Advances in Chitosan-Based Nanoparticles for Drug Delivery
Abstract
:1. Introduction
2. Enhancement of Chitosan Properties by Its Modification
2.1. Hydrophobic Chitosan Derivatives (with Hydrophobic Substituents)
2.2. Amphiphilic Chitosan Derivatives (with Amphiphilic Substituents)
2.3. Ionic Chitosan Derivatives (with Cationic and Anionic Substituents)
2.4. Sugar Bound Chitosan Derivatives
2.5. Chitosan Derivatives with Cyclic Structures
2.6. Chitosan Derivatives with Thiol Groups
2.7. Thiosemicarbazone Linked Chitosan Derivatives
2.8. Chitosan Copolymers (with Polymer Substituents)
2.9. Crosslinked Chitosan Derivatives
3. Enhancement in Drug Delivery by Chitosan Nanoparticles
3.1. Basic Aspects of (Chitosan) Nanoparticle Systems
- (i).
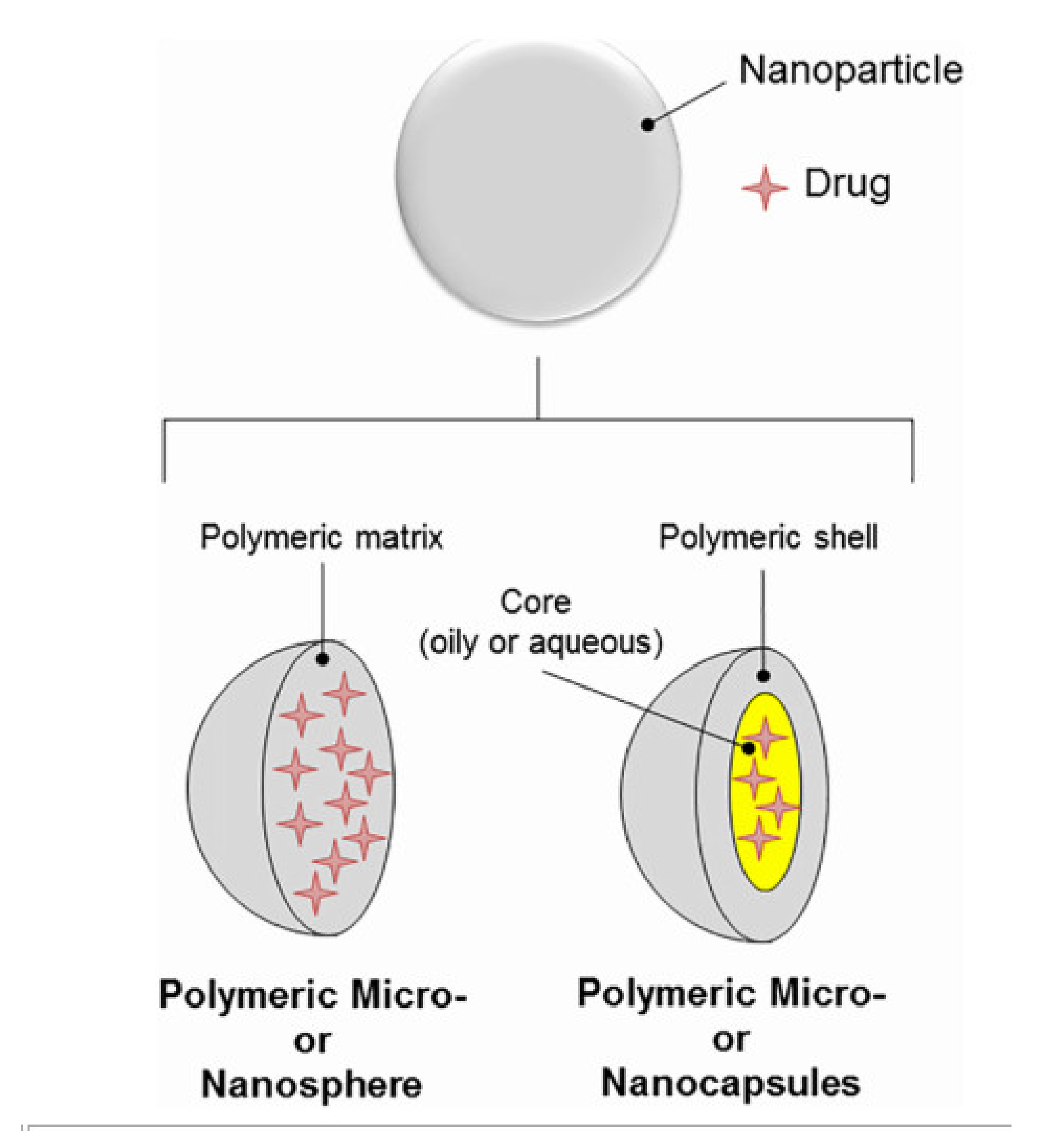
- CS NSs are a matrix system, where the drug may be absorbed in the surface or encapsulated within the CS particle. As an example, Liu et al. [39] constructed the photothermal sensitive carboxymethyl CS nanospheres (CMC NSs) carrier by introducing controllable heat-sensitive groups into CMC molecules. The carrier owned high drug loading and improved the stability of coated-drug DOX. The NSs generated photothermal response through NIR irradiation to improve the drug release amount and to achieve the combined treatment effect of photodynamic therapy and chemotherapy. In vitro photothermal tests proved that the NSs had excellent light stability and photothermal conversion performance. The cytotoxicity test results showed that the NSs had no obvious toxicity, but the drug-loaded nanospheres could effectively inhibit the growth of HepG-2 cells via photo-response to release DOX and Indocyanine green for achieving photothermal-chemotherapy under NIR irradiation.
- (ii).
- CS NCs are vesicular systems in which the drug is generally confined to a cavity consisting of an oily core covered by a CS shell. As an example, Castro et al. [65] evaluated the physicochemical and biological properties of docetaxel (DCX) loaded chitosan nanocapsules (DCX-CS NCs) functionalized with the chimeric monoclonal antibody ChiTn mAb (highly specific antigen for carcinomas) (DCX-CS/PEG-ChiTn mAb NCs) as a potential improvement treatment for cancer therapy. The NCs, formed as a polymeric shell around an oily core, allowed a 99.9% encapsulation efficiency of DCX with a monodispersity particle size in the range of 200 nm and a high positive surface charge that provided substantial stability to the nanosystems. Uptake studies and viability assay conducted in A549 human lung cancer cell line in vitro demonstrated that ChiTn mAb enhanced NPs internalization and cell viability reduction.
- (iii).
- CS NFs can be used in various fields mainly due to the presence of -NH2 and -OH groups, along with their specific structure. Their nanofibrous structure offers enormous possibilities for chemical modifications that create new properties applicable, particularly in the biomedical field. CS NFs can be prepared by electrospinning of CS into ultrafine fibers of nano size. Owing to the large specific surface area, NFs can deliver drugs, peptides, and vaccine antigens. The release of the drug may be immediate, delayed, or modified depending on the type of interactions between the polymer and the drug. Usually, an immediate release is noticed when a composition of a water-soluble substance and a water-soluble polymer is used. The prolonged release can be achieved by integrating the drug into other nanocarriers, such as NPs, liposomes, dendrimers, then loaded into NFs or use hydrophobic polymers [18,66]. As an example, Amiri et al. [67] reported the development of a local antibiotic delivery system using chitosan/polyethylene oxide (CS/PEO) NFs for delivery of teicoplanin. Uniform and bead-less NFs were prepared via electrospinning of a CS/PEO solution containing teicoplanin. The NFs were able to release teicoplanin for up to 12 days. Antibacterial test in agar diffusion and time-kill study on Staphylococcus aureus also demonstrated that loading teicoplanin in CS/PEO NFs enhanced the antibacterial activity up to 1.5- to 2-fold. An in vivo study on a rat full-thickness wound model confirmed the safety and efficacy of applying the teicoplanin-loaded NFs and significant improvement in wound closure were observed especially with the NFs containing 4% teicoplanin.
3.2. Preparation Procedures for Chitosan Nanoparticles
3.2.1. Covalent Cross-Linking
3.2.2. Self-Assembly
Ionic Cross-Linking (Ionic Gelation)
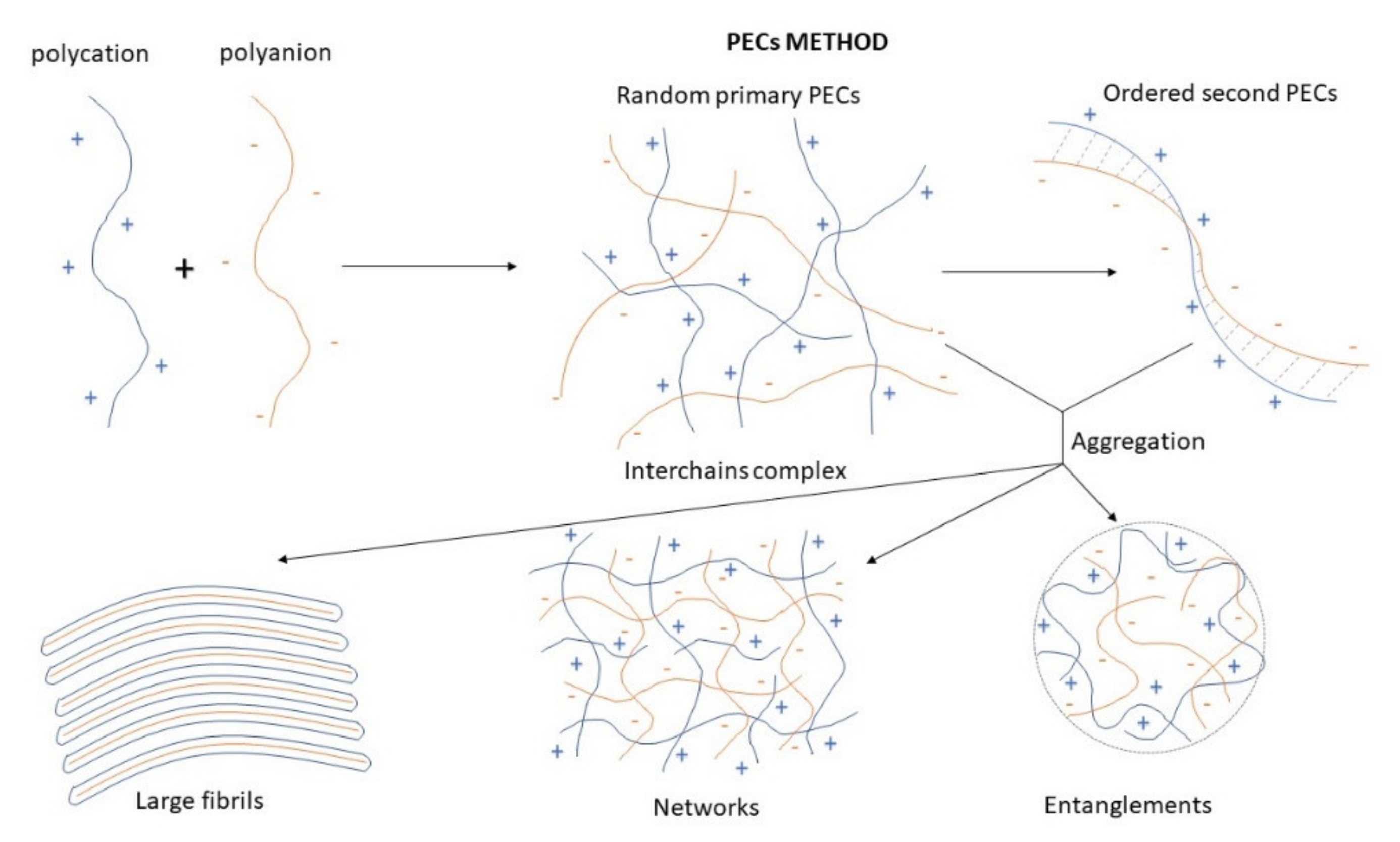
Polyelectrolyte Complex (PEC)
3.2.3. Emulsion Technique
Emulsion Droplet Coalescence (Emulsion Crosslinking and Precipitation)
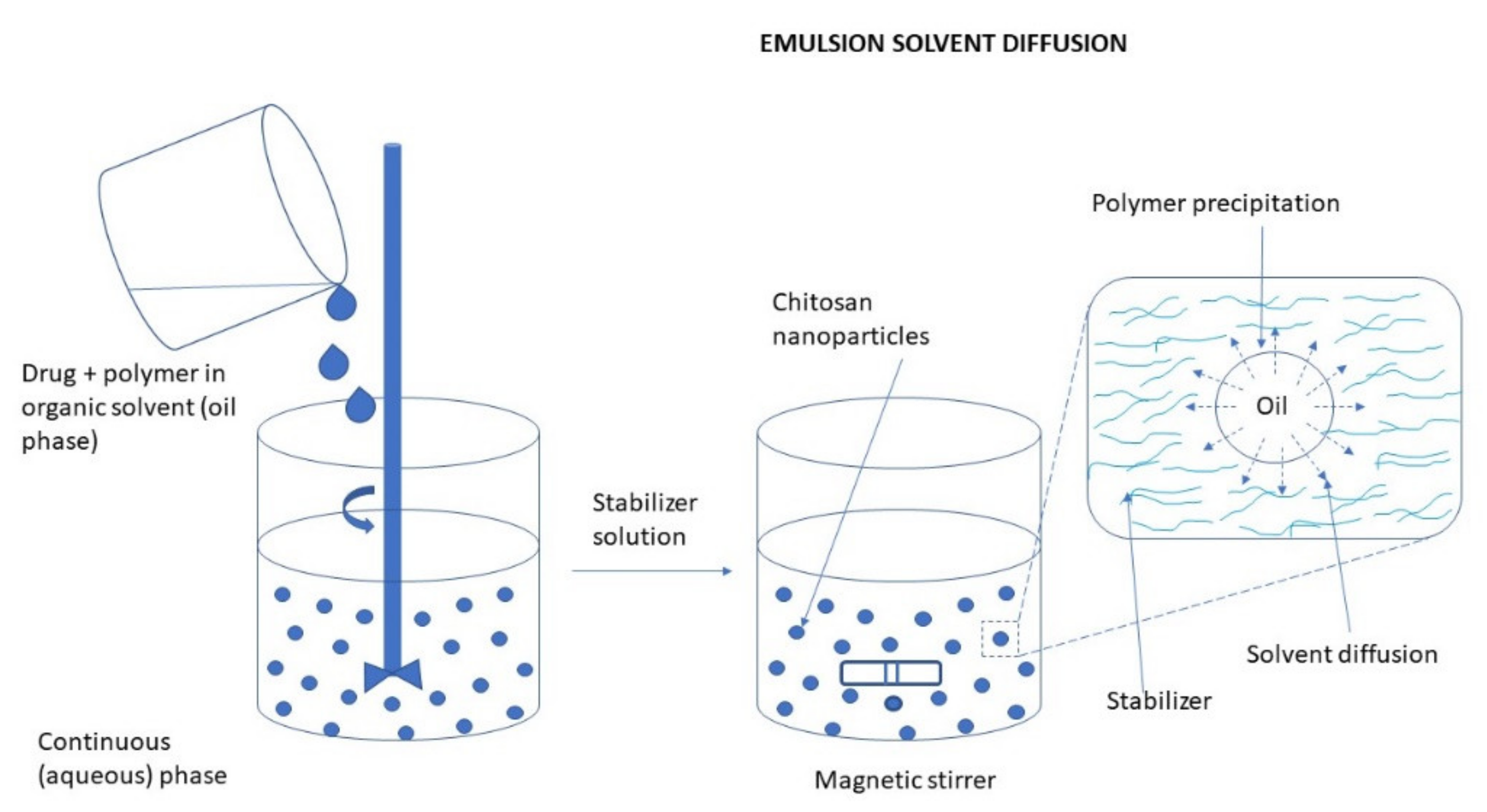
Emulsification Solvent Diffusion
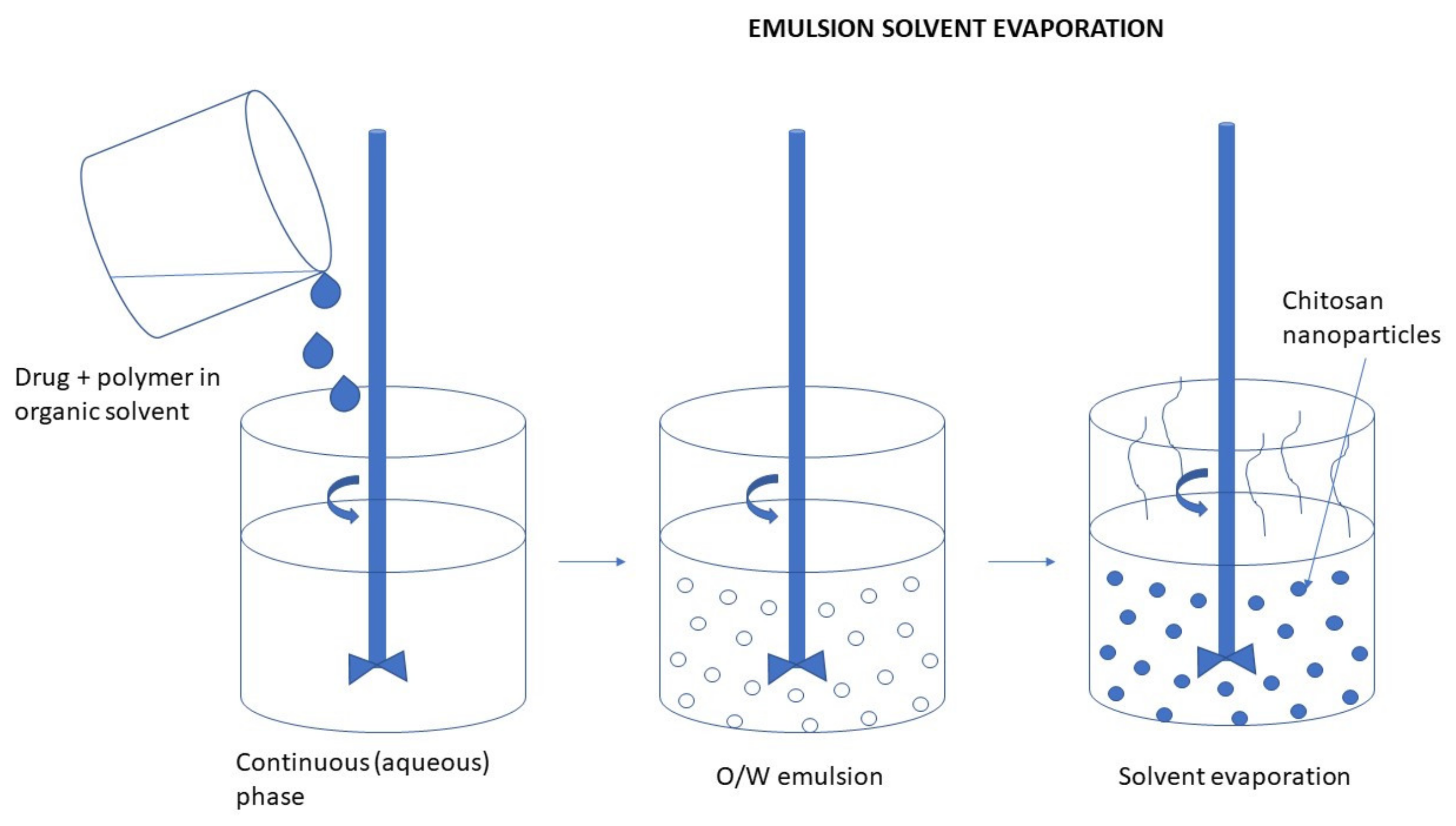
Emulsification Solvent Evaporation
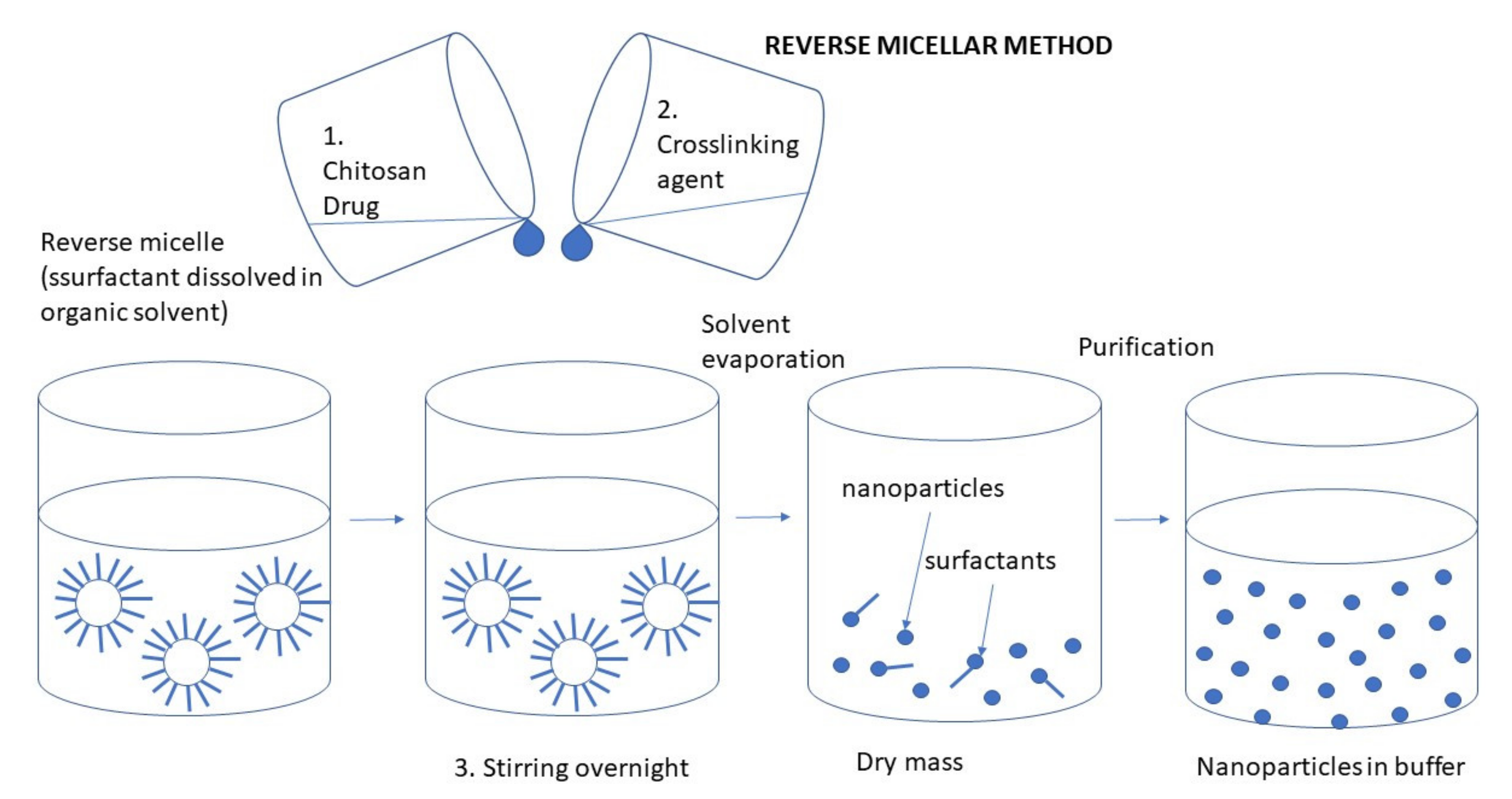
3.2.4. Reverse Micellar Method
3.2.5. Drying Methods
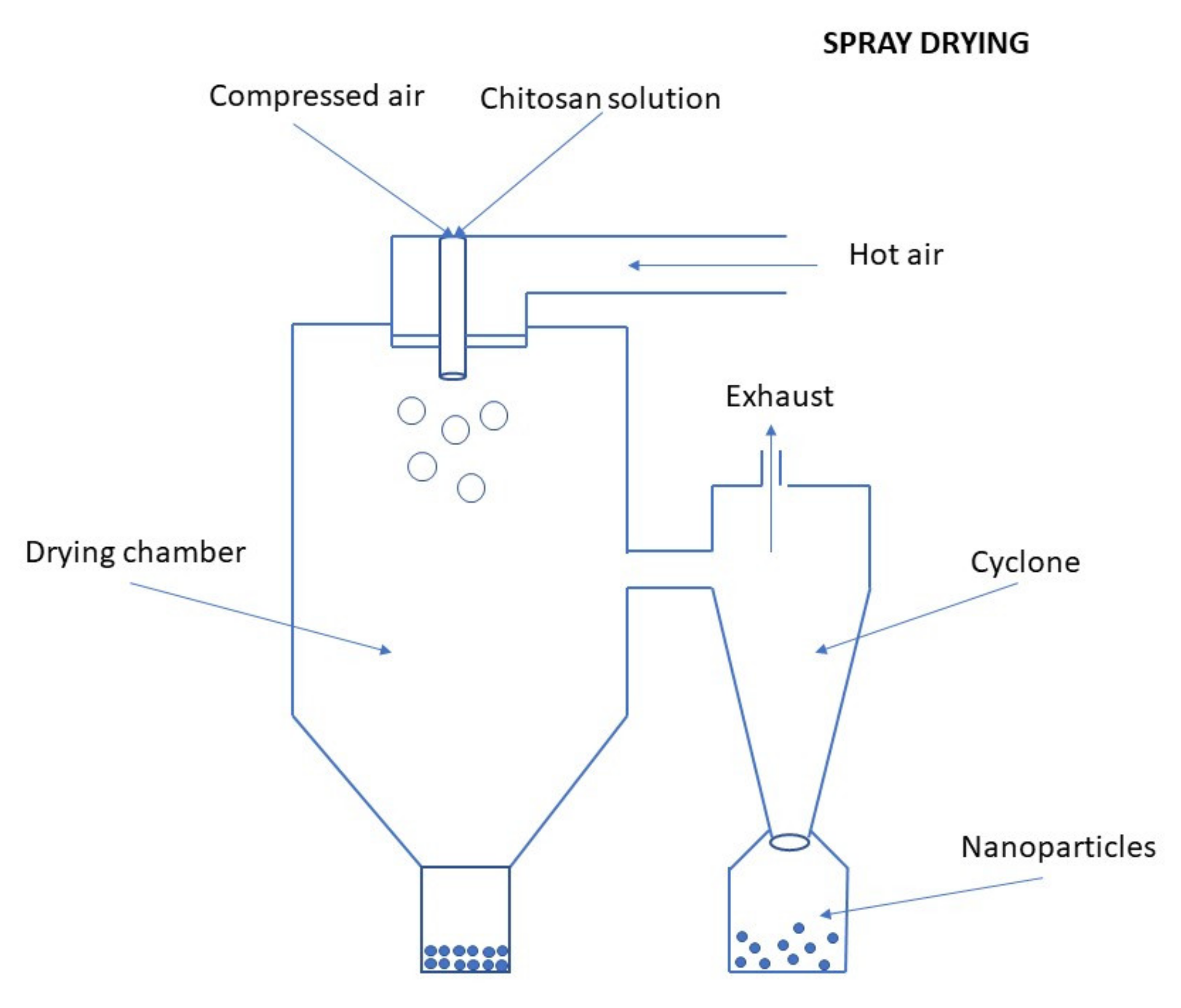
Spray Drying
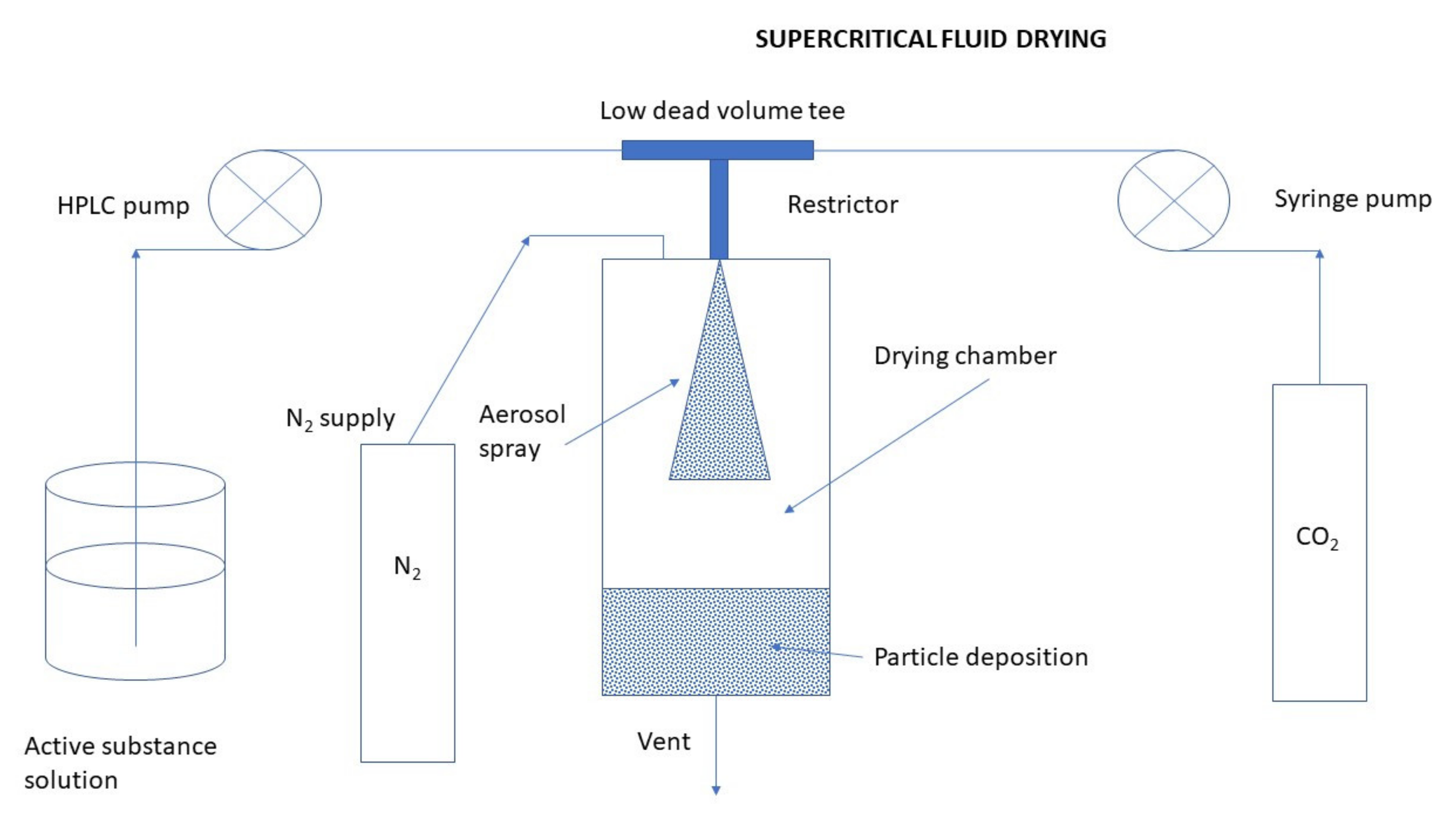
Supercritical Fluid Drying
Electrospraying Technique
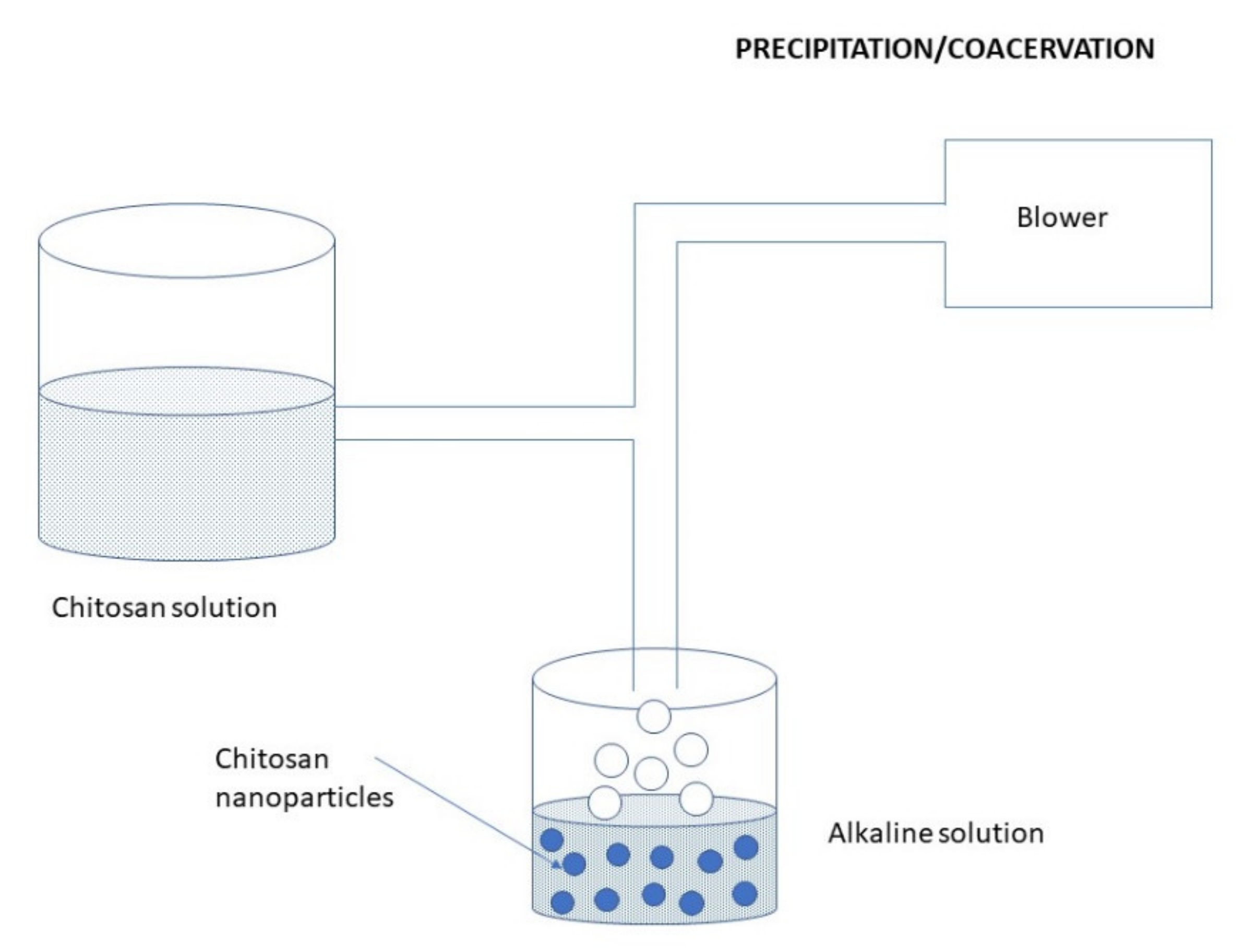
3.2.6. Precipitation/Coacervation
3.2.7. Microfluidic Method
3.3. Chitosan Based-Nanocomposites, Types, Their Properties, and Utilization
3.3.1. Chitosan-Polymer Nanocomposites
Synthetic Polymers
Natural Polymers
3.3.2. Chitosan-Inorganic Material Nanocomposite
Montmorillonite Clay (Mnt)
Mesoporous Silica Nanoparticles (MS NPs)
Magnetic Nanoparticles (Mag NPs)
Graphene Oxide (GO) Modified Nanocomposite
Gold Nanoparticles (Au NPs)
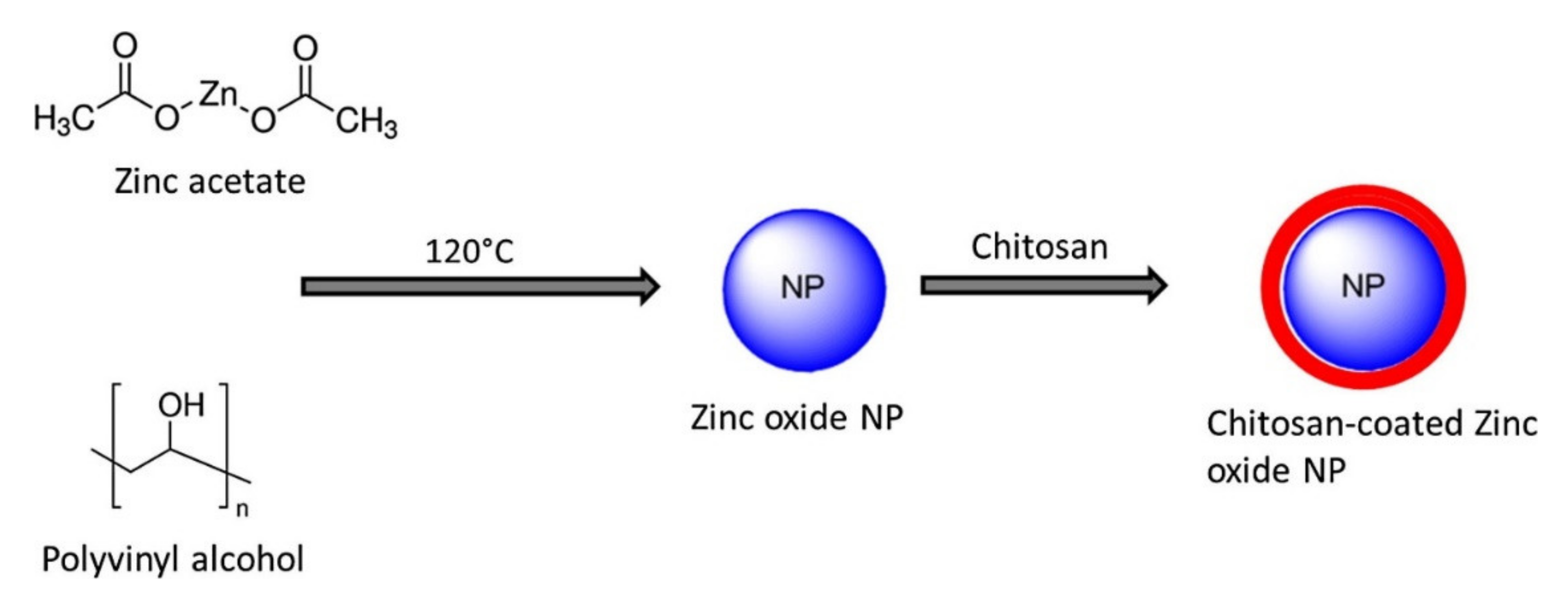
Zinc Oxide Nanoparticles (ZnO NPs)
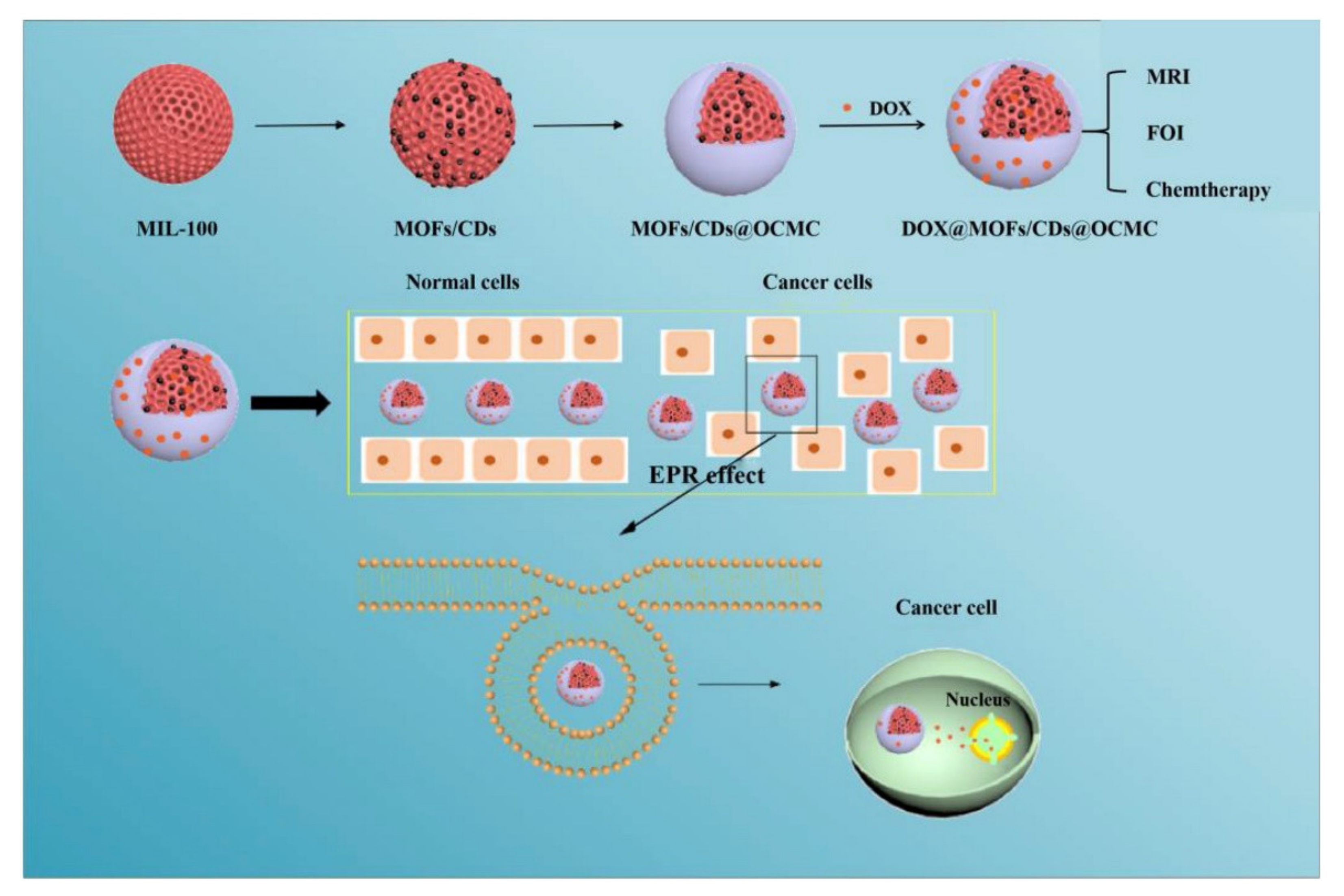
Carbon Quantum Dots (CQDs)
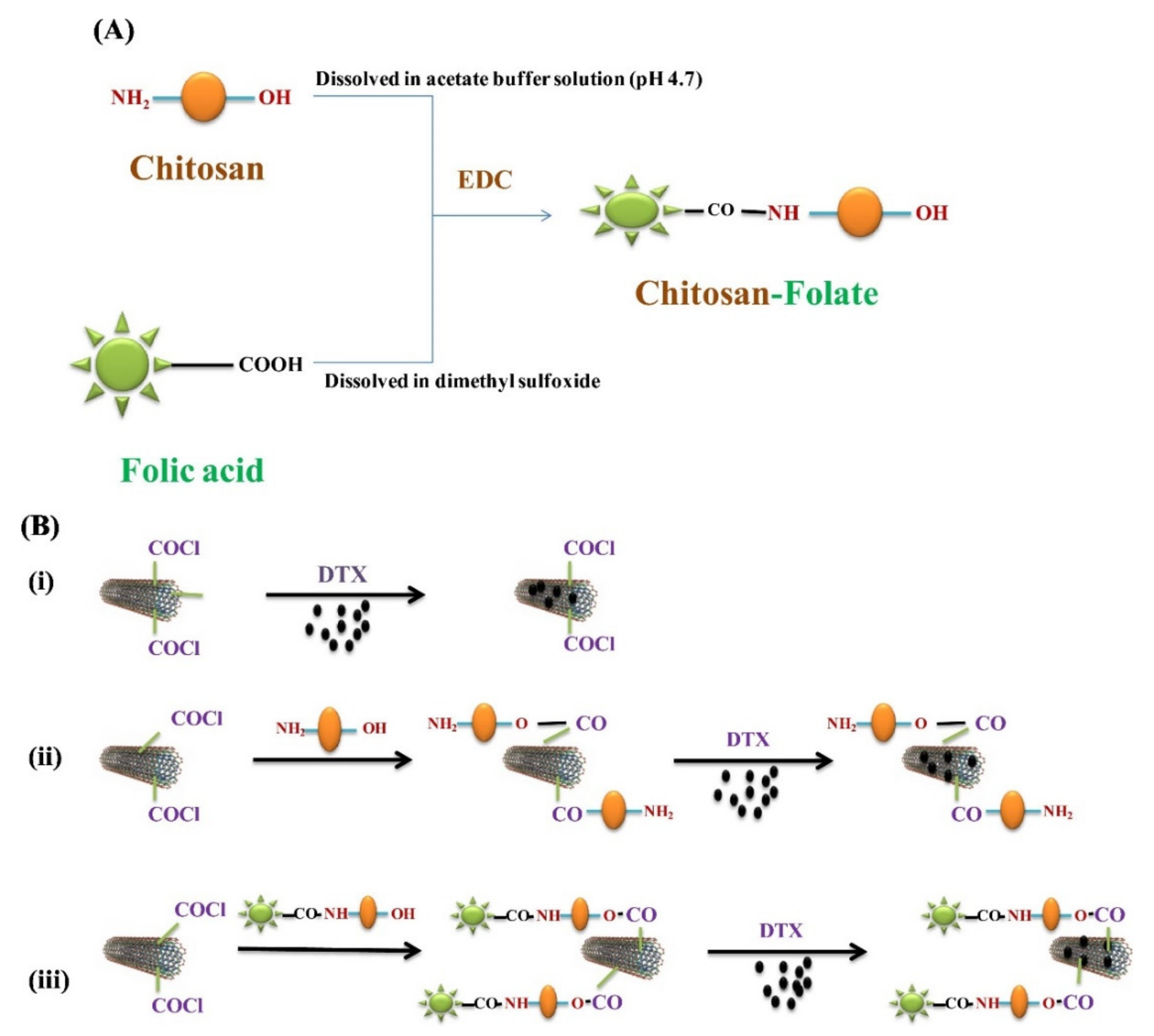
Carbon Nanotubes (CNTs) Composite
Other Inorganic Materials Combined with CS
3.3.3. Stimuli Responsive Chitosan, Chitosan Nanoparticles, and Nanocomposites
3.4. Chitosan Nanoparticles in Drug Delivery
3.4.1. Oral Drug Delivery
Antidiabetic Drugs
Anticancer Drugs
Antihypertensive Drugs
Antioxidants
Anti-inflammatory Drugs
Oral Vaccines
Oher Drugs
3.4.2. Ocular Drug Delivery
3.4.3. Nasal Drug Delivery
Topical Nasal Delivery
Systemic Nasal Delivery
Nose to Brain Delivery
3.4.4. Pulmonary Drug Delivery
3.4.5. Buccal Drug Delivery
3.4.6. Periodontal Drug Delivery
3.4.7. Dermal and Transdermal Drug Delivery
Transdermal Drug Delivery
Dermal Delivery
3.4.8. Wound Healing
3.4.9. Vaginal Drug Delivery
3.4.10. Vaccine Delivery
3.4.11. Gene Delivery
4. Concluding Remarks
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Kumar, A.; Vimal, A.; Kumar, A. Why chitosan? From properties to perspective of mucosal drug delivery. Int. J. Biol. Macromol. 2016, 91, 615–622. [Google Scholar] [CrossRef]
- Shanmuganathan, R.; Edison, N.T.J.I.; Lewis Oscar, F.; Kumar, P.; Shanmugan, S.; Pugazhendhi, A. Chitosan nanopolymers: An overview of drug delivery against cancer. Int. J. Biol. Macromol. 2019, 130, 727–736. [Google Scholar] [CrossRef]
- Taher, F.A.; Ibrahim, S.A.; Abd El-Aziz, A.; El-Nour, M.F.A.; El-Sheikh, M.A.; El-Husseiny, N.; Mohamed, M.M. Anti-Proliferative effect of chitosan nanoparticles (extracted from crayfish Procambarus clarkii, Crustacea: Cambaridae) against MDA-MB-231 and SK-BR-3 human breast cancer cell lines. Int. J. Biol. Macromol. 2019, 126, 478–487. [Google Scholar] [CrossRef]
- El Rabey, H.A.; Almutairi, F.M.; Alalawy, A.I.; Al-Duais, M.A.; Sakran, M.I.; Zidan, N.S.; Tayel, A.A. Augmented control of drug-resistant Candida spp. via fluconazole loading into fungal chitosan nanoparticles. Int. J. Biol. Macromol. 2019, 141, 511–516. [Google Scholar] [CrossRef]
- Lim, C.; Lee, D.W.; Israelachvili, J.N.; Jho, Y.S.; Hwang, D.S. Contact time- and pH-dependent adhesion and cohesion of low molecular weight chitosan coated surfaces. Carbohydr. Polym. 2015, 117, 887–889. [Google Scholar] [CrossRef] [Green Version]
- Lim, C.; Hwang, D.S.; Lee, D.W. Intermolecular interactions of chitosan: Degree of acetylation and molecular weight. Carbohydr. Polym. 2021, 259, 117782. [Google Scholar] [CrossRef]
- Elgadir, A.A.; Muddin, M.S.; Ferdosh, S.; Adam, A.; Chowdhury, A.J.K.; Sarker, M.Z.I. Impact of chitosan composites and chitosan nanoparticle composites on various drug delivery systems: A review. J. Food Drug Anal. 2015, 23, 619–629. [Google Scholar] [CrossRef] [Green Version]
- Bernkop-Schnurch, A.; Dunnhaupt, S. Chitosan-based drug delivery systems. Eur. J. Pharm. Biopharm. 2012, 81, 463–469. [Google Scholar] [CrossRef] [PubMed]
- Saikia, C.; Gogoi, P.; Maji, T.K. Chitosan: A promising biopolymer in drug delivery applications. J. Mol. Genet. Med 2015, S4:006. [Google Scholar] [CrossRef]
- Huang, G.; Liu, Y.; Chen, L. Chitosan and its derivatives as vehicles for drug delivery. Drug Deliv. 2017, 24, 108–113. [Google Scholar] [CrossRef] [PubMed]
- Li, J.; Cai, C.; Li, J.; Li, J.; Li, J.; Sun, T.; Wang, L.; Wu, H.; Yu, G. Chitosan-Based nanomaterials for drug delivery. Molecules 2018, 23, 2661. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Safdar, R.; Omar, A.A.; Arunagiri, A.; Regupathi, I.; Thanabalan, M. Potential of chitosan and its derivatives for controlled drug release application—A review. J. Drug Deliv. Sci. Technol. 2019, 49, 642–659. [Google Scholar] [CrossRef]
- Bakshi, P.S.; Selvakumar, D.; Kadirvelu, K.; Kumar, N.S. Chitosan as an environment friendly biomaterial—A review on recent modififications and applications. Int. J. Biol. Macromol. 2020, 150, 1072–1083. [Google Scholar] [CrossRef] [PubMed]
- Khan, F.; Pham, D.T.N.; Oloketuyi, S.F.; Manivasagan, P.; Oh, J.; Kim, Y.M. Chitosan and their derivatives: Antibiofilm drugs against pathogenic bacteria. Colloids Surf. B Biointerfaces 2020, 158, 11627. [Google Scholar] [CrossRef] [PubMed]
- Ma, Y.; Garrido-Maestu, A.; Jeong, K.C. Application, mode of action, and in vivo activity of chitosan and its micro- and nanoparticles as microbial agents: A review. Carbohydr. Polym. 2017, 176, 257–265. [Google Scholar] [CrossRef] [PubMed]
- Qin, Y.; Li, P.; Gou, Z. Cationic chitosan derivatives as potential antifungals: A review of structural optimization and applications. Carbohydr. Polym. 2020, 236, 116002. [Google Scholar] [CrossRef] [PubMed]
- Hamedi, H.; Moradi, S.; Hudson, M.; Tonelli, A.E. Chitosan based hydrogels and their applications for drug delivery in wound dressings: A review. Carbohydr. Polym. 2018, 199, 445–460. [Google Scholar] [CrossRef]
- Ali, A.; Ahmed, S. A review on chitosan and its nanocomposites in drug delivery. Int. J. Biol. Macromol. 2018, 109, 273–286. [Google Scholar] [CrossRef]
- Negm, N.A.; Hefni, H.H.H.; Abd-Elaal, A.A.A.; Badr, E.A.; Abou Kana, M.T.H. Advancement on modifification of chitosan biopolymer and its potential applications. Int. J. Biol. Macromol. 2020, 152, 681–702. [Google Scholar] [CrossRef]
- Tian, Y.; Sun, Y.; Wang, X.; Kasparis, G.; Mao, S. Chapter 15—Chitosan and its derivatives-based nano-formulations in drug delivery. In Nanobiomaterials in Drug Delivery; Grumezescu, M.A., Ed.; Elsevier: Amsterdam, The Netherlands, 2016; pp. 515–572. [Google Scholar]
