The Novel Benzothiazole Derivative PB11 Induces Apoptosis via the PI3K/AKT Signaling Pathway in Human Cancer Cell Lines
Abstract
1. Introduction
2. Results and Discussion
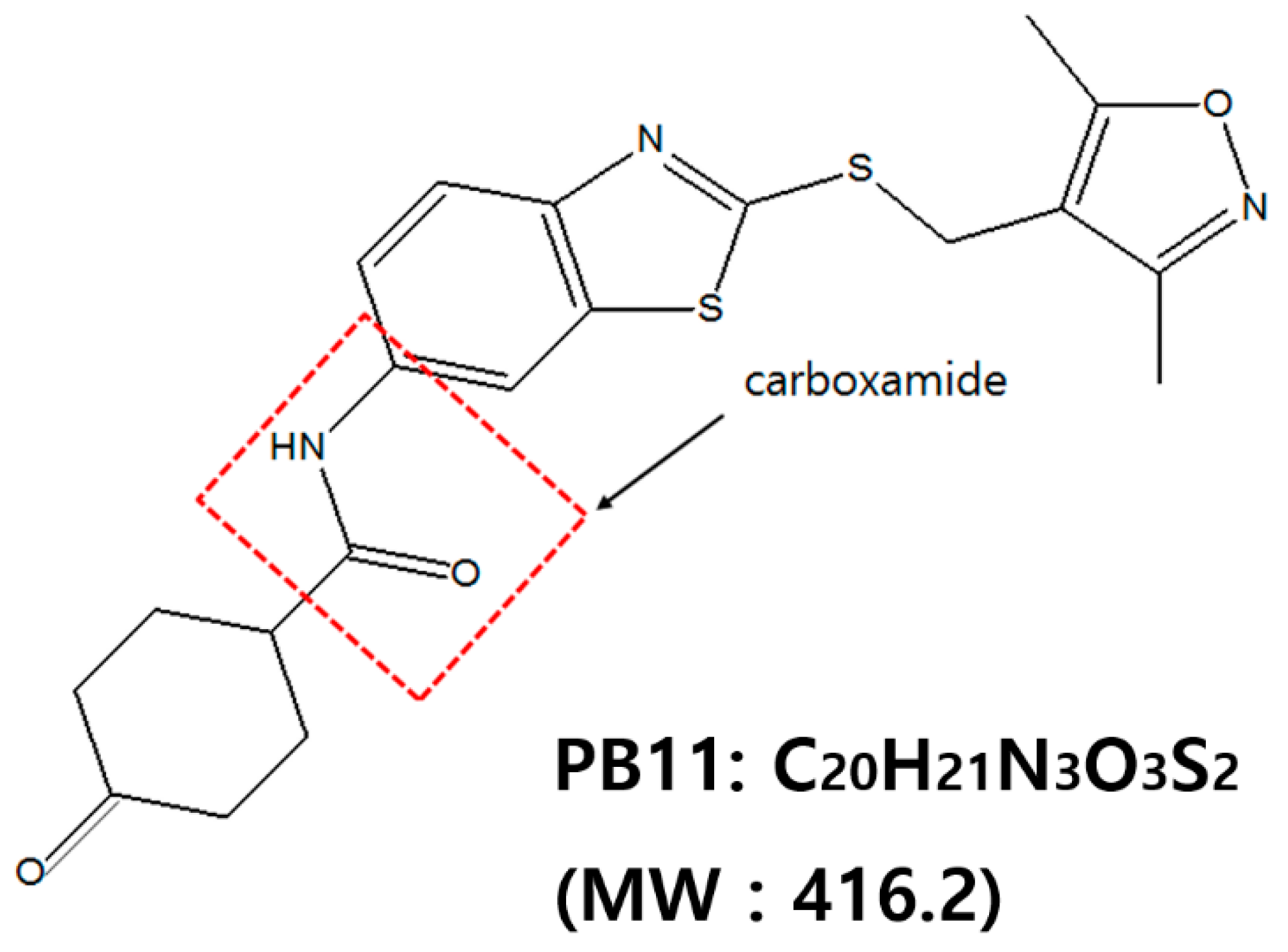
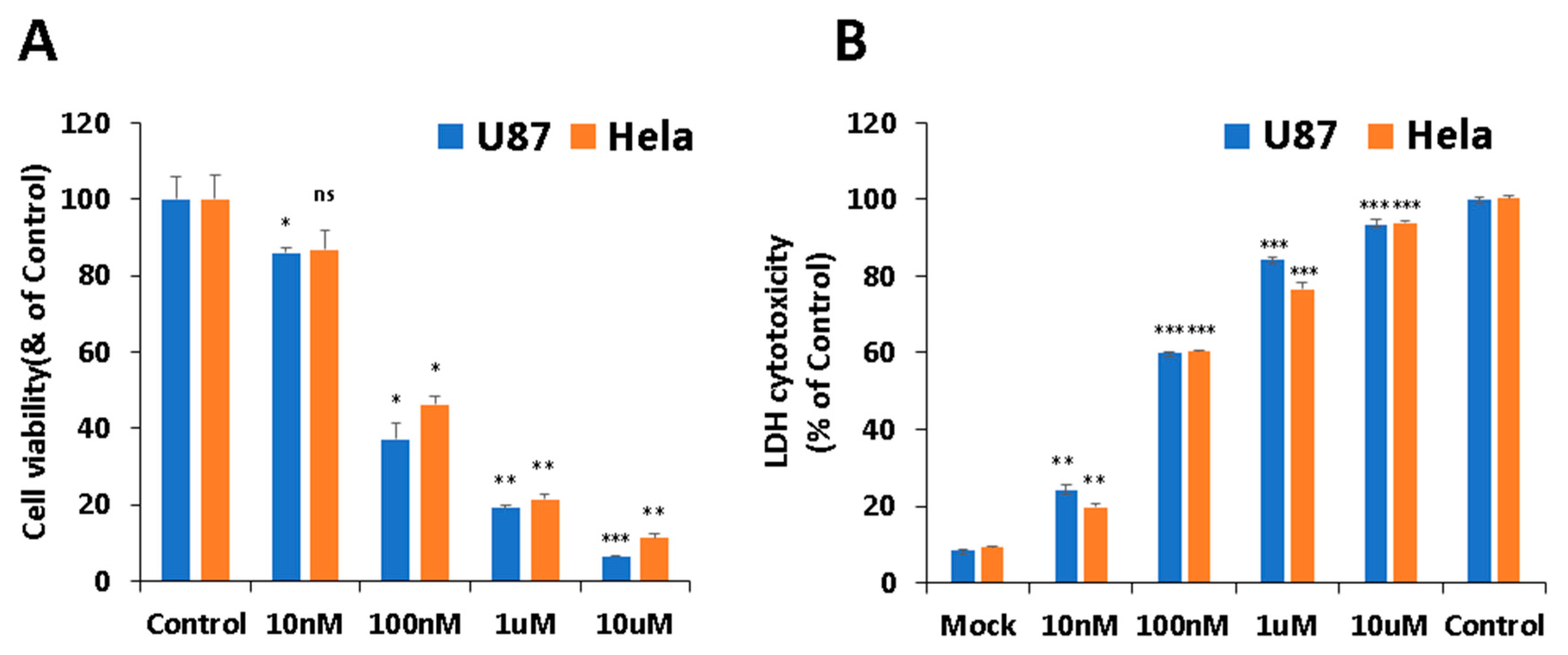
2.1. PB11 Is Highly Cytotoxic at the nM Scale
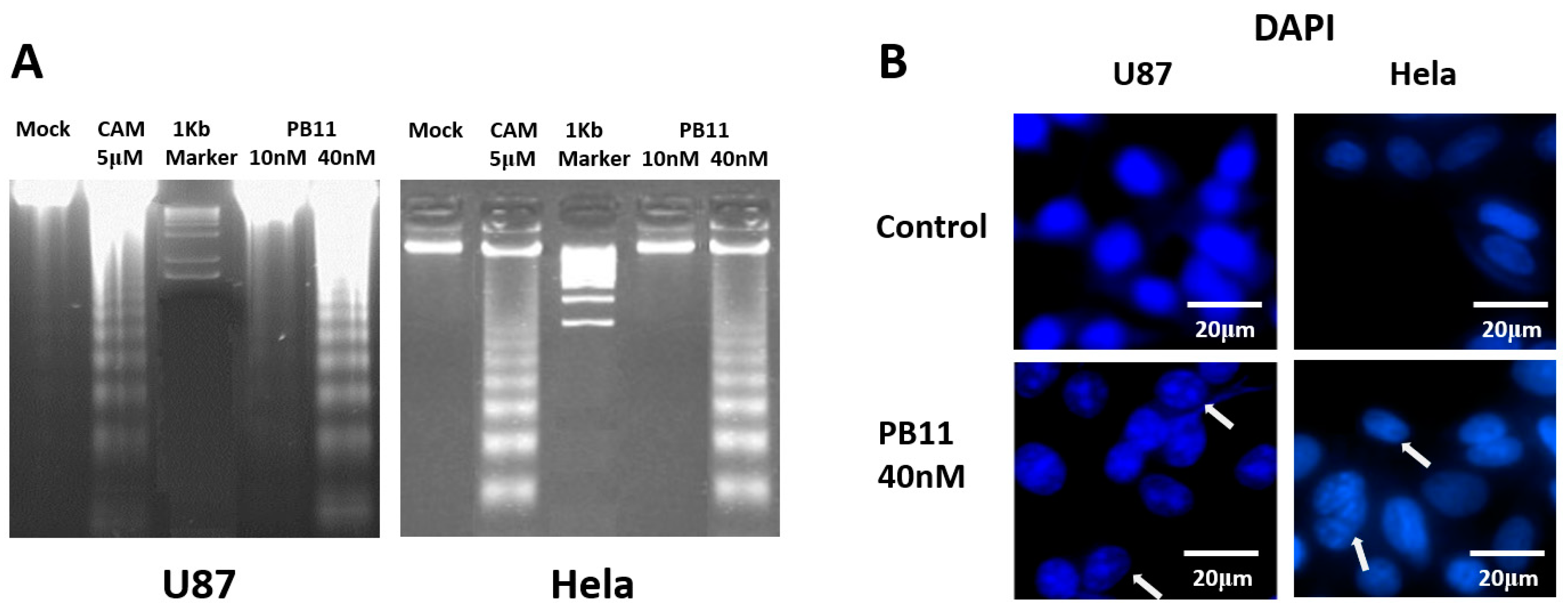
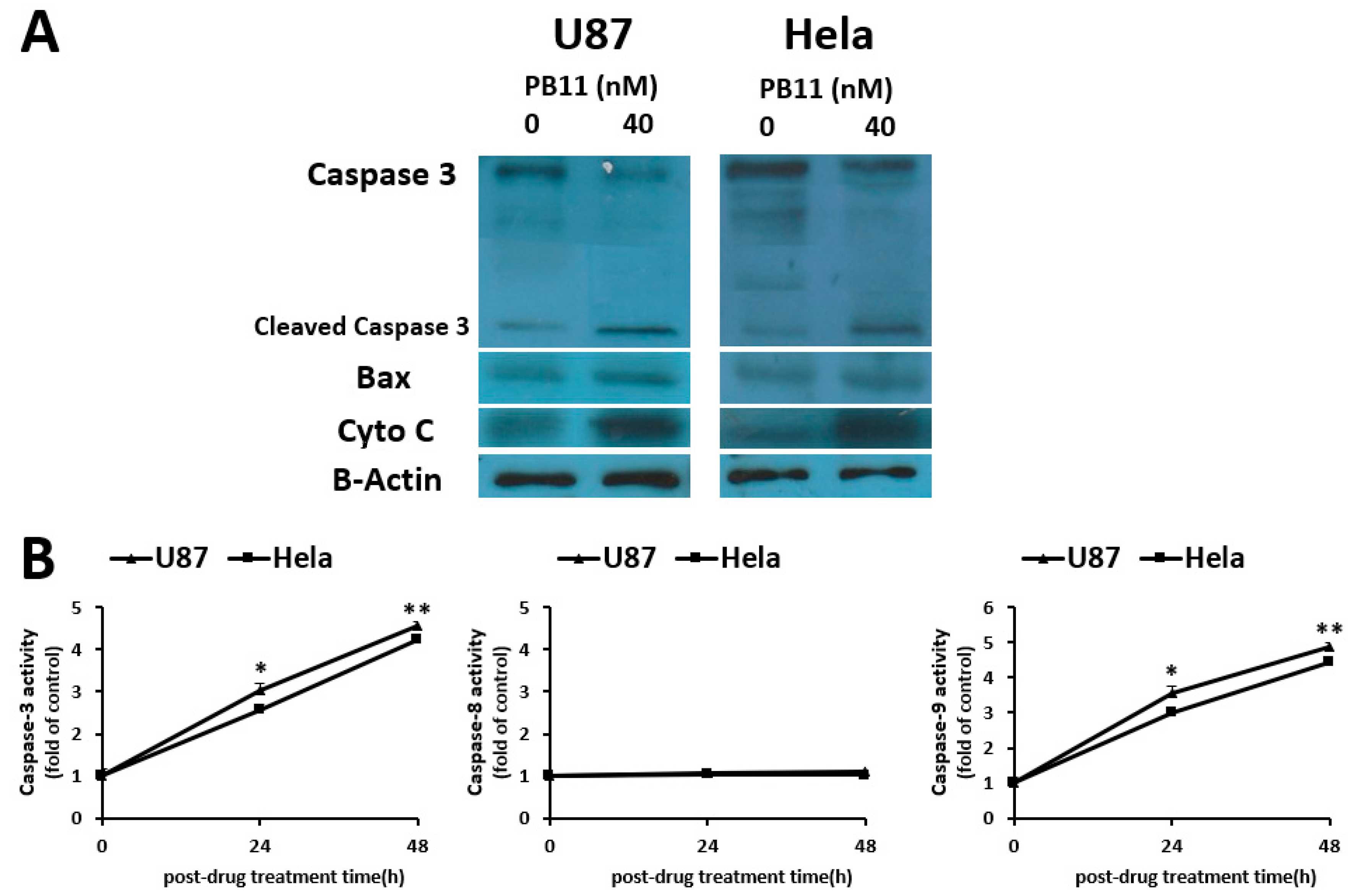
2.2. PB11 Induces Apoptosis through Mitochondria
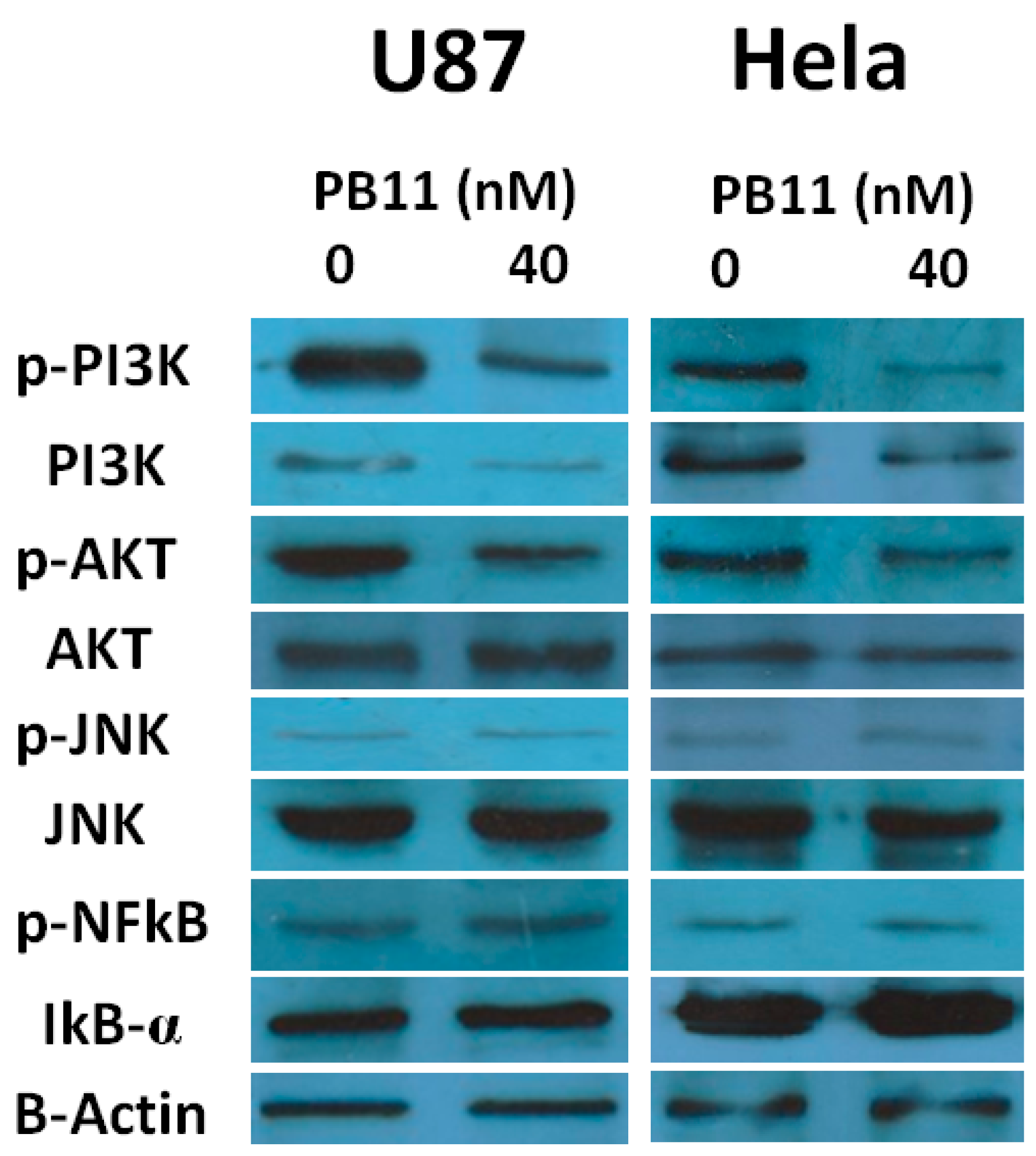
2.3. PB11 Induces Apoptosis via the PI3K/AKT Signaling Pathway
3. Materials and Methods
3.1. Reagents
3.2. Cell Culture
3.3. Cell Viability and Toxicity Tests
3.3.1. MTT Assay
3.3.2. LDH Cytotoxicity Assay
3.4. Assessment of Apoptosis
3.4.1. DNA-Fragmentation Assay
3.4.2. Evaluation of Nuclear Morphology
3.4.3. Caspase Activity Assay
3.5. Western Blotting Analysis
3.6. Statistical Analysis
4. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Palucka, A.K.; Coussens, L.M. The basis of oncoimmunology. Cell 2016, 164, 1233–1247. [Google Scholar] [CrossRef]
- Vacchelli, E.; Bloy, N.; Aranda, F.; Buqué, A.; Cremer, I.; Demaria, S.; Eggermont, A.; Formenti, S.C.; Fridman, W.H.; Fucikova, J.; et al. Trial watch: Immunotherapy plus radiation therapy for oncological indications. Oncoimmunology 2016, 5, e1214790. [Google Scholar] [CrossRef] [PubMed]
