Speech Quality Feature Analysis for Classification of Depression and Dementia Patients
Abstract
1. Introduction
2. Materials and Methods
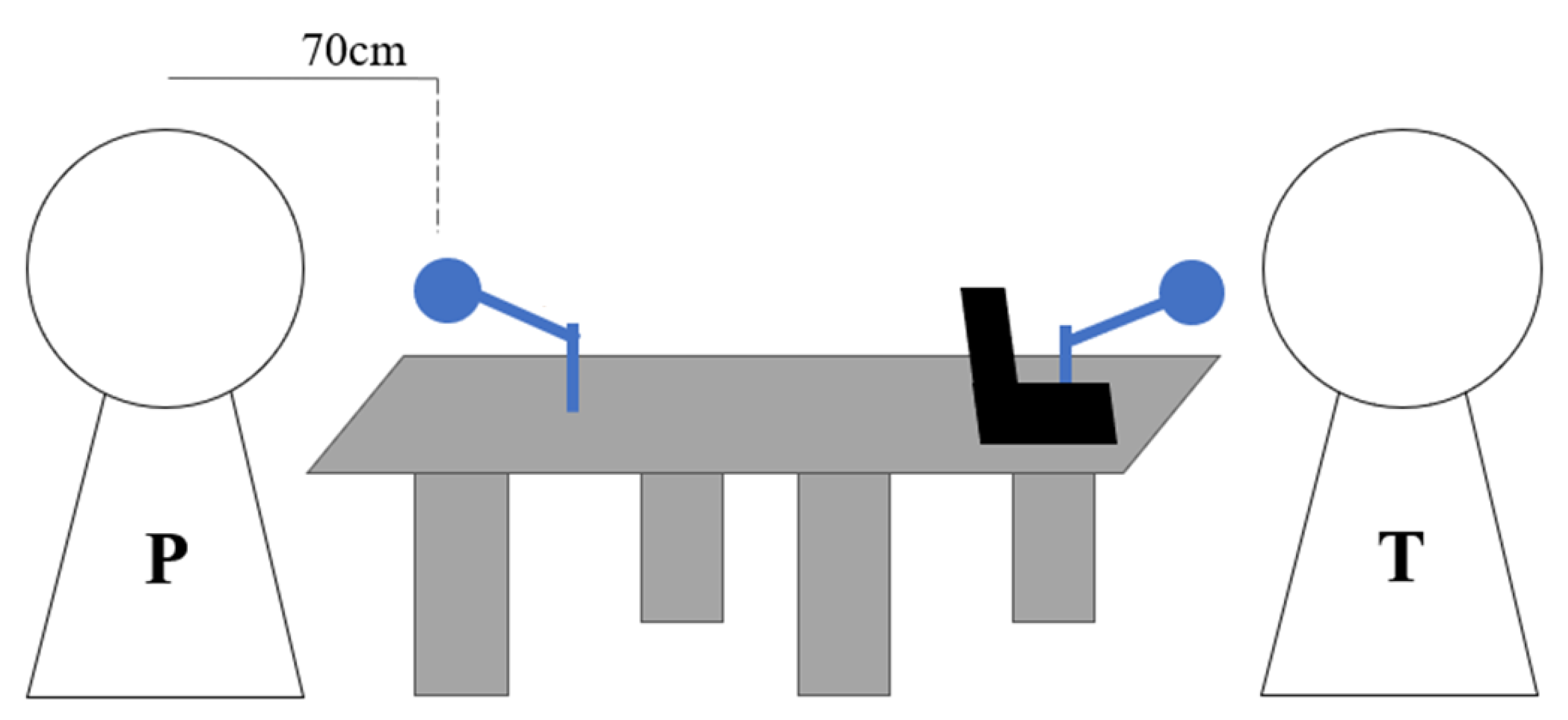
2.1. Data Acquisition
2.2. Participants
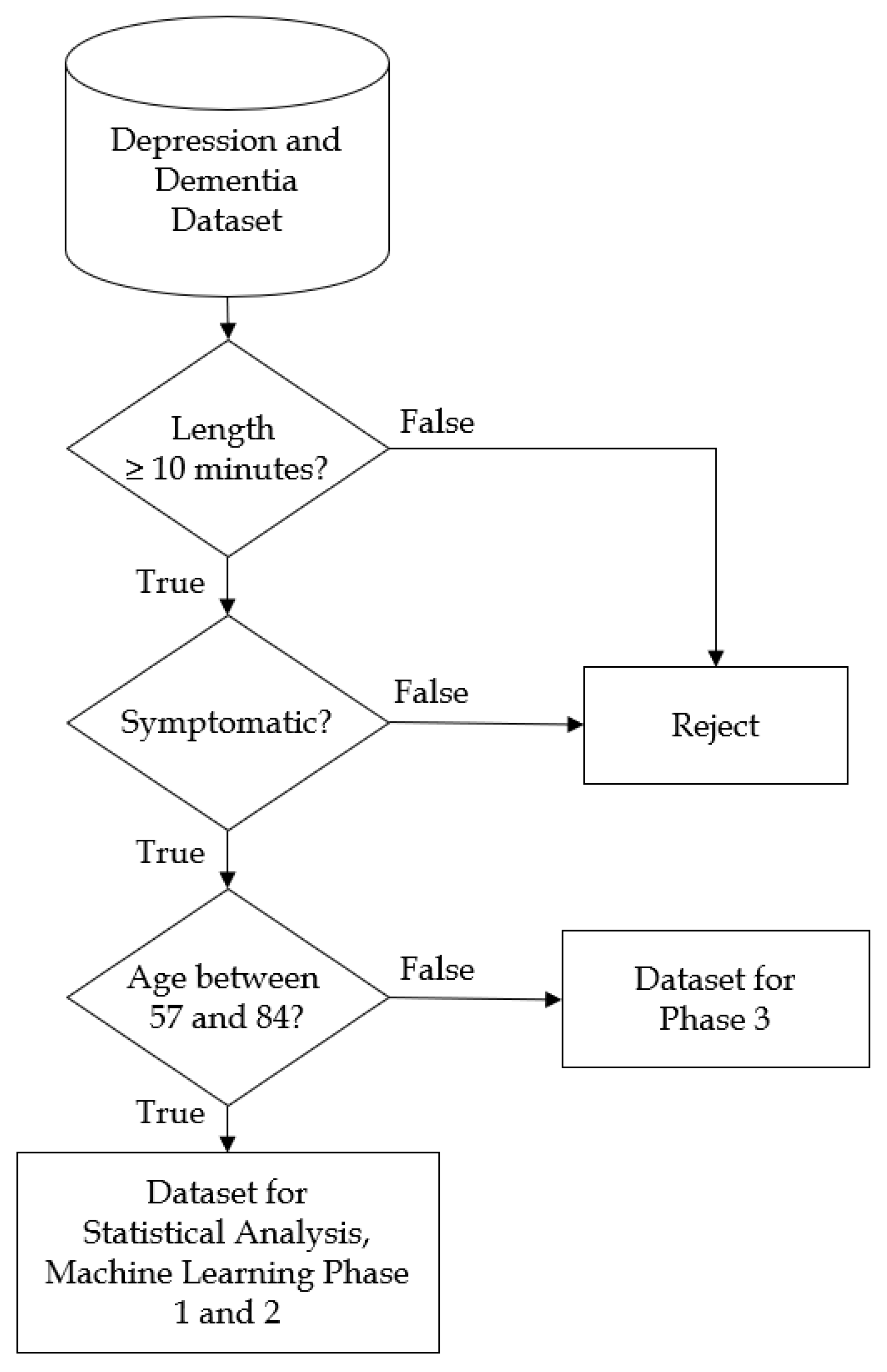
- Age between 57 and 84 years-old; 57 is the lowest age for dementia patients and 84 is the highest age for depression patients. The purpose of this criterion was to remove the effect of age which is positively correlated with Dementia.
- For dementia patients: mini-mental state examination (MMSE) score of 23 or less accompanied with 15-item geriatric depression scale (GDS) score of 5 or less; The purpose of this criterion was to select only patients with dementia symptoms and exclude patients with both symptoms. A person is defined as symptomatic dementia if the MMSE score is 23 or less.
- For depression patients: 17-item Hamilton depression rating scale (HAMD17) of 8 or more. A person is defined to be depressed if one’s score of HAMD17 is 8 or more.
- The recording session was from “free talk” and the length was at least 10 min long. The purpose of this criterion was to ensure enough information contained within the recordings.
- For dementia patients: mini-mental state examination (MMSE) score of 23 or less accompanied with 15-item geriatric depression scale (GDS) score of 5 or less; The age of the patients should be of 85 years or more.
- For depression patients: 17-item Hamilton depression rating scale (HAMD17) of 8 or more. The age of the patients should be no more than 56 years.
- The recording session was from “free talk” and the duration was at least 10 min long.
2.3. Materials
2.4. Audio Signal Analysis
2.4.1. Preprocessing
2.4.2. Feature Extraction
2.4.3. Statistical Analysis
2.4.4. Machine Learning
- Split the datasets into ten smaller groups, maintaining the ratio of the classes
- Perform ten-fold cross validation using these datasets.For each fold:
- (a)
- Split the training group into ten smaller subgroups.
