Relationship between Retinal Vascular Caliber and Coronary Artery Disease in Patients with Non-Alcoholic Fatty Liver Disease (NAFLD)
Abstract
:1. Introduction
2. Materials and Methods
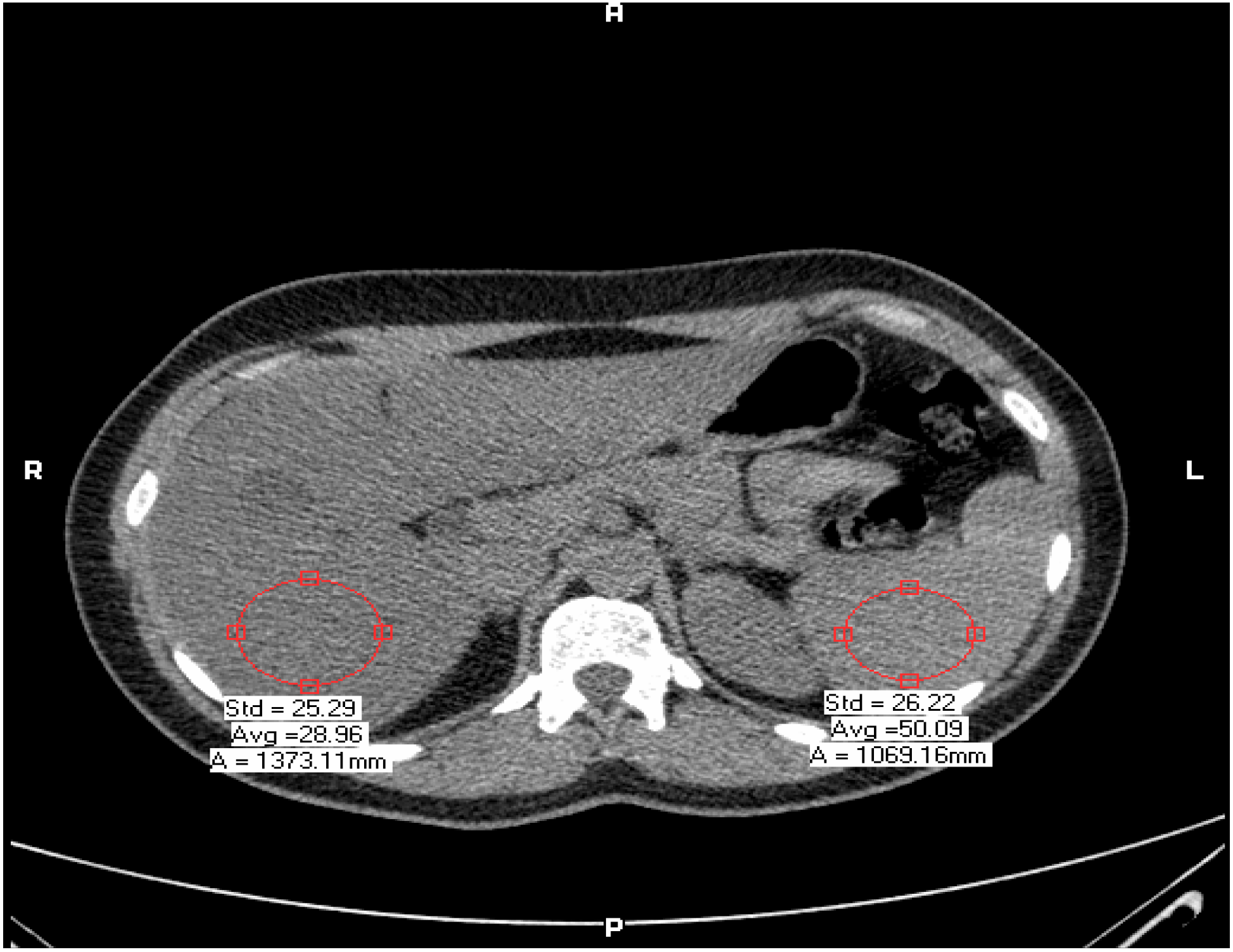
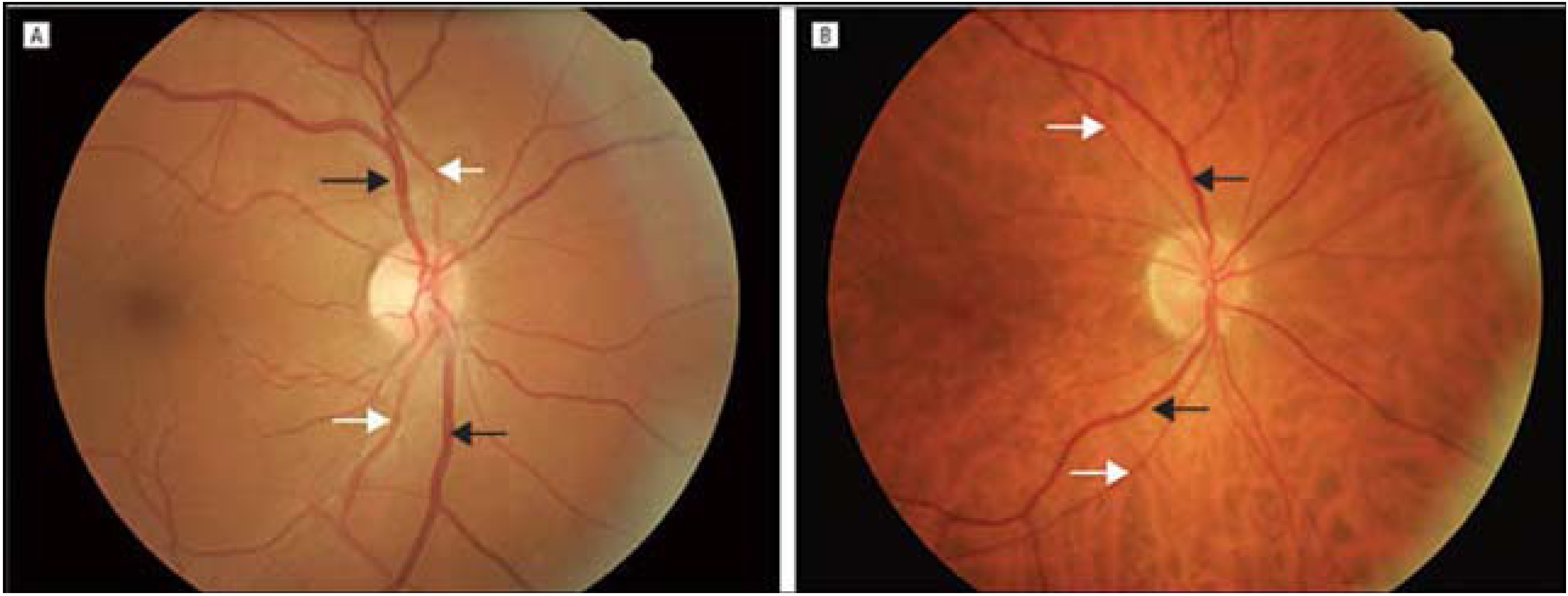
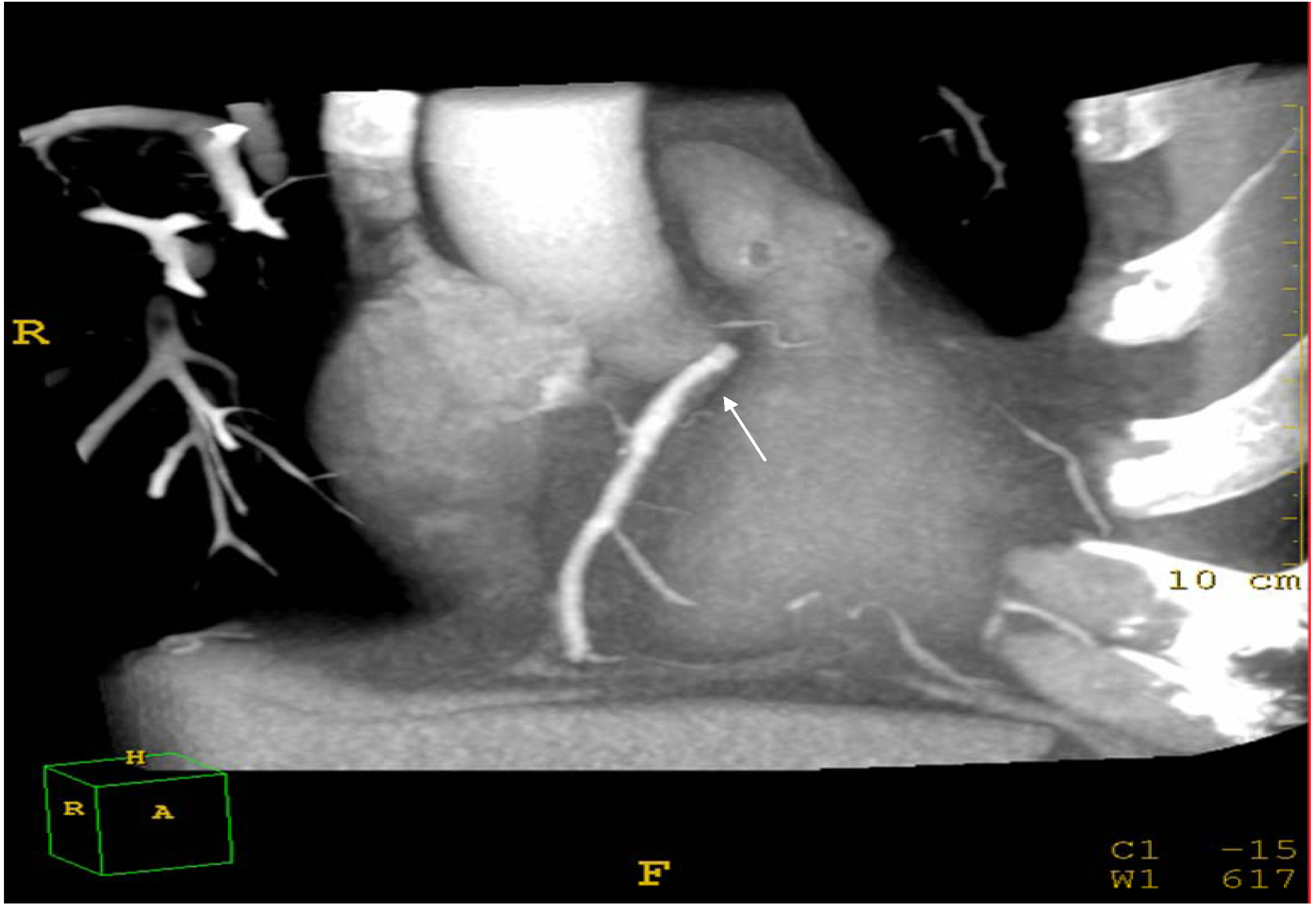
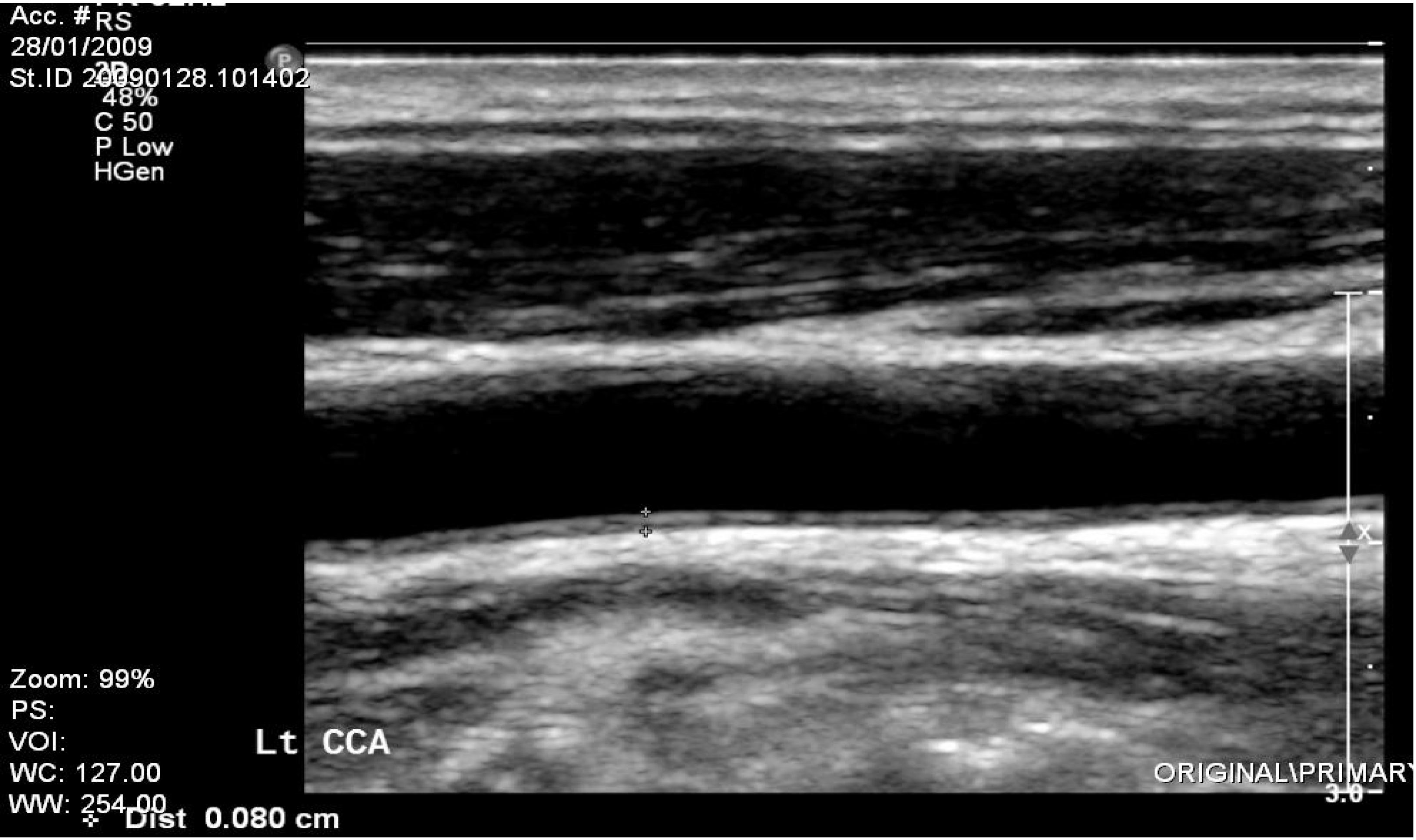
3. Statistical Analysis
4. Results
| With NAFLD N = 29 | Controls N = 22 | p value NAFLD vs. Controls | |
|---|---|---|---|
| Age (years) | 53 ± 7 | 51 ± 10 | 0.3 |
| Sex (male), n, % | 86 | 85 | 0.08 |
| BMI | 30 ± 3 | 30 ± 4 | 0.08 |
| Waist circumference (cm) | 107 ± 8 | 103 ± 11 | 0.03 |
| AST (IU/L) | 27 ± 8 | 24 ± 6 | 0.05 |
| ALT (IU/L) | 36 ± 18 | 25 ± 10 | 0.005 |
