Prognostic Impact of Membranous/Nuclear Epidermal Growth Factor Receptor Localization in Clear Cell Renal Cell Carcinoma
Abstract
:1. Introduction
2. Results
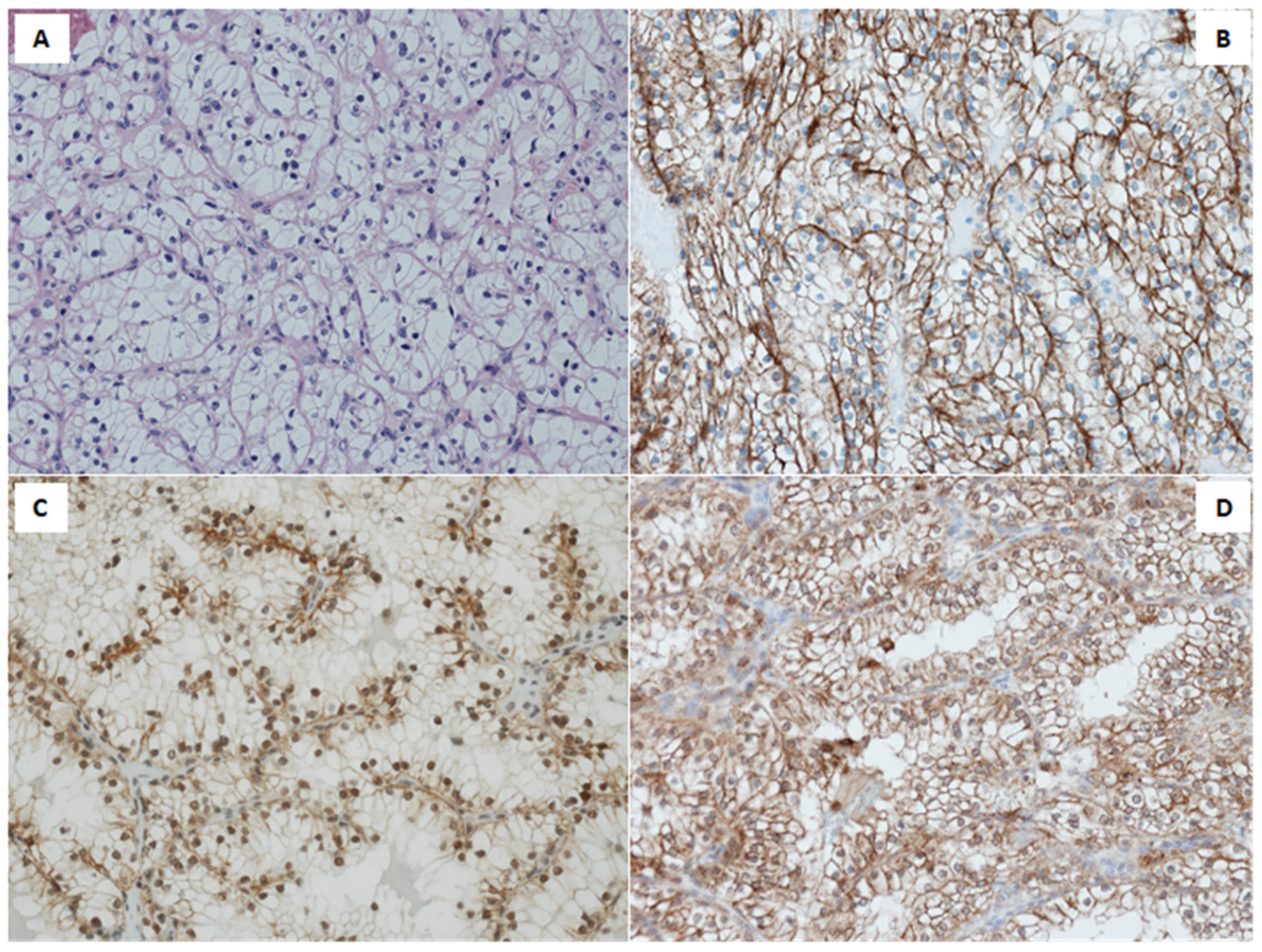
2.1. Immunohistochemical Analysis
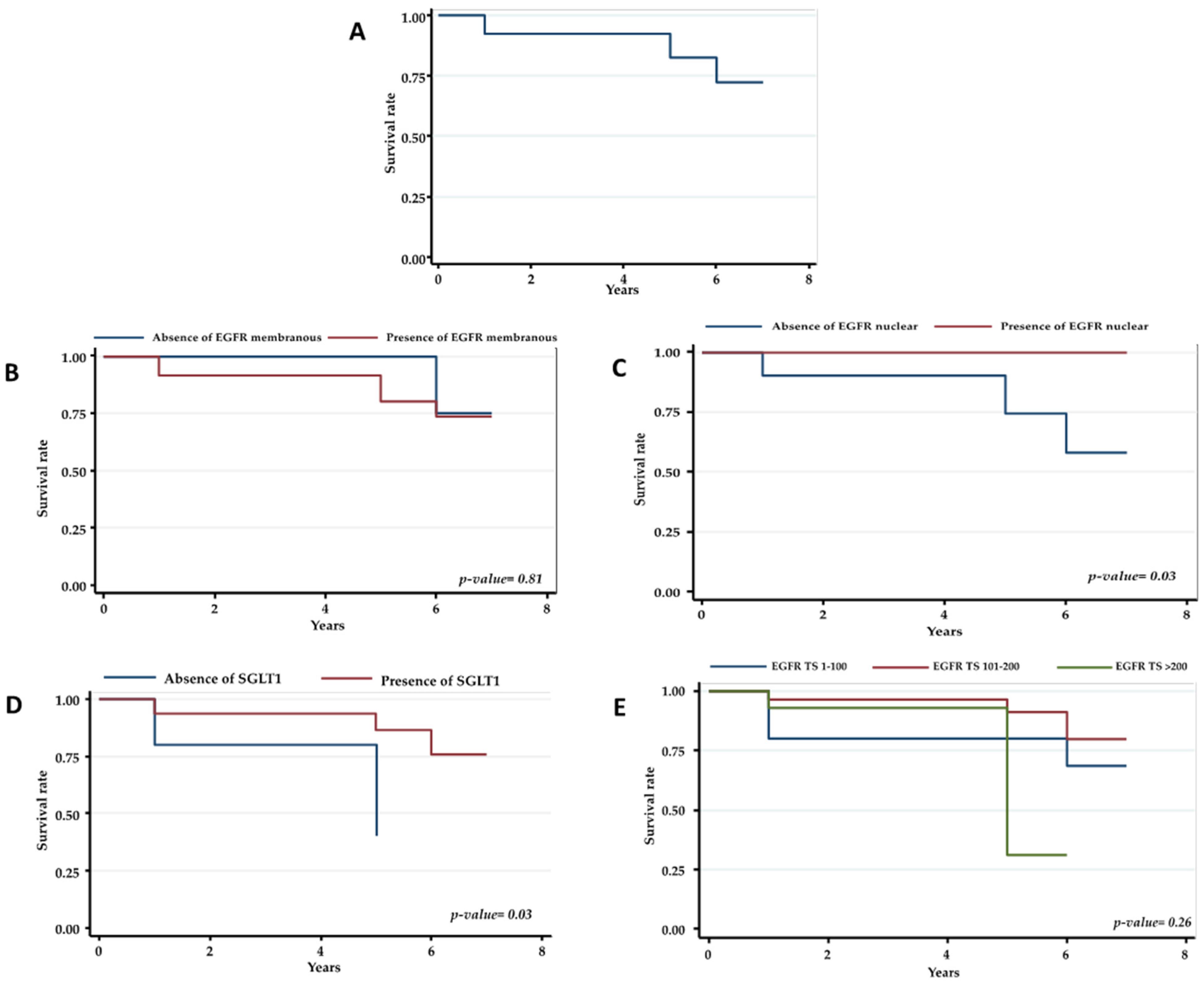
2.2. Statistical Analysis
3. Discussion
4. Materials and Methods
4.1. Recruitment of CCRCC Patients
4.2. Immunohistochemistry
4.3. Statistical Analysis
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| CCRCC | Clear cell renal cell carcinoma |
| RCC | Renal cell carcinoma |
| EGFRvIII | EGFR-variant III |
| NED | No evidence of disease |
| AWD | Alive with disease |
| DOD | Died of disease |
| TS | Total score |
| IHC | Immunohistochemistry |
| FFPE | Formalin-fixed, paraffin embedded |
| pT | Pathologic stage |
| SSIGN | Stage, size, grade, and necrosis |
| TKIs | Tyrosine kinase inhibitors |
| SD | Standard deviation |
| pTNM | Pathological tumor-node-metastasis |
| IQR | Interquartile range |
| OR | Odds ratio |
| CI | Confidence interval |
| PPP | Pentose phosphate pathway |
References
- Ljungberg, B.; Campbell, S.C.; Cho, H.Y.; Jacqmin, D.; Lee, J.E.; Weikert, S.; Kiemeney, L.A. The epidemiology of renal cell carcinoma. Eur. Urol. 2011, 60, 615–621. [Google Scholar] [CrossRef] [PubMed]
- Zerdes, I.; Tolia, M.; Tsoukalas, N.; Mitsis, M.; Kardamakis, D.; Pistevou-Gombaki, K.; Tsekeris, P.; Kyrgias, G. Systemic therapy of metastatic renal cell carcinoma: Review of the current literature. Urol. J. 2019, 86, 3–8. [Google Scholar] [CrossRef] [PubMed]
- de Velasco, G.; Bex, A.; Albiges, L.; Powles, T.; Rini, B.I.; Motzer, R.J.; Heng, D.Y.C.; Escudier, B. Sequencing and Combination of Systemic Therapy in Metastatic Renal Cell Carcinoma. Eur. Urol. Oncol. 2019, 2, 505–514. [Google Scholar] [CrossRef]
- Rizzo, A.; Mollica, V.; Santoni, M.; Ricci, A.D.; Rosellini, M.; Marchetti, A.; Montironi, R.; Ardizzoni, A.; Massari, F. Impact of Clinicopathological Features on Survival in Patients Treated with First-line Immune Checkpoint Inhibitors Plus Tyrosine Kinase Inhibitors for Renal Cell Carcinoma: A Meta-analysis of Randomized Clinical Trials. Eur. Urol. Focus 2021, 10, S2405-4569. [Google Scholar] [CrossRef]
- Stumm, G.; Eberwein, S.; Rostock-Wolf, S.; Stein, H.; Pomer, S.; Schlegel, J.; Waldherr, R. Concomitant overexpression of the EGFR and erbB-2 genes in renal cell carcinoma (RCC) is correlated with dedifferentiation and metastasis. Int. J. Cancer 1996, 69, 17–22. [Google Scholar] [CrossRef]
