Design and Implementation of a Smart Insole System to Measure Plantar Pressure and Temperature
Abstract
1. Introduction
- ✓ Investigation of the different off-the-shelf sensors for smart foot sole design.
- ✓ Detailed characterization procedure for each sensor.
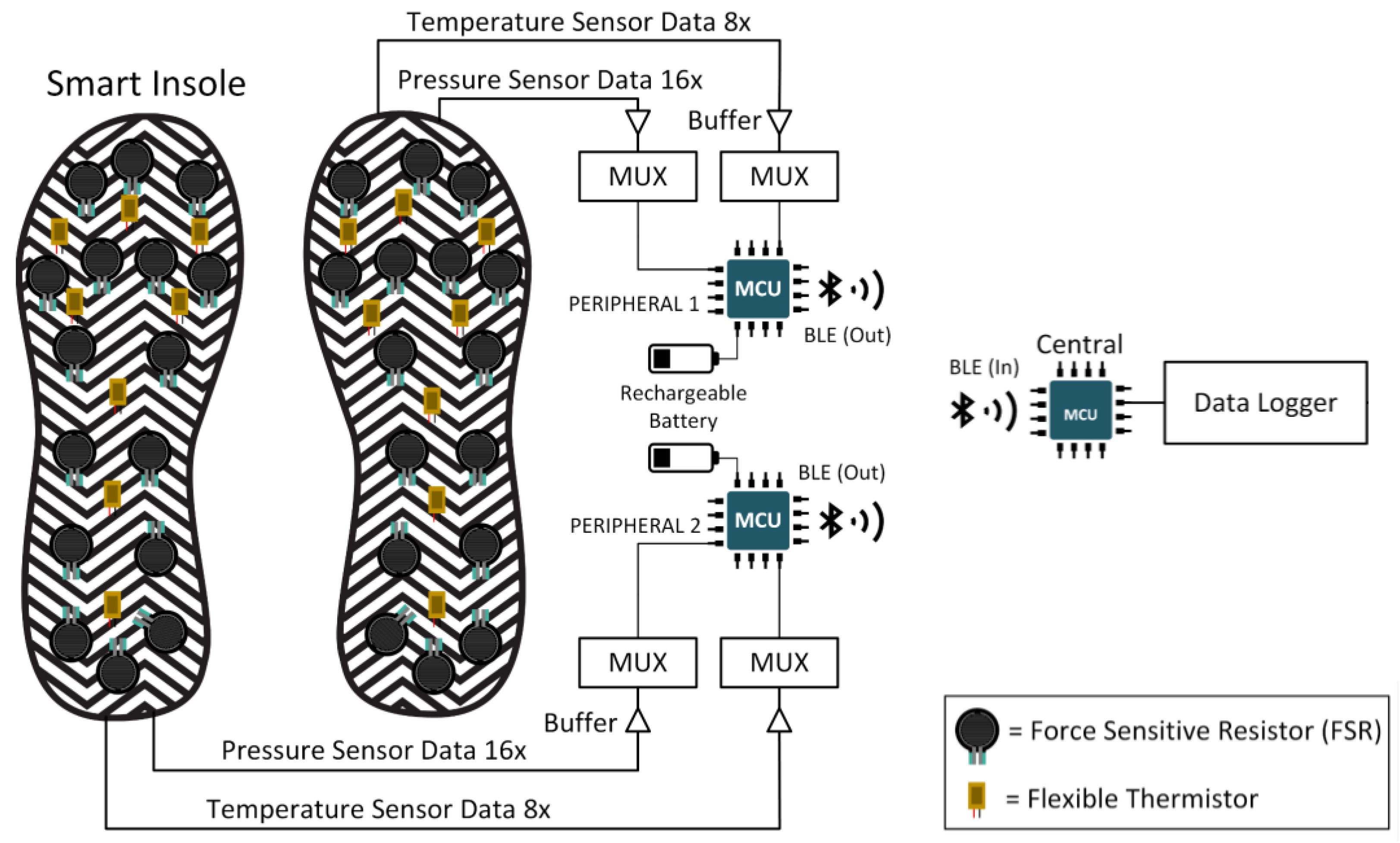
- ✓ A proposed complete framework for smart foot sole design (starting from sensor selection, characterization, multiplexing the different sensors, communication and data logging). Such a framework can be used for more studies in this domain.
- ✓ Provides comparative solution to overcome the limitations present in the electronic design of such solution.
