Sensing and Artificial Intelligent Maternal-Infant Health Care Systems: A Review
Abstract
1. Introduction
- Classification of the healthcare systems based on sensors used and ML techniques exploited.
- Each healthcare system, framework or model are reviewed in chronological order.
- Discourse on the real-world datasets and their details in terms of attributes, size, format, etc.
- Comprehensive discussion about current research issues and challenges linked with these systems.
- Explore potential future work directions for researchers in the relevant domain.
2. Rationale
3. Methods
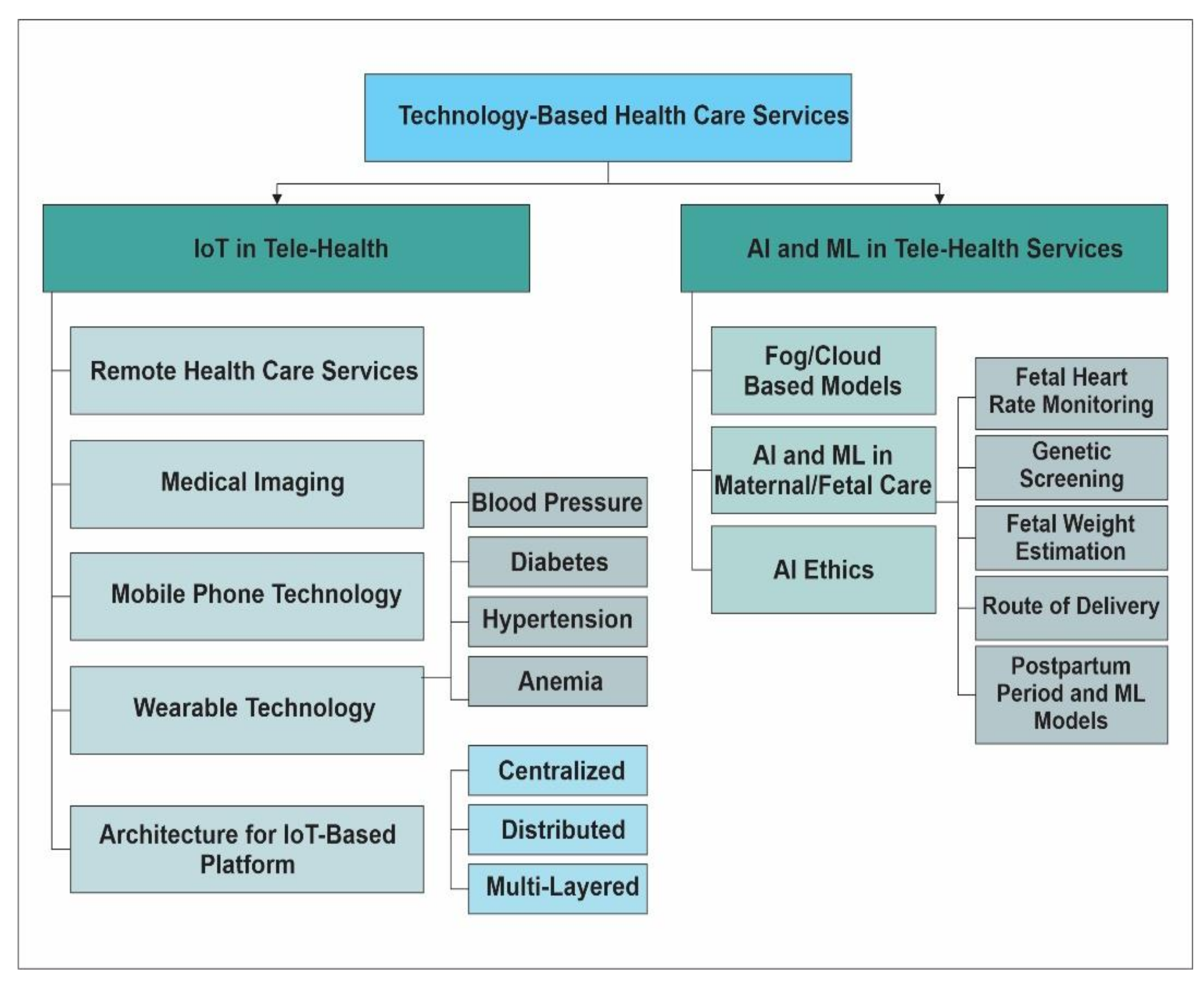
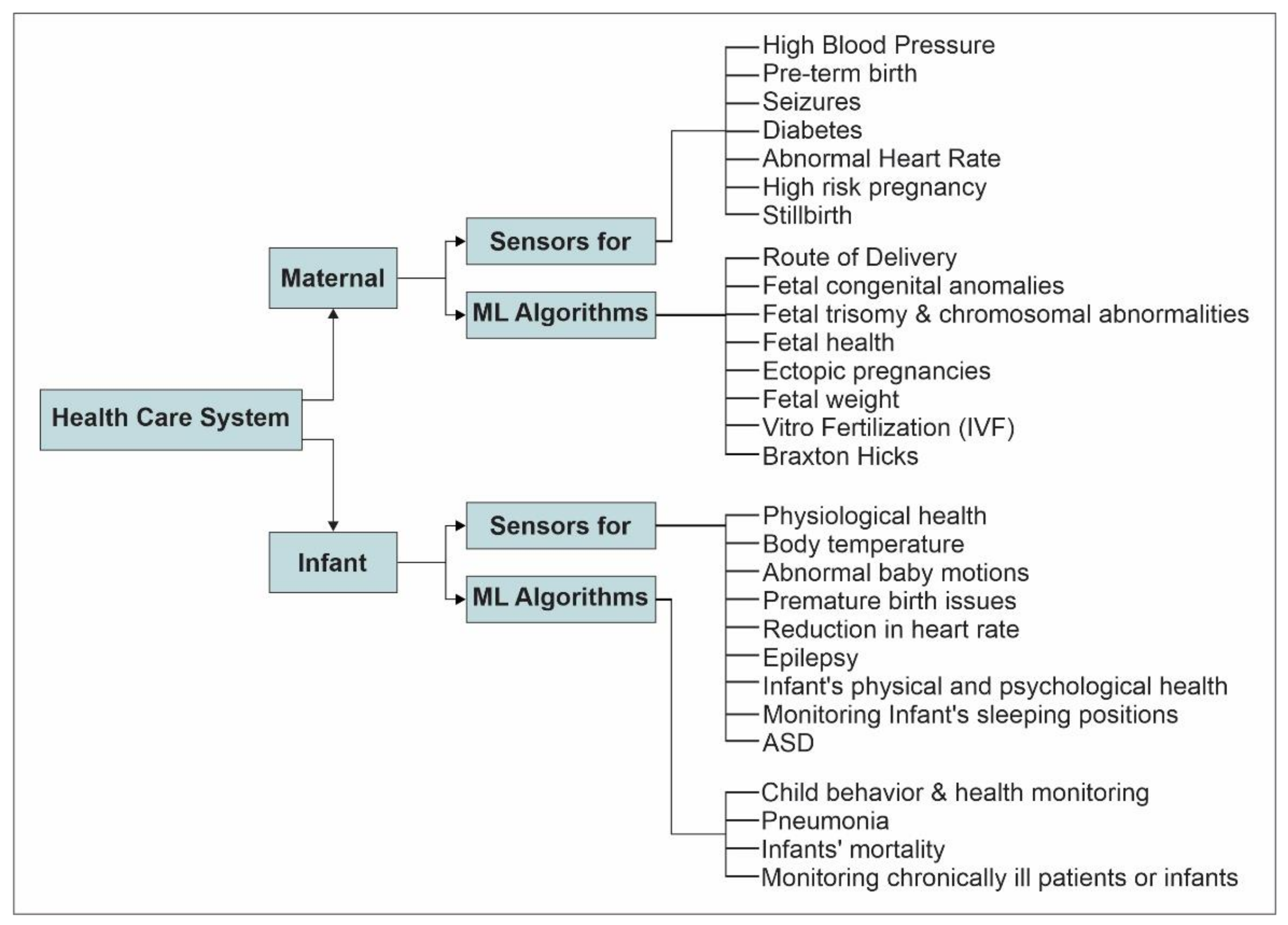
4. Sensing and AI Based Classification of Health Monitoring Systems
4.1. Sensor Used in Maternal Healthcare System
4.2. AI/ML Techniques Used in Maternal Healthcare Systems