- Mateescu, M.A.; Ispas-Szabo, P.; Assaad, E. Chitosan and its derivatives as self-assembled systems for drug delivery In Controlled Drug Delivery: The Role of Self-Assembling Multi-Task Excipients; Elsevier: Amsterdam, The Netherlands, 2015; pp. 85–125. [Google Scholar]
- Fonseca-Santos, B.; Chorilli, M. An overview of carboxymethylated derivatives of chitosan: Their use as biomaterials and drug delivery systems. Mater. Sci. Eng. C 2017, 77, 1349–1362. [Google Scholar] [CrossRef] [Green Version]
- Dimassi, S.; Tabary, N.; Chai, F.; Blanchemain, N.; Martel, B. Sulfonated and sulfated chitosan derivatives for biomedical applications: A review. Carbohydr. Polym. 2018, 202, 382–396. [Google Scholar] [CrossRef] [PubMed]
- Tekade, M.; Maheshwari, N.; Youngren-Ortiz, S.R.; Pandey, V.; Chourasiya, Y.; Soni, V.; Deb, P.K.; Sharma, M.C. Chapter 13—Thiolated-Chitosan: A novel mucoadhesive polymer for better-targeted drug delivery. In Advances in Pharmaceutical Product Development and Research, Biomaterials and Bionanotechnology; Academic Press: Cambridge, MA, USA, 2019; pp. 459–493. [Google Scholar]
- Dang, Y.; Guan, J. Nanoparticle-based drug delivery systems for cancer therapy. Smart Mater. Med. 2020, 1, 10–19. [Google Scholar] [CrossRef]
- Wang, W.; Xue, C.; Mao, X. Chitosan: Structural modification, biological activity and application. Int. J. Biol. Macromol. 2020, 164, 4532–4546. [Google Scholar] [CrossRef] [PubMed]
- Chu, L.; Zhang, Y.; Feng, Z.; Yang, J.; Tian, Q.; Yao, X.; Zhao, X.; Tan, H.; Chen, Y. Synthesis and application of a series of amphipathic chitosan derivatives and the corresponding magnetic nanoparticle-embedded polymeric micelles. Carbohydr. Polym. 2019, 223, 114966. [Google Scholar] [CrossRef]
- Burr, S.J.; Williams, P.A.; Ratcliffe, I. Synthesis of cationic alkylated chitosans and an investigation of their rheological properties and interaction with anionic surfactant. Carbohydr. Polym. 2018, 201, 615–623. [Google Scholar] [CrossRef] [PubMed]
- Nanda, B.; Manjappa, A.S.; Chuttani, K.; Balasinor, N.H.; Mishra, A.K.; Ramachandra Murthy, R.S. Acylated chitosan anchored paclitaxel loaded liposomes: Pharmacokinetic and biodistribution study in Ehrlich ascites tumor bearing mice. Int. J. Biol. Macromol. 2019, 122, 367–379. [Google Scholar] [CrossRef] [PubMed]
- Permadi, R.; Suk, V.R.E.; Misran, M. Synthesis and Characterization of acylated low molecular weight chitosan and acylated low molecular weight phthaloyl chitosan. Sains Malaysiana 2020, 49, 2251–2260. [Google Scholar] [CrossRef]
- Mohamed, N.A.; Abd El-Ghany, N.A.; Abdel-Aziz, M.M. Synthesis, characterization, anti-inflammatory and anti-Helicobacter pylori activities of novel benzophenone tetracarboxylimide benzoyl thiourea cross-linked chitosan hydrogels. Int. J. Biol. Macromol. 2021, 181, 956–965. [Google Scholar] [CrossRef]
- Hanafy, A.F.; Abdalla, A.M.; Guda, T.K.; Gabr, K.E.; Royall, P.G.; Alqurshi, A. Ocular anti-inflammatory activity of prednisolone acetate loaded chitosan-deoxycholate self-assembled nanoparticles. Int. J. Nanomed. 2019, 14, 3679–3689. [Google Scholar] [CrossRef] [Green Version]
- Li, J.; Jin, X.; Yang, Y.; Zhang, L.; Liu, R.; Li, Z. Trimethyl chitosan nanoparticles for ocular baicalein delivery: Preparation, optimization, in vitro evaluation, in vivo pharmacokinetic study and molecular dynamics simulation. Int. J. Biol. Macromol. 2020, 156, 749–761. [Google Scholar] [CrossRef]
- Ravindran, R.; Mitra, K.; Arumugam, S.K.; Doble, M. Preparation of Curdlan sulphate—Chitosan nanoparticles as a drug carrier to target Mycobacterium smegmatis infected macrophages. Carbohydr. Polym. 2021, 258, 117686. [Google Scholar] [CrossRef] [PubMed]
- Ravi Kumar, M.N.V.; Muzzarelli, R.A.A.; Muzzarelli, C.; Sashiwa, H.; Domb, A.J. Chitosan chemistry and pharmaceutical perspectives. Chem. Rev. 2004, 104, 6017–6084. [Google Scholar] [CrossRef] [PubMed]
- Palacio, J.; Monsalve, Y.; Ramírez-Rodríguez, F.; López, B. Study of encapsulation of polyphenols on succinyl-chitosan nanoparticles. J. Drug Deliv. Sci. Technol. 2020, 57, 101610. [Google Scholar] [CrossRef]
- Han, G.; Liu, S.; Pan, Z.; Lin, Y.; Ding, S.; Li, L.; Luo, B.; Jiao, Y.; Zhou, C. Sulfonated chitosan and phosphorylated chitosan coated polylactide T membrane by polydopamine-assisting for the growth and osteogenic differentiation of MC3T3-E1s. Carbohydr. Polym. 2020, 229, 115517. [Google Scholar] [CrossRef]
- Zheng, Z.; Zhang, W.; Sun, W.; Li, X.; Duan, J.; Cui, J.; Feng, Z.; Mansour, H. Inflfluence of the carboxymethyl chitosan anti-adhesion solution on the TGF-β1 in a postoperative peritoneal adhesion rat. J. Mater. Sci. Mater. Med. 2013, 24, 2549–2559. [Google Scholar] [CrossRef]
- Liu, X.; He, Z.; Chen, Y.; Zhou, C.; Wang, C.; Liu, Y.; Feng, C.; Yang, Z.; Li, P. Dual drug delivery system of photothermal-sensitive carboxymethyl chitosan nanosphere for photothermal-chemotherapy. Int. J. Biol. Macromol. 2020, 163, 156–166. [Google Scholar] [CrossRef]
- Wang, C.; Zhang, Z.; Chen, B.; Gu, L.; Li, Y.; Yu, S. Design and evaluation of galactosylated chitosan/graphene oxide nanoparticles as a drug delivery system. J. Colloid Interface Sci. 2018, 516, 332–341. [Google Scholar] [CrossRef]
- Sharma, A.K.; Gupta, L.; Sahu, H.; Qayum, A.; Singh, S.K.; Nakhate, K.T.; Ajazuddin; Gupta, U. Chitosan engineered PAMAM dendrimers as nanoconstructs for the enhanced anti-cancer potential and improved in vivo brain pharmacokinetics of temozolomide. Pharm. Res. 2018, 35, 9. [Google Scholar] [CrossRef]
- Evangelista, T.F.S.; Andrade, G.R.S.; Nascimento, K.N.S.; dos Santos, S.B.; Costa Santos, M.F.; D’Oca, C.R.M.; Estevam, C.S.; Gimenez, I.F.; Almeida, L.E. Supramolecular polyelectrolyte complexes based on cyclodextrin-grafted chitosan and carrageenan for controlled drug release. Carbohydr. Polym. 2020, 245, 116592. [Google Scholar] [CrossRef]
- Yi, Y.; Wang, Y.; Liu, H. Preparation of new crosslinked chitosan with crown ether and their adsorption for silver ion for antibacterial activities. Carbohydr. Polym. 2003, 53, 425–430. [Google Scholar] [CrossRef]
- Guaresti, O.; Maiz–Fernández, S.; Palomares, T.; Alonso-Varona, A.; Eceiza, A.; Pérez-Álvarez, L.; Gabilondo, N. Dual charged folate labelled chitosan nanogels with enhanced mucoadhesion capacity for targeted drug delivery. Eur. Polym. J. 2020, 134, 109847. [Google Scholar] [CrossRef]
- Adhikari, H.S.; Yadav, P.N. Anticancer activity of chitosan, chitosan derivatives, and their mechanism of action. Int. J. Biomater. 2018, 201. [Google Scholar] [CrossRef] [Green Version]
- Qin, Y.; Xing, R.; Liu, S.; Li, K.; Meng, X.; Li, R.; Cui, J.; Li, B.; Li, P. Novel thiosemicarbazone chitosan derivatives: Preparation, characterization, and antifungal activity. Carbohydr. Polym. 2012, 87, 2664–2670. [Google Scholar] [CrossRef]
- Hsu, C.V.; Hsieh, M.H.; Xiao, M.C.; Chou, Y.H.; Wang, T.H.; Chiang, W.H. pH-Responsive polymeric micelles self-assembled from benzoic-imine-containing alkyl-modifified PEGylated chitosan for delivery of amphiphilic drugs. Int. J. Biol. Macromol. 2020, 163, 1106–1116. [Google Scholar] [CrossRef]
- Savin, C.L.; Popa, M.; Delaite, C.; Costuleanu, M.; Costin, S.; Peptu, C.A. Chitosan grafted-poly(ethylene glycol) methacrylate nanoparticles as carrier for controlled release of bevacizumab. Mat. Sci. Eng. C 2019, 98, 843–860. [Google Scholar] [CrossRef] [PubMed]
- Yu, S.; Zhang, X.; Tan, G.; Tian, L.; Liu, D.; Liu, Y.; Yang, X.; Pan, W. A novel pH-induced thermosensitive hydrogel composed of carboxymethyl chitosan and poloxamer cross-linked by glutaraldehyde for ophthalmic drug delivery. Carbohydr. Polym. 2017, 155, 208–217. [Google Scholar] [CrossRef]
- Zhuang, S.; Zhang, Q.; Wang, J. Adsorption of Co2+ and Sr2+ from aqueous solution by chitosan grafted with EDTA. J. Mol. Liq. 2021, 325, 115197. [Google Scholar] [CrossRef]
- Sreekumar, S.; Goycoolea, F.M.; Moerschbacher, B.M.; Rivera-Rodriguez, G.R. Parameters influencing the size of chitosan-TPP nano- and microparticles. Sci. Rep. 2018, 8, 4695. [Google Scholar] [CrossRef] [Green Version]
- Garg, U.; Chauhan, S.; Nagaich, U.; Jain, N. Current advances in chitosan nanoparticles based drug delivery and targeting. Adv. Pharm. Bull. 2019, 9, 195–204. [Google Scholar] [CrossRef] [PubMed]
- Agnihotri, S.A.; Mallikarjuna, N.N.; Aminabhavi, T.M. Recent advances on chitosan-based micro- and nanoparticles in drug delivery. J. Control. Release 2004, 100, 5–28. [Google Scholar] [CrossRef] [PubMed]
- Shoueir, K.R.; El-Desouky, N.; Rashad, M.M.; Ahmed, M.K.; Janowska, I.; El-Kemary, M. Chitosan based-nanoparticles and nanocapsules: Overview, physicochemical features, applications of a nanofibrous scaffold, and bioprinting. Int. J. Biol. Macromol. 2021, 167, 1176–1197. [Google Scholar] [CrossRef]
- Zhang, A.; Meng, K.; Liu, Y.; Pan, Y.; Qu, W.; Chen, D.; Xie, S. Absorption, distribution, metabolism, and excretion of nanocarriers in vivo and their influences. Adv. Colloid Interface Sci. 2020, 284, 102261. [Google Scholar] [CrossRef] [PubMed]
- Cheng, X.; Tian, X.; Wu, A.; Li, J.; Tian, J.; Chong, Y.; Chai, Z.; Zhau, Y.; Chen, C.; Ge, C. Protein corona influences cellular uptake of gold nanoparticles by phagocytic and nonphagocytic cells in a size-dependent manner. ACS Appl. Mater. Interfaces 2015, 37, 20568–20575. [Google Scholar] [CrossRef]
- Malhaire, H.; Gimel, J.; Roger, E.; Benoît, J.; Lagarce, F. How to design the surface of peptide-loaded nanoparticles for efficient oral bioavailability? Adv. Drug Deliv. Rev. 2016, 106, 320–336. [Google Scholar] [CrossRef]
- Lee, J.H.; Sahu, A.; Jang, C.; Tae, G. The effect of ligand density on in vivo tumor targeting of nanographene oxide. J. Control. Release 2015, 209, 219–228. [Google Scholar] [CrossRef]
- Zhao, Z.; Ukidve, A.; Krishnan, V.; Mitragotri, S. Effect of physicochemical and surface properties on in vivo fate of drug nanocarriers. Adv. Drug Deliv. Rev. 2019, 143, 3–21. [Google Scholar] [CrossRef]
- Sharma, G.; Valenta, D.T.; Altman, Y.; Harvey, S.; Xie, H.; Mitragotri, S.; Smith, J.W. Polymer particle shape independently influences binding and internalization by macrophages. J. Control. Release 2010, 147, 408–412. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Banerjee, A.; Qi, J.; Gogoi, R.; Wong, J.; Mitragotri, S. Role of nanoparticle size, shape and surface chemistry in oral drug delivery. J. Control. Release 2016, 238, 176–185. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Elci, S.G.; Jiang, Y.; Yan, B.; Kim, S.T.; Saha, K.; Moyano, D.F.; Tonga, G.Y.; Jackson, L.C.; Rotello, V.M.; Vachet, R.W. Surface Charge Controls the Suborgan Biodistributions of Gold Nanoparticles. Nano 2016, 10, 5536–5542. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Xiao, K.; Li, Y.; Luo, J.; Lee, J.S.; Xiao, W.; Gonik, A.M.; Agarwal, R.G.; Lam, K.S. The effect of surface charge on in vivo biodistribution of PEG-oligocholic acid based micellar nanoparticles. Biomaterials 2011, 32, 3435–3446. [Google Scholar] [CrossRef] [Green Version]
- Wu, L.; Liu, M.; Shan, W.; Zhu, X.; Li, L.; Zhang, Z.; Huymg, Y. Bioinspired butyrate-functionalized nanovehicles for targeted oral delivery of biomacromolecular drugs. J. Control. Release 2017, 262, 273–283. [Google Scholar] [CrossRef]
