Assessing Women’s Negative Sanitation Experiences and Concerns: The Development of a Novel Sanitation Insecurity Measure
Abstract
:1. Introduction
2. Materials and Methods
2.1. Setting
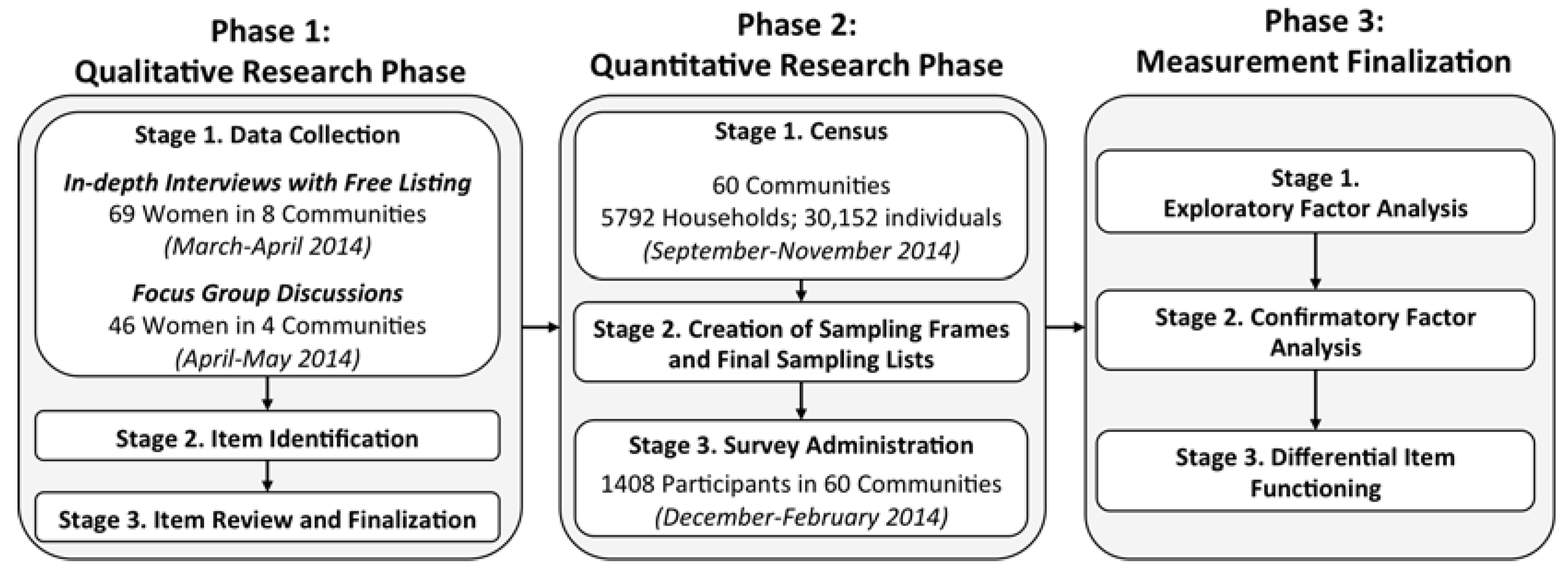
2.2. Overview of Research Design
2.3. Phase 1: Qualitative Research
2.3.1. Phase 1, Stage 1: Data Collection
2.3.2. Phase 1, Stage 2: Item Identification
2.3.3. Phase 1, Stage 3: Item Review and Finalization
2.4. Phase 2: Quantitative Research
2.4.1. Phase 2, Stage 1: Household Census
2.4.2. Phase 2, Stage 2: Creation of Sampling Frames and Final Sampling Lists
2.4.3. Phase 2, Stage 3: Survey Administration
2.5. Phase 3: Measurement Finalization
2.5.1. Phase 3, Stage 1: Exploratory Factor Analysis
2.5.2. Phase 3, Stage 2: Confirmatory Factor Analysis
2.5.3. Phase 3, Stage 1: Assessment of Differential Item Functioning (DIF)
2.6. Sanitation Insecurity Factor Scores
2.7. Ethics
3. Results
3.1. Participant Demographics
3.2. Sanitation Insecurity Survey Items
3.3. Exploratory Factor Analysis
3.4. Confirmatory Factor Analysis
3.5. Assessment of Differential Item Functioning
3.6. Final Measure
3.7. Sanitation Insecurity Scores
4. Discussion
Strengths and Limitations
5. Conclusions
Supplementary Materials
Acknowledgments
Author Contributions
Conflicts of Interest
Appendix A
| Part A. Urination Module | ||||||
| How Often Have You Experienced Any of the Following in the Previous 30 Days When Going to Urinate? | ||||||
| F1 | U01 | Worried about not having a proper facility to urinate | 01 Never | 02 Sometimes | 03 Often | 04 Always |
| F2 | U02 | Could not always go to urinate when there was a need | 01 | 02 | 03 | 04 |
| F1 | U03 | Worried that someone would see me while urinating | 01 | 02 | 03 | 04 |
| F2 | U04 | Experience difficulty controlling the urge to urinate | 01 | 02 | 03 | 04 |
| F1 | U05 | Had difficulty finding a clean place to urinate | 01 | 02 | 03 | 04 |
| F1 | U06 | Felt worried that I would step on urine | 01 | 02 | 03 | 04 |
| F2 | U07 | Worried people would talk about me if they saw me | 01 | 02 | 03 | 04 |
| F1 | U08 | Felt concerned I would get an infection if I was urinating in an unsuitable/dirty place | 01 | 02 | 03 | 04 |
| F1 | U09 | Feared I would be harmed by animals or insects when I went to urinate | 01 | 02 | 03 | 04 |
| F1 | U10 | Feared I would be harmed by someone when I went to urinate | 01 | 02 | 03 | 04 |
| F4 | U11 | Felt scared urinating in the dark at night | 01 | 02 | 03 | 04 |
| F1 | U12 | Felt concerned I would get an infection if I urinated on someone else's urine | 01 | 02 | 03 | 04 |
| F4 | U13 | Felt scared of ghosts when I went to urinate at night | 01 | 02 | 03 | 04 |
| F2 | U14 | Had difficulty finding a private place to urinate | 01 | 02 | 03 | 04 |
| F6 | U15 | Had difficulty or pain sitting or getting up for urination | 01 | 02 | 03 | 04 |
| F3 | U16 | Had difficulty accessing water for urination | 01 | 02 | 03 | 04 |
| F2 | U17 | Had to suppress urge because people were around and could not go | 01 | 02 | 03 | 04 |
| F3 | U18 | Had to do extra work washing clothes because of dirty conditions where urinating | 01 | 02 | 03 | 04 |
| F5 | U19 | Had to leave dependents (like children, sick or elderly) alone to urinate | 01 | 02 | 03 | 04 |
| F2 | U20 | Had to stand while urinating because someone came | 01 | 02 | 03 | 04 |
| F5 | U21 | Had trouble finding someone to watch dependents (like children, sick or elderly) so I could urinate | 01 | 02 | 03 | 04 |
| F3 | U22 | Withheld water to control urge to urinate | 01 | 02 | 03 | 04 |
| F2 | U23 | Had to suppress when workload was high | 01 | 02 | 03 | 04 |
| F2 | U24 | Worried others would get upset if asked to accompany for urination | 01 | 02 | 03 | 04 |
| F2 | U25 | Had to suppress when I got an urge at night | 01 | 02 | 03 | 04 |
| Part B. Defecation Module | ||||||
| How Often Have You Experienced Any of the Following in the Previous 30 Days When Going to Defecate? | ||||||
| F7 | D01 | Worried about not having toilet to defecate | 01 Never | 02 Sometimes | 03 Often | 04 Always |
| F7 | D02 | Had to go far to defecate | 01 | 02 | 03 | 04 |
| F7 | D03 | Defecation process/Activity of defecation took a long time to complete | 01 | 02 | 03 | 04 |
| F7 | D04 | Had difficulty finding a clean place to defecate | 01 | 02 | 03 | 04 |