- Moch, H.; Sauter, G.; Buchholz, N.; Gasser, T.C.; Bubendorf, L.; Waldman, F.M.; Mihatsch, M.J. Epidermal growth factor receptor expression is associated with rapid tumor cell proliferation in renal cell carcinoma. Hum. Pathol. 1997, 28, 1255–1259. [Google Scholar] [CrossRef]
- Amare, P.S.; Varghese, C.; Bharde, S.H.; Narasimhamoorthy, N.K.; Desai, S.; Advani, S.H.; Havaldar, R.; Kulkarni, J.N. Proliferating cell nuclear antigen and epidermal growth factor receptor (EGFr) status in renal cell carcinoma patients with polysomy of chromosome 7. Cancer Genet. Cytogenet. 2001, 125, 139–146. [Google Scholar] [CrossRef]
- Moch, H.; Sauter, G.; Casser, T.C.; Bubendorf, L.; Richter, J.; Presti, J.C.; Waldman, F.M.; Mihatsch, M.J. EGF-r gene copy number changes in renal cell carcinoma detected by fluorescence in situ hybridization. J. Pathol. 1998, 184, 424–429. [Google Scholar] [CrossRef]
- Merseburger, A.S.; Hennenlotter, J.; Simon, P.; Kruck, S.; Koch, E.; Horstmann, M.; Kuehs, U.; Küfer, R.; Stenzl, A.; Kuczyk, M.A. Membranous expression and prognostic implications of epidermal growth factor receptor protein in human renal cell cancer. Anticancer Res. 2005, 25, 1901–1907. [Google Scholar]
- Cohen, D.; Lane, B.; Jin, T.; Magi-Galluzzi, C.; Finke, J.; Rini, B.I.; Bukowski, R.M.; Zhou, M. The prognostic significance of epidermal growth factor receptor expression in clear-cell renal cell carcinoma: A call for standardized methods for immunohistochemical evaluation. Clin. Genitourin. Cancer 2007, 5, 264–270. [Google Scholar] [CrossRef]
- Cossu-Rocca, P.; Muroni, M.R.; Sanges, F.; Sotgiu, G.; Asunis, A.; Tanca, L.; Onnis, D.; Pira, G.; Manca, A.; Dore, S.; et al. EGFR kinase-dependent and kinase-independent roles in clear cell renal cell carcinoma. Am. J. Cancer Res. 2016, 6, 71–83. [Google Scholar] [PubMed]
- Ficarra, V.; Martignoni, G.; Lohse, C.; Novara, G.; Pea, M.; Cavalleri, S.; Artibani, W. External validation of the mayo clinic stage, size, grade and necrosis (SSIGN) score to predict cancer specific survival using a European series of conventional renal cell carcinoma. J. Urol. 2006, 175, 1235–1239. [Google Scholar] [CrossRef]
- Minner, S.; Gärtner, M.; Freudenthaler, F.; Bauer, M.; Kluth, M.; Salomon, G.; Heinzer, H.; Graefen, M.; Bokemeyer, C.; Simon, R.; et al. Marked heterogeneity of ERG expression in large primary prostate cancers. Mod. Pathol. 2013, 26, 106–116. [Google Scholar] [CrossRef]
- Coppin, C.; Kollmannsberger, C.; Le, L.; Porzsolt, F.; Wilt, T.J. Targeted therapy for advanced renal cell cancer (RCC): A Cochrane systematic review of published randomised trials. BJU Int. 2011, 108, 1556–1563. [Google Scholar] [CrossRef] [PubMed]
