Timeline of the Development of Skin-Lightening Active Ingredients in Japan
Abstract
1. Development of Skin-Lightening Active Ingredients
1.1. Ascorbic Acid Derivatives
1.2. Placenta Extract
1.3. Kojic Acid
1.4. Hydroquinone Derivatives and Phenolic Compounds
1.5. Natural Compounds Contained in Plants
1.6. Tanexamic Acid, Adenosine Monophosphate and Dexpantenol
2. Report on the Effectiveness of a Formulation Containing a Lightening Agent and a Spot Remedy for Senile Pigmented Lesions
| 10% Magnesium Ascorbyl Phosphate Formulation | 7% Arbutin Formulation | 0.5% Ellagic Acid Formulation | 1% Kojic Acid and 0.1% Oil-Soluble Licorice Extract Formulation | 2% 4-Hydroxyanisole and 0.01% Vitamin A Acid Formulation | |||
|---|---|---|---|---|---|---|---|
| Test design | Open study | Open study | Open study | Open study | Double-blind controlled study | ||
| Number of cases | 17 | 16 | 13 | 18 | 420 | 421 | |
| Sex | – | – | Women | 5 men, 13 women | Men and women | ||
| Age | – | – | Unknown | 28–50 years old (average 39 years old) | 34–85 years old (average 62.6 years old) | ||
| Location | – | – | Unknown | Face | Forearm | Face | |
| Period | – | 3 months to 1 year | 1 to 3 months | 8 and 16 weeks | 24 weeks | Observation up to 48 weeks after 24 weeks of application | |
| Effectiveness judgment | Skin color value (color difference meter) | Visual observation | Visual observation | Close-up photograph determination and skin color value (image analysis) | Visual observation | Visual observation | |
| Effectiveness ratio | Effective (improved or much improved) or higher | 58.80% | 3 months 0%, 6 months 15.4%, 1 year 66.7% | 30.80% | 8 weeks 5.6%, 16 weeks 22.2% | 52.60% | 56.30% |
| Slightly effective (slightly improved) or more | 88.20% | 3 months 81.2%, 6 months 100%, 1 year 100% | 69.20% | 8 weeks 66.7%, 16 weeks 77.8% | 79.30% | 84.10% | |
| Adverse effects | – | None | None | Irritation in a few cases, but no serious adverse effects | Redness 56%, burning 34%, desquamation 24%, itching 16%, irritation 7%, decoloration 9%. | – | |
| References | [4] | [87] | [36] | [26] | [86] | [86] | |
3. Effectiveness Indices of Lightening Ingredients Developed in Japan
| Effectiveness Indices | Skin-Lightening Ingredients | Test Concentration (%) | General Purpose or Japanese Cosmetics Company | Scientific Articles Providing Evidence | |
|---|---|---|---|---|---|
| A | Effectiveness of same concentration of cosmetic formulations on human pigment spots has been published in scientific journals and is highly recommended. | tranexamic acid | 2 | General purpose | [66] |
| arbutin | 3 | General purpose | [31] | ||
| 3-O-ethyl ascorbic acid (vitamin C ethyl) | 1 | General purpose | [8] | ||
| magnesium L-ascorbyl-2-phosphate (APM) | 3 | General purpose | [2] | ||
| ellagic acid | 0.5 | General purpose | [36] | ||
| kojic acid | 2.5, 0.5 | General purpose | [23,24] | ||
| linoleic acid | 0.1 | General purpose | [52] | ||
| 4-n-butyl resorcinol, | 0.3 | General purpose | [37] | ||
| chamomile extract | 0.5 | Kao Corporation | [51] | ||
| adenosine monophosphate | 3 | Otsuka Pharmaceutical Co., Ltd. | [75] | ||
| B | Effectiveness of higher concentrations than those used in cosmetics on human pigment spots has been published in scientific journals and is recommended. | oil-soluble licorice extract containing 50% glabridin | 0.2 | General purpose | [89] |
| niacinamide | 5, 4 | General purpose | [77,78] | ||
| placenta extract | 3 | General purpose | [17] | ||
| retinol | 0.15 | General purpose | [90] | ||
| ascorbic acid 2-O-α-glucoside (AA-2G) | 20 (iontophoresis) | General purpose | [91] | ||
| azelaic acid. | 20 | General purpose | [92] | ||
| C | No effectiveness for human pigment spots has been published in scientific journals and may be considered, but evidence is insufficient | potassium 4-methoxysalicylate | 1, 3 | Shiseido Co. Ltd. | |
| dexpanthenol | POLA ORBIS HOLDINGS INC. | ||||
| D | Not recommended, because of toxicity data published in scientific journals | Rhododenol | 2 | Kanebo Cosmetics Inc. | [46] |
| Magnolignan | 0.5 | Kanebo Cosmetics Inc. | [46] | ||
| ascorbyl tetra-2-hexyldecanoate | Nikko Chemicals Co. Ltd. | [14,15,16] | |||
4. Issues in Methods for Evaluation of Skin-Lightening Effects
5. Future Development of Skin-Lightening Ingredients
6. Conclusions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- General chapter. Functional Cosmetics Marketing Handbook 2019–2020; Fuji Keizai Group Co., Ltd.: Tokyo, Japan, 2019; pp. 7–32. (In Japanese) [Google Scholar]