4.3. Sensors Used in Infant Healthcare Systems
4.4. AI/ML Techniques Used in Infant Healthcare Systems
5. Datasets
6. Research Opportunities and Challenges
6.1. Application of State-of-the-Art Techniques ML/AI in Maternal and Infant Healthcare Systems
6.2. Lack of Availablity of Real-World Maternal and Infant Datasets
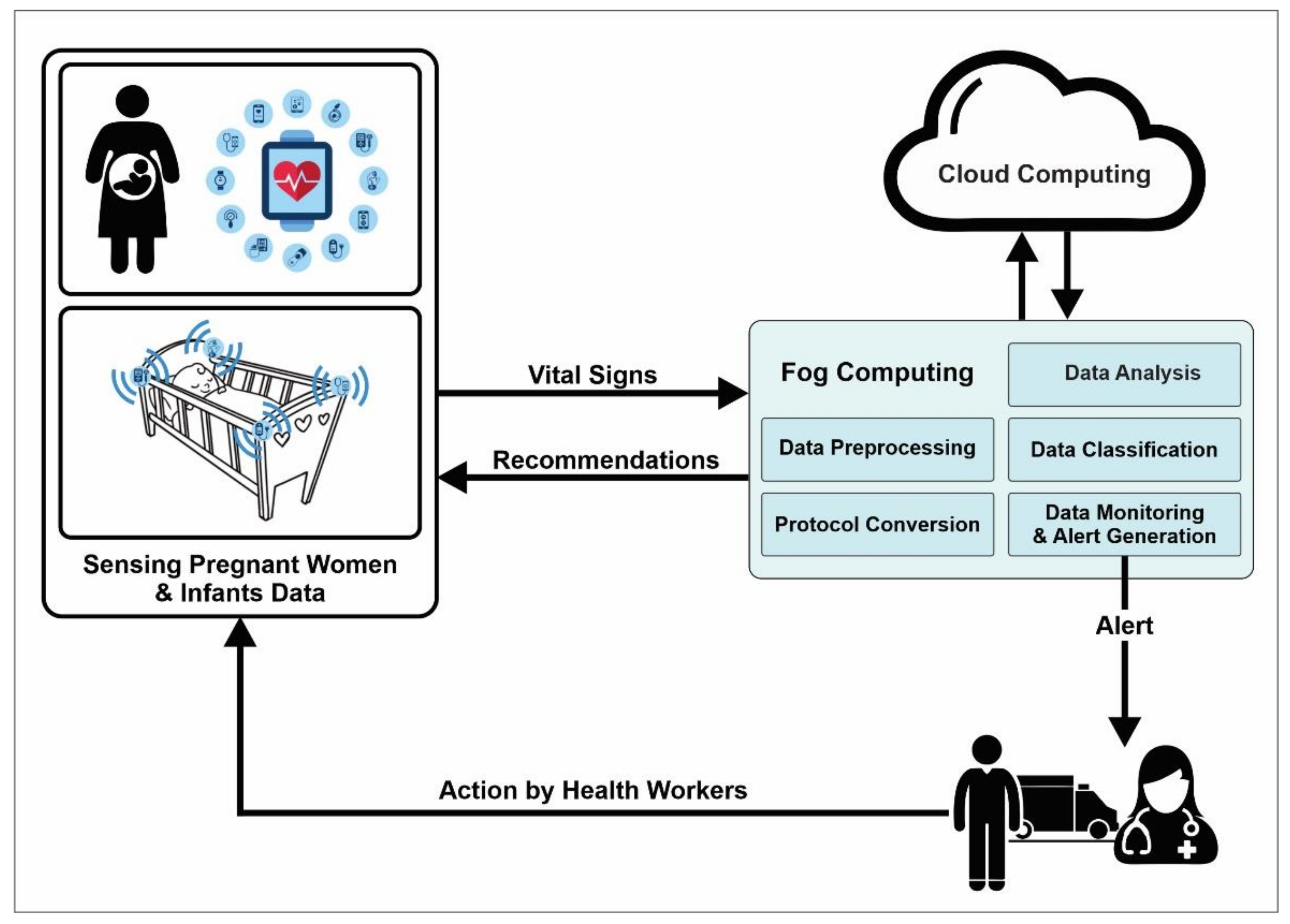
6.3. Need of Advanced Sensory and Monitory Systems Using IoT
6.4. Research Issues Raised Due to IoT-Based Systems
7. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Fernández, A.D.R.; Fernández, D.R.; Sánchez, M.T.P. A Decision Support System for Predicting the Treatment of Ectopic Pregnancies. Int. J. Med. Inform. 2019, 129, 198–204. [Google Scholar] [CrossRef] [PubMed]
- Available online: https://www.Webmd.com/Baby/Guide/Pregnancy-Miscarriage#1 (accessed on 10 March 2021).