- Stadler, W.M. Targeted agents for the treatment of advanced renal cell carcinoma. Cancer 2005, 104, 2323–2333. [Google Scholar] [CrossRef] [PubMed]
- Motzer, R.J.; Amato, R.; Todd, M.; Hwu, W.J.P.; Cohen, R.; Baselga, J.; Muss, H.; Cooper, M.; Yu, R.; Ginsberg, M.S.; et al. Phase II trial of antiepidermal growth factor receptor antibody C225 in patients with advanced renal cell carcinoma. Investig. New Drugs 2003, 21, 99–101. [Google Scholar] [CrossRef] [PubMed]
- Baselga, J.; Arteaga, C.L. Critical update and emerging trends in epidermal growth factor receptor targeting in cancer. J. Clin. Oncol. 2005, 23, 2445–2459. [Google Scholar] [CrossRef] [PubMed]
- Lynch, T.J.; Bell, D.W.; Sordella, R.; Gurubhagavatula, S.; Okimoto, R.A.; Brannigan, B.W.; Harris, P.L.; Haserlat, S.M.; Supko, J.G.; Haluska, F.G.; et al. Activating Mutations in the Epidermal Growth Factor Receptor Underlying Responsiveness of Non–Small-Cell Lung Cancer to Gefitinib. N. Engl. J. Med. 2004, 350, 2129–2139. [Google Scholar] [CrossRef] [PubMed]
- Brand, T.M.; Iida, M.; Luthar, N.; Starr, M.M.; Huppert, E.J.; Wheeler, D.L. Nuclear EGFR as a molecular target in cancer. Radiother. Oncol. 2013, 108, 370–377. [Google Scholar] [CrossRef] [Green Version]
- Hsu, S.C.; Miller, S.A.; Wang, Y.; Hung, M.C. Nuclear EGFR is required for cisplatin resistance and DNA repair. Am. J. Transl. Res. 2009, 1, 249–258. [Google Scholar]
- Lo, H.W.; Hung, M.C. Nuclear EGFR signalling network in cancers: Linking EGFR pathway to cell cycle progression, nitric oxide pathway and patient survival. Br. J. Cancer 2006, 94, 184–188. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lo, H.W.; Xia, W.; Wei, Y.; Ali-Seyed, M.; Huang, S.F.; Hung, M.C. Novel prognostic value of nuclear epidermal growth factor receptor in breast cancer. Cancer Res. 2005, 65, 338–348. [Google Scholar] [PubMed]
- Wang, S.C.; Hung, M.C. Cytoplasmic/nuclear shuttling and tumor progression. Ann. N. Y. Acad. Sci. 2005, 1059, 11–15. [Google Scholar] [CrossRef] [PubMed]
- Hadžisejdi, I.; Mustać, E.; Jonjić, N.; Petković, M.; Grahovac, B. Nuclear EGFR in ductal invasive breast cancer: Correlation with cyclin-D1 and prognosis. Mod. Pathol. 2010, 23, 392–403. [Google Scholar] [CrossRef] [Green Version]
- Psyrri, A.; Yu, Z.; Weinberger, P.M.; Sasaki, C.; Haffty, B.; Camp, R.; Rimm, D.; Burtness, B.A. Quantitative determination of nuclear and cytoplasmic epidermal growth factor receptor expression in oropharyngeal squamous cell cancer by using automated quantitative analysis. Clin. Cancer Res. 2005, 11, 5856–5862. [Google Scholar] [CrossRef] [Green Version]
