Proteomic Analysis of a Rat Streptozotocin Model Shows Dysregulated Biological Pathways Implicated in Alzheimer’s Disease
Abstract
1. Introduction
2. Results
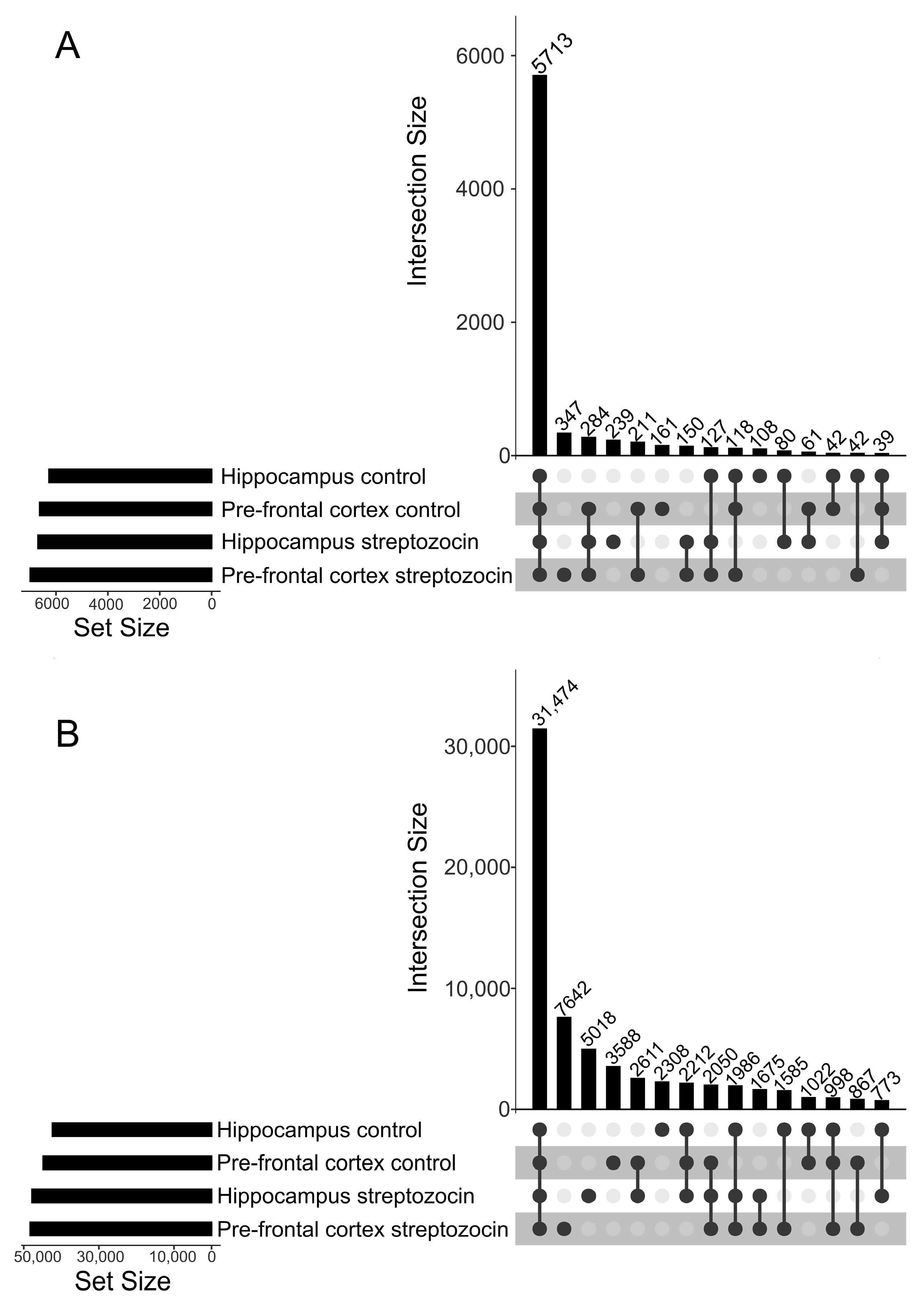
2.1. Overview of the ICV-STZ Model’s Proteome
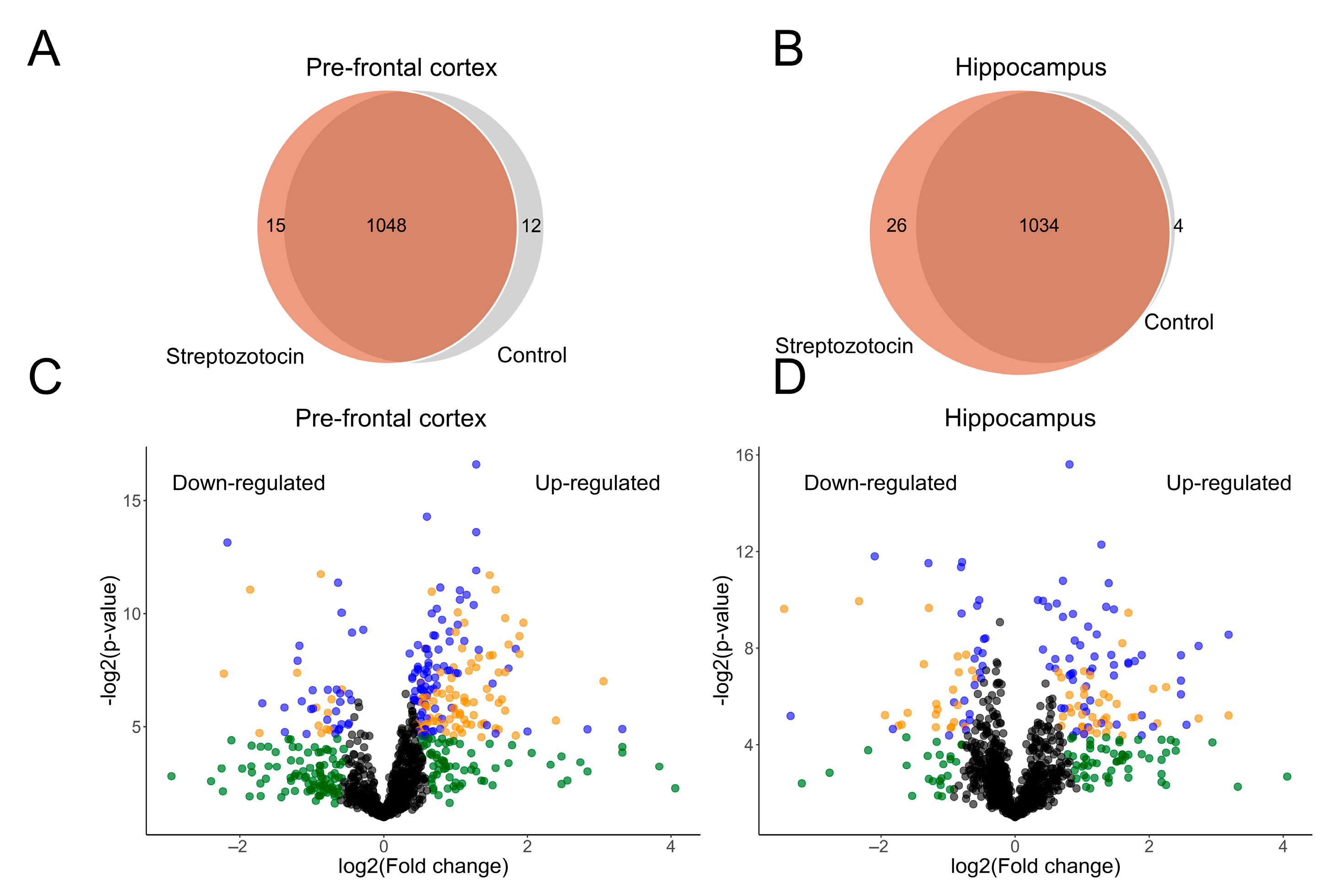
2.2. Identification of Differentially Abundant Proteins (DAPs) in the ICV-STZ Model’s Proteome
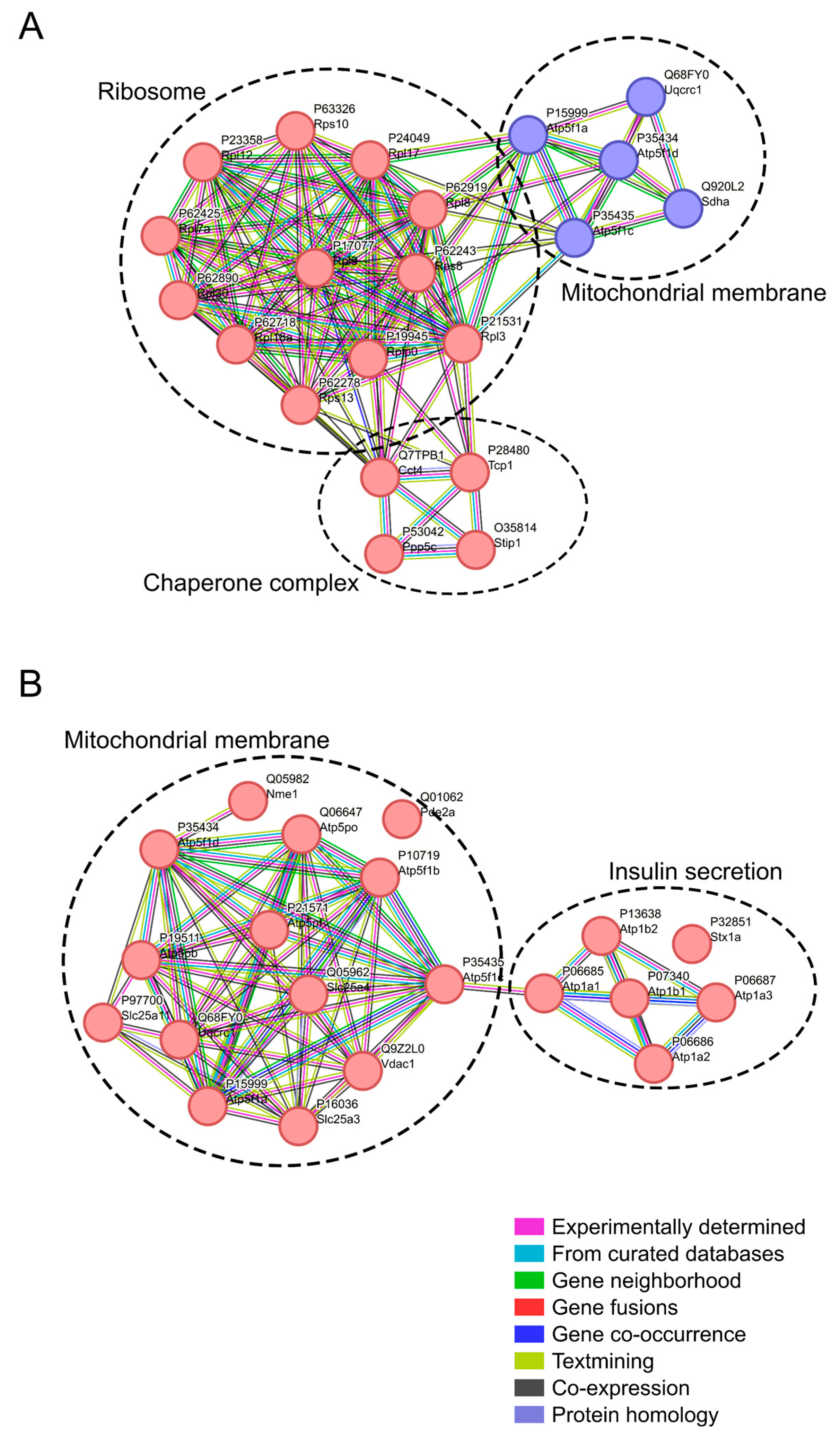
2.3. Identification of Dysregulated Pathways in the ICV-STZ Model
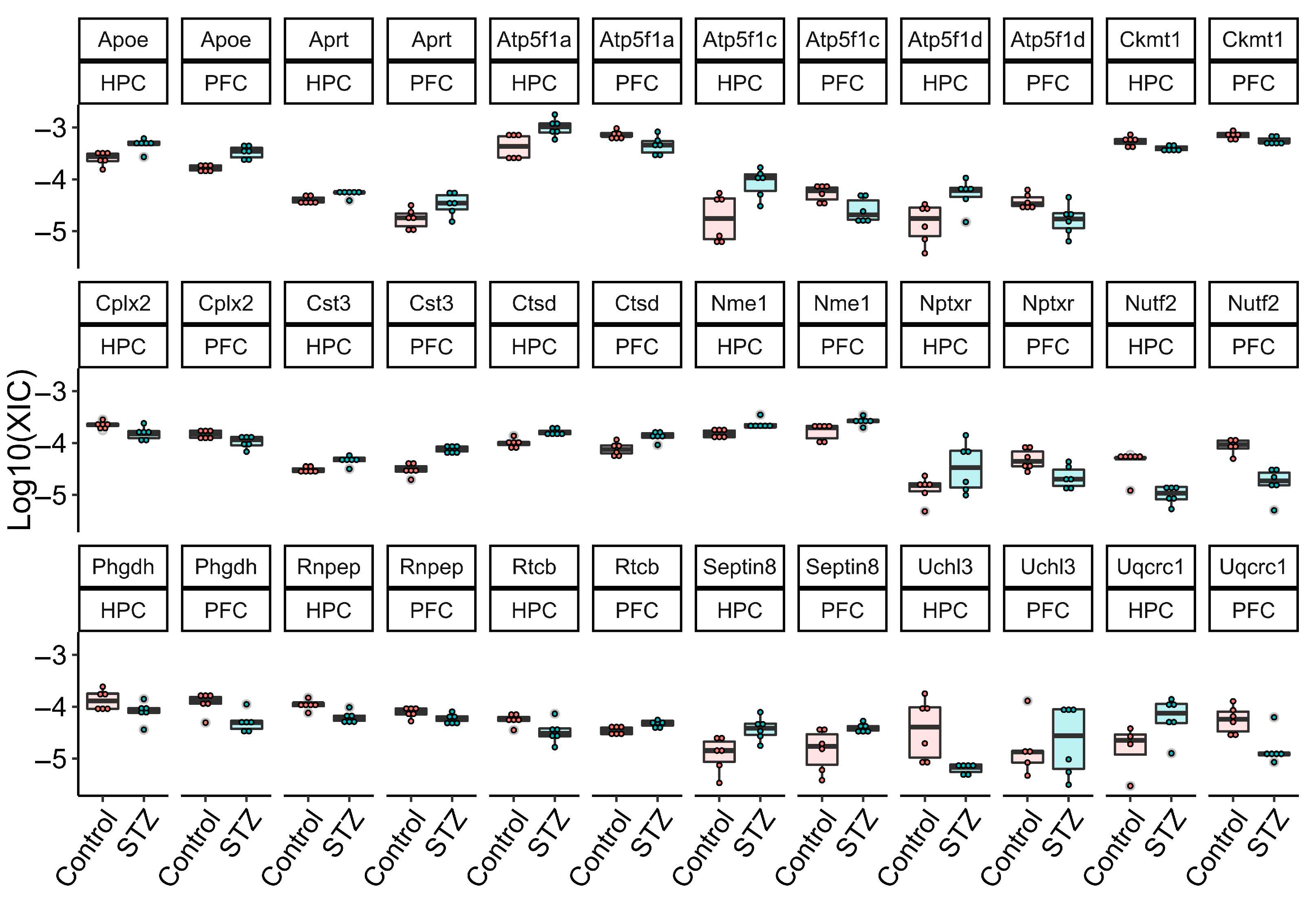
2.4. Experimental Validation of mRNAs through qRT-PCR
3. Discussion
4. Materials and Methods
4.1. Animals
4.2. Stereotaxic Surgery
4.3. Sample Preparation
4.4. Desalting
4.5. Mass Spectrometry
4.6. Protein Identification
4.7. Protein Quantification
4.8. GO Enrichment and Network Analysis
4.9. Quantitative Real Time Polymerase Chain Reaction (qRT-PCR)
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Stelzmann, R.A.; Norman Schnitzlein, H.; Reed Murtagh, F. An English Translation of Alzheimer’s 1907 Paper, “Uber Eine Eigenartige Erkankung Der Hirnrinde”. Clin. Anat. 1995, 8, 429–431. [Google Scholar] [CrossRef]
- Patterson, C.; Lynch, C.; Bliss, A.; Lefevre, M.; Weidner, W. World Alzheimer Report 2018; ADI: London, UK, 2018. [Google Scholar]
- Venkateshappa, C.; Harish, G.; Mahadevan, A.; Srinivas Bharath, M.M.; Shankar, S.K. Elevated Oxidative Stress and Decreased Antioxidant Function in the Human Hippocampus and Frontal Cortex with Increasing Age: Implications for Neurodegeneration in Alzheimer’s Disease. Neurochem. Res. 2012, 37, 1601–1614. [Google Scholar] [CrossRef] [PubMed]
- Preston, A.R.; Eichenbaum, H. Interplay of Hippocampus and Prefrontal Cortex in Memory. Curr. Biol. 2013, 23, R764–R773. [Google Scholar] [CrossRef] [PubMed]
- Reitz, C.; Rogaeva, E.; Beecham, G.W. Late-Onset vs Nonmendelian Early-Onset Alzheimer Disease. Neurol. Genet. 2020, 6, e512. [Google Scholar] [CrossRef] [PubMed]
- O’Brien, R.J.; Wong, P.C. Amyloid Precursor Protein Processing and Alzheimer’s Disease. Annu. Rev. Neurosci. 2011, 34, 185–204. [Google Scholar] [CrossRef] [PubMed]
- Alonso, A.C.; Zaidi, T.; Grundke-Iqbal, I.; Iqbal, K. Role of Abnormally Phosphorylated Tau in the Breakdown of Microtubules in Alzheimer Disease. Proc. Natl. Acad. Sci. USA 1994, 91, 5562–5566. [Google Scholar] [CrossRef] [PubMed]
- Hoyer, S.; Oesterreich, K.; Wagner, O. Glucose Metabolism as the Site of the Primary Abnormality in Early-Onset Dementia of Alzheimer Type? J. Neurol. 1988, 235, 143–148. [Google Scholar] [CrossRef] [PubMed]
