto, F.J.; Sanford, C.P.; Tyroler, H.A. Effects of an angry temperament on coronary heart disease risk: The atherosclerosis risk in communities study. Am. J. Epidemiol. 2001, 154, 230–235. [Google Scholar] [CrossRef] [PubMed]
- Blom, K.; Baker, B.; How, M.; Dai, M.; Irvine, J.; Abbey, S.; Abramson, B.L.; Myers, M.G.; Kiss, A.; Perkins, N.J. Hypertension analysis of stress reduction using mindfulness meditation and yoga: Results from the harmony randomized controlled trial. Am. J. Hypertens. 2013, 27, 122–129. [Google Scholar] [CrossRef] [PubMed]
- Kabat-Zinn, J.; Lipworth, L.; Burney, R. The clinical use of mindfulness meditation for the self-regulation of chronic pain. J. Behav. Med. 1985, 8, 163–190. [Google Scholar] [CrossRef] [PubMed]
- Schneider, R.H.; Grim, C.E.; Rainforth, M.V.; Kotchen, T.; Nidich, S.I.; Gaylord-King, C.; Salerno, J.W.; Kotchen, J.M.; Alexander, C.N. Stress reduction in the secondary prevention of cardiovascular disease: Randomized, controlled trial of transcendental meditation and health education in Blacks. Circ. Cardiovasc. Qual. Outcomes 2012, 5, 750–758. [Google Scholar] [CrossRef] [PubMed]
- Schneider, R.H.; Castillo-Richmond, A.; Alexander, C.N.; Myers, H.; Kaushik, V.; Aranguri, C.; Norris, K.; Haney, C.; Rainforth, M.; Calderon, R.; Nidich, S. Behavioral treatment of hypertensive heart disease in African Americans: Rationale and design of a randomized controlled trial. Behav. Med. 2001, 27, 83–95. [Google Scholar] [CrossRef] [PubMed]
- Gergen Barnett, K.A. In pursuit of the fourth aim in health care: The joy of practice. Med. Clin. N. Am. 2017, 101, 1031–1040. [Google Scholar] [CrossRef] [PubMed]
- Diamond, S.J.; Thomas, C.R.; Desai, S.; Holliday, E.B.; Jagsi, R.; Schmitt, C.; Enestvedt, B.K. Gender differences in publication productivity, academic rank, and career duration among U.S. academic gastroenterology faculty. Acad. Med. J. Assoc. Am. Med. Coll. 2016, 91, 1158–1163. [Google Scholar] [CrossRef] [PubMed]
- Bruce, M.A.; Martins, D.; Duru, K.; Beech, B.M.; Sims, M.; Harawa, N.; Vargas, R.; Kermah, D.; Nicholas, S.B.; Brown, A.; et al. Church attendance, allostatic load and mortality in middle aged adults. PLoS ONE 2017, 12, e0177618. [Google Scholar] [CrossRef] [PubMed]