- ✓ An insole for gathering both pressure and temperature data from the foot and generate plantar temperature and pressure maps.
2. Methodology and Experimental Details
2.1. Pressure Measuring Sensors
2.1.1. Velostat Characterization
2.1.2. FSR Characterization
2.1.3. Piezoelectric Characterization
2.2. Temperature Measuring Sensors
2.3. Communication Protocol
2.4. Microcontroller
2.5. Power Supply Unit
2.6. Multiplexing and Data Logging Unit
2.7. Design and Printing a 3D Box
3. Calibration of Pressure and Temperature Sensors
3.1. Calibration of Pressure Sensor
3.2. Calibration of Temperature Sensor
4. Sensor Selection, Characteristics, Insole Fabrication and Plantar Pressure and Temperature
4.1. Pressure Sensors Selection
4.1.1. Velostat Characterization
4.1.2. FSR Characterization
4.1.3. Piezoelectric Characterization
4.2. Temperature Sensors
4.3. Complete Foot Insole
4.4. Plantar Pressure and Temperature
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Chowdhury, M.E.; Khandakar, A.; Qiblawey, Y.; Reaz, M.B.I.; Islam, M.T.; Touati, F. Machine learning in wearable biomedical systems. In Sports Science and Human Health-Different Approaches; IntechOpen: London, UK, 2020. [Google Scholar]
- Khandakar, A.; Chowdhury, M.E.; Reaz, M.B.I.; Ali, S.H.M.; Hasan, M.A.; Kiranyaz, S.; Rahman, T.; Alfkey, R.; Bakar, A.A.A.; Malik, R.A. A machine learning model for early detection of diabetic foot using thermogram images. Comput. Biol. Med. 2021, 137, 104838. [Google Scholar] [CrossRef]
- Rahman, T.; Al-Ishaq, F.A.; Al-Mohannadi, F.S.; Mubarak, R.S.; Al-Hitmi, M.H.; Islam, K.R.; Khandakar, A.; Hssain, A.A.; Al-Madeed, S.; Zughaier, S.M. Mortality Prediction Utilizing Blood Biomarkers to Predict the Severity of COVID-19 Using Machine Learning Technique. Diagnostics 2021, 11, 1582. [Google Scholar] [CrossRef]
- Al Omar, A.; Jamil, A.K.; Khandakar, A.; Uzzal, A.R.; Bosri, R.; Mansoor, N.; Rahman, M.S. A Transparent and Privacy-Preserving Healthcare Platform with Novel Smart Contract for Smart Cities. IEEE Access 2021, 9, 90738–90749. [Google Scholar] [CrossRef]
- Tavares, C.; Leite, F.; Domingues, M.D.F.; Paixão, T.; Alberto, N.; Ramos, A.; Silva, H.; Antunes, P.F.D.C. Optically Instrumented Insole for Gait Plantar and Shear Force Monitoring. IEEE Access 2021, 9, 132480–132490. [Google Scholar] [CrossRef]
- Bus, S.; Van Netten, S.; Lavery, L.; Monteiro-Soares, M.; Rasmussen, A.; Jubiz, Y.; Price, P. IWGDF guidance on the prevention of foot ulcers in at-risk patients with diabetes. Diabetes/Metab. Res. Rev. 2016, 32, 16–24. [Google Scholar] [CrossRef]
- Reyzelman, A.M.; Koelewyn, K.; Murphy, M.; Shen, X.; Yu, E.; Pillai, R.; Fu, J.; Scholten, H.J.; Ma, R. Continuous temperature-monitoring socks for home use in patients with diabetes: Observational study. J. Med. Internet Res. 2018, 20, e12460. [Google Scholar] [CrossRef]
- Frykberg, R.G.; Gordon, I.L.; Reyzelman, A.M.; Cazzell, S.M.; Fitzgerald, R.H.; Rothenberg, G.M.; Bloom, J.D.; Petersen, B.J.; Linders, D.R.; Nouvong, A. Feasibility and efficacy of a smart mat technology to predict development of diabetic plantar ulcers. Diabetes Care 2017, 40, 973–980. [Google Scholar] [CrossRef]
- Inagaki, N.; Fernanda, N. The impact of diabetic foot problems on health-related quality of life of people with diabetes. Master’s Thesis, University of Alberta, Edmonton, AB, Canada, 2017. [Google Scholar] [CrossRef]
- Crisologo, P.A.; Lavery, L.A. Remote home monitoring to identify and prevent diabetic foot ulceration. Ann. Transl. Med. 2017, 5, 430. [Google Scholar] [CrossRef]
- El-Nahas, M.; El-Shazly, S.; El-Gamel, F.; Motawea, M.; Kyrillos, F.; Idrees, H. Relationship between skin temperature monitoring with Smart Socks and plantar pressure distribution: A pilot study. J. Wound Care 2018, 27, 536–541. [Google Scholar] [CrossRef]