- Hoyer, S.; Nitsch, R.; Oesterreich, K. Predominant Abnormality in Cerebral Glucose Utilization in Late-Onset Dementia of the Alzheimer Type: A Cross-Sectional Comparison against Advanced Late-Onset and Incipient Early-Onset Cases. J. Neural Transm. Park. Dis. Dement. Sect. 1991, 3, 1–14. [Google Scholar] [CrossRef]
- Hoyer, S. The Brain Insulin Signal Transduction System and Sporadic (Type II) Alzheimer Disease: An Update. J. Neural Transm. 2002, 109, 341–360. [Google Scholar] [CrossRef]
- Junod, A.; Lambert, A.E.; Stauffacher, W.; Renold, A.E. Diabetogenic Action of Streptozotocin: Relationship of Dose to Metabolic Response. J. Clin. Investig. 1969, 48, 2129–2139. [Google Scholar] [CrossRef]
- Ganda, O.P.; Rossini, A.A.; Like, A.A. Studies on Streptozotocin Diabetes. Diabetes 1976, 25, 595–603. [Google Scholar] [CrossRef]
- Hoyer, S.; Prem, L.; Sorbi, S.; Amaducci, L. Stimulation of Glycolytic Key Enzymes in Cerebral Cortex by Insulin. Neuroreport 1993, 4, 991. [Google Scholar] [CrossRef]
- Duelli, R.; Schröck, H.; Kuschinsky, W.; Hoyer, S. Intracerebroventricular Injection of Streptozotocin Induces Discrete Local Changes in Cerebral Glucose Utilization in Rats. Int. J. Dev. Neurosci. 1994, 12, 737–743. [Google Scholar] [CrossRef]
- Mayer, G.; Nitsch, R.; Hoyer, S. Effects of Changes in Peripheral and Cerebral Glucose Metabolism on Locomotor Activity, Learning and Memory in Adult Male Rats. Brain Res. 1990, 532, 95–100. [Google Scholar] [CrossRef]
- Knezovic, A.; Osmanovic-Barilar, J.; Curlin, M.; Hof, P.R.; Simic, G.; Riederer, P.; Salkovic-Petrisic, M. Staging of Cognitive Deficits and Neuropathological and Ultrastructural Changes in Streptozotocin-Induced Rat Model of Alzheimer’s Disease. J. Neural Transm. 2015, 122, 577–592. [Google Scholar] [CrossRef]
- Salkovic-Petrisic, M.; Hoyer, S. Central Insulin Resistance as a Trigger for Sporadic Alzheimer-like Pathology: An Experimental Approach. In Neuropsychiatric Disorders An Integrative Approach; Springer: Vienna, Austria, 2007; pp. 217–233. [Google Scholar]
- Knezovic, A.; Loncar, A.; Homolak, J.; Smailovic, U.; Osmanovic Barilar, J.; Ganoci, L.; Bozina, N.; Riederer, P.; Salkovic-Petrisic, M. Rat Brain Glucose Transporter-2, Insulin Receptor and Glial Expression Are Acute Targets of Intracerebroventricular Streptozotocin: Risk Factors for Sporadic Alzheimer’s Disease? J. Neural Transm. 2017, 124, 695–708. [Google Scholar] [CrossRef]
