The Role of Estrogen Receptors and Their Signaling across Psychiatric Disorders
Abstract
1. Introduction
2. Estrogen Receptor Signaling
2.1. Estrogen
2.2. Estrogen Receptors and Their Signaling Mechanisms
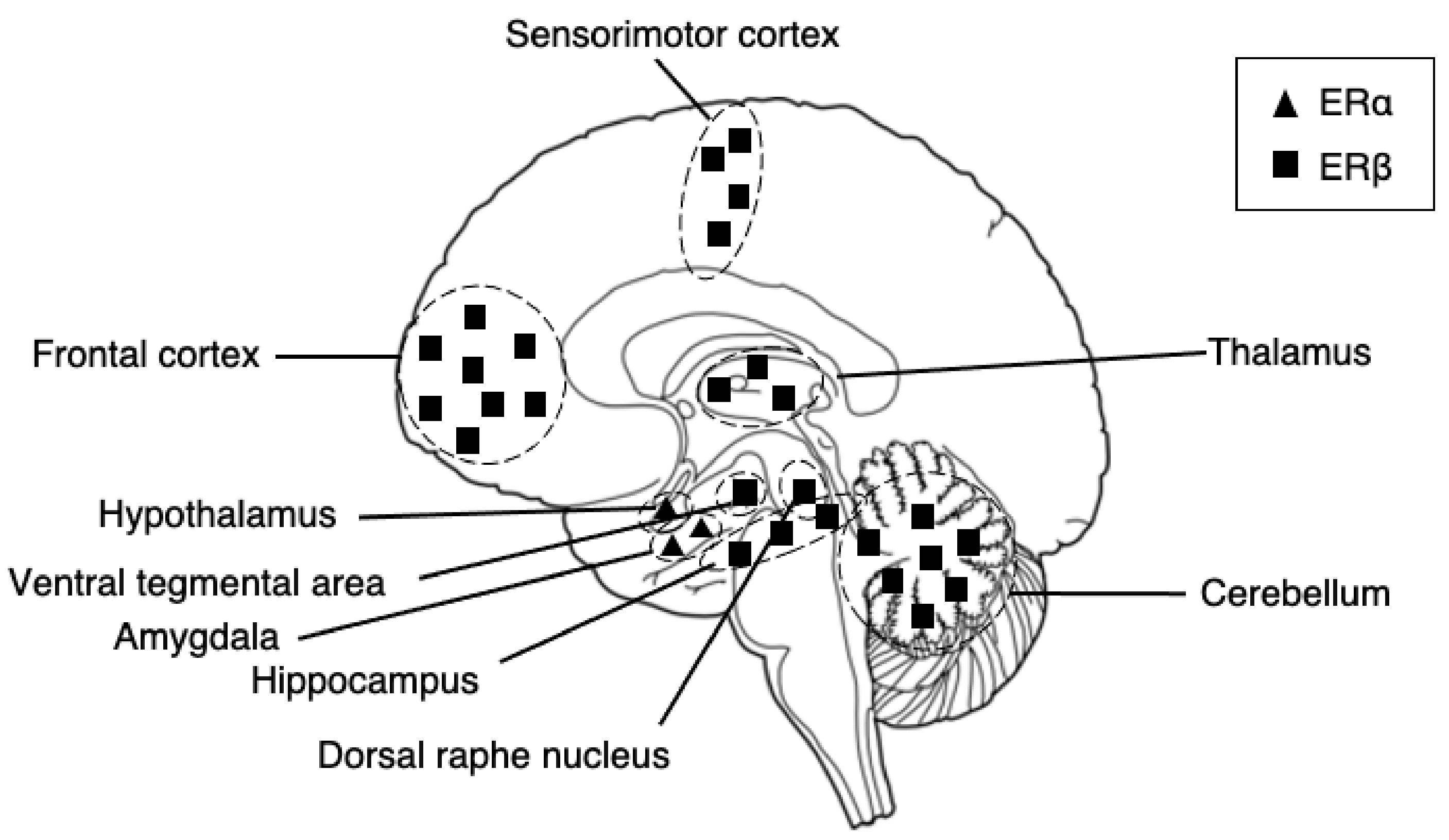
2.3. Estrogen Receptors in the Brain
2.4. Mechanism of Actions on Neurotransmitter Systems
2.5. Estrogen Receptors and Cognition
Beneficial Effects of Selective Estrogen Receptor Modulators (SERMs) on Cognition
2.6. Estrogen and Its Neuroprotective Effects
3. Estrogen Receptor and Psychiatric Disorders
3.1. Schizophrenia
3.2. Bipolar Disorder
3.3. MDD
3.4. ASD
3.5. ADHD
3.6. Anxiety Disorders
3.6.1. Generalized Anxiety Disorder (GAD)
3.6.2. PTSD
3.7. Eating Disorders
3.8. Substance Use Disorder
Alcohol Use Disorder
4. Conclusions
Author Contributions
Funding
Conflicts of Interest
Abbreviations
| ADHD | Attention-deficit hyperactivity disorder |
| Akt | Protein kinase B |
| ASD | Autism spectrum disorder |
| BDNF | Brain-derived neurotrophic factor |
| BPA | Bisphenol A |
| CA1 | Cornu ammonis 1 |
| CA2 | Cornu ammonis 2 |
| CA3 | Cornu ammonis 3 |
| cAMP | Cyclic adenosine monophosphate |
| CSTC | Cortico-striato-thalamo-cortical |
| ERα | Estrogen receptor alpha |
| ERβ | Estrogen receptor beta |
| ERE | Estrogen response elements |
| ERK | Extracellular signal-regulated kinase |
| ERT | Estrogen replacement therapy |
| fMRI | Functional magnetic resonance imaging |
| GPER | G-protein coupled receptor 30 |
| HDAC4 | Histone deacetylase 4 |
| MAPK | Mitogen-activated protein kinase |
| NTD | Amino-terminal domain |
| PI3K | Phosphatidylinositol 3-kinase |
| PKA | Protein kinase A |
| SERMs | Selective estrogen receptor modulators |
| Wnt | Wingless-int |
References
- Our World in Data. Global Mental Health: Five Key Insights Which Emerge from the Data. Available online: https://ourworldindata.org/global-mental-health (accessed on 29 November 2020).
- Findlay, J.K.; Liew, S.H.; Simpson, E.R.; Korach, K.S. Estrogen Signaling in the Regulation of Female Reproductive Functions. Handb. Exp. Pharmacol. 2010, 198, 29–35. [Google Scholar]
- Colzato, L.S.; Hommel, B. Effects of estrogen on higher-order cognitive functions in unstressed human females may depend on individual variation in dopamine baseline levels. Front. Neurosci. 2014, 8, 65. [Google Scholar] [CrossRef] [PubMed]
- Almey, A.; Milner, T.A.; Brake, W.G. Estrogen receptors in the central nervous system and their implication for dopamine-dependent cognition in females. Horm. Behav. 2015, 74, 125–138. [Google Scholar] [CrossRef] [PubMed]
- Frizell, B.; Dumas, J.A. Examining the Relationship Between Neurosteroids, Cognition, and Menopause With Neuroimaging Methods. Curr. Psychiatry Rep. 2018, 20, 96. [Google Scholar] [CrossRef]
- Gasbarri, A.; Pompili, A.; D’Onofrio, A.; Cifariello, A.; Tavares, M.C.; Tomaz, C. Working memory for emotional facial expressions: Role of the estrogen in young women. Psychoneuroendocrinology 2008, 33, 964–972. [Google Scholar] [CrossRef]
- Dreher, J.-C.; Schmidt, P.J.; Kohn, P.; Furman, D.; Rubinow, D.; Berman, K.F. Menstrual cycle phase modulates reward-related neural function in women. Proc. Natl. Acad. Sci. USA 2007, 104, 2465–2470. [Google Scholar] [CrossRef]
- Jacobs, E.; D’Esposito, M. Estrogen shapes dopamine-dependent cognitive processes: Implications for women’s health. J. Neurosci. Off. J. Soc. Neurosci. 2011, 31, 5286–5293. [Google Scholar] [CrossRef]
- Saldanha, C.J. Estrogen as a Neuroprotectant in Both Sexes: Stories From the Bird Brain. Front. Neurol. 2020, 11, 497. [Google Scholar] [CrossRef]
- Azcoitia, I.; Barreto, G.E.; Garcia-Segura, L.M. Molecular mechanisms and cellular events involved in the neuroprotective actions of estradiol. Analysis of sex differences. Front. Neuroendocrinol. 2019, 55, 100787. [Google Scholar] [CrossRef]
- McGregor, C.; Riordan, A.; Thornton, J. Estrogens and the cognitive symptoms of schizophrenia: Possible neuroprotective mechanisms. Front. Neuroendocrinol. 2017, 47, 19–33. [Google Scholar] [CrossRef]
- Gogos, A.; Ney, L.J.; Seymour, N.; Van Rheenen, T.E.; Felmingham, K.L. Sex differences in schizophrenia, bipolar disorder, and post-traumatic stress disorder: Are gonadal hormones the link? Br. J. Pharmacol. 2019, 176, 4119–4135. [Google Scholar] [CrossRef] [PubMed]
- Crider, A.; Pillai, A. Estrogen Signaling as a Therapeutic Target in Neurodevelopmental Disorders. J. Pharmacol. Exp. Ther. 2017, 360, 48–58. [Google Scholar] [CrossRef] [PubMed]
- Cho, M.; Lee, T.Y.; Kwak, Y.B.; Yoon, Y.B.; Kim, M.; Kwon, J.S. Adjunctive use of anti-inflammatory drugs for schizophrenia: A meta-analytic investigation of randomized controlled trials. Aust. N. Z. J. Psychiatry 2019, 53, 742–759. [Google Scholar] [CrossRef] [PubMed]
- Kulkarni, J.; Butler, S.; Riecher-Rössler, A. Estrogens and SERMS as adjunctive treatments for schizophrenia. Front. Neuroendocrinol. 2019, 53, 100743. [Google Scholar] [CrossRef]
- Çakici, N.; van Beveren, N.J.M.; Judge-Hundal, G.; Koola, M.M.; Sommer, I.E.C. An update on the efficacy of anti-inflammatory agents for patients with schizophrenia: A meta-analysis. Psychol. Med. 2019, 49, 2307–2319. [Google Scholar] [CrossRef]
- Dwyer, J.B.; Aftab, A.; Radhakrishnan, R.; Widge, A.; Rodriguez, C.I.; Carpenter, L.L.; Nemeroff, C.B.; McDonald, W.M.; Kalin, N.H. Hormonal Treatments for Major Depressive Disorder: State of the Art. Am. J. Psychiatry 2020, 177, 686–705. [Google Scholar] [CrossRef]
- Jeppesen, R.; Christensen, R.H.B.; Pedersen, E.M.J.; Nordentoft, M.; Hjorthøj, C.; Köhler-Forsberg, O.; Benros, M.E. Efficacy and safety of anti-inflammatory agents in treatment of psychotic disorders—A comprehensive systematic review and meta-analysis. Brain Behav. Immun. 2020, 90, 364–380. [Google Scholar] [CrossRef]
- Sherwin, B.B. Estrogen and Cognitive Functioning in Women: Lessons We Have Learned. Behav Neurosci. 2012, 126, 123–127. [Google Scholar] [CrossRef]
- Liang, J.; Shang, Y. Estrogen and cancer. Annu. Rev. Physiol. 2013, 75, 225–240. [Google Scholar] [CrossRef]
- Sayed, Y.; Taxel, P. The use of estrogen therapy in men. Curr. Opin. Pharmacol. 2003, 3, 650–654. [Google Scholar] [CrossRef]
- Schulster, M.; Bernie, A.M.; Ramasamy, R. The role of estradiol in male reproductive function. Asian J. Androl. 2016, 18, 435–440. [Google Scholar] [PubMed]