- Buric, I.; Farias, M.; Jong, J.; Mee, C.; Brazil, I.A. What is the molecular signature of mind-body interventions? A systematic review of gene expression changes induced by meditation and related practices. Front. Immunol. 2017, 8, 670. [Google Scholar] [CrossRef] [PubMed]
- Duraimani, S.; Schneider, R.H.; Randall, O.S.; Nidich, S.I.; Xu, S.; Ketete, M.; Rainforth, M.A.; Gaylord-King, C.; Salerno, J.W.; Fagan, J. Effects of lifestyle modification on telomerase gene expression in hypertensive patients: A pilot trial of stress reduction and health education programs in african americans. PLoS ONE 2015, 10, e0142689. [Google Scholar] [CrossRef] [PubMed]
- Epel, E.S.; Puterman, E.; Lin, J.; Blackburn, E.H.; Lum, P.Y.; Beckmann, N.D.; Zhu, J.; Lee, E.; Gilbert, A.; Rissman, R.A.; Tanzi, R.E.; Schadt, E.E. Meditation and vacation effects have an impact on disease-associated molecular phenotypes. Transl. Psychiatr. 2016, 6, e880. [Google Scholar] [CrossRef] [PubMed]
- Ellis, J.R.; Tamvakis, K.; Nanopoulos, D.V. Grand unification in simple supergravity. Phys. Lett. B 1982, 121, 123–129. [Google Scholar] [CrossRef]
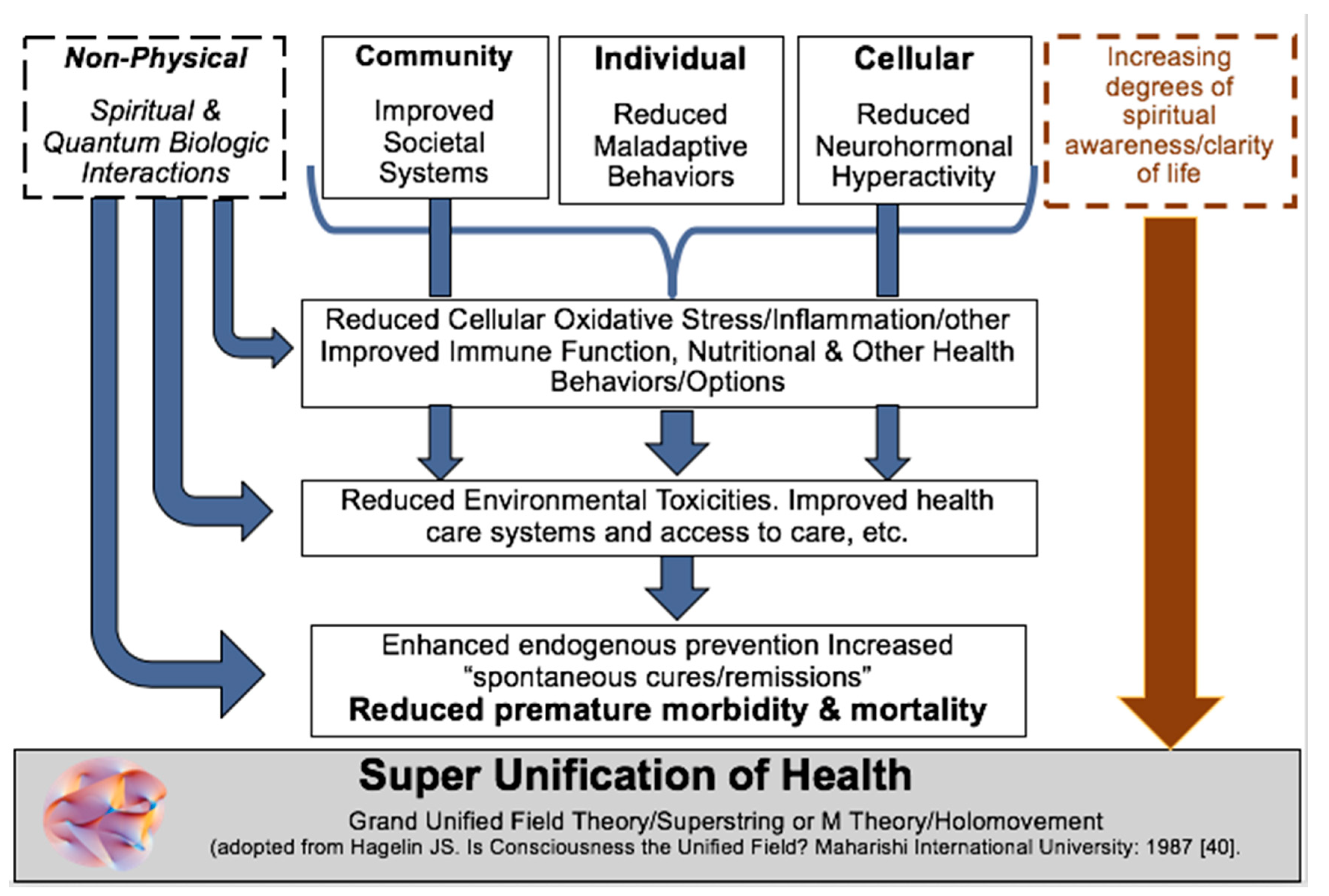
- Hagelin, J.S. Is consciousness the unified field? A field theorist’s perspective. Conscious. Based Educ. Phys. 1987, 1, 29–87. [Google Scholar]
- Aviles, J.M.; Whelan, S.E.; Hernke, D.A.; Williams, B.A.; Kenny, K.E.; O’Fallon, W.M.; Kopecky, S.L. Intercessory prayer and cardiovascular disease progression in a coronary care unit population: A randomized controlled trial. Mayo Clin. Proc. 2001, 76, 1192–1198. [Google Scholar] [CrossRef] [PubMed]
- Coffey, D.S. Self-organization, complexity and chaos: The new biology for medicine. Nat. Med. 1998, 4, 882–885. [Google Scholar] [CrossRef] [PubMed]
- Bohm, D. Wholeness and the Implicate Order; Routledge: New York, NY, USA, 2002. [Google Scholar]
- Koenig, H.G. Spirituality in Patient Care: Why How, When, and What; Templeton Press: West Conshohocken, PA, USA, 2013. [Google Scholar]
- Kim, J.Y.; Chan, M. Poverty, health, and societies of the future. JAMA 2013, 310, 901–902. [Google Scholar] [CrossRef] [PubMed]
- Escoto, K.H.; Milbury, K.; Nguyen, N.; Cho, D.; Roberson, C.; Wetter, D.; McNeill, L.H. Use of complementary health practices in a church-based African American cohort. J. Altern. Complement. Med. 2018. [Google Scholar] [CrossRef] [PubMed]