- Ichikawa, H.; Kawase, H.; Aso, K.; Takeuchi, K. Topical treatment f pigmented dermatoses by modified ascorbic acid. Jpn. J. Clin. Dermatol. 1969, 23, 327–331. (In Japanese) [Google Scholar]
- Tagawa, M.; Murata, T.; Onuma, T.; Kameyama, K.; Sakai, C.; Kondo, S.; Yonemoto, K.; Quigley, J.; Dorsky, A.; Bucks, D.; et al. Inhibitory effects of magnesium ascorbyl phosphate on melanogenesis. SCCJ J. 1993, 27, 409–414. (In Japanese) [Google Scholar]
- Kameyama, K.; Sakai, C.; Kondoh, S.; Yonemoto, K.; Nishiyama, S.; Tagawa, M.; Murata, T.; Ohnuma, T.; Quigley, J.; Dorsky, A.; et al. Inhibitory effect of magnesium L-ascorbyl-2-phosphate (VC-PMG) on melanogenesis in vitro and in vivo. J. Am. Acad. Dermatol. 1996, 34, 29–33. [Google Scholar] [CrossRef]
- Miyai, E.; Yamamoto, I.; Akiyama, J.; Yanagida, M. Inhibitory effect of ascorbic acid 2-O-α-glucoside on the pigmentation of skin by exposure to ultraviolet light. Nishinihon J. Dermatol. 1996, 58, 439–443. (In Japanese) [Google Scholar] [CrossRef]
- Kumano, Y.; Sakamoto, T.; Egawa, M.; Iwai, I.; Tanaka, M.; Yamamoto, I. In vitro and in vivo prolonged biological activities of novel vitamin C derivative, 2-O-α-D-glucopyranosyl-L-ascorbic acid (AA-2G), in cosmetic fields. J. Nutr. Sci. Vitaminol. 1998, 44, 345–359. [Google Scholar] [CrossRef]
- Maeda, K.; Inoue, Y.; Nishikawa, H.; Miki, S.; Urushibata, O.; Miki, T.; Hatao, M. Involvement of melanin monomers in the skin persistent UVA-pigmentation and effectiveness of vitamin C ethyl on UVA-pigmentation. J. Jpn. Cosmet. Sci. Soc. 2003, 27, 257–268. (In Japanese) [Google Scholar]
- Miki, S.; Nishikawa, H. Effectiveness of vitamin C ethyl, Anti-Aging Series 2; N.T.S.: Tokyo, Japan, 2006; pp. 265–278. (In Japanese) [Google Scholar]
- Maeda, K. Action spectrum on UVA irradiation for formation of persistent pigmentation in normal Japanese individuals. Cosmetics 2017, 4, 55. [Google Scholar] [CrossRef]
- Maeda, K.; Hatao, M. Involvement of photo-oxidation of melanogenic precursors in prolonged pigmentation induced by UVA. J. Investig. Dermatol. 2004, 122, 503–509. [Google Scholar] [CrossRef] [PubMed]
- NICNAS. L-Ascorbic acid 3-O-ethyl-(INCI Name: 3-O-ethyl ascorbic acid), Public Report LTD/1879; National Industrial Chemicals Notification and Assessment Scheme (NICAS): Sydney, Australia, 2016; pp. 1–25. [Google Scholar]
- Romita, P.; Foti, C.; Barlusconi, C.; Mercurio, S.; Hansel, K.; Stingeni, L. Allergic contact dermatitis to 3-O-ethyl-L-ascorbic acid: An underrated allergen in cosmetics? Contact Dermat. 2020, 83, 63–64. [Google Scholar] [CrossRef]
- Obayashi, K.; Ochiai, Y.; Masaki, H.; Kurata, Y. Lipid-solble VC derivative ascorbic acid tetra-2-hexyldecanoate (VC-IP) as an anti-aging agent. In Proceedings of the SCSK Conference, Seoul, Korea, 22–24 September 2003; pp. 313–319. [Google Scholar]
- Swinnen, I.; Goossens, A. Allergic contact dermatitis caused by ascorbyl tetraisopalmitate. Contact Dermat. 2011, 64, 241–242. [Google Scholar] [CrossRef] [PubMed]
- Assier, H.; Wolkenstein, P.; Grille, C.; Chosidow, O. Contact dermatitis caused by ascorbyl tetraisopalmitate in a cream used for the management of atopic dermatitis. Contact Dermat. 2014, 71, 60–61. [Google Scholar] [CrossRef]
- Scheman, A.; Fournier, E.; Kerchinsky, L. Allergic contact dermatitis to two eye creams containing tetrahexyldecyl ascorbate. Contact Dermat. 2022, 86, 556–557. [Google Scholar] [CrossRef]
- Shimokawa, Y.; Kamisasanuki, S.; Tashiro, M. Treatment of facial dysmelanosis with cosmetics containing Placen A. Nishinihon J. Dermatol. 1982, 44, 1027–1029. (In Japanese) [Google Scholar]
- Imahara, K.; Ito, Y. Influence of placenta extract on melanin formation. SCCJ J. 1982, 16, 10–14. (In Japanese) [Google Scholar]
- Mallick, S.; Singh, S.K.; Sarkar, C.; Saha, B.; Bahdra, R. Human placental lipid induces melanogenesis by increasing the expression of tyrosinase and its related proteins in vitro. Pigment Cell Res. 2005, 18, 25–33. [Google Scholar] [CrossRef] [PubMed]
- Yamasaki, M.; Hasegawa, S.; Takahashi, H.; Kobayashi, Y.; Sakai, C.; Ashizawa, Y.; Asai, Y.; Kanzaki, M.; Fukui, T. Placental extracts induce the expression of antioxidant enzyme genes and suppress melanogenesis in B16 melanoma cells. Nat. Prod. Res. 2015, 29, 2103–2106. [Google Scholar] [CrossRef] [PubMed]
- Sarkar, C.; Singh, S.K.; Mandal, S.K.; Saha, B.; Bera, R.; Ratha, J.; Datta, P.K.; Bhadra, R. Human placental protein/peptides stimulate melanin synthesis by enhancing tyrosinase gene expression. Mol. Cell Biochem. 2006, 285, 133–142. [Google Scholar] [CrossRef]
