Changes in Access to Health Services of the Immigrant and Native-Born Population in Spain in the Context of Economic Crisis †
Abstract
:1. Introduction
2. Method
2.1. Design
2.2. Study Population and Sample
2.3. Variables
2.4. Statistical Analysis
3. Results
3.1. Sociodemographic Characteristics of the Sample
| Autochthons | Immigrants from low-income countries | |||
|---|---|---|---|---|
| 2006 | 2012 | 2006 | 2012 | |
| n (%) | n (%) | n (%) | n (%) | |
| Sociodemographic characteristics | ||||
| Sex | ||||
| Men | 9470 (51.2) | 6403 (51.0) | 1370 (47.4) | 1150 (48.1) |
| Women | 9034 (48.8) | 6156 (49.0) | 1523 (52.6) | 1240 (51.9) |
| Age | ||||
| 16–29 | 5137 (27.8) | 3153 (25.1) | 1180 (40.8) | 761 (31.8) |
| 30–44 | 7426 (40.1) | 4937 (39.3) | 1242 (42.9) | 1154 (48.3) |
| 45–59 | 5941 (32.1) | 4470 (35.6) | 472 (16.3) | 476 (19.9) |
| Education level | ||||
| No studies | 714 (3.9) | 398 (3.2) | 184 (6.4) | 144 (6.0) |
| Primary | 9091 (49.6) | 5458 (43.5) | 1213 (42.2) | 1019 (42.6) |
| Secondary | 4699 (25.6) | 3131 (24.9) | 1057 (36.8) | 817 (34.2) |
| University | 3827 (20.9) | 3572 (28.4) | 420 (14.6) | 410 (17.2) |
| Time of residence in Spain | ||||
| 0–4 years | 405 (17.1) | |||
| 5–10 years | 1309 (55.2) | |||
| More than 10 years | 659 (27.8) | |||
| Country of birth | ||||
| Europe | 587 (20.3) | 543 (22.7) | ||
| Latin America | 1633 (56.4) | 1243 (52.0) | ||
| Maghreb | 459 (15.9) | 340 (14.2) | ||
| Sub-Saharan Africa | 114 (3.9) | 110 (4.6) | ||
| Asia | 101 (3.5) | 154 (6.4) | ||
| Social class | ||||
| I–II (directors and managers) | 4198 (23.1) | 2523 (20.5) | 293 (10.3) | 121 (5.2) |
| II | 4668 (25.7) | 2703 (22.0) | 288 (10.2) | 223 (9.6) |
| III | 7314 (40.2) | 5238 (42.6) | 1498 (52.8) | 1156 (49.6) |
| IV (unskilled workers) | 2015 (11.1) | 1830 (14.9) | 756 (26.7) | 832 (35.7) |
| Private health insurance | ||||
| Yes | 3115 (16.8) | 1999 (15.9) | 261 (9.3) | 152 (6.4) |
| Employment situation | ||||
| Paid work | 12105 (65.5) | 7457 (59.5) | 2095 (72.5) | 1220 (51.2) |
| Unemployed | 1683 (9.1) | 2247 (17.9) | 297 (10.3) | 641 (26.9) |
| Other a | 4689 (25.4) | 2837 (22.6) | 496 (17.2) | 521 (21.9) |
| Civil status | ||||
| Married | 8359 (45.3) | 5955 (47.4) | 1415 (48.9) | 1115 (46.7) |
| Single. separated or divorced. widowed | 10112 (54.7) | 6596 (52.6) | 1476 (51.1) | 1272 (53.3) |
| Need | ||||
| Perceived health | ||||
| Good (very good or good) | 13,962 (75.5) | 10,147 (80.8) | 2073 (71.7) | 1863 (77.9) |
| Poor (regular. poor or very poor) | 4541 (24.5) | 2412 (19.2) | 820 (28.3) | 528 (22.1) |
| Chronic disease | ||||
| None | 5488 (29.7) | 4743 (37.8) | 1138 (39.3) | 1205 (50.4) |
| One | 4123 (22.3) | 2933 (23.4) | 634 (21.9) | 553 (23.1) |
| Two | 2951 (15.9) | 1780 (14.2) | 415 (14.3) | 237 (9.9) |
| Three or more | 5941 (32.1) | 3103 (24.7) | 705 (24.4) | 396 (16.6) |
| Injury | ||||
| Yes | 1971 (10.7) | 1084 (8..6) | 294 (10.2) | 186 (7.8) |
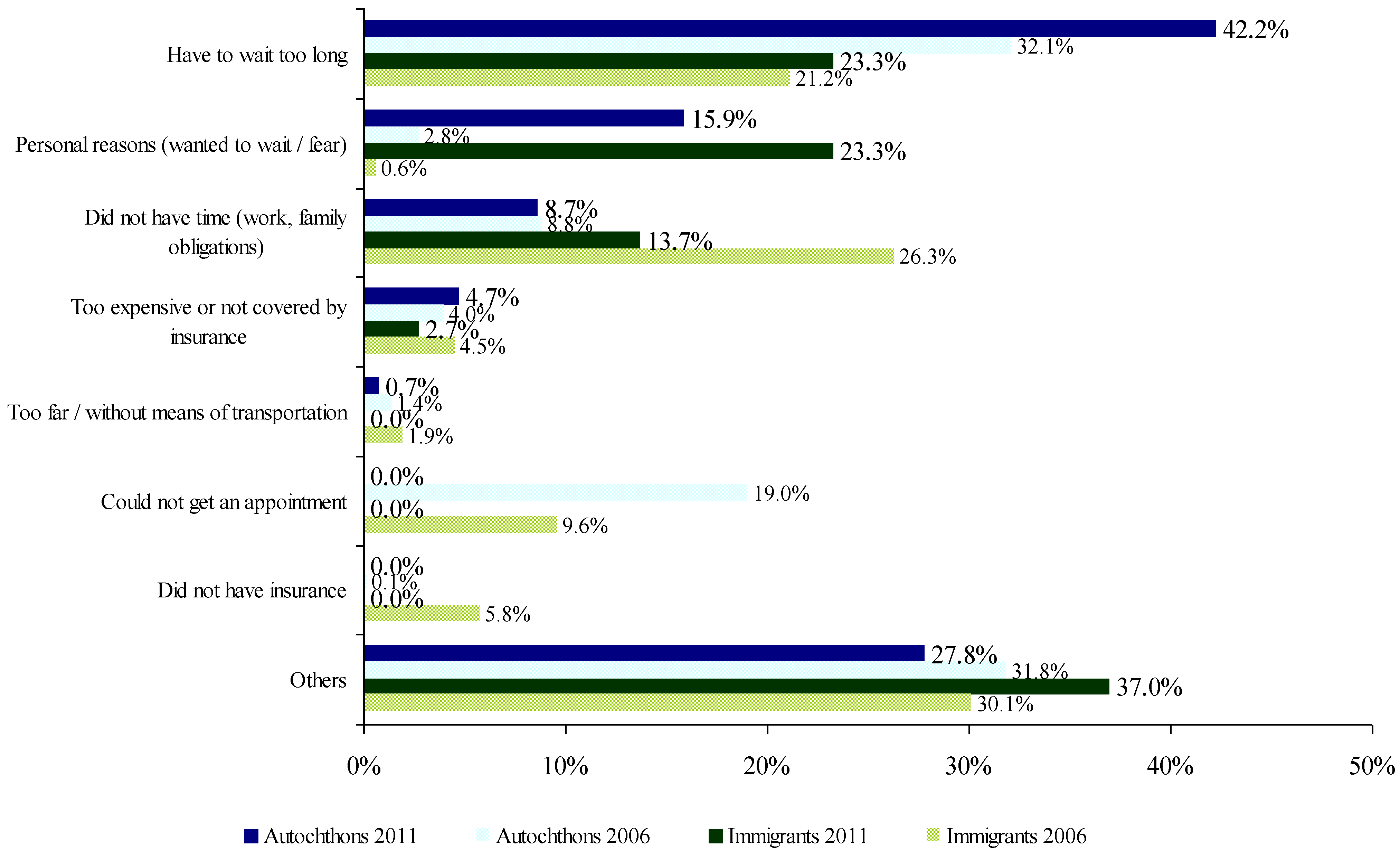
3.2. Unmet Health Needs
3.3. Use of Health Services by Level of Care
| Autochthons | Immigrants | Immigrants Compared to Autochthons | ||||||
|---|---|---|---|---|---|---|---|---|