- Xia, W.; Wei, Y.; Du, Y.; Liu, J.; Chang, B.; Yu, N.L.; Huo, L.F.; Miller, S.; Hung, M.C. Nuclear expression of epidermal growth factor receptor is a novel prognostic value in patients with ovarian cancer. Mol. Carcinog. 2009, 48, 610–617. [Google Scholar] [CrossRef] [Green Version]
- Lipponen, P.; Eskelinen, M. Expression of epidermal growth factor receptor in bladder cancer as related to established prognostic factors, oncoprotein (c-erbB-2, p53) expression and long-term prognosis. Br. J. Cancer 1994, 69, 1120–1125. [Google Scholar] [CrossRef] [Green Version]
- Tervahauta, A.; Syrjänen, S.; Syrjänen, K. Epidermal growth factor receptor, c-erb b-2 proto-oncogene and estrogen receptor expression in human papillomavirus lesions of the uterine cervix. Int. J. Gynecol. Pathol. 1994, 13, 234–240. [Google Scholar] [CrossRef] [PubMed]
- Ahel, J.; Dordevic, G.; Markic, D.; Mozetic, V.; Spanjol, J.; Grahovac, B.; Stifter, S. Nuclear EGFR characterize still controlled proliferation retained in better differentiated clear cell RCC. Med. Hypotheses 2015, 85, 183–185. [Google Scholar] [CrossRef]
- Kankaya, D.; Kiremitci, S.; Tulunay, O.; Baltaci, S. Prognostic impact of epidermal growth factor receptor on clear cell renal cell carcinoma: Does it change with different expression patterns? Indian J. Pathol. Microbiol. 2016, 59, 35–40. [Google Scholar] [CrossRef]
- Langner, C.; Ratschek, M.; Rehak, P.; Schips, L.; Zigeuner, R. Are heterogenous results of EGFR immunoreactivity in renal cell carcinoma related to non-standardised criteria for staining evaluation? J. Clin. Pathol. 2004, 57, 773–775. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Minner, S.; Rump, D.; Tennstedt, P.; Simon, R.; Burandt, E.; Terracciano, L.; Moch, H.; Wilczak, W.; Bokemeyer, C.; Fisch, M.; et al. Epidermal growth factor receptor protein expression and genomic alterations in renal cell carcinoma. Cancer 2012, 118, 1268–1275. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Dordević, G.; Matušan Ilijaš, K.; Hadžisejdić, I.; Maričić, A.; Grahovac, B.; Jonjić, N. EGFR protein overexpression correlates with chromosome 7 polysomy and poor prognostic parameters in clear cell renal cell carcinoma. J. Biomed. Sci. 2012, 19. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Iyevleva, A.G.; Novik, A.V.; Moiseyenko, V.M.; Imyanitov, E.N. EGFR mutation in kidney carcinoma confers sensitivity to gefitinib treatment: A case report. Urol. Oncol. Semin. Orig. Investig. 2009, 27, 548–550. [Google Scholar] [CrossRef]
