Household Air Pollution and Under-Five Mortality in Bangladesh (2004–2011)
Abstract
:1. Introduction
2. Methods
2.1. Data Sources
2.1.1. Under-Five Mortality
2.1.2. Type of Cooking Fuel
2.1.3. Potential Confounders
2.2. Statistical Analysis
2.3. Ethics
3. Results
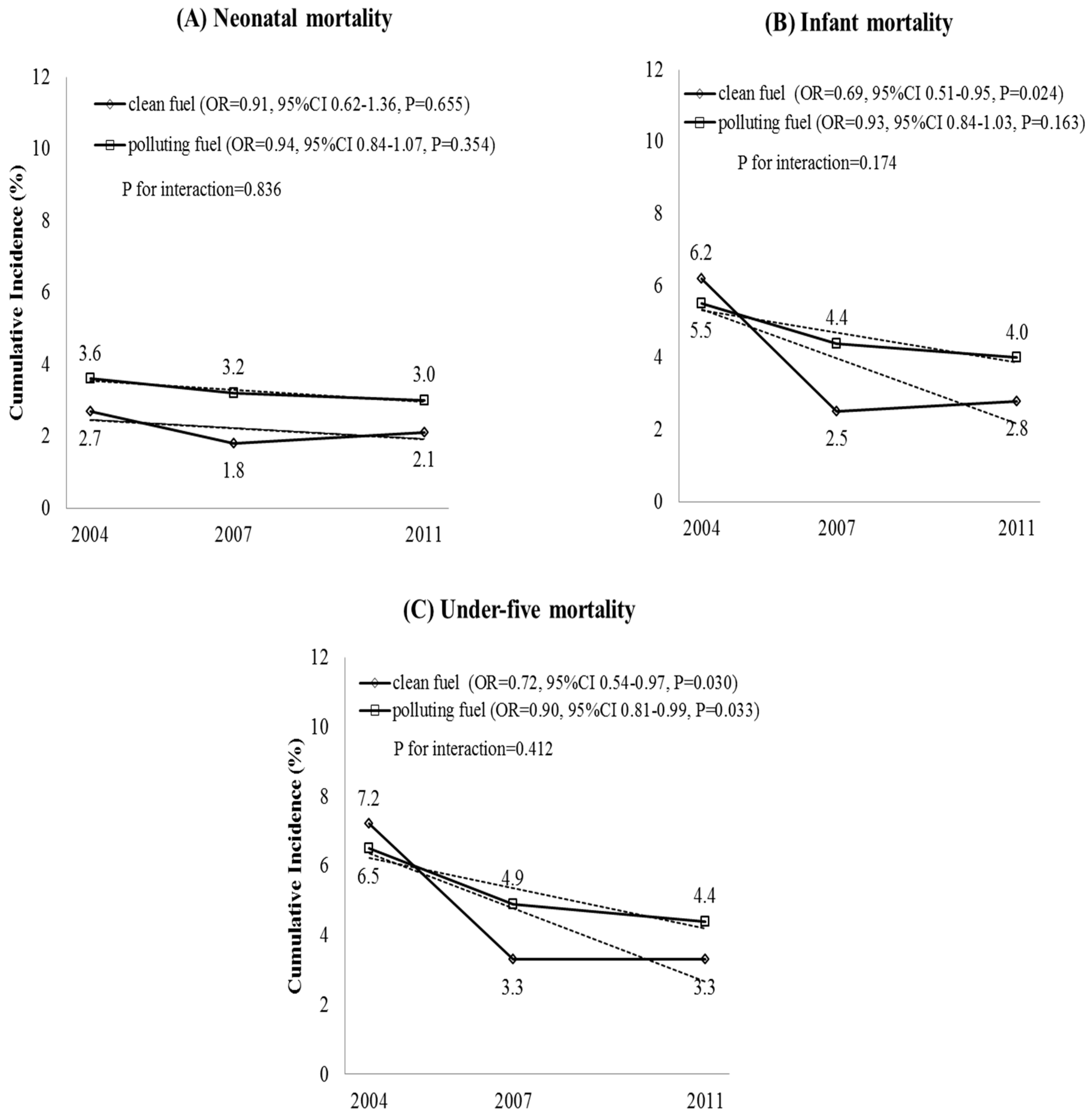
| Neonatal | Infant | Under-Five | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Study Factors | n/N ^ | n (%) P | OR a 95% CI | p Value | n/N ^ | n (%) P | OR a 95% CI | p Value | n/N ^ | n (%) P | OR a 95% CI | p Value |
| Type of Cooking Fuel | ||||||||||||
| Clean fuel R* | 41/1843 | 2.2 | 1.00 | 62/1843 | 3.5 | 1.00 | 73/1843 | 4.2 | 1.00 | |||
| polluting fuel ** | 532/16,465 | 3.3 | 1.49 (1.01–2.22) | 0.043 | 740/16,465 | 4.6 | 1.27 (0.91–1.77) | 0.157 | 850/16,465 | 5.2 | 1.14 (0.83–1.55) | 0.422 |
| Place of Residence | ||||||||||||
| Urban | 176/5888 | 3.0 | 1.00 | 250/5888 | 4.3 | 1.00 | 284/5888 | 5.0 | 1.00 | |||
| Rural | 397/12420 | 3.2 | 1.01 (0.81–1.25) | 0.967 | 552/12,420 | 4.5 | 0.96 (0.80–1.16) | 0.690 | 639/12,420 | 5.2 | 0.98 (0.82–1.17) | 0.799 |
| Wealth Index | ||||||||||||
| Rich R | 95/3512 | 2.7 | 1.00 | 125/3512 | 3.5 | 1.00 | 137/3512 | 3.9 | 1.00 | |||
| Middle | 198/6591 | 3.1 | 0.98 (0.72–1.33) | 0.904 | 272/6591 | 4.2 | 1.03 (0.79–1.35) | 0.822 | 316/6591 | 4.8 | 1.13 (0.87–1.46) | 0.367 |
| Poor | 280/8205 | 3.4 | 1.12 (0.79–1.59) | 0.535 | 405/8205 | 5.0 | 1.15 (0.84–1.57) | 0.373 | 470/8205 | 5.8 | 1.25 (0.93–1.69) | 0.137 |
| Mother’s Age | ||||||||||||
| 40–49 R | 10/492 | 1.9 | 1.00 | 23/492 | 4.7 | 1.00 | 27/492 | 5.6 | 1.00 | |||
| <20 | 115/2669 | 4.4 | 3.88 (1.98–7.59) | <0.001 | 157/2669 | 6.1 | 2.65 (1.65–4.24) | <0.001 | 171/2669 | 6.6 | 2.39 (1.54–3.72) | <0.001 |
| 20–29 | 347/11,266 | 3.2 | 2.08 (1.09–3.96) | 0.027 | 471/11,266 | 4.3 | 1.40 (0.88–2.13) | 0.163 | 542/11,266 | 4.9 | 1.34 (0.89–2.02) | 0.164 |
| 30–39 | 101/3865 | 2.6 | 1.61 (0.83–3.11) | 0.161 | 151/3865 | 3.9 | 1.09 (0.69–1.72) | 0.717 | 183/3865 | 4.8 | 1.12 (0.73–1.71) | 0.602 |