- Castro, A.; Berois, N.; Malanga, A.; Ortega, C.; Oppezzo, P.; Pristch, O.; Mombrú, A.W.; Osinaga, E.; Pardo, E. Docetaxel in chitosan-based nanocapsules conjugated with an anti-Tn antigen mouse/human chimeric antibody as a promising targeting strategy of lung tumors. Int. J. Biol. Macromol. 2021, 182, 806–814. [Google Scholar] [CrossRef]
- Abid, S.; Hussain, T.; Nazir, A.; Zahir, A.; Khenoussi, N. A novel double-layered polymeric nanofiber-based dressing with controlled drug delivery for pain management in burn wounds. Polym. Bull. 2019, 76, 6387–6411. [Google Scholar] [CrossRef]
- Amiri, N.; Ajami, S.; Shahroodi, A.; Jannatabadi, N.; Darban, S.A.; Bazzaz, B.S.F.; Pishavar, E.; Kalalinia, F.; Movaffagh, J. Teicoplanin-loaded chitosan-PEO nanofibers for local antibiotic delivery and wound healing. Int. J. Biol. Macromol. 2020, 162, 645–656. [Google Scholar] [CrossRef]
- Quinones, J.P.; Peniche, H.; Peniche, C. Chitosan based self-assembled nanoparticles in drug delivery. Polymers 2018, 235. [Google Scholar] [CrossRef] [Green Version]
- Roy, H.; Nayak, B.S.; Nandi, S. Chitosan anchored nanoparticles in current drug development utilizing computer-aided pharmacokinetic modeling: Case studies for target specific cancer treatment and future prospective. Curr. Pharm. Des. 2020, 26, 1666–1675. [Google Scholar] [CrossRef] [PubMed]
- Hassani, A.; Hussain, S.A.; Abdullah, N.; Kmaruddin, S. Review on micro-encapsulation with Chitosan for pharmaceutical applications. MOJ Curr. Res. Rev. 2018, 1, 77–84. [Google Scholar] [CrossRef]
- Sang, Z.; Qian, J.; Han, J.; Deng, X.; Shen, J.; Li, G.; Xie, Y. Comparison of three water-soluble polyphosphate tripolyphosphate, phytic acid, and sodium hexametaphosphate as crosslinking agents in chitosan nanoparticle formulation. Carbohydr. Polym. 2020, 230, 115577. [Google Scholar] [CrossRef] [PubMed]
- Pan, C.; Qian, J.; Zhao, C.; Yang, H.; Zhao, X.; Guo, H. Study on the relationship between crosslinking degree and properties of TPP crosslinked chitosan nanoparticles. Carbohydr. Polym. 2020, 241, 116349. [Google Scholar] [CrossRef]
- Echeverri-Cuartas, C.E.; Gartner, C.; Lapitsky, Y. PEGylation and folate conjugation effects on the stability of chitosan-tripolyphosphate nanoparticles. Int. J. Biol. Macromol. 2020, 158, 1055–1062. [Google Scholar] [CrossRef]
- Abdelgawad, A.M.; Hudson, S.M. Chitosan nanoparticles: Polyphosphates cross-linking and protein delivery properties. Int. J. Biol. Macromol. 2019, 136, 133–142. [Google Scholar] [CrossRef] [PubMed]
- Cai, Y.; Lapitsky, Y. Biomolecular uptake effects on chitosan/tripolyphosphate micro- and nanoparticle stability. Colloids Surf. B-Biointerfaces 2020, 193, 111081. [Google Scholar] [CrossRef]
- Cai, Y.; Lapitsky, Y. Pitfalls in analyzing release from chitosan/tripolyphosphate micro- and nanoparticles. Eur. J. Pharm. Biopharm. 2019, 142, 204–215. [Google Scholar] [CrossRef] [PubMed]
- Wu, D.; Zhu, L.; Li, Y.; Zhang, X.; Xu, S.; Yang, G.; Delair, T. Chitosan-Based colloidal polyelectrolyte complexes for drug delivery: A review. Carbohydr. Polym. 2020, 238, 116126. [Google Scholar] [CrossRef] [PubMed]
- Boudoukhani, M.; Yahoum, M.M.; Lefnaoui, S.; Moulai-Mostefa, N.; Banhobre, M. Synthesis, characterization and evaluation of deacetylated xanthan derivatives as new excipients in the formulation of chitosan-based polyelectrolytes for the sustained release of tramadol. Saudi Pharm. J. 2019, 27, 1127–1137. [Google Scholar] [CrossRef]
- Liu, L.; Yang, H.; Lou, Y.; Wu, J.-Y.; Miao, J.; Lu, X.-Y.; Gao, J.-Q. Enhancement of oral bioavailability of salmon calcitonin through chitosan-modified, dual drug-loaded nanoparticles. Int. J. Pharm. 2019, 557, 170–177. [Google Scholar] [CrossRef]
- Luesakul, U.; Puthong, S.; Sansanaphongpricha, K.; Muangsin, N. Quaternizedchitosan-Coated nanoemulsions: A novel platform for improving the stability, anti-inflammatory, anti-cancer and transdermal properties of Plai extract. Carbohydr. Polym. 2020, 230, 115625. [Google Scholar] [CrossRef]
- Chaudhary, S.; Kumar, S.; Kumar, V.; Sharma, R. Chitosan nanoemulsions as advanced edible coatings for fruits and vegetables: Composition, fabrication and developments in last decade. Int. J. Biol. Macromol. 2020, 152, 154–170. [Google Scholar] [CrossRef]
- Shahab, M.S.; Rizwanullah, M.; Alshehri, S.; Imam, S.S. Optimization to development of chitosan decorated polycaprolactone nanoparticles for improved ocular delivery of dorzolamide: In vitro, ex vivo and toxicity assessments. Int. J. Biol. Macromol. 2020, 163, 2392–2404. [Google Scholar] [CrossRef]
- Krishna Sailaja, A.; Amareshwar, P. Preparation of bovine serum albumin loaded chitosan nanoparticles using reverse micelle method. Res. J. Pharm. Biol. Chem. Sci. 2011, 2, 837–846. [Google Scholar]
- Zhang, K.; Xu, Y.; Lu, L.; Shi, C.; Huang, Y.; Mao, Z.; Duan, C.; Ren, X.; Guo, Y.; Huang, C. Hydrodynamic cavitation: A feasible approach to intensify the emulsion cross-linking process for chitosan nanoparticle synthesis. Ultrason. Sonochem. 2021, 74, 105551. [Google Scholar] [CrossRef]
- Zhang, H.; Li, X.; Kang, H. Chitosan coatings incorporated with free or nano-encapsulated Paulownia Tomentosa essential oil to improve shelf-life of ready-to-cook pork chops. LWT Food Sci. Technol. 2019, 116, 108580. [Google Scholar] [CrossRef]
- Riegger, B.R.; Bäurer, B.; Mirzayeva, A.; Tovar, G.E.M.; Bach, M. A systematic approach of chitosan nanoparticle preparation via emulsion crosslinking as potential adsorbent in wastewater treatment. Carbohydr. Polym. 2018, 180, 46–54. [Google Scholar] [CrossRef]
- Kumar, S.; Dilbaghi, N.; Saharan, R.; Bhanjana, G. Nanotechnology as emerging tool for enhancing solubility of poorly water-soluble drugs. BioNanoScience 2012, 4, 227–250. [Google Scholar] [CrossRef]
- Seyam, S.; Nordin, N.A.; Alfatama, M. Recent Progress of Chitosan and Chitosan Derivatives-Based Nanoparticles: Pharmaceutical Perspectives of Oral Insulin Delivery. Pharmaceuticals 2020, 13, 307. [Google Scholar] [CrossRef]
- Essa, D.; Choonara, Y.E.; Kondiah, P.P.D.; Pillay, V. Comparative nanofabrication of PLGA-Chitosan-PEG systems employing microfluidics and emulsification solvent evaporation techniques. Polymers 2020, 12, 1882. [Google Scholar] [CrossRef]
- Orellano, M.S.; Longo, G.S.; Porporatto, C.; Correa, N.M.; Falcone, R.D. Role of micellar interface in the synthesis of chitosan nanoparticles formulated by reverse micellar method. Colloid Surf. A Physicochem. Eng. Asp. 2020, 599, 124876. [Google Scholar] [CrossRef]
- Haidar, M.K.; Demirbolat, G.M.; Timur, S.S.; Gürsoy, R.N.; Nemutlu, E.; Ulubayram, K.; Öner, L.; Eroğlu, H. Atorvastatin-Loaded nanosprayed chitosan nanoparticles for peripheral nerve injury. Bioinspired Biomimetic Nanobiomater. 2020, 9, 74–84. [Google Scholar] [CrossRef]
- Lucas, J.; Ralaivao, M.; Estevinho, B.N.; Rocha, F. A new approach for the microencapsulation of curcumin by a spray drying method, in order to value food products. Powder Technol. 2020, 362, 428–435. [Google Scholar] [CrossRef]
- Ozturk, A.A.; Kıyan, H.T. Treatment of oxidative stress-induced pain and inflammation with dexketoprofen trometamol loaded different molecular weight chitosan nanoparticles: Formulation, characterization and anti-inflammatory activity by using in vivo HET-CAM assay. Microvasc. Res. 2020, 128, 103961. [Google Scholar] [CrossRef] [PubMed]
- Peng, H.H.; Hong, D.X.; Guan, Y.X.; Yao, S.J. Preparation of pH-responsive DOX-loaded chitosan nanoparticles using supercritical assisted atomization with an enhanced mixer. Int. J. Pharm. 2019, 558, 82–90. [Google Scholar] [CrossRef]
- Peng, H.H.; Wang, Z.D.; Guan, Y.X.; Yao, S.J. Supercritical CO2 assisted preparation of chitosan-based nano-in-microparticles with potential for efficient pulmonary drug delivery. J. CO2 Util. 2021, 46, 101486. [Google Scholar] [CrossRef]
- Jalvo, B.; Faraldos, M.; Bahamonde, A.; Rosal, R. Antibacterial surfaces prepared by electrospray coating of photocatalytic nanoparticles. Chem. Eng. J. 2018, 334, 1108–1118. [Google Scholar] [CrossRef]
- Pawar, A.; Thakkar, S.; Misra, M. A Bird’s Eye view of nanoparticles prepared by electrospraying: Advancements in drug delivery field. J. Control. Release. 2018, 286, 179–200. [Google Scholar] [CrossRef]
- Kurakula, M.; Naveen, N.R. Electrospraying: A facile technology unfolding the Chitosan based drug delivery and biomedical applications. Eur. Polym. J. 2021, 147, 110326. [Google Scholar] [CrossRef]
- Wang, Y.; Zhang, R.; Qin, W.; Dai, J.; Zhang, Q.; Lee, K.; Liu, Y. Physicochemical properties of gelatin films containing tea polyphenol-loaded chitosan nanoparticles generated by electrospray. Mater. Des. 2020, 185, 108277. [Google Scholar] [CrossRef]
- Perera, U.M.S.P.; Rajapakse, N. Chitosan nanoparticles: Preparation, characterization, and applications. In Seafood Processing By-Products; Springer: New York, NY, USA, 2014; pp. 371–387. [Google Scholar]
- Gao, Y.; Ma, Q.; Cao, J.; Wang, Y.; Yang, X.; Xu, Q.; Liang, Q.; Sun, Y. Recent advances in microfluidic-aided chitosan-based multifunctional materials for biomedical applications. Int. J. Pharm. 2021, 600, 120465. [Google Scholar] [CrossRef]
- Ma, Q.; Cao, J.; Gao, Y.; Han, S.; Liang, Y.; Zhang, T.; Wang, X.; Sun, Y. Microfluidic-mediated nano-drug delivery systems: From fundamentals to fabrication for advanced therapeutic applications. Nanoscale 2020, 12, 15512–15527. [Google Scholar] [CrossRef]
- Zhu, C.Z.; Yao, R.Y.; Chen, Y.J.; Feng, M.R.; Ma, S.; Zhang, C.C. Self-assembly of fluorinated gradient copolymer in three-dimensional co-flow focusing microfluidic. J. Colloid Interface Sci. 2018, 526, 75–82. [Google Scholar] [CrossRef]
- Collins, D.J.; Neild, A.; de Mello, A.; Liu, A.Q.; Ai, Y. The Poisson distribution and beyond: Methods for microfluidic droplet production and single cell encapsulation. Lab. Chip 2015, 15, 3439–3459. [Google Scholar] [CrossRef] [PubMed]
- Gomez-Mascaraque, L.G.; Sanchez, G.; Lopez-Rubio, A. Impact of molecular weight on the formation of electrosprayed chitosan microcapsules as delivery vehicles for bioactive compounds. Carbohydr. Polym. 2016, 150, 121–130. [Google Scholar] [CrossRef] [Green Version]
- Lari, A.S.; Zahedi, P.; Ghourchian, H.; Khatibi, A. Microfluidic-based synthesized carboxymethyl chitosan nanoparticles containing metformin for diabetes therapy: In vitro and in vivo assessments. Carbohydr. Polym. 2021, 261, 117889. [Google Scholar] [CrossRef]
- Farahani, M.; Moradikhah, F.; Shabani, I.; Soflou, R.K.; Seyedjafari, E. Microfluidic fabrication of berberine-loaded nanoparticles for cancer treatment applications. J. Drug Deliv. Sci. Technol. 2021, 61, 102134. [Google Scholar] [CrossRef]
- Chisty, A.H.; Masud, R.A.; Hasan, M.M.; Khan, M.N.; Mallik, A.K.; Rahman, M.M. Chapter 3—PEGylated chitin and chitosan derivatives. In Handbook of Chitin and Chitosan; Elsevier: Amsterdam, The Netherlands, 2020; pp. 59–100. [Google Scholar]
- Malhotra, M.; Tomaro-Duchesneau, C.; Saha, S.; Prakash, S. Systemic siRNA Delivery via peptide-tagged polymeric nanoparticles, targeting PLK1 gene in a mouse xenograft model of colorectal Cancer. Int. J. Biomater. 2013, 2013, 252531. [Google Scholar] [CrossRef]