- Shek, D.; Longmate, J.; Quinn, D.I.; Margolin, K.A.; Twardowski, P.; Gandara, D.R.; Frankel, P.; Pan, C.X.; Lara, P.N. A phase II trial of gefitinib and pegylated IFNα in previously treated renal cell carcinoma. Int. J. Clin. Oncol. 2011, 16, 494–499. [Google Scholar] [CrossRef] [PubMed]
- Motzer, R.J.; Hudes, G.R.; Ginsberg, M.S.; Baum, M.S.; Harmon, C.S.; Kim, S.T.; Chen, I.; Redman, B.G. Phase I/II trial of sunitinib plus gefitinib in patients with metastatic renal cell carcinoma. Am. J. Clin. Oncol. Cancer Clin. Trials 2010, 33, 614–618. [Google Scholar] [CrossRef] [PubMed]
- Weihua, Z.; Tsan, R.; Huang, W.C.; Wu, Q.; Chiu, C.H.; Fidler, I.J.; Hung, M.C. Survival of Cancer Cells Is Maintained by EGFR Independent of Its Kinase Activity. Cancer Cell 2008, 13, 385–393. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Bianchi, C.; Meregalli, C.; Bombelli, S.; Di Stefano, V.; Salerno, F.; Torsello, B.; De Marco, S.; Bovo, G.; Cifola, I.; Mangano, E.; et al. The glucose and lipid metabolism reprogramming is gradedependent in clear cell renal cell carcinoma primary cultures and is targetable to modulate cell viability and proliferation. Oncotarget 2017, 8, 113502–113515. [Google Scholar] [CrossRef] [Green Version]
- Lucarelli, G.; Loizzo, D.; Franzin, R.; Battaglia, S.; Ferro, M.; Cantiello, F.; Castellano, G.; Bettocchi, C.; Ditonno, P.; Battaglia, M. Metabolomic insights into pathophysiological mechanisms and biomarker discovery in clear cell renal cell carcinoma. Expert Rev. Mol. Diagn. 2019, 19, 397–407. [Google Scholar] [CrossRef]
- Lucarelli, G.; Rutigliano, M.; Sallustio, F.; Ribatti, D.; Giglio, A.; Signorile, M.L.; Grossi, V.; Sanese, P.; Napoli, A.; Maiorano, E.; et al. Integrated multi-omics characterization reveals a distinctive metabolic signature and the role of NDUFA4L2 in promoting angiogenesis, chemoresistance, and mitochondrial dysfunction in clear cell renal cell carcinoma. Aging 2018, 10, 3957–3985. [Google Scholar] [CrossRef]
- Lucarelli, G.; Ferro, M.; Loizzo, D.; Bianchi, C.; Terracciano, D.; Cantiello, F.; Bell, L.N.; Battaglia, S.; Porta, C.; Gernone, A.; et al. Integration of lipidomics and transcriptomics reveals reprogramming of the lipid metabolism and composition in clear cell renal cell carcinoma. Metabolites 2020, 10, 509. [Google Scholar] [CrossRef] [PubMed]
- Dittmann, K.; Mayer, C.; Rodemann, H.P. Inhibition of radiation-induced EGFR nuclear import by C225 (Cetuximab) suppresses DNA-PK activity. Radiother Oncol. 2005, 76, 157–161. [Google Scholar] [CrossRef] [PubMed]
