HIV Education and Welfare Services in Primary Care: An Empirical Model of Integration in Brazil’s Unified Health System
Abstract
:1. Introduction
1.1. Service Integration in Brazil’s Family Health Strategy
1.2. Factors That Influence Integration
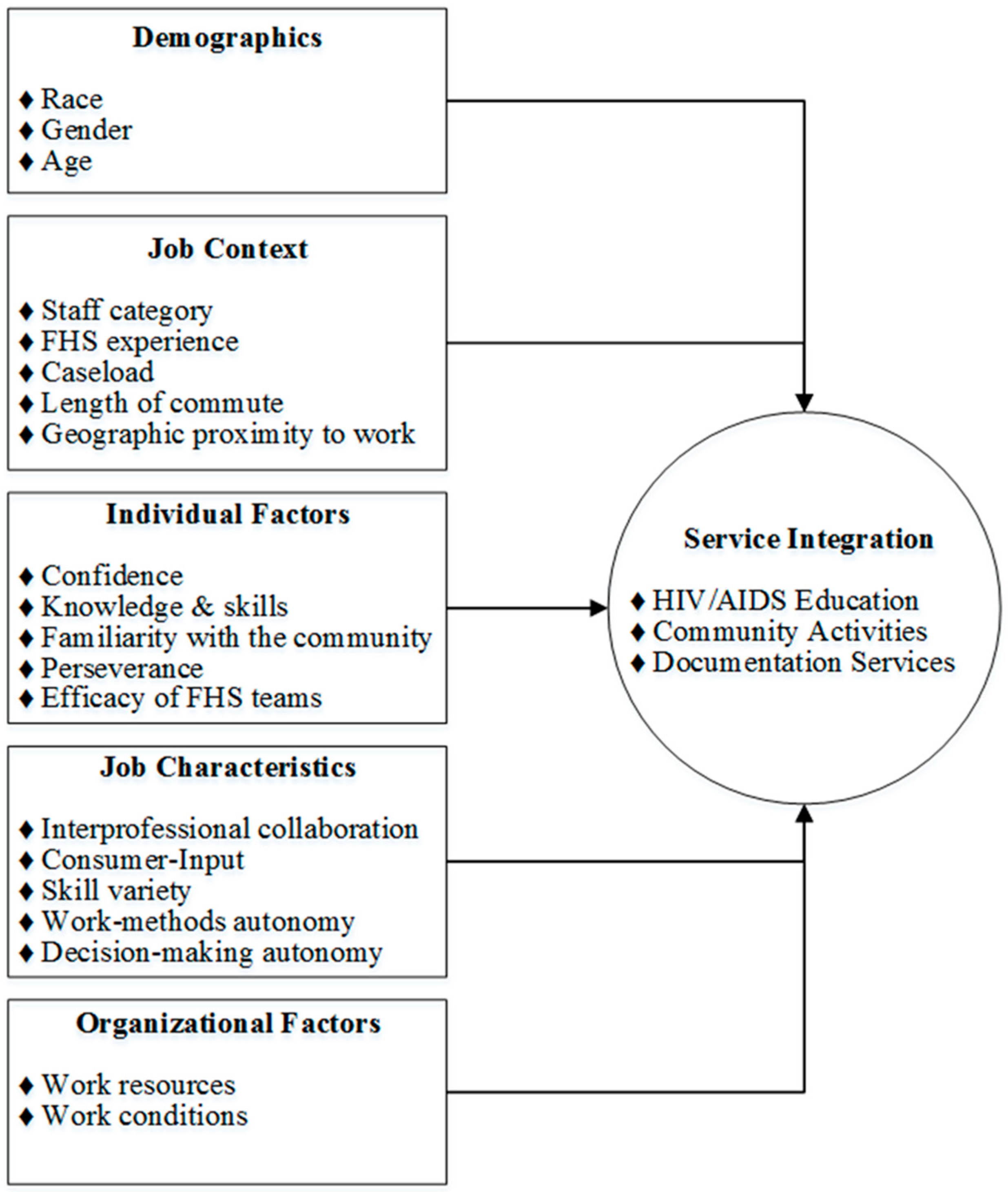
1.3. Theoretical Framework
2. Materials and Methods
2.1. Sampling and Recruitment
2.2. Data Collection
2.3. Multidimensional Survey
2.4. Measures
2.5. Data Analysis
3. Results
3.1. Sample Characteristics
3.2. Predicting Service Integration
4. Discussion
Implications for Policy and Practice
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Singh, G.K.; Azuine, R.E.; Siahpush, M. Global inequalities in cervical cancer incidence and mortality are linked to deprivation, low socioeconomic status, and human development. Int. J. MCH AIDS (IJMA) 2015, 1, 17–30. [Google Scholar] [CrossRef]
- Arreola, S.; Santos, G.-M.; Beck, J.; Sundararaj, M.; Wilson, P.A.; Hebert, P.; Makofane, K.; Do, T.D.; Ayala, G. Sexual stigma, criminalization, investment, and access to HIV services among men who have sex with men worldwide. AIDS Behav. 2015, 19, 227–234. [Google Scholar] [CrossRef] [PubMed]
- Thornton, R.L.; Glover, C.M.; Cené, C.W.; Glik, D.C.; Henderson, J.A.; Williams, D.R. Evaluating strategies for reducing health disparities by addressing the social determinants of health. Health Aff. 2016, 35, 1416–1423. [Google Scholar] [CrossRef] [PubMed]
- Joint United Nations Programme on HIV/Acquired Immune Deficiency Syndrome (UNAIDS). Prevention Gap Report. 2016. Available online: http://www.unaids.org/sites/default/files/media_asset/2016-prevention-gap-report_en.pdf (accessed on 18 December 2016).
- Dean, H.D.; Fenton, K.A. Addressing social determinants of health in the prevention and control of HIV/AIDS, viral hepatitis, sexually transmitted infections, and tuberculosis. Public Health Rep. 2010, 125, 1–5. [Google Scholar] [CrossRef] [PubMed]