- Murali, S.; Miller, K.; McDermott, M. Preeclampsia, Eclampsia, and Posterior Reversible Encephalopathy Syndrome. Handb. Clin. Neurol. 2020, 172, 63–77. [Google Scholar] [PubMed]
- Phipps, E.A.; Thadhani, R.; Benzing, T.; Karumanchi, S.A. Pre-Eclampsia: Pathogenesis, Novel Diagnostics and Therapies. Nat. Rev. Nephrol. 2019, 15, 275–289. [Google Scholar] [CrossRef] [PubMed]
- Saaka, M.; Hammond, A.Y. Caesarean Section Delivery and Risk of Poor Childhood Growth. J. Nutr. Metab. 2020, 2020, 6432754. [Google Scholar] [CrossRef]
- Cooper, N.; O’Brien, S.; Siassakos, D. Training Health Workers to Prevent and Manage Post-Partum Haemorrhage (PPH). Best Pract. Res. Clin. Obstet. Gynaecol. 2019, 61, 121–129. [Google Scholar] [CrossRef]
- Patrick, H.S.; Mitra, A.; Rosen, T.; Ananth, C.V.; Schuster, M. Pharmacologic Intervention for the Management of Retained Placenta: A Systematic Review and Meta-Analysis of Randomized Trials. Am. J. Obstet. Gynecol. 2020, 223, 447.e1–447.e19. [Google Scholar] [CrossRef]
- Yockey, L.J.; Varela, L.; Rakib, T.; Khoury-Hanold, W.; Fink, S.L.; Stutz, B.; Szigeti-Buck, K.; Van den Pol, A.; Lindenbach, B.D.; Horvath, T.L. Vaginal Exposure to Zika Virus during Pregnancy Leads to Fetal Brain Infection. Cell 2016, 166, 1247–1256. [Google Scholar] [CrossRef]
- Polivka, B.J.; Nickel, J.T.; Wilkins III, J.R. Urinary Tract Infection during Pregnancy: A Risk Factor for Cerebral Palsy? J. Obstet. Gynecol. Neonatal Nurs. 1997, 26, 405–413. [Google Scholar] [CrossRef]
- Runkle, J.; Sugg, M.; Boase, D.; Galvin, S.L.; Coulson, C.C. Use of Wearable Sensors for Pregnancy Health and Environmental Monitoring: Descriptive Findings from the Perspective of Patients and Providers. Digit. Health 2019, 5, 2055207619828220. [Google Scholar] [CrossRef]
- Available online: https://www.bmv.cc/En/Bpu60?Gclid=CjwKCAiAz4b_BRBbEiwA5XlVVu72rOVq8TdT1LnA1f6YQv4o0MXRM2I26dcMG3bfb4L-MdWuZN_7mRoC990QAvD_BwE (accessed on 12 March 2021).
- Available online: https://www.Indiamart.com/Proddetail/Cbc-Blood-Test-Machine-19979334512.Html (accessed on 13 March 2021).
- Adank, M.C.; Benschop, L.; Peterbroers, K.R.; Gregoor, A.M.S.; Kors, A.W.; Mulder, M.T.; Schalekamp-Timmermans, S.; Van Lennep, J.E.R.; Steegers, E.A. Is Maternal Lipid Profile in Early Pregnancy Associated with Pregnancy Complications and Blood Pressure in Pregnancy and Long Term Postpartum? Am. J. Obstet. Gynecol. 2019, 221, 150.e1–150.e13. [Google Scholar] [CrossRef]
- Available online: https://Dir.Indiamart.com/Impcat/Cardiotocography-Machine.Html (accessed on 28 February 2021).
- Moreira, M.W.; Rodrigues, J.J.; Oliveira, A.M.; Saleem, K. Smart Mobile System for Pregnancy Care Using Body Sensors. In Proceedings of the 2016 International Conference on Selected Topics in Mobile & Wireless Networking (MoWNeT), Cairo, Egypt, 11–13 April 2016; IEEE: Manhattan, NY, USA, 2016; pp. 1–4. [Google Scholar]
- Peng, C.; Chen, M.; Sim, H.K.; Zhu, Y.; Jiang, X. Noninvasive and Nonocclusive Blood Pressure Monitoring via a Flexible Piezo-Composite Ultrasonic Sensor. IEEE Sens. J. 2020, 21, 2642–2650. [Google Scholar] [CrossRef]
- Renard, E. Implantable Glucose Sensors for Diabetes Monitoring. Minim. Invasive Ther. Allied Technol. 2004, 13, 78–86. [Google Scholar] [CrossRef] [PubMed]
- Parast, V.M.; Paknahad, Z. Antioxidant Status and Risk of Gestational Diabetes Mellitus: A Case-Control Study. Clin. Nutr. Res. 2017, 6, 81. [Google Scholar] [CrossRef] [PubMed]
- Singh, C.; Gupta, Y.; Goyal, A.; Kalaivani, M.; Garg, V.; Bharti, J.; Singhal, S.; Kachhawa, G.; Kulshrestha, V.; Kumari, R. Glycemic Profile of Women with Normoglycemia and Gestational Diabetes Mellitus during Early Pregnancy Using Continuous Glucose Monitoring System. Diabetes Res. Clin. Pract. 2020, 169, 108409. [Google Scholar] [CrossRef]
- Nelson, K.M.; Hoffman, M.K.; Gleghorn, J.P.; Day, E.S. Diseases and Conditions That Impact Maternal and Fetal Health and the Potential for Nanomedicine Therapies. Adv. Drug Deliv. Rev. 2020, 170, 425–438. [Google Scholar] [CrossRef]
- Poudyal, A.; van Heerden, A.; Hagaman, A.; Maharjan, S.M.; Byanjankar, P.; Subba, P.; Kohrt, B.A. Wearable Digital Sensors to Identify Risks of Postpartum Depression and Personalize Psychological Treatment for Adolescent Mothers: Protocol for a Mixed Methods Exploratory Study in Rural Nepal. JMIR Res. Protoc. 2019, 8, e14734. [Google Scholar] [CrossRef] [PubMed]
- Heldt, G.P.; Ward, R.J. Evaluation of Ultrasound-Based Sensor to Monitor Respiratory and Nonrespiratory Movement and Timing in Infants. IEEE Trans. Biomed. Eng. 2015, 63, 619–629. [Google Scholar] [CrossRef] [PubMed]
- Alkema, L.; Chao, F.; You, D.; Pedersen, J.; Sawyer, C.C. National, Regional, and Global Sex Ratios of Infant, Child, and under-5 Mortality and Identification of Countries with Outlying Ratios: A Systematic Assessment. Lancet Glob. Health 2014, 2, e521–e530. [Google Scholar] [CrossRef]
- Woolery, L.K.; Grzymala-Busse, J. Machine Learning for an Expert System to Predict Preterm Birth Risk. J. Am. Med. Inform. Assoc. 1994, 1, 439–446. [Google Scholar] [CrossRef]
- King, Z.D.; Moskowitz, J.; Egilmez, B.; Zhang, S.; Zhang, L.; Bass, M.; Rogers, J.; Ghaffari, R.; Wakschlag, L.; Alshurafa, N. Micro-Stress EMA: A Passive Sensing Framework for Detecting in-the-Wild Stress in Pregnant Mothers. Proc. ACM Interact. Mob. Wearable Ubiquitous Technol. 2019, 3, 1–22. [Google Scholar] [CrossRef]