- Salkovic-Petrisic, M.; Knezovic, A.; Hoyer, S.; Riederer, P. What Have We Learned from the Streptozotocin-Induced Animal Model of Sporadic Alzheimer’s Disease, about the Therapeutic Strategies in Alzheimer’s Research. J. Neural Transm. 2013, 120, 233–252. [Google Scholar] [CrossRef] [PubMed]
- Moreira-Silva, D.; Carrettiero, D.C.; Oliveira, A.S.A.; Rodrigues, S.; dos Santos-Lopes, J.; Canas, P.M.; Cunha, R.A.; Almeida, M.C.; Ferreira, T.L. Anandamide Effects in a Streptozotocin-Induced Alzheimer’s Disease-Like Sporadic Dementia in Rats. Front. Neurosci. 2018, 12, 653. [Google Scholar] [CrossRef]
- Voronkov, D.N.; Stavrovskaya, A.V.; Stelmashook, E.V.; Genrikhs, E.E.; Isaev, N.K. Neurodegenerative Changes in Rat Brain in Streptozotocin Model of Alzheimer’s Disease. Bull. Exp. Biol. Med. 2019, 166, 793–796. [Google Scholar] [CrossRef] [PubMed]
- Grunblatt, E.; Hoyer, S.; Riederer, P. Gene Expression Profile in Streptozotocin Rat Model for Sporadic Alzheimer’s Disease. J. Neural Transm. 2004, 111, 367–386. [Google Scholar] [CrossRef] [PubMed]
- Ali, S.K.; Ali, R.H. Effects of Antidiabetic Agents on Alzheimer’s Disease Biomarkers in Experimentally Induced Hyperglycemic Rat Model by Streptozocin. PLoS ONE 2022, 17, e0271138. [Google Scholar] [CrossRef] [PubMed]
- Haytural, H.; Benfeitas, R.; Schedin-Weiss, S.; Bereczki, E.; Rezeli, M.; Unwin, R.D.; Wang, X.; Dammer, E.B.; Johnson, E.C.B.; Seyfried, N.T.; et al. Insights into the Changes in the Proteome of Alzheimer Disease Elucidated by a Meta-Analysis. Sci. Data 2021, 8, 312. [Google Scholar] [CrossRef] [PubMed]
- Gadhave, K.; Bolshette, N.; Ahire, A.; Pardeshi, R.; Thakur, K.; Trandafir, C.; Istrate, A.; Ahmed, S.; Lahkar, M.; Muresanu, D.F.; et al. The Ubiquitin Proteasomal System: A Potential Target for the Management of Alzheimer’s Disease. J. Cell. Mol. Med. 2016, 20, 1392–1407. [Google Scholar] [CrossRef]
- Eftekharzadeh, B.; Daigle, J.G.; Kapinos, L.E.; Coyne, A.; Schiantarelli, J.; Carlomagno, Y.; Cook, C.; Miller, S.J.; Dujardin, S.; Amaral, A.S.; et al. Tau Protein Disrupts Nucleocytoplasmic Transport in Alzheimer’s Disease. Neuron 2018, 99, 925–940.e7. [Google Scholar] [CrossRef]
- Perez Ortiz, J.M.; Swerdlow, R.H. Mitochondrial Dysfunction in Alzheimer’s Disease: Role in Pathogenesis and Novel Therapeutic Opportunities. Br. J. Pharmacol. 2019, 176, 3489–3507. [Google Scholar] [CrossRef] [PubMed]