- Herman, A.A. Community health workers and integrated primary health care teams in the 21st century. J. Ambul. Care Manag. 2011, 34, 354–361. [Google Scholar] [CrossRef] [PubMed]
- Baral, S.D.; Friedman, M.R.; Geibel, S.; Rebe, K.; Bozhinov, B.; Diouf, D.; Sabin, K.; Holland, C.E.; Chan, R.; Cáceres, C.F. Male sex workers: Practices, contexts, and vulnerabilities for HIV acquisition and transmission. Lancet 2015, 385, 260–273. [Google Scholar] [CrossRef]
- Naidoo, P.; Chirinda, W.; Mchunu, G.; Swartz, S.; Anderson, J. Social and structural factors associated with vulnerability to HIV infection among young adults in South Africa. Psychol. Health Med. 2015, 20, 369–379. [Google Scholar] [CrossRef] [PubMed]
- Valentijn, P.; Boesveld, I.C.; van der Klauw, D.M.; Ruwaard, D.; Struijs, J.N.; Molema, J.J.W.; Bruijnzeels, M.A.; Vrijhoef, H.J.M. Towards a taxonomy for integrated care: A mixed-methods study. Int. J. Integr. Care 2015, 15. [Google Scholar] [CrossRef]
- Winters, S.; Magalhaes, L.; Kinsella, E.A.; Kothari, A. Cross-sector service provision in health and social care: An umbrella review. Int. J. Integr. Care 2016, 16. [Google Scholar] [CrossRef]
- Shigayeva, A.; Atun, R.; McKee, M.; Coker, R. Health systems, communicable diseases and integration. Health Policy Plan. 2010, 25, 4–20. [Google Scholar] [CrossRef] [PubMed]
- Spector, A.Y.; Pinto, R.M.; Rahman, R.; da Fonseca, A. Implementation of Brazil’s “Family Health Strategy”: Factors associated with community health workers’, nurses’, and physicians’ delivery of drug use services. Int. J. Drug Policy 2015, 26, 509–515. [Google Scholar] [CrossRef] [PubMed]
- Ghesquiere, A.R.; Pinto, R.M.; Rahman, R.; Spector, A.Y. Factors Associated with Providers’ Perceptions of Mental Health Care in Santa Luzia’s Family Health Strategy, Brazil. Int. J. Environ. Res. Public Health 2015, 13, 33. [Google Scholar] [CrossRef] [PubMed]