- Saha, B.; Singh, S.K.; Sarkar, C.; Mallick, S.; Bera, R.; Bhadra, R. Transcriptional activation of tyrosinase gene by human placental sphingolipid. Glycoconj. J. 2006, 23, 259–268. [Google Scholar] [CrossRef]
- Mishima, Y.; Ohyama, Y.; Shibata, T.; Seto, H.; Hatae, S. Inhibitory action of kojic acid on melanogenesis and its therapeutic effect for various human hyper-pigmentation disorders. Ski. Res. 1994, 36, 134–150. (In Japanese) [Google Scholar]
- Nakayama, H.; Sakurai, M.; Kume, A.; Hanada, S.; Iwanaga, A. The effect of kojic acid application on various facial pigmentary disorders. Nishinihon J. Dermatol. 1994, 56, 1172–1181. (In Japanese) [Google Scholar] [CrossRef]
- Yamamoto, K.; Ebihara, T.; Nakayama, H.; Okubo, A.; Higa, Y. The result of long term use test of kojic acid mixture pharmaceutical. Nishinihon J. Dermatol. 1998, 60, 849–852. (In Japanese) [Google Scholar]
- Harada, T. Clinical evaluation of whitening cream containing kojic acid and oil-soluble licorice extract for senile pigment fleckle on the face. Ski. Res. 2000, 42, 270–275. (In Japanese) [Google Scholar]
- Takizawa, T.; Mitsumori, K.; Tamura, T.; Nasu, M.; Ueda, M.; Imai, T.; Hirose, M. Hepatocellular tumor induction in heterozygous p53-deficient CBA mice by a 26-week dietary administration of kojic acid. Toxicol. Sci. 2003, 73, 287–293. [Google Scholar] [CrossRef]
- Higa, Y.; Kawabe, M.; Nabae, K.; Toda, Y.; Kitamoto, S.; Hara, T.; Tanaka, N.; Kariya, K.; Takahashi, M. Kojic acid-Absence of tumor-initiating activity in rat liver, and of carcinogenic and photo-genotoxic potential in mouse skin. J. Toxicol. Sci. 2007, 32, 143–159. [Google Scholar] [CrossRef]
- Takabatake, M.; Shibutani, M.; Dewa, Y.; Nishimura, J.; Yasuno, H.; Jin, M.; Muguruma, M.; Kono, T.; Mitsumori, K. Concurrent administration of ascorbic acid enhances liver tumor-promoting activity of kojic acid in rats. J. Toxicol. Sci. 2008, 33, 127–140. [Google Scholar] [CrossRef]
- Quasi-Drugs Containing Kojic Acid, Second Meeting of the Pharmaceutical Affairs and Food Sanitation Council in 2005. Ministry of Health, Labour and Welfare, 2 November 2005. Available online: http://www.mhlw.go.jp/shingi/2005/11/dl/s1102-8c.pdf (accessed on 16 July 2022). (In Japanese)
- Sugai, T. Clinical effects of arbutin in patients with chloasma. Ski. Res. 1992, 34, 522–529. (In Japanese) [Google Scholar]
- Akiu, S.; Suzuki, Y.; Asahara, T.; Fujinuma, Y.; Fukuda, M. Inhibitory effect of arbutin on melanogenesis--biochemical study using cultured B16 melanoma cells. Nihon Hifuka Gakkai Zasshi 1991, 101, 609–613. (In Japanese) [Google Scholar]
- Maeda, K.; Fukuda, M. arbutin: Mechanism of its depigmenting action in human melanocyte culture. J. Pharmacol. Exp. Ther. 1996, 276, 765–769. [Google Scholar]
- Kamide, R.; Arase, S.; Takiwaki, H.; Watanabe, S.; Watanabe, Y.; Kageyama, S. Clinical effects of XSC-29 formulation on UV-induced pigmentation. Nishinihon J. Dermatol. 1995, 57, 136–142. (In Japanese) [Google Scholar] [CrossRef]
- Shimogaki, H.; Tanaka, Y.; Tamai, H.; Masuda, M. In vitro and in vivo evaluation of ellagic acid on melanogenesis inhibition. Int. J. Cosmet. Sci. 2000, 22, 291–303. [Google Scholar] [CrossRef]
- Yokoyama, M. Clinical evaluation of the use of whitening cream containing ellagic acid for the treatment of skin pigmentation conditions. Ski. Res. 2001, 43, 286–291. (In Japanese) [Google Scholar]
- Harada, S.; Matsushima, T.; Toda, K.; Takemura, T.; Kawashima, M.; Sugawara, M.; Mizuno, J.; Iijima, M.; Miyakawa, S. Efficacy of rusinol (4-n-butylresorcinol) on chloasma. Nishinihon J. Dermatol. 1999, 61, 813–819. (In Japanese) [Google Scholar] [CrossRef]
- Katagiri, T.; Okubo, T.; Oyobikawa, M.; Futaki, K.; Shaku, M.; Kawai, M.; Takenouchi, M. Inhibitory action of 4-n-butylresorcinol (Rucinol®) on melanogenesis and its skin whitening effects. J. Cosmet. Chem. Jpn. 2001, 35, 42–49. (In Japanese) [Google Scholar] [CrossRef]
- Kim, D.S.; Kim, S.Y.; Park, S.H.; Choi, Y.G.; Kwon, S.B.; Kim, M.K.; Na, J.I.; Youn, S.W. Inhibitory effects of 4-n-butylresorcinol on tyrosinase activity and melanin synthesis. Biol. Pharm. Bull. 2005, 28, 2216–2219. [Google Scholar] [CrossRef]
- Huh, S.Y.; Shin, J.W.; Na, J.I.; Huh, C.H.; Youn, S.W.; Park, K.C. The Efficacy and Safety of 4-n-butylresorcinol 0.1% Cream for the Treatment of Melasma: A Randomized Controlled Split-face Trial. Ann Dermatol. 2010, 22, 21–25. [Google Scholar] [CrossRef]
- Nakamura, K.; Yoshida, M.; Uchiwa, H.; Kawa, Y.; Mizoguchi, M. Down-regulation of melanin synthesis by a biphenyl derivative and its mechanism. Pigment Cell Res. 2003, 16, 494–500. [Google Scholar] [CrossRef]