- Gruber, C.J.; Tschugguel, W.; Schneeberger, C.; Huber, J.C. Production and actions of estrogens. N. Engl. J. Med. 2002, 346, 340–352. [Google Scholar] [CrossRef] [PubMed]
- Denley, M.C.S.; Gatford, N.J.F.; Sellers, K.J.; Srivastava, D.P. Estradiol and the Development of the Cerebral Cortex: An Unexpected Role? Front. Neurosci. 2018, 12, 245. [Google Scholar] [CrossRef] [PubMed]
- Azcoitia, I.; Arevalo, M.-A.; De Nicola, A.F.; Garcia-Segura, L.M. Neuroprotective actions of estradiol revisited. Trends Endocrinol. Metab. 2011, 22, 467–473. [Google Scholar] [CrossRef] [PubMed]
- Prossnitz, E.R.; Sklar, L.A.; Oprea, T.I.; Arterburn, J.B. GPR30: A novel therapeutic target in estrogen-related disease. Trends Pharmacol. Sci. 2008, 29, 116–123. [Google Scholar] [CrossRef] [PubMed]
- Vrtačnik, P.; Ostanek, B.; Mencej-Bedrač, S.; Marc, J. The many faces of estrogen signaling. Biochem. Med. 2014, 24, 329–342. [Google Scholar] [CrossRef] [PubMed]
- Liu, M.-M.; Albanese, C.; Anderson, C.M.; Hilty, K.; Webb, P.; Uht, R.M.; Price, R.H., Jr.; Pestell, R.G.; Kushner, P.J. Opposing action of estrogen receptors alpha and beta on cyclin D1 gene expression. J. Biol. Chem. 2002, 277, 24353–24360. [Google Scholar] [CrossRef]
- Marino, M.; Galluzzo, P.; Ascenzi, P. Estrogen signaling multiple pathways to impact gene transcription. Curr. Genom. 2006, 7, 497–508. [Google Scholar] [CrossRef]
- Fuentes, N.; Silveyra, P. Estrogen receptor signaling mechanisms. Adv. Protein Chem. Struct. Biol. 2019, 116, 135–170. [Google Scholar]
- Hwang, W.J.; Cho, K.I.K.; Kwak, Y.B.; Lee, J.; Kim, M.; Lee, T.Y.; Kwon, J.S. Intact thalamic microstructure in asymptomatic relatives of schizophrenia patients with high genetic loading. Schizophr. Res. 2020. [Google Scholar] [CrossRef]
- Prossnitz, E.R.; Arterburn, J.B. International Union of Basic and Clinical Pharmacology. XCVII. G Protein-Coupled Estrogen Receptor and Its Pharmacologic Modulators. Pharmacol. Rev. 2015, 67, 505–540. [Google Scholar] [CrossRef] [PubMed]
- Montague, D.; Weickert, C.S.; Tomaskovic-Crook, E.; Rothmond, D.A.; Kleinman, J.E.; Rubinow, D.R. Oestrogen receptor alpha localisation in the prefrontal cortex of three mammalian species. J. Neuroendocrinol. 2008, 20, 893–903. [Google Scholar] [CrossRef] [PubMed]
- Kritzer, M.F. Regional, laminar, and cellular distribution of immunoreactivity for ER alpha and ER beta in the cerebral cortex of hormonally intact, adult male and female rats. Cereb. Cortex 2002, 12, 116–128. [Google Scholar] [CrossRef] [PubMed]
- Shughrue, P.J.; Lane, M.V.; Merchenthaler, I. Comparative distribution of estrogen receptor-alpha and -beta mRNA in the rat central nervous system. J. Comp. Neurol. 1997, 388, 507–525. [Google Scholar] [CrossRef]
- González, M.; Cabrera-Socorro, A.; Pérez-García, C.G.; Fraser, J.D.; López, F.J.; Alonso, R.; Meyer, G. Distribution patterns of estrogen receptor alpha and beta in the human cortex and hippocampus during development and adulthood. J. Comp. Neurol. 2007, 503, 790–802. [Google Scholar] [CrossRef]
- Ostlund, H.; Keller, E.; Hurd, Y.L. Estrogen receptor gene expression in relation to neuropsychiatric disorders. Ann. N. Y. Acad. Sci. 2003, 1007, 54–63. [Google Scholar] [CrossRef]
- Simerly, R.B.; Chang, C.; Muramatsu, M.; Swanson, L.W. Distribution of androgen and estrogen receptor mRNA-containing cells in the rat brain: An in situ hybridization study. J. Comp. Neurol. 1990, 294, 76–95. [Google Scholar] [CrossRef]
- Osterlund, M.K.; Gustafsson, J.A.; Keller, E.; Hurd, Y.L. Estrogen receptor beta (ERbeta) messenger ribonucleic acid (mRNA) expression within the human forebrain: Distinct distribution pattern to ERalpha mRNA. J. Clin. Endocrinol. Metab. 2000, 85, 3840–3846. [Google Scholar]
- Osterlund, M.K.; Keller, E.; Hurd, Y.L. The human forebrain has discrete estrogen receptor alpha messenger RNA expression: High levels in the amygdaloid complex. Neuroscience 2000, 95, 333–342. [Google Scholar] [CrossRef]
- Purves-Tyson, T.D.; Handelsman, D.J.; Double, K.L.; Owens, S.J.; Bustamante, S.; Weickert, C.S. Testosterone regulation of sex steroid-related mRNAs and dopamine-related mRNAs in adolescent male rat substantia nigra. BMC Neurosci. 2012, 13, 95. [Google Scholar] [CrossRef]
- Sánchez, M.G.; Bourque, M.; Morissette, M.; Di Paolo, T. Steroids-dopamine interactions in the pathophysiology and treatment of CNS disorders. CNS Neurosci Ther. 2010, 16, e43–e71. [Google Scholar] [CrossRef]
- Yoest, K.E.; Cummings, J.A.; Becker, J.B. Oestradiol influences on dopamine release from the nucleus accumbens shell: Sex differences and the role of selective oestradiol receptor subtypes. Br. J. Pharmacol. 2019, 176, 4136–4148. [Google Scholar] [CrossRef]
- Wang, J.-X.; Zhuang, J.-Y.; Fu, L.; Lei, Q.; Fan, M.; Zhang, W. How ovarian hormones influence the behavioral activation and inhibition system through the dopamine pathway. PLoS ONE. 2020, 15, e0237032. [Google Scholar]
- Küppers, E.; Beyer, C. Expression of estrogen receptor-alpha and beta mRNA in the developing and adult mouse striatum. Neurosci Lett. 1999, 276, 95–98. [Google Scholar] [CrossRef]
- Mitra, S.W.; Hoskin, E.; Yudkovitz, J.; Pear, L.; Wilkinson, H.A.; Hayashi, S.; Pfaff, D.W.; Ogawa, S.; Rohrer, S.P.; Schaeffer, J.M.; et al. Immunolocalization of estrogen receptor beta in the mouse brain: Comparison with estrogen receptor alpha. Endocrinology 2003, 144, 2055–2067. [Google Scholar] [CrossRef] [PubMed]
- Kruijver, F.P.M.; Balesar, R.; Espila, A.M.; Unmehopa, U.A.; Swaab, D.F. Estrogen-receptor-beta distribution in the human hypothalamus: Similarities and differences with ER alpha distribution. J. Comp. Neurol. 2003, 466, 251–277. [Google Scholar] [CrossRef] [PubMed]
- Bacqué-Cazenave, J.; Bharatiya, R.; Barrière, G.; Delbecque, J.-P.; Bouguiyoud, N.; Di Giovanni, G.; Cattaert, D.; De Deurwaerdère, P. Serotonin in Animal Cognition and Behavior. Int. J. Mol. Sci. 2020, 21, 1649. [Google Scholar] [CrossRef] [PubMed]
- Buhot, M.C. Serotonin receptors in cognitive behaviors. Curr. Opin. Neurobiol. 1997, 7, 243–254. [Google Scholar] [CrossRef]