- Veena, S.; Aravindhar, D.J. Remote Monitoring System for the Detection of Prenatal Risk in a Pregnant Woman. Wirel. Pers. Commun. 2021, 119, 1051–1064. [Google Scholar] [CrossRef]
- Zhang, Y.; Wang, S.; Hermann, A.; Joly, R.; Pathak, J. Development and Validation of a Machine Learning Algorithm for Predicting the Risk of Postpartum Depression among Pregnant Women. J. Affect. Disord. 2021, 279, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Chu, R.; Chen, W.; Song, G.; Yao, S.; Xie, L.; Song, L.; Zhang, Y.; Chen, L.; Zhang, X.; Ma, Y. Predicting the Risk of Adverse Events in Pregnant Women With Congenital Heart Disease. J. Am. Heart Assoc. 2020, 9, e016371. [Google Scholar] [CrossRef] [PubMed]
- Auria, L.; Moro, R. Advantages and Disadvantages of Support Vector Machines. In Credit Risk Assessment Revisited: Methodological Issues and Practical Implications; European Committee of Central Balance Sheet Data Offices: Vienna, Austria, 2007; pp. 49–68. [Google Scholar]
- Shahid, N.; Rappon, T.; Berta, W. Applications of Artificial Neural Networks in Health Care Organizational Decision-Making: A Scoping Review. PLoS ONE 2019, 14, e0212356. [Google Scholar] [CrossRef]
- Davidson, L.; Boland, M.R. Towards Deep Phenotyping Pregnancy: A Systematic Review on Artificial Intelligence and Machine Learning Methods to Improve Pregnancy Outcomes. Brief. Bioinform. 2021, 22, bbaa369. [Google Scholar] [CrossRef]
- Hoodbhoy, Z.; Jeelani, S.M.; Aziz, A.; Habib, M.I.; Iqbal, B.; Akmal, W.; Siddiqui, K.; Hasan, B.; Leeflang, M.; Das, J.K. Machine Learning for Child and Adolescent Health: A Systematic Review. Pediatrics 2021, 147, e2020011833. [Google Scholar] [CrossRef]
- Geman, O.; Chiuchisan, I.; Ungurean, I.; Hagan, M.; Arif, M. Ubiquitous Healthcare System Based on the Sensors Network and Android Internet of Things Gateway. In Proceedings of the 2018 IEEE SmartWorld, Ubiquitous Intelligence & Computing, Advanced & Trusted Computing, Scalable Computing & Communications, Cloud & Big Data Computing, Internet of People and Smart City Innovation (SmartWorld/SCALCOM/UIC/ATC/CBDCom/IOP/SCI), Guangzhou, China, 8–12 October 2018; IEEE: Manhattan, NY, USA, 2018; pp. 1390–1395. [Google Scholar]
- Alam, M.G.R.; Munir, M.S.; Uddin, M.Z.; Alam, M.S.; Dang, T.N.; Hong, C.S. Edge-of-Things Computing Framework for Cost-Effective Provisioning of Healthcare Data. J. Parallel Distrib. Comput. 2019, 123, 54–60. [Google Scholar] [CrossRef]
- Ray, P.P.; Dash, D.; De, D. Edge Computing for Internet of Things: A Survey, e-Healthcare Case Study and Future Direction. J. Netw. Comput. Appl. 2019, 140, 1–22. [Google Scholar] [CrossRef]
- Sodhro, A.H.; Luo, Z.; Sangaiah, A.K.; Baik, S.W. Mobile Edge Computing Based QoS Optimization in Medical Healthcare Applications. Int. J. Inf. Manag. 2019, 45, 308–318. [Google Scholar] [CrossRef]
- Mutlag, A.A.; Abd Ghani, M.K.; Arunkumar, N.; Mohammed, M.A.; Mohd, O. Enabling Technologies for Fog Computing in Healthcare IoT Systems. Future Gener. Comput. Syst. 2019, 90, 62–78. [Google Scholar] [CrossRef]
- Bhatia, M.; Sood, S.K. Exploring Temporal Analytics in Fog-Cloud Architecture for Smart Office Healthcare. Mob. Netw. Appl. 2019, 24, 1392–1410. [Google Scholar] [CrossRef]
- Ullah, A.; Sehr, I.; Akbar, M.; Ning, H. FoG Assisted Secure De-Duplicated Data Dissemination in Smart Healthcare IoT. In Proceedings of the 2018 IEEE International Conference on Smart Internet of Things (SmartIoT), Xi’an, China, 17–19 August 2018; IEEE: Manhattan, NY, USA, 2018; pp. 166–171. [Google Scholar]
- Kumari, A.; Tanwar, S.; Tyagi, S.; Kumar, N. Fog Computing for Healthcare 4.0 Environment: Opportunities and Challenges. Comput. Electr. Eng. 2018, 72, 1–13. [Google Scholar] [CrossRef]
- Mahmoud, M.M.; Rodrigues, J.J.; Saleem, K.; Al-Muhtadi, J.; Kumar, N.; Korotaev, V. Towards Energy-Aware Fog-Enabled Cloud of Things for Healthcare. Comput. Electr. Eng. 2018, 67, 58–69. [Google Scholar] [CrossRef]
- Paul, A.; Pinjari, H.; Hong, W.-H.; Seo, H.C.; Rho, S. Fog Computing-Based IoT for Health Monitoring System. J. Sens. 2018, 2018, 1386470. [Google Scholar] [CrossRef]
- Elazhary, H. Internet of Things (IoT), Mobile Cloud, Cloudlet, Mobile IoT, IoT Cloud, Fog, Mobile Edge, and Edge Emerging Computing Paradigms: Disambiguation and Research Directions. J. Netw. Comput. Appl. 2019, 128, 105–140. [Google Scholar] [CrossRef]
- Shahzad, A.; Lee, Y.S.; Lee, M.; Kim, Y.-G.; Xiong, N. Real-Time Cloud-Based Health Tracking and Monitoring System in Designed Boundary for Cardiology Patients. J. Sens. 2018, 2018, 3202787. [Google Scholar] [CrossRef]
- Tyagi, S.; Agarwal, A.; Maheshwari, P. A Conceptual Framework for IoT-Based Healthcare System Using Cloud Computing. In Proceedings of the 2016 6th International Conference-Cloud System and Big Data Engineering (Confluence), Noida, India, 14–15 January 2016; IEEE: Manhattan, NY, USA, 2016; pp. 503–507. [Google Scholar]
- Li, X.; Lu, Y.; Fu, X.; Qi, Y. Building the Internet of Things Platform for Smart Maternal Healthcare Services with Wearable Devices and Cloud Computing. Future Gener. Comput. Syst. 2021, 118, 282–296. [Google Scholar] [CrossRef]