| Alk-Phos (IU/L) | 74 ± 20 | 76 ± 18 | 0.3 |
| GGT (IU/L) | 37 ± 16 | 32 ± 18 | 0.05 |
| Triglycerides (mg/dL) | 209 ± 88 | 148 ± 70 | 0.005 |
| LDL cholesterol mg/dL) | 117 ± 36 | 113 ± 33 | 0.3 |
| HDL cholesterol (mg/dL) | 43 ± 12 | 46 ± 12 | 0.2 |
| Metabolic syndrome (%) | 62 | 31 | 0.008 |
| Liver-Spleen Density (HU) | −15.3 ± 8.9 | +6.8 ± 6.7 | 0.001 |
| with NAFLD N = 29 | Controls N = 22 | p value NAFLD vs. Controls | |
|---|---|---|---|
| Coronary artery disease (stenosis > 50%) | 30% | 15% | 0.001 |
| Coronary Plaques%Soft Plaques | 70%50% | 30%30% | 0.010.01 |
| IMT, mean Right Carotis (mm) | 0.90 ± 0.19 | 0.8 ± 0.10 | 0.03 |
| Left Carotis (mm) | 0.98 ± 0.30 | 0.8 ± 0.10 | 0.27 |
| Mean Carotis Plaques% | 60% | 40% | 0.01 |
| Retinal artery diameter | 92.4 ± 13.08 | 100.56 ± 7.1 | 0.04 |
| Retinal vein diameter | 136.37 ± 14.42 | 141.5 ± 7.05 | 0.2 |
| AVR | 0.66 ± 0.06 | 0.71 ± 0.02 | 0.01 |
| CRP | 0.41 ± 0.9 | 0.30 ± 0.3 | 0.02 |
| MDA(mM) | 0.09 ± 0.05 | 0.11 ± 0.05 | 0.09 |
| Paroxonase (mM/min) | 0.55 ± 0.1 | 0.57 ± 0.1 | 0.4 |
| HOMA | 4.0 ± 3.4 | 2.0 ± 1.0 | 0.001 |
| OR * | ±95% CI | p | |
|---|---|---|---|
| Fatty Liver (L-S density < −10 HU) | 2.5 | 1–4.0 | 0.001 |
| IMT (>0.80 mm) | 2.3 | 0.9–3 | 0.001 |
| Retinal AVR (>0.7) | 1.5 | 0.5–1.5 | 0.01 |
| HOMA (>3.0) | 0.8 | 0.5–1.5 | 0.08 |
| CRP (>0.5 mg/dL) | 0.7 | 0.5–0.9 | 0.4 |
| Metabolic syndrome (present/absent) | 1.2 | 0.9–3.5 | 0.03 |
5. Discussion
6. Conclusions
Advances in Knowledge
- Carotid atherosclerosis has been documented in patients with non-alcoholic fatty liver disease; and more recently, carotid intima-media thickness has been related to the severity of liver damage.
- Retinal arteriolar abnormalities have been recognized as associating with hypertension and diabetes mellitus.
Implications
- Smaller retinal arterial caliber may indicate an increased risk of cardiovascular disease in patients with NAFLD and may allow intervention at earlier stage.
- More individuals from the general population with sub clinical coronary artery diseases will be detected at earlier stage when fatty liver and retinal vascular changes are identified.