| 2006 | 2012 | PR a (IC 95%) | 2006 | 2012 | PR a (IC 95%) | 2006 | 2012 | |
| n (prev) | n (prev) | n (prev) | n (prev) | PR b (IC 95%) | PR b (IC 95%) | |||
| Unmet need | 731 (4.0) | 277 (2.2) | 0.61 (0.52–0.72) | 162 (5.6) | 73 (3.1) | 0.65 (0.44–0.98) | 1.21 (0.89–1.63) | 1.22 (0.86–1.74) |
| Health service use | ||||||||
| Visit to general practitioner | 4696 (25.5) | 2821 (22.5) | 0.91 (0.87–0.96) | 683 (23.9) | 586 (24.5) | 1.02 (0.86–1.21) | 0.91 (0.80–1.03) | 1.01 (0.89–1.15) |
| Visit to specialist | 2619 (14.3) | 1773 (14.1) | 1.08 (1.01–1.16) | 304 (10.7) | 262 (11.0) | 1.03 (0.79–1.34) | 0.76 (0.63–0.91) | 0.84 (0.70–1.02) |
| Hospitalization (not births) c | 1149 (6.2) | 700 (5.6) | 1.02 (0.91–1.15) | 174 (6.0) | 141 (5.9) | 1.07 (0.73–1.58) | 0.99 (0.74–1.33) | 1.06 (0.80–1.41) |
| Emergency (not births) c | 5242 (28.3) | 3290 (26.2) | 1.02 (0.98–1.07) | 941 (32.5) | 728 (30.4) | 1.04 (0.90–1.18) | 1.06 (0.96–1.17) | 1.06 (0.95–1.18) |
3.4. Factors Associated with the Use of Different Levels of Care
| Autochthons | Immigrants | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 2006 | 2012 | 2006 | 2012 | |||||||||
| Prev | PR (CI 95%) | Prev | PR (CI 95%) | Prev | PR (CI 95%) | Prev | PR (CI 95%) | |||||
| Predisposing factors | ||||||||||||
| Sex | ||||||||||||
| Men | 21.1 | 1 | 18.9 | 1 | 19.3 | 1 | 17.9 | 1 | ||||
| Women | 30.1 | 1.18 (1.10–1.27) | 26.2 | 1.22 (1.13–1.33) | 27.9 | 1.20 (0.91–1.56) | 30.6 | 1.43 (1.09–1.87) | ||||
| Age | ||||||||||||
| 16–29 | 21.5 | 1 | 19.2 | 1 | 21.9 | 1 | 20.1 | 1 | ||||
| 30–44 | 23.3 | 0.90 (0.81–1.01) | 20.9 | 1.02 (0.89–1.16) | 22.6 | 0.90 (0.68–1.18) | 25.5 | 0.99 (0.73–1.34) | ||||
| 45–59 | 31.7 | 0.93 (0.83–1.04) | 26.6 | 1.01 (0.89–1.15) | 32.0 | 1.14 (0.82–1.59) | 29.2 | 0.97 (0.69–1.36) | ||||
| Enabling factors | ||||||||||||
| Social class | ||||||||||||
| I–II (directors and managers) | 20.5 | 1 | 17.4 | 1 | 23.0 | 1 | 30.8 | 1 | ||||
| II | 24.9 | 1.11 (1.01–1.23) | 20.7 | 1.11 (0.97–1.27) | 21.9 | 0.83 (0.50–1.39) | 21.1 | 0.67 (0.39–1.13) | ||||
| III | 27.8 | 1.14 (1.04–1.26) | 23.3 | 1.19 (1.06–1.34) | 24.6 | 1.07 (0.76–1.51) | 21.7 | 0.71 (0.47–1.08) | ||||
| IV (unskilled workers) | 29.2 | 1.16 (1.03–1.32) | 28.9 | 1.24 (1.09–1.43) | 23.6 | 1.11 (0.75–1.63) | 28.1 | 0.79 (0.52–1.22) | ||||
| Private health insurance | ||||||||||||
| No | 26.6 | 1 | 23.1 | 1 | 25.0 | 1 | 24.9 | 1 | ||||
| Yes | 20.2 | 0.85 (0.77–0.94) | 19.0 | 0.92 (0.82–1.04) | 19.3 | 0.80 (0.55–1.16) | 18.4 | 0.80 (0.51–1.25) | ||||
| Employment situation | ||||||||||||
| Workers | 23.5 | 1 | 19.9 | 1 | 21.9 | 1 | 24.8 | 1 | ||||
| Unemployed | 29.1 | 1.05 (0.93–1.18) | 24.5 | 1.08 (0.97–1.19) | 27.1 | 1.12 (0.77–1.62) | 22.2 | 0.96 (0.72–1.27) | ||||
| Other a | 29.4 | 1.04 (0.96–1.12) | 27.6 | 1.14 (1.04–1.26) | 30.2 | 1.21 (0.90–1.63) | 26.5 | 1.15 (0.85–1.56) | ||||
| Civil status | ||||||||||||
| Married | 28.0 | 1 | 23.1 | 1 | 26.7 | 1 | 26.4 | 1 | ||||
| Single. separated. divorced or widowed | 22.5 | 0.93 (0.86–1.01) | 21.8 | 1.05 (0.97–1.14) | 21.0 | 0.86 (0.67–1.09) | 22.0 | 0.84 (0.67–1.05) | ||||
| Need | ||||||||||||
| Self-rated health | ||||||||||||