| F7 | D05 | Could not access preferred location | 01 | 02 | 03 | 04 |
| F6 | D06 | Worried I would fall when going to defecate | 01 | 02 | 03 | 04 |
| F2 | D07 | Had to suppress urge when workload was high | 01 | 02 | 03 | 04 |
| F4 | D08 | Felt scared defecating in the dark at night | 01 | 02 | 03 | 04 |
| F2 | D09 | Worried people would talk about me if they saw me | 01 | 02 | 03 | 04 |
| F1 | D10 | Feared I would be harmed by animals or insects when I went to defecate | 01 | 02 | 03 | 04 |
| F7 | D11 | Had to do extra work washing clothes because of dirty conditions where defecating | 01 | 02 | 03 | 04 |
| F1 | D12 | Worried about getting an infection when going to defecate | 01 | 02 | 03 | 04 |
| F6 | D13 | Had difficulty or pain squatting for defecation | 01 | 02 | 03 | 04 |
| F4 | D14 | Felt scared of ghosts when I went to defecate at night | 01 | 02 | 03 | 04 |
| F3 | D15 | Had difficulty accessing water for defecation | 01 | 02 | 03 | 04 |
| F3 | D16 | Had difficulty cleaning/washing myself after defecation | 01 | 02 | 03 | 04 |
| F2 | D17 | Had to suppress urge because I can only defecate at certain times of the day | 01 | 02 | 03 | 04 |
| F1 | D18 | Feared I would be harmed by someone when I went to defecate | 01 | 02 | 03 | 04 |
| F5 | D19 | Had trouble finding someone to watch dependents (like children, sick or elderly) so I could defecate | 01 | 02 | 03 | 04 |
| F2 | D20 | Had trouble controlling urge to defecate | 01 | 02 | 03 | 04 |
| F7 | D21 | Worried about defecating in the same place as others | 01 | 02 | 03 | 04 |
| F3 | D22 | Withheld food to control urge to defecate | 01 | 02 | 03 | 04 |
| F5 | D23 | Worried about dependents (children, sick or elderly) who need me when I go to defecate | 01 | 02 | 03 | 04 |
| F7 | D24 | Worried that have no money to build or maintain toilet | 01 | 02 | 03 | 04 |
| F7 | D25 | Have had to go back and forth to defecation location because could not find privacy | 01 | 02 | 03 | 04 |
References
- Walker, C.L.F.; Rudan, I.; Liu, L.; Nair, H.; Theodoratou, E.; Bhutta, Z.A.; O’Brien, K.L.; Campbell, H.; Black, R.E. Global burden of childhood pneumonia and diarrhoea. Lancet 2013, 381, 1405–1406. [Google Scholar] [CrossRef]
- Guerrant, R.L.; DeBoer, M.D.; Moore, S.R.; Scharf, R.J.; Lima, A.A. The impoverished gut––A triple burden of diarrhoea, stunting and chronic disease. Nat. Rev. Gastroenterol. Hepatol. 2013, 10, 220–229. [Google Scholar] [CrossRef] [PubMed]
- Berkman, D.S.; Lescano, A.G.; Gilman, R.H.; Lopez, S.L.; Black, M.M. Effects of stunting, diarrhoeal disease, and parasitic infection during infancy on cognition in late childhood: A follow-up study. Lancet 2002, 359, 564–571. [Google Scholar] [CrossRef]
- Dillingham, R.; Guerrant, R.L. Childhood stunting: Measuring and stemming the staggering costs of inadequate water and sanitation. Lancet 2004, 363, 94–95. [Google Scholar] [CrossRef]
- Stocks, M.E.; Ogden, S.; Haddad, D.; Addiss, D.G.; McGuire, C.; Freeman, M.C. Effect of water, sanitation, and hygiene on the prevention of trachoma: A systematic review and meta-analysis. PLoS Med. 2014, 11, e1001605. [Google Scholar] [CrossRef] [PubMed]
- Grimes, J.E.; Croll, D.; Harrison, W.E.; Utzinger, J.R.; Freeman, M.C.; Templeton, M.R. The relationship between water, sanitation and schistosomiasis: A systematic review and meta-analysis. PLoS Negl. Trop. Dis. 2014, 8, e3296. [Google Scholar] [CrossRef] [PubMed]
- Wolf, J.; Prüss-Ustün, A.; Cumming, O.; Bartram, J.; Bonjour, S.; Cairncross, S.; Clasen, T.; Colford, J.M.; Curtis, V.; France, J.; et al. Systematic review: Assessing the impact of drinking water and sanitation on diarrhoeal disease in low-and middle-income settings: Systematic review and meta-regression. Trop. Med. Int. Health 2014, 19, 928–942. [Google Scholar] [CrossRef] [PubMed]
- Ziegelbauer, K.; Speich, B.; Mausezahl, D.; Bos, R.; Keiser, J.; Utzinger, J. Effect of sanitation on soil-transmitted helminth infection: Systematic review and meta-analysis. PLoS Med. 2012, 9, e1001162. [Google Scholar] [CrossRef] [PubMed]
- Caruso, B.A.; Sevilimedu, V.; Fung, I.C.-H.; Patkar, A.; Baker, K.K. Gender disparities in water, sanitation, and global health. Lancet 2015, 386, 650–651. [Google Scholar] [CrossRef]