- Takeda, K.; Yokota, T.; Ikemoto, T.; Kakishima, H.; Matsuo, T. Inhibitory effect of a formuloation containing 0.5% Magnolignan® (5, 5′-dipropyl-biphenyl-2, 2′-diol) on UV-induced skin pigmentation. Nishinihon J. Dermatol. 2006, 68, 288–292. (In Japanese) [Google Scholar] [CrossRef]
- Takeda, K.; Arase, S.; Sagawa, Y.; Shikata, Y.; Okada, H.; Watanabe, S.; Yokota, T.; Ikemoto, T.; Kakishima, H.; Matsuo, T. Clinical evaluation of the topical application of Magnolignan® (5, 5′-dipropyl-biphenyl-2, 2′-diol) for hyperpigmentation on the face. Nishinihon J. Dermatol. 2006, 68, 293–298. (In Japanese) [Google Scholar] [CrossRef]
- Sasaki, M.; Kondo, M.; Sato, K.; Umeda, M.; Kawabata, K.; Takahashi, Y.; Suzuki, T.; Matsunaga, K.; Inoue, S. Rhododendrol, a depigmentation-inducing phenolic compound, exerts melanocyte cytotoxicity via a tyrosinase-dependent mechanism. Pigment. Cell Mmelanoma Res. 2014, 27, 754–763. [Google Scholar] [CrossRef]
- Suzuki, K.; Yagami, A.; Matsunaga, K. Allergic contact dermatitis caused by a skin-lightening agent, 5,5’-dipropylbiphenyl-2,2’-diol. Contact Dermat. 2012, 66, 51–52. [Google Scholar] [CrossRef]
- Gu, L.; Zeng, H.; Takahashi, T.; Maeda, K. In vitro methods for predicting chemical leukoderma caused by quasi-drug cosmetics. Cosmetics 2017, 4, 31. [Google Scholar] [CrossRef]
- Gu, L.; Maeda, K. Metabolism of enantiomers of rhododendrol in human skin homogenate. Metabolites 2022, 12, 412. [Google Scholar] [CrossRef]
- Imokawa, G.; Kobayashi, T.; Miyagishi, M.; Higashi, K.; Yada, Y. The role of endotheln-1 in epidermal hyperpigmentation and signaling mechanisms of mitogenesis and melanogenesis. Pigment Cell Res. 1997, 10, 218–228. [Google Scholar] [CrossRef]
- Ichihashi, M.; Kobayashi, A.; Okuda, M.; Imokawa, G. Effect of chamomilla extracts application on UV-induced pigmentation. Ski. Res. 1999, 41, 475–480. (In Japanese) [Google Scholar]
- Kawashima, M.; Okuda, M.; Kobayashi, A.; Imokawa, G. Inhibitory effect of chamomilla extracts on UV-induced pigmentation. Nishinihon J. Dermatol. 1999, 61, 682–685. (In Japanese) [Google Scholar] [CrossRef]
- Kawashima, M.; Imokawa, G. Mechanism of pigment enhancement in UVB-induced melanosis and lentigo senilis, and anti-spot effect of Chamomile ET. Mon. Book Derma 2005, 98, 43–61. (In Japanese) [Google Scholar]
- Clinical trial group for linoleic acid-containing gel. Clinical trial for liver spots using a linoleic acid-containing gel. Nishinihon J. Dermatol. 1998, 60, 537–542. (In Japanese) [Google Scholar]
- Ando, H.; Ryu, A.; Hashimoto, A.; Oka, M.; Ichihashi, M. Linoleic acid and α-linolenic acid lightens ultraviolet-induced hyperpigmentation of the skin. Arch. Dermatol. Res. 1998, 290, 375–381. [Google Scholar] [CrossRef] [PubMed]
- Shigeta, Y.; Imanaka, H.; Ando, H.; Ryu, A.; Oku, N.; Baba, N.; Makino, T. Skin whitening effect of linoleic acid is enhanced by liposomal formulations. Biol. Pharm. Bull. 2004, 27, 591–594. [Google Scholar] [CrossRef]
- Ando, H.; Watabe, H.; Valencia, J.C.; Yasumoto, K.; Furumura, M.; Funasaka, Y.; Oka, M.; Ichihashi, M.; Hearing, V.J. Fatty acids regulate pigmentation via proteasomal degradation of tyrosinase: A new aspect of ubiquitin-proteasome function. J. Biol. Chem. 2004, 279, 15427–15433. [Google Scholar] [CrossRef]
- Maeda, K.; Naitou, T.; Umishio, K.; Fukuhara, T.; Motoyama, A. A novel melanin inhibitor: Hydroperoxy traxastane-type triterpene from flowers of Arnica montana. Biol. Pharm. Bull. 2007, 30, 873–879. [Google Scholar] [CrossRef][Green Version]
- Dai, L.; Gu, L.; Maeda, K. Inhibitory effect and mechanism of scutellarein on melanogenesis. Cosmetics 2021, 8, 15. [Google Scholar] [CrossRef]
- Maeda, K.; Tomita, Y.; Naganuma, M.; Tagami, H. Phospholipases induce melanogenesis in organ-cultured skin. Photochem. Photobiol. 1996, 64, 220–223. [Google Scholar] [CrossRef] [PubMed]
- Tomita, Y.; Maeda, K.; Tagami, H. Melanocyte-stimulating properties of arachidonic acid metabolites: Possible role in postinflammatory pigmentation. Pigment Cell Res. 1992, 5, 357–361. [Google Scholar] [CrossRef]
- Tomita, Y.; Maeda, K.; Tagami, H. Histamine stimulates normal human melanocytes in vitro: One of the possible inducers of hyperpigmentation in urticaria pigmentosa. J. Dermatol. Sci. 1993, 6, 146–154. [Google Scholar] [CrossRef]
- Maeda, K.; Naganuma, M. Topical trans-4-aminomethylcyclohexanecarboxylic acid prevents ultraviolet radiation-induced pigmentation. J. Photochem. Photobiol. B 1998, 47, 136–141. [Google Scholar] [CrossRef]