- Casey, S.L.; Wilson, L.D. Investigation of Chitosan-PVA composite films and their adsorption properties. J. Geosci. Environ. Prot. 2015, 3, 78–84. [Google Scholar] [CrossRef]
- Menazea, A.A.; Ismail, A.M.; Awwad, N.S.; Ibrahium, H.A. Physical characterization and antibacterial activity of PVA/Chitosan matrix doped by selenium nanoparticles prepared via one-pot laser ablation route. J. Mater. Res. Technol. 2020, 9, 9598–9606. [Google Scholar] [CrossRef]
- Sohail, R.; Abbas, S.R. Evaluation of amygdalin-loaded alginate-chitosan nanoparticles as biocompatible drug delivery carriers for anticancerous effificacy. Int. J. Biol. Macromol. 2020, 153, 36–45. [Google Scholar] [CrossRef]
- Wang, F.; Li, J.; Tang, X.; Huang, K.; Chen, L. Polyelectrolyte three layer nanoparticles of chitosan/dextran sulfate/chitosan for dual drug delivery. Colloid Surf. B Biointerfaces 2020, 190, 110925. [Google Scholar] [CrossRef]
- Hu, Q.; Hu, S.; Fleming, E.; Lee, J.Y.; Luo, Y. Chitosan-Caseinate-Dextran ternary complex nanoparticles for potential oral delivery of astaxanthin with signifificantly improved bioactivity. Int. J. Biol. Macromol. 2020, 151, 747–756. [Google Scholar] [CrossRef]
- Sabra, R.; Roberts, C.J.; Billa, N. Courier properties of modified citrus pectinate-chitosan nanoparticles in colon delivery of curcumin. Colloid Interface Sci. Commun. 2019, 32, 100192. [Google Scholar] [CrossRef]
- Lopes, M.; Shrestha, N.; Correia, A.; Shahbazi, M.A.; Sarmento, B.; Hirvonen, J.; Veiga, F.; Seiça, R.; Ribeiro, A.; Santos, H.A. Dual chitosan/albumin-coated alginate/dextran sulfate nanoparticles for enhanced oral delivery of insulin. J. Control. Release 2016, 232, 29–41. [Google Scholar] [CrossRef] [PubMed]
- Anirudhan, T.S.; Parvathy, J. Novel Thiolated Chitosan-Polyethyleneglycol blend/Montmorillonite composite formulations for the oral delivery of insulin. Bioact. Carbohydr. Diet. Fibre 2018, 16, 22–29. [Google Scholar] [CrossRef]
- Li, J.; Tian, S.; Tao, Q.; Zhao, Y.; Gui, R.; Yang, F.; Zang, L.; Chen, Y.; Ping, Q.; Hou, D. Montmorillonite/Chitosan nanoparticles as a novel controlled-release topical ophthalmic delivery system for the treatment of glaucoma. Int. J. Nanomed. 2018, 13, 3975–3987. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Luo, C.; Yang, Q.; Lin, X.; Qi, C.; Li, G. Preparation and drug release property of tanshinone IIA loaded chitosan montmorillonite microspheres. Int. J. Biol. Macromol. 2019, 125, 721–729. [Google Scholar] [CrossRef]
- Hou, Y.T.; Wu, K.C.E.; Lee, C.Y. Development of glycyrrhizin-conjugated, chitosan-coated, lysine-embedded mesoporous silica nanoparticles for hepatocyte-targeted liver tissue regeneration. Materialia 2020, 9, 100568. [Google Scholar] [CrossRef]
- Chen, C.; Yao, W.; Sun, W.; Guo, T.; Lv, H.; Wang, X.; Ying, H.; Wang, Y.; Wang, P. A self-targeting and controllable drug delivery system constituting mesoporous silica nanoparticles fabricated with a multi-stimuli responsive chitosan-based thin film layer. Int. J. Biol. Macromol. 2019, 122, 1090–1099. [Google Scholar] [CrossRef]
- Qiu, Q.; Quan, Z.; Zhang, H.; Qin, X.; Wang, R.; Yu, J. pH-triggered sustained drug release of multilayer encapsulation system with hollow mesoporous silica nanoparticles/chitosan/polyacrylic acid. Mater. Lett. 2020, 260, 126907. [Google Scholar] [CrossRef]
- Liao, T.; Liu, C.; Ren, J.; Chen, H.; Kuang, Y.; Jiang, B.; Chen, J.; Sun, Z.; Li, C. A chitosan/mesoporous silica nanoparticle-based anticancer drug delivery system with a “tumor-triggered targeting” property. Int. J. Biol. Macromol. 2021, 183, 2017–2029. [Google Scholar] [CrossRef]
- Piosik, E.; Klimczak, P.; Ziegler-Borowska, M.; Chełminiak-Dudkiewicz, A. A detailed investigation on interactions between magnetite nanoparticles functionalized with aminated chitosan and a cell model membrane. Mater. Sci. Eng. C 2020, 109, 110616. [Google Scholar] [CrossRef] [PubMed]
- Salmanian, G.; Hassanzadeh-Tabrizi, S.A.; Koupaei, N. Magnetic chitosan nanocomposites for simultaneous hyperthermia and drug delivery applications: A review. Int. J. Biol. Macromol. 2021, 184, 618–635. [Google Scholar] [CrossRef]
- Araujo, H.C.; Gomes da Silva, A.C.; Paião, L.I.; Magario, M.K.W.; Frasnelli, F.C.T.; Oliveira, S.H.P.; Pessan, J.P.; Monteiro, D.R. Antimicrobial, antibiofilm and cytotoxic effects of a colloidal nanocarrier composed by chitosan-coated iron oxide nanoparticles loaded with chlorhexidine. J. Dent. 2020, 101, 103453. [Google Scholar] [CrossRef] [PubMed]
- Khmara, I.; Molcan, M.; Antosova, A.; Bednarikova, Z.; Zavisova, V.; Kubovcikova, K.; Jurikova, A.; Girman, V.; Baranovicova, E.; Koneracka, M.; et al. Bioactive properties of chitosan stabilized magnetic nanoparticles—Focus on hyperthermic and anti-amyloid activities. J. Magn. Magn. Mater. 2020, 513, 167056. [Google Scholar] [CrossRef]
- Bandeira, A.C.; de Oliveira Matos, A.; Evangelista, B.S.; da Silva, S.M.; Nagib, P.R.A.; de Moraes Crespo, A.; Amaral, A.C. Is it possible to track intracellular chitosan nanoparticles using magnetic nanoparticles as contrast agent? Bioorg. Med. Chem. 2019, 27, 2637–2643. [Google Scholar] [CrossRef] [PubMed]
- Anirudhan, T.S.; Sekhar, V.C.; Athira, V.S. Graphene oxide based functionalized chitosan polyelectrolyte nanocomposite for targeted and pH responsive drug delivery. Int. J. Biol. Macromol. 2020, 150, 468–479. [Google Scholar] [CrossRef] [PubMed]
- Rebekah, A.; Sivaselvam, S.; Viswanathan, C.; Prabhu, D.; Gautam, R.; Ponpandian, N. Magnetic nanoparticle-decorated graphene oxide-chitosan composite as an efficient nanocarrier for protein delivery. Colloid Surf. A Physicochem. Eng. Asp. 2021, 610, 125913. [Google Scholar] [CrossRef]
- Baktash, M.S.; Zarrabi, A.; Avazverdi, E.; Reis, N.M. Development and optimization of a new hybrid chitosan-grafted graphene oxide/magnetic nanoparticle system for theranostic applications. J. Mol. Liq. 2021, 322, 114515. [Google Scholar] [CrossRef]
- Khademi, Z.; Lavaee, P.; Ramezani, M.; Alibolandi, M.; Abnous, K.; Taghdisi, S.M. Co-Delivery of doxorubicin and aptamer against Forkhead box M1 using chitosan-gold nanoparticles coated with nucleolin aptamer for synergistic treatment of cancer cells. Carbohydr. Polym. 2020, 248, 116735. [Google Scholar] [CrossRef]
- Salem, D.S.; Hegazy, S.F.; Obayya, S.S.A. Nanogold-loaded chitosan nanocomposites for pH/light-responsive drug release and synergistic chemo-photothermal cancer therapy. Colloid Interface Sci. Commun. 2021, 41, 100361. [Google Scholar] [CrossRef]
- Saravanakumar, K.; Mariadoss, A.V.A.; Sathiyaseelan, A.; Wang, M.H. Synthesis and characterization of nano-chitosan capped gold nanoparticles with multifunctional bioactive properties. Int. J. Biol. Macromol. 2020, 165, 747–757. [Google Scholar] [CrossRef]
- López-Pérez, G.; Prado-Gotor, R.; Fuentes-Rojas, J.A.; Martin-Valero, M.J. Understanding gold nanoparticles interactions with chitosan: Crosslinking agents as novel strategy for direct covalent immobilization of biomolecules on metallic surfaces. J. Mol. Liq. 2020, 302, 112381. [Google Scholar] [CrossRef]
- Wu, H.; Zhang, J. Chitosan-based zinc oxide nanoparticle for enhanced anticancer effect in cervical cancer: A physicochemical and biological perspective. Saudi Pharm. J. 2018, 26, 205–210. [Google Scholar] [CrossRef]
- Singh, T.A.; Das, J.; Sil, P.C. Zinc oxide nanoparticles: A comprehensive review on its synthesis, anticancer and drug delivery applications as well as health risks. Adv. Colloid Interface Sci. 2020, 286, 102317. [Google Scholar] [CrossRef]
- George, D.; Maheswari, P.U.; Begum, K.M.M.S. Cysteine conjugated chitosan based green nanohybrid hydrogel embedded with zinc oxide nanoparticles towards enhanced therapeutic potential of naringenin. React. Funct. Polym. 2020, 148, 104480. [Google Scholar] [CrossRef]
- Ghaffari, S.B.; Sarrafzadeh, M.H.; Salami, M.; Khorramizadeh, M.R. A pH-sensitive delivery system based on N-succinyl chitosan-ZnO nanoparticles for improving antibacterial and anticancer activities of curcumin. Int. J. Biol. Macromol. 2020, 151, 428–440. [Google Scholar] [CrossRef] [PubMed]
- Kandra, R.; Bajpai, S. Synthesis, mechanical properties of fluorescent carbon dots loaded nanocomposites chitosan film for wound healing and drug delivery. Arab. J. Chem. 2020, 13, 4882–4894. [Google Scholar] [CrossRef]
- Lin, C.; Sun, K.; Zhang, C.; Tan, T.; Xu, M.; Liu, Y.; Xu, C.; Wang, Y.; Li, L.; Whittaker, A. Carbon dots embedded metal organic framework @ chitosan core-shell nanoparticles for vitro dual mode imaging and pH-responsive drug delivery. Microporous Mesoporous Mater. 2020, 293, 109775. [Google Scholar] [CrossRef]
- Sheng, Y.; Dai, W.; Gao, J.; Li, H.; Tan, W.; Wang, J.; Deng, L.; Kong, Y. pH-sensitive drug delivery based on chitosan wrapped graphene quantum dots with enhanced flfluorescent stability. Mater. Sci. Eng. C 2020, 112, 110888. [Google Scholar] [CrossRef] [PubMed]
- Dong, X.; Wei, C.; Liang, J.; Liu, T.; Kong, D.; Lv, F. Thermosensitive hydrogel loaded with chitosan-carbon nanotubes for near infrared light triggered drug delivery. Colloid Surf. B Biointerfaces 2017, 154, 253–262. [Google Scholar] [CrossRef] [PubMed]
- Singh, R.P.; Sonali, G.S.; Singh, S.; Bharti, S.; Pandey, B.L.; Koch, B.; Muthu, M.S. Chitosan-Folate decorated carbon nanotubes for site specific lung cancer delivery. Mater. Sci. Eng. C 2017, 77, 446–458. [Google Scholar] [CrossRef]
- Ghaffar, I.; Imran, M.; Perveen, S.; Kanwal, T.; Saifullah, S.; Bertino, M.F.; Ehrhardt, C.J.; Yadavalli, V.K.; Shah, M.R. Synthesis of chitosan coated metal organic frameworks (MOFs) for increasing vancomycin bactericidal potentials against resistant S. aureus strain. Mater. Sci. Eng. C 2019, 105, 110111. [Google Scholar] [CrossRef]
- Li, L.; Han, S.; Zhao, S.; Li, X.; Liuab, B.; Liu, Y. Chitosan modified metal–organic frameworks as a promising carrier for oral drug delivery. RSC Adv. 2020, 10, 45130–45138. [Google Scholar] [CrossRef]
- Xu, T.; Zhang, J.; Chi, H.; Cao, F. Multifunctional properties of organic-inorganic hybrid nanocomposites based on chitosan derivatives and layered double hydroxides for ocular drug delivery. Acta Biomaterialia 2016, 36, 152–163. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Zhou, L.; Fang, L.; Cao, F. Multifunctional carboxymethyl chitosan derivatives-layered double hydroxide hybrid nanocomposites for effifficient drug delivery to the posterior segment of the eye. Acta Biomaterialia 2020, 104, 104–114. [Google Scholar] [CrossRef] [PubMed]
- Elanchezhiyan, S.S.; Meenakshi, S. Synthesis and characterization of chitosan/Mg-Al layered double hydroxide composite for the removal of oil particles from oil-in-water emulsion. Int. J. Biol. Macromol. 2017, 104, 1586–1595. [Google Scholar] [CrossRef]
- Sabourian, P.; Tavakolian, M.; Yazdani, H.; Frounchi, M.; van de Ven, T.G.M.; Maysinger, D.; Kakkar, A. Stimuli-responsive chitosan as an advantageous platform for efficient delivery of bioactive agents. J. Control. Release 2020, 317, 216–231. [Google Scholar] [CrossRef] [PubMed]
- Constantin, M.; Bucatariu, S.M.; Doroftei, F.; Fundueanu, G. Smart composite materials based on chitosan microspheres embedded in thermosensitive hydrogel for controlled delivery of drugs. Carbohydr. Polym. 2017, 157, 493–502. [Google Scholar] [CrossRef] [PubMed]