- Krolick, K.N.; Zhu, Q.; Shi, H. Effects of Estrogens on Central Nervous System Neurotransmission: Implications for Sex Differences in Mental Disorders. Prog. Mol. Biol. Transl. Sci. 2018, 160, 105–171. [Google Scholar] [PubMed]
- Pecins-Thompson, M.; Brown, N.A.; Kohama, S.G.; Bethea, C.L. Ovarian steroid regulation of tryptophan hydroxylase mRNA expression in rhesus macaques. J. Neurosci. Off. J. Soc. Neurosci. 1996, 16, 7021–7029. [Google Scholar] [CrossRef]
- Maharjan, S.; Serova, L.I.; Sabban, E.L. Membrane-initiated estradiol signaling increases tyrosine hydroxylase promoter activity with ER alpha in PC12 cells. J. Neurochem. 2010, 112, 42–55. [Google Scholar] [CrossRef]
- Becker, J.B. Estrogen rapidly potentiates amphetamine-induced striatal dopamine release and rotational behavior during microdialysis. Neurosci. Lett. 1990, 118, 169–171. [Google Scholar] [CrossRef]
- Becker, J.B.; Ramirez, V.D. Experimental studies on the development of sex differences in the release of dopamine from striatal tissue fragments in vitro. Neuroendocrinology 1981, 32, 168–173. [Google Scholar] [CrossRef]
- Becker, J.; Ramirez, V.D. Dynamics of endogenous catecholamine release from brain fragments of male and female rats. Neuroendocrinology 1980, 31, 18–25. [Google Scholar] [CrossRef]
- Hernández, M.L.; Fernández-Ruiz, J.J.; de Miguel, R.; Ramos, J.A. Time-dependent effects of ovarian steroids on tyrosine hydroxylase activity in the limbic forebrain of female rats. J. Neural Transm. Gen. Sect. 1991, 83, 77–84. [Google Scholar] [CrossRef]
- Wallin-Miller, K.G.; Chesley, J.; Castrillon, J.; Wood, R.I. Sex differences and hormonal modulation of ethanol-enhanced risk taking in rats. Drug Alcohol. Depend. 2017, 174, 137–144. [Google Scholar] [CrossRef]
- Hruska, R.E.; Nowak, M.W. Estrogen treatment increases the density of D1 dopamine receptors in the rat striatum. Brain Res. 1988, 442, 349–350. [Google Scholar] [CrossRef]
- Czoty, P.W.; Riddick, N.V.; Gage, H.D.; Sandridge, M.; Nader, S.H.; Garg, S.; Bounds, M.; Garg, P.K.; Nader, M.A. Effect of menstrual cycle phase on dopamine D2 receptor availability in female cynomolgus monkeys. Neuropsychopharmacol. Off. Publ. Am. Coll. Neuropsychopharmacol. 2009, 34, 548–554. [Google Scholar] [CrossRef]
- Bazzett, T.J.; Becker, J.B. Sex differences in the rapid and acute effects of estrogen on striatal D2 dopamine receptor binding. Brain Res. 1994, 637, 163–172. [Google Scholar] [CrossRef]
- Disshon, K.A.; Boja, J.W.; Dluzen, D.E. Inhibition of striatal dopamine transporter activity by 17beta-estradiol. Eur. J. Pharmacol. 1998, 345, 207–211. [Google Scholar] [CrossRef]
- Rehavi, M.; Goldin, M.; Roz, N.; Weizman, A. Regulation of rat brain vesicular monoamine transporter by chronic treatment with ovarian hormones. Brain Res. Mol. Brain Res. 1998, 57, 31–37. [Google Scholar] [CrossRef]
- Chavez, C.; Hollaus, M.; Scarr, E.; Pavey, G.; Gogos, A.; van den Buuse, M. The effect of estrogen on dopamine and serotonin receptor and transporter levels in the brain: An autoradiography study. Brain Res. 2010, 1321, 51–59. [Google Scholar] [CrossRef]
- Bethea, C.L.; Mirkes, S.J.; Shively, C.A.; Adams, M.R. Steroid regulation of tryptophan hydroxylase protein in the dorsal raphe of macaques. Biol Psychiatry 2000, 47, 562–576. [Google Scholar] [CrossRef]
- Sumner, B.E.; Fink, G. Testosterone as well as estrogen increases serotonin2A receptor mRNA and binding site densities in the male rat brain. Brain Res. Mol. Brain Res. 1998, 59, 205–214. [Google Scholar] [CrossRef]
- Sumner, B.E.; Fink, G. Effects of acute estradiol on 5-hydroxytryptamine and dopamine receptor subtype mRNA expression in female rat brain. Mol. Cell. Neurosci. 1993, 4, 83–92. [Google Scholar] [CrossRef]
- Biegon, A.; Reches, A.; Snyder, L.; McEwen, B.S. Serotonergic and noradrenergic receptors in the rat brain: Modulation by chronic exposure to ovarian hormones. Life Sci. 1983, 32, 2015–2021. [Google Scholar] [CrossRef]
- Cyr, M.; Bossé, R.; Di Paolo, T. Gonadal hormones modulate 5-hydroxytryptamine2A receptors: Emphasis on the rat frontal cortex. Neuroscience 1998, 83, 829–836. [Google Scholar] [CrossRef]
- Gundlah, C.; Pecins-Thompson, M.; Schutzer, W.E.; Bethea, C.L. Ovarian steroid effects on serotonin 1A, 2A and 2C receptor mRNA in macaque hypothalamus. Brain Res. Mol. Brain Res. 1999, 63, 325–339. [Google Scholar] [CrossRef]
- Rivera, H.M.; Santollo, J.; Nikonova, L.V.; Eckel, L.A. Estradiol increases the anorexia associated with increased 5-HT(2C) receptor activation in ovariectomized rats. Physiol. Behav. 2012, 105, 188–194. [Google Scholar] [CrossRef]
- Singh, A.; Lucki, I. Antidepressant-like activity of compounds with varying efficacy at 5-HT1A receptors. Neuropharmacology 1993, 32, 331–340. [Google Scholar] [CrossRef]
- Hoffman, B.J.; Hansson, S.R.; Mezey, E.; Palkovits, M. Localization and dynamic regulation of biogenic amine transporters in the mammalian central nervous system. Front. Neuroendocrinol. 1998, 19, 187–231. [Google Scholar] [CrossRef]
- Holschneider, D.P.; Kumazawa, T.; Chen, K.; Shih, J.C. Tissue-specific effects of estrogen on monoamine oxidase A and B in the rat. Life Sci. 1998, 63, 155–160. [Google Scholar] [CrossRef]
- Ortega-Corona, B.G.; Valencia-Sánchez, A.; Kubli-Garfias, C.; Anton-Tay, F.; Salazar, L.A.; Villarreal, J.E.; Ponce-Monter, H. Hypothalamic monoamine oxidase activity in ovariectomized rats after sexual behavior restoration. Arch. Med. Res. 1994, 25, 337–340. [Google Scholar]
- Gazzaley, A.H.; Weiland, N.G.; McEwen, B.S.; Morrison, J.H. Differential regulation of NMDAR1 mRNA and protein by estradiol in the rat hippocampus. J. Neurosci. Off. J. Soc. Neurosci. 1996, 16, 6830–6838. [Google Scholar] [CrossRef]
- Adams, M.M.; Fink, S.E.; Janssen, W.G.M.; Shah, R.A.; Morrison, J.H. Estrogen modulates synaptic N-methyl-D-aspartate receptor subunit distribution in the aged hippocampus. J. Comp. Neurol. 2004, 474, 419–426. [Google Scholar] [CrossRef]
- Woolley, C.S.; Weiland, N.G.; McEwen, B.S.; Schwartzkroin, P.A. Estradiol increases the sensitivity of hippocampal CA1 pyramidal cells to NMDA receptor-mediated synaptic input: Correlation with dendritic spine density. J. Neurosci. Off. J. Soc. Neurosci. 1997, 17, 1848–1859. [Google Scholar] [CrossRef]