- Unützer, J.; Katon, W.J.; Fan, M.-Y.; Schoenbaum, M.C.; Lin, E.H.B.; Della Penna, R.D.; Powers, D. Long-term cost effects of collaborative care for late-life depression. Am. J. Manag. Care 2008, 14, 95–100. [Google Scholar] [PubMed]
- Ockene, J.K.; Marion, L.N.; Loveland-Cherry, C.J. Integrating evidence-based clinical and community strategies to improve health. Am. J. Prev. Med. 2007, 32, 244–252. [Google Scholar] [CrossRef] [PubMed]
- Unützer, J.; Tang, L.; Oishi, S.; Katon, W.; Williams, J.W., Jr.; Hunkeler, E.; Hendrie, H.; Lin, E.H.B.; Levine, S.; Grypma, L.; et al. Reducing suicidal ideation in depressed older primary care patients. J. Am. Geriatr. Soc. 2006, 54, 1550–1556. [Google Scholar] [CrossRef] [PubMed]
- Brown, L.; Tucker, C.; Domokos, T. Evaluating the impact of integrated health and social care teams on older people living in the community. Health Soc. Care Commun. 2003, 11, 85–94. [Google Scholar] [CrossRef]
- Pinto, R.M.; Wall, M.; Yu, G.; Penido, C.; Schmidt, C. Primary care and public health services integration in Brazil’s Unified Health System. Am. J. Public Health 2012, 102, 69–76. [Google Scholar] [CrossRef] [PubMed]
- Paim, J.; Travassos, C.; Almeida, C.; Bahia, L.; Macinko, J. The Brazilian health system: History, advances, and challenges. Lancet 2011, 377, 1778–1797. [Google Scholar] [CrossRef]
- WHO, Global Health Workforce Alliance. Global Experience of Community Health Workers for Delivery of Health Related Millennium Development Goals: A Systematic Review, Country Case Studies, and Recommendations for Integration Into national Health Systems; WHO, Global Health Workforce Alliance: Geneva, Switzerland, 2010. [Google Scholar]
- Brazil Ministry of Health. Recommendations on Antiretroviral Therapy in HIV-Infected Adults and Adolescent; Department of STD, AIDS and Viral Hepatitis: Brasília, DF, Brazil, 2006. Available online: http://www.aids.gov.br/ (accessed on 13 December 2013).