| Good | 18.7 | 1 | 17.8 | 1 | 19.9 | 1 | 20.0 | 1 | ||||
| Poor | 46.4 | 1.85 (1.71–1.99) | 42.2 | 1.79 (1.64–1.96) | 33.8 | 1.32 (1.03–1.7) | 40.5 | 1.37 (1.06–1.76) | ||||
| Chronic disease | ||||||||||||
| None | 13.4 | 1 | 14.4 | 1 | 17.3 | 1 | 16.3 | 1 | ||||
| One | 20.8 | 1.44 (1.26–1.64) | 20.5 | 1.37 (1.21–1.56) | 21.7 | 1.16 (0.81–1.67) | 25.4 | 1.55 (1.11–2.17) | ||||
| Two | 26.2 | 1.68 (1.46–1.94) | 22.7 | 1.39 (1.21–1.59) | 27.6 | 1.39 (0.97–1.99) | 35.4 | 1.99 (1.41–2.81) | ||||
| Three or more | 39.7 | 2.05 (1.81–2.32) | 36.4 | 1.80 (1.59–2.03) | 34.3 | 1.55 (1.10–2.16) | 41.9 | 2.07 (1.48–2.89) | ||||
| Autochthons | Immigrants | |||||||
|---|---|---|---|---|---|---|---|---|
| 2006 | 2012 | 2006 | 2012 | |||||
| Prev | PR (CI 95%) | Prev | PR (CI 95%) | Prev | PR (CI 95%) | Prev | PR (CI 95%) | |
| Predisposing factors | ||||||||
| Sex | ||||||||
| Men | 10.9 | 1 | 11.1 | 1 | 6.2 | 1 | 6.2 | 1 |
| Women | 17.9 | 1.38 (1.241.53) | 17.3 | 1.32 (1.18–1.47) | 14.6 | 2.08 (1.29–3.36) | 15.4 | 2.24 (1.46–3.46) |
| Age | ||||||||
| 16–29 | 10.7 | 1 | 10.1 | 1 | 8.4 | 1 | 7.6 | 1 |
| 30–44 | 14.6 | 1.06 (0.9–1.25) | 13.5 | 1.01 (0.85–1.21) | 10.9 | 1.11 (0.70–1.76) | 12.0 | 1.46 (0.94–2.27) |
| 45–59 | 17.2 | 0.95 (0.8–1.13) | 17.7 | 1.00 (0.84–1.20) | 15.6 | 1.27 (0.73–2.19) | 13.9 | 1.45 (0.87–2.43) |
| Enabling factors | ||||||||
| Social class | ||||||||
| I–II (directors and managers) | 13.7 | 1 | 15.5 | 1 | 12.5 | 1 | 15.0 | 1 |
| II | 14.9 | 1.04 (0.92–1.19) | 15.9 | 0.96 (0.83–1.11) | 16.7 | 1.36 (0.74–2.50) | 12.1 | 0.84 (0.39–1.81) |
| III | 14.2 | 0.94 (0.83–1.07) | 12.3 | 0.76 (0.66–0.87) | 8.8 | 0.85 (0.52–1.41) | 10.6 | 0.85 (0.43–1.68) |
| IV (unskilled workers) | 14.5 | 0.94 (0.79–1.11) | 15.1 | 0.76 (0.64–0.91) | 11.6 | 1.25 (0.71–2.21) | 10.3 | 0.65 (0.32–1.35) |
| Private health insurance | ||||||||
| No | 13.7 | 1 | 12.8 | 1 | 9.9 | 1 | 10.5 | 1 |
| Yes | 17.4 | 1.34 (1.19–1.50) | 20.9 | 1.62 (1.43–1.83) | 18.4 | 1.83 (1.22–2.75) | 18.4 | 1.92 (1.14–3.23) |
| Employment situation | ||||||||
| Workers | 13.5 | 1 | 13.5 | 1 | 9.3 | 1 | 11.1 | 1 |
| Unemployed | 15.1 | 0.99 (0.84–1.16) | 13.4 | 0.98 (0.85–1.14) | 17.1 | 1.61 (0.99–2.62) | 10.9 | 1.17 (0.79–1.74) |
| Other a | 16.2 | 1.03 (0.92–1.15) | 16.4 | 1.13 (0.99–1.28) | 12.2 | 1.01 (0.63–1.62) | 10.7 | 1.12 (0.71–1.78) |
| Civil status | ||||||||
| Married | 16.0 | 1 | 16.0 | 1 | 8.8 | 1 | 9.9 | 1 |
| Single. separated. divorced or widowed | 12.3 | 0.99 (0.88–1.11) | 12.1 | 0.91 (0.82–1.02) | 12.5 | 0.85 (0.58–1.23) | 12.2 | 1.37 (0.97–1.93) |
| Need | ||||||||
| Self-rated health | ||||||||
| Good | 9.8 | 1 | 9.9 | 1 | 7.9 | 1 | 8.4 | 1 |
| Poor | 28.6 | 2.19 (1.97–2.43) | 31.7 | 2.54 (2.26–2.85) | 17.6 | 1.62 (1.02–2.57) | 20.1 | 1.67 (1.15–2.43) |
| Chronic disease | ||||||||
| None | 6.2 | 1 | 7.3 | 1 | 7.4 | 1 | 7.8 | 1 |
| One | 11.3 | 1.60 (1.33–1.92) | 13.2 | 1.61 (1.36–1.90) | 6.7 | 0.80 (0.45–1.42) | 10.9 | 1.20 (0.74–1.94) |
| Two | 14.9 | 1.95 (1.60–2.37) | 14.8 | 1.54 (1.27–1.87) | 13.0 | 1.24 (0.72–2.14) | 13.1 | 1.33 (0.74–2.40) |
| Three or more | 23.8 | 2.41 (2.03–2.86) | 25.0 | 2.05 (1.74–2.43) | 18.3 | 1.34 (0.68–2.67) | 19.4 | 1.41 (0.87–2.30) |