- Jagadeeswari, V.; Subramaniyaswamy, V.; Logesh, R.; Vijayakumar, V. A Study on Medical Internet of Things and Big Data in Personalized Healthcare System. Health Inf. Sci. Syst. 2018, 6, 1–20. [Google Scholar] [CrossRef]
- Rajkomar, A.; Dean, J.; Kohane, I. Machine Learning in Medicine. N. Engl. J. Med. 2019, 380, 1347–1358. [Google Scholar] [CrossRef]
- Handelman, G.S.; Kok, H.K.; Chandra, R.V.; Razavi, A.H.; Lee, M.J.; Asadi, H. ED Octor: Machine Learning and the Future of Medicine. J. Intern. Med. 2018, 284, 603–619. [Google Scholar] [CrossRef]
- Ramakrishnan, R.; Rao, S.; He, J.-R. Perinatal Health Predictors Using Artificial Intelligence: A Review. Womens Health 2021, 17, 17455065211046132. [Google Scholar] [CrossRef] [PubMed]
- Zhang, D.; Rodrigues, J.J.; Zhai, Y.; Sato, T. Design and Implementation of 5G E-Health Systems: Technologies, Use Cases, and Future Challenges. IEEE Commun. Mag. 2021, 59, 80–85. [Google Scholar] [CrossRef]
- Derbyshire, E.; Dancey, D. Smartphone Medical Applications for Women’s Health: What Is the Evidence-Base and Feedback? Int. J. Telemed. Appl. 2013, 2013, 782074. [Google Scholar] [CrossRef]
- Gritters, J. Wearable Health Trackers: A Revolution in Cancer Care. JNCI J. Natl. Cancer Inst. 2017, 109, djx046. [Google Scholar] [CrossRef] [PubMed]
- Penders, J.; Altini, M.; Van Hoof, C.; Dy, E. Wearable Sensors for Healthier Pregnancies. Proc. IEEE 2015, 103, 179–191. [Google Scholar] [CrossRef]
- Lopez, B.D.B.; Aguirre, J.A.A.; Coronado, D.A.R.; Gonzalez, P.A. Wearable Technology Model to Control and Monitor Hypertension during Pregnancy. In Proceedings of the 2018 13th Iberian Conference on Information Systems and Technologies (CISTI), Caceres, Spain, 13–16 June 2018; IEEE: Manhattan, NY, USA, 2018; pp. 1–6. [Google Scholar]
- Haider, D.; Ren, A.; Fan, D.; Zhao, N.; Yang, X.; Shah, S.A.; Hu, F.; Abbasi, Q.H. An Efficient Monitoring of Eclamptic Seizures in Wireless Sensors Networks. Comput. Electr. Eng. 2019, 75, 16–30. [Google Scholar] [CrossRef]
- Pandey, I.; Tiwari, J.D. A Novel Dual Imprinted Conducting Nanocubes Based Flexible Sensor for Simultaneous Detection of Hemoglobin and Glycated Haemoglobin in Gestational Diabetes Mellitus Patients. Sens. Actuators B Chem. 2019, 285, 470–478. [Google Scholar] [CrossRef]
- Mhajna, M.; Schwartz, N.; Levit-Rosen, L.; Warsof, S.; Lipschuetz, M.; Jakobs, M.; Rychik, J.; Sohn, C.; Yagel, S. Wireless, Remote Solution for Home Fetal and Maternal Heart Rate Monitoring. Am. J. Obstet. Gynecol. MFM 2020, 2, 100101. [Google Scholar] [CrossRef]
- Xu, X.; Chen, Y.; Liu, Z.; Sun, Y.; Zhou, L.; Antonio, J. The Value of Intelligent Ultrasound Sensor Used in the Measurement of Fetal Hemodynamics and Evaluation of Health Factors. Measurement 2020, 158, 107699. [Google Scholar] [CrossRef]
- Abeywardena, C.L.; Vanheusden, F.J.; Walker, K.F.; Arm, R.; Zhang, Q. Fetal Movement Counting Using Optical Fibre Sensors. Sensors 2021, 21, 48. [Google Scholar] [CrossRef]
- Koivu, A.; Sairanen, M. Predicting Risk of Stillbirth and Preterm Pregnancies with Machine Learning. Health Inf. Sci. Syst. 2020, 8, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Betts, K.S.; Kisely, S.; Alati, R. Predicting Postpartum Psychiatric Admission Using a Machine Learning Approach. J. Psychiatr. Res. 2020, 130, 35–40. [Google Scholar] [CrossRef]
- Zhang, Y.; Tayarani, M.; Wang, S.; Liu, Y.; Sharma, M.; Joly, R.; RoyChoudhury, A.; Hermann, A.; Gao, O.; Pathak, J. Identifying Urban Built Environment Factors in Pregnancy Care and Maternal Mental Health Outcomes. BMC Pregnancy Childbirth 2021, 21, 599. [Google Scholar] [CrossRef] [PubMed]
- Hussain, Z.; Borah, M.D. Birth Weight Prediction of New Born Baby with Application of Machine Learning Techniques on Features of Mother. J. Stat. Manag. Syst. 2020, 23, 1079–1091. [Google Scholar] [CrossRef]
- Beksac, M.S.; Tanacan, A.; Bacak, H.O.; Leblebicioglu, K. Computerized Prediction System for the Route of Delivery (Vaginal Birth versus Cesarean Section). J. Perinat. Med. 2018, 46, 881–884. [Google Scholar] [CrossRef] [PubMed]
- Akbulut, A.; Ertugrul, E.; Topcu, V. Fetal Health Status Prediction Based on Maternal Clinical History Using Machine Learning Techniques. Comput. Methods Programs Biomed. 2018, 163, 87–100. [Google Scholar] [CrossRef] [PubMed]
- Neocleous, A.C.; Syngelaki, A.; Nicolaides, K.H.; Schizas, C.N. Two-Stage Approach for Risk Estimation of Fetal Trisomy 21 and Other Aneuploidies Using Computational Intelligence Systems. Ultrasound Obstet. Gynecol. 2018, 51, 503–508. [Google Scholar] [CrossRef] [PubMed]
- Salehi, S.S.M.; Khan, S.; Erdogmus, D.; Gholipour, A. Real-Time Deep Pose Estimation with Geodesic Loss for Image-to-Template Rigid Registration. IEEE Trans. Med. Imaging 2018, 38, 470–481. [Google Scholar] [CrossRef]
- Lu, Y.; Fu, X.; Chen, F.; Wong, K.K. Prediction of Fetal Weight at Varying Gestational Age in the Absence of Ultrasound Examination Using Ensemble Learning. Artif. Intell. Med. 2020, 102, 101748. [Google Scholar] [CrossRef]
- Hassan, M.R.; Al-Insaif, S.; Hossain, M.I.; Kamruzzaman, J. A Machine Learning Approach for Prediction of Pregnancy Outcome Following IVF Treatment. Neural Comput. Appl. 2020, 32, 2283–2297. [Google Scholar] [CrossRef]