- Kawashima, M.; Kawada, A.; Takiwaki, H.; Mizuno, A.; Torii, H.; Hayashi, N.; Nogita, T.; Akiyoshi, E.; Yoshikawa, N.; Watanabe, C.; et al. Clinical efficacy of DH-4243 for Chloasma: A multi-center randomized controlled trial. Rinsho Hifuka 2007, 61, 735–743. (In Japanese) [Google Scholar]
- Na, J.I.; Choi, S.Y.; Yang, S.H.; Choi, H.R.; Kang, H.Y.; Park, K.C. Effect of tranexamic acid on melasma: A clinical trial with histological evaluation. J. Eur. Acad. Dermatol. Venereol. 2013, 27, 1035–1039. [Google Scholar] [CrossRef]
- Lee, H.C.; Thing, T.G.; Goh, C.L. Oral tranexamic acid (TA) in the treatment of melasma: A retrospective analysis. J. Am. Acad. Dermatol. 2016, 75, 385–392. [Google Scholar] [CrossRef]
- Del Rosario, E.; Florez-Pollack, S.; Zapata, L., Jr.; Hernandez, K.; Tovar-Garza, A.; Rodrigues, M. Randomized, placebo-controlled, double-blind study of oral tranexamic acid in the treatment of moderate to severe melasma. J. Am. Acad. Dermatol. 2018, 78, 63–369. [Google Scholar] [CrossRef]
- Kondo, S.; Okada, Y.; Tomita, Y. Clinical study of effect of tranexamic acid emulsion on melasma and freckles. Ski. Res. 2007, 6, 309–315. (In Japanese) [Google Scholar]
- Ebrahimi, B.; Naeini, F.F. Topical tranexamic acid as a promising treatment for melasma. J. Res. Med. Sci. 2014, 19, 753–757. [Google Scholar]
- Banihashemi, M.; Zabolinejad, N.; Jaafari, M.R.; Salehi, M.; Jabari, A. Comparison of therapeutic effects of liposomal tranexamic acid and conventional hydroquinone on melasma. J. Cosmet. Dermatol. 2015, 14, 174–177. [Google Scholar] [CrossRef]
- Na Ayuthaya, P.K.; Niumphradit, N.; Manosroi, A.; Nakakes, A. Topical 5% tranexamic acid for the treatment of melasma in Asians: A double-blind randomized controlled clinical trial. J. Cosmet. Laser Ther. 2012, 14, 150–154. [Google Scholar] [CrossRef]
- Chung, W.C.; Shi, G.Y.; Chow, Y.H.; Chang, L.C.; Hau, J.S.; Lin, M.T.; Jen, C.J.; Wing, L.Y.; Wu, H.L. Human plasmin induces a receptor-mediated arachidonate release coupled with G proteins in endothelial cells. Am. J. Physiol. 1993, 264, C271–C281. [Google Scholar] [CrossRef]
- Kamio, N.; Hashizume, H.; Nakao, S.; Matsushima, K.; Sugiya, H. Plasmin is involved in inflammation via protease-activated receptor-1 activation in human dental pulp. Biochem. Pharmacol. 2008, 75, 1974–1980. [Google Scholar] [CrossRef]
- Wang, N.; Zhang, L.; Miles, L.; Hoover-Plow, J. Plasminogen regulates pro-opiomelanocortin processing. J. Thromb. Haemost. 2004, 2, 785–796. [Google Scholar] [CrossRef]
- Examination Report (1), Cream TX, Examination Report and Summary of Application Materials. Pharmaceuticals and Medical Devices Agency, 16 October 2008. Available online: https://www.pmda.go.jp/quasi_drugs/2009/Q200900001/340109000_22100DZX00896000_Q100_1.pdf (accessed on 28 June 2022). (In Japanese)
- Examination Report (2), Cream TX, Examination Report and Summary of Application Materials. Pharmaceuticals and Medical Devices Agency, 16 October 2008. Available online: https://www.pmda.go.jp/quasi_drugs/2009/Q200900001/340109000_22100DZX00896000_Q101_1.pdf (accessed on 28 June 2022). (In Japanese)
- Kawashima, M.; Mizuno, A.; Murata, Y. Improvement of hyperpigmentation based on accelerated epidermal turnover: Clinical effects of disodium adenosine monophosphate in patients with melasma. Jpn. J. Clin. Dermatol. 2008, 62, 250–257. (In Japanese) [Google Scholar]
- Bissett, D. Topical niacinamide and barrier enhancement. Cutis 2002, 70, 8–12. [Google Scholar]
- Hakozaki, T.; Minwalla, L.; Zhuang, J.; Chhoa, M.; Matsubara, A.; Miyamoto, K.; Greatens, A.; Hillebrand, G.G.; Bissett, D.L.; Boissy, R.E. The effect of niacinamide on reducing cutaneous pigmentation and suppression of melanosome transfer. Br. J. Dermatol. 2002, 147, 20–31. [Google Scholar] [CrossRef]
- Navarrete-Solís, J.; Castanedo-Cázares, J.P.; Torres-Álvarez, B.; Oros-Ovalle, C.; Fuentes-Ahumada, C.; González, F.J.; Martínez-Ramírez, J.D.; Moncada, B. A double-blind, randomized clinical trial of niacinamide 4% versus hydroquinone 4% in the treatment of melasma. Derm. Res. Pract. 2011, 2011, 379173. [Google Scholar] [CrossRef]
- Wohlrab, J.; Kreft, D. Niacinamide-Mechanisms of action and its topical use in dermatology. Ski. Pharmacol. Physiol. 2014, 27, 311–315. [Google Scholar] [CrossRef]
- Proksch, E.; De Bony, R.; Trapp, S.; Boudon, S. Topical use of dexpanthenol: A 70th anniversary article. J. Dermatolog. Treat. 2017, 28, 766–773. [Google Scholar] [CrossRef]
- News release Pola Orbis Holding. 22 April 2019. Available online: http://www.pola-rm.co.jp/pdf/release_20190422.pdf (accessed on 28 June 2022). (In Japanese).