| Autochthons | Immigrants | |||||||
|---|---|---|---|---|---|---|---|---|
| 2006 | 2012 | 2006 | 2012 | |||||
| Prev | PR (CI 95%) | Prev | PR (CI 95%) | Prev | PR (CI 95%) | Prev | PR (CI 95%) | |
| Predisposing factors | ||||||||
| Sex | ||||||||
| Men | 6.6 | 1 | 5.6 | 1 | 5.8 | 1 | 6.2 | 1 |
| Women | 5.8 | 0.74 (0.63–0.87) | 5.5 | 0.83 (0.70–0.99) | 6.2 | 1.00 (0.52–1.91) | 5.7 | 0.77 (0.43–1.37) |
| Age | ||||||||
| 16–29 | 4.8 | 1 | 4.4 | 1 | 5.0 | 1 | 4.9 | 1 |
| 30–44 | 5.5 | 1.04 (0.81–1.35) | 5.1 | 0.98 (0.73–1.30) | 7.0 | 1.11 (0.58–2.09) | 5.6 | 0.97 (0.52–1.81) |
| 45–59 | 8.3 | 1.19 (0.92–1.55) | 6.8 | 0.95 (0.71–1.27) | 5.9 | 0.80 (0.32–2.03) | 8.2 | 1.15 (0.56–2.37) |
| Enabling factors | ||||||||
| Social class | ||||||||
| I–II (directors and managers) | 5.5 | 1 | 4.4 | 1 | 3.8 | 1 | 4.1 | 1 |
| II | 5.8 | 0.95 (0.76–1.19) | 5.9 | 1.22 (0.93–1.60) | 9.0 | 2.11 (0.64–6.94) | 5.8 | 1.30 (0.21–7.85) |
| III | 6.4 | 0.97 (0.79–1.19) | 5.8 | 1.03 (0.79–1.33) | 6.3 | 1.43 (0.53–3.86) | 5.7 | 1.34 (0.26–7.00) |
| IV (unskilled workers) | 7.5 | 1.02 (0.77–1.36) | 6.3 | 0.98 (0.73–1.31) | 5.4 | 1.18 (0.38–3.62) | 6.7 | 1.56 (0.29–8.58) |
| Private health insurance | ||||||||
| No | 6.0 | 1 | 5.2 | 1 | 6.3 | 1 | 3.9 | 1 |
| Yes | 7.3 | 1.41 (1.16–1.73) | 7.6 | 1.63 (1.33–2.00) | 4.6 | 0.65 (0.25–1.70) | 6.0 | 0.58 (0.19–1.77) |
| Employment situation | ||||||||
| Workers | 5.7 | 1 | 4.8 | 1 | 6.3 | 1 | 6.3 | 1 |
| Unemployed | 7.6 | 1.18 (0.90–1.54) | 6.5 | 1.21 (0.97–1.52) | 6.1 | 0.91 (0.42–1.97) | 6.2 | 0.93 (0.51–1.67) |
| Other a | 7.0 | 1.13 (0.93–1.36) | 6.8 | 1.30 (1.05–1.61) | 4.8 | 0.71 (0.35–1.42) | 4.6 | 0.91 (0.40–2.07) |
| Civil status | ||||||||
| Married | 6.4 | 1 | 5.7 | 1 | 6.2 | 1 | 6.7 | 1 |
| Single. separated. divorced or widowed | 5.9 | 1.11 (0.93–1.32) | 5.4 | 1.02 (0.85–1.23) | 5.9 | 1.02 (0.59–1.77) | 5.0 | 0.83 (0.51–1.34) |
| Need | ||||||||
| Self-rated health | ||||||||
| Good | 3.2 | 1 | 3.2 | 1 | 3.6 | 1 | 4.0 | 1 |
| Poor | 15.5 | 4.43 (3.68–5.33) | 15.7 | 4.25 (3.48–5.19) | 12.2 | 2.72 (1.37–5.38) | 12.9 | 2.33 (1.27–4.27) |
| Chronic disease | ||||||||
| None | 3.6 | 1 | 3.4 | 1 | 3.4 | 1 | 3.2 | 1 |
| One | 4.7 | 1.00 (0.75–1.33) | 4.4 | 1.08 (0.82–1.44) | 5.4 | 1.26 (0.56–2.84) | 7.4 | 1.89 (0.87–4.07) |
| Two | 5.9 | 1.10 (0.81–1.49) | 5.4 | 1.09 (0.81–1.48) | 6.7 | 1.23 (0.50–3.03) | 6.8 | 1.58 (0.64–3.88) |
| Three or more | 9.8 | 1.14 (0.87–1.50) | 10.1 | 1.41 (1.08–1.84) | 10.4 | 1.66 (0.65–4.25) | 11.4 | 2.03 (0.96–4.28) |
| Injury | ||||||||
| No | 5.5 | 1 | 4.9 | 1 | 5.6 | 1 | 5.0 | 1 |
| Yes | 11.8 | 1.60 (1.31–1.96) | 12.8 | 2.21 (1.76–2.76) | 9.9 | 1.64 (0.71–3.80) | 16.7 | 2.84 (1.50–5.37) |
| Autochthons | Immigrants | |||||||
|---|---|---|---|---|---|---|---|---|
| 2006 | 2012 | 2006 | 2012 | |||||
| Prev | PR (CI 95%) | Prev | PR (CI 95%) | Prev | PR (CI 95%) | Prev | PR (CI 95%) | |
| Predisposing factors | ||||||||
| Sex | ||||||||
| Men | 27.5 | 1 | 24.3 | 1 | 31.5 | 1 | 28.4 | 1 |
| Women | 29.2 | 1.02 (0.96–1.09) | 28.1 | 1.11 (1.03–1.19) | 33.5 | 0.97 (0.79–1.19) | 32.3 | 1.06 (0.86–1.31) |
| Age | ||||||||
| 16–29 | 35.5 | 1 | 29.1 | 1 | 33.6 | 1 | 33.1 | 1 |
