Is Housing a Health Insult?
Abstract
:1. Introduction
1.1. Housing Bundles vs. Abstracted Components
- (1)
- Who in our population is more exposed to an accumulation of housing insults?
- (2)
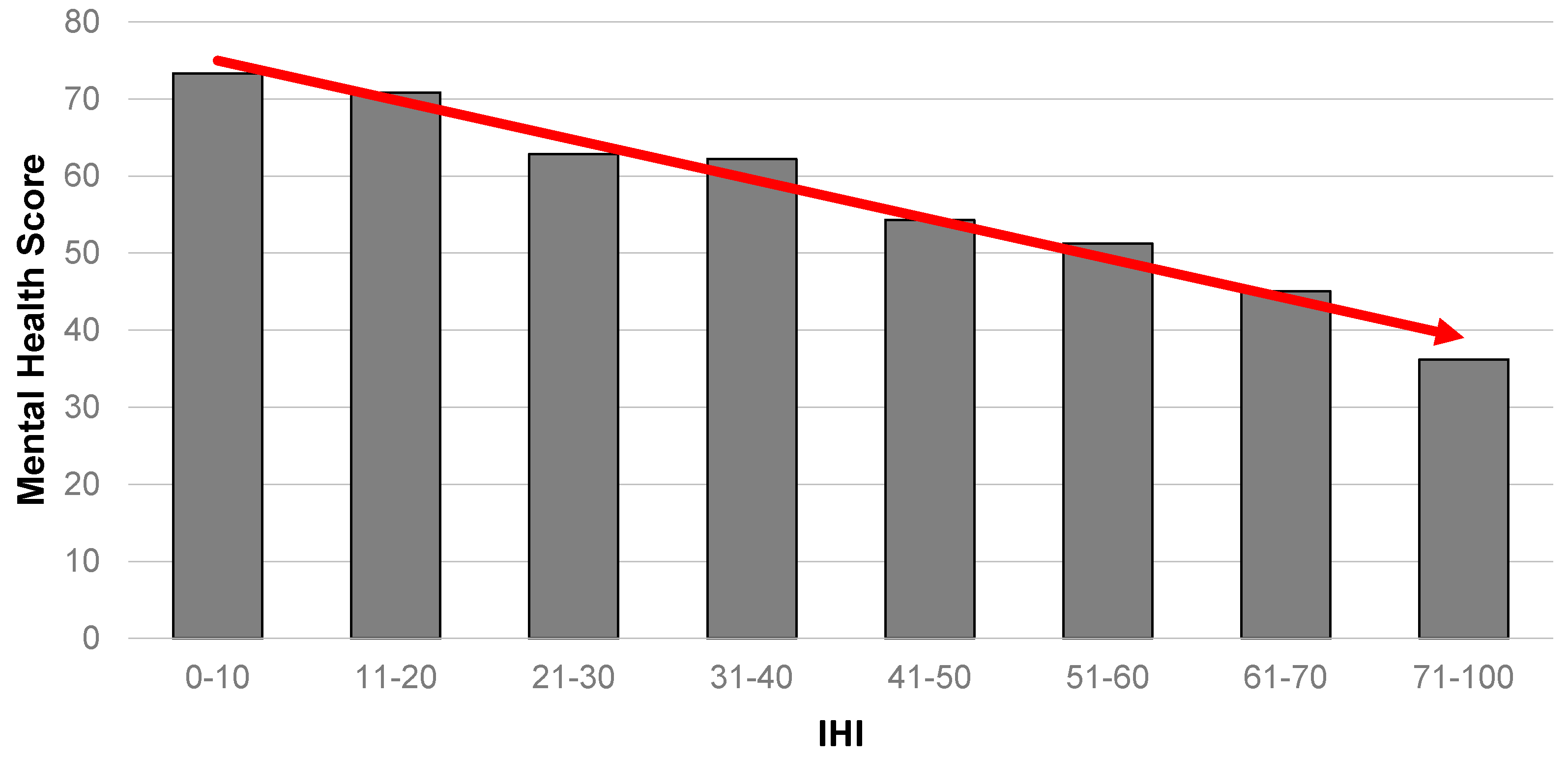
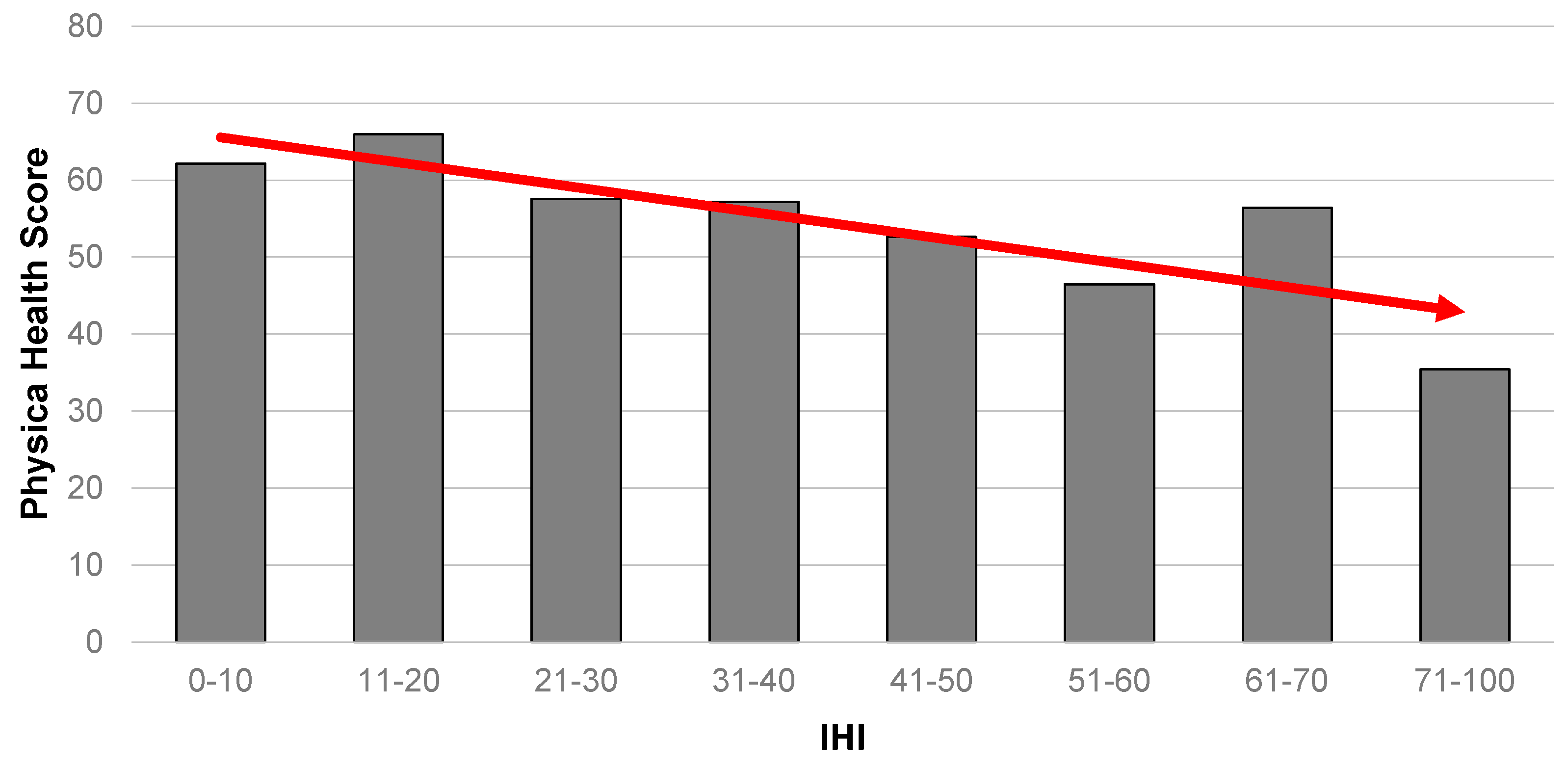
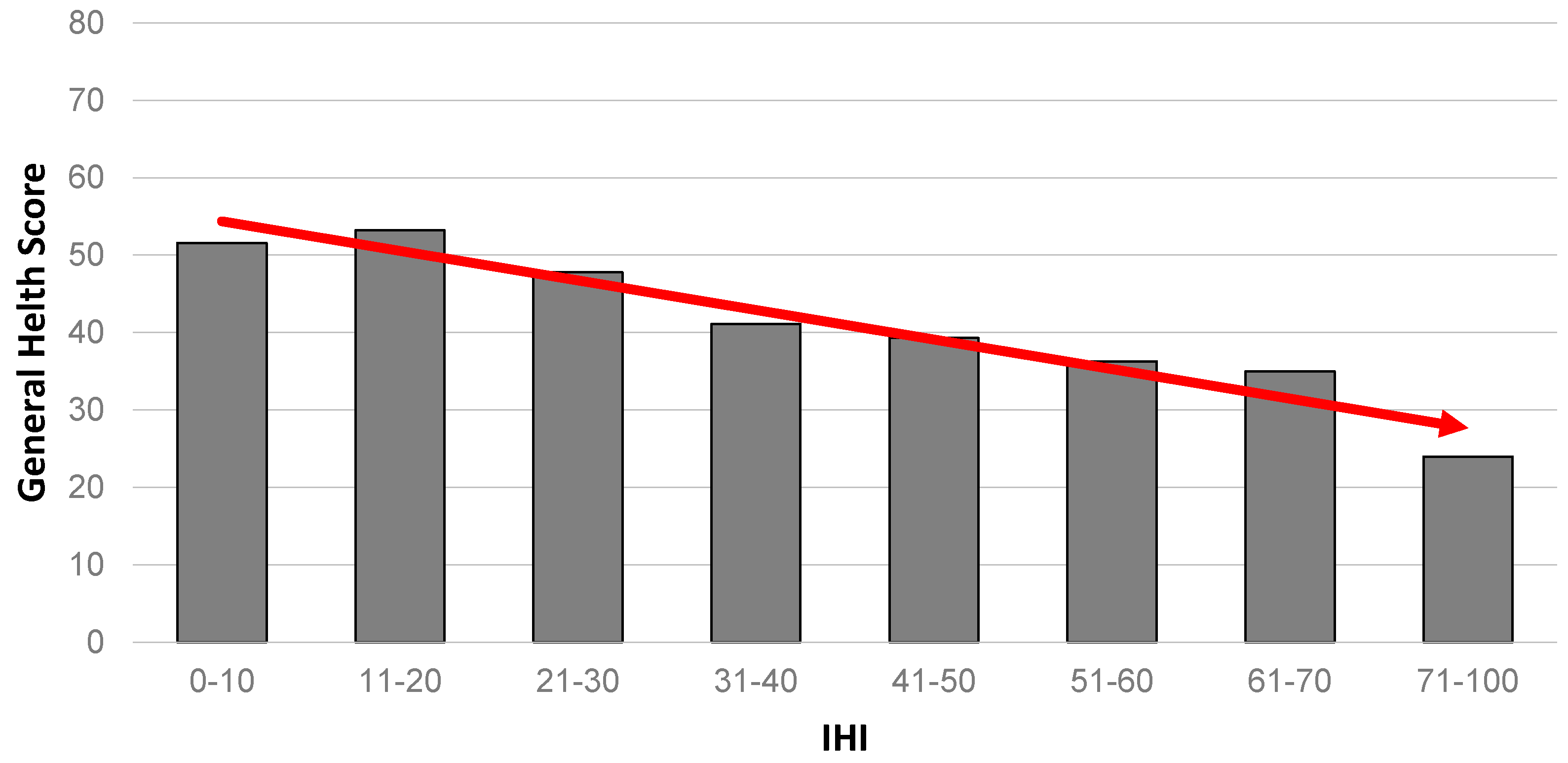