- World Health Organization/The United Nations Children’s Fund. Progress on Drinking Water and Sanitation: 2015 Update and MDG Assessment; World Health Organization (WHO): Geneva, Switzerland, 2015. [Google Scholar]
- Barnard, S.; Routray, P.; Majorin, F.; Peletz, R.; Boisson, S.; Sinha, A.; Clasen, T. Impact of indian total sanitation campaign on latrine coverage and use: A cross-sectional study in orissa three years following programme implementation. PLoS ONE 2013, 8, e71438. [Google Scholar] [CrossRef] [PubMed]
- Coffey, D.; Gupta, A.; Hathi, P.; Khurana, N.; Spears, D.; Srivastav, N.; Vyas, S. Revealed preference for open defecation. Econ. Polit. Wkly. 2014, 49, 43. [Google Scholar]
- Padhi, B.K.; Baker, K.K.; Dutta, A.; Cumming, O.; Freeman, M.C.; Satpathy, R.; Das, B.S.; Panigrahi, P. Risk of adverse pregnancy outcomes among women practicing poor sanitation in rural India: A population-based prospective cohort study. PLoS Med. 2015, 12, e1001851. [Google Scholar] [CrossRef] [PubMed]
- Jadhav, A.; Weitzman, A.; Smith-Greenaway, E. Household sanitation facilities and women’s risk of non-partner sexual violence in India. BMC Public Health 2016, 16, 1139. [Google Scholar] [CrossRef] [PubMed]
- Winter, S.C.; Barchi, F. Access to sanitation and violence against women: Evidence from demographic health survey (DHS) data in Kenya. Int. J. Environ. Health Res. 2016, 26, 291–305. [Google Scholar] [CrossRef] [PubMed]
- Bapat, M.; Agarwal, I. Our needs, our priorities; women and men from the slums in Mumbai and Pune talk about their needs for water and sanitation. Environ. Urban. 2003, 15, 71–86. [Google Scholar] [CrossRef]
- Joshi, D.; Fawcett, B.; Mannan, F. Health, hygiene and appropriate sanitation: Experiences and perceptions of the urban poor. Environ. Urban. 2011, 23, 91–111. [Google Scholar] [CrossRef]
- Lennon, S. Fear and Anger: Perceptions of Risks Related to Sexual Violence Against Women Linked to Water and Sanitation in Delhi, India; LSHTM: London, UK, 2011. [Google Scholar]
- Massey, K. Insecurity and Shame: Exploration of the Impact of the Lack of Sanitation on Women in the Slums of Kampala, Uganda; LSHTM: London, UK, 2011. [Google Scholar]
- Remigios, M.V. Women-water-sanitation: The case of rimuka high-density suburb in Kadoma, Zimbabwe. Agenda 2011, 25, 113–121. [Google Scholar]
- Bisung, E.; Elliott, S.J. “Everyone is exhausted and frustrated”: Exploring psychosocial impacts of the lack of access to safe water and adequate sanitation in Usoma, Kenya. J. Water Sanit. Hyg. Dev. 2016, washdev2016122. [Google Scholar] [CrossRef]
- Sahoo, K.C.; Hulland, K.R.; Caruso, B.A.; Swain, R.; Freeman, M.C.; Panigrahi, P.; Dreibelbis, R. Sanitation-related psychosocial stress: A grounded theory study of women across the life-course in Odisha, India. Soc. Sci. Med. 2015, 139, 80–89. [Google Scholar] [CrossRef] [PubMed]
- Hulland, K.R.; Chase, R.P.; Caruso, B.A.; Swain, R.; Biswal, B.; Sahoo, K.C.; Panigrahi, P.; Dreibelbis, R. Sanitation, stress, and life stage: A systematic data collection study among women in Odisha, India. PLoS ONE 2015, 10, e0141883. [Google Scholar] [CrossRef] [PubMed]
- Hirve, S.; Lele, P.; Sundaram, N.; Chavan, U.; Weiss, M.; Steinmann, P.; Juvekar, S. Psychosocial stress associated with sanitation practices: Experiences of women in a rural community in India. J. Water Sanit. Hyg. Dev. 2015, 5, 115–126. [Google Scholar] [CrossRef]
- Bisung, E.; Elliott, S.J. Psychosocial impacts of the lack of access to water and sanitation in low-and middle-income countries: A scoping review. J. Water Health 2016, wh2016158. [Google Scholar] [CrossRef] [PubMed]
- Hamelin, A.-M.; Beaudry, M.; Habicht, J.-P. Characterization of household food insecurity in Quebec: Food and feelings. Soc. Sci. Med. 2002, 54, 119–132. [Google Scholar] [CrossRef]
- Hadley, C.; Lindstrom, D.; Tessema, F.; Belachew, T. Gender bias in the food insecurity experience of Ethiopian adolescents. Soc. Sci. Med. 2008, 66, 427–438. [Google Scholar] [CrossRef] [PubMed]
- Frongillo, E.A.; Nanama, S. Development and validation of an experience-based measure of household food insecurity within and across seasons in northern Burkina Faso. J. Nutr. 2006, 136, 1409S–1419S. [Google Scholar] [PubMed]
- Frongillo, E.; Nanama, S.; Wolfe, W. Technical Guide to Developing a Direct, Experience-Based Measurement Tool for Household Food Insecurity. Ph.D. Thesis, Food and Nutrition Technical Assistance Project, Academy for Educational Development, Washington, DC, USA, 2004; pp. 1–51. [Google Scholar]