| 30–44 | 27.1 | 0.73 (0.67–0.79) | 27.4 | 0.85 (0.77–0.94) | 33.0 | 0.86 (0.71–1.05) | 28.9 | 0.92 (0.72–1.18) |
| 45–59 | 23.9 | 0.55 (0.51–0.60) | 22.9 | 0.59 (0.53–0.66) | 28.5 | 0.64 (0.47–0.85) | 30.0 | 0.83 (0.62–1.11) |
| Enabling factors | ||||||||
| Social class | ||||||||
| I–II (directors and managers) | 25.8 | 1 | 21.9 | 1 | 29.7 | 1 | 20.0 | 1 |
| II | 27.3 | 1.02 (0.94–1.12) | 25.1 | 1.07 (0.96–1.20) | 35.4 | 1.05 (0.69–1.57) | 30.0 | 1.46 (0.81–2.65) |
| III | 29.5 | 1.03 (0.95–1.12) | 27.7 | 1.11 (1.00–1.22) | 34.0 | 1.08 (0.78–1.50) | 30.4 | 1.48 (0.88–2.49) |
| IV (unskilled workers) | 30.7 | 1.04 (0.93–1.16) | 29.5 | 1.11 (0.98–1.25) | 29.1 | 0.93 (0.65–1.34) | 31.9 | 1.48 (0.87–2.53) |
| Private health insurance | ||||||||
| No | 28.4 | 1 | 26.1 | 1 | 32.7 | 1 | 30.3 | 1 |
| Yes | 27.9 | 1.03 (0.95–1.12) | 26.8 | 1.06 (0.97–1.16) | 34.1 | 0.91 (0.68–1.22) | 32.9 | 1.01 (0.74–1.38) |
| Employment situation | ||||||||
| Workers | 27.8 | 1 | 24.5 | 1 | 31.0 | 1 | 32.6 | 1 |
| Unemployed | 31.8 | 0.97 (0.88–1.08) | 28.8 | 1.03 (0.94–1.13) | 32.7 | 1.09 (0.82–1.45) | 23.7 | 0.75 (0.59–0.96) |
| Other a | 28.4 | 0.95 (0.88–1.03) | 28.3 | 1.01 (0.92–1.10) | 38.8 | 1.23 (0.96–1.57) | 33.6 | 1.05 (0.82–1.35) |
| Civil status | ||||||||
| Married | 25.8 | 1 | 24.8 | 1 | 33.3 | 1 | 27.8 | 1 |
| Single. separated. divorced or widowed | 31.4 | 1.03 (0.96–1.10) | 27.8 | 0.97 (0.9–1.05) | 31.7 | 0.90 (0.74–1.08) | 33.6 | 1.15 (0.94–1.40) |
| Need | ||||||||
| Self-rated health | ||||||||
| Good | 23.0 | 1 | 21.5 | 1 | 26.6 | 1 | 48.9 | 1 |
| Poor | 44.8 | 1.71 (1.6–1.83) | 46.1 | 1.89 (1.74–2.04) | 47.6 | 1.47 (1.21–1.78) | 25.2 | 1.62 (1.31–2.01) |
| Chronic disease | ||||||||
| None | 21.1 | 1 | 19.8 | 1 | 25.3 | 1 | 24.5 | 1 |
| One | 25.0 | 1.15 (1.03–1.27) | 23.9 | 1.20 (1.09–1.33) | 33.0 | 1.23 (0.95–1.58) | 33.7 | 1.27 (0.99–1.63) |
| Two | 29.8 | 1.35 (1.22–1.50) | 27.1 | 1.29 (1.15–1.45) | 25.5 | 0.95 (0.69–1.29) | 29.1 | 1.18 (0.84–1.64) |
| Three or more | 36.6 | 1.50 (1.37–1.65) | 37.5 | 1.56 (1.41–1.72) | 47.9 | 1.64 (1.29–2.08) | 44.8 | 1.33 (1.02–1.72) |
| Injury | ||||||||
| No | 22.7 | 1 | 21.5 | 1 | 27.4 | 1 | 26.5 | 1 |
| Yes | 75.6 | 2.87 (2.71–3.05) | 76.3 | 3.24 (3.03–3.46) | 78.2 | 2.84 (2.38–3.39) | 77.4 | 2.69 (2.23–3.25) |
4. Discussion and Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Instituto Nacional de Estadística. Available online: http://www.ine.es/ (accessed on 4 August 2014).
- Instituto Nacional de Estadística. Estadística del Padrón Continuo. Datos Provisionales a 1 de Enero de 2013. Available online: http://www.ine.es/prensa/np776.pdf (accessed on 4 August 2014). (In Spanish)
- Sanz, B.; Regidor, E.; Galindo, S.; Pascual, C.; Lostao, L.; Díaz, J.M.; Sánchez, E. Pattern of health services use by immigrants from different regions of the world residing in Spain. Int. J. Public Health 2011, 56, 567–576. [Google Scholar] [PubMed]
- Hernández-Quevedo, C.; Jiménez-Rubio, D. A comparison of the health status and health care utilization patterns between foreigners and the national population in Spain: New evidence from the Spanish National Health Survey. Soc. Sci. Med. 2009, 69, 370–378. [Google Scholar] [PubMed]