Summary
Conflicts of Interest
References
- Angulo, P. Nonalcoholic fatty liver disease. N. Engl. J. Med. 2002, 346, 1221–1231. [Google Scholar] [CrossRef]
- Williams, C.D.; Stengel, J.; Asike, M.I.; Torres, D.M.; Shaw, J.; Contreras, M.; Landt, C.L.; Harrison, S.A. Prevalence of nonalcoholic fatty liver disease and nonalcoholic steatohepatitis among a largely middle-aged population utilizing ultrasound and liver biopsy: A prospective study. Gastroenterology 2011, 140, 124–131. [Google Scholar] [CrossRef]
- McCullough, A.J. The clinical features, diagnosis and natural history of nonalcoholic fatty liver disease. Clin. Liver Dis. 2004, 8, 521–533. [Google Scholar] [CrossRef]
- Perseghin, G.; Lattuada, G.; de Cobelli, F.; Ntali, G.; Esposito, A.; Burska, A.; Belloni, E.; Canu, T.; Ragogna, F.; Scifo, P.; et al. Serum resistin and hepatic fat content in nondiabetic individuals. J. Clin. Endocrinol. Metab. 2006, 91, 5122–5125. [Google Scholar] [CrossRef]
- Assy, N.; Bekirov, I.; Mejritsky, Y.; Solomon, L.; Szvalb, S.; Hussein, O. Association between thrombotic risk factors and extent of fibrosis in patients with non-alcoholic fatty liver diseases. World J. Gastroenterol. 2005, 11, 5834–5839. [Google Scholar]
- Ruhl, C.E.; Everhart, J.E. Determinants of the association of overweight with elevated serum alanine aminotransferase activity in the United States. Gastroenterology 2003, 124, 71–79. [Google Scholar] [CrossRef]
- Ballestri, S.; Lonardo, A.; Romagnoli, D.; Carulli, L.; Losi, L.; Day, C.P.; Loria, P. Ultrasonographic fatty liver indicator, a novel score which rules out NASH and is correlated with metabolic parameters in NAFLD. Liver Int. 2012, 32, 1242–1252. [Google Scholar] [CrossRef]
- Akahoshi, M.; Amasaki, Y.; Soda, M.; Tominaga, T.; Ichimaru, S.; Nakashima, E.; Seto, S.; Yano, K. Correlation between fatty liver and coronary risk factors: A population study of elderly men and women in Nagasaki, Japan. Hypertens. Res. 2001, 24, 337–343. [Google Scholar] [CrossRef]
- Anstee, Q.M.; Targher, G.; Day, C.P. Progression of NAFLD to diabetes mellitus, cardiovascular disease or cirrhosis. Nat. Rev. Gastroenterol. Hepatol. 2013, 10, 330–344. [Google Scholar] [CrossRef]
- Malik, S.; Wong, N.D.; Franklin, S.S.; Kamath, T.V.; L’Italien, G.J.; Pio, J.R.; Williams, G.R. Impact of the metabolic syndrome on mortality from coronary heart disease, cardiovascular disease, and all causes in United States adults. Circulation 2004, 110, 1245–1250. [Google Scholar] [CrossRef]
- Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults. Executive summary of the third report of the National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III). JAMA 2001, 285, 2486–2497.
- Hamaguchi, M.; Kojima, T.; Takeda, N.; Nagata, C.; Takeda, J.; Sarui, H.; Kawahito, Y.; Yoshida, N.; Suetsugu, A.; Kato, T.; et al. Nonalcoholic fatty liver disease is a novel predictor of cardiovascular disease. World J. Gastroenterol. 2007, 13, 1579–1584. [Google Scholar]
- Davis, M.; Thomas, A. Thrombosis and acute coronary artery lesions in sudden cardiac ischemic death. N. Engl. J. Med. 1984, 310, 1137–1140. [Google Scholar] [CrossRef]
- Fuster, V.; Badimon, L.; Badimon, J.J.; Chaesebro, J.H. The pathogenesis of coronary artery disease and the acute coronary syndrome. N. Engl. J. Med. 1992, 326, 310–318. [Google Scholar] [CrossRef]
- Theroux, P.; Fuster, V. Acute coronary syndrome: Unstable angina and non-Q-wave myocardial infarction. Circulation 1998, 97, 1195–1206. [Google Scholar] [CrossRef]
- Riouful, G.; Finet, G.; Ginon, I.; André-Fouët, X.; Rossi, R.; Vialle, E.; Desjoyaux, E.; Convert, G.; Huret, J.F.; Tabib, A. Multiple atherosclerotic plaques rupture in acute coronary syndrome. Circulation 2002, 106, 804–808. [Google Scholar] [CrossRef]