- Dittmann, K.; Mayer, C.; Fehrenbacher, B.; Schaller, M.; Raju, U.; Milas, L.; Chen, D.J.; Kehlbach, R.; Rodemann, H.P. Radiation-induced epidermal growth factor receptor nuclear import is linked to activation of DNA-dependent protein kinase. J. Biol. Chem. 2005, 280, 31182–31189. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Eble, J.N.; Togashi, K.; Pisani, P. Tumours of the Kidney. In World Health Organization Classification of Tumours Pathology and Genetics of Tumours of the Urinary System and Male Genital Organs, 3rd ed.; Eble, J.N., Sauter, G., Epstein, J.I., Sesterhenn, I.A., Eds.; IARC Press: Lyon, France, 2004; pp. 9–87. [Google Scholar]
| Variables | n (%) | |
|---|---|---|
| CCRCC | Italy | 63 (52.5) |
| Germany | 57 (47.5) | |
| Males | 71 (59.2) | |
| Mean (SD) age | 62.0 (10.9) | |
| Age ≥ 50 years | 103 (85.8) | |
| Median (IQR) size | 6 (3.5–8.0) | |
| Size > 5 | 68 (56.7) | |
| Nuclear grading according to Fuhrman | 1 | 13 (10.8) |
| 2 | 56 (46.7) | |
| 3 | 42 (35.0) | |
| 4 | 9 (7.5) | |
| Pathologic tumor classification | pT1 | 58 (48.3) |
| pT2 | 17 (14.2) | |
| pT3 | 45 (37.5) | |
| Regional lymph nodes involvment | pNx | 67 (55.8) |
| pN0 | 45 (37.5) | |
| pN1 | 5 (4.2) | |
| pN2 | 3 (2.5) | |
| Distant metastasis | M0 | 87 (72.5) |
| M1 | 33 (27.5) | |
| pTNM Stage | I | 13 (16.1) |
| II | 6 (7.4) | |
| III | 28 (34.6) | |
| IV | 34 (42.0) | |
| Coagulative tumor necrosis | Present | 51 (44.0) |
| Absent | 65 (56.0) | |
| Median (IQR) SSIGN | 5 (2–7) | |
| SSIGN (1) | 0–2 | 39 (32.5) |
| 3–4 | 16 (13.39) | |
| 5–6 | 29 (24.2) | |
| 7–9 | 16 (13.3) | |
| ≥10 | 20 (16.7) | |
| SSIGN (2) | 0–9 | 100 (83.3) |
| ≥10 | 20 (16.7) | |
| Mean (SD) EGFR TS | 177.5 (78.1) | |
| EGFR TS | 0–100 | 20/117 (17.1) |
| 101–200 | 50/117 (42.7) | |
| >201 | 47/117 (40.2) | |
| SGLT1 | Present | 102 (85.0) |
| Absent | 18 (15.0) | |
| EGFR nuclear | Present | 11/57 (19.3) |
| Absent | 46/57 (80.7) | |
| EGFR membranous | Present | 111 (92.5) |
| Absent | 9 (7.5) | |
| Follow-up 5 years | AWD | 32/119 (26.9) |
| DOD | 8/119 (6.7) | |
| NED | 79/119 (66.4) | |
| Variables | rho | p-Value |
|---|---|---|
| Males | 0.07 | 0.470 |
| Age, years | −0.15 | 0.120 |
| Tumor size | 0.15 | 0.120 |
| Nuclear grading according to Fuhrman | 0.35 | 0.0001 |
| Pathological Tumor classification | 0.21 | 0.020 |
| Regional lymph nodes involvement | 0.08 | 0.590 |
| Distant metastasis | 0.12 | 0.220 |
| pTNM stage | 0.12 | 0.310 |
| Coagulative tumor necrosis | −0.03 | 0.720 |
| SSIGN score | 0.25 | 0.007 |
| Presence of SGLT1 | −0.06 | 0.500 |
| Presence of EGFR nuclear | −0.31 | 0.020 |
| Variables | SGLT1 | |||||
|---|---|---|---|---|---|---|