- Muñóz de Bustillo, R.; Antón Pérez, J.I. Use of public health services by Latin American immgrants in Spain. Salud Pública de México 2010, 52, 357–363. (In Spanish) [Google Scholar]
- Perreten, N.A.; Gutiérrez, M.R.; Maceín, J.L.C.; Rieiro, C.R.; González, S.G.; Laso, A.R. Health and its determinants in the immigrant population of the region of Madrid. Gac. Sanit. 2010, 24, 136–144. (In Spanish) [Google Scholar] [PubMed]
- Regidor, E.; Sanz, B.; Pascual, C.; Lostao, L.; Sánchez, E.; Díaz Olalla, J.M. Health services utilization by the immigrant population in Spain. Gac. Sanit. 2009, 23, 4–11. (In Spanish) [Google Scholar] [PubMed]
- Jiménez-Rubio, D.; Hernández-Quevedo, C. Inequalities in the use of health services between immigrants and the native population in Spain: what is driving the differences? Eur. J. Health Econ. 2011, 12, 17–28. [Google Scholar] [CrossRef]
- Torres-Cantero, A.M.; Miguel, A.G.; Gallardo, C.; Ippolito, S. Health care provision for illegal migrants: May health policy make a difference? Eur. J. Public Health 2007, 17, 483–485. [Google Scholar]
- Carmona, R.; Alcázar-Alcázar, R.; Sarría-Santamera, A.; Regidor, E. Use of health services for immigrants and native population: A systematic review. Revista Española de Salud Pública 2014, 88, 135–155. (In Spanish) [Google Scholar] [PubMed]
- Llop-Gironés, A.; Vargas Lorenzo, I.; Garcia-Subirats, I.; Aller Hernández, M.B.; Vázquez Navarrete, M.L. Immigrants’ access to health care in Spain: A review. Rev. Esp. Salud Pública 2014. in press (In Spanish) [Google Scholar]
- Norredam, M.; Nielsen, S.S.; Krasnik, A. Migrant’s utilization of somatic healthcare services in Europe—A systematic review. Eur. J. Public Health 2009, 20, 555–563. [Google Scholar] [PubMed]
- Rodríguez-Álvarez, E.; Lanborena-Elordui, N.; Pereda-Riguera, C.; Rodríguez-Rodríguez, A. Impact in the utilisation of the health services of socio-demographic variables, life-style and self-rated health by immigrant groups living in the Basque Country, Spain. Revista Española de Salud Pública 2005, 82, 209–220. (In Spanish) [Google Scholar]
- Berchet, C. Health care utilisation in France: An analysis of the main drivers of health care use inequalities related to migration. Revue d'Epidémiologie et de Sánte Publique 2013, 61, S69–S79. [Google Scholar] [PubMed]
- Stuckler, D.; Basu, S.; Suhrcke, M.; McKee, M. The health implications of financial crisis: A review of the evidence. Ulst. Med. J. 2009, 78, 142–145. [Google Scholar]
- Rechel, B.; Mladovsky, P.; Ingleby, D.; Mackenbach, J.P.; McKee, M. Migration and health in an increasingly diverse Europe. Lancet 2013, 381, 1235–1245. [Google Scholar] [PubMed]
- Kyriopoulos, I.I.; Zavras, D.; Skroumpelos, A.; Mylona, K.; Athanasakis, K.; Kyriopoulos, J. Barriers in access to healthcare services for chronic patients in times of austerity: An empirical approach in Greece. Int. J. Equity Health 2014, 13. [Google Scholar] [CrossRef]
- Lusardi, A.; Schneider, D.; Tufano, P. The Economic Crisis and Medical Care Usage. NBER Working Paper No. 15843. Available online: http://www.nber.org/papers/w15843 (accessed on 4 August 2014).