- Naik, P.; Reddy, V.; Shettigar, R. Pain Track Analysis during Gestation Using Machine Learning Techniques. Int. J. Electr. Comput. Eng. (2088-8708) 2021, 11, 2128–2133. [Google Scholar] [CrossRef]
- Zhu, Z.; Liu, T.; Li, G.; Li, T.; Inoue, Y. Wearable Sensor Systems for Infants. Sensors 2015, 15, 3721–3749. [Google Scholar] [CrossRef] [PubMed]
- Ishak, D.N.F.M.; Jamil, M.M.A.; Ambar, R. Arduino Based Infant Monitoring System. In Proceedings of the IOP Conference Series: Materials Science and Engineering; IOP Publishing, 2017; Volume 226, p. 012095. [Google Scholar]
- Pawar, P.A. Heart Rate Monitoring System Using IR Base Sensor & Arduino Uno. In Proceedings of the 2014 Conference on IT in Business, Industry and Government (CSIBIG), Indore, India, 8–9 March 2014; IEEE: Manhattan, NY, USA, 2014; pp. 1–3. [Google Scholar]
- Aktas, F.; Kavus, E.; Kavus, Y. A Real-Time Infant Health Monitoring System for Hard of Hearing Parents by Using Android-Based Mobil Devices. Istanb. Univ.-J. Electr. Electron. Eng. 2017, 17, 3107–3113. [Google Scholar]
- Lee, W.K.; Yoon, H.; Han, C.; Joo, K.M.; Park, K.S. Physiological Signal Monitoring Bed for Infants Based on Load-Cell Sensors. Sensors 2016, 16, 409. [Google Scholar] [CrossRef]
- Zakaria, N.A.; Saleh, F.N.B.M.; Razak, M.A.A. IoT (Internet of Things) Based Infant Body Temperature Monitoring. In Proceedings of the 2018 2nd International Conference on Biosignal Analysis, Processing and Systems (ICBAPS), Kuching, Malaysia, 24–26 July 2018; IEEE: Manhattan, NY, USA, 2018; pp. 148–153. [Google Scholar]
- Hussain, T.; Muhammad, K.; Khan, S.; Ullah, A.; Lee, M.Y.; Baik, S.W. Intelligent Baby Behavior Monitoring Using Embedded Vision in IoT for Smart Healthcare Centers. J. Artif. Intell. Syst. 2019, 1, 110–124. [Google Scholar] [CrossRef]
- Jegadeesan, S.; Dhamodaran, M.; Azees, M.; Shanmugapriya, S.S. Computationally Efficient Mutual Authentication Protocol for Remote Infant Incubator Monitoring System. Healthc. Technol. Lett. 2019, 6, 92–97. [Google Scholar] [CrossRef]
- Aviles-Espinosa, R.; Rendon-Morales, E.; Luo, Z.; Dore, H.; Anton, O.; Rabe, H.; Prance, R.J. Neo-SENSE: A Non-Invasive Smart Sensing Mattress for Cardiac Monitoring of Babies. In Proceedings of the 2019 IEEE Sensors Applications Symposium (SAS), Sophia Antipolis, France, 11–13 March 2019; IEEE: Manhattan, NY, USA, 2019; pp. 1–5. [Google Scholar]
- Vieluf, S.; Reinsberger, C.; El Atrache, R.; Jackson, M.; Schubach, S.; Ufongene, C.; Loddenkemper, T.; Meisel, C. Autonomic Nervous System Changes Detected with Peripheral Sensors in the Setting of Epileptic Seizures. Sci. Rep. 2020, 10, 1–8. [Google Scholar] [CrossRef]
- Karino, G.; Senoo, A.; Kunikata, T.; Kamei, Y.; Yamanouchi, H.; Nakamura, S.; Shukuya, M.; Colman, R.J.; Koshiba, M. Inexpensive Home Infrared Living/Environment Sensor with Regional Thermal Information for Infant Physical and Psychological Development. Int. J. Environ. Res. Public Health 2020, 17, 6844. [Google Scholar] [CrossRef]
- Yun, I.; Jeung, J.; Kim, M.; Kim, Y.-S.; Chung, Y. Ultra-Low Power Wearable Infant Sleep Position Sensor. Sensors 2020, 20, 61. [Google Scholar] [CrossRef]
- Wilson, R.B.; Vangala, S.; Elashoff, D.; Safari, T.; Smith, B.A. Using Wearable Sensor Technology to Measure Motion Complexity in Infants at High Familial Risk for Autism Spectrum Disorder. Sensors 2021, 21, 616. [Google Scholar] [CrossRef]
- Binu, P.K.; Akhil, V.; Mohan, V. Smart and Secure IOT Based Child Behaviour and Health Monitoring System Using Hadoop. In Proceedings of the 2017 International Conference on Advances in Computing, Communications and Informatics (ICACCI), Udupi, India, 13–16 September 2017; IEEE: Manhattan, NY, USA, 2017; pp. 418–423. [Google Scholar]
- Correa, M.; Zimic, M.; Barrientos, F.; Barrientos, R.; Román-Gonzalez, A.; Pajuelo, M.J.; Anticona, C.; Mayta, H.; Alva, A.; Solis-Vasquez, L.; et al. Automatic Classification of Pediatric Pneumonia Based on Lung Ultrasound Pattern Recognition. PLoS ONE 2018, 13, e0206410. [Google Scholar] [CrossRef] [PubMed]
- Kim, S.Y.; Kim, S.; Cho, J.; Kim, Y.S.; Sol, I.S.; Sung, Y.; Cho, I.; Park, M.; Jang, H.; Kim, Y.H.; et al. A Deep Learning Model for Real-Time Mortality Prediction in Critically Ill Children. Crit. Care 2019, 23, 279. [Google Scholar] [CrossRef] [PubMed]
- Sheela, K.G.; Varghese, A.R. Machine Learning Based Health Monitoring System. Mater. Today Proc. 2020, 24, 1788–1794. [Google Scholar] [CrossRef]
- Cheggou, R.; Annad, O.; hadi Khoumeri, E. An Intelligent Baby Monitoring System Based on Raspberry PI, IoT Sensors and Convolutional Neural Network. In Proceedings of the 2020 IEEE 21st International Conference on Information Reuse and Integration for Data Science (IRI), Las Vegas, NV, USA, 11–13 August 2020; IEEE: Manhattan, NY, USA, 2020; pp. 365–371. [Google Scholar]
- Richards, J.E.; Xie, W. Brains for All the Ages: Structural Neurodevelopment in Infants and Children from a Life-Span Perspective. Adv. Child Dev. Behav. 2015, 48, 1–52. [Google Scholar] [PubMed]
- Richards, J.E.; Sanchez, C.; Phillips-Meek, M.; Xie, W. A Database of Age-Appropriate Average MRI Templates. Neuroimage 2016, 124, 1254–1259. [Google Scholar] [CrossRef] [PubMed]
- Available online: https://www.Kaggle.com/c/Fiap-Fsbds-Baby-Monitor (accessed on 15 March 2021).