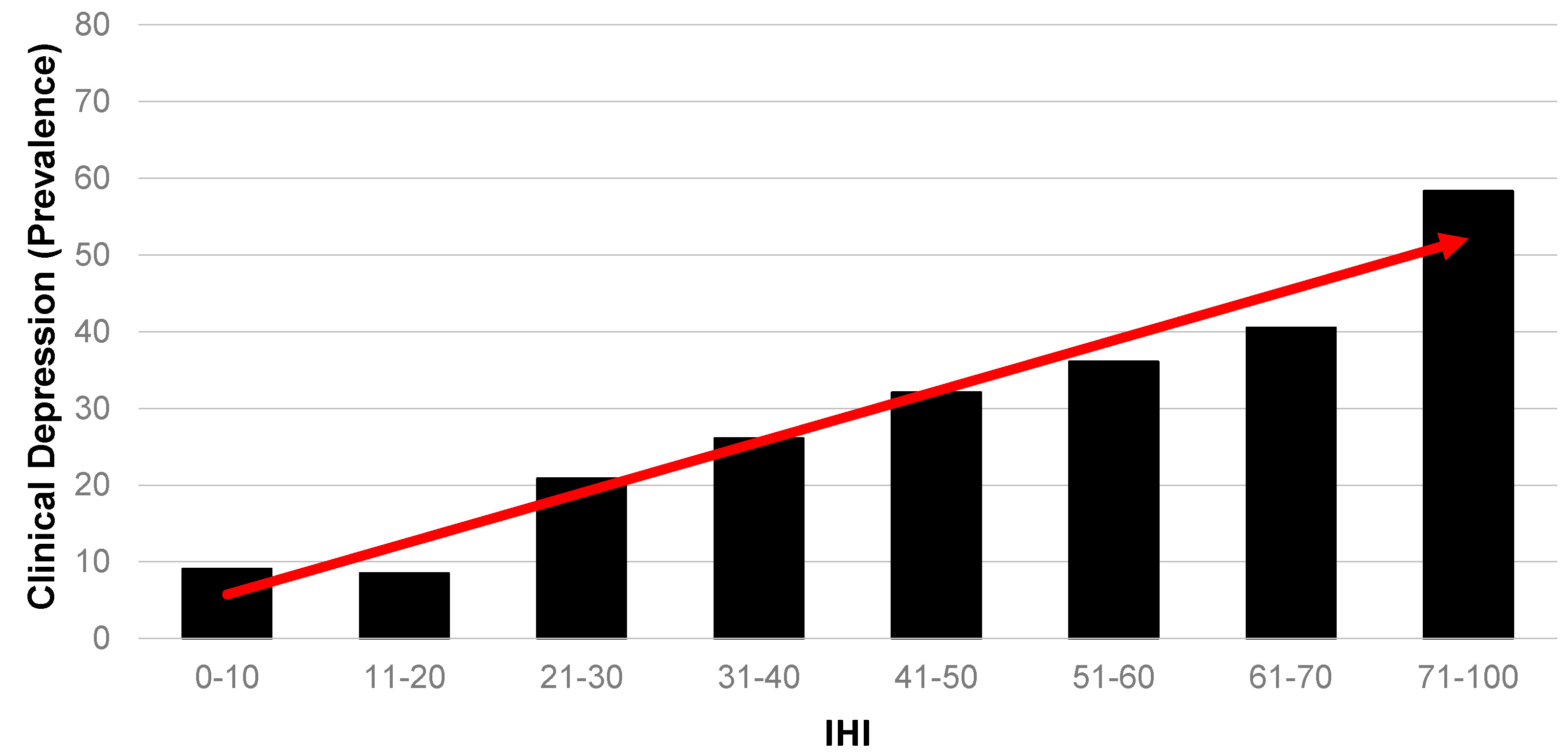
- Is there a corresponding gradient across a range of health measures (mental health, physical health, general health and clinical depression)?