| Mother’s Education | ||||||||||||
| Secondary or higher R | 236/7987 | 3.1 | 1.00 | 295/7987 | 3.8 | 1.00 | 335/7987 | 4.4 | 1.00 | |||
| Primary | 181/5673 | 3.2 | 1.15 (0.93–1.44) | 0.203 | 248/5673 | 4.3 | 1.25 (1.03–1.52) | 0.024 | 284/5673 | 4.9 | 1.22 (1.02–1.47) | 0.029 |
| No education | 156/4648 | 3.4 | 1.28 (1.01–1.63) | 0.047 | 259/4648 | 5.7 | 1.67 (1.36–2.04) | <0.001 | 304/4648 | 6.5 | 1.64 (1.36–1.99) | <0.001 |
| Mother’s Working Status | ||||||||||||
| Working R | 110/3113 | 3.6 | 1.00 | 162/3113 | 5.2 | 1.00 | 186/3113 | 6.0 | 1.00 | |||
| Not working | 463/15,195 | 3.1 | 0.87 (0.69–1.08) | 0.208 | 640/15,195 | 4.3 | 0.85 (0.71–1.03) | 0.100 | 737/15,195 | 5.0 | 0.86 (0.72–1.03) | 0.092 |
| Breastfeeding Status | ||||||||||||
| Ever breastfed | 260/123,377 | 2.1 | 1.00 | 346/12,377 | 2.8 | 1.00 | 408/12,377 | 3.3 | 1.00 | |||
| Never breastfed | 313/5931 | 5.5 | 3.02 (2.52–3.62) | <0.001 | 456/5931 | 8.1 | 3.40 (2.91–3.97) | <0.001 | 515/5931 | 9.2 | 3.23 (2.79–3.73) | <0.001 |
| Wall Material of House | ||||||||||||
| Cement/brick R | 248/8470 | 2.9 | 1.00 | 322 | 3.8 | 1.00 | 362/8470 | 4.2 | 1.00 | |||
| Non-cement/non-brick | 279/8528 | 3.4 | 0.93 (0.73–1.18) | 0.564 | 420 | 5.1 | 1.02 (0.83–1.25) | 0.866 | 494/8528 | 6.0 | 1.04 (0.85–1.26) | 0.727 |
| Year of Survey | ||||||||||||
| 2004 R | 199/5852 | 3.6 | 1.00 | 308 | 5.5 | 1.00 | 364/5852 | 6.5 | 1.00 | |||
| 2007 | 151/4954 | 3.1 | 0.87 (0.68–1.11) | 0.260 | 201 | 4.2 | 0.76 (0.62–0.94) | 0.012 | 229/4954 | 4.8 | 0.74 (0.61–0.91) | 0.003 |
| 2011 | 223/7502 | 2.9 | 0.84 (0.67–1.07) | 0.157 | 293 | 3.8 | 0.77 (0.63–0.94) | 0.010 | 330/7502 | 4.3 | 0.73 (0.61–0.89) | 0.001 |
| Neonatal | Infant | Under-five | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Study Factors | n/N ^ | n (%) P | OR a 95% (CI) | p Value | n/N ^ | n (%) P | OR a 95% (CI) | p Value | n/N ^ | n (%) P | OR a 95% (CI) | p Value |