| Absent n (%) | Present n (%) | p-Value | ||||
| Males | 7/29 (24.1) | 4/28 (14.3) | 0.500 | |||
| Age ≥ 50 years | 0/3 (0.0) | 11/54 (20.4) | 1.000 | |||
| Tumor size > 5 | 8/32 (25.0) | 3/25 (12.0) | 0.320 | |||
| SSIGN score ≥ 10 | 11/54 (20.4) | 0/3 (0.0) | 1.000 | |||
| Coagulative tumor necrosis | 2/23 (8.7) | 9/30 (30.0) | 0.090 | |||
| Regional lymph nodes involvement | pN0 | pN1 | p-value | |||
| Presence of EGFR nuclear, n (%) | 3/12 (25.0) | 0/1 (0.0) | 1.000 | |||
| Distant metastasis | M0 | M1 27/33 (81.8) | p-value | |||
| Presence of EGFR nuclear, n (%) | 11/52 (21.2) | 0/5 (0.0) | 0.570 | |||
| Nuclear grading according to Fuhrman | G1 | G2 | G3–G4 | p-value | ||
| Presence of EGFR nuclear, n (%) | 3/12 (25.0) | 6/29 (20.7) | 2/16 (12.5) | 0.750 | ||
| Pathological Tumor classification | pT1 | pT2 | pT3 | p-value | ||
| Presence of EGFR nuclear, n (%) | 8/35 (22.9) | 1/6 (16.7) | 2/16 (12.5) | 0.780 | ||
| pTNM stage | 1 | 2 | 3 | 4 | p-value | |
| Presence of EGFR nuclear, n (%) | 1/3 (33.3) | 1/1 (100.0) | 2/14 (14.3) | 0/5 (0.0) | 0.160 | |
| Variables | SGLT1 | |||||||
|---|---|---|---|---|---|---|---|---|
| Absent n (%) | Present n (%) | p-Value | ||||||
| Males | 44/49 (89.8) | 58/71 (81.7) | 0.220 | |||||
| Age ≥ 50 years | 14/17 (82.4) | 88/103 (85.4) | 0.720 | |||||
| Tumor size > 5 | 46/52 (88.5) | 56/68 (82.4) | 0.350 | |||||
| SSIGN score ≥ 10 | 84/100 (84.0) | 18/20 (90.0) | 0.730 | |||||
| Coagulative tumor necrosis | 53/65 (81.5) | 45/51 (88.2) | 0.320 | |||||
| Regional lymph nodes involvement | pN0 | pN1 | pN2 | p-value | ||||
| Presence of SGLT1, n (%) | 40/45 (88.9) | 5/5 (100.0) | 3/3 (100.0) | 1.000 | ||||
| Distant metastasis | M0 | M1 | p-value | |||||
| Presence of SGLT1, n (%) | 75/87 (86.29) | 27/33 (81.8) | 0.550 | |||||
| Nuclear grading according to Fuhrman | G1 | G2 | G3–G4 | p-value | ||||
| Presence of SGLT1, n (%) | 11/13 (84.6) | 47/56 (83.9) | 44/51 (86.3) | 0.940 | ||||
| Pathological Tumor classification | pT1 | pT2 | pT3 | p-value | ||||
| Presence of SGLT1, n (%) | 54/58 (93.1) | 13/17 (76.5) | 35/45 (77.8) | 0.040 | ||||
| pTNM stage | 1 | 2 | 3 | 4 | p-value | |||
| Presence of SGLT1, n (%) | 12/13 (92.3) | 6/6 (100.0) | 20/28 (71.4) | 28/34 (82.4) | 0.310 | |||
| Variables | OR (95% CI) | p-Value | OR (95% CI) | p-Value |
|---|---|---|---|---|
| Males | 1.5 (0.7–3.2) | 0.33 | ||
| Age, years | 1.0 (0.9–1.0) | 0.37 | 1.0 (0.9–1.1) | 0.85 |
| Tumor size | 1.3 (1.1–1.4) | 0.001 | 1.0 (0.8–1.3) | 0.78 |
| Nuclear grading according to Fuhrman | 3.5 (1.9–6.4) | <0.0001 | 0.4 (0.1–1.2) | 0.11 |