- Liu, H.; Liu, J.; Xie, X.; Li, X. Development of photo-magnetic drug delivery system by facile-designed dual stimuli-responsive modifed biopolymeric chitosan capped nano-vesicle to improve efficiency in the anesthetic effect and its biological investigations. J. Photochem. Photobiol. B Biol. 2020, 202, 111716. [Google Scholar] [CrossRef] [PubMed]
- Daund, V.; Chalke, S.; Sherje, A.P.; Kale, P.P. ROS responsive mesoporous silica nanoparticles for smart drug delivery: A review. J. Drug Deliv. Sci. Technol. 2021, 64, 102599. [Google Scholar] [CrossRef]
- Jiao, J.; Li, X.; Zhang, S.; Liu, J.; Di, D.; Zhang, Y.; Zhao, Q.; Wang, S. Redox and pH dual-responsive PEG and chitosan-conjugated hollow mesoporous silica for controlled drug release. Mater. Sci. Eng. C 2016, 67, 26–33. [Google Scholar] [CrossRef]
- Lin, J.T.; Liu, Z.K.; Zhu, Q.L.; Rong, X.H. Liang, C.L.; Wang, J.; Ma, D.; Sun, J.; Wan, G.H. Redox-Responsive nanocarriers for drug and gene co-delivery based on chitosan derivatives modifified mesoporous silica nanoparticles. Colloid Surf. B Biointerfaces 2017, 155, 41–50. [Google Scholar] [CrossRef]
- Rastegari, B.; Karbalaei-Heidari, H.R.; Zeinali, S.; Sheardown, H. The enzyme-sensitive release of prodigiosin grafted β-cyclodextrin and chitosan magnetic nanoparticles as an anticancer drug delivery system: Synthesis, characterization and cytotoxicity studies. Colloid Surf. Biointerfaces 2017, 158, 589–601. [Google Scholar] [CrossRef] [PubMed]
- Baghbani, F.; Chegeni, M.; Moztarzadeh, F.; Hadian-Ghazvini, S.; Raz, M. Novel ultrasound-responsive chitosan/perfluorohexane nanodroplets for image-guided smart delivery of an anticancer agent: Curcumin. Mat. Sci. Eng. C 2017, 74, 186–193. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Mathew, S.A.; Prakash, P.A.; Jaabir, M.S.M.; Dhanavel, S.; Manikandan, R.; Stephen, A. Dopamine-Conjugated CuS/chitosan nanocomposite for targeted photothermal drug delivery: In vitro cytotoxicity study to establish bio-compatibility. J. Drug Deliv. Sci. Technol 2021, 61, 102193. [Google Scholar] [CrossRef]
- Bhatta, A.; Krishnamoorthy, G.; Marimuthu, N.; Dihingia, A.; Manna, P.; Biswal, H.T.; Das, M.; Krishnamoorthy, G. Chlorin e6 decorated doxorubicin encapsulated chitosan nanoparticles for photo-controlled cancer drug delivery. Int. J. Biol. Macromol. 2019, 136, 951–961. [Google Scholar] [CrossRef] [PubMed]
- Sudhakar, S.; Chandran, S.V.; Selvamurugan, N.; Nazeer, R.A. Biodistribution and pharmacokinetics of thiolated chitosan nanoparticles for oral delivery of insulin in vivo. Int. J. Biol. Macromol. 2020, 150, 281–288. [Google Scholar] [CrossRef] [PubMed]
- Mumuni, M.A.; Kenechukwu, F.C.; Ofokansi, K.C.; Attama, A.A.; Díaz Díaz, D. Insulin-loaded mucoadhesive nanoparticles based on mucin-chitosan complexes for oral delivery and diabetes treatment. Carbohydr. Polym. 2020, 229, 115506. [Google Scholar] [CrossRef] [PubMed]
- Tsai, L.C.; Chen, C.H.; Lin, C.W.; Ho, Y.C.; Mi, F.L. Development of multifunctional nanoparticles self-assembled from trimethyl chitosan and fucoidan for enhanced oral delivery of insulin. Int. J. Biol. Macromol. 2019, 126, 141–150. [Google Scholar] [CrossRef]
- Wong, C.Y.; Al-Salami, H.; Dass, C.R. Formulation and characterisation of insulin-loaded chitosan nanoparticles capable of inducing glucose uptake in skeletal muscle cells in vitro. J. Drug Deliv. Sci. Technol. 2020, 57, 101738. [Google Scholar] [CrossRef]
- Abdel-Moneim, A.; El-Shahawy, A.; Yousef, A.I.; Abd El-Twab, S.M.; Elden, Z.E.; Taha, M. Novel polydatin-loaded chitosan nanoparticles for safe and efficient type 2 diabetes therapy: In silico, in vitro and in vivo approaches. Int. J. Biol. Macromol. 2020, 154, 1496–1504. [Google Scholar] [CrossRef]
- Coutinho, A.J.; Costa Lima, S.A.; Afonso, C.M.M.; Reis, S. Mucoadhesive and pH responsive fucoidan-chitosan nanoparticles for the oral delivery of methotrexate. Int. J. Biol. Macromol. 2020, 158, 180–188. [Google Scholar] [CrossRef]
- Xavier, F.H., Jr.; Gueutin, C.; Chacun, H.; Vauthier, C.; Egito, E.S.T. Mucoadhesive paclitaxel-loaded chitosan-poly (isobutyl cyanoacrylate) core-shell nanocapsules containing copaiba oil designed for oral drug delivery. J. Drug Deliv. Sci. Technol. 2019, 53, 101194. [Google Scholar] [CrossRef]
- Du, X.; Yin, S. Xu, L.; Ma, J.; Yu, H.; Wang, G.; Li, J. Polylysine and cysteine functionalized chitosan nanoparticle as an efficient platform for oral delivery of paclitaxel. Carbohydr. Polym. 2020, 229, 115484. [Google Scholar] [CrossRef]
- Tran, P.H.L.; Wang, T.; Yang, C.; Tran, T.T.D.; Duan, W. Development of conjugate-by-conjugate structured nanoparticles for oral delivery of docetaxel. Mater. Sci. Eng. C 2020, 107, 110346. [Google Scholar] [CrossRef] [PubMed]
- Sharma, M.; Sharma, R.; Jain, D.K.; Saraf, A. Enhancement of oral bioavailability of poorly water soluble carvedilol by chitosan nanoparticles: Optimization and pharmacokinetic study. Int. J. Biol. Macromol. 2019, 135, 246–260. [Google Scholar] [CrossRef]
- Pauluk, D.; Padilha, A.K.; Khalil, N.M.; Mainardes, R.M. Chitosan-Coated zein nanoparticles for oral delivery of resveratrol: Formation, characterization, stability, mucoadhesive properties and antioxidant. Food Hydrocoll. 2019, 94, 411–417. [Google Scholar] [CrossRef]
- Lin, C.; Kuo, T.C.; Lin, J.C.; Ho, Y.C.; Mi, F.L. Delivery of polysaccharides from Ophiopogon japonicus (OJPs) using OJPs/chitosan/whey protein co-assembled nanoparticles to treat defective intestinal epithelial tight junction barrier. Int. J. Biol. Macromol. 2020, 160, 558–570. [Google Scholar] [CrossRef]
- Ling, K.; Wu, H.; Neish, A.S.; Champion, J.A. Alginate/Chitosan microparticles for gastric passage and intestinal release of therapeutic protein nanoparticles. J. Control. Release 2019, 29, 174–186. [Google Scholar] [CrossRef] [PubMed]
- Muye, H.; Chen, Z.; Huibing, H.; Yu, J.; Yanzuo, C.; Kaiyan, L.; Feng, G. Cyclodextrin/chitosan nanoparticles for oral ovalbumin delivery: Preparation, characterization and intestinal mucosal immunity in mice. Asian J. Pharm. Sci. 2019, 14, 193–203. [Google Scholar] [CrossRef]
- Cole, H.; Bryan, D.; Lancaster, L.; Mawas, F.; Vllasaliu, D. Chitosan nanoparticle antigen uptake in epithelial monolayers can predict T mucosal but not systemic in vivo immune response by oral delivery. Carbohydr. Polym. 2018, 190, 248–254. [Google Scholar] [CrossRef] [PubMed]
- Saraf, S.; Jain, S.; Sahoo, R.N.; Mallick, S. Lipopolysaccharide derived alginate coated Hepatitis B antigen loaded chitosan nanoparticles for oral mucosal immunization. Int. J. Biol. Macromol. 2020, 154, 466–476. [Google Scholar] [CrossRef]
- Yu, X.; Wen, T.; Cao, P.; Shan, L.; Li, L. Alginate-chitosan coated layered double hydroxide nanocomposites for enhanced oral vaccine delivery. J. Colloid Interface Sci. 2019, 556, 258–265. [Google Scholar] [CrossRef] [PubMed]
- Dong, W.; Wang, X.; Liu, C.; Zhang, X.; Zhang, X.; Chen, X.; Kou, Y.; Mao, S. Chitosan based polymer-lipid hybrid nanoparticles for oral delivery of enoxaparin. Int. J. Pharm. 2018, 547, 499–505. [Google Scholar] [CrossRef]
- Murthy, A.; Ravi, P.R.; Kathuria, H.; Vats, R. Self-Assembled lecithin-chitosan nanoparticles improve the oral bioavailability and alter the pharmacokinetics of raloxifene. Int. J. Pharm. 2020, 588, 119731. [Google Scholar] [CrossRef]
- Yu, A.; Shi, H.; Liu, H.; Bao, Z.; Dai, M.; Lin, D.; Lin, D.; Xu, X.; Li, X.; Wang, Y. Mucoadhesive dexamethasone-glycol chitosan nanoparticles for ophthalmic drug delivery. Int. J. Pharm. 2020, 575, 118943. [Google Scholar] [CrossRef]
- Khalil, M.; Hashmi, U.; Riaz, R.; Abbas, S.R. Chitosan coated liposomes (CCL) containing triamcinolone acetonide for sustained delivery: A potential topical treatment for posterior segment Diseases. Int. J. Biol. Macromol. 2020, 143, 483–491. [Google Scholar] [CrossRef]
- Ameeduzzafar; Imam, S.S.; Bukhari, S.N.A.; Ahmad, J.; Ali, A. Formulation and optimization of levoflfloxacin loaded chitosan nanoparticle for ocular delivery: In-vitro characterization, ocular tolerance and antibacterial activity. Int. J. Biol. Macromol. 2018, 108, 650–659. [Google Scholar] [CrossRef]
- Cheng, Y.H.; Ko, Y.C.; Chang, Y.F.; Huang, S.H.; Liu, C.J. Thermosensitive chitosan-gelatin-based hydrogel containing curcuminloaded nanoparticles and latanoprost as a dual-drug delivery system for glaucoma treatment. Exp. Eye Res. 2019, 179, 179–187. [Google Scholar] [CrossRef] [PubMed]
- Abruzzo, A.; Cerchiara, T.; Bigucci, F.; Zuccheri, G.; Cavallari, C.; Saladini, B.; Luppi, B. Cromolyn-Crosslinked chitosan nanoparticles for the treatment of allergic Rhinitis. Eur. J. Pharm. Sci. 2019, 131, 136–145. [Google Scholar] [CrossRef]
- Sun, M.; Yu, X.; Wang, T.; Bi, S.; Liu, Y.; Chen, X. Nasal adaptive chitosan-based nano-vehicles for anti-allergic drug delivery. Int. J. Biol. Macromol. 2019, 135, 1182–1192. [Google Scholar] [CrossRef] [PubMed]
- Dumkliang, E.; Pamornpathomkul, B.; Patrojanasophon, P.; Ngawhirunpat, T.; Rojanarata, T.; Yoksan, S.; Opanasopit, P. Feasibility of chitosan-based nanoparticles approach for intranasal immunisation of live attenuated Japanese encephalitis vaccine. Int. J. Biol. Macromol. 2021, 183, 1096–1105. [Google Scholar] [CrossRef]
- Piazzini, V.; Landucci, E.; D’Ambrosio, M.; Fasiolo, L.T.; Cinci, L.; Colombo, G.; Pellegrini-Giampietro, D.E.; Bilia, A.R.; Luceri, C.; Bergonzi, M.C. Chitosan coated human serum albumin nanoparticles: A promising strategy for nose-to-brain drug delivery. Int. J. Biol. Macromol. 2019, 129, 267–280. [Google Scholar] [CrossRef]
- Chatzitaki, A.T.; Karavasili, S.J.C.; Andreadis, D.; Fatouros, D.G.; Borges, O. Chitosan-Coated PLGA nanoparticles for the nasal delivery of ropinirole hydrochloride: In vitro and ex vivo evaluation of efficacy and safety. Int. J. Pharm. 2020, 589, 119776. [Google Scholar] [CrossRef] [PubMed]
- Cassano, R.; Trapani, A.; Di Gioia, M.L.; Mandracchia, D.; Pellitteri, R.; Tripodo, G.; Trombino, S.; Di Gioia, S.; Conese, M. Synthesis and characterization of novel chitosan-dopamine or chitosantyrosine conjugates for potential nose-to-brain delivery. Int. J. Pharm. 2020, 589, 119829. [Google Scholar] [CrossRef] [PubMed]
- Sava, V.; Fihurka, O.; Khvorova, A.; Sanchez-Ramos, J. Enriched chitosan nanoparticles loaded with siRNA are effective in lowering Huntington’s disease gene expression following intranasal administration. Nanomed. Nanotechnol. Biol. Med. 2020, 24, 102119. [Google Scholar] [CrossRef]
- Khezri, F.A.N.Z.; Lakshmi, C.S.R.; Bukka, R.; Nidhi, M.; Nargund, S.L. Pharmacokinetic study and brain tissue analysis of Zolmitriptan loaded chitosan nanoparticles in rats by LC-MS method. Int. J. Biol. Macromol. 2020, 142, 52–62. [Google Scholar] [CrossRef] [PubMed]
- Bhattamisra, S.K.; Shak, A.T.; Xi, L.W.; Safian, N.H.; Choudhury, H.; Lim, W.M.; Shahzad, N.; Alhakamy, N.A.; Anwer, K.; Radhakrishnan, A.K.; et al. Nose to brain delivery of rotigotine loaded chitosan nanoparticles in human SH-SY5Y neuroblastoma cells and animal model of Parkinson’s disease. Int. J. Pharm. 2020, 579, 119148. [Google Scholar] [CrossRef] [PubMed]