| Combined Association of Residence and Use of Cooking Fuel | ||||||||||||
| Urban residence used clean fuels R* | 38/1703 | 2.1 | 1.00 | 57/1703 | 3.4 | 1.00 | 65/1703 | 3.9 | 1.00 | |||
| Urban residence used polluting fuels ** | 138/4185 | 3.5 | 1.49 (1.03–2.14) | 0.033 | 193/4185 | 4.8 | 1.39 (1.03–1.88) | 0.033 | 219/4185 | 5.6 | 1.38 (1.03–1.84) | 0.028 |
| Rural residence used clean fuels * | 3/140 | 3.0 | 0.99 (0.29–3.19) | 0.958 | 5/140 | 4.5 | 1.09 (0.42–2.78) | 0.863 | 8/140 | 6.9 | 1.56 (0.72–3.37) | 0.255 |
| Rural residence used polluting fuels ** | 394/12,280 | 3.3 | 1.45 (1.03–2.04) | 0.032 | 547/12,280 | 4.5 | 1.35 (1.02–1.79) | 0.036 | 631/12,280 | 5.2 | 1.37 (1.05–1.78) | 0.021 |
| Combined Association of Breastfeeding Status and Use of Cooking Fuel | ||||||||||||
| Ever breastfed & used clean fuels R* | 11/1024 | 1.2 | 1.00 | 20/1024 | 2.1 | 1.00 | 24/1024 | 2.6 | 1.00 | |||
| Ever breastfed & used polluting fuels** | 249/11,353 | 2.2 | 2.05 (1.12–3.78) | 0.020 | 326/11353 | 2.9 | 1.49 (0.94–2.36) | 0.089 | 384/11,353 | 3.4 | 1.46 (0.96–2.22) | 0.080 |
| Never breastfed & used clean fuels * | 30/819 | 3.4 | 3.49 (1.74–7.02) | <0.001 | 42/819 | 5.2 | 2.73 (1.59–4.69) | <0.001 | 49/819 | 6.3 | 2.68 (1.63–4.41) | <0.001 |
| Never breastfed & used polluting fuels** | 283/5112 | 5.8 | 5.39 (2.94–9.92) | <0.001 | 414/5112 | 8.5 | 4.47 (2.83–7.06) | <0.001 | 466/5112 | 9.6 | 4.21 (2.77–6.41) | <0.001 |
| Combined Association of Kitchen Location and Use of Cooking Fuel*** | ||||||||||||
| Outside kitchen used clean fuels R* | 18/835 | 2.3 | 1.00 | 26/835 | 3.3 | 1.00 | 28/835 | 3.7 | 1.00 | |||
| Outside kitchen used polluting fuels ** | 342/10,791 | 3.1 | 1.46 (0.89–2.38) | 0.130 | 450/10,791 | 4.1 | 1.33 (0.89–2.01) | 0.167 | 497/10,791 | 4.5 | 1.35 (0.91–2.02 | 0.134 |
| Inside kitchen used clean fuels * | 12/621 | 1.5 | 0.89 (0.42–1.87) | 0.754 | 14/621 | 1.6 | 0.72 (0.37–1.39) | 0.33 | 20/621 | 2.7 | 0.96 (0.53–1.73) | 0.895 |