1.2. A Bundle of Housing Insults?
2. Materials and Methods
3. Results
3.1. Descriptive
3.2. Bivariate Analysis
3.3. Multivariate Analysis of Outcomes
4. Discussion
4.1. Are Some Groups within Our Population More Exposed to Combined Housing Insults?
4.2. Is There a Corresponding Health Gradient (Across Mental Health, Physical Health, Self-Rated General Health and Clinical Depression Outcome Measures)?
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
Appendix A
| Mental | Physical | |
|---|---|---|
| Dummy Control Variables | ||
| Gender (ref. male) | 1.6224 | −1.0788 |
| Tenure (ref. home purchaser) | ||
| Own House | 3.5182 * | 0.7391 |
| Private Renter | 4.6015 *** | −0.9704 |
| Public Renter | −1.3851 | −1.5037 |
| Other | 2.8258 | 1.3821 |
| Education (ref. did not complete high school) | ||
| SACE/High school | −0.4048 | −1.2277 |
| Trade/Apprenticeship | 2.4696 | −1.5958 |
| Certificate | −1.6421 | 1.471 |
| University | −3.0851 | 1.5361 |
| Age group (ref. >76 years) | ||
| 17–25 | −7.8523 | 8.8588 ** |
| 26–45 | −4.9865 | 7.3293 *** |
| 46–55 | −4.2839 | 6.9478 ** |
| 56–65 | −1.1965 | 1.4824 |
| 66–75 | −3.1916 | 2.0587 |
| Labour force (ref. employed full-time) | ||
| Part-time/Casual | −3.7535 * | −0.6195 |
| Unemployed | −4.4467 | −1.5896 |
| Home | −5.9406 ** | 0.3693 |
| Retired | −0.2594 | −3.987 |
| Student | −9.0457 ** | −0.1002 |
| Unable | −5.1836 ** | −6.0085 *** |
| Marital status (ref. married/partnered) | ||
| Widowed | −3.1065 | −1.0714 |
| Divorced | −0.5377 | −1.6026 |
| Separated | −0.1712 | −0.8565 |
| Never Married | 0.4993 | 0.1727 |
| Weekly Income (ref. A$250–$499) | ||
| No Income | 2.6923 | 1.0862 |
| $1–249 | −1.7453 | −0.3451 |
| $500–799 | 0.5104 | 0.852 |
| $800–1199 | −0.8757 | 0.1218 |
| $1200–1699 | −2.6891 | 0.1918 |
| $1700–2499 | 1.3031 | −0.2972 |
| $2500–3499 | −1.2598 | −2.1897 |
| $3500 plus | −8.8644 | 11.1137 |
| Carer (not a carer) | −0.614 | −4.6530 *** |
| Disability (ref. no disability) | −3.7520 *** | −9.3320 *** |
| _cons | 60.7331 *** | 45.8851 *** |
| N | 471 | 471 |
References
- Snow, J. On the Mode of Communication of Cholera, 2nd ed.; John Churchill: London, UK, 1855. [Google Scholar]
- Dunn, J.R.; Hayes, M.V.; Hulchanski, J.D.; Hwang, S.W.; Potvin, L. Housing as a socio-economic determinant of health: Findings of a national needs, gaps and opportunities assessment. Can. J. Public Health/Rev. Can. Sante’e Publique 2006, 97, S11–S15. [Google Scholar] [CrossRef]
- Marmot, M.; Friel, S.; Bell, R.; Houweling, T.A.; Taylor, S. Commission on Social Determinants of Health. Closing the gap in a generation: Health equity through action on the social determinants of health. Lancet 2008, 372, 1661–1669. [Google Scholar] [CrossRef]
- Kain, J.F.; Quigley, J.M. Measuring the value of housing quality. J. Am. Stat. Assoc. 1970, 65, 532–548. [Google Scholar] [CrossRef]
- Clark, W.W.A.; Dieleman, F.M. Households and Housing: Choice and Outcomes in the Housing Market; Transaction Publishers: Piscataway, NJ, USA, 1996. [Google Scholar]
- Galster, G. On the nature of neighbourhood. Urban Stud. 2001, 38, 2111–2124. [Google Scholar] [CrossRef]
- Waters, A.M. Do Housing Conditions Impact on Health Inequalities between Australia’s Rich and Poor? Final Report; AHURI ANU Research Centre: Canberra, Australia, 2001. [Google Scholar]
- Baker, E.; Bentley, R.; Lester, L.; Beer, A. Housing affordability and residential mobility as drivers of locational inequality. Appl. Geogr. 2016, 72, 65–75. [Google Scholar] [CrossRef]
- Baker, E.; Lester, L. Multiple housing problems: A view through the housing niche lens. Cities 2017, 62, 146–151. [Google Scholar] [CrossRef]
- Bentley, R.; Baker, E.; Mason, K.; Subramanian, S.V.; Kavanagh, A.M. Association between housing affordability and mental health: A longitudinal analysis of a nationally representative household survey in Australia. Am. J. Epidemiol. 2011, 174, 753–760. [Google Scholar] [CrossRef] [PubMed]
- Taylor, M.P.; Pevalin, D.J.; Todd, J. The psychological costs of unsustainable housing commitments. Psychol. Med. 2007, 37, 1027–1036. [Google Scholar] [CrossRef] [PubMed]
- Bonnefoy, X.R.; Braubach, M.; Moissonnier, B.; Monolbaev, K.; Robbel, N. Housing and health in Europe: Preliminary results of a pan-European study. Am. J. Public Health 2003, 93, 1559–1563. [Google Scholar] [CrossRef] [PubMed]