- (b)
- Perform another ten-fold cross-validation using these subgroups.For each inner fold:
- i
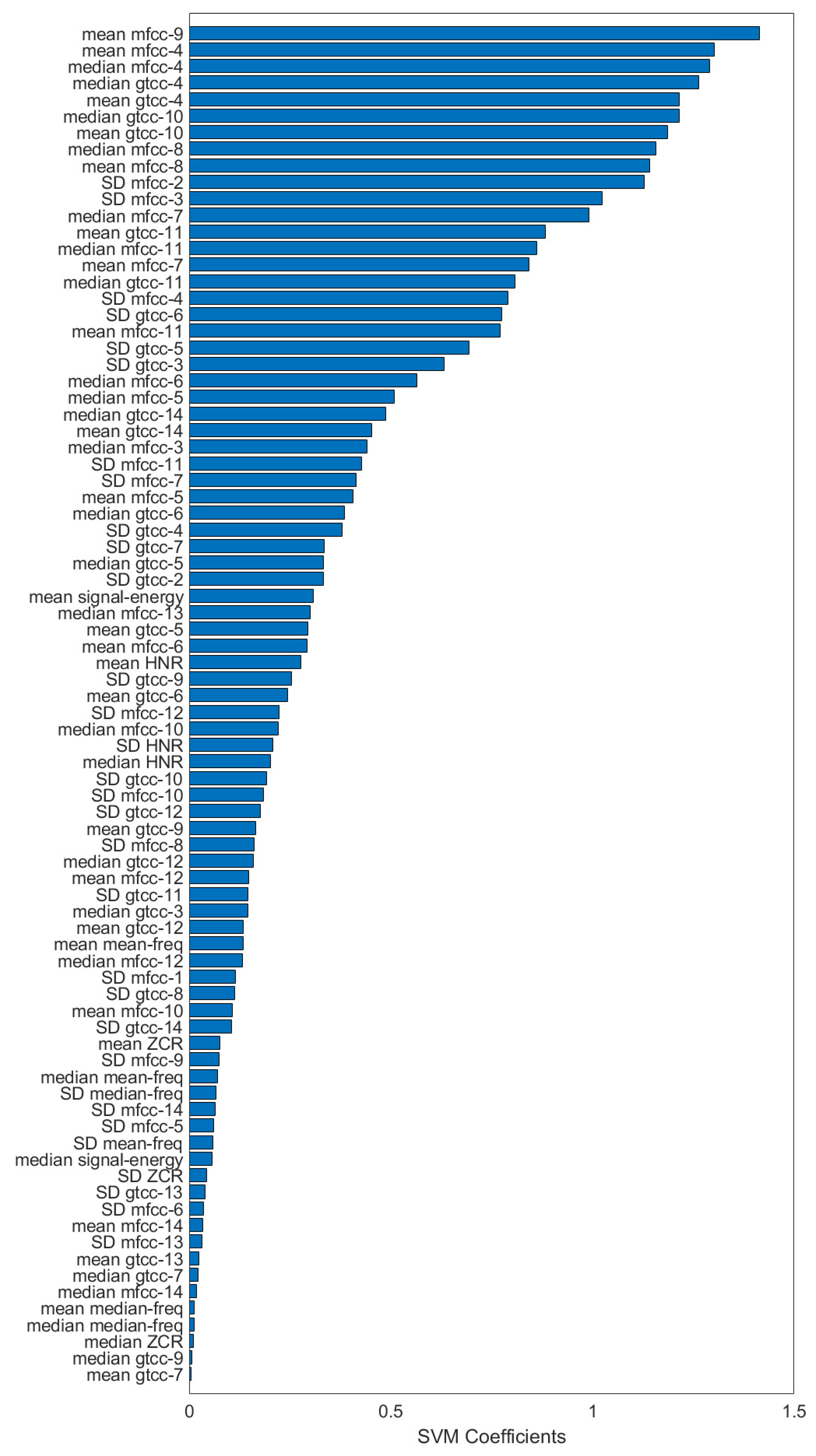
- Perform LASSO regression [44] and obtain the coefficients.The LASSO regression solveswhere is a scalar and is a vector of coefficients, N is the number of observations, is the response at observation i, is the vector of predictors at observation i, and is a nonnegative regularization parameter. High value of results in stricter feature selection and in this study, it is computed automatically such that it is the largest possible value for nonnull model. The performance of the model is not considered.
- ii
- Mark the features with coefficient of less than 0.01.
- (c)
- Perform feature selection by removing features with 10 marks obtained from step 2-b-ii.
- (d)
- Train an SVM model based on features from (c).
- Compute the average performance and standard deviation of the models.
2.4.5. Evaluation Metrics
3. Results
3.1. Demographics
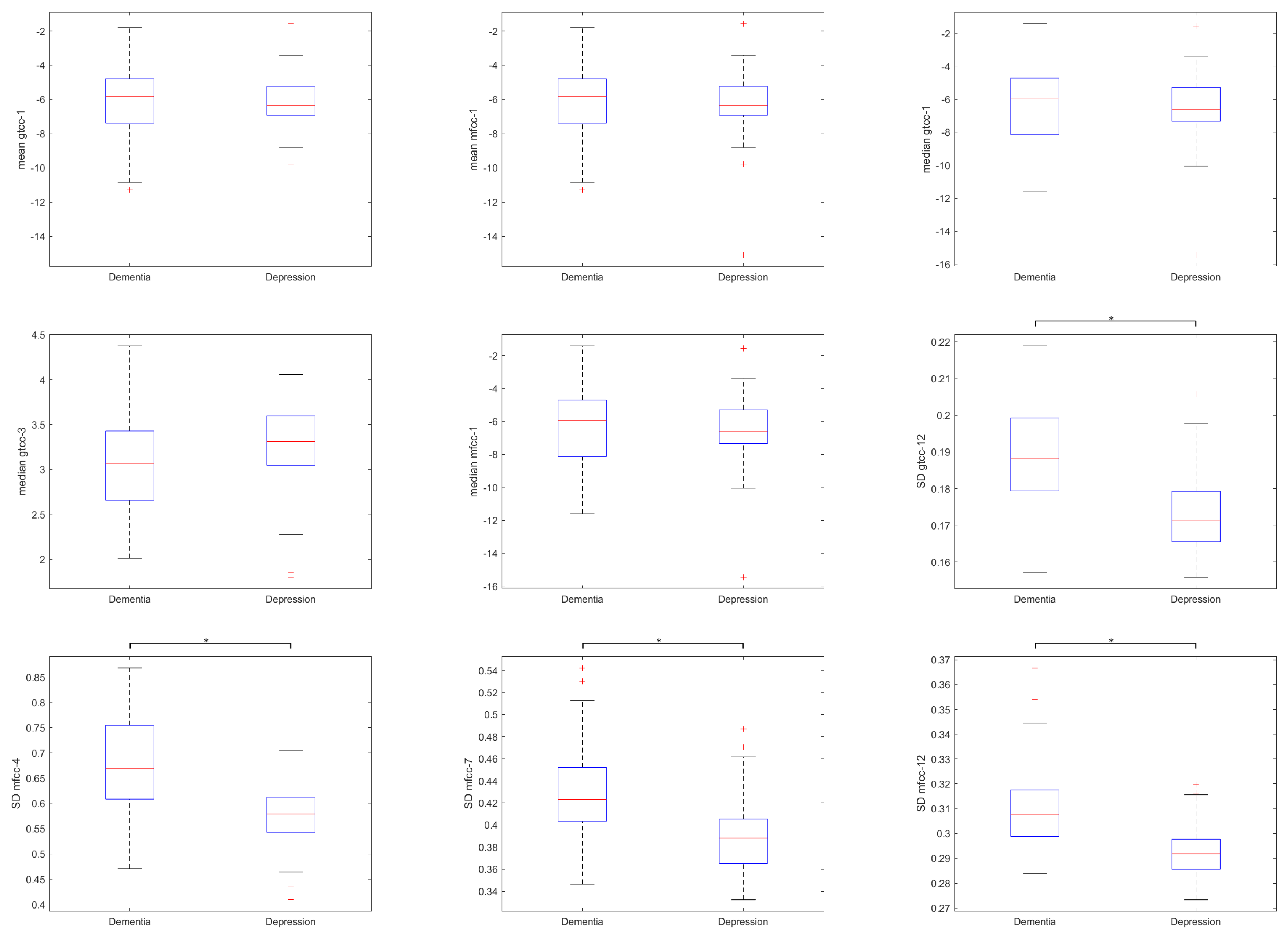
3.2. Statistical Analysis
3.3. Machine Learning
4. Discussion
5. Conclusions
6. Future Work
Author Contributions
Funding
Conflicts of Interest
References
- World Alzheimer Report 2019: Attitudes to Dementia. Available online: https://www.alz.co.uk/research/WorldAlzheimerReport2019.pdf (accessed on 25 June 2020).
- Yang, H.; Bath, P.A. The Use of Data Mining Methods for the Prediction of Dementia: Evidence From the English Longitudinal Study of Aging. IEEE J. Biomed. Health Inform. 2020, 24, 345–353. [Google Scholar] [CrossRef] [PubMed]
- Weiner, J.; Frankenberg, C.; Schroder, J.; Schultz, T. Speech Reveals Future Risk of Developing Dementia: Predictive Dementia Screening from Biographic Interviews. In Proceedings of the 2019 IEEE Automatic Speech Recognition and Understanding Workshop (ASRU), Singapore, 14–18 December 2019; pp. 674–681. [Google Scholar]
- Shigemizu, D.; Akiyama, S.; Asanomi, Y.; Boroevich, K.A.; Sharma, A.; Tsunoda, T.; Matsukuma, K.; Ichikawa, M.; Sudo, H.; Takizawa, S.; et al. Risk prediction models for dementia constructed by supervised principal component analysis using miRNA expression data. Commun. Biol. 2019, 2. [Google Scholar] [CrossRef] [PubMed]
- Ju, R.; Hu, C.; Zhou, P.; Li, Q. Early Diagnosis of Alzheimer’s Disease Based on Resting-State Brain Networks and Deep Learning. IEEE/ACM Trans. Comput. Biol. Bioinf. 2019, 16, 244–257. [Google Scholar] [CrossRef] [PubMed]
- Hwang, A.B.; Boes, S.; Nyffeler, T.; Schuepfer, G. Validity of screening instruments for the detection of dementia and mild cognitive impairment in hospital inpatients: A systematic review of diagnostic accuracy studies. PLoS ONE 2019, 14, e0219569. [Google Scholar] [CrossRef]
- Robinson, L.; Tang, E.; Taylor, J.-P. Dementia: Timely diagnosis and early intervention. BMJ 2015, 350, h3029. [Google Scholar] [CrossRef]