- Olsen, E.A.; Katz, H.I.; Levine, N.; Shupack, J.; Billys, M.M.; Prawer, S.; Gold, J.; Stiller, M.; Lufrano, L.; Thorne, E.G. Tretinoin emollient cream: A new therapy for photodamaged skin. J. Am. Acad. Dermatol. 1992, 26, 215–224. [Google Scholar] [CrossRef]
- Griffiths, C.E.; Finkel, L.J.; Ditre, C.M.; Hamilton, T.A.; Ellis, C.N.; Voorhees, J.J. Topical tretinoin (retinoic acid) improves melasma. A vehicle-controlled, clinical trial. Br. J. Dermatol. 1993, 129, 415–421. [Google Scholar] [CrossRef]
- Griffiths, C.E.; Goldfarb, M.T.; Finkel, L.J.; Roulia, V.; Bonawitz, M.; Hamilton, T.A.; Ellis, C.N.; Voorhees, J.J. Topical tretinoin (retinoic acid) treatment of hyperpigmented lesions associated with photoaging in Chinese and Japanese patients: A vehicle-controlled trial. J. Am. Acad. Dermatol. 1994, 30, 76–84. [Google Scholar] [CrossRef]
- Jarratt, M. Mequinol 2%/tretinoin 0.01% solution: An effective and safe alternative to hydroquinone 3% in the treatment of solar lentigines. Cutis 2004, 74, 319–322. [Google Scholar]
- Fleischer, A.B., Jr.; Schwartzel, E.H.; Colby, S.I.; Altman, D.J. The combination of 2% 4-hydroxyanisole (Mequinol) and 0.01% tretinoin is effective in improving the appearance of solar lentigines and related hyperpigmented lesions in two double-blind multicenter clinical studies. J. Am. Acad. Dermatol. 2000, 42, 459–467. [Google Scholar] [CrossRef]
- Naganuma, M. Whitening cosmetics and its effectiveness in Japan. Ski. Surg. 1999, 8, 2–7. (In Japanese) [Google Scholar]
- Koide, C.; Suzuki, T.; Mizutani, Y.; Hori, K.; Nakajima, A.; Uchiwa, H.; Sasaki, M.; Ifuku, O.; Maeda, K.; Iwabuchi, H.; et al. A questionnaire on pigmented disorders and use of whitening cosmetics in Japanese women. J. Jpn. Cosmet. Sci. Soc. 2006, 30, 306–310. (In Japanese) [Google Scholar]
- Haramoto, I.; Mizoguchi, M. Clinical evaluation of oil-soluble licorice extracts cream on chloasma. Nishinihon J. Dermatol. 1995, 57, 601–608. (In Japanese) [Google Scholar] [CrossRef][Green Version]
- Tucker-Samaras, S.; Zedayko, T.; Cole, C.; Miller, D.; Wallo, W.; Leyden, J.J. A stabilized 0.1% retinol facial moisturizer improves the appearance of photodamaged skin in an eight-week, double-blind, vehicle-controlled study. J. Drugs Dermatol. 2009, 8, 932–936. [Google Scholar] [PubMed]
- Taylor, M.B.; Yanaki, J.S.; Draper, D.O.; Shurtz, J.C.; Coglianese, M. Successful short-term and long-term treatment of melasma and postinflammatory hyperpigmentation using vitamin C with a full-face iontophoresis mask and a mandelic/malic acid skin care regimen. J. Drugs Dermatol. 2013, 12, 45–50. [Google Scholar]
- Verallo-Rowell, V.M.; Verallo, V.; Graupe, K.; Lopez-Villafuerte, L.; Garcia-Lopez, M. Double-blind comparison of azelaic acid and hydroquinone in the treatment of melasma. Acta. Derm. Venereol. Suppl. 1989, 143, 58–61. [Google Scholar]