- European Commission. The Impact of the Financial Crisis on Unmet Needs for Healthcare. Research note July 2013. Available online: ec.europa.eu/social/BlobServlet?docId=11711&langId=en (accessed on 4 August 2014).
- Regidor, E.; Barrio, G.; Bravo, M.J.; de la Fuente, L. Has health in Spain been declining since the economic crisis? J. Epidemiol. Community Health 2014, 68, 280–282. [Google Scholar] [CrossRef]
- Cortés-Franch, I.; González López-Valcárcel, B. The economic-financial crisis and health in Spain. Evidence and viewpoints. SESPAS report 2014. Gac. Sanit. 2014, 28, 1–6. (In Spanish) [Google Scholar] [PubMed]
- Urbanos-Garrido, R.; Puig-Junoy, J. Austerity policies and changes in healthcare use patterns. SESPAS report 2014. Gac. Sanit. 2014, 28, 81–88. (In Spanish) [Google Scholar] [PubMed]
- Vázquez, M.L.; Terraza-Núñez, R.; Vargas, I.; Rodriguez, D.; Lizana, T. Health policies for migrant populations in three European countries: England; Italy and Spain. Health Policy 2011, 101, 70–78. [Google Scholar] [PubMed]
- Vázquez, M.L.; Terraza-Núñez, R.; Hernández, S.; Vargas, I.; Bosch, L.; González, A.; Pequeño, S.; Cantos, R.; Martínez, J.I.; López, L.A. Are migrants health policies aimed at improving access to quality healthcare? An analysis of Spanish policies. Health Policy 2013, 113, 236–246. [Google Scholar] [PubMed]
- Ministerio de Sanidad Servicios Sociales e Igualdad. Encuesta Nacional de Salud 2011–2012. Available online: https://www.msssi.gob.es/estadEstudios/estadisticas/encuestaNacional/encuesta2011.htm (accessed on 4 August 2014).
- Garcia-Subirats, I.; Vargas, I.; Vázquez, M.L. Acceso y utilización de los servicios de salud. In Estado de Salud, Determinantes y Uso de Servicios de la Población Inmigrada en España. Encuestas Nacionales de Salud 2006 y 2012, 1st ed.; Malmusi, D., Gotsens, M., Eds.; Centro de Investigación Biomédica en Red de Epidemiología y Salud Pública CIBERESP: Barcelona, Spain, 2014; Volume 1, pp. 88–105. (In Spanish) [Google Scholar]
- Aday, L.A.; Andersen, R.M. A framework for the study of access to medical care. Health Serv. Res. 1974, 9, 208–220. [Google Scholar] [PubMed]
- Allin, S.; Grignon, M.; le Grand, J. Subjective unmet need and utilization of health care services in Canada: What are the equity implications? Soc. Sci. Med. 2010, 70, 465–472. [Google Scholar] [CrossRef]
- Garcia-Subirats, I.; Vargas, I.; Mogollón-Pérez, A.S.; de Paepe, P.; da Silva, M.R.F.; Unger, J.P.; Vázquez, M.L. Barriers in access to healthcare in countries with different health systems: A cross-sectional study in municipalities of central Colombia and north-eastern Brazil. Soc. Sci. Med. 2014, 106, 204–213. [Google Scholar] [PubMed]
- Minsiterio de Sanidad Servicios Sociales e Igualdad. National Health Survey 2006. Available online: http://www.msssi.gob.es/estadEstudios/estadisticas/encuestaNacional/encuesta2006.htm (accessed on 30 September 2014).
- Minsiterio de Sanidad Servicios Sociales e Igualdad. National Health Survey 2011/12. Available online: http://www.msssi.gob.es/estadEstudios/estadisticas/encuestaNacional/encuesta2011.htm (accessed on 30 September 2014).
- International Monetary Fund. Slowing Growth, Rising Risks; World Economic Outlook: Washington, DC, USA, 2011. [Google Scholar]
- Malmusi, D.; Gotsens, M.; Collazos, F.; de Sanjosé, S.; Ferrer, L.; Garcia-Subirats, I.; Hernando, C.; Qureshi, A.; Rodríguez, V.; Ronda, E.; et al. Estado de Salud, Determinantes y Uso de Servicios de la Población Inmigrada en España. Encuestas Nacionales de Salud 2006 y 2012; CIBERESP: Barcelona, Spain, 2014. (In Spanish) [Google Scholar]
- Instituto Nacional de Estadística. National Health Survey 2011–2012. Methodology; Instituto Nacional de Estadística INE; Ministerio de Sanidad Servicios Sociales e Igualdad: Madrid, Spain, 2012. [Google Scholar]
- Instituto Nacional de Estadística. National Health Survey 2006. Detailed Methodology; Instituto Nacional de Estadística INE; Ministerio de Sanidad Servicios Sociales e Igualdad: Madrid, Spain, 2007. [Google Scholar]
- Domingo-Salvany, A.; Regidor, E.; Alonso, J.; Alvarez-Dardet, C. Proposal for a social class measure. Working Group of the Spanish Society of Epidemiology and the Spanish Society of Family and Community Medicine. Atención Primaria 2000, 25, 350–363. (In Spanish) [Google Scholar] [PubMed]
- Domingo-Salvany, A.; Bacigalupe, A.; Carrasco, J.M.; Espelt, A.; Ferrando, J.; Borrell, C. Proposals for social class classification based on the Spanish national classification of occupations 2011 using neo-Weberian and neo-Marxist approaches. Gac. Sanit. 2013, 27, 263–272. (In Spanish) [Google Scholar] [PubMed]
- Eurostat. Self Reported Unmet Need for Medical Examination or Treatment, by Income Quintile. Available online: http://epp.eurostat.ec.europa.eu/tgm/table.do?tab=table&init=1&plugin=1&language=en&pcode=tsdph270 (accessed on 4 August 2014).