- Silva, T.L.; Dias, E.C.; Ribeiro, E.C.D.O. Knowledge and practices of Community Health Agents in workers’ healthcare. Interface-Comun. Saúde, Educ. 2011, 15, 859–870. [Google Scholar] [CrossRef]
- Howarth, C.; Campbell, C.; Cornish, F.; Franks, B.; Garcia-Lorenzo, L.; Gillespie, A.; Gleibs, I.; Gonvales-Portelinha, I.; Jovchelovitch, S.; Lahlou, S.; et al. Insights from Societal Psychology: The contextual politics of change. J. Soc. Polit. Psychol. 2013, 1, 364–384. [Google Scholar] [CrossRef] [Green Version]
- Gilkey, M.; Garcia, C.C.; Rush, C. Professionalization and the experience-based expert: Strengthening partnerships between health educators and community health workers. Health Promot. Pract. 2011, 12, 178–182. [Google Scholar] [CrossRef] [PubMed]
- Pinto, R.M.; da Silva, S.B.; Soriano, R. Community Health Workers in Brazil’s Unified Health System: A framework of their praxis and contributions to patient health behaviors. Soc. Sci. Med. 2012, 74, 940–947. [Google Scholar] [CrossRef] [PubMed]
- Zanchetta, M.S.; Pinto, R.M.; Galhego-Garcia, W.; da Cunha, Z.; Cordeiro, H.A.; Fagundes-Filho, F.E.; Pinho, M.A.L.; Voet, S.M.V.; Talbot, Y.; Caldas, R.S.; et al. Brazilian Community Health Agents and qualitative primary healthcare information. Prim. Health Care Res. Dev. 2014, 16, 235–245. [Google Scholar] [CrossRef] [PubMed]
- Brownstein, J.N.; Hirsch, G.R.; Rosenthal, E.L.; Rush, C.H. Community Health Workers “101” for Primary Care Providers and Other Stakeholders in Health Care Systems. J. Ambul. Care Manag. 2011, 34, 210–220. [Google Scholar] [CrossRef] [PubMed]
- Ammentorp, J.; Sabroe, S.; Kofoed, P.E.; Mainz, J. The effect of training in communication skills on medical doctors’ and nurses’ self-efficacy: A randomized controlled trial. Patient Educ. Couns. 2007, 66, 270–277. [Google Scholar] [CrossRef] [PubMed]
- Ivbijaro, G.; Patel, V.; Chisholm, D.; Goldberg, D.; Khoja, T.A.; Edwards, T.M.; Enum, Y.; Kolkiewic, L.A. Informing mental health policies and services in the EMR: Cost-effective deployment of human resources to deliver integrated community-based care. East Mediterr. Health J. 2015, 21, 486–492. [Google Scholar] [PubMed]
- Cotton, P.; Hart, P.M. Occupational wellbeing and performance: A review of organisational health research. Aust. Psychol. 2003, 38, 118–127. [Google Scholar] [CrossRef]
- Frigo, J.; Costa, E.R.; Kolhs, M.; Busnello, G. Tasks performed by professional nurses in family health strategy. J. Nurs. UFPE 2013, 7, 5421–5426. [Google Scholar]
- Magalhães, K.A.; Cotta, R.M.M.; de Castro Pereira Martins, T.; Gomes, A.P.; Siqueira-Batista, R. Habitation as a Social Determinant of Health: Perceptions and conditions of families registered under the “Bolsa Família” Program. Saúde Soc. 2013, 22, 57–72. [Google Scholar]
- Falavigna, A.; Canabarro, C.T.; Medeiros, G.S. Health System and Medical Education in Brazil: History, Principles, and Organization. World Neurosurg. 2013, 80, 723–727. [Google Scholar] [CrossRef] [PubMed]
- Teles, M.A.; Barbosa, M.R.; Vargas, A.M.D.; Gomes, V.E.; e Ferreira, E.F.; de Barros Lima Martins, A.M.E.; Ferreira, R.C. Psychosocial work conditions and quality of life among primary health care employees: A cross sectional study. Health Q. Life Outcomes 2014, 12, 72. [Google Scholar] [CrossRef] [PubMed]
- Morgeson, F.P.; Humphrey, S.E. Job and team design. In Research in Personnel and Human Resources Management; Morgeson, F.P., Ed.; Emerald Group Publishing Limited: Bingley, UK, 2008; pp. 39–92. [Google Scholar]
- Obi-Nwosu, H.; Joe-Akunne Chiamaka, O. Job Characteristics as Predictors of Organizational Commitment among Private Sector Workers in Anambra State, Nigeria. Int. J. Asian Soc. Sci. 2013, 3, 482–491. [Google Scholar]
- Brazil Ministry of Health—Secretariat of Health Care. National Primary Health Care Policy. 2012. Available online: http://189.28.128.100/dab/docs/publicacoes/geral/pnab.pdf (accessed on 20 December 2016).