- Konishi, N.; Kawada, A.; Morimoto, Y.; Watake, A.; Matsuda, H.; Oiso, N.; Kawara, S. New approach to the evaluation of skin color of pigmentary lesions using Skin Tone Color Scale. J. Dermatol. 2007, 34, 441–446. [Google Scholar] [CrossRef]
- De Rigal, J.; Abella, M.L.; Giron, F.; Caisey, L.; Lefebvre, M.A. Development and validation of a new Skin Color Chart. Ski. Res. Technol. 2007, 13, 101–109. [Google Scholar] [CrossRef]
- Takiwaki, H.; Shirai, S.; Kanno, Y.; Watanabe, Y.; Arase, S. Quantification of erythema and pigmentation using a videomicroscope and a computer. Br. J. Dermatol. 1994, 131, 85–92. [Google Scholar] [CrossRef]
- Akimoto, M.; Koshiishi, Y.; Ikeda, H.; Maeda, K.; Hata, M. Skin color measurements: Usefulness of the metric hue angle of uniform color spaces for dermatological treatment. In Proceedings of the Progress in Electromagnetics Research Symposium, Guangzhou, China, 25–28 August 2014; pp. 187–191. [Google Scholar]
- Maeda, K. Analysis of pigmentation and microcirculation of skin by spectral polarization imaging technology. Med. Imaging Technol. 2011, 30, 3–10. (In Japanese) [Google Scholar]
- Ly, B.C.K.; Dyer, E.B.; Feig, J.L.; Chien, A.L.; Del Bino, S. Research Techniques Made Simple: Cutaneous Colorimetry: A Reliable Technique for Objective Skin Color Measurement. J. Investig. Dermatol. 2020, 140, 3–12.e1. [Google Scholar] [CrossRef]
- Ulrich, M.; Lange-Asschenfeldt, S. In vivo confocal microscopy in dermatology: From research to clinical application. J. Biomed. Opt. 2013, 18, 061212. [Google Scholar] [CrossRef]
- Task Force Committee for Evaluation of Whitening Function. Guidelines for evaluation of quasi-drug whitening products for new efficacy claims. J. Jpn. Cosmet. Sci. Soc. 2007, 31 (Suppl. S4), 432–438. (In Japanese) [Google Scholar]
- Maeda, K.; Tomita, Y. In vitro effectiveness of several whitening cosmetic components in human melanocytes. J. Soc. Cosmet. Chem. 1991, 42, 361–368. [Google Scholar]
- Javaheri, S.M.; Handa, S.; Kaur, I.; Kumar, B. Safety and efficacy of glycolic acid facial peel in Indian women with melisma. Int. J. Dermatol. 2001, 40, 354–357. [Google Scholar] [CrossRef]
- Sharquie, K.E.; Al-Tikreety, M.M.; Al-Mashhadani, S.A. Lactic acid as a new therapeutic peeling agent in melisma. Dermatol. Surg. 2005, 31, 149–154. [Google Scholar] [CrossRef]
- Zeng, H.; Harashima, A.; Kato, K.; Gu, L.; Motomura, Y.; Otsuka, R.; Maeda, K. Degradation of tyrosinase by melanosomal pH change and a new mechanism of whitening with propylparaben. Cosmetics 2017, 4, 43. [Google Scholar] [CrossRef]
- Maeda, K. Large melanosome complex is increased in keratinocytes of solar lentigo. Cosmetics 2017, 4, 49. [Google Scholar] [CrossRef]
- Maeda, K. New method of measurement of epidermal turnover in humans. Cosmetics 2017, 4, 47. [Google Scholar] [CrossRef]
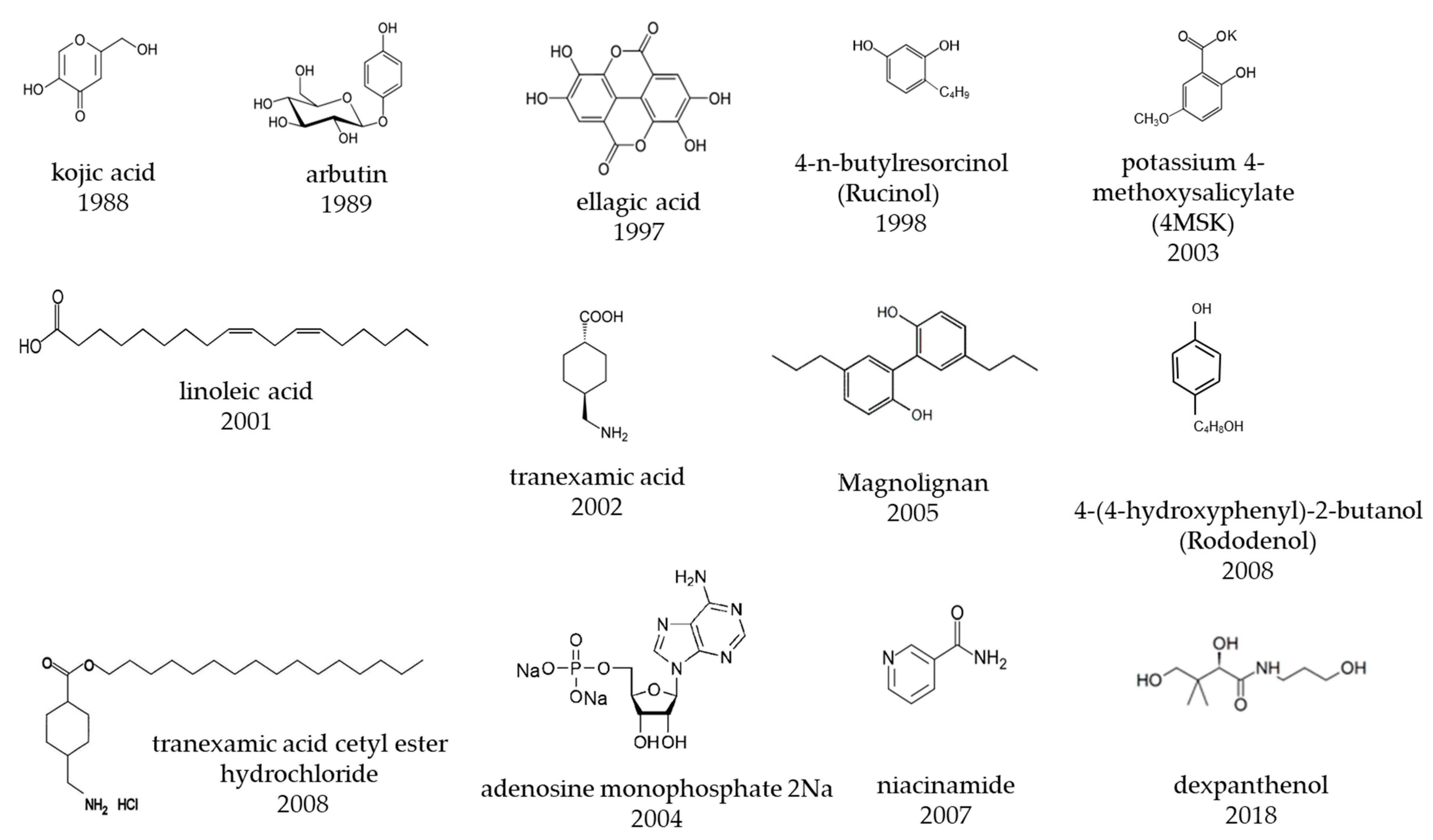
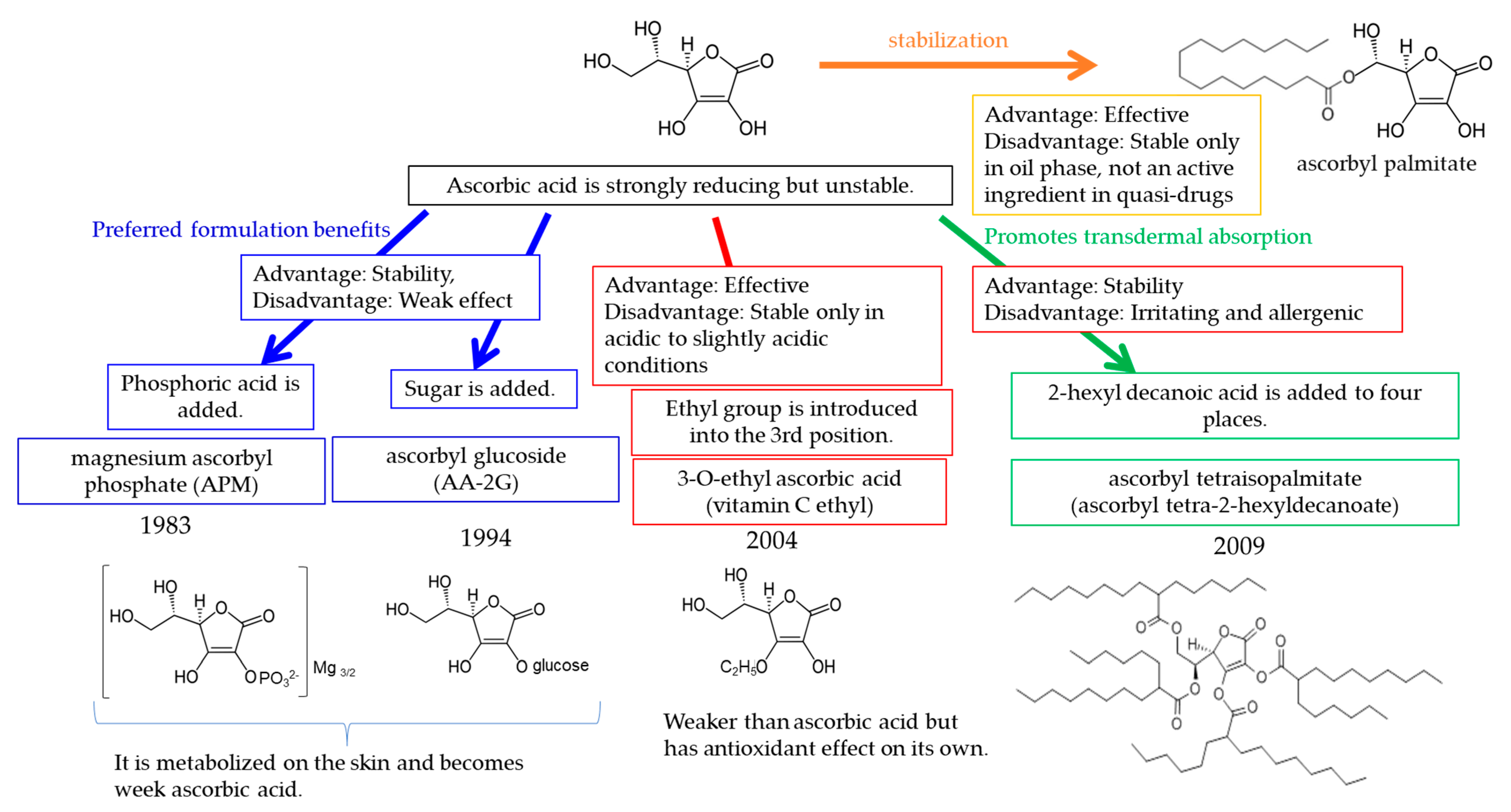

| Approved Year | Generic Name | Development Company | Chemical Name/Substance Name | Main Mechanism of Action |
|---|---|---|---|---|