- Wang, H.; Holgate, J.; Bartlett, S.; Islam, N. Assessment of nicotine release from nicotine-loaded chitosan nanoparticles dry powder inhaler formulations via locomotor activity of C57BL/6 mice. Eur. J. Pharm. Biopharm. 2020, 154, 175–185. [Google Scholar] [CrossRef]
- Ahmad, N.; Ahmad, R.; Alrasheed, R.A.; Almatar, H.M.A.; Al-Ramadan, A.S.; Buheazah, T.M.; AlHomoud, H.S.; Al-Nasif, H.A.; Alam, A. A Chitosan-PLGA based catechin hydrate nanoparticles used in targeting of lungs and cancer treatment. Saudi J. Biol. Sci. 2020, 27, 2344–2357. [Google Scholar] [CrossRef]
- Vieira, A.C.C.; Chaves, L.L.; Pinheiro, M.; Costa Lima, S.; Rolim Neto, P.J.; Ferreira, D.; Sarmento, B.; Reis, S. Lipid nanoparticles coated with chitosan using a one-step association method to target rifampicin to alveolar macrophages. Carbohydr. Polym. 2021, 25, 116978. [Google Scholar] [CrossRef]
- Pardeshi, C.V.; Agnihotri, V.V.; Patil, K.Y.; Pardeshi, S.R.; Surana, S.J. Mannose-Anchored N,N,N-trimethyl chitosan nanoparticles for pulmonary administration of etofylline. Int. J. Biol. Macromol. 2020, 165, 445–459. [Google Scholar] [CrossRef] [PubMed]
- Dhayanandamoorthy, Y.; Antoniraj, M.G.; Kandregula, C.A.B.; Kandasamy, R. Aerosolized hyaluronic acid decorated, ferulic acid loaded chitosan nanoparticle: A promising asthma control strategy. Int. J. Pharm. 2020, 591, 119958. [Google Scholar] [CrossRef]
- Rahbarian, M.; Mortazavian, E.; Dorkoosh, F.A.; Tehrani, M.R. Preparation, evaluation and optimization of nanoparticles composed of thiolated triethyl chitosan: A potential approach for buccal delivery of Insulin. J. Drug Deliv. Sci. Technol. 2018, 44, 254–263. [Google Scholar] [CrossRef]
- Stie, M.B.; Gätke, J.R.; Wan, F.; Chronakis, J.S.; Jacobsen, J.; Nielsen, H.M. Swelling of mucoadhesive electrospun chitosan/polyethylene oxide nanofibers facilitates adhesion to the sublingual mucosa. Carbohydr. Polym. 2020, 24, 116428. [Google Scholar] [CrossRef] [PubMed]
- Martin, V.; Ribeiro, I.A.C.; Alves, M.M.; Gonçalves, L.; Almeida, A.J.; Grenho, L.; Fernandes, M.H.; Santos, C.F.; Gomes, P.S.; Bettencourt, A.F. Understanding intracellular trafficking and anti-inflammatory effects of minocycline chitosan-nanoparticles in human gingival fibroblasts for periodontal disease treatment. Int. J. Pharm. 2019, 572, 118821. [Google Scholar] [CrossRef]
- Dos Santos, D.M.; Chagas, P.A.M.; Leite, I.S.; Inada, N.M.; de Annunzio, S.R.; Fontana, C.R.; Campana-Filho, S.P.; Correa, D.S. Core-sheath nanostructured chitosan-based nonwovens as a potential drug delivery system for periodontitis treatment. Int. J. Biol. Macromol. 2020, 142, 521–534. [Google Scholar] [CrossRef]
- Abd-Allah, H.; Abdel-Aziz, R.T.A.; Nasr, M. Chitosan nanoparticles making their way to clinical practice: A feasibility study on their topical use for acne treatment. Int. J. Biol. Macromol. 2020, 156, 262–270. [Google Scholar] [CrossRef] [PubMed]
- Ushirobira, C.Y.; Afiune, L.A.F.; Pereira, M.N.; Cunha-Filho, M.; Gelfuso, G.M.; Gratieri, T. Dutasteride nanocapsules for hair follicle targeting: Effect of chitosan-coating and physical stimulus. Int. J. Biol. Macromol. 2020, 151, 56–61. [Google Scholar] [CrossRef]
- Takeuchi, I.; Suzuki, T.; Makino, K. Iontophoretic transdermal delivery using chitosan-coated PLGA nanoparticles for transcutaneous immunization. Colloid Surf. A Physicochem. Eng. Asp. 2020, 608, 125607. [Google Scholar] [CrossRef]
- Morad, H.; Jahanshahi, M.; Akbari, J.; Saeedi, M.; Gill, P.; Enayatifard, R. Novel topical and transdermal delivery of colchicine with chitosan based biocomposite nanofiberous system; formulation, optimization, characterization, ex vivo skin deposition/permeation, and anti-melanoma evaluation. Mater. Chem. Phys. 2021, 263, 124381. [Google Scholar] [CrossRef]
- Nawaz, A.; Wong, T.W. Microwave as skin permeation enhancer for transdermal drug delivery of chitosan-5-fluorouracil nanoparticles. Carbohydr. Polym. 2017, 157, 906–919. [Google Scholar] [CrossRef]
- Fahimirad, S.; Abtahi, H.; Satei, P.; Ghaznavi-Rad, E.; Moslehi, M.; Ganji, A. Wound healing performance of PCL/Chitosan based electrospun nanofiber electrosprayed with curcumin loaded chitosan nanoparticles. Carbohydr. Polym. 2021, 259, 117640. [Google Scholar] [CrossRef]
- Shafique, M.; Sohail, M.; Minhas, M.U.; Khaliq, T.; Kousar, M.; Khan, S.; Hussain, Z.; Mahmood, A.; Abbasi, M.; Aziz, H.C.; et al. Bio-Functional hydrogel membranes loaded with chitosan nanoparticles for accelerated wound healing. Int. J. Biol. Macromol. 2021, 170, 207–221. [Google Scholar] [CrossRef] [PubMed]
- Manne, A.A.; Arigela, B.; Giduturi, A.K.; Komaravolu, R.K.; Mangamuri, U.; Poda, S. Pterocarpus marsupium Roxburgh heartwood extract/chitosan nanoparticles loaded hydrogel as an innovative wound healing agent in the diabetic rat model. Mater. Today Commun. 2021, 26, 101916. [Google Scholar] [CrossRef]
- Amaral, A.C.; Saavedra, P.H.V.; Souza, A.C.O.; de Melo, M.T.; Tedesco, A.C.; Morais, P.C.; Felipe, M.S.S.; Bocca, A.L. Miconazole loaded chitosan-based nanoparticles for local treatment of vulvovaginal candidiasis fungal infections. Colloids Surf. B Biointerfaces 2019, 174, 409–415. [Google Scholar] [CrossRef]
- Marciello, M.; Rossi, S.; Caramella, C.; Remunán-López, C. Freeze-Dried cylinders carrying chitosan nanoparticles for vaginal peptide delivery. Carbohydr. Polym. 2017, 170, 43–51. [Google Scholar] [CrossRef] [PubMed]
- Arumugam, G.; Rajendran, R. Callophycin A loaded chitosan and spicules based nanocomposites as an alternative strategy to overcome vaginal candidiasis. Int. J. Biol. Macromol. 2020, 161, 656–665. [Google Scholar] [CrossRef]
- Abdel Allah, N.H.; Gaber, Y.; Rashed, M.E.; Azmy, A.F.; Abou-Taleb, H.A.; Abdel Ghani, S. Alginate-Coated chitosan nanoparticles act as effective adjuvant for hepatitis A vaccine in mice. Int. J. Biol. Macromol. 2020, 152, 904–912. [Google Scholar] [CrossRef]
- Rebbouh, F.; Martin-Eauclaire, M.F.; Laraba-Djebari, F. Chitosan nanoparticles as a delivery platform for neurotoxin II from Androctonus australis hector scorpion venom: Assessment of toxicity and immunogenicity. Acta Tropica 2020, 205, 105353. [Google Scholar] [CrossRef]
- Abdelhamid, H.N.; Dowaidar, M.; Langel, U. Carbonized chitosan encapsulated hierarchical porous zeolitic imidazolate frameworks nanoparticles for gene delivery. Microporous Mesoporous Mater. 2020, 302, 110200. [Google Scholar] [CrossRef]
- Babii, O.; Wang, Z.; Liu, G.; Martinez, E.C.; van den Hurk, S.D.L.; Chen, L. Low molecular weight chitosan nanoparticles for CpG oligodeoxynucleotides delivery: Impact of molecular weight, degree of deacetylation, and mannosylation on intracellular uptake and cytokine induction. Int. J. Biol. Macromol. 2020, 159, 46–56. [Google Scholar] [CrossRef]
- Rahmani, S.; Hakimi, S.; Esmaeily, A.; Samadi, F.Y.; Mortazavian, E.; Nazari, M.; Mohammadi, Z.; Tehrani, N.R.; Tehrani, M.R. Novel chitosan based nanoparticles as gene delivery systems to cancerous and noncancerous cells. Int. J. Pharm. 2019, 560, 306–314. [Google Scholar] [CrossRef]
- Mobarakeh, V.I.; Modarressi, M.H.; Rahimi, P.; Bolhassani, A.; Arefian, E.; Atyabi, F.; Vahabpour, R. Optimization of chitosan nanoparticles as an anti-HIV siRNA delivery vehicle. Int. J. Biol. Macromol. 2019, 129, 305–315. [Google Scholar] [CrossRef]
- Baghaei, M.; Tekie, F.S.M.; Khoshayand, M.R.; Varshochian, R.; Hajiramezanali, M.; Kachousangi, M.J.; Dinarvand, R.; Atyabiet, F. Optimization of chitosan-based polyelectrolyte nanoparticles for gene delivery, using design of experiment: In vitro and in vivo study. Mater. Sci. Eng. C 2021, 118, 111036. [Google Scholar] [CrossRef]
- Yan, L.; Gao, S.; Shui, S.; Liu, S.; Qu, H.; Liu, C.; Zheng, L. Small interfering RNA-loaded chitosan hydrochloride/carboxymethyl chitosan nanoparticles for ultrasound-triggered release to hamper colorectal cancer growth in vitro. Int. J. Biol. Macromol. 2020, 162, 1303–1310. [Google Scholar] [CrossRef]
- Tang, Y.; Liu, Y.; Xie, Y.; Chen, J.; Dou, Y. Apoptosis of A549 cells by small interfering RNA targeting survivin delivery using poly-β-amino ester/guanidinylated O-carboxymethyl chitosan nanoparticles. Asian J. Pharm. Sci. 2020, 15, 121–128. [Google Scholar] [CrossRef]
- Hajizadeh, F.; Ardebili, S.M.; Moornani, M.B.; Masjedi, A.; Atyabi, F.; Kiani, M.; Namdar, A.; Karpisheh, V.; Izadi, S.; Baradaran, B.; et al. Silencing of HIF-1α/CD73 axis by siRNA-loaded TAT-chitosan-spion nanoparticles robustly blocks cancer cell progression. Eur. J. Pharmacol. 2020, 882, 173235. [Google Scholar] [CrossRef]
- Salimifard, S.; Kiani, F.K.; Eshaghi, F.S.; Izadi, S.; Shahdadnejad, K.; Masjedi, A.; Heydari, M.; Ahmadi, A.; Hojjat-Farsangi, M.; Hassannia, H.; et al. Codelivery of BV6 and anti-IL6 siRNA by hyaluronate-conjugated PEGchitosan-lactate nanoparticles inhibits tumor progression. Life Sci. 2020, 260, 118423. [Google Scholar] [CrossRef] [PubMed]
- Nikkhoo, A.; Rostami, N.; Farhadi, S.; Esmaily, M.; Ardebili, S.M.; Atyabi, F.; Baghaei, M.; Haghnavaz, N.; Yousefi, M.; Aliparasti, M.R.; et al. Codelivery of STAT3 siRNA and BV6 by carboxymethyl dextran trimethyl chitosan nanoparticles suppresses cancer cell progression. Int. J. Pharm. 2020, 581, 119236. [Google Scholar] [CrossRef] [PubMed]
- Masjedi, A.; Ahmadi, A.; Atyabi, F.; Farhadi, S.; Irandoust, M.; Khazaei-Poul, Y.; Chaleshtari, M.G.; Fathabad, M.E.; Baghaei, M.; Haghnavaz, N.; et al. Silencing of IL-6 and STAT3 by siRNA loaded hyaluronate-N,N,N-trimethyl chitosan nanoparticles potently reduces cancer cell progression. Int. J. Biol. Macromol. 2020, 149, 487–500. [Google Scholar] [CrossRef]
- Yan, T.; Zhu, S.; Hui, W.; He, J.; Liu, Z.; Cheng, J. Chitosan based pH-responsive polymeric prodrug vector for enhanced tumor targeted co-delivery of doxorubicin and siRNA. Carbohydr. Polym. 2020, 250, 116781. [Google Scholar] [CrossRef]
- Xue, Y.; Wang, N.; Zeng, Z.; Huang, J.; Xiang, Z.; Guan, J.Q. Neuroprotective effect of chitosan nanoparticle gene delivery system grafted with acteoside (ACT) in Parkinson’s disease models. J. Mater. Sci. Technol. 2020, 43, 197–207. [Google Scholar] [CrossRef]
- Lang, X.; Wang, T.; Sun, M.; Chen, X.; Liu, Y. Advances and applications of chitosan-based nanomaterials as oral delivery carriers. Int. J. Biol. Macromol. 2020, 154, 433–445. [Google Scholar] [CrossRef] [PubMed]
- Alhajj, N.; Zakaria, Z.; Naharudin, I.; Ahsan, F.; Li, W.; Wong, T.W. Critical physicochemical attributes of chitosan nanoparticles admixed lactose-PEG 3000 microparticles in pulmonary inhalation. Asian J. Pharm. Sci. 2020, 15, 374–384. [Google Scholar] [CrossRef]
- Macedo, A.S.; Castro, P.M.; Roque, L.; Thome, N.G.; Reis, C.P.; Pintado, M.E.; Fonte, P. Novel and revisited approaches in nanoparticle systems for buccal drug delivery. J. Control. Release 2020, 320, 125–141. [Google Scholar] [CrossRef]
- Matos, B.N.; Pereira, M.N.; Bravo, M.O.; Cunha-Filho, M.; Saldanha-Araújo, F.; Gratieri, T.; Gelfuso, G. Chitosan nanoparticles loading oxaliplatin as a mucoadhesive topical treatment of oral tumors: Iontophoresis further enhances drug delivery ex vivo. Int. J. Biol. Macromol. 2020, 154, 1265–1275. [Google Scholar] [CrossRef]