- Barry, M.J.; Edgman-Levitan, S. Shared decision making—The pinnacle of patient-centered care. N. Engl. J. Med. 2012, 366, 780–781. [Google Scholar] [CrossRef] [PubMed]
- Coelho, F.; Augusto, M. Job characteristics and the creativity of frontline service employees. J. Serv. Res. 2010, 13, 426–438. [Google Scholar] [CrossRef]
- Oldham, G.R.; Hackman, J.R. Not what it was and not what it will be: The future of job design research. J. Organ. Behav. 2010, 31, 463–479. [Google Scholar] [CrossRef] [Green Version]
- Hackman, J.R.; Oldham, G.R. Development of the job diagnostic survey. J. Appl. Psychol. 1975, 60, 159–170. [Google Scholar] [CrossRef]
- Brown, L.D.; Covey, J.G. Development organizations and organization development: Towards an expanded paradigm for organization development. In Research in Organizational Change and Development; Woodman, R.W., Pasmore, W.A., Eds.; JAI Press: Greenwich, CT, USA, 1987. [Google Scholar]
- Burns, T.E.; Stalker, G.M. The Management of Innovation; Tavistock Publisher: London, UK, 1961. [Google Scholar]
- Lawrence, P.R.; Lorsch, J.W. Organization and Environment: Managing Differentiation and Integration; Division of Research, Graduate School of Business Administration, Harvard University Boston: Boston, MA, USA, 1967. [Google Scholar]
- Pinto, R.M.; Spector, A.Y.; Witte, S.S.; Gilbert, L. Systematizing planning and formative phases of HIV prevention research: Case studies from Brazil, Mongolia, and Kazakhstan. Glob. Soc. Welf. 2014, 1, 137–144. [Google Scholar] [CrossRef] [PubMed]
- Pinto, R.M.; Bulhões da Silva, S.; Penido, C.; Spector, A.Y. International participatory research framework: Triangulating procedures to build health research capacity in Brazil. Health Promot. Int. 2012, 27, 435–444. [Google Scholar] [CrossRef] [PubMed]
- DATSTAT Illume. DATSTAT (Data Management Software); DATSTAT Illume: Seattle, WA, USA, 1997. [Google Scholar]
- Brislin, R.W. Back-translation for cross-cultural research. J. Cross-Cult. Psychol. 1970, 1, 185–216. [Google Scholar] [CrossRef]
- Telles, E.E. Race in Another America: The Significance of Skin Color in Brazil; Princeton University Press: Princeton, NJ, USA, 2004. [Google Scholar]
- Cohen, J.; Cohen, P. Applied multiple Regression/Correlation Analysis for the Behavioral Sciences, 2nd ed.; Lawrence Erlbaum: New Jersey, NJ, USA, 1983. [Google Scholar]
- Ho, R. Handbook of Univariate and Multivariate Data Analysis with IBM SPSS, 2nd ed.; CRC Press: Boca Raton, FL, USA, 2013. [Google Scholar]
- Kelloway, E.K. Using Mplus for Structural Equation Modeling: A Researcher’s Guide, 2nd ed.; Sage Publications: London, UK, 2014. [Google Scholar]
- Rocha, N.H.N.; Barletto, M.; Bevilacqua, P.D. Identity of community health agents: Composing emerging rationalities. Interface-Comun. Saúde Educ. 2013, 17, 847–857. [Google Scholar] [CrossRef]
- Mwai, G.W.; Mburu, G.; Torpey, K.; Frost, P.; Ford, N.; Seeley, J. Role and outcomes of community health workers in HIV care in sub-Saharan Africa: A systematic review. J. Int. AIDS Soc. 2013, 16. [Google Scholar] [CrossRef] [PubMed]
- Lin, B.Y.; Lin, Y.K.; Lin, C.C.; Lin, T.T. Job autonomy, its predispositions and its relation to work outcomes in community health centers in Taiwan. Health Promot. Int. 2013, 28, 166–177. [Google Scholar] [CrossRef] [PubMed]