| Inside kitchen used polluting fuels ** | 82/2383 | 3.1 | 1.59 (0.94–2.69) | 0.084 | 126/2383 | 5.1 | 1.69 (1.09–2.62) | 0.019 | 151/2383 | 6.1 | 1.88 (1.23–2.87) | 0.003 |
4. Discussion
5. Conclusions
Supplementary Files
Supplementary File 1Acknowledgements
Author Contributions
Conflicts of Interest
References
- Fullerton, D.G.; Bruce, N.; Gordon, S.B. Indoor air pollution from biomass fuel smoke is a major health concern in the developing world. Trans. R. Soc. Trop. Med. Hyg. 2008, 102, 843–851. [Google Scholar] [CrossRef] [PubMed]
- Smith, K.R.; Mehta, S. The burden of disease from indoor air pollution in developing countries: Comparison of estimates. Int. J. Hyg. Environ. Health 2003, 206, 279–289. [Google Scholar] [CrossRef] [PubMed]
- Desai, M.A.; Mehta, S.; Smith, K. Indoor smoke from solid fuels—Assessing the environmental burden of disease at national and local levels. Environ. Burden Dis. Ser. 2004. [Google Scholar]
- Rehfuess, E.; Bruce, N.; Smith, K. Solid fuel use: Health effect. In Nriagu Jo Encyclopedia of Environmental Health; Elsevier: Burlington, VT, United States, 2011; Volume 5, p. 150161. [Google Scholar]
- WHO. Fuel for Life—Household Energy and Health. 2006. Available online: http://www.who.int/indoorair/publications/fuelforlife.pdf (accessed on 13 October 2015).
- Naeher, L.P.; Brauer, M.; Lipsett, M.; Zelikoff, J.T.; Simpson, C.D.; Koenig, J.Q.; Smith, K.R. Woodsmoke health effects: A review. Inhal. Toxicol. 2007, 19, 67–106. [Google Scholar] [CrossRef] [PubMed]
- WHO. Air Quality Guidelines for Particulate Matter, Ozone, Nitrogen Dioxide and Sulfur Dioxide. Global Update 2005. Available online: http://apps.who.int/iris/bitstream/10665/69477/1/WHO_SDE_PHE_OEH_06.02_eng.pdf (accessed on 13 October 2015).
- WHO. Burden of Disease from Household Air Pollution for 2012. Available online: http://www.who.int/phe/health_topics/outdoorair/databases/FINAL_HAP_AAP_BoD_24March2014.pdf (accessed on 13 October 2015).