- Da Cunha, A.L.V.; de Sousa, L.B.; Mansur, L.L.; Aluisio, S.M. Automatic Proposition Extraction from Dependency Trees: Helping Early Prediction of Alzheimer’s Disease from Narratives. In Proceedings of the 2015 IEEE 28th International Symposium on Computer-Based Medical Systems, Sao Carlos, Brazil, 22–25 June 2015; pp. 127–130. [Google Scholar]
- Borson, S.; Frank, L.; Bayley, P.J.; Boustani, M.; Dean, M.; Lin, P.-J.; McCarten, J.R.; Morris, J.C.; Salmon, D.P.; Schmitt, F.A.; et al. Improving dementia care: The role of screening and detection of cognitive impairment. Alzheimers Dement. 2013, 9, 151–159. [Google Scholar] [CrossRef]
- Du, Z.; Li, Y.; Li, J.; Zhou, C.; Li, F.; Yang, X. Physical activity can improve cognition in patients with Alzheimer’s disease: A systematic review and meta-analysis of randomized controlled trials. Clin. Interv. Aging 2018, 13, 1593–1603. [Google Scholar] [CrossRef]
- Dominguez, L.J.; Barbagallo, M. Nutritional prevention of cognitive decline and dementia. Acta Bio Med. Atenei Parmensis 2018, 89, 276–290. [Google Scholar] [CrossRef]
- Geifman, N.; Brinton, R.D.; Kennedy, R.E.; Schneider, L.S.; Butte, A.J. Evidence for benefit of statins to modify cognitive decline and risk in Alzheimer’s disease. Alzheimers Res. Ther. 2017, 9, 1–10. [Google Scholar] [CrossRef]
- Killin, L.O.J.; Starr, J.M.; Shiue, I.J.; Russ, T.C. Environmental risk factors for dementia: A systematic review. BMC Geriatr. 2016, 16, 175. [Google Scholar] [CrossRef]
- Folstein, M.F.; Folstein, S.E.; McHugh, P.R. “Mini-mental state” a practical method for grading the cognitive state of patients for the clinician. J. Psychiatr. Res. 1975, 12, 189–198. [Google Scholar] [CrossRef]
- Mendes-Santos, L.C.; Mograbi, D.; Spenciere, B.; Charchat-Fichman, H. Specific algorithm method of scoring the Clock Drawing Test applied in cognitively normal elderly. Dement. Neuropsychol. 2015, 9, 128–135. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Yesavage, J.A.; Brink, T.L.; Rose, T.L.; Lum, O.; Huang, V.; Adey, M.; Leirer, V.O. Development and validation of a geriatric depression screening scale: A preliminary report. J. Psychiatr. Res. 1982, 17, 37–49. [Google Scholar] [CrossRef]
- Wright, P.; Stern, J.; Phelan, M. (Eds.) Core Psychiatry, 3rd ed.; Elsevier: Edinburgh, Scotland, 2012; ISBN 978-0-7020-3397-1. [Google Scholar]
- Kiloh, L.G. Pseudo-dementia. Acta Psychiatr. Scand. 1961, 37, 336–351. [Google Scholar] [CrossRef]
- McAllister, W. Overview: Pseudodementia. Am. J. Psychiatry 1983, 528–533. [Google Scholar]
- Prakash, R.; Zhao, F.; Daggubati, V.; Giorgetta, C.; Kang, H.; You, L.; Sarkhel, S. Pseudo-dementia: A neuropsychological review. Ann. Indian Acad. Neurol. 2014, 17. [Google Scholar] [CrossRef]
- American Psychiatric Association (Ed.) Diagnostic and Statistical Manual of Mental Disorders: DSM-5, 5th ed.; American Psychiatric Association: Washington, DC, USA, 2013; ISBN 978-0-89042-554-1. [Google Scholar]
- Jonsson, U.; Bertilsson, G.; Allard, P.; Gyllensvärd, H.; Söderlund, A.; Tham, A.; Andersson, G. Psychological Treatment of Depression in People Aged 65 Years and Over: A Systematic Review of Efficacy, Safety, and Cost-Effectiveness. PLoS ONE 2016, 11, e0160859. [Google Scholar] [CrossRef]