| Pathological Tumor classification | 2.0 (1.3–3.0) | 0.002 | 0.2 (0.1–0.6) | 0.003 |
| Regional lymph nodes involvement | 5.8 (0.8–41.1) | 0.08 | ||
| Distant metastasis | - | - | ||
| pTNM stage | - | - | ||
| Coagulative tumor necrosis | 1.5 (0.7–3.2) | 0.30 | ||
| SSIGN score | 1.8 (1.5–2.2) | <0.0001 | 2.7 (1.8–4.0) | <0.0001 |
| EGFR total score | 1.0 (1.0–1.0) | 0.07 | ||
| Presence of EGFR membranous | 1.8 (0.4–9.3) | 0.46 | ||
| Presence of EGFR nuclear | - | - | ||
| Presence of SGLT1 | 0.6 (0.2–1.6) | 0.30 |
| EGFRm/EGFRn | NED | AWD/DOD | p-Value |
| +/+, n (%) | 9 (20.0) | 0 (0.0) | 0.09 |
| +/−, n (%) | 33 (73.3) | 11 (91.7) | 0.26 |
| −/+, n (%) | 2 (4.4) | 0 (0.0) | 1.00 |
| −/−, n (%) | 1 (2.2) | 1 (8.3) | 0.38 |
| EGFRm/SGLT1 | NED | AWD/DOD | p-Value |
| +/+, n (%) | 62 (78.5) | 30 (75.0) | 0.67 |
| +/−, n (%) | 10 (12.7) | 8 (20.0) | 0.29 |
| −/+, n (%) | 7 (8.9) | 2 (5.0) | 0.72 |
| −/−, n (%) | - | - | - |
| EGFRn/SGLT1 | NED | AWD/DOD | p-Value |
| +/+, n (%) | 10 (22.2) | 0 (0.0) | 0.10 |
| +/−, n (%) | 1 (2.2) | 0 (0.0) | 1.00 |
| −/+, n (%) | 32 (71.1) | 9 (75.0) | 1.00 |
| −/−, n (%) | 2 (4.4) | 3 (25.0) | 0.06 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Muroni, M.R.; Ribback, S.; Sotgiu, G.; Kroeger, N.; Saderi, L.; Angius, A.; Cossu-Rocca, P.; De Miglio, M.R. Prognostic Impact of Membranous/Nuclear Epidermal Growth Factor Receptor Localization in Clear Cell Renal Cell Carcinoma. Int. J. Mol. Sci. 2021, 22, 8747. https://doi.org/10.3390/ijms22168747
Muroni MR, Ribback S, Sotgiu G, Kroeger N, Saderi L, Angius A, Cossu-Rocca P, De Miglio MR. Prognostic Impact of Membranous/Nuclear Epidermal Growth Factor Receptor Localization in Clear Cell Renal Cell Carcinoma. International Journal of Molecular Sciences. 2021; 22(16):8747. https://doi.org/10.3390/ijms22168747
Chicago/Turabian StyleMuroni, Maria Rosaria, Silvia Ribback, Giovanni Sotgiu, Nils Kroeger, Laura Saderi, Andrea Angius, Paolo Cossu-Rocca, and Maria Rosaria De Miglio. 2021. "Prognostic Impact of Membranous/Nuclear Epidermal Growth Factor Receptor Localization in Clear Cell Renal Cell Carcinoma" International Journal of Molecular Sciences 22, no. 16: 8747. https://doi.org/10.3390/ijms22168747
APA StyleMuroni, M. R., Ribback, S., Sotgiu, G., Kroeger, N., Saderi, L., Angius, A., Cossu-Rocca, P., & De Miglio, M. R. (2021). Prognostic Impact of Membranous/Nuclear Epidermal Growth Factor Receptor Localization in Clear Cell Renal Cell Carcinoma. International Journal of Molecular Sciences, 22(16), 8747. https://doi.org/10.3390/ijms22168747