- DeNardo, D.G.; Brennan, D.J.; Rexhepaj, E.; Ruffell, B.; Shiao, S.L.; Madden, S.F.; Gallagher, W.M.; Wadhwani, N.; Keil, S.D.; Junaid, S.A.; et al. Leukocyte complexity predicts breast cancer survival and functionally regulates response to chemotherapy. Cancer Discov. 2011, 1, 54–67. [Google Scholar] [CrossRef] [PubMed]
- Mohanty, R.; Chowdhury, C.R.; Arega, S.; Sen, P.; Ganguly, P.; Ganguly, N. CAR T cell therapy: A new era for cancer treatment (Review). Oncol. Rep. 2019, 42, 2183–2195. [Google Scholar] [CrossRef] [PubMed]
- Wiemann, M.C.; Calabresi, P. Principles of current cancer chemotherapy. Compr. Ther. 1983, 9, 46–52. [Google Scholar] [PubMed]
- Makin, G. Targeting apoptosis in cancer chemotherapy. Expert. Opin. Ther. Targets 2002, 6, 73–84. [Google Scholar] [CrossRef]
- Choo, Z.; Loh, A.; Chen, Z.X. Destined to Die: Apoptosis and Pediatric Cancers. Cancers 2019, 11, 1623. [Google Scholar] [CrossRef] [PubMed]
- Irfan, A.; Batool, F.; Naqvi, S.A.Z.; Islam, A.; Osman, S.M.; Nocentini, A.; Alissa, S.A.; Supuran, C.T. Benzothiazole derivatives as anticancer agents. J. Enz. Inhib. Med. Chem. 2020, 35, 265–279. [Google Scholar] [CrossRef]
