Monitoring and Prognosis System Based on the ICF for People with Traumatic Brain Injury
Abstract
:1. Introduction
- They are used to collect some information about the state of a person or an activity;
- They are validated by a health care institution;
- They are stored in the clinical record [6];
- They refer to specific problems or people;
- Their selection depends on the cultural aspects, organizations and countries.
2. Experimental Section
2.1. Scenario
- Institut Guttmann social scale (ESIG) [5], that analyzes social inclusion;
- Community integration questionnaire (CIQ) [24], that measures home integration, social integration and productive activities;
- Patient competency rating scale (PCRS) [25], that measures activities of daily living, behavioral and emotional functions, cognitive abilities, and physical functions;
- Behavioral scale, PCRSi (informer) [25], that is similar to PCRS but evaluated by an informer;
- Rancho scale levels of cognitive functioning [26], that generates a classification of the patient in one of eight levels;
- Barthel index [27], that it is an ordinal scale used to measure performance in activities of daily living (ADL);
- Disability rating scale (DRS) [28], that addresses impairment, disability and handicap; and
- Extended Glasgow outcome scale (GOSE) [29], that generates a classification of the patient in one of eight levels.
2.2. Monitoring System
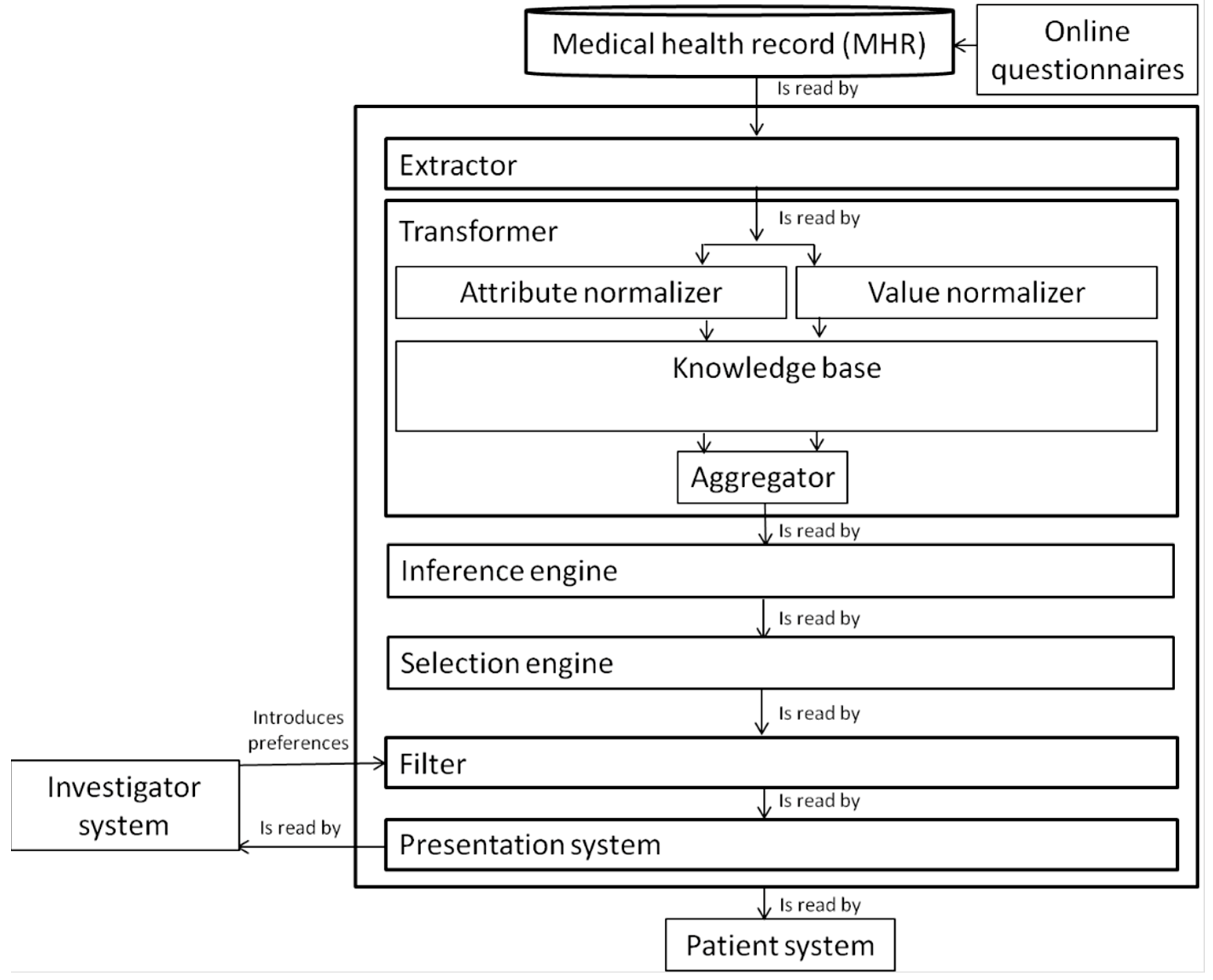
2.3. Clinical Decision Support System (CDSS)
| AttributePrognosis | Emotional Functions (419 people) | Executive Functions (477 people) |
|---|---|---|
| Age | (17,90), mean = 46.7 stdDev = 15.5 | (17,90), mean = 47.2 stdDev = 15.6 |
| Gender | female (145), male (274) | female (164), male (313) |
| Years from diagnosis | (4,67), mean = 17.9 stdDev = 15.7 | (2,72), mean = 19.0 stdDev = 17.0 |