- Lim, S.S.; Vos, T.; Flaxman, A.D.; Danaei, G.; Shibuya, K.; Adair-Rohani, H.; Amann, M.; Anderson, H.R.; Andrews, K.G.; Aryee, M.; et al. A comparative risk assessment of burden of disease and injury attributable to 67 risk factors and risk factor clusters in 21 regions, 1990–2010: A systematic analysis for the global burden of disease study 2010. Lancet 2012, 380, 2224–2260. [Google Scholar] [PubMed]
- Bruce, N.; Perez-Padilla, R.; Albalak, R. Indoor air pollution in developing countries: A major environmental and public health challenge. Bull. World Health Organ. 2000, 78, 1078–1092. [Google Scholar] [PubMed]
- WHO. Children’s health and the environment, A global perspective. Pronczuk-Garbino, M., Ed.; 2005. Available online: http://apps.who.int/iris/bitstream/10665/43162/1/9241562927_eng.pdf (accessed on 13 October 2015).
- WHO. Effects of Air Pollution on Children’s Health and Development. 2005. Available online: http://www.euro.who.int/__data/assets/pdf_file/0010/74728/E86575.pdf (accessed on 13 October 2015).
- Munroe, R.L.; Gauvain, M. Exposure to open-fire cooking and cognitive performance in children. Int. J. Environ. Health Res. 2012, 22, 156–164. [Google Scholar] [CrossRef] [PubMed]
- Bangladesh Demographic and Health Survey (2011). Available online: https://dhsprogram.com/pubs/pdf/FR265/FR265.pdf (accessed on 13 October 2015).
- Baqui, A.H.; Sabir, A.A.; Begum, N.; Arifeen, S.E.; Mitra, S.; Black, R.E. Causes of childhood deaths in bangladesh: An update. Acta Paediatr. 2001, 90, 682–690. [Google Scholar] [CrossRef] [PubMed]
- WHO. Indoor Air Pollution. National Burden of Disease Estimates. 2007. Available online: http://www.who.int/indoorair/publications/indoor_air_national_burden_estimate_revised.pdf (accessed on 13 October 2015).
- UNICEF. Levels & Trends in Child Mortality. 2014. Available online: http://www.unicef.org/media/files/Levels_and_Trends_in_Child_Mortality_2014.pdf (accessed on 13 October 2015).
- Gurley, E.; Homaira, N.; Salje, H.; Ram, P.; Haque, R.; Petri, W.; Bresee, J.; Moss, W.; Breysse, P.; Luby, S. Indoor exposure to particulate matter and the incidence of acute lower respiratory infections among children: A birth cohort study in urban bangladesh. Indoor Air 2013, 23, 379–386. [Google Scholar] [CrossRef] [PubMed]
- Gurley, E.S.; Salje, H.; Homaira, N.; Ram, P.K.; Haque, R.; Petri, W.A.; Bresee, J.; Moss, W.J.; Luby, S.P.; Breysse, P.; et al. Seasonal concentrations and determinants of indoor particulate matter in a low-income community in dhaka, bangladesh. Environ. Res. 2013, 121, 11–16. [Google Scholar] [CrossRef] [PubMed]
- Khalequzzaman, M.; Kamijima, M.; Sakai, K.; Chowdhury, N.A.; Hamajima, N.; Nakajima, T. Indoor air pollution and its impact on children under five years old in bangladesh. Indoor Air 2007, 17, 297–304. [Google Scholar] [CrossRef] [PubMed]
- Khalequzzaman, M.; Kamijima, M.; Sakai, K.; Ebara, T.; Hoque, B.A.; Nakajima, T. Indoor air pollution and health of children in biomass fuel-using households of bangladesh: Comparison between urban and rural areas. Environ. Health Prev. Med. 2011, 16, 375–383. [Google Scholar] [CrossRef] [PubMed]
- Khalequzzaman, M.; Kamijima, M.; Sakai, K.; Hoque, B.A.; Nakajima, T. Indoor air pollution and the health of children in biomass-and fossil-fuel users of bangladesh: Situation in two different seasons. Environ. Health Prev. Med. 2010, 15, 236–243. [Google Scholar] [CrossRef] [PubMed]
- Murray, E.; Brondi, L.; Kleinbaum, D.; McGowan, J.; van Mels, C.; Brooks, W.; Goswami, D.; Ryan, P.; Klein, M.; Bridges, C. Cooking fuel type, household ventilation, and the risk of acute lower respiratory illness in urban bangladeshi children: A longitudinal study. Indoor air 2012, 22, 132–139. [Google Scholar] [CrossRef] [PubMed]
- Bangladesh Demographic and Health Survey (2007); National Institute of Population Research and Training (NIPORT); Mitra and Associates; Dhaka, Bangladesh and Macro International. Calverton, MD, USA, 2009. Available online: http://dhsprogram.com/pubs/pdf/FR207/FR207[April-10-2009].pdf (accessed on 13 October 2015).