- Carvalho, C.; Cardoso, S.; Correia, S.C.; Santos, R.X.; Santos, M.S.; Baldeiras, I.; Oliveira, C.R.; Moreira, P.I. Metabolic Alterations Induced by Sucrose Intake and Alzheimer’s Disease Promote Similar Brain Mitochondrial Abnormalities. Diabetes 2012, 61, 1234–1242. [Google Scholar] [CrossRef] [PubMed]
- Carvalho, C.; Santos, M.S.; Oliveira, C.R.; Moreira, P.I. Alzheimer’s Disease and Type 2 Diabetes-Related Alterations in Brain Mitochondria, Autophagy and Synaptic Markers. Biochim. Biophys. Acta (BBA)-Mol. Basis Dis. 2015, 1852, 1665–1675. [Google Scholar] [CrossRef] [PubMed]
- Park, J.; Won, J.; Seo, J.; Yeo, H.-G.; Kim, K.; Kim, Y.G.; Jeon, C.-Y.; Kam, M.K.; Kim, Y.-H.; Huh, J.-W.; et al. Streptozotocin Induces Alzheimer’s Disease-Like Pathology in Hippocampal Neuronal Cells via CDK5/Drp1-Mediated Mitochondrial Fragmentation. Front. Cell. Neurosci. 2020, 14, 235. [Google Scholar] [CrossRef]
- Qi, C.C.; Chen, X.X.; Gao, X.R.; Xu, J.X.; Liu, S.; Ge, J.F. Impaired Learning and Memory Ability Induced by a Bilaterally Hippocampal Injection of Streptozotocin in Mice: Involved With the Adaptive Changes of Synaptic Plasticity. Front. Aging Neurosci. 2021, 13, 633495. [Google Scholar] [CrossRef]
- Stefanova, N.A.; Ershov, N.I.; Maksimova, K.Y.; Muraleva, N.A.; Tyumentsev, M.A.; Kolosova, N.G. The Rat Prefrontal-Cortex Transcriptome: Effects of Aging and Sporadic Alzheimer’s Disease–Like Pathology. J. Gerontol. Ser. A 2019, 74, 33–43. [Google Scholar] [CrossRef]
- Reddy, P.H.; McWeeney, S.; Park, B.S.; Manczak, M.; Gutala, R.V.; Partovi, D.; Jung, Y.; Yau, V.; Searles, R.; Mori, M.; et al. Gene Expression Profiles of Transcripts in Amyloid Precursor Protein Transgenic Mice: Up-Regulation of Mitochondrial Metabolism and Apoptotic Genes Is an Early Cellular Change in Alzheimer’s Disease. Hum. Mol. Genet. 2004, 13, 1225–1240. [Google Scholar] [CrossRef]
- Hamezah, H.S.; Durani, L.W.; Yanagisawa, D.; Ibrahim, N.F.; Aizat, W.M.; Bellier, J.P.; Makpol, S.; Ngah, W.Z.W.; Damanhuri, H.A.; Tooyama, I. Proteome Profiling in the Hippocampus, Medial Prefrontal Cortex, and Striatum of Aging Rat. Exp. Gerontol. 2018, 111, 53–64. [Google Scholar] [CrossRef] [PubMed]
- Adav, S.S.; Park, J.E.; Sze, S.K. Quantitative Profiling Brain Proteomes Revealed Mitochondrial Dysfunction in Alzheimer’s Disease. Mol. Brain 2019, 12, 8. [Google Scholar] [CrossRef]
- Yoon, J.H.; Hwang, J.; Son, S.U.; Choi, J.; You, S.-W.; Park, H.; Cha, S.-Y.; Maeng, S. How Can Insulin Resistance Cause Alzheimer’s Disease? Int. J. Mol. Sci. 2023, 24, 3506. [Google Scholar] [CrossRef] [PubMed]