- Wolfe, W.S.; Frongillo, E.A. Building household food-security measurement tools from the ground up. Food Nutr. Bull. 2001, 22, 5–12. [Google Scholar] [CrossRef]
- Weaver, L.J.; Hadley, C. Moving beyond hunger and nutrition: A systematic review of the evidence linking food insecurity and mental health in developing countries. Ecol. Food Nutr. 2009, 48, 263–284. [Google Scholar] [CrossRef] [PubMed]
- Wutich, A.; Ragsdale, K. Water insecurity and emotional distress: Coping with supply, access, and seasonal variability of water in a Bolivian squatter settlement. Soc. Sci. Med. 2008, 67, 2116–2125. [Google Scholar] [CrossRef] [PubMed]
- Hadley, C.; Wutich, A. Experience-based measures of food and water security: Biocultural approaches to grounded measures of insecurity. Hum. Organ. 2009, 68, 451–460. [Google Scholar] [CrossRef]
- Stevenson, E.G.; Greene, L.E.; Maes, K.C.; Ambelu, A.; Tesfaye, Y.A.; Rheingans, R.; Hadley, C. Water insecurity in 3 dimensions: An anthropological perspective on water and women’s psychosocial distress in Ethiopia. Soc. Sci. Med. 2012, 75, 392–400. [Google Scholar] [CrossRef] [PubMed]
- Food & Agriculture Organization. The State of Food Insecurity in the World, 2004; Food & Agriculture Organization: Rome, Italy, 2004. [Google Scholar]
- Hadley, C.; Freeman, M.C. Assessing reliability, change after intervention, and performance of a water insecurity scale in rural Ethiopia. Food Secur. Sci. Sociol. Econ. Food Prod. Access Food 2016, 8, 855–864. [Google Scholar] [CrossRef]
- O’Reilly, K. From toilet insecurity to toilet security: Creating safe sanitation for women and girls. Wiley Interdiscip. Rev. Water 2016, 3, 19–24. [Google Scholar] [CrossRef]
- Kandiyoti, D. Bargaining with patriarchy. Gender Soc. 1988, 2, 274–290. [Google Scholar] [CrossRef]
- Khanna, T.; Das, M. Why gender matters in the solution towards safe sanitation? Reflections from rural india. Glob. Public Health 2015, 1–17. [Google Scholar] [CrossRef] [PubMed]
- Routray, P.; Schmidt, W.-P.; Boisson, S.; Clasen, T.; Jenkins, M.W. Socio-cultural and behavioural factors constraining latrine adoption in rural coastal Odisha: An exploratory qualitative study. BMC Public Health 2015, 15, 880. [Google Scholar] [CrossRef] [PubMed]
- Stevenson, E.; Ambelu, A.; Caruso, B.; Tesfaye, Y.; Freeman, M. Community water improvement, household water insecurity, and women’s psychological distress: An intervention and control study in Ethiopia. PLoS ONE 2016, 11, e0153432. [Google Scholar] [CrossRef] [PubMed]
- Clasen, T.; Boisson, S.; Routray, P.; Cumming, O.; Jenkins, M.; Ensink, J.H.; Bell, M.; Freeman, M.C.; Peppin, S.; Schmidt, W.-P. The effect of improved rural sanitation on diarrhoea and helminth infection: Design of a cluster-randomized trial in Orissa, India. Emerg. Themes Epidemiol. 2012, 9, 7. [Google Scholar] [CrossRef] [PubMed]
- Clasen, T.; Boisson, S.; Routray, P.; Torondel, B.; Bell, M.; Cumming, O.; Ensink, J.; Freeman, M.; Jenkins, M.; Odagiri, M. Effectiveness of a rural sanitation programme on diarrhoea, soil-transmitted helminth infection, and child malnutrition in Odisha, India: A cluster-randomised trial. Lancet Glob. Health 2014, 2, e645–e653. [Google Scholar] [CrossRef]
- Clasen, T.F.; Bostoen, K.; Schmidt, W.P.; Boisson, S.; Fung, I.C.; Jenkins, M.W.; Scott, B.; Sugden, S.; Cairncross, S. Interventions to improve disposal of human excreta for preventing diarrhoea. Cochrane Database Syst. Rev. 2010, 16, CD007180. [Google Scholar]
- Boisson, S.; Sosai, P.; Ray, S.; Routray, P.; Torondel, B.; Schmidt, W.-P.; Bhanja, B.; Clasen, T. Promoting latrine construction and use in rural villages practicing open defecation: Process evaluation in connection with a randomised controlled trial in Orissa, India. BMC Res. Notes 2014, 7, 486. [Google Scholar] [CrossRef] [PubMed]
- International Institute of Population Sciences. National Family Health Survey-4 (nfhs-$): District Fact Sheet: Puri Odisha; International Institute of Population Sciences: Mumbai, India, 2016. [Google Scholar]
- Puri Religion Census. Available online: http://www.census2011.co.in/data/religion/district/411-puri.html (accessed on 30 June 2017).