- Ooi, K.E.B.; Lech, M.; Allen, N.B. Multichannel Weighted Speech Classification System for Prediction of Major Depression in Adolescents. IEEE Trans. Biomed. Eng. 2013, 60, 497–506. [Google Scholar] [CrossRef]
- Gavrilescu, M.; Vizireanu, N. Predicting Depression, Anxiety, and Stress Levels from Videos Using the Facial Action Coding System. Sensors 2019, 19, 3693. [Google Scholar] [CrossRef]
- Dadiz, B.G.; Marcos, N. Analysis of Depression Based on Facial Cues on A Captured Motion Picture. In Proceedings of the 2018 IEEE 3rd International Conference on Signal and Image Processing (ICSIP), Shenzhen, China, 13–15 July 2018; pp. 49–54. [Google Scholar]
- Wu, L.; Pu, J.; Allen, J.J.B.; Pauli, P. Recognition of Facial Expressions in Individuals with Elevated Levels of Depressive Symptoms: An Eye-Movement Study. Depress. Res. Treat. 2012, 2012. [Google Scholar] [CrossRef]
- Nakamura, R.; Mitsukura, Y. Feature Analysis of Electroencephalography in Patients with Depression. In Proceedings of the 2018 IEEE Life Sciences Conference (LSC), Montreal, QC, Canada, 28–30 October 2018; pp. 53–56. [Google Scholar]
- Liao, S.-C.; Wu, C.-T.; Huang, H.-C.; Cheng, W.-T.; Liu, Y.-H. Major Depression Detection from EEG Signals Using Kernel Eigen-Filter-Bank Common Spatial Patterns. Sensors 2017, 17, 1385. [Google Scholar] [CrossRef] [PubMed]
- Song, H.; Du, W.; Yu, X.; Dong, W.; Quan, W.; Dang, W.; Zhang, H.; Tian, J.; Zhou, T. Automatic depression discrimination on FNIRS by using general linear model and SVM. In Proceedings of the 2014 7th International Conference on Biomedical Engineering and Informatics, Dalian, China, 14–16 October 2014; pp. 278–282. [Google Scholar]
- Henderson, G.; Ifeachor, E.; Hudson, N.; Goh, C.; Outram, N.; Wimalaratna, S.; Del Percio, C.; Vecchio, F. Development and assessment of methods for detecting dementia using the human electroencephalogram. IEEE Trans. Biomed. Eng. 2006, 53, 1557–1568. [Google Scholar] [CrossRef] [PubMed]
- Warnita, T.; Inoue, N.; Shinoda, K. Detecting Alzheimer’s Disease Using Gated Convolutional Neural Network from Audio Data. In Proceedings of the Interspeech 2018, Hyderabad, India, 2–6 September 2018; pp. 1706–1710. [Google Scholar]
- Kishimoto, T.; Takamiya, A.; Liang, K.; Funaki, K.; Fujita, T.; Kitazawa, M.; Yoshimura, M.; Tazawa, Y.; Horigome, T.; Eguchi, Y.; et al. The Project for Objective Measures Using Computational Psychiatry Technology (PROMPT): Rationale, Design, and Methodology. medRxiv 2019. [Google Scholar] [CrossRef]
- Hamilton, M. A rating scale for depression. J. Neurol. Neurosurg. Psychiatry 1960, 23, 56–62. [Google Scholar] [CrossRef] [PubMed]
- Young, R.C.; Biggs, J.T.; Ziegler, V.E.; Meyer, D.A. A Rating Scale for Mania: Reliability, Validity and Sensitivity. Br. J. Psychiatry 1978, 133, 429–435. [Google Scholar] [CrossRef]