| Disease | Not assigned (2), Guillain-Barre (18), polio (14), plexus (5), mielomeningocele (20), traumatic brain injury (213), multiple sclerosis (43), other progressive diseases (22), children cerebral palsy (103), hemorrhagic stroke (122), thrombotic stroke (26), embolic stroke (12), undetermined ischemic brain stroke (24), other ischemic brain stroke (9), other degenerative diseases not traumatic (84), muscular dystrophy (1), poliradiculoneuritis (7), other (4) | Not assigned (2), Guillain-Barre (14), polio (7), plexus (3), mielomeningocele (14), traumatic brain injury (133), multiple sclerosis (23), other progressive diseases (13), children cerebral palsy (73), hemorrhagic stroke (87), thrombotic stroke (22), embolic stroke (10), undetermined brain stroke (14), other ischemic brain stroke (5), other degenerative diseases not traumatic (51), muscular dystrophy (1), poliradiculoneuritis (3), other (2) |
| Origin | Traumatic (131), medic (208), undefined (80) | Traumatic (134), medic (231), undefined (112) |
| Length of the time series | (3,7), mean = 4.2, stdDev =1.0 | (3,7), mean = 4.2, stdDev = 1.0 |
| Missing values of the time series in the predicted attribute | 2007 (99%), 2008 (80%), 2009 (54%), 2010 (42%), 2011 (39%), 2012 (52%), 2013 (0%) | 2007 (77%), 2008 (69%), 2009 (69%), 2010 (45%), 2011 (37%), 2012 (47%), 2013 (0%) |
| Prediction | No deficiency (120), mild deficiency (130), moderate deficiency (112), severe deficiency (39), complete deficiency (18) | No deficiency (100), mild deficiency (69), moderate deficiency (103), severe deficiency (91), complete deficiency (114) |
3. Results
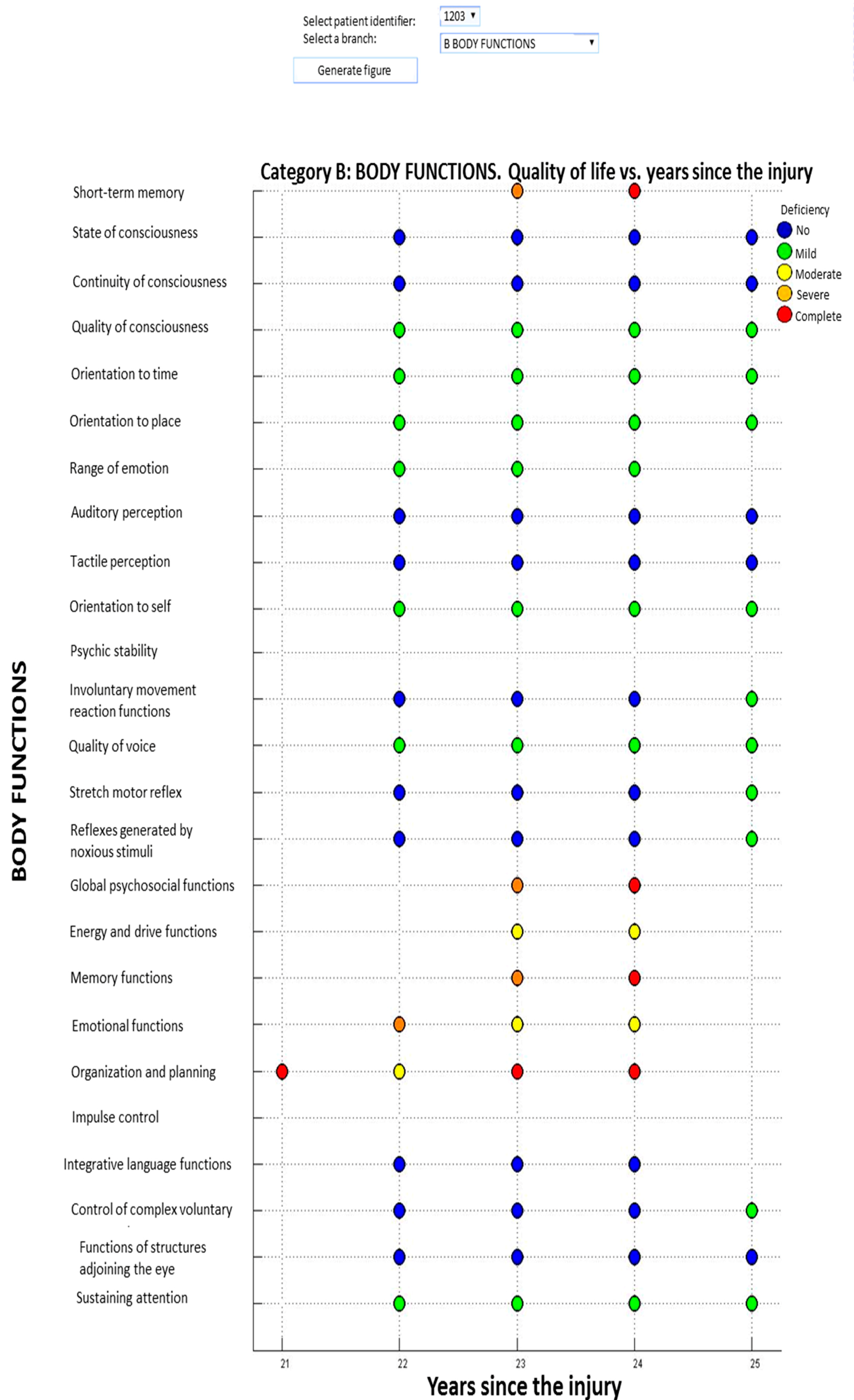
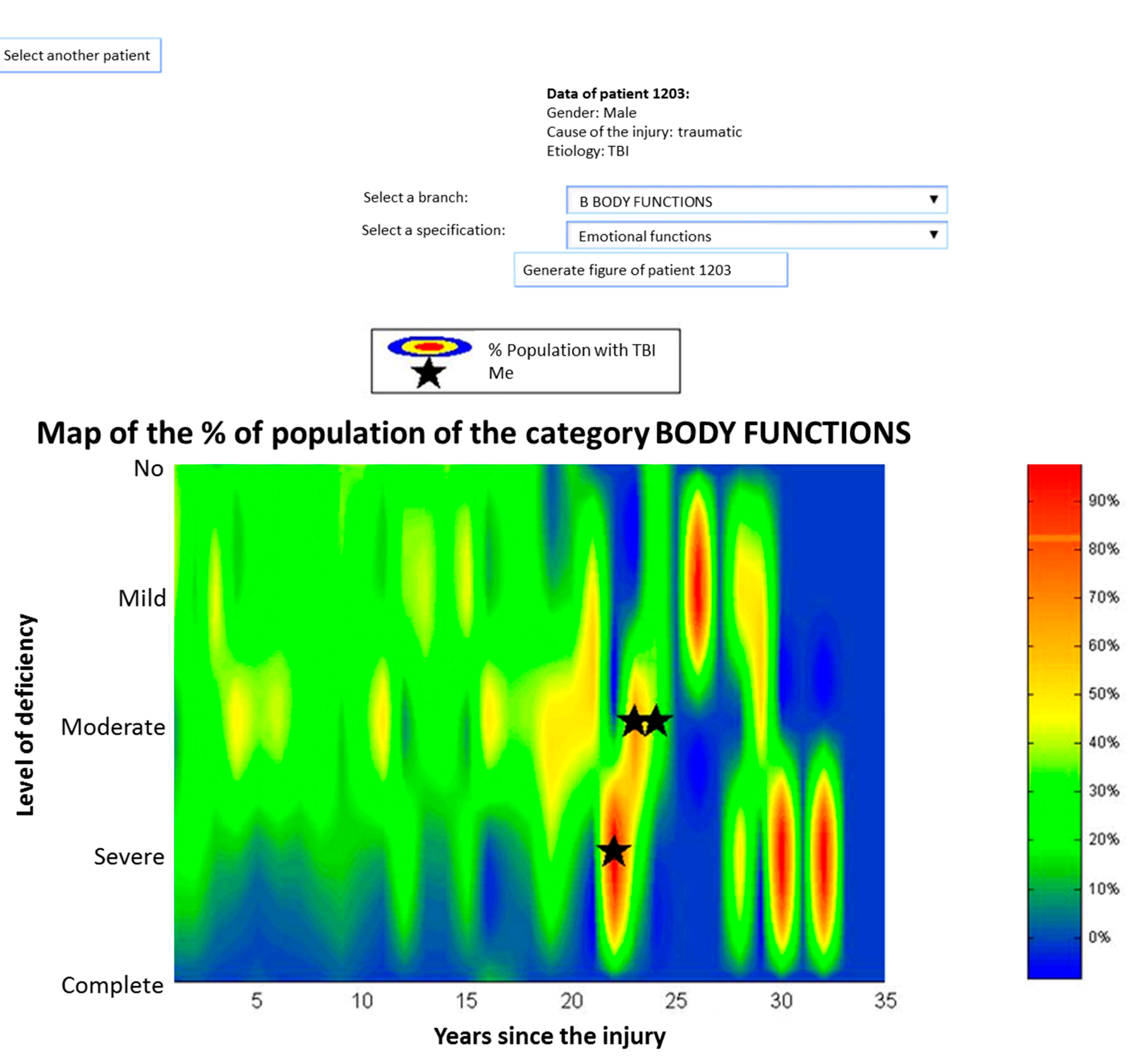
3.1. Individual Representation