- Hong, M.K.; Mintz, G.S.; Lee, C.W.; Kim, Y.H.; Lee, S.W.; Song, J.M.; Han, K.H.; Kang, D.H.; Song, J.K.; Kim, J.J. Comparison of coronary plaque rupture between stable angina and acute myocardial infarction: A three-vessel intravascular US study in 235 patients. Circulation 2004, 110, 928–933. [Google Scholar] [CrossRef]
- Tanaka, A.; Shimada, K.; Sano, T.; Namba, M.; Sakamoto, T.; Nishida, Y.; Kawarabayashi, T.; Fukuda, D.; Yoshikawa, J. Multiple plaque rupture and C-reactive protein in acute myocardial infarction. J. Am. Coll. Cardiol. 2005, 45, 1594–1599. [Google Scholar] [CrossRef]
- Akabame, S.; Hamaguchi, M.; Tomiyasu, K.; Tanaka, M.; Kobayashi-Takenaka, Y.; Nakano, K.; Oda, Y.; Yoshikawa, T. Evaluation of vulnerable coronary plaques and non-alcoholic fatty liver disease (NAFLD) by 64-detector multislice computed tomography (MSCT). Circ. J. 2008, 72, 618–625. [Google Scholar]
- Targher, G.; Bertolini, L.; Padovani, R.; Rodella, S.; Zoppini, G.; Zenari, L.; Cigolini, M.; Falezza, G.; Arcaro, G. Relations between carotid artery wall thickness and liver histology in subjects with nonalcoholic fatty liver disease. Diabetes Care 2006, 29, 1325–1330. [Google Scholar] [CrossRef]
- Hubbard, L.D.; Brothers, R.J.; King, W.N.; Clegg, L.X.; Klein, R.; Cooper, L.S.; Sharrett, A.R.; Davis, M.D.; Cai, J. Methods for evaluation of retinal microvascular abnormalities associated with hypertension/sclerosis in the Atherosclerosis Risk in Communities (ARIC) Study. Ophthalmology 1999, 106, 2269–2280. [Google Scholar] [CrossRef]
- Miller, R.G.; Prince, C.T.; Klein, R.; Orchard, T.J. Retinal vessel diameter and the incidence of coronary artery disease in type 1 diabetes. Am. J. Ophthalmol. 2009, 147, 653–660. [Google Scholar] [CrossRef]
- Montagne, P.; Laroche, P.; Cuillière, M.L.; Varcin, P.; Pau, B.; Duheille, J. Particle-enhanced nephelometric immunoassay for human C-reactive protein. J. Clin. Lab. Anal. 1992, 6, 24–29. [Google Scholar] [CrossRef]
- Clauss, A. Gerinnungsphysiologische Schnellmethode zur Bestimmung des Fibrinogens. Rapid physiological coagulation method in determination of fibrinogen. Acta Haematol. 1957, 17, 237–246. [Google Scholar] [CrossRef]
- Gan, K.N.; Smolen, A.; Eckerson, H.W.; la Du, B.N. Purification of human serum paraoxonase/arylesterase. Evidence for one esterase catalyzing both activities. Drug Metab. Dispos. 1991, 19, 100–106. [Google Scholar]
- Baker, H.; Frank, O.; de Angelis, B.; Feingold, S. Plasma tocopherol in man at various time intervals after ingesting free or acetylated tocopherol. Nutr. Rep. Int. 1980, 21, 531–536. [Google Scholar]
- Yagi, K. Lipid peroxides and human diseases. Chem. Phys. Lipids 1987, 45, 337–351. [Google Scholar] [CrossRef]
- Limanond, P.; Raman, S.; Lassman, C. Macrovesicular hepatic steatosis in living related liver donors: Correlation between CT and histologic findings. Radiology 2004, 230, 276–280. [Google Scholar] [CrossRef]
- Schroeder, S.; Kopp, A.F.; Baumbach, A.; Meisner, C.; Kuettner, A.; Georg, C.; Ohnesorge, B.; Herdeg, C.; Claussen, C.D.; Karsch, K.R. Noninvasive detection and evaluation of atherosclerotic coronary plaques with multislice computed tomography. J. Am. Coll. Cardiol. 2001, 37, 1430–1435. [Google Scholar] [CrossRef]
- De Groot, E.; Hovingh, G.K.; Wiegman, A.; Duriez, P.; Smit, A.J.; Fruchart, J.C.; Kastelein, J.J. Measurement of arterial wall thickness as surrogate marker for atherosclerosis. Circulation 2004, 109, III33–III38. [Google Scholar]
- Ikram, M.K.; de Jong, F.J.; Vingerling, J.R.; Witteman, J.C.; Hofman, A.; Breteler, M.M.; de Jong, P.T. Are retinal arteriolar or venular diameters associated with markers for cardiovascular disorders? The Rotterdam Study. Invest. Ophthalmol. Vis. Sci. 2004, 45, 2129–2134. [Google Scholar] [CrossRef]