- Marchant, T.; Boerma, T.; Diaz, T.; Huicho, L.; Kyobutungi, C.; Mershon, C.-H.; Schellenberg, J.; Somers, K.; Waiswa, P. Measurement and Accountability for Maternal, Newborn and Child Health: Fit for 2030? BMJ Glob. Health 2020, 5, e002697. [Google Scholar] [CrossRef]
- Alkema, L.; New, J.R. Global Estimation of Child Mortality Using a Bayesian B-Spline Bias-Reduction Model. Ann. Appl. Stat. 2014, 8, 2122–2149. [Google Scholar] [CrossRef]
- Available online: https://www.Mchlibrary.Org/Professionals/Datadbs.Php (accessed on 15 March 2021).
- Moreira, M.W.; Rodrigues, J.J.; Kumar, N.; Saleem, K.; Illin, I.V. Postpartum Depression Prediction through Pregnancy Data Analysis for Emotion-Aware Smart Systems. Inf. Fusion 2019, 47, 23–31. [Google Scholar] [CrossRef]


| Sr. No. | Ref. (Year) | Review Methodology | Contribution | Major Difference from This Review |
|---|---|---|---|---|
| 1 | [7] (2020) | Systematic review and meta-Analysis | A study on the effectiveness and safety of pharmacologic interventions for the treatment of retained placenta. | No AI methods and sensing devices are reviewed. Only one maternal problem (retained placenta) is considered. |
| 2. | [30] (2019) | Seminal review | Identifies key characteristics and drivers for market uptake of ANN for healthcare organizational decision making to guide further adoption. | No focus on maternal and infant issues. Sensing devices are also not part of this study. |
| 3 | [31] (2021) | Systematic review | A systematic review on the ways that AI and ML including deep learning methodologies can inform patient care during pregnancy and improve outcomes. | Sensing-based healthcare and infant health issues are not considered in this review. |
| 4 | [32] (2020) | Systematic review | A study to provide an evidence map of the current available evidence on ML in pediatrics and adolescent medicine. | Maternal issues are not a focus. Furthermore, a sensing-based remote patient monitor is not included in this review |
| 5 | [48] (2020) | Systematic review | The main characteristics and outcomes of studies using Computerized Decision Support (CDS) and ML are demonstrated, to advance our understanding toward the development of smart and effective interventions for childhood obesity care. | Maternal issues are not a focus, and only child obesity is the scope of review. |
| 6 | [49] (2019) | Systematic review | A systematic literature review protocol to study how mobile computing assists IoT applications in healthcare is presented. | Maternal and infant healthcare solutions are not studied |
| 7 | [50] (2021) | Nonsystematic comprehensive survey | Review covers AI-based algorithms for novel prediction models, better diagnosis, early identification, and monitoring of women during pregnancy, labor, and postpartum to advance research, clinical practice, and policies, and ensure optimal perinatal health. | No focus on infant issues, and sensor networks are not considered for the monitoring of maternal and infant healthcare |
| 8 | [51] (2018) | Comprehensive review | Authors outlined the medical applications, ethical and international standardization challenges about the 5G e-health systems. | AI is not the primary concern in this review. Moreover, it does not specifically target pregnancy and infant-related problems |
| Sensor Based System | Features | Year | Disease | Dataset Acquisition |
|---|---|---|---|---|
| Wearable Technology, a solution to hypertension during pregnancy [55] | VO7 wearable model | 2018 | High Blood Pressure, Pre-term birth | From mobile application |
| Eclamptic Seizures monitoring by wireless sensors network [56] | 5G wireless sensing system | 2019 | Seizures | Not available |
| Nanocube-based flexible sensors for detection of hemoglobin and glycated hemoglobin [57] | Electrochemical sensors comprising double imprinted nanocubes | 2019 | Diabetes | Blood samples of healthy and diabetic pregnant women |
| Invu System: Home fetal and maternal heart rate monitoring [58] | Wireless electrical and acoustic sensors | 2020 | Abnormal heart rate of mother and child | From 147 participant women |
| Normoglycemia and GDM in early pregnancy through a continuous glucose monitoring system [19] | Continuous glucose monitoring system | 2020 | Diabetes | From 96 participant women |
| Measurement of fetal hemodynamics and evaluation of health factors through intelligent ultrasound sensors [59] | Intelligent ultrasound sensors | 2020 | Diabetes | From questionnaire |
| IoT platform for smart maternal healthcare using wearable devices and cloud computing [46] | IoT-based platform with wearable devices and cloud computing | 2021 | High risk pregnancy | From questionnaire |
| Use of optical fiber sensors for fetal movement counting [60] | Optical Fiber Sensors | 2021 | Stillbirth | From 3 volunteers |
| AI/ML Based Systems | Year | ML Algorithms Used | Disease | Dataset/Availability |
|---|---|---|---|---|
| Computerized Prediction System [65] | 2018 | ANN | Route of delivery | Data consist of 2127, 3548 and 1723 deliveries for the years 1976, 1986 and 1996/No |
| Fetal Health status Prediction using ML [66] | 2018 | Logistic Regression, Locally Deep SVM, Neural Networks, SVM, Averaged Perception, Decision Jungle, Decision Forest, Bayes Point Machine, Boosted Decision Trees | Fetal congenital anomalies | Clinical database of 96 pregnant women/No |
| Two-stage approach using computational Intelligence System [67] | 2018 | ANN | Fetal trisomy and other chromosomal abnormalities | Dataset comprises 72,054 euploid pregnancies/No |