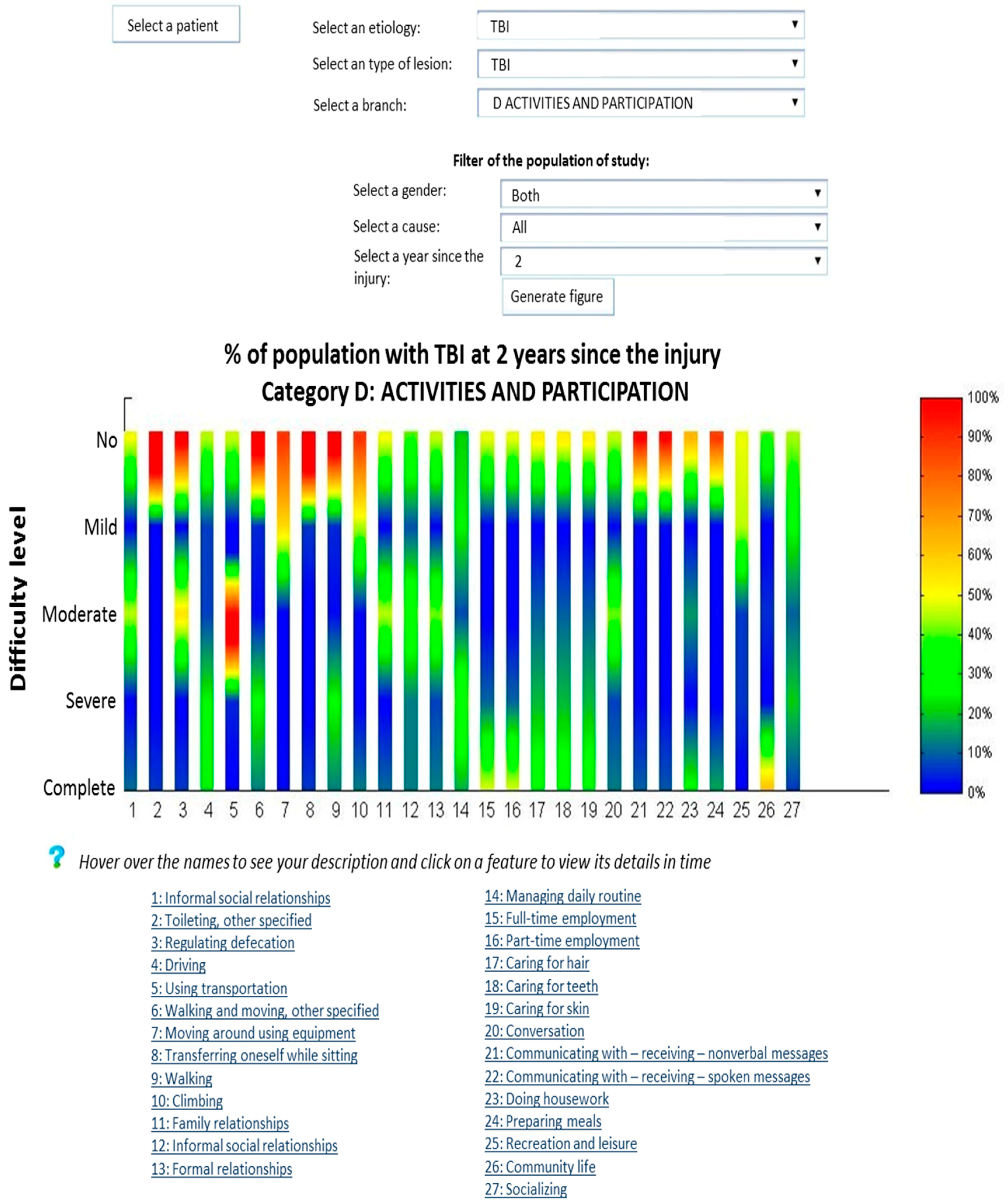
3.2. Population Representation (TBI Population)
| Temporal Representation | Learning | Accuracy | Precision | Recall (or Sensitivity) | Specificity |
|---|---|---|---|---|---|
| Full time-series | KNN (k = 7) | 0.33 | 0.35 | 0.33 | 0.82 |
| Full time-series | NB | 0.37 | 0.38 | 0.37 | 0.79 |
| Full time-series | SVM | 0.41 | 0.41 | 0.41 | 0.85 |
| Full time-series | J48 | 0.38 | 0.34 | 0.37 | 0.84 |
| Previous state | J48 | 0.37 | 0.32 | 0.35 | 0.77 |
- (1).
- Organization and planning (b1641) 2012: 51.93%
- (2).
- Dressing (d540) 2012: 12.29%
- (3).
- Personal economic resources (d8700) 2012: 6.75%
- (4).
- Eating (d550) 2012: 5.57%
- (5).
- Age: 3.56%
- (6).
- Toileting other specified (d5308) 2011: 3.19%
- (7).
- Carrying out daily routine (d230) 2010: 2.78%
- (8).
- Family relationships (d760) 2011: 2.58%
- (9).
- Recreation and leisure (d920) 2012: 2.21%
- (10).