- Evans, J.; Hyndman, S.; Stewart-Brown, S.; Smith, D.; Petersen, S. An epidemiological study of the relative importance of damp housing in relation to adult health. J. Epidemiol. Community Health 2000, 54, 677–686. [Google Scholar] [CrossRef] [PubMed]
- Webb, E.; Blane, D.; de Vries, R. Housing and respiratory health at older ages. J. Epidemiol. Community Health 2013, 67, 280–285. [Google Scholar] [CrossRef] [PubMed]
- Van Ham, M.; Manley, D. The effect of neighbourhood housing tenure mix on labour market outcomes: A longitudinal perspective. J. Econ. Geogr. 2010, 10, 257–282. [Google Scholar] [CrossRef]
- Marmot, M.; Wilkinson, R. (Eds.) Social Determinants of Health; Oxford University Press: Oxford, UK, 2005. [Google Scholar]
- Braveman, P.; Egerter, S.; Williams, D.R. The social determinants of health: Coming of age. Annu. Rev. Public Health 2011, 32, 381–398. [Google Scholar] [CrossRef] [PubMed]
- Gbran, D.; Whitehead, M. “Policies and Strategies to Promote Social 9” Equity in Health; Institute for Future Studies: Stockholm, Sweden, 1991. [Google Scholar]
- Allen, C. On the “Physiological Dope” Problematic in Housing and Illness Research: Towards a critical realism of home and health. Hous. Theory Soc. 2000, 17, 49–67. [Google Scholar] [CrossRef]
- Sayer, A. Realism and geography. In The Future of Geography; Johnston, R.J., Ed.; Methuen: London, UK, 1985; pp. 159–173. [Google Scholar]
- Saegert, S.; Evans, G.W. Poverty, housing niches, and health in the United States. J. Soc. Issues 2003, 59, 569–589. [Google Scholar] [CrossRef]
- Haas, S. Trajectories of functional health: The ‘long arm’ of childhood health and socioeconomic factors. Soc. Sci. Med. 2008, 66, 849–861. [Google Scholar] [CrossRef] [PubMed]
- Shaw, M. Housing and public health. Annu. Rev. Public Health 2004, 25, 397–418. [Google Scholar] [CrossRef] [PubMed]
- Baker, E.; Lester, L.H.; Bentley, R.; Beer, A. Poor housing quality: Prevalence and health effects. J. Prev. Int. Community 2016, 44, 219–232. [Google Scholar] [CrossRef] [PubMed]
- Gibson, M.; Petticrew, M.; Bambra, C.; Sowden, A.J.; Wright, K.E. Housing and health inequalities: A synthesis of systematic reviews of interventions aimed at different pathways linking housing and health. Health Place 2011, 17, 175–184. [Google Scholar] [CrossRef] [PubMed]
- Free, S.; Howden-Chapman, P.; Pierse, N.; Viggers, H. More effective home heating reduces school absences for children with asthma. J. Epidemiol. Community Health 2010, 64, 379–386. [Google Scholar] [CrossRef] [PubMed]
- Thomson, H.; Thomas, S.; Sellstrom, E.; Petticrew, M. The health impacts of housing improvement: A systematic review of intervention studies from 1887 to 2007. Am. J. Public Health 2009, 99, S681–S692. [Google Scholar] [CrossRef] [PubMed]
- Howden-Chapman, P.; Wilson, N. Housing and health. In Social Inequalities in Health: New Zealand, 1999; Howden-Chapman, P., Tobias, M., Eds.; Ministry of Health: Wellington, New Zealand, 2000; pp. 133–145. [Google Scholar]
- Clinch, P.J.; Healy, J.D. Housing standards and excess winter mortality. J. Epidemiol. Community Health 2000, 54, 719–720. [Google Scholar] [CrossRef] [PubMed]
- Mallett, S.; Bentley, R.; Baker, E.; Mason, K.; Keys, D.; Kolar, V.; Krnjacki, L. Precarious Housing and Health Inequalities: What Are the Links? VicHealth: Melbourne, Australia, 2011.
- Smith, S.J. Health status and the housing system. Soc. Sci. Med. 1990, 31, 753–762. [Google Scholar] [CrossRef]
- Hiscock, R.; Kearns, A.; MacIntyre, S.; Ellaway, A. Ontological security and psycho-social benefits from the home: Qualitative evidence on issues of tenure. Hous. Theory Soc. 2001, 18, 50–66. [Google Scholar] [CrossRef]
- Hulse, K.; Milligan, V. Secure occupancy: A new framework for analysing security in rental housing. Hous. Stud. 2014, 29, 638–656. [Google Scholar] [CrossRef]
- Ellaway, A.; Macdonald, L.; Kearns, A. Are housing tenure and car access still associated with health? A repeat cross-sectional study of UK adults over a 13-year period. BMJ Open 2016, 6, e012268. [Google Scholar] [CrossRef] [PubMed]
- Australian Bureau of Statistics (ABS). Housing Occupancy and Costs 2013–2014; Australian Bureau of Statistics: Canberra, Australia, 2015.