- Akhtar, J.; Khan, A.A.; Ali, Z. Structure-activity relationship (SAR) study and design strategies of nitrogen-containing heterocyclic moieties for their anticancer activities. Eur. J. Med. Chem. 2017, 5, 143–189. [Google Scholar] [CrossRef] [PubMed]
- Mats, M.E.; Shani, B.G.; Pasternak, L.; Uritsky, N.; Getter, T.; Viskind, O.; Eckel, J.; Cerasi, E.; Senderowitz, H.; Sasson, S.; et al. Synthesis and mechanism of hypoglycemic activity of benzothiazole derivatives. J. Med. Chem. 2013, 56, 5335–5350. [Google Scholar] [CrossRef]
- Padalkar, S.V.; Gupta, D.V.; Phatangare, R.K.; Patil, V.S.; Sekar, U.N. Synthesis of novel dipodal-benzimidazole, benzoxazole and benzothiazole from cyanuric chloride: Structural, photophysical and antimicrobial studies. J. Saudi Chem. Soc. 2014, 18, 262–268. [Google Scholar] [CrossRef]
- Venkatesh, P.; Pandeya, N.S. Synthesis, characterization and anti-inflammatory activity of some 2-amino benzothiazole derivatives. Int. J. Chem. Tech. Res. 2009, 1, 1354–1358. [Google Scholar]
- Liu, Y.; Wang, Y.; Dong, G.; Zhang, Y.; Wu, S.; Miao, Z.; Yao, J.; Zhang, W.; Sheng, C. Novel benzothiazole derivatives with a broad antifungal spectrum: Design, synthesis and structure–activity relationships. Med. Chem. Commun. 2013, 4, 1551–1561. [Google Scholar] [CrossRef]