- Sports (d9201) 2009: 1.77%
| Temporal Representation | Learning | Accuracy | Precision | Recall (Or Sensitivity) | Specificity |
|---|---|---|---|---|---|
| Full time-series | KNN (k = 7) | 0,32 | 0,30 | 0,32 | 0,82 |
| Full time-series | NB | 0,43 | 0,42 | 0,43 | 0,86 |
| Full time-series | SVM | 0,40 | 0,41 | 0,40 | 0,85 |
| Full time-series | J48 | 0,42 | 0,34 | 0,42 | 0,84 |
| Previous state | J48 | 0,48 | 0,47 | 0,48 | 0,87 |
- (1).
- Organization and planning (b1641) 2011: 56.40%
- (2).
- Personal care providers and personal assistants (e340) 2011: 20.26%
- (3).
- Work and employment other specified and unspecified (d859) 2011: 8.08%
- (4).
- Acquiring a place to live (d610) 2012: 7.61%
- (5).
- Complex economic transactions (d865) 2011: 1.96%
- (6).
- Informal education (d810) 2011: 1.32%
- (7).
- Organization and planning (b1641) 2012: 1.21%
- (8).
- Apprenticeship (work preparation) (d840) 2011: 1.06%
- (9).
- Full-time employment (d8502) 2011: 0.79%
- (10).
- Sports (d9201) 2009: 1.77%
4. Discussion
| ValueMain Target | Person with Disabilities | Professional | Health Center | Administration |
|---|---|---|---|---|
| Saving time | X | X | ||
| Saving costs | X | |||
| More information to make decisions | X | |||
| Interoperability | X | X | X | X |
| Joint decision making | X | X | ||
| Improving the socio-economic evaluation | X |
4.1. Saving Costs and Time
4.2. Having More Information to Make Decisions
4.3. Promoting Interoperability
4.4. Facilitating Joint Decision Making
4.5. Improving Policies for Socio-Economic Assessment of Disease Burden
- quality-adjusted life years (QALYs) - that are earned, calculated from the ICF indicators;
- DALYs averted, calculated from the QALYs; and
- savings calculated from the cost of DALYs averted minus the cost of the rehabilitation process.
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Sassi, F. Calculating QALYs comparing QALY and DALY calculations. Health Policy Plan. 2006, 21, 402–408. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. International Classification of Diseases (ICD-10). 2008. Available online: http://apps.who.int/classifications/icd (accessed on 8 September 2014).
- Traffic Service of the Interior Department of the Goverment of Catalonia. Accident and Disability, some Figs. 2002. Available online: http://guttmannazure.blob.core.windows.net/guttmann-publish/invar/b5ebb29b-5f8f-4066-8ad4-151ef84f0689 (accessed on 8 September 2014).
- Organización Mundial de la Salud. Hoja Informativa N 310. Available online: http://www.who.int/mediacentre/ factsheets/fs310/en/ (accessed on 8 September 2014).
- Institut Guttmann, Qvidlab. Laboratorio de medidas potenciadoras de la autonomía, satisfacción personal y calidad de vida de las personas con lesión medular y daño cerebral: tres años de investigación en calidad de vida y discapacidad: memoria 2006/2008, Technical report. 2009. Available online: http://sid.usal.es/idocs/F8/FDO24054/Memoria_2006_2008_Laboratorio.pdf. (accessed on 17 August 2015).
- Rector, A.; Nowlan, W.; Kay, S. Foundations of an electronic medical record. Methods Inf. Med. 1991, 30, 179–186. [Google Scholar] [PubMed]
- World Health Organization, International Classification of Functioning, Disability and Health (ICF). 2011. Available online: http://apps.who.int/classifications/icf (accessed on 8 September 2014).
- College of American Pathologists and National Health Service. Systematized Nomenclature of Medicine Clinical Terms (SNOMED CT). 2011. Available online: http://purl.bioontology.org/ontology/SNOMEDCT (accessed on 8 September 2014).