- Spears, C.A.; Houchins, S.C.; Bamatter, W.P.; Barrueco, S.; Hoover, D.S.; Perskaudas, R. Perceptions of mindfulness in a low-income, primarily African American treatment-seeking sample. Mindfulness 2017, 8, 1532–1543. [Google Scholar] [CrossRef] [PubMed]
- Zernicke, K.A.; Campbell, T.S.; Speca, M.; McCabe-Ruff, K.; Flowers, S.; Dirkse, D.A.; Carlson, L.E. The eCALM Trial-eTherapy for cancer applying mindfulness: Online mindfulness-based cancer recovery program for underserved individuals living with cancer in Alberta: Protocol development for a randomized wait-list controlled clinical trial. BMC Complement. Altern. Med. 2013, 13, 34. [Google Scholar] [CrossRef] [PubMed]
- Schneider, R.H.; Walton, K.G.; Salerno, J.W.; Nidich, S.I. Cardiovascular disease prevention and health promotion with the transcendental meditation program and Maharishi consciousness-based health care. Ethn. Dis. 2006, 16, S4. [Google Scholar] [PubMed]
- Chödrön, P. The Places that Scare You: A Guide to Fearlessness in Difficult Times; Shambhala Publications: Boston, MA, USA, 2007. [Google Scholar]
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Bruce, M.A.; Skrine Jeffers, K.; King Robinson, J.; Norris, K.C. Contemplative Practices: A Strategy to Improve Health and Reduce Disparities. Int. J. Environ. Res. Public Health 2018, 15, 2253. https://doi.org/10.3390/ijerph15102253
Bruce MA, Skrine Jeffers K, King Robinson J, Norris KC. Contemplative Practices: A Strategy to Improve Health and Reduce Disparities. International Journal of Environmental Research and Public Health. 2018; 15(10):2253. https://doi.org/10.3390/ijerph15102253
Chicago/Turabian StyleBruce, Marino A., Kia Skrine Jeffers, Jan King Robinson, and Keith C. Norris. 2018. "Contemplative Practices: A Strategy to Improve Health and Reduce Disparities" International Journal of Environmental Research and Public Health 15, no. 10: 2253. https://doi.org/10.3390/ijerph15102253
APA StyleBruce, M. A., Skrine Jeffers, K., King Robinson, J., & Norris, K. C. (2018). Contemplative Practices: A Strategy to Improve Health and Reduce Disparities. International Journal of Environmental Research and Public Health, 15(10), 2253. https://doi.org/10.3390/ijerph15102253