- Kurata, K.; Takebayashi, M.; Morinobu, S.; Yamawaki, S. beta-estradiol, dehydroepiandrosterone, and dehydroepiandrosterone sulfate protect against N-methyl-D-aspartate-induced neurotoxicity in rat hippocampal neurons by different mechanisms. J. Pharmacol. Exp. Ther. 2004, 311, 237–245. [Google Scholar] [CrossRef]
- Kajta, M.; Lasoń, W. Oestrogen effects on kainate-induced toxicity in primary cultures of rat cortical neurons. Acta Neurobiol. Exp. 2000, 60, 365–369. [Google Scholar]
- Fischer, B.; Gleason, C.; Asthana, S. Effects of hormone therapy on cognition and mood. Fertil. Steril. 2014, 101, 898–904. [Google Scholar] [CrossRef][Green Version]
- Verghese, J.; Kuslansky, G.; Katz, M.J.; Sliwinski, M.; Crystal, H.A.; Buschke, H.; Lipton, R.B. Cognitive performance in surgically menopausal women on estrogen. Neurology 2000, 55, 872–874. [Google Scholar] [CrossRef]
- Rissman, E.F.; Heck, A.L.; Leonard, J.E.; Shupnik, M.A.; Gustafsson, J.-A. Disruption of estrogen receptor beta gene impairs spatial learning in female mice. Proc. Natl. Acad. Sci. USA 2002, 99, 3996–4001. [Google Scholar] [CrossRef]
- Rissman, E.F.; Wersinger, S.R.; Fugger, H.N.; Foster, T.C. Sex with knockout models: Behavioral studies of estrogen receptor alpha. Brain Res. 1999, 835, 80–90. [Google Scholar] [CrossRef]
- Hara, Y.; Waters, E.M.; McEwen, B.S.; Morrison, J.H. Estrogen Effects on Cognitive and Synaptic Health Over the Lifecourse. Physiol Rev. 2015, 95, 785–807. [Google Scholar] [CrossRef]
- Khan, M.M.; Wakade, C.; de Sevilla, L.; Brann, D.W. Selective estrogen receptor modulators (SERMs) enhance neurogenesis and spine density following focal cerebral ischemia. J. Steroid Biochem. Mol. Biol. 2015, 146, 38–47. [Google Scholar] [CrossRef]
- Lu, Y.; Sareddy, G.R.; Wang, J.; Wang, R.; Li, Y.; Dong, Y.; Zhang, Q.; Liu, J.; O’Connor, J.C.; Xu, J.; et al. Neuron-Derived Estrogen Regulates Synaptic Plasticity and Memory. J. Neurosci. 2019, 39, 2792–2809. [Google Scholar] [CrossRef]
- Hampson, E. Estrogens, Aging, and Working Memory. Curr. Psychiatry Rep. 2018, 20, 109. [Google Scholar] [CrossRef]
- Bastos, C.P.; Pereira, L.M.; Ferreira-Vieira, T.H.; Drumond, L.E.; Massensini, A.R.; Moraes, M.F.D.; Pereira, G.S. Object recognition memory deficit and depressive-like behavior caused by chronic ovariectomy can be transitorialy recovered by the acute activation of hippocampal estrogen receptors. Psychoneuroendocrinology 2015, 57, 14–25. [Google Scholar] [CrossRef]
- Duff, S.J.; Hampson, E. A Beneficial Effect of Estrogen on Working Memory in Postmenopausal Women Taking Hormone Replacement Therapy. Horm. Behav. 2000, 38, 262–276. [Google Scholar] [CrossRef]
- Hussain, D.; Hanafi, S.; Konishi, K.; Brake, W.G.; Bohbot, V.D. Modulation of spatial and response strategies by phase of the menstrual cycle in women tested in a virtual navigation task. Psychoneuroendocrinology 2016, 70, 108–117. [Google Scholar] [CrossRef]
- Wallace, M.; Luine, V.; Arellanos, A.; Frankfurt, M. Ovariectomized rats show decreased recognition memory and spine density in the hippocampus and prefrontal cortex. Brain Res. 2006, 1126, 176–182. [Google Scholar] [CrossRef]
- Tuscher, J.J.; Luine, V.; Frankfurt, M.; Frick, K.M. Estradiol-Mediated Spine Changes in the Dorsal Hippocampus and Medial Prefrontal Cortex of Ovariectomized Female Mice Depend on ERK and mTOR Activation in the Dorsal Hippocampus. J. Neurosci. Off. J. Soc. Neurosci. 2016, 36, 1483–1489. [Google Scholar] [CrossRef]
- Engler-Chiurazzi, E.B.; Singh, M.; Simpkins, J.W. Reprint of: From the 90’s to now: A brief historical perspective on more than two decades of estrogen neuroprotection. Brain Res. 2016, 1645, 79–82. [Google Scholar] [CrossRef]
- Hwang, W.J.; Lee, T.Y.; Shin, W.-G.; Kim, M.; Kim, J.; Lee, J.; Kwon, J.S. Global and Specific Profiles of Executive Functioning in Prodromal and Early Psychosis. Front. Psychiatry 2019, 10, 356. [Google Scholar] [CrossRef]
- Bloemen, A.J.P.; Oldehinkel, A.J.; Laceulle, O.M.; Ormel, J.; Rommelse, N.N.J.; Hartman, C.A. The association between executive functioning and psychopathology: General or specific? Psychol. Med. 2018, 48, 1787–1794. [Google Scholar] [CrossRef]
- Sinkeviciute, I.; Begemann, M.; Prikken, M.; Oranje, B.; Johnsen, E.; Lei, W.U.; Hugdahl, K.; Kroken, R.A.; Rau, C.; Jacobs, J.D.; et al. Efficacy of different types of cognitive enhancers for patients with schizophrenia: A meta-analysis. NPJ Schizophr. 2018, 4, 1–14. [Google Scholar] [CrossRef]
- Goff, D.C.; Hill, M.; Barch, D. The treatment of cognitive impairment in schizophrenia. Pharmacol. Biochem. Behav. 2011, 99, 245–253. [Google Scholar] [CrossRef]
- Keefe, R.S.E.; Meltzer, H.A.; Dgetluck, N.; Gawryl, M.; Koenig, G.; Moebius, H.J.; Lombardo, I.; Hilt, D.C. Randomized, Double-Blind, Placebo-Controlled Study of Encenicline, an α7 Nicotinic Acetylcholine Receptor Agonist, as a Treatment for Cognitive Impairment in Schizophrenia. Neuropsychopharmacol. Off. Publ. Am. Coll. Neuropsychopharmacol. 2015, 40, 3053–3060. [Google Scholar] [CrossRef]
- Pietrzak, R.H.; Olver, J.; Norman, T.; Piskulic, D.; Maruff, P.; Snyder, P.J. A comparison of the CogState Schizophrenia Battery and the Measurement and Treatment Research to Improve Cognition in Schizophrenia (MATRICS) Battery in assessing cognitive impairment in chronic schizophrenia. J. Clin. Exp. Neuropsychol. 2009, 31, 848–859. [Google Scholar] [CrossRef]
- Nuechterlein, K.H.; Green, M.F.; Kern, R.S.; Baade, L.E.; Barch, D.M.; Cohen, J.D.; Essock, S.; Fenton, W.S.; Frese, F.J., 3rd; Gold, J.M.; et al. The MATRICS Consensus Cognitive Battery, part 1: Test selection, reliability, and validity. Am. J. Psychiatry 2008, 165, 203–213. [Google Scholar] [CrossRef]
- Michalopoulou, P.G.; Lewis, S.W.; Drake, R.J.; Reichenberg, A.; Emsley, R.; Kalpakidou, A.K.; Lees, J.; Bobin, T.; Gilleen, J.K.; Pandina, G.; et al. Modafinil combined with cognitive training: Pharmacological augmentation of cognitive training in schizophrenia. Eur. Neuropsychopharmacol. J. Eur. Coll. Neuropsychopharmacol. 2015, 25, 1178–1189. [Google Scholar] [CrossRef]
- Harper-Harrison, G.; Shanahan, M.M. Hormone Replacement Therapy. In StatPearls; StatPearls Publishing: Treasure Island, FL, USA, 2020; Available online: http://www.ncbi.nlm.nih.gov/books/NBK493191/ (accessed on 29 November 2020).