- Creswell, J.W.; Clark, V.L.P. Designing and Conducting Mixed Methods Research, 2nd ed.; SAGE Publications, Inc.: Thousand Oaks, CA, USA, 2011. [Google Scholar]
- Woods, C.M.; Oltmanns, T.F.; Turkheimer, E. Illustration of mimic-model dif testing with the schedule for nonadaptive and adaptive personality. J. Psychopathol. Behav. Assess. 2009, 31, 320–330. [Google Scholar] [CrossRef] [PubMed]
- Borgatti, S.P. Elicitation techniques for cultural domain analysis. In Enhanced Ethnographic Methods: Audiovisual Techniques, Focused Group Interviews, and Elicitation Techniques. Ethnographer Toolkit; Altamira Press: Lanham, MD, USA, 1999; pp. 115–151. [Google Scholar]
- Caruso, B.A.; Clasen, T.; Hadley, C.; Yount, K.M.; Haardoerfer, R.; Rout, M.; Dasmohapatra, M.; Cooper, H.L. Women’s gendered experiences of urination, defecation, and mesntruation in rural Odisha. India: Underst. Defin. Sanit. Insecur. 2017. Submitted. [Google Scholar]
- De-Vet, H.; Terwee, C.B.; Mokkink, L.; Knol, D. Measurement in Medicine; Cambridge University Press: Cambridge, UK, 2011. [Google Scholar]
- DiIorio, C.K. Measurement in Health Behavior: Methods of Research and Evaluation, 1st ed.; John Willey & Sons, Inc.: San Francisco, CA, USA, 2005. [Google Scholar]
- Diez-Roux, A.V. Multilevel analysis in public health research. Annu. Rev. Public Health 2000, 21, 171–192. [Google Scholar] [CrossRef] [PubMed]
- Estes, K. Sample Size Recommendations in Hierarchical Linear Modeling: A Monte Carlo Simulation of n and Predictor-Criterion Correlations; Georgia State University: Atlanta, GA, USA, 2008. [Google Scholar]
- Yount, K.M.; VanderEnde, K.; Zureick-Brown, S.; Minh, T.H.; Schuler, S.R.; Anh, H.T. Measuring attitudes about women’s recourse after exposure to intimate partner violence the att-recourse scale. J. Interpers. Violence 2014, 29, 1579–1605. [Google Scholar] [CrossRef] [PubMed]
- Bandalos, D.; Finney, S. Factor analysis: Exploratory and confirmatory. In The Reviewer’s Guide to Quantitative Methods in the Social Sciences; Hancock, G.R., Mueller, R.O., Eds.; Routledge: New York, NY, USA, 2010; pp. 93–114. [Google Scholar]
- Muthén, L.K.; Muthén, B.O. Mplus User’s Guide, 7th ed.; Muthén & Muthén: Los Angeles, CA, USA, 2014; pp. 1998–2012. [Google Scholar]
- Holgado-Tello, F.P.; Chacon-Moscoso, S.; Barbero-Garcia, I.; Vila‚ÄìAbad, E. Polychoric versus pearson correlations in exploratory and confirmatory factor analysis of ordinal variables. Qual. Quant. 2010, 44, 153–166. [Google Scholar] [CrossRef]
- Baglin, J. Improving your exploratory factor analysis for ordinal data: A demonstration using factor. Pract. Assess. Res. Eval. 2014, 19, 2. [Google Scholar]
- Costello, A.; Osborne, J. Best practices in exploratory factor analysis: Four recommendations for getting the most from your analysis. Pract. Assess. Res. Eval. 2005, 10. Available online: http://pareonline.net/getvn. asp (accessed on 9 June 2016).
- Holland, P.W.; Wainer, H. Differential Item Functioning; Lawrence Erlbaum: Hillsdale, NJ, USA, 1993. [Google Scholar]
- Steven, J. Osterlind, H.T.E. Differential Item Functioning, 2nd ed.; SAGE Publications, Inc.: Thousand Oaks, CA, USA, 2009. [Google Scholar]
- Bradley, D.J.; Bartram, J.K. Domestic water and sanitation as water security: Monitoring, concepts and strategy. Philos. Trans. Royal Soc. A: Math. Phys. Eng. Sci. 2013, 371, 20120420. [Google Scholar] [CrossRef] [PubMed]
- Routray, P.; Torondel, B.; Clasen, T.; Schmidt, W.-P. Women’s role in sanitation decision making in rural coastal Odisha, India. PLoS ONE 2017, 12, e0178042. [Google Scholar] [CrossRef] [PubMed]
- Burt, Z.; Nelson, K.; Ray, I. Towards Gender Equality thRough Sanitation Access; UN Women Headquarters: New York, NY, USA, 2016. [Google Scholar]
- Freshwater Action Network South Asia. The Water Supply and Sanitation Collaborative Council. Leave no One behind: Voices of Women, Adolescent Girls, Elderly and Disabled People, and Sanitation Workers. Available online: https://sanitationupdates.files.wordpress.com/2016/01/leave-no-one-behind-report-2016-wsscc-fansa.pdf (accessed on 6 September 2016).