- Baker, E.; Bentley, R.; Mason, K. The mental health effects of housing tenure: Causal or compositional? Urban Stud. 2013, 50, 426–442. [Google Scholar] [CrossRef]
- Mason, K.E.; Baker, E.; Blakely, T.; Bentley, R.J. Housing affordability and mental health: Does the relationship differ for renters and home purchasers? Soc. Sci. Med. 2013, 94, 91–97. [Google Scholar] [CrossRef] [PubMed]
- Bentley, R.J.; Pevalin, D.; Baker, E.; Mason, K.; Reeves, A.; Beer, A. Housing affordability, tenure and mental health in Australia and the United Kingdom: A comparative panel analysis. Hous. Stud. 2016, 31, 208–222. [Google Scholar] [CrossRef]
- Rohe, W.M.; Burby, R.J. Fear of crime in public housing. Environ. Behav. 1988, 20, 700–720. [Google Scholar] [CrossRef]
- Ormandy, D.; Ezratty, V. Thermal discomfort and health: Protecting the susceptible from excess cold and excess heat in housing. Adv. Build. Energy Res. 2016, 10, 84–98. [Google Scholar] [CrossRef]
- Pollack, C.E.; Griffin, B.A.; Lynch, J. Housing affordability and health among homeowners and renters. Am. J. Prev. Med. 2010, 39, 515–521. [Google Scholar] [CrossRef] [PubMed]
- Lee, T.H.; Park, E.C.; Kim, W.; Kim, J.; Shin, J.; Kim, T.H. Depressive symptoms of house-poor persons: Korean panel data evidence. Int. J. Soc. Psychiatry 2016, 62, 569–577. [Google Scholar] [CrossRef] [PubMed]
- Downing, J. The health effects of the foreclosure crisis and unaffordable housing: A systematic review and explanation of evidence. Soc. Sci. Med. 2016, 162, 88–96. [Google Scholar] [CrossRef] [PubMed]
- Pevalin, D.J. Housing repossessions, evictions and common mental illness in the UK: Results from a household panel study. J. Epidemiol. Community Health 2009, 63, 949–951. [Google Scholar] [CrossRef] [PubMed]
- Hernández, D.; Phillips, D.; Siegel, E.L. Exploring the housing and household energy pathways to stress: A mixed methods study. Int. J. Environ. Res. Public Health 2016, 13, 916. [Google Scholar] [CrossRef] [PubMed]
- Thomson, H.; Petticrew, M.; Morrison, D. Housing interventions and health: A systematic review of intervention studies. Br. Med. J. 2001, 323, 187–190. [Google Scholar] [CrossRef]
- Krieger, J.; Higgins, D.L. Housing and health: Time again for public health action. Am. J. Public Health 2002, 92, 758–768. [Google Scholar] [CrossRef] [PubMed]
- Bonnefoy, X. Inadequate housing and health: An overview. Int. J. Environ. Pollut. 2007, 30, 411–429. [Google Scholar] [CrossRef]
- Pevalin, D.J.; Taylor, M.P.; Todd, J. The dynamics of unhealthy housing in the UK: A panel data analysis. Hous. Stud. 2008, 23, 679–695. [Google Scholar] [CrossRef]
- Evans, G.W.; Wells, N.M.; Chan, H.Y.E.; Saltzman, H. Housing quality and mental health. J. Consult. Clin. Psychol. 2000, 68, 526. [Google Scholar] [CrossRef] [PubMed]
- Curl, A.; Kearns, A.; Mason, P.; Egan, M.; Tannahill, C.; Ellaway, A. Physical and mental health outcomes following housing improvements: Evidence from the GoWell Study. J. Epidemiol. Community Health 2015, 69, 12–19. [Google Scholar] [CrossRef] [PubMed]
- Thomson, H.; Thomas, S.; Sellstrom, E.; Petticrew, M. Housing Improvements for Health and Associated Socio-Economic Outcomes; The Campbell Collaboration: Oslo, Norway, 2013. [Google Scholar]
- Jones-Rounds, M.L.; Evans, G.W.; Braubach, M. The interactive effects of housing and neighbourhood quality on psychological well-being. J. Epidemiol. Community Health 2014, 68, 171–175. [Google Scholar] [CrossRef] [PubMed]
- Beer, A.; Baker, E.; Raftery, P.; Wood, G. Housing policy, housing assistance and the wellbeing dividend: Developing an evidence base for post-GFC economies. Hous. Stud. 2011, 26, 1171–1192. [Google Scholar] [CrossRef]
- Golledge, R.G.; Stimson, R.J. Spatial Behaviour: A Geographic Perspective; Guilford Press: New York, NY, USA, 1997. [Google Scholar]