- Abdelhamid, R.; Luo, J.; Vandevrede, L.; Kundu, I.; Michalsen, B.; Litosh, V.A.; Schiefer, I.T.; Gherezghiher, T.; Yao, P.; Qin, Z.; et al. Benzothiophene Selective Estrogen Receptor Modulators Provide Neuroprotection by a novel GPR30-dependent Mechanism. ACS Chem. Neurosci. 2011, 2, 256–268. [Google Scholar] [CrossRef] [PubMed]
- Bourque, M.; Morissette, M.; Di Paolo, T. Raloxifene activates G protein-coupled estrogen receptor 1/Akt signaling to protect dopamine neurons in 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine mice. Neurobiol. Aging 2014, 35, 2347–2356. [Google Scholar] [CrossRef] [PubMed]
- Salgado, I.K.; Torrado, A.I.; Santiago, J.M.; Miranda, J.D. Tamoxifen and Src kinase inhibitors as neuroprotective/neuroregenerative drugs after spinal cord injury. Neural Regen. Res. 2015, 10, 385–390. [Google Scholar] [PubMed]
- Kuiper, G.G.; Lemmen, J.G.; Carlsson, B.; Corton, J.C.; Safe, S.H.; van der Saag, P.T.; van der Burg, B.; Gustafsson, J.A. Interaction of estrogenic chemicals and phytoestrogens with estrogen receptor beta. Endocrinology 1998, 139, 4252–4263. [Google Scholar] [CrossRef] [PubMed]
- Yazğan, B.; Yazğan, Y.; Övey, İ.S.; Nazıroğlu, M. Raloxifene and Tamoxifen Reduce PARP Activity, Cytokine and Oxidative Stress Levels in the Brain and Blood of Ovariectomized Rats. J. Mol. Neurosci. 2016, 60, 214–222. [Google Scholar] [CrossRef]
- Ishihara, Y.; Itoh, K.; Ishida, A.; Yamazaki, T. Selective estrogen-receptor modulators suppress microglial activation and neuronal cell death via an estrogen receptor-dependent pathway. J. Steroid Biochem. Mol. Biol. 2015, 145, 85–93. [Google Scholar] [CrossRef]
- DonCarlos, L.L.; Azcoitia, I.; Garcia-Segura, L.M. Neuroprotective actions of selective estrogen receptor modulators. Psychoneuroendocrinology 2009, 34 (Suppl. S1), S113–S122. [Google Scholar] [CrossRef]
- Arevalo, M.A.; Santos-Galindo, M.; Lagunas, N.; Azcoitia, I.; Garcia-Segura, L.M. Selective estrogen receptor modulators as brain therapeutic agents. J. Mol. Endocrinol. 2011, 46, R1–R9. [Google Scholar] [CrossRef]
- Brann, D.W.; Dhandapani, K.; Wakade, C.; Mahesh, V.B.; Khan, M.M. Neurotrophic and neuroprotective actions of estrogen: Basic mechanisms and clinical implications. Steroids 2007, 72, 381–405. [Google Scholar] [CrossRef]
- Lu, Y.; Sareddy, G.R.; Wang, J.; Zhang, Q.; Tang, F.-L.; Pratap, U.P.; Tekmal, R.R.; Vadlamudi, R.K.; Brann, D.W. Neuron-Derived Estrogen Is Critical for Astrocyte Activation and Neuroprotection of the Ischemic Brain. J. Neurosci. 2020, 40, 7355–7374. [Google Scholar] [CrossRef]
- Babayan, A.H.; Kramár, E.A. Rapid Effects of Oestrogen on Synaptic Plasticity: Interactions with Actin and its Signaling Proteins. J. Neuroendocrinol. 2013, 25, 1163–1172. [Google Scholar] [CrossRef] [PubMed]
- Lewis-Wambi, J.S.; Jordan, V.C. Estrogen regulation of apoptosis: How can one hormone stimulate and inhibit? Breast Cancer Res. 2009, 11, 206. [Google Scholar] [CrossRef] [PubMed]
- Goodman, Y.; Bruce, A.J.; Cheng, B.; Mattson, M.P. Estrogens attenuate and corticosterone exacerbates excitotoxicity, oxidative injury, and amyloid beta-peptide toxicity in hippocampal neurons. J. Neurochem. 1996, 66, 1836–1844. [Google Scholar] [CrossRef] [PubMed]
- Behl, C.; Widmann, M.; Trapp, T.; Holsboer, F. 17-beta estradiol protects neurons from oxidative stress-induced cell death in vitro. Biochem. Biophys. Res. Commun. 1995, 216, 473–482. [Google Scholar] [CrossRef]
- Rettberg, J.R.; Yao, J.; Brinton, R.D. Estrogen: A master regulator of bioenergetic systems in the brain and body. Front. Neuroendocrinol. 2014, 35, 8–30. [Google Scholar] [CrossRef]
- Villa, A.; Vegeto, E.; Poletti, A.; Maggi, A. Estrogens, Neuroinflammation, and Neurodegeneration. Endocr. Rev. 2016, 37, 372–402. [Google Scholar] [CrossRef]
- Zhang, Z.; Qin, P.; Deng, Y.; Ma, Z.; Guo, H.; Guo, H.; Hou, Y.; Wang, S.; Zou, W.; Sun, Y.; et al. The novel estrogenic receptor GPR30 alleviates ischemic injury by inhibiting TLR4-mediated microglial inflammation. J. Neuroinflamm. 2018, 15, 206. [Google Scholar] [CrossRef]
- Hill, R.A.; van den Buuse, M. Sex-dependent and region-specific changes in TrkB signaling in BDNF heterozygous mice. Brain Res. 2011, 1384, 51–60. [Google Scholar] [CrossRef]
- Brown, C.M.; Mulcahey, T.A.; Filipek, N.C.; Wise, P.M. Production of proinflammatory cytokines and chemokines during neuroinflammation: Novel roles for estrogen receptors alpha and beta. Endocrinology 2010, 151, 4916–4925. [Google Scholar] [CrossRef]
- Scott, E.; Zhang, Q.; Wang, R.; Vadlamudi, R.; Brann, D. Estrogen neuroprotection and the critical period hypothesis. Front. Neuroendocrinol. 2012, 33, 85–104. [Google Scholar] [CrossRef]
- Jablensky, A.; McGrath, J.; Herrman, H.; Castle, D.; Gureje, O.; Evans, M.; Carr, V.; Morgan, V.; Korten, A.; Harvey, C. Psychotic disorders in urban areas: An overview of the Study on Low Prevalence Disorders. Aust. N. Z. J. Psychiatry 2000, 34, 221–236. [Google Scholar] [CrossRef] [PubMed]
- Huber, T.J.; Rollnik, J.; Wilhelms, J.; von zur Mühlen, A.; Emrich, H.M.; Schneider, U. Estradiol levels in psychotic disorders. Psychoneuroendocrinology 2001, 26, 27–35. [Google Scholar] [CrossRef]
- Biegon, A.; McEwen, B.S. Modulation by estradiol of serotonin receptors in brain. J. Neurosci. 1982, 2, 199–205. [Google Scholar] [CrossRef] [PubMed]
- Goldstein, J.M.; Link, B.G. Gender and the expression of schizophrenia. J. Psychiatr. Res. 1988, 22, 141–155. [Google Scholar] [CrossRef]
- Riecher-Rössler, A. Oestrogens, prolactin, hypothalamic-pituitary-gonadal axis, and schizophrenic psychoses. Lancet Psychiatry 2017, 4, 63–72. [Google Scholar] [CrossRef]
- Mahé, V.; Dumaine, A. Oestrogen withdrawal associated psychoses. Acta Psychiatr. Scand. 2001, 104, 323–331. [Google Scholar] [CrossRef]
- Riecher-Rössler, A.; Häfner, H.; Stumbaum, M.; Maurer, K.; Schmidt, R. Can estradiol modulate schizophrenic symptomatology? Schizophr. Bull. 1994, 20, 203–214. [Google Scholar] [CrossRef]
- Gurvich, C.; Gavrilidis, E.; Worsley, R.; Hudaib, A.; Thomas, N.; Kulkarni, J. Menstrual cycle irregularity and menopause status influence cognition in women with schizophrenia. Psychoneuroendocrinology 2018, 96, 173–178. [Google Scholar] [CrossRef]
- Chang, S.S.; Renshaw, D.C. Psychosis and pregnancy. Compr. Ther. 1986, 12, 36–41. [Google Scholar]
- Wei, S.-M.; Berman, K.F. Ovarian hormones, genes, and the brain: The case of estradiol and the brain-derived neurotrophic factor (BDNF) gene. Neuropsychopharmacology 2019, 44, 223–224. [Google Scholar] [CrossRef]
- Damme, K.S.F.; Ristanovic, I.; Vargas, T.; Mittal, V.A. Timing of menarche and abnormal hippocampal connectivity in youth at clinical-high risk for psychosis. Psychoneuroendocrinology 2020, 117, 104672. [Google Scholar] [CrossRef] [PubMed]
- Kulkarni, J.; Gavrilidis, E.; Worsley, R.; Hayes, E. Role of estrogen treatment in the management of schizophrenia. CNS Drugs 2012, 26, 549–557. [Google Scholar] [CrossRef] [PubMed]
- Hoff, A.L.; Kremen, W.S.; Wieneke, M.H.; Lauriello, J.; Blankfeld, H.M.; Faustman, W.O.; Csernansky, J.G.; Nordahl, T.E. Association of Estrogen Levels With Neuropsychological Performance in Women With Schizophrenia. Am. J. Psychiatry 2001, 158, 1134–1139. [Google Scholar] [CrossRef] [PubMed]
- Mendrek, A.; Lakis, N.; Jiménez, J. Associations of sex steroid hormones with cerebral activations during mental rotation in men and women with schizophrenia. Psychoneuroendocrinology 2011, 36, 1422–1426. [Google Scholar] [CrossRef]