- Femminella, G.D.; Livingston, N.R.; Raza, S.; van der Doef, T.; Frangou, E.; Love, S.; Busza, G.; Calsolaro, V.; Carver, S.; Holmes, C.; et al. Does Insulin Resistance Influence Neurodegeneration in Non-Diabetic Alzheimer’s Subjects? Alzheimers Res. Ther. 2021, 13, 47. [Google Scholar] [CrossRef]
- Hernández-Ortega, K.; Garcia-Esparcia, P.; Gil, L.; Lucas, J.J.; Ferrer, I. Altered Machinery of Protein Synthesis in Alzheimer’s: From the Nucleolus to the Ribosome. Brain Pathol. 2016, 26, 593–605. [Google Scholar] [CrossRef] [PubMed]
- Garcia-Esparcia, P.; Sideris-Lampretsas, G.; Hernandez-Ortega, K.; Grau-Rivera, O.; Sklaviadis, T.; Gelpi, E.; Ferrer, I. Altered Mechanisms of Protein Synthesis in Frontal Cortex in Alzheimer Disease and a Mouse Model. Am. J. Neurodegener. Dis. 2017, 6, 15–25. [Google Scholar]
- Suzuki, M.; Tezuka, K.; Handa, T.; Sato, R.; Takeuchi, H.; Takao, M.; Tano, M.; Uchida, Y. Upregulation of Ribosome Complexes at the Blood-Brain Barrier in Alzheimer’s Disease Patients. J. Cereb. Blood Flow Metab. 2022, 42, 2134–2150. [Google Scholar] [CrossRef]
- Ashraf, G.; Greig, N.; Khan, T.; Hassan, I.; Tabrez, S.; Shakil, S.; Sheikh, I.; Zaidi, S.; Akram, M.; Jabir, N.; et al. Protein Misfolding and Aggregation in Alzheimer’s Disease and Type 2 Diabetes Mellitus. CNS Neurol. Disord. Drug Targets 2014, 13, 1280–1293. [Google Scholar] [CrossRef]
- Håkansson, K.; Huh, C.; Grubb, A.; Karlsson, S.; Abrahamson, M. Mouse and Rat Cystatin C: Escherichia Coli Production, Characterization and Tissue Distribution. Comp. Biochem. Physiol. B Biochem. Mol. Biol. 1996, 114, 303–311. [Google Scholar] [CrossRef]
- Mi, W.; Jung, S.S.; Yu, H.; Schmidt, S.D.; Nixon, R.A.; Mathews, P.M.; Tagliavini, F.; Levy, E. Complexes of Amyloid-β and Cystatin C in the Human Central Nervous System. J. Alzheimer’s Dis. 2009, 18, 273–280. [Google Scholar] [CrossRef]
- Anantha, J.; Goulding, S.R.; Wyatt, S.L.; Concannon, R.M.; Collins, L.M.; Sullivan, A.M.; O’Keeffe, G.W. STRAP and NME1 Mediate the Neurite Growth-Promoting Effects of the Neurotrophic Factor GDF5. iScience 2020, 23, 101457. [Google Scholar] [CrossRef]
- Ansoleaga, B.; Jové, M.; Schlüter, A.; Garcia-Esparcia, P.; Moreno, J.; Pujol, A.; Pamplona, R.; Portero-Otín, M.; Ferrer, I. Deregulation of Purine Metabolism in Alzheimer’s Disease. Neurobiol. Aging 2015, 36, 68–80. [Google Scholar] [CrossRef]