- Laxe, S.; Tschiesner, U.; Zasler, N.; López-Blazquez, R.; Tormos, J.M.; Bernabeu, M. What domains of the international classification of functioning, disability and health are covered by the most commonly used measurement instruments in traumatic brain injury research? Clin. Neurol. Neurosurg. 2012, 114, 645–650. [Google Scholar] [PubMed]
- Bernabeu, M.; Laxe, S.; López, R.; Stucki, G.; Ward, A.; Barnes, M.; Kostanjsek, N.; Reed, G.; Tate, R.; Whyte, J.; Zasler, N.; Cieza, A. Developing core sets for persons with traumatic brain injury based on the international classification of functioning, disability, and health. Neurorehabil. Neural. Repair 2009, 23, 464–467. [Google Scholar] [CrossRef] [PubMed]
- Cieza, A.; Brockow, T.; Ewert, T.; Amman, E.; Kollerits, B.; Chatterji, S.; Ustün, T.B.; Stucki, G. Linking health-status measurements to the international classification of functioning, disability and health. J. Rehabil. Med. 2002, 34, 205–210. [Google Scholar] [CrossRef] [PubMed]
- Cieza, A.; Geyh, S.; Chatterji, S.; Kostanjsek, N.; Ustün, B.; Stucki, G. ICF linking rules: An update based on lessons learned. J. Rehabil. Med. 2005, 37, 205–210. [Google Scholar] [CrossRef] [PubMed]
- Bickenbach, J.E.; Cieza, A.; Rauch, A.; Stucki, G. ICF Core Sets. Manual for Clinical Practice. 2012. Available online: http://www.icf-casestudies.org (accessed on 8 September 2014).
- Mpofu, E.; Oakland, T. Rehabilitation and Health Assessment: Applying ICF Guidelines; Springer: New York, NY, USA, 2010. [Google Scholar]
- Ceccaroni, L.; Subirats, L. Interoperable knowledge representation in clinical decision support 368 systems for rehabilitation. Int. J. Appl. Comput. Math. 2012, 11, 303–316. [Google Scholar]
- Subirats, L.; Ceccaroni, L.; Miralles, F. Knowledge representation for prognosis of health status in rehabilitation. Future Internet 2012, 4, 762–775. [Google Scholar] [CrossRef]
- Subirats, L.; Ceccaroni, L.; Gómez-Pérez, C.; Caballero, R.; Lopez-Blazquez, R.; Miralles, F. On Semantic, Rule-Based Reasoning in the Management of Functional Rehabilitation Processes. International Symposium on Management Intelligent Systems (IS-MiS 2013). Advances in Intelligent Systems and Computing. In Management Intelligent Systems; Springer: New York, NY, USA, 2013; pp. 51–58. [Google Scholar]
- Comín, M.C.; Ruiz, C.; Franco, E.; Damian, J.; Tovar, M.R.; de Pedro-Cuesta, J. Grupo Aragonés de Estudio de la Discapacidad (Discaparagon). Producción científico-profesional española sobre discapacidad según el modelo ICF. Revisión de la literatura, 2001–2011. Gaceta Sanit. 2011, 25, 39–46. [Google Scholar] [CrossRef] [PubMed]
- Vargiu, E.; Fernández, J.M.; Miralles, F. Context-Aware based Quality of Life Telemonitoring. Distributed Systems and Applications of Information Filtering and Retrieval. In Computational Intelligence; Springer: New York, NY, USA, 2014. [Google Scholar]
- García-Rudolph, A.; Gibert, K. A data mining approach to identify cognitive neurorehabilitation range in traumatic brain injury patients. Expert Syst. Appl. 2014, 41, 5238–5251. [Google Scholar] [CrossRef]
- Serra, J.; Arcos, J.L.; Garcia-Rudolph, A.; García-Molina, A.; Roig, T.; Tormos, J.M. Cognitive Prognosis Of Acquired Brain Injury Patients Using Machine Learning Techniques. In Proceedings of Advanced Cognitive Technologies and Applications, Iaria, Valencia, Spain, 27 May–1 June 2013.
- Rovlias, A.; Kotsou, S. Classification and regression tree for prediction of outcome after severe head injury using simple clinical and laboratory variables. J. Neurotrauma. 2004, 21, 886–893. [Google Scholar] [CrossRef] [PubMed]
- Espallargues, M.; Pons, J.M.V.; Almazán, C.; de Solà-Morales, O. Health technology assessment in public health interventions: Is prevention better than cure? Gaceta Sanit. 2011, 25, 40–48. [Google Scholar] [CrossRef]
- Dijkers, M. The Community Integration Questionnaire. The Center for Outcome Measurement in Brain Injury. Available online: http://www.tbims.org/combi/ciq (accessed on 31 July 2015).