- Mueller, K.D.; Hermann, B.; Mecollari, J.; Turkstra, L.S. Connected speech and language in mild cognitive impairment and Alzheimer’s disease: A review of picture description tasks. J. Clin. Exp. Neuropsychol. 2018, 40, 917–939. [Google Scholar] [CrossRef]
- Mundt, J.C.; Vogel, A.P.; Feltner, D.E.; Lenderking, W.R. Vocal Acoustic Biomarkers of Depression Severity and Treatment Response. Biol. Psychiatry 2012, 72, 580–587. [Google Scholar] [CrossRef]
- Darby, J.K.; Hollien, H. Vocal and Speech Patterns of Depressive Patients. Folia Phoniatr. Logop. 1977, 29, 279–291. [Google Scholar] [CrossRef]
- Gonzalez, S.; Brookes, M. PEFAC—A pitch estimation algorithm robust to high levels of noise. IEEE Trans. Audio Speech Lang. Process. 2014, 22, 518–530. [Google Scholar] [CrossRef]
- Kim, H.-G.; Moreau, N.; Sikora, T. MPEG-7 Audio and Beyond: Audio Content Indexing and Retrieval; John Wiley & Sons, Ltd.: Chichester, UK, 2005; ISBN 978-0-470-09336-8. [Google Scholar]
- Sahidullah, M.; Saha, G. Design, analysis and experimental evaluation of block based transformation in MFCC computation for speaker recognition. Speech Commun. 2012, 54, 543–565. [Google Scholar] [CrossRef]
- Valero, X.; Alias, F. Gammatone Cepstral Coefficients: Biologically Inspired Features for Non-Speech Audio Classification. IEEE Trans. Multimedia 2012, 14, 1684–1689. [Google Scholar] [CrossRef]
- Peeters, G. A large set of audio features for sound description (similarity and classification) in the CUIDADO project. CUIDADO IST Proj. Rep. 2004, 54, 1–25. [Google Scholar]
- Noble, W.S. What is a support vector machine? Nat. Biotechnol. 2006, 24, 1565–1567. [Google Scholar] [CrossRef] [PubMed]
- Fonti, V.; Belitser, E. Feature Selection using LASSO. VU Amst. Res. Pap. Bus. Anal. 2017, 30, 1–25. [Google Scholar]
- Sugan, N.; Sai Srinivas, N.S.; Kar, N.; Kumar, L.S.; Nath, M.K.; Kanhe, A. Performance Comparison of Different Cepstral Features for Speech Emotion Recognition. In Proceedings of the 2018 International CET Conference on Control, Communication, and Computing (IC4), Thiruvananthapuram, India, 5–7 July 2018; pp. 266–271. [Google Scholar]
- Adiga, A.; Magimai, M.; Seelamantula, C.S. Gammatone wavelet Cepstral Coefficients for robust speech recognition. In Proceedings of the 2013 IEEE International Conference of IEEE Region 10 (TENCON 2013), Xi’an, China, 22–25 October 2013; pp. 1–4. [Google Scholar]
- Cheng, O. Performance Evaluation of Front-end Processing for Speech Recognition Systems; The University of Auckland: Auckland, New Zealand, 2005; Volume 33. [Google Scholar]
- Zvarevashe, K.; Olugbara, O. Ensemble Learning of Hybrid Acoustic Features for Speech Emotion Recognition. Algorithms 2020, 13, 70. [Google Scholar] [CrossRef]


| Feature | Mathematical Functions and References |
|---|---|
| Pitch | [38] |
| Harmonics-to-noise ratio (HNR) | [39] |
| Zero-Crossing Rate (ZCR) | |
| Mel-frequency cepstral coefficients (MFCC) | [40] |
| Gammatone cepstral coefficients (GTCC) | [41] |