- Sun, C.; Wang, J.J.; Mackey, D.A.; Wong, T.Y. Retinal vascular caliber: Systemic, environmental, and genetic associations. Surv. Ophthalmol. 2009, 54, 74–95. [Google Scholar] [CrossRef]
- Gillum, R.F. Retinal arteriolar findings and coronary heart disease. Am. Heart J. 1991, 122, 262–263. [Google Scholar] [CrossRef]
- Samuel, V.T.; Liu, Z.X.; Qu, X.; Elder, B.D.; Bilz, S.; Befroy, D.; Romanelli, A.J.; Shulman, G.I. Mechanism of hepatic insulin resistance in non-alcoholic fatty liver disease. J. Biol. Chem. 2004, 279, 32345–32353. [Google Scholar]
- Nseir, W.; Shalata, A.; Marmor, A.; Assy, N. Mechanisms linking nonalcoholic fatty liver disease with coronary artery disease. Dig. Dis. Sci. 2011, 56, 3439–3449. [Google Scholar] [CrossRef]
- Villanova, N.; Moscatiello, S.; Ramilli, S.; Bugianesi, E.; Magalotti, D.; Vanni, E.; Zoli, M.; Marchesini, G. Endothelial dysfunction and cardiovascular risk profile in nonalcoholic fatty liver disease. Hepatology 2005, 42, 473–480. [Google Scholar] [CrossRef]
- Ridker, P.M.; Danielson, E.; Fonseca, F.A.; Genest, J.; Gotto, A.M., Jr.; Kastelein, J.J.; Koenig, W.; Libby, P.; Lorenzatti, A.J.; MacFadyen, J.G.; et al. Rosuvastatin to prevent vascular events in men and women with elevated C-reactive protein. N. Engl. J. Med. 2008, 359, 2195–2207. [Google Scholar] [CrossRef]
- Kawachi, S.; Takeda, N. Circulating insulin-like growth factor-1 and insulin-like growth factor binding protein-3 are associated with early carotid atherosclerosis. Arterioscler. Thromb. Vasc. Biol. 2005, 25, 617–621. [Google Scholar] [CrossRef]
- Björntorp, P. Portal adipose tissue as a generator of risk factors for cardiovascular disease and diabetes. Arteriosclerosis 1990, 10, 493–496. [Google Scholar] [CrossRef]
- Schwimmer, J.B.; Deutsch, R.; Kahen, T.; Lavine, J.E.; Stanley, C.; Behling, C. Prevalence of fatty liver in children and adolescents. Pediatrics 2006, 118, 1388–1393. [Google Scholar] [CrossRef]
- Licata, G.; Argano, C.; di Chiara, T.; Parrinello, G.; Scaglione, R. Obesity: A main factor of metabolic syndrome? Panminerva Med. 2006, 48, 77–85. [Google Scholar]
- Pundziute, G.; Schuijf, J.D.; Jukema, J.W.; Boersma, E.; de Roos, A.; van der Wall, E.E.; Bax, J.J. Prognostic value of multislice computed tomography coronary angiography in patients with known or suspected coronary artery disease. J. Am. Coll. Cardiol. 2007, 49, 62–70. [Google Scholar] [CrossRef]
- Girould, D.; Li, J.M.; Urban, B.; Rutishhauer, W. Relation of the site of acute myocardial infarction to the most severe coronary arterial stenosis at prior angiography. Am. J. Cardiol. 1992, 69, 729–732. [Google Scholar] [CrossRef]
- Adelman, E.L.; Corly, S.D.; Fisher, L.D.; Chaitman, B.R.; Faxon, D.P.; Foster, E.D.; Killip, T.; Sosa, J.A.; Bourassa, M.G. Five-year angiographic follow up of factors associated with progression of coronary artery disease in the coronary artery surgery study (CASS). CASS participating investigators and staff. J. Am. Coll. Cardiol. 1993, 22, 1141–1154. [Google Scholar]
- Grundy, S.M.; Cleeman, J.I.; Merz, C.N.; Brewer, H.B., Jr.; Clark, L.T.; Hunninghake, D.B.; Pasternak, R.C.; Smith, S.C., Jr.; Stone, N.J.; National Heart, Lung, and Blood Institute; et al. Implication of recent clinical trials for the National cholesterol education program adult treatment panel III guidelines. Circulation 2004, 110, 227–239. [Google Scholar] [CrossRef]
- Smith, S.C., Jr.; Allen, J.; Blair, S.N.; Bonow, R.O.; Brass, L.M.; Fonarow, G.C.; Grundy, S.M.; Hiratzka, L.; Jones, D.; Krumholz, H.M.; et al. AHA/ACC guidelines for secondary prevention for patients with coronary and other atherosclerotic vascular disease: 2006 Update: Endorsed by the National Heart, Lung, and Blood Institute. Circulation 2006, 113, 2363–2372. [Google Scholar] [CrossRef]