- Pedrero-Prieto, C.M.; Flores-Cuadrado, A.; Saiz-Sánchez, D.; Úbeda-Bañón, I.; Frontiñán-Rubio, J.; Alcaín, F.J.; Mateos-Hernández, L.; de la Fuente, J.; Durán-Prado, M.; Villar, M.; et al. Human Amyloid-β Enriched Extracts: Evaluation of in Vitro and in Vivo Internalization and Molecular Characterization. Alzheimers Res. Ther. 2019, 11, 56. [Google Scholar] [CrossRef] [PubMed]
- Yang, Y.S.; Strittmatter, S.M. The Reticulons: A Family of Proteins with Diverse Functions. Genome Biol. 2007, 8, 234. [Google Scholar] [CrossRef] [PubMed]
- Shi, Q.; Ge, Y.; He, W.; Hu, X.; Yan, R. RTN1 and RTN3 Protein Are Differentially Associated with Senile Plaques in Alzheimer’s Brains. Sci. Rep. 2017, 7, 6145. [Google Scholar] [CrossRef] [PubMed]
- Yan, R.; Fan, Q.; Zhou, J.; Vassar, R. Inhibiting BACE1 to Reverse Synaptic Dysfunctions in Alzheimer’s Disease. Neurosci. Biobehav. Rev. 2016, 65, 326–340. [Google Scholar] [CrossRef] [PubMed]
- Kulczyńska-Przybik, A.; Dulewicz, M.; Słowik, A.; Borawska, R.; Kułakowska, A.; Kochanowicz, J.; Mroczko, B. The Clinical Significance of Cerebrospinal Fluid Reticulon 4 (RTN4) Levels in the Differential Diagnosis of Neurodegenerative Diseases. J. Clin. Med. 2021, 10, 5281. [Google Scholar] [CrossRef] [PubMed]
- Lisman, J.; Yasuda, R.; Raghavachari, S. Mechanisms of CaMKII Action in Long-Term Potentiation. Nat. Rev. Neurosci. 2012, 13, 169–182. [Google Scholar] [CrossRef] [PubMed]
- Fang, X.; Tang, W.; Yang, F.; Lu, W.; Cai, J.; Ni, J.; Zhang, J.; Tang, W.; Li, T.; Zhang, D.-F.; et al. A Comprehensive Analysis of the CaMK2A Gene and Susceptibility to Alzheimer’s Disease in the Han Chinese Population. Front. Aging Neurosci. 2019, 11, 84. [Google Scholar] [CrossRef]
- Dunckley, T.; Beach, T.G.; Ramsey, K.E.; Grover, A.; Mastroeni, D.; Walker, D.G.; LaFleur, B.J.; Coon, K.D.; Brown, K.M.; Caselli, R.; et al. Gene Expression Correlates of Neurofibrillary Tangles in Alzheimer’s Disease. Neurobiol. Aging 2006, 27, 1359–1371. [Google Scholar] [CrossRef] [PubMed]
- Kurihara, L.J. Loss of Uch-L1 and Uch-L3 Leads to Neurodegeneration, Posterior Paralysis and Dysphagia. Hum. Mol. Genet. 2001, 10, 1963–1970. [Google Scholar] [CrossRef]
- Chafe, S.C.; Pierce, J.B.; Mangroo, D. Nuclear-Cytoplasmic Trafficking of NTF2, the Nuclear Import Receptor for the RanGTPase, Is Subjected to Regulation. PLoS ONE 2012, 7, e42501. [Google Scholar] [CrossRef] [PubMed]
- Sheffield, L.G.; Miskiewicz, H.B.; Tannenbaum, L.B.; Mirra, S.S. Nuclear Pore Complex Proteins in Alzheimer Disease. J. Neuropathol. Exp. Neurol. 2006, 65, 45–54. [Google Scholar] [CrossRef] [PubMed]