- Deschamps, K.; Matricali, G.A.; Roosen, P.; Desloovere, K.; Bruyninckx, H.; Spaepen, P.; Nobels, F.; Tits, J.; Flour, M.; Staes, F. Classification of forefoot plantar pressure distribution in persons with diabetes: A novel perspective for the mechanical management of diabetic foot? PLoS ONE 2013, 8, e79924. [Google Scholar] [CrossRef] [PubMed]
- Albers, J.W.; Jacobson, R. Decompression nerve surgery for diabetic neuropathy: A structured review of published clinical trials. Diabetes Metab. Syndr. Obes. Targets Ther. 2018, 11, 493. [Google Scholar] [CrossRef]
- Silva, N.C.; Castro, H.A.; Carvalho, L.C.; Chaves, É.C.; Ruela, L.O.; Iunes, D.H. Reliability of infrared thermography images in the analysis of the plantar surface temperature in diabetes mellitus. J. Chiropr. Med. 2018, 17, 30–35. [Google Scholar] [CrossRef] [PubMed]
- Lahiri, B.; Bagavathiappan, S.; Raj, B.; Philip, J. Infrared thermography for detection of diabetic neuropathy and vascular disorder. In Application of Infrared to Biomedical Sciences; Springer: Berlin/Heidelberg, Germany, 2017; pp. 217–247. [Google Scholar]
- Schneider, W.L.; Severn, M. Prevention of plantar ulcers in people with diabetic peripheral neuropathy using pressure-sensing shoe insoles. In CADTH Issues in Emerging Health Technologies; Canadian Agency for Drugs and Technologies in Health: Ottawa, ON, Canada, 2018; PMID: 29369574. [Google Scholar]
- Najafi, B.; Mohseni, H.; Grewal, G.S.; Talal, T.K.; Menzies, R.A.; Armstrong, D.G. An optical-fiber-based smart textile (smart socks) to manage biomechanical risk factors associated with diabetic foot amputation. J. Diabetes Sci. Technol. 2017, 11, 668–677. [Google Scholar] [CrossRef] [PubMed]
- Oks, A.; Katashev, A.; Zadinans, M.; Rancans, M.; Litvak, J. Development of smart sock system for gate analysis and foot pressure control. In Proceedings of the XIV Mediterranean Conference on Medical and Biological Engineering and Computing, Paphos, Cyprus, 31 March–2 April 2016; pp. 472–475. [Google Scholar]
- Tahir, A.M.; Chowdhury, M.E.; Khandakar, A.; Al-Hamouz, S.; Abdalla, M.; Awadallah, S.; Reaz, M.B.I.; Al-Emadi, N. A systematic approach to the design and characterization of a smart insole for detecting vertical ground reaction force (vGRF) in gait analysis. Sensors 2020, 20, 957. [Google Scholar] [CrossRef] [PubMed]
- Abdul Razak, A.H.; Zayegh, A.; Begg, R.K.; Wahab, Y. Foot plantar pressure measurement system: A review. Sensors 2012, 12, 9884–9912. [Google Scholar] [CrossRef] [PubMed]
- Reddy, P.N.; Cooper, G.; Weightman, A.; Hodson-Tole, E.; Reeves, N.D. Walking cadence affects rate of plantar foot temperature change but not final temperature in younger and older adults. Gait Posture 2017, 52, 272–279. [Google Scholar] [CrossRef] [PubMed]
- Beach, C.; Cooper, G.; Weightman, A.; Hodson-Tole, E.F.; Reeves, N.D.; Casson, A.J. Monitoring of dynamic plantar foot temperatures in diabetes with personalised 3d-printed wearables. Sensors 2021, 21, 1717. [Google Scholar] [CrossRef]
- Wang, L.; Jones, D.; Jones, A.; Chapman, G.J.; Siddle, H.J.; Russell, D.; Alazmani, A.; Culmer, P.R. A Portable Insole System to Simultaneously Measure Plantar Pressure and Shear Stress. IEEE Sens. J. 2022, 22, 9104–9113. [Google Scholar] [CrossRef]
- Chatwin, K.E.; Abbott, C.A.; Rajbhandari, S.M.; Reddy, P.N.; Bowling, F.L.; Boulton, A.J.; Reeves, N.D. An intelligent insole system with personalised digital feedback reduces foot pressures during daily life: An 18-month randomised controlled trial. Diabetes Res. Clin. Pract. 2021, 181, 109091. [Google Scholar] [CrossRef] [PubMed]
- Amanda Killeen, D.; Neff, N.; Petersen, B.; Bloom, J.; Walters, J. Remote Temperature Monitoring to Prompt Timely Preventative Debridement a Case Series of Two Patients. Available online: https://www.podimetrics.com/static/Killeen-Preventative-Debridement.pdf (accessed on 5 March 2022).