- Célia Moreira Borella, V.; Seeman, M.V.; Carneiro Cordeiro, R.; Vieira dos Santos, J.; Romário Matos de Souza, M.; Nunes de Sousa Fernandes, E.; Santos Monte, A.; Maria Mendes Vasconcelos, S.; Quinn, J.P.; de Lucena, D.F.; et al. Gender and estrous cycle influences on behavioral and neurochemical alterations in adult rats neonatally administered ketamine. Dev. Neurobiol. 2016, 76, 519–532. [Google Scholar] [CrossRef]
- Gogos, A.; Kwek, P.; van den Buuse, M. The role of estrogen and testosterone in female rats in behavioral models of relevance to schizophrenia. Psychopharmacology 2012, 219, 213–224. [Google Scholar] [CrossRef]
- Gogos, A.; van den Buuse, M. Comparing the effects of 17β-oestradiol and the selective oestrogen receptor modulators, raloxifene and tamoxifen, on prepulse inhibition in female rats. Schizophr. Res. 2015, 168, 634–639. [Google Scholar] [CrossRef]
- Sbisa, A.; Kusljic, S.; Zethoven, D.; van den Buuse, M.; Gogos, A. The effect of 17β-estradiol on maternal immune activation-induced changes in prepulse inhibition and dopamine receptor and transporter binding in female rats. Schizophr. Res. 2020, 223, 249–257. [Google Scholar] [CrossRef]
- Riecher-Rössler, A.; Kulkarni, J. Estrogens and Gonadal Function in Schizophrenia and Related Psychoses. In Biological Basis of Sex Differences in Psychopharmacology; Current Topics in Behavioral Neurosciences; Neill, J.C., Kulkarni, J., Eds.; Springer: Berlin/Heidelberg, Germany, 2011; pp. 155–171. [Google Scholar] [CrossRef]
- Da Silva, T.L.; Ravindran, A.V. Contribution of sex hormones to gender differences in schizophrenia: A review. Asian J. Psychiatry 2015, 18, 2–14. [Google Scholar] [CrossRef]
- Perlman, W.R.; Tomaskovic-Crook, E.; Montague, D.M.; Webster, M.J.; Rubinow, D.R.; Kleinman, J.E.; Weickert, C.S. Alteration in estrogen receptor alpha mRNA levels in frontal cortex and hippocampus of patients with major mental illness. Biol. Psychiatry 2005, 58, 812–824. [Google Scholar] [CrossRef]
- Weickert, C.S.; Miranda-Angulo, A.L.; Wong, J.; Perlman, W.R.; Ward, S.E.; Radhakrishna, V.; Straub, R.E.; Weinberger, D.R.; Kleinman, J.E. Variants in the estrogen receptor alpha gene and its mRNA contribute to risk for schizophrenia. Hum. Mol. Genet. 2008, 17, 2293–2309. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Kinon, B.J.; Gilmore, J.A.; Liu, H.; Halbreich, U.M. Prevalence of hyperprolactinemia in schizophrenic patients treated with conventional antipsychotic medications or risperidone. Psychoneuroendocrinology 2003, 28 (Suppl. S2), 55–68. [Google Scholar] [CrossRef]
- Canuso, C.M.; Goldstein, J.M.; Wojcik, J.; Dawson, R.; Brandman, D.; Klibanski, A.; Schildkraut, J.J.; Green, A.I. Antipsychotic medication, prolactin elevation, and ovarian function in women with schizophrenia and schizoaffective disorder. Psychiatry Res. 2002, 111, 11–20. [Google Scholar] [CrossRef]
- Aston, J.; Rechsteiner, E.; Bull, N.; Borgwardt, S.; Gschwandtner, U.; Riecher-Rössler, A. Hyperprolactinaemia in early psychosis-not only due to antipsychotics. Prog. Neuropsychopharmacol. Biol. Psychiatry 2010, 34, 1342–1344. [Google Scholar] [CrossRef] [PubMed]
- Ittig, S.; Studerus, E.; Heitz, U.; Menghini-Müller, S.; Beck, K.; Egloff, L.; Leanza, L.; Andreou, C.; Riecher-Rössler, A. Sex differences in prolactin levels in emerging psychosis: Indication for enhanced stress reactivity in women. Schizophr. Res. 2017, 189, 111–116. [Google Scholar] [CrossRef] [PubMed]
- Petrikis, P.; Tigas, S.; Tzallas, A.T.; Archimandriti, D.T.; Skapinakis, P.; Mavreas, V. Prolactin levels in drug-naïve patients with schizophrenia and other psychotic disorders. Int. J. Psychiatry Clin. Pract. 2016, 20, 165–169. [Google Scholar] [CrossRef] [PubMed]
- Riecher-Rössler, A.; Rybakowski, J.K.; Pflueger, M.O.; Beyrau, R.; Kahn, R.S.; Malik, P.; Fleischhacker, W.W.; EUFEST Study Group. Hyperprolactinemia in antipsychotic-naive patients with first-episode psychosis. Psychol. Med. 2013, 43, 2571–2582. [Google Scholar]
- Du, X.; Hill, R.A. Hypothalamic-pituitary-gonadal axis dysfunction: An innate pathophysiology of schizophrenia? Gen. Comp. Endocrinol. 2019, 275, 38–43. [Google Scholar] [CrossRef]
- Bergemann, N.; Parzer, P.; Jaggy, S.; Auler, B.; Mundt, C.; Maier-Braunleder, S. Estrogen and comprehension of metaphoric speech in women suffering from schizophrenia: Results of a double-blind, placebo-controlled trial. Schizophr. Bull. 2008, 34, 1172–1181. [Google Scholar] [CrossRef]
- Kulkarni, J.; Gavrilidis, E.; Wang, W.; Worsley, R.; Fitzgerald, P.B.; Gurvich, C.; Van Rheenen, T.; Berk, M.; Burger, H. Estradiol for treatment-resistant schizophrenia: A large-scale randomized-controlled trial in women of child-bearing age. Mol. Psychiatry 2015, 20, 695–702. [Google Scholar] [CrossRef]
- Khodaie-Ardakani, M.-R.; Khosravi, M.; Zarinfard, R.; Nejati, S.; Mohsenian, A.; Tabrizi, M.; Akhondzadeh, S. A Placebo-Controlled Study of Raloxifene Added to Risperidone in Men with Chronic Schizophrenia. Acta Med. Iran. 2015, 53, 337–345. [Google Scholar] [PubMed]
- Kulkarni, J.; Gavrilidis, E.; Gwini, S.M.; Worsley, R.; Grigg, J.; Warren, A.; Gurvich, C.; Gilbert, H.; Berk, M.; Davis, S.R. Effect of Adjunctive Raloxifene Therapy on Severity of Refractory Schizophrenia in Women: A Randomized Clinical Trial. JAMA Psychiatry 2016, 73, 947–954. [Google Scholar] [CrossRef] [PubMed]
- Weickert, T.W.; Weinberg, D.; Lenroot, R.; Catts, S.V.; Wells, R.; Vercammen, A.; O’Donnell, M.; Galletly, C.; Liu, D.; Balzan, R.; et al. Adjunctive raloxifene treatment improves attention and memory in men and women with schizophrenia. Mol. Psychiatry 2015, 20, 685–694. [Google Scholar] [CrossRef] [PubMed]
- Huerta-Ramos, E.; Labad, J.; Cobo, J.; Núñez, C.; Creus, M.; García-Parés, G.; Cuadras, D.; Franco, J.; Miquel, E.; Reyes, J.C.; et al. Effects of raloxifene on cognition in postmenopausal women with schizophrenia: A 24-week double-blind, randomized, parallel, placebo-controlled trial. Eur. Arch. Psychiatry Clin. Neurosci. 2020, 270, 729–737. [Google Scholar] [CrossRef]
- Shivakumar, V.; Venkatasubramanian, G. Successful use of adjuvant raloxifene treatment in clozapine-resistant schizophrenia. Indian J. Psychiatry 2012, 54, 394. [Google Scholar] [CrossRef]
- Orhan, F.Ö.; Kurutaş, E.B.; Doğaner, A.; Türker, E.; Özcü, S.Ş.T.; Güngör, M.; Çakmak, S. Serum levels of GPER-1 in euthymic bipolar patients. Neuropsychiatr. Dis Treat. 2018, 14, 855–862. [Google Scholar] [CrossRef]
- Middle, F.; Jones, I.; Robertson, E.; Morey, J.; Lendon, C.; Craddock, N. Variation in the coding sequence and flanking splice junctions of the estrogen receptor alpha (ERalpha) gene does not play an important role in genetic susceptibility to bipolar disorder or bipolar affective puerperal psychosis. Am. J. Med. Genet. Part B Neuropsychiatr. Genet. Off. Publ. Int. Soc. Psychiatr. Genet. 2003, 118B, 72–75. [Google Scholar] [CrossRef]
- Kealey, C.; Reynolds, A.; Mynett-Johnson, L.; Claffey, E.; McKeon, P. No evidence to support an association between the oestrogen receptor beta gene and bipolar disorder. Psychiatr. Genet. 2001, 11, 223–226. [Google Scholar] [CrossRef]
- Dias, R.S.; Lafer, B.; Russo, C.; Del Debbio, A.; Nierenberg, A.A.; Sachs, G.S.; Joffe, H. Longitudinal follow-up of bipolar disorder in women with premenstrual exacerbation: Findings from STEP-BD. Am. J. Psychiatry 2011, 168, 386–394. [Google Scholar] [CrossRef]
- Perich, T.A.; Roberts, G.; Frankland, A.; Sinbandhit, C.; Meade, T.; Austin, M.-P.; Mitchell, P.B. Clinical characteristics of women with reproductive cycle-associated bipolar disorder symptoms. Aust. N. Z. J. Psychiatry 2017, 51, 161–167. [Google Scholar] [CrossRef]