- Pornpitchanarong, C.; Rojanarata, T.; Opanasopit, P.; Ngawhirunpat, T.; Patrojanasophon, P. Catechol-modified chitosan/hyaluronic acid nanoparticles as a new avenue for local delivery of doxorubicin to oral cancer cells. Colloids Surf. B Biointerfaces 2020, 196, 111279. [Google Scholar] [CrossRef]
- Sah, A.K.; Dewangan, M.; Suresh, P.K. Potential of chitosan-based carrier for periodontal drug delivery. Colloids Surf. B Biointerfaces 2019, 178, 185–198. [Google Scholar] [CrossRef]
- Nair, S.S. Chitosan-based transdermal drug delivery systems to overcome skin barrier functions. J. Drug Deliv. Ther. 2019, 9, 266–270. [Google Scholar] [CrossRef] [Green Version]
- Park, J.; Ramanathan, R.; Pham, L.; Kim, B.S.; Woodrow, A. Chitosan enhances nanoparticle delivery from the reproductive tract to target draining lymphoid organs. Nanomed. Nanotechnol. Biol. Med. 2017, 13, 2015–2025. [Google Scholar] [CrossRef] [PubMed]




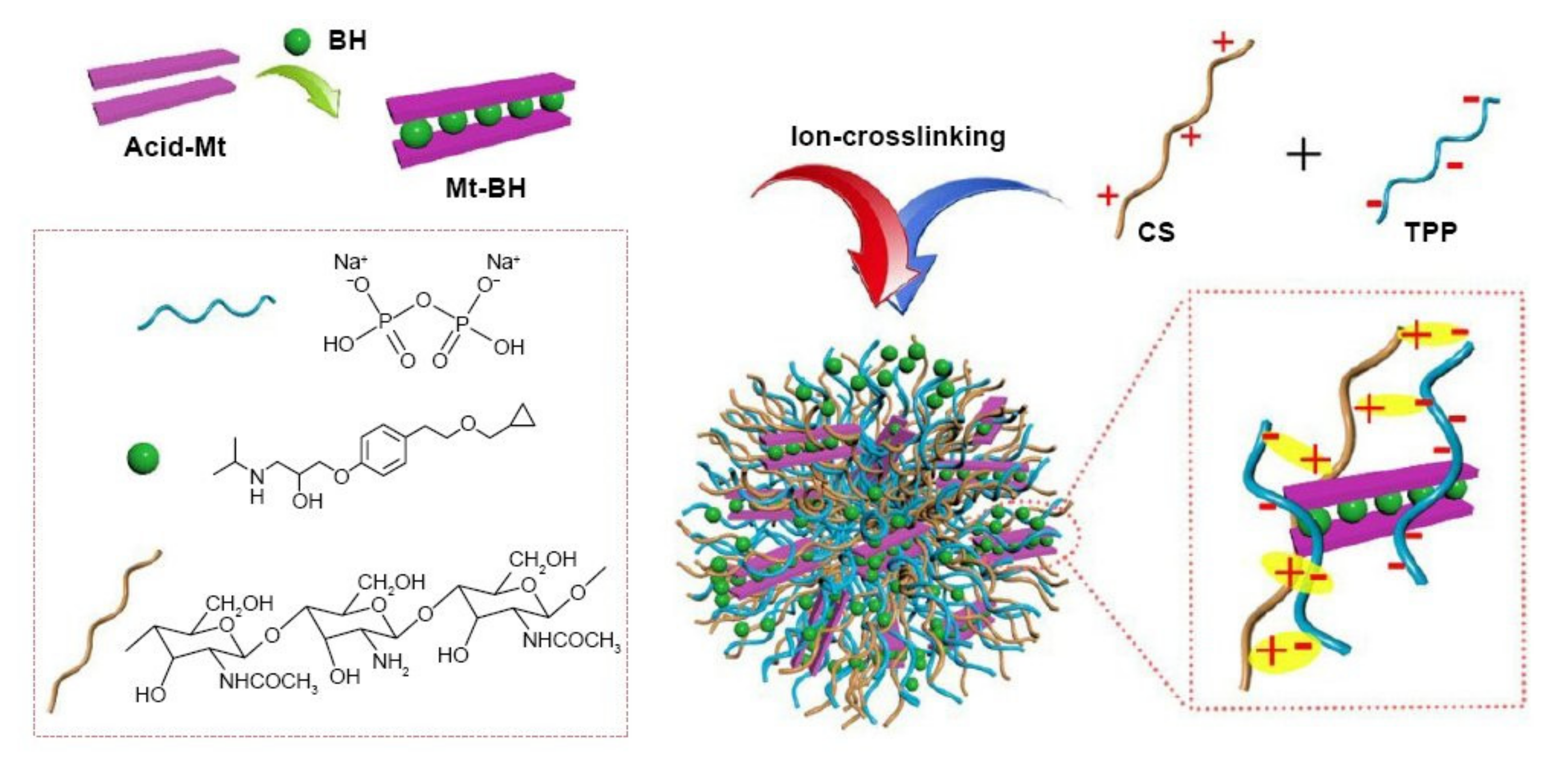

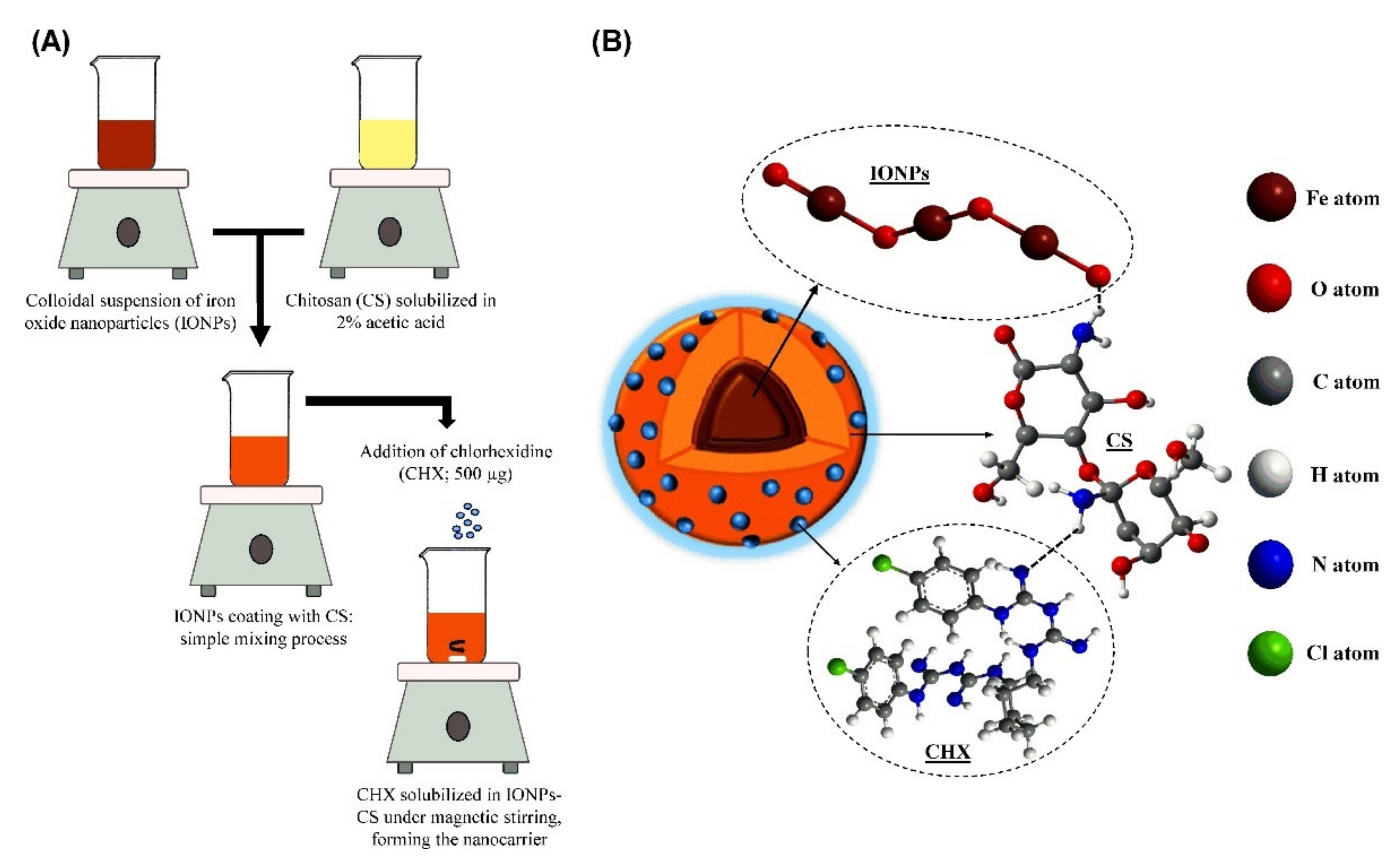

 ) between positively amino groups of CS and negatively charged TPP groups is built via the ionic gelation method. The hydrogen bond interaction (
) between positively amino groups of CS and negatively charged TPP groups is built via the ionic gelation method. The hydrogen bond interaction ( 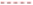 ) occurs between the hydrogen atom and a highly electronegative atom as O or N atom [133]. Reproduced with permission from Elsevier (Copyright©2021).
) occurs between the hydrogen atom and a highly electronegative atom as O or N atom [133]. Reproduced with permission from Elsevier (Copyright©2021).
 ) between positively amino groups of CS and negatively charged TPP groups is built via the ionic gelation method. The hydrogen bond interaction (
) between positively amino groups of CS and negatively charged TPP groups is built via the ionic gelation method. The hydrogen bond interaction ( 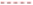 ) occurs between the hydrogen atom and a highly electronegative atom as O or N atom [133]. Reproduced with permission from Elsevier (Copyright©2021).
) occurs between the hydrogen atom and a highly electronegative atom as O or N atom [133]. Reproduced with permission from Elsevier (Copyright©2021).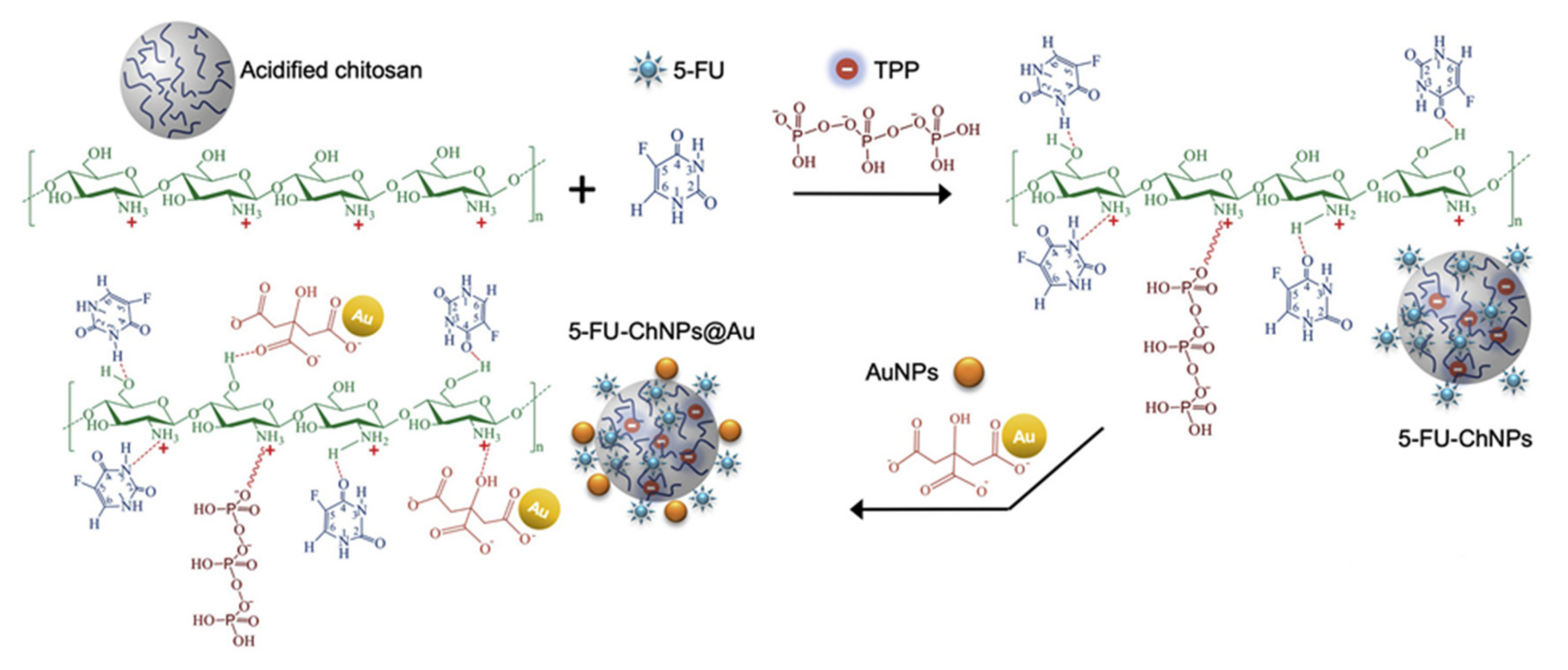





| Chitosan Derivative Groups/Derivatives | Formula |
|---|---|
| Hydrophobic derivatives | |
| Alkylated chitosan | 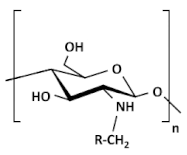 |
| Acylated chitosan | 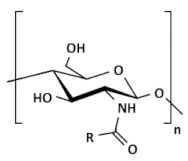 (A) N-acylated chitosan |
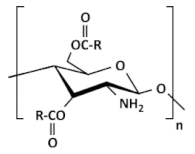 (B) O-acylated chitosan | |
| N-phtaloylated chitosan |  |
| Benzoylated chitosan | 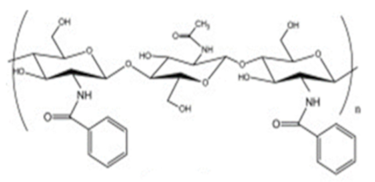 |
| Methacrylated chitosan | 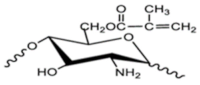 |
| Amphiphilic derivatives | |
| Cholic and deoxycholic acid-modified chitosan | 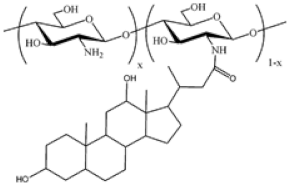 (A) Deoxycholic acid  (B) Cholic acid |
| Ionic derivatives | |
| Quarternary ammonium chitosan derivatives | 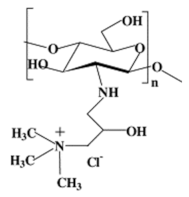 |
| Sulfated chitosan derivatives |  |
| Succinylated chitosan |  |
| Sulfonated chitosan | 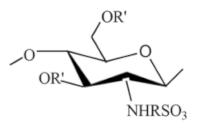 |
| Phosphorylated chitosan | 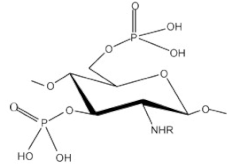 |
| Carboxyalkylated chitosan (carboxymethylchitosan) | 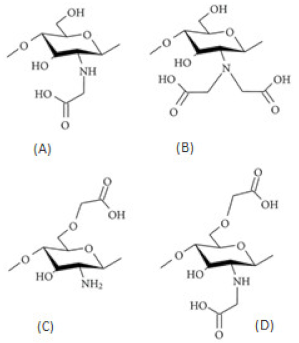 (A) N-CMC, (B) N,N-CMC, (C) O-CMC, and (D) N,O-CMC (showing the modification at the D-glucosamine unit) |
| Chitosan copolymers | |
| PEGylated chitosan |  |
| PEG-methacrylated chitosan |  |
| Derivatives with specific substituents | |
| Sugar bound chitosan derivatives | 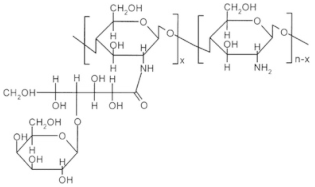 Galactosylated chitosan |
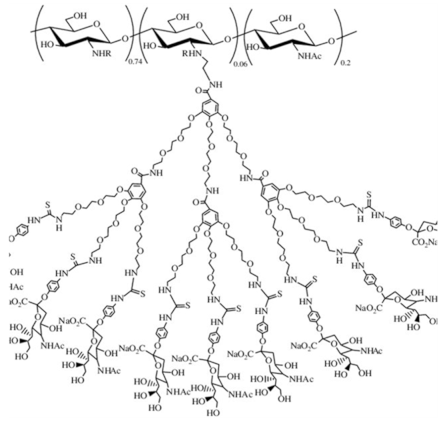 Sialo dendrimer hybrid chitosan | |
| Chitosan derivatives with cyclic structure | 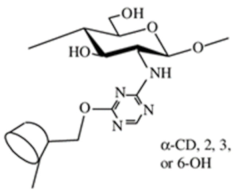 Crown ether-linked chitosan |
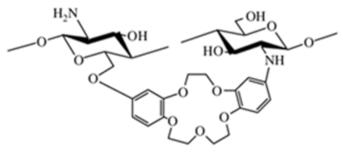 Cyclodextrin-linked chitosan | |
| Chitosan derivatives with thiol groups | 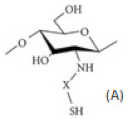 (A) Thiolated chitosan with –SH group |
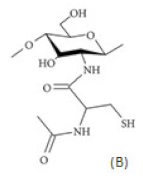 (B) Thiolated chitosan with cysteine: chitosan-N-acetyl-cysteine | |
| Glycol chitosan | 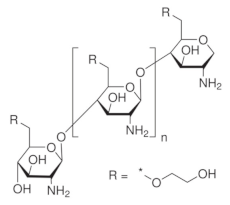 |
| Thiosemicarbazone linked chitosan derivatives | 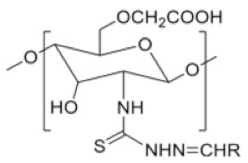 |
| Crosslinked chitosan derivatives | |
| Chitosan-glutaraldehyde crosslinked polymer | 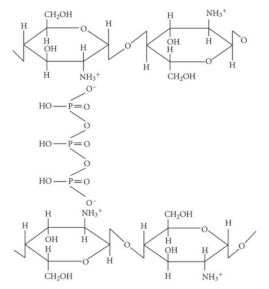 |
| Chitosan-TPP crosslinked polymer | 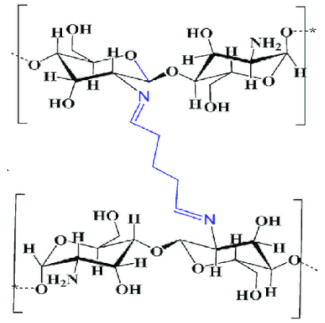 |
| Chitosan-EDTA crosslinked polymer |  |
| Advantages of CS NPs | Disadvantages of CS NPs |
|---|---|
| Less toxicity | Less mechanical resistance |
| Enhanced biocompatibility | Difficult to control pore size |
| Mucoadhesive character | Possible contraction |
| Stability | Difficult electrospinning for pure chitosan |
| Site-specific drug targeting | Preparation by cross-linking can affect intrinsic properties of chitosan |
| The increased therapeutic index of the drug | Low solubility in neutral and alkaline pH |
| Frequent, expensive, and unpleasant dosing is prevented | Method of preparation depends on the drug to be delivered |
| Type of CS NP | Method of CS NP Preparation | Formulated Drug | In Vitro and In Vivo Tests for Biological Activity and Drug Release | Citation |
|---|---|---|---|---|
| Oral drug delivery of antidiabetic drugs | ||||
| TC NPs | Schiff-base linking with PETMP [pentaerythritol tetrakis (3-mercaptopropionate)] | Insulin | In vitro sustained drug release, in vitro cell viability, in vivo biodistribution, and pharmacokinetics | [160] |
| Snail mucin/CS NPs | Self-assembly | Insulin | In vitro drug release, in vivo hypoglycemic activity in diabetic rats, and toxicity | [161] |
| FD/TMC NPs | PEC method | Insulin | In vitro pH-dependent drug release, cytotoxicity, α-glucosidase inhibition assay | [162] |
| CS/Dz13Scr NPs | Complex coacervation | Insulin | In vitro drug release, insulin kinetics, cytotoxicity, mucus permeation, endocytic absorption study | [163] |
| CS NPs | Ionic gelation | Polydatin | In vitro drug release, cytotoxicity, in vivo antidiabetic activity in type 2 diabetic rats | [164] |
| Oral delivery of anticancer drugs | ||||
| FD/CS NPs | PEC method | Methotrexate (MTX) for lung cancer therapy | In vitro mucoadhesive study, in vitro antiproliferative assay and cellular uptake, apoptosis assay | [165] |
| M CS/P NPs | Ionic gelation | Curcumin (CUR) | Cytotoxicity, cellular uptake | [115] |
| chitosan-copaiba oil-poly (isobutyl cyanoacrylate) core-shell nanocapsules | Interfacial polymerization | For colon cancer therapy | In vitro mucoadhesion effect | [166] |
| Cys/PLA/CS NPs | Self-assembly | Paclitaxel (PTX) | In vitro drug release, cytotoxicity, and cellular uptake, in vivo pharmacokinetic study, biodistribution study, antitumor efficacy | [167] |
| TPGS/HPMC/CS NPs | Solvent evaporation method | Paclitaxel (PXT) | In vitro dissolution and swelling, Cytotoxicity, cellular uptake, transport study | [168] |
| Oral delivery of antihypertensive drugs | ||||
| CS NPs | Ionic gelation (TPP) | Carvedilol | In vitro drug release, in vivo pharmacokinetics on rats | [169] |
| Oral delivery of antioxidants | ||||
| CS/Zein NPs | Liquid-liquid dispersion | Resveratrol (RVT) | In vitro drug release, antioxidant activity, in vitro mucoadhesion study | [170] |
| Oral delivery of anti-inflammatory drugs | ||||
| CS/WP-NPs | Self-assembly | polysaccharides from Ophiopogon japonicus (OJPs) IBD treatment | In vitro drug release, Biocompatibility, cytotoxicity, antioxidant activity, gene expression, ex vivo mucoadhesion study | [171] |
| CS NPs | Spray-drying method | Dexketoprofen trometamol (DT) | In vitro prolonged drug release, release kinetics, in vivo anti-inflammatory activity, HET-CAM assay | [93] |
| AvrA NPs-ALG/CS MPs | Flow focusing microfluidic method | Salmonella effector enzyme (AvrA) | In vitro drug release, in vivo reduction of inflammation in murine dextran sulfate sodium (DSS) colitis model | [172] |
| Oral vaccines | ||||
| β-CD/CS NPs | Precipitation/coacervation method | Ovalbumin (OVA) | In vitro drug release, in vivo immune response in Balb/c mice | [173] |
| CS chloride NPs | Ionic gelation (TPP) | Ovalbumin (OVA) | In vitro cell toxicity, permeability study, transepithelial electrical resistance studies, in vivo studies | [174] |
| ALG/CS NPs anchored with lipopolysaccharide (LPS) as an adjuvant | Ionic gelation (TPP) | HBsAg antigen | In vitro drug release and mucoadhesion study, stability, cytotoxicity, in vivo immunization studies | [175] |
| ALG/CS coating LDHs | Co-precipitation-hydrothermal method | BSA | In vitro drug release, cellular uptake, stability in biological fluids | [176] |
| Oral delivery of other drugs | ||||
| Cs PLNs | Self-assembly | Enoxaparin | Mucoadhesive properties, stability, in vivo anticoagulant activity in rats | [177] |
| CS NPS | Double emulsification solvent evaporation method | Salmon calcitonin (sCT) and puerarin (PR) | In vitro drug release, stability, cellular uptake, in vivo pharmacokinetic study | [79] |
| SA/CS and NaCAS/CS NPs | Ionic gelation (oxidized dextran) | Astaxanthin (ASTX) (hepatic fibrosis treatment) | ABTS radical scavenging assay, cytotoxicity, anti-fibrogenic activity | [114] |
| Soy lecithin/CS hybrid NPs | Self-assembly | Raloxifene hydrochloride (RLX) | In vitro drug dissolution and release, MTT assay, intestinal drug uptake, in vivo pharmacokinetic studies, biodistribution, ex-vivo mucoadhesion studies | [178] |
| Ocular drug delivery | ||||
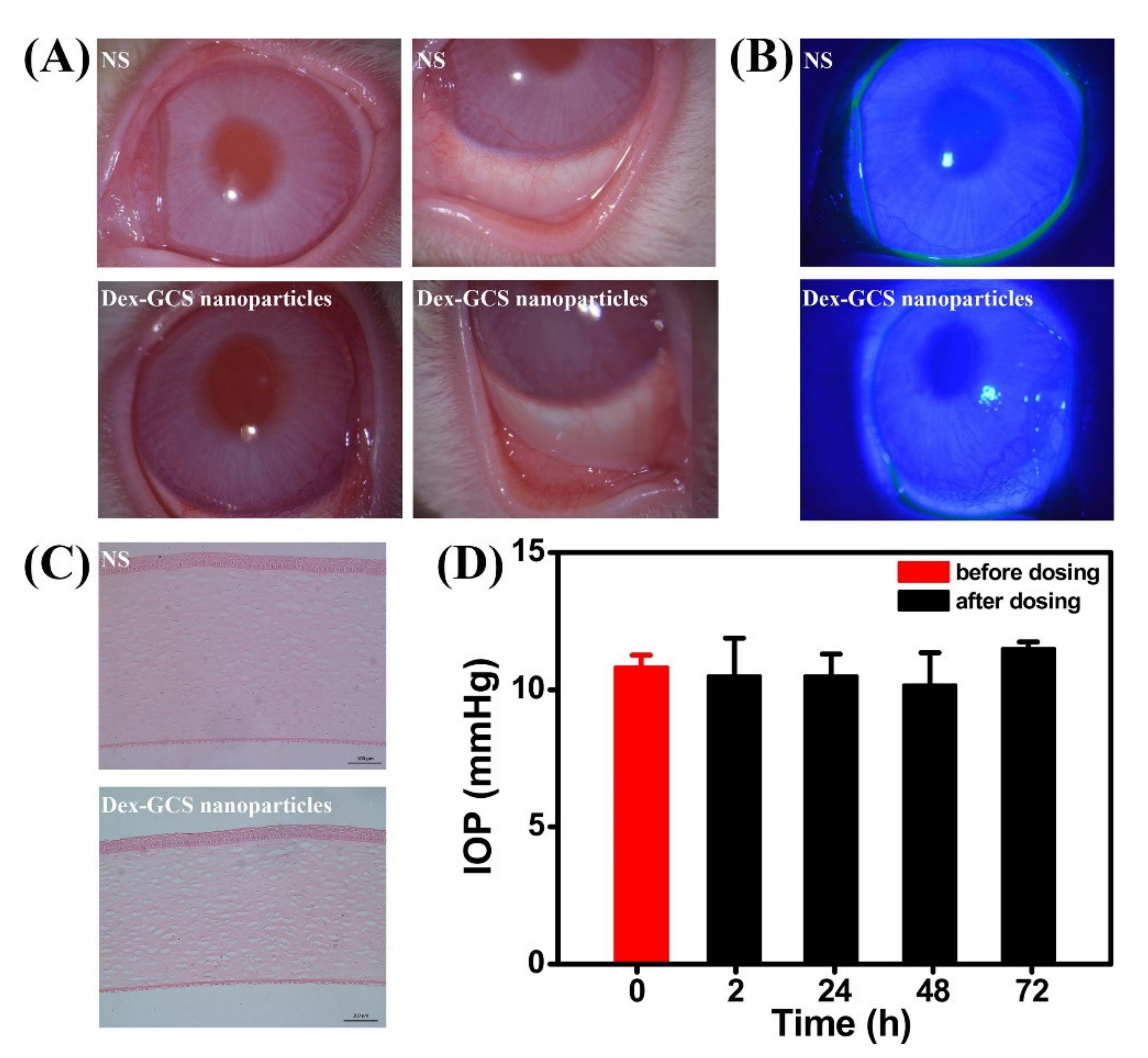
| GCS NPs | Self-assembly | Dexamethasone (DEX) | In vitro drug release, mucoadhesive, cytotoxicity, and anti-inflammatory efficacy, in vivo study: eye irritation test and distribution test | [179] |
| CMC/GSH/GlySar/LDHs | Coprecipitation–hydrothermal method | Dexamethasone disodium phosphate (DEXP) DD to the posterior segment of the eye | In vitro toxicity study on human conjunctival epithelial cells, cellular uptake, the in vivo precorneal retention study, the tissue distribution evaluation of rabbit’s eyes | [148] |
| CS/LIP | Thin-film hydration method | Triamcinolone acetonide (TA) Treatment of posterior eye segment diseases | In vitro drug release, in vivo drug release | [180] |
| TCM/LNPs | Emulsion solvent evaporation method | Baicalein (BAI) | In vitro sustained drug release, in vivo ocular irritation study, pre-corneal retention evaluation, pharmacokinetic study | [33] |
| CS NPs | Ionic gelation (TPP) | Levofloxacin (LFX) Therapy of ocular infections | The antimicrobial study, in vitro ocular tolerance, in vivo pharmacoscintigraphic study | [181] |
| CS/poly(ethylene glycol) methacrylate MNPs | Double crosslinking (ionic and covalent) in reverse emulsion | Bevacizumab Treatment of posterior segment of the eye | In vitro drug release kinetics, hemocompatibility, in vivo study of antiangiogenic effect (eye) | [48] |
| CS/PCL NPs | Single-step emulsification method | Dorzolamide (DRZ) Glaucoma treatment | In vitro drug release, in vivo corneal flux experiment, corneal hydration study, ex vivo bioadhesion study, ocular tolerance study, Hen egg test-chorioallantoic membrane (HET-CAM) test | [82] |