| Deep CNN Regression Model for 3D Pose Estimation [68] | 2019 | CNN | Fetal health | MRI scans of 40 newborns and 93 reconstructed MRI scan of fetus/NO |
| Decision Support System [1] | 2019 | Multi-Layer Perception (MLP), Deep learning, SVM, Naïve Bayes classifier | Ectopic pregnancies | 406 cases of ectopic pregnancies collected from “Virgen de la Arrixaca” hospital in Spain/No |
| Prediction of Fetal Weight using Ensemble Learning [69] | 2020 | Random Forest, XG Boost, Light GBM algorithm Genetic algorithm | Fetal weight | Dataset comprises 4212 intrapartum recordings/No |
| Machine learning approach for IVF treatment [70] | 2020 | Multi-Layer Perception (MLP), SVM, C4.5, CART, RF | In vitro fertilization (IVF) | Data from infertility clinic in Istanbul/No |
| Pain Track Analysis [71] | 2021 | Facial recognition algorithm accompanied by SVM, Decision tree | Braxton Hicks | Database of images/No |
| Sensors Based Systems | Features | Year | Disease | Data Acquisition |
|---|---|---|---|---|
| Load-cell sensors based physiological signal monitoring bed for infants [76] | Load-cell signal sensors | 2016 | Physiological health | 4 infant patients |
| Body temperature monitoring of infant using IoTs [77] | LM35 sensor | 2018 | Body temperature | Not available |
| Use of vision sensors in IoT for intelligent baby behavior monitoring [78] | Vision sensors | 2019 | Abnormal baby motions | Baby’s video |
| Computationally efficient mutual authentication protocol for remote infant incubator monitoring system [79] | Wireless medical sensors | 2019 | Premature birth issues | Not available |
| Cardiac monitoring of babies through non-invasive smart sensing mattress [80] | Electrometer-based amplifier sensors | 2019 | Reduction in HR | Concept tests |
| Autonomic nervous system changes detected with peripheral sensors in the setting of epileptic seizures [81] | Peripheral sensors | 2020 | Epilepsy | 66 patients participated for the study |
| Inexpensive Home Infrared Living/Environment Sensor with Regional Thermal Information [82] | Infrared sensors | 2020 | Infant’s physical and psychological health | Not Available |
| Ultra-Low Power Wearable Infant Sleep Position Sensor [83] | Switch sensors | 2020 | To monitor infant’s sleeping positions | 24 infants |
| Measurement of infant complex motions using wearable sensor technology [84] | Wearable opal sensor technology | 2021 | ASD | 5 infants |
| AI/ML Based Systems | Year | ML Algorithms Used | Disease | Dataset/Availability |
|---|---|---|---|---|
| IoT based child behavior and health monitoring system [85] | 2017 | C4.5, ID3 algorithm Decision Tree | To monitor child behavior and health | Data are self generated/No |
| Automatic Classification of Pneumonia using ANN [86] | 2018 | Artificial Neural Network (ANN) | Pneumonia | 60 ultrasound images/Yes https://osf.io/hmr3w/ Access Date: 11 May 2022 |
| PROMPT [87] | 2019 | CNN | Infants’ mortality | 1977 patients/No |
| ML based Health monitoring system [88] | 2020 | SVM | To monitor chronically ill patients or infants | Data collected through body sensors/No |
| Datasets | Source | Attributes | Format | Language |
|---|---|---|---|---|
| Pregnancy Risk Assessment Monitoring System (PRAMS) | https://data.cityofnewyork.us/d/rqgf-94xs Access Date: 6 February 2022 | Year, source, question, prevalence %, lower 95% confidence interval, upper 95% confidence interval | csv | English |
| Infant Mortality | https://data.cityofnewyork.us/d/fcau-jc6k Access Date: 9 February 2022 | Year, maternal race, infant’s mortality rate, neonatal mortality rate, post neonatal mortality rate, infant death, neonatal infant death, post neonatal mortality rate, No. of live birth | csv | English |
| Baby Monitor Forecast | https://www.kaggle.com/c/fiap-fsbds-baby-monitorforecast/data?select=test.csv Access Date: 11 February 2022 | Id, date, mes, weekday, mergem, Venda, desconto, outdesc, outmg | csv | English |
| Maternal and Child Health Data of UNICEF | https://data.unicef.org/resources/dataset/maternal-health-data/https://data.unicef.org/topic/child-survival/ Access Date: 23 February 2022 | Country, year, mothers’ age, source | csv | English |
| Neuro Developmental MRI Database | https://jerlab.sc.edu/projects/neurodevelopmental-mri-database/ Access Date: 23 February 2022 | Age, 1.5 T, 3.0 T, total, notes | Tar.gz | English |
| Infant Death Dataset | https://www.cdc.gov/nchs/fastats/birth-defects.htm Access Date: 23 February 2022 | No. of infant deaths, infant deaths per 100,000 live births, cause of infant death | English |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Gulzar Ahmad, S.; Iqbal, T.; Javaid, A.; Ullah Munir, E.; Kirn, N.; Ullah Jan, S.; Ramzan, N. Sensing and Artificial Intelligent Maternal-Infant Health Care Systems: A Review. Sensors 2022, 22, 4362. https://doi.org/10.3390/s22124362
Gulzar Ahmad S, Iqbal T, Javaid A, Ullah Munir E, Kirn N, Ullah Jan S, Ramzan N. Sensing and Artificial Intelligent Maternal-Infant Health Care Systems: A Review. Sensors. 2022; 22(12):4362. https://doi.org/10.3390/s22124362
Chicago/Turabian StyleGulzar Ahmad, Saima, Tassawar Iqbal, Anam Javaid, Ehsan Ullah Munir, Nasira Kirn, Sana Ullah Jan, and Naeem Ramzan. 2022. "Sensing and Artificial Intelligent Maternal-Infant Health Care Systems: A Review" Sensors 22, no. 12: 4362. https://doi.org/10.3390/s22124362
APA StyleGulzar Ahmad, S., Iqbal, T., Javaid, A., Ullah Munir, E., Kirn, N., Ullah Jan, S., & Ramzan, N. (2022). Sensing and Artificial Intelligent Maternal-Infant Health Care Systems: A Review. Sensors, 22(12), 4362. https://doi.org/10.3390/s22124362