- Wang, X.; Zhou, X.; Uberseder, B.; Lee, J.; Latimer, C.S.; Furdui, C.M.; Keene, C.D.; Montine, T.J.; Register, T.C.; Craft, S.; et al. Isoform-Specific Dysregulation of AMP-Activated Protein Kinase Signaling in a Non-Human Primate Model of Alzheimer’s Disease. Neurobiol. Dis. 2021, 158, 105463. [Google Scholar] [CrossRef] [PubMed]
- Bassani, T.B.; Bonato, J.M.; Machado, M.M.F.; Cóppola-Segovia, V.; Moura, E.L.R.; Zanata, S.M.; Oliveira, R.M.M.W.; Vital, M.A.B.F. Decrease in Adult Neurogenesis and Neuroinflammation Are Involved in Spatial Memory Impairment in the Streptozotocin-Induced Model of Sporadic Alzheimer’s Disease in Rats. Mol. Neurobiol. 2017, 55, 4280–4296. [Google Scholar] [CrossRef] [PubMed]
- Grieb, P. Intracerebroventricular Streptozotocin Injections as a Model of Alzheimer’s Disease: In Search of a Relevant Mechanism. Mol. Neurobiol. 2016, 53, 1741–1752. [Google Scholar] [CrossRef]
- Paxinos, G.; Watson, C. The Rat Brain in Stereotaxic Coordinates, 6th ed.; Academic Press: San Diego, CA, USA, 2007. [Google Scholar]
- Verissimo, D.C.A.; Camillo-Andrade, A.C.; Santos, M.D.M.; Sprengel, S.L.; Zanine, S.C.; Borba, L.A.B.; Carvalho, P.C.; Fischer, J.d.S.d.G. Proteomics Reveals Differentially Regulated Pathways When Comparing Grade 2 and 4 Astrocytomas. PLoS ONE 2023, 18, e0290087. [Google Scholar] [CrossRef]
- Rappsilber, J.; Ishihama, Y.; Mann, M. Stop and Go Extraction Tips for Matrix-Assisted Laser Desorption/Ionization, Nanoelectrospray, and LC/MS Sample Pretreatment in Proteomics. Anal. Chem. 2003, 75, 663–670. [Google Scholar] [CrossRef]
- Doellinger, J.; Schneider, A.; Hoeller, M.; Lasch, P. Sample Preparation by Easy Extraction and Digestion (SPEED)—A Universal, Rapid, and Detergent-Free Protocol for Proteomics Based on Acid Extraction. Mol. Cell. Proteom. 2020, 19, 209–222. [Google Scholar] [CrossRef]
- Santos, M.D.M.; Lima, D.B.; Fischer, J.S.G.; Clasen, M.A.; Kurt, L.U.; Camillo-Andrade, A.C.; Monteiro, L.C.; de Aquino, P.F.; Neves-Ferreira, A.G.C.; Valente, R.H.; et al. Simple, Efficient and Thorough Shotgun Proteomic Analysis with PatternLab V. Nat. Protoc. 2022, 17, 1553–1578. [Google Scholar] [CrossRef] [PubMed]
- Tavares, R.; de Miranda Scherer, N.; Pauletti, B.A.; Araújo, E.; Folador, E.L.; Espindola, G.; Ferreira, C.G.; Paes Leme, A.F.; de Oliveira, P.S.L.; Passetti, F. SpliceProt: A Protein Sequence Repository of Predicted Human Splice Variants. Proteomics 2014, 14, 181–185. [Google Scholar] [CrossRef] [PubMed]
- Boutet, E.; Lieberherr, D.; Tognolli, M.; Schneider, M.; Bairoch, A. UniProtKB/Swiss-Prot. In Plant Bioinformatics; Humana Press: Totowa, NJ, USA, 2007; pp. 89–112. [Google Scholar]