- Dos Santos Pedrosa, J.I.; Teles, J.B.M. Agreements and disagreements in the Family Health Care Program team. Rev. Saúde Pública 2001, 35, 303–311. [Google Scholar]
- Silveira, D.S.; Facchini, L.A.; Vinholes Siqueira, F.; Piccini, R.X.; Tomasi, E.; Thumé, E.; Manjourany Silva, S.; Dilélio, A.S.; dos Santos Maia, M.F. Management of work, education, information, and communication in primary healthcare in cities in Southern and Northeastern Brazil. Cadernos Saúde Pública 2010, 26, 1714–1726. [Google Scholar] [CrossRef]
| Predictors | Definition | Item(s) and Scale |
|---|---|---|
| Individual Factors | ||
| Knowledge and skills | 10-item composite: abilities to ask client/patients questions to provoke discussions about health, disease prevention, side effects of medications, and available resources (Cronbach α = 0.757) | 5-point Likert scale (1 = strongly disagree to 5 = strongly agree)
|
| Confidence | 3-item composite: appraisals of ability to provide client/patients with adequate services (Cronbach α = 0.521) | 5-point Likert scale (1 = strongly disagree to 5 = strongly agree)
|
| Perseverance | Single item: extent of practitioner commitment to providing the best services | 5-point Likert scale (1 = strongly disagree to 5 = strongly agree)
|
| Efficacy of FHS teams | Single item: practitioner perception of team efficacy | 5-point Likert scale (1 = strongly disagree to 5 = strongly agree)
|
| Familiarity with the community | Single item: extent to which practitioner knew the community | Dichotomous (yes or no)
|
| Job Characteristics | ||
| Inter-professional collaboration | 5-item composite: extent to collaboration between different professions (Cronbach α = 0.640) | 5-point Likert scale (1 = strongly disagree to 5 = strongly agree)
|
| Consumer-Input | 4-item composite: extent practitioner value/use client/patient input (Cronbach α = 0.627) | 5-point Likert scale (1 = strongly disagree to 5 = strongly agree)
|
| Skill variety | 3-item composite: extent of variety in skill sets (Cronbach α = 0.620) | 5-point Likert scale (1 = strongly disagree to 5 = strongly agree)
|
| Work autonomy | Single item: perception of work-related autonomy | Dichotomous: (0 = Disagree; 1 = Agree)
|
| Decision-making autonomy | Single item: perception of work-decision-making | Dichotomous: (0 = Disagree; 1 = Agree)
|
| Job context | ||
| Caseload | Single item: number of patients served | Continuous
|
| FHS Experience | Single item: years in the job | Continuous
|
| Geographic proximity to work | Single item: perception of closeness to community | Dichotomous
|
| Length of commute | Single item: minutes it takes to arrive to work from home | Continuous
|
| Work Environment | ||
| Work conditions | Single item: perception of quality of work conditions | Dichotomous (yes or no)
|
| Work resources | Single item: perception of quality of work resources |
|
| Demographic Variables | CHAs | Nurses | Physicians | Total Sample | p-Value |
|---|---|---|---|---|---|
| n = 169 (%) | n = 62 (%) | n = 31 (%) | n = 262 (%) | ||
| Race | 0.002 a | ||||
| Black | 40 (24) | 13 (21) | 1 (3) | 54 (21) | |
| White | 42 (25.1) | 22 (35) | 18 (58) | 82 (31) | |
| Pardo | 85 (50.9) | 27 (44) | 11 (35) | 123 (47) | |
| Gender | <0.001 a | ||||
| Male | 28 (17) | 4 (6) | 16 (52) | 48 (18) | |
| Female | 141 (83) | 58 (94) | 15 (48) | 214 (82) | |
| Age | 0.138 | ||||