- Anzai, E.; Tripette, J.; Nakajima, K.; Ohta, Y. Comparative study between a novel 7-sensor plantar pressure measurement insole and the F-scan device. In Proceedings of the 2020 IEEE 2nd Global Conference on Life Sciences and Technologies (LifeTech), Kyoto, Japan, 10–12 March 2020; pp. 339–342. [Google Scholar]
- Khandakar, A.; Chowdhury, M.E.; Reaz, M.B.I.; Ali, S.H.M.; Kiranyaz, S.; Rahman, T.; Chowdhury, M.H.; Ayari, M.A.; Alfkey, R.; Bakar, A.A.A. A Novel Machine Learning Approach for Severity Classification of Diabetic Foot Complications Using Thermogram Images. Sensors 2022, 22, 4249. [Google Scholar] [CrossRef] [PubMed]
- Khandakar, A.; Chowdhury, M.E.; Reaz, M.B.I.; Ali, S.H.M.; Abbas, T.O.; Alam, T.; Ayari, M.A.; Mahbub, Z.B.; Habib, R.; Rahman, T. Thermal change index-based diabetic foot thermogram image classification using machine learning techniques. Sensors 2022, 22, 1793. [Google Scholar] [CrossRef] [PubMed]
- Niemann, U.; Spiliopoulou, M.; Szczepanski, T.; Samland, F.; Grützner, J.; Senk, D.; Ming, A.; Kellersmann, J.; Malanowski, J.; Klose, S. Comparative clustering of plantar pressure distributions in diabetics with polyneuropathy may be applied to reveal inappropriate biomechanical stress. PLoS ONE 2016, 11, e0161326. [Google Scholar] [CrossRef] [PubMed]
- Van Netten, J.J.; Van Baal, J.G.; Liu, C.; Van Der Heijden, F.; Bus, S.A. Infrared Thermal Imaging for Automated Detection of Diabetic Foot Complications; SAGE Publications Sage CA: Los Angeles, CA, USA, 2013. [Google Scholar]
- Available online: https://www.littelfuse.com/~/media/electronics/datasheets/thermistor_probes_and_assemblies/littelfuse_thermistor_probes_assemblies_special_usp16673_datasheet.pdf (accessed on 1 January 2020).
- Thermal-Ribbon Flexible RTD and Thermocouple Temperature Sensors. Available online: https://www.mod-tronic.com/Rewind_Sensors/Minco_Thermal-Ribbon_Flexible_Sensors.html (accessed on 1 February 2021).
- ESPRESSIF. Available online: https://www.espressif.com/ (accessed on 1 January 2020).
- Adafruit. Available online: https://www.adafruit.com/product/2821 (accessed on 1 January 2020).
- NORDIC SEMICONDUCTOR. Available online: https://www.nordicsemi.com/ (accessed on 1 January 2021).
- Arduino Nano BLE Sense. Available online: https://www.arduino.cc/en/Guide/NANO33BLESense (accessed on 1 January 2020).
- Sparfun. FSR Force Sensing Resistor Integration Guide and Evaluation Parts Catalog. 2022. Available online: https://www.sparkfun.com/datasheets/Sensors/Pressure/fsrguide.pdf (accessed on 10 September 2022).
- Interlink Electronics. FSR 402 Data Sheet, 1st ed.; Interlink Electronics: Camarillo, CA, USA, 2020; Available online: https://www.trossenrobotics.com/productdocs/2010-10-26-DataSheet-FSR402-Layout2.pdf (accessed on 26 January 2020).