| placenta extract | ||||
| 1983 | magnesium ascorbyl phosphate (APM) | Takeda Pharmaceutical Co., Ltd. | magnesium L-ascorbyl-2-phosphate | tyrosinase inhibition |
| 1988 | kojic acid | Sansho Seiyaku Co., Ltd. | kojic acid | tyrosinase inhibition |
| 1989 | arbutin | Shiseido Co., Ltd. | hydroquinone-β-D-glucopyranoside | tyrosinase inhibition |
| 1994 | ascorbyl glucoside (AA-2G) | Hayashibara Co., Ltd., Kaminomoto Co., Ltd., Shiseido Co., Ltd. | L- ascorbic acid 2-O-α-glucoside | tyrosinase inhibition |
| 1997 | ellagic acid | Lion Corporation | ellagic acid | tyrosinase inhibition |
| 1998 | Rucinol® | Kurarey Co., Ltd. POLA Chemical industries, Inc. | 4-n-butylresorcinol | tyrosinase inhibition |
| 1999 | Chamomile ET | Kao Corporation | Matricaria chamomilla L Extract | endothelin blocker |
| 2001 | linoleic acid S | Sunstar Inc. | linoleic acid | tyrosinase degradation, stimulation of epidermal turn over |
| 2002 | tranexamic acid (t-AMCHA) | Shiseido Co., Ltd. | trans-4-aminocyclohexane carboxylic acid | inhibition of prostaglandin E2 production by anti-plasmin |
| 2003 | 4MSK | Shiseido Co., Ltd. | potassium 4-methoxysalicylate | tyrosinase inhibition |
| 2004 | Vitamin C ethyl | Nippon Hypox Laboratories, Inc. | 3-O-ethyl ascorbic acid | tyrosinase inhibition |
| 2004 | Energy signal AMP® | Otsuka Pharmaceutical Co., Ltd. | adenosine mono phosphate | stimulation of epidermal turnover |
| 2005 | Magnolignan® | Kanebo Cosmetics Inc. | 5,5-dipropyl-biphenyl-2,2-diol | inhibition of tyrosinase maturation, cytotoxicity to melanocytes |
| 2007 | D-Melano (niacinamide W) | P&G Maxfactor | niacinamide | suppression of melanosome transfer |
| 2008 | Rhododenol® | Kanebo Cosmetics Inc. | 4-(4-hydroxyphenyl)-2-butanol, Rhododendrol | tyrosinase inhibition, cytotoxicity of melanocytes |
| 2008 | TXC | CHANEL | tranexamic acid cetyl ester hydrochloride | inhibition of prostaglandin E2 production |
| 2009 | ascorbyl tetraisopalmitate | Nikko Chemicals Co., Ltd. | ascorbyl tetra-2-hexyldecanoate | tyrosinase inhibition |
| 2018 | dexpanthenol W (PCE–DP) | POLA ORBIS Holdings Inc. | dexpanthenol | enhance energy production of epidermal cells |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the author. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Maeda, K. Timeline of the Development of Skin-Lightening Active Ingredients in Japan. Molecules 2022, 27, 4774. https://doi.org/10.3390/molecules27154774
Maeda K. Timeline of the Development of Skin-Lightening Active Ingredients in Japan. Molecules. 2022; 27(15):4774. https://doi.org/10.3390/molecules27154774
Chicago/Turabian StyleMaeda, Kazuhisa. 2022. "Timeline of the Development of Skin-Lightening Active Ingredients in Japan" Molecules 27, no. 15: 4774. https://doi.org/10.3390/molecules27154774
APA StyleMaeda, K. (2022). Timeline of the Development of Skin-Lightening Active Ingredients in Japan. Molecules, 27(15), 4774. https://doi.org/10.3390/molecules27154774