- Galon, T.; Briones-Vozmediano, E.; Agudelo-Suárez, A.A.; Felt, E.B.; Benavides, F.G.; Ronda, E. Understanding sickness presenteeism through the experience of immigrant workers in a context of economic crisis. Amer. J. Ind. Med. 2014, 57, 950–959. [Google Scholar] [CrossRef]
- Terraza-Núñez, R.; Toledo, D.; Vargas, I.; Vázquez, M.L. Perception of the Ecuadorian population living in Barcelona regarding access to health services. Int. J. Public Health 2010, 55, 381–390. [Google Scholar] [PubMed]
- Antón, J.I.; Muñóz de Bustillo, R. Health care utilisation and immigration in Spain. Eur. J. Health Econ. 2010, 11, 487–498. [Google Scholar] [PubMed]
- Palencia, L.; Espelt, A.; Rodriguez-Sanz, M.; Rocha, K.B.; Pasarín, M.I.; Borrell, C. Trends in social class inequalities in the use of health care services within the Spanish National Health System, 1993–2006. Eur. J. Health Econ. 2013, 14, 211–219. [Google Scholar] [PubMed]
- Borrell, C.; Fernández, E.; Schiaffino, A.; Benach, J.; Rajmil, L.; Villalbi, J.R.; Segura, A. Social class inequalities in the use of and access to health services in Catalonia, Spain: What is the influence of supplemental private health insurance? Int. J. Qual. Health Care 2001, 13, 117–125. [Google Scholar] [CrossRef]
- De Maio, F.G. Immigration as pathogenic: A systematic review of the health of immigrants to Canada. Int. J. Equity Health 2010, 9. [Google Scholar] [CrossRef]
- Torres, A.M.; Sanz, B. Health care provision for illegal immigrants: Should public health be concerned? J. Epidemiol. Community Health 2000, 54, 478–479. [Google Scholar]
- Vázquez, M.L.; Vargas, I.; Aller, M.B. The impact of the economic crisis on the health and healthcare of the immigrant population. SESPAS report 2014. Gac. Sanit. 2014, 28, 142–146. (In Spanish) [Google Scholar] [PubMed]
- Real Decreto-Ley 16/2012, de 20 de Abril, de Medidas Urgentes Para Garantizar la Sostenibilidad del Sistema Nacional de Salud y Mejorar la Calidad y Seguridad de Sus Prestaciones. Boletín Oficial del Estado, No. 98(24 April 2012). Available online: http://www.boe.es/boe/dias/2012/04/24/pdfs/BOE-A-2012-5403.pdf (accessed on 28 September 2014). (In Spanish)
- Repullo, J.R. Changes in the regulation and government of the health system. SESPAS report 2014. Gac. Sanit. 2014, 28, 62–68. (In Spanish) [Google Scholar] [PubMed]
- González-Rábago, Y.; la Parra, D.; Martín, U.; Malmusi, D. Participation and representation of the immigrant population in the Spanish National Health Survey 2011–2012. Gac. Sanit. 2014, 28, 281–286. (In Spanish) [Google Scholar] [PubMed]
- Medina, C.; Salvador, X.; Faixedas, M.T.; Gallo, P. Health services utilization patterns in Catalonia, Spain. Medicina Clínica 2011, 137, 42–48. (In Spanish) [Google Scholar] [PubMed]
© 2014 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Garcia-Subirats, I.; Vargas, I.; Sanz-Barbero, B.; Malmusi, D.; Ronda, E.; Ballesta, M.; Vázquez, M.L. Changes in Access to Health Services of the Immigrant and Native-Born Population in Spain in the Context of Economic Crisis. Int. J. Environ. Res. Public Health 2014, 11, 10182-10201. https://doi.org/10.3390/ijerph111010182
Garcia-Subirats I, Vargas I, Sanz-Barbero B, Malmusi D, Ronda E, Ballesta M, Vázquez ML. Changes in Access to Health Services of the Immigrant and Native-Born Population in Spain in the Context of Economic Crisis. International Journal of Environmental Research and Public Health. 2014; 11(10):10182-10201. https://doi.org/10.3390/ijerph111010182
Chicago/Turabian StyleGarcia-Subirats, Irene, Ingrid Vargas, Belén Sanz-Barbero, Davide Malmusi, Elena Ronda, Mónica Ballesta, and María Luisa Vázquez. 2014. "Changes in Access to Health Services of the Immigrant and Native-Born Population in Spain in the Context of Economic Crisis" International Journal of Environmental Research and Public Health 11, no. 10: 10182-10201. https://doi.org/10.3390/ijerph111010182
APA StyleGarcia-Subirats, I., Vargas, I., Sanz-Barbero, B., Malmusi, D., Ronda, E., Ballesta, M., & Vázquez, M. L. (2014). Changes in Access to Health Services of the Immigrant and Native-Born Population in Spain in the Context of Economic Crisis. International Journal of Environmental Research and Public Health, 11(10), 10182-10201. https://doi.org/10.3390/ijerph111010182