- Hutchinson, I.; Bradshaw, T.D.; Matthews, C.S.; Stevens, M.F.G.; Westwell, A.D. Antitumour benzothiazoles. Part 20: 3′-cyano and 3′-alkynyl-substituted 2-(4′-aminophenyl) benzothiazoles as new potent and selective analogues. Bioorg. Med. Chem. Lett. 2003, 13, 471–474. [Google Scholar] [CrossRef]
- Cai, J.; Sun, M.; Wu, X.; Chen, J.; Wang, P.; Zong, X.; Ji, M. Design and synthesis of novel 4-benzothiazole amino quinazolines Dasatinib derivatives as potential anti-tumor agents. Eur. J. Med. Chem. 2013, 63, 702–712. [Google Scholar] [CrossRef] [PubMed]
- Hegde, M.; Vartak, S.V.; Kavitha, C.V.; Ananda, H.; Prasanna, D.S.; Gopalakrishnan, V.; Choudhary, B.; Rangappa, K.S.; Raghavan, S.C. A Benzothiazole Derivative (5g) Induces DNA Damage and Potent G2/M Arrest in Cancer Cells. Sci. Rep. 2017, 7, 2533. [Google Scholar] [CrossRef]
- Rodrigues, J.R.; Charris, J.; Camacho, J.; Barazarte, A.; Gamboa, N.; Antunes, F. Cytotoxic effects of N’-formyl-2-(5-nitrothiophen-2-yl) benzothiazole-6-carbohydrazide in human breast tumor cells by induction of oxidative stress. Antican. Res. 2012, 32, 2721–2726. [Google Scholar]