| 20–30 years | 76 (45) | 27 (44) | 12 (39) | 114 (44) | |
| 30–40 years | 56 (33) | 15 (24) | 10 (32) | 81 (31) | |
| 41–50 years | 27 (16) | 12 (19) | 3 (10) | 42 (16) | |
| 51–70 years | 7 (4) | 7 (11) | 5 (16) | 19 (7) | |
| FHS experience | 0.008 a | ||||
| ≤1 year | 27 (16) | 8 (13) | 8 (26) | 43 (16) | |
| 1–5 years | 123 (73) | 37 (60) | 15 (48) | 175 (67) | |
| 6–15 years | 19 (11) | 17 (27) | 8 (26) | 44 (17) | |
| Caseload per Month | <0.001 a | ||||
| ≤250 | 131 (77) | 2 (3) | - | 135 (51) | |
| 251–500 | 35 (21) | 1 (2) | 2 (6) | 38 (14) | |
| >500 | 3 (2) | 59 (95) | 29 (94) | 91 (35) | |
| Length of Commute | <0.001 a | ||||
| 0–10 min | 114 (67) | 12 (19) | 3 (10) | 129 (50) | |
| 11–30 min | 47 (28) | 30 (48) | 11 (35) | 88 (34) | |
| >30 min | 6 (4) | 20 (32) | 17 (55) | 43 (16) | |
| Geographic Proximity to work | <0.001 a | ||||
| Yes | 153 (91) | 28 (45) | 5 (16) | 186 (71) | |
| No | 15 (9) | 34 (55) | 26 (84) | 75 (29) |
| Service Integration | ||
|---|---|---|
| B (SE) | p-Value | |
| Demographic | ||
| CHAs vs. physicians | 0.373 | 0.118 |
| Nurses vs. physicians | 0.043 | 0.814 |
| Race: black vs. pardo | 0.012 | 0.92 |
| Race: white vs. pardo | −0.182 | 0.125 |
| Male vs. Female | −0.19 | 0.128 |
| Age | 0.15 | 0.236 |
| Job Context | ||
| FHS experience | 0.258 b | 0.06 |
| Caseload | 0.05 | 0.736 |
| Commute 0–10 min vs. >30 min | −0.122 | 0.595 |
| Commute 11–30 min vs. >30 min | 0.219 | 0.237 |
| Geographic proximity to work | −0.085 | 0.629 |
| Individual factors | ||
| Confidence | 0.322 a | 0.02 |
| Knowledge & skills | 0.448 a | 0.006 |
| Familarity with community | 0.153 | 0.177 |
| Perseverance | 0.237 b | 0.036 |
| Efficacy of FHS teams | −0.073 | 0.536 |
| Job Characteristics | ||
| Interprofessional collaboration | −0.209 | 0.121 |
| Consumer-Input | 0.033 | 0.819 |
| Skill variety | 0.355 a | 0.017 |
| Work-methods autonomy | −0.222 b | 0.097 |
| Decision-making autonomy | −0.237 b | 0.075 |
| Organizational factors | ||
| Work resources | –0.063 | 0.677 |
| Work conditions | 0.044 | 0.756 |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license ( http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Rahman, R.; Pinto, R.M.; Wall, M.M. HIV Education and Welfare Services in Primary Care: An Empirical Model of Integration in Brazil’s Unified Health System. Int. J. Environ. Res. Public Health 2017, 14, 294. https://doi.org/10.3390/ijerph14030294
Rahman R, Pinto RM, Wall MM. HIV Education and Welfare Services in Primary Care: An Empirical Model of Integration in Brazil’s Unified Health System. International Journal of Environmental Research and Public Health. 2017; 14(3):294. https://doi.org/10.3390/ijerph14030294
Chicago/Turabian StyleRahman, Rahbel, Rogério M. Pinto, and Melanie M. Wall. 2017. "HIV Education and Welfare Services in Primary Care: An Empirical Model of Integration in Brazil’s Unified Health System" International Journal of Environmental Research and Public Health 14, no. 3: 294. https://doi.org/10.3390/ijerph14030294
APA StyleRahman, R., Pinto, R. M., & Wall, M. M. (2017). HIV Education and Welfare Services in Primary Care: An Empirical Model of Integration in Brazil’s Unified Health System. International Journal of Environmental Research and Public Health, 14(3), 294. https://doi.org/10.3390/ijerph14030294