- Clark, W.A.V.; Onaka, J.L. Life cycle and housing adjustment as explanations of residential mobility. Urban Stud. 1983, 20, 47–57. [Google Scholar] [CrossRef]
- Rossi, P.H. Why Families Move, 2nd ed.; Sage Publications: Beverly Hills, CA, USA, 1980. [Google Scholar]
- Kintrea, K.; Clapham, D. Housing choice and search strategies within an administered housing system. Environ. Plan. A 1986, 18, 1281–1296. [Google Scholar] [CrossRef]
- Evans, G.W.; Li, D.; Wipple, S.S. Cumulative risk and child development. Psychol. Bull. 2013, 139, 1342. [Google Scholar] [CrossRef] [PubMed]
- Babbie, E. The Basics of Social Research; Thomas Wadsworth: Belmont, CA, USA, 2005. [Google Scholar]
- Baker, E.; Beer, A. Developing a workable model of housing need: Applying geographical concepts and techniques to a problem of public policy. Appl. Geogr. 2007, 27, 165–180. [Google Scholar] [CrossRef]
- Hinkin, T.R. A Review of Scale Development Practice in the Study of Organizations. J. Manag. 1995, 21, 967–989. [Google Scholar] [CrossRef]
- Billor, N.; Hadi, A.S.; Velleman, P.F. BACON: blocked adaptive computationally efficient outlier nominators. Comput. Stat. Data Anal. 2000, 34, 279–298. [Google Scholar] [CrossRef]
- Lu, M. Determinants of residential satisfaction: Ordered logit vs. regression models. Growth Chang. 1999, 30, 264–276. [Google Scholar] [CrossRef]
- Yates, J. Towards a reassessment of the private rental market. Hous. Stud. 1996, 11, 35–50. [Google Scholar] [CrossRef]
- Beer, A.; Faulkner, D.; Paris, C.; Clower, T. Housing Transitions through the Life Course: Aspirations, Needs and Policy; Policy Press: Bristol, UK, 2011; ISBN 978-1-84742-428-0. [Google Scholar]
- Keall, M.D.; Pierse, N.; Howden-Chapman, P.; Cunningham, C.; Cunningham, M.; Guria, J.; Baker, M.G. Home modifications to reduce injuries from falls in the Home Injury Prevention Intervention (HIPI) study: A cluster-randomised controlled trial. Lancet 2015, 385, 231–238. [Google Scholar] [CrossRef]
- Boelhouwer, P.; Priemus, H. Demise of the Dutch social housing tradition: Impact of budget cuts and political changes. J. Hous. Built Environ. 2014, 29, 221–235. [Google Scholar] [CrossRef]
- Oliver, J.R.; Pierse, N.; Stefanogiannis, N.; Jackson, C.; Baker, M.G. Acute rheumatic fever and exposure to poor housing conditions in New Zealand: A descriptive study. J. Paediatr. Child Health 2017, 53, 358–364. [Google Scholar] [CrossRef] [PubMed]
- Chantarat, S.; Barrett, C.B. Social network capital, economic mobility and poverty traps. J. Econ. Inequal. 2012, 10, 299–342. [Google Scholar] [CrossRef]
- Scanlon, K.; Fernández Arrigoitia, M.; Whitehead, C.M. Social Housing in Europe. Eur. Policy Anal. 2015, 17, 1–12. [Google Scholar]
- Flood, J.; Baker, E. Housing Implications of Economic, Social and Spatial Change; AHURI: Melbourne Australia, 2010. [Google Scholar]
- Australian Bureau of Statistics, Census Data 2001 and 2011. Available online: http://www.abs.gov.au/census (accessed on 12 May 2017).
- Commission on Social Determinants of Health. Closing the Gap in a Generation: Health Equity through Action on the Social Determinants of Health: Final Report of the Commission on Social Determinants of Health; Commission on Social Determinants of Health: Geneva, Switzerland, 2008. [Google Scholar]
- Smith, S.J.; Easterlow, D.; Munro, M.; Turner, K.M. Housing as health capital: How health trajectories and housing paths are linked. J. Soc. Issues 2003, 59, 501–525. [Google Scholar] [CrossRef]
- Bennett, J.; Howden-Chapman, P.; Chisholm, E.; Keall, M.; Baker, M.G. Towards an agreed quality standard for rental housing: Field testing of a New Zealand housing WOF tool. Aust. N. Z. J. Public Health 2016, 40, 405–411. [Google Scholar] [CrossRef] [PubMed]
- Australian Bureau of Statistics. Australian Housing Survey—Housing Characteristics, Costs and Conditions; Australian Bureau of Statistics: Canberra, Australia, 2000.