- Bangladesh Demographic and Health Survey (2004); National Institute of Population Research and Training (NIPORT); Mitra and Associates; Dhaka, Bangladesh and Macro International. Calverton, MD, USA, 2005. Available online: http://dhsprogram.com/pubs/pdf/fr165/fr-bd04[fr165].pdf (accessed on 13 October 2015).
- Choi, J.-Y.; Baumgartner, J.; Harnden, S.; Alexander, B.H.; Town, R.J.; D’Souza, G.; Ramachandran, G. Increased risk of respiratory illness associated with kerosene fuel use among women and children in urban Bangalore, India. Occup. Environ. Med. 2015, 72, 114–122. [Google Scholar] [CrossRef] [PubMed]
- Epstein, M.B.; Bates, M.N.; Arora, N.K.; Balakrishnan, K.; Jack, D.W.; Smith, K.R. Household fuels, low birth weight, and neonatal death in India: The separate impacts of biomass, kerosene, and coal. Int. J. Hyg. Environ. Health 2013, 216, 523–532. [Google Scholar] [CrossRef] [PubMed]
- Wichmann, J.; Voyi, K. Influence of cooking and heating fuel use on 1–59 month old mortality in South Africa. Matern. Child Health J. 2006, 10, 553–561. [Google Scholar] [CrossRef] [PubMed]
- Ezeh, O.K.; Agho, K.E.; Dibley, M.J.; Hall, J.J.; Page, A.N. The effect of solid fuel use on childhood mortality in Nigeria: Evidence from the 2013 cross-sectional household survey. Environ. Health 2014, 13. [Google Scholar] [CrossRef] [PubMed]
- Kashima, S.; Yorifuji, T.; Tsuda, T.; Ibrahim, J.; Doi, H. Effects of traffic-related outdoor air pollution on respiratory illness and mortality in children, taking into account indoor air pollution, in Indonesia. J. Occup. Environ. Med. 2010, 52, 340–345. [Google Scholar] [CrossRef] [PubMed]
- Pandey, S.; Lin, Y. Adjusted effects of domestic violence, tobacco use, and indoor air pollution from use of solid fuel on child mortality. Matern. Child Health J. 2013, 17, 1499–1507. [Google Scholar] [CrossRef] [PubMed]
- Rehfuess, E.A.; Tzala, L.; Best, N.; Briggs, D.J.; Joffe, M. Solid fuel use and cooking practices as a major risk factor for alri mortality among African children. J. Epidemiol. Community Health 2009, 63, 887–892. [Google Scholar] [CrossRef]
- Rinne, S.T.; Rodas, E.J.; Rinne, M.L.; Simpson, J.M.; Glickman, L.T. Use of biomass fuel is associated with infant mortality and child health in trend analysis. Am. J. Trop. Med. Hyg. 2007, 76, 585–591. [Google Scholar] [PubMed]
- Filmer, D.; Pritchett, L.H. Estimating wealth effects without expenditure data-or tears: An application to educational enrollments in states of India. Demography 2001, 38, 115–132. [Google Scholar] [PubMed]
- Bassani, D.G.; Jha, P.; Dhingra, N.; Kumar, R. Child mortality from solid-fuel use in india: A nationally-representative case-control study. BMC Public Health 2010, 10, 491. [Google Scholar] [PubMed]
- Tielsch, J.M.; Katz, J.; Thulasiraj, R.D.; Coles, C.L.; Sheeladevi, S.; Yanik, E.L.; Rahmathullah, L. Exposure to indoor biomass fuel and tobacco smoke and risk of adverse reproductive outcomes, mortality, respiratory morbidity and growth among newborn infants in south India. Int. J. Epidemiol. 2009, 38, 1351–1363. [Google Scholar] [CrossRef] [PubMed]
- Dasgupta, S.; Wheeler, D.; Huq, M.; Khaliquzzaman, M. Improving indoor air quality for poor families: A controlled experiment in bangladesh. Indoor Air 2009, 19, 22–32. [Google Scholar] [CrossRef] [PubMed]