- Routray, P.; Torondel, B.; Jenkins, M.W.; Clasen, T.; Schmidt, W.-P. Processes and challenges of community mobilisation for latrine promotion under Nirmal Bharat Abhiyan in rural Odisha, India. BMC Public Health 2017, 17, 453. [Google Scholar] [CrossRef] [PubMed]
- Hafskjold, B.; Pop-Stefanija, B.; Giles-Hansen, C.; Weerts, E.; Flynn, E.; Wilbur, J.; Brogan, K.; Ackom, K.; Farrington, M.; Peuschel, M. Taking stock: Incompetent at incontinence—Why are we ignoring the needs of incontinence sufferers? Waterlines 2016, 35, 219–227. [Google Scholar] [CrossRef]
- Erhard, L.; Degabriele, J.; Naughton, D.; Freeman, M.C. Policy and provision of wash in schools for children with disabilities: A case study in Malawi and Uganda. Glob. Public Health 2013, 8, 1000–1013. [Google Scholar] [CrossRef] [PubMed]
- Internet Relay Chat (IRC). Towards Effective Programming for Wash in Schools: A Manual on Scaling up Programmes for Water, Sanitation and Hygiene in Schools; IRC International Water and Sanitation Centre: Delft, The Netherlands, 2007. [Google Scholar]
- The United Nations Children’s Fund. Design and Construction Manual for Water Supply and Sanitary Facilities in Primary Schools in Ethiopia; UNICEF: New York, NY, USA, 2012. [Google Scholar]
- Sommer, M. Putting menstrual hygiene management on to the school water and sanitation agenda. Waterlines 2010, 29, 268–277. [Google Scholar] [CrossRef]
- Joint Monitoring Programme. Wash Post-2015: Proposed Targets and Indicators for Households, Schools and Health Centers. Available online: https://data.unicef.org/wp-content/uploads/2015/12/JMP_FactSheets_2_FINAL_156.pdf (accessed on 6 September 2016).
| Characteristics | All | 1. Unmarried (UM) | 2. Recently Married (<3 Years) (RM) | 3. Married (>3 Years) (M) | 4. Over 49 (OW) | |||||
|---|---|---|---|---|---|---|---|---|---|---|
| Number of Participants | 1408 | 341 | 320 | 395 | 352 | |||||
| Village Status | ||||||||||
| Control | 707 | 50% | 175 | 51% | 162 | 51% | 193 | 49% | 177 | 50% |
| Intervention | 701 | 50% | 166 | 49% | 158 | 49% | 202 | 51% | 175 | 50% |
| Age | 36 | (18) | 21 | (3) | 24 | (3) | 35 | (7) | 63.6 | (10) |
| Education | ||||||||||
| None | 335 | 24% | 3 | 1% | 7 | 2% | 80 | 20% | 245 | 70% |
| Some Primary | 410 | 29% | 53 | 16% | 68 | 21% | 190 | 48% | 99 | 28% |
| Some Secondary | 588 | 42% | 235 | 69% | 232 | 73% | 114 | 29% | 8 | 2% |
| Higher than Secondary | 75 | 5% | 50 | 15% | 13 | 4% | 12 | 3% | 0 | 0% |
| Possession of Government Assistance Card 1 | ||||||||||
| Yes | 1033 | 73% | 259 | 76% | 223 | 70% | 286 | 73% | 265 | 75% |
| Religion | ||||||||||
| Hindu | 1389 | 99% | 339 | 99% | 315 | 98% | 386 | 98% | 349 | 99% |
| Muslim | 19 | 1% | 2 | 1% | 5 | 2% | 9 | 2% | 3 | 1% |
| Caste 1 | ||||||||||
| Brahmin | 38 | 3% | 10 | 3% | 8 | 3% | 12 | 3% | 8 | 2% |
| Forward/General | 672 | 48% | 150 | 44% | 151 | 47% | 171 | 43% | 155 | 44% |
| Scheduled Caste (SC) | 247 | 18% | 51 | 15% | 59 | 19% | 76 | 19% | 61 | 17% |
| Other Backward Caste (OBC) | 464 | 33% | 124 | 37% | 92 | 29% | 128 | 32% | 120 | 34% |
| Scheduled Tribe (ST) | 11 | 1% | 2 | 1% | 2 | 1% | 3 | 1% | 4 | 1% |
| Don’t Know | 19 | 1% | 3 | 1% | 7 | 2% | 5 | 1% | 4 | 1% |
| Has children | 906 | 64% | 0 | 1% | 180 | 56% | 382 | 97% | 344 | 98% |
| Number of Children | 2 | (2) | 0 | (0) | 1 | (1) | 2 | (1) | 5 | (2) |
| Primary Drinking Water Source Location 2 | ||||||||||
| In Dwelling | 131 | 10% | 15 | 5% | 43 | 15% | 33 | 9% | 40 | 12% |
| In Compound | 273 | 20% | 68 | 21% | 71 | 24% | 70 | 19% | 64 | 19% |
| Outside Compound | 927 | 70% | 240 | 74% | 183 | 62% | 271 | 72% | 233 | 69% |
| Household Latrine Ownership 2 | ||||||||||
| Yes | 414 | 29% | 71 | 21% | 128 | 40% | 103 | 26% | 112 | 32% |
| No | 815 | 58% | 226 | 66% | 155 | 48% | 241 | 61% | 193 | 55% |
| Under Construction | 177 | 13% | 44 | 13% | 37 | 12% | 49 | 13% | 47 | 13% |
| Factors and Associated Items | Item | Final EFA (N1 = 703) | CFA (N2 = 705) | Baseline MIMIC Model (N2 = 705) | Final MIMIC Model 1 (N2 = 705) | Final CFA 2 (N2 = 705) |
|---|---|---|---|---|---|---|
| Factor 1: Potential Harms | ||||||
| Felt concerned I would get an infection if I was urinating in an unsuitable/dirty place | U10 | 0.822 | 0.963 * | 0.962 * | 0.962 * | 0.964 * |
| Felt concerned I would get an infection if I urinated on someone elses urine | U15 | 0.810 | 0.953 * | 0.951 * | 0.951 * | 0.956 * |
| Worried about getting an infection when going to defecate | D15 | 0.779 | 0.958 * | 0.961 * | 0.961 * | 0.943 * |
| Had difficulty finding clean place to urinate | U06 | 0.773 | 0.883 * | 0.889 * | 0.889 * | 0.885 * |