- Kolakowsky-Hayner, S. The Patient Competency Rating Scale. The Center for Outcome Measurement in Brain Injury. Available online: http://www.tbims.org/combi/pcrs (accessed on 31 July 2015).
- Sander, A. The Level of Cognitive Functioning Scale. The Center for Outcome Measurement in Brain Injury. Available online: http://www.tbims.org/combi/lcfs (accessed on 31 July 2015).
- Mahoney, F.I.; Barthel, D. Functional evaluation: The Barthel Index. Maryland State Med. J. 1965, 14, 56–61. [Google Scholar]
- Wright, J. The Disability Rating Scale. The Center for Outcome Measurement in Brain Injury. Available online: http://www.tbims.org/combi/drs (accessed on 31 July 2015).
- Sander, A. The Extended Glasgow Outcome Scale. The Center for Outcome Measurement in Brain Injury. Available online: http://www.tbims.org/combi/gose (accessed on 31 July 2015).
- Miralles, F.; Ceccaroni, L.; Subirats, L.; Tormos, M.J.M.; Gil, O.A.; Lopez, B.R.; Garcia, R.A.; Mohammadian, S.D. System and Method for Extracting and Monitoring Multidimensional Attributes Regarding Personal Health Status and Evolution. Patent Application PCT/EP2011/074267, WO/2013/09. Available online: https://patentscope.wipo.int/search/en/detail.jsf?docId=WO2013097905&recNum=284&docAn=EP2011074267&queryString=adapter&maxRec=619197 (accessed on 14 August 2015).
- Subirats, L.; Ceccaroni, L.; Lopez-Blazquez, R.; Miralles, F.; García-Rudolph, A.; Tormos, J.M. Circles of Health: Towards an advanced social network about disabilities of neurological origin. J. Biomed. Inform. 2013, 46, 1006–1029. [Google Scholar] [CrossRef] [PubMed]
- BigML.com is Machine Learning for Everyone. Available online: https://bigml.com (accessed on 31 July 2015).
- Calvo, M.; Subirats, L.; Ceccaroni, L.; Maroto, J.M.; de Pablo, C.; Miralles, F. Automatic assessment of socioeconomic impact in cardiac rehabilitation. Int. J. Environ. Res. Public Health. 2013, 10, 5266–5283. [Google Scholar]
© 2015 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Subirats, L.; Lopez-Blazquez, R.; Ceccaroni, L.; Gifre, M.; Miralles, F.; García-Rudolph, A.; Tormos, J.M. Monitoring and Prognosis System Based on the ICF for People with Traumatic Brain Injury. Int. J. Environ. Res. Public Health 2015, 12, 9832-9847. https://doi.org/10.3390/ijerph120809832
Subirats L, Lopez-Blazquez R, Ceccaroni L, Gifre M, Miralles F, García-Rudolph A, Tormos JM. Monitoring and Prognosis System Based on the ICF for People with Traumatic Brain Injury. International Journal of Environmental Research and Public Health. 2015; 12(8):9832-9847. https://doi.org/10.3390/ijerph120809832
Chicago/Turabian StyleSubirats, Laia, Raquel Lopez-Blazquez, Luigi Ceccaroni, Mariona Gifre, Felip Miralles, Alejandro García-Rudolph, and Jose María Tormos. 2015. "Monitoring and Prognosis System Based on the ICF for People with Traumatic Brain Injury" International Journal of Environmental Research and Public Health 12, no. 8: 9832-9847. https://doi.org/10.3390/ijerph120809832
APA StyleSubirats, L., Lopez-Blazquez, R., Ceccaroni, L., Gifre, M., Miralles, F., García-Rudolph, A., & Tormos, J. M. (2015). Monitoring and Prognosis System Based on the ICF for People with Traumatic Brain Injury. International Journal of Environmental Research and Public Health, 12(8), 9832-9847. https://doi.org/10.3390/ijerph120809832