- m. I. i. Electronics. Piezoelectric Ceramic Sensors (PIEZOTITE). 2001. Available online: https://www.farnell.com/datasheets/43406.pdf (accessed on 1 March 2001).
- Suprapto, S.; Setiawan, A.; Zakaria, H.; Adiprawita, W.; Supartono, B. Low-cost pressure sensor matrix using velostat. In Proceedings of the 2017 5th International Conference on Instrumentation, Communications, Information Technology, and Biomedical Engineering (ICICI-BME), Bandung, Indonesia, 6–7 November 2017; pp. 137–140. [Google Scholar]
- Lesson 5: Force-Sensitive Resistors. Available online: https://makeabilitylab.github.io/physcomp/arduino/force-sensitive-resistors.html (accessed on 1 March 2022).














| Force Sensitive Resistor | Piezoelectric Sensor | Velostat | F-Scan System | |
|---|---|---|---|---|
| Solution Purpose | Research | Research | Research | Commercial |
| Number of Sensing Units per Insole | 16 | 16 | 1 | 960 |
| Modularity | Highly Modular | Highly Modular | Low Modularity, requires to cut into pieces to achieve some modularity | Not Applicable |
| Cross-talk | Minimum Cross-talk due to having independent units | Minimum Cross-talk due to having independent units | Higher Cross-Talk in the Velostat sheet [41] | Minimum Cross-talk due to having independent units |
| Dynamic Response | Can provide dynamic, real-time data | Can provide dynamic, real-time data | Velostats are slower [20] | Can provide dynamic, real-time data |
| Hysteresis | Low hysteresis | Low hysteresis | High hysteresis [20], less suitable for dynamic gait cycle | Low hysteresis |
| Recording Complete Gait Cycle | Can produce full Gait Cycle in real-time | Can identify only heel strike and toe off [20] | Not dynamic enough to plot fast changing gait cycle in real-time | Can produce full Gait Cycle in real-time |
| Pressure Map Generation | Able to generate static to highly dynamic pressure maps | Cannot produce pressure map due to no static response | Able to generate static and less dynamic pressure maps [41] | Able to generate static to highly dynamic pressure maps |
| Comparative Cost (USD) | ~170 | ~30 | ~10 | 20,000+ |
| Number of Subjects | Age (Year) | Weight (kg) | Height (cm) | BMI | Genders |
|---|---|---|---|---|---|
| 12 | 20–59 | 52–125 | 153–185 | 18–36.5 | Female and Male |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Khandakar, A.; Mahmud, S.; Chowdhury, M.E.H.; Reaz, M.B.I.; Kiranyaz, S.; Mahbub, Z.B.; Ali, S.H.M.; Bakar, A.A.A.; Ayari, M.A.; Alhatou, M.; et al. Design and Implementation of a Smart Insole System to Measure Plantar Pressure and Temperature. Sensors 2022, 22, 7599. https://doi.org/10.3390/s22197599
Khandakar A, Mahmud S, Chowdhury MEH, Reaz MBI, Kiranyaz S, Mahbub ZB, Ali SHM, Bakar AAA, Ayari MA, Alhatou M, et al. Design and Implementation of a Smart Insole System to Measure Plantar Pressure and Temperature. Sensors. 2022; 22(19):7599. https://doi.org/10.3390/s22197599
Chicago/Turabian StyleKhandakar, Amith, Sakib Mahmud, Muhammad E. H. Chowdhury, Mamun Bin Ibne Reaz, Serkan Kiranyaz, Zaid Bin Mahbub, Sawal Hamid Md Ali, Ahmad Ashrif A. Bakar, Mohamed Arselene Ayari, Mohammed Alhatou, and et al. 2022. "Design and Implementation of a Smart Insole System to Measure Plantar Pressure and Temperature" Sensors 22, no. 19: 7599. https://doi.org/10.3390/s22197599
APA StyleKhandakar, A., Mahmud, S., Chowdhury, M. E. H., Reaz, M. B. I., Kiranyaz, S., Mahbub, Z. B., Ali, S. H. M., Bakar, A. A. A., Ayari, M. A., Alhatou, M., Abdul-Moniem, M., & Faisal, M. A. A. (2022). Design and Implementation of a Smart Insole System to Measure Plantar Pressure and Temperature. Sensors, 22(19), 7599. https://doi.org/10.3390/s22197599