- Fallah, E.; Arman, S.; Najafi, M.; Shayegh, B. Effect of Tamoxifen and Lithium on Treatment of Acute Mania Symptoms in Children and Adolescents. Iran. J. Child Neurol. 2016, 10, 16–25. [Google Scholar] [PubMed]
- Palacios, J.; Yildiz, A.; Young, A.H.; Taylor, M.J. Tamoxifen for bipolar disorder: Systematic review and meta-analysis. J. Psychopharmacol. Oxf. Engl. 2019, 33, 177–184. [Google Scholar] [CrossRef] [PubMed]
- Valvassori, S.S.; Dal-Pont, G.C.; Resende, W.R.; Varela, R.B.; Peterle, B.R.; Gava, F.F.; Mina, F.G.; Cararo, J.H.; Carvalho, A.F.; Quevedo, J. Lithium and Tamoxifen Modulate Behavior and Protein Kinase C Activity in the Animal Model of Mania Induced by Ouabain. Int. J. Neuropsychopharmacol. 2017, 20, 877–885. [Google Scholar] [CrossRef] [PubMed]
- Bäckström, T.; Sanders, D.; Leask, R.; Davidson, D.; Warner, P.; Bancroft, J. Mood, sexuality, hormones, and the menstrual cycle. II. Hormone levels and their relationship to the premenstrual syndrome. Psychosom. Med. 1983, 45, 503–507. [Google Scholar] [CrossRef] [PubMed]
- Findikli, E.; Kurutas, E.B.; Camkurt, M.A.; Karaaslan, M.F.; Izci, F.; Fındıklı, H.A.; Kardaş, S.; Dag, B.; Altun, H. Increased Serum G Protein-coupled Estrogen Receptor 1 Levels and Its Diagnostic Value in Drug Naïve Patients with Major Depressive Disorder. Clin. Psychopharmacol. Neurosci. Off. Sci. J. Korean Coll. Neuropsychopharmacol. 2017, 15, 337–342. [Google Scholar] [CrossRef] [PubMed]
- Skovlund, C.W.; Mørch, L.S.; Kessing, L.V.; Lange, T.; Lidegaard, Ø. Association of Hormonal Contraception with Suicide Attempts and Suicides. Am. J. Psychiatry 2018, 175, 336–342. [Google Scholar] [CrossRef] [PubMed]
- Skovlund, C.W.; Mørch, L.S.; Kessing, L.V.; Lidegaard, Ø. Association of Hormonal Contraception with Depression. JAMA Psychiatry 2016, 73, 1154–1162. [Google Scholar] [CrossRef]
- Frye, C.A.; Walf, A.A. Changes in progesterone metabolites in the hippocampus can modulate open field and forced swim test behavior of proestrous rats. Horm. Behav. 2002, 41, 306–315. [Google Scholar] [CrossRef]
- Rachman, I.M.; Unnerstall, J.R.; Pfaff, D.W.; Cohen, R.S. Estrogen alters behavior and forebrain c-fos expression in ovariectomized rats subjected to the forced swim test. Proc. Natl. Acad. Sci. USA 1998, 95, 13941–13946. [Google Scholar] [CrossRef]
- Hodis, H.N.; Mack, W.J.; Henderson, V.W.; Shoupe, D.; Budoff, M.J.; Hwang-Levine, J.; Li, Y.; Feng, M.; Dustin, L.; Kono, N.; et al. Vascular Effects of Early versus Late Postmenopausal Treatment with Estradiol. N. Engl. J. Med. 2016, 374, 1221–1231. [Google Scholar] [CrossRef]
- Loomes, R.; Hull, L.; Mandy, W.P.L. What Is the Male-to-Female Ratio in Autism Spectrum Disorder? A Systematic Review and Meta-Analysis. J. Am. Acad. Child Adolesc. Psychiatry 2017, 56, 466–474. [Google Scholar] [PubMed]
- Baron-Cohen, S.; Auyeung, B.; Nørgaard-Pedersen, B.; Hougaard, D.M.; Abdallah, M.W.; Melgaard, L.; Cohen, A.S.; Chakrabarti, B.; Ruta, L.; Lombardo, M.V. Elevated fetal steroidogenic activity in autism. Mol. Psychiatry 2015, 20, 369–376. [Google Scholar] [CrossRef] [PubMed]
- Crespi, B.J. Oxytocin, testosterone, and human social cognition. Biol. Rev. Camb. Philos. Soc. 2016, 91, 390–408. [Google Scholar] [CrossRef] [PubMed]
- Baron-Cohen, S. The extreme male brain theory of autism. Trends Cogn. Sci. 2002, 6, 248–254. [Google Scholar] [CrossRef]
- Srivastava, D.P.; Woolfrey, K.M.; Liu, F.; Brandon, N.J.; Penzes, P. Estrogen receptor ß activity modulates synaptic signaling and structure. J. Neurosci. Off. J. Soc. Neurosci. 2010, 30, 13454–13460. [Google Scholar] [CrossRef]
- Crider, A.; Thakkar, R.; Ahmed, A.O.; Pillai, A. Dysregulation of estrogen receptor beta (ERβ), aromatase (CYP19A1), and ER co-activators in the middle frontal gyrus of autism spectrum disorder subjects. Mol. Autism 2014, 5, 46. [Google Scholar] [CrossRef]
- Chakrabarti, B.; Dudbridge, F.; Kent, L.; Wheelwright, S.; Hill-Cawthorne, G.; Allison, C.; Banerjee-Basu, S.; Baron-Cohen, S. Genes related to sex steroids, neural growth, and social-emotional behavior are associated with autistic traits, empathy, and Asperger syndrome. Autism Res. Off. J. Int. Soc. Autism Res. 2009, 2, 157–177. [Google Scholar] [CrossRef]
- Rucklidge, J.J. Gender differences in attention-deficit/hyperactivity disorder. Psychiatr. Clin. N. Am. 2010, 33, 357–373. [Google Scholar] [CrossRef]
- Quinn, P.O. Treating adolescent girls and women with ADHD: Gender-specific issues. J. Clin. Psychol. 2005, 61, 579–587. [Google Scholar] [CrossRef]
- Sahin, N.; Altun, H.; Kurutaş, E.B.; Fındıklı, E. Evaluation of estrogen and G protein-coupled estrogen receptor 1 (GPER) levels in drug-naïve patients with attention deficit hyperactivity disorder (ADHD). Bosn. J. Basic Med. Sci. 2018, 18, 126–131. [Google Scholar] [CrossRef]
- Schug, T.T.; Blawas, A.M.; Gray, K.; Heindel, J.J.; Lawler, C.P. Elucidating the links between endocrine disruptors and neurodevelopment. Endocrinology 2015, 156, 1941–1951. [Google Scholar] [CrossRef] [PubMed]
- Matsuda, S.; Matsuzawa, D.; Ishii, D.; Tomizawa, H.; Sutoh, C.; Nakazawa, K.; Amano, K.; Sajiki, J.; Shimizu, E. Effects of perinatal exposure to low dose of bisphenol A on anxiety like behavior and dopamine metabolites in brain. Prog. Neuropsychopharmacol. Biol. Psychiatry 2012, 39, 273–279. [Google Scholar] [CrossRef] [PubMed]
- Wilens, T.E. Effects of methylphenidate on the catecholaminergic system in attention-deficit/hyperactivity disorder. J. Clin. Psychopharmacol. 2008, 28 (Suppl. S2), S46–S53. [Google Scholar] [CrossRef] [PubMed]
- Casas, M.; Forns, J.; Martínez, D.; Avella-García, C.; Valvi, D.; Ballesteros-Gómez, A.; Luque, N.; Rubio, S.; Julvez, J.; Sunyer, J.; et al. Exposure to bisphenol A during pregnancy and child neuropsychological development in the INMA-Sabadell cohort. Environ. Res. 2015, 142, 671–679. [Google Scholar] [CrossRef] [PubMed]
- Rochester, J.R.; Bolden, A.L.; Kwiatkowski, C.F. Prenatal exposure to bisphenol A and hyperactivity in children: A systematic review and meta-analysis. Environ. Int. 2018, 114, 343–356. [Google Scholar] [CrossRef] [PubMed]
- McLean, C.P.; Asnaani, A.; Litz, B.T.; Hofmann, S.G. Gender differences in anxiety disorders: Prevalence, course of illness, comorbidity and burden of illness. J. Psychiatr. Res. 2011, 45, 1027–1035. [Google Scholar] [CrossRef] [PubMed]
- Hayward, C.; Sanborn, K. Puberty and the emergence of gender differences in psychopathology. J. Adolesc. Health 2002, 30 (Suppl. S1), 49–58. [Google Scholar] [CrossRef]
- Fındıklı, E.; Camkurt, M.A.; Karaaslan, M.F.; Kurutas, E.B.; Altun, H.; İzci, F.; Fındıklı, H.A.; Kardas, S. Serum levels of G protein-coupled estrogen receptor 1 (GPER1) in drug-naive patients with generalized anxiety disorder. Psychiatry Res. 2016, 244, 312–316. [Google Scholar] [CrossRef]
- Zheng, Y.; Wu, M.; Gao, T.; Meng, L.; Ding, X.; Meng, Y.; Jiao, Y.; Luo, P.; He, Z.; Sun, T.; et al. GPER-Deficient Rats Exhibit Lower Serum Corticosterone Level and Increased Anxiety-Like Behavior. Neural Plast. 2020, 2020, 8866187. [Google Scholar] [CrossRef]
- Solomon, M.B.; Herman, J.P. Sex differences in psychopathology: Of gonads, adrenals and mental illness. Physiol. Behav. 2009, 97, 250–258. [Google Scholar] [CrossRef]
- Dombret, C.; Naulé, L.; Trouillet, A.-C.; Parmentier, C.; Hardin-Pouzet, H.; Mhaouty-Kodja, S. Effects of neural estrogen receptor beta deletion on social and mood-related behaviors and underlying mechanisms in male mice. Sci. Rep. 2020, 10, 6242. [Google Scholar] [CrossRef] [PubMed]