| Felt worried that I would step on urine | U08 | 0.758 | 0.853 * | 0.856 * | 0.856 * | 0.855 * |
| Feared I would be harmed by someone when I went to urinate | U12 | 0.910 | 0.817 * | 0.803 * | 0.803 * | 0.825 * |
| Worried about not having a proper facility to urinate | U01 | 0.697 | 0.825 * | 0.830 * | 0.830 * | 0.824 * |
| Worried that someone would see me while urinating | U03 | 0.714 | 0.828 * | 0.824 * | 0.824 * | 0.819 * |
| Feared I would be harmed by animals or insects when I went to urinate | U11 | 0.821 | 0.806 * | 0.799 * | 0.799 * | 0.811 * |
| Feared I would be harmed by someone when I went to defecate | D26 | 0.706 | 0.798 * | 0.808 * | 0.808 * | 0.794 * |
| Feared I would be harmed by animals or insects when I went to defecate | D12 | 0.791 | 0.724 * | 0.733 * | 0.733 * | 0.717 * |
| Factor 2: Social expectations resultant repercussions | ||||||
| Had difficulty finding a private place to urinate | U17 | 0.760 | 0.866 * | 0.864 * | 0.863 * | 0.871 * |
| Had to suppress urge because people were around and could not go | U20 | 0.766 | 0.852 * | 0.850 * | 0.849 * | 0.855 * |
| Worried people would talk about me if they saw me | D11 | 0.803 | 0.816 * | 0.814 * | 0.814 * | 0.811 * |
| Worried people would talk about me if they saw me | U09 | 0.863 | 0.785 * | 0.780 * | 0.779 * | 0.792 * |
| Had to suppress urge because I can only defecate at certain times of the day | D25 | 0.661 | 0.792 * | 0.790 * | 0.789 * | 0.771 * |
| Had to stand while urinating because someone came | U25 | 0.610 | 0.760 * | 0.762 * | 0.761 * | 0.752 * |
| Had trouble controlling urge to defecate | D28 | 0.553 | 0.700 * | 0.729 * | 0.728 * | 0.695 * |
| Worried others would get upset if asked to accompany for urination | U31 | 0.856 | 0.707 * | 0.704 * | 0.703 * | 0.684 * |
| Could not always go to urinate when there was a need | U02 | 0.766 | 0.680 * | 0.695 * | 0.694 * | 0.681 * |
| Experienced difficulty controlling urge to urinate | U04 | 0.702 | 0.658 * | 0.681 * | 0.680 * | 0.656 * |
| Had to suppress urge [to defecate] when workload was high | D09 | 0.563 | 0.656 * | 0.655 * | 0.654 * | 0.636 * |
| Had to suppress when I got an urge at night | U32 | 0.704 | 0.593 * | 0.598 * | 0.597 * | 0.586 * |
| Had to suppress [urination] when workload was high | U29 | 0.594 | 0.587 * | 0.583 * | 0.582 * | 0.580 * |
| Had to suppress urge because did not have someone to accompany me ✢ | U26 | 0.773 | 0.724 * | 0.723 * | 0.676 * | – |
| Factor 3: Physical exertion or strain | ||||||
| Had difficulty accessing water for defecation | D21 | 0.674 | 0.906 * | 0.882 * | 0.884 * | 0.915 * |
| Had difficulty accessing water for urination | U19 | 0.612 | 0.833 * | 0.872 * | 0.873 * | 0.852 * |
| Had difficulty cleaning/washing myself after defecation | D23 | 0.709 | 0.835 * | 0.825 * | 0.828 * | 0.848 * |
| Had to do extra work washing clothes because of dirty conditions where urinating | U23 | 0.715 | 0.758 * | 0.755 * | 0.758 * | 0.752 * |
| Withheld food to control urge to defecate | D31 | 0.585 | 0.694 * | 0.700 * | 0.703 * | 0.669 * |
| Withheld water to control urge to urinate | U28 | 0.387 | 0.567 * | 0.568 * | 0.571 * | 0.564 * |
| Experienced pain during urination ✢ | U05 | 0.601 | 0.583 * | 0.639 * | 0.636 * | – |
| Experienced pain during defecation ✢ | D04 | 0.492 | 0.370 * | 0.433 * | 0.426 * | – |
| Had frequent pressure to urinate ✢ | U22 | 0.431 | – | – | – | – |
| Factor 4: Night Concerns | ||||||
| Felt scared of ghosts when I went to urinate at night | U16 | 0.870 | 0.950 * | 0.946 * | 0.946 * | 0.952 * |
| Felt scared urinating in the dark at night | U13 | 0.809 | 0.919 * | 0.923 * | 0.923 * | 0.920 * |
| Felt scared defecating in the dark at night | D10 | 0.722 | 0.918 * | 0.920 * | 0.920 * | 0.914 * |
| Felt scared of ghosts when I went to defecate at night | D18 | 0.793 | 0.915 * | 0.918 * | 0.918 * | 0.914 * |
| Factor 5: Social support | ||||||
| Had trouble finding someone to watch dependents (children, sick, elderly) so I could urinate | U27 | 0.928 | 0.939 * | 0.945 * | 0.956 * | 0.962 * |
| Had trouble finding someone to watch dependents so I could defecate | D27 | 0.933 | 0.919 * | 0.913 * | 0.928 * | 0.942 * |
| Worried about dependents (children, sick or elderly) who need me when I go to defecate | D33 | 0.920 | 0.906 * | 0.905 * | 0.918 * | 0.933 * |
| Had to leave dependents (like children, sick, or elderly) alone to urinate | U24 | 0.907 | 0.889 * | 0.880 * | 0.897 * | 0.915 * |
| Had to find someone to look after my work so I could defecate ✢ | D20 | 0.619 | 0.791 * | 0.769 * | 0.881 * | – |