- Arifeen, S.; Black, R.E.; Antelman, G.; Baqui, A.; Caulfield, L.; Becker, S. Exclusive breastfeeding reduces acute respiratory infection and diarrhea deaths among infants in Dhaka Slums. Pediatrics 2001, 108. [Google Scholar] [CrossRef]
- Black, R.E.S.S.J. Where and why are 10 million children dying every year? Lancet 2003, 361, 2226–2234. [Google Scholar] [CrossRef]
- Cushing, A.H.; Samet, J.M.; Lambert, W.E.; Skipper, B.J.; Hunt, W.C.; Young, S.A.; McLaren, L.C. Breastfeeding reduces risk of respiratory illness in infants. Am. J. Epidemiol. 1998, 147, 863–870. [Google Scholar] [CrossRef] [PubMed]
- Heinig, M.J. Host defense benefits of breastfeeding for the infant: Effect of breastfeeding duration and exclusivity. Pediatr. Clin. North Am. 2001, 48, 105–123. [Google Scholar] [CrossRef]
- Institute for Health Metrics and Evaluation (IHME). The Global Burden of Diseases Study. 2010. Available online: https://www.healthdata.org/sites/default/files/files/country_profiles/GBD/ihme_gbd_country_report_bangladesh.pdf (accessed on 13 October 2015).
- Dasgupta, S.; Huq, M.; Khaliquzzaman, M.; Pandey, K.; Wheeler, D. Indoor air quality for poor families: New evidence from bangladesh. Indoor Air 2006, 16, 426–444. [Google Scholar] [CrossRef] [PubMed]
- Lahiri-Dutt, K. Energy Resources: Will they be the last frontier in South Asia? Available online: https://crawford.anu.edu.au/acde/asarc/pdf/papers/2006/WP2006_10.pdf (accessed on 13 October 2015).
- Rouse, J.R. Indoor air pollution: Issues for Bangladesh. 2004. Available online: http://stoves.bioenergylists.org/stovesdoc/Rouse/rouiap.pdf (accessed on 13 October 2015).
- Ahmed, L.A. Women’s roles in addressing indoor air pollution issues in bangladesh: Knowledge and attitude. Brown University: Providence, RI, United States, 2003. [Google Scholar]
- Polsky, D.; Ly, C. The Health Consequences of Indoor Air Pollution: A Review of The Solutions And Challenges; White paper; Philadelphia: University of Pennsylvania, Retrieved October; 2012; Volumn 8, p. 2012. [Google Scholar]
- Barnes, B.R. Behavioural change, indoor air pollution and child respiratory health in developing countries: A review. Int. J. Environ. Res. Public Health 2014, 11, 4607–4618. [Google Scholar] [PubMed]
© 2015 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Naz, S.; Page, A.; Agho, K.E. Household Air Pollution and Under-Five Mortality in Bangladesh (2004–2011). Int. J. Environ. Res. Public Health 2015, 12, 12847-12862. https://doi.org/10.3390/ijerph121012847
Naz S, Page A, Agho KE. Household Air Pollution and Under-Five Mortality in Bangladesh (2004–2011). International Journal of Environmental Research and Public Health. 2015; 12(10):12847-12862. https://doi.org/10.3390/ijerph121012847
Chicago/Turabian StyleNaz, Sabrina, Andrew Page, and Kingsley Emwinyore Agho. 2015. "Household Air Pollution and Under-Five Mortality in Bangladesh (2004–2011)" International Journal of Environmental Research and Public Health 12, no. 10: 12847-12862. https://doi.org/10.3390/ijerph121012847
APA StyleNaz, S., Page, A., & Agho, K. E. (2015). Household Air Pollution and Under-Five Mortality in Bangladesh (2004–2011). International Journal of Environmental Research and Public Health, 12(10), 12847-12862. https://doi.org/10.3390/ijerph121012847