- Xia, Y.; Lei, Q.; Zhu, Y.; Ye, T.; Wang, N.; Li, G.; Shi, X.; Liu, Y.; Shao, B.; Yin, T.; et al. SKLB316, a novel small-molecule inhibitor of cell-cycle progression, induces G2/M phase arrest and apoptosis in vitro and inhibits tumor growth in vivo. Cancer Lett. 2014, 355, 297–309. [Google Scholar] [CrossRef] [PubMed]
- Osmaniye, D.; Levent, S.; Karaduman, A.B.; Ilgın, S.; Özkay, Y.; Kaplancıklı, Z.A. Synthesis of new benzothiazole acylhydrazones as anticancer agents. Molecules 2018, 23, 1054. [Google Scholar] [CrossRef] [PubMed]
- Kim, T.W.; Hong, D.W.; Park, J.W.; Hong, S.H. CB11, a novel purine-based PPARɣ ligand, overcomes radio-resistance by regulating ATM signalling and EMT in human non-small-cell lung cancer cells. Br. J. Cancer 2020, 123, 1737–1748. [Google Scholar] [CrossRef]
- Kim, T.W.; Hong, D.W.; Kang, C.M.; Hong, S.H. A novel PPARɣ ligand, PPZ023, overcomes radioresistance via ER stress and cell death in human non-small-cell lung cancer cells. Exp. Mol. Med. 2020, 52, 1730–1743. [Google Scholar] [CrossRef] [PubMed]
- Kim, T.W.; Hong, D.W.; Hong, S.H. CB13, a novel PPARγ ligand, overcomes radio-resistance via ROS generation and ER stress in human non-small cell lung cancer. Cell Death Dis. 2020, 11, 848. [Google Scholar] [CrossRef] [PubMed]