- Beer, A.; Bentley, R.; Baker, E.; Mason, K.; Mallett, S.; Kavanagh, A.; LaMontagne, T. Neoliberalism, economic restructuring and policy change: Precarious housing and precarious employment in Australia. Urban Stud. 2015, 53, 1542–1558. [Google Scholar] [CrossRef]
- Beck, U. Ulrich Beck: A Critical Introduction to Risk Society; Pluto Press: London, UK, 2004. [Google Scholar]
- Burns, L.S.; Grebler, L. The Housing of Nations: Analysis and Policy in a Comparative Framework; Wiley: New York, NY, USA, 1977. [Google Scholar]
| Affordability Domain |
|
| Security Domain |
|
| Quality of Dwelling Domain |
|
| Quality of Residential Area Domain |
|
| Access to Services and Support Domain |
|
| 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 | 11 | ||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 1 | Housing affordability | 1 | ||||||||||
| 2 | Financial problems | 0.09 | 1 | |||||||||
| 3 | Tenure security | 0.12 | 0.13 | 1 | ||||||||
| 4 | Residential safety | −0 | 0.32 | 0.00 | 1 | |||||||
| 5 | Dwelling adequacy | −0.1 | 0.38 | 0.31 | 0.50 | 1 | ||||||
| 6 | Physical dwelling problems | −0.1 | 0.49 | 0.20 | 0.44 | 0.66 | 1 | |||||
| 7 | Dwelling meets personal care needs | 0.17 | 0.04 | −0.1 | 0.12 | 0.17 | 0.07 | 1 | ||||
| 8 | Dwelling condition | 0.02 | 0.35 | 0.22 | 0.38 | 0.68 | 0.59 | 0.14 | 1 | |||
| 9 | Neighbourhood quality | 0.00 | 0.10 | −0 | 0.15 | 0.09 | 0.10 | 0.01 | 0.08 | 1 | ||
| 10 | Dwelling access to services | 0.15 | 0.15 | 0.02 | 0.19 | 0.23 | 0.15 | 0.44 | 0.11 | 0.03 | 1 | |
| 11 | Dwelling access to family support | 0.25 | 0.04 | 0.11 | 0.13 | 0.17 | 0.08 | 0.79 | 0.15 | 0.02 | 0.60 | 1 |
| Index of Housing Insults | Mean | n | 95% CI | |
|---|---|---|---|---|
| Population age | 36 | 638 | 35 | 38 |
| Age cohort | ||||
| 17–24 | 45 | 12 | 36 | 54 |
| 25–34 | 35 | 33 | 29 | 42 |
| 35–44 | 39 | 117 | 36 | 43 |
| 45–54 | 36 | 134 | 33 | 39 |
| 55–64 | 36 | 130 | 33 | 39 |
| 65+ | 33 | 200 | 31 | 35 |
| Long term disability/health condition | ||||
| Yes | 39 | 309 | 37 | 41 |
| No | 34 | 329 | 32 | 35 |
| Labour force/employment status | ||||
| Full-time employed | 29 | 91 | 26 | 32 |
| Part-time employed | 35 | 103 | 31 | 38 |
| Unemployed | 42 | 32 | 36 | 48 |
| Not in Labour Force (NLF) | 37 | 396 | 36 | 39 |
| Self-rated general health | ||||
| Poor | 43 | 72 | 39 | 47 |
| Fair | 40 | 192 | 38 | 43 |
| Good | 35 | 236 | 33 | 37 |
| Very good | 30 | 109 | 27 | 33 |
| Excellent | 25 | 25 | 20 | 29 |
| Marital status | ||||
| Married/de facto | 32 | 233 | 30 | 35 |
| Widowed | 33 | 78 | 30 | 37 |
| Divorced | 39 | 161 | 36 | 41 |
| Separated | 38 | 43 | 33 | 43 |
| Never married | 41 | 118 | 37 | 44 |
| Tenure | ||||
| Home owner/purchaser | 29 | 234 | 28 | 31 |
| Private rent (no assistance) | 41 | 45 | 37 | 45 |
| Rent assistance | 49 | 103 | 46 | 52 |
| Public renter | 36 | 252 | 34 | 38 |
| Gender | ||||
| Male | 35 | 233 | 33 | 38 |
| Female | 37 | 401 | 35 | 38 |
| Indigenous | ||||
| Yes | 34 | 23 | 28 | 41 |
| No | 36 | 590 | 35 | 38 |
| Carer | ||||
| Yes | 37 | 166 | 35 | 40 |
| No | 36 | 439 | 34 | 37 |
| In your household | 39 | 130 | 36 | 42 |
| Elsewhere | 35 | 52 | 30 | 40 |
| Clinical depression | ||||
| No | 33 | 474 | 32 | 35 |
| Yes | 44 | 164 | 41 | 47 |
| Mental Health | Physical Health | |
|---|---|---|
| IHI | −0.2457 *** | −0.0314 |
| General Health OR | Diagnosed Clinical Depression OR | |
|---|---|---|
| IHI | 0.9651 *** | 1.0323 *** |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Baker, E.; Beer, A.; Lester, L.; Pevalin, D.; Whitehead, C.; Bentley, R. Is Housing a Health Insult? Int. J. Environ. Res. Public Health 2017, 14, 567. https://doi.org/10.3390/ijerph14060567
Baker E, Beer A, Lester L, Pevalin D, Whitehead C, Bentley R. Is Housing a Health Insult? International Journal of Environmental Research and Public Health. 2017; 14(6):567. https://doi.org/10.3390/ijerph14060567
Chicago/Turabian StyleBaker, Emma, Andrew Beer, Laurence Lester, David Pevalin, Christine Whitehead, and Rebecca Bentley. 2017. "Is Housing a Health Insult?" International Journal of Environmental Research and Public Health 14, no. 6: 567. https://doi.org/10.3390/ijerph14060567
APA StyleBaker, E., Beer, A., Lester, L., Pevalin, D., Whitehead, C., & Bentley, R. (2017). Is Housing a Health Insult? International Journal of Environmental Research and Public Health, 14(6), 567. https://doi.org/10.3390/ijerph14060567