- Szklarczyk, D.; Gable, A.L.; Lyon, D.; Junge, A.; Wyder, S.; Huerta-Cepas, J.; Simonovic, M.; Doncheva, N.T.; Morris, J.H.; Bork, P.; et al. STRING V11: Protein–Protein Association Networks with Increased Coverage, Supporting Functional Discovery in Genome-Wide Experimental Datasets. Nucleic Acids Res. 2019, 47, D607–D613. [Google Scholar] [CrossRef] [PubMed]

| Pre-Frontal Cortex | Hippocampus | |||
|---|---|---|---|---|
| Streptozocin | Control | Streptozocin | Control | |
| N. of total proteins | 6992 | 6629 | 6693 | 6269 |
| N. of proteins with unique peptides | 2952 | 2766 | 2785 | 2565 |
| N. of peptides | 48,798 | 45,619 | 48,883 | 42,977 |
| N. of unique peptides | 23,738 | 21,974 | 23,494 | 20,839 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
da Silva, E.M.G.; Fischer, J.S.G.; Souza, I.d.L.S.; Andrade, A.C.C.; Souza, L.d.C.e.; Andrade, M.K.d.; Carvalho, P.C.; Souza, R.L.R.; Vital, M.A.B.F.; Passetti, F. Proteomic Analysis of a Rat Streptozotocin Model Shows Dysregulated Biological Pathways Implicated in Alzheimer’s Disease. Int. J. Mol. Sci. 2024, 25, 2772. https://doi.org/10.3390/ijms25052772
da Silva EMG, Fischer JSG, Souza IdLS, Andrade ACC, Souza LdCe, Andrade MKd, Carvalho PC, Souza RLR, Vital MABF, Passetti F. Proteomic Analysis of a Rat Streptozotocin Model Shows Dysregulated Biological Pathways Implicated in Alzheimer’s Disease. International Journal of Molecular Sciences. 2024; 25(5):2772. https://doi.org/10.3390/ijms25052772
Chicago/Turabian Styleda Silva, Esdras Matheus Gomes, Juliana S. G. Fischer, Isadora de Lourdes Signorini Souza, Amanda Caroline Camillo Andrade, Leonardo de Castro e Souza, Marcos Kaoann de Andrade, Paulo C. Carvalho, Ricardo Lehtonen Rodrigues Souza, Maria Aparecida Barbato Frazao Vital, and Fabio Passetti. 2024. "Proteomic Analysis of a Rat Streptozotocin Model Shows Dysregulated Biological Pathways Implicated in Alzheimer’s Disease" International Journal of Molecular Sciences 25, no. 5: 2772. https://doi.org/10.3390/ijms25052772
APA Styleda Silva, E. M. G., Fischer, J. S. G., Souza, I. d. L. S., Andrade, A. C. C., Souza, L. d. C. e., Andrade, M. K. d., Carvalho, P. C., Souza, R. L. R., Vital, M. A. B. F., & Passetti, F. (2024). Proteomic Analysis of a Rat Streptozotocin Model Shows Dysregulated Biological Pathways Implicated in Alzheimer’s Disease. International Journal of Molecular Sciences, 25(5), 2772. https://doi.org/10.3390/ijms25052772