- Smith, S.M.; Wunder, M.B.; Norris, D.A.; Shellman, Y.G. A simple protocol for using a LDH-based cytotoxicity assay to assess the effects of death and growth inhibition at the same time. PLoS ONE 2011, 6, e26908. [Google Scholar] [CrossRef] [PubMed]
- Liu, L.F.; Dauann, P.; Lin, C.T.; D’Arpa, P.; Wu, J. Mechanism of action of Camptothecin. Ann. N. Y. Acad. Sci. 1996, 803, 44–49. [Google Scholar] [CrossRef] [PubMed]
- Thomberry, N.A. Caspase: A decade of death research. Cell Death Differ. 1999, 6, 1023–1027. [Google Scholar] [CrossRef]
- Chang, F.; Lee, J.T.; Navolanic, P.M.; Steelman, L.S.; Shelton, J.G.; Blalock, W.L.; Franklin, R.A.; McCubrey, J.A. Involvement of PI3K/AKT pathway in cell cycle progression, apoptosis, and neoplastic transformation: A target for cancer chemotherapy. Leukemia 2003, 17, 590–603. [Google Scholar] [CrossRef]
- Zeke, A.; Misheva, M.; Remenyi, A.; Bogoyevitch, M. JNK signaling: Regulation and functions based on complex protein-protein partnerships. Microbiol. Mol. Biol. Rev. 2016, 80, 793–835. [Google Scholar] [CrossRef] [PubMed]
- Liu, T.; Zhang, L.; Joo, D.; Sun, S. NF-κB signaling in inflammation. Sign. Transducer Target. Ther. 2017, 2, e17023. [Google Scholar] [CrossRef] [PubMed]