- Miller, C.K.; Krentzel, A.A.; Patisaul, H.B.; Meitzen, J. Metabotropic glutamate receptor subtype 5 (mGlu5) is necessary for estradiol mitigation of light-induced anxiety behavior in female rats. Physiol. Behav. 2020, 214, 112770. [Google Scholar] [CrossRef] [PubMed]
- Kessler, R.C.; Aguilar-Gaxiola, S.; Alonso, J.; Benjet, C.; Bromet, E.J.; Cardoso, G.; Degenhardt, L.; de Girolamo, G.; Dinolova, R.V.; Ferry, F.; et al. Trauma and PTSD in the WHO World Mental Health Surveys. Eur. J. Psychotraumatol. 2017, 8 (Suppl. S5), 1353383. [Google Scholar] [CrossRef] [PubMed]
- Wade, D.; Varker, T.; Kartal, D.; Hetrick, S.; O’Donnell, M.; Forbes, D. Gender difference in outcomes following trauma-focused interventions for posttraumatic stress disorder: Systematic review and meta-analysis. Psychol. Trauma Theory Res. Pract. Policy 2016, 8, 356–364. [Google Scholar] [CrossRef]
- Ney, L.J.; Matthews, A.; Bruno, R.; Felmingham, K.L. Modulation of the endocannabinoid system by sex hormones: Implications for posttraumatic stress disorder. Neurosci. Biobehav. Rev. 2018, 94, 302–320. [Google Scholar] [CrossRef]
- Glover, E.M.; Jovanovic, T.; Norrholm, S.D. Estrogen and Extinction of Fear Memories: Implications for Posttraumatic Stress Disorder Treatment. Biol. Psychiatry 2015, 78, 178–185. [Google Scholar] [CrossRef]
- Nillni, Y.I.; Pineles, S.L.; Patton, S.C.; Rouse, M.H.; Sawyer, A.T.; Rasmusson, A.M. Menstrual cycle effects on psychological symptoms in women with PTSD. J. Trauma. Stress 2015, 28, 1–7. [Google Scholar] [CrossRef]
- Lind, M.J.; Marraccini, M.E.; Sheerin, C.M.; Bountress, K.; Bacanu, S.-A.; Amstadter, A.B.; Nugent, N.R. Association of Posttraumatic Stress Disorder With rs2267735 in the ADCYAP1R1 Gene: A Meta-Analysis. J. Trauma. Stress 2017, 30, 389–398. [Google Scholar] [CrossRef]
- Maddox, S.A.; Kilaru, V.; Shin, J.; Jovanovic, T.; Almli, L.M.; Dias, B.G.; Norrholm, S.D.; Fani, N.; Michopoulos, V.; Ding, Z.; et al. Estrogen-dependent association of HDAC4 with fear in female mice and women with PTSD. Mol. Psychiatry 2018, 23, 658–665. [Google Scholar] [CrossRef]
- Feng, Y.; Su, M.; Si, Y.J.; Guo, Q.W.; Lin, J.; Cao, T.; Zhang, X.; Fan, M.; Fang, D.Z. Longitudinal interplays of estrogen receptor alpha gene rs9340799 with social-environmental factors on post-traumatic stress disorder in Chinese Han adolescents after Wenchuan earthquake. Am. J. Med. Genet. Part B Neuropsychiatr. Genet. Off. Publ. Int. Soc. Psychiatr. Genet. 2018, 177, 337–345. [Google Scholar] [CrossRef]
- Feng, Y.; Lin, J.; Su, M.; Zhang, X.; Fang, D.Z. Interplays of estrogen receptor alpha gene rs2234693 with post-traumatic stress disorder influence serum glucose and lipids profiles in Chinese adolescents. J. Clin. Neurosci. Off. J. Neurosurg. Soc. Australas 2019, 61, 36–43. [Google Scholar] [CrossRef] [PubMed]
- Sartin-Tarm, A.; Ross, M.C.; Privatsky, A.A.; Cisler, J.M. Estradiol Modulates Neural and Behavioral Arousal in Women with Posttraumatic Stress Disorder During a Fear Learning and Extinction Task. Biol. Psychiatry Cogn. Neurosci. Neuroimaging 2020, 5, 1114–1122. [Google Scholar] [PubMed]
- Udo, T.; Grilo, C.M. Prevalence and Correlates of DSM-5-Defined Eating Disorders in a Nationally Representative Sample of U.S. Adults. Biol. Psychiatry 2018, 84, 345–354. [Google Scholar] [CrossRef] [PubMed]
- Culbert, K.M.; Sinclair, E.B.; Hildebrandt, B.A.; Klump, K.L.; Sisk, C.L. Perinatal testosterone contributes to mid-to-post pubertal sex differences in risk for binge eating in male and female rats. J. Abnorm. Psychol. 2018, 127, 239–250. [Google Scholar] [CrossRef]
- Mikhail, M.E.; Culbert, K.M.; Sisk, C.L.; Klump, K.L. Gonadal hormone contributions to individual differences in eating disorder risk. Curr. Opin. Psychiatry 2019, 32, 484–490. [Google Scholar] [CrossRef]
- Asarian, L.; Geary, N. Sex differences in the physiology of eating. Am. J. Physiol. Regul. Integr. Comp. Physiol. 2013, 305, R1215–R1267. [Google Scholar] [CrossRef]
- Klump, K.L.; Fowler, N.; Mayhall, L.; Sisk, C.L.; Culbert, K.M.; Burt, S.A. Estrogen moderates genetic influences on binge eating during puberty: Disruption of normative processes? J. Abnorm. Psychol. 2018, 127, 458–470. [Google Scholar] [CrossRef]
- Lutter, M.; Khan, M.Z.; Satio, K.; Davis, K.C.; Kidder, I.J.; McDaniel, L.; Darbro, B.W.; Pieper, A.A.; Cui, H. The Eating-Disorder Associated HDAC4A778T Mutation Alters Feeding Behaviors in Female Mice. Biol. Psychiatry 2017, 81, 770–777. [Google Scholar] [CrossRef]
- McElroy, S.L.; Guerdjikova, A.I.; Mori, N.; Keck, P.E. Psychopharmacologic treatment of eating disorders: Emerging findings. Curr. Psychiatry Rep. 2015, 17, 35. [Google Scholar] [CrossRef]
- Brady, K.T.; Randall, C.L. Gender differences in substance use disorders. Psychiatr. Clin. N. Am. 1999, 22, 241–252. [Google Scholar] [CrossRef]
- Agabio, R.; Campesi, I.; Pisanu, C.; Gessa, G.L.; Franconi, F. Sex differences in substance use disorders: Focus on side effects. Addict. Biol. 2016, 21, 1030–1042. [Google Scholar] [CrossRef] [PubMed]
- Szabo, G. Women and alcoholic liver disease-warning of a silent danger. Nat. Rev. Gastroenterol. Hepatol. 2018, 15, 253–254. [Google Scholar] [CrossRef] [PubMed]
- Martel, M.M.; Eisenlohr-Moul, T.; Roberts, B. Interactive effects of ovarian steroid hormones on alcohol use and binge drinking across the menstrual cycle. J. Abnorm. Psychol. 2017, 126, 1104–1113. [Google Scholar] [CrossRef] [PubMed]
- Satta, R.; Hilderbrand, E.R.; Lasek, A.W. Ovarian Hormones Contribute to High Levels of Binge-Like Drinking by Female Mice. Alcohol. Clin. Exp. Res. 2018, 42, 286–294. [Google Scholar] [CrossRef]
- Vandegrift, B.J.; Hilderbrand, E.R.; Satta, R.; Tai, R.; He, D.; You, C.; Chen, H.; Xu, P.; Coles, C.; Brodie, M.S.; et al. Estrogen Receptor α Regulates Ethanol Excitation of Ventral Tegmental Area Neurons and Binge Drinking in Female Mice. J. Neurosci. Off. J. Soc. Neurosci. 2020, 40, 5196–5207. [Google Scholar] [CrossRef]
| Prevalence(Male:Female) | Menstrual Cycle Effects | Effects of Menopause | |
|---|---|---|---|
| Schizophrenia | 1.4:1 | ↑ sx in low hormone phase | ↑ sx , ↑ prevalence |
| Bipolar disorder | 1:1 | ↑ sx in low hormone phase | ↑ sx |
| MDD | 1:1.6 | ↑ sx in low hormone phase | ↑ sx , ↑ prevalence |
| ASD | 1:4 | ↑ sx in low hormone phase | ↑ sx |
| ADHD | 1:2 | ↑ sx in low hormone phase | ↑ sx , ↑ prevalence |
| GAD | 2:1 | ↑ sx in low hormone phase | ↑ sx , ↑ prevalence |
| PTSD | 2:1 | ↑ sx in low hormone phase | ↑ prevalence |
| Eating disorder | 3 to 10 times in women | ↑ sx in low hormone phase in bulimia,N/A in anorexia | ↑ sx , ↑ prevalence |
| Substance use disorder | 1:2 | Reinforcing effects of stimulants (Estrogen, ↑;Progesterone, ↓) | ↑ prevalence in alcohol abuse |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Hwang, W.J.; Lee, T.Y.; Kim, N.S.; Kwon, J.S. The Role of Estrogen Receptors and Their Signaling across Psychiatric Disorders. Int. J. Mol. Sci. 2021, 22, 373. https://doi.org/10.3390/ijms22010373
Hwang WJ, Lee TY, Kim NS, Kwon JS. The Role of Estrogen Receptors and Their Signaling across Psychiatric Disorders. International Journal of Molecular Sciences. 2021; 22(1):373. https://doi.org/10.3390/ijms22010373
Chicago/Turabian StyleHwang, Wu Jeong, Tae Young Lee, Nahrie Suk Kim, and Jun Soo Kwon. 2021. "The Role of Estrogen Receptors and Their Signaling across Psychiatric Disorders" International Journal of Molecular Sciences 22, no. 1: 373. https://doi.org/10.3390/ijms22010373
APA StyleHwang, W. J., Lee, T. Y., Kim, N. S., & Kwon, J. S. (2021). The Role of Estrogen Receptors and Their Signaling across Psychiatric Disorders. International Journal of Molecular Sciences, 22(1), 373. https://doi.org/10.3390/ijms22010373