- Targher, G.; Bertolini, L.; Poli, F.; Rodella, S.; Scala, L.; Tessari, R.; Zenari, L.; Falezza, G. Nonalcoholic fatty liver disease and risk of future cardiovascular events among type 2 diabetic patients. Diabetes 2005, 54, 3541–3546. [Google Scholar] [CrossRef]
- Fracanzani, A.L.; Burdick, L.; Raselli, S.; Pedotti, P.; Grigore, L.; Santorelli, G.; Valenti, L.; Maraschi, A.; Catapano, A.; Fargion, S. Carotid artery intima-media thickness in nonalcoholic fatty liver disease. Am. J. Med. 2008, 121, 72–78. [Google Scholar] [CrossRef]
- Klein, R.; Sharrett, A.R.; Klein, B.E.; Chambless, L.E.; Cooper, L.S.; Hubbard, L.D.; Evans, G. Are retinal arteriolar abnormalities related to atherosclerosis? The atherosclerosis risk in communities study. Arterioscler. Thromb. Vasc. Biol. 2000, 20, 1644–1650. [Google Scholar] [CrossRef]
- Mitsutake, R.; Niimura, H.; Miura, S.; Zhang, B.; Iwata, A.; Nishikawa, H.; Kawamura, A.; Kumagai, K.; Shirai, K.; Matsunaga, A.; Saku, K. Clinical significance of the coronary calcification score by multidetector row computed tomography for the evaluation of coronary stenosis in Japanese patients. Circ. J. 2006, 70, 1122–1127. [Google Scholar] [CrossRef]
- Walsh, J.B. Hypertensive retinopathy. Description, classification, and prognosis. Ophthalmology 1982, 89, 1127–1131. [Google Scholar]
- Ross, R. Atherosclerosis—An inflammatory disease. N. Engl. J. Med. 1999, 340, 115–126. [Google Scholar] [CrossRef]
- Tabatabaee, A.; Asharin, M.R.; Dehghan, M.H.; Pourbehi, M.R.; Nasiri-Ahmadabadi, M.; Assadi, M. Retinal vessel abnormalities predict coronary artery diseases. Perfusion 2013, 28, 232–237. [Google Scholar] [CrossRef]
- Feitosa, M.F.; Reiner, A.P.; Wojczynski, M.K.; Graff, M.; North, K.E.; Carr, J.J.; Borecki, I.B. Sex-influenced association of nonalcoholic fatty liver disease with coronary heart disease. Atherosclerosis 2013, 227, 420–424. [Google Scholar] [CrossRef]
- Lonardo, A.; Sookoian, S.; Chonchol, M.; Loria, P.; Targher, G. Cardiovascular and systemic risk in nonalcoholic fatty liver disease—Atherosclerosis as a major player in the natural course of NAFLD. Curr. Pharm. Des. 2013, 19, 5177–5192. [Google Scholar] [CrossRef]
- Ballestri, S.; Meschiari, E.; Baldelli, E.; Musumeci, F.E.; Romagnoli, D.; Trenti, T.; Zennaro, R.G.; Lonardo, A.; Loria, P. Relationship of serum fetuin—A levels with coronary atherosclerotic burden and NAFLD in Patients undergoing elective coronary angiography. Metab. Syndr. Relat. Disord. 2013, 11, 189–295. [Google Scholar] [CrossRef]
© 2013 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Josef, P.; Ali, I.; Ariel, P.; Alon, M.; Nimer, A. Relationship between Retinal Vascular Caliber and Coronary Artery Disease in Patients with Non-Alcoholic Fatty Liver Disease (NAFLD). Int. J. Environ. Res. Public Health 2013, 10, 3409-3423. https://doi.org/10.3390/ijerph10083409
Josef P, Ali I, Ariel P, Alon M, Nimer A. Relationship between Retinal Vascular Caliber and Coronary Artery Disease in Patients with Non-Alcoholic Fatty Liver Disease (NAFLD). International Journal of Environmental Research and Public Health. 2013; 10(8):3409-3423. https://doi.org/10.3390/ijerph10083409
Chicago/Turabian StyleJosef, Pikkel, Ibrahim Ali, Prober Ariel, Marmor Alon, and Assy Nimer. 2013. "Relationship between Retinal Vascular Caliber and Coronary Artery Disease in Patients with Non-Alcoholic Fatty Liver Disease (NAFLD)" International Journal of Environmental Research and Public Health 10, no. 8: 3409-3423. https://doi.org/10.3390/ijerph10083409
APA StyleJosef, P., Ali, I., Ariel, P., Alon, M., & Nimer, A. (2013). Relationship between Retinal Vascular Caliber and Coronary Artery Disease in Patients with Non-Alcoholic Fatty Liver Disease (NAFLD). International Journal of Environmental Research and Public Health, 10(8), 3409-3423. https://doi.org/10.3390/ijerph10083409