- Yoshida, M.; Hayakawa, I.; Hayashi, N.; Agatsuma, T.; Oda, Y.; Tanzawa, F.; Iwasaki, S.; Koyama, K.; Furukawa, H.; Kurakata, S.; et al. Synthesis and biological evaluation of benzothiazole derivatives as potent antitumor agents. Bioorg. Med. Chem. Lett. 2005, 15, 3328–3332. [Google Scholar] [CrossRef] [PubMed]
- Cindrić, M.; Perić, M.; Kralj, M.; Martin-Kleiner, I.; David-Cordonnier, M.H.; Paljetak, H.Č.; Matijašić, M.; Verbanac, D.; Karminski-Zamola, G.; Hranjec, M. Antibacterial and antiproliferative activity of novel 2-benzimidazolyl- and 2-benzothiazolyl-substituted benzo[b]thieno-2-carboxamides. Mol. Divers. 2018, 22, 637–646. [Google Scholar] [CrossRef]
- Hennessy, B.T.; Smith, D.L.; Ram, P.T.; Lu, Y.; Mills, G.B. Exploiting the PI3K/AKT pathway for cancer drug discovery. Nat. Rev. Drug Discov. 2005, 4, 988–1004. [Google Scholar] [CrossRef] [PubMed]
- Hossain, M.A.; Wongsrikaew, N.; Yoo, G.W.; Han, J.; Shin, C.G. Cytotoxic effects of polymethoxyflavones isolated from Kaempferia parviflora. J. Korean Soc. Appl. Biol. Chem. 2012, 55, 471–476. [Google Scholar] [CrossRef]
- Lee, G.E.; Shin, C.G. Influence of pretreatment with immunosuppressive drugs on viral proliferation. J. Microbiol. Biotechnol. 2018, 28, 1716–1722. [Google Scholar] [CrossRef] [PubMed]