| Mean frequency | Mean of power spectrum from the signal |
| Median frequency | Median of power spectrum from the signal |
| Signal energy (E) | |
| Spectral centroid (c) | [42] |
| Spectral rolloff point (r) | [42] |
| Metric | Mathematical Formula |
|---|---|
| Accuracy (ACC) | |
| True positive rate (TPR) | |
| True negative rate (TNR) | |
| Positive predictive value (PPV) | |
| Negative predictive value (NPV) | |
| F1 score | |
| Cohen’s kappa | |
| Matthew’s correlation coefficient (MCC) |
| Demographics | Depression | Dementia | |
|---|---|---|---|
| Symptomatic | n (dataset/subject) | 300/77 | 119/43 |
| age (mean ± s.d. years) | 50.4 ± 15.1 | 80.8 ± 8.3 | |
| sex (female %) | 54.5 | 72.1 | |
| Age-matched | n (dataset/subject) | 89/24 | 88/29 |
| age (mean ± s.d. years) | 67.8 ± 7.1 | 77.0 ± 7.5 | |
| sex (female %) | 83.3 | 72.4 | |
| Young depression, Old dementia | n (dataset/subject) | 211/53 | 31/14 |
| age (mean ± s.d. years) | 42.5 ± 10.4 | 88.5 ± 1.9 | |
| sex (female %) | 41.5 | 71.4 | |
| Feature Description | Pearson’s Correlation | |
|---|---|---|
| HAMD Depression | MMSE Dementia | |
| mean GTCC_1 | −0.346 | 0.226 |
| mean MFCC_1 | −0.346 | 0.226 |
| median GTCC_1 | −0.325 | 0.219 |
| median GTCC_3 | −0.224 | 0.230 |
| median MFCC_1 | −0.325 | 0.219 |
| SD GTCC_12 | −0.218 | 0.257 |
| SD MFCC_4 | −0.289 | 0.329 |
| SD MFCC_7 | −0.221 | 0.274 |
| SD MFCC_12 | −0.259 | 0.224 |
| Metric | kMeans (%) |
|---|---|
| Accuracy (ACC) | 62.7 |
| True positive rate (TPR) | 89.9 |
| True negative rate (TNR) | 35.2 |
| Positive predictive value (PPV) | 58.3 |
| Negative predictive value (NPV) | 77.5 |
| F1 score | 70.8 |
| Cohen’s kappa | 25.2 |
| Matthew’s correlation coefficient (MCC) | 30.0 |
| Metrices | Training (Mean ± SD %) | Testing (Mean ± SD %) | ||
|---|---|---|---|---|
| No LASSO | With LASSO | No LASSO | With LASSO | |
| Accuracy (ACC) | 90.1 ± 2.4 | 95.2 ± 0.7 | 84.2 ± 5.3 | 93.3 ± 7.7 |
| True positive rate (TPR) | 94.4 ± 0.9 | 98.3 ± 0.9 | 88.8 ± 10.5 | 97.8 ± 4.7 |
| True negative rate (TNR) | 85.7 ± 4.6 | 92.6 ± 1.2 | 79.6 ± 11.5 | 89.4 ± 13.7 |
| Positive predictive value (PPV) | 87.1 ± 3.5 | 92.1 ± 1.2 | 82.5 ± 8.8 | 90.4 ± 11.7 |
| Negative predictive value (NPV) | 93.8 ± 1.0 | 98.4 ± 0.8 | 88.8 ± 8.9 | 98.0 ± 4.2 |
| F1 score | 90.6 ± 2.0 | 95.1 ± 0.7 | 84.8 ± 5.5 | 93.5 ± 7.2 |
| Cohen’s kappa | 80.2 ± 4.7 | 90.5 ± 1.4 | 68.3 ± 10.5 | 86.7 ± 15.0 |
| Matthew’s correlation coefficient (MCC) | 80.5 ± 4.4 | 90.6 ± 1.4 | 69.8 ± 10.3 | 87.8 ± 13.5 |
| Metrices | Training (Mean ± SD %) | Testing (Mean ± SD %) | ||
|---|---|---|---|---|
| No LASSO | With LASSO | No LASSO | With LASSO | |
| Accuracy (ACC) | 91.5 ± 3.1 | 94.6 ± 8.1 | 79.1 ± 7.6 | 89.7 ± 11.4 |
| True positive rate (TPR) | 96.4 ± 2.4 | 99.1 ± 1.0 | 85.3 ± 10.8 | 96.7 ± 5.4 |
| True negative rate (TNR) | 86.5 ± 4.0 | 90.0 ± 16.1 | 72.6 ± 14.3 | 83.1 ± 22.9 |
| Positive predictive value (PPV) | 87.9 ± 3.5 | 92.3 ± 9.9 | 76.9 ± 8.3 | 87.6 ± 13.8 |