| Worried others would get upset if asked to accompany for defecation ✢ | D32 | 0.481 | 0.876 * | 0.867 * | 1.033 * | – |
| Factor 6: Physical agility | ||||||
| Had difficulty or pain squatting for defecation | D17 | 0.920 | 0.951 * | 0.936 * | 0.936 * | 0.954 * |
| Had difficulty or pain sitting or getting up for urination | U18 | 0.878 | 0.925 * | 0.920 * | 0.920 * | 0.920 * |
| Worried I would fall when going to defecate | D07 | 0.801 | 0.758 * | 0.782 * | 0.782 * | 0.763 * |
| Had difficulty walking to defecation place ✢ | D19 | 0.713 | – | – | – | – |
| Factor 7: Defecation place | ||||||
| Worried about defecating in the same place as others | D29 | 0.852 | 0.944 * | 0.938 * | 0.937 * | 0.963 * |
| Worried about not having a toilet to defecate | D01 | 0.945 | 0.885 * | 0.886 * | 0.885 * | 0.900 * |
| Worried have no money to build or maintain toilet | D34 | 0.913 | 0.872 * | 0.875 * | 0.874 * | 0.890 * |
| Had difficulty finding a clean place to defecate | D05 | 0.879 | 0.876 * | 0.884 * | 0.884 * | 0.888 * |
| Could not access preferred location | D06 | 0.739 | 0.865 * | 0.870 * | 0.869 * | 0.885 * |
| Had to go back and forth to defecation location because could not find privacy | D36 | 0.765 | 0.860 * | 0.874 * | 0.873 * | 0.860 * |
| Had to go far to defecate | D02 | 0.851 | 0.799 * | 0.806 * | 0.804 * | 0.808 * |
| Defecation process/ activity of defecation took a long time to complete | D03 | 0.804 | 0.782 * | 0.797 * | 0.795 * | 0.801 * |
| Had to do extra work washing clothes because of dirty conditions where defecating | D14 | 0.683 | 0.770 * | 0.772 * | 0.770 * | 0.779 * |
| Worried that someone would see me defecating ✢ | D08 | 0.828 | 0.869 * | 0.859 * | 0.813 * | – |
| Had to suppress the urge to defecate because people were around ✢ | D24 | 0.799 | 0.851 * | 0.845 * | 0.821 * | – |
| Characteristics | Physical Environmental Factors | Social Environment Factors | Personal Constrains Factors | ||||
|---|---|---|---|---|---|---|---|
| Factor 1: Potential Harms 1 | Factor 4: Night Concerns | Factor 7: Defecation Place 2 | Factor 2: Social Expectations & Repercussions 3 | Factor 5: Social Support | Factor 3: Physical Exertion or Strain 4 | Factor 6: Physical Agility | |
| All | 1.78 (0.76) | 2.5 (1.09) | 2.12 (0.91) | 1.43 (0.43) | 1.15 (0.43) | 1.11 (0.28) | 1.47 (0.75) |
| Life Stage | |||||||
| Unmarried Women (Ref.) | 1.99 (0.81) | 2.56 (1.06) | 2.28 (0.90) | 1.52 (0.45) | 1.04 (0.20) | 1.14 (0.34) | 1.20 (0.42) |
| Recently Married Women | 1.86 (0.77) ** | 2.49 (1.12) | 1.94 (0.97) ** | 1.49 (0.48) | 1.41 (0.65) ** | 1.13 (0.33) | 1.31 (0.58) * |
| Married Women | 1.78 (0.74) ** | 2.07 (1.03) ** | 2.21 (0.92) | 1.45 (0.41) * | 1.16 (0.43) ** | 1.10 (0.24) | 1.30 (0.55) * |
| Older Women | 1.50 (0.64) ** | 1.67 (0.92) ** | 2.01 (0.83) ** | 1.27 (0.29) ** | 1.03 (0.15) | 1.08 (0.18) * | 2.01 (1.00) ** |
| Ownership of Functional Latrine | |||||||
| Owns (Ref.) | 1.46 (0.61) | 1.8 (1.00) | 1.20 (0.41) | 1.27 (0.34) | 1.13 (0.40) | 1.08 (0.22) | 1.38 (0.72) |
| Does Not Own | 1.95 (0.78) ** | 2.4 (1.08) ** | 2.62 (0.70) ** | 1.52 (0.44) ** | 1.17 (0.45) | 1.14 (0.31) ** | 1.51 (0.77) * |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Caruso, B.A.; Clasen, T.; Yount, K.M.; Cooper, H.L.F.; Hadley, C.; Haardörfer, R. Assessing Women’s Negative Sanitation Experiences and Concerns: The Development of a Novel Sanitation Insecurity Measure. Int. J. Environ. Res. Public Health 2017, 14, 755. https://doi.org/10.3390/ijerph14070755
Caruso BA, Clasen T, Yount KM, Cooper HLF, Hadley C, Haardörfer R. Assessing Women’s Negative Sanitation Experiences and Concerns: The Development of a Novel Sanitation Insecurity Measure. International Journal of Environmental Research and Public Health. 2017; 14(7):755. https://doi.org/10.3390/ijerph14070755
Chicago/Turabian StyleCaruso, Bethany A., Thomas Clasen, Kathryn M. Yount, Hannah L. F. Cooper, Craig Hadley, and Regine Haardörfer. 2017. "Assessing Women’s Negative Sanitation Experiences and Concerns: The Development of a Novel Sanitation Insecurity Measure" International Journal of Environmental Research and Public Health 14, no. 7: 755. https://doi.org/10.3390/ijerph14070755
APA StyleCaruso, B. A., Clasen, T., Yount, K. M., Cooper, H. L. F., Hadley, C., & Haardörfer, R. (2017). Assessing Women’s Negative Sanitation Experiences and Concerns: The Development of a Novel Sanitation Insecurity Measure. International Journal of Environmental Research and Public Health, 14(7), 755. https://doi.org/10.3390/ijerph14070755