- Hyun, U.; Lee, D.H.; Lee, C.; Shin, C.G. Apoptosis induced by enniatins H and MK1688 isolated from Fusarium oxysporum FB1501. Toxicon 2009, 53, 723–728. [Google Scholar] [CrossRef]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kim, J.; Hong, S.H.; Jeon, S.H.; Park, M.H.; Shin, C.-G. The Novel Benzothiazole Derivative PB11 Induces Apoptosis via the PI3K/AKT Signaling Pathway in Human Cancer Cell Lines. Int. J. Mol. Sci. 2021, 22, 2718. https://doi.org/10.3390/ijms22052718
Kim J, Hong SH, Jeon SH, Park MH, Shin C-G. The Novel Benzothiazole Derivative PB11 Induces Apoptosis via the PI3K/AKT Signaling Pathway in Human Cancer Cell Lines. International Journal of Molecular Sciences. 2021; 22(5):2718. https://doi.org/10.3390/ijms22052718
Chicago/Turabian StyleKim, Jinsun, Sung Hee Hong, So Hyun Jeon, Min Ho Park, and Cha-Gyun Shin. 2021. "The Novel Benzothiazole Derivative PB11 Induces Apoptosis via the PI3K/AKT Signaling Pathway in Human Cancer Cell Lines" International Journal of Molecular Sciences 22, no. 5: 2718. https://doi.org/10.3390/ijms22052718
APA StyleKim, J., Hong, S. H., Jeon, S. H., Park, M. H., & Shin, C.-G. (2021). The Novel Benzothiazole Derivative PB11 Induces Apoptosis via the PI3K/AKT Signaling Pathway in Human Cancer Cell Lines. International Journal of Molecular Sciences, 22(5), 2718. https://doi.org/10.3390/ijms22052718