| Negative predictive value (NPV) | 95.9 ± 2.7 | 98.9 ± 1.2 | 84.1 ± 9.9 | 96.9 ± 5.0 |
| F1 score | 91.9 ± 2.9 | 95.3 ± 6.1 | 80.3 ± 6.9 | 91.1 ± 8.2 |
| Cohen’s kappa | 82.9 ± 6.3 | 89.2 ± 16.2 | 58.0 ± 15.2 | 79.7 ± 21.7 |
| Matthew’s correlation coefficient (MCC) | 83.3 ± 6.2 | 90.1 ± 13.7 | 59.4 ± 14.6 | 81.8 ± 17.9 |
| Metrices | Training (Mean ± SD %) | Testing (Mean ± SD %) | ||
|---|---|---|---|---|
| No LASSO | With LASSO | No LASSO | With LASSO | |
| Accuracy (ACC) | 90.4 ± 6.2 | 95.6 ± 1.9 | 75.3 ± 12.4 | 88.7 ± 7.9 |
| True positive rate (TPR) | 96.4 ± 2.9 | 98.8 ± 1.0 | 77.5 ± 16.6 | 91.0 ± 10.3 |
| True negative rate (TNR) | 84.3 ± 10.2 | 92.4 ± 3.0 | 72.9 ± 17.3 | 86.1 ± 13.1 |
| Positive predictive value (PPV) | 86.7 ± 7.9 | 93.0 ± 2.6 | 75.6 ± 13.8 | 88.3 ± 10.4 |
| Negative predictive value (NPV) | 95.7 ± 3.7 | 98.6 ± 1.2 | 77.6 ± 14.6 | 91.3 ± 8.9 |
| F1 score | 91.2 ± 5.4 | 95.8 ± 1.7 | 75.7 ± 12.5 | 89.1 ± 7.9 |
| Cohen’s kappa | 80.8 ± 12.3 | 91.2 ± 3.7 | 50.5 ± 24.8 | 77.3 ± 15.9 |
| Matthew’s correlation coefficient (MCC) | 81.5 ± 11.7 | 91.4 ± 3.6 | 51.8 ± 25.0 | 78.3 ± 15.4 |
| Metrics | Linear | Polynomial | RBF | |||
|---|---|---|---|---|---|---|
| All Feats | LASSO | All Feats | LASSO | All Feats | LASSO | |
| Accuracy (ACC) | 83.5 | 82.6 | 80.2 | 81.4 | 65.7 | 81.0 |
| True positive rate (TPR) | 87.7 | 83.9 | 82.5 | 82.9 | 66.8 | 82.9 |
| True negative rate (TNR) | 54.8 | 74.2 | 64.5 | 71.0 | 58.1 | 67.7 |
| Positive predictive value (PPV) | 93.0 | 95.7 | 94.1 | 95.1 | 91.6 | 94.6 |
| Negative predictive value (NPV) | 39.5 | 40.4 | 35.1 | 37.9 | 20.5 | 36.8 |
| F1 score | 90.2 | 89.4 | 87.9 | 88.6 | 77.3 | 88.4 |
| Cohen’s kappa | 36.5 | 42.8 | 34.6 | 39.3 | 13.9 | 37.3 |
| Matthew’s correlation coefficient (MCC) | 37.2 | 45.7 | 37.0 | 42.2 | 17.3 | 39.9 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sumali, B.; Mitsukura, Y.; Liang, K.-c.; Yoshimura, M.; Kitazawa, M.; Takamiya, A.; Fujita, T.; Mimura, M.; Kishimoto, T. Speech Quality Feature Analysis for Classification of Depression and Dementia Patients. Sensors 2020, 20, 3599. https://doi.org/10.3390/s20123599
Sumali B, Mitsukura Y, Liang K-c, Yoshimura M, Kitazawa M, Takamiya A, Fujita T, Mimura M, Kishimoto T. Speech Quality Feature Analysis for Classification of Depression and Dementia Patients. Sensors. 2020; 20(12):3599. https://doi.org/10.3390/s20123599
Chicago/Turabian StyleSumali, Brian, Yasue Mitsukura, Kuo-ching Liang, Michitaka Yoshimura, Momoko Kitazawa, Akihiro Takamiya, Takanori Fujita, Masaru Mimura, and Taishiro Kishimoto. 2020. "Speech Quality Feature Analysis for Classification of Depression and Dementia Patients" Sensors 20, no. 12: 3599. https://doi.org/10.3390/s20123599
APA StyleSumali, B., Mitsukura, Y., Liang, K.-c., Yoshimura, M., Kitazawa, M., Takamiya, A., Fujita, T., Mimura, M., & Kishimoto, T. (2020). Speech Quality Feature Analysis for Classification of Depression and Dementia Patients. Sensors, 20(12), 3599. https://doi.org/10.3390/s20123599