| CS/gelatin gel with CUR-NPs | - | Latanoprost (LP) and curcumin (CUR) Glaucoma treatment | In vitro drug release, in vitro biocompatibility, in vivo incompatibility in rabbits | [182] |
| Nasal drug delivery (topical) | ||||
| CS NPs | Ionic gelation | Cromolyn Therapy of allergic rhinitis | In vitro drug release, permeation, and penetration, mucoadhesion assay | [183] |
| DCHBC NPs | Dialysis method | Cetirizine (CTZ) Therapy of allergic rhinitis | In vitro stimuli-responsive drug release, cytotoxicity, hemolysis test, protein adsorption | [184] |
| CS or CS maleimide NPs | Ionic gelation (TPP) | Japanese encephalitis-chimeric virus vaccineNasal vaccine | Mucoadhesive properties, antigen uptake study, in vivo study of immunization of mice | [185] |
| Nose to brain delivery | ||||
| CS/HSA NPs | Desolvation method | Tacrine and R-flurbiprofen | mucoadhesion properties, in vitro drug release, permeation, uptake, ex vivo diffusion experiments on rabbit nasal mucosa | [186] |
| PLGA NPs and PLGA/CS NPs | Nanoprecipitation | Ropinirole hydrochloride Antiparkinson therapy | In vitro drug release, mucoadhesion, hemolysis assay, stability study, studies on peripheral blood mononuclear cells and RAW 264.7 macrophage cell line—cytotoxicity, cellular uptake ex vivo permeability studies | [187] |
| N,O-CMC NPs | Emulsion solvent evaporation method | Dopamine (DOPA) orTyrosine (Tyr) | In vitro drug release, mucoadhesive properties, cytotoxicity, cellular uptake | [188] |
| CS NPs | - | Therapy of Huntington disease | Gene silencing studies | [189] |
| CS NPs | Ionic gelation (TPP) | Zolmitriptan (ZOL) Therapy of migraine | In vivo stability, in vivo pharmacokinetic study on Wistar rats | [190] |
| CS NPs | Ionic gelation (TPP) | Rotigotine (R) Treatment of Parkinson’s disease | In vitro cellular uptake, cytotoxicity assay, neuroprotective activity, antioxidant activity, in vivo pharmacodynamic and pharmacokinetic study | [191] |
| Pulmonary (inhalation) drug delivery | ||||
| CS NPs | Emulsion method | Nicotine hydrogen tartrate (NHT) Treatment of nicotine addiction | In vitro evaluation of nose-only inhalation device, assessment of bioactivity of NHT-CS NPs via locomotor test by injection, histopathological analysis of lung tissues | [192] |
| CS/PLGA NPs followed by coating with chitosan | Solvent evaporation (double-emulsion) method | Catechin hydrate (CTH) | In vitro drug release, ex-vivo permeation study on the nasal mucosa, cytotoxicity, in vivo comparative pulmokinetic study | [193] |
| CS/SLNs | Hot ultrasonication | Rifampicin (RIF) Tuberculosis treatment | In vitro drug release, mucoadhesive properties, in vitro cell viability and permeability studies, stability studies | [194] |
| Mn-TMC NPs | Ionic gelation (TPP) | Etofylline (ETO) Asthma treatment | Sustained drug release, biodegradation studies, stability, safety, and aerodynamic behavior | [195] |
| HA/CS NPs | Self-assembly | Ferulic acid (FA) Asthma treatment | In vivo inhalation toxicity assessment | [196] |
| Buccal delivery | ||||
| CS NPs | Ionic gelation (TPP) | Oxiplatin Anticancer therapy | ex vivo its penetration in porcine mucosa under both passive and iontophoretic topical treatments | [102] |
| Cat/CS/HA NPs | Ionic gelation | Doxorubicin (DOX) Oral cancer treatment | Ex vivo mucoadhesive study, in vitro drug release, cytotoxicity, cellular uptake, cancer cells death | [103] |
| TTEC NPs | PEC method | Insulin | In vitro drug release, ex vivo permeation study on rabbit mucosa, MTT assay | [197] |
| CS/PEO NFs | Electrospinning | Sublingval delivery | Ex vivo adhesion on porcine mucosa, swelling, compatibility | [198] |
| Periodontal delivery | ||||
| CS NPs | Ionic gelation | Minocycline, tetracycline Periodontal disease | Human gingival fibroblasts behavior, Cell viability and culture metabolic activity, cellular uptake, inflammatory gene expression | [199] |
| Core-sheath NFs: shell layer: CS core: PVA containing drug | Coaxial electrospinning and ionic gelation (genipin) | Tetracycline hydrochloride (TH) Periodontitis treatment | In vitro sustained drug release, in vitro antimicrobial activity, cytotoxicity | [200] |
| CS/IO NPs | - | Chlorhexidine (CHX) Antimicrobial and antibiofilm effect against oral disease | Determination of MIC, cytotoxicity by MTT assay | [126] |
| Dermal drug delivery | ||||
| CS NPs | Ionic gelation (TPP) | Nicotinamide | Clinical test, skin bioadhesion, deposition of drug in different skin layers | [201] |
| Poly-(ε-caprolactone)-lipid core NCs nad CS/poly-(ε-caprolactone)-lipid-core NCs | Interfacial deposition technique | Dutasteride Hair follicle targeting after massage procedure | In vitro drug release, stability, in vitro skin permeation | [202] |
| Transdermal drug delivery | ||||
| CS Hydroxypropyltrimonium chloride/PLGA NPs | Antisolvent diffusion method | Hen egg-white lysozyme (HEL) allergen immunotherapy to hair follicles using iontophoresis | In vitro cellular uptake, ex vivo skin accumulation study, in vivo transcutaneous immunization experiment | [203] |
| CS NFs | Electrospinning | Colchicine Anti-skin cancer therapy | Ex vivo skin permeation, deposition analysis, release kinetic and anti-melanoma efficiency against A-375 cell line | [204] |
| CS NPs | Nanospray-drying technique | 5-fluorouracil (FU) | Synergistic microwave delivery of anti-cancer | [205] |
| Wound healing | ||||
| CS/PEO NFs | Electrospinning | Teicoplanin Local antibiotic wound healing | In vitro drug release, antibacterial test, cytotoxicity, in vivo study on rat full-thickness wound model | [67] |
| PCL/CS NFs | Electrospinning | Curcumin (CUR) Wound dressing | antibacterial, antioxidant properties, cell viability, and in vivo wound healing efficiency and histological assay | [206] |
| hydrogel membranes based on HA/PU/PVA loaded with cefepime-CS NPs | Ionic gelation (TPP) | Cefepime | In vitro drug release, bacterial inhibition | [207] |
| CS NPs loaded hydrogel | Ionic gelation (TPP) | Pterocarpus marsupium heartwood extract (PM) Therapy of diabetic wounds | In vitro drug release efficiency, in-vitro anti-microbial activity, in vivo wound healing action in streptozotocin administered diabetic rat models | [208] |
| Vaginal drug delivery | ||||
| CS NPs | Ionic gelation (TPP) | Miconazole nitrate Therapy of vulvovaginal candidiasis | In vivo evaluation on vulvovaginal murine model | [209] |
| CS NPs encapsulated in hydrophilic freeze-dried cylinders | Ionic gelation (TPP) | Insulin Peptide-based vaccines or delivery of microbicides | In vitro drug release, ex vivo insulin penetration across porcine vaginal mucosa | [210] |
| CS and spicules NPs | Ionic gelation (TPP) | Calophycin A (Cal A)—seaweed-derived metabolite Therapy of vaginal candidiasis | In vitro anti-candidal activity, in vivo on mice | [211] |
| Vaccine delivery | ||||
| CS and ALG coated CS NPs | Precipitation/coacervation method | Hepatitis A vaccine (HAV) | Assay of HAV-specific antibodies and their isotypes, lymphoproliferation assay, the effect of HAV formulation on the splenocytes proliferation in vaccinated mice | [212] |
| CS NPs | Ionic gelation (TPP) | Aah II toxin isolated from Androctonus australis hector (scorpion) venom | In vitro toxin-release study, in vivo immunization trial | [213] |
| Gene delivery | ||||
| MPC derived from carbonized CTS echitosan capsulated ZIF-8 | Carbonization | Luciferase-expressing plasmid (pGL3), and splice correction oligonucleotides (SCO) | Cell biocompatibility, transfection efficiency, mechanism of uptake | [214] |
| LMW mannosylated CS NPs | Ionic gelation | CpG oligodeoxynucleotides | Cytotoxicity, cellular uptake, immunostimulatory effect-cytokine release in RAW264.7 cells, efficient vector for intracellular CpG ODN delivery | [215] |
| TMC Cys, MABCMC, and CysMABC NPs | Ionic gelation | Plasmid DNA pEGFP-N1 | In vitro DNA transfection efficiency, cytotoxicity | [216] |
| CS, PEI, and CMD NPs | Self-assembly | Anti-HIV siRNA HIV therapy | In vitro cytotoxicity assay and siRNA delivery in two mammalian cell lines, macrophage RAW264.7, and HEK293 | [217] |
| TMC/DS or ALG NPs | PEC method | hSET1 antisense—silencing oligonucleotide Cancer therapy | In vitro cell viability, cellular uptake, in vivo study on mice | [218] |
| CMC NPs labelled with FITC NPs (FITCCS/CMC) | Self-assembly | Anti-β-catenin siRNA Ultrasound-triggered targeted therapy of colon cancer | In vitro drug release, cytotoxic assay, cellular uptake, therapeutic evaluation | [219] |
| Guanidinylated O-CMC NPs (GOCMCS) | Self-assembly | SiRNA delivery | In vitro cell transfection studies with A549 cells, cellular uptake | [220] |
| SPION NPs encapsulated with TAT peptide/TC and TMC | Electrostatic interaction | siRNA Targeted anti-cancer therapy | Cytotoxicity, cellular internalization, in vivo pharmacokinetic and biodistribution, colony formation assay, wound healing assay, Chick chorioallantoic membrane (CAM) assay | [221] |
| HA/PCL NPs | Ionic gelation (TPP) | IL6-specific siRNA and BV6 treatment of breast and colon cancer | In vitro drug release, cellular uptake, MTT assay, apoptosis assay, Chick chorioallantoic membrane assay, wound healing assay, a clonogenic assay of tumor cells in vitro, transwell migration assay, in vivo antitumor efficacy on mice | [222] |
| CMD/TMC NPs | Nanoprecipitation | Codelivery of NIK/STAT3-specific siRNA and BV6 Cancer therapy | Stability of NPs, in vitro drug release, cellular uptake, transfection of cells, MTT assay, Chick chorioallantoic membrane (CAM) assay, wound healing assay, colony formation assay | [223] |
| HA/TMC NPs | PEC method | IL-6- and STAT3-specific siRNAs Cancer therapy | In vitro drug release, stability in serum, MTT cytotoxicity assay, cellular uptake, transfection efficiency, Colony formation assay Wound healing assay | [224] |
| CS NPs | - | Doxorubicin (DOX) and Bcl-2 siRNA co-delivery of therapeutics and si-RNA Cancer therapy | In vitro drug release, in vivo tumor suppression test | [225] |
| Polyethyleneglycol-poly lactic acid CS (PP CS NPs) | - | Nerve growth factor (NGF), acteoside (ACT), and plasmid DNA (pDNA) Treatment of Parkinson’s disease | Plasmid DNA (pDNA), nerve growth factor (NGF), acteoside (Act) | [226] |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Mikušová, V.; Mikuš, P. Advances in Chitosan-Based Nanoparticles for Drug Delivery. Int. J. Mol. Sci. 2021, 22, 9652. https://doi.org/10.3390/ijms22179652
Mikušová V, Mikuš P. Advances in Chitosan-Based Nanoparticles for Drug Delivery. International Journal of Molecular Sciences. 2021; 22(17):9652. https://doi.org/10.3390/ijms22179652
Chicago/Turabian StyleMikušová, Veronika, and Peter Mikuš. 2021. "Advances in Chitosan-Based Nanoparticles for Drug Delivery" International Journal of Molecular Sciences 22, no. 17: 9652. https://doi.org/10.3390/ijms22179652
APA StyleMikušová, V., & Mikuš, P. (2021). Advances in Chitosan-Based Nanoparticles for Drug Delivery. International Journal of Molecular Sciences, 22(17), 9652. https://doi.org/10.3390/ijms22179652







